Herpes gladiatorum
Herpes gladiatorum also known as “mat herpes”, is a skin infection caused by herpes simplex virus (HSV) involving the face, arms, neck and upper trunk, typically seen in wrestlers and participants in some contact sports such as rugby. The usual culprit is herpes simplex virus type 1 (HSV-1), with herpes simplex virus type 2 (HSV-2) responsible for a minority of cases 1. In wrestling, 94% to 97% of HSV infections are caused by type 1 infection 2. Herpes simplex virus type 1 (HSV-1) infection is promoted by trauma to the skin sustained during matches. Transmission generally occurs primarily through skin-to-skin contact 3, for example, by exposure of abraded skin or mucosa to the lesions or mucocutaneous secretions of an infected individual 4. Herpes simplex virus type 1 (HSV-1) infections are very common and it causes cold sores on your lips. In the United States, 30% to 90% of people are exposed to herpes by adulthood, although many people never develop symptoms. Herpes simplex virus type 1 (HSV-1) infection of the eye can be serious and requires immediate medical attention.
Up to 90% of herpes gladiatorum infections are misdiagnosed by physicians at first presentation 5.
The distribution of herpes gladiatorum lesions tends to be more diffuse than in typical HSV infections. Herpes gladiatorum lesions occur on body surface areas that frequently come in contact with an opponent, such as the face, head, neck, ears, and upper extremities 6, reinforcing the theory that transmission is primarily through skin-to-skin contact. Lesion location frequently reflects the wrestler’s handedness 7; that is, lesions commonly occur on a wrestler’s dominant side, believed to result from the common “lock-up” position 3. Because herpes gladiatorum lesions are often abraded during competition, lesions frequently have an atypical appearance and can be mistaken for many other cutaneous diseases 8.
After the first outbreak resolves and latency is established, reactivation and recurrent outbreaks can be triggered by factors such as stress, fever, sun exposure, temperature extremes, trauma, or immunosuppression 9. Recurrences occur at the site of the initial outbreak (a fact that aids in diagnosis) 10, tend to be milder than the initial infection,66 and are of shorter duration 9.
Careful examination of the eyes and oral and nasal cavities is imperative when herpes gladiatorum is suspected because mucosal and ocular involvement by HSV can occur 11. Inoculation of the eyes was seen in an herpes gladiatorum epidemic among high school wrestlers in Minnesota; approximately 8% developed ocular involvement 12. Ocular involvement is of particular concern because herpetic keratitis, if it arises, may cause corneal scarring and blindness 11. Inoculation of the oral mucosa causes gingivostomatitis 4. Autoinoculation while shaving can result in hair follicle lesions (herpetic sycosis) 9, which can be indistinguisable from bacterial folliculitis.
The annual estimated incidence of herpes gladiatorum in National Collegiate Athletic Association (NCAA) wrestlers is 20% to 40% 3. From 1993 to 2004, herpes gladiatorum was the most common reported cutaneous infection leading to lost practice time in NCAA wrestlers, accounting for 40.5% of all such infections 13. Numerous wrestling team and training camp epidemics have highlighted the substantial transmission potential of HSV 14.
If you suspect you have herpes gladiatorum (HSV-1 infection), inform your coach immediately, early identification and treatment of skin infections is important for your health and the health of your teammates and opponents.
HSV replicates in skin cells and neurons and then travels to sensory dorsal root ganglia, where lifelong latency is established 15. An incubation period of 4 to 7 days from exposure to lesion appearance has been observed in a population of wrestlers during an epidemic 7. A prodrome of burning, tingling, or stinging may occur, and the infected individual may have a variety of systemic signs and symptoms 6. Numerous grouped painful vesicles or pustules on an erythematous base develop and then evolve into moist ulcerations, followed by crusted plaques (see Figure 1). Herpes gladiatorum lesions generally appear 1 to 2 days after prodromal symptoms begin and healing occurs within 10 days after the initial appearance without scarring 4.
Some cases of herpes are mild and may not need treatment. However, athletes should not practice, play, or compete until a medical provider determines that the lesions are no longer infectious (contagious).
