What is aphthous ulcer
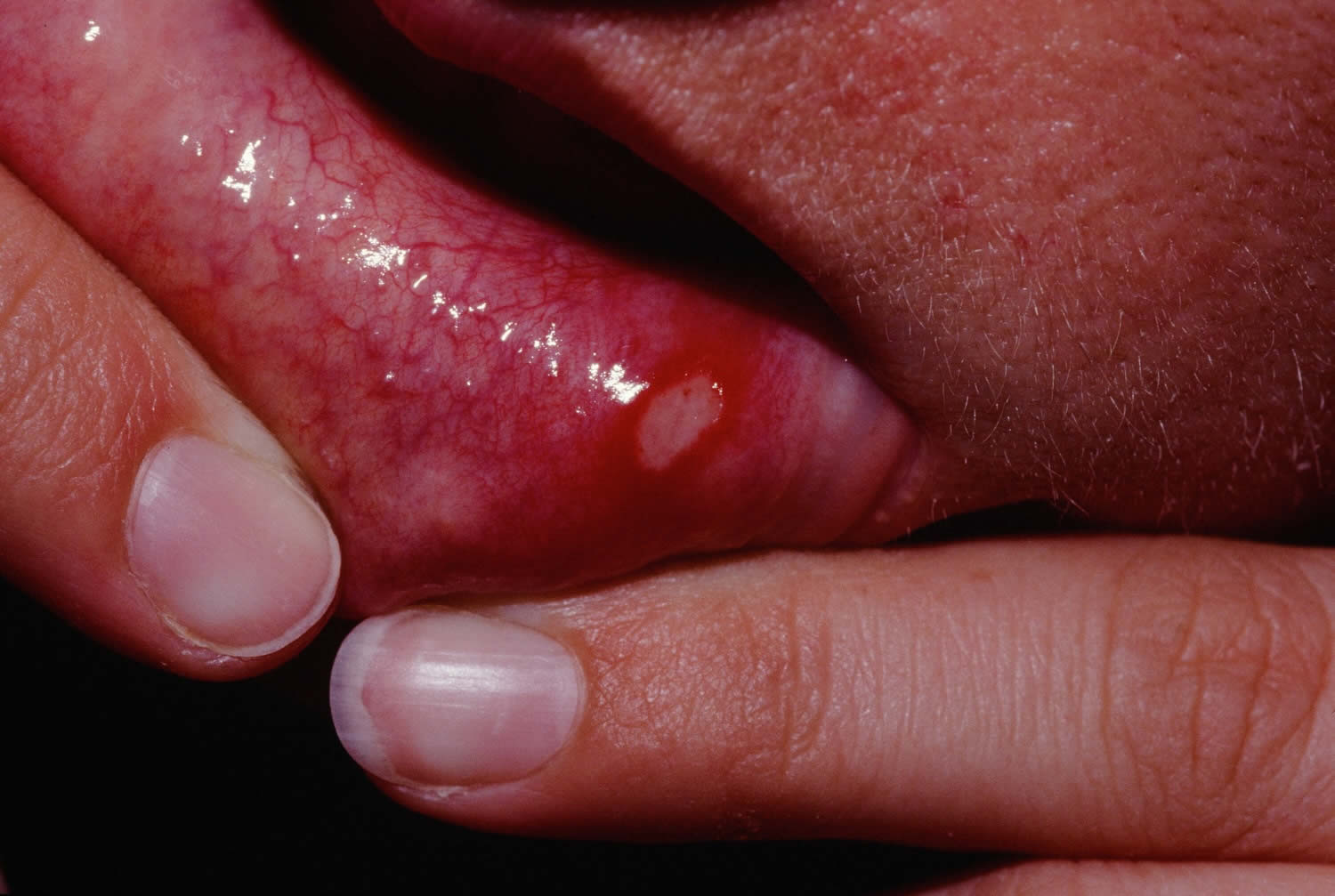
An aphthous ulcer is a painful superficial oral ulcer that forms on the mucous membranes. Aphthous ulcers are also called aphthae, aphthosis, aphthous stomatitis and canker sores. Aphthous stomatitis often come in crops. Trauma may induce them. The majority of cases arise spontaneously with unknown cause. An aphthous ulcer is typically a recurrent round or oval sore or ulcer inside the mouth on an area where the skin is not tightly bound to the underlying bone, such as on the inside of the lips and cheeks or underneath the tongue. Aphthous ulcers can also affect the genitalia in males and females.
