Fundal height
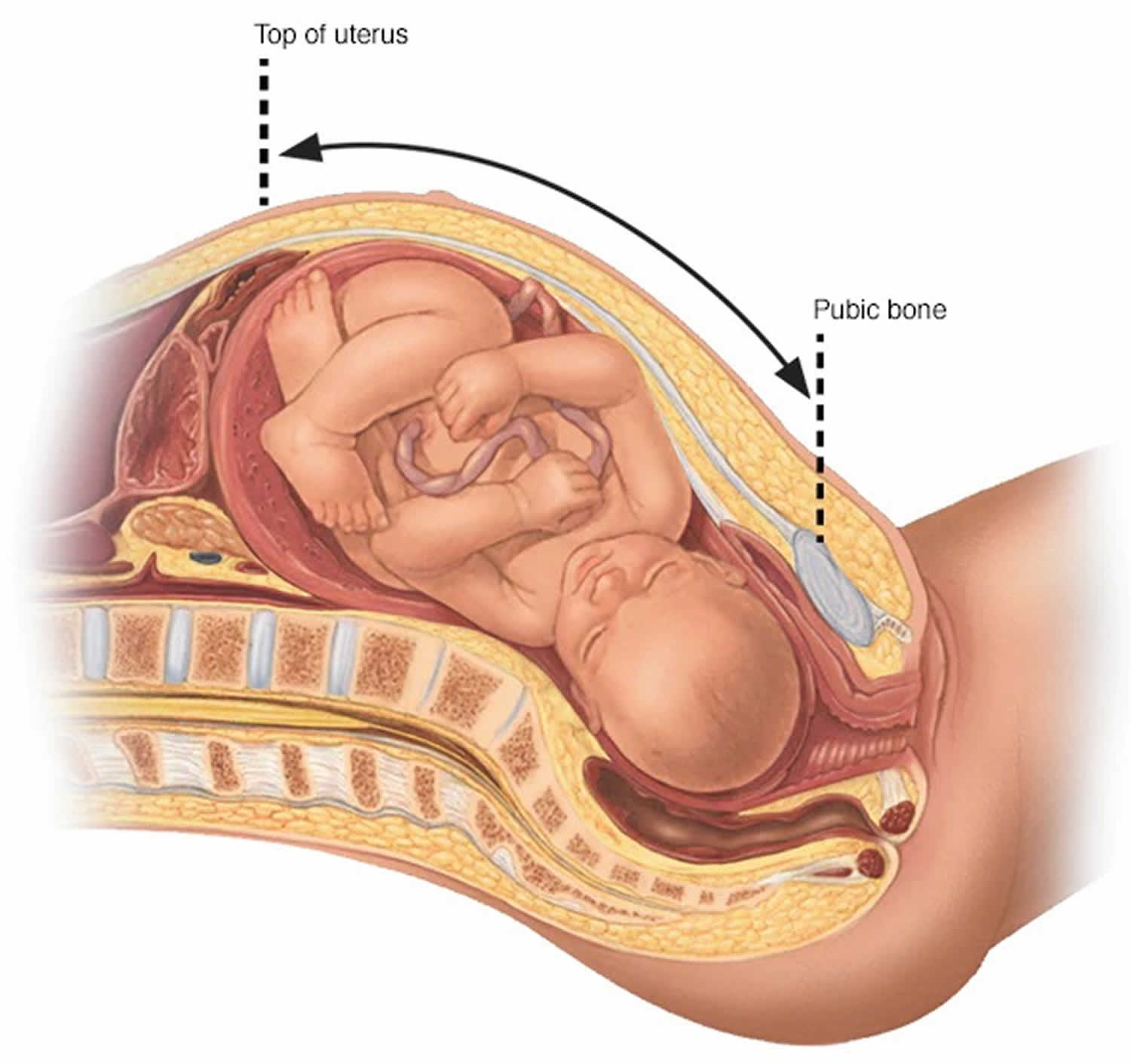
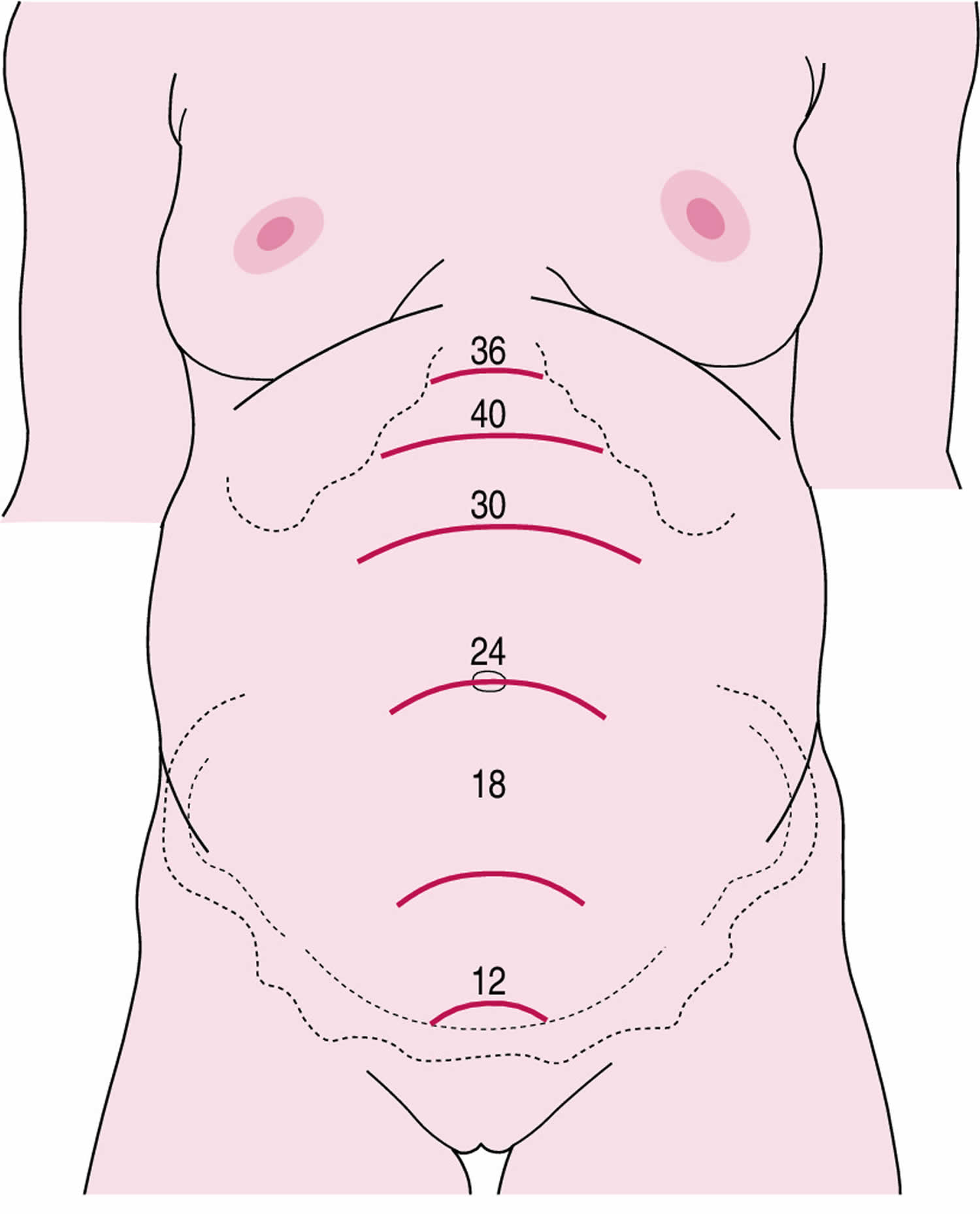
Fundal height is generally defined as the distance from the pubic bone to the top of the uterus measured in centimeters. After 20 weeks of pregnancy, your fundal height measurement often matches the number of weeks you’ve been pregnant 1. For example, if you’re 27 weeks pregnant, your health care provider would expect your fundal height to be about 27 centimeters.
