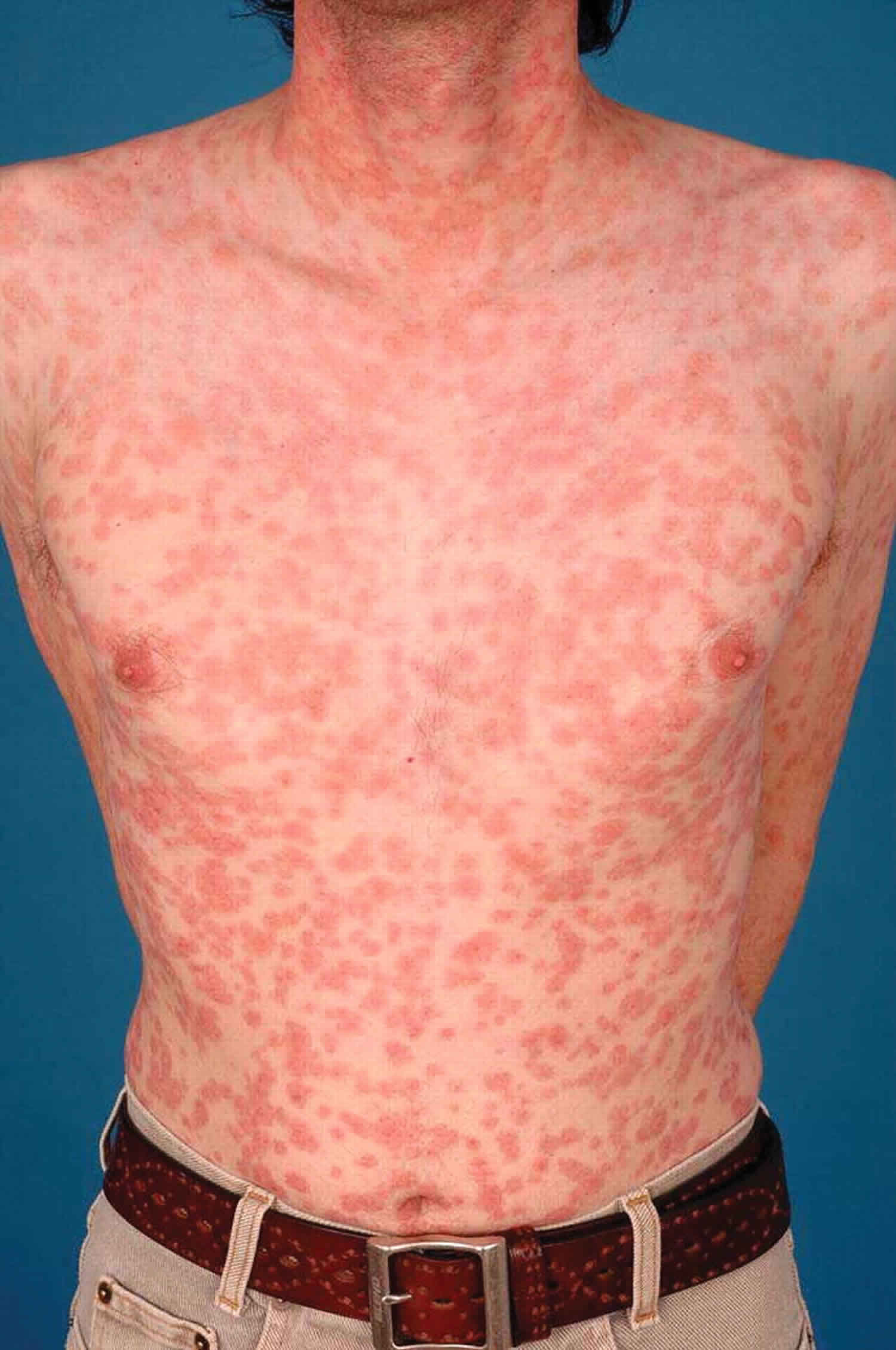
Jarisch Herxheimer reaction
Jarisch-Herxheimer reaction is a self-limited reaction associated with initiation of anti-treponemal therapy that most often occurs in persons treated for spirochetal infections such early syphilis presumably because bacterial burdens are higher during these stages, Lyme disease, leptospirosis, and relapsing fever 1. Following treatment with penicillin, the dying organisms often release inflammatory cytokines that lead to the Jarisch Herxheimer reaction. The Jarisch-Herxheimer reaction is an immune-mediated self-limited reaction that occurs within 2 to 24 hours of treatment and is characterized by high fever, malaise, nausea, vomiting, headache, muscle pain, intensification of skin rashes, tachycardia, malaise and less frequently, chills and exacerbation of a secondary syphilis rash 2. Case reports indicate that the Jarisch-Herxheimer reaction can also include uterine contractions in pregnancy, worsening liver and renal function, acute respiratory distress syndrome (ARDS), myocardial injury, hypotension, meningitis, alterations in consciousness, seizures, and strokes 1. Jarisch-Herxheimer reaction almost always occurs within 24 hours after initiating antimicrobial therapy and usually resolves within 24 hours. For patients who develop a Jarisch-Herxheimer reaction, the clinician should clarify this reaction is not an allergic reaction to penicillin. It occurs more frequently after treatment with penicillin and treatment of early syphilis, especially at the secondary syphilis. Jarisch-Herxheimer reaction is rarely fatal, except in neonates and in pregnancy for African women whose babies showed high perinatal mortality because of low birth weight 1. The treatment is supportive, antipyretics and sedation (eg, with diazepam or haloperidol) can be used to manage symptoms associated with the Jarisch-Herxheimer reaction, but they do not prevent this reaction 3. Pregnant women who develop Jarisch Herxheimer reaction need to be observed closely as it can lead to obstetric complications.
