The Average American Diet – Showing what America Eats Every Day
The typical American diet is about 50% carbohydrate, 15% protein, and 35% fat. The Standard American Diet or “Western-style” dietary patterns with more red meat or processed meat, sugared drinks, sweets, refined carbohydrates, or potatoes-have been linked to obesity 1, 2, 3, 4. The Average American (Western-style) dietary pattern is also linked to increased risk of heart disease, diabetes, and other chronic conditions.
Meal frequency and snacking have increased over the past 30 years in the U.S. 5 on average, children get 27 percent of their daily calories from snacks, primarily from desserts and sugary drinks, and increasingly from salty snacks and candy.
Since the 1970s, portion sizes have increased both for food eaten at home and for food eaten away from home, in adults and children 6, 7. Short-term studies clearly demonstrate that when people are served larger portions, they eat more. One study, for example, gave moviegoers containers of stale popcorn in either large or medium-sized buckets; people reported that they did not like the taste of the popcorn-and even so, those who received large containers ate about 30 percent more popcorn than those who received medium-sized containers 8. Another study showed that people given larger beverages tended to drink significantly more, but did not decrease their subsequent food consumption 9. An additional study provided evidence that when provided with larger portion sizes, people tended to eat more, with no decrease in later food intake 10. There is an intuitive appeal to the idea that portion sizes increase obesity, but long-term prospective studies would help to strengthen this hypothesis.
Over the past century, rates of chronic diseases—many of which are related to poor quality diet and physical inactivity—have increased. About half of all American adults (117 million individuals) —have one or more preventable chronic diseases, many of which are related to diet-related chronic diseases due to poor quality eating patterns and physical inactivity, including cardiovascular disease, high blood pressure, type 2 diabetes, and overweight and obesity , some cancers and poor bone health 11. More than two-thirds of adults and nearly one-third of children and youth are overweight or obese. Trends in food intake show that Americans are not consuming healthy eating patterns.
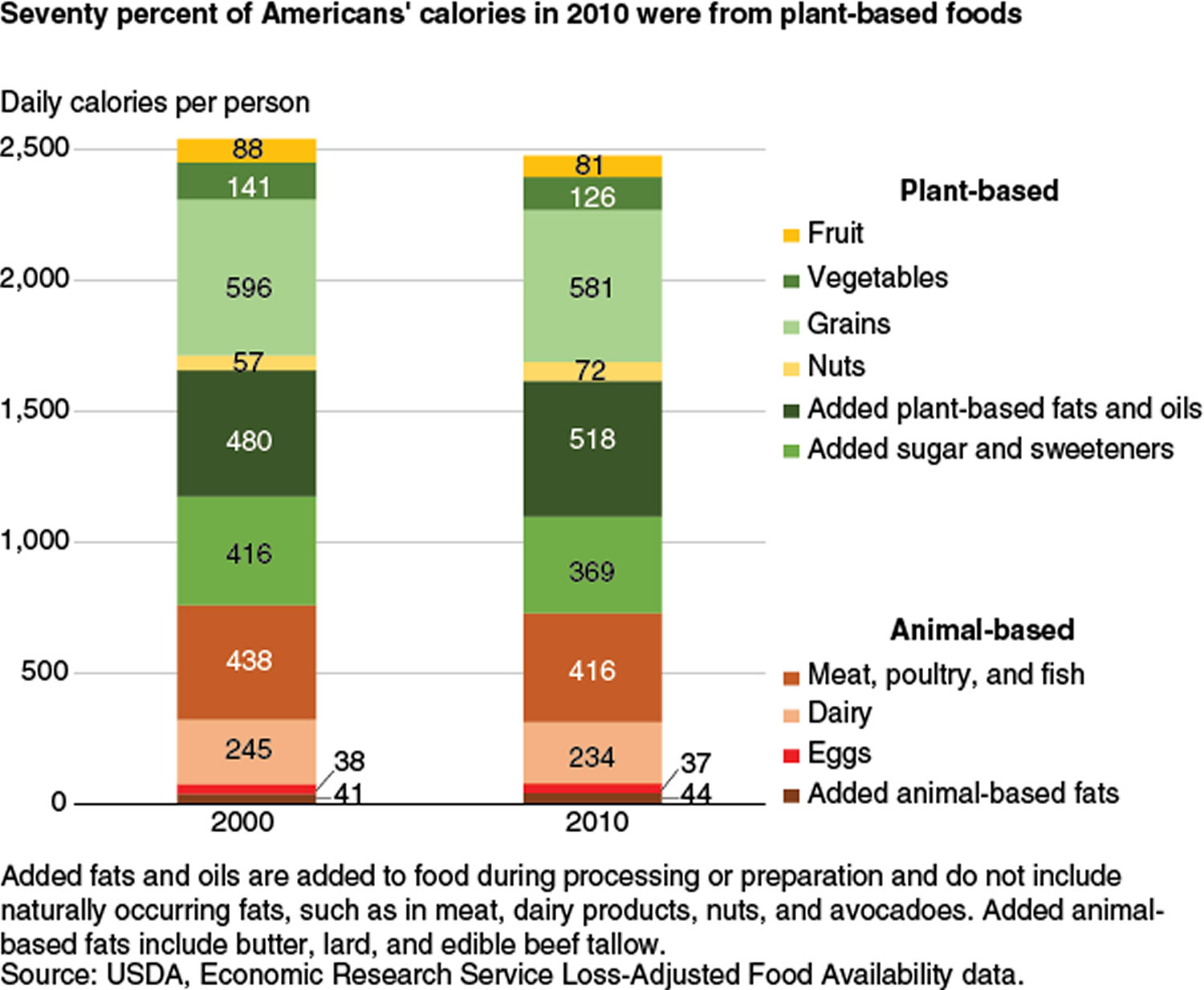
