What does a crease in the earlobe mean
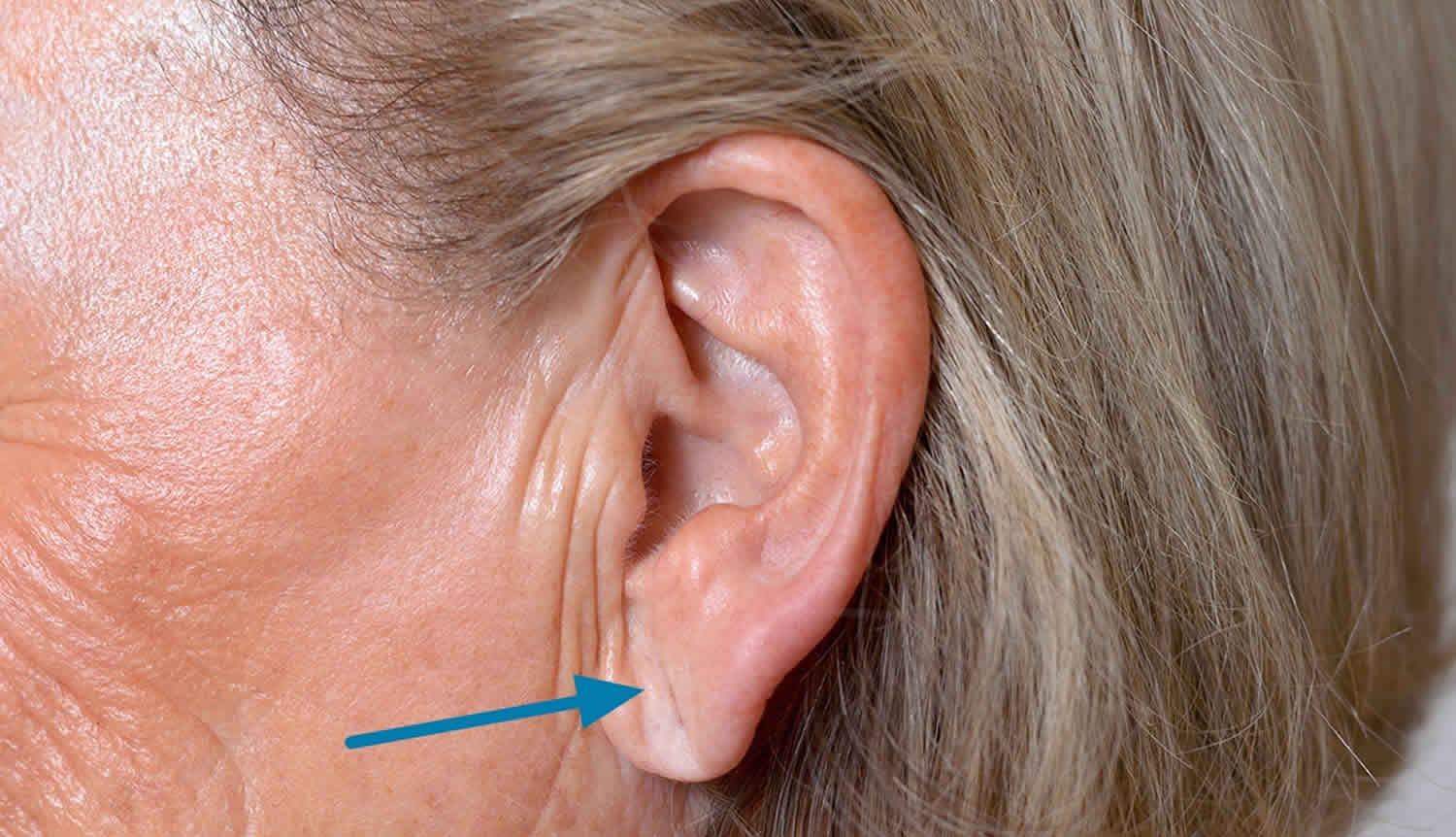
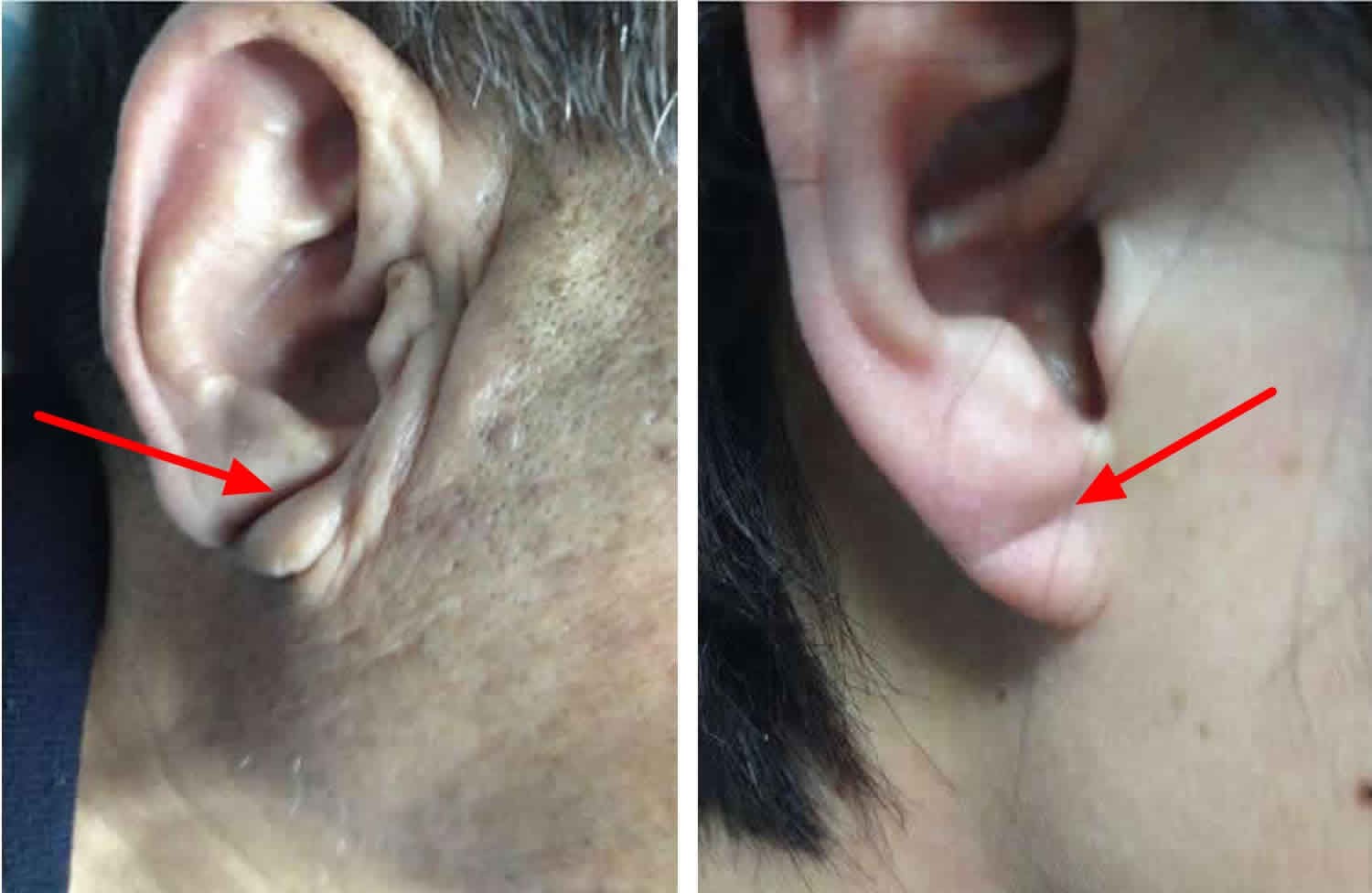
Ear lobe crease also called Frank’s sign, has been defined as a deep wrinkle that extends backwards from the tragus to the auricle. It has been proposed that ear lobe crease or diagonal earlobe crease is a predictor of coronary artery disease (coronary heart disease) 1. The ear lobe crease was first described by Frank in 1973 2 as a potential predictor of coronary artery disease.
