What is amaurosis fugax
Amaurosis fugax is a temporary loss of vision in one or both eyes, usually described as a period of an absolute or near absolute field defect in one eye, due to a lack of blood flow to the retina. The retina is the light-sensitive layer of tissue at the back of the eyeball. Amaurosis fugax is also used widely in medicine to refer to any cause of transient monocular visual loss 1.
Amaurosis fugax is not itself a disease. Instead, amaurosis fugax (transient loss of vision in one eye) is a sign of other disorders. Amaurosis fugax can occur from different causes. One cause is when a blood clot or a piece of plaque blocks an artery in the eye. The blood clot or plaque usually travels from a larger artery, such as the carotid artery in the neck or an artery in the heart, to an artery in the eye. Plaque is a hard substance that forms when fat, cholesterol, and other substances build up in the walls of arteries.
Amaurosis fugax usually occurs in patients over the age of 50 who have other vascular risk factors which include hypertension, hypercholesterolemia, smoking, previous episodes of transient ischemic attacks (TIAs), and claudication. The risk of hemispheric stroke in patients with amaurosis fugax is estimated to be 2% per year and 3% per year for those presenting with retinal emboli 1. In a 2012 study, approximately 1 of every 4 patients with amaurosis fugax (transient loss of vision in one eye) had acute brain infarctions on brain magnetic resonance imaging (MRI) performed with diffusion-weighted imaging 2. In other words, there was evidence of an asymptomatic stroke. More recent studies in both the stroke and ophthalmic literature have shown remarkably similar results 3, 4. For instance, a 2014 study reinforced the strong correlation between the presence of abnormalities on brain magnetic resonance imaging (MRI) performed with diffusion-weighted imaging and positive results on the stroke workup for a major cause of stroke (such as a source of emboli), underscoring the usefulness of immediate brain magnetic resonance imaging (MRI), even in patients who appear neurologically asymptomatic 5.
The first study of choice is an ultrasound of the carotid artery to determine the presence of carotid artery stenosis. When an individual has been diagnosed with amaurosis fugax, it is vital to refer the patient first to a neurologist to confirm the diagnosis and examine for any other neurological deficits. Since many of these patients are smokers and diabetics and may have hypertension, they need a thorough presurgical workup to ensure that they can undergo general or local anesthesia. The time to undergo carotid endarterectomy is variable but expert opinion states that it should be within 4 to 8 weeks 6.
While awaiting surgery, the patient and the family should be educated on the dangers of smoking and the importance of blood pressure control. Your doctor should make sure that you’re is on aspirin and compliant with your blood pressure and diabetes medications. Before surgery, patient should be advised to stop all blood thinners.
Treatment of amaurosis fugax depends on its cause. When amaurosis fugax is due to a blood clot or plaque, the concern is to prevent a stroke. The following can help prevent a stroke:
- Avoid fatty foods and follow a healthy, low-fat diet. DO NOT drink more than 1 to 2 alcoholic drinks a day.
- Exercise regularly: 30 minutes a day if you are not overweight; 60 to 90 minutes a day if you are overweight.
- Quit smoking.
- Most people should aim for a blood pressure below 120 to 130/80 mm Hg. If you have diabetes or have had a stroke, your doctor may tell you to aim for a lower blood pressure.
- If you have diabetes, heart disease, or hardening of the arteries, your LDL (bad) cholesterol should be lower than 70 mg/dL.
- Follow your doctor’s treatment plans if you have high blood pressure, diabetes, high cholesterol, or heart disease.
Your doctor may also recommend:
- No treatment. You may only need regular visits to check the health of your heart and carotid arteries.
- Aspirin, warfarin (Coumadin), or other blood-thinning drugs to lower your risk for stroke.
If a large part of the carotid artery appears blocked, carotid endarterectomy surgery is done to remove the blockage. The decision to do surgery is also based on your overall health.