The Jarisch–Herxheimer reaction was named after European dermatologists who described in 1895 and 1902 patients with syphilis who developed exacerbations of their skin lesions after treatment with mercurial compounds 4. After penicillin became the drug of choice for syphilis in the 1940s, the Jarisch–Herxheimer reaction occurred during the first 24 hours of treatment in primary and secondary disease as well in general paresis of the insane manifesting as fever, chills, headache, myalgias, and intensification of skin rashes.
In other spirochetal infections, including Lyme disease, leptospirosis, and relapsing fever, a similar Jarisch–Herxheimer reaction was reported after treatments with penicillins, tetracyclines, and erythromycin. In addition, newer antimicrobials such as cephalosporins, meropenem, ciprofloxacin, levofloxacin, clarithromycin, and azithromycin can also provoke the Jarisch–Herxheimer reaction 5.
Jarisch Herxheimer causes
Jarisch–Herxheimer reaction can be regarded as an adverse effect of antibiotics, necessary for achieving a cure of spirochetal infections. Experimental evidence indicates Jarisch–Herxheimer reaction is caused by nonendotoxin pyrogen and spirochetal lipoproteins 1. Mediation of the Jarisch–Herxheimer reaction in relapsing fever by the pro-inflammatory cytokines tumor necrosis factor (TNF), interleukin (IL)-6, and IL-8 has been proposed, consistent with measurements in patients’ blood and inhibition by anti-TNF antibodies 1. Accelerated phagocytosis of spirochetes by polymorphonuclear leukocytes before rise in cytokines is responsible for removal of organisms from the blood, suggesting an early inflammatory signal from polymorphonuclear leukocytes.
Inflammatory substances in spirochetes
Clinical observations of patients with the Jarisch–Herxheimer reaction suggested a role for endotoxin 6, but experimental studies showed that spirochetes do not have biologically active endotoxin as defined by the limulus test 7. Substances other than endotoxin as well as mechanisms were described 8. In Treponema pallidum, lipoproteins were identified as likely responsible for inflammatory signs because they stimulate macrophages to produce tumor necrosis factor (TNF) 9. In Borrelia Burgdorferi, the outer surface protein A lipoprotein stimulates cells in culture to produce transcription factors for cytokines 10. Borrelia recurrentis from human plasma was also negative for endotoxin by the limulus test but was pyrogenic in rabbits 11. The nonendotoxin pyrogen could be the same as the lipoprotein. Lipoprotein of the outer membrane proteins of leptospires caused inflammation in mouse kidney cells 8.
Cytokines.
In patients with relapsing fever, plasma concentrations of the cytokines TNF, interleukin IL-6, and IL-8 were measured as sharply increasing at 2–4 hours after penicillin treatment when patients were experiencing a Jarisch–Herxheimer reaction, with a return toward baseline levels 12 hours after therapy 12. Anti-TNF antibodies administered before antibiotic treatment prevented or attenuated the Jarisch–Herxheimer reaction, while also reducing levels of IL-6 and IL-8 during the reactions 13. The cytokine response to Borrelia spirochetes requires recognition by Toll-like receptor 2 (TLR2) or TLR1/TLR2 heterodimers on the surfaces of phagocytes 14. The anti-inflammatory cytokine IL-10 was very elevated in louse-borne relapsing fever (LBRF) patients, but treatment of patients with recombinant IL-10 did not prevent Jarisch–Herxheimer reaction and did not inhibit rises of TNF, IL-6, or IL-8 during the Jarisch–Herxheimer reaction 15.
Phagocytosis
At the onset of the Jarisch–Herxheimer reaction of louse-borne relapsing fever, about 2 hours after antibiotic treatment, phagocytosis of spirochetes by blood polymorphonuclear cells had increased from a mean of 5% of cells that contained spirochetes before treatment to 23%, and addition of antibiotic to blood obtained before treatment caused a sharp rise in numbers of polymorphonuclear cells containing spirochetes during 0.5–2 hours of incubation.69 Spirochetes were demonstrated in polymorphonuclear cells with the Dieterle silver stain and in phagocytic vacuoles by electron microscopy.
In vitro studies of phagocytosis by monocytes showed that live, whole B. burgdorferi spirochetes stimulated ingesting monocytes to produce cytokines better than heat-killed or lysates of organisms 16. Apoptosis or programmed cell death of monocytes after phagocytosis of Borrelia could also be a factor driving the Jarisch–Herxheimer reaction 16. After phagocytosis, B. burgdorferi uses TLR2 signaling to give a pro-inflammatory cytokine response via the adapter molecule MyD88 17.
Disseminated intravascular coagulation
Biopsy of the petechiae was performed in patients with relapsing fever and resulted in thrombocytopenia due to disseminated intravascular coagulation (DIC) but not vasculitis or endothelial damage 11. Conjunctival hemorrhages in a patient in Spain was also associated with thrombocytopenia 18.
