What is septoplasty
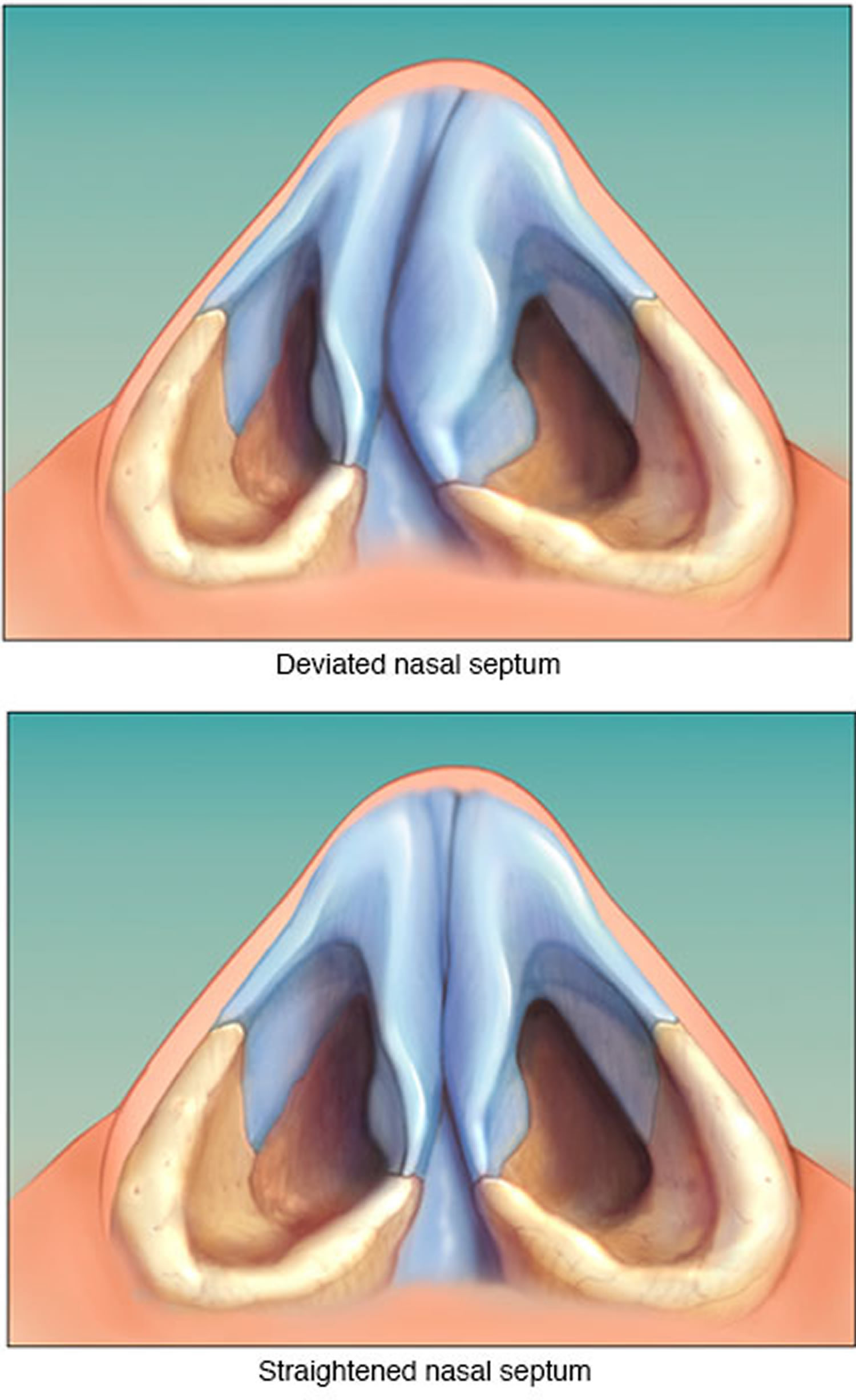
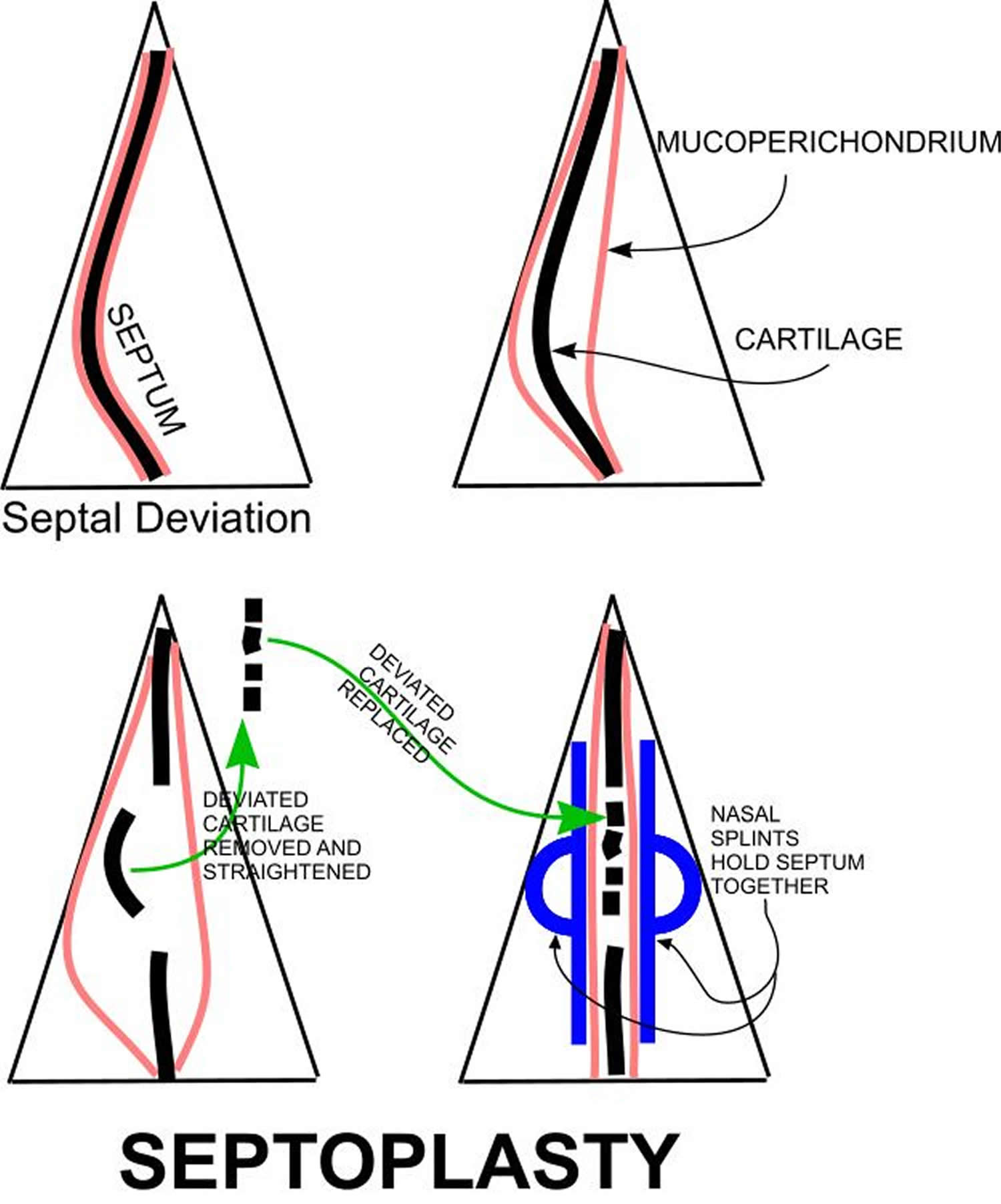
Septoplasty is a surgical procedure to correct a deviated nasal septum — a displacement of the bone and cartilage that divides your two nostrils (see Figure 3). Most people naturally have some nasal septum deviation – only people with severe deviations need treatment. Septal deviations commonly occur due to nasal trauma. Septoplasty is most commonly performed surgical procedure to correct a deviated nasal septum and to help relieve nasal obstruction. During septoplasty, your nasal septum is straightened and repositioned in the middle of your nose. This may require your surgeon to cut and remove parts of your nasal septum before reinserting them in the proper position. Sometimes, septoplasty is a necessary part of other surgical procedures like sinus surgery or nasal tumor removal.
