Oral cavity cancer
Oral cavity cancer is also called oral cancer or mouth cancer that starts in cells of the mouth. The medical term for the mouth is the oral cavity. A cancerous (malignant) tumor is a group of cancer cells that can grow into and destroy nearby tissue. Oral cavity cancer can also spread (metastasize) to other parts of the body. The most common place oral cancer spreads to is the lymph nodes in the neck. Lymph nodes are small bean shaped glands that are part of the lymphatic system. There are major groups of lymph nodes in your neck. Cancers starting in the mouth and oropharynx can spread to these lymph nodes because they are close by 1.
Oral cancer is divided into two categories – those occurring in the oral cavity (the mouth) and those occurring in the oropharynx (the part of the throat just behind the mouth).
Mouth cancer can start anywhere in the oral cavity or in different parts of the mouth, including your lips, inside lining of your cheeks and lips (buccal mucosa), gums (gingiva), the front 2/3 of your tongue, floor of your mouth, the bony roof of your mouth (hard palate) and the area behind your wisdom teeth (retromolar trigone) (see Figure 3 below). The mouth is covered by a lining called the oral mucosa (mucous membrane). The oral mucosa is made up of squamous cells called the squamous epithelium. More than 90% of oral cancer starts in these flat, thin squamous cells 2. This type of cancer is called squamous cell carcinoma of the mouth. There are minor salivary glands distributed throughout all surfaces of the oral cavity, so salivary gland cancers are also found. Rarer types of oral cancer can also develop, these include melanoma and lymphomas 3.
In contrast, the oropharynx is the part of the throat just behind the mouth (see Figure 4 below). Cancer starting in this area is called oropharyngeal cancer. The oropharynx is the part of the throat (pharynx) just behind the mouth. It includes tonsil cancer and cancer in the back 1/3 of the tongue, soft area at the back of the roof of the mouth (soft palate), the 2 ridges of tissue in front of and behind the tonsils (tonsillar pillars) and back wall of the throat.
Oral cavity and oropharyngeal cancers occur most often in the following sites 4:
- The tongue
- The tonsils and oropharynx
- The gums, floor of the mouth, and other parts of the mouth
The rest are found in the lips, the minor salivary glands (which often occur in the roof of the mouth), and other sites.
To avoid confusion, it is important to know the exact type of cancer you have. Mouth cancer is one of several types of cancers grouped in a category called head and neck cancers. Mouth cancer and other head and neck cancers are often treated similarly. Cancers arising in the oral cavity are often first treated by head and neck surgeons.
Since an overwhelming predominance of oral cavity cancers are squamous cell carcinomas (SCC), most information about risk factors relates to that histologic entity. Tobacco and alcohol use are the two strongest risk factors for oral cavity squamous cell carcinoma 5. The risk of oral squamous cell carcinoma is reported to be almost 2 times higher in male smokers compared with nonsmokers, and 3 times higher in female smokers. Reverse smoking, in which the lit end of a tobacco cigarette is held in the mouth during inhalation, is also causative of oral squamous cell carcinoma, with particular risk of cancer of the hard palate. Consumption of 1 to 2 alcoholic drinks per day increases cancer risk by a factor of 1.7 compared with nondrinkers 6. Individuals who use both tobacco and alcohol have a cancer risk substantially higher than that derived from use of either one by itself. Exposure to smokeless tobacco products is also a risk factor for oral squamous cell carcinoma, with a risk 4 times higher in users than nonusers 7.
In South and Southeast Asia, betel nut (areca nut) wrapped in betel leaf is commonly chewed for its mild stimulant properties. This habit is associated with development of oral squamous cell carcinoma. Preparations often include tobacco as well.
Mouth cancer may not be found until it is relatively advanced because there might not be any pain or symptoms. A dentist is the person most likely to discover a mouth cancer, so it’s important to have regular dental check-ups.
The American Cancer Society’s most recent estimates for oral cavity and oropharyngeal cancers in the United States for 2022 are 4, 8:
- New cases: About 54,000 new cases of oral cavity or oropharyngeal cancer.
- Deaths: About 11, 230 deaths from oral cavity or oropharyngeal cancer.
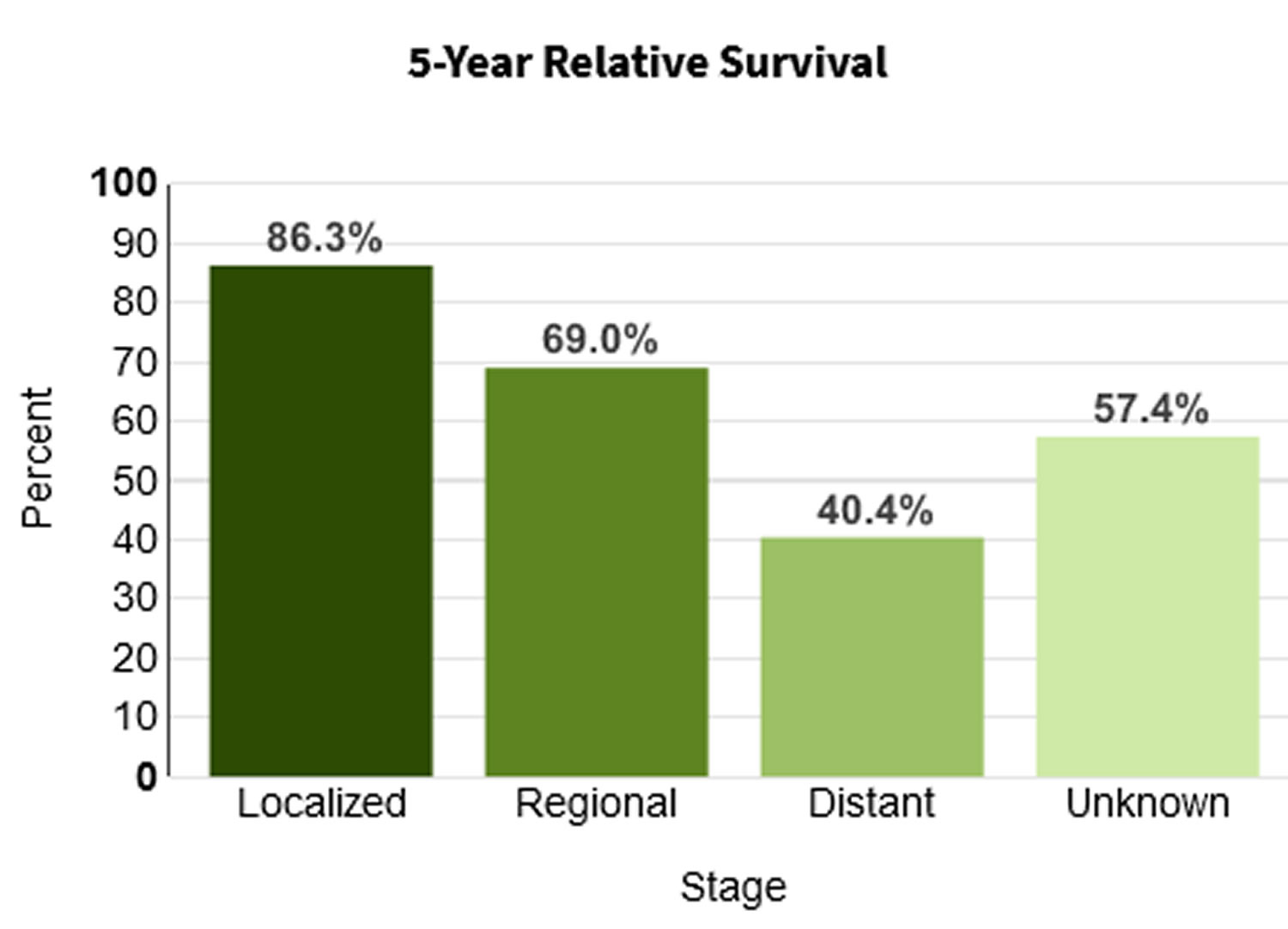
- 5-Year Relative Survival: 68%. Relative survival is an estimate of the percentage of patients who would be expected to survive the effects of their cancer. It excludes the risk of dying from other causes. Because survival statistics are based on large groups of people, they cannot be used to predict exactly what will happen to an individual patient. No two patients are entirely alike, and treatment and responses to treatment can vary greatly.
- Oral cavity or oropharyngeal cancer deaths as a percentage of All Cancer Deaths: 1.8%. The overall death rate for these cancers has been decreasing over the last 30 years.
- Rate of New Cases and Deaths per 100,000: The rate of new cases of oral cavity and pharynx cancer was 11.5 per 100,000 men and women per year. The death rate was 2.5 per 100,000 men and women per year. These rates are age-adjusted and based on 2015–2019 cases and deaths.
- Lifetime Risk of Developing Cancer: Approximately 1.2 percent of men and women will be diagnosed with oral cavity and pharynx cancer at some point during their lifetime, based on 2017–2019 data.
- In 2019, there were an estimated 410,376 people living with oral cavity and pharynx cancer in the United States.
The average age of most people diagnosed with oral cavity or oropharyngeal cancers is 63, but they can occur in young people. Just over 20% (1 in 5) of cases occur in patients younger than 55.
Oral cavity and oropharyngeal cancers are more than twice as common in men as in women. They are slightly more common in White people than Black people.
Overall, the lifetime risk of developing oral cavity and oropharyngeal cancer is: about 1 in 60 (1.7%) for men and 1 in 140 (0.71%) for women. Oral cancer appears to occur most frequently in developing countries particularly India, Pakistan and Bangladesh. In fact, in some parts of India, oral cancer accounts for more than 50% of all cancer.
The overall rate of new cases of oral cavity and oropharyngeal cancers has risen only slightly over the past 20 years 4. But during this same time, there has been an increase specifically in oropharyngeal cancers associated with an human papilloma virus (HPV) infection. Around 70 out of 100 oral cavity and oropharyngeal cancers (around 70%) are linked to the human papillomavirus (HPV). This is a common virus that causes no harm in most people. But in some people, the human papillomavirus (HPV) can cause changes in the throat making them more likely to become cancerous in the future. These HPV-positive cancers tend to act differently than HPV-negative cancers. HPV positive oropharyngeal cancer is seen in younger people aged between 40 and 50 years, who do not smoke 9.
Doctors test your oropharyngeal cancer cells to see if they contain the HPV virus. This affects what stage your cancer is and your outlook (prognosis). Doctors know that oropharyngeal cancers containing HPV tend to do better than cancers that don’t contain HPV. Doctors are looking at this in research to see if people with HPV positive cancers can have less intense treatments in the future 10.
Treatment of oral cancer depends on the type of cancer and the stage of the cancer. In general, diagnosis and treatment during the early stages of cancer have a much better outcome. Oral cancer squamous cell carcinoma is generally treated by surgery and/or radiation therapy. Chemotherapy may also be used, particularly in patients with confirmed metastases to other tissues and organs.