Complement activation, kinins, and histamine
Serum levels of hemolytic complement and properdin were reduced in patients with relapsing fever before and after antibiotic treatment, suggesting consumption of complement in the alternative complement pathway due to phagocytosis of Borrelia 19. Other studies of relapsing fever, however, indicated that complement was not activated 20. Elevated blood levels of histamine and kinins were measured in patients with syphilis and relapsing fever before and after the Jarisch–Herxheimer reaction, suggesting roles for these mediators of inflammation 21.
Syphilis
Syphilis is still the leading spirochetal infection that gives rise to a Jarisch–Herxheimer reaction. The common signs of Jarisch–Herxheimer reaction were fever and exacerbation of skin rashes. Frequency of Jarisch–Herxheimer reaction occurrences in syphilis and other spirochetal infections shown in Table 1 varied from 1 to 100% in observations about antimicrobial therapy 22, indicating large variations in patients’ susceptibilities as well as varying criteria used by observers of the reaction.
In a prospective study of 33 pregnant women in Texas with syphilis, who were treated with benzathine penicillin, 15 (45%) developed a Jarisch–Herxheimer reaction that was more common in primary and secondary infections than in latent infections; it started 2–8 hours after therapy, peaked at 6–12 hours, and resulted in fever and uterine contractions in most women, resulting in delivery of three infants with congenital syphilis 23. In 13 pregnant women in Chicago with syphilis who developed a Jarisch–Herxheimer reaction, uterine contractions were noted that resolved within 24 hours 24. A woman in Texas with preterm labor given penicillin for prophylaxis of Streptococcus agalactiae vaginal carriage developed chills and tachycardia, only to be found seropositive for syphilis with papulosquamous skin lesions after delivery of her baby with congenital infection 25. A woman in Japan presented in labor, received ampicillin prophylaxis for Streptococcus agalactiae and delivered 6 hours later a baby with a diffuse skin rash including blisters that suggested a Jarisch–Herxheimer reaction along with signs of congenital syphilis; after delivery, the baby received ampicillin, followed an hour later by fever and tachypnea, suggesting another Jarisch–Herxheimer reaction 26.
Case reports revealed the Jarisch–Herxheimer reaction in syphilis to be multifaceted in organs affected. A characteristic patient in New York, a 45-year-old human immunodeficiency virus (HIV)–positive man with rash, was treated with penicillin intravenously. An hour later, he developed a chill with a pulse rate of 140 and respirations of 28 per minute. This Jarisch–Herxheimer reaction was initially attributed to penicillin allergy 27. In a 45-year-old man in Ottawa with secondary syphilis as well as coinfection with HIV and hepatitis C virus, penicillin caused a Jarisch–Herxheimer reaction along with worsening liver function 28. From six case reports of neurosyphilis, additional neurological dysfunctions during the Jarisch–Herxheimer reaction occurred 29. Hallucinations or changes in consciousness or orientation were noted in three cases, seizures in three, abnormal magnetic resonance imaging or electroencephalograph in three, hemiparesis in two, and one each of facial nerve weakness and diplopia. In a Japanese man with dementia, treatment of neurosyphilis with penicillin provoked a Jarisch–Herxheimer reaction, from which he recovered, but his dementia persisted 30.
Table 1. Frequency of Jarisch–Herxheimer reaction in spirochetal infections in prospective studies, randomized trials of antimicrobial drugs, surveys, and meta-analyses
| Clinical condition | Frequency as percent of treated patients who developed a Jarisch–Herxheimer reaction | Reference |
|---|---|---|
| Syphilis | ||
| Primary, secondary, and early latent treated with penicillin | ||
| RPR titer ≥ 1:32 | 41 | 22 |
| RPR titer < 1:32 | 16 | 22 |
| HIV positive | 35 | 22 |
| HIV negative | 25 | 22 |
| Penicillin | 56 | 31 |
| Azithromycin | 14 | 31 |
| Secondary syphilis treated with penicillin | 9 | 32 |
| Syphilis in pregnancy | 40–45 | 24 |
| Neurosyphilis | 8–75 | 33 |
| Lyme disease, early with erythema migrans | ||
| Azithromycin | 7 | 34 |
| Amoxicillin | 15 | 34 |
| Amoxicillin | 8 | 35 |
| Cefuroxime axetil | 8 | 35 |
| Amoxicillin | 10 | 36 |
| Clarithromycin | 11 | 36 |
| Cefuroxime axetil | 12 | 37 |
| Doxycycline | 12 | 37 |
| Cefuroxime axetil | 29 | 38 |
| Doxycycline | 8 | 38 |
| Erythromycin, penicillin, tetracycline | 14 overall, more with penicillin and tetracycline than with erythromycin | 39 |
| Azithromycin | 13 | 40 |
| Doxycycline | 12 | 40 |
| Azithromycin | 5 | 41 |
| Doxycycline | 10 | 41 |
| Azithromycin | 30 | 42 |
| Doxycycline | 30 | 42 |
| Penicillin | 19 | 42 |
| Leptospirosis | ||
| Meta-analysis of 976 cases in trials | 9, mostly treated with penicillin or ampicillin | 43 |
| Family of four persons | 50, those treated with ceftriaxone or meropenem and doxycycline | 44 |
| Penicillin | 83 | 45 |
| Relapsing fever | ||
| Tick-borne | ||
| Surveys of cases in United States and Canada | 39 | 46 |
| Surveys in Iran | 1 | 47 |
| Louse-borne | ||
| Meta-analysis of 438 patients in six randomized trials | ||
| Penicillin | 37 | 48 |
| Tetracycline | 48 | 48 |
| Erythromycin | 80 | 49 |
| Penicillin | 67 | 49 |
| Tetracycline | 96 | 49 |
| Slow-release penicillin* | 100 | 20 |
| Tetracycline* | 100 | 20 |
| Tetracycline | 47 | 50 |
| Procaine penicillin 400,000 units | 31 | 50 |
| Procaine penicillin 200,000 units | 28 | 50 |
| Procaine penicillin 100,000 units | 5 | 50 |
Footnote: *Frank rigors in only 1/6 patients treated with penicillin, but all patients treated with tetracycline had rigors.
