What is maltodextrin
Maltodextrin is a polysaccharide that is used as a food additive and as a carbohydrate supplement. As a supplement, maltodextrin is used to provide and sustain energy levels during endurance-oriented workouts or sports, to help build muscle mass and support weight gain. Maltodextrin is produced from starch and is usually found as a creamy-white hygroscopic powder. Polysaccharides are polymeric carbohydrate molecules composed of long chains of monosaccharide units bound together by glycosidic linkages, and on hydrolysis give the constituent monosaccharides or oligosaccharides. Maltodextrin is easily digestible, being absorbed as rapidly as glucose. Maltodextrin can be derived from any starch. They are industrially produced by enzymatic or acid hydrolysis of the starch, followed by purification and spray drying 1. In the US, this starch is usually rice, corn or potato; elsewhere, such as in Europe, it is commonly wheat. This is important for people with celiac disease, since the wheat-derived maltodextrin can contain traces of gluten. There have been recent reports of people with celiac disease reacting to maltodextrin in the United States. This might be a consequence of the shift of corn to ethanol production and its replacement with wheat in the formulation. The fast food chain, Wendy’s, footnotes maltodextrin in its list of gluten-free foods, which may be a sign of them receiving reports of this. Foods containing maltodextrin may contain traces of amino acids, including glutamic acid as a manufacturing by-product. The amino acid traces would be too small to have any dietary significance.
Maltodextrins the commercially available mostly white powders are of high purity and microbiological safety and are used in a wide range of food and beverage products, including baked goods and sports drinks 2. Although confusing to the average consumer, both digestible and resistant-to-digestion type of maltodextrins are commercially exploited as food ingredients under the same denominator 3. Maltodextrins can also be rendered indigestible to be used as a dietary fiber or prebiotic 4. Resistant maltodextrins are typically produced by purposeful rearrangement of starch or hydrolyzed starch to convert a portion of the normal alpha‐1,4‐glucose linkages to random 1,2‐,1,3‐, and 1,4‐alpha or ‐beta linkages. The human digestive system effectively digests only alpha‐1,4‐linkages, therefore the other linkages render the molecules resistant to digestion. The Glycemic Index (GI) of resistant maltodextrins is reported as less than 5, so indeed they are indigestible, as well as being tasteless.
