What is heterochromia
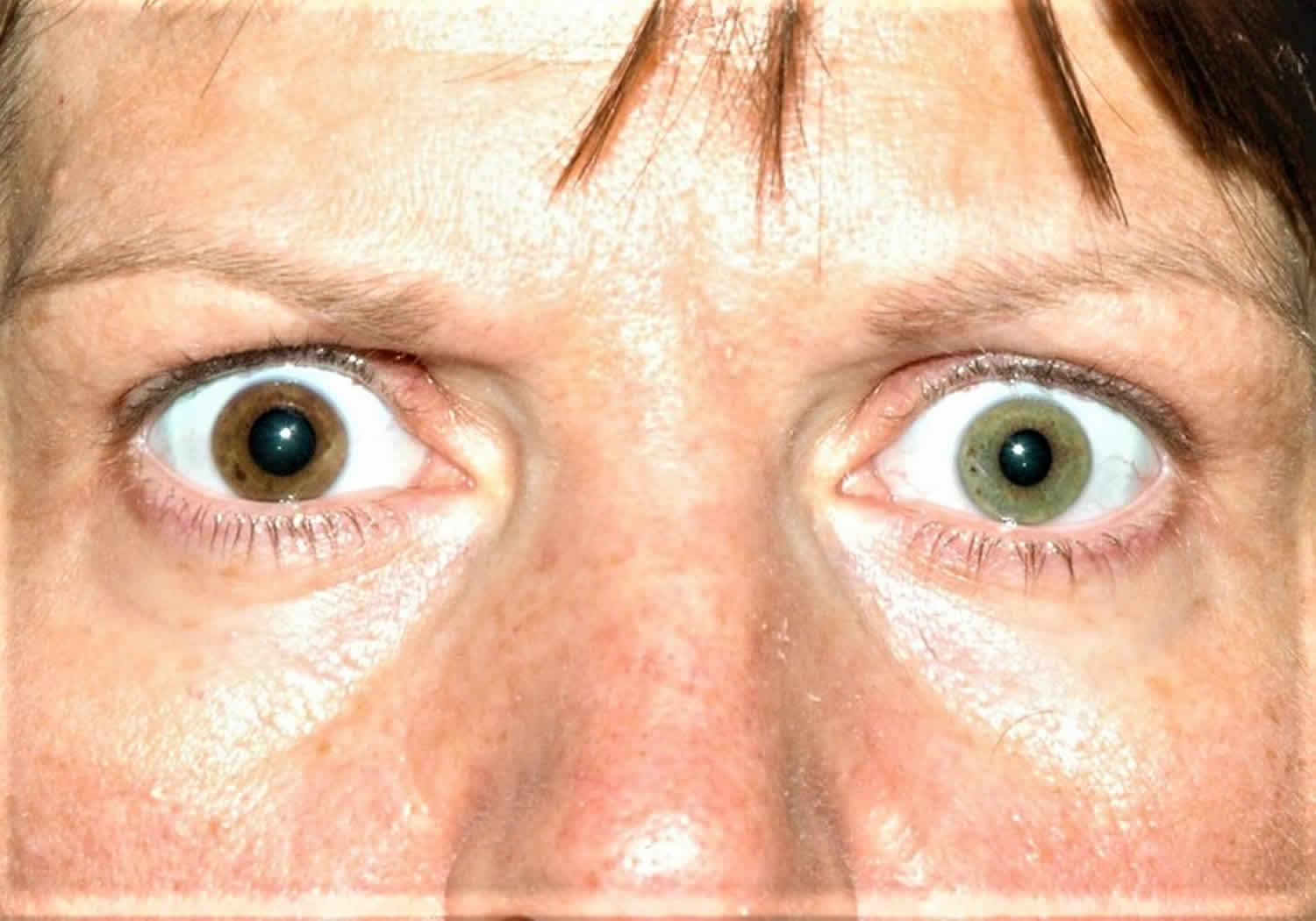
Heterochromia is different colored eyes in the same person. Heterochromia is when a person’s irises (the colored part of the eye) are different colors. Heterochromia is also called heterochromia iridum or heterochromia iridis. Heterochromia is uncommon in humans. Heterochromia is quite common in dogs (such as Dalmatians and Australian sheep dogs), cats, and horses.
