What is arcus senilis
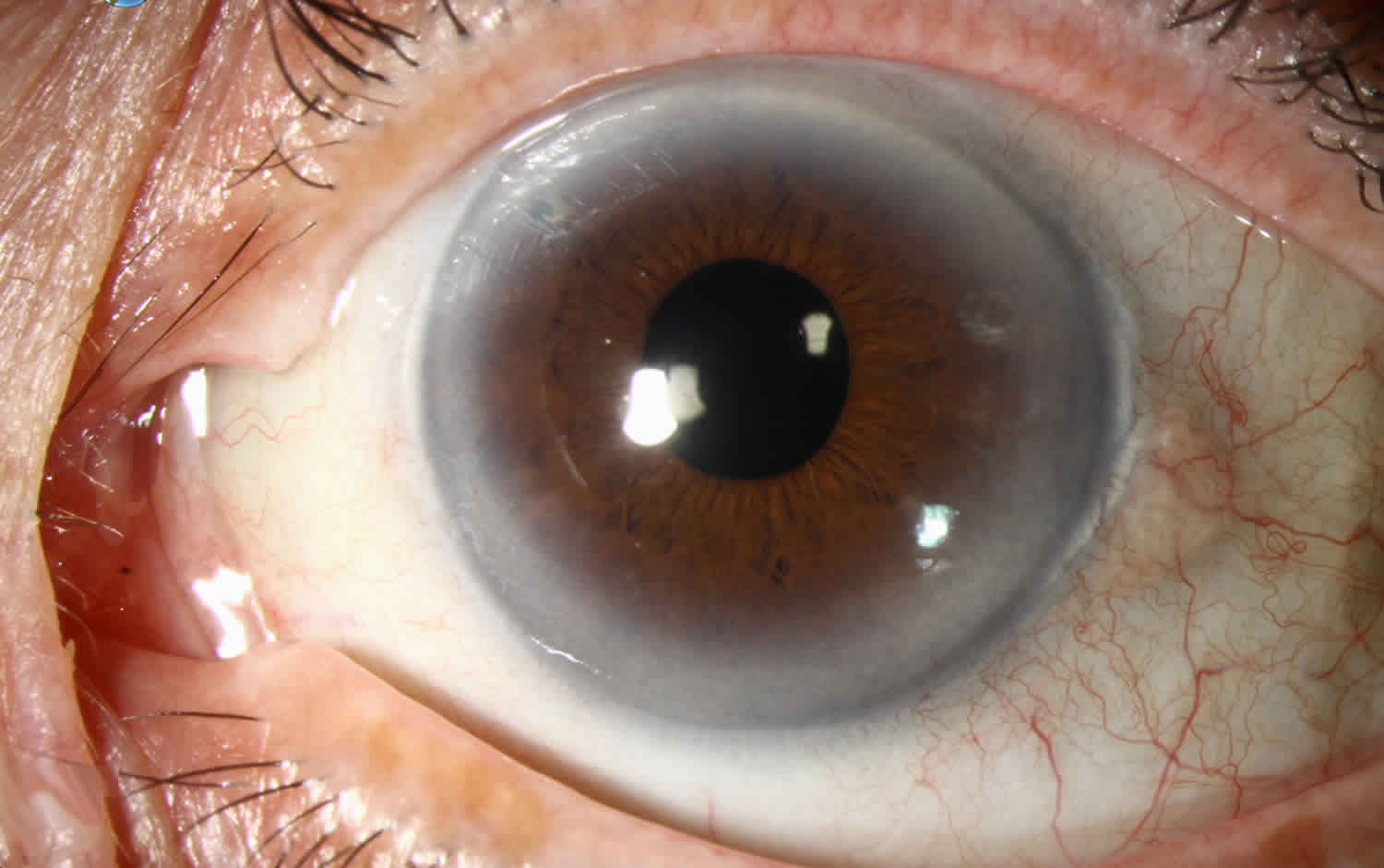
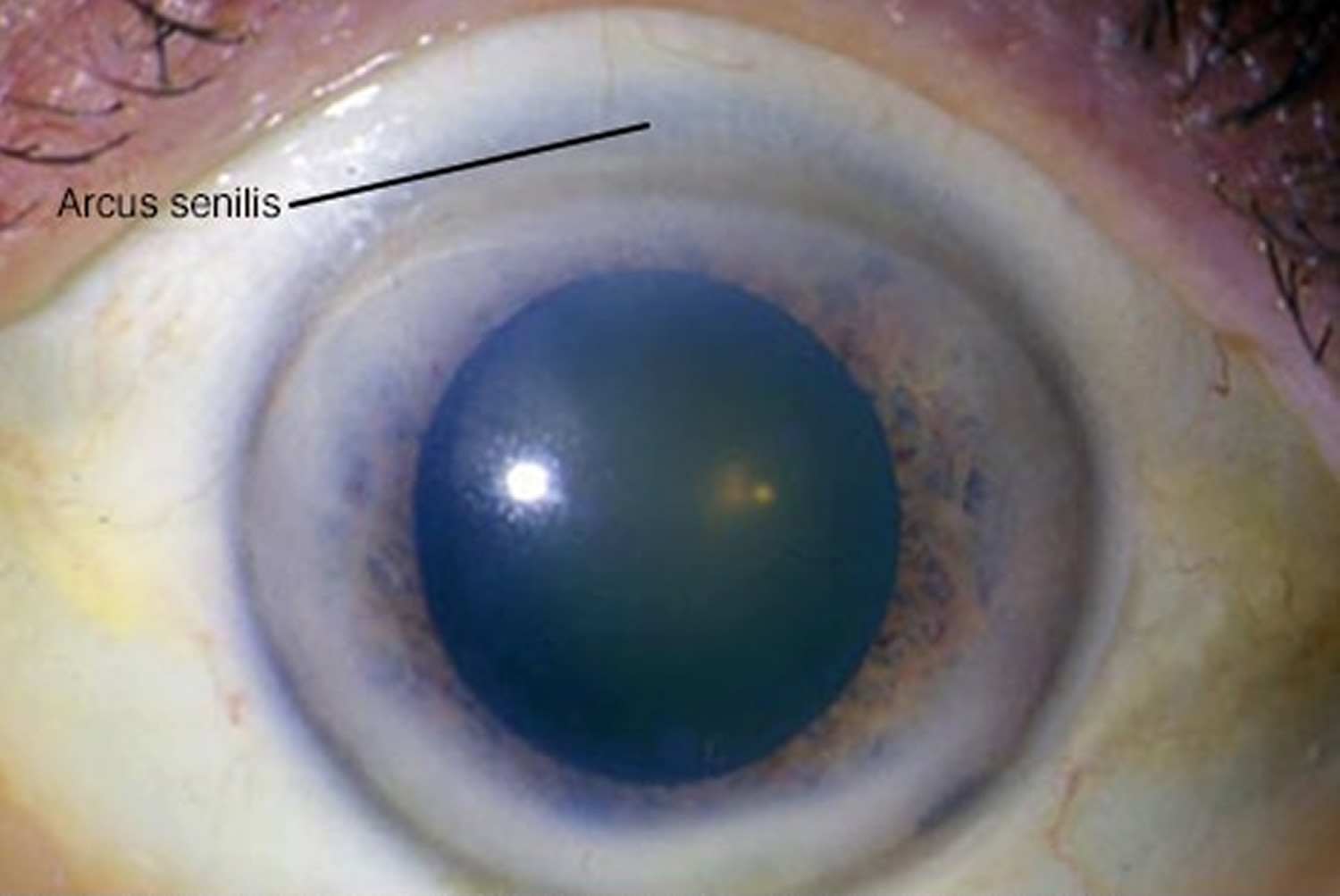
Arcus senilis is a gray or white arc or ring like opacity around the outer part of the cornea (the corneal limbus) in many older adults formed from lipid deposition 1. Arcus senilis is also known as gerontoxon, arcus lipoides, arcus cornae, or corneal arcus, is a deposition of lipid in the peripheal cornel stroma. Arcus senilis is the most common peripheral corneal opacity. Arcus senilis typically begins above and below and eventually encircling the entire corneal circumference 2. Arcus senilis can be associated with hyperlipidemia, especially in elderly individuals, and may be associated with dyslipidemia in younger patients (termed arcus juvenilis) 3. Arcus senilis overall has a good prognosis with little to no effect on visual acuity and ocular health.
Figure 1. Arcus senilis
Arcus senilis causes
The cause of arcus senilis is not entirely known though it has been linked to hyperlipidemia and dyslipidemia.
Arcus senilis is associated with older age, male gender, smoking, systolic hypertension 4, African American heritage 5, and increased fasting serum triglyceride 6. Due to arcus senilis association with hyperlipidemia, arcus senilis is particularly common in people with familial hypercholesterolemia and xanthelasma 7.
Despite the risk factors of hyperlipidemia and dyslipidemia, there have been conflicting studies with regards to the association of arcus senilis with cardiovascular disease. In a population-based cross-sectional study in 2011 of 3397 ethnic Indians aged 40 to 80 in Singapore, presence of arcus senilis was associated with cardiovascular disease independent of the risk factors in the paragraph above 8. However, a prospective cohort study of 12,745 Danes followed up for a mean of 22 years found that arcus senilis had no clinical value as a predictor of cardiovascular disease 9. In a third study of 3,930 white men and 2,139 women non-hormone users, ages 30-69, followed for an average of 8.4 years as part of the Lipid Research Clinics Mortality Follow-up Study, arcus senilis was associated with coronary heart disease (coronary artery disease) and cardiovascular disease mortality only in hyperlipidemic men ages 30-49 years 10.
