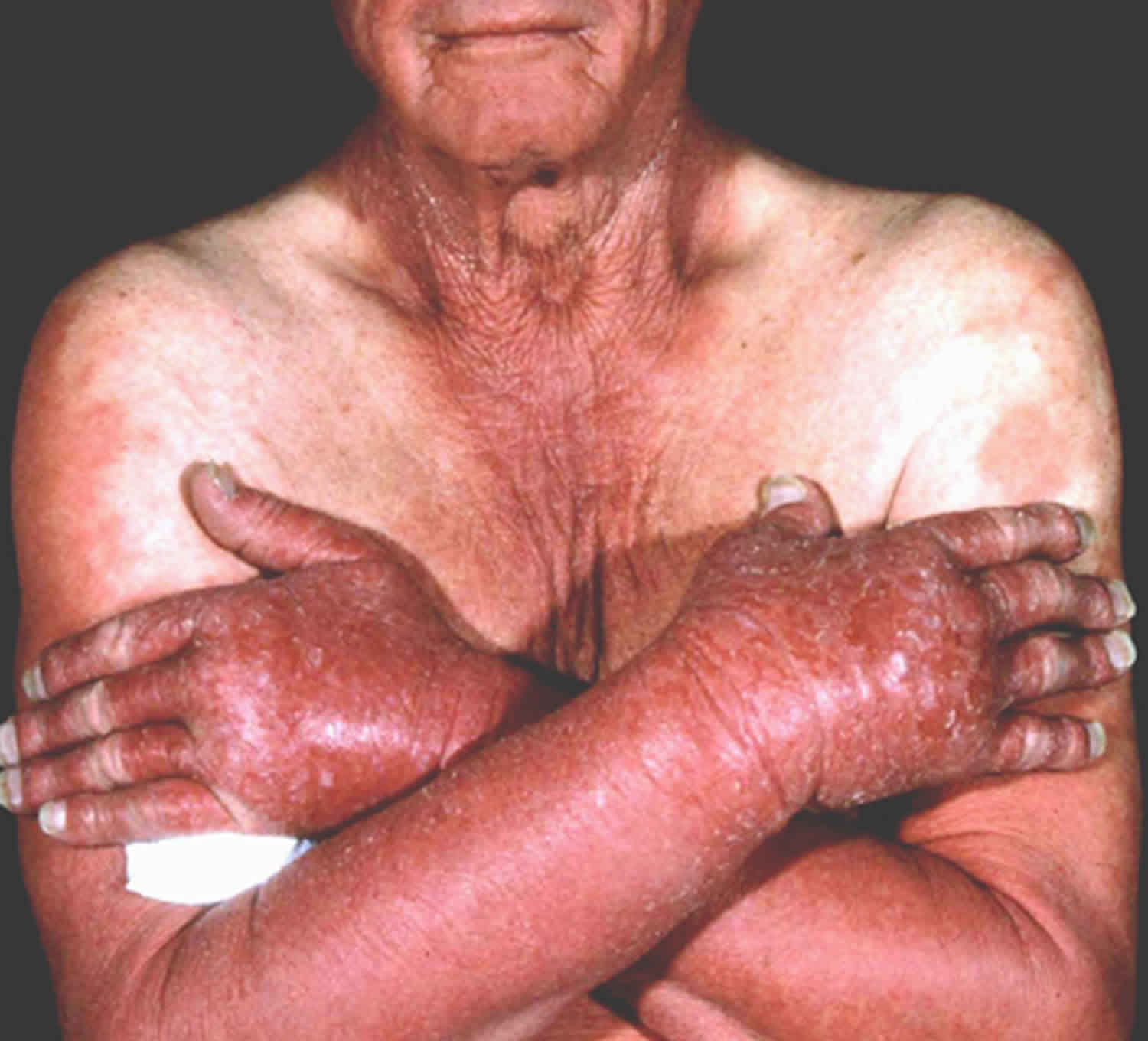
Chronic actinic dermatitis
Chronic actinic dermatitis is a rare chronic inflammatory skin condition triggered by abnormal sensitivity to sunlight (photosensitivity). Chronic actinic dermatitis is also known as chronic photosensitivity dermatitis, actinic reticuloid syndrome (this name comes from the histological findings of skin biopsies which resemble a reticulosis or cutaneous T-cell lymphoma) or persistent light reaction. ‘Actinic’ means ‘caused by sun’ and ‘dermatitis’ is ‘inflammation of the skin’. Chronic actinic dermatitis is considered a chronic complaint as it usually lasts for several years.
