Vascular congestion
Vascular congestion is the engorgement of the blood vessels with blood.
Pulmonary vascular congestion
Pulmonary vascular congestion means the blood vessels in your lungs are engorged as seen on chest x-ray (see Figure 2 below). Pulmonary vascular congestion is commonly associated with congestive heart failure or simply heart failure. Heart failure is a condition in which your heart can’t pump enough blood to meet your body’s needs. Heart failure does not mean that your heart has stopped or is about to stop working. It means that your heart is not able to pump blood the way it should. It can affect one or both sides of the heart.
About 5.7 million people in the United States have heart failure. The number of people who have this condition is growing.
Heart failure is more common in:
- People who are age 65 or older. Aging can weaken the heart muscle. Older people also may have had diseases for many years that led to heart failure. Heart failure is a leading cause of hospital stays among people on Medicare.
- Blacks are more likely to have heart failure than people of other races. They’re also more likely to have symptoms at a younger age, have more hospital visits due to heart failure, and die from heart failure.
- People who are overweight. Excess weight puts strain on the heart. Being overweight also increases your risk of heart disease and type 2 diabetes. These diseases can lead to heart failure.
- People who have had a heart attack. Damage to the heart muscle from a heart attack and can weaken the heart muscle.
Children who have congenital heart defects also can develop heart failure. These defects occur if the heart, heart valves, or blood vessels near the heart don’t form correctly while a baby is in the womb. Congenital heart defects can make the heart work harder. This weakens the heart muscle, which can lead to heart failure. Children don’t have the same symptoms of heart failure or get the same treatments as adults.
The weakening of the heart’s pumping ability causes:
- Blood and fluid to back up into the lungs
- The buildup of fluid in the feet, ankles and legs – called edema
- Tiredness and shortness of breath
Pulmonary vascular congestion causes
Conditions that damage or overwork the heart muscle can cause heart failure. Over time, the heart weakens. It isn’t able to fill with and/or pump blood as well as it should. As the heart weakens, certain proteins and substances might be released into the blood. These substances have a toxic effect on the heart and blood flow, and they worsen heart failure.
Causes of heart failure include:
- Ischemic heart disease
- Diabetes
- High blood pressure
- Other heart conditions and diseases also can lead to heart failure, such as:
- Arrhythmia. Happens when a problem occurs with the rate or rhythm of the heartbeat.
- Cardiomyopathy. Happens when the heart muscle becomes enlarged, thick, or rigid.
- Congenital heart defects. Problems with the heart’s structure are present at birth.
- Heart valve disease. Occurs if one or more of your heart valves doesn’t work properly, which can be present at birth or caused by infection, other heart conditions, and age.
- Other factors also can injure the heart muscle and lead to heart failure. Examples include:
- Alcohol abuse or cocaine and other illegal drug use
- HIV/AIDS
- Thyroid disorders (having either too much or too little thyroid hormone in the body)
- Too much vitamin E
- Treatments for cancer, such as radiation and chemotherapy
Common causes of heart failure are coronary artery disease, high blood pressure and diabetes. It is more common in people who are 65 years old or older, African Americans, people who are overweight, and people who have had a heart attack. Men have a higher rate of heart failure than women.