Maltodextrins has an energy value of approximately 16 kJ/g (4 kcal/g), as underlined by international food law standards 5, digestible maltodextrins used in foods and beverages have long been considered to be a good source of energy 6. Most maltodextrins are fully soluble in water and exert other important functionalities, such as gelling or freeze control 7. As such, maltodextrins have found numerous applications in the food, beverage, dietetic, and medical food products, as well as in the pharmaceutical industry in tablet and powder applications 2.
Maltodextrins are classified by dextrose equivalent (glucose equivalent) and have a dextrose equivalent (glucose equivalent) between 3 and 20. The dextrose equivalent (glucose equivalent) corresponds to the amount of reducing sugars (in g) expressed as dextrose on 100 g dry matter in the product. Free D-glucose (dextrose) has a dextrose equivalent (glucose equivalent) of 100. The dextrose equivalent (glucose equivalent) of a maltodextrin correlates to the ratio of amylose and amylopectin content in the starch used to produce it; a higher amylopectin content correlates to a higher dextrose equivalent of a maltodextrin 8. Dried glucose syrups are, by definition, dried starch hydrolysis products with a dextrose equivalent greater than 20, whereas maltodextrins are defined as dried starch hydrolysis products with a dextrose equivalent equal to or lower than 20, but higher than 3 9. The higher the dextrose equivalent (glucose equivalent) value, the shorter the glucose chains, the higher the sweetness, the higher the solubility, and the lower heat resistance. Above dextrose equivalent (glucose equivalent) 20, the European Union’s CN code calls it glucose syrup; at dextrose equivalent (glucose equivalent) 10 or lower the customs CN code nomenclature classifies maltodextrins as dextrins. This crude yet relatively simple measurement is often used to express the degree of hydrolysis of starch; the higher the degree of hydrolysis, the higher the dextrose equivalent (glucose equivalent) 10.
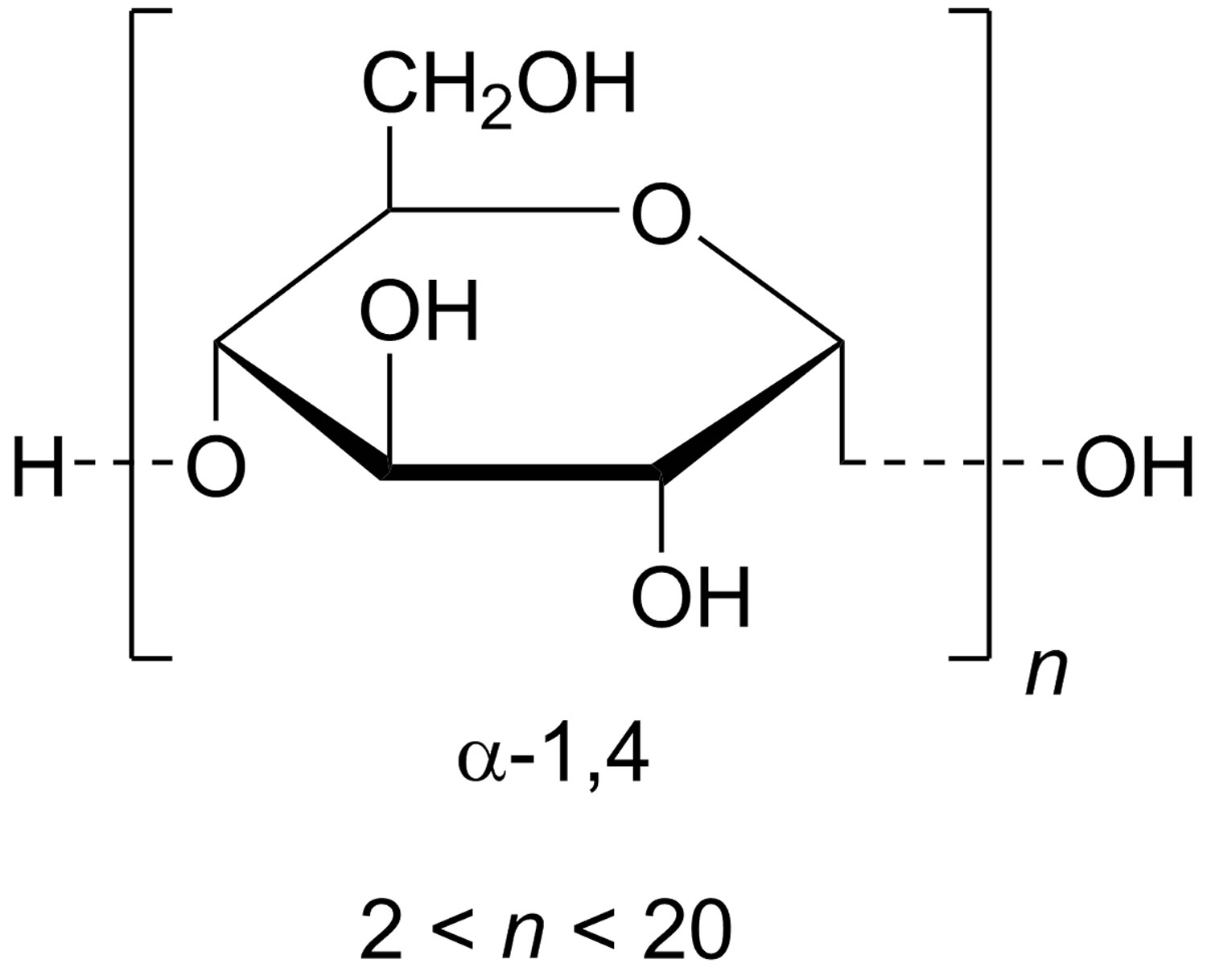
Figure 1. Maltodextrin (maltodextrin consists of D-glucose units connected in chains of variable length. The glucose units are primarily linked with α(1→4) glycosidic bonds. Maltodextrin is typically composed of a mixture of chains that vary from three to 17 glucose units long)
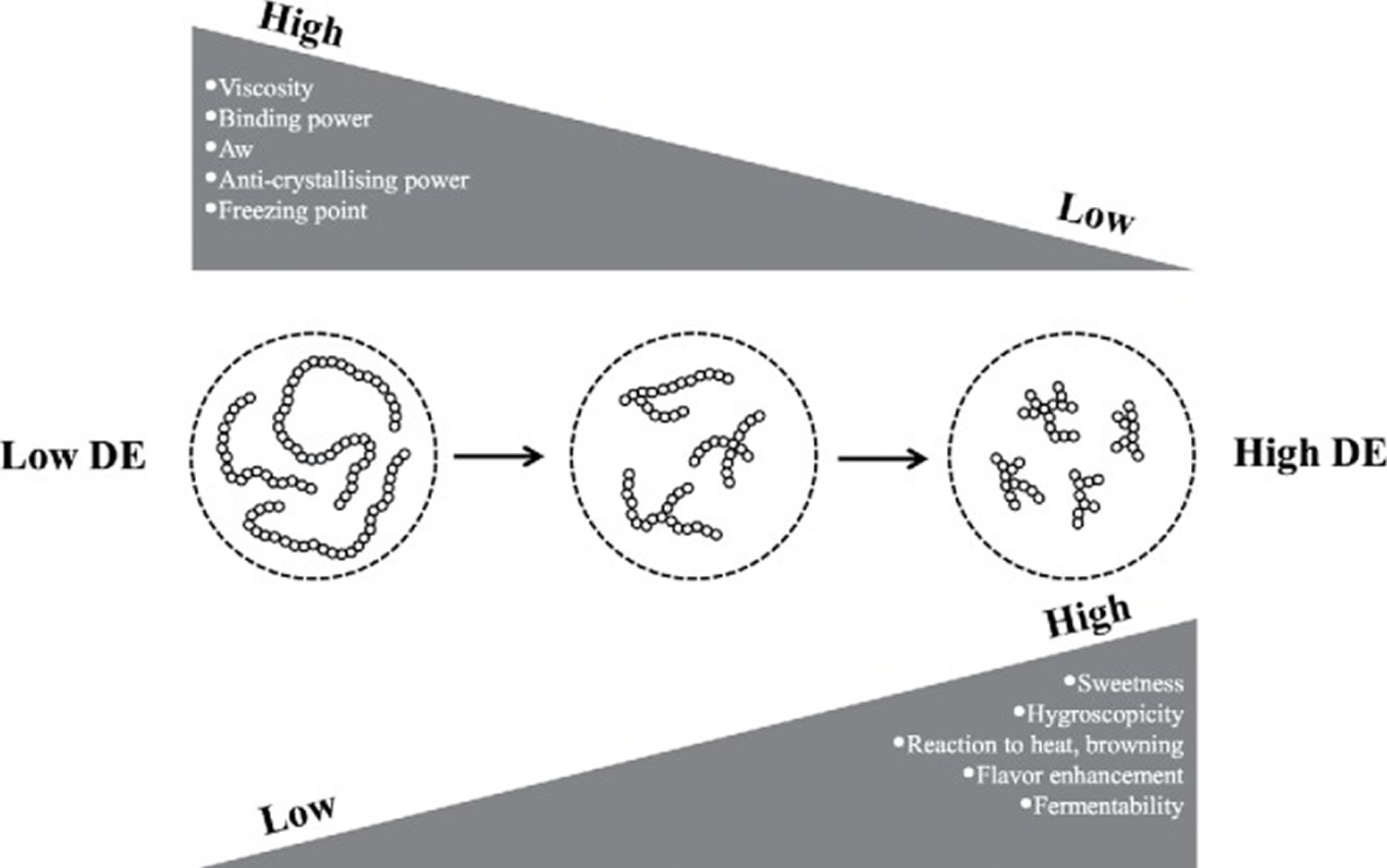
 The applicability of maltodextrins in food products is highly influenced by specific physicochemical and technological properties. Among these properties are viscosity, fermentability, solubility, hygroscopicity, freezing point depression, and osmolality. In turn, these properties of maltodextrins strongly depend on their botanical source, production process, and therefore dextrose equivalence. An overview of the relationships between several important physicochemical properties and different dextrose equivalents is depicted in Figure 2.
