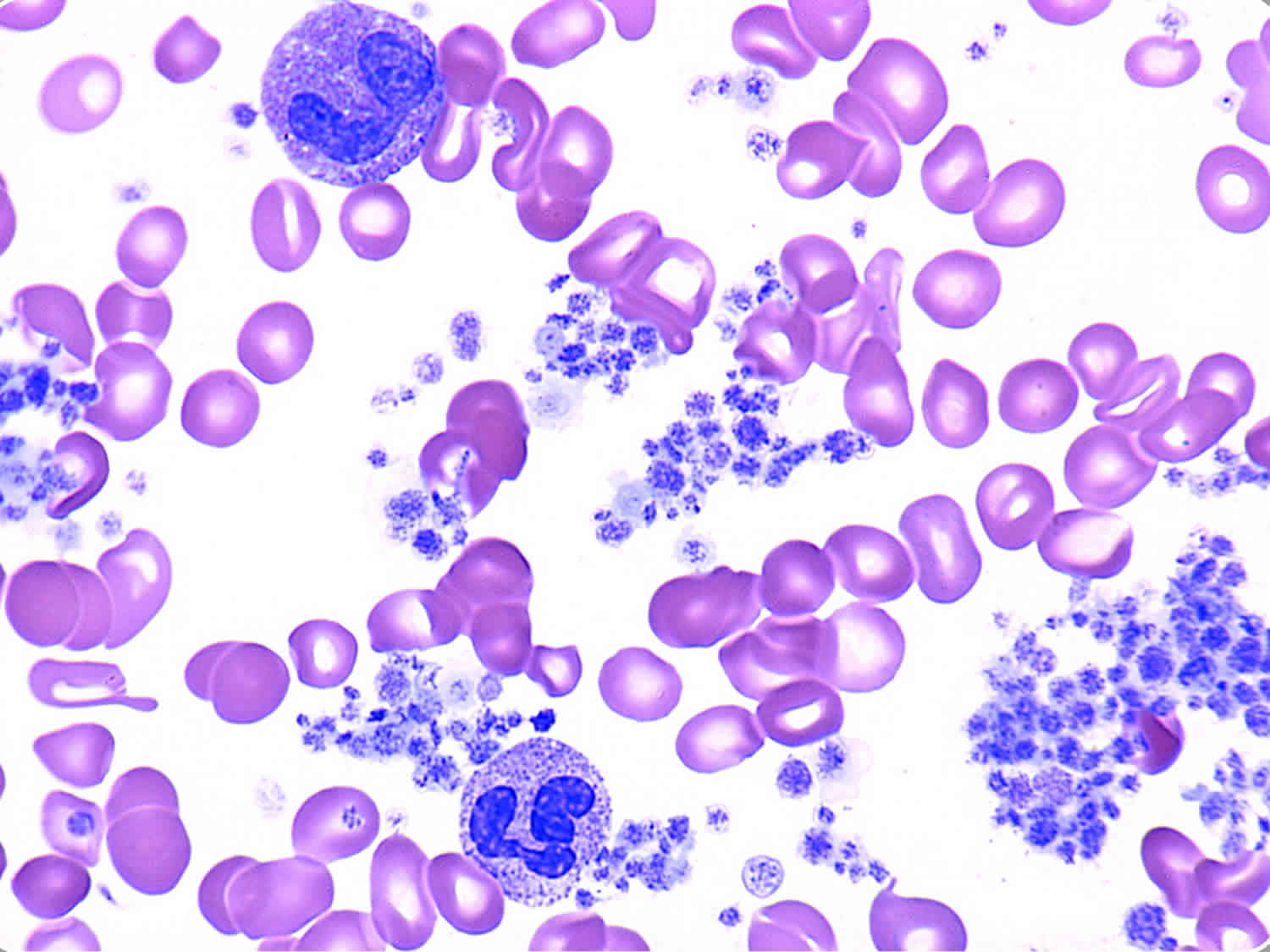
What is thrombocytosis
Thrombocytosis and thrombocythemia, are conditions in which your blood has a higher than normal number of platelets. Platelets also are called thrombocytes because a blood clot also is called a thrombus. Platelets are blood cell fragments. Platelets are made in your bone marrow along with other kinds of blood cells. Platelets travel through your blood vessels and stick together (clot). Clotting helps stop any bleeding that may occur if a blood vessel is damaged.
A normal platelet count ranges from 150,000 to 450,000 platelets per microliter of blood.