Septoplasty procedure is not generally performed on minors, because the cartilaginous septum grows until around age 18.
When planning septoplasty, your surgeon considers your symptoms — such as breathing difficulties — and the physical structure and features of your nose. Talk with your surgeon about what septoplasty can achieve for you.
Septoplasty is a procedure that is done in the operating room under anesthesia. The procedure is typically performed under general anesthesia, but your doctor can help you decide if local anesthesia is an option for you. You may only have had local anesthetic in the area having surgery but this is less likely. Septoplasty surgery takes about 1 to 1 ½ hours. Septoplasty procedure is typically performed on an outpatient basis. This means that patients come in and go home the same day.
What you can expect with septoplasty
Septoplasty straightens the nasal septum by trimming, repositioning and replacing cartilage or bone. The surgeon works through incisions inside the nose. Occasionally it is necessary to make a small incision between the nostrils. If the nasal bones are crooked and pushing the septum off to one side, it may be necessary to make cuts in the bones of the nose to reposition them. Spreader grafts are small, reinforcing strips of cartilage that can be used to help correct a deviated septum when the problem is along the bridge of the nose. Sometimes these are necessary to effectively straighten the septum.
Who is a good candidate for septoplasty?
Septoplasty may be necessary to correct a deviated septum and alleviate breathing difficulties. Your physician will discuss treatment options and decide if this surgery is recommended.
In general, you may be a good candidate for septoplasty if you:
- Have a deviated septum that causes difficulty breathing
