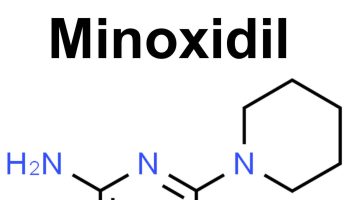
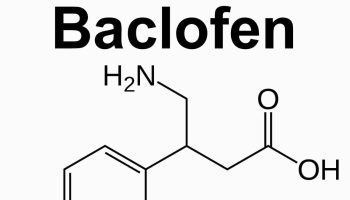
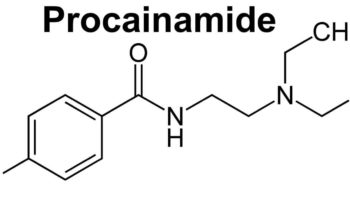
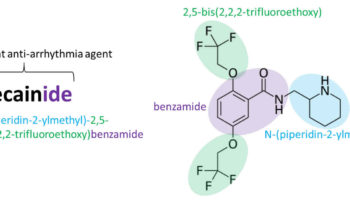
What is Excedrin-Migraine
Excedrin-Migraine is a medicine that contains active ingredients in a combination of Acetaminophen (paracetamol), Aspirin, and Caffeine. Acetaminophen is a pain reliever and a fever reducer. Aspirin is acetylsalicylic acid in a group of drugs called salicylates, classified as a non-steroidal anti-inflammatory drug (NSAID). Aspirin works by reducing substances in your body that cause pain, fever, and inflammation. Caffeine is a central nervous system stimulant. Caffeine relaxes muscle contractions in blood vessels to improve blood flow.
Excedrin-Migraine is used to treat migraine headaches.
Interestingly, the products sold as Excedrin, Excedrin Menstrual and Excedrin Tension Headache contain identical active ingredients even though advertised for different conditions!
- If Excedrin-Migraine isn’t effectively controlling your migraines, your doctor may refer you to a specialist migraine clinic for further investigation and treatment. A specialist may recommend other treatments such as transcranial magnetic stimulation.
- Transcranial magnetic stimulation involves holding a small electrical device to your head that delivers magnetic pulses through your skin. It’s not clear exactly how transcranial magnetic stimulation works in treating migraines, but studies have shown that using it at the start of a migraine can reduce its severity. It can also be used in combination with the medications mentioned above without interfering with them. However, transcranial magnetic stimulation isn’t a cure for migraines and it doesn’t work for everyone. The evidence for its effectiveness isn’t strong and is limited to people who have migraine with aura. There’s also little evidence about the potential long-term effects of the treatment, although studies into the treatment have so far only reported minor and temporary side effects, including:
- slight dizziness
- drowsiness and tiredness
- a muscle tremor that can make it difficult to stand
- irritability
Excedrin-Migraine ingredients
The active ingredients in Excedrin-Migraine are Acetaminophen 250 mg + Aspirin 250 mg + Caffeine 65 mg.
Acetaminophen
Acetaminophen (paracetamol) is a common painkiller used to treat aches and pain. It can also be used to reduce fever (100.4 °F [38 °C] and above).
Acetaminophen (paracetamol) is used to relieve mild to moderate pain from headaches, muscle aches, menstrual periods, colds and sore throats, toothaches, backaches, and reactions to vaccinations (shots), and to reduce fever. Acetaminophen may also be used to relieve the pain of osteoarthritis (arthritis caused by the breakdown of the lining of the joints). Acetaminophen is in a class of medications called analgesics (pain relievers) and antipyretics (fever reducers). It works by changing the way the body senses pain and by cooling the body.
Acetaminophen (paracetamol) is also available combined with other painkillers and anti-sickness medicines. It’s an ingredient in a wide range of cold and flu remedies.
Key facts on Acetaminophen
- Acetaminophen (paracetamol) takes up to an hour to work.
- The usual dose of Acetaminophen (paracetamol) is one or two 500mg tablets at a time.
- Don’t take Acetaminophen (paracetamol) with other medicines containing Acetaminophen (paracetamol).
Who can and can’t take Acetaminophen
Most people can take Acetaminophen (paracetamol) safely, including pregnant and breastfeeding women.
However, some people need to take extra care with Acetaminophen (paracetamol).
Check with your doctor or pharmacist if you:
- have had an allergic reaction to Acetaminophen (paracetamol) or any other medicines in the past
- have liver or kidney problems
- regularly drink more than the maximum recommended amount of alcohol (14 units a week)
- take medicine for epilepsy
- take medicine for tuberculosis (TB)
- take the blood-thinner warfarin and you may need to take Acetaminophen (paracetamol) on a regular basis
Before taking acetaminophen
- tell your doctor and pharmacist if you are allergic to acetaminophen, any other medications, or any of the ingredients in the product. Ask your pharmacist or check the label on the package for a list of ingredients.
- tell your doctor and pharmacist what prescription and nonprescription medications, vitamins, nutritional supplements, or herbal products you are taking or plan to take. Be sure to mention anticoagulants (‘blood thinners’) such as warfarin (Coumadin); isoniazid (INH); certain medications for seizures including carbamazepine (Tegretol), phenobarbital, and phenytoin (Dilantin); medications for pain, fever, coughs, and colds; and phenothiazines (medications for mental illness and nausea). Your doctor may need to change the doses of your medications or monitor you carefully for side effects.
- tell your doctor if you have ever developed a rash after taking acetaminophen.
- tell your doctor if you are pregnant, plan to become pregnant, or are breast-feeding. If you become pregnant while taking acetaminophen, call your doctor.
- if you drink three or more alcoholic beverages every day, do not take acetaminophen. Ask your doctor or pharmacist about the safe use of alcoholic beverages while taking acetaminophen.
- you should know that combination acetaminophen products for cough and colds that contain nasal decongestants, antihistamines, cough suppressants, and expectorants should not be used in children younger than 2 years of age. Use of these medications in young children can cause serious and life-threatening effects or death. In children 2 through 11 years of age, combination cough and cold products should be used carefully and only according to the directions on the label.
- if you have phenylketonuria (PKU, an inherited condition in which a special diet must be followed to prevent mental retardation), you should know that some brands of acetaminophen chewable tablets may be sweetened with aspartame, a source of phenylalanine.
Side effects of Acetaminophen
Acetaminophen (paracetamol) very rarely causes side effects if you take it at the right dosage.
If you’re worried about a side effect or notice anything unusual, talk to your pharmacist or doctor.
Serious allergic reaction
In rare cases, it’s possible to have a serious allergic reaction to Acetaminophen (paracetamol).
If you experience any of the following symptoms, stop taking acetaminophen and call your doctor immediately or get emergency medical attention:
- red, peeling or blistering skin
- rash
- hives
- itching
- swelling of the face, throat, tongue, lips, eyes, hands, feet, ankles, or lower legs
- hoarseness
- difficulty breathing or swallowing
Acetaminophen may cause other side effects. Call your doctor if you have any unusual problems while you are taking this medication.
Cautions with other medicines
It’s safe to take Acetaminophen (paracetamol) with most prescription medicines, including antibiotics.
Acetaminophen (paracetamol) isn’t suitable for some people. Talk to your doctor if you take:
- the blood-thinner warfarin (Acetaminophen (paracetamol) can increase the risk of bleeding if you take it regularly)
- medicine to treat epilepsy
- medicine to treat tuberculosis (TB)
Mixing Acetaminophen (paracetamol) with herbal remedies and supplements
Check with your doctor or pharmacist if you’re taking the herbal medicine St John’s wort for depression as you may need to reduce your Acetaminophen (paracetamol) dose.
Otherwise, Acetaminophen (paracetamol) isn’t generally affected by also taking herbal remedies or supplements.
Acetaminophen Overdose
An overdose of acetaminophen can damage your liver or cause death. If someone takes more than the recommended dose of acetaminophen, get medical help immediately, even if the person does not have any symptoms.
The first signs of an acetaminophen overdose include loss of appetite, nausea, vomiting, stomach pain, sweating, and confusion or weakness. Later symptoms may include pain in your upper stomach, dark urine, and yellowing of your skin or the whites of your eyes.
