What is senile purpura
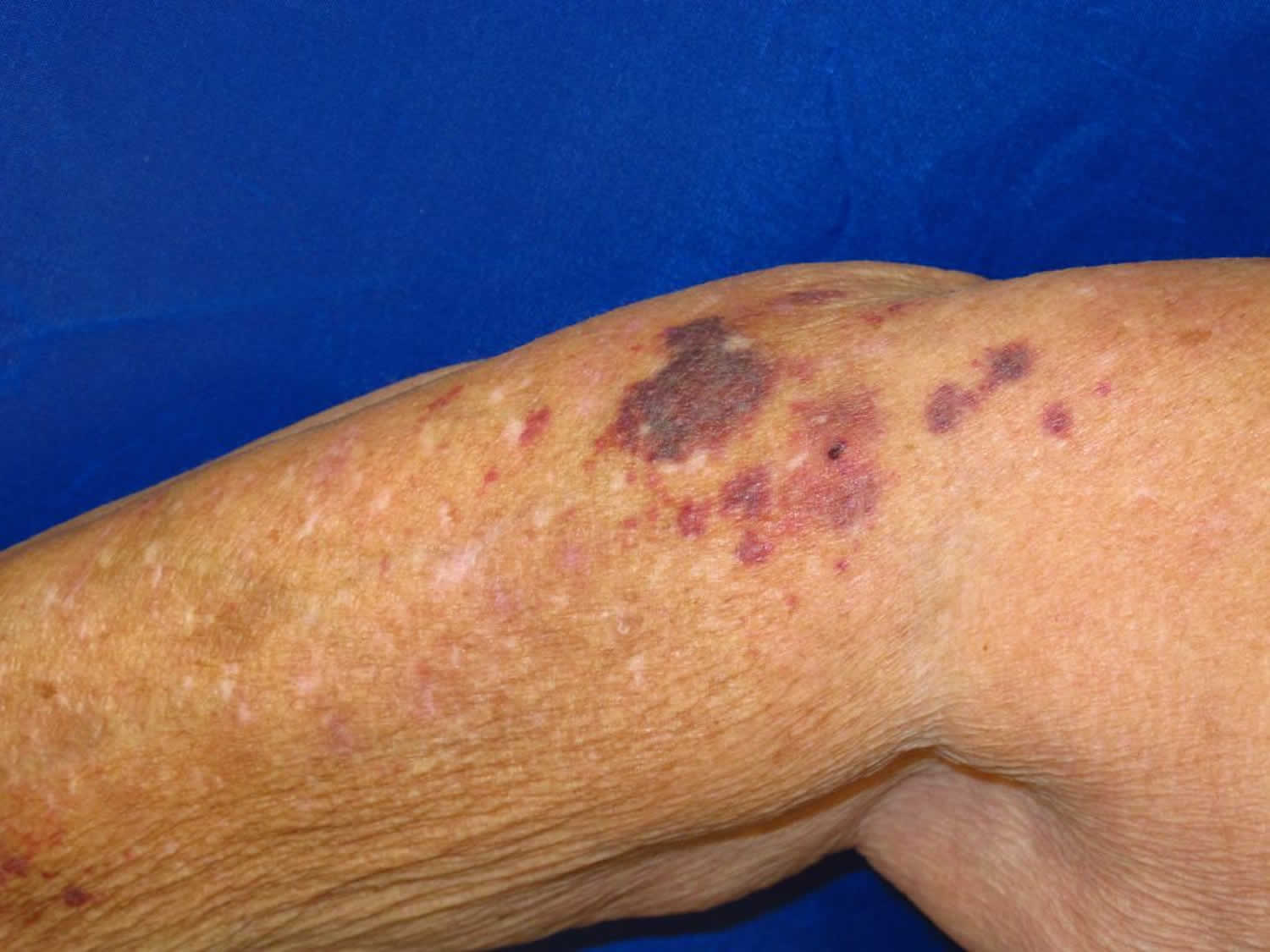
Senile purpura also known as Bateman senile purpura or actinic purpura, is a common, benign skin condition characterized by the recurrent formation of purple ecchymoses (bruises) on the extensor surfaces of forearms following minor trauma. Senile purpura appears to be caused by dermal and vascular fragility induced by chronic sun exposure 1. Senile purpura usually affects elderly individuals, and it is characterized by dark purple blotches on the photo-exposed areas, especially the back of the hands and the extensor surfaces of the forearm. The term solar purpura has been used by some authors as a synonym to senile purpura, but it is preferable to reserve it to purpuric lesions that occur acutely after sun exposure 2.
Senile purpura affects over 10% of those aged over 50 years old, especially those with fair skin (skin types 1 and 2) who are more sensitive to sun exposure. Senile purpura is estimated to be present in about 12% of individuals after the age of 50 years and up to 30% after age 75. It is equally common in males and females 3.
Other risk factors include chronic sunlight exposure and the use of oral or topical corticosteroids and anticoagulants (blood thinners).
