Hyporeflexia
Hyporeflexia refers to reduced, weak or absent neurologic deep tendon reflexes or muscle stretch reflexes such as the knee-jerk reaction. Hyporeflexia can be detected through the use of a reflex hammer. It is the opposite of hyperreflexia. Isolated hyporeflexia or hyperreflexia without other clinical findings is generally not considered pathological 1.
Below are the 6 commonly tested muscle stretch reflexes, in the following format 1:
Name: Spinal level, peripheral nerve, location struck to elicit.
- Biceps: C5-C6, musculocutaneous, just anterior to the elbow
- Triceps: C7-C8 (predominantly C7), radial, just posterior to the elbow
- Brachioradialis: C5-C6, radial, about 10 cm above the wrist on the radial aspect of the forearm
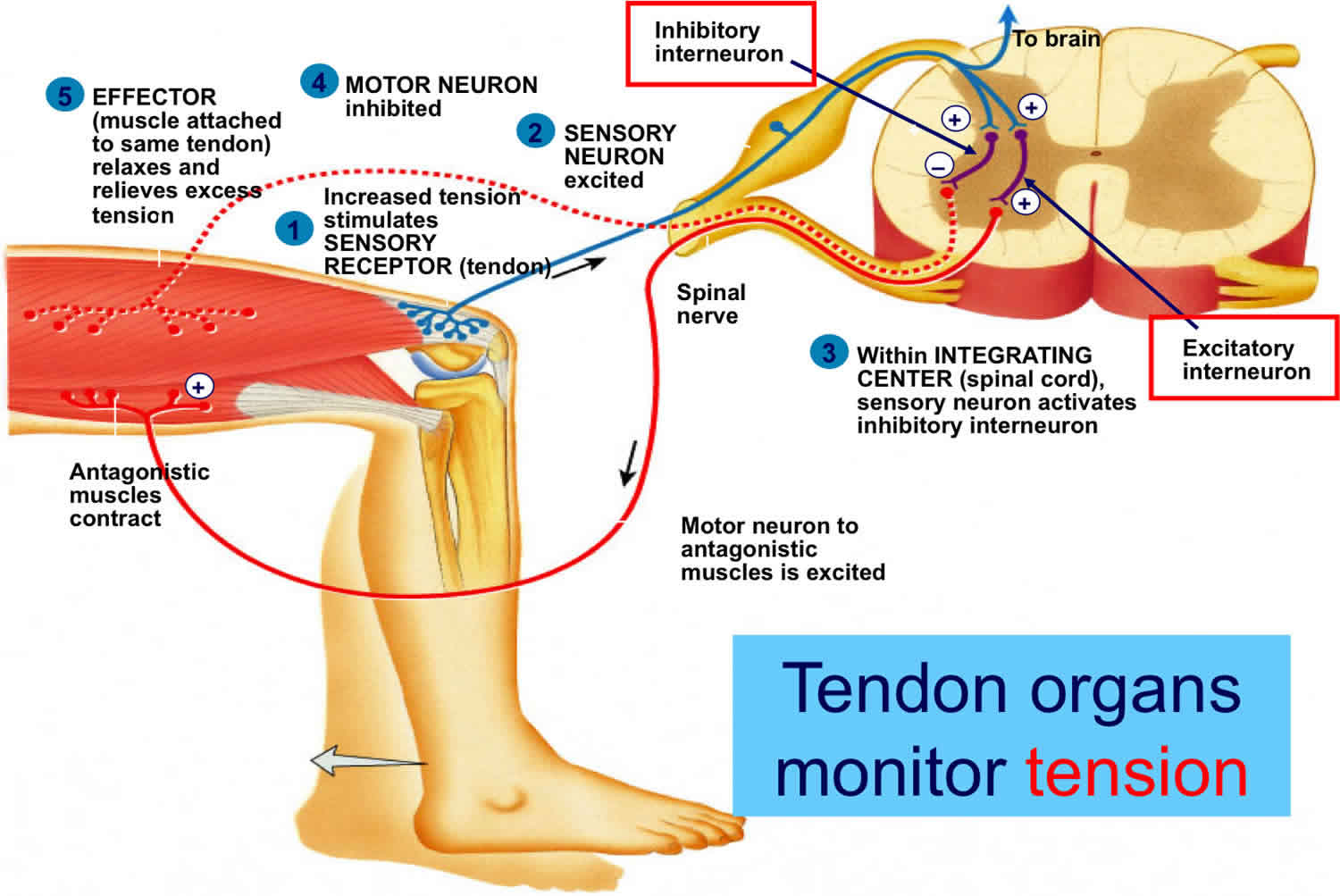
- Knee (quadriceps, patellar): L2-L4 (predominately L4), femoral, just inferior to the patella
- Ankle (Achilles): S1, tibial, posterior to the ankle joint on the achilles tendon (or for alternative location see below)
- Jaw Jerk (masseter): Pons, mandibular branch of trigeminal, chin (mental protuberance)
Reflexes are graded based on amplitude. Various scales have been used to grade reflexes. The National Institute of Neurological Disorders and Stroke Muscle Stretch Reflex Scale is frequently used and empirically supported[5]:
National Institute of Neurological Disorders and Stroke Scale 2:
- 0: Reflex absent
- 1: Reflex small, less than normal; includes a trace response or a response brought out only with reinforcement
- 2: Reflex in lower half of normal range
- 3: Reflex in upper half of normal range
- 4: Reflex enhanced, more than normal; includes clonus if present, which optionally can be noted in an added verbal description of the reflex
Plus or minus can indicate that the reflex was in between whole grades. Occasionally “5” is used to denote sustained clonus. One-half can alternatively indicate reinforcement was used.