Figure 1. Diagonal ear lobe crease
Earlobe crease and heart disease
The possible association between earlobe crease and coronary artery disease was first described by Frank in 1973 2, when he observed that 19 out of 20 patients with an earlobe crease had at least one of the known risk factors for coronary artery disease. Small studies with less than 10 subjects suggested an association between earlobe crease and coronary artery disease 3.
The first controlled study that examined the relationship between earlobe crease and coronary artery disease was carried out in a USA coronary-care unit 4. Lichstein et al. 4 found that 47% of 531 patients from New York who had acute heart attack had earlobe crease (unilateral or bilateral), which was significantly greater than the 30% observed among 305 age-matched control subjects with no clinical evidence of coronary artery disease.
Others (publishing in the form of letters to editors) have also supported the possible association between earlobe crease and coronary artery disease 5. Christiansen et al. 6 examined the prevalence of diagonal earlobe crease among 523 Danes (320 men) admitted to a medical-surgical unit. The prevalence of earlobe crease in patients with an acute heart attack aged from 50 to 59 (46.8%) was significantly greater than in an age-matched control group (31.6%) 6. Similar results were obtained in a group aged 60 to 69 years but not in those aged 70–79 years and > 80 years. The investigators concluded that a significant correlation was found between earlobe crease and both coronary artery disease and increasing age of the patients. Of note, a stronger correlation was found between coronary artery disease and earlobe crease than between coronary artery disease and other risk factors such as hypertension, smoking and diabetes 6.
In an autopsy study, Lichtstein et al. 5 found a positive correlation between diagonal earlobe crease and severe coronary artery disease. Subjects with bilateral earlobe crease had more severe coronary artery disease than those without earlobe crease and with unilateral earlobe crease.
In 1978, Kaukola 7 reported that 69% of the men and 69% of the women among 219 patients from Finland (165 men, age range: 32–65 years) who sustained a heart attack had a diagonal earlobe crease. The prevalence of earlobe crease was significantly greater when compared with the prevalence of 24% in a group of 290 healthy, similarly aged subjects (236 men).
In another Finnish study by Kaukola et al. 8, from 286 patients (age range: 26–66) who underwent coronary angiography because of typical symptoms or signs of coronary artery disease or atypical chest pain, 200 (174 men; mean age: 48) had ≥ 50% stenosis (coronary artery disease) in ≥ 1 coronary artery and 86 individuals (35 men; mean age: 50 years) were without any significant stenosis (≤ 50%). The prevalence of earlobe crease in the group with coronary artery disease was 72%, whereas in the group without coronary artery disease it was only 21% (p < 0.001). The authors 8 concluded that the prevalence of diagonal earlobe crease increases with age and severity of coronary artery disease but showed no correlation between earlobe crease and other coronary risk factors such as high cholesterol, high triglycerides, low high-density lipoprotein cholesterol, hypertension, smoking, diabetes and obesity 8.
In 1982, the same author 9 examined the possibility that earlobe crease is inherited. He evaluated 41 male patients (mean age: 44 years) with previous heart attack and their 134 first-degree relatives, in order to document the prevalence of earlobe crease 9. The earlobe crease was present in 59% of the patients with heart attack. From the 74 relatives of this group, those with coronary artery disease, approximately 50% of the parents, approximately 25% of healthy brothers and 31% of healthy sisters also had earlobe crease. None of the children had earlobe crease. Kaukola 9 concluded that those results do support an association between earlobe crease and coronary artery disease but do not indicate that earlobe crease is an inheritable sign.
Sprague 10 examined 222 patients in the USA, who were scheduled for elective surgery. He 10 found that earlobe crease increased with age as only 3 patients out of 120 under 40 years old had the sign whereas the sign was visible in 61 out of the remaining 102 patients who were older than 40 years. Among those 102 patients, 50 had coronary artery disease. The prevalence rate of earlobe crease in patients with coronary artery disease was 82%, and this was significantly higher than the 38.5% observed in the remaining 52 patients without coronary artery disease. Sprague 10 concluded that earlobe crease was positively related with coronary artery disease, age and increased complications of anaesthesia.
Doering et al. 11 compared 50 patients with coronary artery disease with 38 patients without coronary artery disease in the USA on the basis of age, weight, smoking history, diabetes and the presence of an earlobe crease. All the above factors were correlated with coronary artery disease, but the strongest correlation was noted between coronary artery disease and earlobe crease 11.
Kristensen 12 found a positive correlation between bilateral diagonal earlobe crease and coronary artery disease in 74 male hypertensive Danes when compared with 29 normotensive control age-matched males. On the other hand, no genetic factor seemed to be involved in the cause and development of the earlobe crease 12.
A very strong relationship between earlobe crease and coronary artery disease was found in a Polish study 13 where 72 patients out of 160 with coronary artery disease and only 23 patients out of 340 without coronary artery disease had earlobe crease.
In a study from Israel, Shoenfeld et al. 14 found a higher prevalence (77%) of earlobe crease in 421 patients with MI when compared with a 40% prevalence rate of 421 controls, regardless of age. Moreover, the prevalence of earlobe crease was even higher in MI patients with diabetic retinopathy, hypertension, and in Ashkenazi Jews compared with non-Ashkenazi Jews 14.