Abbreviations: HIV = human immunodeficiency virus; JHR = Jarisch–Herxheimer reaction; RPR = rapid plasma reagin.
Lyme disease
In trials shown in Table 1, the range of Jarisch–Herxheimer reaction frequency was 7–30%, indicating a trend toward lower frequency than for syphilis. Furthermore, the reactions in lyme disease were clinically milder than in the other diseases, without organ dysfunction or need for hospitalization. A severe case was a 31-year-old woman in Connecticut with a tick bite followed by erythema migrans, who received amoxicillin, which an hour later provoked chills, a temperature of 40°C, and hypotension that resolved over 3 hours while getting 3 L of intravenous saline 51.
Leptospirosis
A review of 976 cases of leptospirosis treated with antibiotics revealed detection of Jarisch–Herxheimer reaction in 92 patients, for an incidence of 9% 52. Only one of the patients died. He was a 20-year-old man in Ireland with jaundice and renal failure, who deteriorated after receiving penicillin, expiring the next day 53. Most of the cases of Jarisch–Herxheimer reaction were from one study in Malaya in 1957 that reported a Jarisch–Herxheimer reaction in 70 of 84 (83%) patients who received intramuscular penicillin injections 45.
A 29-year-old woman in France, who acquired leptospirosis 10 days after falling into a river while canoeing, experienced a Jarisch–Herxheimer reaction 4 hours after receiving amoxicillin when nuchal rigidity also developed; her spinal fluid showed elevated polymorphonuclear cells and high protein concentration 54. A 59-year-old man in Japan, 2 weeks after drinking swamp water in Okinawa, presented with fever and jaundice leading to a diagnosis of leptospirosis; 2 hours after treatment with ceftriaxone, he became more febrile with shock requiring vasopressors and intubation before recovering 5. Two hours after treatment with ceftriaxone for leptospirosis, a 49-year-old man in United Kingdom manifested a Jarisch–Herxheimer reaction with rising temperature, tachycardia, and elevation of creatinine necessitating intensive care unit (ICU) monitoring and hemodialysis before recovering 55. A 42-year-old man in Japan with leptospirosis treated with ceftriaxone developed on the next day multi-organ failure, hemoptysis, and radiographic signs of pulmonary alveolar hemorrhage with recovery 6 days later 56. Two of four family members in Switzerland after a white-water rafting trip to Thailand acquired leptospirosis and developed a Jarisch–Herxheimer reaction after treatment with ceftriaxone, meropenem, and doxycycline with serious consequences of hypotension, requiring adrenergic therapy in one case, as well as impaired liver and renal function 44. A 60-year-old farmer in Australia with fever, confusion, and thrombocytopenia developed a Jarisch–Herxheimer reaction 2 hours after receiving penicillin and ceftriaxone followed by uncomplicated recovery 57. A 51-year-old man in United Kingdom with fever, jaundice, and renal failure developed a Jarisch–Herxheimer reaction 5 hours after penicillin therapy and required hemodialysis before recovering 58. A 21-year-old man in United Kingdom after falling into a river from his canoe became febrile with vomiting and diarrhea; a Jarisch–Herxheimer reaction occurred 4 hours after penicillin treatment followed by an uneventful recovery 58.