Athletes who have severe or prolonged outbreaks (especially if it is the first episode), immune system problems, or frequent outbreaks may be prescribed antiviral medications.
While herpes gladiatorum (HSV-1) can be treated, once infected with the virus, a person is infected for life. People with herpes gladiatorum can have periods where the virus is inactive and cannot be spread to others. However, the virus can reactivate at any time and be transmitted to others, even if there are no symptoms (such as sores). This is why prevention is so important.
Figure 1. Herpes gladiatorum lesions on the forehead
Footnote: Herpes gladiatorum lesions on the forehead of this wrestler appear as grouped vesicles and crusted plaques.
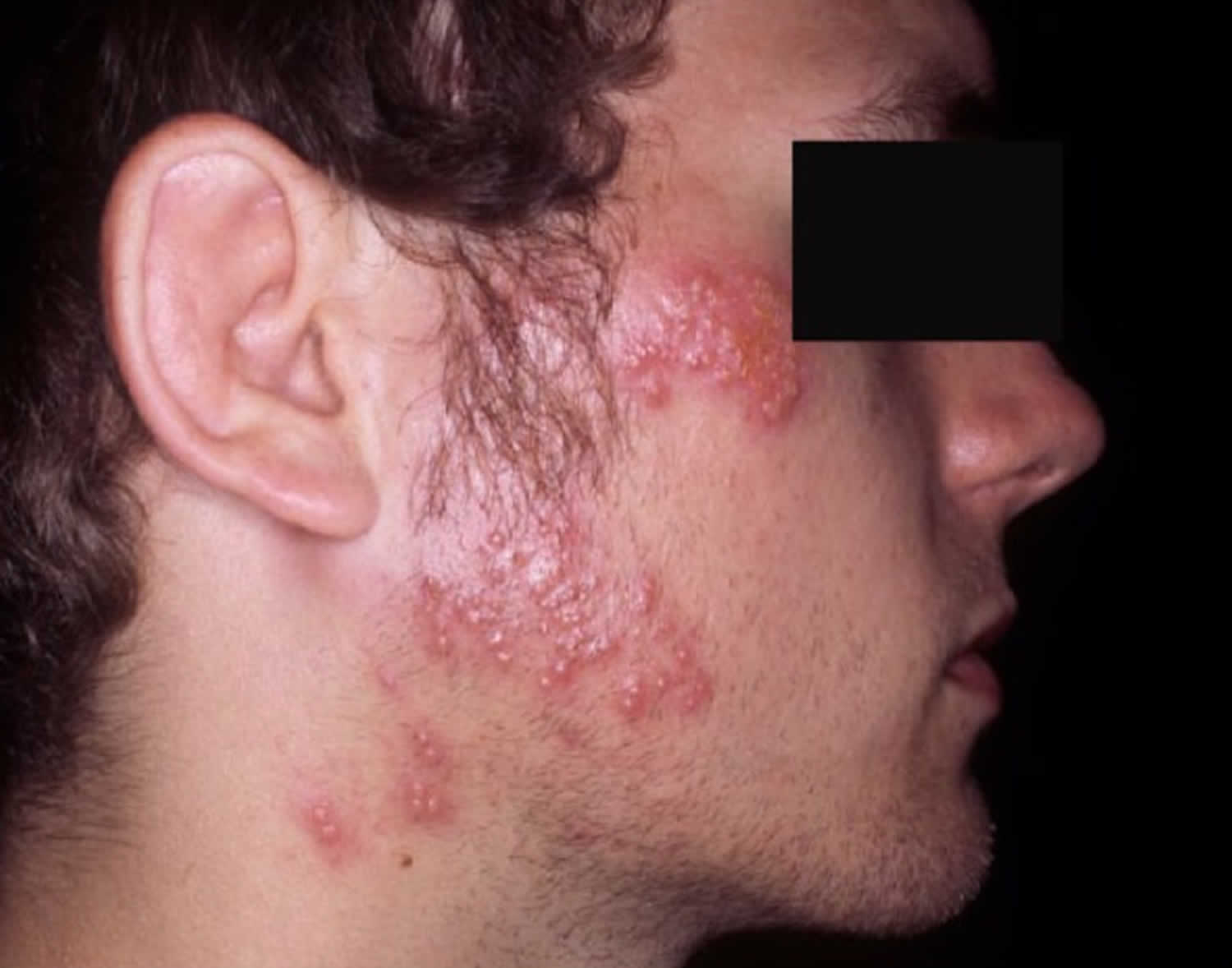
[Source 1 ]Figure 2. Herpes gladiatorum (primary herpes gladiatorum)
Footnote: Primary herpes gladiatorum. Note multiple areas of involvement and regional adenopathy.
