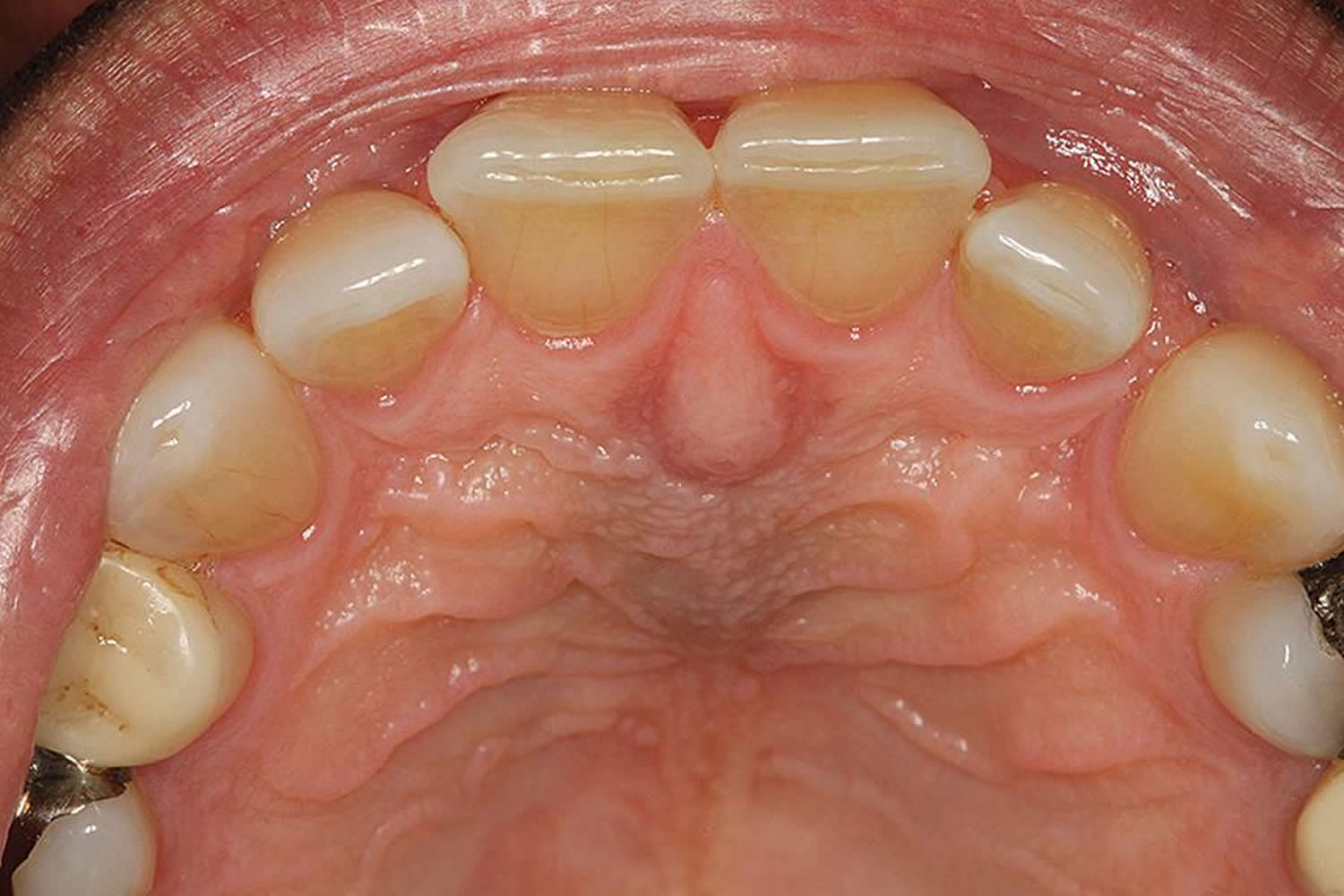
What is nasopalatine duct cyst
Nasopalatine duct cyst is a common developmental, epithelial, benign (concancerous) cysts that are considered to be the most common (32.8-73.2%) of the nonodontogenic cysts 1. Nasopalatine duct cysts usually present as unilateral pathology, but they may also occur bilaterally approximately 0.25% of all cases 2. Nasopalatine duct cyst is one of many pathologic processes that may occur within the jawbones, but it is unique in that it develops in only a single location, which is the midline anterior maxilla 3.
