Bladder training
Bladder training is a program of urinating on schedule that will enable you to gradually increase the amount of urine you can comfortably hold 1. Bladder training is a mainstay of treatment for urinary frequency and overactive bladder in both women and men, alone or in conjunction with medications or other techniques. Bladder training can also help prevent or lessen symptoms of overactive bladder that may emerge after surgery for stress incontinence. The overall aim of bladder training is to restore the normal function of your bladder. You can try it on your own or with the guidance and support of a health professional. Because bladder training is low-cost and low-risk, your clinician may encourage you to try it first, even before specific diagnostic tests are performed.
The normal bladder can hold approximately 600-800 mls of urine. It is usual to empty your bladder about four to six times per day. It is normal to make it to the toilet without rushing, or to be able to put off emptying the bladder if it is not convenient for you.
Normal adult female bladder function
- Bladder capacity of approximately 500mls
- Normal void is 350-700 mls of urine
- Normally voids four to seven times a day
- Normally wakes to void at least once a night
- With each decade after 60 years of age one extra void during the day or night is normal
- No urinary urgency (feeling of being ‘desperate’ to pass urine or unable to delay urination) and frequency (going to the toilet often, then only passing small amounts).
Some techniques which may help you control your urge
- Stop and relax – do not rush to the toilet.
- Breathe slowly and evenly.
- Perineal / Vaginal pressure:
- Sit on the arm of a chair or the edge of a desk.
- Sit on a rolled-up towel.
- Cross your legs.
- Curl your toes repeatedly or hold firmly.
- Stretch your calf muscles and hold the stretch.
- If you are walking, slow your pace and emphasize heel-toe walking.
- Press or rub the trigger point on the inside of your leg just above your ankle.
- Press or rub the trigger point at the base of your nose.
- Squeeze and lift your pelvic floor muscles – hold them tight!
- Distract yourself. Do not think about the toilet or about leaking. Distract yourself with a physical or mental task e.g. count backwards from 100 by 3’s or 7’s; think of 3 American towns starting with A, then with B, then C etc.
- When you have performed the technique, walk to the toilet in a slow and controlled manner.