There are a few kinds of heterochromia. In people affected by complete heterochromia, the iris of one eye is a different color than the iris of the other eye. When part of one iris is a different color than the rest of it, this is called partial heterochromia. Segmental heterochromia occurs when areas of the same iris are different in color. Central heterochromia is when there is an inner ring that is a different color than the outer area of the iris.
A person’s eye color results from pigmentation of a structure called the iris, which surrounds the small black hole in the center of the eye (the pupil) and helps control how much light can enter the eye. The color of the iris ranges on a continuum from very light blue to dark brown. Most of the time eye color is categorized as blue, green/hazel, or brown. Brown is the most frequent eye color worldwide. Lighter eye colors, such as blue and green, are found almost exclusively among people of European ancestry.
Eye color is determined by variations in a person’s genes. Most of the genes associated with eye color are involved in the production, transport, or storage of a pigment called melanin. Eye color is directly related to the amount and quality of melanin in the front layers of the iris. People with brown eyes have a large amount of melanin in the iris, while people with blue eyes have much less of this pigment.
Most cases of heterochromia iridis occur sporadically and are not associated with any other symptoms or problems. Rarely, heterochromia iridis is part of a congenital (present from birth) syndrome such as Waardenburg syndrome, Sturge-Weber syndrome, Parry-Romberg syndrome, or Horner’s syndrome. Treatment for heterochromia iridis generally targets the underlying cause and/or any associated symptoms (if present).