Symptoms of acetaminophen overdose may include the following:
- nausea
- vomiting
- loss of appetite
- sweating
- extreme tiredness
- unusual bleeding or bruising
- pain in the upper right part of the stomach
- yellowing of the skin or eyes (jaundice)
- flu-like symptoms
Aspirin
Aspirin is also known as acetylsalicylic acid in a class of drug called nonsteroidal anti-inflammatory drugs (NSAIDs) that is similar to non-steroidal inflammatory (NSAIDs) like Ibuprofen (Motrin or Advil) and naproxen (Aleve). Aspirin works by reducing substances in your body that cause pain, fever, and inflammation.
Aspirin can prevent the formation of blood clots which can make it useful in treating or preventing some conditions like heart attacks and strokes. The dosage for aspirin can range from 50 to 6000 milligrams (mg) per day depending on the condition being treated, and aspirin may be used in combination with other medications.
Aspirin is used to treat pain, and reduce fever or inflammation. It is sometimes used to treat or prevent heart attacks, strokes, and chest pain (angina).
Aspirin is a common medicine that has a number of uses, from relieving pain to reducing the risk of serious problems such as heart attacks and strokes.
Aspirin may be harmful to an unborn baby’s heart, and may also reduce birth weight or have other dangerous effects. Tell your doctor if you are pregnant or plan to become pregnant while you are taking Excedrin-Migraine.
Aspirin can be used to treat:
- Mild to moderate pain
- Fever
- Swollen, red and tender body tissues
- Rheumatoid arthritis
- Rheumatic fever 1
It is also used in the prevention of blood clots, heart attacks, strokes and bowel cancer 1.
Aspirin should be used for cardiovascular conditions only under the supervision of a doctor.
Uses for aspirin
At high doses – usually 300mg – aspirin can relieve pain, reduce a high temperature (fever) and reduce swelling.
Aspirin is often used for short-term relief from:
- headaches and migraines
- toothache
- period pains
- general aches and pains
- colds and flu
Long-term treatment with low doses of aspirin – usually 75mg – has an antiplatelet effect, which means it makes the blood less sticky and can stop blood clots developing.
A doctor may recommend low doses of aspirin (75mg) if you have or have had:
- a heart attack or angina
- a stroke or transient ischemic attack (TIA)
- peripheral arterial disease
- coronary artery bypass surgery or another operation on your heart or blood vessels
Aspirin may also be prescribed for children after heart surgery or to treat Kawasaki disease. But it shouldn’t be given to anyone under 16 years old without medical supervision.
Who can and can’t take Aspirin
Most people can take aspirin safely. But you should get advice from a pharmacist or doctor before taking it if you:
- have had an allergic reaction to aspirin or non-steroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen, in the past
- have asthma
- have had stomach ulcers in the past
- have severe liver or kidney problems
- have hemophilia or another bleeding disorder
- have uncontrolled high blood pressure
- are looking for medication for a child under 16 – medication containing aspirin shouldn’t be given to children under 16
- are over 65 years of age
- are pregnant, breastfeeding or trying to get pregnant
- are taking other medications
You may still be able to take aspirin in these cases, but you should only do so if advised that it’s safe by a healthcare professional.
If you can’t take aspirin, a different medicine, such as paracetamol (for pain) or clopidogrel (to prevent blood clots), may be recommended instead.
Before taking aspirin
- tell your doctor and pharmacist if you are allergic to aspirin, other medications for pain or fever, tartrazine dye, or any other medications.
- tell your doctor and pharmacist what prescription and nonprescription medications, vitamins, nutritional supplements, and herbal products you are taking or plan to take. Be sure to mention any of the following: acetazolamide (Diamox); angiotensin-converting enzyme (ACE) inhibitors such as benazepril (Lotensin), captopril (Capoten), enalapril (Vasotec), fosinopril (Monopril), lisinopril (Prinivil, Zestril), moexipril (Univasc), perindopril, (Aceon), quinapril (Accupril), ramipril (Altace), and trandolapril (Mavik); anticoagulants (‘blood thinners’) such as warfarin (Coumadin) and heparin; beta blockers such as atenolol (Tenormin), labetalol (Normodyne), metoprolol (Lopressor, Toprol XL), nadolol (Corgard), and propranolol (Inderal); diuretics (‘water pills’); medications for diabetes or arthritis; medications for gout such as probenecid and sulfinpyrazone (Anturane); methotrexate (Trexall); other nonsteroidal anti-inflammatory drugs (NSAIDs) such as naproxen (Aleve, Naprosyn); phenytoin (Dilantin); and valproic acid (Depakene, Depakote). Your doctor may need to change the doses of your medications or monitor you more carefully for side effects.
- if you are taking aspirin on a regular basis to prevent heart attack or stroke, do not take ibuprofen (Advil, Motrin) to treat pain or fever without talking to your doctor. Your doctor will probably tell you to allow some time to pass between taking your daily dose of aspirin and taking a dose of ibuprofen.
tell your doctor if you have or have ever had asthma, frequent stuffed or runny nose, or nasal polyps (growths on the linings of the nose). If you have these conditions, there is a risk that you will have an allergic reaction to aspirin. Your doctor may tell you that you should not take aspirin. - tell your doctor if you often have heartburn, upset stomach, or stomach pain and if you have or have ever had ulcers, anemia, bleeding problems such as hemophilia, or kidney or liver disease.
- tell your doctor if you are pregnant, especially if you are in the last few months of your pregnancy, you plan to become pregnant, or you are breast-feeding. If you become pregnant while taking aspirin, call your doctor. Aspirin may harm the fetus and cause problems with delivery if it is taken during the last few months of pregnancy.
- if you are having surgery, including dental surgery, tell the doctor or dentist that you are taking aspirin.
- if you drink three or more alcoholic drinks every day, ask your doctor if you should take aspirin or other medications for pain and fever.
How to take aspirin
Your pharmacist or doctor can tell you how often to take your aspirin and how much you should take. You can also check the recommendations in the leaflet that comes with your medicine.
Generally speaking:
- high-dose aspirin (to relieve pain) can be taken three or four times a day, with at least four hours between each dose, until your symptoms improve
- low-dose aspirin (to prevent blood clots) is taken once a day, usually for the rest of your life
Some medicine leaflets advise taking aspirin with water, while others may recommend taking it before or after food.
Follow the instructions in the leaflet or label that comes with your medicine. Ask your pharmacist if you’re not sure.
Aspirin interactions with other medicines, food and alcohol
Aspirin can potentially interact with other medications, including some complementary and herbal medicines, which could alter their effects or increase your risk of side effects.
Medicines that can interact with aspirin include:
- NSAIDs – such as ibuprofen or naproxen
- steroid medication – such as prednisolone
- anticoagulant medicines – such as warfarin or heparin
- SSRI antidepressants – such as citalopram, fluoxetine or paroxetine
- some medications used to treat high blood pressure – such as ACE inhibitors or diuretics
- some medicines used to treat epilepsy – such as phenytoin
- other medicines containing aspirin – including cold and flu remedies where aspirin is one of the ingredients
Taking aspirin with warfarin (anticoagulant medicine or blood thinner) or some blood pressure medicines may increase the risk of bleeding.
This is not a complete list. If you want to check whether a medicine is safe to take with aspirin, ask your doctor or pharmacist, or read the leaflet that comes with the medicine.
There are no known interactions between aspirin and food.
The risk of bleeding in the stomach may be higher if you drink alcohol while taking aspirin, so you may want to consider reducing how much you drink or avoiding alcohol completely.
Side effects of aspirin
Like all medications, there’s a risk of side effects from aspirin.
The most common side effects are:
- Indigestion and stomach aches – taking your medicine with food may help reduce this risk
- Bleeding or bruising more easily than normal
Other side effects of aspirin:
- Dizziness, ringing in the ears, blurred vision
- Drowsiness, fatigue, depression
- Thirst, sweating, fluid retention, swollen ankles
- Abdominal discomfort or bloating
- Nausea, heartburn, diarrhea, constipation
Uncommon and rare side effects include:
- hives – a raised, itchy rash
- tinnitus – hearing sounds that come from inside your body
- breathing difficulties or an asthma attack
- an allergic reaction – this can cause breathing problems, swelling of the mouth, lips or throat, and a sudden rash
- bleeding in the stomach – this can cause dark, tar-like stools or vomiting blood
- bleeding in the brain – this can cause a sudden, severe headache, vision problems and stroke symptoms, such as slurred speech and weakness on one side of the body
Long-term effects of taking aspirin:
Regular use of aspirin may eventually cause the following effects. It’s best to discuss the side effects of long term use with a medical practitioner.