Nasopalatine duct cyst originates from epithelial remnants from the nasopalatine duct 3. The cells may be activated spontaneously during life or are eventually stimulated by the irritating action of various agents (infection, etc.). Nasopalatine duct cyst is different from a radicular cyst.
A reported 71.8% of nasopalatine duct cysts have squamous, columnar, cuboidal, or some combination of these epithelial types; respiratory epithelium is seen in only 9.8% 4.
Nasopalatine duct cysts affect a wide age range; however, most present in the fourth through sixth decades of life, and most studies show a significantly higher frequency in men than woman, with the ratio being 2.5 : 1 5. Patients may be asymptomatic, with the lesion being detected on routine radiographs; however, many will present with one or more symptoms. Complaints are often found to be associated with an infection of a previously asymptomatic nasopalatine duct cysts and consist primarily of swelling, drainage, and pain 6. The vitality of nearby teeth should not be affected; however, it is not uncommon to see evidence of endodontic therapy because the nasopalatine duct cyst was previously clinically misdiagnosed as a periapical cyst or granuloma.
Data concerning the prevalence of nasopalatine duct cysts differ considerably, with rates of 0.08% 7 to 33% 8 having been reported. Nasopalatine duct cysts account for approximately 12% of all jaw cyst tumors 9. They occur in both black and white populations 10. During last 50 years in the English-language literature, fewer than 500 cases have been published 11.
No racial predilection is known. Nasopalatine duct cysts that occur in young Afro-Caribbeans appears to be more clinically aggressive than those that occur in other ethnic groups 12.
The definite diagnosis should be based on clinical, radiological, and histopathological findings. The treatment is enucleation of the cystic tissue, and only in rare cases a marsupialisation needs to be performed 3
Nasopalatine duct cyst cause
The cause of nasopalatine duct cyst is unknown 13 or reactive 14. It has been postulated that localized trauma such as previous endodontic treatment, implant placement or infection or mucous retention may initiate the cellular proliferation and may give rise to nasopalatine duct cyst 14. It has also been reported to present in association with impacted mesiodens 15. It is not been associated with any habits such as smoking or alcoholism 16.
Nasopalatine duct cyst arises from the epithelial lining of nasopalatine duct or from the vomer nasal organ of Jacobson or mucous glands present in the nasal mucosa 17. Histologically, the nasopalatine duct exhibits different epithelial cells in different region. The epithelium close to the nasal floor has ciliated columnar epithelium, and the one closer to the oral cavity has squamous epithelium and the one in the middle has cuboidal epithelium. It has also been reported containing nerve fibers and melanin or lipofuscin pigments 18. Hence, the nasopalatine cyst also exhibits the mixed nature of the epithelial lining.
Nasopalatine duct cyst symptoms
Small nasopalatine duct cysts in the early stages of their development are frequently (40-87%) asymptomatic and are likely to be recognized on routine radiographic examinations during dental treatment 19.
Large nasopalatine duct cysts can be responsible for a variety of symptoms, including swelling in the anterior part of the midline of the palate (52-88%), discharge (25%), pain defined as a burning sensation in the anterior part of the maxilla that occasionally radiates into the bridge of the nose, and in a person who wears a dental prothesis, a pressure sensation underneath the prosthesis (20-23%); secondly, tooth movement can occur. The pain also can be caused by super infection. About 70% of patients experience a combination of these symptoms. Sometimes, fistula formation or an inability to wear dentures is observed 11.
Paradoxically, patients with small cysts may have disproportionately severe symptoms, whereas patients with large ones may experience few or no symptoms. In all cases in which there is an expansion of the cyst into nasal cavity, symptoms are more severe 20.
A salty taste in the mouth and devitalization of the pulps of associated teeth have been reported 21.
Large and more destructive nasopalatine duct cysts that have perforated the labial and palatal bony plates may present as expansile, fluctuant swellings of the anterior palate and the palate.
Extrabony cysts that develop within the soft tissues of the incisive papilla area of the anterior hard palate (called the cyst of the incisive papilla) may present as a translucent or bluish colored, dome-shaped swelling. The clinically apparent discoloration is due to the accumulation of fluid contents within the cyst.
Nasopalatine duct cysts clinically demonstrate slow and progressive growth, sometimes exceeding 60 mm in diameter.
Tooth displacement is a common finding, having been reported to occur in 78% of patients 22, whereas bony expansion is noted in only 1.4% of patients 23. The literature describes an untreated case that caused destruction of bone and mucosa and movement of teeth, with ensuing disability 24.