Oral health needs are addressed prior to cancer therapy. This is to minimize oral disease and post-therapeutic complications. It appears that up to 97% of patients require oral healthcare before treatment of cancer can begin. Some of the complications that may occur post-cancer treatment are radiotherapy- or chemotherapy-induced mucositis (inflamed mouth), oral ulceration, bleeding, infections, pain, xerostomia (dry mouth) and caries (holes in the teeth).
Surgery is aimed at removing the primary tumor and some of the surrounding normal tissue to make sure the cancer has been completely removed. If done during the early stages of cancer there is usually little or no post-treatment disfigurement. Surgery performed at later stages may also require reconstruction of parts of the mouth or face.
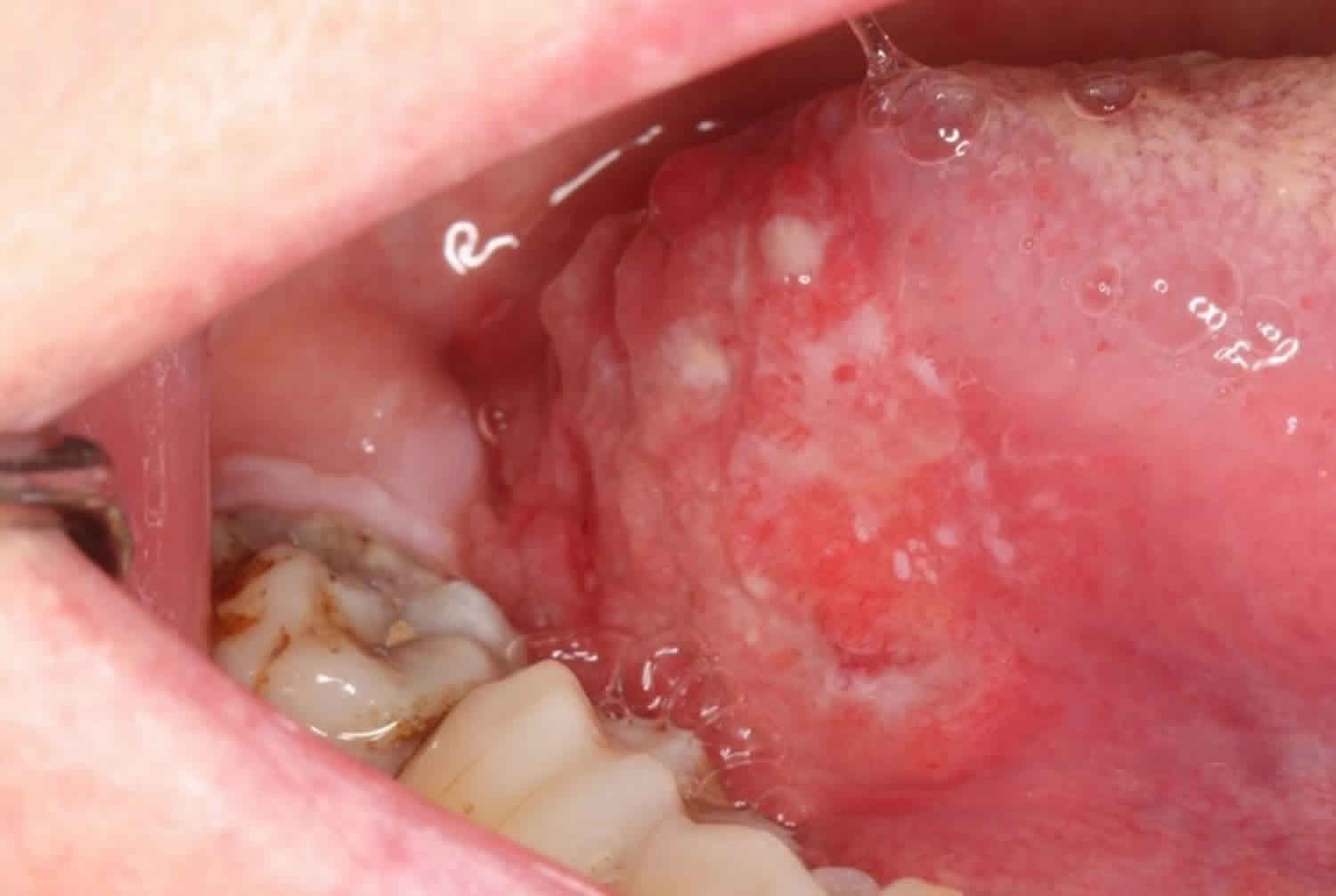
Figure 1. Oral cavity cancer
Footnote: Mouth cancer white patches. Mouth cancer signs may include bleeding, swelling, white patches or redness in your mouth.
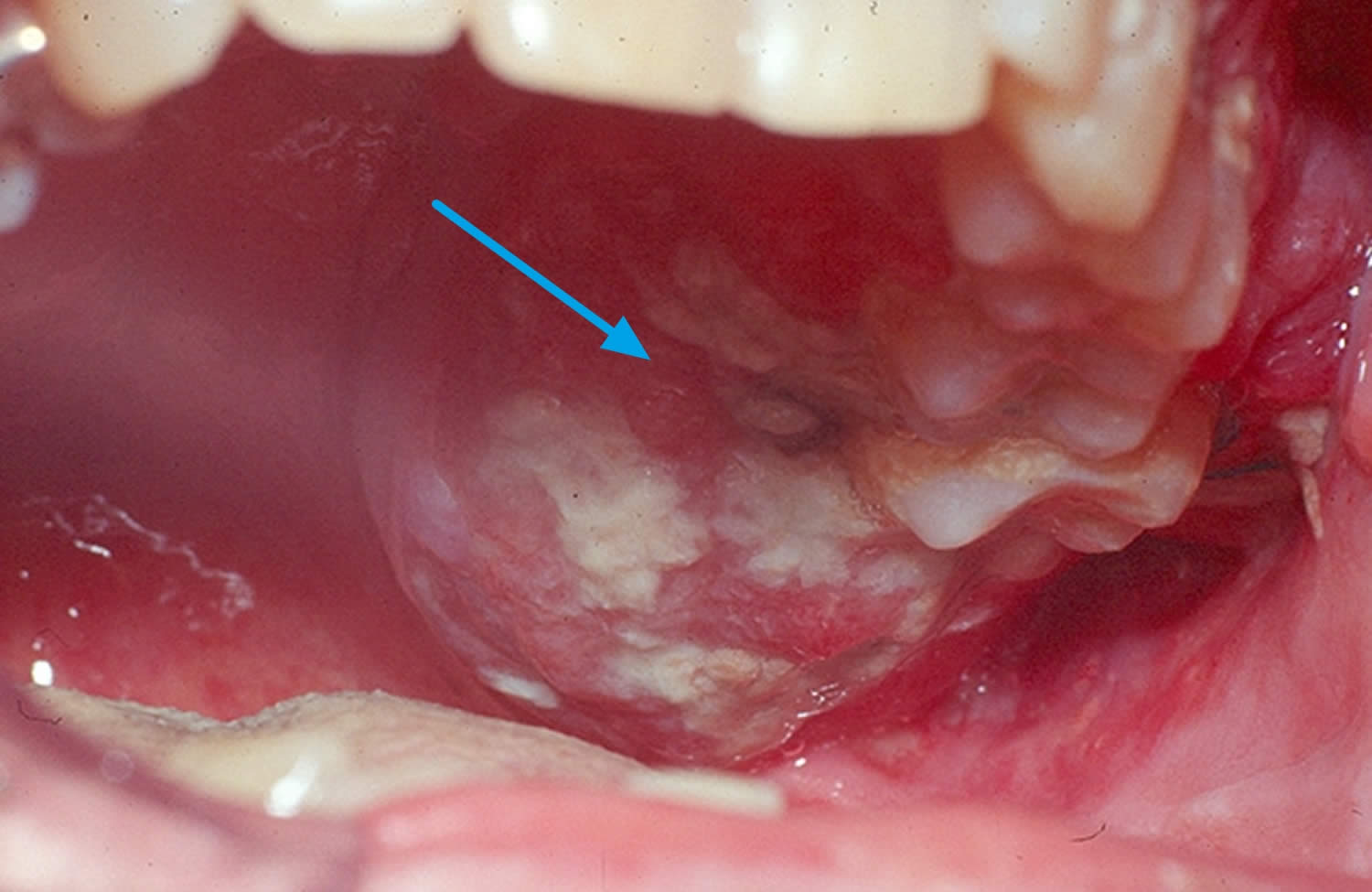
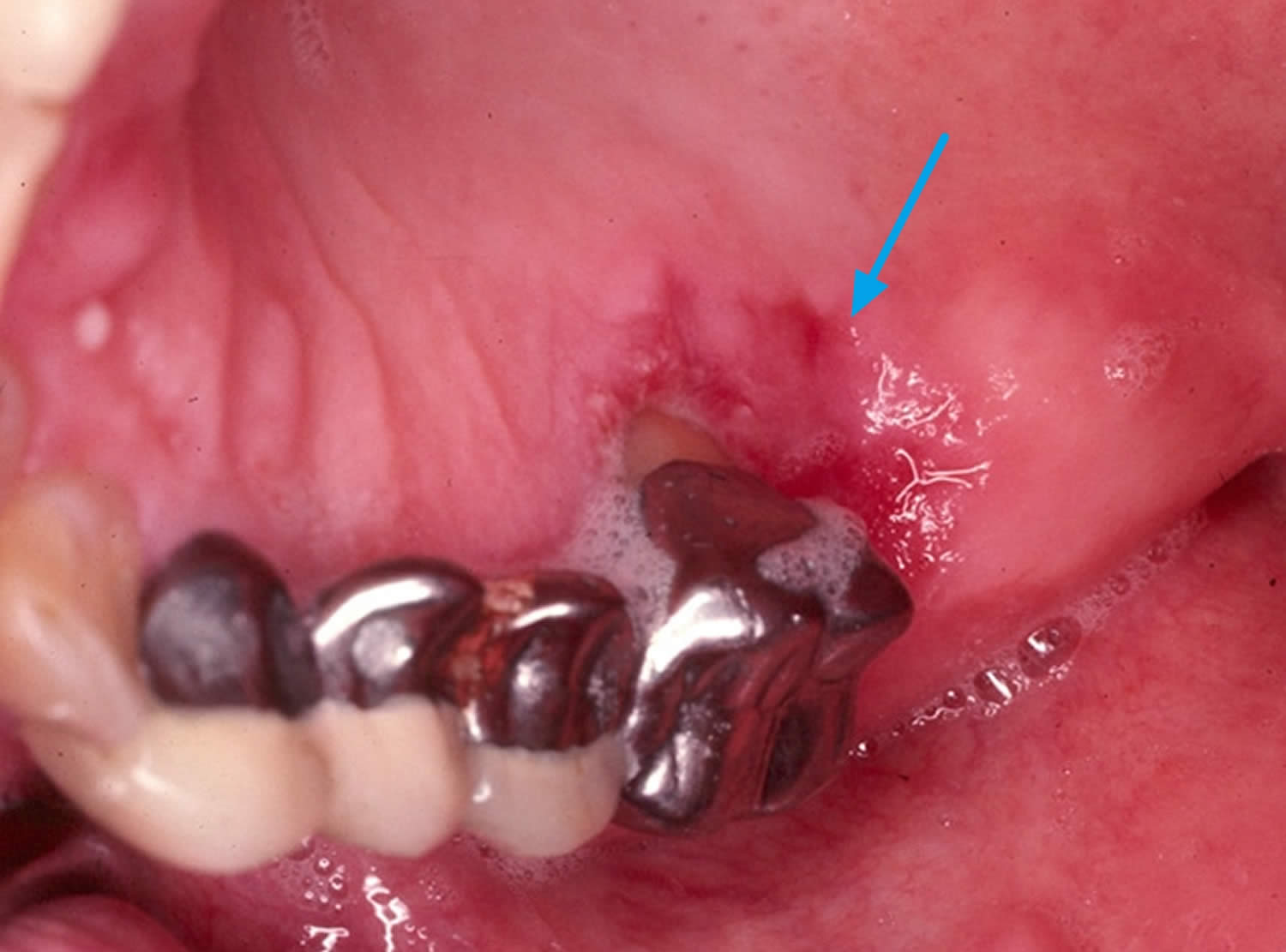
Figure 2. Oral cancer
Footnote: Mouth cancer red sore. Mouth cancer signs may include red sores that don’t heal.