Remember: your bladder does not have eyes or ears; it cannot see the toilet nor know how far away you are. If you feel you may leak on the way it is just anxiety. Relax, stay calm and walk slowly.
Remember: different techniques work for different people. By practicing these techniques you will find out which ones work for you.
Use the above techniques to gradually increase the time between toileting and to stop getting out of bed at night when you feel the urge to go to the toilet.
Step-by-step bladder-training technique
- Keep track. For a day or two, keep track of the times you urinate or leak urine during the day.
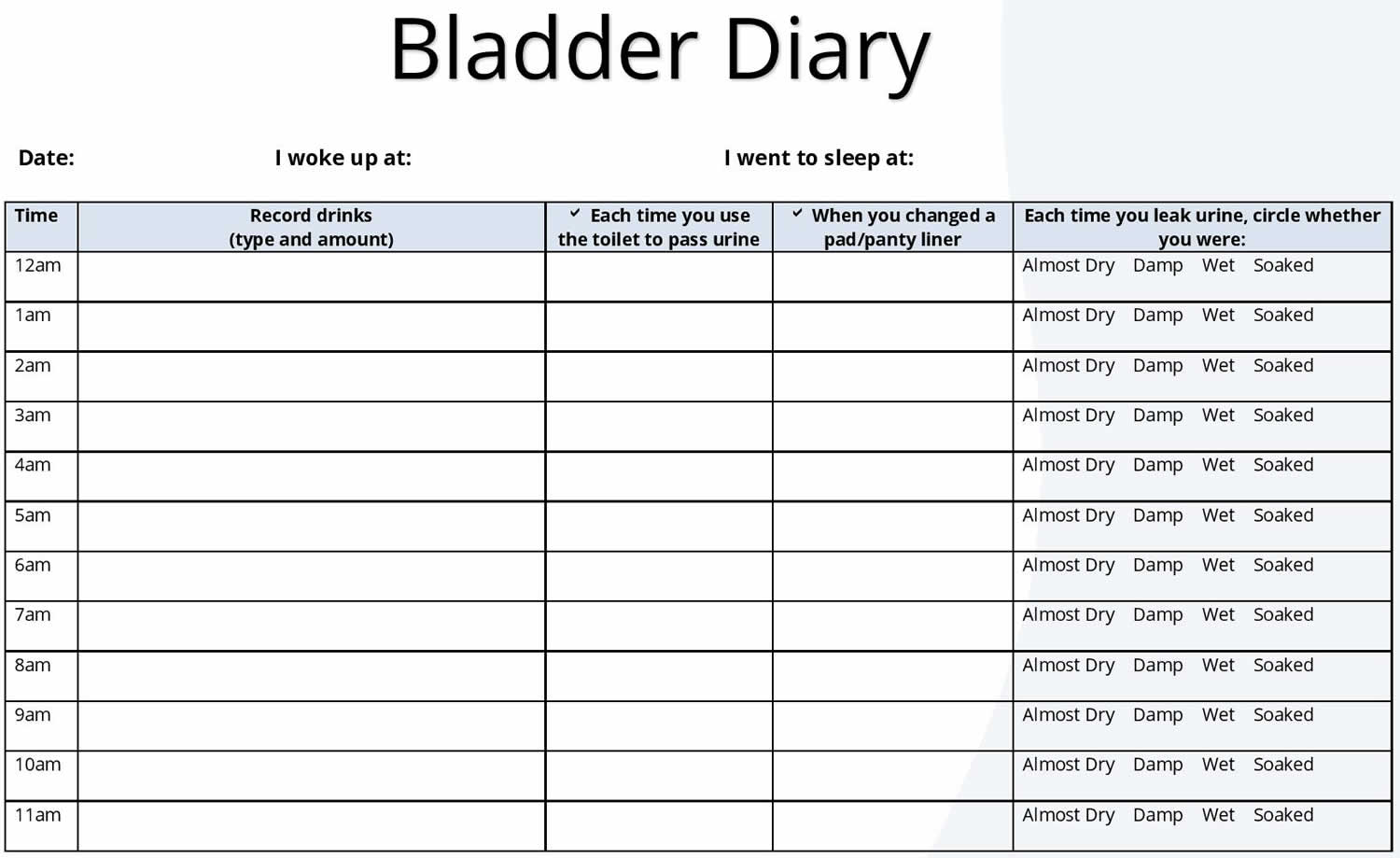
- Keeping a bladder diary
- Complete the information for two consecutive 24-hour periods. Record both day and night.
- Begin with first urination upon arising.
- Record intake amount in ounces and type of fluid (for example, coffee, juice, water, etc.).
- Record approximate urine output and time of urination.
- Keeping a bladder diary
- Calculate. On average, how many hours do you wait between urinations during the day?
- Choose an interval. Based on your typical interval between urinations, select a starting interval for training that is 15 minutes longer. If your typical interval is one hour, make your starting interval one hour and 15 minutes.
- Hold back. When you start training, empty your bladder first thing in the morning and not again until the interval you’ve set. If the time arrives before you feel the urge, go anyway. If the urge hits first, remind yourself that your bladder isn’t really full, and use whatever techniques you can to delay going. Try the pelvic floor exercises sometimes called Kegels, or simply try to wait another five minutes before walking slowly to the bathroom.
- Increase your interval. Once you are comfortable with your set interval, increase it by 15 minutes. Over several weeks or months, you may find you are able to wait much longer and that you experience far fewer feelings of urgency or episodes of urge incontinence.
People with an overactive or weak bladder have to rush off to find a bathroom because of an urge to urinate, or may gradually lose urine drop by drop before arriving at a toilet. Bladder training can then help you to regain at least some control over your bladder.
The bladder muscle can be trained to stretch more so that the bladder is able to hold more urine. Bladder training also includes various behavioral treatment approaches and a particular drinking and voiding schedule (bathroom visit schedule).