[Source 2 ]How does herpes gladiatorum spread?
The skin infection is spread by direct skin-to-skin contact. Sports that involve close contact, such as rugby and wrestling, may spread the infection from one affected athlete to another. Other names for the disease include “wrestlers herpes” or “mat pox” (after wrestling).
Is herpes gladiatorum only spread between athletes?
No. HSV-1, the virus that causes herpes gladiatorum, can be spread to others through direct skin contact with lesions, this includes kissing or sharing beverage containers, eating utensils, cell phones, or lip balm with others.
How long is someone with herpes gladiatorum infectious to others?
Someone with a herpes gladiatorum skin lesion is generally infectious during the time when the blisters are not dry and healed. However, people with no visible sores may also be contagious.
What are the long-term effects of herpes gladiatorum?
Once infected with the virus, a person is infected for life. People with herpes gladiatorum can go long periods of time during which the virus is inactive and cannot be spread to others. However, the virus can reactivate at any time and be transmitted to others, even if there are no symptoms. This is why prevention is so important.
Herpes gladiatorum causes
Herpes gladiatorum also known as “mat herpes”, is a skin infection caused by herpes simplex virus (HSV) involving the face, arms, neck and upper trunk, typically seen in wrestlers and participants in some contact sports such as rugby. In wrestling, 94% to 97% of HSV infections are caused by type 1 infection 2. Herpes simplex virus type 1 (HSV-1) infection is promoted by trauma to the skin sustained during matches. Transmission is almost exclusively from direct skin-to-skin contact. Multiple studies have indicated that training mats and other fomites do not significantly contribute to the spread of infection 16. A total of 29% to 30% of high school wrestlers are infected or colonized with HSV, but only 3% are aware they carry the virus 17. This discrepancy is the primary reason that large outbreaks seem to occur for unknown reasons and leads to the lack of proper suspicion when such outbreaks do develop.
Risk factors for herpes gladiatorum include participation in high-contact sports such as rugby, wrestling, MMA, and boxing.
HSV-1 is typically spread through direct contact with contaminated saliva or other infected bodily secretions, as opposed to HSV-2, which is spread primarily by sexual contact. HSV-1 begins to replicate at the site of infection (mucocutaneous) and then proceeds to travel by retrograde flow down an axon to the dorsal root ganglia. It is in the dorsal root ganglia that latency is established. This latency period allows the virus to remain in a non-infectious state for a variable amount of time before reactivation. HSV-1 is sly in its ability to evade the immune system via several mechanisms. One such mechanism is inducing an intercellular accumulation of CD1d molecules in antigen presenting cells. Normally, these CD1d molecules are transported to the cell surface, where the antigen is presented resulting in the stimulation of natural killer T-cells, thus promoting immune response. When CD1d molecules are sequestered intercellularly, the immune response is inhibited. HSV-1 has several other mechanisms by which it down-regulates various immunologic cells and cytokines 18.
Herpes gladiatorum prevention
As with all herpes simplex virus (HSV) infections, prevention of herpes gladiatorum transmission is difficult. Up to 87.4% of HSV outbreaks are subclinical and go unnoticed 19. A large number of potentially infected but asymptomatic athletes can lead to large outbreaks at inopportune times, including during camps and postseason competition. Oral valacyclovir has been shown to decrease risk of HSV acquisition and prevent recurrence of previous herpes gladiatorum 20. A recent 10-year study of wrestlers at a 28-day wrestling camp demonstrated that daily oral valacyclovir decreased recurrent herpes gladiatorum outbreaks by 89.5% and prevented contraction of the virus in HSV-naive wrestlers 20. Overall, there is strong evidence that the use of oral valacyclovir dramatically decreases risk of both acquiring HSV and having an herpes gladiatorum outbreak in both HSV-seropositive wrestlers and those that are HSV-naive 20. For those considering anti-viral prophylaxis of herpes gladiatorum, it is generally best to start the medication at least 5 days before the season, camp, or tournament begins to ensure adequate drug levels in the ganglia 20. Complete recommendations for treatment and prophylaxis of herpes gladiatorum are presented in Table 1 below (treatment section).