Recurrent aphthous ulcers are mostly a minor nuisance, but they are associated with significant health problems in some people. Some have suggested that recurrent aphthous stomatitis may have an immunogenetic background owing to cross-reactivity with Streptococcus sanguis. Recurrent aphthous stomatitis typically has its onset in from 10-30 years of age. A small percentage of patients have a hematinic deficiency (e.g., iron, folate, vitamin B-12) 1. Case reports of isolated causes include zinc deficiency and fluoride allergy.
Anyone can get an aphthous ulcer; 20% of the population have one or more, at least occasionally. They usually first appear in childhood or adolescence, and more commonly affect females than males.
Aphthous ulcer triggers
Many triggers have been reported including spicy foods, citrus, walnuts, pineapple, trauma (e.g., from the toothebrush, self-biting, dental procedures), menstruation, pregnancy, menopause and stress.
Aphthous ulcer is classified into three types:
- Recurrent minor aphthous ulcer (80%). This is less than 5 mm in diameter and heals within 1–2 weeks.
- Major aphthous ulcer, which is large (often more than 10 mm) and takes weeks or months to heal and leaves a scar.
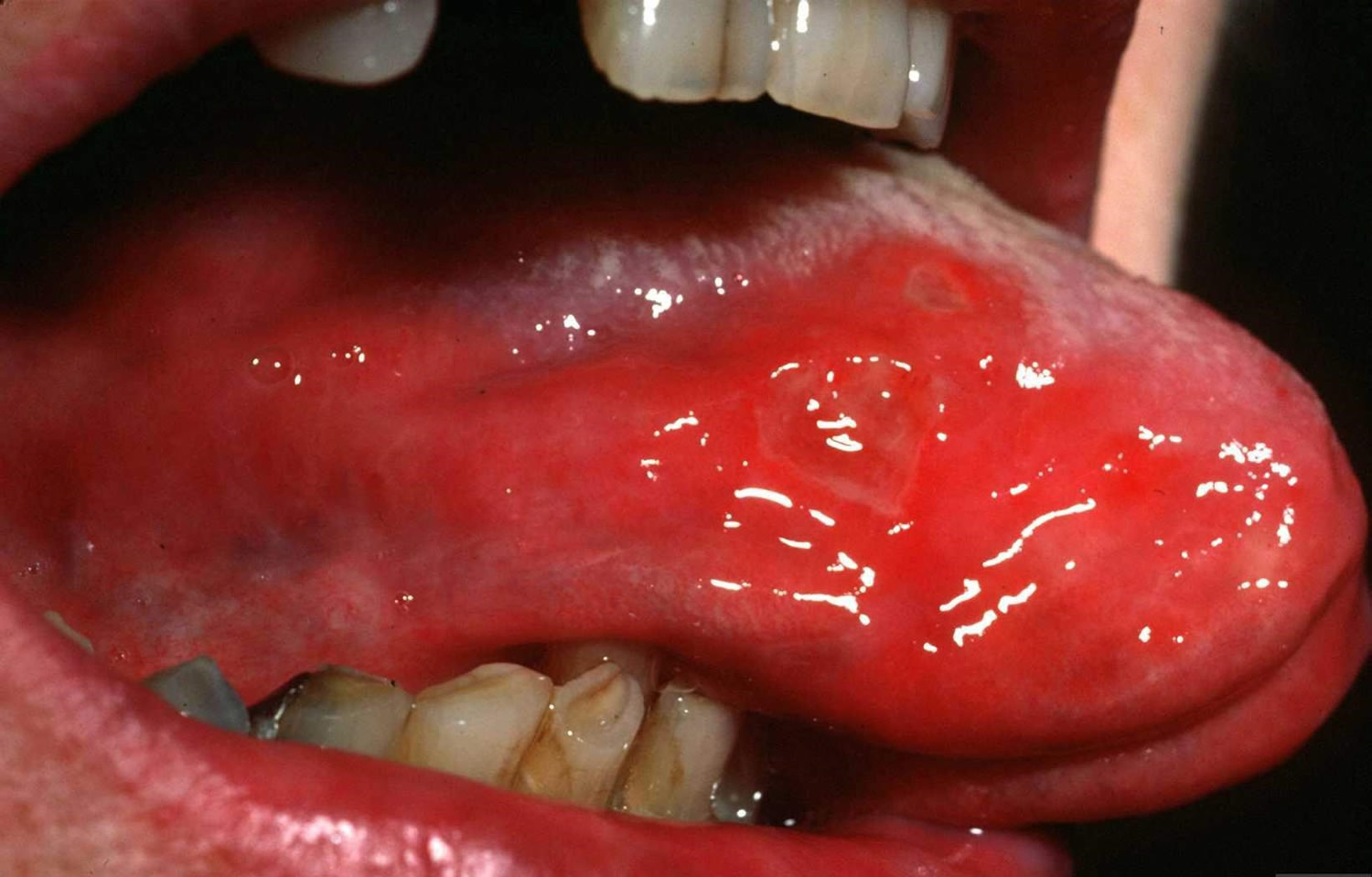
- Herpetiform ulcers, which are multiple pinpoint ulcers that heal within a month. These are most commonly on the tongue.