Relapsing fever
In relapsing fever, the frequency, severity, and timing of the Jarisch–Herxheimer reaction are more predictable than in other infections. Relapsing fever differs from other infections by having large numbers of organisms visible in blood plasma, convenient for rapid diagnosis in blood smears as well as following clearance of spirochetes after treatment. During the Jarisch–Herxheimer reaction, which occurs in most patients 1–2 hours after antibiotic treatment, spirochetes disappear from the blood within about 5 hours. Except in Ethiopia, where louse-borne relapsing fever (LBRF) is prevalent, all cases reported in recent years from other African countries, North America, the Middle East, and Spain are tick-borne relapsing fever (TBRF) 59. An exception was two young male migrants from Eritrea in Netherlands in 2015, who had traveled through Ethiopia, had louse-borne relapsing fever, and developed severe Jarisch–Herxheimer reactions 2 hours after treatment, and recovered after care in the ICU 60. In the United States and Canada between 1977 and 2000, 450 patients with tick-borne relapsing fever were recorded 46. Only one death occurred, in a neonate, whose mother was also infected. In 129 patients with clinical information about treatment available, 50 of them (39%) showed a Jarisch–Herxheimer reaction (Table 1). Most had reactions within 2 hours after treatment, consisting usually of chills, sweating, tachycardia, and hypotension without cutaneous manifestations. In one patient, the Jarisch–Herxheimer reaction started 30 minutes after an intravenous dose of doxycycline. In a meta-analysis of six studies in Ethiopia of patients with relapsing fever, a Jarisch–Herxheimer reaction occurred in 89 of 239 patients (37%) treated with penicillin and in 96 of 199 patients (48%) treated with tetracycline 48. Only four deaths were reported in each group for a case-fatality rate of 8/438, or 2%. A 59-year-old woman in the United States on steroids for thrombocytopenia with a heavy infection was treated with doxycycline and ceftriaxone 61. She did not show a Jarisch–Herxheimer reaction initially, perhaps because of steroid treatment before antibiotics, but was hospitalized 3 days later with acute respiratory distress syndrome and pulmonary edema, requiring mechanical ventilation with eventual recovery. A 75-year-old woman in United States developed a Jarisch–Herxheimer reaction 4 hours after receiving levofloxacin that was followed by chest pain and low back pain as well as a rise in troponin I before recovering 62. Two hours after intravenous doxycycline for tick-borne relapsing fever, a 12-year-old girl in Spain developed vomiting, diminished consciousness, a blood pressure of 60/30 mmHg, and cardiac dysfunction shown by decreased ventricular ejection fraction and a rise in blood level of troponin I requiring mechanical ventilation and positive end-expiratory pressure for recovery 59. After returning from travel in Senegal, a 47-year-old Belgian woman developed relapsing fever and experienced a Jarisch–Herxheimer reaction after treatment with doxycycline 63.
Among 137 pregnant women in Tanzania with treated relapsing fever, 80 went into labor with the sad result that 38 infants died (47.5%), mostly because of low birthweight; however, only 1.5% of the women were noted to have a Jarisch–Herxheimer reaction and 1.5% of the women died. In these 80 women, it was unclear whether their premature labor was caused by their relapsing fever infections mainly or by the antibiotic treatment 64. A 19-year-old woman in Tanzania with relapsing fever delivered her baby, after which she was treated with penicillin, only to die the same day during a Jarisch–Herxheimer reaction 65. Neonatal infections, likely acquired from maternal infections during birth or across the placenta before birth, are rare but often fatal. In a report of five cases of neonatal relapsing fever in Tanzania, three died within a few hours after penicillin treatment 66. Heavy spirochetemia was blamed for their deaths, but Jarisch–Herxheimer reaction cannot be excluded in case reports without information about changes in vital signs after treatment.
Jarisch Herxheimer reaction symptoms
Jarisch-Herxheimer reaction is an immune-mediated self-limited reaction that occurs within 2 to 24 hours of treatment and is characterized by high fever, malaise, nausea, vomiting, headache, muscle pain, intensification of skin rashes, tachycardia, malaise and less frequently, chills and exacerbation of a secondary syphilis rash 2. Case reports indicate that the Jarisch-Herxheimer reaction can also include uterine contractions in pregnancy, worsening liver and renal function, acute respiratory distress syndrome (ARDS), myocardial injury, hypotension, meningitis, alterations in consciousness, seizures, and strokes 1. Jarisch-Herxheimer reaction almost always occurs within 24 hours after initiating antimicrobial therapy and usually resolves within 24 hours. For patients who develop a Jarisch-Herxheimer reaction, the clinician should clarify this reaction is not an allergic reaction to penicillin. It occurs more frequently after treatment with penicillin and treatment of early syphilis, especially at the secondary syphilis. Jarisch-Herxheimer reaction is rarely fatal, except in neonates and in pregnancy for African women whose babies showed high perinatal mortality because of low birth weight 1.
Jarisch Herxheimer treatment
Jarisch-Herxheimer reaction treatment is supportive, antipyretics and sedation (eg, with diazepam or haloperidol) can be used to manage symptoms associated with the Jarisch-Herxheimer reaction, but they do not prevent this reaction 3. Pregnant women who develop Jarisch Herxheimer reaction need to be observed closely as it can lead to obstetric complications.
Admit the patient to the hospital if neurologic involvement is noted. Otherwise, treat with steroids and antipyretics, as indicated 67.
Corticosteroids (eg, prednisone at 20 mg 4 times per day for 3 days started 1 day prior to antitreponemal treatment) have been used to prevent adverse effects. Salicylates/antipyretics are prescribed for symptomatic relief 68.