What can I do to prevent getting herpes gladiatorum?
Good personal hygiene is essential for preventing the spread of Herpes gladiatorum and other skin infections. This is especially important for athletes who participate in direct contact sports. Athletes should shower immediately after practice and use their own soap, towels, and razors. Towels should be washed after each use with hot water and detergent with bleach then dried on high heat. Practice and competition gear should be cleaned after each use. Athletes should be encouraged to wash their hands often, and discouraged from picking or squeezing skin sores because what drains may be very infectious. Athletes should report any suspicious skin lesions to their coach or athletic trainer immediately. Cleaning and disinfecting the sports environment (e.g., mats) is also important in preventing infections.
Herpes gladiatorum symptoms
Lesions of herpes gladiatorum will be seen on the lateral neck, side of the face, and forearms within 4 to 11 days after exposure. A high suspicion for this diagnosis is crucial in athletes, as this is commonly misdiagnosed as bacterial folliculitis.
The face is involved in more than 70% of herpes outbreaks in wrestling 7. Infection of the fingers or thumb (herpetic whitlow) and of other commonly abraded areas of the body account for most of the remaining 30% 7. Underlying skin conditions, such as eczema, can increase the risk of HSV skin infection. Occasionally, ocular involvement can occur. Herpes keratitis (corneal involvement) can lead to scarring and, with repeated outbreaks, may result in permanent clouding of the cornea, requiring corneal transplantation to preserve proper vision. Rarely, but more seriously, retinal necrosis can occur and lead to blindness 21. Herpes-induced retinal necrosis is the most common source of blindness from an infectious source in the United States 21.
Primary herpes gladiatorum outbreaks typically present with systemic symptoms, including malaise, low-grade fever, sore throat, and swollen/tender anterior and posterior cervical adenopathy 22. One to 2 days later, 1- to 2-mm-diameter diffuse patches of 3 to 10 vesicles will coalesce with a minimally reddened base (see Figure 2). The majority (90%-93%) of infections will occur within 8 days of exposure 23. The virus is transmitted via viral replication in ganglia and spread along sensory nerve tissue. Multiple dermatomes and both sides of the face, head, and neck may be involved. Occasionally this may extend to the upper extremities as well 22. Distribution of lesions commonly reflects the wrestler’s dominant hand, and lesions are more likely to occur on the side of the head of the wrestler’s preferred tie position 24.
Recurrent herpes gladiatorum typically involves fewer vesicles, and outbreaks are shorter in duration. Reactivation of dormant virus in ganglia leads to new outbreaks that occur, and will reoccur, in the same dermatomal or peripheral nerve pattern 25. Systemic symptoms are much less common in recurrent herpes gladiatorum, and symptoms typically last only 7 to 10 days. Treatment with oral antiviral medications can shorten the duration of illness by 2 to 5 days, allowing the athlete to return to play sooner 21.
Symptoms of herpes gladiatorum (HSV-1 infection) include the following:
- Symptoms usually begin about 8 days after exposure to HSV-1.
- Fever (especially during the first episode).
- Swollen glands (enlarged lymph nodes).
- A tingling feeling at the affected area.
- A cluster (usually more than one) of clear, fluid-filled blisters that may be surrounded by redness — these blisters may or may not be painful.
- Blisters and lesions usually heal within 7 to 10 days.
- People with HSV-1 infection are infected for life, may have periodic outbreaks, and can transmit the virus to others.