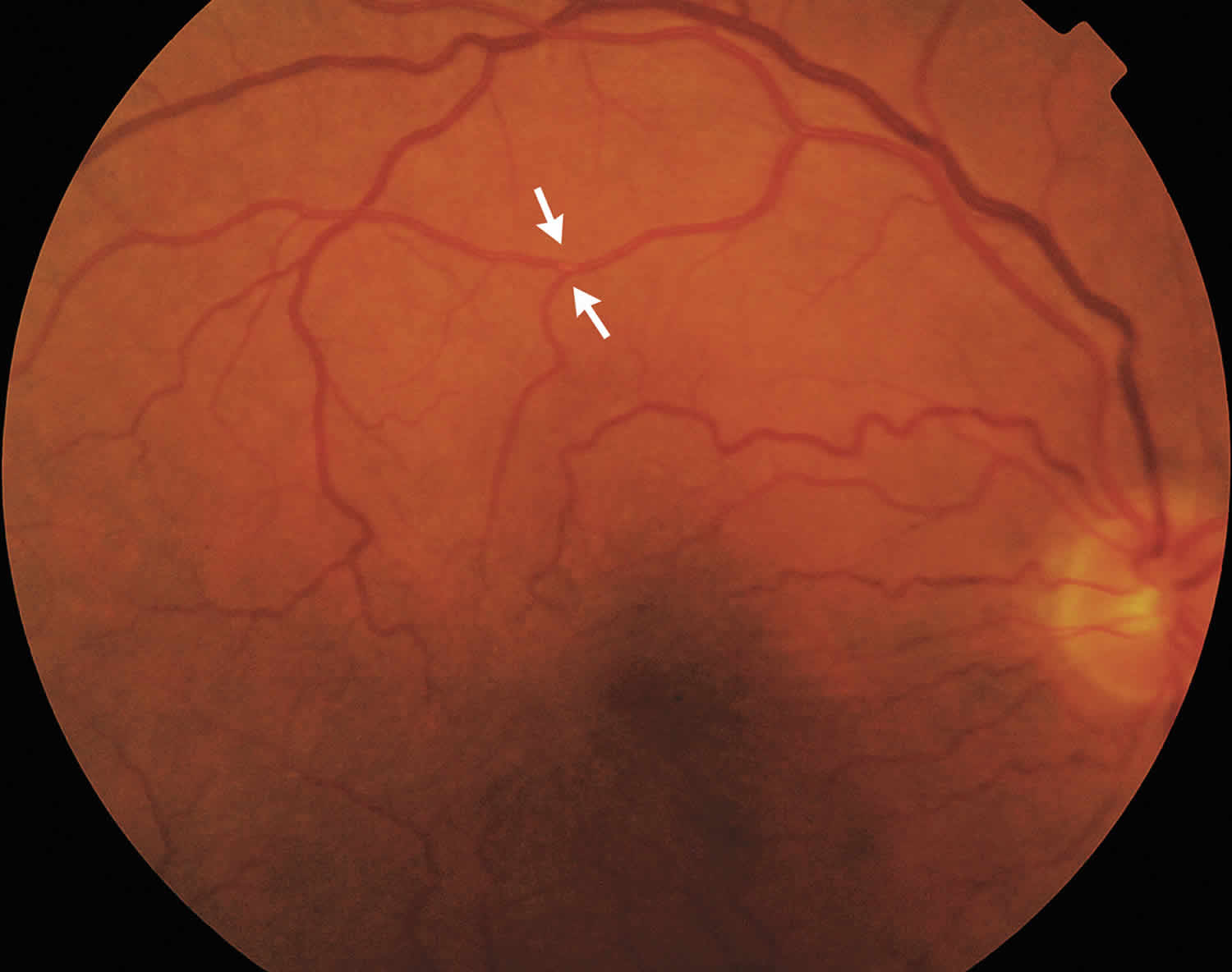
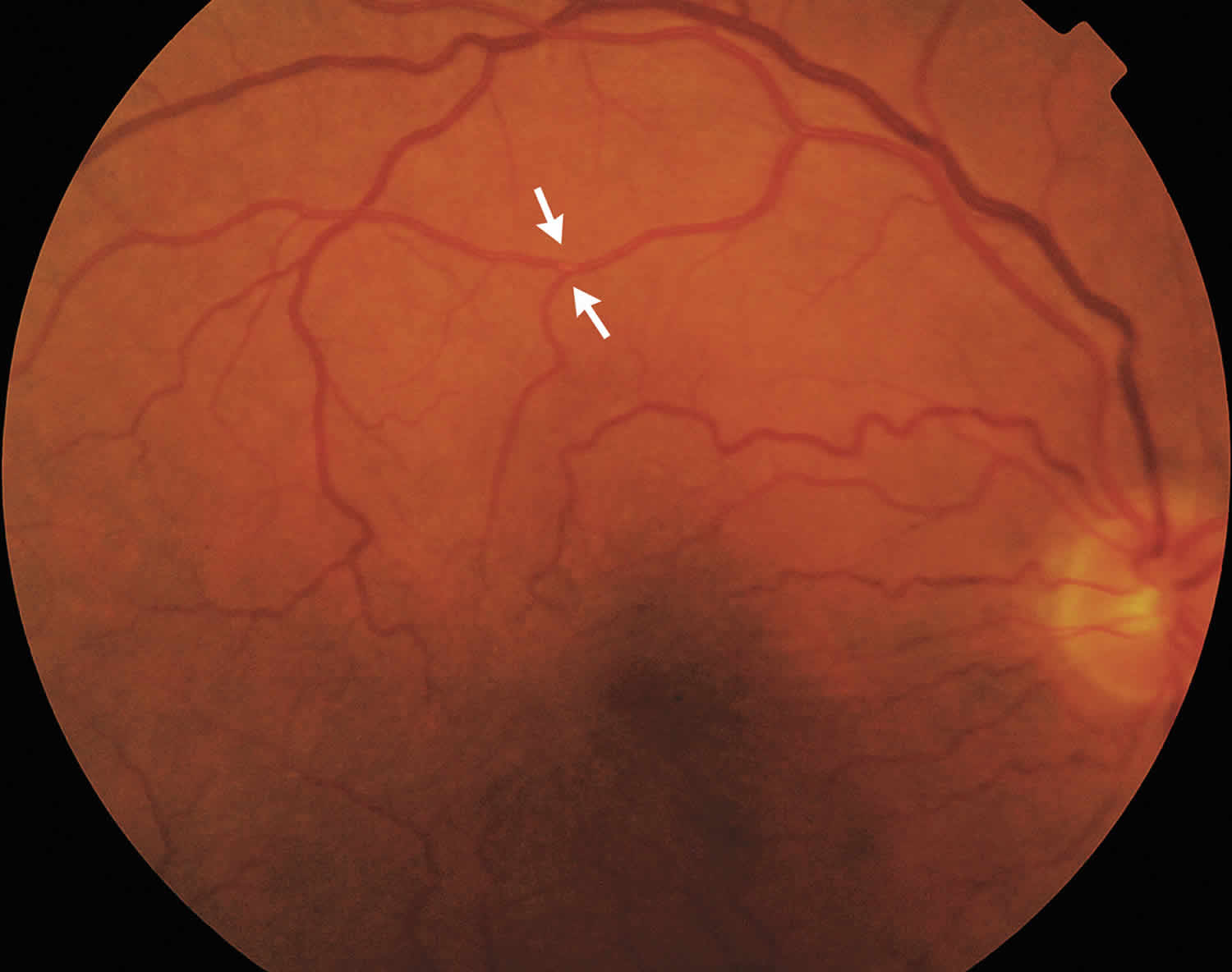
The video below shows a 77-year-old man’s retina (on dilated fundus examination), a motile embolus is visible as a pulsating point of light in the right superior branch of the retinal-artery bifurcation. The man reported having three episodes of blurred vision in his right eye during the past hour, with each episode lasting approximately 5 minutes. The still photograph of the same man is shown in Figure 1 below.
Figure 1. Amaurosis fugax
Footnote: A 77-year-old man presented to the ophthalmology clinic reporting three episodes of blurred vision in his right eye, each lasting approximately 5 minutes, during the past hour. He had been taking statins for hypercholesterolemia for the past 5 years, and his ocular history was unremarkable. The dilated fundus examination revealed a visible motile embolus in the right superior branch of the retinal artery bifurcation; the motile embolus followed the arterial pulsation circle. The diagnostic workup was notable for 80% stenosis of the right internal carotid artery. The patient underwent successful carotid endarterectomy. Twelve months later, his visual acuity was normal, and he had no residual visual symptoms.
