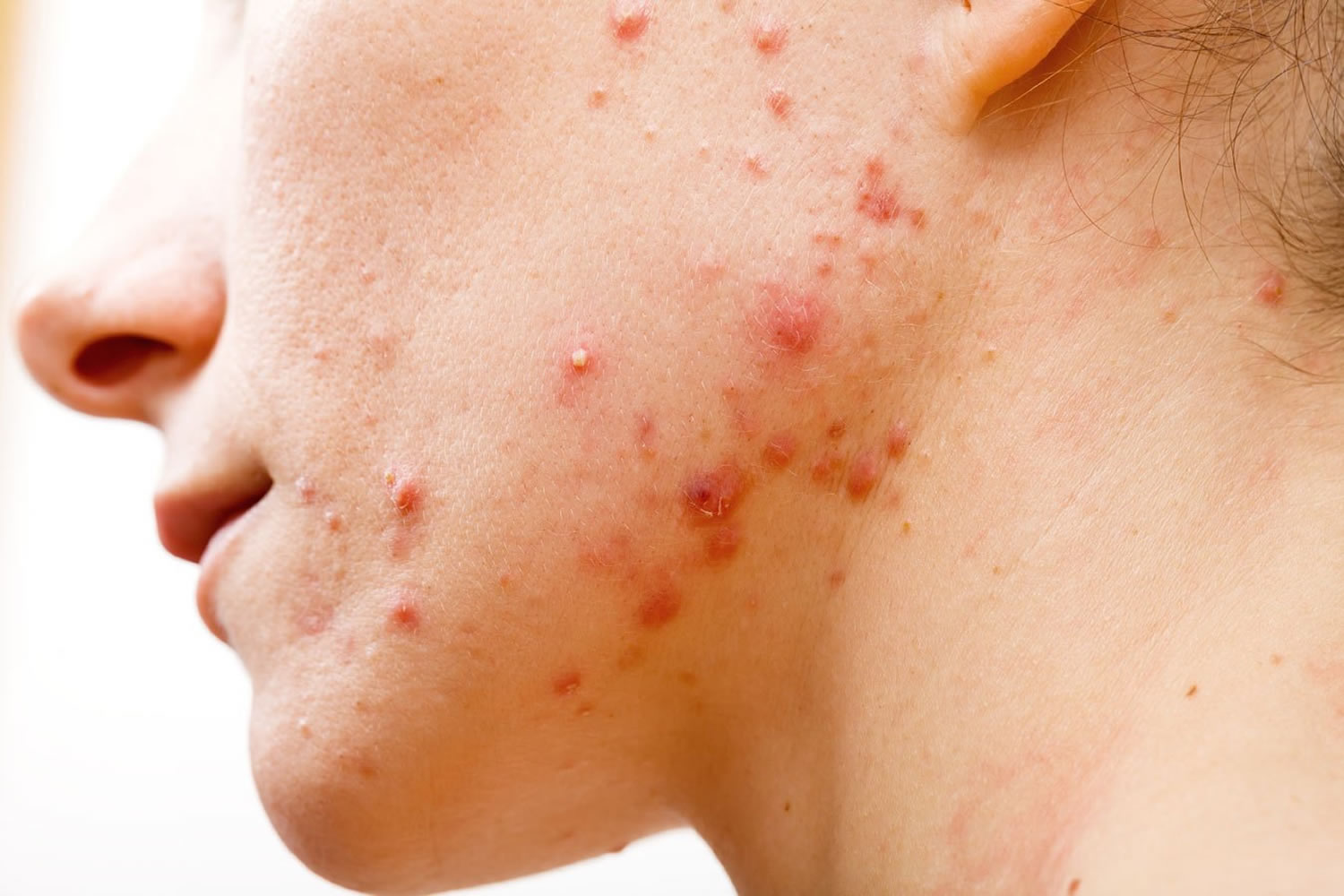
What is cystic acne
Cystic or nodulocystic acne is the most severe of the four main types of acne, which are comedonal, papular, pustular, and cystic that can affect the face, chest and back. It is characterized by multiple inflamed and uninflamed nodules and frequently, scars 1. It is more common in adolescent males.
The name cystic acne implies there are nodules (firm lumps) and cysts (fluid-filled cavities lined by epithelium) enclosing a mixture of keratin and sebum in varying proportions. However, the fluctuant lesions are not true cysts as there is no lining. They are sometimes called pseudocysts.
Cystic acne may result in low self-esteem, restriction of daily activity, and could lead to clinical depression. That is why it is important to treat cystic acne aggressively when starting therapy. The goal of treatment is not only to improve the patient’s appearance, but to reduce the risk of permanent scarring.
Conglobate acne is a severe cystic acne with nodules and suppurative lesions, and if associated with systemic symptoms is called acne fulminans.
