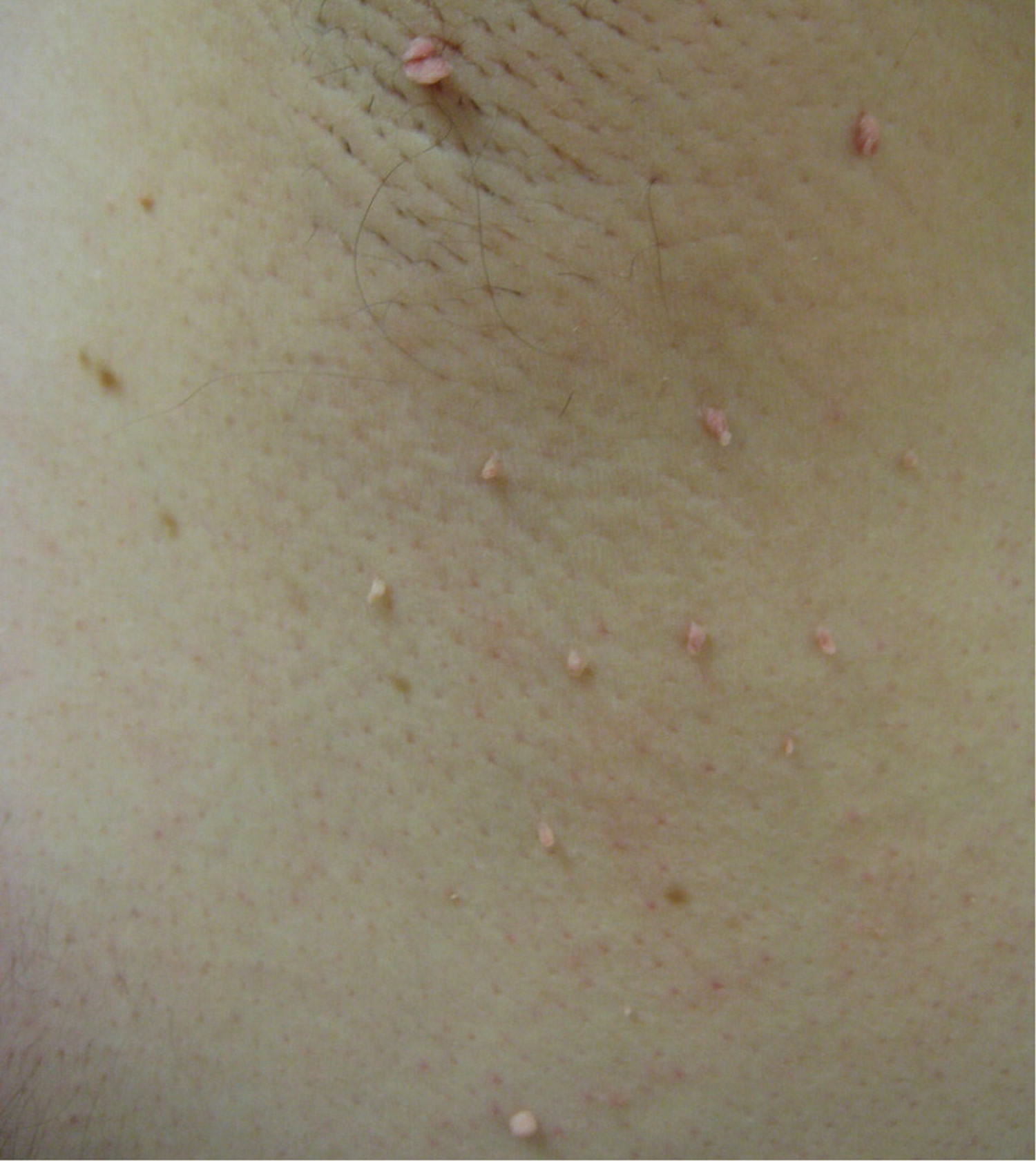
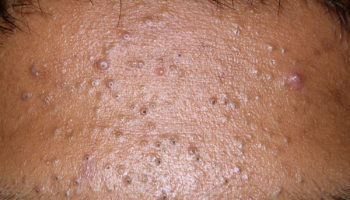
A cutaneous skin tag also known as acrochordons or fibroepithelial polyps, is an extremely common skin growth, reportedly 46% of the general population, increasing in frequency with patient age. Skin tags are small, and typically pedunculated benign neoplasms 1. Most of the time, skin tags are harmless 2. Skin tags consist of hyperplastic soft dermis and epidermis and are usually skin colored or brownish (Figure 1). They are generally 2 to 5 mm in size, although they may become larger. The most common locations are in skin folds (e.g., neck, armpits, groin), where skin irritation can be a causative factor.