According to United States Department of Agriculture’s food availability data 12, total daily calories per person decreased by 2 percent between 2000 and 2010 from 2,545 to 2,481 calories. The share of calories from animal- and plant-based foods was the same in both years at 30 percent and 70 percent, respectively. In both years, grains were the primary contributor to daily calories per capita (596 in 2000 and 581 in 2010). Added plant-based fats and oils—such as salad and cooking oil, margarine, and shortening—ranked second (480 in 2000 and 518 in 2010), followed by meat, poultry, and fish (438 in 2000 and 416 in 2010).
Between the 10 years, only 3 of the 10 food categories had changes in calorie amounts greater than 10 percent. Per capita availability of calories from nuts showed the largest percentage change with a 25-percent increase to 72 calories in 2010. There was an 11-percent decrease in calories from both the vegetable and added sugar and sweeteners categories.
While calorie shares of the broad food categories may not have changed, the amount of calories from individual food commodities in the categories did. For example, the proportion of calories from meat, poultry, and fish stayed the same at 17 percent of total calories in both 2000 and 2010, but within this category, there was an increase in calories per capita from poultry and fish and a decrease in calories from red meat. In the vegetables category, per-capita calories from kale and sweet potatoes increased, while per-capita calories available from head lettuce and white potatoes decreased.
Early 2016, the US Department of Health and Human Services’ Office of Disease Prevention and Health Promotion and the US Department of Agriculture’s Center for Nutrition Policy and Promotion released the 2015-2020 Dietary Guidelines for Americans 13.
The Healthy Eating Index (HEI) is a measure of diet quality in terms of conformance with the Dietary Guidelines for Americans, which are the basis of nutrition policy for the United States government and the foundation of all federal nutrition guidance. The Dietary Guidelines are issued every 5 years by the USDA and U.S. Department of Health and Human Services. The 2015–2020 Dietary Guidelines is designed to help Americans eat a healthier diet. USDA’s primary use of the HEI is to monitor the diet quality of the U.S. population and the low-income subpopulation. The HEI is also used to examine relationships between diet and health-related outcomes, and to assess the quality of food assistance packages, menus, and the US food supply 14. The original HEI was created by the Center for Nutrition Policy and Promotion in 1995. Updates to the HEI are through collaboration between the Center for Nutrition Policy and Promotion and partners at the National Cancer Institute. Plans to update the HEI to align with the 2015-2020 Dietary Guidelines for Americans are currently underway 14.