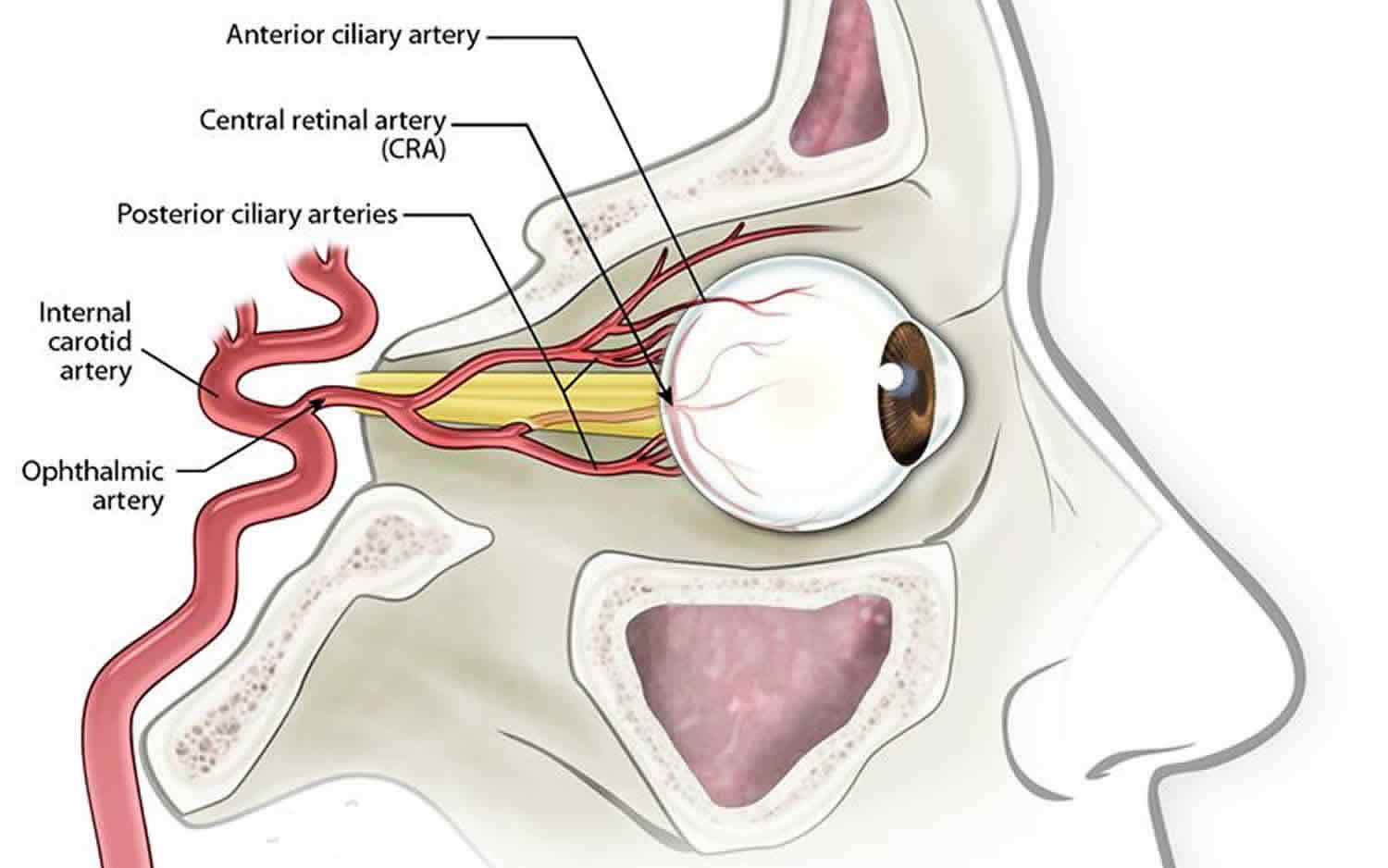
[Source 7 ]Figure 2. Arteries of the eye
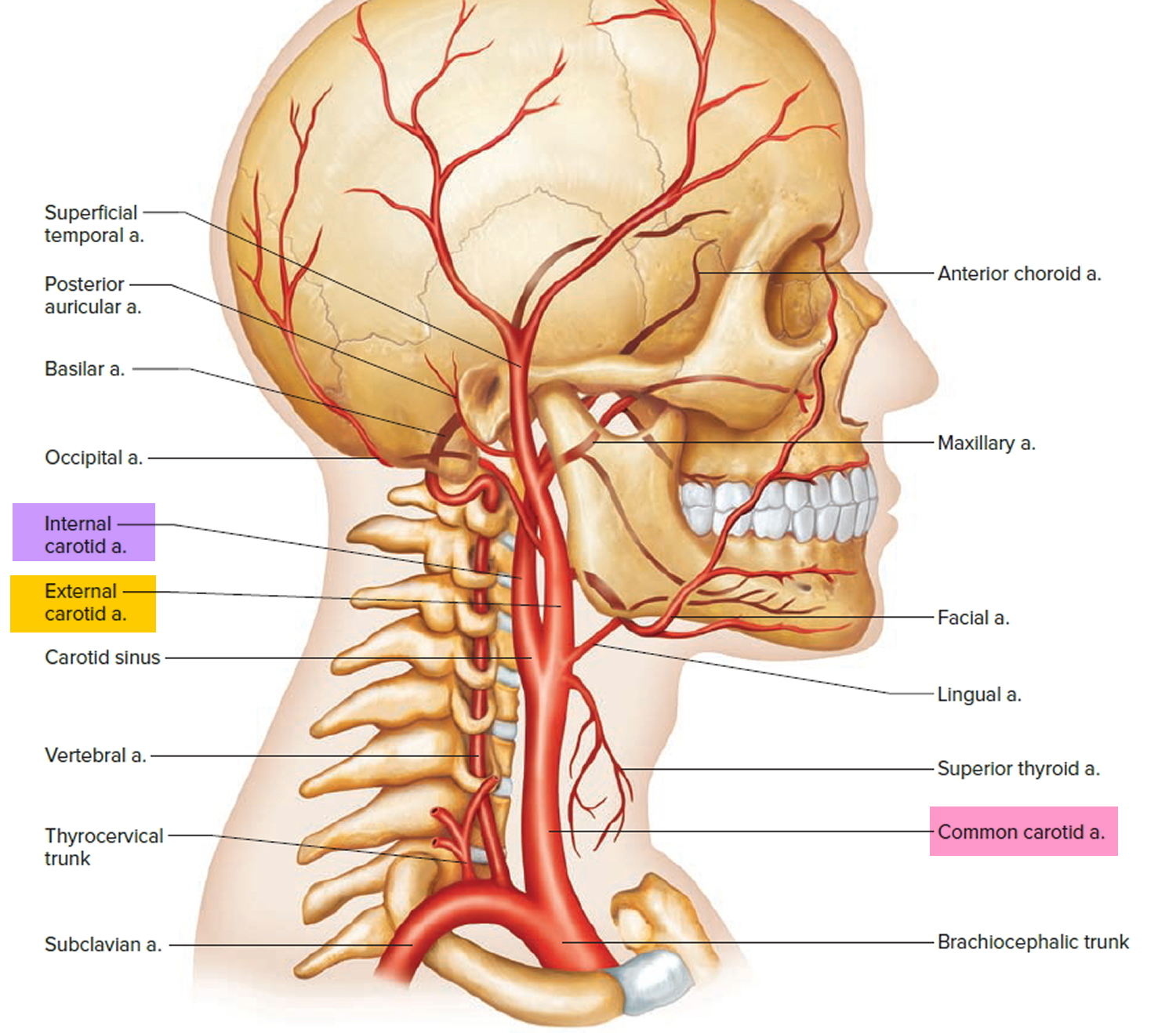
Figure 3. External and Internal carotid artery
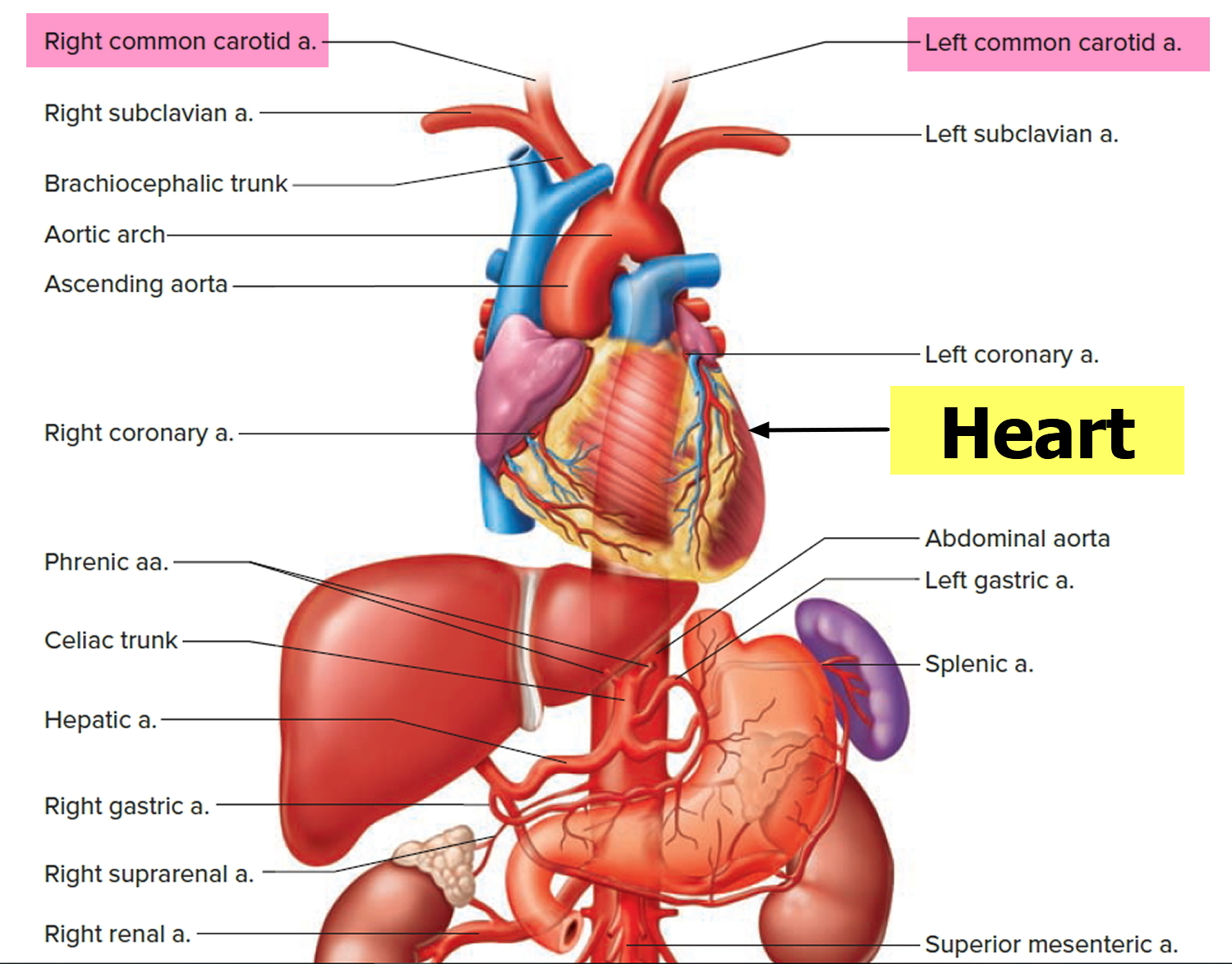
Figure 4. Common carotid artery
Amaurosis fugax causes
Amaurosis fugax is a result of an occlusion or stenosis of the internal carotid artery circulation 1. Thromboembolism originating from the carotid circulation, as well as, hypoperfusion caused by the stenosis of this circulation, are the underlying mechanisms. The ocular ischemic syndrome results from the chronic hypoperfusion due to unilateral or bilateral carotid artery occlusion 8.