How mouth cancer spreads
Cancer cells can spread from the mouth to other parts of the body. This spread is called metastasis.
There are 2 ways mouth cancer can spread:
- Directly, by spreading to nearby tissue, such as surrounding skin or to the back of the jaw
- Through the lymphatic system, which is the network of vessels and glands found throughout your body which produces special cells that are needed by your immune system to fight infection
Mouth cancer that spreads to another part of the body is known as metastatic oral cancer, which are often called secondaries. The lymph glands in the neck are usually the first place where mouth cancer forms secondaries.
If oral cancer spreads, it can spread to the following:
- other parts of the mouth
- muscle surrounding the mouth
- lymph nodes in the neck (called cervical lymph nodes)
- bone surrounding the mouth (the upper or lower jawbone)
- skin on the face
- salivary glands
- liver
- lung
- distant bone, such as the base of the skull or the spine
- brain
Oral cavity and oropharyngeal cavity anatomy
The oral cavity or the mouth extends from the border between the skin and the lips (skin-vermilion junctions of the anterior lips) to the junction of the hard and soft palates above and to the line of circumvallate papillae below and is divided into the following specific areas:
- Lips
- Anterior two thirds of tongue
- The inner lining of the cheeks (buccal mucosa)
- Floor of mouth
- Lower gingiva (the gums)
- Retromolar trigone
- Upper gingiva (the gums)
- The teeth and alveolar ridge (the ridge-like border of the jaws that contains the sockets of the teeth)
- The upper jawbone (maxilla)
- Hard palate (the bony part at the front of the roof of the mouth formed by part of the upper jawbone)
- The uvula
- The lower jawbone (mandible)
The roof of the mouth is formed by the hard palate and the soft palate. The mouth leads into the oropharynx (the middle part of the pharynx) and the soft palate separates the mouth from the nasopharynx (the upper part of the pharynx). The inner surface of the cheeks forms the sides of the mouth. The tongue takes up most of the floor of the mouth (the lowest part of the mouth).
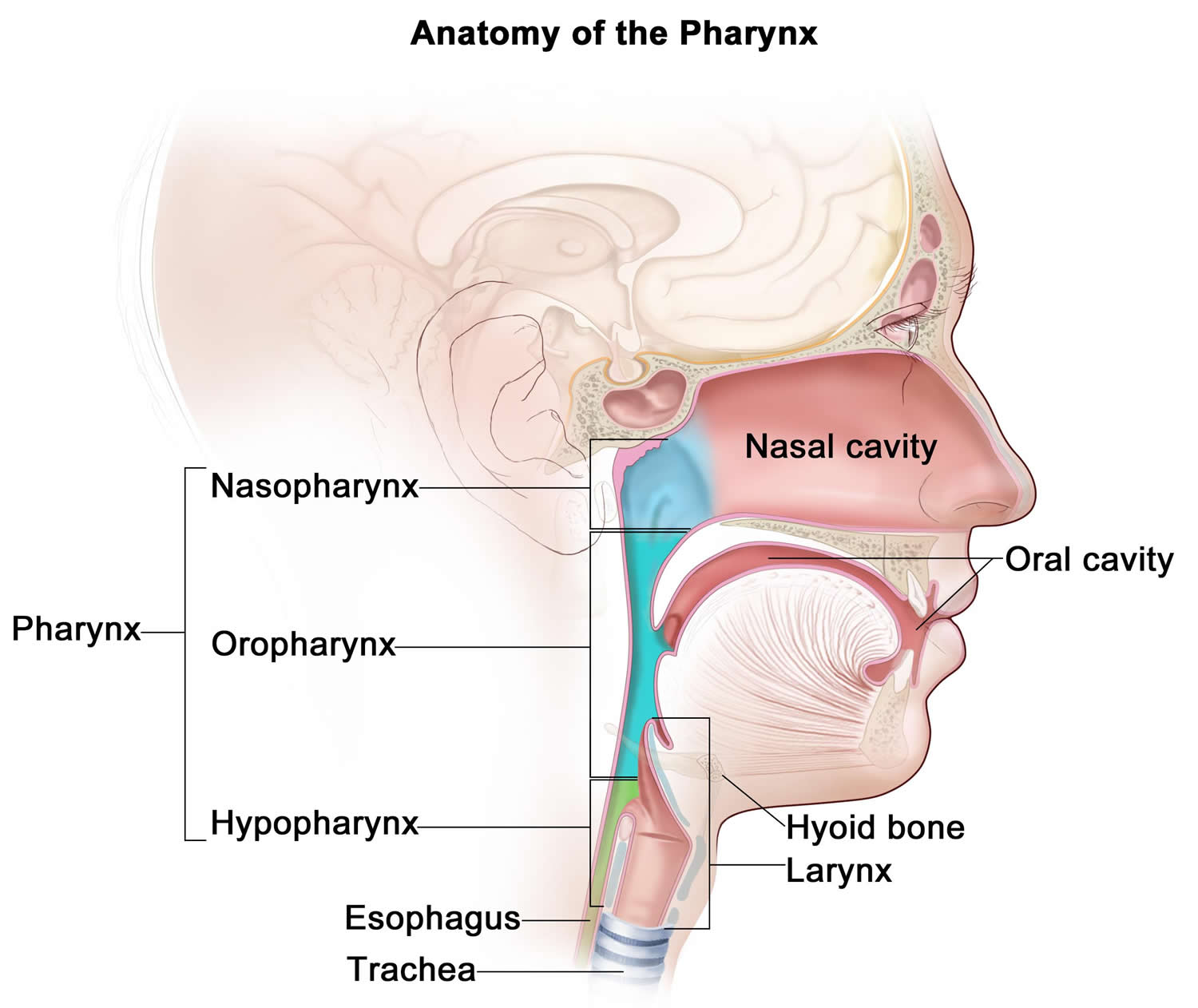
The pharynx or the throat is divided into 3 parts (see Figure 4).
The parts are:
- Oropharynx
- Nasopharynx
- Laryngopharynx
The oropharynx is the part of the throat just behind the mouth. Cancer starting in this area is called oropharyngeal cancer.
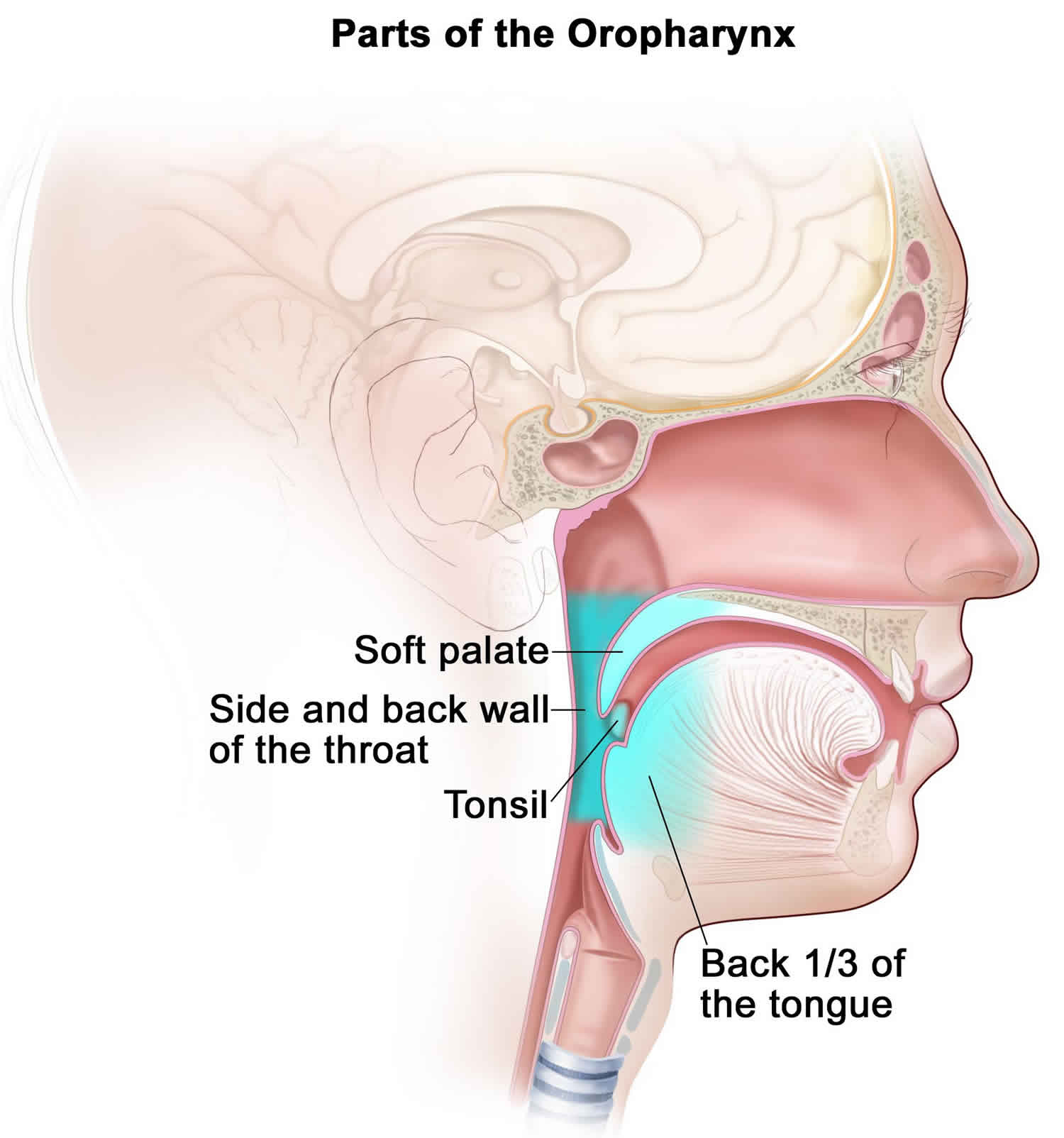
The oropharynx includes the (Figure 5):
- back 1/3 of the tongue
- soft area at the back of the roof of the mouth (soft palate)
- the tonsils and 2 ridges of tissue in front of and behind the tonsils (tonsillar pillars)
Your mouth and oropharynx help you breathe, talk, eat, chew and swallow.