- Butler T. The Jarisch-Herxheimer Reaction After Antibiotic Treatment of Spirochetal Infections: A Review of Recent Cases and Our Understanding of Pathogenesis. Am J Trop Med Hyg. 2017;96(1):46–52. doi:10.4269/ajtmh.16-0434 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5239707[↩][↩][↩][↩][↩][↩][↩]
- Brown ST. Adverse reactions in syphilis therapy. J Am Vener Dis Assoc. 1976;3:172-6.[↩][↩]
- Syphilis. https://www.std.uw.edu/go/pathogen-based/syphilis/core-concept/all#treatment[↩][↩]
- Belum GR, Belum VR, Arudra SKC, Reddy BSN. The Jarisch-Herxheimer reaction revisited. Travel Med Infect Dis. 2013;11:231–237.[↩]
- Takamizawa S, Gomi H, Shimizu Y, Isono H, Shirokawa T, Kato M. Leptospirosis and Jarisch-Herxheimer reaction. QJM. 2015;108:967–968.[↩][↩]
- Gelfand JA, Elin RJ, Berry FW, Frank MM. Endotoxemia associated with the Jarisch-Herxheimer reaction. N Engl J Med. 1976;295:211–213.[↩]
- Takayama K, Rothenberg RJ, Barbour AG. Absence of lipopolysaccharide in the lyme disease spirochete, Borrelia burgdorferi. Infect Immun. 1987;55:2311–2313.[↩]
- Yang C-W, Hung C-C, Wu M-S, Tian Y-C, Chang C-T, Pan M-J, Vandewalle A. Toll-like receptor 2 mediates early inflammation by leptospiral outer membrane proteins in proximal tubule cells. Kidney Int. 2006;69:815–822.[↩][↩]
- Akins DR, Purcell BK, Mitra MM, Norgard MV, Radolf JD. Lipid modification of the 17-kilodalton membrane immunogen of Treponema pallidum determines macrophage activation as well as amphiphilicity. Infect Immun. 1993;61:1202–1210.[↩]
- Bulut Y, Faure E, Thomas L, Equils O, Arditi M. Cooperation of Toll-like receptor 2 and 6 for cellular activation by soluble tuberculosis factor and Borrelia burgdorferi outer surface protein A lipoprotein: role of toll-interacting protein and IL-1 receptor signaling molecules in Toll-like receptor 2 signaling. J Immunol. 2001;167:987–994.[↩]
- Butler T, Hazen P, Wallace CK, Awoke S, Habte-Michael A. Borrelia recurrentis infection: pathogenesis of fever and petechiae. J Infect Dis. 1979;140:665–675.[↩][↩]
- Negussie Y, Remick DG, DeForge LE, Kunkel SL, Eynon A, Griffin GE. Detection of plasma tumor necrosis factor, interleukins 6, and 8 during the Jarisch-Herxheimer reaction of relapsing fever. J Exp Med. 1992;175:1207–1212.[↩]
- Coxon RE, Fekade D, Knox K, Hussein K, Melka A, Daniel A, Griffin GG, Warrell DA. The effect of antibody against TNF alpha on cytokine response in Jarisch-Herxheimer reactions of louse-borne relapsing fever. QJM. 1997;90:213–221.[↩]
- Oosting M, ter Hofstede H, Sturm P, Adema GJ, Kulberg B-J, van der Meer JWM, Netea MG, Joosten LAB. TLR1/TLR2 heterodimers play an important role in the recognition of Borrelia spirochetes. PLoS One. 2011;6:e25998[↩]
- Cooper PJ, Fekade D, Remick DG, Grint P, Wherry J, Griffin GE. Recombinant human interleukin-10 fails to alter proinflammatory production or physiogic changes associated with the Jarisch-Herxheimer reaction. J Infect Dis. 2000;181:203–209.[↩]
- Cruz AR, Moore MW, La Vake CJ, Eggers CH, Salazar JC, Radolf JD. Phagocytosis of Borrelia burgdorferi, the lyme disease spirochete, potentiates innate immune activation and induces apoptosis in human monocytes. Infect Immun. 2008;76:56–70.[↩][↩]
- Petnicki-Ocwieja T, Chung E, Acosta DI, Ramos LT, Shin OS, Ghosh S, Kobzik L, Li X, Hu LT. TRIF mediates Toll-like receptor 2-dependent inflammatory responses to Borrelia burgdorferi. Infect Immun. 2013;81:402–410.[↩]
- Castilla-Guerra L, Alvarez-Suero J, Fernandez-Moreno MDC, Fontana ER. Tick-borne relapsing fever: conjunctival haemorrhages. BMJ Case Rep. 2009;2009 pii:bcro6.2008.0114[↩]
- Galloway RE, Levin J, Butler T, Naff GB, Goldsmith GH, Saito H, Awoke S, Wallace CK. Activation of protein mediators on inflammation and evidence for endotoxemia in Borrelia recurrentis infection. Am J Med. 1977;63:933–938.[↩]
- Warrell DA, Perine PL, Krause DW, Bing DH, MacDougal SJ. Pathophysiology and immunology of the Jarisch-Herxheimer-like reaction in louse-borne relapsing fever: comparison of tetracycline and slow-release penicillin. J Infect Dis. 1983;147:898–909.[↩][↩][↩]
- Loveday C, Bingham JS. Changes in intravascular complement, kininogen, and histamine during Jarisch-Herxheimer reaction in secondary syphilis. Genitourin Med. 1985;61:27–32.[↩]