Figure 1. Cystic acne on chin
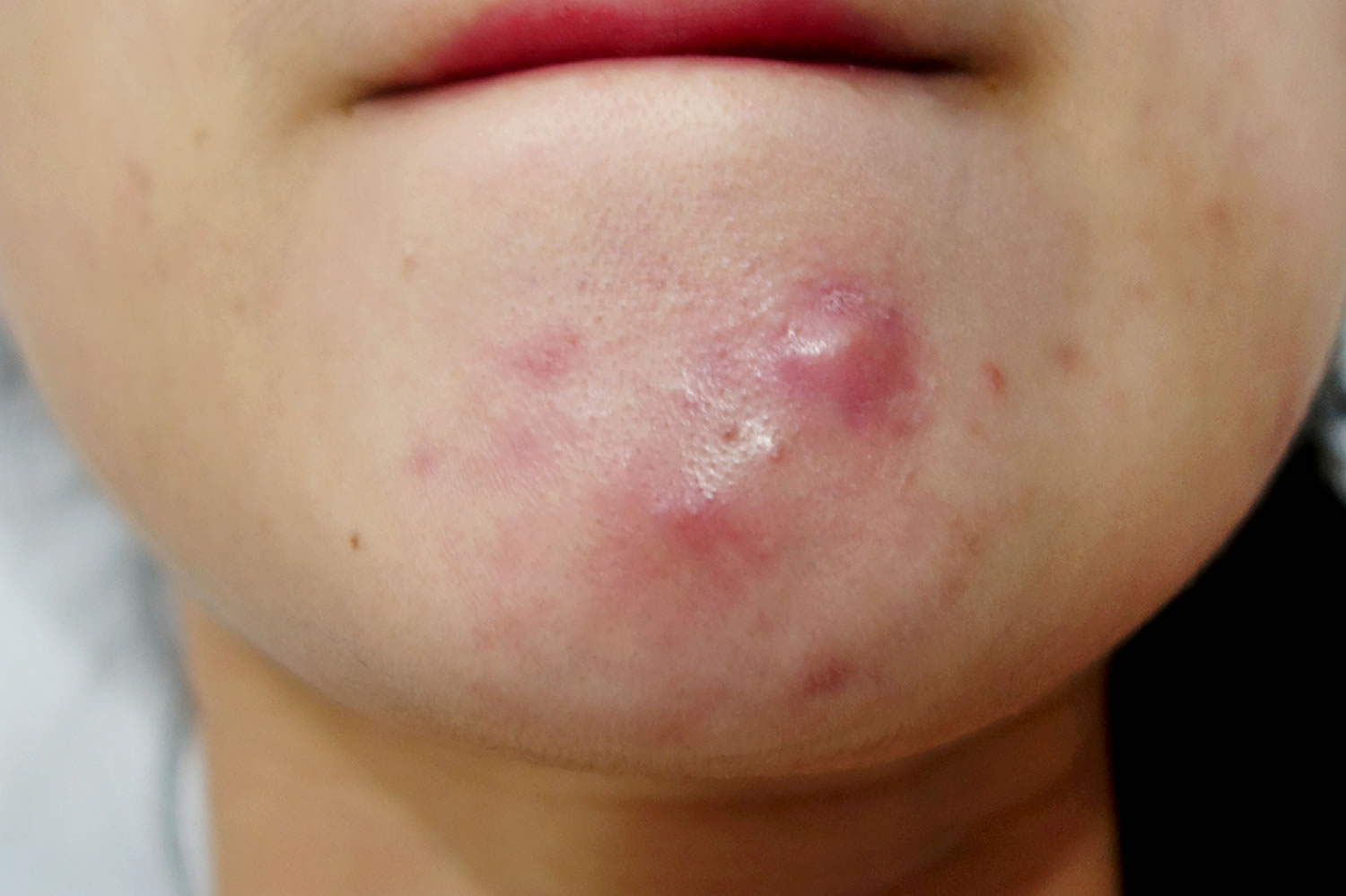
What causes cystic acne
The cause of cystic acne is multifactorial. The key factor is genetics 2. Acne develops as a result of an interplay of the following four factors 3:
- Release of inflammatory mediators into the skin
- Follicular hyperkeratinization with subsequent plugging of the follicle
- Cutibacterium acnes (previously called Proprionibacterium acnes) follicular colonization
- Excess sebum production
- Endogenous and exogenous androgenic hormones
- Distension and occlusion of the hair follicles
Research has shown that inflammatory responses actually occur before hyperkeratinization. Cytokines produced by CD4+ T cells and macrophages activate local endothelial cells to up-regulate inflammatory mediators such as vascular cell adhesion molecule-1 (VCAM-1), intercellular adhesion molecule-1 (ICAM-1), and human leukocyte antigen (HLA)–DR in the vessels around the pilosebaceous follicle 4.
Follicular hyperkeratinization involves increased keratinocyte proliferation and decreased desquamation, leading to sebum- and keratin-filled microcomedones 5.
Cutibacterium acnes is an anaerobic organism present in acne lesions. The presence of Cutibacterium acnes promotes inflammation through a variety of mechanisms. Cutibacterium acnes stimulates inflammation by producing proinflammatory mediators that diffuse through the follicle wall. Studies have shown that Cutibacterium acnes activates the toll-like receptor 2 on monocytes and neutrophils 6. Activation of the toll-like receptor 2 then leads to the production of multiple proinflammatory cytokines, including interleukins 12 and 8 and tumor necrosis factor. Hypersensitivity to Cutibacterium acnes may also explain why some individuals develop inflammatory acne vulgaris while others do not 7.
Excess sebum is another key factor in the development of acne vulgaris. Sebum production and excretion are regulated by a number of different hormones and mediators. In particular, androgen hormones promote sebum production and release 8. The degree of comedonal acne in prepubertal girls correlates with circulating levels of the adrenal androgen dehydroepiandrosterone sulfate (DHEAS) 9.