Pasternac and Sami 15 assessed 340 Canadian patients who underwent coronary arteriography; 75.6% of them had coronary artery disease. The prevalence of coronary artery disease in patients with earlobe crease was 91.1%. This was significantly higher when compared with the 60.5% for patients without earlobe crease. Of note, the positive predictive value of earlobe crease in men was 95.7% while in women it was much lower (66.7%) 15. The authors concluded that earlobe crease has a high predictive value for coronary artery disease, but its absence does not rule out such a disease 15.
In a large study, Elliot 16 suggested that earlobe crease should be regarded as a risk factor of coronary artery disease. Among 1000 patients who were admitted to large urban medical centres in St. Louis, Missouri (USA), earlobe crease was present in 275 out of 376 patients with coronary artery disease, whereas it was seen in only 98 out of 624 patients without coronary artery disease 16. Similar results were seen in a subgroup analysis of the above study; among 205 patients who underwent coronary angiography 121 out of 148 patients with coronary artery disease had earlobe crease 16. In another prospective, subgroup analysis of the same study, in 112 patients who underwent cine coronary angiography only earlobe crease and previous heart attack were found to significantly correlate with coronary artery disease proved by angiography 16. Of note, patients were considered as having coronary artery disease if coronary angiography showed > 75% stenosis of ≥ 1 major coronary artery and if they had an acute heart attack or history of angina 16.
Similar results were obtained in 1000 Japanese patients (573 men) 17. The earlobe crease was present in 58 out of 237 (24.5%) patients with coronary artery disease, a prevalence which was significantly greater than that of 35 out of 720 (4.8%) patients without coronary artery disease. In addition, in a subgroup analysis of the above study 17, in 200 patients who underwent coronary angiography earlobe crease was present in 31 out of 119 (26.1%) patients with > 50% stenosis of ≥ 1 major coronary artery but in only 3 out of 81 (3.7%) without coronary artery disease. The earlobe crease was also found to correlate significantly with male sex, age older than 50 years, hypertension and smoking. However, in a multivariate analysis in the 200 patients who underwent coronary angiography, coronary artery disease and age > 50 years were significantly related to the presence of earlobe crease while the other risk factors appeared to be unrelated 17. The authors concluded that, apart from the increased prevalence of earlobe crease with advancing age, earlobe crease is an independent predictor for coronary artery disease in Japanese adults. Of note, the prevalence of earlobe crease in this population is very low when compared with the results of studies in Europe and America 17.
The overall incidence of bilateral diagonal earlobe crease in 350 non-selected patients was 45%, with a significant increase over the age of 50 years old 18. The coronary artery disease was present in 65% of patients with earlobe crease, a prevalence that was significantly greater than that of 23% of patients without earlobe crease. In addition, it was shown that diagonal earlobe crease is significantly associated with hypertension, sex (higher incidence of earlobe crease was observed in males (66%) than in females (34%), smoking and hypercholesterolaemia (p < 0.05), but no relationship was observed with diabetes mellitus and obesity 18.
Lesbre et al. 19 found a significant association between earlobe crease and coronary artery disease (> 75% stenosis in ≥ 1 main coronary artery) in 172 patients. Sensitivity, specificity and positive predictive value of earlobe crease for detecting coronary artery disease were 75, 57.5 and 80.3%, respectively. The authors 19 concluded that earlobe crease should be considered as a marker of coronary artery disease, independently of other risk factors.
In an autopsy study, Cumberland et al. 20 examined the relationship between earlobe crease and severe coronary artery disease (> 75% stenosis of ≥ 1 major coronary artery) in 800 patients in the USA. The authors found that the presence of earlobe crease was significantly correlated with severe coronary artery disease and that the absence of earlobe crease is a predictor of the absence of severe coronary atherosclerosis 20.
Similar results were seen in 376 postmortems (206 men) carried out in the UK 21. The risk of death from heart attack in men with earlobe crease was 2.50 whereas in women it was 3.70. In addition, the relative risk of a male with bilateral diagonal earlobe crease having severe coronary artery disease (> 75% stenosis of a coronary artery) was 1.64 and for females it was 3.65. The sensitivity and specificity of bilateral diagonal earlobe crease for detecting severe coronary artery disease were 62.1% and 65.9% for men and 69.2% and 78% for women, respectively. The authors concluded that earlobe crease could be a useful sign of atherosclerosis 21.
In another necropsy study in the UK, Kirkham et al. 22 found a strong association between earlobe crease and a cardiovascular cause of death in men and women after age, height, and diabetes had been adjusted for.
In an Indian population, Verma et al. 23 reported that bilateral diagonal earlobe crease was significantly more pronounced in patients with documented coronary artery disease and that the prevalence of earlobe crease increases with advancing age. Of note, the combined presence of earlobe crease and ear canal hair represented a more sensitive index of coronary artery disease 24.
In 1989, in the Copenhagen City Heart Study 25, 14 223 healthy persons were followed for 6.5 years in order to determine the relationship between diagonal earlobe crease and the development of a first acute heart attack. Of note, the right earlobe crease was examined. After adjusting for age and sex, the authors concluded that those with earlobe crease had a risk of acute heart attack, 1.4 times greater than those without 25. The same team 2 years later reported similar results 26. In addition, in a recent (2014) prospective cohort study, Christoffersen et al. followed up the same population until 2011 27. The authors concluded that visible signs such as earlobe crease, male pattern baldness and xanthelasmata, alone or in combination, are associated with increased risk of coronary artery disease and heart attack in the general population, independent of age and cardiovascular risk factors 27.
Miric et al. 28 found that among 243 patients from Croatia, earlobe crease was present in 72.7% of 143 with proven coronary artery disease and in 48% of the remaining 100 patients without coronary artery disease. Additionally, earlobe crease was more prevalent in patients older than 50 years than in younger patients 28.
In a Japanese autopsy study 29, where 100 men aged from 50 to 79 years old, who died free of vascular diseases or related conditions, were studied, Ishii et al. 29 concluded that earlobe crease provides a significant external marker for atherosclerosis.