Heterochromia in humans appears either as a hereditary trait unassociated with other disease, as a symptom of various syndromes or as the result of a trauma.
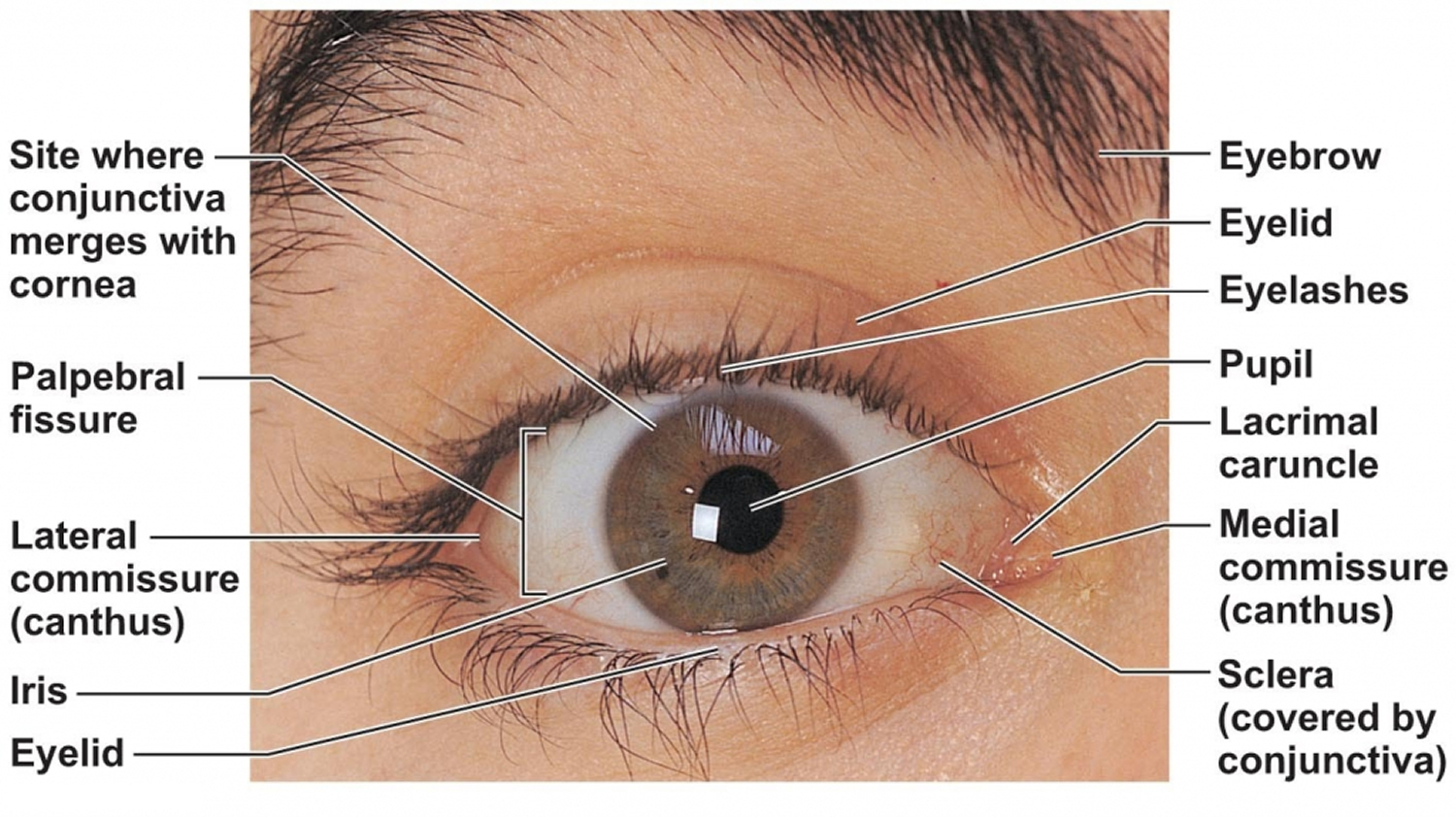
Figure 1. Human eye
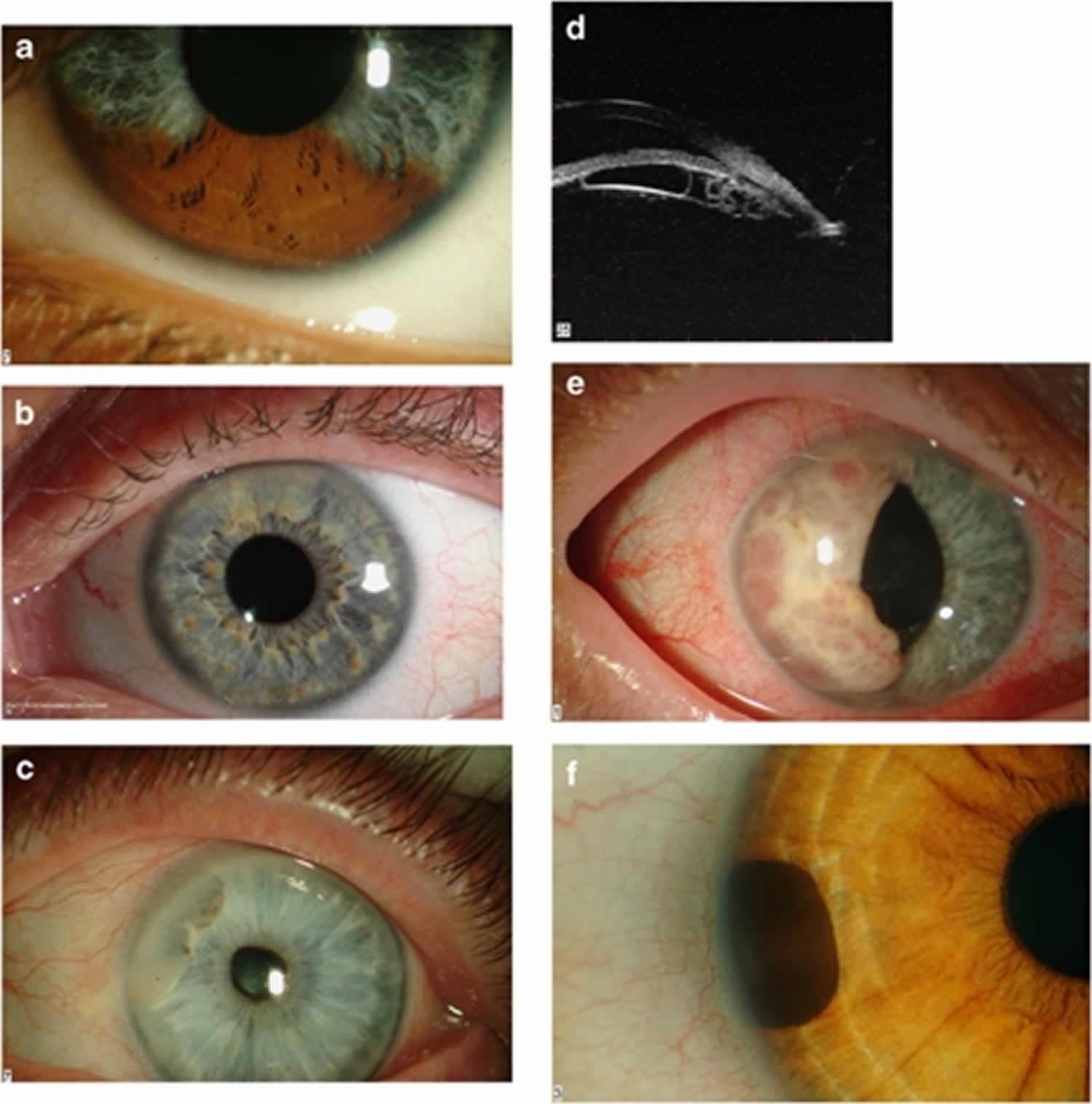
[Source 1 ]Figure 3. Heterochromia
Footnote: (a) Sectorial pigmentation in Waardenburg syndrome. (b) Lisch nodules in neurofibromatosis type-I. Note the predominant inferior location. (c) Anterior stromal cyst containing a turbid sediment. (d) Multiple posterior pigment epithelial cysts. This patient presented with raised intraocular pressure. Note the plateaux iris configuration. (e) A large iris metastasis in a patient with an occult bronchiogenic carcinoma. (f) A peripheral iris melanocytoma.
[Source 2 ]See to your health care provider if you notice new changes in the color of one eye, or two differently colored eyes in your infant. A thorough eye exam is needed to rule out a medical problem.
Some conditions and syndromes associated with heterochromia, such as pigmentary glaucoma, can only be detected by a thorough eye exam.
An infant with heterochromia should be examined by both a pediatrician and an ophthalmologist for other possible problems.
A complete eye exam can rule out most causes of heterochromia. If there doesn’t seem to be an underlying disorder, no further testing may be needed. If another disorder is suspected diagnostic tests, such as blood tests or chromosome studies, may be done to confirm the diagnosis.
Should I be concerned that my son has different colors within his iris?