Numerous other mediators and receptors, including growth hormone and insulinlike growth factor, as well as peroxisome proliferator-activated receptors also regulate the sebaceous gland and may contribute to the development of acne 10. Furthermore, the sebaceous gland acts a neuroendocrine-inflammatory organ that is activated via corticotrophin-releasing hormones in response to stress and normal functions 11.
How to treat cystic acne
Treatment of nodulocystic acne can be challenging and may require a combination of medicines. Topical treatment is usually ineffective.
The causative factors for cystic acne must be removed or avoided to achieve successful treatment.
Systemic therapy is necessary for clinical improvement because topical agents do not penetrate deeply enough to affect change. The three primary groups of drugs used to treat cystic acne are systemic antibiotics, systemic hormonal or antiandrogen therapy, and systemic retinoids.
The recommended treatment for nodulocystic acne is usually isotretinoin, which should be commenced early to prevent scarring. The treatment is required for at least five months, and further courses are sometimes necessary.
Patients often need additional treatments, such as:
- Oral antibiotics
- Intralesional steroids
- Hormonal therapy in women.
What is isotretinoin ?
Isotretinoin (13-cis retinoic acid) is a vitamin-A derivative (retinoid). The liver naturally makes small quantities of isotretinoin from vitamin-A, but the drug doctors prescribe is made synthetically.
Isotretinoin was developed in the 1950s, but only started being used in the mid 1970s. The original brand names were Accutane® and Roaccutane®, but there are now many generic versions on the market, of varying potency.
Physicians, distributors, pharmacies, and patients must register in the iPLEDGE program (http://www.ipledgeprogram.com) before using isotretinoin. This program was established to prevent pregnancy in patients taking the medication. Isotretinoin is a potent teratogen (an agent which causes malformation of an embryo) and is associated with abnormalities of the face, eyes, ears, skull, central nervous system, cardiovascular system, thymus, and parathyroid glands. Negative pregnancy tests are mandated before starting therapy, then monthly before receiving a prescription refill, immediately after taking the last dose and one month after taking the last dose. The use of isotretinoin has been suggested to worsen depression and increase the risk of suicide, but no causal relationship has been established 12. Required laboratory monitoring during therapy includes a complete blood count, fasting lipid panel, and measurement of liver transaminase levels. Common adverse effects include headaches, dry skin and mucous membranes, and gastrointestinal upset 13.
What is isotretinoin used for ?
Isotretinoin is a very effective medication for the treatment of acne. Originally licensed for use in severe disease, it is increasingly prescribed for all grades of acne.
Isotretinoin is also useful for other follicular conditions, such as:
- Rosacea
- Seborrhoea
- Hidradenitis suppurativa
- Scalp folliculitis
It is also prescribed for many other skin diseases. Examples include:
- Discoid lupus erythematosus
- Granuloma annulare
- Grover disease
- Sarcoidosis
- Extensive actinic keratoses
- Prevention of squamous cell carcinoma
- As an adjuvant in neuroblastoma
Contraindications to isotretinoin
- Isotretinoin must not be taken in pregnancy, or if there is a significant risk of pregnancy.
- Blood donation by males and females on isotretinoin is not allowed in case the blood is used for a pregnant woman.
Precautions when taking isotretinoin
- Isotretinoin should be used with caution during breastfeeding.
- Commercial pilots may be subject to flying restrictions if they take isotretinoin.
- High dose isotretinoin in very young children has been associated with premature epiphyseal closure, leading to shorter stature (not seen in low dose for the treatment of acne).
Special precautions for pilots considering isotretinoin
Good night vision is important for airline pilots and those flying after dark. Night vision may be affected by isotretinoin. Pilots taking isotretinoin or considering a course of isotretinoin must report to their national aviation authority to discuss how this treatment affects their flying privileges.
How does isotretinoin work ?
In acne, isotretinoin:
- Reduces sebum production
- Shrinks the sebaceous glands
- Reduces follicular occlusion
- Inhibits growth of bacteria
- Has anti-inflammatory properties
What is the usual dose of isotretinoin ?
The range of doses used each day for acne is less than 0.1 to over 1 mg/kg body weight. Some patients may only need a small dose once or twice a week. A course of treatment may be completed in a few months or continue for several years. For acne, some prescribers have targeted a total cumulative dose of 120–140 mg/kg, in the hope of reducing relapse, but the evidence for this remains controversial. The general trend has been to use lower dosages, unrelated to body weight (eg 10 mg/day).
The individual dose prescribed by the dermatologist depends on:
- Prescriber preference
- Patient body weight
- The specific condition being treated
- Severity of the skin condition
- Response to treatment
- Other treatment used at the same time
- Side effects experienced
Isotretinoin is better taken with water or milk after food to help with its absorption. It may be taken on an empty stomach, but absorption may be halved. There is no particular advantage in splitting the dose over the day. A newer formulation (isotretinoin-lidose) can be taken without food.
For how long is isotretinoin taken ?
Most patients should be treated until their skin condition clears and then for a further few months. However, courses have often been restricted to 16–30 weeks (4–7 months) to minimise risk of teratogenicity (risk of congenital abnormalities), and to comply with local regulatory authorities. Isotretinoin may be prescribed for years, usually in low dose or intermittently.