Amaurosis fugax may occur due to the following:
- Thromboembolism from the carotid plaque
- Hypoperfusion
- Vasospasm
- Elevated plasma viscosity, for example with leukemia, multiple myeloma
- Atherosclerotic cerebrovascular disease
Amaurosis fugax can also occur because of other disorders such as:
- Other eye problems, such as inflammation of the optic nerve (optic neuritis)
- Blood vessel disease called polyarteritis nodosa
- Migraine headaches
- Brain tumor
- Head injury
- Multiple sclerosis (MS), inflammation of the nerves due to the body’s immune cells attacking the nervous system
- Systemic lupus erythematosus (SLE), an autoimmune disease in which the body’s immune cells attack healthy tissue throughout the body
The prevalence of amaurosis fugax was 12.18% in central retinal artery occlusion, 14.20% in branch retinal artery occlusion, 15.38% in ocular ischemic syndrome, 4.86% in central retinal vein occlusion, 37.84% in central retinal vein occlusion with cilioretinal artery occlusion, 13.43% in hemi-central retinal vein occlusion, 0.35% in branch retinal vein occlusion and 2.54% in nonarteritic anterior ischemic optic neuropathy 9.
The relative prevalence of amaurosis fugax was highest in giant cell arteritis with vision loss; 32.4% of patients with giant cell arteritis with ocular involvement had a history of amaurosis fugax 9.