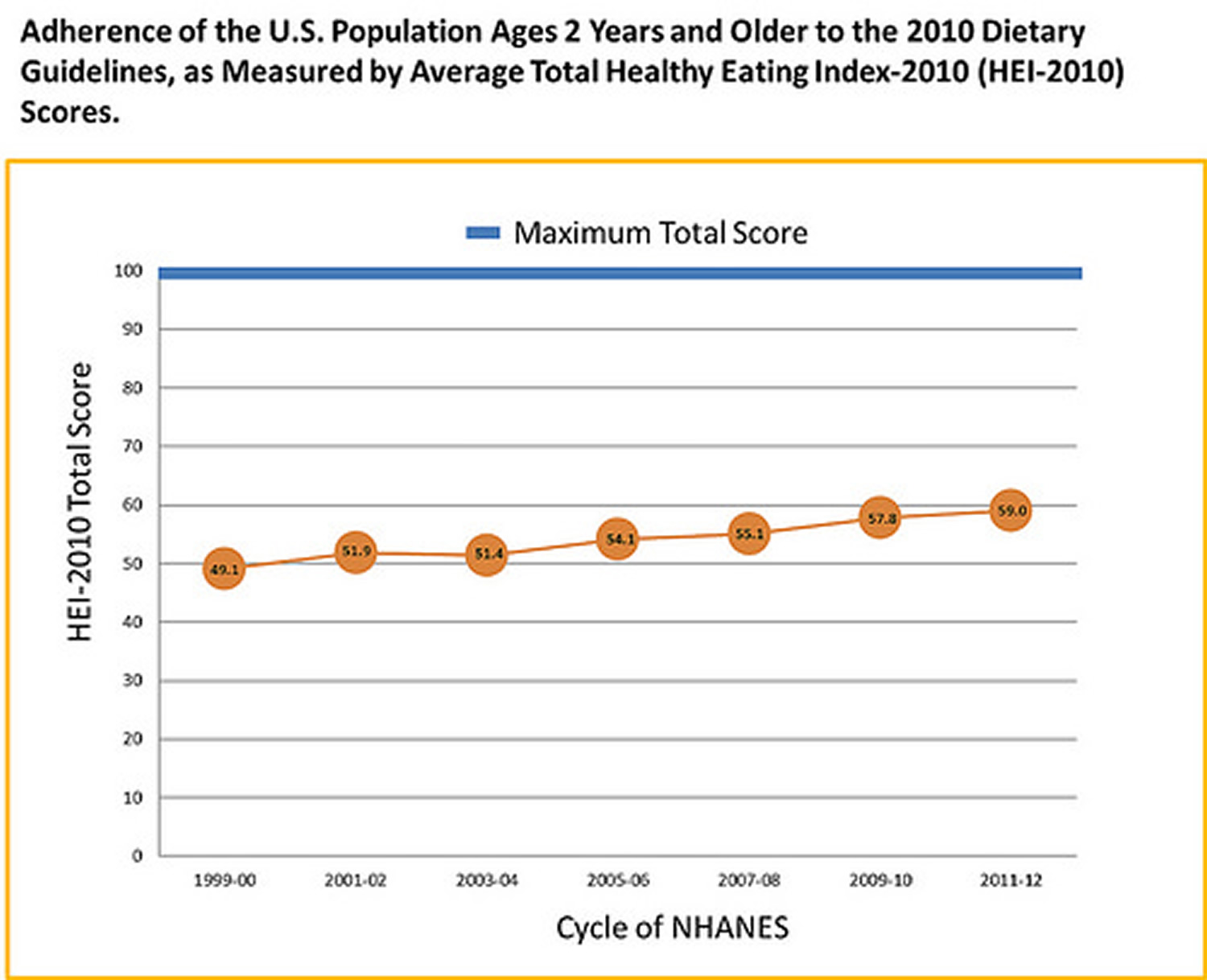
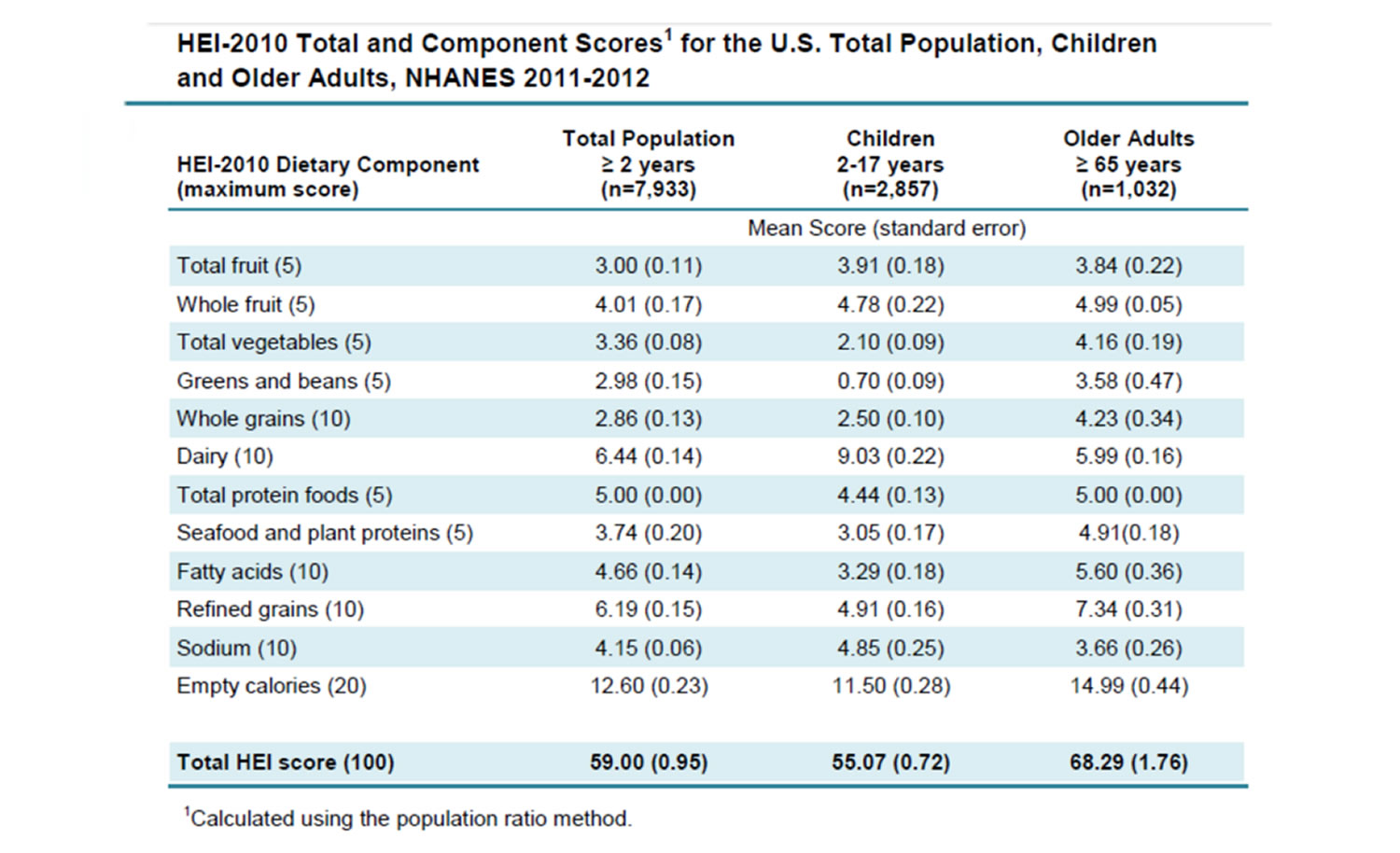
The Healthy Eating Index (HEI) measures how the Americans’ food choices align with the 2015-2020 Dietary Guidelines for Americans and in order to measure progress towards America’s national nutrition goals. The Americans’ current HEI score is 59 out of 100. The HEI score in previous years was even lower, in 1999–2000 the HEI score was 49 15. At the same time, diet-related chronic disease rates over the last 25 years have risen and remain high. Given the robust science behind the Dietary Guidelines, it is not an understatement to suggest that if Americans were to eat closer to the Dietary Guidelines – and saw the nation’s HEI scores get closer to 100 – we would see reductions in the prevalence of diet-related chronic disease. The current HEI-2010 scores the average American diet based on intakes of total fruit, whole fruit, total vegetables, greens and beans, whole and refined grains, total protein foods, seafood and plant-based protein foods, sodium, and calories from solid fats, added sugar, and alcohol beyond a moderate level. A diet that meets the Healthy People 2020 objectives and the 2010 Dietary Guidelines for Americans objectives would receive a score of 74, and, by definition, a diet that meets the 2010 Dietary Guidelines for Americans would receive a score of 100. Trends in HEI-2010 component scores vary; all HEI-2010 component scores except sodium have increased over time.