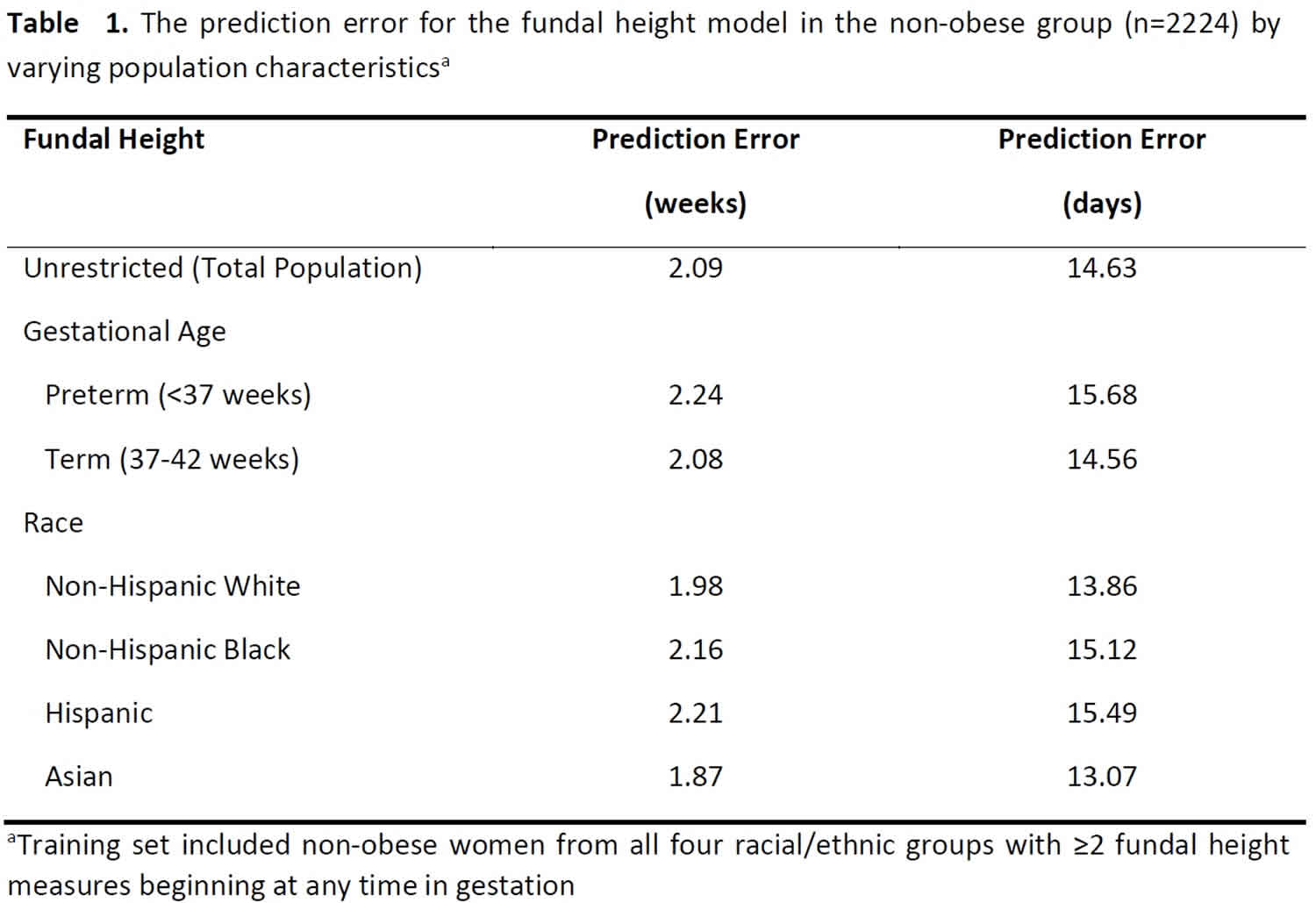
Overall, the prediction of gestational age from longitudinal measures of fundal height in a non-obese population was robust when applied to individual maternal races and preterm versus term deliveries with a variation of only 13.1 to 15.5 days (see Table 1 below) 2. Table 2 illustrates the accuracy of longitudinal measures of fundal height in predicting gestational age under varying clinical situations such as the frequency of prenatal visits or onset of prenatal care. The prediction error improved by 2.31 days as the frequency of measurements increased from two to four visits. The inclusion of fundal height measurements beginning after 20 weeks [Median (SD) number of measurements; 11 (3.3)] versus including measurements prior to 20 weeks minimally improved the accuracy of the predictor (14.1 versus 14.6 days). The error was slightly increased (15.4 days) when the gestational age of 20 weeks was estimated based on a 20cm fundal height [Median (SD) number of measurements; 11 (3.4)]. Furthermore, in potential scenarios of late prenatal care with measurements beginning after 28 weeks [Median (SD) number of measurements; 8 (2.7)], the error increased from 14.1 to 16.1 days 2.