In a prospective cohort study 30 which was conducted in St. Louis (USA), 108 patients were followed up for 8 to 10 years in order to ascertain whether the diagonal earlobe crease is associated prospectively with future death or cardiac events. During that time 58 deaths occurred. The prevalence of death due to acute heart attack, sudden cardiac death or heart failure was greater in patients with earlobe crease whether they had coronary artery disease or not compared with patients without earlobe crease 30. In addition, the prevalence of cardiac events such as cardiac death, nonfatal MI, or coronary artery bypass surgery was also higher in patients with earlobe crease whether they had coronary artery disease or not compared with those without earlobe crease 30. In this study, Elliott and Karrison 30 suggested that diagonal earlobe crease is associated with increased all-cause and cardiac morbidity and mortality. Apart from the above findings, Elliott and Powel 31 additionally demonstrated for the first time in a living population (264 patients) a graded association between the number of creased ears (i.e. unilateral or bilateral) and future coronary risk.
In a Brazilian study of 1464 patients (760 men), Tranchesi et al. 32 found that earlobe crease was present in 220 out of 338 patients (65%) with coronary artery disease (> 70% stenosis of ≥ 1 coronary artery documented by angiography), and this prevalence was significantly greater when compared with the 28% of 1086 patients without coronary artery disease. In addition, the sensitivity of earlobe crease was 65%, the specificity 72%, the positive predictive value 42% and the negative predictive value 87% for the diagnosis of coronary artery disease. Of note, earlobe crease was more prevalent in the white (41%) than in the non-white population (23%). However, the prevalence of earlobe crease in both populations was significantly greater in patients with coronary artery disease 32. Moreover, the presence of earlobe crease was also related to the severity of coronary artery disease. When the stenosis was present in 1 to 3 coronary arteries, the prevalence of earlobe crease increased from 55% to 78% 32.
The association between earlobe crease and coronary artery disease was found to be significant in 247 patients admitted to an acute general hospital in Dublin, Ireland 33. The prevalence of earlobe crease did not differ between males and females. In addition, no correlation was found between earlobe crease and smoking, hypercholesterolemia, hypertension, peripheral arterial disease or stroke.
Similar results were found in a non-cardiac patient population in London 34. Motamed et al. 34 reported a significant association between earlobe crease and a history of coronary artery disease and that the earlobe crease and coronary artery disease correlation was higher than that of coronary artery disease and other risk factors. However, the sensitivity, specificity and positive predictive value of the sign was 48%, 88% and 16%, respectively. These findings are of little clinical importance.
In a Croatian case-control study, Miric et al. 35 found that diagonal earlobe crease was present in 62.9% of 842 men (< 60 years old) admitted for the first non-fatal heart attack, and that this prevalence was greater than that of 46% of 712 age-matched controls admitted with non-cardiac diagnoses and without clinical signs of coronary artery disease. The relative risk ratio of heart attack for men with earlobe crease was 1.37. This did not change when it was adjusted for age and other risk factors 35. The authors concluded that dermatological signs such as baldness, thoracic hairiness and diagonal earlobe crease indicate an additional risk of heart attack in men under the age of 60 years, independently of age and other established coronary risk factors 35. One of the authors of the above study suggests that the presence of these dermatological signs (earlobe crease, baldness, hair greying and wrinkling of the skin) in patients could be indicators of atherosclerosis 36.
Kuri et al. 37 evaluated the usefulness of the earlobe crease sign as a marker of coronary artery disease in 530 Japanese patients, aged > 40 years old, who were undergoing elective surgery. The authors 37 concluded that earlobe crease may be a useful marker for the presence of coronary artery disease in patients for whom little or no history and investigations are available.
In a large study in Turkey, 3722 individuals (1250 males) were evaluated for the presence of earlobe crease in diseases such as diabetes mellitus, hypertension, heart attack and coronary artery disease 38. The authors suggested that earlobe crease could be a valuable sign in diagnosing and screening such diseases. Of note, earlobe crease was more pronounced in males than in females 38.
In 2004, also in Turkey, Evrengül et al. 39 examined 415 patients (306 men) for the presence of bilateral earlobe crease. There was a greater prevalence of earlobe crease in 296 patients with documented coronary artery disease (> 70% stenosis of 1 of the 3 major coronary arteries) by angiography (51.4%) than in 119 patients (15.1%) without coronary artery disease 39. Sensitivity of bilateral earlobe crease was 51.3%, specificity was 84.8%, the positive predictive value was 89.4% and the negative predictive value was 41.2% for the diagnosis of coronary artery disease. The earlobe crease was an independent variable for coronary artery disease. Of note, the presence of bilateral earlobe crease was significantly associated not only with coronary artery disease but also with other coronary risk factors such as hypertension, male gender and smoking. There was no association between earlobe crease, diabetes, lipidaemia and obesity. The authors concluded that bilateral earlobe crease might be a useful sign in clinical practice 39.
In a Swedish autopsy study 40, 55% of 520 subjects (420 males, mean age 56) had diagonal earlobe crease. There was no significant difference between the presence of earlobe crease in males (53.8%) and females (60%). The earlobe crease was unilateral in 8.8% and bilateral in 91.2% of the subjects. The prevalence of earlobe crease was 65.4% in those with coronary artery disease and 73.3% in victims of sudden cardiac death, a difference which was significant when compared with 46.1% and 57.9%, respectively in the control groups 40. The sensitivity, specificity and positive and negative predictive values for those younger than 40 years old were 0.68, 0.84, 0.80, 0.72, respectively; for those between ages 40 and 50 years old, they were 0.68, 0.60, 0.63, 0.66, respectively; and for those over 60 years old they were 0.79, 0.33, 0.51, 0.61, respectively 40. The authors 40 concluded that earlobe crease could be useful in screening for premature coronary artery disease in younger individuals. Of note, there was a significantly greater heart weight in patients with earlobe crease than in those without earlobe crease and in those dying from sudden cardiac death compared with deaths from other causes 40.
In a Spanish study, Lamot et al. 41 found a significant relation between the presence of a diagonal earlobe crease and coronary artery disease and suggested that this sign could be useful in clinical practice, mainly among patients aged between 30 and 60 years.
In a recent study carried out in the USA 42, the relation between diagonal earlobe crease and coronary artery disease was examined in 430 patients without history of coronary artery disease who underwent coronary angiography. Severe coronary artery disease was documented when > 50% stenosis was found in ≥ 1 coronary artery in the angiography. The coronary artery disease was categorized as any coronary artery disease, significant coronary artery disease, ≥ 2 diseased vessels and ≥ 3 diseased segments. All categories of coronary artery disease were more prevalent in the group with diagonal earlobe crease than in the group without diagonal earlobe crease. Diagonal earlobe crease was present in 71% of all the patients and, similarly, the prevalence of any coronary artery disease was 71% of all the patients. The prevalence of any coronary artery disease in 307 patients with diagonal earlobe crease was 77%. This was significantly greater when compared with that of 55% of 123 patients without diagonal earlobe crease. In addition, sensitivity, specificity, positive and negative predictive values for diagonal earlobe crease to diagnose any coronary artery disease were 78, 43, 77 and 45%, respectively 42. Of note, Shmilovich et al. 42 were the first to report that diagonal earlobe crease is associated with the presence, extent, and severity of coronary artery disease and that this association remained even after adjusting for age, male gender and other risk factors for coronary artery disease.
