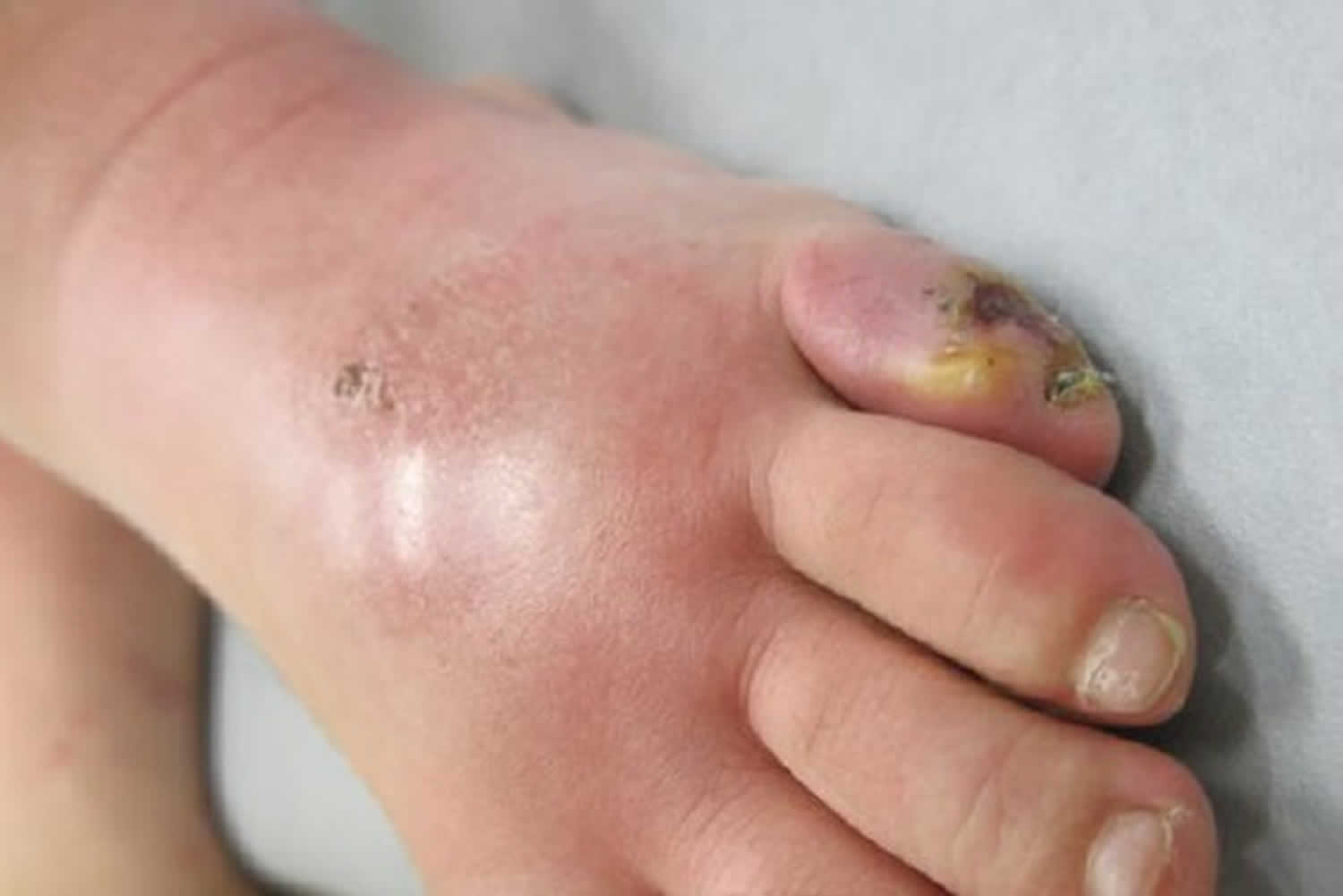
Phlegmon
Phlegmon is a medical term describing an expanding soft tissue non-specific inflammatory mass which may or may not be related to infection 1. Both historically and contemporaneously, phlegmon is used in an inconsistent fashion. Some use it to refer to a frank abscess, whilst others have used it exclusively for skin and subcutaneous infections. Phlegmon is usually caused by an infection and produces pus. The name phlegmon comes from the Greek word phlegmone, meaning inflammation or swelling. Factors affecting the development of phlegmons are virulence of bacteria and human’s immunity strength defenses.
As with any form of inflammation, phlegmon presents with inflammatory signs dolor (localized pain), calor (increase local tissue temperature), rubor (skin redness/hyperemia), tumor (either clear or non-clear bordered tissue swelling), functio laesa (diminish affected function). There may be systemic signs of infection, such as fever, general fatigue, chills, sweating, headache, loss of appetite.
Phlegmon causes
Phlegmon is commonly caused by bacteria – staphylococci, streptococci, pneumococci, spore and non-spore forming anaerobes. Non-infectious causes of phlegmon include acute pancreatitis, where inflammation is caused by leaking of pancreatic digestive enzymes into the surrounding tissues.
Phlegmon symptoms
Systemic features of infection like increased body temperature (up to 38-40°C), general fatigue, chills, sweatings, headache, and loss of appetite may be present. Severity of patient condition with phlegmons is directly proportional to the degree of intoxication level i.e the severe the condition, the higher degree of intoxication level.
Inflammatory signs:
- local redness and swelling,
- increase local tissue temperature,
- suppurative discharge,
- fever, rigor, signs and symptoms of severe infection.
Laboratory findings:
- elevated C-reactive protein levels
- white blood cell count leucocytosis.
Phlegmon treatment
Since phlegmon describes an area of inflammation, and not a specific disease process, the treatment depends on the cause and severity of the inflammation. Bacterial infections such as cellulitis may be treated by antibiotic therapy, depending on the severity. Phlegmon is best treated by following first principles: release of the relevant compartment, taking samples for microbiological surveillance and subsequent directed therapy, excision of the phlegmon and any devitalised tissue, thorough washout, elevation and antibiotics, and arranging a second look. If patients condition is mild and the signs of inflammatory process is presence without signs of infiltrates, then conservative treatment with antibiotics is sufficient. The most common types of targeted antibiotic therapy include: linezolid, vancomycin, cloxacillinum, teicoplanin, amoxicillin, imipenem, cefoperazone with sulbactam, sulfamethoxazole – trimethoprim and ceftazidime 2.
References- William Alexander Newman Dorland. Dorland’s Illustrated Medical Dictionary. (2018) ISBN: 978141602364
- Ławiński M, Forysiński K, Bzikowska A, Kostro JZ, Gradowska A, Pertkiewicz M. A comparison of two methods of treatment for central catheter tunnel phlegmon in home parenteral nutrition patients. Prz Gastroenterol. 2016;11(3):170–175. doi:10.5114/pg.2015.56556 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5047963