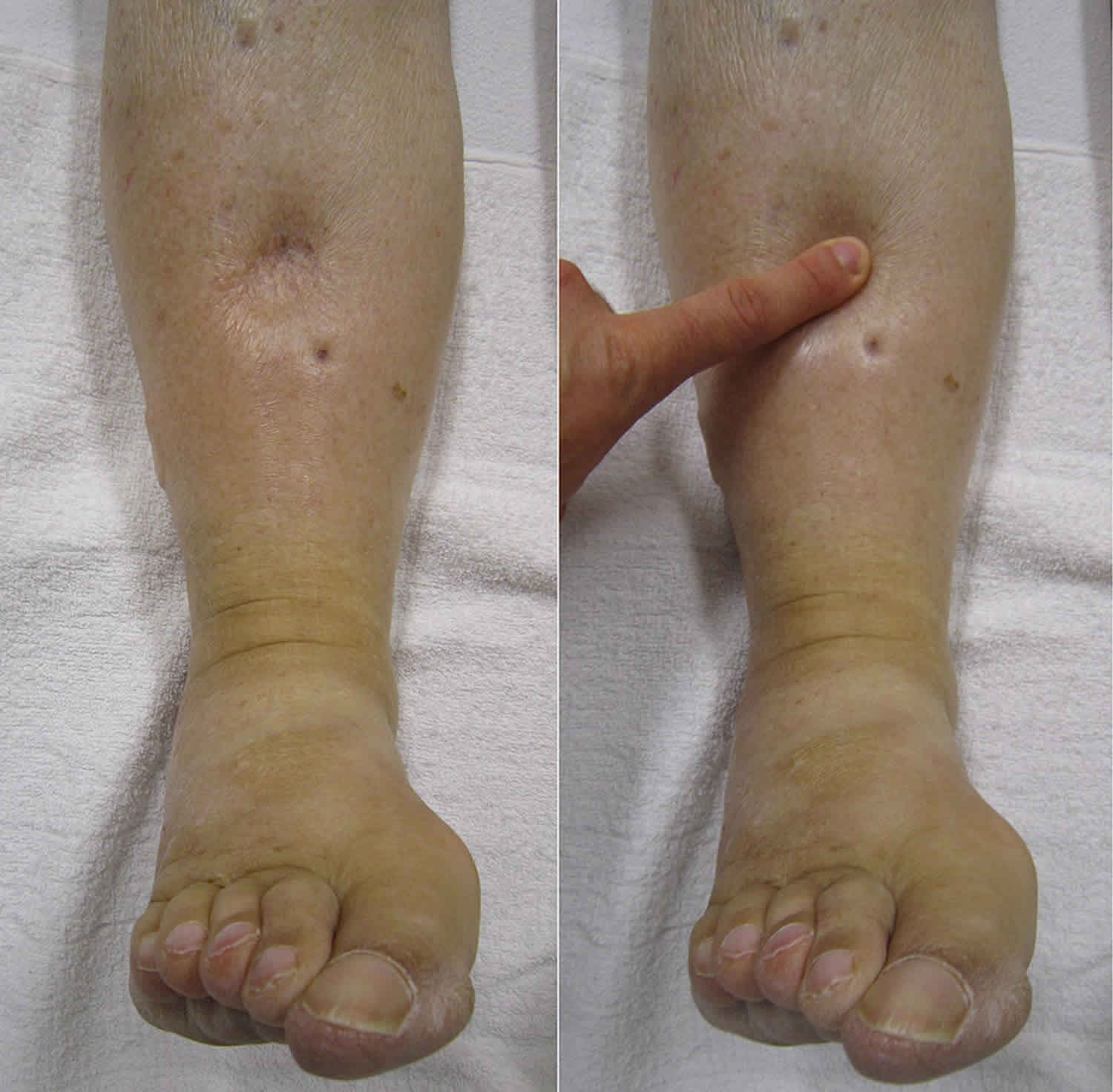
Heat edema
Heat edema is swelling in the legs and hands, which can occur when you sit or stand for a long time in a hot environment. Heat causes the blood vessels to expand (dilate), so body fluid moves into the hands or legs by gravity. The balance of salt in the body is also a risk factor for heat edema. If salt loss is less than normal, the increased salt level draws fluid into the hands and legs.