(Source 14).
What Americans Eat: Top 10 sources of calories in the U.S. diet
- Grain-based desserts (cakes, cookies, donuts, pies, crisps, cobblers, and granola bars)
- Yeast breads
- Chicken and chicken-mixed dishes
- Soda, energy drinks, and sports drinks
- Pizza
- Alcoholic beverages
- Pasta and pasta dishes
- Mexican mixed dishes
- Beef and beef-mixed dishes
- Dairy desserts(Source: Report of the 2010 Dietary Guidelines Advisory Committee)
Fast food is known for its large portions, low prices, high palatability, and high sugar content, and there’s evidence from studies in teens and adults that frequent fast-food consumption contributes to overeating and weight gain 16, 17, 18, 19, 20, 10. A study on the effect of fast-food consumption on risk of obesity and type 2 diabetes, for example, followed 3,000 young adults for 13 years. People who had higher fast-food-intake levels at the start of the study weighed an average of about 13 pounds more than people who had the lowest fast-food-intake levels. They also had larger waist circumferences and greater increases in triglycercides, and double the odds of developing metabolic syndrome 17.
The typical eating patterns currently consumed by many in the United States do not align with the Dietary Guidelines. As shown below, when compared to the Healthy U.S.-Style Pattern (the Healthy Diet):

(Source Health.gov – What We Eat in America, NHANES 2007-2010 for average intakes by age-sex group).
The bar graph above showing the percentage of the U.S. population ages 1 year and older with intakes below the recommendation or above the limit for different food groups and dietary components.
- Vegetables: 87% have intakes below the goal;
- Fruit: 75% have intakes below the goal;
- Total Grains: 44% have intakes below the goal;
- Dairy: 86% have intakes below the goal;
- Protein Foods: 42% have intakes below the goal;
- Oils: 72% have intakes below the goal;
- Added sugars: 70% have intakes above the limit;
- Saturated fats: 71% have intakes above the limit;
- Sodium: 89% have intakes above the limit.
- Most Americans exceed the recommendations for added sugars, saturated fats, and sodium. Most people say that if there is a healthy choice on a menu they will take it. But observations and research show this is generally not the case. Instead, people tend to make choices based on how food tastes. Typically, the more sugar, salt and fat in the food, the more we will like it.
- About three-fourths of the population has an eating pattern that is low in vegetables, fruits, dairy, and oils.
- More than half of the population is meeting or exceeding total grain and total protein foods recommendations, but, are not meeting the recommendations for the subgroups within each of these food groups.
In addition, the eating patterns of many are too high in calories. Calorie intake over time, in comparison to calorie needs, is best evaluated by measuring body weight status. The high percentage of the population that is overweight or obese suggests that many in the United States over consume calories. More than two-thirds of all adults and nearly one-third of all children and youth in the United States are either overweight or obese.
For the 20-30 year old the top sources of “Nutrition” are:
- Regular soft drinks 8.8% of total energy
- Pizza 5.1% of total energy
- Beer 3.9%
- Hamburgers and meat loaf 3.4%
- White bread 3.3%
- Cake, doughnuts and pastries 3.3%
- French fries and fried potatos 3.0%
- Potato chips, corn chips and popcorn 2.7%
- Rice 2.6%
- Cheese and cheese spread 2.5%
Vitamins and Micronutrients Deficiency (Americans):
- Vitamin D – 70% of Americans of deficient (food source: oil fish – salmon, trout, mackerel, sardines)
- Vitamin E – 60% of Americans of deficient
- Magnesium – 45% of Americans of deficient (food source: green vegetables)
- Vitamin K – 35% of Americans of deficient (food source: dark green vegetables)
- Calcium – 35% of Americans of deficient (food source: fortified ready-to-eat cereals, cheese)
- Vitamin A – 34% of Americans of deficient (food source: red or orange vegetables)
- Vitamin C – 25% of Americans of deficient
- Omega 3 – very high % of Americans of deficient (food source: oily fish)
- Zinc – 8% of Americans of deficient
The low intake of micronutrients result in insidious increased DNA damage, that over time leads to the acceleration of aged-associated diseases e.g. increased cancer.