The applicability of maltodextrins in food products is highly influenced by specific physicochemical and technological properties. Among these properties are viscosity, fermentability, solubility, hygroscopicity, freezing point depression, and osmolality. In turn, these properties of maltodextrins strongly depend on their botanical source, production process, and therefore dextrose equivalence. An overview of the relationships between several important physicochemical properties and different dextrose equivalents is depicted in Figure 2.Figure 2. Maltodextrin properties related to the level of dextrose equivalence (DE)
Maltodextrin production
Maltodextrins are produced by hydrolysis of starch from different botanical sources. During the production process, native starch is heated in the presence of water, causing the crystalline structure of starch granules to swell and be broken irreversibly. This gelatinization process makes starch available for enzymatic or acidic degradation, or a combination of both 2. After degradation, chains of D-glucose units are left with varying length and appearance. Digestible maltodextrins (C6H10O5)nH2O) have a relatively short chain length and can be defined as saccharide polymers obtained from edible starch having a so-called dextrose equivalency (glucose equivalent) of less than 20 11.
What is maltodextrin glycemic index?
- Maltodextrin has Glycemic Index of 90-110 12
- Maltodextrin-Sucrose (mixture of 75% maltodextrin and 25% sucrose, adapted for sweetness) commonly found in sugar-sweetened beverages has Glycemic Index of 90
- Soy milk 250 gram, full-fat (3%), Original, 0 mg calcium, 17 gram of carbohydrate with maltodextrin has Glycemic Index of 44 and Glycemic Load of 8
- Soy milk 250 gram, full-fat (3%), Calciforte, 120 mg calcium, 18 gram of carbohydrate with maltodextrin has Glycemic Index of 36 and Glycemic Load of 6
- Soy milk 250 gram, reduced-fat (1.5%), Light, 120 mg calcium, 17 gram of carbohydrate with maltodextrin has Glycemic Index of 44 and Glycemic Load of 8
The Glycemic Index (GI) is the measure of the glycemic response (the extent to which blood glucose levels rise) obtained after the ingestion of a carbohydrate-containing food. The reference source is frequently 50 g of glucose; it (equals 100) is often used as a standard, whereas white bread is used less frequently 13. The Glycemic Load (GL) is the product of the amount of available carbohydrate in a specific serving size and the Glycemic Index value (using glucose as the reference food), divided by 100 14. It takes into account both quality and quantity of available carbohydrate 15.
Is maltodextrin gluten free?
According to the Celiac Disease Foundation 16, maltodextrin is considered gluten free. That is maltodextrin is generally considered gluten-free even when derived from corn, due to the processing. However, as we pointed earlier, wheat-derived maltodextrin can contain traces of gluten. There have been recent reports of people with celiac disease reacting to maltodextrin in the United States. This might be a consequence of the shift of corn to ethanol production and its replacement with wheat in the formulation.
The ‘wheat’ origin does not need to be labeled in the European Union. In Europe, maltodextrins are seen as gluten-free carbohydrate sources and are used in gluten-free products 5. Wheat-based maltodextrins are published on Annex II as products causing non-allergies or intolerances.
What does the term gluten-free mean?
- It means the product is less than 20-parts per million of gluten.
About how much gluten does it take to damage the villi of most people with celiac disease?
- About an eighth of a teaspoon of wheat flour contains enough gluten to damage the villi of most people with celiac disease. There are a portion of people with celiac who cannot even tolerate this much, but the vast majority that can tolerate this amount is how the 20-parts per million was determined.
Can you absorb gluten through your skin?
- No, you cannot absorb it through your skin.
Gluten-Containing Grains and Their Derivatives
- Wheat
- Varieties and derivatives of wheat such as:
- wheatberries
- durum
- emmer
- semolina
- spelt
- farina
- farro
- graham
- KAMUT® khorasan wheat
- einkorn wheat
- Rye
- Barley
- Triticale
- Malt in various forms including: malted barley flour, malted milk or milkshakes, malt extract, malt syrup, malt flavoring, malt vinegar
- Brewer’s Yeast
- Wheat Starch that has not been processed to remove the presence of gluten to below 20ppm and adhere to the U.S. Food and Drug Administration (FDA) Labeling Law*
*According to the FDA, if a food contains wheat starch, it may only be labeled gluten-free if that product has been processed to remove gluten, and tests to below 20 parts per million of gluten. With the enactment of this law on August 5th, 2014, individuals with celiac disease or gluten intolerance can be assured that a food containing wheat starch and labeled gluten-free contains no more than 20ppm of gluten. If a product labeled gluten-free contains wheat starch in the ingredient list, it must be followed by an asterisk explaining that the wheat has been processed sufficiently to adhere to the FDA requirements for gluten-free labeling.
When the U.S. Food and Drug Administration surveyed food products labeled “gluten free,” what percentage met that definition?
- Almost 99% of the products on the market indeed fell below 20-parts per million of gluten.
