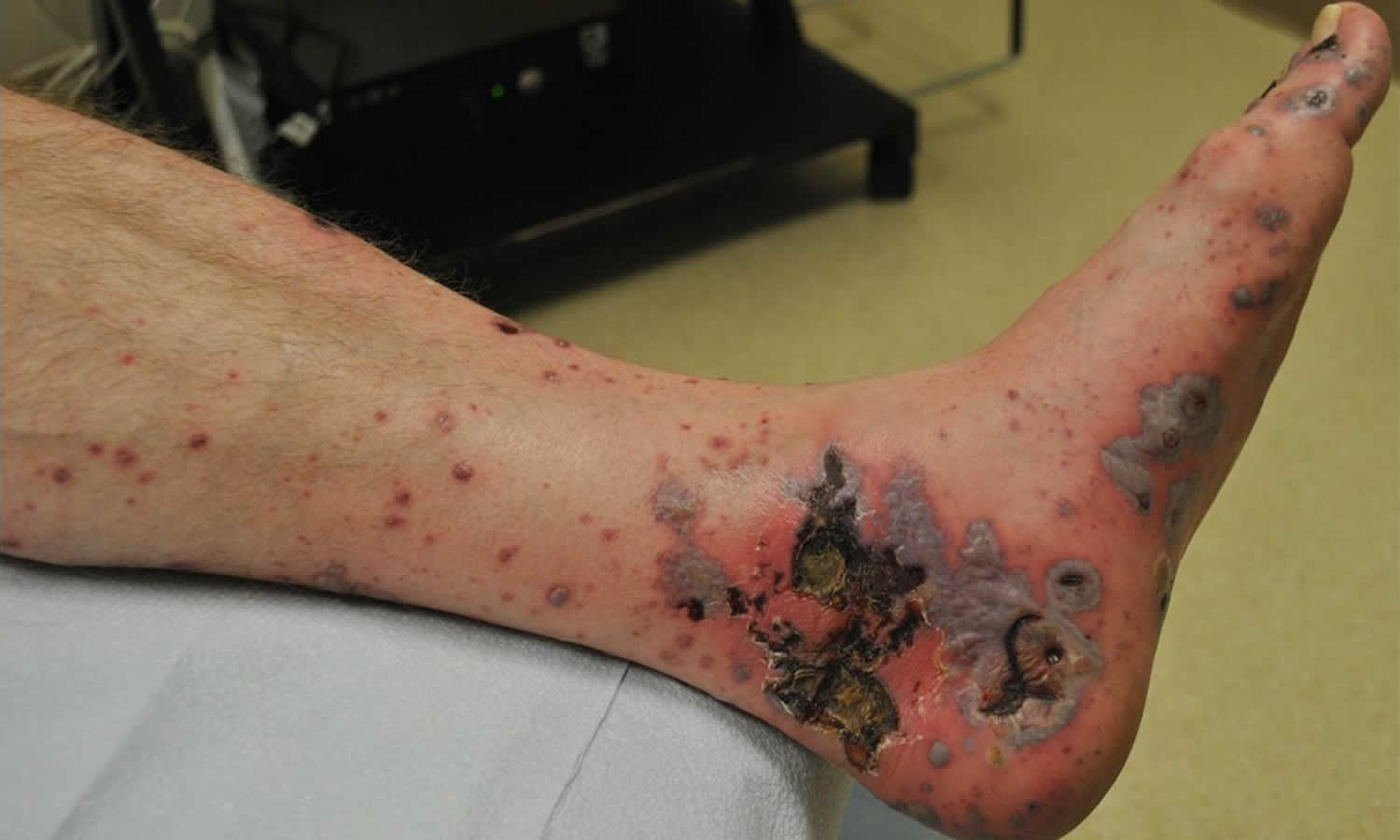
What is vasculitis
Vasculitis is a term for a group of rare diseases that have in common inflammation of blood vessels 1. It happens when the body’s immune system attacks the blood vessel by mistake. These vessels include arteries, veins and capillaries. Arteries are vessels that carry blood from the heart to the body’s organs. Veins are the vessels that carry blood back to the heart. Capillaries are tiny blood vessels that connect the small arteries and veins.