- Snore excessively that may disrupt your sleep or gives you trouble sleeping
- Are physically healthy
- Are a nonsmoker
If you’re considering surgery, spend some time reviewing septoplasty benefits and risks and learning about what to expect during recovery. Preparation ahead of time helps patients have reasonable expectations and a smoother recovery.
Why septoplasty is done
Having some deviation of the septum is common. When a deviated septum is severe, it can block one side of your nose and reduce airflow, causing difficulty breathing through one or both sides of your nose (see Figure 5 below).
The additional exposure of a deviated septum to the drying effect of airflow through the nose may sometimes contribute to crusting or bleeding in certain individuals. Septoplasty straightens the nasal septum by trimming, repositioning and replacing cartilage, bone or both.
If you experience symptoms — such as difficulty breathing through your nose — that significantly affect your quality of life, you may consider surgery to correct a deviated septum.
The nose
- Provides an airway for respiration.
- Moistens and warms entering air.
- Filters inhaled air to cleanse it of foreign particles.
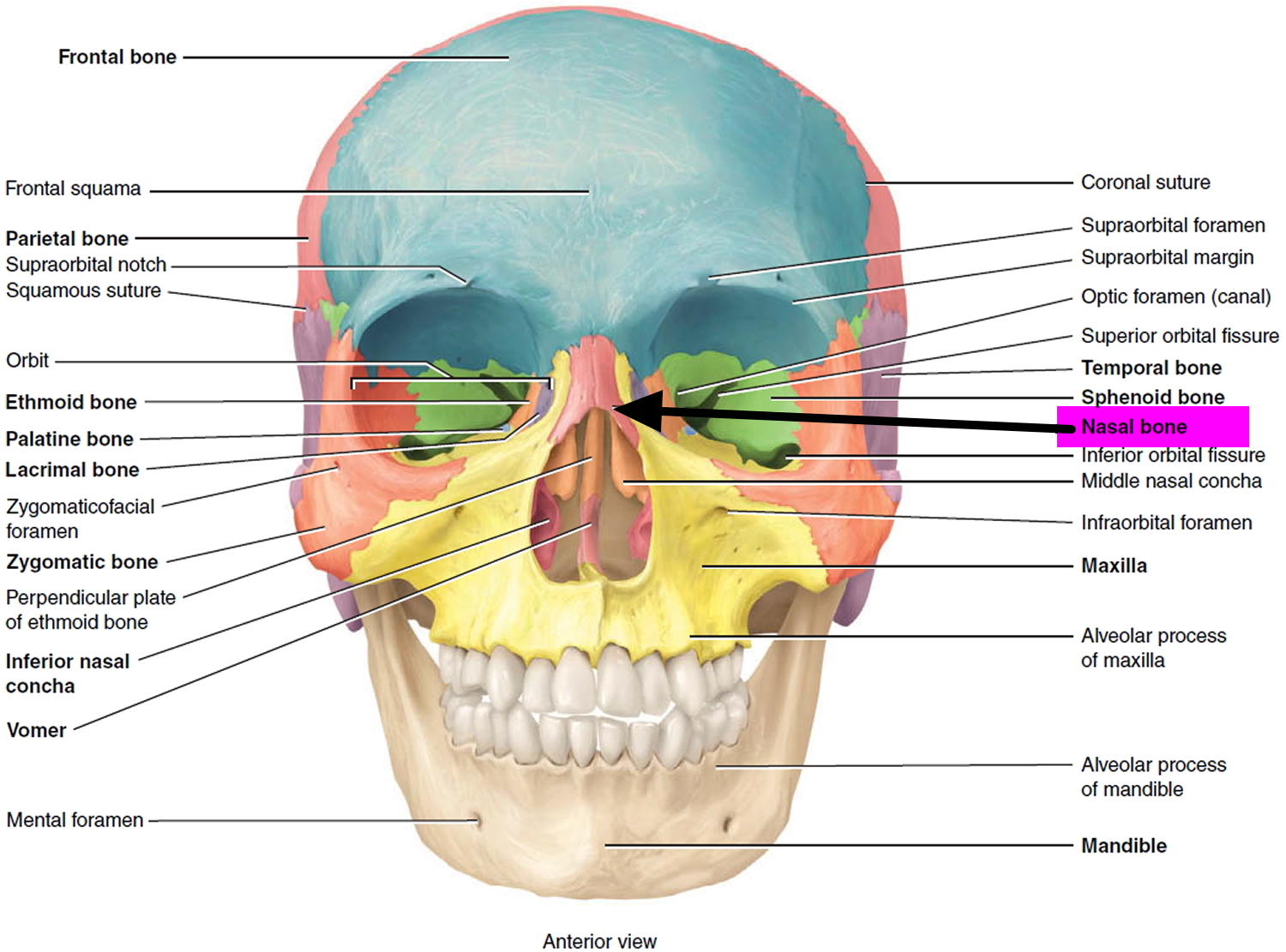
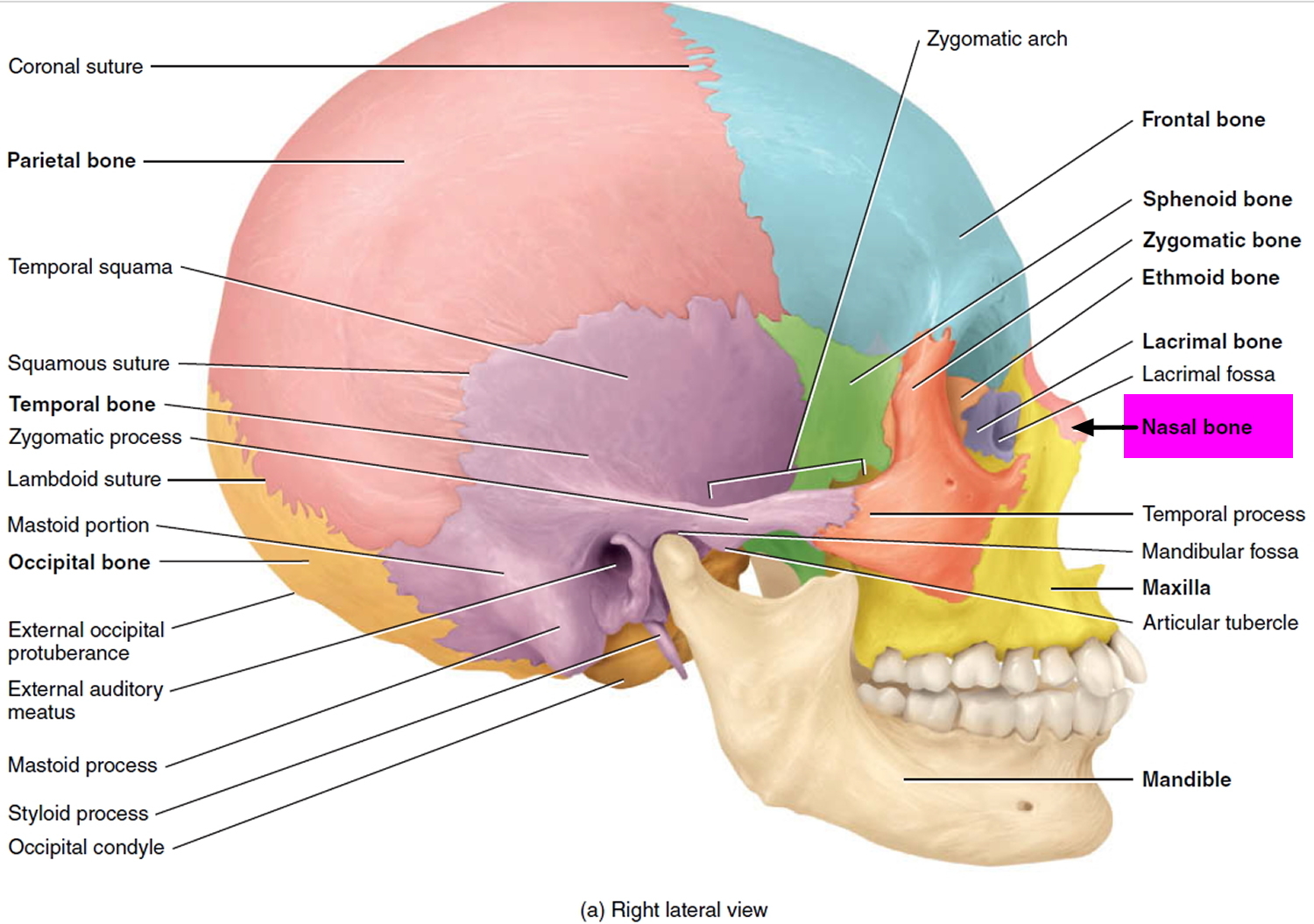
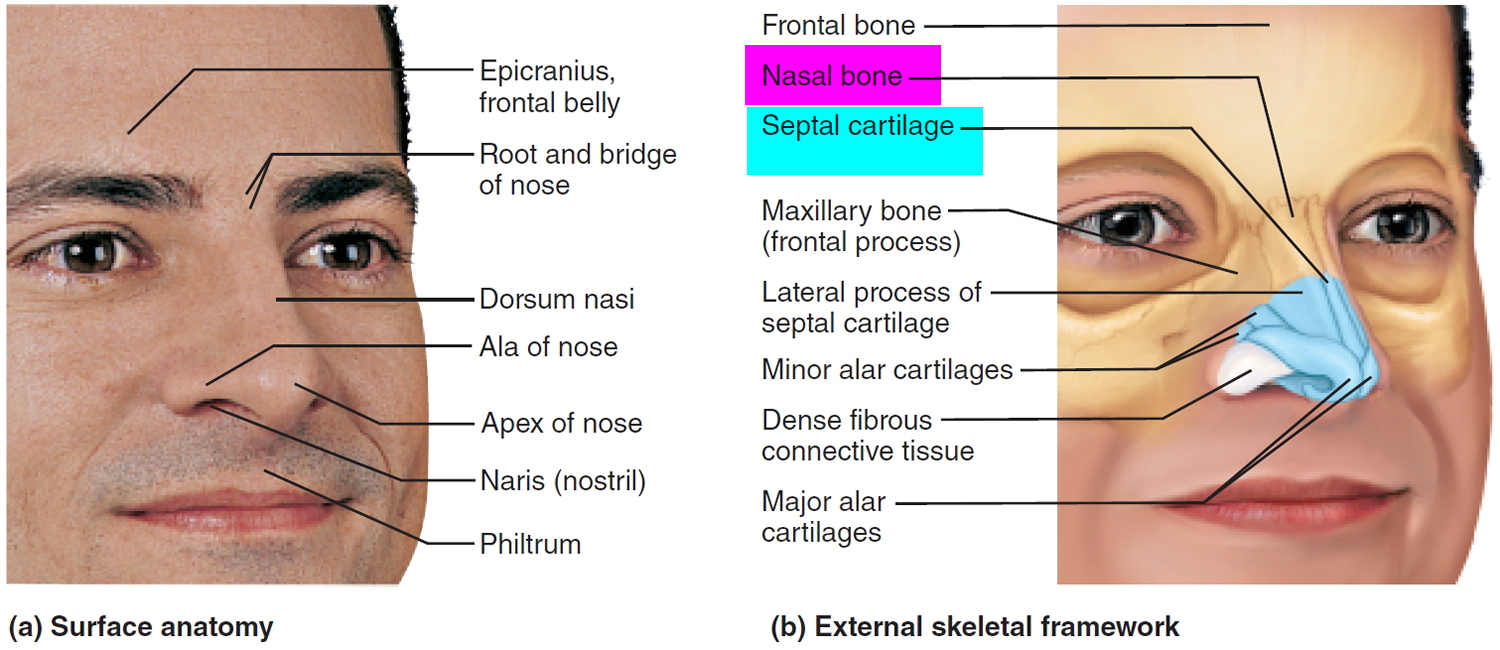
The paired nasal bones are small, flattened, rectangular-shaped bones that form the bridge of the nose (see Figures 1 and 2). These small bones protect the upper entry to the nasal cavity and provide attachment for a couple of thin muscles of facial expression. For those of you who wear glasses, they are the bones that form the resting place for the bridge of the glasses. The major structural portion of the nose consists of cartilage (see Figures 3 and 4).
