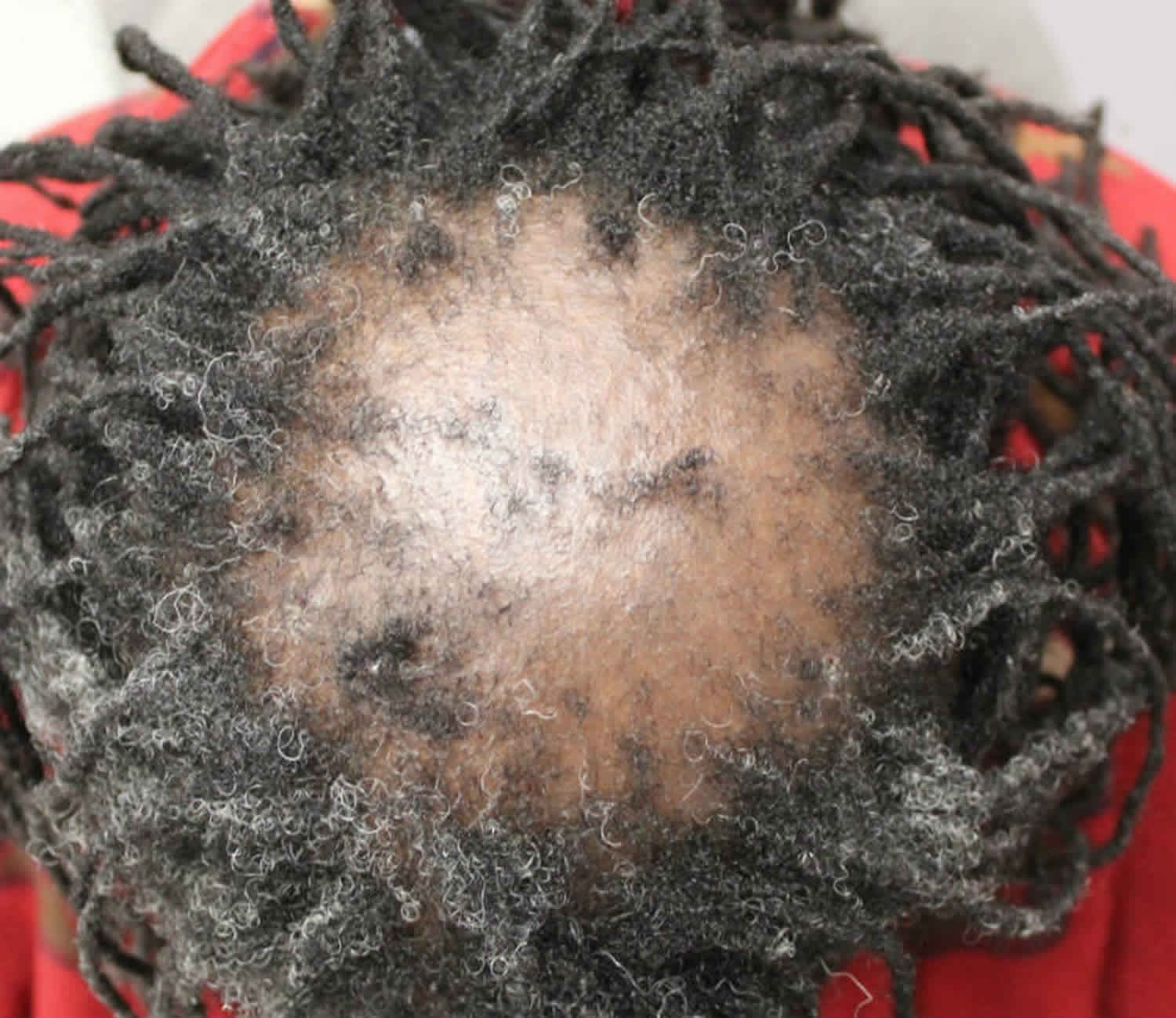
Central centrifugal cicatricial alopecia
Central centrifugal cicatricial alopecia (CCCA) is a form of scarring alopecia (hair loss) on the scalp that results in permanent hair loss. Central centrifugal cicatricial alopecia is the most common form of scarring hair loss seen in black women (African ethnicity). However, it may be seen in men and among persons of all races and hair color (though rarely). Middle-aged women are most commonly affected. Central centrifugal cicatricial alopecia usually presents in the fourth decade with a female to male ratio of approximately 3:1.