Heterochromia is the presence of different colors in the iris either between both eyes or in the same eye. While a baby’s eye color changes commonly during the first year of life, you may be able to tell if there is sectorial heterochromia, where a portion of the eye is a different color. Since ocular melanoma (cancer of the eye) is very rare in childhood, often this is a benign (harmless) increase in pigment (color) in the iris. However, discolorations of a portion of the iris could represent signs of other conditions, which need to be treated. A pediatric ophthalmologist can evaluate the iris of your infant and guide you further if any investigation is warranted.
How rare is heterochromia?
Heterochromia iridis is rare, affecting fewer than 200,000 people in the United States 1.
Normal eye color and pigmentation of the iris
Anatomically the iris is composed of two layers of different embryological origin. The anterior layer is the iris stroma, which is derived from the mesoderm and consists of a loose collagenous network, which contains the sphincter pupillae muscle, blood vessels, nerves, and cellular elements, including fibroblasts, melanocytes, clump cells, and mast cells. The anterior border layer is a condensation of connective tissue of the anterior stroma and contains numerous pigment cells. Iris stromal, ciliary body, and choroidal melanocytes are all derived from the neural crest, a transient population of cells, unique to vertebrates 3. Uveal melanocytes differ from their cutaneous counterparts in one important respect: cutaneous melanocytes ‘inoculate’ melanosomes into the surrounding epithelial cells; by contrast, uveal melanocytes remain continent and do not release melanosomes into the surrounding tissues. The posterior pigment epithelium forms the posterior layer and is neuroectodermal in origin. The posterior pigment epithelium is derived from the anterior portion of the optic cup. It consists of two layers of cuboidal pigment cells, which are tightly joined to each other by numerous intercellular junctions 4.