The term “thrombocythemia” is preferred when the cause of a high platelet count isn’t known. The condition sometimes is called primary or essential thrombocythemia. Essential thrombocythemia (primary thrombocythemia) is a blood and bone marrow disease. This condition occurs if faulty cells in the bone marrow make too many platelets. Bone marrow is the sponge-like tissue inside the bones. It contains stem cells that develop into red blood cells, white blood cells, and platelets. What causes the bone marrow to make too many platelets often isn’t known.
With primary thrombocythemia (essential thrombocythemia), a high platelet count may occur alone or with other blood cell disorders. This condition isn’t common.
When another disease or condition (e.g., infection) causes a high platelet count, the term “thrombocytosis” is preferred. This condition often is called secondary or reactive thrombocytosis. Secondary thrombocytosis is more common than primary thrombocythemia.
Often, a high platelet count doesn’t cause signs or symptoms. Rarely, serious or life-threatening symptoms can develop, such as blood clots and bleeding. These symptoms are more likely to occur in people who have primary thrombocythemia.
People who have primary thrombocythemia with no signs or symptoms don’t need treatment, as long as the condition remains stable.
Other people who have this condition may need medicines or procedures to treat it. Most people who have primary thrombocythemia will live a normal lifespan.
Your doctor might detect thrombocytosis in a routine blood test result that shows a high platelet level. If your blood test indicates thrombocytosis, it’s important to determine whether it’s reactive thrombocytosis or essential thrombocythemia to know how to manage the condition.
Treatment and outlook for secondary thrombocytosis (reactive thrombocytosis) depend on its underlying cause.
Thrombocytosis causes
Bone marrow — spongy tissue inside your bones — contains stem cells that can become red blood cells, white blood cells or platelets. Platelets stick together, helping blood to form a clot that stops bleeding when you damage a blood vessel, such as when you cut yourself. Thrombocytosis occurs when your body produces too many platelets.
Reactive thrombocytosis or Secondary thrombocytosis
This is the more common type of thrombocytosis. Reactive thrombocytosis or secondary thrombocytosis occurs if another disease, condition, or outside factor causes the platelet count to rise. For example, 35 percent of people who have high platelet counts also have cancer—mostly lung, gastrointestinal, breast, ovarian, and lymphoma. Sometimes a high platelet count is the first sign of cancer.
Reactive thrombocytosis or secondary thrombocytosis is caused by an underlying medical problem, such as:
- Acute bleeding and blood loss
- Cancer
- Infections such as tuberculosis
- Iron deficiency or iron-deficiency anemia
- Removal of your spleen
- Hemolytic anemia — a type of anemia in which your body destroys red blood cells faster than it produces them, often due to certain blood diseases or autoimmune disorders
- Inflammatory disorders, such as connective tissue disorders, rheumatoid arthritis, sarcoidosis or inflammatory bowel disease
- Surgery or other type of trauma
- Reactions to medicine
Some conditions can lead to a high platelet count that lasts for only a short time. Examples of such conditions include:
- Recovery from serious blood loss
- Recovery from a very low platelet count caused by excessive alcohol use and lack of vitamin B12 or folate
- Acute (short-term) infection or inflammation
- Response to physical activity
Although the platelet count is high in secondary thrombocytosis, the platelets are normal (unlike in primary thrombocythemia). Thus, people who have secondary thrombocytosis have a lower risk of blood clots and bleeding.
Essential thrombocythemia
The cause of primary thrombocythemia is unclear but it often appears to be connected to mutations in a variety of genes. Your bone marrow produces too many of the cells that form platelets and these platelets are often abnormal. This poses a much higher risk of clotting or bleeding complications than does reactive thrombocytosis.
In primary thrombocythemia, faulty stem cells in the bone marrow make too many platelets. What causes this to happen usually isn’t known. When this process occurs without other blood cell disorders, it’s called essential thrombocythemia.
A rare form of thrombocythemia is inherited. (“Inherited” means the condition is passed from parents to children through the genes.) In some cases, a genetic mutation may cause the condition.
In addition to the bone marrow making too many platelets, the platelets also are abnormal in primary thrombocythemia. They may form blood clots or, surprisingly, cause bleeding when they don’t work well.
Bleeding also can occur because of a condition that develops called von Willebrand disease. This condition affects the blood clotting process.
After many years, scarring of the bone marrow can occur.
Risk factors for thrombocythemia and thrombocytosis
Primary thrombocythemia
Thrombocythemia isn’t common. The exact number of people who have the condition isn’t known. Some estimates suggest that 24 out of every 100,000 people have primary thrombocythemia.
Primary thrombocythemia is more common in people aged 50 to 70, but it can occur at any age. For unknown reasons, more women around the age of 30 have primary thrombocythemia than men of the same age.