The Following Ingredients ARE SAFE On The Gluten-Free Diet 16:
- Caramel colors
- Dextrin
- Distilled vinegar
- Maltodextrin
- Maltose
- Natural flavors
- Yeast extract
The Following Ingredients Are NOT Safe On The Gluten-Free Diet 16:
- Malt
- Malt extract
- Malt flavor
- Malt syrup
Maltodextrin in food products
Through advances in science and technology, the knowledge on the (functional) application possibilities of maltodextrins in food and beverage products has improved significantly during the last 20 years. Due to their specific technological/functional properties and easy applicability, maltodextrins can substitute sucrose 17 or fat 18 and are being used in ice cream, dried instant food formulations, confectionary, cereals, snacks, and beverages 1.
Maltodextrin is sometimes used in beer brewing to increase the specific gravity of the final product. This improves the mouthfeel of the beer, increases head retention and reduces the dryness of the drink. Maltodextrin is not fermented by yeast, so it does not increase the alcohol content of the brew. It is also used in some snacks such as potato chips and jerky. It is used in “light” peanut butter to reduce the fat content, but keep the texture. Maltodextrin is also sometimes taken as a supplement by bodybuilders and other athletes in powder form or in gel packets.
Maltodextrin is used as an inexpensive additive to thicken food products such as infant formula. It is also used as a filler in sugar substitutes and other products.
Infant Nutrition
There is a strong nutritional reliance on lactose as a source of energy in early human development 19, preferably as part of the mother’s breast milk. However, lactase deficiency resulting in the inability to digest may lead to malabsorption-induced osmotic diarrhea in which approximately 40% of the energy provided may be lost 20. In such cases, maltodextrins can be used as a substitute for lactose to provide energy 21. In this respect, it is suggested also that the use of maltodextrins, instead of glucose is favorable since this helps reduce osmotic load and related intestinal distress 22. Maltodextrins are also used as a carbohydrate source in nonallergic infant formulae containing nondairy proteins (soy) or hydrolyzed proteins (hypoallergenic formulas).
Clinical Nutrition
In clinical nutrition, maltodextrins are applied in enteral and parenteral nutrition in which they can be combined with proteins for use of preoperative feeding and drinks 23. Administering preoperative drinks containing maltodextrins and protein, instead of using the conventional method of preoperative fasting, to patients undergoing major surgery for gastrointestinal malignancies seems to be a practical approach. For example, in one study, patients undergoing gastrointestinal surgery either received preoperative drinks containing 11% proteins, 70% maltodextrins, and 19% sucrose (intervention group) or fasted prior to their surgery (control group). Results showed that the average postoperative hospital stay of patients in the intervention group was 50% lower compared to the controls. In addition, the patients in the intervention group had a lower postoperative inflammatory reaction than the patients who did not receive the preoperative drinks 24. A different study investigated the effects of the administration of a preoperative drink containing maltodextrin and glutamine (maltodextrin and glutamine group) or only maltodextrin group prior to laparoscopic cholecystectomy. Patients included in the control group fasted prior to their surgery. Results showed a reduced biological response to surgical trauma by improving insulin sensitivity in patients in the maltodextrin and glutamine group, but not the maltodextrin group, compared to the control group 25.
Oral Rehydration Drinks
Early studies have indicated benefits of using maltodextrins in oral rehydration solutions (ORS) for individuals suffering from diarrhea over the use of glucose. In this respect, an early paper of Sandhu et al. 26 concluded that solutions with lower sodium and glucose-polymer content, compared to higher sodium content and higher osmolality due to the use of glucose, might be of nutritional benefit in the oral rehydration of acute infantile diarrhea.
At the same dry-weight concentration, the osmolality increases with increasing dextrose equivalence of the saccharide 27. Compared on a weight basis, the osmolality of maltodextrins is significantly lower than that of disaccharide sugars 28. El-Mougi et al 29 studied the use of maltodextrins in oral rehydration solutions and observed that the osmolality of a solution containing 50 g/L maltodextrin with a dextrose equivalent of 11–14 still had a slightly lower osmolality than a solution containing only 20 g/L glucose (227 mmol/L vs. 311 mmol/L, respectively).
Sports Rehydration Drinks
A low beverage osmolality supports gastric emptying rate and helps reduce gastrointestinal stress 30. Accordingly, aiming at a low beverage osmolality, maltodextrins are being used to replace sucrose or glucose in sport drinks. This is relevant since hypertonicity and related postingestion gastrointestinal distress symptoms are significant performance-limiting factors during running events such as marathons and triathlons exercise 31. Another effect of beverage hypertonicity is that it reduces water absorption rate. Vist and Maughan 30 evaluated the impact of carbohydrate load and osmolality on gastric emptying rate. In this respect, they compared drinks with markedly different osmolalities and caloric contents. Two concentrated drinks containing either 18.8% glucose (1300 mOsmol/kg) or 18.8% maltodextrins (237 msmol/kg) were consumed. The concentrated (188 g/L) maltodextrins emptied much faster (T1/2 = 64 + 8 min) than the corresponding concentrated isoenergetic glucose solution (HG, 1300 mosmol/kg, T1/2 = 130 + 18 min). The strong hyperosmolality induced by an equivalent amount of glucose but avoided by the use of maltodextrins appeared to have impacted significantly on gastric emptying rate. Recently, this area of research was reviewed by Shi and Passe 32. They concluded that water absorption in the human small intestine is influenced by osmolality, solute absorption, and the anatomical structures of gut segments 32.
Combining maltodextrins with a fructose supplying carbohydrate source may be beneficial when a high rate of carbohydrate supply is warranted. Shi et al 28 studied intestinal absorption of solutions containing either glucose or fructose combined with a glucose, either as free or directly transportable monosaccharides (glucose, fructose), bound as a disaccharide (sucrose), or as oligomers (maltodextrins). The authors showed that combining a glucose source with fructose resulted in better carbohydrate-water absorption rates, while using maltodextrins enabled osmolality to remain on the low side. The use of maltodextrins can play a significant role in this respect especially at carbohydrate concentration exceeding 40 g/l.
