What is dacryoadenitis
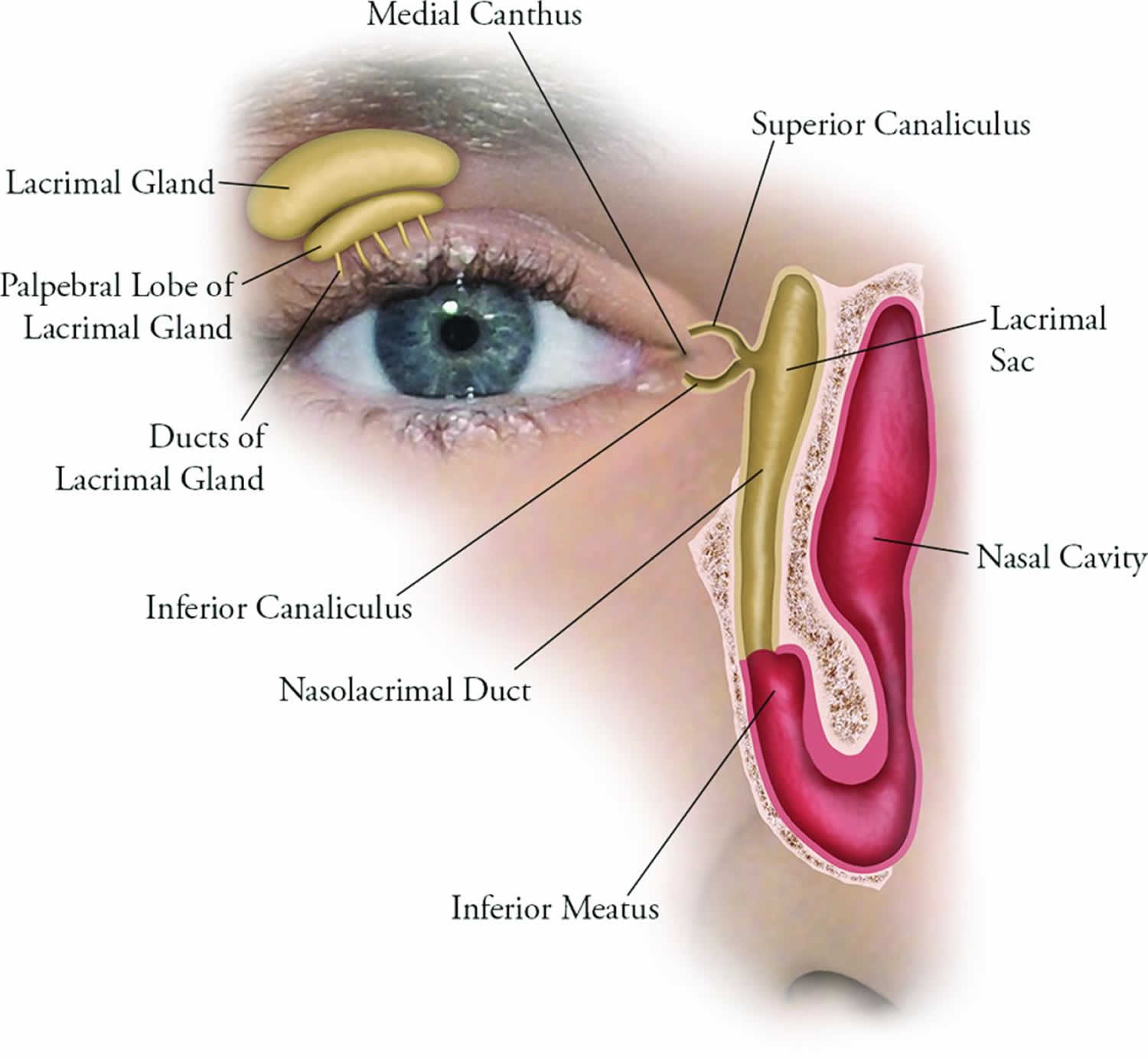
Dacryoadenitis refers to inflammation of the lacrimal gland and may be unilateral or bilateral. The lacrimal gland is located superotemporally to the globe, within the extraconal orbital fat (see Figure 1). The lacrimal gland consists of palpebral and orbital lobes, which are separated by the lateral horn of the levator aponeurosis. Inflammation of the lacrimal gland can be due to infectious or inflammatory sources but may be idiopathic. Dacryoadenitis may be separated into acute and chronic syndromes with infectious or systemic cause. Viral dacryoadenitis is self-resolving, while bacterial sources may require antibiotic administration. Inflammatory causes may respond to steroids, or demonstrate a chronic relapsing course requiring long-term treatment to maintain remission.