- Yang C-J, Lee N-Y, Lin Y-H, Lee H-C, Ko W-C, Liao C-H, Wu C-H, Hsieh C-Y, Wu P-Y, Liu W-C, Chang Y-C, Hung C-C. Jarisch-Herxheimer reaction after penicillin therapy among patients with syphilis in the era of the HIV infection epidemic: incidence and risk factors. Clin Infect Dis. 2010;51:976–979.[↩][↩][↩][↩][↩]
- Klein VR, Cox SM, Mitchell MD, Wendel GD. The Jarisch-Herxheimer reaction complicating syphilotherapy in pregnancy. Obstet Gynecol. 1990;75:375–380.[↩]
- Myles TD, Elam G, Park-Hwang E, Nguyen T. The Jarisch-Herxheimer reaction and fetal monitoring changes in pregnant women treated for syphilis. Obstet Gynecol. 1998;92:859–864.[↩][↩]
- Rac MWF, Greer LG, Wendel GD. Jarisch-Herxheimer reaction triggered by group B Streptococcus intrapartum antibiotic prophylaxis. Obstet Gynecol. 2010;116:552–556.[↩]
- Hori H, Sato Y, Shitara T. Congenital syphilis presenting as Jarisch-Herxheimer reaction at birth. Pediatr Int. 2015;57:299–301.[↩]
- See S, Scott EK, Levin MW. Penicillin-induced Jarisch-Herxheimer reaction. Ann Pharmacother. 2005;39:2128–2130.[↩]
- Cooper C, MacPherson P, Angel JB. Liver toxicity resulting from syphilis and Jarisch-Herxheimer reaction in cases of co-infection with HIV and hepatitis C virus. Clin Infect Dis. 2005;40:1211–1212.[↩]
- Bucher JB, Golden MR, Heald AE, Marra CM. Stroke in a patient with human immunodeficiency virus and syphilis treated with penicillin and antiretroviral therapy. Sex Transm Dis. 2011;38:442–444.[↩]
- Hagiya H, Deguchi K, Kawada K, Otsuka F. Neurosyphilis is a long-forgotten disease but still a possible etiology for dementia. Intern Med. 2015;54:2769–2773.[↩]
- Tsai M-S, Yang C-J, Lee N-Y, Hsieh S-M, Lin Y-H, Sun H-Y, Sheng W-H, Lee K-Y, Yang S-P, Liu W-C, Wu P-Y, Ko W-C, Hung C-C. Jarisch-Herxheimer reaction among HIV positive patients with early syphilis: azithromycin versus benzathine penicillin G therapy. J Int AIDS Soc. 2014;17:18993[↩][↩]
- Miller WM, Gorini F, Botelho G, Moreira C, Barbosa AP, Pinto ARSB, Dias MF, Sousa LM, Asensi MD, da Costa Nery JA. Jarisch-Herxheimer reaction among syphilis patients in Rio de Janeiro, Brazil. Int J STD AIDS. 2010;21:806–809.[↩]
- Punia V, Rayi A, Sivaraju A. Stroke after initiating IV penicillin for neurosyphilis: a possible Jarisch-Herxheimer reaction. Case Rep Neuro Med. 2014;2014:548179[↩]
- Arnež M, Ružić-Sabljić E. Azithromycin is equally effective as amoxicillin in children with solitary erythema migrans. Pediatr Infect Dis. 2015;34:1045–1048.[↩][↩]
- Eppes SC, Childs JA. Comparative study of cefuroxime axetil versus amoxicillin in children with early lyme disease. Pediatrics. 2002;109:1173–1177.[↩][↩]
- Nizič T, Velikanje E, Ružić-Sabljić E, Arnež M. Solitary erythema migrans in children: comparison of treatment with clarithromycin and amoxicillin. Wien Klin Wochenschr. 2012;124:427–433.[↩][↩]
- Luger SW, Paparone P, Wormser GP, Nadelman RB, Grunwald E, Gomez G, Wisniewski M, Collins JJ. Comparison of cefuroxime axetil and doxycycline in treatment of patients with early lyme disease associated with erythema migrans. Antimicrob Agents Chemother. 1995;39:661–667.[↩][↩]
- Nadelman RB, Luger SW, Frank E, Wisniewski M, Collins JJ, Wormser GP. Comparison of cefuroxime axetil and doxycycline in the treatment of early lyme disease. Ann Intern Med. 1992;117:273–280.[↩][↩]
- Steere AC, Hutchinson GJ, Rahn DW, Sigal LH, Craft JE, DeSanna ET, Malawista SE. Treatment of the early manifestations of lyme disease. Ann Intern Med. 1983;99:22–26.[↩]
- Strle F, Preac-Mursic V, Cimperman J, Ružić E, Maraspin V, Jereb M. Azithromycin versus doxycycline for treatment of erythema migrans: clinical and microbiological findings. Infection. 1993;21:83–88.[↩][↩]
- Strle F, Maraspin V, Lotric-Furlan S, Ružić-Sabljić E, Cimperman J. Azithromycin and doxycycline for treatment of Borrelia culture-positive erythema migrans. Infection. 1996;24:66–70.[↩][↩]
- Strle F, Ružić E, Cimperman J. Erythema migrans: comparison of treatment with azithromycin, doxycycline and phenoxymethylpenicillin. J Antimicrob Chemother. 1992;30:543–550.[↩][↩][↩]
- Guerrier G, D’Ortenzio E. The Jarisch-Herxheimer reaction in leptospirosis: a systematic review. PLoS One. 2013;8:e59266.[↩]
