What is umbilical hernia
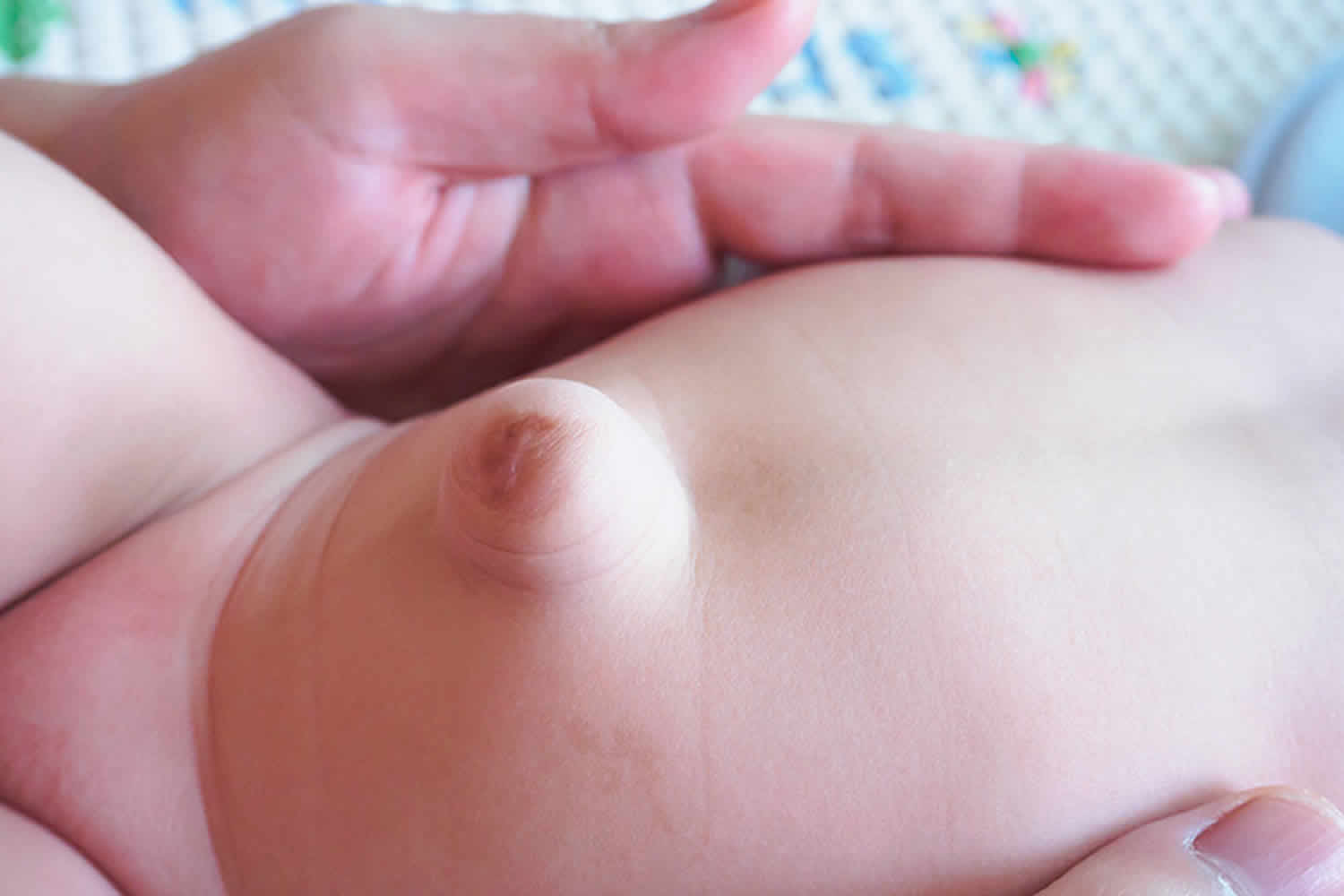
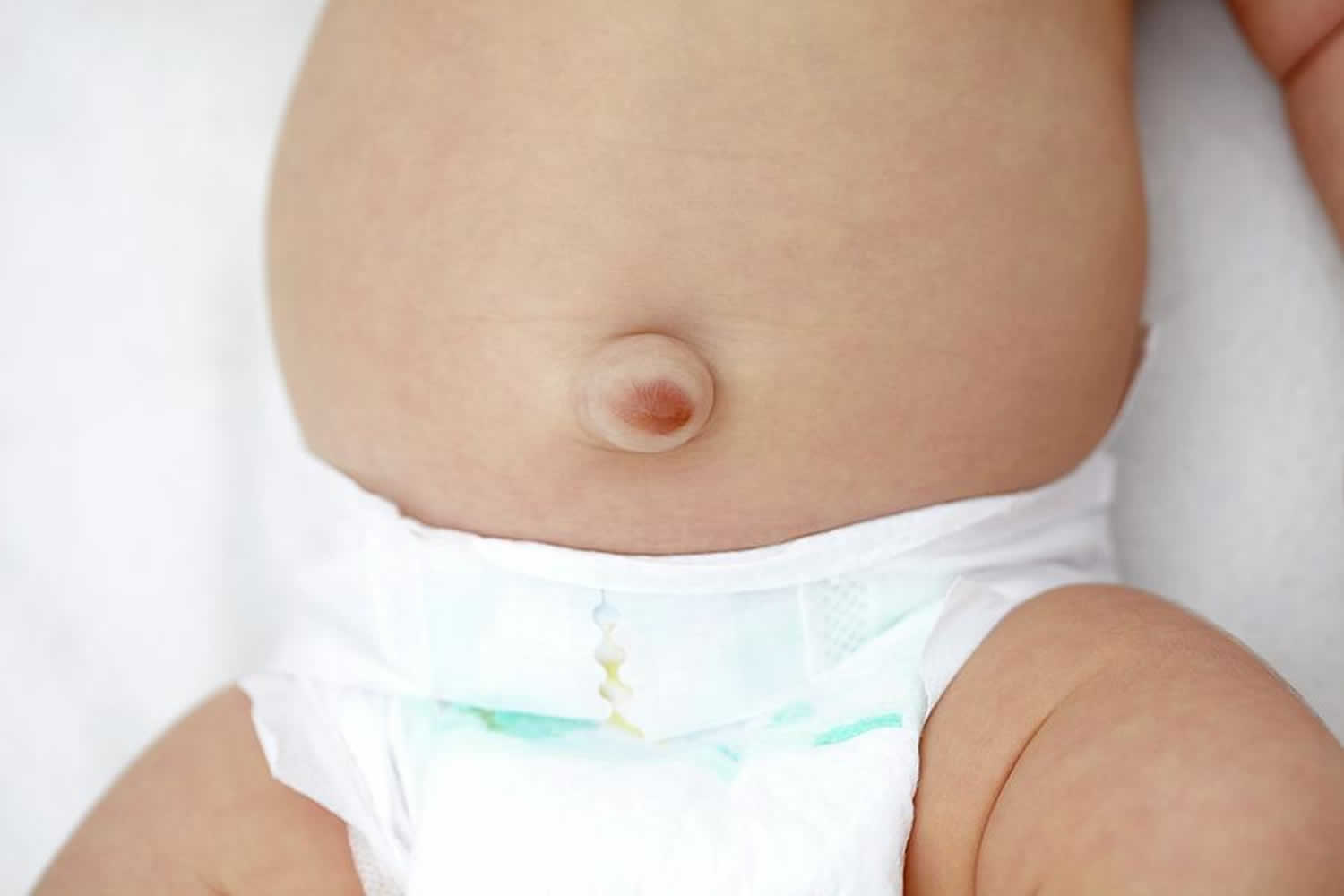
An umbilical hernia is a bulge or protrusion of your intestine that is seen or felt in the area of your belly button. An umbilical hernia is the result of a failure of the abdominal wall to completely close during fetal development, leaving an opening for a portion of the intestine and fluid to come through. Umbilical hernias are present at birth but may become more noticeable during times when your child is bearing down – crying, coughing, or straining to have a bowel movement. The umbilical hernia bulge may seem to disappear when the child is quiet or resting. Umbilical hernias are common and typically harmless. Umbilical hernias do not usually cause pain.