Usually, the anterior teeth react positively to pulp sensitivity testing. In some cases when the electric pulp test is negative or when endodontic treatment has already been performed in the incisor region, the correct diagnosis is more difficult 25.
Nasopalatine duct cyst complications
Very large, untreated nasopalatine duct cysts may resorb the roots of the adjacent teeth and display the roots. Other complications may include perforation of the vestibular bone, nasal cavity, and maxillary sinus 26 ; a large cyst can cause complete destruction of the anterior palate and pyriform rim 27. Paresthesia to the anterior palate may occur in 10% of cases if components of the long sphenopalatine nerve are removed or damaged during surgery 11. In addition, devitalization of central incisors, postoperative wound infection, and postoperative fistula can occur 20. There is a statistically significant correlation between the presence of postoperative and late complications with cyst diameter, surface area, and volume.
Nasopalatine duct cyst diagnosis
Imaging Studies
Panoramic, occlusal, and periapical radiographs are standard in the radiographic evaluation of suspected nasopalatine duct cyst. A radiological examination in a minimum of 2 projections (periapical and occlusal) should be performed 11. In some cases, obtaining a 3-dimensional view of the lesion may be necessary.
CT scanning
Harris and Brown 28 advocate a second periapical radiograph taken perpendicular to the first, a CT scan (shows imaging information as direct axial or coronal slices or as reformatted coronal or sagittal slices), and linear tomography through the area of interest in an alternative plane.
In 2000, Pevsner et al 29 reported CT scan characteristics believed to be unique to nasopalatine duct cysts. These include (1) a midline position of the lesion; (2) pressure erosion of the tooth apices and exclusion of contiguous tooth numbers 8 and 9 rather than incorporation of the apices of these teeth within the cyst; and (3) smooth, noninflammatory bony expansion of the lesion with sclerotic margins. The expansile change of the posterior midline maxilla and smooth elevation of the nasal cavity with tilting of the nasal septum suggest a long-term process that is likely developmental and consistent with a nasopalatine duct cyst.
In 2011 Suter et al 20 applied cone-beam CT scanning to describe nasopalatine duct cysts.
MRI
MRIs of nasopalatine duct cysts show homogeneous high-signal intensity on T2-weighted images and intermediate signal intensity on T1-weighted images in the area of the contents of nasopalatine duct cysts (keratin and viscous fluids). MRI is more specific than CT 30.
Radiography
Radiographic examination typically discloses a well-defined, ovoid, round or inverted, pear-shaped radiolucency located in the midline of the maxilla, which is inter-radicular and apical to the roots of the maxillary central incisor teeth; larger lesions resorb the surrounding maxillary cortex 30.
Radiography
The mean radiographic diameter is reported to be 17.1 mm 21. The mean cyst surface area reportedly is 566 mm2 (84-4,516 mm2), and the mean cyst volume is reported to be 1,735 mm3 (65-25,350 mm3) 31.
Superimposition of the nasal spine can impart a heart-shaped appearance to the cyst.
Peripheral sclerosis, an indication of a slowly developing growth and intrabony expansion, may or may not be present. The roots of the central incisors may show divergence.
Destruction of the floor of the maxillary antrum has been described 32.
In some individuals, a prominent incisive canal can appear as a radiolucent area and mimic nasopalatine duct cyst.
Most authors agree that 6 mm should be considered the upper limit for a normal incisive canal. Radiolucencies larger than this should be considered potentially pathologic and merit further investigation 33.
Procedures
Aspiration of pathologic jaw radiolucencies can provide useful information in distinguishing solid processes from cystic processes but is not itself diagnostic of an entity. A clear or straw-colored fluid aspirate is suggestive of nasopalatine duct cyst; however, other cystic processes (eg, lateral radicular cyst, cystic ameloblastoma) cannot be excluded on the basis of this finding alone. Bloody fluid is more indicative of a central hemangioma, a central giant cell lesion, an arteriovenous malformation, or an aneurysmal bone cyst. Negative aspiration indicates a solid process (eg, odontogenic myxoma, solid ameloblastoma).
Tooth vitality testing may be necessary. In the absence of caries, traumatic injury, or other obvious cause of pulpal necrosis, the adjacent maxillary central incisor teeth should be vitality tested to exclude the possibility of a pulpal-periapical inflammatory pathogenesis (eg, lateral radicular cyst, dental granuloma, periapical cyst, periapical abscess).