It is believed that there are four main factors, which determine iris color: the pigment granules within the posterior pigment epithelium, the concentration of pigment within the iris stromal melanocytes, the nature of melanin pigment within the iris melanocytes, and the light-scattering and absorption properties of the extracellular stromal matrix 5. It is generally considered that the concentration of melanosomes in the posterior pigment epithelium is relatively constant in normal individuals and as a result it has little impact differences in normal eye color. The posterior pigment epithelium is only an important determinant of eye color when it is deficient in normal melanosomes in conditions such as albinism.
The density of the iris stroma is the main determinant of color in blue irides. The blue appearance is a result of backscatter of incident light by stromal collagen fibres. Light of longer wavelength readily penetrates the iris and is absorbed, whereas light with a shorter wavelength is reflected back and scattered by the stromal matrix 3. The pigment content of the iris stroma and anterior border layer is responsible for determining all of the shades of iris color from green to dark brown. Increasing pigment within the iris stroma leads to greater light absorption and the resulting darker eye color 6. While increasing stromal pigment content undoubtedly influences iris color, some controversy still remains as to whether this is due to an increased number of pigment cells, the density of pigment within the cells (melanosome density in size), or the type of melanin contained within the melanosome. Although studies by Fuchs 7 and Dietrich 8 supported the notion that the number of melanocytes in the anterior border layer accounted for the differences in iris color, other studies have concluded that the number of melanocytes within the anterior border layer are relatively constant, irrespective of eye color 9. Further studies using electron microscopy and immunohistochemistry to examine the morphology and quantity of stromal melanocytes have again concluded that the relative numbers of these cells is not a major determinant to iris color 10. It would appear based on the electron microscopy of the iris stroma that the number and size of melanosomes contained within melanocytes may have a significant role in determining eye color 11.
Melanin is an inert biopolymer that exists in two distinct forms: brown-black eumelanin and red-yellow pheomelanin. Melanocytes have the capacity to produce both forms of melanin; however, the ratio of the two forms can vary widely in individuals, producing different shades of hair and skin color 12. In a recent study Prota et al 5 characterized the type of melanin, which occurred in human irides. They concluded that the melanocytes within the posterior pigment epithelium contained essentially eumelanin, whereas those extracted from iris tissue in which the pigment epithelium had been removed by scraping (consisting of mainly stroma and anterior iris pigment epithelium) contained both eumelanin and pheomelanin. Furthermore, they noted that pheomelaninic-type pigmentation was associated with green irides, whereas green blue mixed color irides contained mostly eumelanin. By contrast, they were unable to categorise green-brown or brown irides into either of the two forms and concluded that they probably contained mixed pigment content.
The final adult iris color is not present at birth, and in Caucasians the neonatal iris is blue as a result of a paucity of stromal melanocytes, which, presumably, have yet to migrate from the neural crest or differentiate from the primitive precursor cells. In non-White races the iris appears slate grey at birth. The iris normally adopts its true adult color by the age of 3–5 months 4.
The genetics of eye color
Researchers used to think that eye color was determined by a single gene and followed a simple inheritance pattern in which brown eyes were dominant to blue eyes. Under this model, it was believed that parents who both had blue eyes could not have a child with brown eyes. However, later studies showed that this model was too simplistic. Although it is uncommon, parents with blue eyes can have children with brown eyes. The inheritance of eye color is more complex than originally suspected because multiple genes are involved. While a child’s eye color can often be predicted by the eye colors of his or her parents and other relatives, genetic variations sometimes produce unexpected results.