When a blood vessel becomes inflamed, it can:
- Narrow, making it more difficult for blood to get through
- Close off completely so that blood can’t get through
- Stretch and weaken so much that it bulges. The bulge is called an aneurysm. If it bursts, it can cause dangerous bleeding inside the body.
Vasculitis can result in poor blood flow to tissues throughout the body, such as the lungs, nerves and skin.
Vasculitis has a wide range of signs and symptoms, such as:
- Shortness of breath and cough
- Numbness or weakness in a hand or foot
- Red spots on the skin (“purpura”), lumps (“nodules”) or sores (“ulcers”)
On the other hand, vasculitis of the kidneys may produce no symptoms at first but is still a serious problem. Vasculitis can be mild or disabling, or even lead to death. Patients can have one episode of vasculitis or have repeated episodes over several years.
Vasculitis can happen because of an infection, a medicine, or another disease. There are many types of vasculitis, and they may vary greatly in symptoms, severity and duration. Most types of vasculitis are rare, and the causes are generally unknown. Vasculitis affects persons of both sexes and all ages. A few forms of vasculitis affect certain groups of people. For instance, Kawasaki disease occurs only in children. IgA Vasculitis (Henoch-Schönlein) is much more common in children than adults. On the other hand, giant cell arteritis occurs only in adults over 50 years old.
Symptoms of vasculitis can vary, but usually include fever, swelling and a general sense of feeling ill. The main goal of treatment is to stop the inflammation. Steroids and other medicines to stop inflammation are often helpful.
Complications of vasculitis
Vasculitis complications depend on the type and severity of your condition. Or they may be related to side effects of the prescription medications you use to treat the condition. Complications of vasculitis include:
- Organ damage. Some types of vasculitis can be severe, causing damage to major organs.
- Blood clots and aneurysms. A blood clot may form in a blood vessel, obstructing blood flow. Rarely, vasculitis will cause a blood vessel to weaken and bulge, forming an aneurysm.
- Vision loss or blindness. This is a possible complication of untreated giant cell arteritis.
- Infections. These include serious and life-threatening conditions, such as pneumonia and blood infection (sepsis).
Types of vasculitis
There are many types of vasculitis, and most of them are rare. Vasculitis might affect just one organ, or several. The condition can be short term (acute) or long lasting (chronic).
Vasculitis can affect anyone, though some types are more common among certain groups. Depending on the type you have, you may improve without treatment. Some types require medications to control the inflammation and prevent flare-ups.
- Behcet’s disease
- Buerger’s disease
- Churg-Strauss syndrome
- Cryoglobulinemia
- Giant cell arteritis
- Granulomatosis with polyangiitis
- Henoch-Schonlein purpura
- Kawasaki disease
- Takayasu’s arteritis
Vasculitis can also be associated with some infection or diseases such as cancer.
Largest arteries: aorta and major branches
- Giant cell arteritis
- Takayasu’s arteritis
- Aortitis in Cogan’s syndrome
- Aortitis in spondylarthropathies
- Isolated aortitis
Medium-sized arteries
- Kawasaki disease
- Polyarteritis nodosa
Small and medium-sized arteries
- ANCA (antineutrophil cytoplasmic antibodies)-associated vasculitis
- Granulomatosis with polyangiitis (former name: Wegener’s granulomatosis) Microscopic polyangiitis
- Eosinophilic granulomatosis with polyangiitis (Churg-Strauss )
- Primary angiitis of the central nervous system
Small arteries
- IgA Vasculitis (Henoch-Schönlein)
- Vasculitis related to rheumatoid arthritis, systemic lupus erythematosus and Sjögren’s syndrome
- Cryoglobulinemic vasculitis
- Anti-glomerular basement membrane disease (Goodpasture’s disease)
- Drug-induced vasculitis
Arteries and veins of various sizes
- Behçet’s disease
- Relapsing polychondritis
Vasculitis causes
Doctors do not know what causes most types of vasculitis. Genetic factors (different genes) appear be somewhat important in the disease. Vasculitis is thought to be an autoimmune disease, which means the body comes under attack by its own immune system. In vasculitis, the immune system attacks blood vessels. Some cases of vasculitis are caused by reactions to medicines. Also, some chronic (long-term) infections, including with hepatitis C or hepatitis B virus, can cause vasculitis.