Herpes gladiatorum diagnosis
The gold standard for diagnosing HSV-1 infection is HSV-1 serology (antibody detection via western blot) 26. The most sensitive and specific mechanism is viral polymerase chain reaction (PCR). However, serology remains the gold standard. Viral culture, direct fluorescent antibody assay, and Tzanck smear are alternative methods of diagnosing. It is important to note that the Tzanck smear identifies multinucleated giant cells, so it cannot distinguish between HSV and varicella zoster virus (VZV). The direct fluorescent antibody assay, however, can distinguish between the 2 entities 27.
Microbiological testing may be helpful in the diagnosis of herpes gladiatorum 7. One study revealed that more than 90% of herpes gladiatorum cases were misdiagnosed by physicians, who used viral culture only 18% of the time 28, suggesting both a role for microbiological testing and a lack of testing being performed in the community. Testing a lesion is best accomplished by unroofing an intact vesicle, absorbing the vesicular fluid, and scraping the lesion’s base with a swab 9 that lacks calcium alginate (an inhibitor of HSV growth) and has a plastic or metal shaft (to avoid cell toxicity in cultures potentially caused by wood) 29. Diagnostic yield is highest from samples obtained within the first 24 to 48 hours 9. Viral culture has variable sensitivity, depending on the state of the lesion at the time of sampling and sampling technique (52% to 93% for vesicles, 41% to 72% for ulcers, and 19% to 27% for crusted lesions) and a near 100% specificity 30. Real-time polymerase chain reaction is a substantially more sensitive option, with specificity comparable with that of culture 30 (sensitivity and specificity of 98% to 100%) 31, but its utility is limited by substantially higher cost and availability. The choice of diagnostic testing should be guided by the provider’s expertise and by test availability; lesions should be sampled as early as possible.
Herpes gladiatorum treatment
The cornerstone of herpes gladiatorum management is the early detection and isolation of infected wrestlers. Treatment of an acute herpes gladiatorum eruption includes oral antiviral medications (Table 1), started within 24 hours of developing symptoms 32. In a placebo-controlled study, valacyclovir (500 mg twice daily for 7 days) was effective in decreasing the duration of visible herpes gladiatorum lesions and viral shedding during recurrent outbreaks 33.
The Sports Medicine Advisory Committee of the National Federation of State High School Associations (NFHS) and the National Collegiate Athletic Association (NCAA) recommend consideration of season-long oral antiviral prophylaxis for wrestlers with a history of an herpes gladiatorum outbreak 1. A double-blind study found that oral valacyclovir was significantly more effective than a placebo for prophylaxis against acute herpes gladiatorum reactivation in wrestlers10; effective doses were 500 mg per day for wrestlers with a history of more than 2 years and 1000 mg per day for wrestlers with a history of less than 2 years. Valacyclovir prophylaxis has not been associated with substantial side effects 34.
Table 1. Select oral medications for herpes gladiatorum
| Indication | Medication | Dosing Regimen |
|---|---|---|
| Primary infection | ||
| Adult | Acyclovir | 400 mg, orally, 3×/day, or 200 mg, orally, 5×/day for 7-10 days |
| Famciclovir | 250 mg, orally, 3×/day for 7-10 days | |
| Valacyclovir | 1000 mg, orally, 2×/day for 7-10 days | |
| ≤ 12 years old | Acyclovir | 40-80 mg/kg daily in 3 divided doses for 5-10 day (max, 1 g/day) |
| Valacyclovir | 20 mg/kg, orally, 3×/day for 5-10 days | |
| Recurrent infection | ||
| Adulta | Acyclovir | 800 mg, orally, 2×/day for 5 days, or 400 mg, orally, 3×/day for 5 days |
| Famciclovir | 125 mg, orally, 2×/day for 5 days, or 1 g, orally, 2× for 1 day | |
| Valacyclovir | 1 g, orally, daily for 5 days, or 500 mg, orally, 2×/day for 3-7 days | |
| Prophylaxis | ||
| > 12 years oldb | Acyclovir | 400 mg, orally, 2×/day |
| Famciclovir | 250 mg, orally, 2×/day | |
| Valacyclovir | 500 mg, orally, once daily, or 1 g, orally, once daily | |
Footnote: (a) Same as for primary infection, ≤ 12 years old. (b) Insufficient evidence to recommend use of prophylaxis in children < 12 years old.