Muscle stretch reflexes can indicate pathology along a particular nerve route, to a section of the spinal cord, or even reveal something about the general state of a patient’s peripheral nerves. For instance, presence of an ankle jerk reflex is a better predictor of peripheral neuropathy in diabetics than neuropathic symptoms, duration of diabetes, or retinopathy 3. An alteration in reflexes can also provide information on a patient’s electrolyte status due to the role of these charged molecules in the conduction of nerve impulses 4.
Due to the roles of the various pathways indicated in the anatomy section, hyperreflexia can indicate an upper motor neuron lesion, whereas hyporeflexia can indicate a lower motor neuron lesion 1. In other words, a lesion at C5 would cause hyporeflexia in the biceps reflex (C5-C6), but could produce hyperreflexia in the triceps reflex. This is because the lesion is above the spinal segments (C7-C8) that contribute to the lower motor neuron reflex arc but would affect the upper motor neuron modulation (which are generally inhibitory signals) of that arc instead 1. This is why one of the “lower motor neuron signs” is considered hyporeflexia (along with weakness, atrophy, and fasciculations), and conversely, “upper motor neuron signs” include hyperreflexia (along with weakness, spasticity, and Babinski sign) 1.. Put another way: inhibiting the inhibitor causes hyperreflexia, and this is what occurs with upper motor neuron lesions.
Hyporeflexia causes
Common causes of hyporeflexia:
- Becker muscular dystrophy
- Brown-Sequard syndrome
- Bulimia nervosa
- Charcot-Marie-Tooth disease
- Centronuclear myopathy
- Down’s syndrome
- Drug side effects of all-trans retinoic acid, cevimeline, clonidine, fluphenazine
- Folate deficiency
- Friedreich ataxia
- Guillain–Barré syndrome
- Lambert-Eaton myasthenic syndrome
- Lower motor neuron lesion
- Opioid intoxication
- Polyneuropathy (Achilles and plantar reflexes)
- Vitamin E deficiency
- Stroke
Life threatening causes of hyporeflexia:
Life-threatening causes include conditions which may result in death or permanent disability within 24 hours if left untreated.
- Spinal cord compression
- Stroke
- Penetrating neck injuries
Note that, in spinal shock, which is commonly seen in the transection of the spinal cord (spinal cord injury), areflexia can transiently occur below the level of the lesion and can, after some time, become hyperreflexic. Furthermore, cases of severe muscle atrophy or destruction could render the muscle too weak to show any reflex and should not be confused with a neuronal cause.
Hyporeflexia may have other causes, including hypothyroidism, electrolyte imbalance (e.g. excess magnesium), drug induced (e.g. the symptoms of benzodiazepine intoxication include confusion, slurred speech, ataxia, drowsiness, dyspnea, and hyporeflexia).
Hyporeflexia treatment
Hyporeflexia treatment involves treating the underlying cause.
References- Zimmerman B, Hubbard JB. Anatomy, Deep Tendon Reflexes (Stretch Reflexes) [Updated 2019 Jul 16]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2019 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK531502
- Hallett M. NINDS myotatic reflex scale. Neurology. 1993 Dec;43(12):2723.
- Shehab DK, Al-Jarallah KF, Abraham M, Mojiminiyi OA, Al-Mohamedy H, Abdella NA. Back to basics: ankle reflex in the evaluation of peripheral neuropathy in type 2 diabetes mellitus. QJM. 2012 Apr;105(4):315-20.
- Nick JM. Deep tendon reflexes, magnesium, and calcium: assessments and implications. J Obstet Gynecol Neonatal Nurs. 2004 Mar-Apr;33(2):221-30.