Risk factors for amaurosis fugax
Amaurosis fugax risk factors include:
- Heart disease, especially irregular heartbeat
- Alcohol abuse
- Cocaine use
- Diabetes
- Family history of stroke
- High blood pressure
- High cholesterol
- Increasing age
- Smoking (people who smoke one pack a day double their risk for a stroke)
Amaurosis fugax differential diagnosis
The differential diagnosis of unilateral vision loss includes the following:
- Central retinal artery/vein occlusion
- Giant cell arteritis
- Multiple sclerosis
- Papilledema
- Epilepsy
- Sickle cell anemia
Amaurosis fugax symptoms
Symptoms include the sudden loss of vision in one or both eyes. In amaurosis fugax, the loss of vision is usually unilateral, painless and transient. In most cases, the vision loss may vary from a few seconds to a few minutes. Afterward, vision returns to normal. Some people describe the loss of vision as a “gray” or “black” or “dim” shade coming down over the eye. Some patients describe a “curtain over the eye” effect where the vision loss seems to close in from one direction.
In some patients, particularly those with the ocular ischemic syndrome, exposure to bright lights can provoke amaurosis fugax episodes, as the same side severe internal carotid occlusion causes hypoperfusion of the retinal circulation and the resulting vascular insufficiency of the retinal photoreceptors combined with increased metabolic demand leads to blurred or decreased vision in those patients 1. Vision usually returns to normal once the photoreceptors have completely hyperpolarized.
Patients with the ocular ischemic syndrome typically present with blurred vision that can be transient. The visual acuity declines with the progression of the disease. The affected eye shows episcleral injection and, on slit-lamp examination, minimal anterior chamber inflammation is present. Intraocular pressure can be low or normal due to the decreased perfusion of the ciliary body which is responsible for aqueous production. Fundus examination usually demonstrates dilated and tortuous retinal veins with narrowed arterioles accompanied by mid-peripheral dot-and-blot retinal hemorrhages. With persistent hypoperfusion, ischemia progresses and manifests as neovascularization of the iris, anterior chamber angle, retina, and optic disc. Ocular pain is a hallmark of the disease and is usually alleviated in the supine position. The latter is a result of ischemia of the ocular and orbital branches of the trigeminal nerve 10.
Amaurosis fugax diagnosis
Your doctor will perform a complete eye and nervous system exam. During the retinal examination, your health care provider may see the cholesterol plaque lodged within a retinal artery. It is known as a Hollenhorst plaque (cholesterol plaque), and the cholesterol particle appears refractile yellow and bright 11.
Tests that may be done include:
- Carotid Doppler ultrasound is a non-invasive test used to assess the extracranial and intracranial status of the vessels.
- Magnetic resonance angiography (MRA) and computed tomography angiography can also be used to evaluate the patency of the internal carotid arteries and to check for blood clots or plaque.
- Complete blood count (CBC), blood glucose level, lipid profile, prothrombin time and partial thromboplastin time, erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP) 12
- Because vasospastic amaurosis has been associated with polyarteritis nodosa and eosinophilic vasculitis, additional autoimmune serologies (ANA and ANCA) should be considered.
- Tests of the heart, such as an electrocardiogram (ECG) as well as Holter monitoring, to check its electrical activity.
- In some cases, transesophageal echocardiography (TEE), should be obtained to rule out any possible source of rhythmic disturbance or cardiac emboli.
- In addition, the CT brain scan can help rule out a hemorrhagic lesion in the brain.
Amaurosis fugax prognosis
Amaurosis fugax is a harbinger of an imminent stroke. Amaurosis fugax increases your risk for stroke. The risk of hemispheric stroke in patients with amaurosis fugax is estimated to be 2% per year and 3% per year for those presenting with retinal emboli 1. There is plenty of evidence that treating patients with amaurosis fugax can prevent a full-blown stroke.
Amaurosis fugax treatment
Treatment is first aimed at controlling and treating the underlying vascular risk factors, such as hypertension, diabetes, and hyperlipidemia.
The treatment of carotid artery stenosis is in a state of flux. Carotid artery stenosis can also be managed with angioplasty and stenting. For patients who are unfit for surgery or those who are asymptomatic, the endovascular approach may be viable, but symptomatic patients need an open procedure. There still remains debate as to which procedure is safer and the data are mixed and confusing because of the heterogeneity of the patients. The most important thing is to ensure that a patient with amaurosis fugax gets the appropriate referral to a neurologist first to confirm the diagnosis. The choice between a vascular or an endovascular procedure depends on personal preference. Both are safe procedures, and both have a role in the treatment of this serious disorder 13. Whatever choice one makes, the person doing the procedure must be experienced.