Nasopalatine duct cyst treatment
Nasopalatine duct cysts are treated by enucleation via a palatine or buccal approach; transnasal endoscopic marsupialization can also be applied 34.
Recurrence is uncommon, having been reported in 0-11% of patients 21.
If components of the long sphenopalatine nerve are removed during surgery, it may cause paresthesia to the anterior palate 35.
Complete bone regeneration within the bony defect is expected postoperatively.
In some cases, a marsupialization is necessary, such as when the capsule shows adhesion with the surrounding area and enucleation is difficult to perform.
Nasopalatine duct cyst prognosis
Complete postsurgical bony regeneration is expected in most patients. After surgical treatment, recurrence is uncommon, having been reported in 0-11% of patients 36. Only two cases of malignant change in the lining epithelium of a nasopalatine duct cyst have been published 37.
References- Nonaka CFW, Henriques ACG, de Matos FR, de Souza LB, Pinto LP. Nonodontogenic cysts of the oral and maxillofacial region: demographic profile in Brazilian population over a 40-year period. Eur Arch Otorhinolaryngol. 2011. 268:917-922.
- Cicciù M, Grossi GB, Borgonovo A, Santoro G, Pallotti F, Maiorana C. Rare bilateral nasopalatine duct cysts: a case report. Open Dent J. 2010. 4:8-12.
- Dedhia P, Dedhia S, Dhokar A, Desai A. Nasopalatine duct cyst. Case Rep Dent. 2013;2013:869516. doi:10.1155/2013/869516 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3834977
- Vasconcelos R, de Aguiar MF, Castro W, de Araujo VC, Mesquita R. Retrospective analysis of 31 cases of nasopalatine duct cyst. Oral Diseases. 1999;5(4):325–328.
- Shear M, Speight PM. Cysts of the Oral and Maxillofacial Regions. 4th edition. Oxford, UK: Blackwell Munksgaard; 2007
- Swanson KS, Kaugars GE, Gunsolley JC. Nasopalatine duct cyst: an analysis of 334 cases. Journal of Oral and Maxillofacial Surgery. 1991;49(3):268–271
- Killey HC, Kay LW. Benign Cystic Lesions of the Jaws, Their Diagnosis and Treatment. 2nd ed. New York, NY: Churchill Livingstone; 1977.
- Burket LW. Nasopalatine duct structures and peculiar bony pattern observed in the anterior maxillary region. Arch Path. 1937. 23:793-800.
- Righini CA, Bettega G, Boubagra K, Reyt E. Nasopalatine duct cyst (NPDc): one case report. Acta Otorhinolaryngol Belg. 2004. 58(2):129-33.
- Elliott KA, Franzese CB, Pitman KT. Diagnosis and surgical management of nasopalatine duct cysts. Laryngoscope. 2004 Aug. 114(8):1336-40.
- Szubert P, Sokalski J, Krauze A, Kondziela I, Splawa-Neyman A. Nasopalatine duct cyst – case reports. Dent Med Probl. 2010. 47(4):508-12.
- Nortje CJ, Farman AG. Nasopalatine duct cyst. An aggressive condition in adolescent Negroes from South Africa?. Int J Oral Surg. 1978 Apr. 7(2):65-72.
- Escoda Francoli J, Almendros Marques N, Berini Aytes L, Gay Escoda C. Nasopalatine duct cyst: report of 22 cases and review of the literature. Med Oral Patol Oral Cir Bucal. 2008 Jul 1. 13(7):E438-43
- Sankar D, Muthusubramanian V, Nathan JA, Nutalapati RS, Jose YM, Kumar YN. Aggressive nasopalatine duct cyst with complete destruction of palatine bone. J Pharm Bioallied Sci. 2016;8(Suppl 1):S185–S188. doi:10.4103/0975-7406.191956 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5074029
- Gopal D, Telang A, Telang LA, Loganathan K, Reddy BT. Nasopalatine duct cyst associated with a mesiodens: Misdiagnosis or missed diagnosis? J Clin Diagn Res. 2015;9:ZD21–2.
- Escoda Francolí J, Almendros Marqués N, Berini Aytés L, Gay Escoda C. Nasopalatine duct cyst: Report of 22 cases and review of the literature. Med Oral Patol Oral Cir Bucal. 2008;13:E438–43.