The same author, in a more recent study 43, probably in the same population as for the above study, found that diagonal earlobe crease is a superior predictor of coronary artery disease (> 50% stenosis of coronary arteries) than the Diamond Forester algorithm. The authors suggested that, in patients with chest pain, the combination of the diagonal earlobe crease and Diamond-Forester algorithm was a better predictor of coronary artery disease than each alone 43.
In a Chinese study 44 of 100 patients, the prevalence of earlobe crease in 50 patients with coronary artery disease was significantly greater than in those without coronary artery disease. The sensitivity, specificity and positive predictive value for diagonal earlobe crease to diagnose coronary artery disease were 61%, 58% and 59.3%, respectively 44. The authors suggested that earlobe crease was associated with the presence of coronary artery disease 44.
In a Chinese cohort study 45, among 449 consecutive Chinese patients who underwent coronary artery angiography, the prevalence of diagonal earlobe crease was 75.2% in 250 patients with coronary artery disease, which was significantly greater than that of 46.2% of 199 patients without coronary artery disease. Moreover, sensitivity, specificity, positive and negative predictive values for diagonal earlobe crease to diagnose coronary artery disease in the whole population were 75.2%, 53.8%, 67.1% and 63.3%, respectively. Diagonal earlobe crease remained a positive predictor for coronary artery disease even after adjusting for age, gender and traditional risk factors, but not for hypertension, diabetes mellitus, hypercholesterolaemia and hypertriglyceridaemia. The authors 45 concluded that there is a significant association between diagonal earlobe crease and coronary artery disease independent of established risk factors among Chinese people.
Ear lobe crease and other diseases
Numerous other studies have tried to associate earlobe crease with other diseases or coronary risk factors such as hypertension, diabetes, stroke, metabolic syndrome, peripheral arterial disease, carotid intima-media thickness, obesity, stress and alcohol use. Park et al. 46 found a strong correlation between earlobe crease and hemorrhagic stroke. More specifically, earlobe crease was independently associated with subarachnoid haemorrhage and intracerebral haemorrhage 46. In a recent case report 47, earlobe crease was observed in a patient with sub-acute occipital infarction in the left posterior cerebral artery. Others suggested or tried to correlate earlobe crease with stress 48, anxiety 49, schizophrenia and bipolar disorder 50. Several studies significantly correlated the presence of earlobe crease with hypertension 51, while others failed to find a positive correlation of earlobe crease with hypercholesterolaemia [99]. Furthermore, others reported an association of earlobe crease with metabolic syndrome 52 or obesity 53. Controversial results have been produced regarding the association of earlobe crease with diabetic retinopathy 54. Of note, a negative association was found between the presence of earlobe crease and alcohol use in 625 white women 55. Interestingly, in several reports the presence of earlobe crease was significantly correlated with carotid intima-media thickness 56, whereas only one study did not reach significance 57. Pieri et al. 58 reported 2 histological lesions in the ear lobes of diabetic patients: perivascular cellular infiltration and thickening of adventitia reticularis in arterioles, precapillaries, capillaries and venules. Several studies suggested using an arterialized ear lobe blood sample for the measurement of arterial O2 pressure (pO2) while others indicated that arterialized ear lobe blood underestimates the real value 59. Recent studies found a significant correlation of earlobe crease with peripheral arterial disease 60. In addition, earlobe crease was found to have a significant correlation with brachial-ankle pulse wave velocity 61, and with the cardio-ankle vascular index 62.
Studies showing no association between earlobe crease and coronary heart disease
Several studies have reported no significant correlation between earlobe crease and coronary heart disease. The first report was an American study 63 of 211 patients undergoing coronary angiography in which no significant association between earlobe crease and coronary heart disease was found.
In a letter to the editor, Burton refers to a British study 64 which found no significant difference between the presence of bilateral earlobe crease in 52% of 48 males with heart attack and in 58% of 48 age-matched controls.
In 1977, among 1237 Japanese-American men, the prevalence of earlobe crease was 30% in 71 patients with any coronary heart disease (angina, coronary insufficiency and heart attack), 22% in 37 patients with heart attack and in 32% of patients without coronary heart disease. Rhoads et al. 65 concluded that no significant relation was found between earlobe crease and coronary heart disease in Japanese-American men.
Similar results were obtained in 216 Native American Indians, where no correlation between earlobe crease and coronary heart disease was found.
In a small controlled study (Northern Ireland) 66 which included 23 patients with acute heart attack and 23 matched controls, Farrell and Gilchrist found no correlation between earlobe crease in the occurrence of heart attack.
Jorde et al. 67 reported lack of an association between earlobe crease and coronary risk factors such as hypertension, diabetes mellitus, smoking and obesity in 686 Americans.
Moreover, no significant correlations were found between earlobe crease and coronary heart disease in 100 adult Caucasian (Vermont, USA) patients (68 men) with the clinical diagnosis of aortic stenosis who underwent coronary angiography 68. The authors 68 concluded that earlobe crease is of little clinical importance.
In 261 consecutive men who underwent coronary angiography, earlobe crease was present in 67% of this population 69. The prevalence of coronary heart disease in 175 men with earlobe crease was 85% and in 86 men without earlobe crease it was also 85%. The authors 69 found no correlation between earlobe crease and coronary heart disease and concluded that their association is justifiable due to the fact that earlobe crease and coronary heart disease both increase with age.
In several articles, Cheng 70 refers to a large study from China which concluded that earlobe crease has no predictive value for coronary heart disease in 3155 persons; earlobe crease was attributed to age.
In a prospective Irish study 71, among 125 consecutive patients who underwent coronary angiography, earlobe crease was present in 65 patients. The authors found no relation between earlobe crease and age, sex, smoking, previous heart attack, hypertension, family history of heart disease, body mass index or angiographically defined coronary heart disease. In this context, the authors 71 concluded that earlobe crease is not a marker of coronary heart disease.
In an Austrian prospective clinical investigation 72, 233 patients with coronary heart disease were evaluated. Eber and Delgado 72 suggested that the presence and extent of diagonal earlobe crease may not be regarded as a general prognostic factor for coronary atherosclerosis.