A fundal height measurement might be less accurate, however, if you:
- Are obese
- Have a history of fibroids
- Are carrying twins or other multiples
A fundal height that measures smaller or larger than expected — or increases more or less quickly than expected — could indicate conditions such as:
- Slow fetal growth (intrauterine growth restriction)
- A significantly larger than average baby (fetal macrosomia)
- Too little amniotic fluid (oligohydramnios)
- Too much amniotic fluid (polyhydramnios)
Depending on the circumstances, your health care provider might recommend an ultrasound to determine what’s causing the unusual measurements or more closely monitor your pregnancy.
But fundal height is only a tool for gauging fetal growth — it’s not an exact science. Typically, fundal height measurements offer reassurance of a baby’s steady growth. If you’re concerned about your fundal height measurements, ask your health care provider for details.
Figure 1. Fundal height measurement
[Source 2 ]Table 2. The prediction error for gestational age using fundal height alone by the timing and frequency of measurements in the non-obese group (n=2224)a
| Fundal Height Model Measurement Constraintsb | Prediction Error (weeks) | Prediction Error (days) |
|---|---|---|
| Frequency of Measurementsc | ||
| Only 2 measurements | 2.69 | 18.83 |
| Only 3 measurements | 2.51 | 17.57 |
| Only 4 measurements | 2.36 | 16.52 |
| Timing of Measurements | ||
| >20 weeks | 2.02 | 14.14 |
| >20 cm | 2.20 | 15.40 |
| >28 weeks | 2.30 | 16.10 |
Footnote:
(a) Training set included non-obese women from all four racial/ethnic groups with ≥2 fundal height measures beginning at any time in gestation
(b) Limited in the test set only
(c) Randomly selected
Fundal height measurement
Fundal height is the distance from the pubic bone to the top of the uterus measured in centimeters. After 20 weeks of pregnancy, fundal height often matches the number of weeks you’ve been pregnant. It should match the fetus’ gestational age in weeks within 1 to 3 cm, e.g., a pregnant woman’s uterus at 22 weeks should measure 19 to 25 cm. A lag in fundal height of 4 cm or more suggests intrauterine growth restriction (IUGR). The most widely used definition of intrauterine growth restriction (IUGR) is a fetus whose estimated weight is below the 10th percentile for its gestational age and whose abdominal circumference is below the 2.5th percentile 3. At term, the cutoff birth weight for intrauterine growth restriction (IUGR) is 2,500 g (5 lb, 8 oz) 3.
Position of the patient
The patient should lie in the supine position and should have an empty bladder. Therefore the measurement is best done after the ultrasound scan when the woman has voided the bladder.
Technique for measuring uterine height 4:
- Uterine height should be measured only using the metric tape of non-elastic material provided by the study.
- Measurements are to be blinded, by turning the tape measure so that no numbers are visible during the measurement.
- Hold the 0 cm marking of the tape with one hand, securing it over the upper border of the symphysis pubis bone.