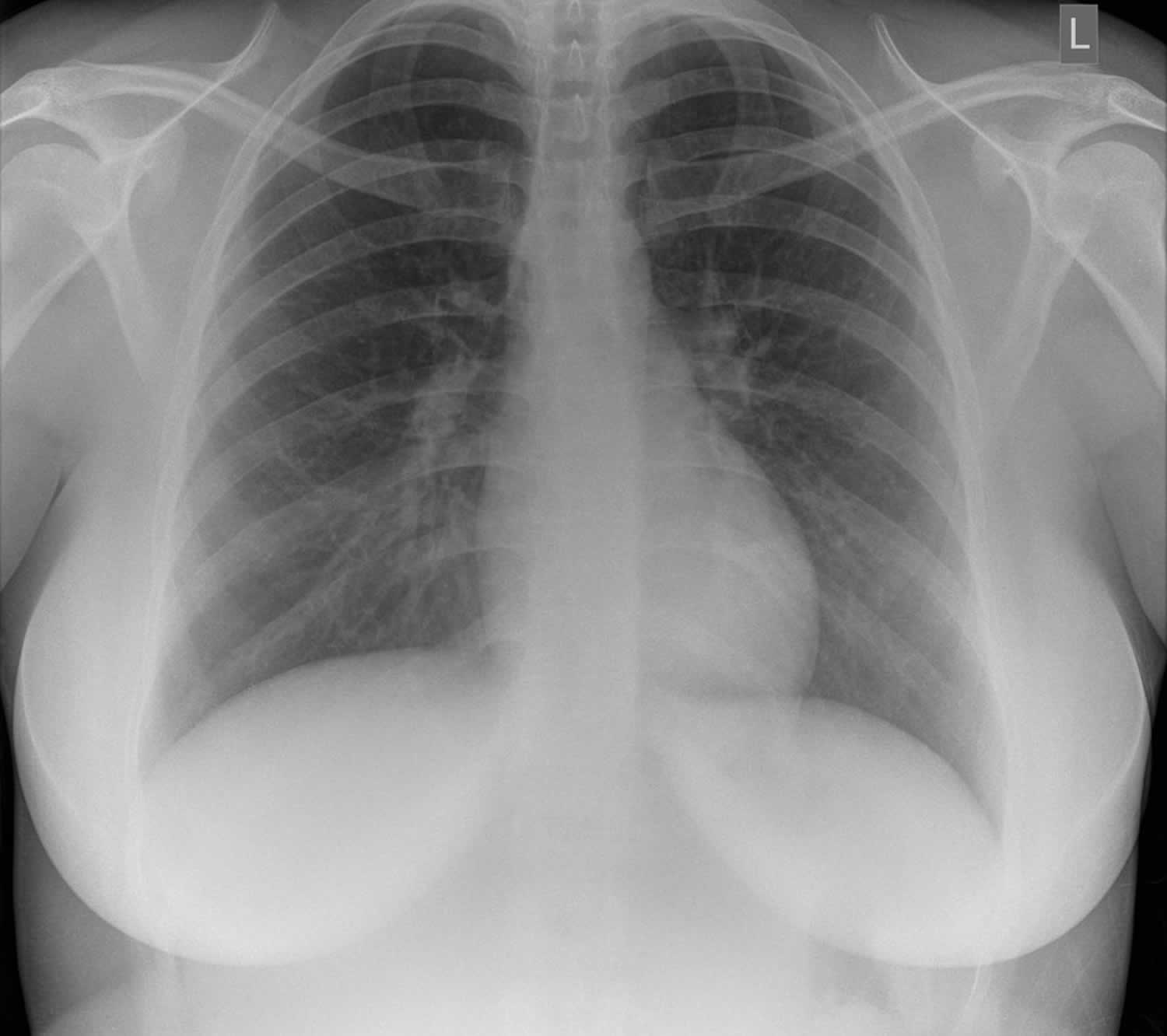
Figure 1. Normal chest x-ray
Footnote: This is a normal chest radiograph. The anatomy of the chest radiograph (young adult female) is well illustrated.