Kuon et al. 73 assessed 670 German patients who underwent coronary angiography. The prevalence of coronary heart disease (> 70% stenosis of coronary arteries) was 55% in patients with earlobe crease and 55.9% in patients without earlobe crease. No significance was found. The authors 73 concluded that although earlobe crease is associated with age and overweight, it does not predict coronary heart disease.
In a subgroup analysis of the Fremantle Diabetes Study 74, which included 1022 diabetic patients, the prevalence of earlobe crease was 55%. Although patients with an earlobe crease were more likely to have coronary heart disease than those without an earlobe crease, the sensitivity, specificity, positive predictive value and negative predictive value of earlobe crease for detecting coronary heart disease were 60, 48, 37 and 71%, respectively. After adjusting for coronary risk factors, the authors concluded that earlobe crease is not a predictor of coronary heart disease 74. Similar conclusions were reached concerning diabetic retinopathy 74.
In 2009, Koracevic and Atanaskovic 75 reported their unpublished data from a study which they had conducted 13 years before in Serbia. They evaluated 78 hospitalized patients (60 men) with mean age 60.4 years 75. They concluded that whether or not patients had unilateral or bilateral diagonal earlobe crease, or whether the crease was deep or superficial, it did not represent a marker of coronary heart disease 75.
Summary
It is difficult to explain why there is so much variation in the studies described above 1. Even 41 years after the earlobe crease sign was first described there is still uncertainty regarding its relevance 1.
It is important to establish whether earlobe crease is a coronary risk factor and whether this physical sign can improve vascular risk assessment. Although the majority of studies suggested an association between earlobe crease and coronary heart disease, there are some limitations. Age, gender, race, and ear lobe shape should not be neglected if we want to evaluate the validity of earlobe crease as a predictor of coronary heart disease. A study by Overfield and Call 76 examined 324 healthy adult subjects (70 south western Alaskan Eskimos, 167 Navajos and 87 whites). The authors 76 found that earlobe crease is more frequent with age in healthy adults, creasing is related to the shape of the ear lobe, and the age of onset of creasing is influenced by race.
The mechanisms leading to the concurrent development of earlobe crease and coronary heart disease remain uncertain. Ethnic differences may play an important role in the prevalence of earlobe crease. Petrakis and Koo 77 evaluated the prevalence of earlobe crease in various racial groups using police arrest photographs. They found an age-related increase in the frequency of earlobe crease in White, Black and Latin-American males but no increase among the Chinese and Hawaiian-Samoans 77. It should also be considered that earlobe crease may only predict coronary heart disease within a limited age range 76. This is because the earlobe crease is absent at birth and rarely seen in the young, whereas it is more common in the elderly 78.
The presence of the earlobe crease may be influenced by the time of the day 79. This is because the earlobe crease may become more apparent after sleeping and distorting the ear lobe. This factor may need to be taken into account when the prevalence of earlobe crease is assessed.
Medication administered to treat vascular risk factors (e.g. statins) can delay, arrest or even reverse coronary heart disease progression 80, even in the elderly 81. Does such treatment (or lifestyle measures such as smoking cessation) also affect the progression/development of earlobe crease? If so, then studies including patients on such treatment would have some limitations. This possibility has to be considered in the light of evidence that risk factors (hypertension, smoking, hypercholesterolaemia and diabetes) are associated with an increased prevalence of earlobe crease, at least in some studies (as discussed above).
A large meta-analysis 82 that investigated the possible association of earlobe crease with coronary heart disease was recently published. In this meta-analysis which included > 31,100 patients, the overall sensitivity was 62% and the specificity was 67%. Thus, 62% of patients with coronary heart disease would be expected to have earlobe crease, while 67% of those without coronary heart disease would be expected not to have earlobe crease. In addition, the risk of coronary heart disease is 3.3-fold higher in patients with earlobe crease compared with those without earlobe crease, a conclusion that suggests earlobe crease as a marker for coronary heart disease 82.
Earlobe crease may also be associated with factors affecting arterial inflammation 83 or elastance 84. Both these processes may be involved in the pathogenesis of earlobe crease and vascular disease. Additional markers such as metalloproteinases 85 should also be considered in the pathogenesis of coronary heart disease and earlobe crease. There is also a need to explore the relationship between various risk engines and the presence of earlobe crease.
Conclusion
Large-scale clinical studies are needed to reach more robust conclusions regarding the clinical significance of earlobe crease as a predictor of coronary heart disease 1. Future studies should consider the variables of age, race and ear lobe shape. In addition, these studies should also address whether there are common features involved in the pathogenesis of earlobe crease and coronary heart disease, as little is known in this field. Moreover, prospective cohort studies should follow up the newly diagnosed patients with coronary heart disease and observe any changes in their ear lobes as the disease progresses. In this context, a grading system for earlobe crease has been proposed 86.
After taking all the evidence into consideration, scientists still cannot state with confidence that earlobe crease represents a marker of coronary heart disease. However, researchers suggest that patients with earlobe crease may benefit from being monitored more closely for the potential presence of coronary heart disease.
References- Agouridis AP, Elisaf MS, Nair DR, Mikhailidis DP. Ear lobe crease: a marker of coronary artery disease?. Arch Med Sci. 2015;11(6):1145-55. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4697048/
- Aural sign of coronary-artery disease. Frank ST. N Engl J Med. 1973 Aug 9; 289(6):327-8.
- Griffing G. Images in clinical medicine. Frank’s sign. N Engl J Med. 2014;370:e15
- Lichstein E, Chadda KD, Naik D, et al. Diagonal ear-lobe crease: prevalence and implications as a coronary risk factor. N Engl J Med. 1974;290:615–6
- Lichtstein E, Chapman I, Gupta PK, et al. Diagonal ear-lobe crease and coronary artery sclerosis. Ann Intern Med. 1976;85:337–8
- Christiansen JS, Mathiesen B, Andersen AR, et al. Diagonal ear-lobe crease in coronary heart disease. N Engl J Med. 1975;293:308–9.
- Kaukola S. The diagonal ear-lobe crease, a physical sign associated with coronary heart disease. Acta Med Scand Suppl. 1978;619:1–49
- Kaukola S, Manninen V, Valle M, et al. Ear-lobe crease and coronary atherosclerosis. Lancet. 1979;2:1377.
- Kaukola S. The diagonal ear-lobe crease, heredity and coronary heart disease. Acta Med Scand Suppl. 1982;668:60–3
- Sprague DH. Diagonal ear-lobe crease as an indicator of operative risk. Anesthesiology. 1976;45:362–4.
- Doering C, Ruhsenberger C, Phillips DS. Ear lobe creases and heart disease. J Am Geriatr Soc. 1977;25:183–5.