Review any lifestyle factors which may be contributing to poor bladder function.
Lifestyle measures
- Regulating your fluid intake: Your professional advisor can help you regulate your fluid intake so you drink the correct volume for your body and level of activity at the right times. Too much fluid can overfill the bladder and too little can concentrate the urine, which irritates the bladder. Drinking about 1.5L of fluid per day (mostly water) aim to regularly pass 300ml or more urine.
- Limit alcohol and caffeine-based drinks: Alcohol, caffeine-based drinks and fizzy drinks are known to irritate the bladder, which exacerbates symptoms of overactive bladder. Alcohol also has a diuretic effect, which can cause more frequent urination.
- Avoid constipation: Constipation can trigger or worsen symptoms of overactive bladder. Straining on the toilet can also weaken the pelvic floor.
- Keep your weight in the healthy range: there is evidence that losing weight decreases the severity and frequency of symptoms of overactive bladder. Maintain a healthy weight by walking for at least thirty minutes each day
- Only going to the toilet when you need to go (not going “just-in-case”)
- Get rid of any cough or sneezing
- Exercise your pelvic floor muscles as you have been shown.
- It is important to have strong pelvic floor muscles. Please see facts sheets on Pelvic Floor Exercises and Preventing Constipation for more information.
- Do persevere. You have the ability to make your brain the boss and retrain your bladder!
- Do speak to your physiotherapist, doctor or continence consultant about any concerns or problems you encounter.
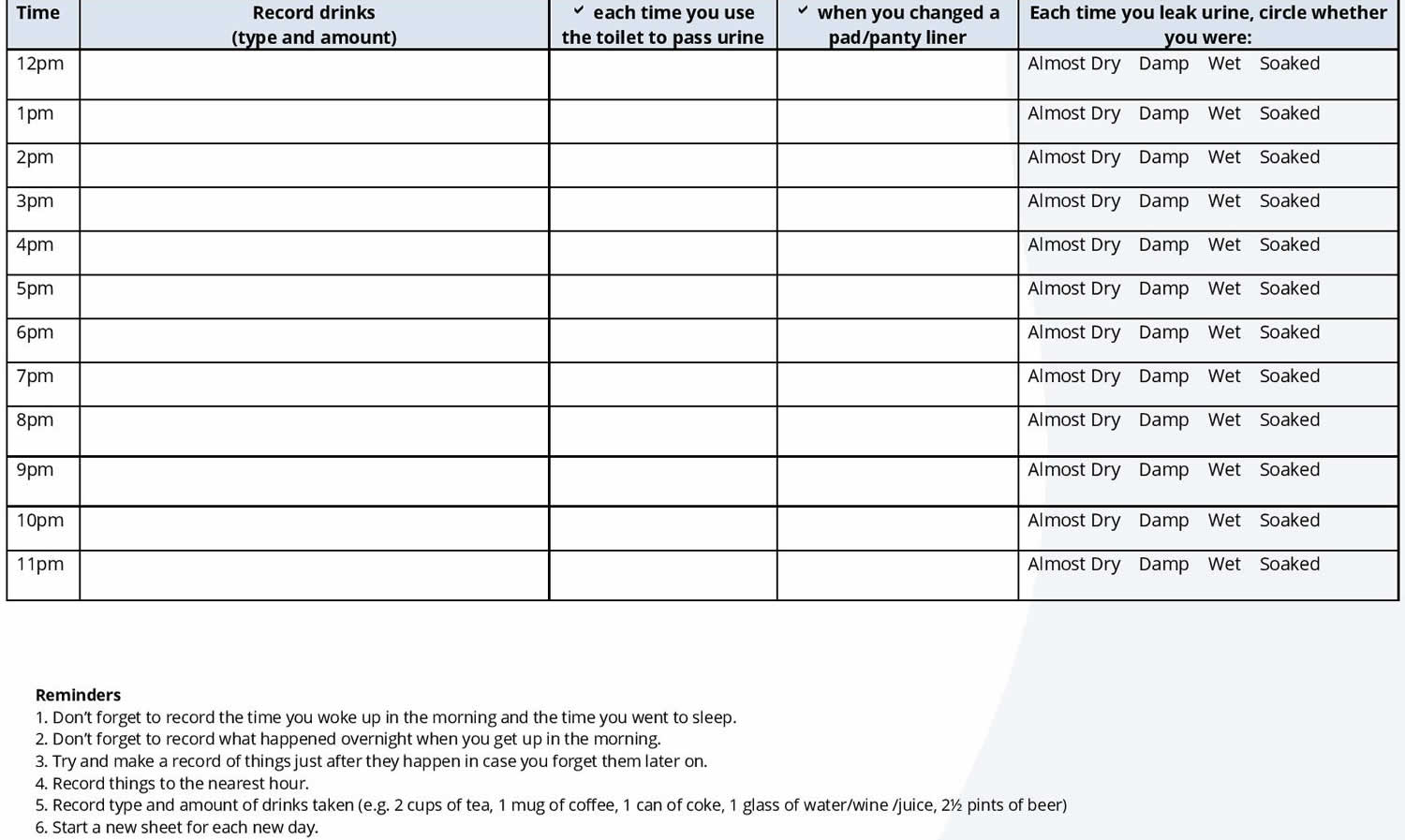
Figure 1. Bladder diary
What are normal bladder habits?
A healthy bladder can hold 300-400 mls of urine during the day and about 800 mls at night. It is normal to pass urine five or six times a day if you drink between 6-8 glasses of fluid. It is usual to empty your bladder when you get out of bed in the morning, three times during the day, and before you go to bed at night. As we age this pattern may change, as older people tend to make more urine at night.
How do I measure my urine?
To measure the amount of urine you pass, put a container (like an ice cream container) in the toilet bowl. Sit on the toilet and pass urine into the container. When you have finished, measure the urine by tipping it into a measuring jug. For men, you may prefer to stand and pass urine directly into the measuring jug. You should note the measurement from the jug in your bladder diary, then tip the urine into the toilet and flush.