Two large studies, the North American Symptomatic Carotid Endarterectomy Trial (NASCET) and the European Carotid Surgery Trial (ECST), found that endarterectomy in symptomatic patients who have carotid stenosis greater than 70% reduces future risks of stroke 1. However, these studies did not address ocular transient ischemic attacks (TIAs) separately. The North American Symptomatic Carotid Endarterectomy Trial (NASCET) further compared patients with hemispheric transient ischemic attacks (TIAs) and ocular transient ischemic attacks (TIAs) demonstrating that patients with hemispheric transient ischemic attacks (TIAs) had a 2-year stroke incidence of about 44% compared to about 17% in ocular transient ischemic attacks (TIAs). The patients with ocular transient ischemic attacks (TIAs) did not experience a major stroke episode, which was defined as a functional deficit persisting for more than 90 days. Both groups also had similar grades of carotid stenosis (about 83%) 14.
Therefore, the clinician needs to address if the risks of death and preoperative stroke in patients undergoing endarterectomy outweigh the low risk of observing these specific patients and treating them with anticoagulants alone, such as aspirin, warfarin or clopidogrel.
It is important to note that both the North American Symptomatic Carotid Endarterectomy Trial (NASCET) and the European Carotid Surgery Trial (ECST) evaluated open endarterectomy but, since then, carotid stenting has become commonly used. Carotid stenting is comparable to endarterectomy, regarding treatment, and has similar low risks of death, stroke and myocardial infarction in patients with asymptomatic severe carotid artery stenosis 15.
Treatment of ocular ischemic syndrome involves reducing the oxygen drive to the eye to decrease the neovascularization. This involves panretinal photocoagulation or intravitreal injections of anti-vascular endothelial growth factor (VEGF).
- Najem K, Margolin E. Amaurosis Fugax. [Updated 2018 Nov 14]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2018 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK470528[↩][↩][↩][↩][↩][↩]
- Helenius J et al. Ann Neurol. 2012;72(2):286-293.[↩]
- Golsari A et al. Stroke. 2017;48:1392-1396.[↩]
- Lauda F et al. Cerebrovasc Dis. 2015;40(3-4):151-156.[↩]
- Lee J et al. Am J Ophthalmol. 2014;157(6):1231-1238.[↩]
- Meyer D, Karreman E, Kopriva D. Factors associated with delay in carotid endarterectomy for patients with symptomatic severe internal carotid artery stenosis: a case-control study. CMAJ Open. 2018 May 15;6(2):E211-E217.[↩]
- Amaurosis Fugax Caused by a Branch Retinal Artery Embolus. N Engl J Med 2015; 373:e26 https://www.nejm.org/doi/full/10.1056/NEJMicm1500779[↩]
- Makhkamova DК. [Etiopathogenesis of ocular ischemic syndrome]. Vestn Oftalmol. 2017;133(2):120-124.[↩]
- AMAUROSIS FUGAX IN OCULAR VASCULAR OCCLUSIVE DISORDERS: Prevalence and Pathogeneses. Retina: January 2014 – Volume 34 – Issue 1 – p 115–122 doi: 10.1097/IAE.0b013e31829234b5[↩][↩]
- Kvickström P, Lindblom B, Bergström G, Zetterberg M. Amaurosis fugax: risk factors and prevalence of significant carotid stenosis. Clin Ophthalmol. 2016;10:2165-2170[↩]
- McCullough HK, Reinert CG, Hynan LS, Albiston CL, Inman MH, Boyd PI, Welborn MB, Clagett GP, Modrall JG. Ocular findings as predictors of carotid artery occlusive disease: is carotid imaging justified? J. Vasc. Surg. 2004 Aug;40(2):279-86.[↩]
- Hagiwara Y, Shimizu T, Hasegawa Y. Contrast-enhanced transoral carotid ultrasonography for the diagnosis and follow-up of extracranial internal carotid artery dissection: A case report. J Clin Ultrasound. 2018 Jun;46(5):368-371[↩]
- Pothof AB, Zwanenburg ES, Deery SE, O’Donnell TFX, de Borst GJ, Schermerhorn ML. An update on the incidence of perioperative outcomes after carotid endarterectomy, stratified by type of preprocedural neurologic symptom. J. Vasc. Surg. 2018 Mar;67(3):785-792.[↩]
- Hayreh SS, Zimmerman MB. OCULAR ARTERIAL OCCLUSIVE DISORDERS AND CAROTID ARTERY DISEASE. Ophthalmol Retina. 2017 Jan-Feb;1(1):12-18.[↩]
- Pribán V, Fiedler J, Chlouba V. [Ocular symptoms as an indication for carotid endarterectomy]. Cesk Slov Oftalmol. 2006 Sep;62(5):354-9.[↩]