- Kristensen BO. Ear-lobe crease and vascular complications in essential hypertension. Lancet. 1980;1:265.
- Wermut W, Jaszczenko S, Ruszel A. Ear lobe crease as a risk factor in coronary disease [Polish] Wiad Lek. 1980;33:435–8.
- Shoenfeld Y, Mor R, Weinberger A, et al. Diagonal ear lobe crease and coronary risk factors. J Am Geriatr Soc. 1980;28:184–7
- Pasternac A, Sami M. Predictive value of the ear-crease sign in coronary artery disease. Can Med Assoc J. 1982;126:645–9
- Elliott WJ. Ear lobe crease and coronary artery disease. 1,000 patients and review of the literature. Am J Med. 1983;75:1024–32
- Toyosaki N, Tsuchiya M, Hashimoto T, et al. Earlobe crease and coronary heart disease in Japanese. Heart Vessels. 1986;2:161–5
- Gutiu I, el Rifai C, Mallozi M. Relation between diagonal ear lobe crease and ischemic chronic heart disease and the factors of coronary risk. Med Interne. 1986;24:111–6
- Lesbre JP, Castier B, Tribouilloy C, et al. Frank’s sign and coronary disease. Ann Cardiol Angeiol (Paris) 1987;36:37–41.
- Cumberland GD, Riddick L, Vinson R. Earlobe creases and coronary atherosclerosis. The view from forensic pathology. Am J Forensic Med Pathol. 1987;8:9–11.
- Patel V, Champ C, Andrews PS, et al. Diagonal earlobe creases and atheromatous disease: a postmortem study. J R Coll Physicians Lond. 1992;26:274–7.
- Kirkham N, Murrells T, Melcher DH, et al. Diagonal earlobe creases and fatal cardiovascular disease: a necropsy study. Br Heart J. 1989;61:361–4.
- Verma SK, Khamesra R, Bordia A. Ear-lobe crease and ear-canal hair as predictors of coronary artery disease in Indian population. Indian J Chest Dis Allied Sci. 1988;30:189–96.
- Verma SK, Khamesra R, Mehta LK, et al. Ear-lobe crease and ear-canal hair as predictors of coronary artery disease in Indian population. Indian Heart J. 1989;41:86–91
- Nyboe J, Jensen G, Appleyard M, et al. Risk factors for acute myocardial infarction in Copenhagen. I: Hereditary, educational and socioeconomic factors. Copenhagen City Heart Study. Eur Heart J. 1989;10:910–6.
- Jensen G, Nyboe J, Appleyard M, et al. Risk factors for acute myocardial infarction in Copenhagen, II: Smoking, alcohol intake, physical activity, obesity, oral contraception, diabetes, lipids, and blood pressure. Eur Heart J. 1991;12:298–308.
- Christoffersen M, Frikke-Schmidt R, Schnohr P, et al. Visible age-related signs and risk of ischemic heart disease in the general population: a prospective cohort study. Circulation. 2014;129:990–8.
- Miric D, Rumboldt Z, Pavic M, et al. The role of the diagonal ear lobe crease in the clinical evaluation of coronary risk. Lijec Vjesn. 1990;112:206–7
- Ishii T, Asuwa N, Masuda S, et al. Earlobe crease and atherosclerosis. An autopsy study. J Am Geriatr Soc. 1990;38:871–6.
- Elliott WJ, Karrison T. Increased all-cause and cardiac morbidity and mortality associated with the diagonal earlobe crease: a prospective cohort study. Am J Med. 1991;91:247–54
- Elliott WJ, Powell LH. Diagonal earlobe creases and prognosis in patients with suspected coronary artery disease. Am J Med. 1996;100:205–11
- Tranchesi B, Jr, Barbosa V, de Albuquerque CP, et al. Diagonal earlobe crease as a marker of the presence and extent of coronary atherosclerosis. Am J Cardiol. 1992;70:1417–20.
- Moraes D, McCormack P, Tyrrell J, et al. Ear lobe crease and coronary heart disease. Ir Med J. 1992;85:131–2
- Motamed M, Pelekoudas N. The predictive value of diagonal ear-lobe crease sign. Int J Clin Pract. 1998;52:305–6
- Miric D, Fabijanic D, Giunio L, et al. Dermatological indicators of coronary risk: a case-control study. Int J Cardiol. 1998;67:251–5
- Fabijanic D, Culic V. Diagonal ear lobe crease and coronary artery disease. Am J Cardiol. 2012;110:1385–6.
- Kuri M, Hayashi Y, Kagawa K, et al. Evaluation of diagonal earlobe crease as a marker of coronary artery disease: the use of this sign in pre-operative assessment. Anaesthesia. 2001;56:1160–2.
- Bahcelioglu M, Isik AF, Demirel B, et al. The diagonal ear-lobe crease. As sign of some diseases. Saudi Med J. 2005;26:947–51
- Evrengül H, Dursunoglu D, Kaftan A, et al. Bilateral diagonal earlobe crease and coronary artery disease: a significant association. Dermatology. 2004;209:271–5
- Edston E. The earlobe crease, coronary artery disease, and sudden cardiac death: an autopsy study of 520 individuals. Am J Forensic Med Pathol. 2006;27:129–33
- Lamot SB, Lonegro GG, Hernandez M, et al. Diagonal earlobe crease, a sign of coronary artery disease. Medicina (B Aires) 2007;67:321–5
- Shmilovich H, Cheng VY, Rajani R, et al. Relation of diagonal ear lobe crease to the presence, extent, and severity of coronary artery disease determined by coronary computed tomography angiography. Am J Cardiol. 2012;109:1283–7
- Shmilovich H, Cheng VY, Nakazato R, et al. Incremental value of diagonal earlobe crease to the diamond-forrester classification in estimating the probability of significant coronary artery disease determined by computed tomographic angiography. Am J Cardiol. 2014;114:1670–5
- Kwai-Ping Suen L, Lau YK, Ma HC, et al. Predictive value of auricular diagnosis on coronary heart disease. Evid Based Complement Alternat Med. 2012;2012:706249
- Wu XL, Yang DY, Zhao YS, et al. Diagonal earlobe crease and coronary artery disease in a Chinese population. BMC Cardiovasc Disord. 2014;14:43.
- Park JK, Kim HJ, Chang SJ, et al. Risk factors for hemorrhagic stroke in Wonju, Korea. Yonsei Med J. 1998;39:229–35.
- Zapata-Wainberg G, Vivancos J. Images in clinical medicine: bilateral earlobe creases. N Engl J Med. 2013;368:e32.
- Muckle TJ. Ear-crease sign and coronary artery disease. Can Med Assoc J. 1982;126:1373–4.