Umbilical hernias are most common in infants, but they can affect adults as well. In an infant, an umbilical hernia may be especially evident when the infant cries, causing the bellybutton to protrude. This is a classic sign of an umbilical hernia.
Umbilical hernias that appear during adulthood are more likely to need surgical repair. For adults, surgery is typically recommended to avoid possible complications, especially if the umbilical hernia gets bigger or becomes painful. During surgery, a small incision is made at the base of the bellybutton. The herniated tissue is returned to the abdominal cavity, and the opening in the abdominal wall is stitched closed. In adults, surgeons often use mesh to help strengthen the abdominal wall.
Most umbilical hernias (about 90 percent) close on their own by the time the child is 4-5 years old. Children’s umbilical hernias often close on their own in the first two years of life, though some remain open into the fifth year or longer. Therefore, your surgeon may recommend waiting until your child is 4-5 years old before undergoing a surgical repair. Waiting has benefits even if the umbilical hernia does not close on its own. Umbilical hernia generally gets smaller, which simplifies the repair procedure. Waiting also allows the muscle wall to thicken and mature, which makes the repair more robust.
In some cases, such as a large hernia or incarceration, surgical repair may be recommended prior to 4-5 years of age. Incarceration of the umbilical hernia occurs when the intestine gets trapped in the defect and is unable to go back into the abdomen. An incarcerated umbilical hernia will often cause a painful, firm, discolored bulge. If your child has signs of an incarcerated umbilical hernia, he or she should be brought to the Emergency Department for immediate evaluation by a medical professional to prevent any damage to the intestines.
It is estimated that umbilical hernias occur in 10-15 percent of all infants, with boys and girls affected equally. African Americans, low birth weight and premature infants are at a greater risk for having an umbilical hernia. How the umbilical cord is clamped or cut after birth has no effect on whether an umbilical hernia will develop or not develop.
Figure 1. Umbilical hernia baby
If you suspect that your baby has an umbilical hernia, talk with the baby’s pediatrician.
Seek medical care immediately if your child has any signs or symptoms of incarceration:
- An umbilical hernia that is stuck out and not able to be reduced (gently pushed back into the abdomen)
- A painful, firm, discolored bulge
- Begins to vomit
Similar guidelines apply to adults. Talk with your doctor if you have a bulge near your navel. Seek emergency care if the bulge becomes painful or tender. Prompt diagnosis and treatment can help prevent complications.
Umbilical hernia and pregnancy
Umbilical hernias are most common in women than men. Pregnancy may cause herniation or render a preexisting umbilical hernia apparent, because of progressively raised intra-abdominal pressure. The incidence of umbilical hernia among pregnancies is 0.08% 1.
Umbilical hernia symptoms present in the second trimester in most patients 1. An umbilical hernia may be diagnosed during first, second, or third pregnancies 2. The incidence of an umbilical hernia in pregnant women has been reported to be as low as 0.08% in a very recent large series involving 20,714 women 3. It is possible to meet complicated cases, like a full-term pregnancy in umbilical hernia 4, peritonitis due to skin ulceration 5, or incarcerated pregnant uterus within the hernia rims 6.
A surgical algorithm for a pregnant woman with a hernia is not clear to date, but newer and better scientific data has been cumulated 3. There is no consensus about the timing of surgery for an umbilical hernia in a woman who is already pregnant or planning a pregnancy 1. In fact, these two types of cases should be taken into consideration separately. Augustin and Majerovic 7 recommended that umbilical hernias that are symptomless or have minimal symptoms—including slight discomfort or pain—should be examined regularly and cured electively after delivery and uterine involution. Recently, it has been shown that watchful waiting, even up to 5 years, appears to be a safe strategy for ventral hernias in the adult population 8.
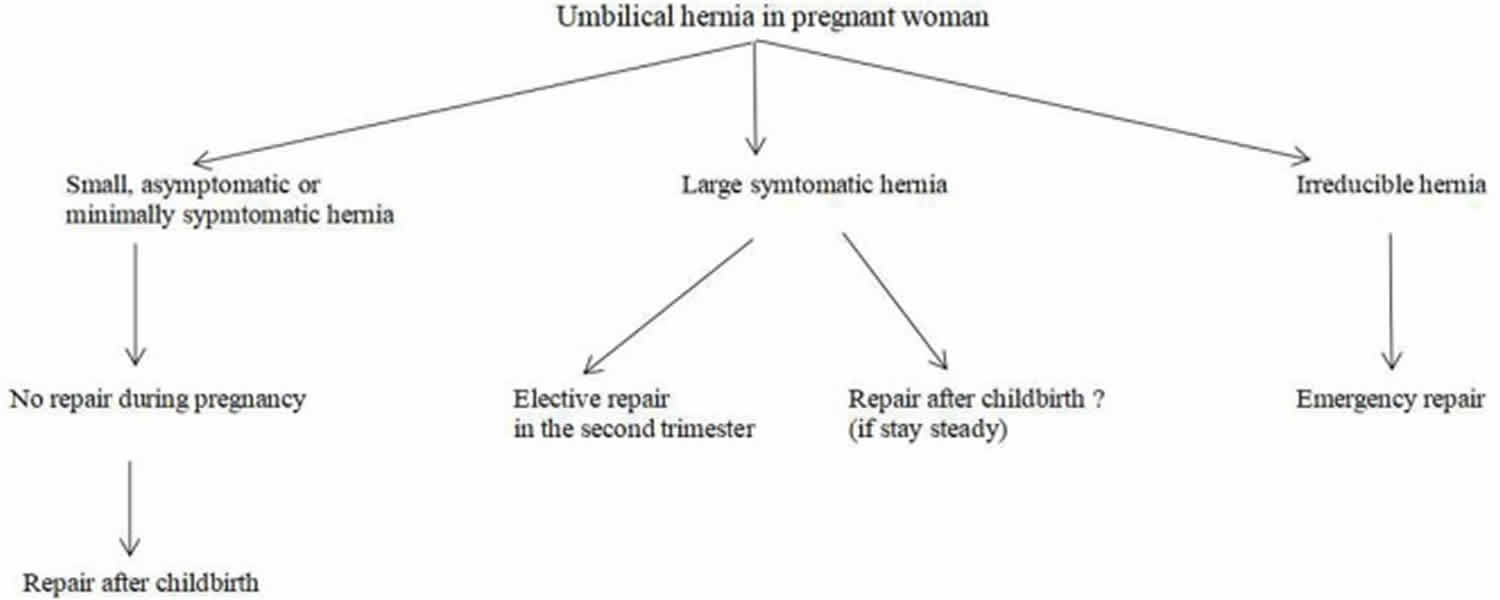
There is no consensus about the timing of surgery for an umbilical hernia in a woman who is already pregnant or planning a pregnancy. If the hernia is incarcerated or strangulated at the time of diagnosis, an emergency repair is inevitable. If the hernia is not complicated, but symptomatic, an elective repair should be proposed. If the hernia is repaired by suture, the risk of recurrence is high during pregnancy. Repair with a mesh may restrict the flexibility of the abdominal wall and may cause pain during a subsequent pregnancy. When the patient has a small and asymptomatic hernia, it may be better to postpone the repair until she gives birth.