Senile purpura causes
With age and sun damage, the dermal connective tissues become thin and increase the fragility of blood vessels. As a result, superficial vessels tear and rupture even with negligible trauma. The subsequent extravasation of blood into the surrounding dermis after a minor trauma, results in the development of dark purple ecchymoses (bruises). It is one of the signs of dermatoporosis, which indicates the skin fragility as well as skin atrophy and stellate pseudoscars 4.
Persistent brown pigmentation following the resolution of the bruises results from the deposition of hemosiderin, a component of red blood cells.
Senile purpura symptoms
Senile purpura is characterized by irregularly-shaped macules, 1 cm to 4 cm in diameter on average, that are dark purple with well-defined margins. The lesions may appear dark purple and have extensive ecchymosis. The lesions often are present on the forearm and the back of the hands. However, they can affect other areas, such as the legs, neck, and face. The surrounding skin is typically thin, inelastic and pigmented in association with others signs of skin ageing and sun damage such as lentigos and actinic keratoses. The lesions do not undergo the color changes of a bruise and take up to three weeks to resolve.
The lesions are most commonly distributed on the extensor surface of forearms and dorsal aspect of hands. Infrequently, they also occur on necks and faces.
The patient may recall minor blunt trauma to skin preceding the appearance of the lesions. They may also note multiple similar lesions which have appeared in the past but now resolved.
Senile purpura diagnosis
Senile purpura can be diagnosed based on clinical appearance alone. In the rare cases where a biopsy is performed, the histological study will show a thinned epidermis ascending on an altered dermis with quantitatively reduced collagen fibers replaced by abnormal elastic fibers. The walls of the dermal vessels have a normal tensile structure, but there is extravasation of the red blood cells and hemosiderin deposits marked by Perls staining. In about 10% of cases, there is a neutrophilic infiltration that may lead to the misdiagnosis of actinic purpura as neutrophilic dermatosis or leukocytoclastic vasculitis 5.
Coagulation studies are rarely necessary and will typically be unremarkable.
Senile purpura treatment
Senile purpura is benign and self-resolving condition that does not require specific treatment, particularly since other lesions continue to appear throughout life.
The best treatment is preventive and involves protection from the sun via the application of sunscreen and wearing long-sleeved shirts. One should apply sunscreens with a high protection index (sun protection factor (SPF) greater than 50 [SPF 50+]) daily to provide sufficient protection against the ultraviolet (UVB and UVA) rays. The sunscreen should be liberally applied to all sun-exposed areas regularly 6.
The therapeutic possibilities available for the actinic purpura lesions already formed are restricted. Tretinoin or retinoic acid (0.1%) is a derivative of vitamin A, which could theoretically reverse severe skin damage induced by ultraviolet light. Indeed, topical tretinoin is known for its role in the regeneration of dermal collagen and the reduction of the quality of abnormal elastin damaged by solar exposure. However, some authors demonstrate that the developed plaques of actinic purpura do not improve under local treatment with tretinoin.
In 2002, actinic purpura was successfully treated in one patient with tissue-engineered skin; however, no similar cases have been reported.
More recently, it has been demonstrated that human epidermal growth factor may be a viable treatment of actinic purpura. It has been shown to increase the average skin thickness and reduce the number of purpuric lesions when applied twice daily for six weeks.
A citrus bioflavonoid blend has been tested for the treatment of actinic purpura. After six weeks, the treated group showed a 50% decrease in purpuric plaques with no reported side effects.
Laser therapy, which is widely used for the treatment of aging skin manifestations, is not indicated in actinic purpura. Moisturizing creams may be useful to treat frequently associated skin xerosis.
Senile purpura prognosis
Although cosmetically displeasing, senile purpura is benign and unrelated to any systemic diseases or blood dyscrasias. It is, however, a risk factor for skin tears in institutionalized patients.
The purpuric lesions resolve over one to three weeks and may produce residual brown pigmentation of the skin. Unfortunately, senile purpura is recurrent and associated with lifelong reappearance of new lesions.
- Hafsi W, Badri T. Actinic Purpura. [Updated 2019 May 2]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2019 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK448130[↩]
- Ceilley RI. Treatment of Actinic Purpura. J Clin Aesthet Dermatol. 2017 Jun;10(6):44-50.[↩]
- Luger A. [The skin in the elderly]. Z Gerontol. 1988 Sep-Oct;21(5):264-6.[↩]
- Brouwer MW, Kemperman PM. [A woman with red-purple blotches]. Ned Tijdschr Geneeskd. 2013;156(0):A3305.[↩]
- Griffiths CE. The clinical identification and quantification of photodamage. Br. J. Dermatol. 1992 Sep;127 Suppl 41:37-42.[↩]
- Demetriou C. Reversing precancerous actinic damage by mixing wavelengths (1064 nm, 532 nm). J Cosmet Laser Ther. 2011 Jun;13(3):113-9.[↩]