- Anemia (low red blood cell count)
- Easy bruising and abnormal bleeding
- Inflamed stomach lining, stomach bleeding and peptic ulcers
- Vomiting blood that may look like coffee grounds and bowel motions that look like black tar
- An allergic-type reaction, wheezy breathing and a tightness in the chest in adults, hives in children, and in some rare cases swelling of the face, lips, tongue or around the eyes
- Reduced kidney and liver function
Speak to your doctor if you experience any concerning or troublesome side effects while taking aspirin.
Call your emergency number for an ambulance or go to your nearest accident and emergency (A&E) department if you think you’re having a severe allergic reaction, or you have symptoms of bleeding in your stomach or brain.
Aspirin Overdose
If the dose is too high, you might overdose. If you have any of these symptoms, call an ambulance straight away by dialing your local emergency number.
- Headaches
- Confusion
- Fever
- Deafness
- Vomiting
- Rapid and shallow breathing
- Seizures
- Stop breathing, coma and death
- Burning pain in the throat or stomach
- Decreased urination
- Restlessness
- Irritability
- Talking a lot and saying things that do not make sense
- Fear or nervousness
- Dizziness
- Double vision
- Uncontrollable shaking of a part of the body
- Abnormally excited mood
- Hallucination (seeing things or hearing voices that are not there)
- Drowsiness
- Loss of consciousness for a period of time
Caffeine
Caffeine is a stimulant drug, which means it speeds up the messages traveling between the brain and your body.
It’s found in the seeds, nuts and leaves of a number of different plants, including:
- Coffea Arabica (used for coffee)
- Camelia sinensis (used for tea)
- Cola acuminate (used as a nut, tea or in soft drinks including cola)
- Theobroma cacao (used in cocoa and chocolate)
- Paulinia cupana (used as guarana in snack bars and energy drinks)
Caffeine is used in a number of different products. The amount of caffeine in these products can vary dramatically, so it’s always best to check the label. The average amounts are listed below.
- 2 tablets of Excedrin-Migraine = 130mg caffeine
The table below shows the amount of caffeine in common food and drinks. The caffeine amounts are averages, so they may change depending on the brand or how the food or drink is made. Check the package label on food and drinks to know how much caffeine they contain.
The amount of caffeine in foods and drinks varies a lot. For coffee and tea, the amount of caffeine depends on:
- The brand
- How it’s prepared
- The type of beans or leaves used
- The way it’s served (for example, as espresso or latte)
- The size of the cup. Not all coffee cups are the same size, even though you think of them as a cup. Check to see how many ounces your cup has, especially if you’re buying a cup of coffee or tea. If you’re making coffee or tea at home, measure to check the size of the cup.
Table 1. The amount of Caffeine used in a number of different products (approximates only)
| Product | Average caffeine content (mg/100 ml) |
|---|---|
| Red Bull® | 32.0 |
| Mountain Dew® | 15.0 |
| Coca Cola® | 9.7* |
| Diet Coke® | 9.7* |
| Coke Zero® | 9.6* |
| Brewed black tea | 22.5 |
| Brewed green tea | 12.1 |
| Coffee, cappuccino | 101.9 |
| Coffee, flat white | 86.9 |
| Coffee, long black | 74.7 |
| Coffee, from ground coffee beans, espresso style | 194.0 |
| Chocolate, milk with added milk solids | 20.0 |
| Chocolate, dark, high cocoa solids | 59.0 |
Some energy drinks contain large amounts of caffeine. For example, a 24-ounce energy drink may have up to 500 milligrams of caffeine. Energy drinks may have a lot of sugar, too, and they may contain ingredients that may be harmful to your baby during pregnancy. Because we don’t know a lot about all the ingredients in energy drinks, it’s best not to have them when you’re pregnant.
The amount of caffeine you get from food and drinks throughout the day adds up. So if you have a cup of coffee in the morning, you may want to limit or give up having other food and drinks during the day that have caffeine.
Effects of caffeine
Caffeine’s main effect is making people feel more awake for a short time. Caffeine aids the release of acid in the stomach, which can result in an upset stomach. Caffeine also helps get rid of fluids from the body (a diuretic).
There is no safe level of drug use. Use of any drug always carries some risk. It’s important to be careful when taking any type of drug.
Caffeine affects everyone differently, based on:
- Size, weight and health
- Whether the person is used to taking it
- Whether other drugs are taken around the same time
- The amount taken
The following effects may be experienced between 5 to 30 minutes after consuming caffeine, and may continue for up to 12 hours:
- Feeling more alert and active
- Restlessness, excitability and dizziness
- Anxiety and irritability
- Dehydration and needing to urinate more often
- Higher body temperature
- Faster breathing and heart rate
- Headache and lack of concentration
- Stomach pains 3
Children and young people who consume energy drinks containing caffeine may also suffer from sleep problems, bed-wetting and anxiety 4.
I am trying to become pregnant. Is it true that drinking caffeinated beverages will lower my chance to become pregnant?
Results from studies have been mixed. Some studies have suggested that high levels of caffeine (more than 300mg/day) might make it harder to conceive, but these findings are not proven. Low (less than 200mg/day) to moderate (about 200-300mg/day) caffeine consumption probably does not make it harder for a woman to get pregnant.
How does caffeine affect you and your baby during pregnancy?
Caffeine slightly increases your blood pressure and heart rate and the amount of urine your body makes. Caffeine may cause you to feel jittery, have indigestion or have trouble sleeping. During pregnancy, you may be especially sensitive to caffeine because it may take you longer to clear it from your body than if you weren’t pregnant.
When you have caffeine during pregnancy, it passes through the placenta to your baby. The placenta grows in your uterus (womb) and supplies the baby with food and oxygen through the umbilical cord.
You may have heard that too much caffeine can cause miscarriage (when a baby dies in the womb before 20 weeks of pregnancy). Some studies say this is true, and others don’t. Until scientists know more about how caffeine can affect pregnancy, it’s best to limit the amount you get to 200 milligrams each day. This is about the amount in 2 x 8-ounce cups of coffee or one 12-ounce cup of coffee. Be sure to check the size of your cup to know how much caffeine you’re getting.
Can caffeine cause or make it more likely to have a miscarriage?
There are many studies that have looked at this question. To date, researchers have not reported an association between low levels of caffeine and an increased risk for miscarriage. Most studies on moderate use of caffeine have not found an increased risk of miscarriage. Some studies suggest that taking very high levels (over 800 mg per day) or taking it in high doses with cigarettes or alcohol (both of which are known to increase the risk of miscarriage) may increase the risk for miscarriage.
Will drinking caffeinated beverages during my pregnancy cause birth defects in my baby?
No. Large amounts of caffeine have not been shown to cause an increased chance for birth defects.
Large amounts of caffeine could affect babies in the same way as it does adults. Some reports suggest that children born to mothers who consumed more than 500mg/day were more likely to have faster heart rates, shaking, increased breathing rate, and spend more time awake in the days following birth.
Does drinking caffeinated beverages in pregnancy cause long-term problems in behavior or learning for the baby?
Most studies find no effect on learning or behavior in young school aged children whose mothers consumed caffeine during pregnancy.
Can I drink caffeinated beverages while I breastfeed?
Caffeine passes into breast milk and it suggested that you limit how much you have. If you’re breastfeeding, limit caffeine to no more than two cups of coffee a day. The infant should also be watched for irritability and trouble with sleeping. It’s important to keep drinking water while breastfeeding. Be sure to talk to your health care provider about all your options for breastfeeding.
Is it a problem if the baby’s father consumes a lot of caffeine?
Studies on caffeine and male fertility or sperm quality have not reported consistent findings. In general, exposures that fathers have are unlikely to increase risks to a pregnancy.
Coming down
Some people consume drinks with caffeine so that they can continue working or studying at night. However, the after-effect is that they will feel tired and lethargic the next day.