Sports Energy Drinks
Since there is a close relation between muscle fiber glycogen content and its ability to execute repeated high intensity contractions, either a reduced rate of glycogen breakdown or an increased glycogen content may help reduce fatigue and thus support performance capacity in field settings 33. Examining the effects of maltodextrins ingestion during exercise it was found that the ingestion of maltodextrin, like any other carbohydrate, decreases net glycogen breakdown during long-duration exercise while maintaining a high whole-body carbohydrate oxidation 34. Such responses appear to be similar for men and women 35.
One of the questions that has been answered recently concerned maximizing carbohydrate supply in periods of a high need, when absorption rate may be a limiting factor. It was shown that the synchronous intake of glucose + fructose favors a higher rate of carbohydrate absorption than glucose sources only. Accordingly, recent research has been done on the favorable ratio of glucose to fructose. Wallis et al. 36 studied the oxidation of combined ingestion of maltodextrins and fructose during exercise. They showed that with ingestion of substantial amounts of maltodextrin and fructose during cycling exercise, exogenous carbohydrate oxidation can reach peak values of approximately 1.5 g·min, and this is markedly higher than oxidation rates from ingesting maltodextrin alone.
Commercially available sports beverages generally consist of 6–10% concentrations of carbohydrates, of which high-glycaemic index (GI) carbohydrate sources such as maltodextrin are common constituents 37. Paradoxically, high-GI carbohydrates consumed within an hour of commencing a single bout of exercise may elicit rebound hypoglycemia 15–30 min into subsequent activity 38; a response for which the mechanisms, and performance consequences, are currently unclear 39. In a study aimed to examine the physiological and performance effects of high- and low-Glycemic Index (GI) carbohydrates consumed at two time-points before and during 120 min of simulated soccer-specific exercise 37. Blood glucose concentrations were better maintained throughout exercise and the magnitude of the exercise-induced rebound glycemic response was lowered in isomaltulose when compared to Maltodextrin. Furthermore, isomaltulose proved more effective in lowering the epinephrine response to prolonged exercise. Therefore, when limited opportunities exist to consume fluids during exercise, the consumption of low-GI isomaltulose before soccer-specific exercise may offer an alternative to the use of high-GI carbohydrates (e.g. maltodextrin) 37.
Sports Recovery Drinks
It has been shown that a combination of maltodextrins with protein and/or amino acids can promote enhanced glycogen recovery and stimulate muscle protein synthesis following an intense exercise protocol 40. Some observations suggest that effects on postexercise glycogen recovery and also muscle protein synthesis can be enhanced when a combination of different carbohydrates and protein is used 41. This observation is often used by the sports nutrition industry to promote carbohydrate–protein mixes for improving muscle strength, muscle power, and sports performance. However, results of studies into the effects of maltodextrins + protein on postglycogen recovery are mixed, with some showing positive effects and some showing no effect 42.
Applications Related to Oral Health
Frequent exposure of sugars to teeth is known to cause dental caries 43. This is a result of the fermentation of the sugars by microorganisms in dental plaque, leading to the formation of organic acids which in turn leads to the demineralization of enamel 44. Acid in drinks (as common in soft drinks and in juices) enhances this effect further 45.
For the last 10–15 years, food industry has increasingly been adding ‘new’ carbohydrates, such as maltodextrins and glucose syrups, to soft drinks instead of sucrose and fructose-glucose syrups 44. The effect of maltodextrins on oral health has been addressed in a number of studies 46. The general outcome of these studies has been first that maltodextrins are less potent in increasing acidity in the oral cavity compared to sucrose, and further that the rate of fermentation and acid formation increases with increasing dextrose equvalence. Al-Khatib et al 46 investigated the effect of three different maltodextrins on the pH of dental plaque in vivo in 10 adult volunteers using the plaque harvesting method. The three maltodextrins tested in this study were dextrose equvalent = 5.5, 14.0, and 18.5, made up as 10% solutions. Three commercially available maltodextrin-containing children’s drinks were also evaluated for their acidogenicity. 10% sucrose and 10% sorbitol solutions were used as positive and negative controls, respectively. The minimum pH achieved for dextrose equvalent = 5.5, 14.0, and 18.5 were 5.83 ± 0.30, 5.67 ± 0.24, and 5.71 ± 0.29, respectively, and were significantly higher compared with that for 10% sucrose (5.33 ± 0.17). The area under the curve was the least for dextrose equvalent = 5.5 (12.03 ± 4.64), followed by dextrose equvalent = 18.5 (13.13 ± 8.87) and dextrose equvalent = 14.0 (17.35 ± 6.43), but were all significantly smaller as compared with 10% sucrose (24.50 ± 8.64). It was concluded that, although a 10% maltodextrins solution was significantly less acidogenic than a 10% sucrose solution, both solution were impacting on tooth enamel.
Applications as Fat Replacer
Maltodextrins can be used as fat replacers due to their ability to form smooth, fat-like gels and their relatively high viscosity (depending on dextrose equvalent/the average number of monosaccharide units per molecule). Possible food categories for fat replacement via maltodextrins are low-fat salad dressings, spreads, margarines and butters, mayonnaise, and dairy products 47. Exchanging fat for maltodextrins, on a w/w basis, will reduce the energy content of the food, as maltodextrins contain less energy/g (resp. 16kJ vs. 38kJ). In this respect, it should be noted, however, that a replacement for fat will not necessarily lead to a reduction of food/energy intake 48.
One of the most important differences between maltodextrins and fats is the hydrophilic behavior of maltodextrins versus the lipophilic behavior of fats, properties that may affect the solubility of flavors and other compounds in a product. Recent findings suggest that the use of maltodextrins in high-energetic food products may help reduce the fat content up to 50%, thus reducing energy density without altering important properties and characteristics of these products 18. In practice, maltodextrins do not mimic all sensory properties of fat, making its use as fat replacer complex 18. Next to their fat-mimicking ability, research has shown that an additional benefit of the use of maltodextrins is their inhibition of the release of volatile odor compounds, making them, for example, suitable as fat-replacers in low-fat meat products 49.