Secondary Thrombocytosis
You might be at risk for secondary thrombocytosis if you have a disease, condition, or factor that can cause it. (For more information, go to “What Causes Thrombocythemia and Thrombocytosis?”)
Secondary thrombocytosis is more common than primary thrombocythemia. Studies have shown that most people who have platelet counts over 500,000 have secondary thrombocytosis.
Thrombocytosis prevention
You can’t prevent primary thrombocythemia. However, you can take steps to reduce your risk for complications. For example, you can control many of the risk factors for blood clots, such as high blood cholesterol, high blood pressure, diabetes, and smoking.
To reduce your risk, quit smoking, adopt healthy lifestyle habits, and work with your doctor to manage your risk factors.
It’s not always possible to prevent conditions that lead to secondary thrombocytosis. But, if you have routine medical care, your doctor may detect these conditions before you develop a high platelet count.
Thrombocytosis symptoms
People with thrombocytosis or thrombocythemia often don’t have signs or symptoms. These conditions might be discovered only after routine blood tests. Signs and symptoms of reactive thrombocytosis, if they do occur, relate to the underlying condition.
People who have primary thrombocythemia are more likely than those who have secondary thrombocytosis to have serious signs and symptoms.
The signs and symptoms of a high platelet count are linked to blood clots and bleeding. They include weakness, bleeding, headache, dizziness, chest pain, and tingling in the hands and feet.
People with essential thrombocythemia might have signs and symptoms related to blood clots and bleeding, including:
- Headache
- Dizziness or lightheadedness
- Chest pain
- Weakness
- Numbness or tingling of the hands and feet
Blood clots
In primary thrombocythemia, blood clots most often develop in the brain, hands, and feet. But they can develop anywhere in the body, including in the heart and intestines.
Blood clots in the brain may cause symptoms such as chronic (ongoing) headache and dizziness. In extreme cases, stroke may occur.
Blood clots in the tiny blood vessels of the hands and feet leave them numb and red. This may lead to an intense burning and throbbing pain felt mainly on the palms of the hands and the soles of the feet.
Other signs and symptoms of blood clots may include:
- Changes in speech or awareness, ranging from confusion to passing out
- Seizures
- Upper body discomfort in one or both arms, the back, neck, jaw, or abdomen
- Shortness of breath and nausea (feeling sick to your stomach)
In pregnant women, blood clots in the placenta can cause miscarriage or problems with fetal growth and development.
Women who have primary thrombocythemia or secondary thrombocytosis and take birth control pills are at increased risk for blood clots.
Blood clots are related to other conditions and factors as well. Older age, prior blood clots, diabetes, high blood pressure, and smoking also increase your risk for blood clots.
Bleeding
If bleeding occurs, it most often affects people who have platelet counts higher than 1 million platelets per microliter of blood. Signs of bleeding include nosebleeds, bruising, bleeding from the mouth or gums, or blood in the stools.
Although bleeding usually is associated with a low platelet count, it also can occur in people who have high platelet counts. Blood clots that develop in thrombocythemia or thrombocytosis may use up your body’s platelets. This means that not enough platelets are left in your bloodstream to seal off cuts or breaks on the blood vessel walls.
Another cause of bleeding in people who have very high platelets counts is a condition called von Willebrand Disease. This condition affects the blood clotting process.
In rare cases of primary thrombocythemia, the faulty bone marrow cells will cause a form of leukemia. Leukemia is a cancer of the blood cells.
Thrombocytosis diagnosis
Your doctor will diagnose thrombocythemia or thrombocytosis based on your medical history, a physical exam, and test results. A hematologist also may be involved in your care. This is a doctor who specializes in blood diseases and conditions.
During an exam for a routine physical or another condition, your doctor might find that your spleen is enlarged or you have signs or symptoms of an infection or another condition. In that case, your doctor might order a complete blood count. This test can determine whether your platelet count is higher than normal.
Because a number of conditions can cause a temporary rise in your platelet count, your doctor likely will repeat the blood test to see if your platelet count remains high over time.
Your doctor might also order tests to check for:
- Abnormal levels of iron in your blood
- Markers of inflammation
- Undiagnosed cancer
- Associated gene mutations
You might also need a procedure that uses a needle to remove a small sample of your bone marrow for testing.
Complete Blood Count
A complete blood count (CBC) measures the levels of red blood cells, white blood cells, and platelets in your blood. For this test, a small amount of blood is drawn from a blood vessel, usually in your arm.
If you have thrombocythemia or thrombocytosis, the CBC results will show that your platelet count is high.
Blood Smear
A blood smear is used to check the condition of your platelets. For this test, a small amount of blood is drawn from a blood vessel, usually in your arm. Some of your blood is put on a glass slide. A microscope is then used to look at your platelets.