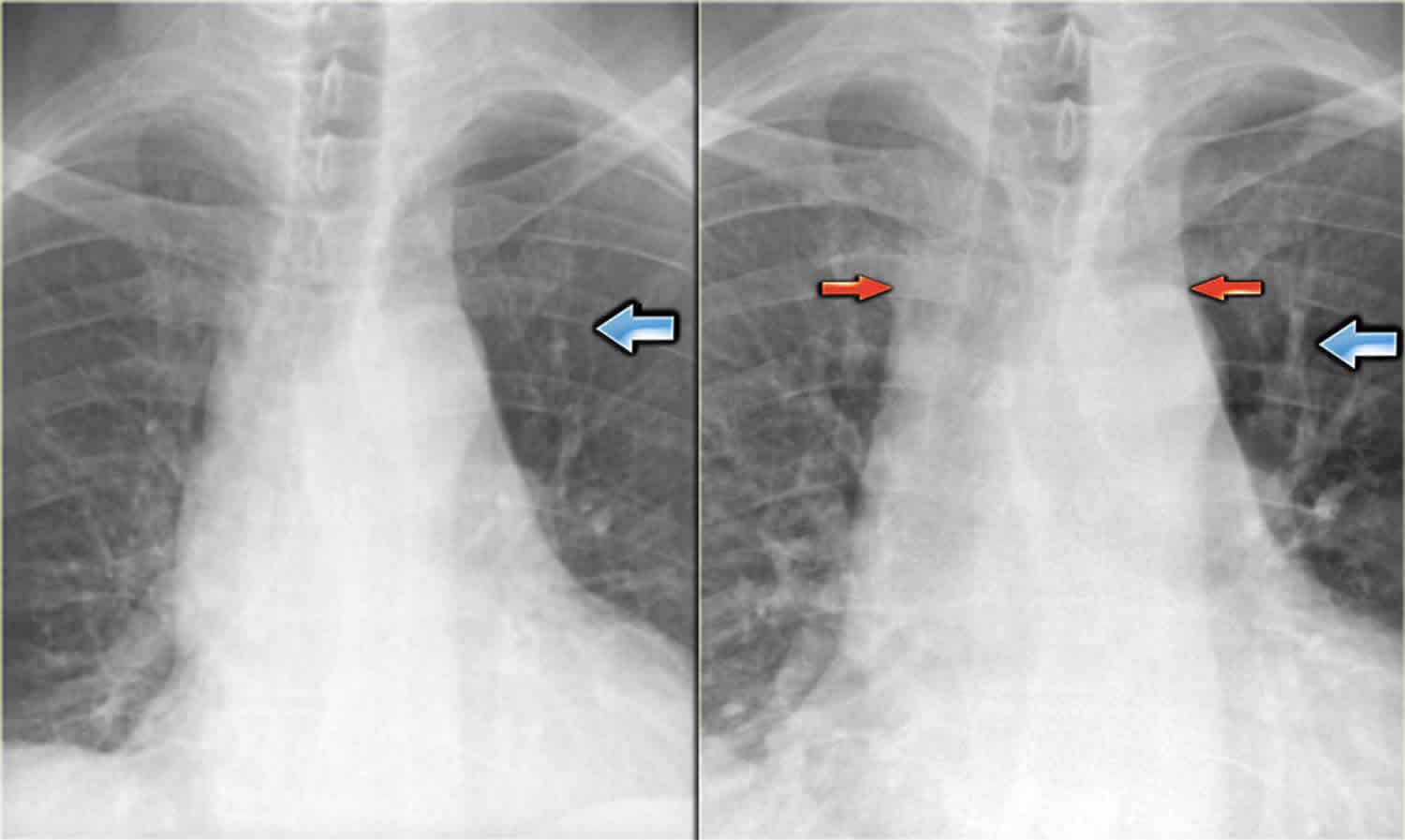
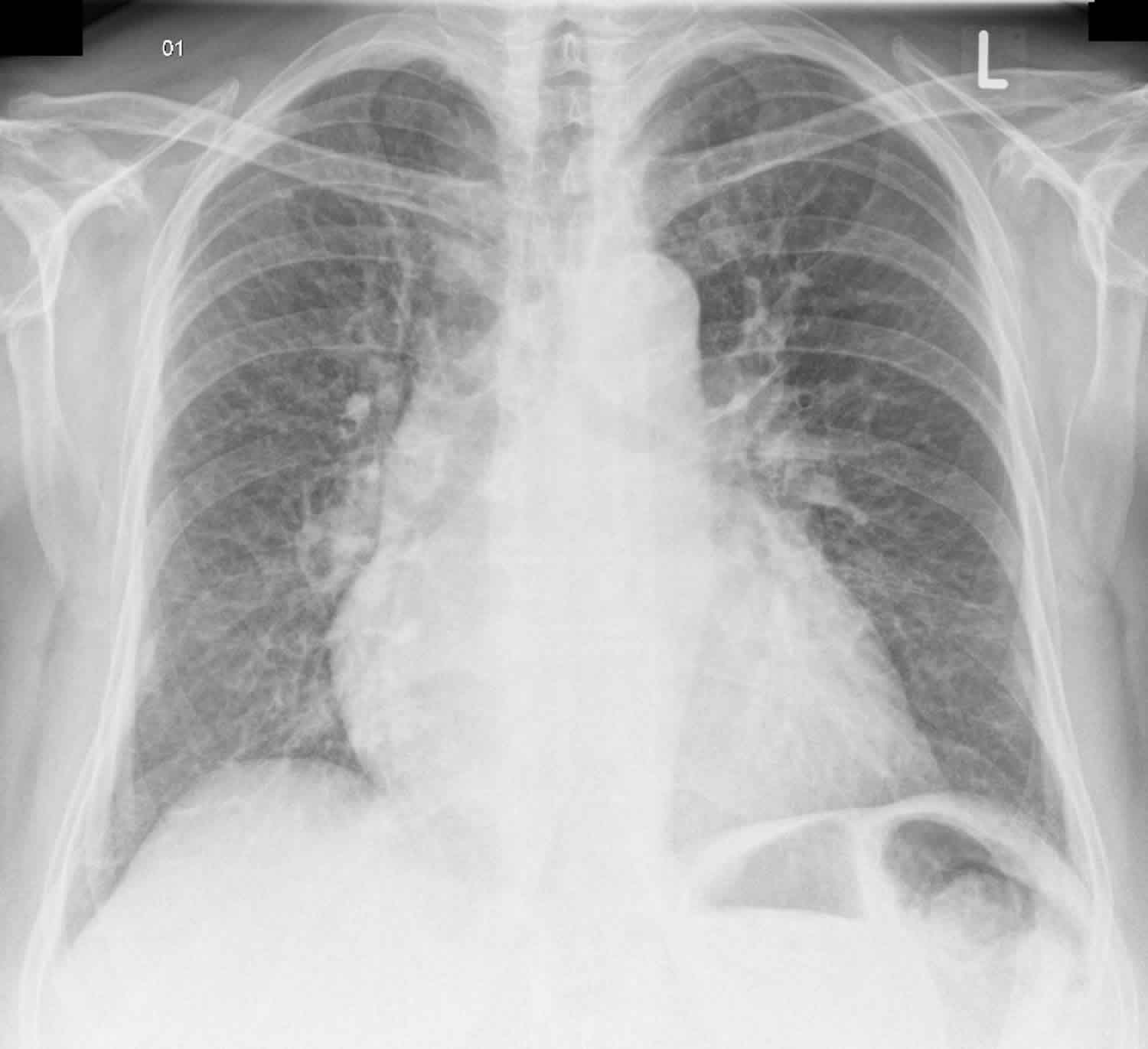
Figure 2. Pulmonary vascular congestion
Footnote: 75 year old female with severe shortness of breath (dyspnea) and history of myocardial infarction (heart attack). Chest X-ray shows cardiomegaly (heart occupies more than half of the thoracic diameter) and pulmonary vascular congestion (cephalisation of the lung vasculature) and Kerley B lines.
Pulmonary vascular congestion symptoms
The most common signs and symptoms of heart failure are:
- Shortness of breath or trouble breathing
- Fatigue (tiredness)
- Swelling in the ankles, feet, legs, abdomen, and veins in the neck
All of these symptoms are the result of fluid buildup in your body. When symptoms start, you may feel tired and short of breath after routine physical effort, like climbing stairs.
As your heart grows weaker, symptoms get worse. You may begin to feel tired and short of breath after getting dressed or walking across the room. Some people have shortness of breath while lying flat.
Fluid buildup from heart failure also causes weight gain, frequent urination, and a cough that’s worse at night and when you’re lying down. This cough may be a sign of acute pulmonary edema. This is a condition in which too much fluid builds up in your lungs. The condition requires emergency treatment.
Pulmonary vascular congestion diagnosis
Your doctor will diagnose heart failure by doing a physical exam and heart tests. However, no single test can diagnose heart failure. If you have signs and symptoms of heart failure, your doctor may recommend one or more tests.
Your doctor also may refer you to a cardiologist. A cardiologist is a doctor who specializes in diagnosing and treating heart diseases and conditions.
