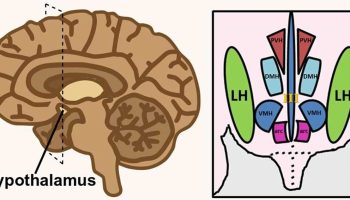
What is perimenopause
The gradual transition between the reproductive years and menopause (the cessation of menstrual periods) is called perimenopause (literally meaning “around menopause”) 1. Perimenopause is also called the menopausal transition. Perimenopause is generally a transition that is many years long and can be associated with shorter menstrual intervals, irregular menses, night sweats, and other symptoms. In some women, these symptoms are troublesome enough to need medical intervention.
Women start perimenopause at different ages. You may notice signs of progression toward menopause, such as menstrual irregularity, sometime in your 40s. But some women notice changes as early as their mid-30s 2.
- However, the perimenopause transition phase most often begins between ages 45 and 55 and may last for 4 to 8 years (usually lasts about 7 years), but can last as long as 14 years.
- Perimenopause begins with changes in the length of time between periods and ends 1 year after the final menstrual period.
The level of estrogen — the main female hormone — in your body rises and falls unevenly during perimenopause. Your menstrual cycles may lengthen or shorten, and you may begin having menstrual cycles in which your ovaries don’t release an egg (ovulate). You may also experience menopause-like symptoms, such as hot flashes, sleep problems and vaginal dryness. Treatments are available to help ease these symptoms.
Once you’ve gone through 12 consecutive months without a menstrual period, you’ve officially reached menopause, and the perimenopause period is over.
Perimenopause symptoms
The signs and symptoms that many women experience during perimenopause are caused by gradually decreasing levels of estrogen. You may have only a few symptoms, or you may have many. Symptoms may be mild, or they may be severe.
Throughout the perimenopause (menopausal transition), some subtle — and some not-so-subtle — changes in your body may take place.
Each woman’s perimenopause experience is different. Many women who undergo natural menopause report no physical changes at all during the perimenopausal years except irregular menstrual periods that eventually stop when they reach menopause. Other changes may include hot flashes, difficulty sleeping, memory problems, mood disturbances, vaginal dryness, and weight gain. Not all these changes are hormone-related, and some, such as hot flashes and memory problems, tend to resolve after menopause. Maintaining a healthy lifestyle during this time of transition is essential for your health and can even prevent or blunt some of these changes.
You might experience 2:
Changes in Your Menstrual Cycle
A common sign of perimenopause is a change in your menstrual cycle. Cycles may become longer than usual for you, or they may become shorter. You may begin to skip periods. The amount of flow may become lighter or heavier. Although changes in menstrual bleeding are normal as you approach menopause, you still should report them to your health care provider.
- Irregular periods. As ovulation becomes more unpredictable, the length of time between periods may be longer or shorter, your flow may be light to heavy, and you may skip some periods. If you have a persistent change of seven days or more in the length of your menstrual cycle, you may be in early perimenopause. If you have a space of 60 days or more between periods, you’re likely in late perimenopause.
Abnormal bleeding may be a sign of a problem. Talk to your health care provider if you have any of the following:
- Bleeding between periods
- Bleeding after sex
- Spotting at anytime in the menstrual cycle
- Bleeding that is heavier or lasts for more days than usual
- Any bleeding after menopause
Although the removal of the uterus (a hysterectomy) ends menstrual periods, it does not cause menopause unless the ovaries also are removed. This type of surgery is called an oophorectomy. An oophorectomy causes immediate menopause signs and symptoms if it is done before a woman reaches menopause.
Hot Flashes
Hot flashes are one of the most common symptoms of perimenopause.
- A hot flash is a sudden feeling of heat that spreads over the face and body. The skin may redden like a blush. You also may break out in a sweat. A hot flash may last from a few seconds to several minutes or longer. Hot flashes are not harmful, but they sometimes are embarrassing and may interfere with daily life. Some women have hot flashes a few times a month. Others have them several times a day. Hot flashes that happen at night (night sweats) may wake you up and cause you to feel tired and sluggish during the day. The intensity, length and frequency vary. Although their exact cause still isn’t fully understood, hot flashes are thought to be the result of changes in the hypothalamus, the part of the brain that regulates the body’s temperature. If the hypothalamus mistakenly senses that a woman is too warm, it starts a chain of events to cool her down. Blood vessels near the surface of the skin begin to dilate (enlarge), increasing blood flow to the surface in an attempt to dissipate body heat. This produces a red, flushed look to the face and neck in light-skinned women. It may also make a woman perspire to cool the body down. The heart may beat faster, and women may sense that rapid heartbeat. A cold chill often follows a hot flash. A few women experience only the chill.
