Frontal fibrosing alopecia
Frontal fibrosing alopecia is a type of scarring hair loss along the frontal scalp hair margin (i.e. the forehead and sideburns). This happens due to inflammation and destruction of the hair follicles. There may also be hair loss from the scalp near the ears and from the eyebrows. Sometimes hair loss can also occur from other parts of the body, but this is less common 1. Frontal fibrosing alopecia was first described in a group of Australian post-menopausal women in 1994 2. Frontal fibrosing alopecia is believed to be localized form of lichen planopilaris. It most often affects white postmenopausal women over the age of 50, but it can also affect men and younger women and people of other ethnicities. Frontal fibrosing alopecia incidence is reported to be increasing in white-skinned women (possibly because of greater awareness of the condition), and it is uncommon in women with dark skin.
Frontal fibrosing alopecia may be due to hormonal changes or an autoimmune response, the exact cause of this condition is not yet known.
Frontal fibrosing alopecia presents as a progressive symmetric band-like alopecia (hair loss), affecting the frontal hair line, the preauricular scalp and, less commonly and distinctively, the retroauricular areas. ”Orphaned” hairs ie isolated hairs, may remain in areas of hair loss. The eyebrows are often affected and this may occur before the frontal scalp. Clinical inflammation is not observed in the eyebrows. The other vellus or terminal hair of the face can be involved, including the eyelashes. Additional clinical features – atrophy of affected sites with prominent forehead veins and facial papules. Progression, for the majority, is relatively slow
Dermoscopic features – clearly perifollicular, with keratin scale surrounding and extending along the proximal part of the hair shafts. Erythema often mild or absent.
There are a number of treatments that are used for frontal fibrosing alopecia to help to slow down or halt further hair loss in some people. Unfortunately, their success is variable and some people cannot find a treatment that is effective for them. Treatments used to slow the progression of the condition include oral corticosteroids, intralesional steroid injections, anti-inflammatory antibiotics such as tetracyclines, or anti-malarial tablets (hydroxychloroquine). All these treatments aim to lower the activity of the immune system and slow down the attack on the hair follicles.
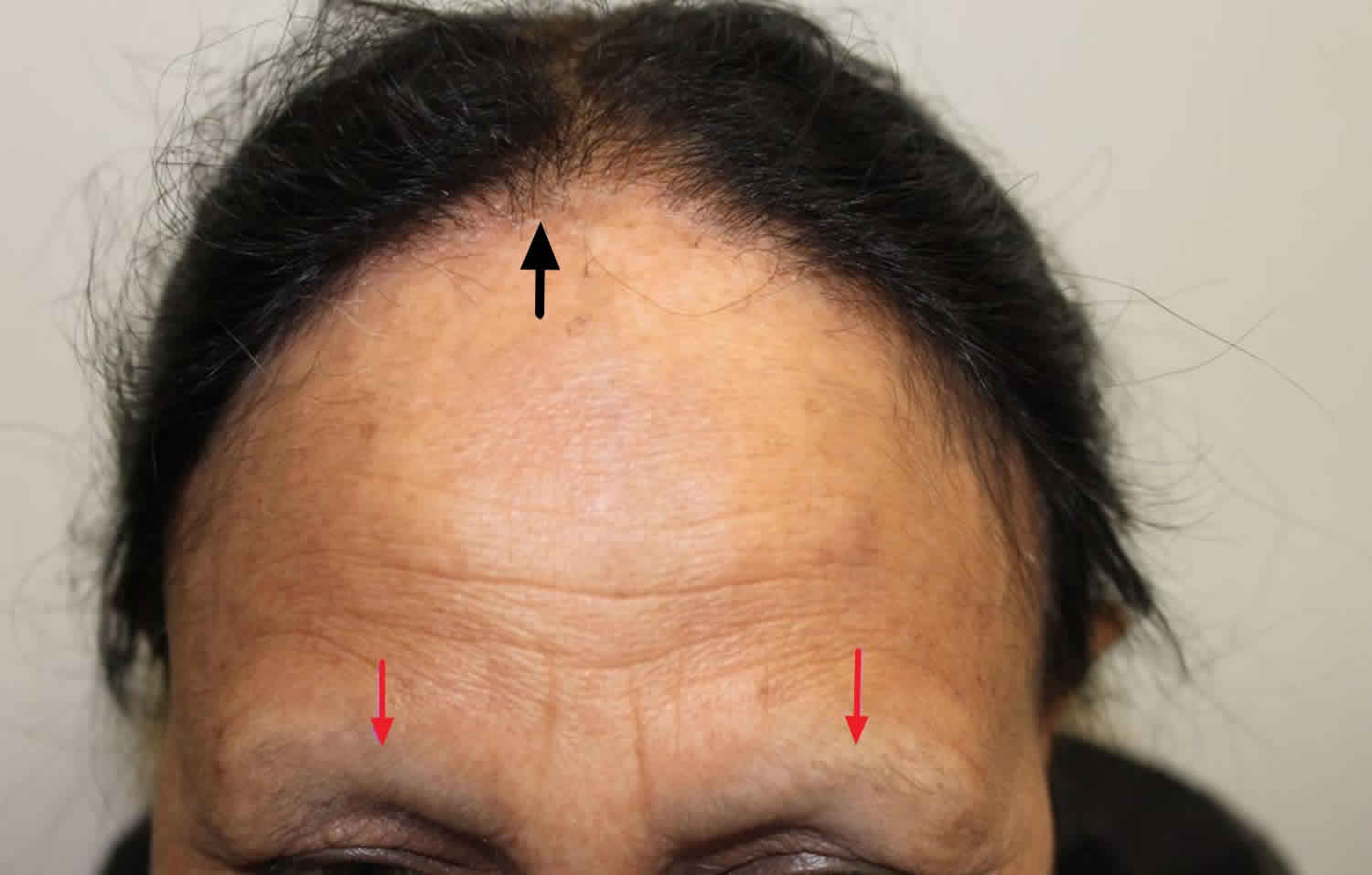
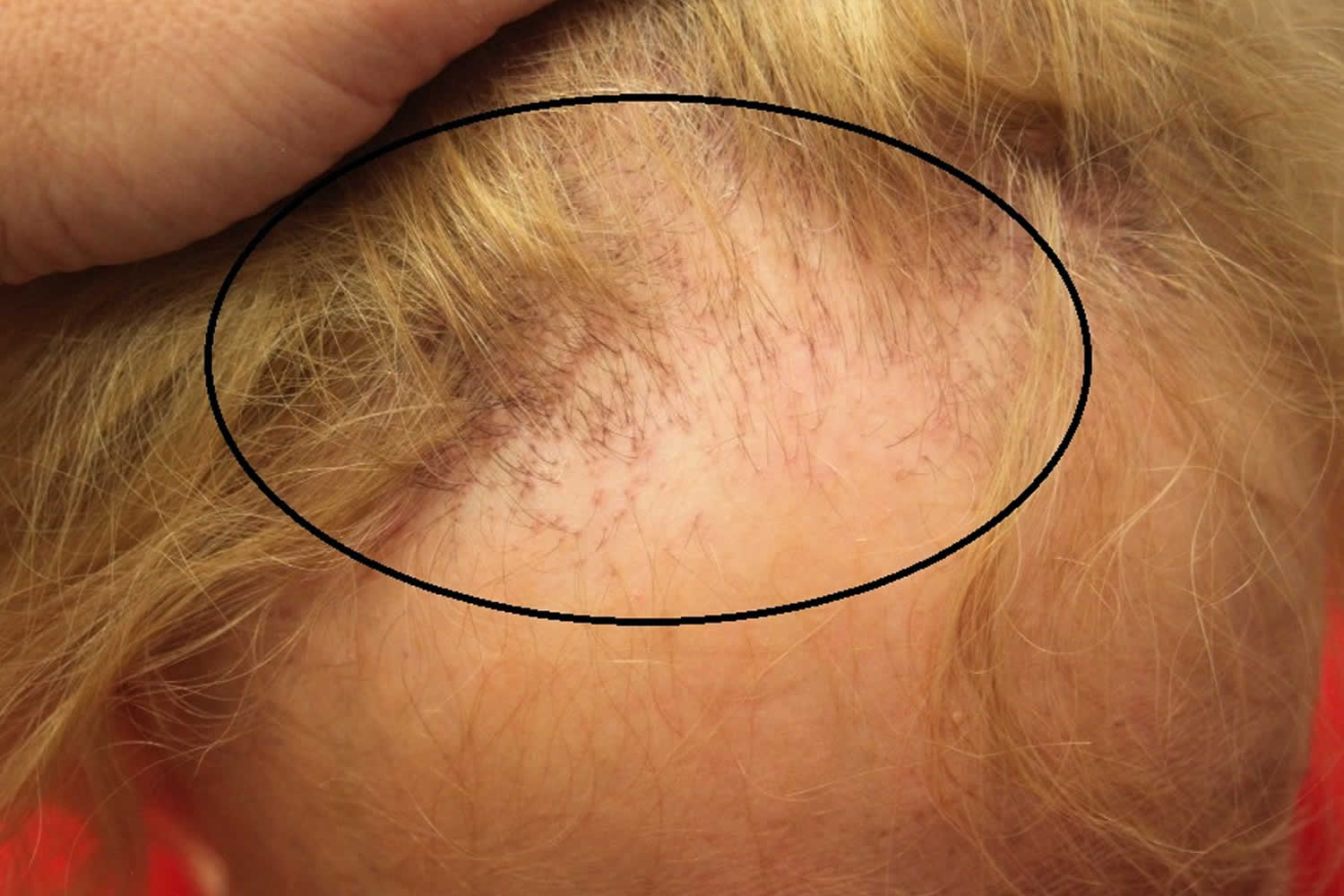
Figure 1. Frontal fibrosing alopecia
Is frontal fibrosing alopecia permanent?