- Romoli M, Tordini G, Giommi A. Diagonal ear-lobe crease: possible significance as cardio-vascular risk factor and its relationship to ear-acupuncture. Acupunct Electrother Res. 1989;14:149–54.
- Praharaj SK, Sarkar S, Sinha VK. External ear abnormalities in existing scales for minor physical anomalies: are they enough? Psychiatry Res. 2012;198:324–6.
- Kobayashi Y, Fukuo Y, Nakazawa Y, et al. The evaluation of the diagonal ear lobe crease (ELC) as a atherosclerotic sign. Nihon Ronen Igakkai Zasshi. 1987;24:525–31
- Kang EH, Kang HC. Association between earlobe crease and the metabolic syndrome in a cross-sectional study. Epidemiol Health. 2012;34:e2012004
- Kuon E, Pfahlbusch K, Lang E. The diagonal ear lobe crease for evaluating coronary risk. Z Kardiol. 1995;84:512–9.
- Raman R, Rani PK, Kulothungan V, et al. Diagonal ear lobe crease in diabetic south Indian population: is it associated with Diabetic Retinopathy? Sankara Nethralaya Diabetic Retinopathy Epidemiology And Molecular-genetics Study (SN-DREAMS, Report no. 3) BMC Ophthalmol. 2009;9:11.
- Petrakis NL. Earlobe crease in women: evaluation of reproductive factors, alcohol use, and Quetelet index and relation to atherosclerotic disease. Am J Med. 1995;99:356–61
- Shrestha I, Ohtsuki T, Takahashi T, et al. Diagonal ear-lobe crease is correlated with atherosclerotic changes in carotid arteries. Circ J. 2009;73:1945–9.
- Nagatsuka K. Ear-lobe crease as a marker of carotid artery arthrosclerosis. Circ J. 2009;73:1801–2.
- Pieri A, Scarpelli P, Rizzo M. Small blood vessel involvement in diabetes mellitus: light microscope study of specimens obtained by ear lobe biopsy. Diabetologia. 1965;1:109–15.
- Hughes JM. Blood gas estimations from arterialized capillary blood versus arterial puncture: are they different? Eur Respir J. 1996;9:184–5.
- Korkmaz L, Agac MT, Acar Z, et al. Earlobe crease may provide predictive information on asymptomatic peripheral arterial disease in patients clinically free of atherosclerotic vascular disease. Angiology. 2014;65:303–7.
- Choi SI, Kang HC, Kim CO, et al. Relationship between earlobe crease and brachial-ankle pulse wave velocity in non-hypertensive, non-diabetic adults in Korea. Epidemiol Health. 2009;31:e2009002.
- Korkmaz L, Agac MT, Erkan H, et al. Association between diagonal earlobe crease and cardio-ankle vascular index in asymptomatic hypertensive patients. Med Princ Pract. 2013;22:530–4
- Mehta J, Hamby RI. Diagonal ear-lobe crease as a coronary risk factor. N Engl J Med. 1974;291:260.
- Burton JL. Ear-lobe crease. Lancet. 1979;1:328.
- Rhoads GG, Klein K, Yano K, et al. The earlobe crease: sign of obesity in middle-aged Japanese men. Hawaii Med J. 1977;36:74–7.
- Farrell RP, Gilchrist AM. Diagonal ear-lobe crease: an independent risk factor in coronary heart disease? Ulster Med J. 1980;49:171–2.
- Jorde LB, Williams RR, Hunt SC. Lack of association of diagonal earlobe crease with other cardiovascular risk factors. West J Med. 1984;140:220–3.
- Gibson TC, Ashikaga T. The ear lobe crease sign and coronary artery disease in aortic stenosis. Clin Cardiol. 1986;9:388–90
- Brady PM, Zive MA, Goldberg RJ, et al. A new wrinkle to the earlobe crease. Arch Intern Med. 1987;147:65–6
- Cheng TO. More research needed on the association between diagonal earlobe crease and coronary artery disease. Arch Intern Med. 2000;160:2396–7.
- Kenny DJ, Gilligan D. Ear lobe crease and coronary artery disease in patients undergoing coronary arteriography. Cardiology. 1989;76:293–8.
- Eber B, Delgado P. More on the diagonal earlobe crease as a marker of coronary artery disease. Am J Cardiol. 1993;72:861
- Kuon E, Pfahlbusch K, Lang E. The diagonal ear lobe crease for evaluating coronary risk. Z Kardiol. 1995;84:512–9
- Davis TM, Balme M, Jackson D, et al. The diagonal ear lobe crease (Frank’s sign) is not associated with coronary artery disease or retinopathy in type 2 diabetes: the Fremantle Diabetes Study. Aust N Z J Med. 2000;30:573–7
- Koracevic G, Atanaskovic V. Ear lobe crease: point of disagreement in evidence-based medicine. Am J Forensic Med Pathol. 2009;30:89.
- Overfield T, Call EB. Earlobe type, race, and age: effects on earlobe creasing. J Am Geriatr Soc. 1983;31:479–81
- Petrakis NL, Koo L. Earlobe crease. Lancet. 1980;1:376
- Williams RR. Myocardial infarction risk, earlobe crease, and sleep apnoea syndrome. Lancet. 1989;2:676–7.
- Sapira JD. Earlobe creases and macrophage receptors. South Med J. 1991;84:537–8
- Singh M, Bedi US. Is atherosclerosis regression a realistic goal of statin therapy and what does that mean? Curr Atheroscler Rep. 2013;15:294.
- Rizzo M, Nikolic D, Banach M, et al. Statin treatment in the elderly: how much do we know? Arch Med Sci. 2013;9:585–8.
- Lucenteforte E, Romoli M, Zagli G, et al. Ear lobe crease as a marker of coronary artery disease: a meta-analysis. Int J Cardiol. 2014;175:171–5
- Athyros VG, Kakafika AI, Karagiannis A, et al. Do we need to consider inflammatory markers when we treat atherosclerotic disease? Atherosclerosis. 2008;200:1–12.
- Sinha N, Devabhaktuni S, Kadambi A, et al. Can echocardiographically estimated pulmonary arterial elastance be a non-invasive predictor of pulmonary vascular resistance? Arch Med Sci. 2014;10:692–700.
- Gluba-Brzozka A, Michalska-Kasiczak M, Franczyk-Skora B, et al. Markers of increased cardiovascular risk in patients with chronic kidney disease. Lipids Health Dis. 2014;13:135.
- Gibson TC, Ashikaga T. The ear lobe crease sign and coronary artery disease in aortic stenosis. Clin Cardiol. 1986;9:388–90.