- Most women experience hot flashes for 6 months to 2 years, although some reports suggest that they last considerably longer—as long as 10 years, depending on when they began. For a small proportion of women, they may never go away. It is not uncommon for women to experience a recurrence of hot flashes more than 10 years after menopause, even into their 70s or beyond. There is no reliable way of predicting when they will start—or stop.
Sleep problems
- Sleep problems are often due to hot flashes or night sweats, but sometimes sleep becomes unpredictable even without them. However, there are many reasons for sleep disturbances besides menopausal night sweats (simply, hot flashes at night). Your sleep disturbances may be caused by factors that affect many women beginning at midlife, such as sleep-disordered breathing (known as sleep apnea), restless legs syndrome, stress, anxiety, depression, painful chronic illnesses, and even some medications. Any treatment should first focus on improving your sleep routine—use regular hours to sleep each night, avoid getting too warm while sleeping, avoid stimulants such as caffeine and dark chocolate. When lifestyle changes fail to alleviate sleep disturbances, your clinician may want to refer you to a sleep center to rule out sleep-related disorders before initiating prescription treatment. If your sleep disturbance is related solely to hot flashes, hormone therapy is likely to help.
Mood changes
- Mood changes. Mood swings, irritability or increased risk of depression may happen during perimenopause. The cause of these symptoms may be sleep disruption associated with hot flashes. Mood changes may also be caused by factors not related to the hormonal changes of perimenopause. Most women make the transition into menopause without experiencing depression, but many women report symptoms of moodiness, depressed mood, anxiety, stress, and a decreased sense of well-being during perimenopause. Women with a history of clinical depression or a history of premenstrual syndrome (PMS) or postpartum depression seem to be particularly vulnerable to recurrent depression during perimenopause, as are women who report significant stress, sexual dysfunction, physical inactivity, or hot flashes. The idea of growing older may be difficult or depressing for some women. Sometimes menopause just comes at a bad time in a woman’s life. She may have other challenges to deal with at midlife, and menopause gives her one more problem on her list. It has been suggested that mood symptoms may be related to erratic fluctuations in estrogen levels, but limited data exist on why this occurs. Antidepressants are the primary pharmacologic treatment for menopause-associated depression. Menopause hormone therapy and hormone contraceptives can be used as off-label therapies, especially in women with concurrent hot flashes. The wide range of psychological symptoms reported during the menopause transition, from irritability and blue moods to the recurrence of major depression, can be identified and often treated by a woman’s primary care provider or a menopause practitioner.
Vaginal and Urinary Tract Changes
As estrogen levels decrease, changes take place in the vagina. Over time, the vaginal lining gets thinner, dryer, and less elastic. Vaginal dryness may cause pain during sexual intercourse. Vaginal infections also may occur more often.
The urinary tract also changes with age. The urethra can become dry, inflamed, or irritated. Some women may need to urinate more often. Women may have an increased risk of urinary tract infections after menopause.
- Vaginal and bladder problems. When estrogen levels diminish, your vaginal tissues may lose lubrication and elasticity, making intercourse painful. Low estrogen may also leave you more vulnerable to urinary or vaginal infections. Loss of tissue tone may contribute to urinary incontinence.
Decreasing fertility
- As ovulation becomes irregular, your ability to conceive decreases. However, as long as you’re having periods, pregnancy is still possible. If you wish to avoid pregnancy, use birth control until you’ve had no periods for 12 months.
Changes in sexual function
- During perimenopause, sexual arousal and desire may change. But if you had satisfactory sexual intimacy before menopause, this will likely continue through perimenopause and beyond.
- Sexual desire decreases with age in both sexes, and low desire is common in women in their 40s and 50s, but not universal. Some women have increased interest, while others notice no change at all. There is no major drop in testosterone at menopause. If lack of interest is related to discomfort with intercourse, estrogen may help. What’s important to remember is that there is a full range of psychological, cultural, personal, interpersonal and biological factors that can contribute to declining sexual interest, so if the decline in desire is bothering you, tell your healthcare provider. A clinical evaluation can identify any underlying medical or psychological causes of low sexual desire, which then can be treated as appropriate.