Vasculitis can be a part of other rheumatic diseases, mainly including systemic lupus erythematosus, rheumatoid arthritis and Sjögren’s syndrome. Most patients with vasculitis have none of these diseases.
Blood vessels affected by vasculitis may bleed or become inflamed. Inflammation can cause the layers of the blood vessel wall to thicken. This narrows the blood vessels, reducing the amount of blood — and therefore oxygen and vital nutrients — that reaches your body’s tissues and organs.
Risk factors for vasculitis
Vasculitis can occur in any sex or race or at any age. But some factors can increase the risk, such as:
- Smoking
- Having chronic hepatitis B or C infections
- Having some types of autoimmune conditions, including rheumatoid arthritis, scleroderma or lupus
Vasculitis symptoms
The signs and symptoms of vasculitis vary greatly. They’re often related to decreased blood flow throughout the body.
General signs and symptoms common to most vasculitis types
General signs and symptoms of vasculitis include:
- Fever
- Headache
- Fatigue
- Weight loss
- General aches and pains
- Night sweats
- Rash
- Nerve problems, such as numbness or weakness
Signs and symptoms for specific types of vasculitis
Other signs and symptoms are related only to certain types of vasculitis. The symptoms can develop early and rapidly or in later stages of the disease.
- Behcet’s disease. This condition causes inflammation of your arteries and veins. Signs and symptoms include mouth and genital ulcers, eye inflammation, and acne-like skin lesions.
- Buerger’s disease. This condition causes inflammation and clots in the blood vessels of your hands and feet, resulting in pain and ulcers in these areas. Rarely, Buerger’s disease can affect blood vessels in the abdomen, brain and heart. It is also called thromboangiitis obliterans.
- Churg-Strauss syndrome (Eosinophilic granulomatosis with polyangiitis). This condition is very rare. It mainly affects the lungs, skin, kidneys, heart and nerves in your limbs. Signs and symptoms vary greatly and include asthma, skin changes, nerve pain and nasal allergies.
- Cryoglobulinemia. This condition results from abnormal proteins in the blood. Signs and symptoms include rash, joint pain, weakness, and numbness or tingling.
- Giant cell arteritis (also called temporal arteritis). This condition is an inflammation of the arteries in your head, especially at the temples. Giant cell arteritis can cause headaches, scalp tenderness, jaw pain, blurred or double vision, and even blindness.
- Granulomatosis with polyangiitis. This condition causes inflammation of the blood vessels in your nose, sinuses, throat, lungs and kidneys. Signs and symptoms include nasal stuffiness, sinus infections, nosebleeds and possibly coughing up blood. But most people don’t have noticeable symptoms until the damage is more advanced.
- Henoch-Schonlein purpura (IgA vasculitis). This condition is more common in children than in adults, and causes inflammation of the smallest blood vessels (capillaries) of your skin, joints, bowel and kidneys. Signs and symptoms include abdominal pain, blood in the urine, joint pain, and a rash on your buttocks or lower legs.
- Hypersensitivity vasculitis. Sometimes called allergic vasculitis or leukocytoclastic vasculitis, the primary sign of this condition is red spots on your skin, usually on your lower legs. It can be triggered by an infection or an adverse reaction to medicine.
- Kawasaki disease. This condition most often affects children younger than age 5. Signs and symptoms include fever, rash and redness of the eyes. It is also called mucocutaneous lymph node syndrome.
- Microscopic polyangiitis. This form of vasculitis affects small blood vessels, usually those in the kidneys, lungs or nerves. You may develop abdominal pain and a rash, fever, muscle pain and weight loss. If the lungs are affected, you may cough up blood.
- Polyarteritis nodosa. This form of vasculitis usually affects the kidneys, the digestive tract, the nerves and the skin. Signs and symptoms include a rash, general malaise, weight loss, muscle and joint pain, abdominal pain after eating, high blood pressure, muscle pain and weakness, and kidney problems.
