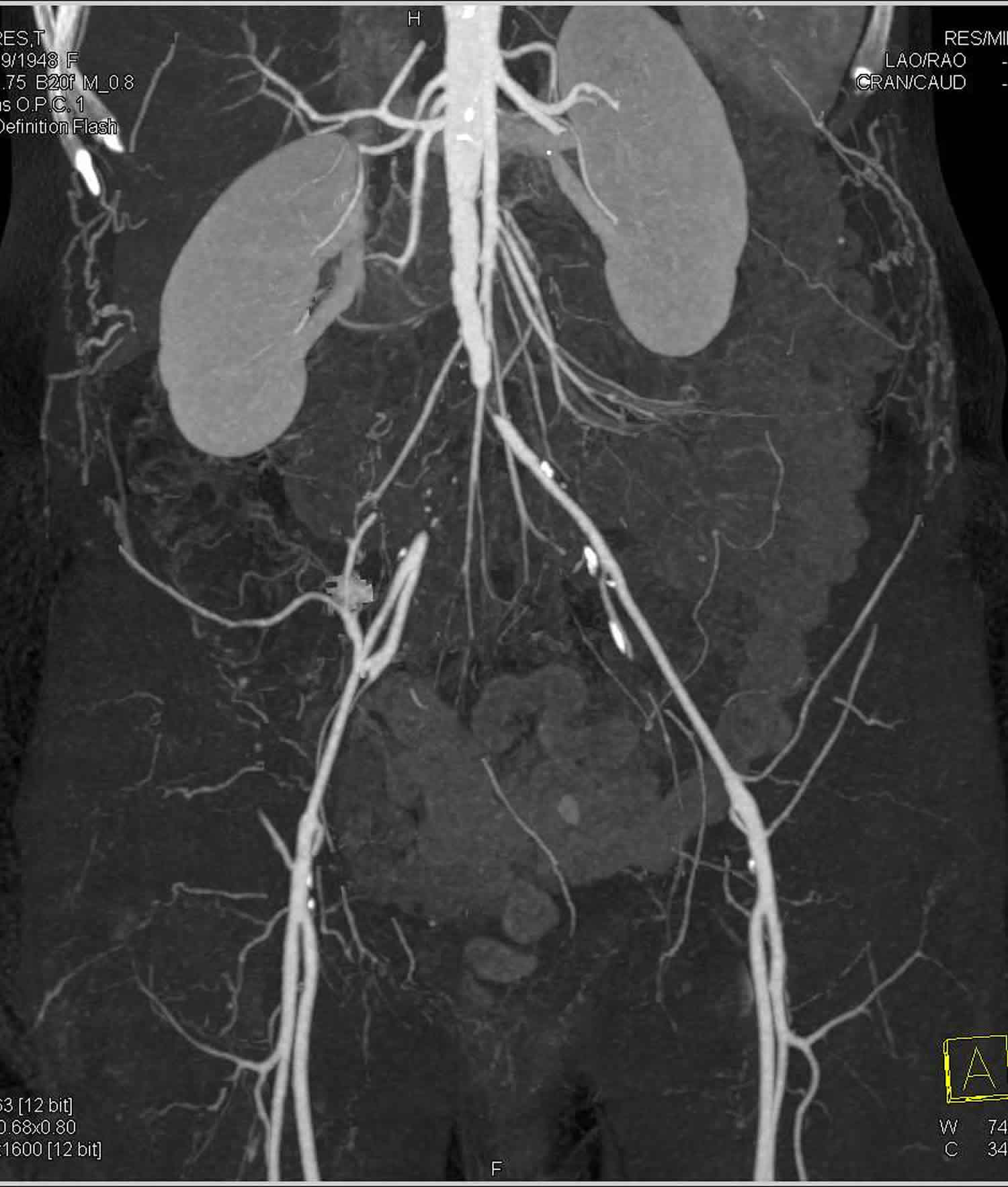
What is Leriche syndrome
Leriche syndrome is an aorta-iliac occlusive disease resulting from thrombotic occlusion of the region just above the abdominal aorta bifurcation 1. Leriche syndrome is a product of atherosclerosis affecting the distal abdominal aorta, iliac arteries, and femoropopliteal vessels 2. Aorta-iliac occlusive disease is classified as Type 1 (confined to the distal abdominal aorta and common iliac arteries), Type 2 (predominately distal abdominal aorta with disease extension into common iliac and external iliac arteries), and Type 3 (affecting the aortoiliac segment and femoropopliteal vessels) 3.
Leriche syndrome (aorta-iliac occlusive disease), when symptomatic, classically presents with a triad of hip and throat claudication, absence of the femoral pulse, or general weakening and impotence 4. Claudication refers to cramping leg pain that is reproducible by exercise. Leriche syndrome can have atypical presentations, such as renal infarction 5. Additionally, Leriche syndrome (aorta-iliac occlusive disease) is more prevalent among males and the non-Hispanic black race.