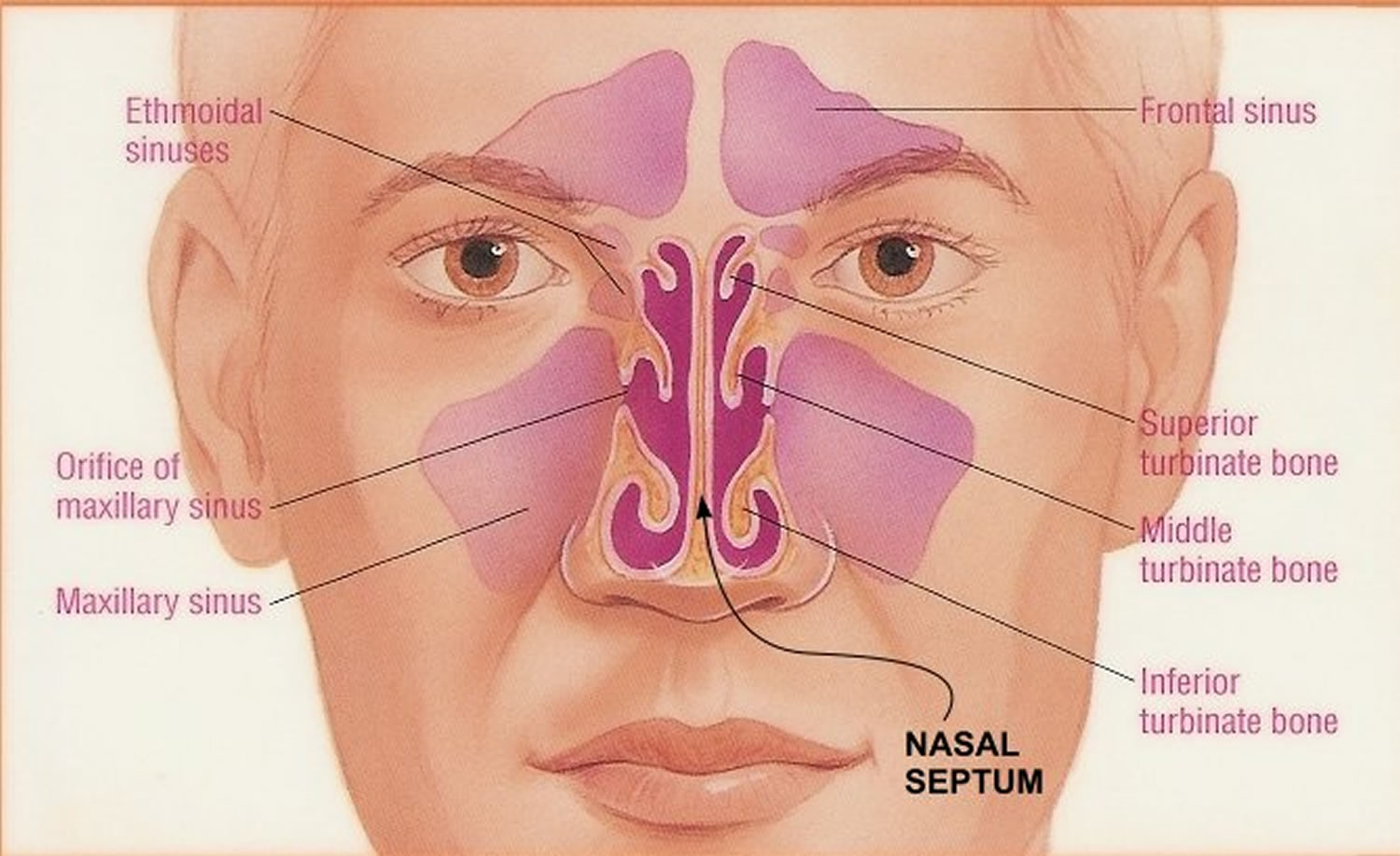
The nasal septum
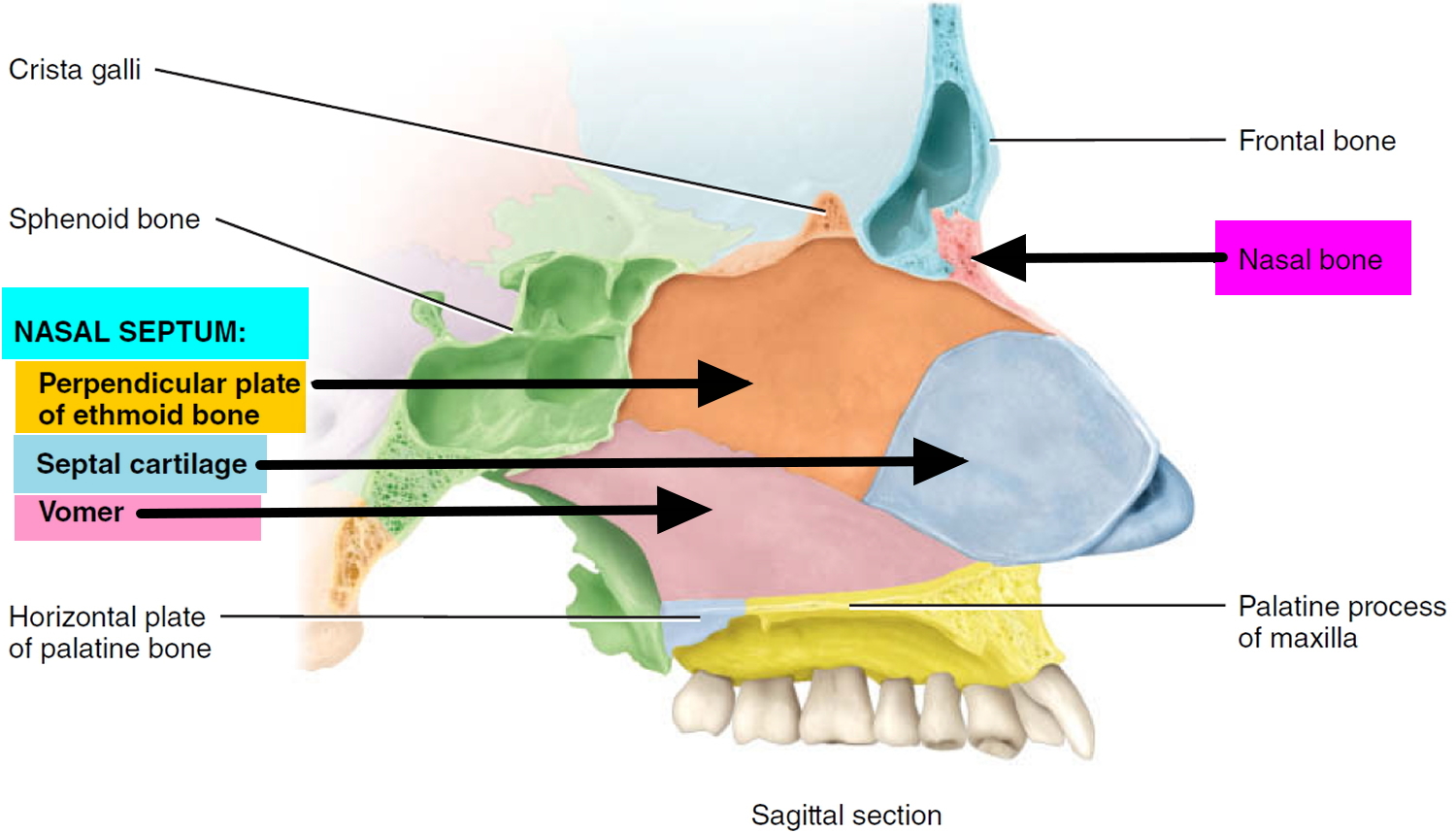
The nasal septum is made of cartilage and bone. The nasal septum is the wall dividing the nasal cavity into halves. The cartilage and bone of the septum are lined by a thin membrane called mucosa. This layer acts like a layer of skin for the inside of the nose. This layer covers and protects the cartilage and bone. It also helps to keep the inside of the nose moist.
The front portion of this natural partition is a firm but bendable structure made mostly of cartilage and is covered by skin that has a substantial supply of blood vessels. The ideal nasal septum is exactly midline, separating the left and right sides of the nose into passageways of equal size.
When the nasal septum is deviated, one or both sides of the nose can become blocked. In these instances, surgery can help correct the deviation and improve airflow.
The vomer is a roughly triangular bone on the floor of the nasal cavity that articulates superiorly with the perpendicular plate of the ethmoid bone and sphenoid bone and inferiorly with both the maxillae and palatine bones along the midline (see Figure3). It forms the inferior portion of the bony nasal septum, the partition that divides the nasal cavity into right and left sides.
Figure 1. Nasal bones
Figure 2. Nasal bones
Figure 4. Nose external anatomy
Deviated nasal septum
A deviated nasal septum is a condition in which the nasal septum (the bone and cartilage that divide the nose in half) is crooked (see Figure 3 above). Estimates are that 80 percent of all nasal septums are off-center, a condition that is generally not noticed. A “deviated septum” occurs when the septum is severely shifted away from the midline. The most common symptom from a badly deviated or crooked septum is difficulty breathing through the nose. The symptoms are usually worse on one side, and sometimes actually occur on the side opposite the bend. In some cases the crooked septum can interfere with the drainage of the sinuses, resulting in repeated sinus infections.