Arcus senilis is due to a deposition of lipid in the peripheral cornea and is generally considered a normal aging process and expected in the elderly patient. It is believed that increased permeability of limbal vessels with age allows for low-density lipoproteins to pass through the cornea, which may explain why it is found in > 70% of patients over the age of 60 6. Tissue necrosis and atrophy are not present with this anomaly 10. There is no increase in cellularity, fragmentation of the laminae, phagocytosis, unusual vascularity, nor any difference in lipogenesis on histological examination 11.
The lipid in arcus senilis is found to be concentrated mainly in two layers of the peripheral cornea: Descemet membrane and Bowman layer, with more deposition in the former 10. Lipid deposition may not be confined to the cornea, and may be found in the ciliary body, ciliary processes, and iris as well 12.
Arcus senilis prevention
Primary prevention of arcus senilis would be directed towards management of hyperlipidemia and dyslipidemia, the main risk factor for development of arcus senilis.
Arcus senilis signs and symptoms
Arcus senilis is usually an incidental finding on exam, as the ring itself is beyond the visual axis and therefore usually asymptomatic. Family members or friends may note a whitish or bluish looking ring-like opacity in the peripheral cornea by the limbus.
Arcus senilis diagnosis
Diagnosis of arcus senilis is clinically made. Gross examination or a slit lamp examination are all that is needed to diagnosis arcus senilis. There are no lab tests or imaging to be performed to determine a diagnosis. However a lipid panel can help identify risk factors. Lab abnormalities associated with arcus senilis include elevated fasting serum triglyceride levels, total cholesterol and low density lipoprotein 13.
Physical examination
Stromal lipid initially deposits in the superior and inferior perilimbal cornea, progressing circumferentially to form a mat-white or yellow-white band about 1 mm wide. The band is usually wider in the vertical than the horizontal meridian. The central border is diffuse and the peripheral edge is sharp and separated from the limbus by a clear interval that may undergo mild thinning 7.
Rarely, arcus senilis may contain scintillating crystals or “crystalloid” edges which are characteristic of many lipid keratopathies. Though, these opacities are not regularly fluorescent on exam 11.
Certain changes in the biomechanical properties of the cornea have been noted to be different when arcus senilis is present. One study found that corneal hysteresis and corneal resistance factor values of eyes with arcus senilis were lower when compared with age-matched controls, but there were no differences in other parameters, such as intraocular pressure, central corneal thickness, spherical equivalent value of the refractive error, axial length measurements, and mean keratometry 14.
Arcus senilis treatment
As arcus senilis is asymptomatic, no treatment is necessary. Patients can be followed at yearly intervals as would be expected for follow up in a patient with a normal eye exam. There is no specific management necessary.
Prognosis is generally good in terms of vision and ocular health.
References- Arcus senilis. https://eyewiki.org/Arcus_Senilis
- Corneal arcus (arcus senilis). https://webeye.ophth.uiowa.edu/eyeforum/atlas/pages/Arcus/index.htm
- Kanski, J. J. & Bowling, B. Clinical Ophthalmology: A Systematic Approach. Elsevier Health Sciences, 2011.
- Hashemi, H., Khabazkhoob, M., Emamian, M. H., Shariati, M. & Fotouhi, A. A population-based study of corneal arcus and its risk factors in Iran. Ophthalmic Epidemiol. 21, 339–344, 2014.
- Patterson, L. Arcus senilis. Am. J. Forensic Med. Pathol. 3, 115–118, 1982.
- Raj, K. M., Reddy, P. A. S. & Kumar, V. C. Significance of corneal arcus. J. Pharm. Bioallied Sci. 7, S14–5, 2015
- Kanski, J. J. & Bowling, B. Clinical Ophthalmology: A Systematic Approach. Elsevier Health Sciences, 2011
- Ang, M. et al. Corneal Arcus is a Sign of Cardiovascular Disease, Even in Low-Risk Persons. Am. J. Ophthalmol. 152, 864–871.e1, 2011
- Chambless, L. E. et al. The association of corneal arcus with coronary heart disease and cardiovascular disease mortality in the Lipid Research Clinics Mortality Follow-up Study. Am. J. Public Health 80, 1200–1204, 1990
- Walton, K. W. & Dunkerley, D. J. Studies on the pathogenesis of corneal arcus formation II. Immunofluorescent studies on lipid deposition in the eye of the lipid-fed rabbit. J. Pathol. 114, 217–229, 1974.
- Patterson, L. Arcus senilis. Am. J. Forensic Med. Pathol. 3, 115–118, 1982
- Walton, K. W. & Dunkerley, D. J. Studies on the pathogenesis of corneal arcus formation II. Immunofluorescent studies on lipid deposition in the eye of the lipid-fed rabbit. J. Pathol. 114, 217–229, 1974
- Macchiaiolo, M. et al. Corneal arcus as first sign of familial hypercholesterolemia. J. Pediatr. 164, 670, 2014
- Ayhan, Z., Ozturk, T., Kaya, M., Arikan, G. & Gunenc, U. Corneal Biomechanical Properties in Patients With Arcus Senilis. Cornea 35, 980–982, 2016