- EKG (Electrocardiogram): An EKG or ECG is a simple, painless test that detects and records the heart’s electrical activity. The test shows how fast your heart is beating and its rhythm (steady or irregular). An EKG also records the strength and timing of electrical signals as they pass through your heart. An EKG may show whether the walls in your heart’s pumping chambers are thicker than normal. Thicker walls can make it harder for your heart to pump blood. An EKG also can show signs of a previous or current heart attack.
- Chest X Ray: A chest x ray takes pictures of the structures inside your chest, such as your heart, lungs, and blood vessels. This test can show whether your heart is enlarged, you have fluid in your lungs, or you have lung disease.
- Brain natriuretic peptide (BNP) Blood Test: This test checks the level of a hormone in your blood called BNP (brain natriuretic peptide). The level of this hormone rises during heart failure.
- Echocardiography: Echocardiography (echo) uses sound waves to create a moving picture of your heart. The test shows the size and shape of your heart and how well your heart chambers and valves work. Echocardiogram also can identify areas of poor blood flow to the heart, areas of heart muscle that aren’t contracting normally, and heart muscle damage caused by lack of blood flow. Echocardiogram might be done before and after a stress test. A stress echo can show how well blood is flowing through your heart. The test also can show how well your heart pumps blood when it beats.
- Doppler Ultrasound: A Doppler ultrasound uses sound waves to measure the speed and direction of blood flow. This test often is done with echo to give a more complete picture of blood flow to the heart and lungs. Doctors often use Doppler ultrasound to help diagnose right-side heart failure.
- Holter Monitor: A Holter monitor records your heart’s electrical activity for a full 24- or 48-hour period, while you go about your normal daily routine. You wear small patches called electrodes on your chest. Wires connect the patches to a small, portable recorder. The recorder can be clipped to a belt, kept in a pocket, or hung around your neck.
- Nuclear Heart Scan: A nuclear heart scan shows how well blood is flowing through your heart and how much blood is reaching your heart muscle. During a nuclear heart scan, a safe, radioactive substance called a tracer is injected into your bloodstream through a vein. The tracer travels to your heart and releases energy. Special cameras outside of your body detect the energy and use it to create pictures of your heart. A nuclear heart scan can show where the heart muscle is healthy and where it’s damaged.
- Positron emission tomography (PET) scan is a type of nuclear heart scan. It shows the level of chemical activity in areas of your heart. This test can help your doctor see whether enough blood is flowing to these areas. A PET scan can show blood flow problems that other tests might not detect.
- Cardiac Catheterization: During cardiac catheterization, a long, thin, flexible tube called a catheter is put into a blood vessel in your arm, groin (upper thigh), or neck and threaded to your heart. This allows your doctor to look inside your coronary (heart) arteries. During this procedure, your doctor can check the pressure and blood flow in your heart chambers, collect blood samples, and use x rays to look at your coronary arteries.
- Coronary Angiography: Coronary angiography usually is done with cardiac catheterization. A dye that can be seen on x ray is injected into your bloodstream through the tip of the catheter. The dye allows your doctor to see the flow of blood to your heart muscle. Angiography also shows how well your heart is pumping.
- Stress Test: Some heart problems are easier to diagnose when your heart is working hard and beating fast. During stress testing, you exercise to make your heart work hard and beat fast. You may walk or run on a treadmill or pedal a bicycle. If you can’t exercise, you may be given medicine to raise your heart rate. Heart tests, such as nuclear heart scanning and echo, often are done during stress testing.
- Cardiac MRI (magnetic resonance imaging): Cardiac MRI (magnetic resonance imaging) uses radio waves, magnets, and a computer to create pictures of your heart as it’s beating. The test produces both still and moving pictures of your heart and major blood vessels. A cardiac MRI can show whether parts of your heart are damaged. Doctors also have used MRI in research studies to find early signs of heart failure, even before symptoms appear.
- Thyroid Function Tests: Thyroid function tests show how well your thyroid gland is working. These tests include blood tests, imaging tests, and tests to stimulate the thyroid. Having too much or too little thyroid hormone in the blood can lead to heart failure.
Pulmonary vascular congestion treatment
Early diagnosis and treatment can help people who have heart failure live longer, more active lives. Treatment includes treating the underlying cause of your heart failure, the type of heart failure and severity of your heart failure. Currently, heart failure has no cure. You’ll likely have to take medicine and follow a treatment plan for the rest of your life.