Older adults have an increased risk of heat edema, especially if they have other medical conditions that affect their circulation.
People visiting hot climates from colder climates may also have an increased risk of heat edema.
Make an appointment to see your doctor if you have swelling, stretched or shiny skin, or skin that retains a dimple after being pressed (pitting). See your doctor immediately if you experience:
- the swelling is only in 1 ankle, foot or leg and there’s no obvious cause, such as an injury
- the swelling is severe, painful or starts very suddenly
- the swollen area is red or feels hot to the touch
- your temperature is very high, or you feel hot and shivery
- you have diabetes
Call your local emergency services number if:
- you feel short of breath or are struggling to breathe
- your chest feels tight, heavy or painful
You could have a blood clot in your lungs or pulmonary edema, which needs immediate treatment in hospital.
If you’ve been sitting for a prolonged period, such as on a long flight, and you develop leg pain and swelling that won’t go away, call your doctor. Persistent leg pain and swelling can indicate a blood clot deep in your vein (deep vein thrombosis, or DVT).
Common causes of swollen ankles, feet and legs
Swelling in the ankles, feet and legs is often caused by a build-up of fluid in these areas, called edema. Edema occurs when tiny blood vessels in your body (capillaries) leak fluid. The fluid builds up in surrounding tissues, leading to swelling.
Edema is usually caused by:
- gravity – standing or sitting in the same position for too long, allowing fluid to ‘pool’ in the tissues of your lower legs
- hot weather – the body tends to be less efficient at removing fluid from tissues during the summer months
- eating too much salty food
- being overweight
- being pregnant – hormones encourage the body to hold onto excess fluid
- taking certain medicines – such as some high blood pressure medicines (antihypertensives), corticosteroids and nonsteroidal anti-inflammatory drugs (NSAIDs) or antidepressants are known to cause fluid retention
Edema can also be caused by:
- an injury – such as a strain or sprain
- an insect bite or sting
- problems with your kidneys, liver or heart
- a blood clot
- an infection
- burns – including sunburn. The skin retains fluid and swells in response to burn injuries
- menstrual cycle – some women experience edema in the two weeks prior to menstruation
- contraceptive pills – oral contraceptives that include estrogen can trigger fluid retention
- dietary deficiency – such as insufficient protein or vitamin B1 (thiamine) in the diet
- chronic venous insufficiency – weakened valves in the veins of your legs fail to efficiently return blood to the heart. The pooling of blood can result in varicose veins. Sudden onset of swelling in one leg accompanied by pain in your calf muscle can be due to a blood clot (deep vein thrombosis, or DVT) in one of your leg veins. If this occurs, seek medical help immediately.
Medical conditions that may cause edema or fluid retention
Fluid retention may be a symptom of serious underlying medical conditions, including:
- Kidney disease – such as nephrotic syndrome and acute glomerulonephritis. Damage to the tiny, filtering blood vessels in your kidneys can result in nephrotic syndrome. In nephrotic syndrome, declining levels of protein (albumin) in your blood can lead to fluid accumulation and edema.
- Congestive heart failure – if the heart does not pump effectively, the body compensates in various ways. it starts to retain fluid and increase the volume of blood. This results in congestion of the veins, enlargement of the liver, and the accumulation of fluid in body cavities like the abdominal cavity (ascites) and in subcutaneous tissues, causing swelling (edema) of the legs. Sometimes, congestive heart failure can cause fluid to accumulate in your lungs (pulmonary edema), which can lead to shortness of breath.
- Chronic lung diseases – such as severe emphysema, which put excessive pressure on the heart’s right ventricle, leading to its failure
- Liver disease – such as severe cirrhosis that triggers liver failure. Fluid may accumulate in your abdominal cavity (ascites) and in your legs as a result of liver damage (cirrhosis).
- Malignant lymphedema – cancerous tumors that block structures of the lymphatic system, such as the lymph nodes
- Thyroid disease – such as hypothyroidism (underactive thyroid)
- Arthritis – joints affected by some types of arthritis tend to swell with fluid
- Allergic reaction – in susceptible people, the body tends to swell in response to particular allergens, such as an insect bite. In some cases, the reaction is severe (anaphylaxis) and requires urgent medical attention. this swelling is short-lived rather than ongoing
- Autoimmune diseases such as lupus.