You can also use abosrbent pads to work out how much urine you leak over one or two days. This is done by using a dry pad that has been weighed in a plastic bag. When you change the wet pad you put it back in the plastic bag and weight it. If you take away the weight of the dry pad from the weight of the wet pad you can work out how much urine you have leaked. One milliliter (ml) of urine weighs one gram.
For example:
- Wet pad = 350 grams
- Dry pad = 150 grams
Weight difference
- 200 grams
Amount leaked
- 200 mls
How will I know if bladder training is working?
You may not notice an improvement immediately, but gradually you will become aware of not having to go to the toilet as often, being able to stop yourself going, passing more urine each time you
go, having less urgency, and not getting up to the toilet at night time.
Bladder training takes time. You may have good and bad days. Persevere and you will eventually be the boss of your bladder.
What happens if bladder training doesn’t work?
Despite best efforts, in a few cases, the bladder will not respond to the bladder training program. In these cases, some medications, prescribed by the doctor, may assist. If you decide to take medications it is important to still continue your bladder training strategies.
Bladder training program
When you do bladder training you are aiming to:
- decrease the number of times you go to the toilet
- increase the amount of urine you pass each time
- hold on for longer or put off emptying your bladder.
Every person will have different needs in regard to bladder training.
The first step is to complete a two to three-day bladder diary to get information about your bladder function (see Figure 1 above). From your diary you will be able to identify how long your bladder can hold on until it needs to be emptied. From here, you can set realistic goals that can help your bladder become stronger. Set yourself achievable goals. When you have set your goals, try not to rush to the toilet as soon as the time is up. Try if possible to resist that further urge. For example, if you start with a break of one hour between emptying your bladder, your initial goal may be to “hang on” for 5 or 10 minutes. The aim is to gradually increase the time you can “hang-on”. Discuss appropriate goals with your continence consultant, doctor or physiotherapist.
At night, empty your bladder before you go to bed and try and resist any urges to further empty your bladder before you go to sleep.