Long-term effects of taking caffeine
Regular, heavy use of caffeine (such as more than 4 cups of coffee a day) may eventually cause:
- Osteoporosis
- High blood pressure and heart disease
- Heartburn
- Ulcers
- Difficulty sleeping
- Infertility (in men and women)
- Anxiety
- Depression
- Needing to use more to get the same effect
- Dependence on caffeine 5
Caffeine Withdrawal
Giving up caffeine after using it for a long time is challenging because the body has to get used to functioning without it. Withdrawal symptoms usually start within 24 hours after the last dose – or even within 6 hours for people who consume a lot of caffeine regularly. The symptoms can last for around 36 hours, or even longer for people who consume a lot.
These symptoms can include:
- Headache
- Tiredness
- Sweating
- Muscle pains
- Anxiety and tension 6
Caffeine Overdose
If a large amount of caffeine is consumed it could also cause an overdose. If you experience any of the following effects, call an ambulance straight away by dialing your local emergency number.
- Tremors
- Nausea and vomiting
- Very fast and irregular heart rate
- Confusion and panic attack
- Seizures 7
It’s possible to die from having too much caffeine, but this is extremely rare. This would usually only happen if 5–10g of caffeine (or 80 cups of strong coffee) were consumed one after the other 5.
In small children, caffeine poisoning can happen if a lower amount, such as around 1g of caffeine (equal to around 12 energy drinks) is consumed one after the other 8.
How much caffeine in Excedrin-Migraine
- Excedrin-Migraine: Acetaminophen 250mg + Caffeine 65 mg + Aspirin 250mg
- Excedrin Tension Headache: Acetaminophen 500mg + Caffeine 65 mg
- Excedrin Extra Strength: Acetaminophen 250 mg + Caffeine 65 mg + Aspirin 250 mg
In comparison a typical 8 ounce (236 ml) serving of brewed coffee contains at least 95-100mg of caffeine.
If you’re pregnant, limit the amount of caffeine you have to 200 milligrams (mg) a day. This is about the same as 2 x 8 ounce (236 ml) of instant coffee.
High levels of caffeine in pregnancy can result in babies having a low birthweight, which can increase the risk of health problems in later life. Too much caffeine can also cause a miscarriage.
Taking Excedrin-Migraine with other painkillers
It’s safe to take Excedrin-Migraine with acetaminophen or codeine.
But don’t take Excedrin-Migraine with similar painkillers like aspirin or naproxen (Aleve) without talking to a doctor.
Excedrin-Migraine, aspirin and naproxen belong to the same group of medicines called non-steroidal anti-inflammatory drugs (NSAIDs). If you take them together, Excedrin-Migraine plus aspirin or naproxen may increase the chance of you getting side effects like stomach ache.
Alternatives to Excedrin-Migraine
For treating migraine, an alternative to Excedrin-Migraine is acetaminophen (Tylenol).
For migraine pain, ask your doctor or pharmacist for an alternative if Excedrin-Migraine is not suitable for you. Your health professional may suggest you try:
- Acetaminophen (paracetamol)
- Another medicine from the NSAID family
- A medicine that combines codeine with acetaminophen in the same tablet.
If your pain is severe, your doctor may prescribe you a stronger pain reliever or recommend another treatment, such as triptans or ergots.
Ergotamine and caffeine combination drugs (Migergot, Cafergot) are less effective than triptans. Ergots seem most effective in those whose pain lasts for more than 48 hours. Ergots are most effective when taken soon after migraine symptoms start.
Ergotamine may worsen nausea and vomiting related to your migraines, and it may also lead to medication-overuse headaches.
Dihydroergotamine (D.H.E. 45, Migranal) is an ergot derivative that is more effective and has fewer side effects than ergotamine. It’s also less likely to lead to medication-overuse headaches. It’s available as a nasal spray and in injection form.
Treating migraine without medicine
The following non-medicine treatments may help you to prevent frequent or troublesome migraines — you can use them either instead of, or as well as, medicine treatments:
- physical therapies (e.g., physiotherapy or chiropractic treatment), especially if neck problems are thought to be contributing to your migraines — it’s essential to seek out a therapist with specialist training in this area, however, as there have been very rare reports of stroke after spinal manipulation of the neck
- physical exercise
- relaxation training (e.g., yoga, meditation), which can help manage underlying problems with stress
- cognitive behavioral therapy (CBT), a psychological therapy that teaches you to identify and challenge stress generating thoughts
- acupuncture. If medication is unsuitable, or it doesn’t help to prevent migraines, you may want to consider acupuncture.
Medicines for an acute migraine attack
There’s currently no cure for migraines, although a number of treatments are available to help ease the symptoms.
Most people find that sleeping or lying in a darkened room is the best thing to do when having a migraine attack.
Others find that eating something helps, or they start to feel better once they’ve been sick.
It may take time to work out the best treatment for you. You may need to try different types or combinations of medicines before you find the most effective ones.
Doctors recommend a stepped approach to treatment for acute migraine attack; that is, trying the simplest remedy first. If this fails to manage your pain — as a general rule on 3 consecutive occasions — then you should try the next treatment.
- Step 1. Simple pain relief medicine alone
Most simple pain relief medicines are available to buy over-the-counter in pharmacies and supermarkets.
Many people who have migraines find that over-the-counter painkillers, such as acetaminophen (Tylenol), aspirin and ibuprofen (Advil, Advil-Migraine or Motrin IB), can help to reduce their symptoms.
They tend to be most effective if taken at the first signs of a migraine attack, as this gives them time to absorb into your bloodstream and ease your symptoms.
It’s not advisable to wait until the headache worsens before taking painkillers as it’s often too late for the medication to work. Soluble painkillers (tablets you dissolve in a glass of water) like Advil-Migraine are a good alternative because they’re absorbed quickly by your body.
If you can’t swallow painkillers because of nausea or vomiting, suppositories may be a better option. These are capsules that are inserted into the anus (back passage).
Take pain relief medicine at the first sign of migraine symptoms. As a migraine progresses, your stomach emptying can slow and this can affect the absorption of pain relievers into your bloodstream, making them less effective. This is especially important if you experience nausea and vomiting with migraine.
- Step 2. Simple pain reliever and medicine for nausea and vomiting
If nausea is a problem, or if a pain reliever alone does not relieve your migraine pain, you can take the pain reliever with medicine to treat nausea and vomiting.
Medication for nausea is usually combined with other medications. Frequently prescribed medications are chlorpromazine, metoclopramide (Reglan) or prochlorperazine (Compro).
- Step 3. Anti-migraine medicine: the triptans
If you find you can’t manage your migraines using over-the-counter medicines, your doctor may prescribe something stronger.
Triptans work differently to pain relievers. Triptan medicines are a specific painkiller for migraine headaches. There are a number of different triptans available in the US and you will need to get a prescription from your doctor.
Triptans are thought to work by reversing the changes in the brain that may cause migraine headaches.
They cause the blood vessels around the brain to contract (narrow). This reverses the dilating (widening) of blood vessels that’s believed to be part of the migraine process.
Triptans are available as tablets, injections and nasal sprays.
Common side effects of triptans include:
- warm-sensations
- tightness
- tingling
- flushing
- feelings of heaviness in the face, limbs or chest
Some people also experience nausea, dry mouth and drowsiness. These side effects are usually mild and improve on their own.
As with other painkillers, taking too many triptans can lead to medication overuse headache.
Your doctor will usually recommend having a follow-up appointment once you’ve finished your first course of treatment with triptans. This is so you can discuss their effectiveness and whether you had any side effects.
If the medication was helpful, treatment will usually be continued. If they weren’t effective or caused unpleasant side effects, your doctor may try prescribing a different type of triptan since responses can be highly variable.
- Step 4. Preventive therapy
If you are experiencing two or more severe migraine attacks a month, you could be a candidate for preventive therapy. Preventive therapy is used in addition to treatments for acute attack, not in place of it.
The aim of migraine preventive therapy is to reduce the number of attacks to a manageable level, either because:
- the medicines used to treat attacks don’t control your symptoms adequately, or
- migraine attacks, even though well controlled, are happening far too often, placing you at risk of developing medication overuse headache.
Note that it may take some months for the full effect of preventive therapy to be seen.