The prevalence of dacryoadenitis is not reported, but it is less common than dacryocystitis (inflammation or infection of the lacrimal sac). Acute dacryoadenitis is most commonly identified in children and young adults 1. Dacryoadenitis that is associated with an autoimmune disease appears to be more prevalent in women than in men, consistent with the gender predilection in systemic autoimmune disease overall 2.
Figure 1. Lacrimal gland
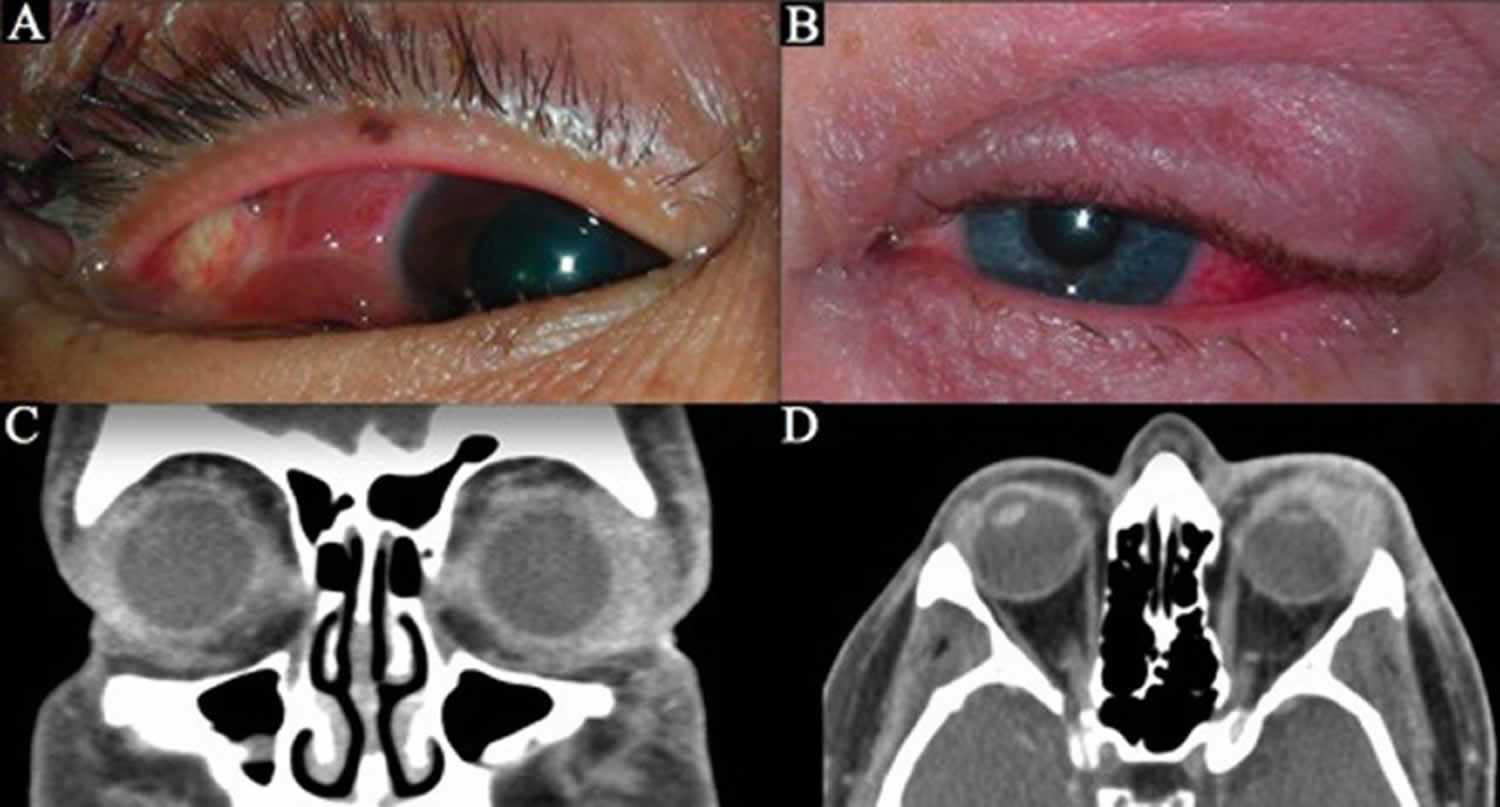
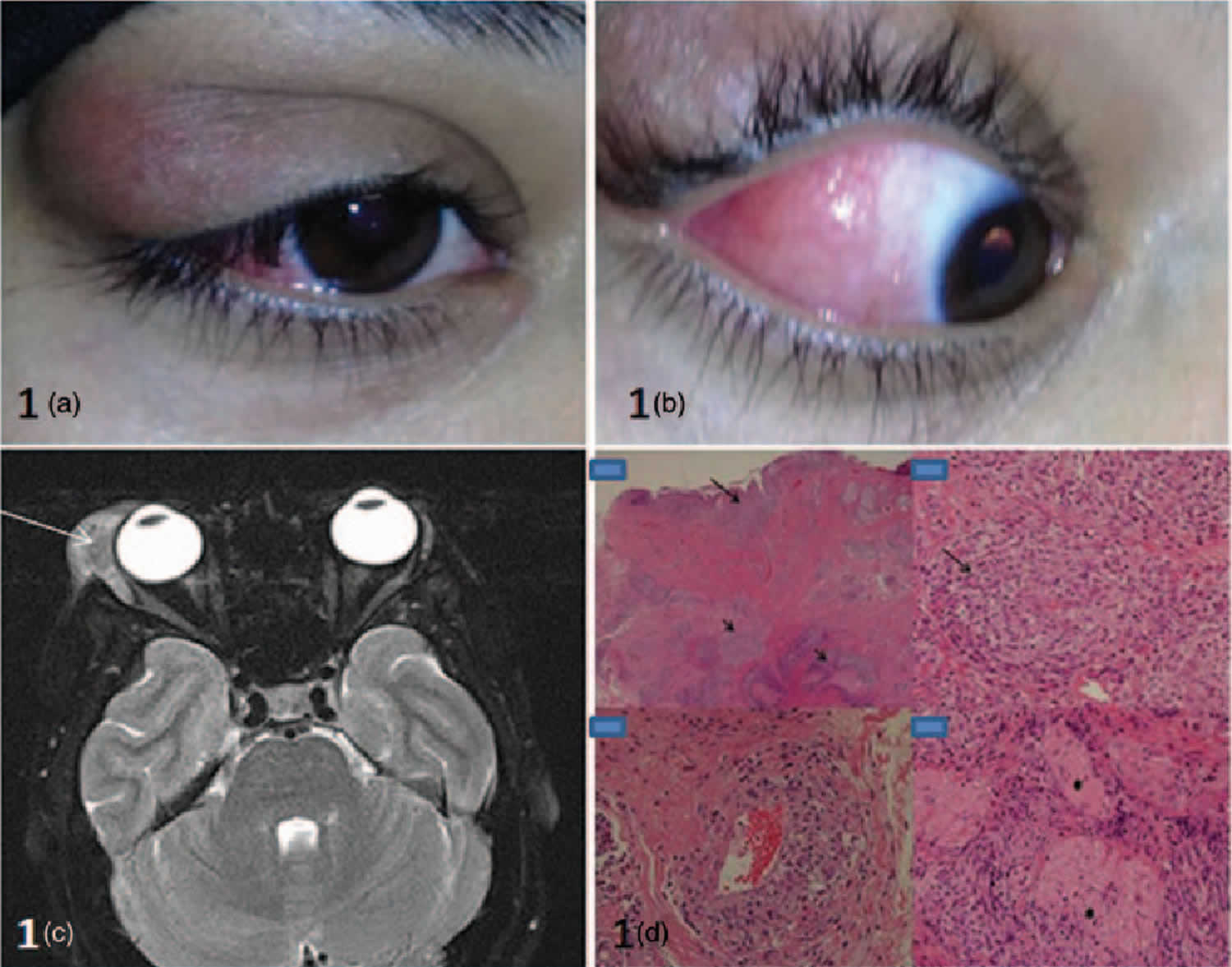
Figure 2. Dacryoadenitis
Footnote: (a): right upper lid swelling localized to lacrimal gland fossa. The swelling was painless. 1(b): salmon patch appearance of conjunctiva. 1(c): MRI image showing soft tissue mass originating from right lacrimal gland, extending around the lateral rectus muscle into extraconal space. 1(d): Histopathology (H&E stain). Low magnification: conjunctival infiltration with dense subepithelial inflammatory cell infiltrate (long arrow) and dense inflammatory aggregates in stroma (short arrows). High magnification revealing non-necrotizing granulomas composed of lymphocytes and histiocytes, surrounding blood vessels and nerves (asterisks).