Applications Related to Appetite Control
There is a strong correlation between the macronutrient composition of foods and differences in the way and intensity that foods induce satiety. In order of satiating potential the macronutrients are generally classified as follows: protein > carbohydrate > fat 50.
Maltodextrins, as a source of glucose, are suggested to enhance feelings of satiety. To test this hypothesis, Yeomans et al. 51 investigated the effects of consuming a soup with added maltodextrins on food intake, rated hunger, and fullness in 24 male volunteers. The soup was tested relative to a non-maltodextrin control soup, which was matched for sensory properties. Soup preloads were consumed 30 minutes before lunch and condition-order counterbalanced. Interestingly, the food intake at lunch was reduced significantly by 77 g (407 kJ) after the maltodextrin preload, and this reduced intake was associated with a significant reduction in eating rate but not in meal duration. Hunger ratings were significantly lower and fullness ratings significantly higher during the start of the meal after the maltodextrin preload when compared with the control 51. These results imply that the maltodextrin meal preloads can result in a reduced desire to eat, by mechanisms which remain to be clarified 52. However, several studies and a recent critical analysis of the literature revealed that the methodological set-up of satiety studies, using liquid meal pre-loads, has a significant influence on the outcomes of the studies 53. Accordingly, there is a lot of debate on the meaning of pre-load study results in relation to real life conditions.
Is maltodextrin bad?
In recent years, concerns have been raised about the increased use of refined carbohydrates, including isolated starches and maltodextrins, in food and beverage and its relation to increased obesity rates 54. One of the main reasons for concern is that, depending on the quantity consumed, refined carbohydrate sources can have a strong impact on the post-ingestion blood glucose, insulin, and lipid levels. Discernible changes in these markers have been linked to potential health risks, especially in vulnerable individuals such as diabetic patients 55. There is also report of maltodextrins in beer may be responsible for the phenomenon known as beer belly 56. In a rat experiment 57, ad libitum access (unlimited access) to maltodextrin produced at least as rapid weight gain as sucrose (sugar) and in rat experiment #2 a study to compare the impact of 10% sucrose with that of maltodextrin, retroperitoneal fat mass was greater in the two carbohydrate groups than in the control group (a control group maintained on standard chow and water alone). Moreover, in Experiment #3, impaired performance on a location recognition task was also found in both carbohydrate groups (sucrose and maltodextrin) after only 17 days on the diets. These results indicate that the harmful effects of excess sucrose consumption can also be produced by maltodextrin, another rapidly absorbed carbohydrate that does not contain fructose 57.
In the United States, maltodextrins are regulated under the Food and Drug Administration’s (FDA’s) Code of Federal Regulations (CFR) as a GRAS substance, meaning it is Generally Recognized As Safe 58 for use as an ingredient and a dietary fiber in milk and milk products; meat, poultry, fish and mixtures; dry beans, peas, other legumes, nuts and seeds; grain products; fruits and fruit products; vegetable products; fats, oils, and salad dressings, sugars, sweets, and beverages at levels ranging from 3.2 to 6.3 grams per serving.
The digestive end product of maltodextrins is glucose and glucose participates in many basic metabolic processes in your body. Maltodextrins are considered to be a good source of energy since glucose obtained from its digestion is readily absorbed in the small intestine and subsequently used in metabolism 59.
The rise in consumption of refined carbohydrate sources has been linked to an increased health risk 60. Although no causal relationship between the consumption of maltodextrins and negative health effects has been reported 61, this does not mean that overconsumption of foods containing maltodextrins will have no effect. The regular intake of calorie dense, low-fiber/protein foods or drinks with high levels of refined added carbohydrates, in particular soft drinks and sweet snacks, may easily induce a persistent positive energy balance resulting in weight gain, impaired insulin sensitivity as well as increased blood cholesterol and blood lipids 62, 63. Accordingly, consumers should consume in moderation and food and beverage producers should reduce the energy density of food and beverage while taking care for an appropriate nutrient, fiber, and protein level where possible.
References- Takeiti C., Kieckbusch T., Collares-Queiroz F. Morphological and physicochemical characterization of commercial maltodextrins with different degrees of dextrose-equivalent. Int. J. Food Propert. 2010:411–425.
- BeMiller J. N., Whistler R. L. Starch: Chemistry and Technology. London: Academic Press; 2009.
- The wars of the carbohydrates, part 6: what a name! Whelan WJ. IUBMB Life. 2008 Aug; 60(8):555-6. https://www.ncbi.nlm.nih.gov/pubmed/18543287/
- Physiological and metabolic properties of a digestion-resistant maltodextrin, classified as type 3 retrograded resistant starch. Brouns F, Arrigoni E, Langkilde AM, Verkooijen I, Fässler C, Andersson H, Kettlitz B, van Nieuwenhoven M, Philipsson H, Amado R. J Agric Food Chem. 2007 Feb 21; 55(4):1574-81. https://www.ncbi.nlm.nih.gov/pubmed/17253707/
- EC Regulation (EC) No 1169/2011 of the European Parliament and of the council of 25 October 2011 on the provision of food information to consumers. Off. J. Eur. Union. 2011:18–63.
- Altschul A. M. Low-calorie foods—a scientific status summary by the Institute of Food Technologists’ expert panel of food safety and nutrition. Food Techno. 1989:113.
- Stephen M. S., Philips G. O., Williams P. A. Food Polysaccharides and Their Applications. CRC Press; Boca Raton: 2006
- Coultate T. Food: The Chemistry of its Components. 2009
- On the molecular characteristics, compositional properties, and structural-functional mechanisms of maltodextrins: a review. Chronakis IS. Crit Rev Food Sci Nutr. 1998 Oct; 38(7):599-637.
- Fetzer W., Crosby E., Engel C., Kirst L. Effect of acid and heat on dextrose and dextrose polymers. Ind. Eng. Chem. 1953:1075–1083.