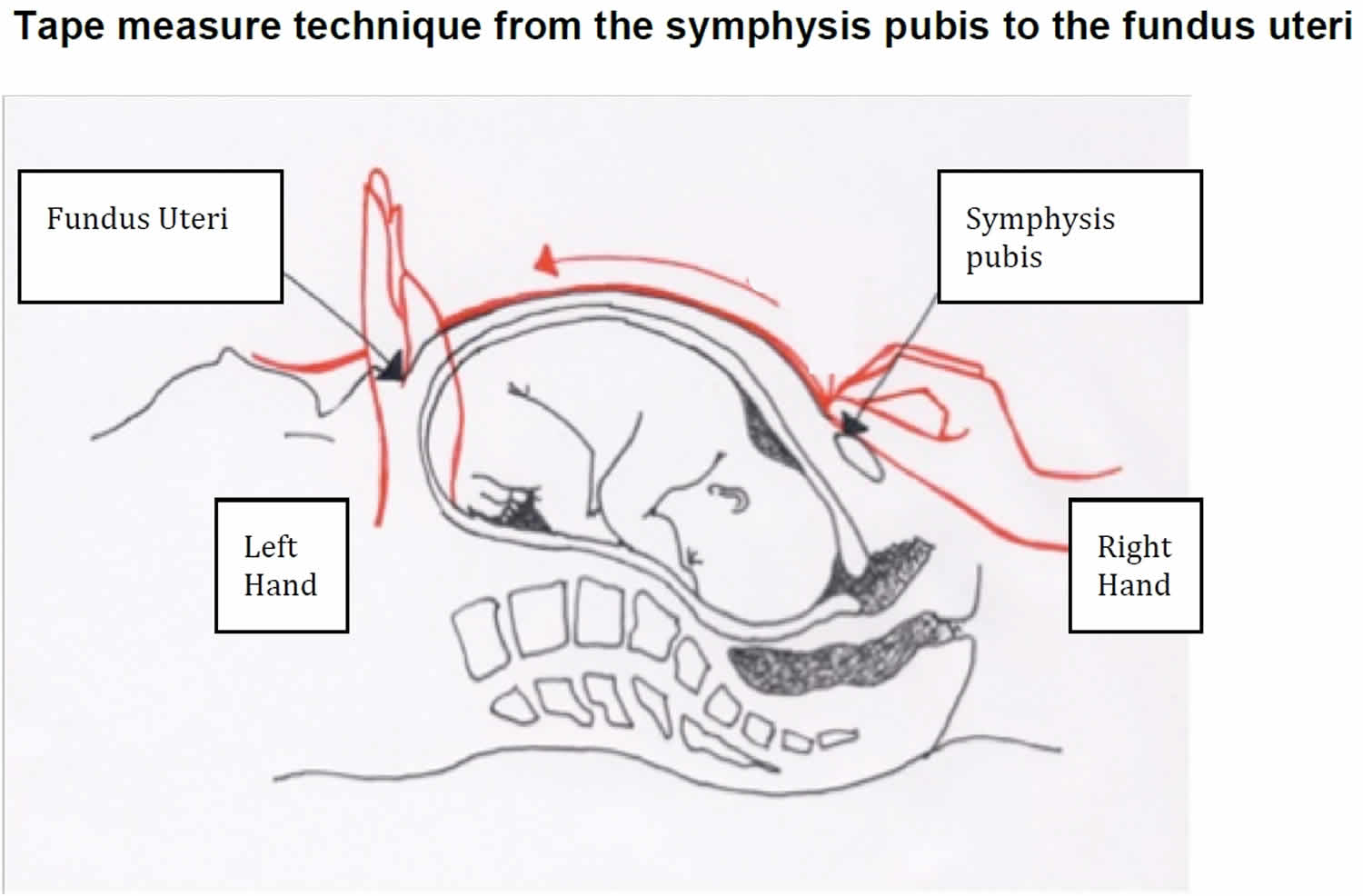
- With the palm of the other hand on the abdomen, pass the tape in a straight line from the symphysis pubis over the uterus to the fundus uteri until you feel a resistance in the abdominal wall. DO NOT HOLD THE TAPE BETWEEN THE FINGERS.
- Use the cubital edge of the hand to sustain the tape in place at the point of the fundus uteri.
- Carefully fold the paper at the level of the fundus. The tape should then be turned so that the numbers are visible and the value can be recorded. Please be aware that the tape has both cm and inches but that values should be recorded in cm only.
- Record the measurements to the nearest complete millimeter. Repeat the whole process a second time and record the second measurement.
Figure 2. Technique for measuring uterine height
A shorter measure can happen for one of the following reasons:
- Fetus descent into the pelvis, seen normally two to four weeks before delivery
- Error in estimated date of conception
- Fetus is healthy but physically small
- Oligohydramnios
- Fetus positioned sideways
- Breech birth
- Small for gestational age
On the other side, a longer measure can be caused by:
- Twins, or more
- Error in estimated date of conception
- Fetus is healthy but physically large
- Polyhydramnios
- Large for gestational age
- Hydatidiform Mole
As a pregnancy approaches its end, the fundal height will become less accurate.