Despite treatment, symptoms may get worse over time. You may not be able to do many of the things that you did before you had heart failure. However, if you take all the steps your doctor recommends, you can stay healthier longer.
Researchers also might find new treatments that can help you in the future.
The goals of treatment for all stages of heart failure include:
- Treating the condition’s underlying cause, such as ischemic heart disease, high blood pressure, or diabetes
- Reducing symptoms
- Stopping the heart failure from getting worse
- Increasing your lifespan and improving your quality of life
Treatments usually include heart-healthy lifestyle changes, medicines, and ongoing care. If you have severe heart failure, you also may need medical procedures or surgery.
Heart-healthy lifestyle changes
Your doctor may recommend heart-healthy lifestyle changes if you have heart failure. Heart-healthy lifestyle changes include:
- Heart-healthy eating
- Aiming for a healthy weight
- Physical activity
- Quitting smoking
Medicines
Your doctor will prescribe medicines based on the type of heart failure you have, how severe it is, and your response to certain medicines. The following medicines are commonly used to treat heart failure:
- ACE inhibitors lower blood pressure and reduce strain on your heart. They also may reduce the risk of a future heart attack.
- Aldosterone antagonists trigger the body to remove excess sodium through urine. This lowers the volume of blood that the heart must pump.
- Angiotensin receptor blockers relax your blood vessels and lower blood pressure to decrease your heart’s workload.
- Beta blockers slow your heart rate and lower your blood pressure to decrease your heart’s workload.
- Digoxin makes the heart beat stronger and pump more blood.
- Diuretics (fluid pills) help reduce fluid buildup in your lungs and swelling in your feet and ankles.
- Isosorbide dinitrate/hydralazine hydrochloride helps relax your blood vessels so your heart doesn’t work as hard to pump blood. Studies have shown that this medicine can reduce the risk of death in blacks. More studies are needed to find out whether this medicine will benefit other racial groups.
Take all medicines regularly, as your doctor prescribes. Don’t change the amount of your medicine or skip a dose unless your doctor tells you to. You should still follow a heart healthy lifestyle, even if you take medicines to treat your heart failure.
Ongoing care
You should watch for signs that heart failure is getting worse. For example, weight gain may mean that fluids are building up in your body. Ask your doctor how often you should check your weight and when to report weight changes.
Getting medical care for other related conditions is important. If you have diabetes or high blood pressure, work with your health care team to control these conditions. Have your blood sugar level and blood pressure checked. Talk with your doctor about when you should have tests and how often to take measurements at home.
Try to avoid respiratory infections like the flu and pneumonia. Talk with your doctor or nurse about getting flu and pneumonia vaccines.
Many people who have severe heart failure may need treatment in a hospital from time to time. Your doctor may recommend oxygen therapy, which can be given in a hospital or at home.
Medical procedures and surgery
As heart failure worsens, lifestyle changes and medicines may no longer control your symptoms. You may need a medical procedure or surgery.
In heart failure, the right and left sides of the heart may no longer contract at the same time. This disrupts the heart’s pumping. To correct this problem, your doctor might implant a cardiac resynchronization therapy device (a type of pacemaker) near your heart. This device helps both sides of your heart contract at the same time, which can decrease heart failure symptoms.
Some people who have heart failure have very rapid, irregular heartbeats. Without treatment, these heartbeats can cause sudden cardiac arrest. Your doctor might implant an implantable cardioverter defibrillator (ICD) near your heart to solve this problem. An ICD checks your heart rate and uses electrical pulses to correct irregular heart rhythms.
People who have severe heart failure symptoms at rest, despite other treatments, may need:
- A mechanical heart pump, such as a left ventricular assist device. This device helps pump blood from the heart to the rest of the body. You may use a heart pump until you have surgery or as a long-term treatment.
- Heart transplant. A heart transplant is an operation in which a person’s diseased heart is replaced with a healthy heart from a deceased donor. Heart transplants are done as a life-saving measure for end-stage heart failure when medical treatment and less drastic surgery have failed.