Drug interactions with isotretinoin
Care should be taken with the following medications:
- Vitamin-A (retinoic acid): side effects are cumulative and could be severe. Beta-carotene (provitamin-A) is permitted.
- Tetracyclines (including doxycycline, minocycline): these could increase the risk of headaches and blurred vision due to raised intracranial pressure.
- Warfarin: monitor INR carefully.
What are the side effects and risks of isotretinoin ?
The side effects of isotretinoin are dose dependent; at 1 mg/kg/day, nearly all patients will have some side effects, whereas at 0.1 mg/kg/day, most patients will not. The range and severity of the side effects also depends on personal factors and the disease being treated.
Patients with significant liver or kidney disease, high blood fats, diabetes and depression may be advised not to take isotretinoin or to be on a lower dose than usual and to have regular follow-up visits.
Cutaneous and mucocutaneous side effects
Most of the side effects due to isotretinoin are cutaneous or mucocutaneous and relate to the mode of action of the drug. The most common are listed here. When side effects are troublesome, isotretinoin may need to be withheld or the dose reduced.
- Acne flare-up (particularly if starting dose is >0.5 mg/kg/day)
- Dry lips, cheilitis (sore, cracked or scaly lips) (100% of patients on 1 mg/kg/day)
- Dry skin, fragile skin, eczema/dermatitis (itchy, red patches of skin). Note: atopic eczema may improve.
- Increased sweating
- Dry nostrils, epistaxis (nose bleeds)
- Dry, watery or irritable eyes (especially in contact lens wearers), conjunctivitis, keratitis
- Dry anal mucosa, bleeding at the time of a bowel motion
- Dry genitals, dyspareunia (discomfort during intercourse)
- Facial erythema
- Sunburn on exposure to the sun
- Temporary hair loss
- Brittle nails
- Skin infections: impetigo, acute paronychia, pyogenic granuloma
Treatment of mucocutaneous side effects
- Reduce the dosage (eg to 5–10 mg/day)
- Emollients, lip balm, petroleum jelly, sunscreen, eye drops and lubricants should be applied frequently and liberally when needed
- Dermatitis can be treated with topical steroids
- Take short, cool showers without using soap
- Use mild or diluted shampoo
- Do not start wearing contact lenses for the first time
- Do not have elective eye surgery while on isotretinoin or for 6 months afterwards.
- Do not have ablative laser treatments (eg CO2 resurfacing) while on isotretinoin or for 6 months afterwards. Other laser and light treatments may be performed with care
- Shave rather than wax
- Topical and/or oral antibiotics may be prescribed for impetigo
- Headache
- Myalgia (muscle aches) and arthralgia (joint aches), especially after exercise
- Tiredness (lethargy and drowsiness)
- Disturbed night vision and slow adaptation to the dark. Drivers may experience increased glare from car headlights at night
- Hypertriglyceridaemia (high levels of triglyceride in the blood), usually of no clinical relevance
- Irregular or heavy menstrual periods
Rare side effects of isotretinoin
- Causality of the listed side effects may not have been confirmed
- Severe headache with blurred vision due to raised intracranial pressure
- Mood changes and depression. Note: depression is more often related to the skin condition being treated or other health or psychosocial problems.
- Antidepressant medications may be helpful
- Corneal opacities and cataracts
- High-tone deafness
- Accelerated diffuse interstitial skeletal hyperostosis (bony change)
- Abnormal liver function tests or symptomatic hepatitis
- Diarrhoea or bleeding from the bowel
- Pancreatitis
- Allergy to isotretinoin causing liver disease and a febrile illness
Treatment of systemic side effects
- Drink minimal alcohol
- Take paracetamol for headache and for mild aches and pains
- Seek medical attention early, if unwell
Monitoring isotretinoin
- Pregnancy must be excluded before and during treatment with isotretinoin.
In an otherwise healthy individual, blood tests are generally not needed. However, consider the following if using high dose (1 mg/kg/day), prolonged courses (>12 months), or if patients have specific risk factors (eg family history of dyslipidaemia, higher risk of viral hepatitis, etc):
- Cholesterol and triglyceride levels
- Liver function tests
- Blood count
Contraception in females considering isotretinoin
- Isotretinoin must NOT be taken in pregnancy because of a very high risk of serious congenital abnormalities in the baby. Caution needs to be used during breast-feeding as it enters the breast milk and might affect the baby.
All females who could biologically have a child should take the following precautions during treatment with isotretinoin and for four weeks after the medication has been discontinued:
- Abstinence. The most reliable method of avoiding pregnancy is not to have sex. No method of contraception is completely reliable. “Natural” family planning is particularly risky.
- If sexually active, two reliable methods of contraception should be used. Discuss contraception with your doctor (general practitioner, family planning specialist, gynaecologist or dermatologist). The combined oral contraceptive, IUD (intrauterine device), progesterone implant, or medroxyprogesterone injections may be suitable.
- The low-dose progesterone mini-pill on its own is not recommended.
A prescription for emergency contraception may be available from a medical practitioner (GP or family planning clinic) or accredited pharmacy. It prevents 85% of pregnancies if taken within 72 hours of unprotected sexual intercourse.