It is very important that the patient’s fundal height be measured and properly recorded by their doctor or midwife on every prenatal visit. Measuring the fundal height is an indicator of proper fetal growth and amniotic fluid development.
Fundal height by week
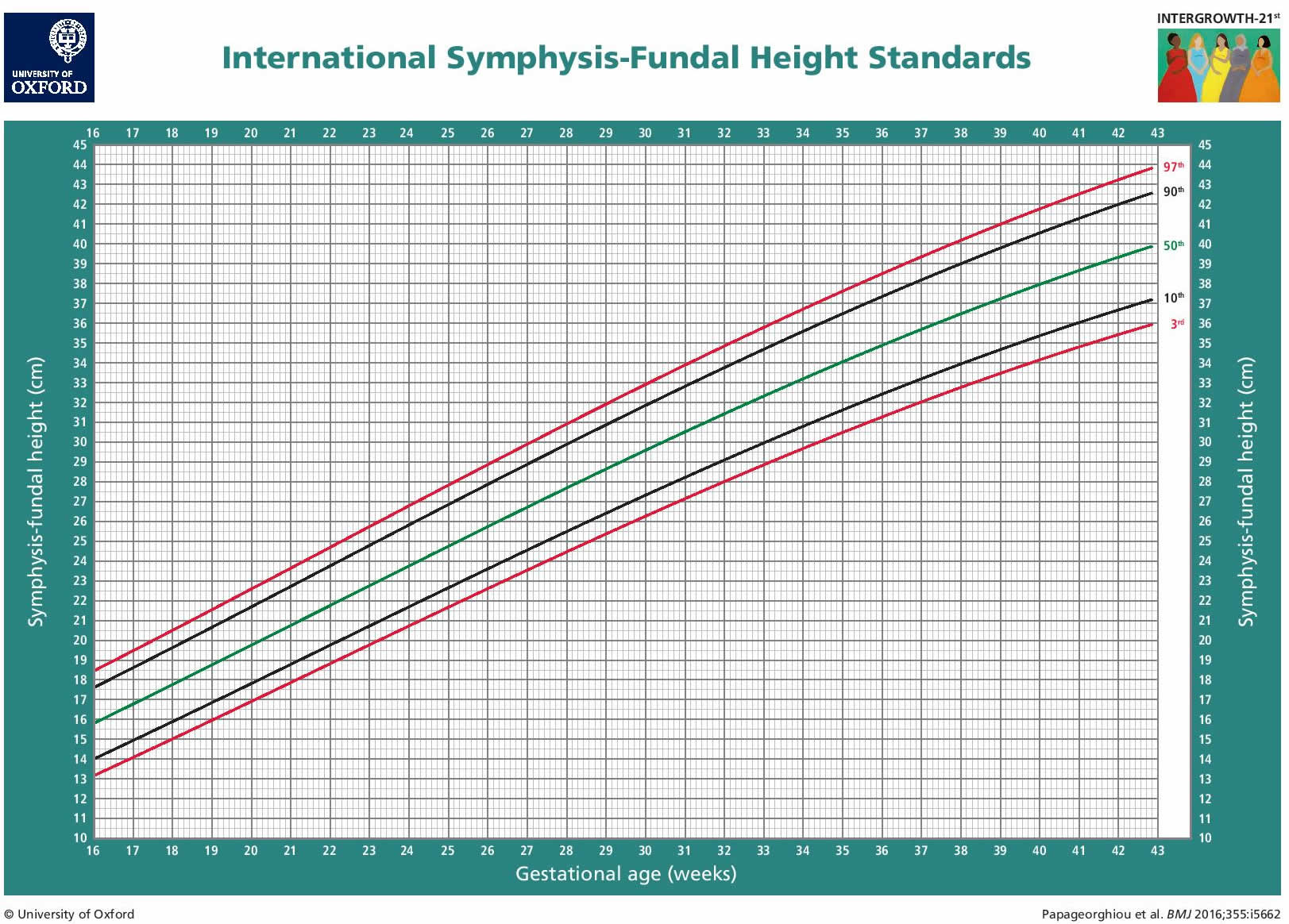
Table 3. International symphysis-fundal height standards for clinical use, rounded to the nearest 0.5 cm
| Gestational age (exact weeks*) | Centiles of fundal height (cm) | ||||||
|---|---|---|---|---|---|---|---|
| 3rd | 5th | 10th | 50th | 90th | 95th | 97th | |
| 16 | 13.0 | 13.5 | 14.0 | 16.0 | 17.5 | 18.0 | 18.5 |
| 17 | 14.0 | 14.5 | 15.0 | 17.0 | 18.5 | 19.0 | 19.5 |
| 18 | 15.0 | 15.5 | 16.0 | 18.0 | 19.5 | 20.0 | 20.5 |
| 19 | 16.0 | 16.5 | 17.0 | 19.0 | 20.5 | 21.0 | 21.5 |
| 20 | 17.0 | 17.5 | 18.0 | 20.0 | 21.5 | 22.0 | 22.5 |
| 21 | 18.0 | 18.0 | 19.0 | 21.0 | 22.5 | 23.5 | 23.5 |
| 22 | 19.0 | 19.0 | 20.0 | 22.0 | 24.0 | 24.5 | 24.5 |
| 23 | 20.0 | 20.0 | 20.5 | 23.0 | 25.0 | 25.5 | 25.5 |
| 24 | 20.5 | 21.0 | 21.5 | 24.0 | 26.0 | 26.5 | 27.0 |
| 25 | 21.5 | 22.0 | 22.5 | 24.5 | 27.0 | 27.5 | 28.0 |