Bone Changes and Osteoporosis
Bones are constantly changing throughout life. Old bone is removed in a process called resorption. New bone is built in a process called formation. During the teen years, bone is formed faster than it is broken down. The amount of bone in the body (sometimes called the “bone mass”) reaches its peak during the late teen years. In midlife, the process begins to reverse: Bone is broken down faster than it is made. A small amount of bone loss after age 35 years is normal for men and women. But during the first 4–8 years after menopause, women lose bone more rapidly. This rapid loss occurs because of the decreased levels of estrogen. If too much bone is lost, it can increase your risk of osteoporosis (a disease that causes fragile bones). Osteoporosis increases the risk of bone fracture. The bones of the hip, wrist, and spine are affected most often.
Changing cholesterol levels
- Declining estrogen levels may lead to unfavorable changes in your blood cholesterol levels, including an increase in low-density lipoprotein (LDL) cholesterol — the “bad” cholesterol — which contributes to an increased risk of heart disease. At the same time, high-density lipoprotein (HDL) cholesterol — the “good” cholesterol — decreases in many women as they age, which also increases the risk of heart disease.
Headaches
- Studies suggest that hormones may play a role in headaches. Women at increased risk for hormonal headaches during perimenopause are those who have already had headaches influenced by hormones, such as those with a history of headaches around their menstrual periods (so-called menstrual migraines) or when taking oral contraceptives. Hormonal headaches typically stop when menopause is reached and hormone levels are consistently low. Most headaches do not require treatment or can be treated with nonprescription pain medications. Some headaches, however, can be serious. More serious headaches, including migraines, may require prescription drugs; however, care should be taken to monitor the use of these drugs. If a headache is unusually painful or different from those you have had before, seek medical help promptly.
Memory changes
- Your memory and other cognitive abilities change throughout life. Difficulty concentrating and remembering are common complaints during perimenopause and the years right after menopause. Some data imply that even though there is a trend for memory to be worse during the menopause transition, memory after the transition is as good as it was before. Memory problems may be more related to normal cognitive aging, mood, and other factors than to menopause or the menopause transition. Maintaining an extensive social network, remaining physically and mentally active, consuming a healthy diet, not smoking, and consuming alcohol in moderation may all help prevent memory loss. Atherosclerosis (hardening of the arteries) may also contribute to mental decline. Aim for normal cholesterol, normal weight, and normal blood pressure to help protect your brain. Women who are concerned about declining cognitive performance are advised to consult with their healthcare providers.
When to see a doctor
Some women seek medical attention for their perimenopausal symptoms. But others either tolerate the changes or simply don’t experience symptoms severe enough to need attention. Because symptoms may be subtle and come on gradually, you may not realize at first that they’re all connected to the same thing — rising and falling levels of estrogen and progesterone, another key female hormone.
If you have symptoms that interfere with your life or well-being, such as hot flashes, mood swings or changes in sexual function that concern you, see your doctor.
Causes of perimenopause
As you go through perimenopause, your body’s production of estrogen and progesterone rises and falls. Many of the changes you experience during perimenopause are a result of decreasing estrogen.
Risk factors of perimenopause
Menopause is a normal phase in life. But it may occur earlier in some women than in others. Although not always conclusive, some evidence suggests that certain factors may make it more likely that you start perimenopause at an earlier age, including:
- Smoking. The onset of menopause occurs one to two years earlier in women who smoke than in women who don’t smoke.
- Family history. Women with a family history of early menopause may experience early menopause themselves.
- Cancer treatment. Treatment for cancer with chemotherapy or pelvic radiation therapy has been linked to early menopause.
- Hysterectomy. A hysterectomy that removes your uterus, but not your ovaries, usually doesn’t cause menopause. Although you no longer have periods, your ovaries still produce estrogen. But such surgery may cause menopause to occur earlier than average. Also, if you have one ovary removed, the remaining ovary might stop working sooner than expected.
Complications of perimenopause
Irregular periods are a hallmark of perimenopause. Most of the time this is normal and nothing to be concerned about. However, see your doctor if:
- Bleeding is extremely heavy — you’re changing tampons or pads every hour or two for two or more hours
- Bleeding lasts longer than seven days
- Bleeding occurs between periods
- Periods regularly occur less than 21 days apart
Signs such as these may mean there’s a problem with your reproductive system that requires diagnosis and treatment.
Diagnosis of Perimenopause
Perimenopause is a process — a gradual transition. No one test or sign is enough to determine if you’ve entered perimenopause. Your doctor takes many things into consideration, including your age, menstrual history, and what symptoms or body changes you’re experiencing.