- Shear M, Speight P. Cysts of the Oral and Maxillofacial Regions. 4th ed. Oxford: Blackwell Publishing Ltd; 2007. pp. 108–18.
- Cecchetti F, Ottria L, Bartuli F, Bramanti NE, Arcuri C. Prevalence, distribution, and differential diagnosis of nasopalatine duct cysts. Oral Implantol (Rome) 2012;5:47–53.
- Francoli JE, Marques NA, Aytes LB, Escoda CG. Nasopalatine duct cyst: Report of 22 cases and review of the literature. Med Oral Patol Oral Cir Bucal. 2008. 13:e438-43.
- Suter VG, Sendi P, Reichart PA, Bornstein MM. The nasopalatine duct cyst: an analysis of the relation between clinical symptoms, cyst dimensions, and involvement of neighboring anatomical structures using cone beam computed tomography. J Oral Maxillofac Surg. 2011 Oct. 69(10):2595-603.
- Gnanasekhar JD, Walvekar SV, al-Kandari AM, al-Duwairi Y. Misdiagnosis and mismanagement of a nasopalatine duct cyst and its corrective therapy. A case report. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 1995 Oct. 80(4):465-70.
- Anneroth G, Hall G, Stuge U. Nasopalatine duct cyst. Int J Oral Maxillofac Surg. 1986 Oct. 15(5):572-80.
- Swanson KS, Kaugars GE, Gunsolley JC. Nasopalatine duct cyst: an analysis of 334 cases. J Oral Maxillofac Surg. 1991 Mar. 49(3):268-71
- Perumal CJ. An unusually large destructive nasopalatine duct cyst: a case report. J Maxillofac Oral Surg. 2013 Mar. 12(1):100-4.
- Suter VG, Büttner M, Altermatt HJ, Reichart PA, Bornstein MM. Expansive nasopalatine duct cysts with nasal involvement mimicking apical lesions of endodontic origin: a report of two cases. J Endod. 2011 Sep. 37(9):1320-6.
- Scolozzi P, Martinez A, Richter M, Lombardi T. A nasopalatine duct cyst in a 7-year-old child. Pediatr Dent. 2008 Nov-Dec. 30(6):530-4.
- Sankar D, Muthusubramanian V, Nathan JA, Nutalapati RS, Jose YM, Kumar YN. Aggressive nasopalatine duct cyst with complete destruction of palatine bone. J Pharm Bioallied Sci. 2016 Oct. 8 (Suppl 1):S185-S188.
- Harris IR, Brown JE. Application of cross-sectional imaging in the differential diagnosis of apical radiolucency. Int Endod J. 1997 Jul. 30(4):288-90.
- Pevsner PH, Bast WG, Lumerman H, Pivawer G. CT analysis of a complicated nasopalatine duct cyst. N Y State Dent J. 2000 Jun-Jul. 66(6):18-20.
- Tanaka S, Iida S, Murakami S, Kishino M, Yamada C, Okura M. Extensive nasopalatine duct cyst causing nasolabial protrusion. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2008 Oct. 106(4):e46-50.
- Suter VG, Warnakulasuriya S, Reichart PA, Bornstein MM. Radiographic volume analysis as a novel tool to determine nasopalatine duct cyst dimensions and its association with presenting symptoms and postoperative complications. Clin Oral Investig. 2015 Sep. 19 (7):1611-8.
- Hertzanu Y, Cohen M, Mendelsohn DB. Nasopalatine duct cyst. Clin Radiol. 1985 Mar. 36(2):153-8.
- Swanson KS, Kaugars GE, Gunsolley JC. Nasopalatine duct cyst: an analysis of 334 cases. J Oral Maxillofac Surg. 1991 Mar. 49(3):268-71.
- Honkura Y, Nomura K, Oshima H, Takata Y, Hidaka H, Katori Y. Bilateral endoscopic endonasal marsupialization of nasopalatine duct cyst. Clin Pract. 2015 Jan 28. 5 (1):748.
- Bodin I, Isacsson G, Julin P. Cysts of the nasopalatine duct. Int J Oral Maxillofac Surg. 1986 Dec. 15(6):696-706.
- Nelson BL, Linfesty RL. Nasopalatine duct cyst. Head Neck Pathol. 2010. 4:121-122.
- Takagi R, Ohashi Y, Suzuki M. Squamous cell carcinoma in the maxilla probably originating from a nasopalatine duct cyst: report of case. J Oral Maxillofac Surg. 1996 Jan. 54(1):112-5