An Americanization of food habits has been recognized throughout the world, characterized by a high-energy diet, with increasing consumption of industrially processed foods. These foods usually contain large amounts of salt, simple sugars, saturated and trans fats, which food industries offer in response to consumers’ demands. Consequently, the intake of complex carbohydrates, fibres, fruits and vegetables has decreased. The energy and animal proteins consumed largely exceed World Health Organization recommendations, while, generally, a smaller variety of foods is being consumed.
The American Diet Quality: Where it is, Where it is Heading, and What it Could Be
Diet quality is critically important to the prevention of many types of chronic disease. The Federal government provides recommendations for optimal diet quality through the Dietary Guidelines for Americans and sets benchmarks for progress towards these recommendations through the Healthy People objectives. Nearly half of all American adults have one or more chronic diseases that are related to poor quality diet 21, 22, 23, 24. The burden of these diet-related diseases in this country, including associated morbidities, mortality, health care costs and lost wages, is enormous 25, 26, 27, 28 and suggests dietary improvements should be an imperative.
American diet quality is generally improving over time, with the HEI-2010 total score increasing from 49 in 1999/2000 to 59 in 2011/2012. If this current trend continued to the year 2019/2020, mean diet quality in the U.S. would reach a HEI-2010 score of 65. This is 9 points lower than the HEI-2010 score would be if they met the Healthy People 2020 objectives and 35 points lower than the HEI-2010 score would be if they met the 2010 Dietary Guidelines for Americans. Meeting either of the current national benchmarks for American diet quality by the year 2019/2020 would require dramatic shifts from current trends. If current trends continue, the Healthy People 2020 objectives for food and nutrient intakes will not be met until after the year 2030, more than a decade after the goal date.
The trends in diet quality vary by component. Generally, component scores have increased over time, indicating improvements in most components of diet quality. However, sodium scores have decreased over time, indicating an increase in sodium density in the American diet. The increase in sodium density (and the increase in absolute sodium intake underlying this trend) is alarming given that excess sodium intake can lead to hypertension and, in turn, heart disease, which is the leading cause of mortality nationally 29.
The progress towards the national benchmarks of the Healthy People 2020 Objectives and the 2010 Dietary Guidelines for Americans also varies by component. Americans met the Healthy People 2020 target for empty calories in the year 2011/2012 and are on track to surpass the target by the year 2019/2020. Consumption of whole grains is increasing over time, but not in large enough increments to meet the Healthy People target by 2019/2020. The slow progress towards the whole grain target in the Healthy People 2020 objectives is notable as the target is set at less than half of the intake recommended by the 2010 DGAs. Whole fruit density is increasing, and is projected to approach the HEI-2010 standard for this component by 2019/2020. However, total fruit density is not increasing in parallel, due in part to a decrease in fruit juice density over time. Similarly, consumption of greens and beans is increasing while total vegetable density in the diet remains constant. The increase in both whole fruit and greens and beans is promising, though they have not yet translated into a notable increase in total fruit density or total vegetable density in the diet. The increase in greens and beans score is particularly encouraging because intake of this component in 2010 was among the farthest from the amounts recommended in the USDA food patterns 30, 31, 32, and improvement in this component may indicate that the focus on this subgroup of foods in the HEI-2010 has been effective 30.
The analysis of the current trajectory in American diet quality to national benchmarks and found that if the current trajectory continues the country will not meet the Healthy People 2020 objectives by the year 2020, and that Americans will fall short of the 2010 Dietary Guidelines for Americans in nearly every component of diet quality measured 15.