In general, medicines used as preventive therapy are more commonly prescribed for the treatment of other conditions (eg, high blood pressure or depression) but have unrelated anti-migraine effects — for example:
- beta-blockers — Propranolol (Deralin), atenolol (Noten, Anselol), metoprolol (Betaloc, Lopressor)
- amitriptyline (Endep).
Other medicines occasionally used to prevent migraines include antiepileptic medicines (especially sodium valproate [Epilim, Valpro] and topiramate [Epiramax, Tamate]), methysergide (Deseril) and botulinum toxin (botox).
Treatment can be complicated and is best managed by a specialist (neurologist).
Excedrin-Migraine Important Information
Do not give Excedrin-Migraine to a child or teenager with a fever, flu symptoms, or chicken pox. Aspirin can cause Reye’s syndrome, a serious and sometimes fatal condition in children.
Do not take more Excedrin-Migraine than is recommended. An overdose of acetaminophen can damage your liver or cause death. Call your doctor at once if you have nausea, pain in your upper stomach, itching, loss of appetite, dark urine, clay-colored stools, or jaundice (yellowing of your skin or eyes).
Aspirin may cause stomach or intestinal bleeding, which can be fatal. Call your doctor at once if you have symptoms such as bloody or tarry stools, or coughing up blood or vomit that looks like coffee grounds.
In rare cases, acetaminophen may cause a severe skin reaction. Stop taking Excedrin-Migraine and call your doctor right away if you have skin redness or a rash that spreads and causes blistering and peeling.
Excedrin-Migraine Pregnancy Warnings
Two cases of acetaminophen overdose in late pregnancy have been reported. In both cases neither the neonate nor the mother suffered hepatic toxicity 9.
Investigations have revealed conflicting results with regards to the pharmacokinetic disposition of acetaminophen in pregnant women 10, 11. One study has suggested that the oral clearance of acetaminophen is 58% higher and the elimination half-life is 28% longer in pregnant women compared to nonpregnant women 10. Another study has suggested that the elimination half-life is not different in patients who are pregnant. That study also suggested that the volume of distribution of acetaminophen may be higher in pregnant women 12.
One study has suggested that acetaminophen in typical oral doses may result in a reduced production of prostacyclin in pregnant women 13. That study also suggested that acetaminophen does not affect thromboxane production.
The frequency of fetal exposure to aspirin reported in many studies may be underestimated because aspirin (and other salicylates) occur in many over-the-counter preparations and women may fail to recall taking aspirin and over-the-counter drugs 14.
Increased maternal bleeding can occur during delivery when aspirin is used 1 week prior to and/or during labor and delivery 15, 16, 17. Prolonged gestation and labor have been reported due to aspirin’s inhibition of prostaglandin.
A study 18 of the use of low-dose aspirin (60 mg per day) to prevent and treat preeclampsia in 9364 pregnant women (the Collaborative Low-dose Aspirin Study in Pregnancy–CLASP) did “not support routine prophylactic or therapeutic administration of antiplatelet therapy in pregnancy to all women at increased risk of preeclampsia or IUGR.” In that study, no excess of intraventricular hemorrhage, neonatal bleeds, or mortality attributable to bleeding were observed. The investigators did identify a possible role for low-dose aspirin in the treatment of early-onset preeclampsia severe enough to need very preterm delivery.
Another study 19 of low-dose aspirin (follow-up from the Italian Study of Aspirin in Pregnancy) has suggested that “low dose aspirin in pregnancy is safe with respect to the risks of malformation and of major impairment in development at 18 months of age.”
High-dose aspirin (2 g per day) has been associated with stillbirths, cerebral hemorrhage, oculoauriculovertebral dysplasia, neonatal salicylate toxicity, constricted ductus arteriosus, cyclopia, and neonatal acidosis. Some cases of congenital heart defects have been reported 19, 15. However, a case control study of aspirin use in the first trimester concluded that aspirin “does not increase the risk of congenital heart defects in relation to that of other structural malformations”.
In a study of 2817 fertile women, no evidence of adverse effects from caffeine was found. The fecundability ratio (adjusted for known risk factors for time to conceive) was 1.03 between fertile women who consumed more than 7000 mg caffeine per month and those who consumed 500 mg or less per month. Furthermore, caffeine was not associated with infertility in 1818 infertile women and their primiparous controls. In another study (n=441) no evidence was found that moderate caffeine use increased the risk of spontaneous abortion, intrauterine growth retardation, or microcephaly.
Aspirin has been assigned to pregnancy category C by the FDA. However, aspirin is considered to be in pregnancy category D by the FDA if full dose aspirin is taken in the third trimester. Use of nonsteroidal anti-inflammatory drugs during the third trimester of pregnancy should be avoided due to effects on the fetal cardiovascular system (closure of the ductus arteriosus). Aspirin use in pregnancy has been associated with alterations in both maternal and fetal hemostasis. In addition, high doses have been associated with increased perinatal mortality, intrauterine growth retardation, and teratogenic effects.
Acetaminophen has not been formally assigned to pregnancy category by the FDA. It is routinely used for short-term pain relief and fever in all stages of pregnancy. Acetaminophen is believed to be safe in pregnancy when used intermittently for short durations.
Caffeine has been assigned to pregnancy category B by the FDA. Both human and animal studies have failed to reveal evidence of significant mutagenic or carcinogenic effects. Caffeine crosses the placenta. Fetal blood and tissue levels in the fetus are similar to those in the mother. Caffeine has been reported to be an animal teratogen only with doses high enough to cause toxicity in the mother. In 1980, the Food and Drug Administration issued an advisory (based primarily on animal evidence) which stated that pregnant women should limit there intake of caffeine to a minimum. During the first two trimesters of pregnancy, the combination of acetaminophen, aspirin, and caffeine should only be given during pregnancy when clearly needed and when benefit outweighs risk. Because of the aspirin component of this combination drug, during the last trimester of pregnancy, this combination product is only recommended for use when there are no alternatives and benefits outweigh risk.
Excedrin-Migraine Breastfeeding Warnings
One small study has reported that following a 1000 mg dose of acetaminophen to nursing mothers, nursing infants receive less than 1.85% of the weight-adjusted maternal oral dose 20.
Aspirin is excreted into human milk in small amounts 21, 22. Peak milk salicylate levels have been reported at nine hours after maternal dosing (and measured at 1.1 mg/dL). Use of large doses of aspirin can result in rashes, platelet abnormalities, and bleeding in nursing infants. Because of a single case report of metabolic acidosis, the American Academy of Pediatrics 23 characterizes aspirin as a drug that has been “associated with significant effects on some nursing infants and should be given to nursing mothers with caution.”
Acetaminophen is excreted into human milk in small concentrations 21. One case of a rash has been reported in a nursing infant. Acetaminophen is considered compatible with breast-feeding by the American Academy of Pediatrics.
Caffeine is excreted into human milk in small amounts 24. Adverse effects in the nursing infant are unlikely. However, irritability and poor sleep patterns have been reported in nursing infants. The amount of caffeine generally found in caffeinated beverages is considered to usually be compatible with breast-feeding by the American Academy of Pediatrics. Because caffeine is excreted into human milk and because caffeine is metabolized slowly by nursing infants, consumption of more than moderate levels of caffeine by nursing mothers is not recommended.
Before taking Excedrin-Migraine Precautions
Do not give Excedrin-Migraine to a child or teenager with a fever, flu symptoms, or chicken pox. Aspirin can cause Reye’s syndrome, a serious and sometimes fatal condition in children.
You should not use Excedrin-Migraine if you are allergic to acetaminophen (Tylenol), aspirin, caffeine, or any NSAIDs (Advil, Motrin, Aleve, Orudis, Indocin, Lodine, Voltaren, Toradol, Mobic, Relafen, Feldene, and others).
Aspirin may cause stomach or intestinal bleeding, which can be fatal. These conditions can occur without warning while you are taking Excedrin-Migraine.
Ask a doctor or pharmacist if it is safe for you to take Excedrin-Migraine if you have other medical conditions, especially:
- liver disease, cirrhosis, a history of alcoholism, or if you drink more than 3 alcoholic beverages per day;
- asthma or seasonal allergies;
- fever with a stiff neck;
- stomach ulcer, stomach or intestinal bleeding, ulcerative colitis;
- a bleeding or blood clotting disorder such as hemophilia;
- kidney disease; or
- if you use medicine to treat glaucoma or prevent blood clots.