- Inadequate lymphatic system. Your body’s lymphatic system helps clear excess fluid from tissues. If this system is damaged — for example, by cancer surgery — the lymph nodes and lymph vessels draining an area may not work correctly, and edema can occur.
- Severe, long-term protein deficiency. An extreme lack (deficiency), of protein in your diet over a long period of time can lead to fluid accumulation and edema.
Heat edema signs and symptoms
Common early signs of heat edema or peripheral edema include the following:
- An arm or leg starts feeling full or heavy.
- The arm or leg starts to look swollen.
- When you press the swelling, it leaves a dent.
- Your clothing or jewelry starts to feel tight and uncomfortable.
- The skin near the edema feels tight or warm.
- It becomes harder to move any joints that are affected.
- There is a sensation of tautness or even pain in the surrounding area.
Heat edema diagnosis
To understand what might be causing your edema, your doctor will first perform a physical exam and ask you questions about your medical history. This information is often enough to determine the underlying cause of your edema. In some cases, X-rays, ultrasound exams, magnetic resonance imaging, blood tests or urine analysis may be necessary.
The underlying cause of the edema must be found before treatment can begin. Diagnostic tests may include:
- physical examination
- medical history
- detailed questioning about the fluid retention, such as when it started, any factors that worsen the swelling and whether it is constant or intermittent
- blood tests
- urine tests
- liver function tests
- kidney function tests
- chest x-ray
- heart function tests, such as electrocardiogram (ECG).
Heat edema treatment
Swelling in your ankles, feet or legs should go away on its own, but there are some things you can try to help.
Depending on the underlying cause, treatment may include:
- a low-salt diet
- diuretics (water pills)
- treatment for the underlying medical condition: for example, hormone replacement (thyroxine) in the case of hypothyroidism
- lifestyle changes in response to the underlying medical condition: for example, avoidance of alcohol if liver disease is the cause
- changes to medication or dosage, if drugs are the cause
- dietary adjustments, if malnutrition is the cause
- ongoing medical supervision
- aids such as support stockings.
More-severe edema may be treated with drugs that help your body expel excess fluid in the form of urine (diuretics). One of the most common diuretics is furosemide (Lasix). However, your doctor will determine whether these types of medications are a good option for you based on your personal medical history.
Long-term management typically focuses on treating the underlying cause of the swelling. If edema occurs as a result of medication use, your doctor may adjust your prescription or check for an alternative medication that doesn’t cause edema.
Self-care options for fluid retention
Mild fluid retention can be helped in the following ways:
- Reduce the amount of salt in your diet; for instance, don’t add salt during the cooking process and stop salting your meals at the table. Avoid foods like potato chips and salted peanuts. Be wary of processed foods such as manufactured meats, which tend to contain ‘hidden’ salt.
- Vitamin B6 (pyridoxine) is thought to help in cases of mild fluid retention. Good sources of vitamin B6 include brown rice and red meat.
- Vitamin B5 (pantothenic acid), calcium and vitamin D help the body to excrete excess fluids. Include fresh fruits and low-fat dairy foods in your daily diet.
- Supplements may help in the case of fluid retention caused by the menstrual cycle: for example calcium, magnesium, manganese, evening primrose oil and chaste tree.
- Herbal diuretics include dandelion leaf, corn silk and horsetail.
- Make sure to discuss the use of supplements with your doctor or health care professional, particularly if you are on any type of medication.
- Drink plenty of water. It may sound contradictory, but a well-hydrated body is less likely to retain fluid.
- Cut back on dehydrating drinks such as tea, coffee and alcohol.
- Cranberry juice has a mild diuretic action.
- Lie down and use pillows to raise your legs higher than your head, when possible.
- Exercise regularly, like walking, to improve your blood flow.
- Wear support stockings.
- Wear wide, comfortable shoes with a low heel and soft sole
- Wash, dry and moisturize your feet to avoid infections
DON’T
- do not stand or sit for long periods of time
- do not wear clothes, socks or shoes that are too tight
See a doctor if your ankle, foot or leg is swollen and:
- it has not improved after treating it at home for a few days
- it gets worse.