- Schulze MB, Fung TT, Manson JE, Willett WC, Hu FB. Dietary patterns and changes in body weight in women. Obesity (Silver Spring). 2006;14:1444-53. https://www.ncbi.nlm.nih.gov/pubmed/16988088[↩]
- Newby PK, Muller D, Hallfrisch J, Andres R, Tucker KL. Food patterns measured by factor analysis and anthropometric changes in adults. Am J Clin Nutr. 2004;80:504-13. https://www.ncbi.nlm.nih.gov/pubmed/15277177[↩]
- Schulz M, Nothlings U, Hoffmann K, Bergmann MM, Boeing H. Identification of a food pattern characterized by high-fiber and low-fat food choices associated with low prospective weight change in the EPIC-Potsdam cohort. J Nutr. 2005;135:1183-9. https://www.ncbi.nlm.nih.gov/pubmed/15867301[↩]
- Newby PK, Muller D, Hallfrisch J, Qiao N, Andres R, Tucker KL. Dietary patterns and changes in body mass index and waist circumference in adults. Am J Clin Nutr. 2003;77:1417-25. https://www.ncbi.nlm.nih.gov/pubmed/12791618[↩]
- Popkin BM, Duffey KJ. Does hunger and satiety drive eating anymore? Increasing eating occasions and decreasing time between eating occasions in the United States. Am J Clin Nutr. 2010;91:1342-7. https://www.ncbi.nlm.nih.gov/pubmed/20237134[↩]
- Nielsen SJ, Popkin BM. Patterns and trends in food portion sizes, 1977-1998. JAMA. 2003;289:450-3. https://www.ncbi.nlm.nih.gov/pubmed/12533124[↩]
- Piernas C, Popkin BM. Food portion patterns and trends among U.S. children and the relationship to total eating occasion size, 1977-2006. J Nutr. 2011;141:1159-64. https://www.ncbi.nlm.nih.gov/pubmed/21525258[↩]
- Wansink B, Kim J. Bad popcorn in big buckets: portion size can influence intake as much as taste. J Nutr Educ Behav. 2005;37:242-5. https://www.ncbi.nlm.nih.gov/pubmed/16053812[↩]
- Rolls, B. J., L. S. Roe, et al. (2007). “The effect of large portion sizes on energy intake is sustained for 11 days.” Obesity (Silver Spring) 15(6): 1535-1543.[↩]
- Rosenheck R. Fast food consumption and increased caloric intake: a systematic review of a trajectory towards weight gain and obesity risk. Obes Rev. 2008;9:535-47. https://www.ncbi.nlm.nih.gov/pubmed/18346099[↩][↩]
- U.S. Department of Agriculture. The Healthy Eating Index: How Is America Doing ? https://www.usda.gov/media/blog/2016/03/16/healthy-eating-index-how-america-doing[↩]
- USDA, Economic Research Service, December 2016. A Look at Calorie Sources in the American Diet. https://www.ers.usda.gov/amber-waves/2016/december/a-look-at-calorie-sources-in-the-american-diet/[↩]
- 2015–2020 Dietary Guidelines for Americans. https://health.gov/dietaryguidelines/2015/[↩]
- United States Department of Agriculture, Center for Nutrition Policy and Promotion. Healthy Eating Index (HEI). https://www.cnpp.usda.gov/healthyeatingindex[↩][↩][↩]
- J Acad Nutr Diet. 2016 Feb; 116(2): 302–310.e1. Published online 2015 Nov 21. doi: 10.1016/j.jand.2015.09.020. American Diet Quality: Where it is, Where it is Heading, and What it Could Be. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4733413/[↩][↩]
- Duffey KJ, Gordon-Larsen P, Jacobs DR, Jr., Williams OD, Popkin BM. Differential associations of fast food and restaurant food consumption with 3-y change in body mass index: the Coronary Artery Risk Development in Young Adults Study. Am J Clin Nutr. 2007;85:201-8. https://www.ncbi.nlm.nih.gov/pubmed/17209197[↩]
- Duffey KJ, Gordon-Larsen P, Steffen LM, Jacobs DR, Jr., Popkin BM. Regular consumption from fast food establishments relative to other restaurants is differentially associated with metabolic outcomes in young adults. J Nutr. 2009;139:2113-8. https://www.ncbi.nlm.nih.gov/pubmed/19776183[↩][↩]