If contraception fails, termination of pregnancy (an abortion) may be advised if pregnancy arises during treatment with isotretinoin or within a month of discontinuing it.
What happens if a pregnant woman takes isotretinoin ?
Isotretinoin has a very high chance of resulting in a spontaneous miscarriage or a severe birth deformity if a fetus is exposed to it during the first half of pregnancy. The deformities affect the growth of tissues developing at the time of exposure to the drug:
- Cranium (skull and brain)
- Cardiac (heart)
- Eye, ear
- Limbs
No contraceptive precautions are necessary for men
Isotretinoin has no effect on sperm or male fertility and has not been shown to cause birth defects in children fathered by men taking it.
Does acne ever fail to clear on isotretinoin ?
Although isotretinoin is usually very effective for acne, occasionally it responds unexpectedly slowly and incompletely.
Poor response is associated with:
- Macrocomedones (large whiteheads)
- Nodules (large, deep inflammatory lesions)
- Secondary infection
- Smoking
- Polycystic ovarian syndrome
- Younger age (<14 years)
Options available to slow responders include:
- Electrocautery of comedones
- Prolonged course of isotretinoin
- Additional treatment with oral antibiotics and oral steroids
Can isotretinoin be used again if acne recurs ?
At least fifty per cent of patients with acne have a long lasting response after a single adequate course of isotretinoin. In others, acne may recur a few months to a few years after the medication has been discontinued. Relapse is more common in females than in males, and in patients >25 years of age. These patients may receive one or more further courses of isotretinoin.
Long-term treatment (>1 year) is often used for patients with:
- Persistent acne
- Seborrhoea
- Rosacea
- Scalp folliculitis
- Skin cancer.
Oral antibiotics
Oral antibiotics are effective for the treatment of moderate to severe acne (Table 1) 12. The best-studied antibiotics include tetracycline and erythromycin. Based on expert consensus on relative effectiveness, the American Academy of Dermatology recommends using doxycycline and minocycline (Minocin) rather than tetracycline 12. Trimethoprim/sulfamethoxazole (Bactrim, Septra) and trimethoprim alone may be used if tetracycline or erythromycin cannot be tolerated. Because of the potential for bacterial resistance with the use of an oral antibiotic, it is recommended that benzoyl peroxide be added to any regimen of oral antibiotics 14. Tetracycline is preferred over erythromycin because of the higher rates of resistance associated with erythromycin 12.
After individual treatment goals have been met, oral antibiotics can be discontinued and replaced with topical retinoids for maintenance therapy 14. Topical retinoids are sufficient to prevent relapses in most patients with acne vulgaris, especially if the disease was originally classified as mild or moderate. If the patient’s acne was initially classified as severe inflammatory, benzoyl peroxide with or without an antibiotic can be added for maintenance therapy 14.
Table 1. Selected Oral Antibiotics for the Treatment of Cystic Acne
| Agent | FDA pregnancy category | Adverse effects | Dosage | Estimated cost generic (brand)* |
|---|---|---|---|---|
Doxycycline | D | Photosensitivity, pseudotumor cerebri, esophageal irritation | 50 to 100 mg once or twice per day | $15 ($71 to $363) |
Erythromycin | B | Gastrointestinal upset | 250 to 500 mg two to four times per day | $73 to $340 (NA) |
Minocycline (Minocin) | D | Vestibular dysfunction, photophobia, hepatotoxicity, lupus-like reaction, pseudotumor cerebri | 50 to 100 mg once or twice per day | $21 to $59 ($173 to $675) |
Tetracycline | C | Gastrointestinal upset, photosensitivity, pseudotumor cerebri | 250 to 500 mg once or twice per day | $8 (NA) |
Trimethoprim/sulfamethoxazole (Bactrim, Septra) | C | Allergic reactions | 160/800 mg twice per day | $33 ($194) |
FDA = U.S. Food and Drug Administration; NA = not available.
*—Estimated retail price of one month’s treatment based on information obtained at http://www.lowestmed.com.
Side effects and risks of oral antibiotics
Allergy – oral antibiotics can cause a variety of rashes in those susceptible. These can be mild or life-threateningly severe. Allergy to a tetracycline or to erythromycin is very uncommon, but more than 2% of those on trimethoprim or cotrimoxazole become allergic to it. Tell your doctor if you have ever reacted badly to an antibiotic.
Photosensitivity may be a problem for those taking doxycycline. Taking the medicine after the evening meal reduces the risk of sunburn. Dress up and protect your skin from exposure to the sun.
Gastrointestinal disturbance affects about 5% of patients and includes nausea, colicky pain and diarrhoea.
Thrush (Candida albicans infection) affects 5% of treated women and most often affects the vagina. Thrush can also affect the oral mucosa or body folds (intertrigo), particularly in diabetics or in obesity. Thrush is less likely with erythromycin than with tetracycline.
Bacterial resistance may occur but is less common with the use of oral antibiotics than with topical antibiotics.
Acne antibiotics are unlikely to result in failure of the oral contraceptive pill but if you are concerned, add a barrier method and talk to your doctor about your risks.
Controversies in use of antibiotics for acne
Antibiotics are moderately effective for acne and are frequently used for moderate to severe acne treatment. They are often prescribed for months or years, because acne is a chronic skin condition. However, many physicians are concerned about the use of antibiotics for acne, mainly because of reports of increasing rates of bacterial resistance to antibiotics.