[Source 1 ]Guidelines for return to competition for herpes gladiatorum in wrestlers
National Collegiate Athletic Association (NCAA) 35
- Primary infection
- Wrestler must be free of systemic symptoms of viral infection (fever, malaise, etc.).
- Wrestler must have developed no new blisters for 72 hours before the examination.
- Wrestler must have no moist lesions; all lesions must be dried and surmounted by a FIRM ADHERENT CRUST.
- Wrestler must have been on appropriate dosage of systemic antiviral therapy for at least 120 hours before and at the time of the meet or tournament.
- Active herpetic infections shall not be covered to allow participation
- Recurrent infection
- Blisters must be completely dry and covered by a FIRM ADHERENT CRUST at time of competition, or wrestler shall not participate.
- Wrestler must have been on appropriate dosage of systemic antiviral therapy for at least 120 hours before and at the time of the meet or tournament.
- Active herpetic infections shall not be covered to allow participation.
- Questionable cases
- Tzanck prep and/or HSV antigen assay (if available).
- Wrestler’s status deferred until Tzanck prep and/or HSV assay results complete.
Wrestlers with a history of recurrent herpes labialis or herpes gladiatorum could be considered for season long prophylaxis. This decision should be made after consultation with the team physician.
National Federation of State High School Associations (NFHS) 36:
- In dealing with HSV-1, treatment requires 10-14 days with a primary outbreak. Recurrent outbreaks require 120 hours of treatment before returning to practice and/or competition. Treating herpes within the athletic arena is different than the non-athletic population. Non-wrestlers use antiviral medication to treat symptoms, whereas in wrestling the treatment focuses on clearance of the virus to prevent transmission to teammates and opponents. If antiviral therapy used, withhold from wrestling for 5 days 1.
- Wilson EK, Deweber K, Berry JW, Wilckens JH. Cutaneous infections in wrestlers. Sports Health. 2013;5(5):423–437. doi:10.1177/1941738113481179 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3752190
- Peterson AR, Nash E, Anderson BJ. Infectious Disease in Contact Sports. Sports Health. 2019;11(1):47–58. doi:10.1177/1941738118789954 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6299350
- Johnson R. Herpes gladiatorum and other skin diseases. Clin Sports Med. 2004;23:473-484
- Pecci M, Comeau D, Chawla V. Skin conditions in the athlete. Am J Sports Med. 2009;37:406-418
- Dworkin MS, Shoemaker PC, Spitters C, et al. Endemic spread of herpes simplex virus type 1 among adolescent wrestlers and their coaches. Pediatr Infect Dis J. 1999;18:1108-1109.
- Zinder SM, Basler RSW, Foley J, Scarlata C, Vasily DB. National Athletic Trainers’ Association position statement: skin diseases. J Athl Train. 2010;45:411-428
- Anderson BJ. The epidemiology and clinical analysis of several outbreaks of herpes gladiatorum. Med Sci Sports Exerc. 2003;35:1809-1814
- Ergin S, Ergin C, Erdogan BS, Kaleli I, Evliyaoglu D. An experience from an outbreak of tinea capitis gladiatorum due to Trichophyton tonsurans. Clin Exp Dermatol. 2006;31:212-214
- Usatine RP, Tinitigan R. Nongenital herpes simplex virus. Am Fam Physician. 2010;82:1075-1082
- Landry GL, Chang CJ. Herpes and tinea in wrestling: managing outbreaks, knowing when to disqualify. Phys Sportsmed. 2004;32:34-41
- Goldman L, Schafer AI, eds. Goldman’s Cecil Medicine. 24th ed. Philadelphia, PA: Elsevier; 2012
- Holland EJ, Mahanti RL, Belongia EA, et al. Ocular involvement in an outbreak of herpes gladiatorum. Am J Ophthalmol. 1992;114:680-684
- Agel J, Ransone J, Dick R, Oppliger R, Marshall SW. Descriptive epidemiology of collegiate men’s wrestling injuries: National Collegiate Athletic Association Injury Surveillance System, 1988-1989 through 2003-2004. J Athl Train. 2007;42:303-310
- Anderson BJ. Prophylactic valacyclovir to prevent outbreaks of primary herpes gladiatorum at a 28-day wrestling camp. Jpn J Infect Dis. 2006;59:6-9
- van der Wouden JC, van der Sande R, van Suijlekom-Smit LWA, et al. Interventions for cutaneous molluscum contagiosum. Cochrane Database Syst Rev. 2009;4:CD004767
- Anderson BJ, McGuire DP, Reed M, Foster M, Ortiz D. Prophylactic valacyclovir to prevent outbreaks of primary herpes gladiatorum at a 28-day wrestling camp: a 10-year review. Clin J Sport Med. 2016;26:272-278.
