Erythema marginatum
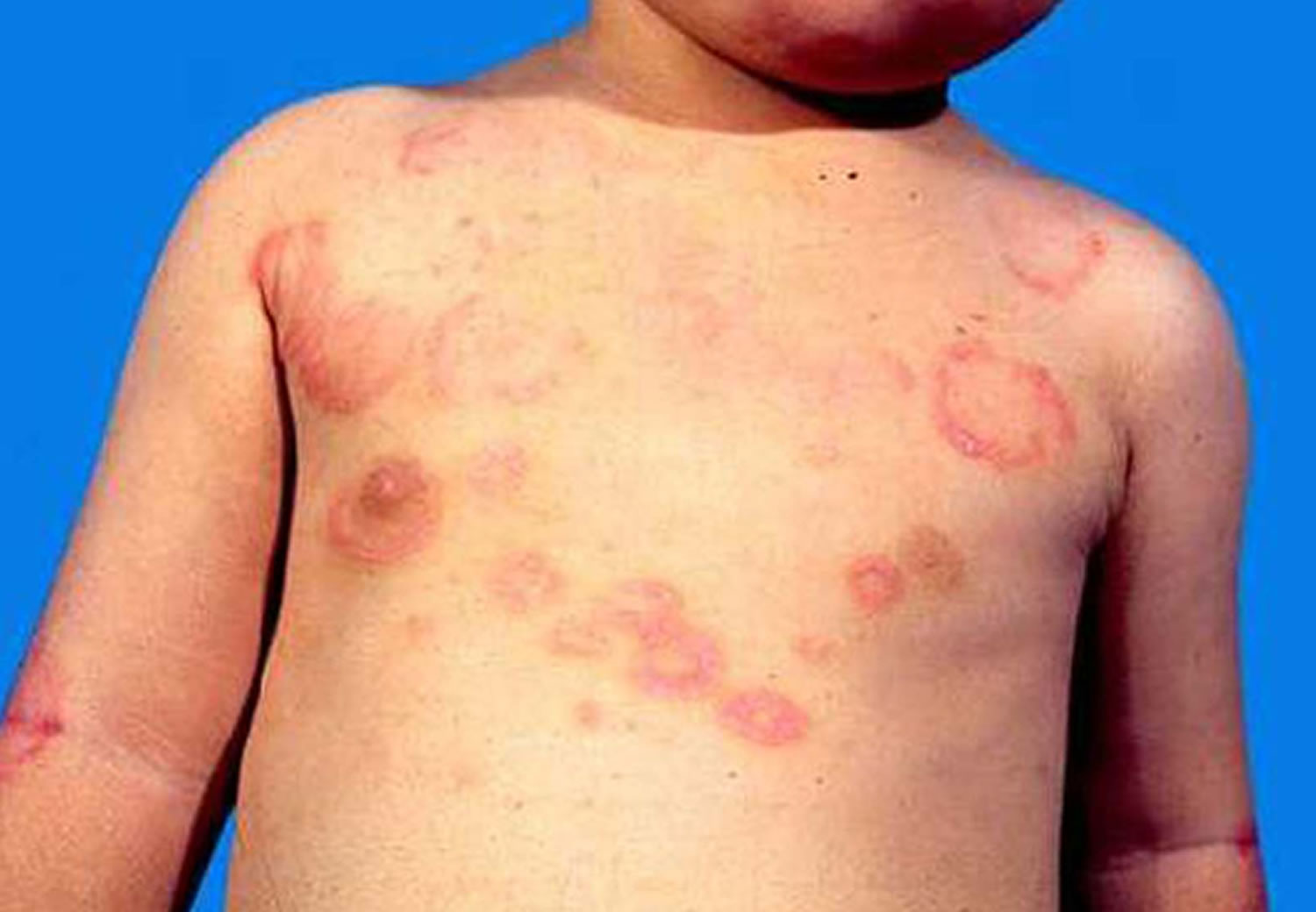
Erythema marginatum is described as the presence of pink rings with pale centers and rounded or serpiginous margins on the trunk and inner surfaces of the arms and legs which spread outwards in a circular shape and come and go (evanescent) for as long as several months. The rings are barely raised and are non-pruritic 1. The face is generally spared. Heat can induce its appearance, and it blanches with pressure. As with other rashes, erythema marginatum may be harder to detect in dark-skinned individuals. Erythema marginatum is a rash of acute rheumatic fever and may be associated with mild carditis (inflammation of heart muscle) 2.