Umbilical hernia repair during pregnancy can be performed with minimal morbidity to the mother and no fetal loss even in emergency cases. If a small hernia becomes larger and symptomatic, the second trimester is a proper period for surgery. Umbilical hernias can be repaired following childbirth or at the time of C-section. Patient satisfaction is high for combined C-section and hernia repair. However, a high recurrence rate is expected.
Elective repair after childbirth is well-documented. It is possible as early as the postpartum at 8 weeks. There is no need for surgery for small asymptomatic hernias in the early postpartum period. A 1-year interval can give the patient a very smooth convalescence, including hormonal stabilization and return to normal body weight. Surgery can be postponed for a longer time, even after another pregnancy, if the patient would like to have more children.
Table 1. Pros and cons for specific conditions in the relation of umbilical hernia and pregnancy.
| Suture repair | Mesh repair | ||
|---|---|---|---|
| Umbilical hernia in woman planning a new baby | High risk of recurrence | Pain in third trimester | Repair is postponed until birth for small and asymptomatic hernias |
| Umbilical hernia diagnosed during pregnancy | High risk of recurrence | Infection risk for pregnant woman especially in emergency repairs | Repair is postponed until birth for small and asymptomatic hernias |
| Cesarean section and simultaneous hernia repair | Easier | Requires separate incision | Patient satisfaction can be high |
| May be performed without separate incision | Lengthen operative time | Patient’s preference should be asked | |
| High risk of recurrence | Infection risk in puerperium | ||
| Hernia repair after childbirth | No exact recommendation for timing | No exact recommendation for timing | A 1-year interval may be recommended |
| Repair can be postponed for another pregnancy | |||
| Concomitant diastasis recti | High risk of recurrence | Recommended | Patient should be informed about diastasis |
Umbilical hernia in women planning for a pregnancy
In this situation, doctors have several concerns.
- Should your doctor repair the hernia before pregnancy?
- Which repair technique should be used?
- Can the repair remain intact during pregnancy?
- Can the repair cause pain and discomfort during pregnancy?
- How long should the interval between the hernia repair and the pregnancy or birth be?
- What complications can happen during pregnancy if we leave the hernia unrepaired?
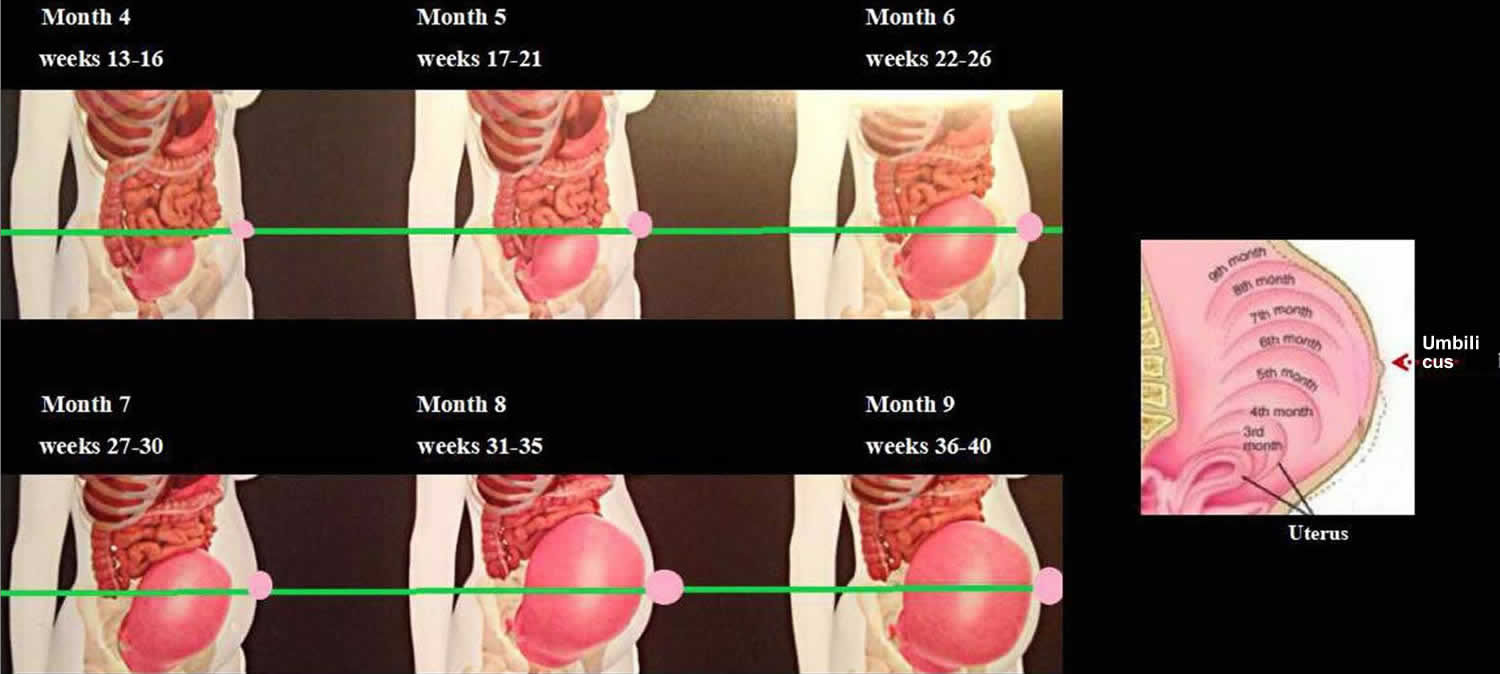
When the umbilical hernia is incarcerated or strangulated at the time of diagnosis, an emergency repair is inevitable. If the umbilical hernia is not complicated, but symptomatic, an elective repair should be proposed. A symptom may be pain or a large bulging. When the patient has a small and asymptomatic umbilical hernia, it may be better to postpone the repair until after she gives birth. Fortunately, most of the cases doctors encounter are in this group. During pregnancy, the enlarged uterus pushes the intestinal loops to superior and posterior parts of the abdominal cavity. The size and pushing force of the uterus during the first trimester does not seem enough to push the intestines into a small umbilical opening. The uterus reaches the level of the umbilicus at about the 20th–22nd week 9. Thereafter, no close contiguity between umbilical hernia defect and intestinal segments exist (Figure 2). If an incarceration occurs during this time, there is less concern about the surgical intervention, because an operation in the first or second trimester would not carry high risks for preterm labor or other adverse effects 10.