The mouth has many jobs. It analyzes food and other materials that are put into it so you can decide if they should or shouldn’t be swallowed. The first step of digesting food happens in the mouth. We use our teeth to chew food. Chemicals in our saliva start to break down starches (carbohydrates). Saliva in the mouth also makes food slippery so it can be swallowed more easily. Taste buds on the tongue tell us what our food tastes like. The tongue and soft palate also move food around in the mouth to help with chewing and swallowing.
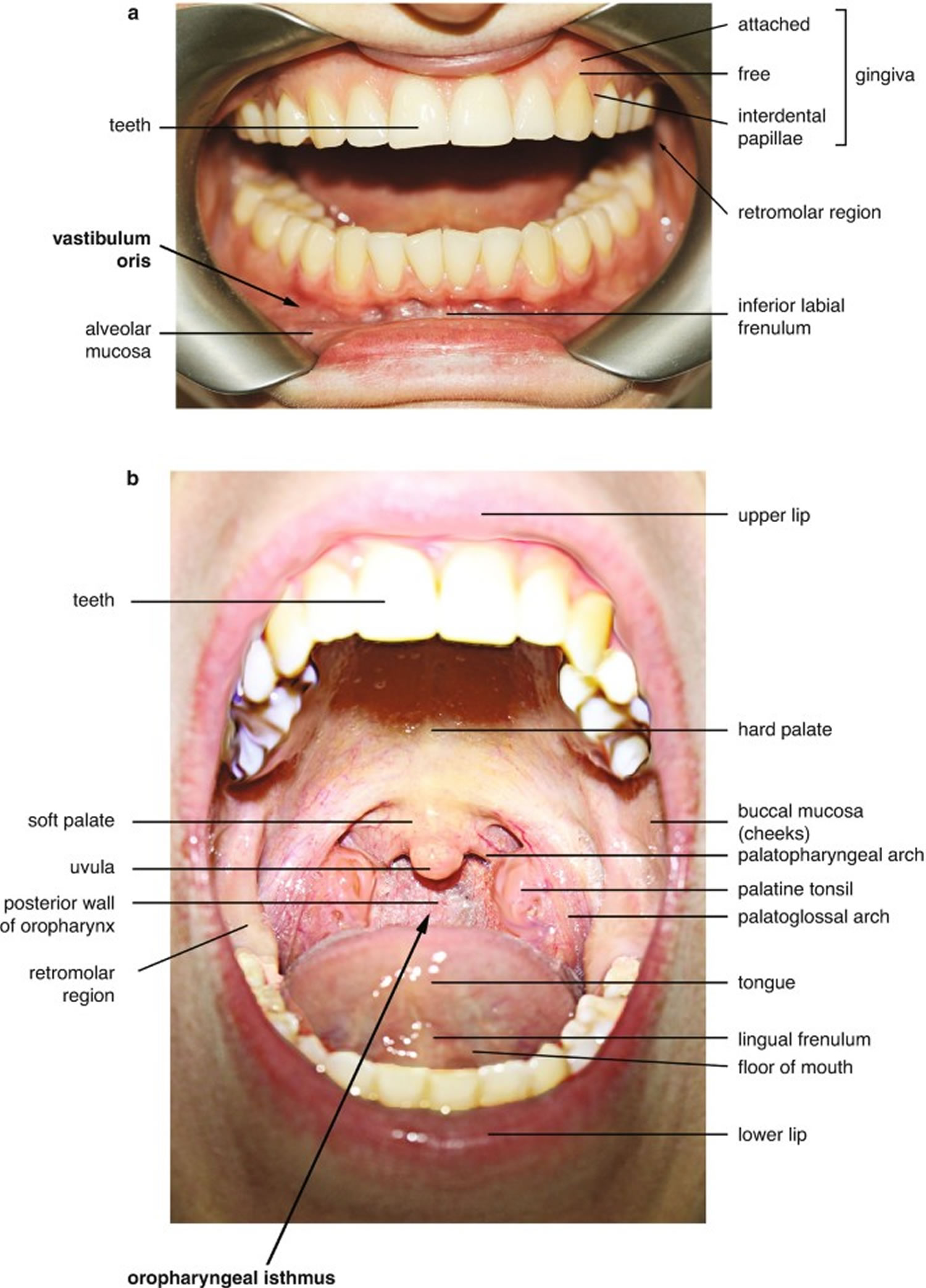
Figure 3. Oral cavity anatomy
Footnote: Anatomy of the oral cavity. The oral cavity includes the lips, hard palate (the bony front portion of the roof of the mouth), soft palate (the muscular back portion of the roof of the mouth), retromolar trigone (the area behind the wisdom teeth), front two-thirds of the tongue, gingiva (gums), buccal mucosa (the inner lining of the lips and cheeks), and floor of the mouth under the tongue.
Figure 4. Oropharynx anatomy
Figure 5. Oropharynx parts
Types of oral cancer
The type of cancer tells you what type of cell the cancer started in. The different parts of the oral cavity and oropharynx are made up of many types of cells. Different cancers can start in each type of cell. These differences are important, because they can determine a person’s treatment options and prognosis (outlook).
Most mouth and oropharyngeal cancers start in squamous cells and are called squamous cell carcinoma (SCC). Squamous cell carcinoma is the most common type of mouth cancer, accounting for 9 out of 10 cases. Squamous cells are found in many areas of the body, including the inside of the mouth and in the skin.
Other less common types of mouth and oropharyngeal cancers include:
- salivary gland cancer (adenocarcinoma, which is cancers that develop inside the salivary glands)
- adenoid cystic tumors
- basal cell carcinoma
- sarcoma, which grows from abnormalities in bone, cartilage, muscle or other tissue
- lymphoma, which grows from cells usually found in lymph glands, but they can also grow in the mouth
- oral malignant melanoma, where cancer starts in the cells that produce skin pigment or color (melanocytes). These appear as very dark, mottled swellings that often bleed
Some abnormal areas and growths in the mouth and oropharynx are not cancerous (benign). Sometimes, patches in the mouth contain abnormal cells that can turn into cancer if left untreated. These patches are described as pre-cancerous.
Squamous cell carcinoma of the oral cavity and oropharynx
Almost all of the cancers in the oral cavity and oropharynx are squamous cell carcinomas, also called squamous cell cancers. These cancers start in squamous cells, which are flat, thin cells that form the lining of the mouth and throat.
The earliest form of squamous cell cancer is called carcinoma in situ. This means that the cancer cells are only in the layer of cells called the epithelium (the top layer of cells lining the oral cavity and oropharynx). This is different from invasive squamous cell cancer, where the cancer cells have grown past the epithelium, into the deeper layers of the oral cavity or oropharynx.
HPV-related cancers: Infection with certain high-risk types of the human papillomavirus (HPV) causes most of the squamous cell cancers of the oropharynx (called HPV-positive cancer). HPV is rarely associated with oral cavity cancer. HPV-positive cancers are seen more often in young people with no history of tobacco or alcohol use. These cancers tend to have a better outcome (prognosis) than squamous cell cancers not related to an HPV infection (HPV-negative cancer). This is most likely because HPV-positive cancers shrink when treated with chemotherapy and radiation.
Verrucous carcinoma is a rare type of squamous cell cancer that is most often found in the gums and cheeks. It’s a low-grade (slow growing) cancer that hardly ever spreads to other parts of the body.
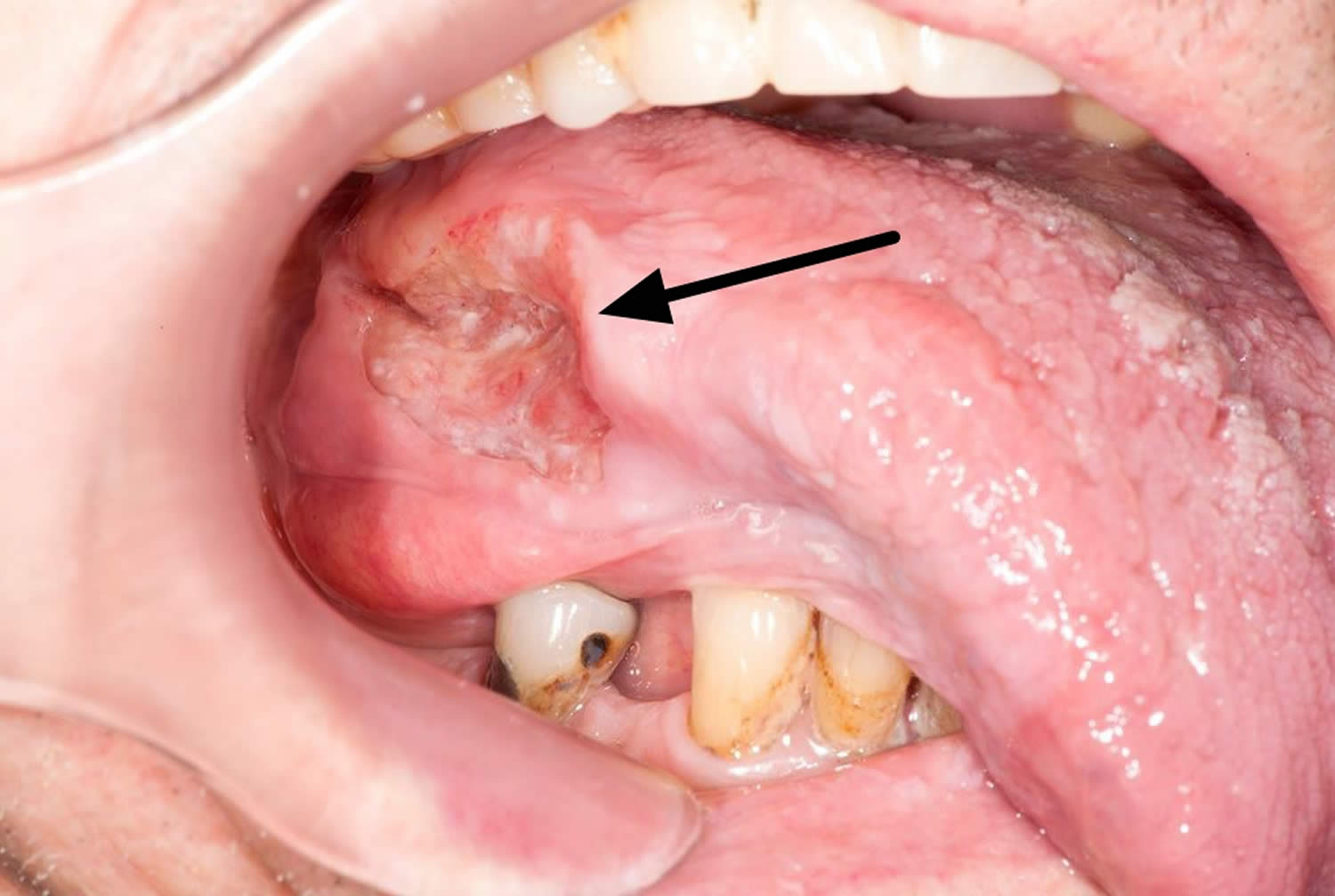
Figure 6. Squamous cell carcinoma tongue (squamous cell cancer of the tongue)
Minor salivary gland cancers
These cancers can start in the minor salivary glands in the lining of the mouth and oropharynx. There are many types of minor salivary gland cancers, including adenoid cystic carcinoma, mucoepidermoid carcinoma, and polymorphous low-grade adenocarcinoma. Minor salivary gland cancers are mostly a type of cancer called adenocarcinoma. Adenocarcinomas are a type of cancer that starts in glandular tissue.