Skin tags may bother patients because of associated symptoms such as itching, pain, and rubbing against clothes or simply because of their appearance. There may be a familial predisposition for developing these lesions, as well as the established association with obesity and insulin resistance.
Diagnosis is based on the appearance and location of lesions. They must be differentiated from neurofibromas, seborrheic keratoses, and pedunculated nevi. There have been rare case reports of skin tags that were found to be basal or squamous cell carcinomas. Treatment consists of cryosurgery, electrodesiccation, or simple scissor or shave excision. Electrodesiccation causes less hypopigmentation than cryotherapy and is the preferred treatment in nonwhite patients. An ear speculum placed over a small lesion may be helpful in directing the freeze pattern during cryosurgery.
A cutaneous tag usually occurs in older adults. They are thought to occur from skin rubbing against skin.
Skin tags are strongly associated with obesity and insulin resistance. Along with many other types of common benign skin lesions found on a skin exam of most adult patients (benign melanocytic nevi, seborrheic keratoses, cherry angiomas), they develop increasingly with age, and despite their benign nature, they can be of great concern and impact a patient’s quality of life. Other common benign lesions can mimic acrochordons, including benign melanocytic nevi and neurofibromas 3.
Skin tags occur in 25% to 46% of adults and increase with age and during pregnancy 4. Studies 5, 6 have found that skin tags are associated with the metabolic syndrome (obesity, dyslipidemia, hypertension, insulin resistance, and elevated C-reactive protein levels). This suggests they may be viewed as cutaneous clues for cardiovascular disease.
One inherited syndrome is frequently discussed in the context of skin tags. This syndrome, Birt-Hogg-Dube syndrome, is a rare autosomal dominant genodermatosis characterized by multiple fibrofolliculomas and trichodiscomas that may be indistinguishable from acrochordons 3. Birt-Hogg-Dube syndrome is caused by a mutation in the FLCN gene that produces folliculin, a tumor suppressor protein. Reported associations with Birt-Hogg-Dube syndrome include spontaneous pneumothorax and renal cell carcinoma (especially chromophobe and hybrid oncocytic carcinomas) 3.
In addition, one variant of basal cell carcinoma may present with clinical overlap with skin tags 3. The fibroepithelioma of Pinkus is a subtype of basal cell carcinoma that is classically reported as a pink acrochordon-like lesion (pedunculated papule) appearing on the lower back. This was first described by Hermann Pinkus in 1953 as a premalignant fibroepithelial tumor 3.
Figure 1. Skin tags
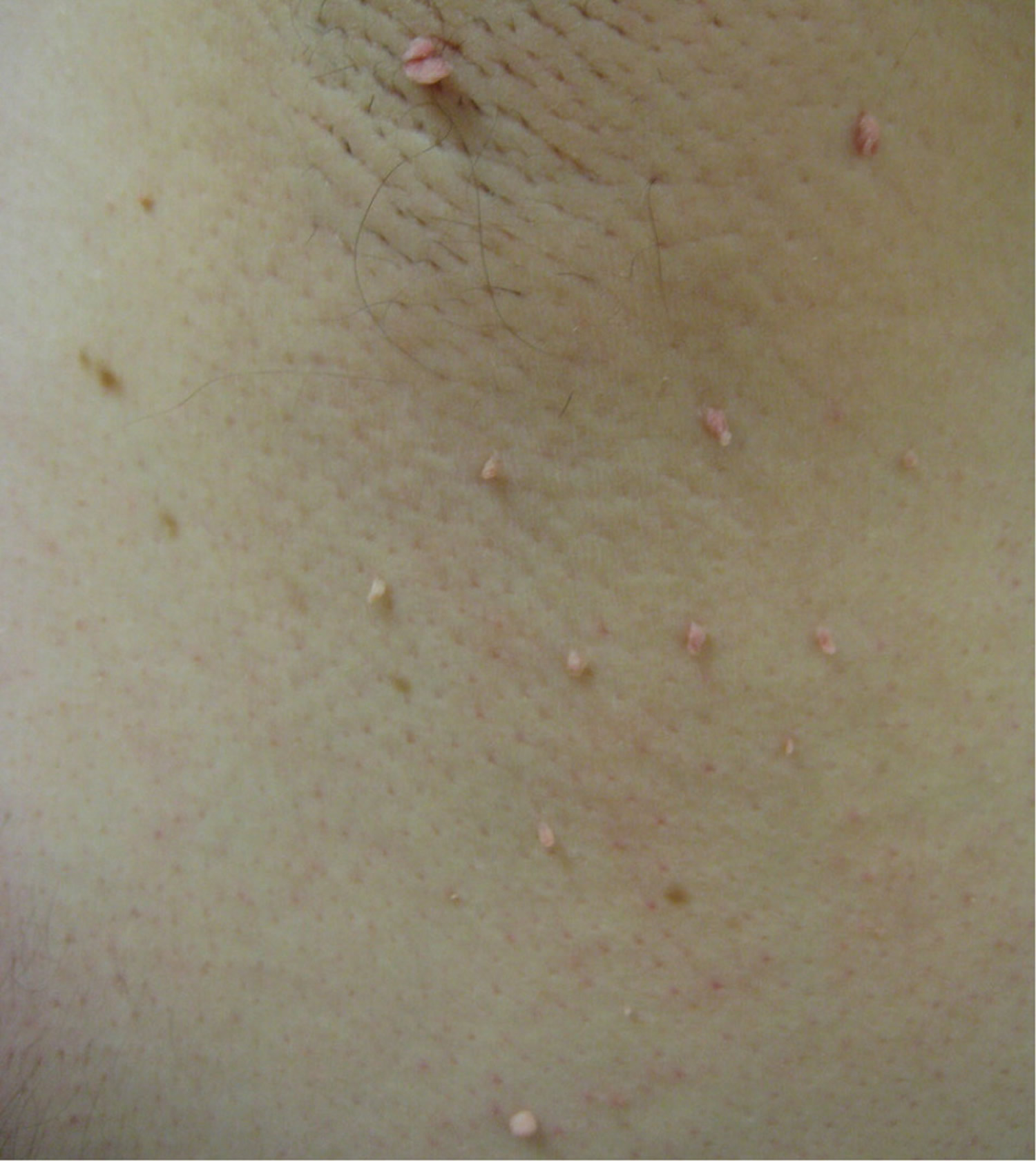
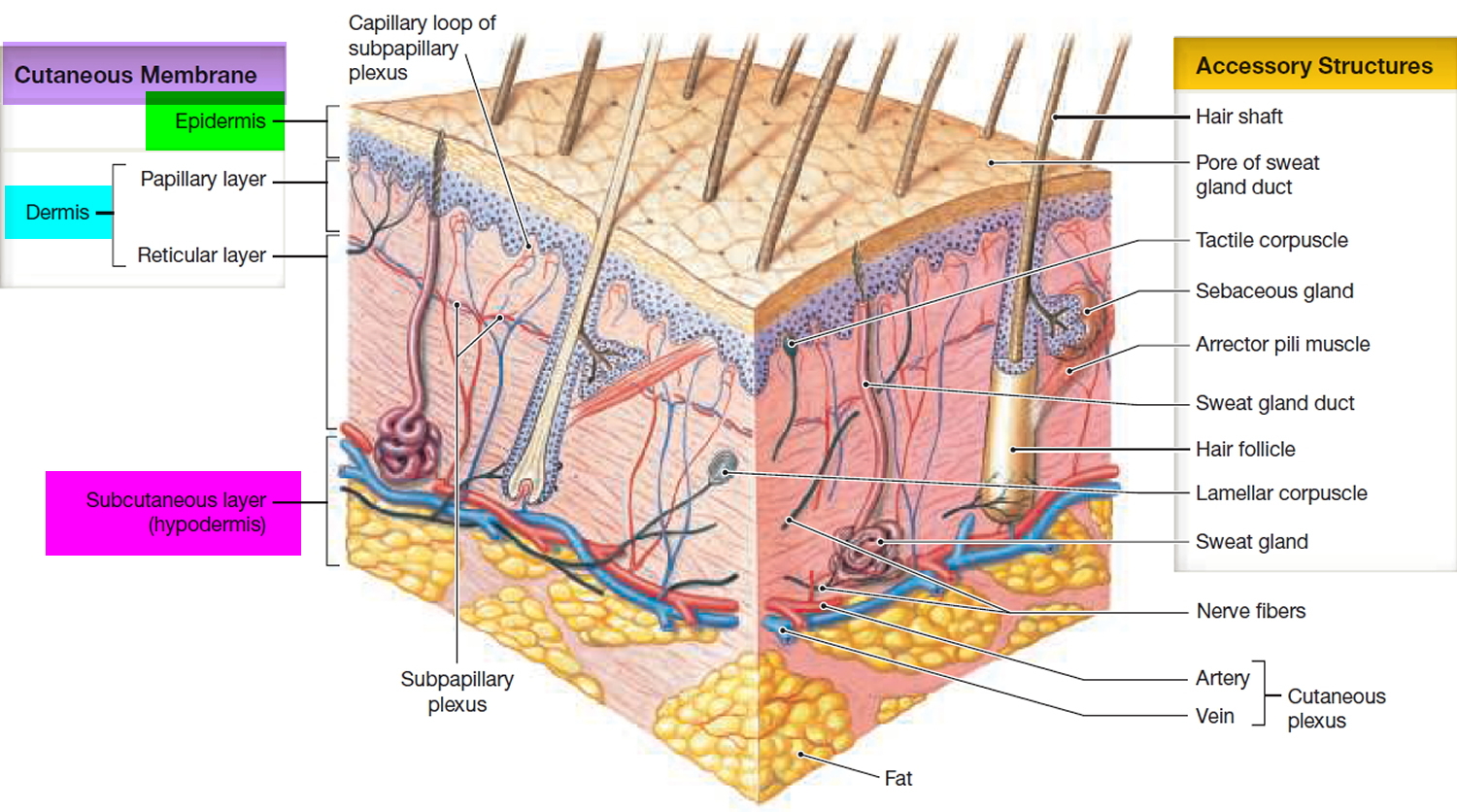
Figure 2. Skin structure
Skin Tags Signs and Symptoms
The skin tag sticks out of the skin and may have a short, narrow stalk connecting it to the surface of the skin. Some skin tags are as long as a half an inch (1 centimeter). Most skin tags are the same color as skin, or a little darker.