Figure 2. Umbilical hernia during pregnancy
Footnote: Changes in the size of the uterus and its relation to the umbilicus by the weeks of pregnancy.
[Source 1 ]A proper repair technique for an umbilical hernia in a woman planning a pregnancy is also a question. It has been shown that mesh repairs provide better outcomes than suture repairs 11. Repairing with only sutures may bring a recurrence during pregnancy 12. Lappen et al. 13 reported that pregnancy caused an increased risk of abdominal hernia recurrence. This information should be given to the patients who are planning an elective hernia repair before a subsequent gestation. As the uterus enlarges and intra-abdominal pressure rises, even mesh repairs will not make a pregnant woman immune to hernia recurrence. In concordance, Oma et al. 14 reported that pregnancy after umbilical hernia repair was independently associated with ventral hernia recurrence and mesh use could not lower the risk of recurrence. A repair with mesh may restrict the flexibility of the abdominal wall 15 and may cause pain during a subsequent pregnancy 16.
Unfortunately, there is no substantial evidence about the adequate interval between hernia repair and pregnancy or birth. Surgeons usually advise their patients that a pregnancy is not allowed until after the first year of the surgical repair. However, no clinical or experimental studies exist on this specific case. There is no consensus on if this 1-year interval ends at the beginning of the pregnancy or at the time of birth. It can only be said that an early pregnancy may cause recurrence.
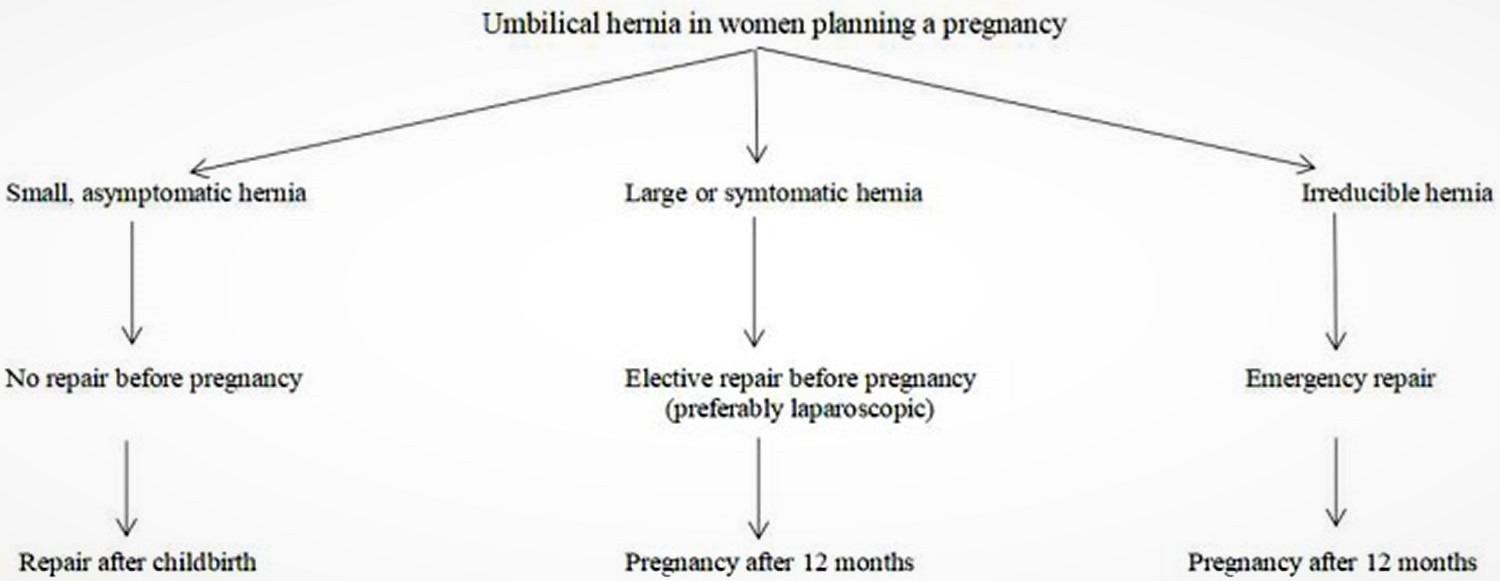
Every hernia carries a risk of incarceration and strangulation. Therefore, patients with an umbilical hernia and planning a gestation should be instructed about this risk. No one can predict which hernias will become complicated or when this will occur. However, every surgeon can tell his or her patient what the malicious effects of an incarcerated or strangulated hernia are on the mother and the baby. An emergency repair, especially during the first or third trimester, will bring the burden of anesthesia and surgical trauma. It should be recommended that patients with large hernias, including intestinal loops, umbilical hernias with a suspicious history of incarceration, and recurrent umbilical hernias previously repaired with a mesh undergo a definitive repair before planning a pregnancy (Figure 3).
Figure 3. Surgical strategy for umbilical hernia in women planning a pregnancy
[Source 1 ]Umbilical hernia found during pregnancy
Again, there is no solid recommendation for this type of case. Unfortunately, no randomized controlled trial or prospective analysis about hernia repairs in pregnancy existed in the literature 5. However, a small asymptomatic or minimally symptomatic umbilical hernia diagnosed in the early stage of a pregnancy can be managed like a hernia in women planning to become pregnant (Figure 4). Symptomatic umbilical hernias can emerge in every trimester of pregnancy, and they may get incarcerated or strangulated during pregnancy, although the exact rates of these complications have never been reported. Haskins et al. 16 reviewed the American College of Surgeons National Surgical Quality Improvement Program and found that 126 pregnant women were operated on for umbilical hernia repair in a 10-year period. Ninety-five percent of the repairs performed with open technique. Incarceration or strangulation existed in half of the cases. Surgery was achieved with minimal 30-day morbidity for the mother and no fetal loss, even in cases of emergencies. Buch diagnosed five female patients with umbilical hernias occurring during pregnancy at the Mount Sinai Medical Center from September 2004 to July 2006 2. All patients presented with symptoms in the second trimester with reducible hernias. None of them developed incarceration until an open repair following delivery. This finding supports watchful waiting approach during pregnancy 2.
Thirty-one papers, including twenty-three case reports, were found in a recent literature search by Jensen et al. 12. Apart from the above cases mentioned by Haskins 17 and Buch 2, seven patients with an umbilical hernia underwent emergency repair during pregnancy. Suture repair was used in all cases, but one. Wai et al. 18 from Yale University, reported the unique case, describing an intraperitoneal mesh repair for an irreducible umbilical hernia in a woman in the second trimester. In Jensen et al.’s 12 literature review, no postoperative complications were recorded. This included Ahmed’s emergency repair case 19 with spontaneous rupture in a young, multiparous woman in 28th week of pregnancy. In that case, there was skin ulceration due to pressure, and the uterus was completely in the hernia sac with gangrenous intestinal loops of approximately 75 cm. The hernia defect was closed with a suture and the patient gave birth uneventfully 6 weeks later 19.