Most salivary gland cancers start in the parotid glands. Around 80 in 100 (around 80%) salivary gland cancers start here. Just over 10 in 100 (just over 10%) start in the submandibular glands. The rest starts in either the sublingual glands or the minor glands.
Adenoid cystic tumor
This is a rare type of tumor and can develop from glandular tissue in the salivary glands or the mouth. The parotid gland is the most common place to find this type of cancer.
Basal cell carcinoma
Basal cell carcinoma (BCC) is a type of skin cancer that develops from basal cells, and can be found on the lips. Basal cell carcinoma (BCC) is the most common type of skin cancer. About 75 out of every 100 non melanoma skin cancers (about 75%) are BCCs. They are usually treated by surgery. The outlook for this cancer type is very good.
Oral melanoma
Melanomas develop from the pigment producing cells called melanocytes that give skin its color. It is not a very common type of mouth or oropharyngeal cancer. Around 1 out of every 100 (around 1%) of oral cavity cancers are melanomas.
Melanomas of the head and neck can occur anywhere on the skin or inside the nose or mouth (oral cavity).
Some treatments for melanomas in the oral cavity are different to squamous cell cancers.
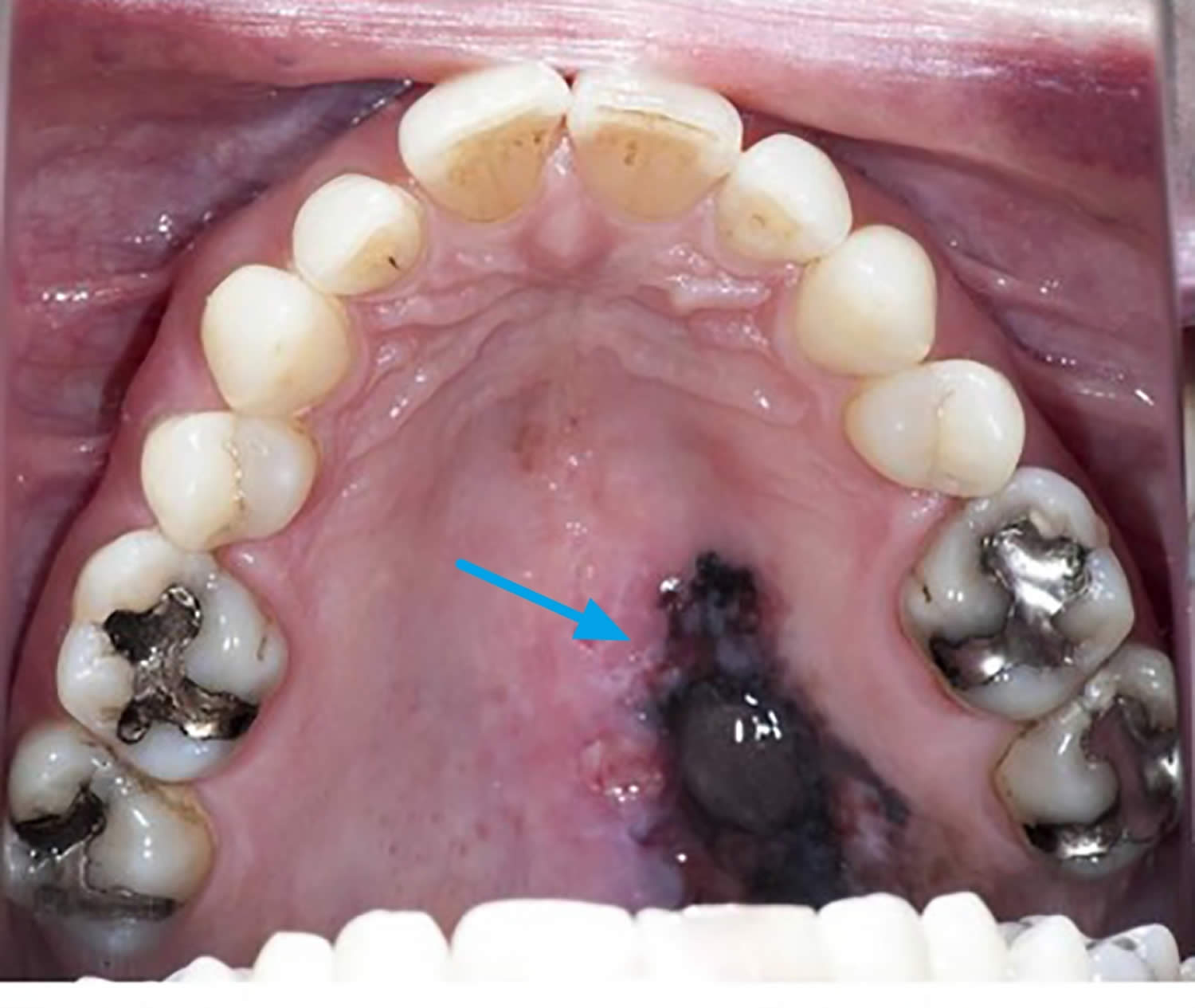
Figure 7. Oral melanoma
[Source 11 ]Lymphomas
Lymphoma is a cancer of the lymphatic system, which is part of the body’s germ-fighting network. Lymphomas are cancers that start in white blood cells called lymphocytes. Lymphocytes are part of the body’s immune system. The lymphatic system includes the lymph nodes (lymph glands), spleen, thymus gland and bone marrow. The tonsils and base of the tongue contain immune system (lymphoid) tissue, where cancers called lymphomas can start. Lymphoma can also affect all those areas as well as other organs throughout the body. The World Health Organization’s (WHO) classification system identifies more than 90 different subtypes of lymphoma 12.
There are many types of lymphoma. The main types of lymphoma are:
- Hodgkin’s lymphoma (Hodgkin disease): Hodgkin’s lymphoma (Hodgkin disease) is a cancer that starts in white blood cells called lymphocytes. Hodgkin’s lymphomas contain cells called Reed Sternberg cells. Treatment for Hodgkin’s lymphoma is different from other types of lymphoma. Hodgkin’s lymphoma is one of the most curable forms of cancer. The five-year relative survival rate is 94.3 percent for people who were less than 45 years old at diagnosis. Hodgkin lymphoma is most commonly diagnosed at 20 to 34 years of age; however, the median age at death is 68 because of the higher survival rate among younger patients 13.
- Non-Hodgkin’s lymphoma (NHL): Non-Hodgkin lymphoma (NHL) is a cancer that starts in cells called lymphocytes, which are part of the body’s immune system. About 90 percent of people diagnosed with lymphoma have non-Hodgkin’s lymphoma (NHL). Incidence of non-Hodgkin lymphoma is higher in men and whites, and it increases with age. The median age of patients at diagnosis of non-Hodgkin lymphoma is 67 years, and the median age at death is 76 14.
They behave, spread, and respond to treatment differently, so it’s important for you to know which one you have. Knowing which type of lymphoma you have is important because it affects your treatment options and your outlook (prognosis). If you aren’t sure which type you have, ask your doctor so you can get the right information.
What lymphoma treatment is best for you depends on your lymphoma type and its severity. Lymphoma treatment may involve chemotherapy, immunotherapy medications, radiation therapy or a bone marrow transplant.
Precancerous lesions of oral cavity
Precancerous lesions of the mouth are changes to cells of the mouth that make them more likely to develop into cancer. These conditions are not yet cancer, but there is a chance that they may become oral cancer if they aren’t treated. The most common precancerous conditions of the mouth are leukoplakia, erythroplakia, and mixed erythroleukoplakia 15. Leukoplakia, the most common of the three conditions, is defined by the World Health Organization as “a white patch or plaque that cannot be characterized clinically or pathologically as any other disease” 16. The diagnosis of leukoplakia is one of exclusion; conditions such as candidiasis, lichen planus, leukoedema, and others must be ruled out before a diagnosis of leukoplakia can be made 15.
The prevalence of leukoplakia in the United States is decreasing; this decline has been related to reduced tobacco consumption 17. Although erythroplakia is not as common as leukoplakia, it is much more likely to be associated with dysplasia or carcinoma 18.