[Source 3 ]What causes dacryoadenitis?
Dacryoadenitis (lacrimal gland inflammation) can be acute or chronic. Cases of acute dacryoadenitis are frequently infectious and are typically unilateral 1. Infection most commonly ascends from the conjunctiva, but also may be from the skin, penetrating trauma, or seeding in the setting of bacteremia. The causative pathogens are more often viral than bacterial, particularly in children and young adults. Viruses typically result in acute non-suppurative dacryoadenitis. The most common viral cause is Epstein-Barr virus (EBV); others include adenovirus, mumps, herpes simplex, and herpes zoster 4. Bacterial sources tend to induce suppuration; while the primary bacterial pathogen is Staphylococcus aureus, others include Streptococcus pneumoniae and gram-negative rods. Rarely, fungal sources such as Histoplasma, Blastomyces, or Nocardia may be found. Chronic infectious dacryoadenitis is uncommon, with most cases attributed to Mycobacterium tuberculosis 5.
More often chronic cases of dacryoadenitis are inflammatory. Associated conditions include Sjogren syndrome, sarcoidosis, Crohn disease, and granulomatosis with polyangiitis. Despite a new understanding of and testing for these conditions, a large portion of inflammatory cases remains idiopathic. There has also been academic interest in the recently described immunoglobulin G4 (IgG4)-related dacryoadenitis, which accounts for 23% to 35% of reports of previously idiopathic orbital inflammation 6.
Infectious dacryoadenitis
Causes of viral dacryoadenitis (most common) include the following:
- Mumps (most common, especially in childhood)
- Epstein-Barr virus (EBV)
- Herpes zoster
- Mononucleosis
- Cytomegalovirus (CMV)
- Echoviruses
- Coxsackievirus A
Causes of bacterial dacryoadenitis include the following:
- Staphylococcus aureus 7 and Streptococcus
- Neisseria gonorrhoeae
- Treponema pallidum
- Chlamydia trachomatis
- Mycobacterium leprae
- Mycobacterium tuberculosis
- Borrelia burgdorferi 8
Causes of fungal dacryoadenitis (rare) include the following:
- Histoplasmosis
- Blastomycosis
- Parasite (rare)
- Schistosoma haematobium
- Protozoa (rare)
- Acanthamoeba keratitis associated
Inflammatory dacryoadenitis
Causes of inflammatory dacryoadenitis include the following:
- Sarcoidosis
- Graves disease
- Sjögren syndrome 9
- Orbital inflammatory syndrome
- Benign lymphoepithelial lesion
Dacryoadenitis symptoms
Acute dacryoadenitis frequently presents with erythema and tenderness over the superotemporal orbit, with enlargement of the gland causing the lateral portion of the eyelid to fall, creating a characteristic S-shaped curve of the eyelid margin. There can also be associated suppurative discharge from lacrimal ducts, pouting of the lacrimal ductules, conjunctival chemosis, and swollen preauricular and cervical lymph nodes. Fever and malaise may be present. Inflammatory causes of dacryoadenitis may present subacutely with typically painless swelling of the lacrimal glands and may be bilateral.
Acute dacryoadenitis is characterized by the following:
- Unilateral, severe pain, redness, and pressure in the supratemporal region of the orbit
- Rapid onset (hours to days)
Chronic dacryoadenitis is characterized by the following:
- Can be bilateral, painless enlargement of the lacrimal gland present for more than a month
- More common than acute dacryoadenitis.
Dacryoadenitis complications
While complications from infectious dacryoadenitis are rare, a lacrimal gland abscess may develop, or the infection may lead to preseptal or orbital cellulitis.
Dacryoadenitis diagnosis
Acute dacryoadenitis that presents in association with a viral illness does not require biopsy or comprehensive laboratory evaluation. However, if there are atypical features or if the swelling does not resolve with treatment, an additional workup is merited. Occurrence in older adults, bilateral presentation, and systemic symptoms may suggest a malignant or systemic autoimmune process, in which case additional workup is strongly advisable.