Bacterial resistance and serious infections including cellulitis, pneumonia, tuberculosis and diarrhoeal illnesses are a global threat. New, more expensive antibiotics are often less well tolerated than older agents and are unavailable in many countries. Very few new antibiotics are being discovered or brought to market.
What is Intralesional steroid injection ?
Intralesional steroid injection involves a corticosteroid, such as triamcinolone acetonide or betamethasone suspension, which is injected directly into a lesion on or immediately below the skin.
Shorter-acting corticosteroid preparations, such as dexamethasone or betamethasone acetate, are sometimes administered in combination with triamcinolone.
What are intralesional steroids used for ?
Intralesional steroid injection may be indicated for the following skin conditions:
- alopecia areata
- discoid lupus erythematosus
- keloids/hypertrophic scars
- granuloma annulare
- Other granulomatous disorders such as cutaneous sarcoidosis or granuloma faciale
- hypertrophic lichen planus
- lichen simplex chronicus (neurodermatitis)
- localised psoriasis
- necrobiosis lipoidica
- acne cysts (nodulocystic acne)
- small infantile haemangiomas
- other localised inflammatory skin diseases.
Contraindications to intralesional steroid
Intralesional steroids should not be injected at the site of active skin infection e.g., impetigo (school sores) or herpes simplex (cold sores).
They must not be used if there is a previous history of triamcinolone hypersensitivity (allergy).
When large doses of triamcinolone acetonide injections are used as an alternative to oral steroids such as prednisone, they are considered to be systemic steroids. These should be avoided in patients with the following disorders.
- Active tuberculosis or systemic fungal infections
- Extensive plaque psoriasis, pustular psoriasis or erythrodermic psoriasis – systemic steroids may destabilise condition
- Active peptic ulcer disease
- Uncontrolled diabetes, heart failure or severe hypertension
- Severe depression or psychosis
Side effects arising at the site of intralesional steroid injection
Side effects and risks of intralesional triamcinolone may be separated into early and delayed effects.
Early effects tend to be self-limited. They include:
- Pain, bleeding, bruising
- Infection
- Contact allergic dermatitis due to the preservative, benzyl alcohol
- Impaired wound healing
- Sterile abscess, sometimes requiring surgical drainage
Delayed adverse effects include:
- Cutaneous and subcutaneous lipoatrophy (most common) appearing as skin indentations or dimples around the injection sites a few weeks after treatment; these may be permanent.
- White marks (leukoderma) or brown marks (postinflammatory pigmentation) at the site of injection or spreading from the site of injection – these may resolve or persist long term.
- Telangiectasia, or small dilated blood vessels at the site of injection. These can be treated if necessary by laser or intense pulsed light (IPL).
- Increased hair growth at the site of injection (localised hypertrichosis) – this resolves eventually.
- Localised or distant steroid acne: steroids increase growth hormone, leading to increased sebum (oil) production by the sebaceous glands. Steroid acne generally improves once the steroid has been stopped.
Systemic side effects of triamcinolone injections
Allergic reactions are very rare, and dose independent but may include local or generalised urticaria (wheal and flare), and in more severe cases, anaphylaxis (angioedema, swollen face/tongue, respiratory distress, hypotension/shock).
Other systemic side-effects are not likely to follow intralesional injection of localised skin disease because the dose used is very small.
What is anti-androgen therapy ?
Anti-androgen therapy refers to medication taken by women to counteract the effect of male sex hormones such as testosterone on the skin.
- Anti-androgens are not suitable for skin problems in men.
What are anti-androgens used for ?
Anti-androgen medications are used to treat signs of hyperandrogenism, including the following skin and hair disorders:
- Acne
- Seborrhoea
- Hirsutism
- Female pattern hair loss
- Hidradenitis suppurativa
How does anti-androgen therapy work ?
Anti-androgen therapy may:
- Block androgen receptor
- Reduce adrenal androgen production
- Reduce ovarian androgen production
- Reduce pituitary production of prolactin
- Inhibit 5-alpha reductase (this enzyme acts in the skin to increase dihyroxytestosterone)
- Reduce insulin resistance
Which drugs have anti-androgenic action ?
Androgen receptor blockers act on the sebaceous gland and base of the hair follicle. They include:
- Oral contraceptive (birth control pill) containing ethinylestrodiol (oestrogen) and an antiandrogenic progesterone. These include cyproterone acetate (co-cyprindiol or Diane™-35, Estelle™ 35 and Ginet-84™), drospirenone (Yasmin™, Yaz™) or dienogest (Valette™).
- Other low-dose combined oral contraceptives with minimal androgen effect. These contain ethinylestrodiol and desorgestrel, gestodene or norgestimate.
- Spironolactone 25-200 mg daily (Aldactone™, Spirotone™, Spiractin™), which is most useful in women over the age of 30 years.
- Cyproterone acetate 50 to 200 mg (Androcur™, Procur™, Siterone™ – available on prescription). This powerful anti-androgen is usually taken on days 1 to 10 of the menstrual cycle (conventionally, day 1 is the first day of menstruation).