Oma et al. 3 published the most recent series. In this series, 17 pregnant women with an umbilical hernia were recorded within 20,714 pregnancies in a single institution. There were five pregnant patients with an umbilical hernia. Two women noticed the hernia during previous pregnancies, one patient in the present gestation, and the other two at 5th week of pregnancy. All patients completed their pregnancies with no hernia complication.
Figure 4. Surgical strategy for an umbilical hernia found during pregnancy
[Source 1 ]Cesarean Section and simultaneous hernia repair
Hernia repair during C-section is a common surgical approach. However, these simultaneous surgeries were not well-documented until the 2000s. In 2004, Ochsenbein-Kölble et al. 20 reported the first case series of C-sections and simultaneous inguinal or umbilical hernia repairs. Three patients were offered and underwent combined surgery with their informed consent. In one of them, the sign for C-section was the presence of the umbilical hernia itself. The duration of surgery was longer in cases with inguinal hernia repair, but not umbilical hernia repair versus C-section alone. However, Ghnnam et al. 21 reported that the simultaneous umbilical hernia repair and cesarean needed more time than only a cesarean. They compared 48 patients, who underwent cesarean delivery along with paraumbilical hernia repair versus 100 patients undergoing a C-section. Inpatient periods were similar. Only two patients complained of pain at the umbilicus. The control group needed significantly fewer analgesics. Combined surgery was preferred by all patients. One hernia recurred (2.8%), following suture repair within 2 years 21. Mesh repairs were free of recurrence.
Gabriele et al. 22 reported on 28 pregnant women with an inguinal or an umbilical hernia. These patients who underwent simultaneous C-section and hernia repair were compared with 100 patients who only underwent a C-section. Combined surgeries took more time for both an umbilical and inguinal hernia than C-section alone. Surgeries were uneventful, and no recurrence developed. The authors concluded that combined surgery is safe and avoids readmissions. Also, Jensen et al. 12 came to a solid conclusion after their literature search that combined hernia repair and C-section is the optimal therapeutic option.
Steinemann et al. 23 recently published a retrospective cohort–control study. Fourteen patients underwent suture repair of umbilical hernia during C-section by using different techniques. External umbilical hernia repair with suture was used in seven cases via a paraumbilical semilunar skin incision after the closure of the Pfannenstiel incision. Internal umbilical hernia repair with suture was used in the other seven patients. Internal suturing required less time than external suturing. Both approaches lengthen the time in operation compared to the control group. Unfortunately, two recurrences were revealed by ultrasonography in each repair subgroup (28%). The authors recommended mesh repairs in these cases 23.
Interestingly, no patient underwent combined surgery in Haskins et al.’s most recent review 17. However, the reason for the absence of any case with simultaneous C-section and hernia repair are not explained in the paper.
Hernia repair after childbirth following an interval
Some pregnant women with an umbilical hernia do not undergo simultaneous hernia repair at the time of C-section. The reason for that may be a patient’s or surgeon’s choice.
Oma et al. 3 followed eight women with an umbilical hernia and no surgical intervention throughout their pregnancy. The umbilical hernia persisted in all these patients who had a clinical re-evaluation postpartum and no spontaneous disappearance of the hernia was recorded. Elective umbilical hernia repairs were done in five patients within 5 months to 3 years after delivery 3.
Buch et al. 2 reported five cases that underwent hernia repair in the postpartum period. The patients underwent surgery at postpartum for 8–52 weeks. No complications or recurrence were recorded in postoperative follow-up for 2–34 weeks. Two out of five women conceived again after hernia repair. The authors concluded that pregnant patients presenting with reducible groin or umbilical hernias during pregnancy can safely be managed non-operatively during their pregnancy and undergo surgical repair in the postpartum period 2.
Combined surgery may not increase the risk of local and systemic complication 20, however, there are still other concerns about simultaneous surgery. Apart from maternal and fetal health, there are issues regarding the quality and durability of the hernia repair. What would be the advantages of surgical repair in the postpartum period rather than during C-section? In other words, could a concomitant repair during C-section be less reliable?
Changes in Muscles and Fascial Structures during Pregnancy
The gross structure of rectus abdominis muscle is altered during pregnancy. Significant increases happen in muscle length, separation, and angles of insertions as the pregnancy progressed 24. The functional ability of the abdominal muscles is also altered, and the ability to stabilize the pelvis is decreased. For all abdominal exercises, upper rectus abdominis relative integrated electromyography (EMG) increased while external oblique and lower rectus abdominis relative integrated EMG decreased. Relative EMG for all tested muscles returned to levels seen at 18 weeks and 26 gestations by 18 weeks post-birth. Functional changes found in the rectus abdominis and external and internal obliques. During the immediate post-birth period, separation of the rectus abdominis was resolved by 4 weeks post-birth and abdominal muscle inter-relationships returned to early pregnancy levels by 8 weeks post-birth. However, the ability to stabilize the pelvis remained low at 8 weeks post-birth. This sustained decrement in the ability to stabilize the pelvis at 8 weeks post-birth may reflect the poor resolution of abdominal muscle length increases due to pregnancy 24.
In fact, the meaning of the alterations in abdominal muscle groups for the fate of an umbilical hernia repair is obscure. Whether the changes increase or decrease, hernia recurrence rates is unknown to surgeons. However, the abdominal muscles during pregnancy differ from usual. It may be better to wait for a while to let the muscles return to their normal anatomy and function before repairing the umbilical hernia. However, there is no recommendation in the literature for the exact time to wait for a repair.
Another issue that may affect the fate of hernia repair in a pregnant or early postpartum woman is hormonal changes during gestation. Relaxin is a peptide hormone in the insulin family, secreted by the corpus luteum 25. It is also released from the placenta during pregnancy. It relaxes pelvic ligaments and softens and widens the cervix. Relaxin reduces extracellular matrix (ECM) synthesis and induces collagen degradation 26. In a study on rats, relaxin caused a significant reduction in tissue collagen content 27. Relaxin limited collagen production, while stimulating increased collagen degradation 28. Also, Naqvi et al. 29 documented relaxin’s degradative effects on joint fibrocartilaginous tissue with matrix degradation by metalloproteinases (MMPs).
Collagen, extracellular matrix, and metalloproteinases have important implications for hernia formation. Collagen is the most abundant extracellular matrix protein. Collagenase, a member of the metalloproteinase family, is the principal enzyme in collagen degradation 30.
Considering the studies on the relationship between collagen, extracellular matrix, and metalloproteinases, we can think any endogenous or exogenous substance that affects these mechanisms may cause recurrence after hernia repair, especially following suture repairs. Therefore, we can say there may be a risk of recurrence when the repair is done and the relaxin level is high. Although there is no evidence for this supposition, there are interesting reports in the literature. It has been reported that a higher expression of relaxin receptors within the muscles of the pelvic diaphragm in dogs with a perineal hernia. This may suggest that relaxin plays a role in the pathogenesis of this type of hernia by causing muscular atrophy 31. Relaxin may also be a factor in perineal hernia formation with connective tissue degeneration in dogs 32. In human beings, there is only one report on the relation between relaxin and abdominal hernias 33. In this study, all the children born in Malmö, Sweden in a 5-year period were checked for congenital dislocation of the hip (CDH) and for an inguinal hernia. Hernia was diagnosed five times more frequently in girls with congenital dislocation of the hip than girls without, and three times in boys with congenital dislocation of the hip than boys without. The authors stated that relaxin could stimulate collagenase, induce structural changes in the connective tissue, and cause development of both congenital dislocation of the hip and the hernia 33. This paper was published in 1988 and no further data on the subject has been collected since.