If you take Excedrin-Migraine to treat headache pain, seek medical attention if you have:
- a headache so bad you have to lie down;
- a headache that causes vomiting;
- what feels like the worst headache you’ve ever had;
- a headache that seems different from your usual headaches;
- a headache every day;
- a headache after coughing, bending, exercising, or head injury;
- if you have never had migraines diagnosed by a doctor; or
- if you are having your first headache after age 50.
Aspirin may be harmful to an unborn baby’s heart, and may also reduce birth weight or have other dangerous effects. Tell your doctor if you are pregnant or plan to become pregnant while you are taking Excedrin-Migraine.
Aspirin, acetaminophen, and caffeine can pass into breast milk and may harm a nursing baby. You should not breast-feed while using Excedrin-Migraine.
How should I take Excedrin-Migraine?
Use Excedrin-Migraine exactly as directed on the label, or as it has been prescribed by your doctor. Do not take more of this medication than is recommended. An overdose of acetaminophen can damage your liver or cause death.
Take Excedrin-Migraine with food or milk if it makes your stomach upset.
Call your doctor if your symptoms do not improve after 7 days of treatment, or if you have a fever lasting longer than 3 days, or any swelling or pain lasting longer than 10 days.
This medication can cause unusual results with certain lab tests for glucose (sugar) in the urine. Tell any doctor who treats you that you are using Excedrin-Migraine.
If you need surgery, tell the surgeon ahead of time that you are using Excedrin-Migraine. You may need to stop using the medicine for a short time.
Store Excedrin-Migraine at room temperature away from moisture and heat.
What should I avoid?
Avoid drinking alcohol while you are taking Excedrin-Migraine. Alcohol may increase your risk of stomach bleeding while taking aspirin, or liver damage while taking acetaminophen.
Ask a doctor or pharmacist before using any other cough, cold, allergy, pain, menstrual symptom, or fever medication. Acetaminophen (paracetamol) is contained in many combination medicines. Taking certain products together can cause you to get too much acetaminophen which can lead to a fatal overdose. Aspirin and caffeine are also contained in many combination medicines. Check the label to see if a medicine contains acetaminophen (paracetamol), aspirin, or caffeine.
Avoid taking another NSAID (nonsteroidal anti-inflammatory drug) such as aspirin, ibuprofen (Advil, Motrin), naproxen (Aleve), celecoxib, diclofenac, indomethacin, meloxicam, and others.
Avoid coffee, tea, cola, energy drinks or other sources of caffeine while taking Excedrin-Migraine. They can add to the side effects of the caffeine in the medication.
What happens if I miss a dose?
Since Excedrin-Migraine is used when needed, you may not be on a dosing schedule. If you are on a schedule, use the missed dose as soon as you remember. Skip the missed dose if it is almost time for your next scheduled dose. Do not use extra medicine to make up the missed dose.
Excedrin-Migraine dosage
Excedrin Migraine Caplets or Geltabs
Active ingredients: Acetaminophen 250 mg + Caffeine 65 mg + Aspirin 250 mg [a Non-Steroidal Anti-Inflammatory Drug (NSAID)]
Inactive Ingredients: benzoic acid, carnauba wax, FD&C blue #1, hydroxypropylcellulose, hypromellose, light mineral oil, microcrystalline cellulose, polysorbate 20, povidone, propylene glycol, simethicone emulsion, sorbitan monolaurate, stearic acid, titanium dioxide
Excedrin migraine Migraine uses:
- Treats Migraines
Excedrin migraine Migraine Directions of Use:
- Do not use more than directed. If symptoms persist or worsen, ask your doctor
- Drink a full glass of water with each dose
- Adults: Take 2 caplets with a glass of water. Do not take more than 2 caplets in 24 hours, unless directed by a doctor.
- Under 18 years of age: Ask a doctor
Keep out of reach of children.
In case of overdose, get medical help or contact a Poison Control Center right away. Quick medical attention is critical for adults as well as for children even if you do not notice any signs or symptoms.
Other information:
- store at at room temperature 20°-25°C (68°-77°F)
- close cap tightly after use
- read all product information before using. Keep box for important information
Excedrin-Migraine Warnings
Reye’s syndrome
Children and teenagers who have or are recovering from chicken pox or flu-like symptoms should not use this product. When using this product, if changes in behavior with nausea and vomiting occur, consult a doctor because these symptoms could be an early sign of Reye’s syndrome, a rare but serious illness.
Medication overuse headache warning
Headaches may worsen if this product is used for 10 or more days per month.
Allergy alert
Acetaminophen may cause severe skin reactions.
Symptoms may include:
- skin reddening
- blisters
- rash
If a skin reaction occurs, stop use and seek medical help right away.
Allergy alert
Aspirin may cause a severe allergic reaction which may include:
- hives
- facial swelling
- asthma (wheezing)
- shock
Ask a doctor or pharmacist before use if:
- you are pregnant or breastfeeding. It is especially important not to use aspirin during the last 3 months of pregnancy unless definitely directed to do so by a doctor because it may cause problems in the unborn child or complications during delivery.
- you are taking a prescription drug for diabetes, gout, or arthritis
- you are taking any other drug, or are under a doctor’s care for any serious condition
- taking any other product that contains aspirin, acetaminophen, or any other pain reliever/fever reducer
Ask a doctor before use if:
- you have never had migraines diagnosed by a health professional
- you have a headache that is different from your usual migraines
- you have the worst headache of your life
- you have fever and stiff neck
- you have headaches beginning after or caused by head injury, exertion, coughing or bending
- you experienced your first headache after the age of 50
- you have daily headaches
- you have a migraine so severe as to require bed rest
- you have liver disease
- stomach bleeding warning applies to you
- you have a history of stomach problems, such as heartburn
- you have high blood pressure, heart disease, liver cirrhosis, or kidney disease
- you are taking a diuretic
- you have asthma
- you have problems or serious side effects from taking pain relievers or fever reducers
- you have vomiting with your migraine headache
Liver warning
This product contains acetaminophen. Severe liver damage may occur if you take:
- more than 2 caplets in 24 hours, which is the maximum daily amount
- with other drugs containing acetaminophen
- 3 or more alcoholic drinks every day while using this product
Stomach bleeding warning
This product contains an NSAID, which may cause severe stomach bleeding. The chance is higher if you:
- are age 60 or older
- have had stomach ulcers or bleeding problems
- take a blood thinning (anticoagulant) or steroid drug
- take other drugs containing prescription or nonprescription NSAlDs (aspirin, ibuprofen, naproxen, or others)
- have 3 or more alcoholic drinks every day while using this product
- take more or for a longer time than directed
Do NOT use:
- if you have ever had an allergic reaction to acetaminophen, aspirin or any other pain reliever/fever reducer
- with any other drug containing acetaminophen (prescription or nonprescription). If you are not sure whether a drug contains acetaminophen, ask a doctor or pharmacist.
Caffeine warning
The recommended dose of this product contains about as much caffeine as a cup of coffee. Limit the use of caffeine-containing medications, foods, or beverages while taking this product because too much caffeine may cause nervousness, irritability, sleeplessness, and, occasionally, rapid heartbeat.
Stop use and ask a doctor if:
- an allergic reaction occurs. Seek medical help right away.
- you experience any of the following signs of stomach bleeding:
- feel faint
- vomit blood
- have bloody or black stools
- have stomach pain that does not get better
- your migraine is not relieved or worsens after first dose
- ringing in the ears or loss of hearing occurs
- any new or unexpected symptoms occur
These could be signs of a serious condition.
Keep out of reach of children.
In case of overdose, get medical help or contact a Poison Control Center right away. Quick medical attention is critical for adults as well as for children even if you do not notice any signs or symptoms.
Excedrin-Migraine side effects
General
General side effects including caffeinism have been reported. Consumption of higher doses of caffeine (>600 mg/day) has been reported to have lead to caffeinism. Caffeinism is a syndrome characterized by anxiety, restlessness, and sleep disorders (similar to anxiety states). It has also been reported that chronic, heavy caffeine ingestion may be associated with depression. Caffeine may cause anxiety and panic in panic disorder patients and may aggravate premenstrual syndrome (PMS).