- Gallardo C, Williams-Smith J, Jaton K, Asner S, Cheseaux JJ, Troillet N, Manuel O, Berthod D. Leptospirosis in a family after whitewater rafting in Thailand. Rev Med Suisse. 2015;11:872–876.[↩][↩]
- MacKay-Dick J, Robinson JF. Penicillin in the treatment of 84 cases of leptospirosis in Malaya. J R Army Med Corps. 1957;103:186–197.[↩][↩]
- Dworkin MS, Shoemaker PC, Fritz CL, Dowell ME, Anderson DE. The epidemiology of tick-borne relapsing fever in the United States. Am J Trop Med Hyg. 2002;66:753–758.[↩][↩]
- Asi HM, Goya MM, Vatandoost H, Zahraei SM, Mafi M, Asmar M, Piazak N, Aghighi Z. The epidemiology of tick-borne relapsing fever in Iran during 1997–2006. Travel Med Infect Dis. 2009;7:160–164.[↩]
- Guerrier G, Doherty T. Comparison of antibiotic regimens for treating louse-borne relapsing fever: a meta-analysis. Trans R Soc Trop Med Hyg. 2011;105:483–490.[↩][↩][↩]
- Butler T, Jones PK, Wallace CK. Borrelia recurrentis infection: single-dose antibiotic regimens and management of the Jarisch-Herxheimer reaction. J Infect Dis. 1978;137:573–577.[↩][↩][↩]
- Seboxa T, Rahlenbeck SI. Treatment of louse-borne relapsing fever with low dose penicillin or tetracycline: a clinical trial. Scand J Infect Dis. 1995;27:29–31[↩][↩][↩][↩]
- Maloy AL, Black RD, Segurola RJ. Lyme disease complicated by the Jarisch-Herxheimer reaction. J Emerg Med. 1998;16:437–438.[↩]
- Guerrier G, D’Ortenzio E. The Jarisch-Herxheimer reaction in leptospirosis: a systematic review. PLoS One. 2013;8:e59266[↩]
- Vaughn C, Cronin CC, Walsh EK, Whelton M. The Jarisch-Herxheimer reaction in leptospirosis. Postgrad Med J. 1994;70:118–121.[↩]
- Tattevin P, Jaureguiberry S, Michelet C. Meningitis as a possible feature of the Jarisch-Herxheimer reaction. Eur J Clin Microbiol Infect Dis. 2003;22:449.[↩]
- Pimenta D, Democratis J. Risky behaviour: a rare complication of an uncommon disease in a returning traveller. BMJ Case Rep. 20132013 pii:bcr-2013-201075[↩]
- Hashimoto T, Akata S, Park J, Harada Y, Hirayama Y, Otaki J, Tokuuye K. High-resolution computed tomography findings in a case of severe leptospira infection (Weil disease) complicated with Jarisch-Herxheimer reaction. J Thorac Imaging. 2012;27:W24–W26.[↩]
- Markham R, Slack A, Gerrard J. The Jarisch-Herxheimer reaction in a patient with leptospirosis: a foreseeable problem in managing spirochaete infections. Med J Aust. 2012;197:276–277.[↩]
- Friedland JS, Warrell DA. The Jarisch-Herxheimer reaction in leptospirosis: possible pathogenesis and review. Rev Infect Dis. 1991;13:207–210.[↩][↩]
- Garcia-Soler P, Nunez-Cuadros E, Milano-Manso G, Sanchez PR. Severe Jarisch-Herxheimer reaction in tick-borne relapsing fever. Enferm Infecc Microbiol Clin. 2011;29:710–711.[↩][↩]
- Wilting KR, Stienstra Y, Sinha B, Braks M, Cornish D, Grundmann H. Louse-borne relapsing fever (Borrelia recurrentis) in asylum seekers from Eritrea, The Netherlands, July 2015. Euro Surveill. 2015;20 20.30.21196[↩]
- Badger MS. Tick talk: unusually severe case of tick-borne relapsing fever with acute respiratory distress syndrome—case report and review of literature. Wild Env Med J. 2008;19:280–286.[↩]
- Hoekstra KA, Kelly MT. Elevated troponin and Jarisch-Herxheimer reaction in tick-borne relapsing fever: a case report. Case Rep Infect Dis. 2011;2011:950314[↩]
- Colebunders R, De Serrano P, Van Gompel A, Wynants H, Blot K, Van Den Enden E, Van Den Ende J. Imported relapsing fever in European tourists. Scand J Infect Dis. 1993;25:533–536.[↩]
- Jongen VHWM, van Roosmalen J, Tiems J, Holten JV, Wetsteyn JCFM. Tick-borne relapsing fever and pregnancy outcome in rural Tanzania. Acta Obstet Gynecol Scand. 1997;76:834–838.[↩]
- Rustenhoven-Spaan I, Melkert P, Nelissen E, van Roosmalen J. Maternal mortality in a rural Tanzanian hospital: fatal Jarisch-Herxheimer reaction in a case of relapsing fever in pregnancy. Trop Doct. 2013;43:138–141.[↩]
- Melkert PWJ, Stel HV. Neonatal Borrelia infections (relapsing fever): report of 5 cases and review of the literature. East Afr Med J. 1991;68:999–1005.[↩]
- Silberstein P, Lawrence R, Pryor D, Shnier R. A case of neurosyphilis with a florid Jarisch-Herxheimer reaction. J Clin Neurosci. 2002 Nov. 9(6):689-90.[↩]
- Workowski KA, Berman SM, Centers for Disease Control and Prevention. Sexually transmitted diseases treatment guidelines, 2006. MMWR Recomm Rep. 2006 Aug 4. 55(RR-11):1-94.[↩]