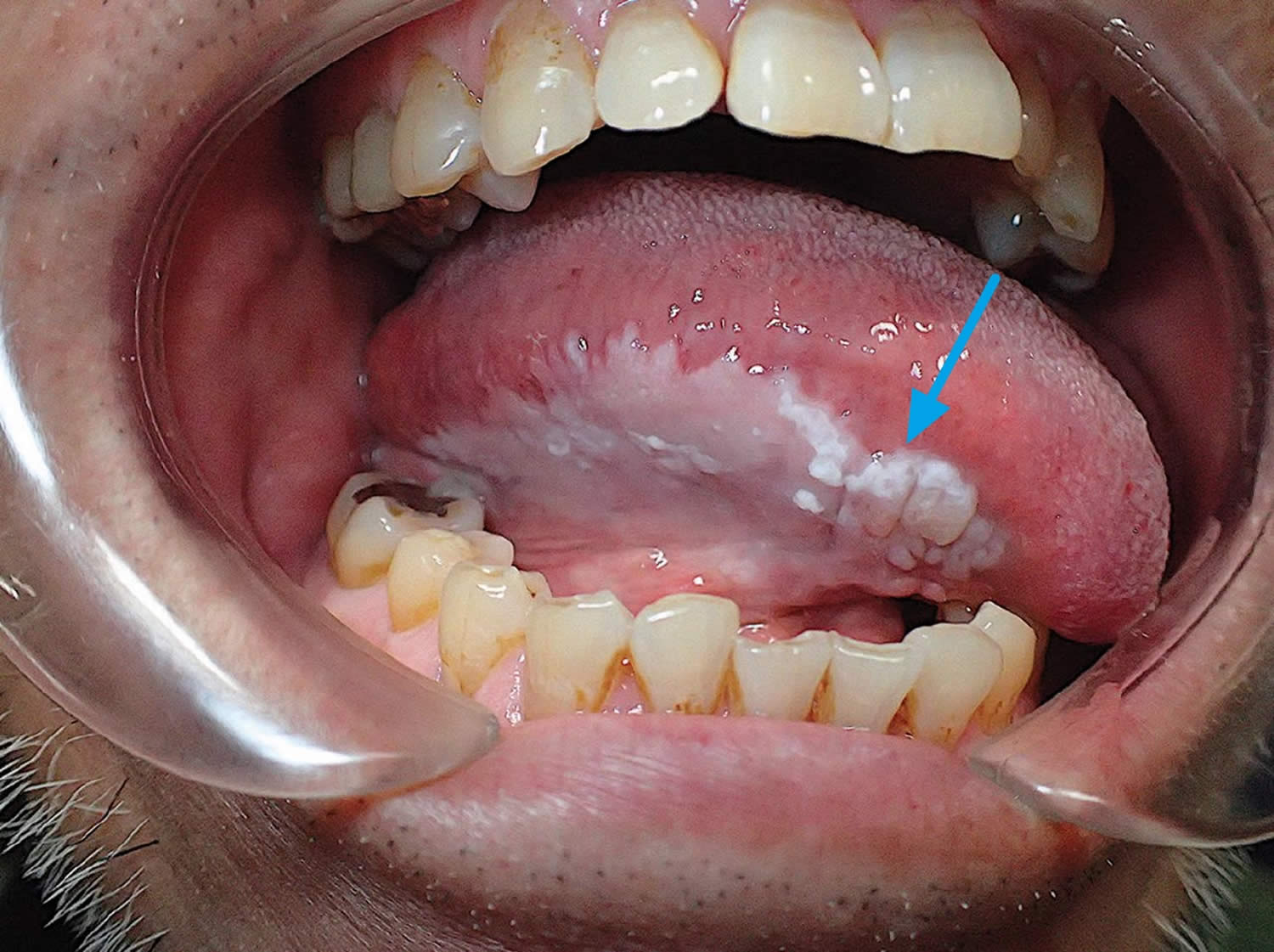
Oral leukoplakia
Oral leukoplakia describes an abnormal white patch or plaque or grey area that develops on the tongue, the inside of the cheek, the gums or the floor of your mouth that cannot be characterized clinically or pathologically as any other disease 19. Leukoplakia is the most common chronic keratotic lesion of the oral cavity and is potentially pre-malignant lesion that is associated with squamous cell carcinoma (SCC) 20. Malignant transformation occurs in 2% to 3% of cases. Features associated with a higher rate of malignant transformation are nonhomogeneous oral leukoplakia, presence of red lesions (erythroplakia), large lesion size (> 200 mm), location on the tongue or floor of the mouth, age over 50, female sex, no history of smoking, and the presence of severe dysplasia 21, 22. Candida and human papillomavirus (HPV) are infectious risk factors 23.
Oral leukoplakia is a clinical diagnosis and is characterized predominantly by adherent white plaques of the oral mucosa 24. Oral leukoplakia has an estimated prevalence of 0.1% 24 and is mostly found on the tongue of middle-aged and older men who smoke 23. There is a strong association with tobacco smoking (leukoplakia is six times more common in smokers than non-smokers) and alcohol intake (independent of drinking pattern or beverage type). It is also associated with betel quid chewing and oral submucous fibrosis.
The following risk factors increase your chance of developing leukoplakia:
- smoking heavily
- chewing tobacco
- excessive alcohol use
The presence of leukoplakia does not necessarily mean cancer. The risk of developing oral cancer depends on how different the abnormal cells are in shape, size and appearance compared to normal mouth cells. This abnormality is called dysplasia. Doctors or dentists will closely watch people who have leukoplakia to look for signs of cancer.
For the initial management of oral leukoplakia, incisional biopsy for histopathologic study is the gold standard 25. The histopathologic appearance of oral leukoplakia can range from hyperkeratosis to various degrees of epithelial dysplasia 24. The clinical diagnosis of leukoplakia should change to a pathohistologic diagnosis in the presence of in situ carcinoma, squamous cell carcinoma, or verrucous carcinoma 24.
The treatment of oral leukoplakia depends on its cause. The approach to management—ie, surgical resection, laser treatment, or careful monitoring—should be selected based on the histopathologic degree of dysplasia and on clinical features 21. Nonsurgical treatments have included administration of retinoids, vitamin C, beta carotene supplements, 5-fluorouracil, and bleomycin 24. These treatments may be effective for resolution of the lesions; however, there is no evidence that they prevent malignant transformation 26. But regardless of the treatment, long-term observation and periodic biopsy are important to monitor for recurrence and for evidence of malignant transformation 24.
Figure 8. Leukoplakia
Footnote: Homogeneous flat white plaque measuring 45 mm × 20 mm and with slight corrugations was seen on the right lateral border of the tongue.
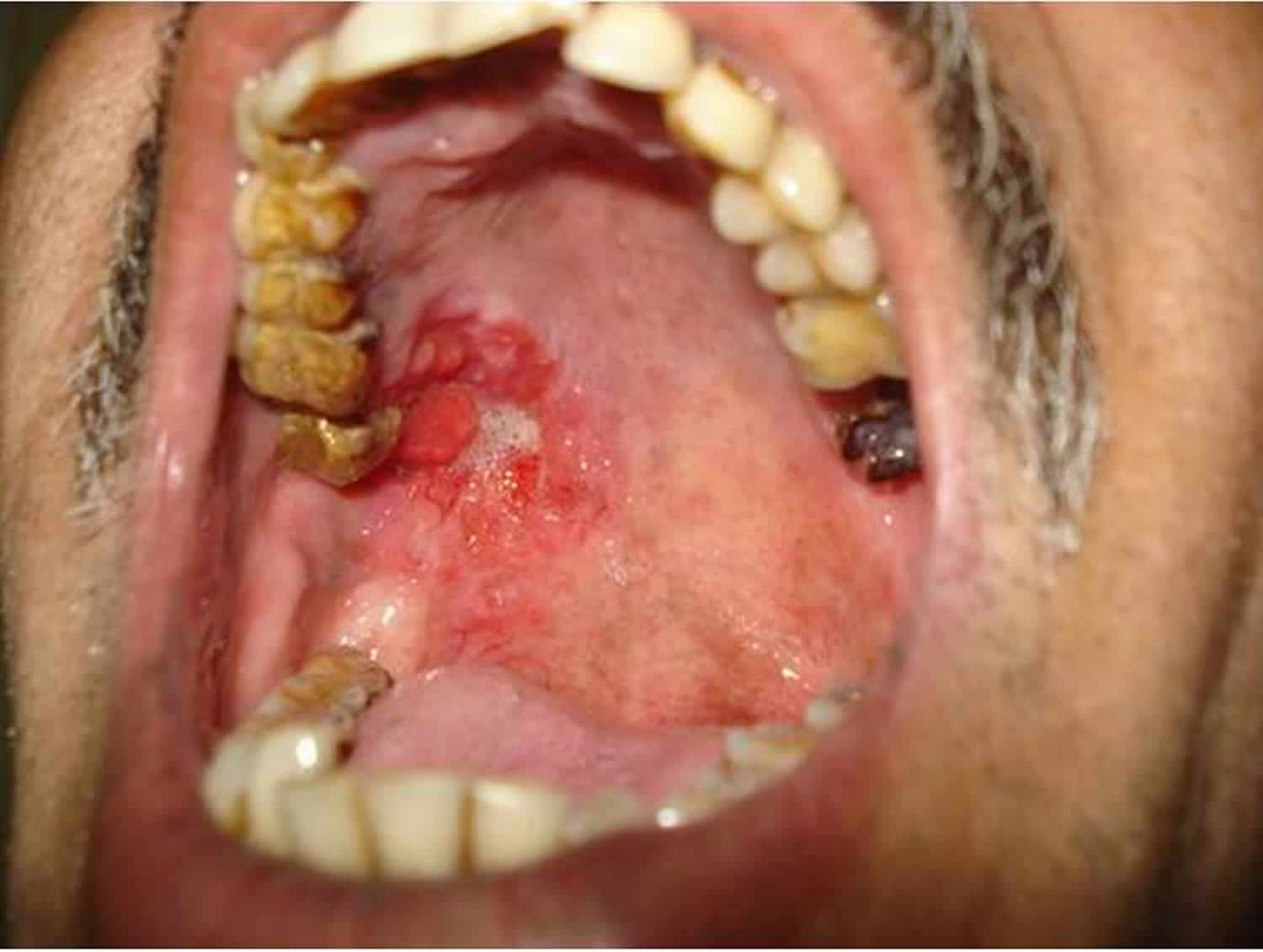
[Source 25 ]Oral erythroplakia
Erythroplakia is an abnormal red area or group of red spots that forms on the mucous membrane lining the mouth with no clear cause. The World Health Organization (WHO) originally defined erythroplakia as ‘any lesion of the oral mucosa that presents as bright red velvety plaques which cannot be characterized clinically or pathologically as any other recognizable condition’. There is no universally accepted definition of oral erythroplakia, however, the majority of modern definitions, are more or less reductive of the original WHO definition. The most frequently used definition in the literature described as oral erythroplakia as a red patch or red flat area or slightly raised or worn away red area that results when the lining of the mouth thins that cannot be accounted for by any specific disease entity or condition 27. The area appears red because the underlying capillaries are more visible. Oral erythroplakia is the rarer form of oral pre-malignant lesion and has been identified as the one with the highest malignant transformation rates 28. About 50% of these lesions develop into squamous cell carcinoma (SCC).
The following risk factors increase your chance of developing erythroplakia:
- smoking heavily
- chewing tobacco
- excessive alcohol use
Erythroplakia is usually asymptomatic, although some patients may complain of a sore, burning or metallic sensation. The development of pain or soreness may be associated with a malignant change.
For diagnosis, your dentist or doctor will ask you about any symptoms you have and do a dental or oral exam. They may take a sample of cells from the abnormal area (called a biopsy) so they can be tested in a lab.
Treatment options for erythroplakia may include:
- careful watching (active surveillance) and frequent follow-up
- surgery
- cryosurgery
- laser surgery
Because erythroplakia can develop into cancer, people with this condition should avoid known risk factors, such as using tobacco and drinking alcohol.
Figure 9. Erythroplakia
Footnote: Erythroplakia. Note the red velvety lesion involving the posterior aspect of the right side of the hard palate. Note the raised irregular area along the anterolateral aspect of the lesion which is clinically suspicious of malignant transformation.
Oral cancer signs and symptoms
Oral cavity (mouth) and oropharyngeal (throat) cancers might cause one or more of these signs or symptoms:
- A lip or mouth sore that doesn’t heal
- A sore throat that does not get better after a few days
- Mouth ulcers that are painful and do not heal within several weeks
- A white or reddish patch on the inside of your mouth or tongue. These can be early signs of cancer, so they should also be checked
- Loose teeth for no clear reason or teeth sockets that do not heal after extractions
- Pain around the teeth
- Dentures that start to fit poorly or become uncomfortable
- A growth or lump inside your mouth or throat
- Unexplained, persistent lumps in the mouth or the neck that do not go away
- A sore throat or a feeling that something is caught in your throat that doesn’t go away
- Mouth pain
- Ear pain that does not get better in a few days
- Difficult or painful swallowing
- Difficulty moving your jaw or chewing
- Trouble moving your tongue
- Unexplained, persistent numbness or an odd feeling on the tongue, lip, or other area of the mouth
- A lump or thickening of your lip
- Changes in speech, such as a lisp
- Unexplained weight loss
- Bad breath
- Unusual bleeding in your mouth
- Voice changes
Many of these signs and symptoms can also be caused by diseases other than cancer, or even by other cancers. See a doctor or dentist if these symptoms do not get better within 2 weeks, particularly if you drink or smoke.