Leriche syndrome is named after René Leriche, the famous French surgeon who performed the first operative treatment for this disease. Leriche syndrome is more common in smokers, in patients of hypercholesterolemia, and in those with peripheral arterial disease 6. For the diagnosis of Leriche syndrome, ankle brachial index measurement, duplex Doppler ultrasonography, and CT angiography are important imaging modalities. Conventional surgical treatment for aortoiliac occlusive diseases include aortoiliac endarterectomy and aortobifemoral bypass. For high-risk patients, axillofemoral bypass (extra-anatomic technique) and percutaneous angioplasty are also viable alternatives 5.
Leriche syndrome causes
Leriche Syndrome is caused by atherosclerosis 7. Modifiable risk factors for atherosclerosis include hypertension, diabetes mellitus, nicotine, hyperlipidemia, hyperglycemia, and homocysteine. Non-modifiable risk factors for atherosclerosis include age, gender, race, and family history 8.
Leriche Syndrome occurs secondary to atherosclerotic induced arterial wall injury leading to two out of three factors involved in Virchow triad, endothelial damage, and thrombosis. Once endothelial damage occurs, a resultant inflammatory response leads to lipid accumulation in smooth muscle cells and macrophages, which eventually leads to the formation of a plaque in the arterial lumen. Eventually, aortoiliac segments become stenotic by more than 50%, the resultant oxygen debt during exercise causes claudication. Once peripheral arterial disease becomes extensive in the aortoiliac segment, the majority of men with Leriche Syndrome present with impotence and sexual dysfunction secondary to reduced penile arterial flow 8.
Leriche syndrome symptoms
Patients with Leriche syndrome (aorta-iliac occlusive disease) commonly present with claudication, which is cramping in the lower extremities (hips, thighs, buttocks) reproducible by exercise. A detailed history is essential in determining the location, severity, and duration of symptoms. While impotence and sexual dysfunction may occur in the majority of patients, the hallmark of Leriche Syndrome is reduced or absent femoral pulses 9. However, due to collateral vasculature, limb-threatening ischemia is not universal 10.
Leriche syndrome complications
Limb ischemia 11 is a potential complication of Leriche syndrome as well as heart failure, myocardial ischemia/infarction, gangrene, and even death 12.
Leriche syndrome diagnosis
A serum lipid profile (total cholesterol, LDL, HDL, TG) as well as HbA1c (if diabetic), lipoprotein A, and homocysteine levels should be obtained 8. An ankle-brachial index (ABI) should also be performed to evaluate the perfusion of the lower extremities. An ankle-brachial index (ABI) is often the first screening test performed as it is non-invasive, inexpensive, and reliable. An ankle-brachial index (ABI) provides the ratio of the ankle systolic blood pressure divided by the brachial systolic blood pressure detected using a Doppler probe. An ankle-brachial index (ABI) lower than 0.9 is considered abnormal and indicates the patient has peripheral arterial disease significant enough to cause claudication 13. Duplex ultrasonography and CT angiography are performed to determine the location and degree of stenosis while planning an intervention 10. Coronary artery disease (coronary heart disease) is seen in 10% – 71% of patients with peripheral arterial disease, so obtaining an EKG as well to rule out coronary heart disease is recommended 14.
Leriche syndrome treatment
Surgical treatment options for Leriche Syndrome include thromboendarterectomy, aortobifemoral bypass and percutaneous transluminal angioplasty (PTA) with or without stenting 8. Aortobifemoral bypass is preferred over thromboendarterectomy, mainly when intervention is necessary for arteries deep in the pelvis. Long-term patency of surgically repaired vessels in aortobifemoral bypass have been recognized as superior to thromboendarterectomy and percutaneous transluminal angioplasty with or without stenting in surgically fit patients. The long-term patency rates of aortobifemoral bypass approach 85-90% at five years and 75-80% at ten years 8. Percutaneous transluminal angioplasty and stenting is the intervention of choice in patients with multiple comorbidities, particularly those resulting in reduced lung function. Medical management includes smoking cessation, management of diabetes, antiplatelet and statin therapy, in addition to antihypertensive therapy. Implementation of a walking exercise program has been shown to improve walking ability by 50% – 200%. The exercise program should consist of daily 30-minute walking sessions. Intolerable claudication pain should be the endpoint for each session 15, cessation and lowering glucose and lipid levels (LDL <100 mg/dL and HbA1c below 7%) are primary objectives of medical management. Cilostazol, a phosphodiesterase III inhibitor, may be administered to treat claudication symptoms of the patient. Cilostazol may also have benefit in graft patency and prevention of stenosis 16.
Leriche syndrome prognosis
Without treatment, the prognosis of Leriche Syndrome is poor. However, with modern medicine outcomes are good. In some cases with slow progression or onset of Leriche syndrome, collaterals may develop as a self-compensating mechanism 17.