Erythema marginatum occurs in less than 5% of patients with rheumatic fever, but is considered a major Jones criterion when it does occur. The four other major criteria include carditis, polyarthritis, Sydenham’s Chorea, and subcutaneous (Aschoff) nodules.
Some sources distinguish erythema marginatum into the following:
- Erythema marginatum rheumaticum
- Erythema marginatum perstans
Acute rheumatic fever is caused by a reaction to a bacterial infection with particular strains of group A streptococcus. It has long been thought that acute rheumatic fever only follows streptococcal pharyngitis (sore throat), however recent studies from Aboriginal populations in Australia have suggested streptococcal skin infection may precede some cases of acute rheumatic fever. Those who have experienced one episode of acute rheumatic fever are more likely to suffer recurrent attacks with subsequent group A streptococcal infections.
Acute rheumatic fever usually affects children aged 5–15 years. Most cases of acute rheumatic fever currently occur in developing countries. Worldwide there is an estimated 470 000 new cases of acute rheumatic fever annually (60% of whom eventually develop rheumatic heart disease). In most developed countries acute rheumatic fever is now rare, with a few notable exceptions; the highest documented rates of acute rheumatic fever in the world are in Maori and Pacific people in New Zealand, Aboriginal Australians, and those in Pacific Island nations.
Rheumatic fever is associated with poverty, overcrowding and poor sanitation facilities. It is suspected that there are genes that make some families more susceptible to the disease.
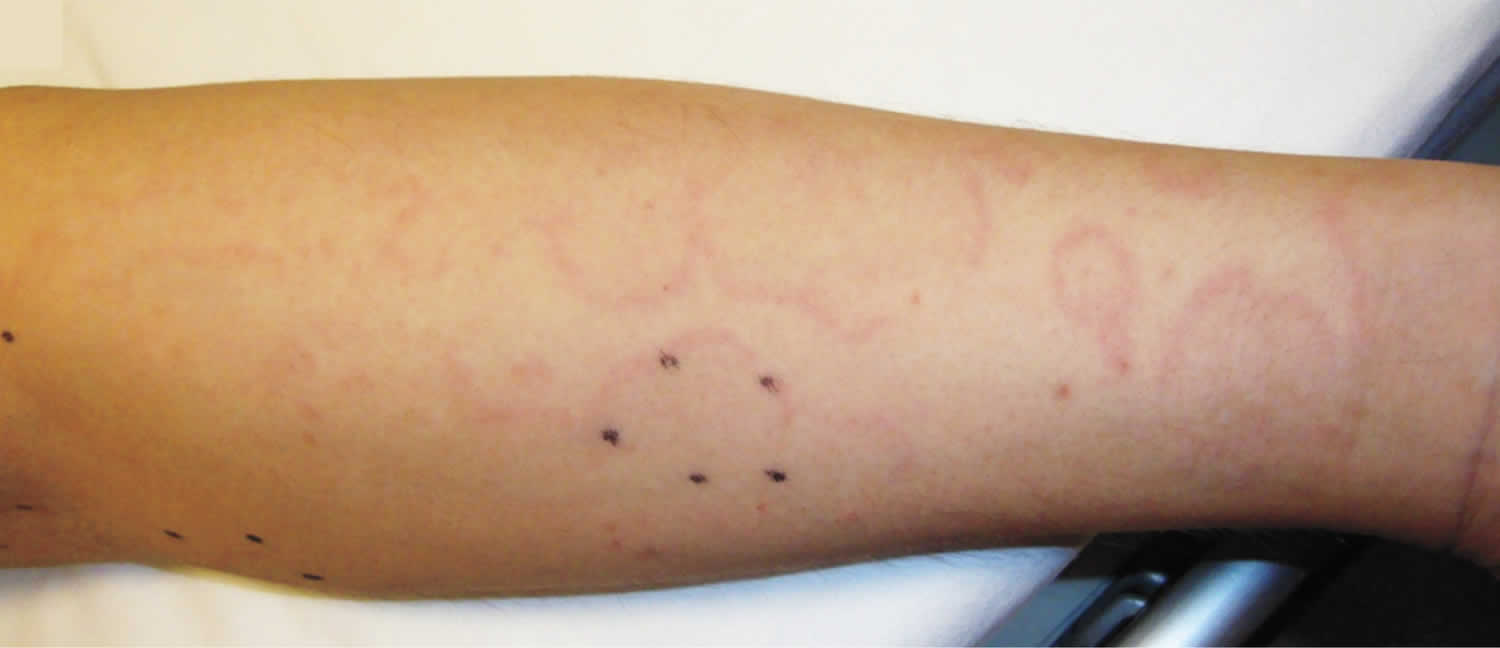
Figure 1. Erythema marginatum rash
Footnote: A previously healthy 36-year-old man presented with a 1-month history of fever and pain in both shoulders and knees, which had been preceded by a sore throat 2 weeks before the onset of fever. Laboratory studies were notable for a white-cell count of 13,800 per cubic millimeter (85% neutrophils), a C-reactive protein level of 26 mg per deciliter (reference value, ≤0.3), and an antistreptolysin O titer of 1478 IU per milliliter (reference value, <241). Transthoracic echocardiography revealed mild aortic regurgitation. His fever and arthralgias abated after the administration of a nonsteroidal antiinflammatory drug. One week later, painless, nonpruritic, red annular macules appeared on the upper limbs and abdomen. Image shows the right forearm; black ink dots indicate the diameter of one lesion 10 hours before the time that the photograph was taken). The rash migrated within hours and then faded over the course of a few days while new lesions appeared.
[Source 3 ]Clinical features of rheumatic fever