The following are some things that may help make your bladder retraining successful:
- Plan your retraining schedule clearly with realistic and achievable goals.
- Focus on success – not on setbacks.
- Be patient; bladder retraining will not be a success overnight. You will need to work hard at it for some weeks.
- Be aware of any fears or worries associated with your bladder problem. In some cases these fears or worries will need to be tackled before long-lasting success is possible.
If you are frightened of having an accident while training, consider wearing light protection. Perhaps an absorbent pad in your pants, or special underwear designed to mop up small leakages. These will remove the worry and the hassle of having to change frequently during training.
If you find you are getting nowhere after 2 to 3 weeks of work, then consider consulting your doctor or a specialist continence nurse or physiotherapist. It may be that some other medical cause is preventing your success like a persistent infection or some damage to your bladder mechanism.
First step: Keep a bladder diary
The basis of bladder training is keeping a bladder diary. You can use it to write down:
- How often you go to the bathroom,
- How much urine comes out and time of urination,
- How much you drink throughout the day,
- Complete the information for two consecutive 24-hour periods. Record both day and night.
It is also important to record information about any medications you take and about situations in which you accidentally leak urine. These notes can be helpful when talking to your doctor and might provide important clues about the cause of the problem.
Voiding schedule: Regularity matters
- Regular rhythm: It is important to go to the toilet at regular intervals so that your bladder gets used to a certain frequency. A voiding (bathroom visit) schedule can be helpful here. Bladder training programs often recommend that, once you have emptied your bladder first thing in the morning and perhaps again after breakfast, you try to keep the intervals between bathroom visits as regular as possible.
- Avoid going to the bathroom “just in case”: If you go to the toilet too frequently “just in case,” you might end up making the overactive bladder symptoms worse, because the bladder is then “trained” to send a signal that you need to urinate as soon as there is only a small amount of urine in it.
- Do not go to the bathroom straight away: Even if you have a very strong urge to go to the bathroom, it usually only lasts a few minutes and then dies down again. You can practice not emptying your bladder as soon as you feel the need to go. Going to the bathroom calmly and at a slow pace rather than rushing to get there can help too.
- Increase the intervals between emptying your bladder: You can try to wait longer between trips to the bathroom, but do so at a slow pace and without any stress. A voiding schedule can be helpful here too. You can use it to remember, for example, that you want to try to wait 5 minutes before emptying your bladder in the first few days, and then keep this up for about half a week. You can then lengthen that “waiting period” to 10, 15 and finally 20 minutes.
It takes a lot of effort to stick to the training at night. Positive results are more easily achieved during the day. After some time, the training can then be done at night as well.
Distraction techniques
If you are trying not to go to the bathroom as soon as you feel the urge, and want to wait longer between emptying your bladder, several techniques might help to distract you:
- Whenever you feel like you have to “go,” you could try to relax and distract yourself with positive thoughts. For example, you could tell yourself: “I will go to the bathroom in 5 minutes, and think about something else until then.”
- It can also be helpful to sit on a chair and bend your hips to lean the upper part of your body forward as is you were leaning down to tie your shoelace. You can hold this position until the urge passes. Leaning forward changes the pressure in your abdomen and the position of your urethra, so you have less of an urge to urinate.
- You could also sit upright and tense your pelvic floor muscles, pulling up and in.
Drinking schedule: Drinking frequently and enough
A lot of people who have a weak bladder drink too little because they are afraid that they will not make it to the bathroom in time. But regularity not only helps when emptying your bladder, it is also important when filling your bladder. Because of this, bladder training usually includes both a voiding schedule and a drinking schedule, in which you record when and how much you drink. Many people find it helpful to use a timer that makes a sound to remind them to stick to the schedule.
- Drinking enough is important for another reason: If your urine is too concentrated, the substances in it might irritate the lining of your bladder after a while. This can make the symptoms worse.
- You can try to drink one to two glasses of still water before every meal and may drink juices between meals, as well as small amounts of coffee and black tea.