Yes, in frontal fibrosing alopecia, the hair follicles are destroyed and turned into scar tissue. Frontal fibrosing alopecia is a slowly progressive condition, which means that the areas of the scalp that are affected by the condition will gradually increase over time. In some people, the condition stops progressing and there have been some rare reports of regrowth.
Can frontal fibrosing alopecia be cured?
There are treatments that help to slow down or halt further hair loss in some people. These may be of help in follicles that are inflamed but not yet lost. Unfortunately once hair follicles have been completely lost, the skin develops a smooth shiny appearance, and the follicles and their hair cannot then regrow. There is no treatment that can cure frontal fibrosing alopecia, in areas where the follicles have gone.
Who gets frontal fibrosing alopecia?
Although the typical patient with frontal fibrosing alopecia was described as a Caucasian post-menopausal woman over the age of 50, younger women, men, and children, and all ethnic groups including Asians, Hispanics, and those of African descent can be affected.
The incidence is reported to be increasing worldwide.
Frontal fibrosing alopecia is frequently reported in patients with hypothyroidism, contact allergy to fragrances, regular sunscreen use, and autoimmune diseases including lupus erythematosus and rheumatoid arthritis.
How do clinical features differ in various types of skin?
Women of African descent with frontal fibrosing alopecia present differently from Caucasian women. Typically they present at a younger age, often in their early 40s before menopause. Itch, redness, and scale are less obvious. Lichen planus pigmentosus is commonly associated, and usually precedes the hair loss. Speckled pigmentation of hair follicles along the frontal hair margin is seen on dermoscopy. Frontal fibrosing alopecia may be overlooked due to associated traction alopecia.
What is lichen planopilaris?
Lichen planopilaris is a rare inflammatory condition that results in patchy progressive permanent hair loss mainly on the scalp. Three forms are recognized 3:
- Classic lichen planopilaris, also known as follicular lichen planus
- Frontal fibrosing alopecia
- Graham Little syndrome
Lichen planopilaris usually affects young adult women, although the age range is wide and it also affects men. It commonly develops in association with lichen planus affecting the skin, mucosa and nails.
The cause of lichen planopilaris is unknown.
Although lichen planopilaris is rare, it is one of the common causes of scarring hair loss of the scalp.
The hair loss caused by lichen planopilaris cannot be reversed, however, progression of the condition can be limited in some people. Treatments used to slow the progression of the condition include anti-inflammatory agents, including corticosteroids, ciclosporin and hydroxychloroquine. Some recent reports have also shown success using JAK-inhibitors to treat lichen planopilaris in a small number of patients.
Frontal fibrosing alopecia causes
The exact underlying cause of frontal fibrosing alopecia is unknown. Genetic studies of frontal fibrosing alopecia suggest that this is an autoimmune condition, in which an affected person’s immune system mistakenly attacks the hair follicles (structures in the skin that make hair) and destroys them. There is a disturbed immune response to some component of the intermediate-sized and vellus scalp hair follicles. Although triggers are not yet clear, hormones and other environmental factors are thought be involved. A 2016 study suggests that there are both genetic and environmental components involved in frontal fibrosing alopecia. An androgen-dependent etiology has been suggested by the predominance of post-menopausal patients. Contact allergy or photocontact allergy to cosmetics, moisturizing creams, hair dye, and sunscreens have been suggested as possible but unconfirmed causative factors 4.
There are several descriptions of multiple family members all being affected by frontal fibrosing alopecia, so there is likely to be a hereditary element to this condition, although not everyone with frontal fibrosing alopecia has a relative with the condition. Genetic studies, however, have been lacking.
Frontal fibrosing alopecia has been considered a variant of lichen planopilaris due to the resemblance on histology and an association with various forms of lichen planus, but there are also many differences that raise doubts.