Central centrifugal cicatricial alopecia is a diagnostic category adopted by the North American Hair Research Society to encompass terms such as hot comb alopecia, follicular degeneration syndrome, pseudopelade in African Americans, and central elliptical pseudopelade in whites 1. Despite the many attempts to clarify and unify the terminology of central centrifugal cicatricial alopecia patterns of scarring alopecia, CCCA is not clearly a diagnostic entity in and of itself.
Clinically there is a diffuse scarring alopecia that begins at the crown and spreads forwards. The alopecia is incomplete with a number of hairs remaining within the area of scarring. There tends to be little or no redness.
No ideal treatment currently exists. Minimal hair grooming is recommended, but many patients find this difficult. If there are signs of inflammation (clinically or histologically) the use of a potent topical or intralesional corticosteroid may arrest or slow progression. Occasionally pustules are seen in which case a systemic tetracycline such as doxycycline or lymecycline may be of value. Other treatments occasionally used in the presence of inflammation include those used for lichen planopilaris.
Cicatricial alopecia
Cicatricial alopecia the generic term used to describe a group of conditions that destroy hair follicles resulting in circular or oval shaped patches of scarring (cicatricial) alopecia.
Hair follicles are the part of the skin where the hair grows. The follicles are replaced with scar tissue. This means the hair will fall out and not grow back.
Hair follicles undergo a repetitive sequence of growth and rest known as the hair cycle. To understand the different causes of alopecia or hair loss it is important to have a comprehension of the hair cycle:
- Anagen – is the period of active growth and may last for several years. Under normal circumstances 80-90% of hair follicles on the human scalp are in anagen at any one time
- Catagen – at the end of anagen, epithelial cell division declines and ceases, the hair follicle enters an involutionary phase known as catagen
- Telogen – the period between the completion of follicular regression and the onset of the next anagen phase is known as telogen, during which time the hair is shed
- Kenogen – in the human scalp, hair follicles may remain in a state of latency, also known as kenogen, for a prolonged period after the hair is shed
Cicatricial alopecias or scarring alopecias have loss of follicular ostia, or atrophy. Clinical inflammation is frequently, but not always, present. Histologic inflammation may be present. Ultimately, histologic confirmation is the best method to confirm the presence of a fibrosing or scarring process with loss of hair follicles.
The following conditions are all associated with cicatricial alopecia 2:
- Lichen planopilaris
- Follicular erythema and keratotic plugs, which are commonly located at the periphery of expanding areas of alopecia
- Dermoscopic features – perifollicular scale and inflammation.
- The diagnosis of lichen planopilaris is confirmed by a combination of clinical and histologic features. The following subtypes are recognized 1:
- Frontal fibrosing alopecia: This is a potential clinical variant of lichen planopilaris, with similar histologic features. Frontal fibrosing alopecia has been associated with the postmenopausal state (ie, postmenopausal frontal fibrosing alopecia), although not all patients with this diagnosis are postmenopausal.
- Fibrosing alopecia in pattern distribution: This also is a potential clinical variant of lichen planopilaris, with similar histologic features. Additionally, fibrosing alopecia in pattern distribution has some histologic/clinical overlap with androgenetic alopecia. Fibrosing alopecia in pattern distribution may also be an overlap of lichen planopilaris with androgenetic alopecia.
- Graham-Little syndrome: This entity is also a possible overlapping condition, with features of lichen planopilaris and other alopecia types.