Chronic actinic dermatitis is characterized by severely itchy, red, inflamed, and thickened dry skin, mainly in areas that have been exposed to sunlight or artificial light.
Chronic actinic dermatitis mainly affects men over the age of 50 years, particularly those who spend a lot of time outdoors. Chronic actinic dermatitis is more common in temperate countries and its appearance worsens in summer or after sun exposure. All races may be affected, and it is not genetically inherited.
In many patients with chronic actinic dermatitis there is frequently a history of other kinds of dermatitis (inflammatory skin conditions), including atopic dermatitis, seborrheic dermatitis, allergic contact dermatitis (especially to plants such as chrysanthemum) and photocontact dermatitis for many years before the photosensitivity develops. In these cases it is sometimes called persistent light reaction. There may also be an association with HIV infection.
The first form of treatment is usually a strong steroid cream or ointment applied once a day to the affected areas. Moisturizers are used to treat dry skin with a fragrance- free soap substitute for skin cleansing. Non-steroid anti-inflammatory agents (Tacrolimus and Pimecrolimus) may be useful alternatives to steroids.
Short courses of steroid tablets are sometimes given for a flare of chronic actinic dermatitis and longer term immune suppressing medication with drugs such as azathioprine or ciclosporin may be needed in severe cases. These drugs need careful monitoring and are given under the supervision of a dermatologist.
Sometimes, a course of UV therapy can be successful in desensitising the skin. Psoralen UVA (PUVA) treatment is usually chosen as treatment with UVB usually triggers a flare.
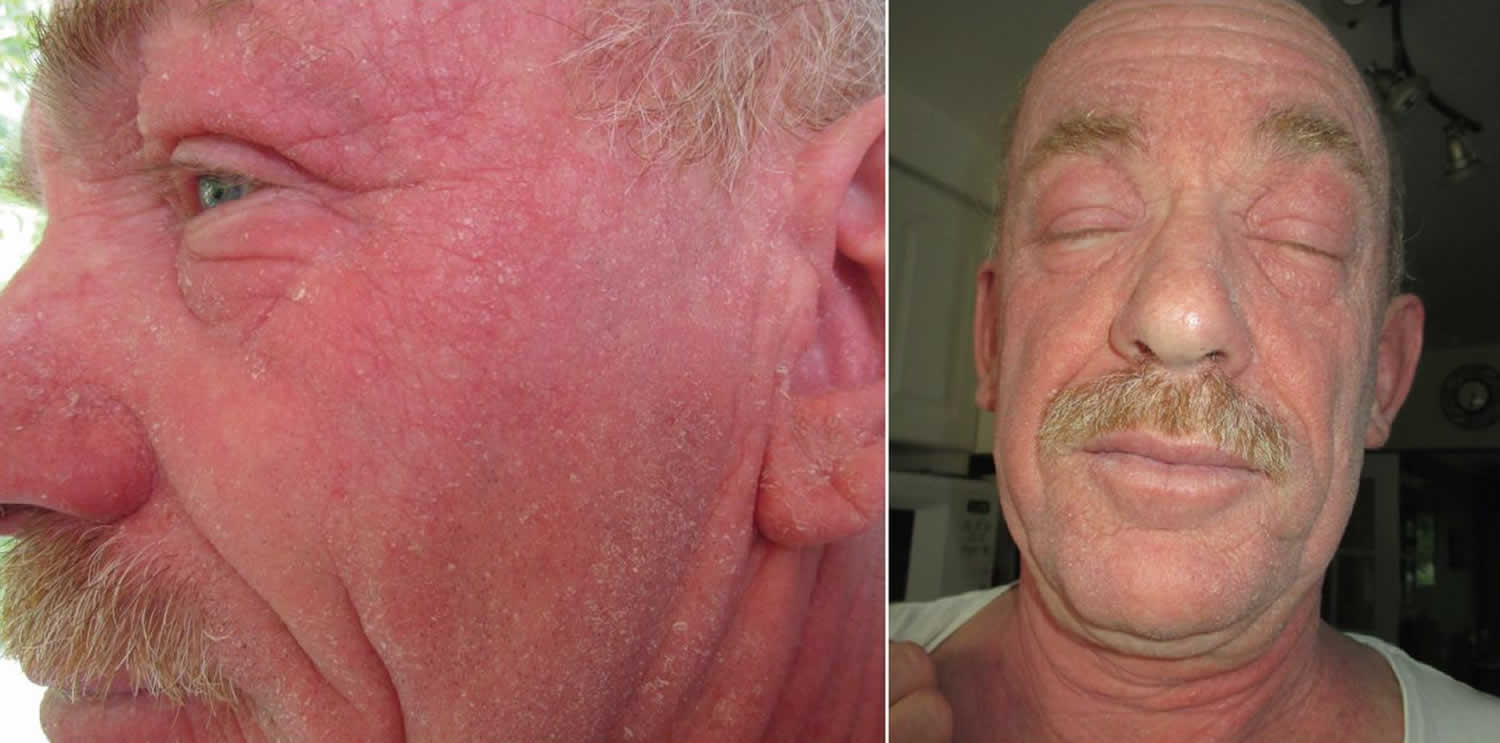
Figure 1. Chronic actinic dermatitis
Footnote: Chronic actinic dermatitis in a 60-year-old man with typical photo-distribution, affecting areas of his face and neck that were exposed to light while sparing the skin underneath the chin and the nasolabial folds.
[Source 1 ]Can chronic actinic dermatitis be cured?