Some doctors may order tests to check your hormone levels. But other than checking thyroid function, which can affect hormone levels, hormone testing is rarely necessary or useful to evaluate perimenopause.
Treatment of Perimenopause
Drug therapy is often used to treat perimenopausal symptoms.
- Hormone therapy. Systemic estrogen therapy — which comes in pill, skin patch, gel or cream form — remains the most effective treatment option for relieving perimenopausal and menopausal hot flashes and night sweats. Depending on your personal and family medical history, your doctor may recommend estrogen in the lowest dose needed to provide symptom relief for you. If you still have your uterus, you’ll need progestin in addition to estrogen. Systemic estrogen can help prevent bone loss.
- Vaginal estrogen. To relieve vaginal dryness, estrogen can be administered directly to the vagina using a vaginal tablet, ring or cream. This treatment releases just a small amount of estrogen, which is absorbed by the vaginal tissue. It can help relieve vaginal dryness, discomfort with intercourse and some urinary symptoms.
- Antidepressants. Certain antidepressants related to the class of drugs called selective serotonin reuptake inhibitors (SSRIs) may reduce menopausal hot flashes. An antidepressant for management of hot flashes may be useful for women who can’t take estrogen for health reasons or for women who need an antidepressant for a mood disorder.
- Gabapentin (Neurontin). Gabapentin is approved to treat seizures, but it has also been shown to help reduce hot flashes. This drug is useful in women who can’t use estrogen therapy for health reasons and in those who also have migraines.
Before deciding on any form of treatment, talk with your doctor about your options and the risks and benefits involved with each. Review your options yearly, as your needs and treatment options may change.
What are the treatments for hot flashes ?
Although the available treatments for hot flashes do not cure hot flashes, they do offer relief. Hot flashes usually fade away eventually without treatment, and no treatment is necessary unless hot flashes are bothersome. A few women have an occasional hot flash forever. There are a number of low-risk coping strategies and lifestyle changes that may be helpful for managing hot flashes, but if hot flashes remain very disruptive, prescription therapy may be considered. Prescription hormone therapy approved by the US Food and Drug Administration (FDA) and by Health Canada include systemic estrogen therapy and estrogen-progestogen therapy (for women with a uterus)—are the standard treatment. Another FDA-approved hormone product, for women with a uterus, combines estrogen with bazedoxifene instead of a progestogen. Bazedoxifene is an estrogen agonist/antagonist, which means that it works like estrogen in some tissues while inhibiting estrogen activity in others. In this case, it helps to protect the uterus from cancer.
For women who prefer not to take hormones or cannot hormones, nonhormone drugs approved to treat depression, called selective serotonin-reuptake inhibitors (SSRIs), have been found to be effective in treating hot flashes in women who don’t have depression. The only SSRI FDA has approved thus far for treating hot flashes is paroxetine 7.5 mg.
Perimenopause birth control: What are your options ?
If you don’t intend to have any children in the future, one option is permanent sterilization for either you or your partner. Otherwise, if you’re generally in good health, and you don’t have any medical conditions that might preclude their use, hormonal forms of birth control may be an option, too.
For a woman during perimenopause, birth control options include:
- A combination estrogen-progestin pill or ring, if you don’t have a medical reason not to take contraceptive-strength doses of estrogen.
- A progestin-only contraceptive, such as the levonorgestrel intrauterine system (Mirena, Skyla), the etonogestrel subdermal implant (Nexplanon), or the progestin-only minipill, which also provide protection from cancer of the endometrium — the tissue that lines your uterus.
- An estrogen-progestin skin patch, if you’re not at risk of blood clots or other bleeding disorder. However, caution is needed when using this form of birth control. A patch that contains both estrogen and progestin, such as the skin path containing norelgestromin and ethinyl estradiol (Ortho Evra), increases blood clot risk compared with other forms of estrogen-progestin contraception, such as a pill or vaginal ring.
- A sterilization procedure, such as vasectomy or tubal ligation, which provides a permanent form of birth control.
Whichever method you choose, doctors generally recommend that you continue birth control during perimenopause and for about 12 months after your menstrual periods naturally stop.
Lifestyle and home remedies for perimenopause
Making these healthy lifestyle choices may help ease some symptoms of perimenopause and promote good health as you age:
- Ease vaginal discomfort. Use over-the-counter, water-based vaginal lubricants (Astroglide, K-Y jelly, others) or moisturizers (Replens, Vagisil, others). Choose products that don’t contain glycerin, which can cause burning or irritation in women who are sensitive to that chemical. Staying sexually active also helps by increasing blood flow to the vagina. DO NOT use petroleum jelly. DO NOT use mineral oils or other oils if you use condoms, as these may damage latex condoms or diaphragms.