- In order to try to get the best night’s sleep possible, it can help to drink less or stop drinking about two hours before going to sleep.
- Coffee, black tea, green tea and alcoholic drinks are diuretics. This means they increase the production of urine. Other kinds of tea have this effect too, such as kidney and bladder teas or stinging nettle tea. It can help to avoid these drinks just before going to sleep.
- It can also be helpful to avoid diuretic drinks before taking part in social activities that involve being out and about a lot.
Change your drinking habits
There are a number of drinks that may irritate the bladder. If you do have these drinks, try to have them less often or stop having them completely, to see if this helps.
Drinks which may irritate the bladder are:
- drinks containing caffeine such as tea and coffee• carbonated (fizzy) drinks
- drinks containing aspartame (an artificial sweetener, which can be found in diet drinks. It can also be labelled as E951)
- hot chocolate
- alcohol
- green tea and mint tea
- blackcurrant juice
- citrus fruit juices (e.g. orange and grapefruit).
Drinks which are believed not to irritate the bladder are:
- water (definitely not a bladder irritant)
- fruit teas
- caffeine-free tea and coffee (make sure all the caffeine has been removed). However, some people’s bladders can also be irritated by de-caffeinated drinks. Try de-caffeinated drinks for a month to see if this improves your symptoms.
- milk
- diluted fruit juice.
Many people with an overactive bladder reduce the amount they drink. However, this can make the problem worse, as the bladder then never gets full and so loses the ability to stretch. Also, the urine becomes concentrated, which can irritate the bladder even further. Aim to drink 1.5 to 2 liters a day (although this amount will vary depending on the weather, your activity levels and your weight. You need to drink a certain amount of fluid for your weight; your healthcare team will talk about this with you).
Medications
Medicines that may help. There are various medicines that you can try. They work for some people, but not all. It’s worth trying them for one to two months before deciding if they are suitable for you. If they do work, they will work best alongside the bladder techniques described here. You can continue to take them for as long as you need them.
The medicines are called antimuscarinics (anticholinergics) or a newer medication called mirabegron (Betmiga). Antimuscarinics work by blocking certain nerve impulses to the bladder, which stops it contracting and helps it to hold on to more urine. They need to be taken for at least 4 weeks to notice any benefit.
Mirabegron relaxes the bladder muscle. This reduces the activity of an overactive bladder and treats urge and urge incontinence. It starts to work about eight weeks after you begin taking it.
You may need to try different medicines to find one that works best for you. All medicines have possible side effects. The most common side effects from antimuscarinics are a dry mouth and constipation. Ask your doctor or specialist nurse for more information on side effects and make sure they know your medical history before recommending the medicines.
There is another form of therapy using a bacterial toxin (Botox) which can help an overactive bladder. However, it is an invasive procedure involving injections into the bladder and is only performed as a last resort. This would need to be discussed carefully with your doctor or specialist nurse.
Medications that may make the problem worse
If you take diuretics (water tablets) they can make you pass more urine, so it may be worth changing the time you take them. For example, don’t take them late at night as you will pass urine a lot during the night. However, you may not wish to take them in the morning if that is the time of day when you want to go out. Speak to your doctor before you change the pattern of taking your diuretics.
Other medicines can also adversely affect your bladder. Your doctor or specialist nurse will be able to give you more specific information.
Do not let setbacks discourage you
- Keep up your bladder diary. That is the only way to record positive results and gives you an overview of possible setbacks.
- It is also good to know that setbacks are completely normal, particularly during times when you are feeling exhausted or stressed.
- Setbacks can be caused by other things too, like common colds, urinary tract infections or wet, windy weather.
Bladder training is not always a suitable treatment for weak bladder. It is a good idea to talk to your doctor about whether this might be a good approach for you.
Overactive bladder bladder training
Overactive bladder is common women particularly after the menopause. The exact cause is unknown but it is more common in women who have had children and after menopause.