Oral cancer causes
Doctors and scientists can’t say for sure what causes each case of oral cavity or oropharyngeal cancer. But they do know many of the risk factors and how some of them may lead to cells becoming cancer.
Cancers can be caused by DNA mutations (gene changes) that turn on oncogenes or turn off tumor suppressor genes. This leads to cells growing out of control. Changes in many different genes are usually needed to cause oral cavity and oropharyngeal cancer.
Some genes control when cells grow, divide, and die:
- Genes that help cells normally grow, divide, and stay alive are called proto-oncogenes. When a proto-oncogene mutates (changes), the gene becomes abnormal and is then called an oncogene.
- Genes that help keep cell growth under control or make cells die at the right time are called tumor suppressor genes.
Scientists believe that some risk factors, such as tobacco or heavy alcohol use, may cause these cancers by damaging the DNA of cells that line the inside of the mouth and throat.
When tobacco and alcohol damage the cells lining the mouth and throat, the cells in this layer need to divide more often and make more copies of themselves. This increases the chance to make mistakes when copying their DNA, which may increase the possibility of becoming cancer.
Many of the chemicals found in tobacco can damage DNA directly. Scientists are not sure whether alcohol directly damages DNA, but they have shown that alcohol helps many DNA-damaging chemicals get into cells more easily. This may be why the combination of tobacco and alcohol damages DNA far more than tobacco alone. Acetaldehyde, a breakdown product of alcohol, is found in saliva (spit). It has been shown to get in the way of normal DNA repair, as well as disturb other functions of DNA. The level of acetaldehyde goes up as people drink more alcohol which may be one way alcohol damages the cells lining the oral cavity.
This damage can cause certain genes (for example, those in charge of starting or stopping cell growth) to not work well. Abnormal cells can begin to grow out of control, forming a tumor.
Oral cancer risk factors
A risk factor is something that increases the risk of developing cancer. Smoking and excessive alcohol intake (>5 standard drinks/day) are regarded as the main risk factors for the development of oral squamous cell carcinoma in United States. Smoking confers a 7 × relative risk of the development of oral squamous cell carcinoma and alcohol intake of >50 g/day confers a 6 × relative risk of developing oral cancer 29. In subcontinental countries, betel nut chewing is an important risk factor in the development of oral cancer, where oral cancers represent almost 50% of all total cancer diagnoses (compared with <1% in United States). There is an additional subgroup of non-smoking non-drinking mostly middle age female patients who are also recognized 30.
Tobacco and alcohol use
Tobacco use is one of the strongest risk factors for head and neck cancers, including oral cavity and oropharyngeal cancer. The risk for these cancers is 3 times higher in people who smoke than in people who don’t 31. Most people with these cancers have a history of smoking or other tobacco exposure, like chewing tobacco. The more you smoke, the greater your risk. Smoke from cigarettes, pipes, and cigars all increase your risk of getting these cancers. Some studies have also found that long-term exposure to secondhand smoke might increase the risk of these cancers, but more research is needed to confirm this 32. Pipe smoking is linked to a very high risk for cancer in the part of the lips that touch the pipe stem.
Oral tobacco products (snuff, dip, spit, chew, or dissolvable tobacco) are linked with cancers of the cheek, gums, and inner surface of the lips. Using oral tobacco products for a long time is linked to a very high risk. These products also cause gum disease, destruction of the bone sockets around teeth, and tooth loss.
When diagnosed with oral cavity or oropharyngeal cancer, it’s important for people who smoke or use oral tobacco, to quit smoking and quit all oral tobacco products. People who continue to smoke while getting cancer treatment can have trouble with wound healing, more side effects from radiation therapy or chemotherapy, a higher risk of infection, and worse outcomes. Also, continuing to smoke and use oral tobacco products after cancer treatment, greatly increases the risk of developing a second cancer in the mouth, throat, larynx (voice box), lung and other organs.
Drinking alcohol increases the risk of developing oral cavity and oropharyngeal cancers. Heavy drinkers have a higher risk than light drinkers.
Smoking and drinking alcohol together multiplies the risk of these cancers. The risk of these cancers in people who drink and smoke heavily is about 30 times higher than the risk in people who don’t smoke or drink.
Smokeless tobacco
Smokeless tobacco products include:
- chewing tobacco
- snuff – powdered tobacco designed to be snorted
Smokeless tobacco products are not harmless and may increase your risk of mouth cancer, as well as other cancers, such as liver cancer, pancreatic cancer and esophageal cancer 33. This practice is most common in Scandinavia and North America 33.
Betel quid and gutka
In Southeast Asia, South Asia, and certain other areas of the world, many people chew betel quid, which is made up of areca nut (betel nut), spices, lime, and other ingredients. Many people in these areas also chew gutka, a mixture of betel quid and tobacco. People who chew betel quid or gutka have an increased risk of cancer of the mouth 31.
Human papillomavirus (HPV) infection
Human papillomavirus (HPV) is a group of more than 200 types of viruses. They’re called papillomaviruses because some of them cause a type of growth commonly called a papilloma or wart.
Infection with certain types of HPV can cause some forms of cancer, including cancers of the penis, cervix, vulva, vagina, anus, mouth, and throat. HPV type 16 (HPV16) is the type most often linked to cancer of the oropharynx, especially those in the tonsil and base of tongue. HPV DNA (a sign of HPV infection) is found in about 2 out of 3 oropharyngeal cancers and in a much smaller portion of oral cavity cancers.
The number of oropharyngeal cancers linked to HPV has risen greatly over the past few decades. These cancers are becoming more common in younger people who have a history of multiple sex partners (including oral sex) and no history of alcohol abuse or tobacco use. Oropharyngeal cancers linked to HPV infection tend to have better outcomes (prognoses) than tumors not caused by HPV because chemotherapy and radiation treatments work better for these cancers. This improvement in outcome however is not seen in people with HPV-related oropharyngeal cancers who also smoke.
Stem cell transplants
Patients who have undergone hemopoietic stem cell transplants are 4 to 7 times more likely to develop oral cancer compared with the average population 34. People who have a stem cell transplant may develop graft-versus-host-disease (GVHD). GVHD is when the healthy transplanted stem cells see the body as foreign and start to destroy the body’s cells, including cells in the mouth. Damage to cells in the mouth from graft-versus-host-disease (GVHD) increases the risk of developing oral cancer. Symptoms include mucositis, xerostomia, and lichenoid changes. The tongue and salivary gland are the most common cancer sites developing 5 to 9 years after transplant 34.
Weakened immune system
Your immune system can be weakened after an organ transplant or treatment for an immune system disease. People with a weakened immune system have a higher risk of developing oral cancer, especially lip cancer. The higher risk may be due to taking drugs that suppress your immune system. People with weakened immune systems are also more likely to get an HPV infection, which increases the risk for oral cancer.
Previous cancer
People who have had oral cancer have a higher risk of developing another oral cancer, especially if they continue to use tobacco or alcohol. Having cancer of the esophagus, larynx, lung or cervix also increases your risk of oral cancer.
Family history of squamous cell carcinoma (SCC)
Squamous cell carcinoma (SCC) is the most common type of oral cancer. There is a higher risk of developing SCC in the head and neck region (including the mouth) if a first-degree family member (parent, sibling or child) has been diagnosed with SCC of the head and neck.
Gender
Oral cavity and oropharyngeal cancers are twice as common in men than in women. This might be because men have been more likely to use tobacco and alcohol in the past. HPV-related oropharyngeal cancers are also seen more often in men.
Unhealthy diet
There’s evidence that an unhealthy diet can increase your risk of getting some types of mouth cancer. Many studies show that not eating enough vegetables and fruit increases the risk of developing oral cancer. Substances like carotenoids, which are common in vegetables and fruit, are linked with a lower risk of oral cancer. Eating a healthy, balanced diet that includes plenty of fruits and vegetables is thought to reduce your risk of developing mouth cancer.
Excess body weight
Having too much body weight appears to increase the risk of cancers of the oropharynx and larynx. Eating more plant-based foods, such as nonstarchy vegetables and whole fruit, might help people lose weight as well as reduce their risk of oropharyngeal and laryngeal cancer from poor nutrition.
Age
Cancers of the oral cavity and oropharynx usually take many years to develop, so they’re not common in young people. Most patients with these cancers are older than 55 when the cancers are first found. HPV-linked cancers tend to be diagnosed in people younger than 50.
Ultraviolet (UV) light
Sunlight is the main source of UV light for most people. Cancers of the lip are more common in people who have outdoor jobs where they are exposed to sunlight for long periods of time.
Poor nutrition
Several studies have found that a diet low in fruits and vegetables is linked with an increased risk of cancers of the oral cavity and oropharynx.
Genetic syndromes
People with syndromes caused by inherited defects (mutations) in certain genes have a very high risk of mouth and middle throat cancer.
- Fanconi anemia: People with this syndrome often have blood problems at an early age, which may lead to leukemia or myelodysplastic syndrome. They also have a very high risk of cancers of the mouth and throat.
- Dyskeratosis congenita: This is a genetic syndrome that can cause aplastic anemia, skin rashes, and abnormal fingernails and toenails. People with this syndrome also have a very high risk of developing head and neck cancers, especially of the mouth and throat, at a young age.
Mouthwash
Some studies have suggested that mouthwash with a high alcohol content might be linked to a higher risk of oral and oropharyngeal cancers. But recent research has questioned these results. Studying this possible link is complicated by the fact that people who smoke and frequent drinkers (who already have an increased risk of these cancers) are more likely to use mouthwash than people who neither smoke nor drink.
Irritation from dentures
It’s been suggested that long-term irritation of the lining of the mouth caused by poorly fitting dentures is a risk factor for oral cancer. But many studies have found no increased risk in denture wearers overall.
Poorly fitting dentures can tend to trap agents that have been proven to cause oral cancer, such as alcohol and tobacco particles, so denture wearers should have them checked by a dentist regularly to ensure a good fit. All denture wearers should remove their dentures at night and clean and rinse them thoroughly every day.
Poor oral health
As cancer is sometimes linked with long-standing wounds, there’s a small chance that jagged, broken teeth, which cause persistent ulcers or wounds on the tongue, can increase the chance of mouth cancer developing there. Studies have also suggested the overall health of the mouth, teeth, and gums may impact oral cavity and oropharyngeal cancer risk because of changes in the normal bacteria in the mouth. Poor oral hygiene, which can lead to tooth loss, may also be linked to these cancers. Overall survival may also be affected. More research is needed, but regular dental visits, as well as brushing and flossing, may lessen these risks and have many other health benefits, too.