What causes deviated septum?
Most people are born with a slightly crooked nasal septum, but it is often never noticed. In some people, the deviation is visible early in life.
Some people develop a deviated septum (also called deviated nasal septum) as a result of trauma to their nose. For example: a car accident, sport, tripping over or just a bump while playing around.
Deviated septum prevention
Many people with a deviated septum were born with the condition. However, you may be able to prevent injuries to your nose by:
- wearing a seatbelt when in a car
- wearing a helmet when playing contact sports or riding a bike.
Deviated septum symptoms
Most people with a deviated septum have no symptoms at all, but some people may have:
- a blocked nose, which may be just one nostril, or may change from one nostril to the other
- frequent nosebleeds
- frequent sinus infections
- nasal congestion, sometimes one-sided
Some people also experience more general symptoms, such as:
- headaches or facial pain
- noisy breathing during sleep (in infants and young children)
- postnasal drip
- disturbed sleep.
In some cases, a person with a mildly deviated septum has symptoms only when he or she also has a “cold” (an upper respiratory tract infection). In these individuals, the respiratory infection triggers nasal inflammation that temporarily amplifies any mild airflow problems related to the deviated septum. Once the “cold” resolves, and the nasal inflammation subsides, symptoms of a deviated septum often resolve, too.
Deviated septum diagnosis
Your doctor will talk to you and examine you. The doctor may use a nasal endoscope – a long tube with a bright light at the tip – to see further back into your nose.
Nasal congestion can be caused by conditions other than a deviated septum. For example, you may have a different kind of structural problem inside your nose, chronic sinusitis, or allergies. In rare cases, bleeding and blockage can be signs of a nasal tumor.
Deviated septum treatment
Specific medications designed to help you breathe through your nose may help treat the symptoms of a deviated septum, such as:
- decongestants
- antihistamines
- nasal corticosteroid sprays.
If medications do not help, septoplasty surgery may be needed to straighten the nasal septum. In some cases, surgery to reshape the nose (rhinoplasty) may also be needed. While nose surgery is usually safe, there is a small risk of complications such as bleeding, infection, or numbness around the nose or front teeth.
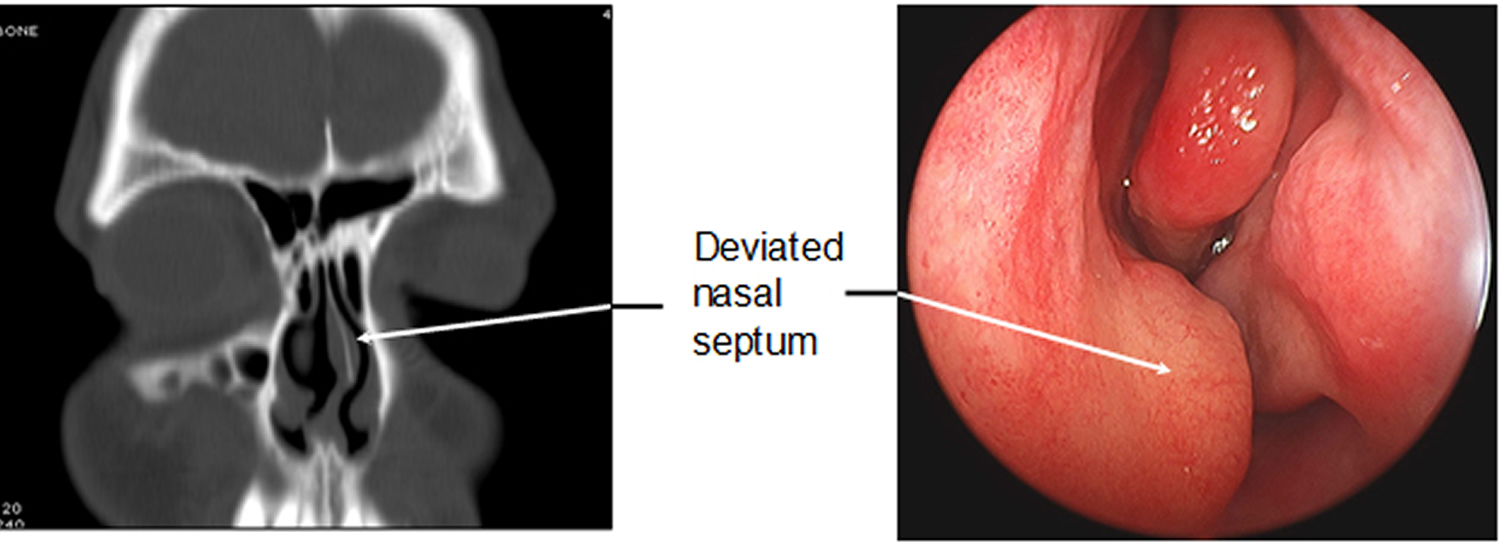
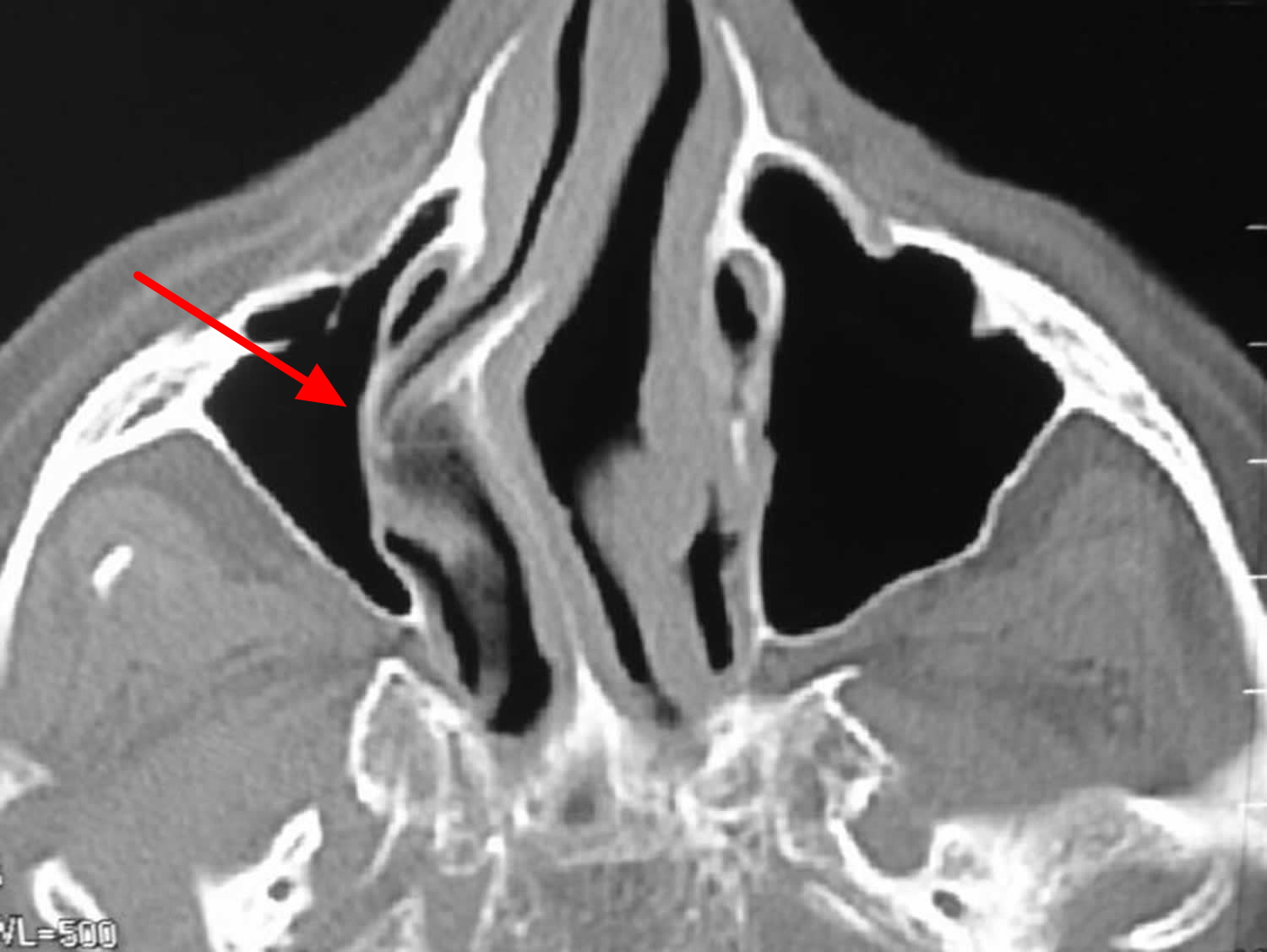
Figure 5. Deviated septum occurs when your nasal septum is significantly displaced to one side, making one nasal air passage smaller than the other.