Frontal fibrosing alopecia symptoms
Frontal fibrosing alopecia is characterized primarily by a usually symmetrical band of hair loss (alopecia) and scarring on the front and sides of the scalp, resulting in a receding frontal hair line. The edge may appear moth-eaten, and single ‘lonely’ hairs may persist in the bald areas. The band of hair loss on the front and sides of the scalp is usually symmetrical and slowly progressive (worsening over time). Atypical patterns of loss include a diffuse zig-zag pattern, a pseudo-fringe-sign, or continuous involvement all the way around the hair margin both front and back. Approximately half of all affected people experience eyebrow thinning or loss (madarosis) as well, which often precedes the scalp changes. Less commonly, the eyelashes may also be involved. Some people with frontal fibrosing alopecia develop hair loss in areas other than the scalp and face. Hair loss can affect all parts of the body, and almost total loss from limbs is common. In men, loss of beard and sideburns is described and may be the only site of involvement. Some women with frontal fibrosing alopecia also have female pattern hair loss, which is associated with thinning of hair on the scalp due to increased hair shedding and/or a reduction in hair volume.
Itch and pain are common early symptoms, and may occur before any obvious loss of hair density. Facial rashes are another potentially early sign. These may present as skin colored or yellowish follicular papules located on the forehead and temples, diffuse erythema or red dots around hairs 5.
The skin in the affected area lacks the sundamage seen on the forehead, allowing assessment of the extent of the recession. It looks pale, shiny, or mildly scarred, without visible hair follicle openings. During the active phase, close inspection or dermatoscopy, shows redness and scaling is visible around involved hairs. Single ‘lonely’ hairs often persist in the bald areas. The hair pull test is negative.
Trichoscopy (dermoscope for the scalp and hair) reveals absent follicles, white dots, tubular perifollicular scale and perifollicular erythema. In skin that tans easily, perifollicular pigmentation may be observed.
Androgenetic alopecia (male pattern hair loss, female pattern hair loss) is commonly associated and may lead to missed diagnosis.
Frontal fibrosing alopecia diagnosis
The clinical features of frontal fibrosing alopecia are characteristic. Frontal fibrosing alopecia is usually diagnosed using a combination of trichoscopy (examining the hair and scalp using a microscope) often accompanied by a scalp biopsy from the edge of the affected area to confirm the diagnosis. The histopathological features of frontal fibrosing alopecia are identical to those of lichen planopilaris.
Biopsy of skin papules may also show a lichenoid pattern of inflammation, fibrosing alopecia, and sebaceous gland hyperplasia.
Frontal fibrosing alopecia diagnostic criteria have been proposed:
- Major criteria:
- scarring hair loss of the frontal, frontotemporal, or temporal scalp in the absence of follicular keratotic papules on the body
- scarring loss of eyebrows.
- Minor criteria:
- redness and scale around hair follicles, or solitary ‘lonely’ hairs, best seen on dermoscopy
- characteristic histology on skin biopsy
- similar clinical signs involving other body sites
- noninflammatory facial papules
- itch or pain preceding or concurrently at sites of involvement.
Diagnosis requires two major criteria or one major and two minor criteria.
Recommended blood tests include hematology, biochemistry, thyroid function tests and ANA. Hormone status may assessed if there are other clinical features to suggest hyperandrogenism. Patch testing should be considered.
Frontal fibrosing alopecia differential diagnosis
Important diagnoses to consider include female pattern hair loss, chronic telogen effluvium and alopecia areata.
- Female pattern hair loss is a non-scarring progressive miniaturization of the hair follicle with one of three different characteristic patterns.
- Chronic telogen effluvium is an idiopathic disease causing increased hair shedding and bi-temporal recession, usually in middle aged women.
- Alopecia areata is an autoimmune attack of hair follicles that usually causes hair to fall out in small round patches.
Frontal fibrosing alopecia treatment
The hair loss caused by frontal fibrosing alopecia cannot be reversed and there are no truly effective treatments to date. Treatments used to slow the progression of hair loss include oral corticosteroids, intralesional steroid injections, anti-inflammatory antibiotics such as tetracyclines, or anti-malarial tablets (hydroxychloroquine). All these treatments aim to lower the activity of the immune system and slow down the attack on the hair follicles.
Frontal fibrosing alopecia treatments include:
- Topical corticosteroids. Potent steroid gels, lotions or creams applied to the skin on the front of the scalp can be helpful. They may also be used alongside other treatments as they may not slow hair line recession on their own.
- Topical Tacrolimus. An ointment or cream that acts by suppressing the immune system and calming the inflammation where it is applied.