Laboratory evaluation for the cause of dacryoadenitis may include a complete blood count, anti-nuclear antibody (ANA), and anti-neutrophil cytoplasmic antibody (ANCA). Angiotensin-converting enzyme is an unreliable marker of sarcoidosis. Testing for anti-Ro and anti-La antibodies in cases of suspected Sjogren syndrome is reasonable, although the yield is low.
Radiologic imaging with CT or MRI reveals diffuse, potentially oblong, enlargement of the lacrimal gland. Imaging of acute dacryoadenitis may reveal adjacent lateral rectus myositis, periscleritis, or scleritis 10. Chronic inflammatory conditions are not associated with scleral enhancement.
Lacrimal gland biopsy may be of use in cases of dacryoadenitis that are atypical, of unclear cause or fail to respond appropriately to therapy. In a review of biopsy performed on 60 cases of lacrimal gland inflammation of unknown cause, 61.7% were found to have specific histopathology, and 38% connected to systemic diseases 2. As steroids can alter the histologic demonstration, it is advisable to avoid systemic steroids before the biopsy when possible. A biopsy is generally performed via a transcutaneous approach, sampling the orbital lobe to avoid the tear ducts that drain through the palpebral lobe to the temporal conjunctival fornix. Submitted tissue samples may be fixed in formalin while fresh tissue is required for flow cytometry. When performing a biopsy of a lacrimal gland with unknown etiology, always contact your laboratory to ensure they are aware that you will be sending a fresh sample and one in formalin. Some laboratories have specific requirements of how to transport the specimen, especially for flow cytometry.
Laboratory Studies
Acute dacryoadenitis
The following laboratory studies may be used in the workup of acute dacryoadenitis (dependent on clinical presentation):
- Smear and culture if purulent discharge is noted.
- Blood cultures to rule out N gonorrhoeae infections
- Immunoglobulin titers to specific virus; not usually indicated (see Causes)
Chronic dacryoadenitis
Chronic dacryoadenitis is usually seen with chronic systemic conditions (eg, sarcoidosis, Sjögren syndrome, Graves disease). Lacrimal gland biopsy may provide helpful information.
Rule out infectious causes (rare). They include syphilis, leprosy, tuberculosis, and trachoma.
Imaging Studies
Acute dacryoadenitis
CT scan of the orbits with contrast can be helpful. The affected lacrimal gland shows diffuse enlargement, oblong shape, and marked enhancement with contrast.
No compressive changes in the contiguous bone or globe are noted.
Chronic dacryoadenitis
CT scan of the orbits with contrast show similar findings when compared to acute dacryoadenitis, except that chronic lesions show no marked enhancement with contrast. In addition, the lacrimal gland changes may be bilateral in contrast to acute dacryoadenitis.
Again, no compressive changes in the contiguous bone or globe are noted. If these changes are noted, then consider lacrimal gland tumors.
Dacryoadenitis treatment
The treatment of dacryoadenitis varies with onset (acute versus chronic) and the cause. Acute viral dacryoadenitis is typically self-resolving within 4 to 6 weeks. Self-limiting, supportive measures (eg, warm compresses, oral nonsteroidal anti-inflammatories) may help. The benefit of oral antiviral medications is uncertain 11. Bacterial dacryoadenitis requires systemic antibiotic therapy, and coverage for methicillin-resistant S. aureus (MRSA) is prudent. When purulence is present, obtaining cultures of the discharge can guide antibiotic therapy. Abscess formation may necessitate surgical drainage.
Corticosteroids will induce shrinkage of an enlarged lacrimal gland from almost all sources of dacryoadenitis; therefore, a trial of steroids for diagnostic purposes is not warranted. One study suggests that idiopathic dacryoadenitis may respond to surgical debulking, with a low relapse rate 12. Refractory cases of inflammatory dacryoadenitis may benefit from orbital radiotherapy, methotrexate, or rituximab. IgG4-related disease has a high rate of remission with rituximab, but this effect may be temporary 13.
Management of IgG4-related dacryoadenitis is still debated. An initial trial of corticosteroids is reasonable. Immunosuppression is only rarely necessary. There are reports suggesting that sclerosing dacryoadenitis that is associated with IgG4 can go on to develop lymphoma 14.