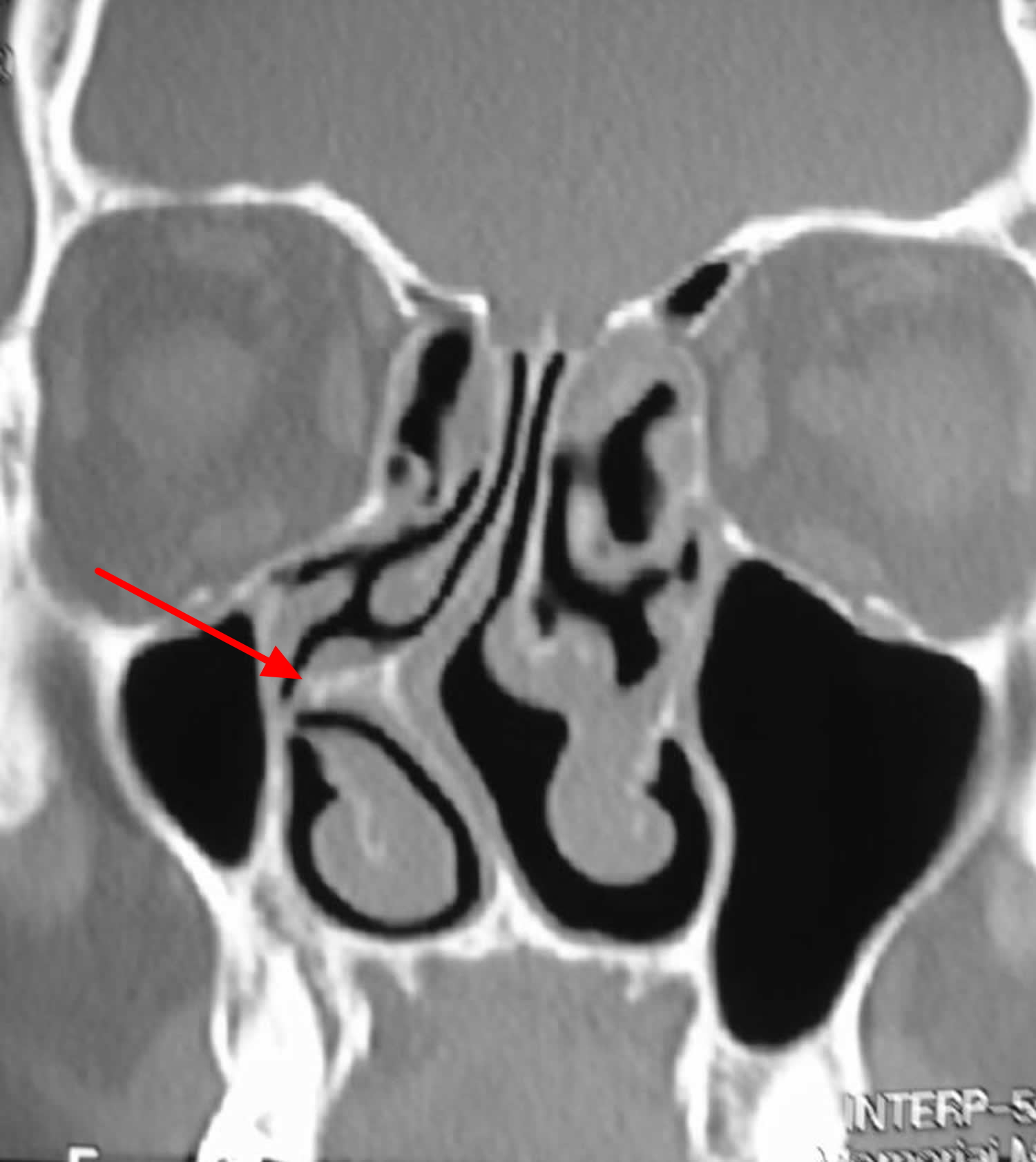
Figure 6. Deviated nasal septum – the CT scan and picture of the nose shown below demonstrate show examples of a deviated nasal septum. Both of these images point to a deviated nasal septum on the left side of the nose.
Septoplasty complications
As with any major surgery, septoplasty carries risks, such as bleeding, infection and an adverse reaction to the anesthetic.
Other possible risks specific to septoplasty include:
- Excessive bleeding: Most nasal surgery involves some degree of bleeding, which is generally well tolerated. In very rare situations, significant bleeding may require termination of the procedure. Blood transfusion is rarely necessary and is given only in an emergency. You should stop use of blood thinners such as aspirin, ibuprofen, omega 3 and vitamin E at least a week before surgery. If you require prescription blood thinners, please make sure you discuss this with your surgeon. Your surgeon will provide guidelines on when these medications can be stopped and re-started.
- Persistent in previous symptoms, such as nasal obstruction, despite surgery: The goal of surgery is to improve the structural problems that are leading to your nasal blockage. A large majority of patients (over 90%) have significant improvement in their nasal obstruction symptoms after surgery. However, many different factors can impact the final outcome, and some patients may have persistent nasal obstruction after surgery. In very rare instances, patients may notice no improvement or worsening of their obstruction symptoms.
- Infection: The nose is not a sterile environment, and infection can occur after septal and turbinate surgery. Fortunately, infections after septal and turbinate surgery are rare.
- Toxic Shock Syndrome: A very rare infection called “Toxic Shock Syndrome” can also occur, usually when packing is placed, but sometimes when no packing is used. This is a life threatening infection and requires immediate treatment. If you note a change in your blood pressure, heart rate, fever and unusual symptoms of skin discoloration, please notify your surgeon immediately. The incidence of toxic shock syndrome is thought to be less than one case in one hundred thousand septoplasty procedures.
- Tooth and nose numbness: The nerves that go to the gums and front teeth of the upper jaw come through the nose. Surgery on the septum can lead to stretching or injury to these nerves. This can lead to some numbness of the incisors of the upper jaw. In most instances, the numbness is temporary. Similarly, the tip of the nose may be numb after septoplasty. Sometimes, sensation can take weeks or even months to return. Temporary numbness or pain in these teeth postoperatively is common, but it almost always resolves within several months. Rarely, some patients can have persistent numbness of this area.
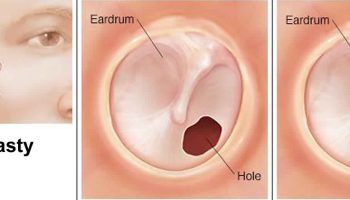
- Septal perforation: A septal perforation is a hole in the nasal septum. This can develop during or after surgery, especially if there is an infection. Sometimes, a perforation can lead to crusting and obstruction. Great care is taken during your procedure to prevent such a complication, but there is still a small risk this may occur. If the perforation does not cause any symptoms such as bleeding or crusting, then nothing further need be done. For symptomatic perforations, surgical closure or placement of a synthetic septal button can be performed.