Would lifting and carrying baby create a Burden on the umbilical hernia repair?
Surgeons generally put patients on a weight lifting restriction after hernia repairs. Even mesh repairs are vulnerable to rises in intra-abdominal pressure in the early postoperative period. Biomechanical studies have revealed that the tensile strength provided by tissue ingrowth into the mesh reaches approximately 80% after only 6 weeks 34. Although there is no consensus on weight lifting restriction after hernia repairs, surgeons do not want their patients to lift any weight for the first 2 weeks. Moderate lifting (<10 kg) is allowed after 2–4 weeks. Patients are advised to lift over 10 kg only after 8 weeks 35. In fact, carrying and lifting a baby would stay within the limits of the advice. However, a woman who does not have a baby and undergoes umbilical hernia repair would be on a weightlifting restriction for a much longer time.
Although umbilical hernia repair can be performed after childbirth, there is no need for surgery on small asymptomatic hernias in the early postpartum period. A 1-year interval can give the patient a very smooth convalescence, including hormonal stabilization and return to normal body weight. Surgery can be postponed for a longer time, even after another pregnancy, if the patient would like to have more children.
Significance of the concomitant diastasis recti
During pregnancy, the growing uterus stretches the muscles in the abdomen. This can cause the two large parallel bands of muscles that meet in the middle of the abdomen (rectus muscles) to become separated by an abnormal distance — a condition called diastasis recti or diastasis recti abdominis. Diastasis recti is an impairment, but not a true hernia, and does not carry a risk for incarceration.
Diastasis recti might cause a bulge in the middle of the abdomen where the two muscles separate. The condition might be noticeable only when the abdominal muscles are tense, such as when you move from lying down to sitting up. Diastasis recti can weaken the abdominal muscles, causing lower back pain and making it difficult to lift objects or do other routine daily activities.
You might be more likely to develop diastasis recti as a result of pregnancy if you have carried multiples 36 or a large baby to term and are of small stature and fit or are age 35 or older.
The prevalence of diastasis recti during pregnancy is about 30–70%. The normal width of the linea alba is 15 mm at the level of xiphoid, 22 mm at the level of 3 cm cranial to the umbilicus, and 16 mm at the level of 3 cm caudal to the umbilicus in nulliparous women 37. Mechanical forces and hormonal changes during pregnancy may play a role in the etiology.
The most frequent localization is in the periumbilical region and persistence postpartum is found in about 60% of cases 38. Liaw et al. 39 reported that diastasis may persist in the postpartum period and the abdominal muscle function improved, but did not return to normal, even after 6 months. Sperstad et al. 40 followed 300 first-time pregnant women from pregnancy until 12 months postpartum. They reported that diastasis recti existed in 33.1, 60.0, 45.4, and 32.6% of the women at 21 weeks of pregnancy, and at 6 weeks, 6 months, and 12 months following delivery, respectively. This study revealed that the risk for diastasis recti was twofold higher in women reporting heavy lifting 20 times a week or more than in women reporting less weight lifting. The authors did not describe the heavy lifting in the text, but we can assume that a postpartum woman lifts her baby many times a week. The weight of a baby is about 8 kg at 6 months and 10 kg at 12 months 41. These weights are enough to raise intra-abdominal pressure as high as a Valsalva maneuver does 35.
Although diastasis recti is not a hernia, it may cause recurrence as a larger hernia following umbilical hernia repairs. In umbilical hernia repairs with sutures, the bites pass through a weak rectus sheet at the region of diastasis. This may cause tears and create button hole defects, consequently resulting in recurrence. Köhler et al. 42 evaluated 231 suture repairs for small primary umbilical or epigastric hernias. Hernia defects were smaller than 2 cm. Patients with rectus diastasis developed hernia recurrence at a significantly increased rate. The authors hypothesized that thin and stretched rectus sheath is a risk factor for recurrence. They recommended mesh repair for umbilical hernia patients with rectus diastasis. Although Emanuelsson et al.’s 43 recent prospective randomized study showed that two-row suture plication with delayed absorbable material provided similarly good results with retromuscular lightweight polypropylene mesh without an increase in recurrence rate in treatment of diastasis recti, mesh use remains a better option for patients with concomitant umbilical hernia and diastasis recti 42. In addition, one can assume that a recurrence still may develop from the sites of mesh fixation if there is a vulnerable linea alba due to diastasis recti. Therefore, it is better to use no fixation in case of strong restoration of the line alba or to use an autraumatic mesh fixation like glues (e.g., fibrin) 44 or a self-gripping mesh in retromuscular mesh repairs 45.
Umbilical hernia causes
During gestation, the umbilical cord passes through a small opening in the baby’s abdominal muscles. The opening normally closes just after birth. If the muscles don’t join together completely in the midline of the abdominal wall, an umbilical hernia may appear at birth or later in life.
Umbilical hernias in adults are usually acquired and are more common in women or patients with increased intra-abdominal pressure as in pregnancy, obesity, ascites, or chronic abdominal distention 46. This is due to the presence of a single midline aponeurotic decussation as compared to the normal decussation of fibers from all three lateral abdominal muscles.
In adults, too much abdominal pressure contributes to umbilical hernias. Causes of increased pressure in the abdomen include:
- Obesity
- Multiple pregnancies
- Fluid in the abdominal cavity (ascites)
- Previous abdominal surgery
- Long-term peritoneal dialysis to treat kidney failure
The incidence of umbilical hernias ranges from 10% to 25% and is increased in females; specifically African American children and low-birth-weight babies 46. Umbilical hernias also are associated with several congenital syndromes and medical conditions such as hypothyroidism, mucopolysaccharidosis, Down syndrome, Beckwith–Wiedemann syndrome, and exomphalos–macroglossia syndrome 47.
Risk factors for umbilical hernia
Umbilical hernias are most common in infants — especially premature babies and those with low birth weights. In the United States, African American infants appear to have a slightly increased risk of umbilical hernias. The condition affects boys and girls equally.
For adults, being overweight or having multiple pregnancies may increase the risk of developing an umbilical hernia. This type of hernia tends to be more common in women.
Umbilical hernia symptoms
An umbilical hernia creates a soft swelling or bulge near the navel (umbilicus). In babies who have an umbilical hernia, the bulge may be visible only when they cry, cough or strain.
Umbilical hernias in children are usually painless. Umbilical hernias that appear during adulthood may cause abdominal discomfort.
Umbilical hernia complications
For children, complications of an umbilical hernia are rare. Complications can occur when the protruding abdominal tissue becomes trapped (incarcerated) and can no longer be pushed back into the abdominal cavity. This reduces the blood supply to the section of trapped intestine and can lead to umbilical pain and tissue damage. If the trapped portion of intestine is completely cut off from the blood supply (strangulated hernia), tissue death (gangrene) may occur. Infection may spread throughout the abdominal cavity, causing a life-threatening situation.