There is no cure for aphthous ulcer. Most recurrent minor aphthous ulcers heal within 1–2 weeks without any treatment. The main goal of treatment is to lessen pain and discomfort, and promote healing.
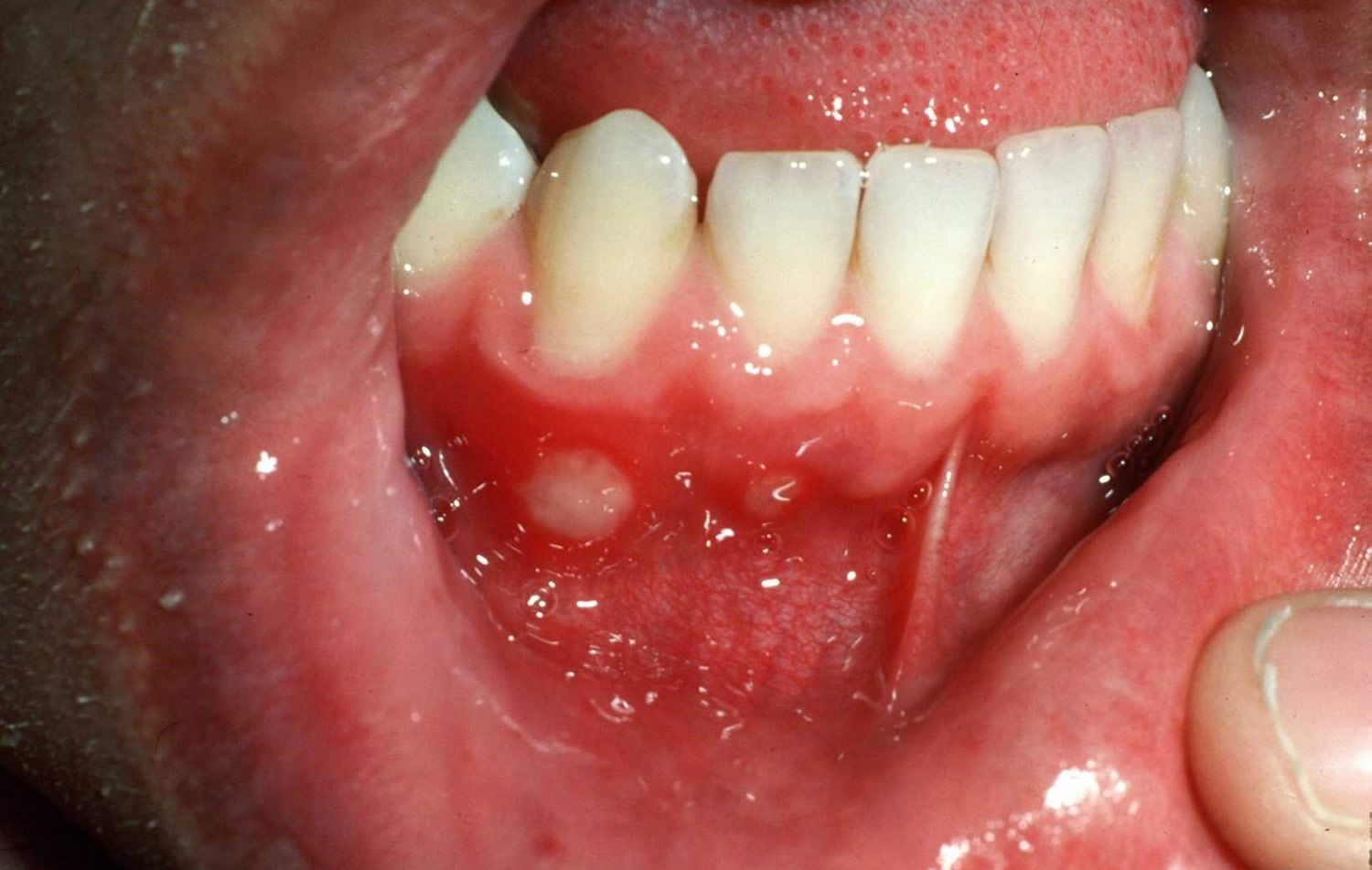
Figure 1. Aphthous stomatitis
Figure 2. Aphthous ulcer tongue