- Discoid lupus erythematosus
- Much more common in women
- Scarring alopecia occurs in 20% of men and 50% of women with discoid lupus erythematosus
- Although discoid lupus erythematosus often presents on the face, the scalp can be the only affected site
- The scalp is often itchy
- Affected patches are erythematous and scaly with follicular plugging
- Dermoscopic features – often chaotic with yellow rough looking follicular plugs, telangiectasia and white or dark areas. Erythema and scale may be more pronounced around the periphery of areas of alopecia
- Patients are treated along the lines of cutaneous lupus with UV-protection, super-potent topical steroids, intralesional steroids and antimalarial therapy (hydroxychloroquine +/- mepacrine). Other treatments sometimes used include retinoids (studies undertaken used acitretin), dapsone, thalidomide and occasionally immunosuppressive therapies.
- Folliculitis decalvans
- Patients usually present with one or more round patches of scarring alopecia usually surrounded by pustules, crusting and sometimes erosions
- Nearly always starts on the crown and expands outwards
- Dermoscopic features – marked ‘dolls hair’ tufting, scale, perifollicular and interfollicular erythema, pustules. Crusting will be present if the inflammation is very active.
- Central centrifugal cicatricial alopecia (CCCA).
Is cicatricial alopecia contagious?
Cicatricial alopecia is not contagious. Anyone can get cicatricial alopecia, but it is not common in children. Cicatricial alopecia usually affects only one family member.
What causes cicatricial alopecia?
No one knows what causes cicatricial alopecia. What is known is that redness, heat, pain, or swelling occurs at the upper part of the hair follicle. This destroys a special type of cell and oil glands that are important for hair to grow. Hair falls out and can’t grow back when this happens.
What are the symptoms of cicatricial alopecia?
Common symptoms when the hair falls out very fast are itching, pain, and burning. When the hair falls out very slowly there are usually no symptoms.
Cicatricial alopecia diagnosis
To see if you have cicatricial alopecia, your doctor may:
- Take samples from where you’ve lost hair.
- Look at your head for signs of redness and infection and to see how much hair you’ve lost.
- Ask you if there are areas on your head where you feel itching, burning, or soreness.
- See if hairs easily pull out.
- Look at the hairs that were pulled out to see if they are growing or not.
Cicatricial alopecia treatment
Dermatologists treat cicatricial alopecia. These are doctors trained to diagnose and treat diseases of the skin, hair, and nails.
Medication
Medicines could be taken by mouth, applied to the top of the skin, or injected into areas where you lost hair. If taken early in the disease, the medicines might be able to help grow hair before the damage becomes permanent.
Treatment usually lasts a long time. It continues until hair loss slows or stops. Treatment may need to be restarted if the disease starts up again.
Surgery
If you haven’t had hair loss from the disease for 1 to 2 years, surgery can help put hair back on bald areas. The surgeon may take hairs from the back of the head and implant them into the bare areas. Or the surgeon may cut out bald spots and pull the scalp together to cover the gap. The disease may come back even after these surgeries.
Central centrifugal cicatricial alopecia causes
The exact cause of CCCA is unknown, but it has often been linked to hair styling practices, which include: heat (hot combs/hair straighteners, hair dryers and curling irons); traction (tight braids/cornrows, weaves, tight ponytails or hair extensions that pull on the hair); and use of chemical relaxers (especially lye relaxers).
More recently, changes in a gene called PADI3, which encodes peptidyl arginine deiminase type III (PADI3), an enzyme that modifies proteins that are essential to formation of the hair-shaft have been linked with development of the condition in about 25% of cases. Other proposed causative factors include fungal infections, bacterial infections, autoimmune disease, and genetics. Several studies have also reported an association of type 2 diabetes with hair loss, and potentially with CCCA.
Traction (from heated styling instruments or chemical straighteners), pattern hair loss and iron-deficiency may co-exist. Central centrifugal cicatricial alopecia is also associated with hirsutism.