In general, many side effects noted with aspirin use are dose-related.
Common Excedrin-Migraine side effects may include:
- upset stomach, heartburn;
- depressed mood, feeling anxious or restless; or
- sleep problems (insomnia).
Excedrin-Migraine serious side effects
Get emergency medical help if you have any of these signs of an allergic reaction to Excedrin-Migraine: hives; difficulty breathing; swelling of your face, lips, tongue, or throat.
In rare cases, acetaminophen may cause a severe skin reaction that can be fatal. This could occur even if you have taken acetaminophen in the past and had no reaction. Stop taking Excedrin-Migraine and call your doctor right away if you have skin redness or a rash that spreads and causes blistering and peeling. If you have this type of reaction, you should never again take any medicine that contains acetaminophen.
Stop using Excedrin-Migraine and call your doctor at once if you have:
- severe anxiety, agitation, confusion, panic;
- easy bruising or bleeding;
- a light-headed feeling, like you might pass out;
- if you feel very thirsty or hot, are unable to urinate, and have heavy sweating or hot and dry skin;
- symptoms of stomach bleeding–bloody or tarry stools, coughing up blood or vomit that looks like coffee grounds;
- high potassium–slow heart rate, weak pulse, muscle weakness, tingly feeling; or
- liver problems–nausea, upper stomach pain, itching, loss of appetite, dark urine, clay-colored stools, jaundice (yellowing of the skin or eyes).
Even though it may be rare, some people may have very bad and sometimes deadly side effects when taking a drug. Tell your doctor or get medical help right away if you have any of the following signs or symptoms that may be related to a very bad side effect:
- Signs of an allergic reaction, like rash; hives; itching; red, swollen, blistered, or peeling skin with or without fever; wheezing; tightness in the chest or throat; trouble breathing, swallowing, or talking; unusual hoarseness; or swelling of the mouth, face, lips, tongue, or throat.
- Signs of liver problems like dark urine, feeling tired, not hungry, upset stomach or stomach pain, light-colored stools, throwing up, or yellow skin or eyes.
- Signs of bleeding like throwing up blood or throw up that looks like coffee grounds; coughing up blood; blood in the urine; black, red, or tarry stools; bleeding from the gums; vaginal bleeding that is not normal; bruises without a reason or that get bigger; or any bleeding that is very bad or that you cannot stop.
- Feeling confused.
- Feeling very tired or weak.
- Very bad dizziness or passing out.
- Ringing in ears.
- Hearing loss.
- Very bad headache or if headache is not better after the first dose.
- A very bad skin reaction (Stevens-Johnson syndrome/toxic epidermal necrolysis) may happen. It can cause very bad health problems that may not go away, and sometimes death. Get medical help right away if you have signs like red, swollen, blistered, or peeling skin (with or without fever); red or irritated eyes; or sores in your mouth, throat, nose, or eyes.
- Very bad stomach ulcers or bleeding can happen with this drug. Taking it in high doses or for a long time, smoking, or drinking alcohol raises the chance of these side effects. Taking this drug with food will not lower the chance of these effects. Call your doctor or get medical help right away if you get very bad stomach or back pain; black, tarry, or bloody stools; throwing up blood or throw up that looks like coffee grounds; or weight gain or swelling that is not normal.
Other side effects of Excedrin-Migraine
All drugs may cause side effects. However, many people have no side effects or only have minor side effects. Call your doctor or get medical help if any of these side effects or any other side effects bother you or do not go away:
- Belly pain or heartburn.
- Upset stomach.
These are not all of the side effects that may occur. If you have questions about side effects, call your doctor. Call your doctor for medical advice about side effects.
Hepatic
Alcoholic patients may develop hepatotoxicity after even modest doses of acetaminophen. In healthy patients, approximately 15 grams of acetaminophen is necessary to deplete liver glutathione stores by 70% in a 70 kg person. However, hepatotoxicity has been reported following smaller doses. Glutathione concentrations may be repleted by the antidote N-acetylcysteine. One case report has suggested that hypothermia may also be beneficial in decreasing liver damage during overdose.
In a recent retrospective study of 306 patients admitted for acetaminophen overdose, 6.9% had severe liver injury but all recovered. None of the 306 patients died.
One study has suggested that acetaminophen may precipitate acute biliary pain and cholestasis. The mechanism of this effect may be related to inhibition of prostaglandin and alterations in the regulation of the sphincter of Oddi.
Cases of acute pancreatitis have been reported rarely with the use of acetaminophen.
A 19 year old female developed hepatotoxicity, reactive plasmacytosis and agranulocytosis followed by a leukemoid reaction after acute acetaminophen toxicity.
Hepatic side effects including hepatotoxicity and hepatitis have been reported.
In alcoholic patients, severe and sometimes fatal dose dependent hepatitis has been reported with acetaminophen use. Hepatotoxicity has been increased during fasting.
Cases of aspirin induced hepatotoxicity and cholestatic hepatitis, particularly at high doses, have been reported rarely.
Gastrointestinal
Endoscopically identifiable gastric mucosal lesions occur in most patients who receive a single dose of aspirin. Clinically evident gastrointestinal bleeding has been reported in as many as 3% of treated elderly patients. Anorectal ulceration and rectal stenosis have been reported in patients who abuse aspirin containing rectal suppositories. One case controlled study has suggested that an association between aspirin (and other NSAID) consumption and appendicitis may exist.
Gastrointestinal side effects have been common and have included epigastric distress (in as many as 83% of patients treated with regular aspirin), abdominal discomfort or pain, endoscopically identifiable gastric mucosal lesions, nausea, and vomiting. More serious gastrointestinal effects include hemorrhage, peptic ulcers, perforation, and esophageal ulcerations.
In clinical trials of caffeine citrate, five cases of necrotizing enterocolitis were reported among the 46 infants exposed to the caffeine citrate injection.
Gastrointestinal side effects have been rare with the use of acetaminophen, except in alcoholics and after overdose.
Renal
The mechanism of an aspirin induced decrease in renal function may be related to inhibition of renal prostaglandin synthesis with consequent decreases in renal blood flow. Vasodilating renal prostaglandins may be particularly important in patients who exhibit arterial underfilling (i.e. heart failure, cirrhosis). The administration of high doses of NSAIDs to such patients has produced acute renal failure in rare instances.
Acetaminophen: Acute tubular necrosis usually occurs in conjunction with liver failure, but has been observed as an isolated finding in rare cases. A possible increase in the risk of renal cell carcinoma has been associated with chronic acetaminophen use as well.
A case control study of patients with end stage renal disease suggested that long term consumption of acetaminophen may significantly increase the risk of end stage renal disease particularly in patients taking more than two pills per day.
Renal side effects of aspirin have included reduction in glomerular filtration rate (particularly in patients who are sodium restricted or who exhibit diminished effective arterial blood volume, such as patients with advanced heart failure or cirrhosis), interstitial nephritis, papillary necrosis, elevations in serum creatinine, elevations in blood urea nitrogen, proteinuria, hematuria, and renal failure.
Renal side effects have been rare with acetaminophen use and have included acute tubular necrosis and interstitial nephritis. Adverse renal effects are most often observed after overdose, after chronic abuse (often with multiple analgesics), or in association with acetaminophen related hepatotoxicity.
Hypersensitivity
Hypersensitivity side effects of aspirin have included bronchospasm, rhinitis, conjunctivitis, urticaria, angioedema, and anaphylaxis. Approximately 10% to 30% of asthmatics are aspirin sensitive (with the clinical triad of aspirin sensitivity, bronchial asthma, and nasal polyps).
Hypersensitivity reactions such as anaphylaxis and fixed drug eruptions have rarely been reported in association with acetaminophen use.
The mechanism of aspirin induced hypersensitivity may be related to an up-regulation of the 5-lipoxygenase pathway of arachidonic acid metabolism with a resulting increase in the products of 5-lipoxygenase (such as leukotrienes).
Hematologic
Hematologic side effects of aspirin (in addition to predictable antiplatelet effects which may result in hemorrhage) have included increased blood fibrinolytic activity. In addition, hypoprothrombinemia, thrombocytopenia, thrombocyturia, megaloblastic anemia, and pancytopenia have been reported rarely. Aplastic anemia has also been reported.