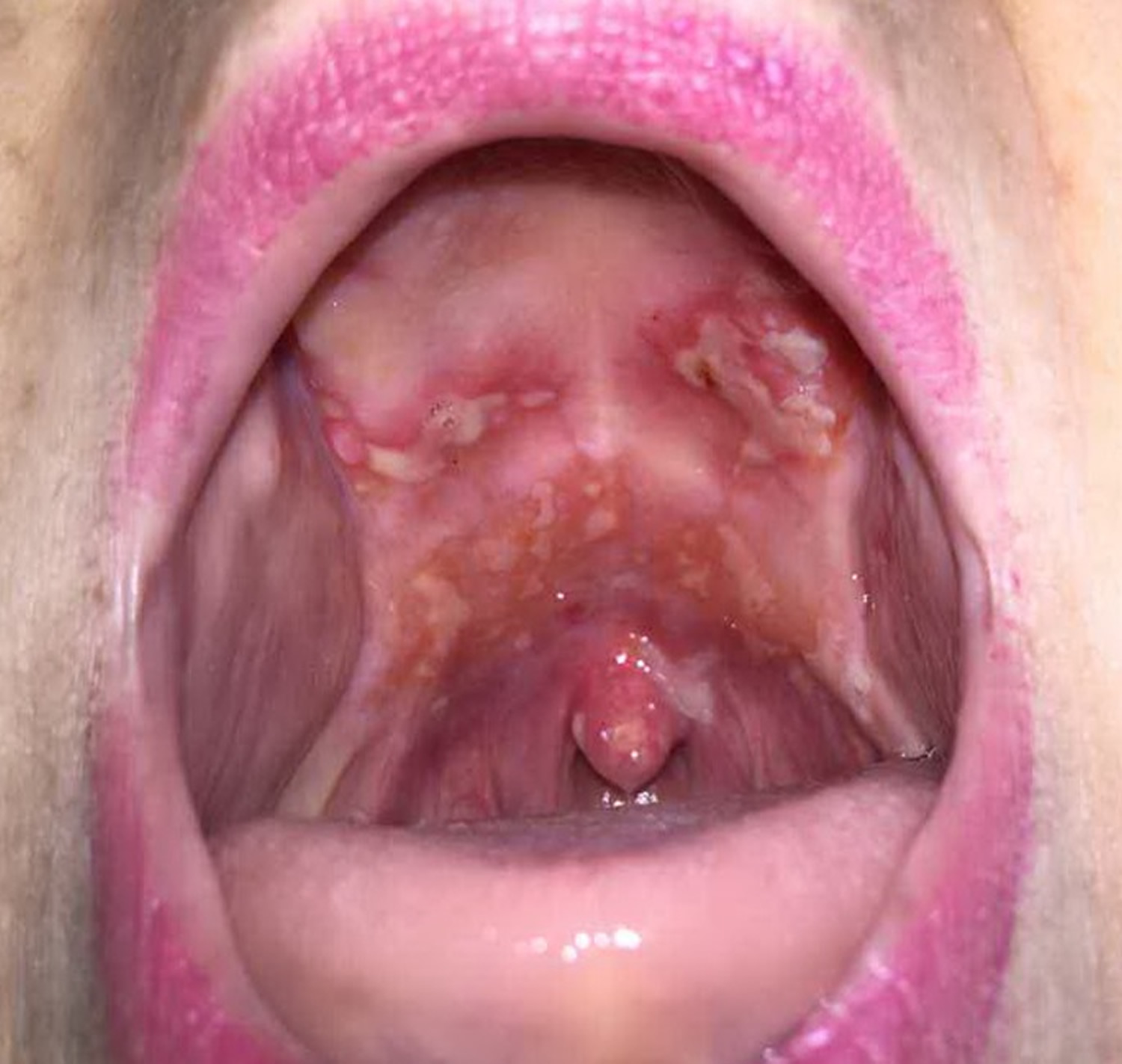
Figure 3. Major aphthous stomatitis
Aphthous ulcer signs and symptoms
Aphthous ulcers appear as white or gray oval areas with a bright red surrounding erythema in the oral cavity. Aphthous ulcers most commonly occur on the buccal and labial mucosa.