Recent studies suggest that eye color is inherited as a polygenic trait, which, as yet, is incompletely understood 2. A number of pigment genes have been implicated in determining eye color: these include OCA2, HERC2, TYR, TYRP1, MAPT, MYO5A, ASIP, IRF4, SLC24A4, SLC24A5, SLC45A2 and TPCN2 13. A particular region on chromosome 15 plays a major role in eye color. Within this region, there are two genes located very close together: OCA2 and HERC2. Of these, the OCA2 gene, which is located in the long arm of chromosome-15 (15q11.2–15q-12) would appear to be the most influential 14. The protein produced from the OCA2 gene, known as the P protein, is involved in the maturation of melanosomes, which are cellular structures that produce and store melanin. The P protein therefore plays a crucial role in the amount and quality of melanin that is present in the iris. Several common variations (polymorphisms) in the OCA2 gene reduce the amount of functional P protein that is produced. Less P protein means that less melanin is present in the iris, leading to blue eyes instead of brown in people with a polymorphism in this gene. Mutation of OCA2 is the underlying cause of oculocutaneous albinism type-2. Moreover, deletion of the region encompassing this gene on chromosome-15 has been associated with the hypo-pigmentation of hair, skin, and eyes found in the Angelman and Prader–Willi syndromes 15. Duffy et al. 15 have recently reported that a three-single-nucleotide polymorphism haplotype in intron-1 of the OCA2 gene can explain most of the variation in human eye color.
A region of the nearby HERC2 gene known as intron 86 contains a segment of DNA that controls the activity (expression) of the OCA2 gene, turning it on or off as needed. At least one polymorphism in this area of the HERC2 gene has been shown to reduce the expression of OCA2, which leads to less melanin in the iris and lighter-colored eyes.
Several other genes play smaller roles in determining eye color. Some of these genes are also involved in skin and hair coloring. Genes with reported roles in eye color include ASIP, IRF4, SLC24A4, SLC24A5, SLC45A2, TPCN2, TYR, and TYRP1. The effects of these genes likely combine with those of OCA2 and HERC2 to produce a continuum of eye colors in different people.
Several disorders that affect eye color have been described. Ocular albinism is characterized by severely reduced pigmentation of the iris, which causes very light-colored eyes and significant problems with vision. Another condition called oculocutaneous albinism affects the pigmentation of the skin and hair in addition to the eyes. Affected individuals tend to have very light-colored irises, fair skin, and white or light-colored hair. Both ocular albinism and oculocutaneous albinism result from mutations in genes involved in the production and storage of melanin. Another condition called heterochromia is characterized by different-colored eyes in the same individual. Heterochromia can be caused by genetic changes or by a problem during eye development, or it can be acquired as a result of a disease or injury to the eye.
What causes heterochromia
There are many types and causes of heterochromia. An infant can be born with heterochromia or develop heterochromia soon after birth. In these cases, it is called congenital heterochromia.
In most cases, children born with heterochromia will experience no other symptoms. They do not have any other problems with their eyes or general health. However, in some cases heterochromia can be a symptom of another condition.
Most cases of heterochromia iridis occur sporadically in people with no family history of the condition. However, heterochromia iridis is rarely part of an inherited genetic syndrome. For example, heterochromia iridis is reported in some people affected by Waardenburg syndrome which is generally inherited in an autosomal dominant manner 16. Sometimes, one eye may change color following certain diseases or injuries.
Causes of heterochromia in infants can include:
- Horner’s syndrome
- Benign heterochromia
- Sturge-Weber syndrome
- Waardenburg syndrome
- Piebaldism
- Hirschsprung disease
- Bloch-Sulzberger syndrome
- von Recklinghausen disease
- Bourneville disease
- Parry-Romberg syndrome
- Familial heterochromia
When a person gets heterochromia later in life, this is called acquired heterochromia.