Normally, the bladder slowly distends with urine until it reaches a good volume of urine (approx. 300-400mls). Then, via nerves to the brain the bladder informs the brain that a toilet will soon be needed. Urgency should only occur if urination is delayed and the bladder distends to even larger volumes. The bladder emptying process then begins once the woman has consciously decided to urinate (that is, when you are on the toilet).
Overactive bladder symptoms
- Urgency: The feeling of being ‘desperate’ to pass urine or unable to delay urination. Often triggered by psychological events such as putting the key in the lock, running water or as the feet hit the floor when getting out of bed.
- Frequency: going to the toilet too often, usually only to pass small amounts (normal is between six to eight times)
- Urges Incontinence: when urgency is so strong it results in leakage of urine from just a few drops to a whole bladder full
- Nocturia: being woken up by the need to go to the toilet more than twice during the night.
You might be teaching your bladder some bad habits, habits that can gradually result in urinary incontinence or frequent bathroom breaks. For example, if you routinely urinate before your bladder is full, it learns to signal the need to go when less volume is present. That can set up a vicious cycle, as you respond to the new urges and teach your bladder to cry ‘run’ when less and less urine is present. Luckily, old bladders can learn new tricks.
Bladder training
Bladder training involves three steps. These are:
- Increasing bladder fill volume
- Deferral strategies
- Make less sensitive to your triggers
Step 1. Increasing bladder fill volume
Aim is to toilet less often and increasing your urine volume each time. When you first feel the need to go to the toilet, try and ignore it. If the ‘need” is a strong urge, use the strategies below to defer the urge. Put off going to the toilet until the next time you feel the urge. Initially this may only be a few minutes. As you improve, you should be able to defer for 30 minutes or longer. During the night if you wake up at night with the urge to go, get up and go immediately.
Step 2. Deferral strategies
These are strategies that will quieten your bladder and suppress the overwhelming urgency of overactive bladder. You should experiment as to which ones work the best for you and use them to dampen the urge, until it goes away and your bladder can continue to fill.
- Pelvic floor muscle contractions. This is one of the most effective methods, if your pelvic floor is strong enough. Try one big tight squeeze or several repeated four to five second contractions
- Use perineal or clitoral pressure, (hand pressure over the crotch), sitting on the edge of a chair or table.
- Roll up a bath towel and keep it on a chair. Sit on this roll when you have a strong urge to urinate. Tighten and hold your Pelvic floor muscles until the urge passes.
- Cross your legs and tighten your buttock muscles.
- Toe curling, marching on the spot or tap your heel onto the ground repetitively.
Once the urge has passed make a decision, is the bladder full?
- If not defer and when the urge is gone “get on with life”.
- If the bladder is full, use the following techniques to help get you to the toilet dry.
- Stand carefully and relax your chest
- Breathe easily and walk quietly to the toilet
- Count your steps and use distraction techniques to help get you the toilet dry.
Keep practicing until you can make the urge go away
Step 3. Become less sensitive to your triggers
Identify your triggers, the most common being running water, the key in the lock coming home, or entering the bathroom. The idea of making less sensitive to your triggers is to approach the trigger in a least delicate state first (i.e. with an empty bladder) and then approach the trigger in gradually increasing periods of time after emptying your bladder.
Tips for success:
- Believe that you will be successful.
- Remember to do your pelvic floor muscle exercises after each voiding.
- Follow the above program directions to the letter.
- Give the program a full six weeks.
- Don’t be discouraged by setbacks. Your bladder control may be worse when:
- a. You are tired.
- b. You have your mind on many other things.
- c. You are tense or nervous.
- d. You are about to start your menstrual period.
- e. You are outside on cold, rainy, or windy days.
- Drink plain water (add lemon). Avoid alcohol, caffeine drinks, and citrus juices.
- Avoid going to the toilet “just in case”.
- Avoid constipation.
- InformedHealth.org [Internet]. Cologne, Germany: Institute for Quality and Efficiency in Health Care (IQWiG); 2006-. Bladder training. 2013 Nov 12 [Updated 2016 Dec 30]. Available from: https://www.ncbi.nlm.nih.gov/books/NBK279430[↩]