People may experience a single ulcer or multiple ulcers. Multiple ulcers tend to be widely distributed throughout a person’s mouth.
Occasionally, patients may have a more severe presentation with larger or more persistent lesions. The term major aphthous stomatitis has been used and is defined as ulcers greater than 1 cm that are present for more than two weeks and often heal with scarring.
Recurrent aphthous ulcer usually begins as a round yellowish elevated spot surrounded by a red halo. This then breaks down into a punched-out ulcer, which is covered with a loosely attached white, yellow or greyish membrane. Surrounding tissue is healthy and unaffected. The ulcer can be painful, particularly if irritated by movement or eating certain types of food such as citrus fruit.
Aphthous ulcer causes
The exact reason why aphthous ulcer develops is not yet clearly defined. Approximately 40% of people who get aphthous ulcers have a family history of aphthous ulcer. Current thinking is that the immune system is disturbed by some external factor and reacts abnormally against a protein in mucosal tissue.
When aphthous ulcer occur in children, PFAPA syndrome (periodic fever, aphthous stomatitis, pharyngitis and cervical adenitis syndrome) should be considered (high fever and aphthous ulcer occurring every 4 weeks).
Factors that seem to trigger outbreaks of aphthous ulcers include:
- Emotional stress and lack of sleep
- Mechanical trauma, for example self-inflicted bite
- Nutritional deficiency, particularly of vitamin B, iron, and/or folic acid
- Certain foods, including chocolate
- Certain toothpastes; this may relate to sodium laureth sulfate (the foaming component of toothpaste)
- Menstruation
- Certain medications, including nicorandil, given for angina
- Viral infections.
Other causes of mouth ulcer should also be considered, including:
- Herpes simplex
- Herpangina
- Erythema multiforme
- Fixed drug eruption.
What tests should be done in aphthous ulcer?
Most people affected by occasional minor aphthous ulceration do not require tests. Blood tests are undertaken if there are recurrent attacks of multiple or severe oral aphthous ulcers, or complex aphthosis.
Blood work for HIV, iron, zinc, folate and vitamin B12 may be measured. The history may be reviewed for inflammatory bowel disease or any signs of other skin problems, e.g. vasculitis, genital ulcerations (Behcets Syndrome).
Blood tests may include:
- Blood count, iron, vitamin B12, zinc and folate studies
- Blood work for HIV
- Gluten antibody tests for celiac disease
- Fecal calprotectin test for Crohn’s disease
Swabs for microbiology evaluate the presence of Candida albicans, Herpes simplex virus and Vincent’s organisms.
Aphthous ulcer treatment
There is no cure for aphthous ulcer. Most recurrent minor aphthous ulcers heal within 1–2 weeks without any treatment. The main goal of treatment is to lessen pain and discomfort, and promote healing.
General measures:
- Protective pastes that form a barrier over the ulcer so that exposure to irritating substances is reduced.
- Superficial tissue cauterization using silver nitrate stick
- Local anaesthetics benzocaine and lignocaine (lidocaine) to reduce pain
- Medicated toothpaste without sodium laureth sulfate
- Antibacterial mouthwashes to reduce secondary infection.
- Avoidance of foods that trigger or exacerbate the ulcers.
- Dietary supplements of vitamins or minerals, if diet is deficient.
- Reduction in stress
- Gentle dental care, e.g., use soft toothbrush
- Vitamin B12, e.g., 1000 mcg sublingual nightly
- Amlexanox
- Magic Mouthwash
Aphthous stomatitis medications
Topical prescription medicines include:
- Tetracycline suspension as mouthwash
- Topical corticosteroids as lotions, creams or paste, often triamcinolone in dental paste
- Calcineurin inhibitors: topical pimecrolimus or tacrolimus.