- Takayasu’s arteritis. This form of vasculitis affects the larger arteries in the body, including the aorta. Signs and symptoms include joint pain, loss of pulse, high blood pressure, night sweats, fever, general malaise, appetite loss, headaches and visual changes.
Vasculitis diagnosis
Your doctor likely will start by taking your medical history and performing a physical exam. He or she may have you undergo one or more diagnostic tests and procedures to either rule out other conditions that mimic vasculitis or diagnose vasculitis.
Tests and procedures might include:
- Blood tests. These tests look for signs of inflammation, such as a high level of C-reactive protein. A complete blood cell count can tell whether you have enough red blood cells. Blood tests that look for certain antibodies — such as the anti-neutrophil cytoplasmic antibodies test — can help diagnose vasculitis.
- Urine tests. These tests may reveal whether your urine contains red blood cells or has too much protein, which can signal a medical problem.
- Imaging tests. Noninvasive imaging techniques can help determine what blood vessels and organs are affected. They can also help the doctor monitor whether you are responding to treatment. Imaging tests for vasculitis include X-rays, ultrasound, computerized tomography (CT), magnetic resonance imaging (MRI) and positron emission tomography (PET).
- X-rays of your blood vessels (angiography). During this procedure, a flexible catheter, resembling a thin straw, is inserted into a large artery or vein. A special dye (contrast medium) is then injected into the catheter, and X-rays are taken as the dye fills the artery or vein. The outlines of your blood vessels are visible on the resulting X-rays.
- Biopsy. This is a surgical procedure in which your doctor removes a small sample of tissue from the affected area of your body. Your doctor then examines this tissue for signs of vasculitis.
The most common tests are:
- Biopsy—surgical removal of a small piece of tissue for inspection under a microscope
- Angiography—a type of X-ray to look for abnormalities of blood vessels
- Blood tests
For most patients, doctors can detect the type of vasculitis based on the size of the affected blood vessels (see Types of Vasculitis above) and the organs involved. To find small-vessel vasculitis, doctors most often do a biopsy, such as of the skin or a kidney. Detection of medium-vessel vasculitis happens by either biopsy (for instance, of skin, nerve or brain) or angiography. Angiography also is the test that often finds large-vessel vasculitis. Detecting giant cell arteritis often involves a biopsy of an artery in the scalp.
A few forms of vasculitis, such as Behçet’s disease and Kawasaki disease, are usually detected on the basis of a collection of clinical findings rather than biopsy or angiography.
Some blood tests are so suggestive of a certain type of vasculitis that a positive (abnormal) test can be enough evidence to help doctors make the diagnosis. The most useful of these tests is for “antineutrophil cytoplasmic antibodies”—often referred to as ANCA. A positive antineutrophil cytoplasmic antibodies (ANCA) test can help detect these types of vasculitis: granulomatosis with polyangiitis (Wegener’s), microscopic polyangiitis or eosinophilic granulomatosis with polyangiitis (Churg-Strauss). Other lab tests can show damage to organs, but the tests are not enough to prove vasculitis.
Vasculitis treatment
Treatment focuses on controlling the inflammation with medications and resolving any underlying disease that triggered your vasculitis. For your vasculitis, you may go through two treatment phases — first stopping the inflammation and then preventing relapse (maintenance therapy).
Both phases involve prescription drugs. Which drugs and how long you need to take them depend on the type of vasculitis, the organs involved and how serious your condition is.
Some people have initial success with treatment, then experience flare-ups later. Others may never see their vasculitis completely go away and need ongoing treatment.
Patients with vasculitis often benefit from seeing experts in the organ systems that are or might become affected. Doctors that patients may need to see include a rheumatologist the specialist with the most overall knowledge about vasculitis, dermatologist (skin doctor), neurologist (expert in nervous system diseases), ophthalmologist (eye doctor), otorhinolaryngologist (ear, nose and throat doctor), nephrologist (kidney doctor) or pulmonologist (lung doctor).