Spironolactone and cyproterone may be effectively combined with cyproterone acetate/ethinyloestradiol or other oral contraceptive agent, partly because they cause menstrual irregularities and partly to prevent pregnancy. The combined treatment is not necessary in post-menopausal women.
What are the clinical effects of anti-androgen therapy ?
In acne, the effects of anti-androgens include:
- Reduced sebum production
- Reduced comedone formation
They can be combined with other topical and oral treatments for acne.
Spironolactone
Spironolactone is a potassium-sparing medication used as a diuretic medication for heart failure, liver disease and high blood pressure. However, it has also been found useful for hirsutism, acne and seborrhoea because it has anti-androgenic properties. Spironolactone mainly works by blocking androgen receptors.
Spironolactone (Aldactone®), at a dose of 100mg daily, works well as an antiandrogen, but must be used in combination with oral contraceptives in women of childbearing age.
Side-effects for Spironolactone are rare but may include menstrual irregularities, breast tenderness, dizziness, and fatigue. Hypokalemia is extremely rare in patients who are not taking concurrent diuretics.
The dose of spironolactone is usually slowly increased from 25 to 200 mg daily, taken at night. It is sometimes prescribed cyclically to reduce menstrual irregularities, eg, for 3 weeks out of every 4 weeks or days 5–21 of the menstrual cycle. It may take six or more months to see improvement in the skin condition.
Side effects of spironolactone include:
- Nausea, diarrhoea, gastrointestinal bleeding
- Drowsiness (possibly due to high blood potassium levels)
- Headache and dizziness
- Menstrual cycle irregularities including increased frequency of menstruation, bleeding in the middle of the month or stopping periods altogether (amenorrhoea)
- Breast pain
Potassium, other electrolytes and creatinine levels in the blood are often monitored. This is especially necessary in older women, if high doses are prescribed, in patients taking other medicines (due to drug interactions) and in those with heart or kidney problems. Spironolactone should not be taken in pregnancy or during lactation.
Serum potassium should be ≤5.0mmol/L and renal function should be normal before starting spironolactone.
Monitor potassium and creatinine after one week on spironolactone, monthly for the first 3 months and then 2 to 4 times each year
Spironolactone is prohibited in athletic competition (requires therapeutic use exemption).
Systemic Hormonal Therapy Treatment (for Women)
Hormonal therapy can be used whether or not hormonal abnormalities have been demonstrated.
Progesterone-only oral contraceptives are not effective in the management of androgen-mediated skin conditions.
Combined oral contraceptives contain two hormones, ethinyloestrodiol 20–35 mcg (an oestrogen) and a progesterone. They prevent pregnancy by suppressing ovulation and changing cervical mucus. There are various kinds of progesterone, which may be androgenic in nature and thus unsuitable for those androgen-mediated skin conditions (particularly levonorgesterol and norgestrel). Anti-androgenic or minimally androgenic progesterones (see above) are indicated in these women.
- The progestational antiandrogen-containing contraceptives, i.e., 2mg cyproterone acetate and 0.35ìg ethinyl estradiol (Diane-35®), or 3.0mg drospirenone and 0.030mg ethinyl estradiol (Yasmin®) work best. The side-effect profile is similar to other oral contraceptive pills.
Their effect in hyperandrogenism is to reduce production of androgens by the ovaries, by the adrenals and at the receptor level in the skin. They also decrease circulating testosterone by increasing sex hormone binding globulin (SHBG).
Combined oral contraceptives are available as 21-day and 28-day packs; start on Day 1 (conventionally, day 1 is the first day of menstruation) and take one a day for 21 days. Then have a 7-day break (21-day pack) or take the placebo tablets for a week (28-day pack) before starting the cycle again. During this time, you can expect a withdrawal bleed (a period).
Combined oral contraceptives can increase the risk of thromboembolism (blood clots blocking blood vessels), especially in those with an inherited tendency (“thrombophilia”), or who smoke.
The combined oral contraceptive may be unsuitable if the patient:
- Has had a previous blood clot (thrombosis, embolism or ‘DVT’)
- Has high blood pressure (hypertension) or heart disease
- Smokes
- Is significantly overweight (obese)
- Has recently undergone surgery or trauma or is immobile
- Is undertaking long distance air travel (4 hours or more)
- Has a family member aged less than 50 years who has had blood clots or high blood pressure
Many of these women can instead use progesterone-only contraceptive pills while they are being treated with spironolactone or cyproterone.
Oral contraceptives can sometimes aggravate migraine and are inadvisable in those with significant liver disease. They may occasionally increase the risk of certain uncommon forms of breast cancer. They must not be taken in pregnancy.
On the other hand, the combined oral contraceptive reduces the risk of ovarian and endometrial cancer, benign breast disease, ectopic pregnancy, painful periods, iron deficiency anaemia and pelvic inflammatory disease.
Cyproterone acetate/ethinyloestradiol (co-pyrindiol) should be discontinued in the following circumstances:
- Severe migraine (headache, visual disturbance, numb feelings)
- Any form of thrombosis (such as heart attack, stroke) or increased blood pressure
- In case of immobility (including due to surgery) or trauma (eg bad sprains)
- If an increase in number or severity of epileptic seizures occurs, or liver disease arises during treatment
- Pregnancy
As with other oral contraceptives, minor side effects may arise, especially in the first few weeks. These include:
- Breast tenderness (20%) and increase in bra size
- “Spotting” (irregular mild bleeding between periods) occurs in 10% of women in the first month, but only affects 3% by the sixth month. Rarely, periods may stop altogether (amenorrhoea). If you have spotting (bleeding in between periods), see your doctor. He or she may advise you to take the active medication continuously for 3 months or more. This is quite safe and often prevents unwanted bleeding.