- Seyithanoglu M, Gundag M, Dogan K, Kitis S, Aydin T, Peru C. Leriche syndrome with lumbar disc hernia: first case report in literature. J Neurol Sci. 2012; 28: 641-5.[↩]
- Pascarella L, Aboul Hosn M. Minimally Invasive Management of Severe Aortoiliac Occlusive Disease. J Laparoendosc Adv Surg Tech A. 2018 May;28(5):562-568.[↩]
- Wooten C, Hayat M, du Plessis M, Cesmebasi A, Koesterer M, Daly KP, Matusz P, Tubbs RS, Loukas M. Anatomical significance in aortoiliac occlusive disease. Clin Anat. 2014 Nov;27(8):1264-74. [↩]
- Toker, İbrahim & Çalışkan, Feriyde & Akbaydogan Dundar, Gullu. (2018). Leriche Syndrome. Eurasian Journal of Emergency Medicine. 17. 209-210. 10.5152/eajem.2018.52533.[↩]
- Lin CW, Liu CY, Chen CH. Acute renal infarction: an atypical presentation of Leriche syndrome. Intern Med. 2012; 51: 2485.[↩][↩]
- Lee WJ, Cheng YZ, Lin HJ. Leriche syndrome. Int J Emerg Med. 2008; 1: 223.[↩]
- Brown KN, Gonzalez L. Leriche Syndrome. [Updated 2019 Feb 18]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2019 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK538248[↩]
- Frederick M, Newman J, Kohlwes J. Leriche syndrome. J Gen Intern Med. 2010 Oct;25(10):1102-4.[↩][↩][↩][↩][↩]
- Wooten C, Hayat M, du Plessis M, Cesmebasi A, Koesterer M, Daly KP, Matusz P, Tubbs RS, Loukas M. Anatomical significance in aortoiliac occlusive disease. Clin Anat. 2014 Nov;27(8):1264-74.[↩]
- Ahmed S, Raman SP, Fishman EK. CT angiography and 3D imaging in aortoiliac occlusive disease: collateral pathways in Leriche syndrome. Abdom Radiol (NY). 2017 Sep;42(9):2346-2357.[↩][↩]
- Pillai J, Monareng T, Rangaka TB, Yazicioglu C, Jayakrishnan R, Veller MG. Aorto-internal iliac artery endovascular reconstruction for critical limb ischaemia: a case report. S Afr J Surg. 2015 Oct 08;53(1):26-7.[↩]
- Kashou AH, Braiteh N, Zgheib A, Kashou HE. Acute aortoiliac occlusive disease during percutaneous transluminal angioplasty in the setting of ST-elevation myocardial infarction: a case report. J Med Case Rep. 2018 Jan 11;12(1):6.[↩]
- de Groote P, Millaire A, Deklunder G, Marache P, Decoulx E, Ducloux G. Comparative diagnostic value of ankle-to-brachial index and transcutaneous oxygen tension at rest and after exercise in patients with intermittent claudication. Angiology. 1995 Feb;46(2):115-22.[↩]
- Diehm C, Schuster A, Allenberg JR, Darius H, Haberl R, Lange S, Pittrow D, von Stritzky B, Tepohl G, Trampisch HJ. High prevalence of peripheral arterial disease and co-morbidity in 6880 primary care patients: cross-sectional study. Atherosclerosis. 2004 Jan;172(1):95-105.[↩]
- Fakhry F, Spronk S, van der Laan L, Wever JJ, Teijink JA, Hoffmann WH, Smits TM, van Brussel JP, Stultiens GN, Derom A, den Hoed PT, Ho GH, van Dijk LC, Verhofstad N, Orsini M, van Petersen A, Woltman K, Hulst I, van Sambeek MR, Rizopoulos D, Rouwet EV, Hunink MG. Endovascular Revascularization and Supervised Exercise for Peripheral Artery Disease and Intermittent Claudication: A Randomized Clinical Trial. JAMA. 2015 Nov 10;314(18):1936-44.[↩]
- Tara S, Kurobe H, de Dios Ruiz Rosado J, Best CA, Shoji T, Mahler N, Yi T, Lee YU, Sugiura T, Hibino N, Partida-Sanchez S, Breuer CK, Shinoka T. Cilostazol, Not Aspirin, Prevents Stenosis of Bioresorbable Vascular Grafts in a Venous Model. Arterioscler. Thromb. Vasc. Biol. 2015 Sep;35(9):2003-10.[↩]
- Morotti A, Busso M, Cinardo P, Bonomo K, Angelino V, Cardinale L, Veltri A, Guerrasio A. When collateral vessels matter: asymptomatic Leriche syndrome. Clin Case Rep. 2015 Nov;3(11):960-1.[↩]