No, there is no cure for chronic actinic dermatitis and many people with chronic actinic dermatitis remain sensitive to sunlight for several years. However, most people are able to help the problem by careful sun avoidance and with medication. One study found that chronic actinic dermatitis cleared in half of all sufferers after about 15 years.
Chronic actinic dermatitis causes
People with chronic actinic dermatitis are over-sensitive to sunlight and get an eczema skin reaction that can be triggered by very brief sun exposure, sometimes less than a minute. It mainly affects areas of skin that are exposed to the sunlight every day i.e. face, neck, upper chest and the back of the hands/forearms. It is usually worse in the summer when the sunlight is strongest. There can be a delay of several days between sun exposure and the skin reaction, so people with chronic actinic dermatitis are not always aware that the two are linked. It is thought that chronic actinic dermatitis is caused by an allergic reaction to sunlight, but it is unclear why this happens.
Ultraviolet (UV) radiation causes an inflammatory reaction in the skin; specifically, UVB, UVA and rarely, visible wavelengths of light. The reaction is similar to that seen in allergic contact dermatitis, and it is thought that an antigen in the skin is sensitised by light to stimulate an allergic reaction by the body’s immune system.
Other points about chronic actinic dermatitis:
- It is more common in men than women
- It usually starts after the age of 50
- People often develop chronic actinic dermatitis after having an in-built tendency to atopic or seborrhoeic dermatitis
- It is associated with skin contact allergies in 75% of cases
- It can affect any racial group
- It is more common in temperate countries away from the equator
Chronic actinic dermatitis symptoms
Chronic actinic dermatitis rash may develop in all areas exposed to the sun, with the face, neck, upper chest in a V distribution and backs of hands most commonly affected. The lesions are usually red and inflamed with scaling and lichenification (thickened and hardened patches of skin). The rash can be very itchy. The rash may spread to other areas of the body where the skin is covered by clothing.