Symptoms of acute rheumatic fever generally develop several weeks after an episode of streptococcal pharyngitis. However, many patients do not recall having a sore throat. Non-specific symptoms include:
- Fever
- Abdominal pain
- Muscle aches
Acute rheumatic fever causes a variety of more specific clinical features:
- Polyarthritis (multiple inflamed joints) — Most often ankles, knees, elbows, wrists. Arthritis can migrate from one joint to another.
- Carditis (inflammation of the heart) – This involves the heart valves, heart muscle, and membrane surrounding the heart.
- Sydenham chorea – This is a disorder of the nervous system characterised by personality changes, muscle weakness, and involuntary movements.
Skin signs in acute rheumatic fever may include:
- Erythema marginatum rheumaticum – This is a characteristic type of annular erythema that occurs in about 10% of first attacks of acute rheumatic fever in children; it is very rare in adults. The rash can be difficult to detect in dark-skinned people. When present, it is found on the trunk and upper arms and legs, but almost never on the face, palms or soles. The rash appears as pink or red macules (flat spots) or papules (small lumps), which spread outwards in a circular shape. As the lesions advance, the edges become raised and red, and the centre clears. The lesions are not itchy or painful, and sometimes go unnoticed by the patient. The lesions can fade and reappear within hours, reappearing in hot conditions. Erythema marginatum may persist intermittently for weeks to months, even after successful treatment of acute rheumatic fever.
- Subcutaneous nodules (small lumps under the skin) – These are uncommon, occurring in less than 2% of patients with acute rheumatic fever. The painless nodules are found on extensor surfaces at specific joints such as the elbows, knees, ankles, wrists, and knuckles, the back of the scalp, and along the spinous processes of the thoracic and lumbar vertebrae. The nodules are firm, round, mobile, and range from 0.5-2 cm in size. The nodules are more often observed in patients who also have carditis. They usually resolve within one month but may persist for longer. They have not been found to have racial or population variability. As with erythema marginatum, subcutaneous nodules almost never occur as the sole major manifestation of acute rheumatic fever.
Rheumatic fever complications
The most severe complication of recurrent acute rheumatic fever is permanent damage to heart valves, known as rheumatic heart disease. The disease can result in permanent damage to:
- Heart valves, particularly the mitral valve and aortic valve, which can lead to valvular stenosis and/or regurgitation.