Occasionally, skin tag lesions may be hyperkeratotic or filiform (a warty appearance), and may, in fact, have a concurrent wart (verruca vulgaris). Around the neck and axilla, acrochordons may present concurrently with acanthosis nigricans, the velvety brown plaques that may also occur in these same areas. The parallel presentation of both acrochordons and acanthosis nigricans is not surprising as both are commonly associated with obesity and insulin resistance and diabetes. Along these lines, acanthosis nigricans may have a component of papillomatous changes apparent on histopathology.
In most cases, a skin tag is painless and does not grow or change. However, it may become irritated from rubbing by clothing or other materials.
Places where skin tags occur include:
- Neck
- Underarms
- Middle of the body, or under folds of skin
- Eyelids
- Inner thighs
- Other body areas
Your health care provider can diagnose this condition by looking at your skin. Skin tags typically do not need to be examined with histopathology. Given the general lack of clinical concern when presented with these lesions on the exam, no laboratory, radiographic, or other tests are typically necessary to investigate patients with skin tags.
Sometimes a skin biopsy is done. When sampled, pathology reveals a papillary dermis composed of loosely arranged collagen fibers and dilated capillaries and lymphatic vessels, without appendageal structures (hair follicles, sweat glands). It is still possible, however, unlikely, to have a concerning lesion present clinically as an skin tag or as a component of an skin tag. This includes such neoplasms as malignant melanoma, squamous cell carcinoma, or basal cell carcinoma (notably, the basal cell carcinoma subtype fibroepithelioma of Pinkus, which may present as an acrochordon-like pink papule in the lower back).
These cases are exceedingly rare, however, and it would not be considered cost-effective to regularly evaluate acrochordon-like lesions with pathology unless there is a particular indication. These indications include clinical suspicion for one of these more concerning lesions (dysplastic or atypical nevi, malignant melanoma, basal cell carcinoma, squamous cell carcinoma), presentation of the acrochordon-like growth as a new or changing lesion, or concern for Birt-Hogg-Dube or similar syndrome.
Treatment is often not needed because skin tags are benign. If irritated or cosmetically undesired, skin tags may be treated with any destructive modality, but they are most commonly treated by snip excision (with scissors) or liquid nitrogen cryotherapy. Other options may include shave excision, electrocautery, and ligation (tying a string or suture around the lesion).
- Do not cut it yourself, because it can bleed a lot.
See your doctor if the skin tag changes, or if you want it removed.
Your doctor may recommend treatment if the skin tag is irritating, or you don’t like how it looks.
Treatment may include:
- Surgery to remove it
- Freezing it (cryotherapy)
- Burning it off (cauterization)
- Tying string or dental floss around it to cut off the blood supply so that it will eventually fall off.
A skin tag is most often harmless (benign). It may become irritated if clothing rubs against it. In most cases, the growth usually does not grow back after it is removed. However, new skin tags may form on other parts of the body.
References- Diagnosing Common Benign Skin Tumors. Am Fam Physician. 2015 Oct 1;92(7):601-607. http://www.aafp.org/afp/2015/1001/p601.html
- Cutaneous skin tag. Medline Plus. https://medlineplus.gov/ency/article/000848.htm
- Lipoff J, Chatterjee K. Acrochordon. [Updated 2017 Aug 23]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2017 Jun-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK448169/
- Banik R, Lubach D. Skin tags: localization and frequencies according to sex and age. Dermatologica. 1987;174(4):180–183.
- Tamega AA, Aranha AM, Guiotoku MM, Miot LD, Miot HA. Association between skin tags and insulin resistance [in Portuguese]. An Bras Dermatol. 2010;85(1):25–31.
- Sari R, Akman A, Alpsoy E, Balci MK. The metabolic profile in patients with skin tags. Clin Exp Med. 2010;10(3):193–197.