Medications
Your doctor may prescribe a corticosteroid drug, such as prednisone or methylprednisolone (Medrol), to help control inflammation. Corticosteroid drugs (prednisone, prednisolone or others), often referred to as “steroids,” are an important part of treating most forms of vasculitis. The dose and length of treatment depend on how bad the disease is and how long the patient has had it. These drugs help reduce inflammation but can have long-term side effects. Side effects of corticosteroids can be severe, especially if you take them for a long time. Possible side effects include weight gain, diabetes and bone thinning (osteoporosis). If a corticosteroid is needed for long-term (maintenance) therapy, you’ll likely receive the lowest dose possible.
Other medications may be prescribed with corticosteroids to control the inflammation so that the dosage of corticosteroids can be tapered more quickly. These medications are sometimes called steroid-sparing and may include methotrexate (Trexall), azathioprine (Imuran, Azasan), mycophenolate (Cellcept) or cyclophosphamide.
Cyclophosphamide is one of the strongest of these drugs, and doctors may prescribe it when severe disease endangers vital organs.
For less serious vasculitis, patients may receive methotrexate, azathioprine or other immune-suppressing drugs. Doctors often prescribe these drugs to treat other rheumatic diseases, but they are useful for vasculitis, too.
Newer drugs designed to treat other autoimmune and inflammatory diseases may also help vasculitis. Researchers found biologic therapies such as rituximab (Rituxan) or tocilizumab (Actemra) effectively treats severe cases of certain forms of vasculitis. These include granulomatosis with polyangiitis, microscopic polyangiitis and cryoglobulinemic vasculitis. Some patients with the most severe cases of these diseases may receive plasma exchange (“plasmapheresis”) or intravenous immunoglobulin (often called “IVIg”).
Surgery
Sometimes, vasculitis causes a balloonlike bulge (aneurysm) to form in the wall of a blood vessel. This bulge may need surgery. Blocked arteries also may require surgical treatment.
Depending on where the damage is, other possible operations are sinus surgery or a kidney transplant.
Living with vasculitis
Vasculitis can be short term or lifelong. Doctors often focus, with good reason, on preventing permanent damage to vital organs (such as the lungs, kidneys and brain) and the nerves. It is crucial, of course, to prevent death and long-term disability from vasculitis. Yet, other issues often trouble patients. These include fatigue (feeling very tired), pain, arthritis, nose and sinus problems, and many other problems.
Side effects from medications, especially glucocorticoids, also can be troubling. Patients taking immunosuppressants are at risk of infections. Follow your doctor’s advice on how to reduce your infection risk.
Fortunately, with current treatments, the outcome for patients with vasculitis is often good.
Coping and support
One of your greatest challenges of living with vasculitis may be coping with side effects of your medication. The following suggestions may help:
- Understand your condition. Learn everything you can about vasculitis and its treatment. Know the possible side effects of the drugs you take, and tell your doctor about any changes in your health.
- Follow your treatment plan. Your treatment plan may include seeing your doctor regularly, undergoing more tests and checking your blood pressure.
- Choose a healthy diet. Eating well can help prevent potential problems that can result from your medications, such as thinning bones, high blood pressure and diabetes. Choose a diet that emphasizes fresh fruits and vegetables, whole grains, low-fat dairy products, and lean meats and fish. If you’re taking a corticosteroid drug, ask your doctor if you need to take a vitamin D or calcium supplement.
- Get routine vaccinations. Keeping up to date on vaccinations, such as for the flu and pneumonia, can help prevent problems that can result from your medications, such as infection. Talk to your doctor about vaccinations.
- Exercise most days of the week. Regular aerobic exercise, such as walking, can help prevent bone loss, high blood pressure and diabetes that can be associated with taking corticosteroids. It also benefits your heart and lungs. In addition, many people find that exercise improves their mood and overall sense of well-being. If you’re not used to exercising, start out slowly and build up gradually. Your doctor can help you plan an exercise program that’s right for you.
- Maintain a strong support system. Family and friends can help you as you cope with this condition. If you think it would be helpful to talk with other people who are living with vasculitis, ask a member of your health care team about connecting with a support group.