Bone Marrow Tests
Bone marrow tests check whether your bone marrow is healthy. Blood cells, including platelets, are made in the bone marrow. The two bone marrow tests are aspiration and biopsy.
Bone marrow aspiration might be done to find out whether your bone marrow is making too many platelets. For this test, your doctor removes a sample of fluid bone marrow through a needle. He or she examines the sample under a microscope to check for faulty cells.
A bone marrow biopsy often is done right after an aspiration. For this test, your doctor removes a small amount of bone marrow tissue through a needle. He or she examines the tissue to check the number and types of cells in the bone marrow.
With thrombocythemia and thrombocytosis, the bone marrow has a higher than normal number of the very large cells that make platelets.
Other Tests
Your doctor may recommend other blood tests to look for genetic factors that can cause a high platelet count.
Thrombocytosis treatment
Reactive thrombocytosis
Secondary thrombocytosis is treated by addressing the condition that’s causing it.
- If you’ve had significant blood loss from a recent surgery or an injury, your elevated platelet count might resolve on its own.
- If you have a chronic infection or an inflammatory disease, your platelet count likely will remain high until the condition is under control. In most cases, your platelet count will return to normal after the cause is resolved.
- If you’ve had your spleen removed (splenectomy), you might have lifelong thrombocytosis, but you’re unlikely to need treatment.
People who have secondary thrombocytosis usually don’t need platelet-lowering medicines or procedures. This is because their platelets usually are normal (unlike in primary thrombocythemia).
Also, secondary thrombocytosis is less likely than primary thrombocythemia to cause serious problems related to blood clots and bleeding.
Essential thrombocythemia
People with this condition who have no signs or symptoms are unlikely to need treatment as long as the condition is stable. Your doctor might recommend that you take daily, low-dose aspirin to help thin your blood if you’re at risk of blood clots. Don’t take aspirin without checking with your doctor.
You might need to take drugs or have procedures to lower your platelet counts if you:
- Have a history of blood clots and bleeding
- Have risk factors for heart disease
- Are older than 60
- Have a platelet count greater than 1 million.
Your doctor might prescribe platelet-lowering drugs primarily in the form of hydroxyurea (Droxia, Hydrea) or interferon alfa (Intron A).
Hydroxyurea. This platelet-lowering medicine is used to treat cancers and other life-threatening diseases. Hydroxyurea most often is given under the care of doctors who specialize in cancer or blood diseases. Patients on hydroxyurea are closely monitored.
Currently, hydroxyurea plus aspirin is the standard treatment for people who have primary thrombocythemia and are at high risk for blood clots.
Anagrelide. This medicine also has been used to lower platelet counts in people who have thrombocythemia. However, research shows that when compared with hydroxyurea, anagrelide has worse outcomes. Anagrelide also has side effects, such as fluid retention, palpitations, arrhythmias, heart failure, and headaches.
Interferon alfa. This medicine lowers platelet counts, but 20 percent of patients can’t handle its side effects. Side effects include a flu-like feeling, decreased appetite, nausea (feeling sick to the stomach), diarrhea, seizures, irritability, and sleepiness. Doctors may prescribe this medicine to pregnant women who have primary thrombocythemia because it’s safer for a fetus than hydroxyurea and anagrelide.
Platelets can be removed from your blood by a procedure that’s similar to dialysis. A needle connected to a tube is placed in a vein and your blood is fed through a machine that filters out platelets. Then the filtered blood is returned to your body through an intravenous (IV) line. This procedure is used only in emergencies, such as if essential thrombocythemia has caused a stroke.
Living with thrombocythemia and thrombocytosis
If you have thrombocythemia or thrombocytosis:
- See your doctor for ongoing medical care.
- Control risk factors for blood clots—for example, quit smoking and work to manage risk factors such as high blood cholesterol, high blood pressure, and diabetes.
- Watch for signs and symptoms of blood clots and bleeding and report them to your doctor right away.
- Take all medicines as prescribed.
If you’re taking medicines to lower your platelet count, tell your doctor or dentist about them before any surgical or dental procedures. These medicines thin your blood and may increase bleeding during these procedures.
Medicines that thin the blood also may cause internal bleeding. Signs of internal bleeding include bruises, bloody or tarry-looking stools, pink or bloody urine, increased menstrual bleeding, bleeding gums, and nosebleeds. Contact your doctor right away if you have any of these signs.
Avoid over-the-counter pain medicines such as ibuprofen (except Tylenol®). These medicines may raise your risk of bleeding in the stomach or intestines and may limit the effect of aspirin. Be aware that cold and pain medicines and other over-the-counter products may contain ibuprofen.