- Taveras EM, Berkey CS, Rifas-Shiman SL, et al. Association of consumption of fried food away from home with body mass index and diet quality in older children and adolescents. Pediatrics. 2005;116:e518-24. https://www.ncbi.nlm.nih.gov/pubmed/16199680[↩]
- French SA, Harnack L, Jeffery RW. Fast food restaurant use among women in the Pound of Prevention study: dietary, behavioral and demographic correlates. Int J Obes Relat Metab Disord. 2000;24:1353-9. https://www.ncbi.nlm.nih.gov/pubmed/11093299[↩]
- Pereira MA, Kartashov AI, Ebbeling CB, et al. Fast-food habits, weight gain, and insulin resistance (the CARDIA study): 15-year prospective analysis. Lancet. 2005;365:36-42. www.ncbi.nlm.nih.gov/pubmed/15639678[↩]
- U.S. Department of Agriculture. Human Nutrition Information Service. Dietary Guidelines Advisory Committee., U.S. Agricultural Research Service. Scientific Report of the 2015 Dietary Guidelines Advisory Committee: Advisory Report to the Secretary of Health and Human Services and the Secretary of Agriculture. Washington, D.C: United States Dept. of Health and Human Services : United States Dept. of Agriculture; 2015. [↩]
- Evidence Analysis Library Division, Center for Nutrition Policy and Promotion. A Series of Systematic Reviews on the Relationship Between Dietary Patterns and Health Outcomes. Alexandria, VA: U.S. Department of Agriculture; Mar, 2014.[↩]
- American Institute for Cancer Research, World Cancer Research Fund. Food, Nutrition, Physical Activity and the Prevention of Cancer: A Global Perspective. Washington, D.C: American Institute for Cancer Research; 2007.[↩]
- Ward BW, Schiller JS, Goodman RA. Multiple Chronic Conditions Among US Adults: A 2012 Update. Prev Chronic Dis. 2014;11(130389). https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3992293/[↩]
- Finkelstein EA, Trogdon JG, Brown DS, Allaire BT, Dellea PS, Kamal-Bahl SJ. The lifetime medical cost burden of overweight and obesity: implications for obesity prevention. Obesity. 2008;16(8):1843–1848. https://www.ncbi.nlm.nih.gov/pubmed/18535543[↩]
- Finkelstein EA, Trogdon JG, Cohen JW, Dietz W. Annual medical spending attributable to obesity: payer-and service-specific estimates. Health Aff (Millwood) 2009;28(5):w822–831. https://www.ncbi.nlm.nih.gov/pubmed/19635784[↩]
- Kasman M, Hammond RA, Werman A, Mack-Crane A, McKinnon RA. An In-Depth Look at the Lifetime Economic Cost of Obesity. Brookings. 2015 May 12;[↩]
- Chatterjee A, Kubendran S, King J, DeVol R. Checkup Time: Chronic Disease and Wellness in America. Santa Monica, CA: Milken Institute; Jan, 2014.[↩]
- Centers for Disease Control and Prevention (CDC) Trends in the Prevalence of Excess Dietary Sodium Intake — United States, 2003–2010. MMWR Morb Mortal Wkly Rep. 2013;62(50).[↩]
- Guenther PM, Casavale KO, Reedy J, et al. Update of the Healthy Eating Index: HEI-2010. J Acad Nutr Diet. 2013;113(4):569–580. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3810369/[↩][↩]
- Epidemiology and Genomics Research Program, National Cancer Institute. [Accessed Sep 11, 2015];Usual Dietary Intakes: Food Intakes, U.S. Population, 2007–2010. https://epi.grants.cancer.gov/diet/usualintakes/pop/2007-10/[↩]
- Britten P, Cleveland LE, Koegel KL, Kuczynski KJ, Nickols-Richardson SM. Updated US Department of Agriculture Food Patterns meet goals of the 2010 dietary guidelines. J Acad Nutr Diet. 2012;112(10):1648–1655. https://www.ncbi.nlm.nih.gov/pubmed/22853987[↩]