Adults with umbilical hernias are somewhat more likely to experience incarceration or obstruction of the intestines. Emergency surgery is typically required to treat these complications.
Umbilical hernia diagnosis
The diagnosis of an umbilical hernia is confirmed by a thorough health history and physical examination. Imaging studies are almost never needed to diagnose umbilical hernias. However, imaging studies — such as an abdominal ultrasound or a CT scan — are used to screen for complications.
Umbilical hernia treatment
Most umbilical hernias in babies close on their own by age 1 or 2. Your doctor may even be able to push the bulge back into the abdomen during a physical exam. Don’t try this on your own, however. Although some people claim a hernia can be fixed by taping a coin down over the bulge, this “fix” doesn’t help and germs may accumulate under the tape, causing infection.
If your child’s umbilical hernia does not close on its own by the time he or she is 4-5 years old, your doctor will recommend a surgical procedure to repair the hernia.
For children, surgery is typically reserved for umbilical hernias that:
- Are painful
- Are slightly larger than 1/2 inch (1 to 2 centimeters) in diameter
- Are large and don’t decrease in size over the first two years of life
- Don’t disappear by age 4 or 5
- Become trapped or block the intestine
Umbilical hernia surgery
The surgery to repair an umbilical hernia is a day surgery, meaning your child will go home the same day as the procedure. The procedure will be done under general anesthesia.
A small curved incision (resembling a smile) will be made under your child’s belly button. The opening will be closed, usually with absorbable sutures, and the overlying skin will be closed with a combination of absorbable stitches below the skin and dermabond. If dermabond is not used, your child may have a dressing over the site, which should be removed 48 hours after surgery.
Dermabond is a sterile, liquid adhesive that will hold the edges of your child’s wound together and act as a waterproof dressing. It usually stays in place for 5-10 days before it starts to fall off. You should not pick, peel or rub the dermabond, as this could cause your child’s wound to open before it is healed.
Once it sets, the adhesive can get wet (as in a shower) the same day as the procedure, but should not routinely be submerged under water (as in swimming) for 5-10 days. Do not apply any ointments such as Vaseline or Neosporin to the incision while the dermabond is in place.
In adults, small defects are closed primarily after separation of the sac from the overlying umbilicus and surrounding fascia. Defects greater than 3 cm are closed using prosthetic mesh. Currently, no prospective data have conclusively found clear advantages of one technique over another.
Options for mesh implantation include bridging the defect and placing a preperitoneal underlay of mesh reinforced with suture repair. The laparoscopic technique requires general anesthesia and is reserved for large defects or recurrent umbilical hernias 48.
Complications related to surgery:
- Hematoma
- Seroma
- Bowel injury
- Recurrence of hernia
- Wound infection
Umbilical hernia surgery recovery
After surgery, your child’s belly button may appear to be slightly swollen, but this will go away over the next few weeks. Your child will not be able to participate in physical education or sports for 2-3 weeks after surgery. Your doctor will schedule your child for a follow-up appointment 2-4 weeks after the procedure, at which time we will evaluate the repair and your child’s recovery.
Even after repair, there is a very small risk of recurrence of the hernia. If it appears that your child’s hernia has come back at any point, please make an appointment with your doctor to be evaluated.
References- Kulacoglu H. Umbilical Hernia Repair and Pregnancy: Before, during, after…. Front Surg. 2018;5:1. Published 2018 Jan 29. doi:10.3389/fsurg.2018.00001 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5796887
- Buch KE, Tabrizian P, Divino CM. Management of hernias in pregnancy. J Am Coll Surg (2008) 207(4):539–42.10.1016/j.jamcollsurg.2008.04.030
- Oma E, Bay-Nielsen M, Jensen KK, Jorgensen LN, Pinborg A, Bisgaard T. Primary ventral or groin hernia in pregnancy: a cohort study of 20,714 women. Hernia (2017) 21(3):335–9.10.1007/s10029-017-1618-7
- Punguyire D, Iserson KV, Apanga S. Full-term pregnancy in umbilical hernia. Pan Afr Med J (2011) 8:6.10.11604/pamj.2011.8.6.465
- Wydell SH. Umbilical hernia in pregnancy. Br Med J (1963) 1(5342):1413–4.10.1136/bmj.1.5342.1413-a
- Shaw WG, Nichols EE. Abdominal pregnancy incarcerated into an umbilical hernia. Case report. Am J Obstet Gynecol (1962) 1(84):72–5.10.1016/0002-9378(62)90675-0
- Augustin G, Majerovic M. Non-obstetrical acute abdomen during pregnancy. Eur J Obstet Gynecol Reprod Biol (2007) 131(1):4–12.10.1016/j.ejogrb.2006.07.052
- Kokotovic D, Sjølander H, Gögenur I, Helgstrand F. Watchful waiting as a treatment strategy for patients with a ventral hernia appears to be safe. Hernia (2016) 20(2):281–7.10.1007/s10029-016-1464-z
- Lowdermilk DL. Anatomy and physiology of pregnancy. 11th ed In: Lowdermilk DL, Perry SE, Cashion MC, Alden KR, editors. , editors. Maternity and Women’s Health Care – E-Book. St. Louis: Elsevier; (2004). p. 283–300.
- Visser BC, Glasgow RE, Mulvihill KK, Mulvihill SJ. Safety and timing of nonobstetric abdominal surgery in pregnancy. Dig Surg (2001) 18(5):409–17.10.1159/000050183
- Kulacoglu H. Current options in umbilical hernia repair in adult patients. Ulus Cerrahi Derg (2015) 31(3):157–61.10.5152/UCD.2015.2955
- Jensen KK, Henriksen NA, Jorgensen LN. Abdominal wall hernia and pregnancy: a systematic review. Hernia (2015) 19(5):689–96.10.1007/s10029-015-1373-6
- Lappen JR, Sheyn D, Hackney DN. Does pregnancy increase the risk of abdominal hernia recurrence after prepregnancy surgical repair? Am J Obstet Gynecol (2016) 215(3):390.e1–5.10.1016/j.ajog.2016.05.003
- Oma E, Jensen KK, Jorgensen LN. Recurrent umbilical or epigastric hernia during and after pregnancy: a nationwide cohort study. Surgery (2016) 159(6):1677–83.10.1016/j.surg.2015.12.025
- Junge K, Klinge U, Prescher A, Giboni P, Niewiera M, Schumpelick V. Elasticity of the anterior abdominal wall and impact for reparation of incisional hernias using mesh implants. Hernia (2001) 5(3):113–8.10.1007/s100290100019
- Schoenmaeckers E, Stirler V, Raymakers J, Rakic S. Pregnancy following laparoscopic mesh repair of ventral abdominal wall hernia. JSLS (2012) 16(1):85–8.10.4293/108680812X13291597716104
- Haskins IN, Rosen MJ, Prabhu AS, Amdur RL, Rosenblatt S, Brody F, et al. Umbilical hernia repair in pregnant patients: review of the American College of Surgeons National Surgical Quality Improvement Program. Hernia (2017) 21(5):767–70.10.1007/s10029-017-1633-8
- Wai PY, Ruby JA, Davis KA, Roberts AC, Roberts KE. Laparoscopic ventral hernia repair during pregnancy. Hernia (2009) 13(5):559–63.10.1007/s10029-009-0476-3
- Ahmed A, Stephen G, Ukwenya Y. Spontaneous rupture of umbilical hernia in pregnancy: a case report. Oman Med J (2011) 26(4):285–7.10.5001/omj.2011.70
- Ochsenbein-Kölble N, Demartines N, Ochsenbein-Imhof N, Zimmermann R. Cesarean section and simultaneous hernia repair. Arch Surg (2004) 139(8):893–5.10.1001/archsurg.139.8.893
- Ghnnam WM, Helal AS, Fawzy M, Ragab A, Shalaby H, Elrefaay E. Paraumbilical hernia repair during cesarean delivery. Ann Saudi Med (2009) 29(2):115–8.10.4103/0256-4947.51798
- Gabriele R, Conte M, Izzo L, Basso L. Cesarean section and hernia repair: simultaneous approach. J Obstet Gynaecol Res (2010) 36(5):944–9.10.1111/j.1447-0756.2010.01283.x
- Steinemann DC, Limani P, Ochsenbein N, Krähenmann F, Clavien PA, Zimmermann R, et al. Suture repair of umbilical hernia during caesarean section: a case-control study. Hernia (2013) 17(4):521–6.10.1007/s10029-013-1087-6
- Gilleard WL. The Structure and Function of the Abdominal Muscles during Pregnancy and the Immediate Post-Birth Period. Master thesis, Wollongong, Australia: University of Wollongong; (1992).