Causes of acquired heterochromia include:
- Acquired Horner’s syndrome
- Benign and malignant tumors of the iris
- Bleeding (hemorrhage) in the eye
- Central retinal vein occlusion
- Chediak-Higashi syndrome
- Diabetes mellitus
- Eye injury
- Eye surgery
- Foreign object in the eye
- Fuchs’ heterochromic cyclitis
- Glaucoma and some medications used to treat it
- Iris ectropion syndrome
- Latisse, a repurposed glaucoma medication used cosmetically to thicken eyelashes
- Mild inflammation affecting only one eye
- Neurofibromatosis
- Ocular melanosis
- Pigment dispersion syndrome
- Posner-Schlossman syndrome
- Swelling, due to iritis or uveitis
Heterochromia diagnosis and treatment
If your infant has heterochromia, he or she should be examined by an ophthalmologist. The ophthalmologist will confirm the appearance of heterochromia and look for any underlying causes. In most cases, there will be no concerning disease or condition causing the eye color variation. However, it is important to rule out these conditions.
If you get heterochromia as an adult or it changes in appearance, see your ophthalmologist. He or she can perform a detailed eye exam to rule out any underlying causes and come up with a treatment plan if necessary.
Treatment for heterochromia focuses on treating any underlying causes for the condition. If there are no other issues with the eyes, no treatment may be needed.
- Ur Rehman H. Heterochromia. CMAJ. 2008;179(5):447-8. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2518194[↩][↩]
- Rennie IG. Don’t it make my blue eyes brown: heterochromia and other abnormalities of the iris. Eye (Lond). 2011;26(1):29-50. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3259577/[↩][↩]
- Imesch PD, Wallow IH, Albert DM. The colour of the human eye: a review of morphologic correlates and of some conditions that affect iridial pigmentation. Surv Ophthalmol. 1997;41 (Suppl 2:S117–S123.[↩][↩]
- Bron AJ, Tripathi RC, Tripathi BJ. Wolff’s Anatomy of the Eye and Orbit8th edn.Chapman & Hall Medical: London; 1997[↩][↩]
- Prota G, Hu DN, Vincensi MR, McCormick SA, Napolitano A. Characterization of melanins in human irides and cultured uveal melanocytes from eyes of different colours. Exp Eye Res. 1998;67 (3:293–299.[↩][↩]
- Wilkerson CL, Syed NA, Fisher MR, Robinson NL, Wallow IH, Albert DM. Melanocytes and iris colour. Light microscopic findings. Arch Ophthalmol. 1996;114 (4:437–442.[↩]
- Fuchs E. Normal pigmentierte und albinotische iris. Graefes Arch Clin Exp Ophthalmol. 1913;84/85:521.[↩]
- Dieterich CE. [The fine structure of melanocytes in the human iris] Graefes Arch Clin Exp Ophthalmol. 1972;183 (4:317–333.[↩]
- Wolfrum P. Über den Bau der Irisvorderfläche des menschlichen Auges mit vergleichend anatomischen Bemerkungen. Graefes Arch Clin Exp Ophthalmol. 1922;109:106–153.[↩]
- Eagle RC., Jr Iris pigmentation and pigmented lesions: an ultra structural study. Trans Am Ophthalmol Soc. 1988;86:581–687.[↩]
- Imesch PD, Bindley CD, Khademian Z, Ladd B, Gangnon R, Albert DM, et al. Melanocytes and iris colour. Electron microscopic findings. Arch Ophthalmol. 1996;114 (4:443–447.[↩]
- Sturm RA, Frudakis TN. Eye colour: portals into pigmentation genes and ancestry. Trends Genet. 2004;20 (8:327–332[↩]
- Sturm RA, Frudakis TN. Eye colour: portals into pigmentation genes and ancestry. Trends Genet. 2004;20 (8:327–332.[↩]
- Sturm RA. Molecular genetics of human pigmentation diversity. Hum Mol Genet. 2009;18:9–17.[↩]
- Duffy DL, Montgomery GW, Chen W, Zhao ZZ, Le L, James MR, et al. A three-single-nucleotide polymorphism haplotype in intron 1 of OCA2 explains most human eye-colour variation. Am J Hum Genet. 2007;80 (2:241–252.[↩][↩]
- Classification of iris colour: review and refinement of a classification schema. Clin Exp Ophthalmol. 2011 Jul;39(5):462-71. doi: 10.1111/j.1442-9071.2010.02487.x. Epub 2011 Mar 16.[↩]