- Takeiti C., Kieckbusch T., Collares-Queiroz F. Morphological and physicochemical characterization of commercial maltodextrins with different degrees of dextrose-equivalent. Int. J. Food Propert. 2010:411–425
- Stevenson EJ, Watson A, Theis S, Holz A, Harper LD, Russell M. A comparison of isomaltulose versus maltodextrin ingestion during soccer-specific exercise. European Journal of Applied Physiology. 2017;117(11):2321-2333. doi:10.1007/s00421-017-3719-5. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5700989/
- Forbes L.E., Storey K.E., Fraser S.N., Spence J.C., Plotnikoff R.C., Raine K.D., Hanning R.M., McCargar L.J. Dietary patterns associated with glycemic index and glycemic load among Alberta adolescents. Appl. Physiol. Nutr. Metab. 2009;34:648–658. doi: 10.1139/H09-051
- Atkinson F.S., Foster-Powell K., Brand-Miller J.C. International tables of glycemic index and glycemic load values: 2008. Diabetes Care. 2008;31:2281–2283. doi: 10.2337/dc08-1239
- Salmeron J., Manson J.E., Stampfer M.J., Colditz G.A., Wing A.L., Willett W.C. Dietary fiber, glycemic load, and risk of non-insulin-dependent diabetes mellitus in women. JAMA. 1997;277:472–477. doi: 10.1001/jama.1997.03540300040031
- Sources of Gluten. Celiac Disease Foundation. https://celiac.org/live-gluten-free/glutenfreediet/sources-of-gluten/
- O’Brien-Nabors L. Alternative Sweeteners. Boca Raton, Florida, USA: CRC Press; 2011.
- Hadnađev M., Dokić L., Hadnađev T. D., Pajin B., Krstonošić V. The impact of maltodextrin-based fat mimetics on rheological and textural characteristics of edible vegetable fat. J. Texture Stud. 2011:404–411.
- Urashima T., Fukuda K., Messer M. Evolution of milk oligosaccharides and lactose: a hypothesis. Animal. 2011:369.
- Siddiqui Z., Osayande A. S. Selected disorders of malabsorption. Primary Care. 2011:395–414. vii.
- Maldonado J., Gil A., Narbona E., Molina J. A. Special formulas in infant nutrition: a review. Early Hum. Dev. 1998;(Supplement 1):S23–S32.
- Gregorio G. V., Gonzales M. L. M., Dans L. F., Martinez E. G. Cochrane review: Polymer-based oral rehydration solution for treating acute watery diarrhoea. Evid. Based Child Health: A Cochrane Rev. J. 2010:1612–1675.
- Cabre E., Gonzalez-Huix F., Abad-Lacruz A., Esteve M., Acero D., Fernandez-Bañares F., Xiol X., Gassull M. A. Effect of total enteral nutrition on the short-term outcome of severely malnourished cirrhotics. A randomized controlled trial. Gastroenterology. 1990:715–720.
- Pexe-Machado P. A., de Oliveira B. D., Dock-Nascimento D. B., de Aguilar-Nascimento J. E. Shrinking preoperative fast time with maltodextrin and protein hydrolysate in gastrointestinal resections due to cancer. Nutrition. 2013:1054–1059.
- Dock-Nascimento D. B., de Aguilar-Nascimento J. E., Faria M. S. M., Caporossi C., Slhessarenko N., Waitzberg D. L. Evaluation of the effects of a preoperative 2-hour fast with maltodextrine and glutamine on insulin resistance, acute-phase response, nitrogen balance, and serum glutathione after laparoscopic cholecystectomy a controlled randomized trial. J. Parent. Enteral Nutr. 2012:43–52.
- Sandhu B. K., Jones B., Brook C., Silk D. Oral rehydration in acute infantile diarrhoea with a glucose-polymer electrolyte solution. Arch. Disease Childhood. 1982:152–154.
- Marchal L. M. 1999Towards a rational design of commercial maltodextrins: a mechanistic approach Trends in Food Science & Technology 10
- Shi X., Summers R. W., Schedl H. P., Flanagan S. W., Chang R., Gisolfi C. V. Effects of carbohydrate type and concentration and solution osmolality on water absorption. Med. Sci. Sports Exer. 1995:1607.
- El-Mougi M., Hendawi A., Koura H., Hegazi E., Fontaine O., Pierce N. Efficacy of standard glucose-based and reduced-osmolarity maltodextrin-based oral rehydration solutions: effect of sugar malabsorption. Bull. World Health Org. 1996:471.
- Vist G. E., Maughan R. J. The effect of osmolality and carbohydrate content on the rate of gastric emptying of liquids in man. J. Physiol. 1995:523–531.
- Delzenne N., Blundell J., Brouns F., Cunningham K., De Graaf K., Erkner A., Lluch A., Mars M., Peters H., Westerterp-Plantenga M. Gastrointestinal targets of appetite regulation in humans. Obes. Rev. 2010:234–250.
- Shi X., Passe D. H. Water and solute absorption from carbohydrate-electrolyte solutions in the human proximal small intestine: a review and statistical analysis. Int. J. Sport Nutr. Exer. Metabol. 2010:427–442.
- Brouns F. Essentials of Sports Nutrition. West-Sussex, UK: Wiley; 2003.
- Harger-Domitrovich S. G., McClaughry A. E., Gaskill S. E., Ruby B. C. Exogenous carbohydrate spares muscle glycogen in men and women during 10 h of exercise. Med. Sci. Sports Exer. 2007:2171.
- Wallis G. A., Dawson R., Achten J., Webber J., Jeukendrup A. E. Metabolic response to carbohydrate ingestion during exercise in males and females. American J. Physiol.-Endocrinol. Metabol. 2006:E708–E715.
- Wallis G. A., Rowlands D. S., Shaw C., Jentjens R., Jeukendrup A. E. Oxidation of combined ingestion of maltodextrins and fructose during exercise. Med. Sci. Sports Exerc. 2005:426–432.