- Eat healthy. Because your risk of osteoporosis and heart disease increases at this time, a healthy diet is more important than ever. Adopt a low-fat, high-fiber diet that’s rich in fruits, vegetables and whole grains. Add calcium-rich foods. Ask your doctor if you should also take a calcium supplement and if so, what type and how much — also ask if you need more vitamin D, which helps your body absorb calcium. Avoid alcohol and caffeine if they seem to trigger hot flashes.
- Be active. Regular exercise and physical activity helps prevent weight gain, improves your sleep and elevates your mood. Try to exercise for 30 minutes or more on most days of the week, although not right before bedtime. Regular exercise has been shown to reduce hip fracture risk in older women and to strengthen bone density.
- Get enough sleep. Try to keep a consistent sleep schedule. Avoid caffeine, which can make it hard to get to sleep, and avoid drinking too much alcohol, which can interrupt sleep.
- Practice stress reduction techniques. Practiced regularly, stress-reduction techniques, such as meditation or yoga, can promote relaxation and good health throughout your lifetime, but they may be particularly helpful during the menopausal transition.
To help control hot flashes:
- Dress lightly and in layers. Try to keep your environment cool.
- Practice slow, deep breathing whenever a hot flash starts to come on. Try taking six breaths per minute.
- Try relaxation techniques such as yoga, tai chi, or meditation.
Watching what you eat or drink can improve your symptoms and help you sleep:
- Eat at regular times each day. Eat a healthy diet that is low in fat and includes lots of fruits and vegetables.
- Milk and other dairy products contain tryptophan, which may help induce sleep.
- If you can, avoid coffee, colas with caffeine, and energy drinks completely. If you cannot avoid them, try not to have any after the early part of the afternoon.
- Alcohol may make your symptoms worse and often leads to a more disrupted sleep.
Nicotine stimulates the body and will make it harder to fall asleep. This includes both cigarettes and smokeless tobacco. So if you smoke, consider quitting.
Alternative medicine for perimenopause
In addition to conventional therapies, many women transitioning toward menopause want to know more about complementary and alternative approaches to treating symptoms. Researchers are looking into these therapies to determine their safety and effectiveness, but evidence is still often lacking.
Some of the options studied include:
Black cohosh. This herb extract is used by some women to treat hot flashes and other menopausal symptoms. There’s not enough evidence to support its use. Experts also are unsure of what risks taking black cohosh poses. Past studies suggested that black cohosh was harmful to the liver, but a more recent review of studies found no evidence that this is true. Researchers also question whether the herb extract is safe for women with or at risk of breast cancer.
Phytoestrogens. These estrogens occur naturally in certain foods. Two main types of phytoestrogens are isoflavones and lignans. Isoflavones are found in soybeans, chickpeas and other legumes. Lignans occur in flaxseed, whole grains, and some fruits and vegetables. There are also plant-derived compounds that have estrogen-like properties.
Isoflavone supplements generally come from soy or red clover. Lignans come mainly from flaxseed. Studies on phytoestrogens — whether from food or supplements — conflict on whether they help reduce menopausal symptoms. Studies also conflict on whether it’s possible that phytoestrogens could increase the risk of breast cancer or interfere with the effectiveness of tamoxifen.
Bioidentical hormones. The term “bioidentical” implies the hormones in the product are chemically identical to those your body produces. However, compounded bioidentical hormones aren’t regulated by the Food and Drug Administration (FDA), so quality and risks could vary. There’s also no evidence that compounded bioidentical hormones are safer or more effective than convention hormone therapy.
Dehydroepiandrosterone (DHEA). This natural steroid produced by your adrenal gland is available as a dietary supplement and has been used by some to improve sexual interest. But evidence on its effectiveness is mixed, and there are some concerns about possible harmful effects.
Low-risk complementary therapies, such as acupuncture, yoga and paced breathing may help reduce stress and improve psychological well-being. Research on acupuncture for decreasing hot flashes is inconclusive, but promising. Relaxation can help reduce stress, which may in turn help improve menopausal symptoms.
Talk with your doctor before taking any herbal or dietary supplements for perimenopausal or menopausal symptoms. The FDA does not regulate herbal products, and some can be dangerous or interact with other medications you take, putting your health at risk.
References