Rare cases of thrombocytopenia associated with acetaminophen have been reported. Methemoglobinemia with resulting cyanosis has also been observed in the setting of acute overdose.
Dermatologic
Dermatologic side effects from the use of aspirin including Stevens-Johnson syndrome and a lichenoid eruption have been reported rarely.
Dermatologic side effects associated with acetaminophen includes the risk of rare but potentially fatal serious skin reactions known as Stevens-Johnson syndrome (SJS), toxic epidermal necrolysis and acute generalized exanthematous pustulosis (AGEP). Erythematous skin rashes associated with acetaminophen have been reported, but are rare. Acetaminophen associated bullous erythema and purpura fulminans have been reported.
Respiratory
Respiratory side effects including hyperpnea, pulmonary edema, and tachypnea have occurred in patients receiving aspirin.
A case of acetaminophen induced eosinophilic pneumonia has been reported.
Cardiovascular
Two cases hypotension have been reported following the administration of acetaminophen. Both patients experienced significant decreases in blood pressure. One of the two patients required pressor agents to maintain adequate mean arterial pressures. Neither episode was associated with symptoms of anaphylaxis. Neither patient was rechallenged after resolution of the initial episode.
Cardiovascular side effects of aspirin have been reported rarely and have included salicylate induced variant angina, ventricular ectopy, conduction abnormalities, and hypotension, particularly during salicylate toxicity.
Several cases of hypotension have been reported following the administration of acetaminophen.
Metabolic
Metabolic side effects of aspirin have included dehydration and hyperkalemia. Respiratory alkalosis and metabolic acidosis, particularly during salicylate toxicity, have been reported. A case of hypoglycemia has also been reported in a patient on hemodialysis.
Nervous system
Nervous system side effects in patients receiving aspirin have included agitation, cerebral edema, coma, confusion, dizziness, headache, cranial hemorrhage, lethargy, and seizures. Some investigators have reported that modest doses may result in decreased frequency selectivity and may therefore impair hearing performance, particularly in the setting of background noise.
Regarding the use of aspirin, some investigators have suggested that tinnitus may be a less reliable indicator of salicylate toxicity than previously believed. Patients with high frequency hearing loss may have difficulty perceiving tinnitus. In a study of rheumatoid arthritis patients, those with tinnitus had no greater salicylate levels than those without tinnitus. Elderly patients may be less likely to perceive tinnitus than younger patients.
Musculoskeletal
Musculoskeletal side effects including rhabdomyolysis have occurred in patients receiving aspirin.
Endocrine
Endocrine side effects of aspirin use have included hypoglycemia and hyperglycemia.
Ocular
Ocular side effects including cases of localized periorbital edema have been reported rarely in patients receiving aspirin.
Oncologic
Oncologic side effects have been reported. Several epidemiologic studies have suggested that chronic aspirin use may decrease the risk of large bowel neoplasms. However, other studies have not found this beneficial effect.
Other side effects
Other side effect have also been reported. In one study of the effects of caffeine, 634 women with fibrocystic breast disease (compared to 1066 women without the disease), the occurrence of fibrocystic breast disease was positively associated with average daily consumption of caffeine. Women who consumed 31 to 250 mg/day of caffeine were reported to have a 1.5 times increase in odds to have the disease. Women who consumed over 500 mg/day of caffeine were reported to have a 2.3 times increase in odds.
Reye’s syndrome, although rare, has been associated with aspirin use in children with an acute viral illness. Reye’s syndrome has also been reported even more rarely in adults.
Prolonged labor and pregnancy, decreased infant birth weight and stillborn births, antepartum and postpartum bleeding have occurred due to aspirin use by women during the third trimester of pregnancy.
Reye’s syndrome typically involves vomiting, neurologic dysfunction, and hepatic dysfunction during or shortly after an acute viral infection.
Excedrin-Migraine overdose
In case of overdose, call the poison control helpline at 1-800-222-1222. Information is also available online at https://www.poisonhelp.org/help. This is a free and confidential service. All local poison control centers in the United States use this national number. You should call if you have any questions about poisoning or poison prevention. It does NOT need to be an emergency. You can call for any reason, 24 hours a day, 7 days a week.
References- Upfal J. (2006) The Australian Drug Guide (7th Ed.) Melbourne: Black Inc.
- Food Regulation Standing Committee, Caffeine Working Group. (2013). The regulation of caffeine in foods.
- Upfal, J. (2006). The Australian drug guide. (7th ed.). Melbourne: Black Inc.
- Seifer, S., Schaechter, J., Hershorin, E. & Lepshultz, S. (2011). Health effects of energy drinks on children, adolescents, and young adults. Pediatrics, 127(3). 511–528. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3065144/
- Brands, B., Sproule, B., & Marshman, J. (Eds.). (1998). Drugs & drug abuse (3rd ed.). Ontario: Addiction Research Foundation.
- American Psychiatric Association. (2013). Diagnostic and Statistical Manual of Mental Disorders. (5th ed). Washington: American Psychiatric Publishing.
- NPS Medicinewise. (2013). https://www.nps.org.au/news#Information
- Arria, A., Calderia, K., Kasperski, S., O’Grady, K., Vincent, K., Griffiths, R. & Wish, E. (2010). Increased alcohol consumption, nonmedical prescription drug use, and illicit drug use are associated with energy drink consumption among college students. Journal of Addiction Medicine, 4(2). 74–80. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2923814/
- Byer AJ, Traylor TR, Semmer JR “Acetaminophen overdose in the third trimester of pregnancy.” JAMA 247 (1982): 3114-5
- Rayburn W, Shukla U, Stetson P, Piehl E “Acetaminophen pharmacokinetics: comparison between pregnant and nonpregnant women.” Am J Obstet Gynecol 155 (1986): 1353-6
- Galinsky RE, Levy G “Absorption and metabolism of acetaminophen shortly before parturition.” Drug Intell Clin Pharm 18 (1984): 977-9
- Beaulac-Baillargeon L, Rocheleau S “Paracetamol pharmacokinetics during the first trimester of human pregnancy.” Eur J Clin Pharmacol 46 (1994): 451-4
- O’Brien WF, Krammer J, O’Leary TD, Mastrogiannis DS “The effect of acetaminophen on prostacyclin production in pregnant women.” Am J Obstet Gynecol 168 (1993): 1164-9
- Briggs GG, Freeman RK, Yaffe SJ.. “Drugs in Pregnancy and Lactation. 5th ed.” Baltimore, MD: Williams & Wilkins;1998
- Rudolph AM “Effects of aspirin and acetaminophen in pregnancy and in the newborn.” Arch Intern Med 141 (1981): 358-63
- Karlowicz MG, White LE “Severe intracranial hemorrhage in a term neonate associated with maternal acetylsalicylic acid ingestion.” Clin Pediatr (Phila) 32 (1993): 740-3
- Schoenfeld A, Bar Y, Merlob P, Ovadia Y “NSAIDs: maternal and fetal considerations.” Am J Reprod Immunol 28 (1992): 141-7
- “Clasp: a randomised trial lf low-dose aspirin for the prevention and treatment of pre-eclampsia among 9364 pregnant women.” Lancet 343 (1994): 619-29
- Parazzini F, Bortolus R, Chatenoud L, Restelli S, Benedetto C “Follow-up of children in the italian study of aspirin in pregnancy.” Lancet 343 (1994): 1235
- Committee on Drugs, 1992 to 1993 “The transfer of drugs and other chemicals into human milk.” Pediatrics 93 (1994): 137-50
- Matheson I, Lunde PK, Notarianni L “Infant rash caused by paracetamol in breast milk.” Pediatrics 76 (1985): 651-2
- Erickson SH, Oppenheim GL “Aspirin in breast milk.” J Fam Pract 8 (1979): 189-90
- Roberts RJ, Blumer JL, Gorman RL, et al “American Academy of Pediatrics Committee on Drugs: Transfer of drugs and other chemicals into human milk.” Pediatrics 84 (1989): 924-36
- Berlin CM Jr, Denson HM, Daniel CH, Ward RM “Disposition of dietary caffeine in milk, saliva, and plasma of lactating women.” Pediatrics 73 (1984): 59-63