- Heart muscles, reducing pumping action ie causing heart failure.
- The membrane around the heart, causing pericarditis.
- Irregular heart rhythms, such as atrial fibrillation.
Rheumatic fever diagnosis
There is no definitive diagnostic test for acute rheumatic fever. The diagnosis of acute rheumatic fever is challenging, as there are no clinical features or diagnostic tests available to confirm or rule out this condition. Instead, the diagnosis is made using the Jones criteria. These criteria require evidence of a preceding group A streptococcus infection, and various combinations of the characteristic features above and other non-specific clinical features. A 2015 revised version of the Jones Criteria endorsed by the American Heart Association now includes the addition of subclinical carditis as a major criteria and stratification of the major and minor criteria based upon epidemiologic risk (e.g., low, moderate, or high risk populations) 4.
Tests to confirm evidence of a group A streptococcal infection include:
- Blood tests to look for elevated or rising antibodies to group A streptococcus. The most commonly used tests are the plasma antistreptolysin O and the antideoxyribonuclease B titres.
- Culture of throat swabs and rapid antigen tests for group A streptococcus are less accurate.
Other tests used in the assessment of a patient with suspected acute rheumatic fever include:
- Blood tests – markers of inflammation, such as erytrocyte sedimentation rate (ESR) or C-reactive protein (CRP), may be raised
- Electrocardiogram and echocardiogram to identify heart involvement
- Doppler and colour flow mapping to detect minor valvular defects not evident clinically
Table 1: Revised Jones Criteria for diagnosing acute rheumatic fever
| Part A. For all patient populations with evidence of preceding group A strep infection | ||
|---|---|---|
| Diagnosis: Initial acute rheumatic fever | 2 major manifestations or 1 major plus 2 minor manifestations | |
| Diagnosis: Recurrent acute rheumatic fever | 2 major manifestations or 1 major plus 2 minor manifestations or 3 minor manifestations | |
| Low-risk populations* | Moderate- and high-risk populations* | |
| Part B. Major manifestations | Carditis
Arthritis
Chorea Erythema marginatum Subcutaneous nodules | Carditis
Arthritis
Chorea Erythema marginatum Subcutaneous nodules |
| Part C. Minor manifestations | PolyarthralgiaFever (≥38.5oC) Elevated acute phase reactants (ESR ≥60 mm in the first hour and/or CRP ≥3.0 mg/dl) Prolonged PR interval on electrocardiography, after accounting for age variability (unless carditis is a major criterion) | MonoarthralgiaFever (≥38oC) Elevated acute phase reactants (ESR ≥30 mm/hr and/or CRP >3.0 mg/dl) Prolonged PR interval on electrocardiography, after accounting for age variability (unless carditis is a major criterion) |
Footnote: * Low-risk population is defined as an acute rheumatic fever incidence of <2 per 100,000 school-aged children or all age rheumatic heart disease prevalence of ≤1 per 1000 population per year. Those not included in the low-risk population are defined as moderate or high risk depending upon their reference population.
Abbreviations: ARF = acute rheumatic fever; ESR = erythrocyte sedimentation rate; CRP = C-reactive protein; mm = millimeters; mg/dl = milligrams per deciliter
Erythema marginatum causes
Erythema marginatum is the skin manifestation of acute rheumatic fever, which is is a delayed complication of pharyngitis due to Streptococcus pyogenes, which are also called group A Streptococcus or group A strep.
Risk factors for rheumatic fever
Inadequate or lack of antibiotic treatment of streptococcal pharyngitis increases the risk of someone developing acute rheumatic fever. In approximately one-third of patients, acute rheumatic fever follows subclinical streptococcal infections or infections for which medical attention was not sought 5.
Individuals with a history of acute rheumatic fever have an increased risk of recurrence with subsequent streptococcal pharyngeal infections 6. The risk of recurrence after streptococcal infection is highest within the first few years after the initial attack and then declines.
The incidence of acute rheumatic fever is highest in children between the ages of 5 and 15 years. Acute rheumatic fever is very rare in children 3 years of age and younger in the United States. First-onset acute rheumatic fever is rare in adults, although recurrence may occur through adulthood 7.