- Nausea, loss of appetite and bloating
- Headaches
- Increased appetite and weight increase (uncommon)
- Mood changes including depression and reduced libido
- Melasma (facial pigmentation)
- Hair loss (it is more common for hair fall to occur when the medication has been discontinued however)
- Acne.
Combined oral contraceptives with anti-androgenic components have advantages:
- They regulate the menstrual cycle in the majority of women
- Lighter, less painful periods occur in the majority of women
- Iron deficiency anaemia is less common because of less bleeding
- Increased “good” HDL cholesterol may protect against atherosclerosis (hardened arteries predisposing to heart disease)
- A decrease in the number and size of ovarian cysts occurs in polycystic ovarian syndrome
- Sebum production is reduced by 30%, resulting in worthwhile improvement in 80% of those with seborrhoea
- Acne usually improves by 40-50% by the third cycle and by 80-90% by the ninth cycle.
- More than 40% of women with facial hair (hirsutism) find it improves within 9 months, and many get worthwhile reduction in hair growth elsewhere as well.
Studies have demonstrated that the skin condition continues to improve even after the medication has been taken for a year. Combined oral contraceptives can usually be taken safely for many years.
Unfortunately, the skin condition tends to deteriorate again within a few months after the medication has been stopped.
New forms of oral contraceptive are introduced from time to time, to increase efficacy and reduce side effects.
Cyproterone acetate
Higher doses of cyproterone acetate are indicated for more severe cases of androgenetic skin conditions. It is effective for 70% of those with hirsutism.
Several different regimes are prescribed with doses ranging from 25 to 200 mg daily. Prior to the menopause, the medication is usually combined with cyproterone acetate/ethinyloestradiol or other oral contraceptive agent:
- To regulate menstrual cycle irregularities caused by the high dose cyproterone
- To prevent pregnancy; there are concerns that cyproterone could harm a male fetus by “feminising” it.
One system is to take the high dose cyproterone for the first ten days of the cycle.
Postmenopausal women and women who have had a hysterectomy can take cyproterone every day. It may be advisable to have a 7-day break every month. They may also take spironolactone.
Occasional significant side effects include:
- Liver disturbance
- Tiredness and depression
- Weight increase
- Nodulocystic acne. https://www.dermnetnz.org/topics/nodulocystic-acne/
- Goulden V, McGeown CH, Cunliffe WJ. The familial risk of adult acne: a comparison between first-degree relatives of affected and unaffected individuals. Br J Dermatol. 1999 Aug. 141(2):297-300.
- Thiboutot D, Gollnick H, Bettoli V, Dréno B, Kang S, Leyden JJ, et al. New insights into the management of acne: an update from the Global Alliance to Improve Outcomes in Acne group. J Am Acad Dermatol. 2009 May. 60(5 Suppl):S1-50.
- Jeremy AH, Holland DB, Roberts SG, Thomson KF, Cunliffe WJ. Inflammatory events are involved in acne lesion initiation. J Invest Dermatol. 2003 Jul. 121(1):20-7.
- Norris JF, Cunliffe WJ. A histological and immunocytochemical study of early acne lesions. Br J Dermatol. 1988 May. 118(5):651-9.
- Kim J, Ochoa MT, Krutzik SR, et al. Activation of toll-like receptor 2 in acne triggers inflammatory cytokine responses. J Immunol. 2002 Aug 1. 169(3):1535-41.
- Webster GF. Inflammatory acne represents hypersensitivity to Propionibacterium acnes. Dermatology. 1998. 196(1):80-1.
- Pochi PE, Strauss JS. Sebaceous gland activity in black skin. Dermatol Clin. 1988 Jul. 6(3):349-51.
- Lucky AW, Biro FM, Simbartl LA, Morrison JA, Sorg NW. Predictors of severity of acne vulgaris in young adolescent girls: results of a five-year longitudinal study. J Pediatr. 1997 Jan. 130(1):30-9.
- Trivedi NR, Cong Z, Nelson AM, Albert AJ, Rosamilia LL, Sivarajah S, et al. Peroxisome proliferator-activated receptors increase human sebum production. J Invest Dermatol. 2006 Sep. 126(9):2002-9.
- Zouboulis CC, Böhm M. Neuroendocrine regulation of sebocytes — a pathogenetic link between stress and acne. Exp Dermatol. 2004. 13 Suppl 4:31-5.
- Strauss JS, Krowchuk DP, Leyden JJ, American Academy of Dermatology/American Academy of Dermatology Association, et al. Guidelines of care for acne vulgaris management. J Am Acad Dermatol. 2007;56(4):651–663.
- James WD. Clinical practice. Acne. N Engl J Med. 2005;352(14):1463–1472.
- Thiboutot D, Gollnick H, Bettoli V, et al. New insights into the management of acne: an update from the Global Alliance to Improve Outcomes in Acne group. J Am Acad Dermatol. 2009;60(5 suppl):S1–S50.