In patients with dacryoadenitis who respond to treatment but the lacrimal mass does not resolve by 3 months, a lacrimal gland biopsy after appropriate scanning is necessary 15.
Dacryoadenitis prognosis
Infectious dacryoadenitis may require antibiotics but typically resolves without complications. Inflammatory dacryoadenitis is more resistant to therapy and depends on the underlying systemic process if present. These cases may require an extended steroid taper, chronic immunomodulatory therapy, or surgical debulking 12. As with any non-specific inflammation in the orbit, if there is a recurrence or failure to resolve, a biopsy or repeat biopsy is necessary.
References- Mafee MF, Haik BG. Lacrimal gland and fossa lesions: role of computed tomography. Radiol. Clin. North Am. 1987 Jul;25(4):767-79.
- Luemsamran P, Rootman J, White VA, Nassiri N, Heran MKS. The role of biopsy in lacrimal gland inflammation: A clinicopathologic study. Orbit. 2017 Dec;36(6):411-418.
- Al-Busaidi, T., Wali, U.K., Al-Shirawi, A., & Al-Mujaini, A. (2013). Dacryoadenitis as first presenting feature in systemic lupus erythematosus. Lupus, 22 13, 1431-2
- Rhem MN, Wilhelmus KR, Jones DB. Epstein-Barr virus dacryoadenitis. Am. J. Ophthalmol. 2000 Mar;129(3):372-5.
- Madge SN, Prabhakaran VC, Shome D, Kim U, Honavar S, Selva D. Orbital tuberculosis: a review of the literature. Orbit. 2008;27(4):267-77
- Andrew NH, Sladden N, Kearney DJ, Selva D. An analysis of IgG4-related disease (IgG4-RD) among idiopathic orbital inflammations and benign lymphoid hyperplasias using two consensus-based diagnostic criteria for IgG4-RD. Br J Ophthalmol. 2015 Mar;99(3):376-81.
- Kubal A, Garibaldi DC. Dacryoadenitis caused by methicillin-resistant Staphylococcus aureus. Ophthal Plast Reconstr Surg. 2008 Jan-Feb. 24(1):50-1.
- Nieto JC, Kim N, Lucarelli MJ. Dacryoadenitis and orbital myositis associated with lyme disease. Arch Ophthalmol. 2008 Aug. 126(8):1165-6.
- Kamao T, Miyazaki T, Soga Y, et al. Genetic dissociation of dacryoadenitis and sialadenitis in a Sjogren’s syndrome mouse model with common and different susceptibility gene loci. Invest Ophthalmol Vis Sci. 2009 Feb 14.
- Andrew NH, Kearney D, Sladden N, McKelvie P, Wu A, Sun MT, McNab A, Selva D. Idiopathic Dacryoadenitis: Clinical Features, Histopathology, and Treatment Outcomes. Am. J. Ophthalmol. 2016 Mar;163:148-153.e1
- Patel R, Patel BC. Dacryoadenitis. [Updated 2019 Jun 4]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2019 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK535384
- Mombaerts I, Cameron JD, Chanlalit W, Garrity JA. Surgical debulking for idiopathic dacryoadenitis: a diagnosis and a cure. Ophthalmology. 2014 Feb;121(2):603-9
- Ebbo M, Patient M, Grados A, Groh M, Desblaches J, Hachulla E, Saadoun D, Audia S, Rigolet A, Terrier B, Perlat A, Guillaud C, Renou F, Bernit E, Costedoat-Chalumeau N, Harlé JR, Schleinitz N. Ophthalmic manifestations in IgG4-related disease: Clinical presentation and response to treatment in a French case-series. Medicine (Baltimore). 2017 Mar;96(10):e6205
- Cheuk W, Yuen HK, Chan AC, Shih LY, Kuo TT, Ma MW, Lo YF, Chan WK, Chan JK. Ocular adnexal lymphoma associated with IgG4+ chronic sclerosing dacryoadenitis: a previously undescribed complication of IgG4-related sclerosing disease. Am. J. Surg. Pathol. 2008 Aug;32(8):1159-67
- Rose GE. A personal view: probability in medicine, levels of (Un)certainty, and the diagnosis of orbital disease (with particular reference to orbital “pseudotumor”). Arch. Ophthalmol. 2007 Dec;125(12):1711-2