The rash can be provoked by as little as 30 seconds exposure to daylight. It is condition that is often present throughout the year. Patients are at risk even on dull days and through window glass. Some of them also react to artificial light sources, especially naked fluorescent lamps.
Testing shows chronic actinic dermatitis is due to abnormal reactions to UVB, UVA and in severe cases to visible light.
Chronic actinic dermatitis diagnosis
Patients with chronic actinic dermatitis usually have severe dermatitis of the head and neck and they get referred to a dermatologist for assessment. The distribution of the dermatitis can be a helpful pointer to diagnosis, but it can be difficult to tell chronic actinic dermatitis apart from other types of facial eczema just from the appearance. Further tests are usually needed including:
- Phototesting (light tests) can be used to confirm the diagnosis. Phototests (light tests)– to investigate abnormal skin sensitivity to ultraviolet (UV) or visible light. This involves specialized tests in which areas of skin are exposed to known amounts of light of specific wavelengths. This is usually UVB, but sometimes there is also an excessive reaction to UVA or even visible light. Finding out which wavebands are triggering a person’s chronic actinic dermatitis can help guide best treatment with sunscreens and other forms of light protection. The reactions that develop confirm the presence of an abnormal reaction to the light.
- Patch testing and photopatch testing are also used to identify any chemical allergies i.e. allergic contact dermatitis. These include natural fragrances and plants, preservative chemicals, medicaments and sunscreens. It has been found that positive patch-test reactions to one or more allergens occur in 75% of patients with chronic actinic dermatitis, most often fragrance, sunscreens, colophony and a sesquiterpene lactones (found in the daisy family of plants).
Chronic actinic dermatitis treatment
Patients with chronic actinic dermatitis must take measures to avoid sun exposure by following sun protection strategies. In severe cases it may be necessary to admit the patient to a dark room in hospital.
In addition, if a contact allergy in involved the patient must try to avoid the offending substance.
Treatment also includes:
- Emollients
- Topical corticosteroids
- Topical tacrolimus or pimecrolimus cream
In severe cases, oral immune suppressive treatments may be required. These include:
- Systemic corticosteroids
- Azathioprine
- Ciclosporin
Extremely cautious desensitizing with photochemotherapy (PUVA) or narrowband UVB with systemic steroid cover has been successful in some cases.
The condition may spontaneously resolve, sometimes many years after the onset of the disease. For most people it is a lifelong condition that requires significant lifestyle changes to avoid sunlight as well as contact allergens.
Sun protection
The most important aspect of managing chronic actinic dermatitis is to protect the skin from sunlight. This can be done by staying indoors when the sun is at its brightest (between 11am and 3 pm). It is essential to cover the skin as much as possible when outside, even on dull days. Close weaved, long sleeve clothing is good at blocking the sun’s rays and a hat is needed to shade the face. Some people also use visors, UV-protective goggles and cotton gloves. Protecting the skin from sun may help the condition and should stop it worsening.
A high factor, broad sunscreen, non-fragranced sunscreen should be used to protect any exposed areas of skin. A reflectant mineral sunscreen is needed to give protection to individuals who are also daylight sensitive. These can be obtained as tinted creams to match different skin tones.
People who work outdoors or have outdoor hobbies are advised to try and adjust their lifestyle to minimize sun exposure. The light from a television or computer screen is safe, but compact fluorescent lamps can emit enough UV to aggravate chronic actinic dermatitis. People who are sensitive to UVA may need to use a special photo-protective films on the windows of their car and home to filter out the UV rays. These usually need to be replaced after about 5 years. Some car manufacturers offer UV protective glass as an optional extra.
Chronic actinic dermatitis prognosis
One study reported that the disease resolves in 10% of people after 5 years, 20% after 10 years and 50% after 15 years. Although it may spontaneously resolve, more commonly it is a chronic condition that persists for life. The symptoms can be controlled with careful sun avoidance and sun protection.
References