- Bani D. Relaxin: a pleiotropic hormone. Gen Pharmacol (1997) 28(1):13–22.10.1016/S0306-3623(96)00171-1
- Samuel CS, Lekgabe ED, Mookerjee I. The effects of relaxin on extracellular matrix remodeling in health and fibrotic disease. Adv Exp Med Biol (2007) 612:88–103.10.1007/978-0-387-74672-2_7
- Samuel CS, Coghlan JP, Bateman JF. Effects of relaxin, pregnancy and parturition on collagen metabolism in the rat pubic symphysis. J Endocrinol (1998) 159(1):117–25.10.1677/joe.0.1590117
- Samuel CS. Relaxin: antifibrotic properties and effects in models of disease. Clin Med Res (2005) 3(4):241–9.10.3121/cmr.3.4.241
- Naqvi T, Duong TT, Hashem G, Shiga M, Zhang Q, Kapila S. Relaxin’s induction of metalloproteinases is associated with the loss of collagen and glycosaminoglycans in synovial joint fibrocartilaginous explants. Arthritis Res Ther (2005) 7(1):R1–11.10.1186/ar1451
- Donahue TR, Hiatt JR, Busuttil RW. Collagenase and surgical disease. Hernia (2006) 10(6):478–85.10.1007/s10029-006-0146-7
- Merchav R, Feuermann Y, Shamay A, Ranen E, Stein U, Johnston DE, et al. Expression of relaxin receptor LRG7, canine relaxin, and relaxin-like factor in the pelvic diaphragm musculature of dogs with and without perineal hernia. Vet Surg (2005) 34(5):476–81.10.1111/j.1532-950X.2005.00072.x
- Niebauer GW, Shibly S, Seltenhammer M, Pirker A, Brandt S. Relaxin of prostatic origin might be linked to perineal hernia formation in dogs. Ann N Y Acad Sci (2005) 1041:415–22.10.1196/annals.1282.062
- Udén A, Lindhagen T. Inguinal hernia in patients with congenital dislocation of the hip. A sign of general connective tissue disorder. Acta Orthop Scand (1988) 59(6):667–8.10.3109/17453678809149421
- Majercik S, Tsikitis V, Iannitti DA. Strength of tissue attachment to mesh after ventral hernia repair with synthetic composite mesh in a porcine model. Surg Endosc (2006) 20:1671–4.10.1007/s00464-005-0660-1
- Forbes J, Fry N, Hwang H, Karimuddin AA. Timing of return to work after hernia repair: recommendations based on a literature review. B C Med J (2012) 54(7):341–5.
- Turan V, Colluoglu C, Turkyilmaz E, Korucuoglu U. Prevalence of diastasis recti abdominis in the population of young multiparous adults in Turkey. Ginekol Pol (2011) 82(11):817–21
- Beer GM, Schuster A, Seifert B, Manestar M, Mihic-Probst D, Weber SA. The normal width of the linea alba in nulliparous women. Clin Anat (2009) 22(6):706–11.10.1002/ca.20836
- Kimmich N, Haslinger C, Kreft M, Zimmermann R. [Diastasis recti abdominis and pregnancy]. Praxis (Bern 1994) (2015) 104(15):803–6.10.1024/1661-8157/a002075
- Liaw LJ, Hsu MJ, Liao CF, Liu MF, Hsu AT. The relationships between inter-recti distance measured by ultrasound imaging and abdominal muscle functionin postpartum women: a 6-month follow-up study. J Orthop Sports Phys Ther (2011) 41(6):435–43.10.2519/jospt.2011.3507
- Sperstad JB, Tennfjord MK, Hilde G, Ellström-Engh M, Bø K. Diastasis recti abdominis during pregnancy and 12 months after childbirth: prevalence, risk factors and report of lumbopelvic pain. Br J Sports Med (2016) 50(17):1092–6.10.1136/bjsports-2016-096065
- World Health Organization, Department of Nutrition for Health and Development. WHO Child Growth Standards 1 Year 2 Years 3 Years 4 Years 5 Years Length/Height for Age, Weight for Age, Weight for Length, Weight for Height and Body Mass Index for Age: Methods and Development. (2006).
- Köhler G, Luketina RR, Emmanuel K. Sutured repair of primary small umbilical and epigastric hernias: concomitant rectus diastasis is a significant risk factor for recurrence. World J Surg (2015) 39(1):121–6; discussion 127.10.1007/s00268-014-2765-y
- Emanuelsson P, Gunnarsson U, Dahlstrand U, Strigård K, Stark B. Operative correction of abdominal rectus diastasis (ARD) reduces pain and improves abdominal wall muscle strength: a randomized, prospective trial comparing retromuscular mesh repair to double-row, self-retaining sutures. Surgery (2016) 160(5):1367–75.10.1016/j.surg.2016.05.035
- Canziani M, Frattini F, Cavalli M, Agrusti S, Somalvico F, Campanelli G. Sutureless mesh fibrin glue incisional hernia repair. Hernia (2009) 13(6):625–9.10.1007/s10029-009-0555-5
- Privett BJ, Ghusn M. Proposed technique for open repair of a small umbilical hernia and rectus divarication with self-gripping mesh. Hernia (2016) 20(4):527–30.10.1007/s10029-016-1470-1
- Coste AH, Bhimji SS. Hernia, Umbilical. [Updated 2018 Nov 2]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2018 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK459312
- Nacef K, Chaouch MA, Chaouch A, Khalifa MB, Ghannouchi M, Boudokhane M. Trocar site post incisional hernia: about 19 cases. Pan Afr Med J. 2018;29:183.
- Halm JA, Heisterkamp J, Veen HF, Weidema WF. Long-term follow-up after umbilical hernia repair: are there risk factors for recurrence after simple and mesh repair. Hernia. 2005 Dec;9(4):334-7.