- Spinal fluid leak: Because the top of the nasal septum is located below the skull, there is a rare chance of creating a leak of cerebrospinal fluid (the fluid that surrounds and cushions the brain) or injuring the brain. Should the rare complication of a spinal fluid leak occur, it may create a potential pathway for infection, which could result in meningitis. If a spinal fluid leak were to occur, additional surgery and hospitalization may be necessary. This is an extremely rare problem after septoplasty.
- A change in the shape of your nose
- A collection of blood in the nasal space that would need to be drained (septal hematoma)
- Other risks: Other uncommon risks of surgery include alteration of sense of smell or taste; persistence and/or worsening of facial pain; change in the resonance or quality of the voice; and swelling or bruising of the area around the eye. There is a very small risk of a subtle change in the external appearance of the nose after a septoplasty.
Additional surgery may be required to treat some of these complications or if the outcome of the surgery doesn’t match your expectations. Talk to your doctor about your specific risks before surgery.
Septoplasty surgery
How you prepare for a septoplasty
Before scheduling septoplasty, you must meet with your surgeon to discuss benefits and risks of the surgery. This meeting generally includes:
- Your medical history. Your doctor asks questions about conditions you have or have had, as well as any current medications.
- A physical examination. Your doctor conducts a physical examination, including any relevant testing. He or she also inspects your skin and the inside and outside of your nose.
- Photographs. Someone from your doctor’s office may take photographs of your nose from different angles. Your doctor may use these photos for discussion before septoplasty or for reference during and after surgery.
- A discussion of your expectations. You and your doctor should talk about your expectations. He or she explains what septoplasty can and can’t do for you and what your results might be.
Food and medications
Avoid medications containing aspirin or ibuprofen (Advil, Motrin IB, others) for about two weeks before surgery and after surgery. These medications may increase bleeding. Take only those medications approved or prescribed by your surgeon.
Other precautions
If you smoke, stop smoking. Smoking disturbs the healing process after surgery.
During the septoplasty procedure
Septoplasty is a surgical procedure performed entirely through the nostrils, accordingly, no bruising or external signs occur. The surgery might be combined with a rhinoplasty, in which case the external appearance of the nose is altered and swelling/bruising of the face is evident. Septoplasty may also be combined with sinus surgery.
Septoplasty requires local or general anesthesia, depending on your and your surgeon’s preferences and on the complexity of the surgery.
- Local anesthesia. This type of anesthesia is limited to your nose. Your doctor injects the pain-numbing medication (anesthetic) into your nasal tissues. If you will also have sedation, this is produced with medication injected through a catheter placed in a vein — an intravenous (IV) line. The medication makes you groggy but not fully unconscious.
- General anesthesia. With general anesthesia, you inhale an anesthetic agent or receive an anesthetic through an IV line. This type of anesthesia affects your entire body and induces a temporary state of unconsciousness.
Discuss with your doctor beforehand which kind of anesthesia is best in your case.
Most people receive general anesthesia for septoplasty. You will be asleep and pain-free. Some people have the surgery under local anesthesia, which numbs the area to block pain. You will stay awake if you have local anesthesia. Surgery takes about 1 to 1½ hours. Most people go home the same day.
During a septoplasty surgery, your surgeon will attempt to straighten the cartilage and bone that have led to the nasal septum being deviated. During the procedure, the lining (the mucosa) is first lifted off the cartilage and bone. The cartilage and bone can then be reshaped. Sometimes, portions of the cartilage and bone need to be removed. The lining is then laid back down.
Because the septal cartilage has ‘memory’–it has a tendency to assume its initial shape– the septal cartilage can sometimes bend after the surgery.
You may have splints or packing inside your nose during the healing process. In some instances, there may be nothing more than dissolving stitches inside your nose. Your surgeon can let you know whether packing or splints will be placed in your nose and how long they will stay in place.
Soft silicone splints may be inserted inside each nostril to support the septum. To prevent postoperative bleeding, your doctor may place bandage-like material in your nose.
After the surgery, you’re moved to a recovery room, where the staff monitors you and watches for any complications. This procedure is typically performed on an outpatient basis, so you’ll likely be able to go home the same day.
A septoplasty procedure includes the following steps
Step 1 – Anesthesia
Medications are administered for your comfort during the surgical procedure. The choices include intravenous sedation and general anesthesia. Your doctor will recommend the best choice for you.
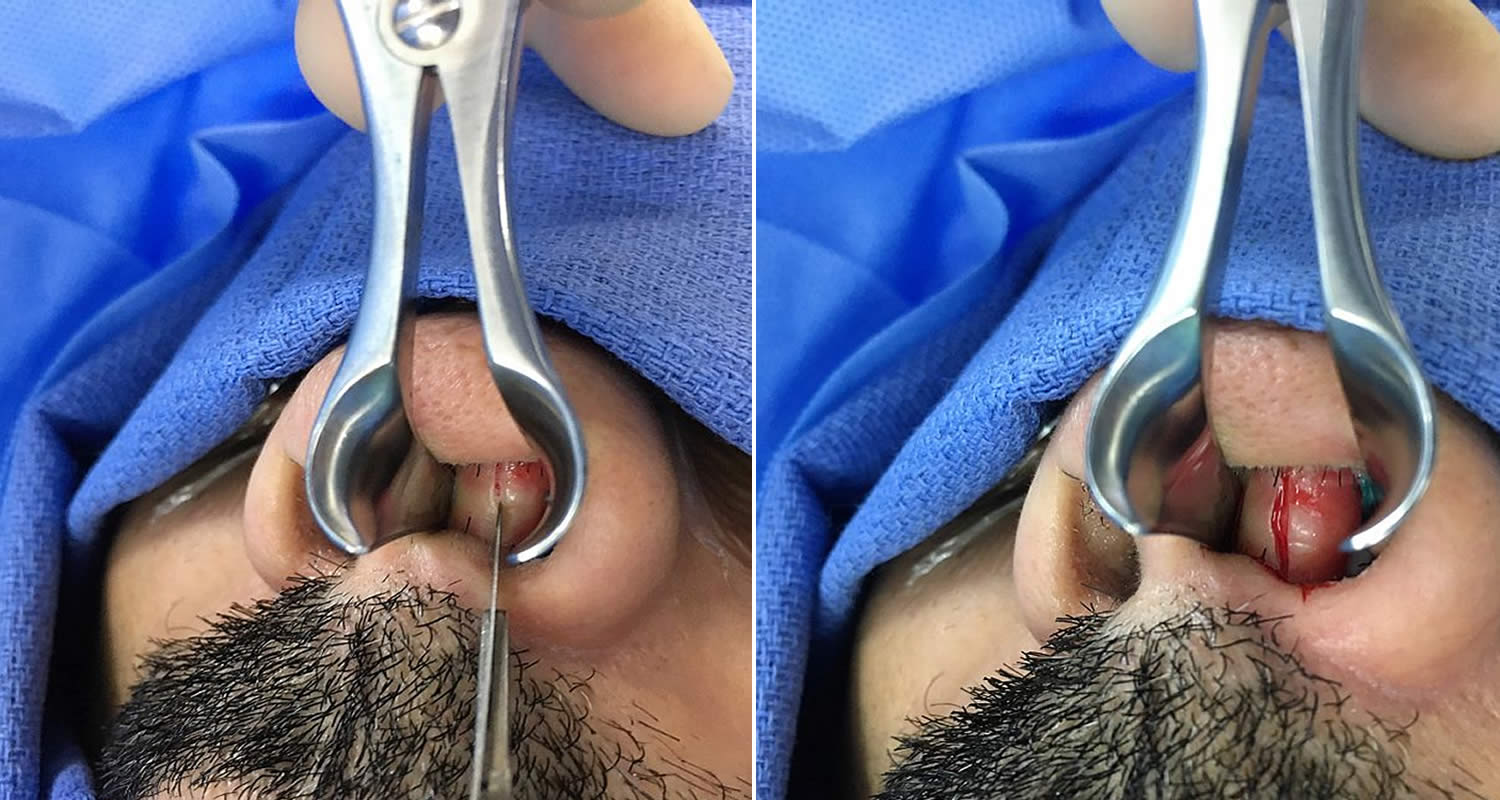
Step 2 – The incision
If septoplasty is performed in isolation, the incisions are often within the nasal cavity. For difficult septoplasties or some of those performed with rhinoplasties, a small incision may be made across the columella, the narrow strip of tissue that separates the nostrils.