- Intralesional steroids. Injections of steroid into the skin on the front of the scalp can be used. This helps to settle the inflammation and slow or halt the progression of hair line recession. This treatment may need to be repeated.
- Antibiotics e.g. tetracycline, doxycycline. Thesemedicines are chiefly used to help reduce inflammation and not for their antibiotic action. They can help to relieve the symptoms and redness of the scalp.
- Hydroxychloroquine. This may help frontal fibrosing alopecia become inactive in some people. It will usually require a trial of 4-6 months. It is uncertain how this drug works in this condition. It carries a small risk of damage to your eyesight and annual eye tests are required.
- Immunomodulatory drugs e.g. mycophenolate mofetil. These can help to dampen down the immune system and prevent the inflammation around the hair follicles. In some people it can slow or halt hair loss.
- Antiandrogen treatments e.g. oral finasteride and dutasteride. These treatments work by maintaining levels of testosterone (a hormone naturally found in men and women) in the hair follicles. Reduced levels of testosterone have been associated with a different type of hair loss called female/male pattern alopecia. This may occur with frontal fibrosing alopecia also contributing to hair loss. Treatment with antiandrogens may be of benefit where the two conditions occur together.
The 5-alpha-reductase inhibitors finasteride and dutasteride have been reported to stop further hair loss but this may be due to associated androgenetic alopecia 6. Immunosuppressants tried include ciclosporin and mycophenolate mofetil.
The use of the antidiabetic agent pioglitazone (off-label) for the treatment of frontal fibrosing alopecia was reported to reduce symptoms, inflammation, and progression of frontal fibrosing alopecia 7, but its use has not been supported by further investigations 8. Side effects include ankle swelling and weight gain.
Rituxomab and adalimumab are novel new treatments. Adalimumab, a tumor necrosis factor-alpha (TNFα) inhibitor, has also been reported to be effective in a few patients 9.
Hair grafting may be considered once disease activity has settled.
Frontal fibrosing alopecia cure
Unfortunately, there is currently no cure for frontal fibrosing alopecia.
Frontal fibrosing alopecia prognosis
The long-term outlook (prognosis) for people with frontal fibrosing alopecia varies. Usually, frontal fibrosing alopecia is slowly progressive (worsening over time); however, the condition does stabilize after a few years in some patients. The hair line recedes on average of 1.8-2.6 cm. As it is a scarring alopecia, hair does not regrow unless treatment is instituted early in the process. Hair regrowth has been reported in some patients.
References- Arakelyan, Hayk. (2019). Frontal Fibrosing Alopecia. https://www.researchgate.net/publication/337006698_Frontal_Fibrosing_Alopecia
- Kossard S. Postmenopausal frontal fibrosing alopecia. Scarring alopecia in a pattern distribution [published correction appears in Arch Dermatol 1994 Nov;130(11):1407]. Arch Dermatol. 1994;130(6):770–774. doi:10.1001/archderm.1994.01690060100013
- Lichen planopilaris. https://dermnetnz.org/topics/lichen-planopilaris
- Kumaran MS, Razmi T M, Vinay K, Parsad D. Clinical, dermoscopic, and trichoscopic analysis of frontal fibrosing alopecia associated with acquired dermal macular hyperpigmentation: A cross sectional observational case-control study. J Am Acad Dermatol. 2018;79(3):588–591. doi:10.1016/j.jaad.2018.03.001
- Pirmez, Rodrigo et al. Histopathology of facial papules in frontal fibrosing alopecia and therapeutic response to oral isotretinoin. Journal of the American Academy of Dermatology , Volume 78 , Issue 2 , e45. https://doi.org/10.1016/j.jaad.2017.10.038
- Frontal fibrosing alopecia. https://dermnetnz.org/topics/frontal-fibrosing-alopecia
- Mesinkovska, Natasha Atanaskova et al. The use of oral pioglitazone in the treatment of lichen planopilaris. J Am Acad Dermatol 2015; 72:355–356
- Tziotzios C, Brier T, Lee JYW, Saito R, Hsu CK, Bhargava K, Stefanato CM, Fenton DA, McGrath JA. Lichen planus and lichenoid dermatoses: Conventional and emerging therapeutic strategies. J Am Acad Dermatol. 2018 Nov;79(5):807-818. doi: 10.1016/j.jaad.2018.02.013
- Alam MS, LaBell B. Treatment of lichen planopilaris with adalimumab in a patient with hidradenitis suppurativa and rheumatoid arthritis. JAAD Case Reports 2020; 6(3): 219 – 221.