| 26 | 22.5 | 23.0 | 23.5 | 25.5 | 28.0 | 28.5 | 29.0 |
| 27 | 23.5 | 24.0 | 24.5 | 26.5 | 29.0 | 29.5 | 30.0 |
| 28 | 24.5 | 25.0 | 25.5 | 27.5 | 30.0 | 30.5 | 31.0 |
| 29 | 25.5 | 26.0 | 26.5 | 28.5 | 31.0 | 31.5 | 32.0 |
| 30 | 26.5 | 26.5 | 27.5 | 29.5 | 32.0 | 32.5 | 33.0 |
| 31 | 27.0 | 27.5 | 28.0 | 30.5 | 33.0 | 33.5 | 34.0 |
| 32 | 28.0 | 28.5 | 29.0 | 31.5 | 34.0 | 34.5 | 35.0 |
| 33 | 29.0 | 29.5 | 30.0 | 32.5 | 34.5 | 35.5 | 36.0 |
| 34 | 29.5 | 30.0 | 31.0 | 33.0 | 35.5 | 36.5 | 36.5 |
| 35 | 30.5 | 31.0 | 31.5 | 34.0 | 36.5 | 37.0 | 37.5 |
| 36 | 31.5 | 31.5 | 32.5 | 35.0 | 37.5 | 38.0 | 38.5 |
| 37 | 32.0 | 32.5 | 33.0 | 35.5 | 38.0 | 39.0 | 39.5 |
| 38 | 33.0 | 33.0 | 34.0 | 36.5 | 39.0 | 39.5 | 40.0 |
| 39 | 33.5 | 34.0 | 34.5 | 37.0 | 40.0 | 40.5 | 41.0 |
| 40 | 34.0 | 34.5 | 35.5 | 38.0 | 40.5 | 41.5 | 42.0 |
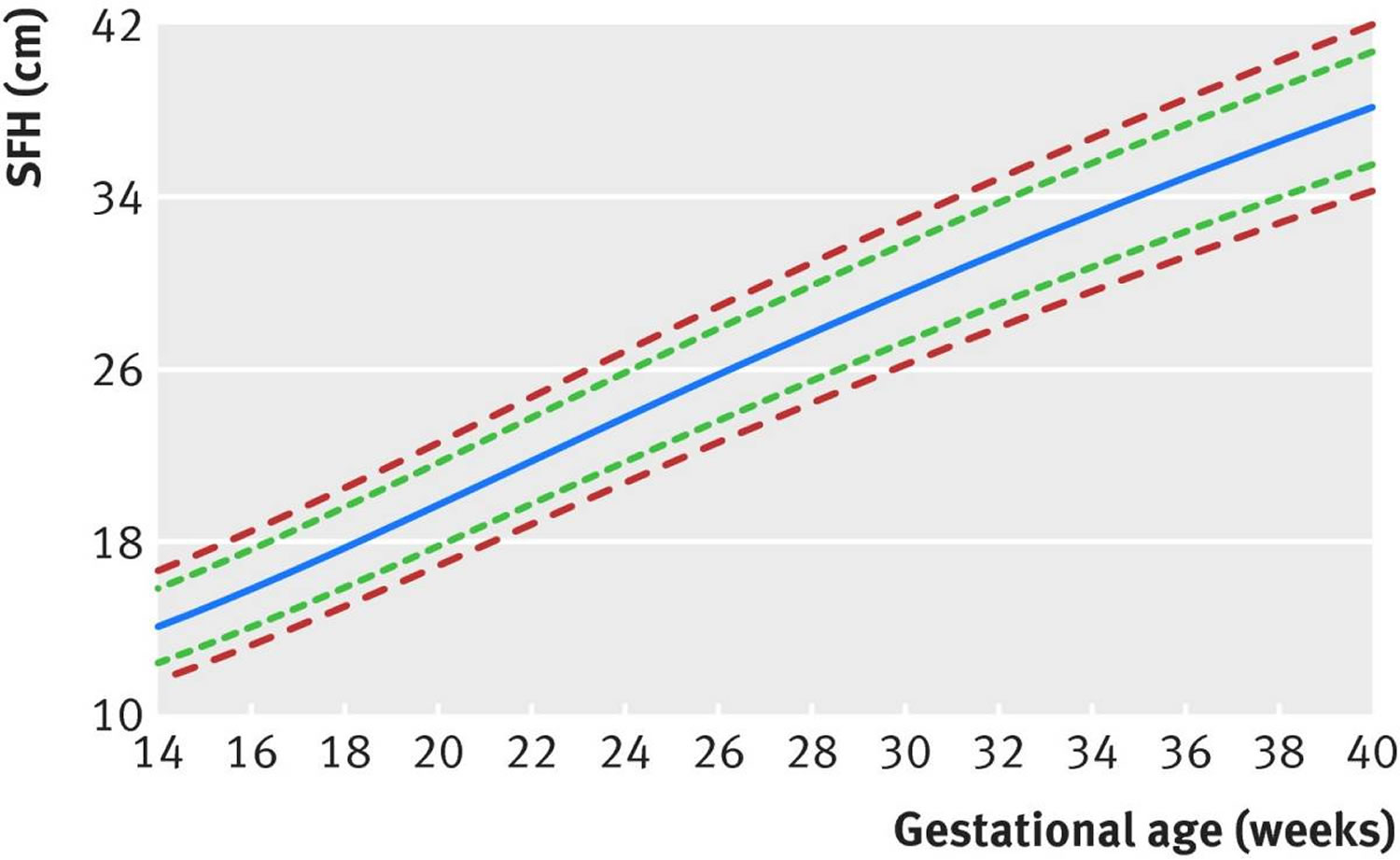
Figure 3. Fundal height by week
Footnote: International fundal height standards for clinical use. Lines (from bottom to top)=3rd, 10th, 50th, 90th, and 97th centiles.
[Source 5 ] References- Naidu K, Fredlund KL. Gestational Age Assessment. [Updated 2018 Oct 27]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2019 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK526000
- Pugh SJ, Ortega-Villa AM, Grobman W, et al. Estimating gestational age at birth from fundal height and additional anthropometrics: a prospective cohort study. BJOG. 2018;125(11):1397–1404. doi:10.1111/1471-0528.15179 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6107439
- Intrauterine Growth Restriction: Identification and Management. Am Fam Physician. 1998 Aug 1;58(2):453-460. https://www.aafp.org/afp/1998/0801/p453.html
- Measurement of Symphysis Fundus Height. https://www.medscinet.net/Intergrowth/patientinfodocs/Measurement%20of%20Symphysis%20Fundus%20Height.pdf
- Papageorghiou AT, Ohuma EO, Gravett MG, et al. International standards for symphysis-fundal height based on serial measurements from the Fetal Growth Longitudinal Study of the INTERGROWTH-21st Project: prospective cohort study in eight countries. BMJ. 2016;355:i5662. Published 2016 Nov 7. doi:10.1136/bmj.i5662 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5098415