Crowding, such as found in schools, military barracks, and daycare centers, increases the risk of spreading group A strep and thus increases the risk of developing acute rheumatic fever.
Erythema marginatum differential diagnosis
Several skin conditions should be considered in the differential diagnosis of erythema marginatum. Conditions to consider include other forms of annular erythema.
- Erythema perstans — a paraneoplastic eruption associated with underlying malignancy in which there are concentric and whirling rings.
- Erythema gyratum repens — a paraneoplastic rash with a typical ‘wood grain’ appearance from rapidly expanding erythematous lines in a concentric pattern.
- Necrolytic migratory erythema — ring-shaped red rashes that blister, erode, and crust over time. It classically occurs with an underlying glucagonoma.
- Erythema annulare centrifugum — is a chronic reactive form of annular erythema characterized by erythematous, circular, arciform and polycyclic lesions with characteristic delicate scale behind the advancing edge (‘trailing scale’). It is characterized by a small pink, infiltrated papule which slowly enlarges and forms a ring as the central area flattens and fades. The disease may be self limiting or chronic with periodic fluctuations or persistent over many years. It represents an isolated condition.
- Erythema multiforme — targetoid lesions occurring on the backs of hands and tops of feet (but may occur anywhere). The lesions consist of sharply demarcated reddish pink macules that gradually enlarge to form plaques. The central part changes colour or clears, creating rings.
- Erythema migrans (the first stage of Lyme disease) — an expanding red patch of skin that starts at the site of the tick bite and gradually expands to reach several dozens of centimetres in size.
Other disorders to be considered include:
- Tinea (dermatophyte infection) — gradually enlarging, itchy and scaly annular lesions with central clearing
- Granuloma annulare — an annular rash with a rubbery raised smooth erythematous edge with central clearing
- Erythema papulatum centrifugum — a sweat-related itchy condition where erythematous papules form enlarging annular and arciform structures on the trunk and limbs
- Secondary syphilis may present with scaly annular and polycyclic plaques which tend not to be itchy
- Cutaneous lupus erythematosus especially subacute cutaneous lupus erythematosus and systemic lupus erythematosus.
- Annular urticaria (pruriginous and not associated with systemic symptoms of rheumatic fever)
- Still’s disease (skin rash is different: it is maculo-papular, salmon pink in colour and usually occurs at the same time as high fever)
- Hereditary periodic fever syndromes (recurrent febrile episodes associated to erisipela-like erythemas, positive familial anamnesis for periodic fever)
- Kawasaki syndrome (the diagnosis requires fever (>39° C) of at least 5 days duration and the presence of four of the following: changes in extremities including erythema, edema, and desquamation, bulbar conjunctivitis, polymorphous rash, Cervical lymphadenopathy, changes in the lips and oral cavity such as pharyngeal erythema, fissured lips, and strawberry tongue).
- Hereditary angioedema (an appearance similar to erythema marginatum can precede this condition).
- Psittacosis (erythema marginatum has been reported in association with this pneumologic infection).
Annular scaly plaques are also common in discoid eczema, chronic plaque psoriasis, seborrhoeic dermatitis, pityriasis rosea, porokeratosis, and sarcoidosis.
Erythema marginatum treatment
Erythema marginatum rash has no specific therapy. Its clinical course is unaltered by the treatment of the underlying rheumatic fever. Lesions are asymptomatic, with at least mild pruritus. In this case, oral antihistamines could be used: Cetrizine (2-6 years: 5mg/day; >6 years: 10mg/day); Oxatomide (<15 kg: 0.5 mg/kg twice/day; 15-35 kg: 15 mg twice/day; adults: 30 mg twice/day.
Patients with acute rheumatic fever should start on therapy for the symptomatic management of acute rheumatic fever, including salicylates and anti-inflammatory medicines to relieve inflammation and decrease fever, as well as management of cardiac failure. These patients should also be started on antibiotics for treatment of group A strep pharyngitis, regardless of the presence or absence of pharyngitis at the time of diagnosis, in order to eradicate any residual group A strep carriage 6.