Figure 7. Septoplasty surgery – incision
Step 3 – Mucosal lining separation
The nasal mucosal lining, the membrane that covers the surface of the septum, is then lifted away from the septum at one side. This is a critical step that is carefully performed since the lining is fragile, which may result in a tear or hole in the lining as the mucosa is lifted away from the septum. Similarly the mucosal lining on the opposite side is lifted away from the septum.
Step 4 – Deviated septum correction
The deviated septum (bone and/or cartilage) is removed, leaving behind the special mucosal lining.
Step 5 – Closing the incision
Once the septum is in the desired position and straightened, the nasal mucosal lining is repositioned around it and sutured back together.
Step 6 – The results
The newly constructed septum may be stabilized by splints or packing, which are removed shortly after surgery. Internal sutures used during the surgery dissolve on their own over time.
Figure 8. Septoplasty splints
After the septoplasty procedure
To further decrease the chances of bleeding and swelling, your doctor may ask that you follow these precautions for several weeks after surgery. Depending on the extent of your surgery, you may not be asked to comply with all of them:
- Avoid strenuous activities, such as aerobics and jogging. This is to decrease the chance of a blood pressure elevation that could cause a nosebleed.
- Don’t blow your nose.
- Elevate your head when you’re sleeping.
- Wear clothes that fasten in the front; don’t pull clothing, such as shirts or sweaters, over your head.
Septoplasty results
Though results are most often stable, cartilage and tissue may gradually move or reshape over time. The nasal tissues are relatively stable by three to six months after surgery. However, some changes can still occur for up to a year or more after surgery.
Most people find that septoplasty improves their symptoms, such as difficulty breathing, caused by a deviated septum. The level of improvement you can expect with septoplasty may vary.
Some people find that their symptoms continue even after surgery and opt to undergo a revision septoplasty to further refine the nose and septum.
Septoplasty recovery
You can expect to have pain, fatigue, nasal stuffiness, and mild nasal drainage after your surgery. Pain is generally mild with this type of septoplasty surgery and is typically well controlled with oral pain medications. The stuffiness typically results from swelling after the procedure, and typically generally starts to improve after the first week. You may have drainage of some mucus and blood from your nose after surgery. This is a normal part of the healing process.
You may be asked to use saline sprays or irrigations after your surgery. Please check with your surgeon about any post-operative care you will need to perform to allow your nose to heal properly.
Septoplasty is surgery to correct any problems in the nasal septum. The nasal septum is the wall inside the nose that separates the nostrils.
What to expect at home
During your septoplasty recovery, you may have either packing (to stop bleeding) or splints (to hold the tissues in place) inside your nose.
If a rhinoplasty is performed at the same same time, external bandages or a splint will also be placed on the outside of the nose. The packing can be removed by your physician in the office 24 to 36 hours after surgery. Splints may be left in place for as long as 1 to 2 weeks.
You may have swelling in your face for 2 to 3 days after surgery. Your nose may drain and bleed a little for 2 to 5 days after surgery.
Your nose, cheeks, and upper lip may be numb. The numbness on the tip of your nose may take several months to completely go away.
It may take a few months for you to expect the full benefits of septoplasty. During the initial healing period, there may be minor pain and difficulty breathing. Your physician will prescribe appropriate pain medication. Over-the-counter pain medication such as aspirin or ibuprofen should be avoided as these drugs may thin the blood. Your physician may also recommend irrigation using saline (salt water) to wash away any crust or surgical debris.
You will be given specific instructions that may include:
- How to care for your surgical site following surgery.
- Medications to apply or take orally to aid healing and reduce the risk of infection.
- Specific concerns to look for at the surgical site or in your general health.
- When to follow up with your plastic surgeon.
Be sure to ask your plastic surgeon specific questions about what you can expect during your individual recovery period.
- What medication will I be given or prescribed after surgery?
- Will I have dressings/bandages after surgery? When will they be removed?
- When can I bathe or shower?
- When can I resume normal activity and exercise?
- When do I return for follow-up care?
Healing will continue for several weeks as swelling decreases. It is important for your final result to continue to follow your plastic surgeon’s instructions and attend follow-up visits as scheduled.
Self-care
Rest all day after surgery. DO NOT touch or rub your nose. Avoid blowing your nose (it is normal to feel stuffed up for several weeks).
You may apply ice packs to your nose and eye area to help with pain and swelling, but make sure to keep your nose dry. Cover the ice pack with a clean, dry cloth or small towel. Sleeping propped up on 2 pillows will also help reduce swelling.
You will get a prescription for pain medicines. Get it filled when you go home so you have it when you need it. Take pain medicines, such as acetaminophen (Tylenol) or a prescription painkiller, the way you have been told to take them. Take your medicine when pain first starts. DO NOT let pain get very bad before taking it.
You should not drive, operate machinery, drink alcohol, or make any major decisions for at least 24 hours after surgery. Your anesthesia may make you groggy and it will be hard to think clearly. The effects should wear off in about 24 hours.
Limit activities that could make you fall or put more pressure on your face. Some of these are bending over, holding your breath, and tightening muscles during bowel movements. Avoid heavy lifting and hard physical activity for 1 to 2 weeks. You should be able to go back to work or school 1 week after surgery.
DO NOT take baths or showers for 24 hours. Your nurse will show you how to clean your nose area with Q-tips and hydrogen peroxide or another cleaning solution if needed.
You may go outside a few days after surgery, but DO NOT stay in the sun for more than 15 minutes.
Follow up with your provider as you have been told. You may need to have stitches removed. Your provider will want to check your healing.
When to call the doctor
Call your health care provider if you have:
- Trouble breathing
- A heavy nosebleed, and you cannot stop it
- Pain that is getting worse, or pain that your pain medicines are not helping with
- High fever and chills
- Headaches
- Disorientation
- Neck stiffness
Septoplasty recovery time
The wounds in/on the nose will heal quickly and improvement in breathing is expected to improve shortly after the surgery. The overall healing process will be slow as cartilage and nasal tissue can take 3-6 months to fully settle. However, changes in the septum, cartilage and nasal tissue may occur for up to a year or more after surgery.
Most patients find their symptoms, such as difficulty breathing, to improve greatly after surgery and healing. Other improvements include better sleep and reduction of snoring. These level of improvements expected from septoplasty vary from patient to patient.
Most patients who undergo septoplasty do not experience any ongoing symptoms. However, the practice of medicine and surgery is not an exact science. While good results are expected, there is no guarantee. In some cases, the cartilage and nasal tissue may shift and block the nasal pathway and airflow. Therefore, patients who continue to have symptoms may elect to have a second septoplasty procedure to reshape the nose and further refine the septum.
Following your physician’s instructions is key to a successful septoplasty postoperative outcomes. It is important that the nose and septum are not subjected to excessive force, abrasion or motion during the time of healing. Your doctor will give you specific instructions on how to care for yourself.