- Anderson BJ. Prophylactic valacyclovir to prevent outbreaks of primary herpes gladiatorum at a 28-day wrestling camp. Jpn J Infect Dis. 2006;59:6-9.
- Rajasagi NK, Rouse BT. Application of our understanding of pathogenesis of herpetic stromal keratitis for novel therapy. Microbes Infect. 2018 Oct – Nov;20(9-10):526-530.
- Genital Herpes – CDC Fact Sheet (Detailed). https://www.cdc.gov/std/herpes/stdfact-herpes-detailed.htm
- Anderson BJ, McGuire DP, Reed M, Foster M, Ortiz D. Prophylactic valacyclovir to prevent outbreaks of primary herpes gladiatorum at a 28-day wrestling camp: a 10-year review. Clin J Sport Med. 2016;26:272-278
- Usatine RP, Tinitigan R. Nongenital herpes simplex virus. Am Fam Physician. 2010;82:1075-1082.
- Pecci M, Comeau D, Chawla V. Skin conditions in the athlete. Am J Sports Med. 2009;37:406-418.
- Anderson BJ. The epidemiology and clinical analysis of several outbreaks of herpes gladiatorum. Med Sci Sports Exerc. 2003;35:1809-1814.
- Zinder SM, Basler RS, Foley J, Scarlata C, Vasily DB. National Athletic Trainers’ Association position statement: skin diseases. J Athl Train. 2010;45:411-428.
- Wilson EK, Deweber K, Berry JW, Wilckens JH. Cutaneous infections in wrestlers. Sports Health. 2013;5:423-437.
- Saleh D, Sharma S. Herpes Simplex Type 1. [Updated 2019 Dec 27]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK482197
- Giraldo D, Wilcox DR, Longnecker R. The Type I Interferon Response and Age-Dependent Susceptibility to Herpes Simplex Virus Infection. DNA Cell Biol. 2017 May;36(5):329-334
- Dworkin MS, Shoemaker PC, Spitters C, et al. Endemic spread of herpes simplex virus type 1 among adolescent wrestlers and their coaches. Pediatr Infect Dis J. 1999;18:1108-1109
- Mandell GL, Bennett JE, Dolin R, eds. Mandell, Douglas, and Bennett’s Principles and Practice of Infectious Diseases. 7th ed. Philadelphia, PA: Churchill Livingstone; 2010
- Geretti AM. Genital herpes. Sex Transm Infect. 2006;82:31-34
- Schmutzhard J, Merete Riedel H, Zweygberg Wirgart B, Grillner L. Detection of herpes simplex virus type 1, herpes simplex virus type 2 and varicella-zoster virus in skin lesions: comparison of real-time PCR, nested PCR and virus isolation. J Clin Virol. 2004;29:120-126
- Bope ET, Kellerman ED. Conn’s Current Therapy 2012: Expert Consult. Philadelphia, PA: Elsevier; 2012
- Anderson BJ. Valacyclovir to expedite the clearance of recurrent herpes gladiatorum. Clin J Sport Med. 2005;15:364-366
- Baker DA, Blythe JG, Miller JM. Once-daily valacyclovir hydrochloride for suppression of recurrent genital herpes. Obstet Gynecol. 1999;94:103-106
- 2013-14 NCAA Sports Medicine Handbook. https://www.ncaa.org/sites/default/files/SMHB%20Mental%20Health%20INterventions.pdf
- Prevention Key to Reducing Skin Infections in High School Wrestling. https://www.nfhs.org/articles/prevention-key-to-reducing-skin-infections-in-high-school-wrestling