Secondary prevention of rheumatic fever requires antibiotic prophylaxis to reduce the likelihood of recurrent attacks in persons with a history of acute rheumatic fever. Because acute rheumatic fever frequently recurs with subsequent group A strep pharyngitis infections, long-term prophylaxis duration should be individually tailored but is usually indicated at least until age 21. Prophylaxis typically involves an intramuscular injection of benzathine penicillin every 4 weeks or oral penicillin V twice daily. Sulfadiazine or oral macrolides can be taken daily by individuals who are allergic to penicillin 8. Current American Heart Association guidelines no longer recommend bacterial endocarditis prophylaxis for patients with rheumatic heart disease, unless the patient has a prosthetic valve 9.
The spread of group A strep infection can be reduced by good hand hygiene, especially after coughing and sneezing and before preparing foods or eating, and respiratory etiquette (e.g., covering your cough or sneeze). Treating an infected person with an antibiotic for 24 hours or longer generally eliminates their ability to transmit the bacteria. Thus, people with group A strep pharyngitis should stay home from work, school, or daycare until afebrile and until at least 24 hours after starting appropriate antibiotic therapy.
References- Sailer, Christian, Wasner, Susanne. Differential Diagnosis Pocket. Hermosa Beach, CA: Borm Bruckmeir Publishing LLC, 2002:77 ISBN 1591032016
- Kahan, Scott, Smith, Ellen G. In A Page: Signs and Symptoms. Malden, Massachusetts: Blackwell Publishing, 2004:68 ISBN 140510368X
- Acute Rheumatic Fever with Erythema Marginatum. N Engl J Med 2016; 375:2480 DOI: 10.1056/NEJMicm1601782 https://www.nejm.org/doi/full/10.1056/NEJMicm1601782
- Gewitz MH, Baltimore RS, Tani LY, et al. Revision of the Jones Criteria for the diagnosis of acute rheumatic fever in the era of Doppler echocardiography: A scientific statement from the American Heart AssociationExternal. Circulation. 2015;131:1806. https://ahajournals.org/doi/full/10.1161/CIR.0000000000000205
- Shulman ST, Bisno AL. Nonsupprative poststreptococcal sequelae: Rheumatic fever and glomerulonephritis. In Bennett J, Dolin R, Blaser M, editors. 8th Mandell, Douglas, and Bennett’s Principles and Practice of Infectious Diseases. Philadelphia (PA): Elsevier. 2015;2:2300–9.
- Gerber MA, Baltimore RS, Eaton CB, et al. Prevention of rheumatic fever and diagnosis and treatment of acute streptococcal pharyngitis: A scientific statement from the American Heart Association Rheumatic Fever, Endocarditis, and Kawasaki Disease Committee of the Council on Cardiovascular Disease in the Young, the Interdisciplinary Council on Functional Genomics and Translational Biology, and the Interdisciplinary Council on Quality of Care and Outcomes Research: Endorsed by the American Academy of PediatricsExternal. Circulation. 2009;119(11):1541–51.
- Shulman ST, Bisno AL, Clegg HW, Gerber MA, Kaplan EL, Lee G, et al. Clinical practice guideline for the diagnosis and management of group A streptococcal pharyngitis: 2012 update by the Infectious Diseases Society of AmericaExternal. Clin Infect Dis. 2012;55(10):1279–82.
- Committee on Infectious Diseases. Group A streptococcal infectionsExternal. In Kimberlin DW, Brady MT, Jackson MA, Long SS, editors. 30th ed. Red Book: 2015 Report of the Committee on Infectious Diseases. Elk Grove Village (IL): American Academy of Pediatrics; 2015:732–7.
- Wilson W, Taubert K, Gewitz M, et al. Prevention of Infective Endocarditis: Guidelines from the American Heart Association: A Guideline from the American Heart Association Rheumatic Fever, Endocarditis, and Kawasaki Disease Committee, Council on Cardiovascular Disease in the Young, and the Council on Clinical Cardiology, Council on Cardiovascular Surgery and Anesthesia, and the Quality of Care and Outcomes Research Interdisciplinary Working GroupExternal. Circulation. 2007;116:1736–54.