Central centrifugal cicatricial alopecia symptoms
In CCCA hair tends to start falling out in the middle of the scalp. Hair loss then gradually spreads out from that point in a centrifugal manner. Often, people with CCCA notice hair being more brittle and breaking more easily. Other symptoms include itching, pain or tenderness of the scalp, a spongy texture to the scalp, and flaking or redness of the affected areas.
There is loss of the follicular openings on examination of the scalp. Thus, the scalp may appear shiny. While some persons do not have symptoms, tenderness, itch and burning are common. Hair breakage may also be an early sign of central centrifugal cicatricial alopecia. Hair loss is slowly progressive. A photographic scale has been developed to rate the severity of the central hair loss.
Central centrifugal cicatricial alopecia diagnosis
Early diagnosis of central centrifugal cicatricial alopecia is important because medical intervention can prevent further progression that often results in extensive, permanent hair loss. Diagnosis is based on clinical features, scalp biopsy and exclusion of other hair loss disorders.
Scalp biopsy should be taken from an active edge of a patch of alopecia rather than the center of a scarred area. Histopathology reveals a lymphocytic inflammatory infiltrate (inflammatory cells) around the infundibulum (base of the hair follicle), and fibrosis (scarring). Premature desquamation (peeling) of the inner root sheath is a common feature.
Mycology to rule out tinea capitis is recommended.
Central centrifugal cicatricial alopecia treatment
The goal of therapy is to halt progression of disease and prevent further hair loss. In areas where the hair follicle has been replaced with fibrosis, regrowth is not possible. As the exact cause is not known, targeted therapy for central centrifugal cicatricial alopecia is not available.
Usually, your doctor will prescribe topical or injected corticosteroids, which help to dampen down the inflammation. Other treatments include tetracyline (an antibiotic), ciclosporin (a drug that slows down the immune attack on the hair follicles) or hydroxychloroquine (an anti-malaria drug that also helps to suppress the immune system). People with CCCA are also recommended to use natural hair styles.
Treatment options for central centrifugal cicatricial alopecia include anti-inflammatory agents such as 3:
- Potent topical steroids (e.g., clobetasol) or intralesional steroids
- Calcineurin inhibitors: tacrolimus ointment, pimecrolimus cream
- Tetracyclines (eg doxycycline 100 mg twice daily, taken for several weeks to months)
- Hydroxychloroquine
- Ciclosporin.
Hair transplantation can be considered in individuals with well-controlled central centrifugal cicatricial alopecia for at least one year. However, graft survival is low.
Minoxidil solution may help stimulate growth in viable follicles. Seborrheic dermatitis should be treated with appropriate medicated shampoos and topical anti-inflammatory agents as needed.
Discontinuation of traumatic hair care practices is an essential aspect of treatment of central centrifugal cicatricial alopecia.
Women with central centrifugal cicatricial alopecia are encouraged to consider natural hairstyles:
- Relaxers should be performed by a professional, no more frequently than every 6-8 weeks. The scalp should not burn as a result of relaxer application.
- Minimize heat application (hooded dryers, blow dryers, hot combs and flat irons)
- Avoid tight braids and weaves/extensions
- Avoid hair style practices associated with discomfort, scalp irritation or scale
- It is important for providers to know that frequency of shampooing the hair varies among Black women. Many shampoo every 1–2 weeks. This is the norm and prevents excessive dryness.
- Zinkernagel MS, Trüeb RM. Fibrosing alopecia in a pattern distribution: patterned lichen planopilaris or androgenetic alopecia with a lichenoid tissue reaction pattern?. Arch Dermatol. 2000 Feb. 136(2):205-11.[↩][↩]
- Scarring Alopecia. https://emedicine.medscape.com/article/1073559-overview[↩]
- Central centrifugal cicatricial alopecia. https://dermnetnz.org/topics/central-centrifugal-cicatricial-alopecia[↩]