- Stevenson EJ, Watson A, Theis S, Holz A, Harper LD, Russell M. A comparison of isomaltulose versus maltodextrin ingestion during soccer-specific exercise. European Journal of Applied Physiology. 2017;117(11):2321-2333. doi:10.1007/s00421-017-3719-5 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5700989/
- The influence of pre-exercise glucose ingestion on endurance running capacity. Chryssanthopoulos C, Hennessy LC, Williams C. Br J Sports Med. 1994 Jun; 28(2):105-9. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1332041/pdf/brjsmed00014-0035.pdf
- Effects of pre-exercise ingestion of trehalose, galactose and glucose on subsequent metabolism and cycling performance. Jentjens RL, Jeukendrup AE. Eur J Appl Physiol. 2003 Jan; 88(4-5):459-65. https://www.ncbi.nlm.nih.gov/pubmed/12527978/
- Kerksick C., Harvey T., Stout J., Campbell B., Wilborn C., Kreider R., Kalman D., Ziegenfuss T., Lopez H., Landis10 J. International Society of Sports Nutrition position stand: Nutrient timing. J. Int. Soc. Sports Nutr. 2008:17.
- Nakhostin-Roohi B., Khorshidi M. The effect of glutamine and maltodextrin acute supplementation on anaerobic power. Asian J. Sports Med. 2013
- Coletta A., Thompson D. L., Raynor H. A. The influence of commercially-available carbohydrate and carbohydrate-protein supplements on endurance running performance in recreational athletes during a field trial. J. Int. Soc. Sports Nutr. 2013:17.
- Anderson C., Curzon M., Van Loveren C., Tatsi C., Duggal M. Sucrose and dental caries: a review of the evidence. Obes. Rev. 2009:41–54.
- Tahmassebi J. F., Duggal M. S., Malik-Kotru G., Curzon M. E. Soft drinks and dental health: a review of the current literature. J. Dent. 2006:2–11.
- Cheng R., Yang H., Shao M., Hu T., Zhou X. Dental erosion and severe tooth decay related to soft drinks: a case report and literature review. J. Zhejiang Univ. Sci. B. 2009:395–399.
- Al-Khatib G. R., Duggal M. S., Toumba K. J. An evaluation of the acidogenic potential of maltodextrins in vivo. J. Dent. 2001:409–414.
- Sajilata M., Singhal R. S. Specialty starches for snack foods. Carbohydr. Polym. 2005:131–151.
- Stubbs J., Ferres S., Horgan G. Energy density of foods: effects on energy intake. Crit. Rev. Food Sci. Nutr. 2000:481–515
- Junsi M., Usawakesmanee W., Siripongvutikorn S. Effect of using starch on off-odors retention in tuna dark meat. Int. Food Res. J. 2012:709–714.
- Klaauw A. A., Keogh J. M., Henning E., Trowse V. M., Dhillo W. S., Ghatei M. A., Farooqi I. S. High protein intake stimulates postprandial GLP1 and PYY release. Obesity21(8):1602–1607 2013
- Yeomans M. R., Gray R. W., Conyers T. H. B. Maltodextrin preloads reduce food intake without altering the appetiser effect. Physiol. Behav. 1998:501–506.
- Booth D. A. Learnt reduction in the size of a meal. Measurement of the sensory-gastric inhibition from conditioned satiety. Appetite. 2009:745–749.
- Allison D. B. Liquid calories, energy compensation and weight: what we know and what we still need to learn. Brit. J. Nutr. 2013 111(3):384–386.
- Prevalence of obesity and trends in body mass index among US children and adolescents, 1999-2010. Ogden CL, Carroll MD, Kit BK, Flegal KM. JAMA. 2012 Feb 1; 307(5):483-90. https://jamanetwork.com/journals/jama/fullarticle/1104932
- Parker K., Salas M., Nwosu V. C. High fructose corn syrup: Production, uses and public health concerns. Biotechnol. Mol. Biol. Rev. 2010:71–78.
- Whelan, W. J. ( 2004) The wars of the carbohydrates, Part 3: Maltose. IUBMB Life 56, 641. https://doi.org/10.1080/15216540400022458
- Maltodextrin can produce similar metabolic and cognitive effects to those of sucrose in the rat. Appetite Volume 77, 1 June 2014, Pages 1-12. https://doi.org/10.1016/j.appet.2014.02.011
- GRAS Notices. https://www.accessdata.fda.gov/scripts/fdcc/index.cfm?set=GRASNotices&id=610
- Effect of total enteral nutrition on the short-term outcome of severely malnourished cirrhotics. A randomized controlled trial. Cabre E, Gonzalez-Huix F, Abad-Lacruz A, Esteve M, Acero D, Fernandez-Bañares F, Xiol X, Gassull MA. Gastroenterology. 1990 Mar; 98(3):715-20.
- Caloric sweetener consumption and dyslipidemia among US adults. Welsh JA, Sharma A, Abramson JL, Vaccarino V, Gillespie C, Vos MB. JAMA. 2010 Apr 21; 303(15):1490-7 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3045262/
- Hofman DL, van Buul VJ, Brouns FJPH. Nutrition, Health, and Regulatory Aspects of Digestible Maltodextrins. Critical Reviews in Food Science and Nutrition. 2016;56(12):2091-2100. doi:10.1080/10408398.2014.940415. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4940893/
- Fructose-induced hyperuricemia is associated with a decreased renal uric acid excretion in humans. Lecoultre V, Egli L, Theytaz F, Despland C, Schneiter P, Tappy L. Diabetes Care. 2013 Sep; 36(9):e149-50. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3747900/
- Public health: The toxic truth about sugar. Lustig RH, Schmidt LA, Brindis CD. Nature. 2012 Feb 1; 482(7383):27-9. https://www.ncbi.nlm.nih.gov/pubmed/22297952/