In severe cases, particularly if there are systemic symptoms, anti-inflammatory oral medications may be considered (off-label use):
- Tetracycline, e.g. doxycycline 50-100mg daily for 3-6 months or longer.
- Dapsone
- Colchicine
- Potent topical steroids (and even intralesional) along with:
- Colchicine
- Dapsone
- Combination colchicine and dapsone
- Apremilast
- Oral prednisone short course
- Immunosuppressive agents such as azathioprine, methotrexate, ciclosporin
- Tumor necrosis factor (TNF) antagonists (adalimumab, etanercept, infliximab)
- Thalidomide (e.g. 50-100 mg at bedtime).
Vitamin B12
Vitamin B12 (cobalamin) has been reported effective in several studies for recurrent aphthous stomatitis. It may be taken the standard way as a pill that is swallowed. However, because of concerns about gut absorption, multiple other delivery methods are available including a sublingual tablet (e.g., 1000 mcg/day), lozenge or oral spray, intranasal spray, and by prescription as a subcutaneous weekly injection. In one double blind placebo controlled clinical trial of one sublingual vitamin B12 tablet (1000 mcg of vitamin B12) at bedtime, there was a significant reduction of the number of lesions at 6 months, 74.1% vs 32.0% “aphthous ulcer free” for one month 2. This intervention was beneficial regardless of the Vitamin B level. In one double blind placebo controlled clinical trial, topical vitamin B12 greatly reduced pain compared to placebo after 2 days 3.
Topical Steroids
What follows is off label and the patient should be informed as such and they must accept that this is “experimental”. A high-potency topical steroid (e.g., clobetasol ointment) may be applied 3-5 times per day directly to the ulcer. The patient should massage the steroid into the ulcer for 30-60 seconds and then not eat or drink for 30 minutes. There is an increased risk of Candida and the patient should be monitored. If the patient finds it hard to keep the topical steroid on the lesion, applying the steroid to a gauze and applying to the lesion for ten minutes several times a day may be done. Alternatively, Kenalog in Orobase applied every night at bedtime and every morning may be tried. Other options include applying a steroid pill directly onto the ulcer and allowing it to dissolve; spraying an asthma steroid inhaler directly onto the ulcer; gargle with tacrolimus solution for 30 seconds and spit; do the same with cyclosporin oral solution; or 5 drops of clobetasol solution in a capful of over-the-counter Biotene oral rinse, swish 3-5 minutes, then spit.
Oral Steroids
A short course of prednisone e.g., 40 mg/day x 4 days can rapidly heal ulcers.
Antibiotics
50 mg penicillin G potassium troches (Cankercillin) speeded healing time in a double blind placebo controlled clinical trial 4. Alternatively, the contents of a 250 mg capsule of tetracycline mixed in water, swished and held in the mouth for 2-3 minutes three times a day may be tried. In one double blind placebo controlled clinical trial 5, the contents of a single crushed doxycycline tablet was applied with denture adhesive and a few drops of saline directly to the ulcer(s). Just one application sped healing and reduced pain.
Magic Mouthwash
The Magic Mouthwash can be quite soothing of any oral ulcerations. Various recipes exist. Key ingredients include Maalox, viscous lidocaine, diphenhydramine elixir and dexamethasone. In the case of aphthous ulcers, the contents of tetracycline or doxycycline capsules may be added.
Miscellaneous
Apremilast cleared one patient with recalcitrant disease completely after 6 weeks 6.
Good oral hygiene and the use of a low allergenic over-the-counter toothpaste has been recommended.
One patient noted with certainty that sweets (e.g., chocolate, cookies) in the diet were positively correlated with outbreaks. Avoiding sweets nearly prevented outbreaks.
Thalidomide is the treatment of choice for severe disease. It may be given at a dose of 100-200 mg/day and 2-3 months may be needed to see an effect. Others start at 300 mg/day. Once controlled, the thalidomide may be tapered to alternate day to every third day dosage as possible. Alternative oral medications that have been tried include azathioprine, cyclosporin, colchicine, pentoxifylline and dapsone.
A double blind placebo controlled clinical trial of a multivitamin as treatment to prevent recurrent aphthous ulcers did not show any benefit 7.
References