Drinking very hot beverages
Some studies found that people who drink very hot beverages may have a higher risk for oral cancer. The hot beverage may cause damage to the cells in the mouth, which may develop into a cancer.
Lichen planus
Lichen planus is a chronic condition that forms a rash or sores on the skin and inside the mouth, usually on the tongue, gums and lining of the cheeks. Sometimes the sores can develop into ulcers. Having lichen planus with ulcers in the mouth for a long time increases the risk of developing oral cancer.
Oral cancer prevention
Not all cases of oral cavity (mouth) and oropharyngeal (middle throat) cancer can be prevented, but the risk of developing these cancers can be greatly reduced if you take steps to avoid certain risk factors.
Avoid tobacco and alcohol
Use of tobacco and alcohol are among the most important risk factors for these cancers. Not starting to smoke or use oral tobacco products is the best way to limit the risk of getting these cancers. Quitting tobacco also greatly lowers your risk of developing these cancers, even after many years of use. Heavy alcohol use is a risk factor on its own. It also greatly increases the cancer-causing effect of tobacco. So it’s especially important to avoid smoking and alcohol as well as the combination of alcohol and smoking.
Avoid HPV infection or get the HPV vaccine
The risk of human papillomavirus (HPV) infection of the mouth and middle throat is increased in those who have oral sex and multiple sex partners. These infections are also more common in people who smoke, which may be because the smoke damages their immune system or the cells that line the mouth and throat.
HPV is very common and rarely causes symptoms. And even though HPV infection is linked to most cases of oropharyngeal cancer, most people with HPV infections of the mouth and throat do not go on to develop this cancer.
Vaccines that reduce the risk of infection with certain types of HPV are available. These vaccines were originally meant to lower the risk of cervical cancer, but they have been shown to lower the risk of other cancers linked to HPV, such as cancers of the penis, anus, vulva, vagina, and mouth and throat.
Since these vaccines are most effective if given before someone is infected with HPV, they’re recommended to be given when a person is young, before they’re likely to become sexually active. But certain adults can also get the HPV vaccine.
Limit exposure to ultraviolet (UV) light
Ultraviolet radiation is an important and avoidable risk factor for cancer of the lips, as well as for skin cancer. If possible, limit the time you spend outdoors during the middle of the day, when the sun’s UV rays are strongest. If you are out in the sun, wear a wide-brimmed hat and use sunscreen and lip balm with a sun protection factor (SPF) of at least 30+.
Maintain a healthy weight and eating pattern
Poor nutrition and excess body weight have been linked to oral cavity and oropharyngeal cancers. Following a healthy eating pattern with more plant-based foods, such as non-starchy vegetables and whole fruit may help lower your risk of these cancers (and many others).
The American Cancer Society recommends following a healthy eating pattern that includes plenty of fruits, vegetables, and whole grains, and that limits or avoids red and processed meats, sugary drinks, and highly processed foods. In general, eating a healthy diet is much better than adding vitamin supplements to an otherwise unhealthy diet.
Get regular dental checkups
Areas of leukoplakia or erythroplakia (pre-cancer growths) in the mouth sometimes turn into cancer. Doctors often remove these areas, especially if a biopsy shows they contain areas of dysplasia (abnormal growth) when looked at closely in the lab.
But removing areas of leukoplakia or erythroplakia doesn’t always keep someone from getting oral cavity cancer. Studies have found that even when these areas are completely removed, people with certain types of erythroplakia and leukoplakia still have a higher chance of developing a cancer in some other area of their mouth. This may be because the whole lining of the mouth has probably been exposed to the same cancer-causing agents that led to these pre-cancers (like tobacco). This means that the entire area may already have early changes that can lead to cancer.
It’s important for people who have had these areas removed to continue having check-ups to look for cancer and new areas of leukoplakia or erythroplakia.
If you wear dentures, make sure they fit properly. Avoiding sources of oral irritation (such as dentures that don’t fit properly) may help lower your risk for oral cancer.
Oral cancer screening
There’s no routine screening test or program for oral cavity and oropharyngeal cancers 35. Some dentists and doctors recommend that you look at your mouth in a mirror every month to check for any changes, like white patches (leukoplakia), sores, or lumps. This is very important if you use or have used tobacco, and/or if you routinely drink alcohol, as these put you at much higher risk for these cancers.
Regular dental check-ups that include an exam of the entire mouth are also important in finding oral and oropharyngeal cancers (and pre-cancers) early.
Along with a clinical exam of the mouth and throat, some dentists and doctors may use special dyes and/or lights to look for abnormal areas, especially if you are at higher risk for these cancers. If an abnormal area is spotted, tests might also be used to help decide if they might be cancer (and need to be biopsied) or to choose the best spot to take tissue from for a biopsy.
Here are some of the tests used most often:
- One method uses a dye called toluidine blue. If the dye is spread over an abnormal area, it will turn a darker blue than the areas around it.
- Another method uses fluorescent light. When the light is reflected off abnormal tissue, it looks different from the light reflected off normal tissue.
If an abnormal area is found, sometimes it can be tested by exfoliative cytology. To do this, the abnormal area is scraped with a stiff brush (brush biopsy). The cells from the scraping are sent to a lab where they are checked to see if there are pre-cancer or cancer cells.
And even though HPV is a risk factor for oropharyngeal cancers, there is no approved test to screen for HPV in the throat like there is for cervical cancer.
Oral cancer diagnosis
If you have symptoms of mouth cancer, a doctor or dentist will do a physical examination and ask about your symptoms. Early detection can boost your chance of survival from 50% to 90%. This is why you should report any symptoms to your dentist or doctor if they do not get better after 2 weeks. If mouth cancer is suspected, you’ll be referred to specialists for further tests. These specialists are oral and maxillofacial surgeons or head and neck surgeons. They are also known as ear, nose, and throat (ENT) doctors or otolaryngologists.
Tests to find oral cavity or oropharyngeal cancer
Your doctor or dentist will ask you about symptoms, possible risk factors, and any other medical problems you may have.
Your doctor or dentist will look for possible signs of mouth or throat cancer or pre-cancer. These could be bumps or other changed areas on your head, face or neck, or problems with the nerves of the face and mouth. The doctor will look at the entire inside of your mouth, and might feel around in it with a gloved finger. Other tests might be used to look for abnormal areas in your mouth or throat.
Complete head and neck exam
If there is a reason to think you might have cancer, your doctor will refer you to a specialist. The specialist will most likely do a complete head and neck exam, as well as order other exams and tests.
The specialist will pay special attention to the head and neck area, being sure to look and feel for any abnormal areas. This exam will include the lymph nodes in your neck, which will be felt carefully for any swelling.
Because the oropharynx is deep inside the neck, some parts are not easy to see. The doctor may use mirrors or special fiber-optic scopes to look at these areas. Both of these exams can be done in the doctor’s office. The doctor may first spray the back of your throat with numbing medicine to help make the exam easier.
- Indirect pharyngoscopy and laryngoscopy: Small mirrors on long, thin handles are used to look at your throat, the base of your tongue, and part of the larynx (voice box).
- Direct (flexible) pharyngoscopy and laryngoscopy: A flexible fiber-optic scope (called an endoscope) is put in through your mouth or nose to look at areas that can’t easily be seen with mirrors. It can get a clearer look at areas of change that were seen with the mirrors and also the part behind the nose (nasopharynx) and the larynx (voice box).
Panendoscopy
Since tobacco and alcohol use are risk factors for oral cavity and oropharyngeal cancers, as well as cancers of the esophagus and lung, there is a chance (up to 10%) of finding more than one cancer at the same time. To make sure there are no other cancers in the esophagus or lung, a panendoscopy might be done. This procedure is also helpful if it is unclear where the cancer started or if the lymph nodes in the bottom part of the neck seem abnormal.
During a panendoscopy, the doctor uses different types of endoscopes passed down the mouth or nose to do a laryngoscopy/pharyngoscopy, esophagoscopy, and (at times) bronchoscopy. This lets the doctor thoroughly examine the oral cavity, oropharynx, larynx (voice box), esophagus (tube leading to the stomach), and the trachea (windpipe) and bronchi (breathing passages in the lungs).
This exam is usually done in an operating room while you are asleep under general anesthesia. The doctor uses a laryngoscope to look for tumors in the throat and voice box. Other parts of your mouth, nose, and throat are examined, too. The doctor might also use an esophagoscope to look into the esophagus or a bronchoscope to look into the trachea (windpipe) and bronchi.
Your doctor will look at these areas through the scopes to find any tumors, see how big they are, and see how far they might have spread to nearby areas. A small piece of tissue from any tumors or other abnormal areas might be taken out to be looked at closely (biopsied) to see if they contain cancer. Biopsies can be done with special tools that are used through the scopes.
Nasendoscopy
A nasendoscope is a long, thin, flexible tube with a camera and a light at one end. It’s guided through the nose and into the throat. Nasendoscopy is usually used if the suspected cancer is inside your nose, throat (pharynx) or voice box (larynx). A nasendoscopy takes about 30 seconds. Local anaesthetic may be sprayed into your nose and throat first, to reduce any discomfort.
Occasionally, tissue may be taken using a telescopic punch biopsy.
Biopsy
In a biopsy, the doctor removes a small piece of tissue or a sample of cells, so it can be looked at closely in the lab for cancer cells. A biopsy is the only way to know for sure that oral cavity or oropharyngeal cancer is present. A sample of tissue or cells is always needed to confirm a cancer diagnosis before treatment is started. Several types of biopsies may be used, depending on each case.
Exfoliative cytology
For exfoliative cytology, the doctor scrapes the changed area and smears the collected tissue onto a glass slide. The sample is then stained with a dye so the cells can be seen clearly. If any of the cells look abnormal, the area can then be biopsied.
The advantage of this test is that it’s easy to do and causes very little pain. This can lead to an earlier diagnosis and a greater chance of treatment being successful if cancer is found. But this method doesn’t show all cancers. And sometimes it’s not possible to tell the difference between cancer cells and abnormal cells that aren’t cancer (such as dysplasia), so a different type of biopsy would still be needed.
Incisional biopsy
For an incisional biopsy, a small piece of tissue is cut from the area that looks abnormal. This is the most common type of biopsy used to check changes in the mouth or throat.
The biopsy can be done either in the doctor’s office or in the operating room, depending on where the tumor is and how easy it is to get a good tissue sample. If it can be done in the doctor’s office, the area around the tumor will be numbed before the biopsy is done. If the tumor is deep inside the mouth or throat, the biopsy might be done in the operating room while you are in a deep sleep under general anesthesia.
Fine needle aspiration (FNA) biopsy
For a fine needle aspiration (FNA) biopsy, a very thin, hollow needle attached to a syringe pulls out (aspirates) some cells from a tumor or lump. These cells are then looked at closely in the lab to see if cancer is present.
FNA biopsy is not used to sample abnormal areas in the mouth or throat, but it’s sometimes used for a neck lump (mass) that can be felt or seen on a CT scan. FNA can be helpful in some situations, such as:
- Finding the cause of a new neck mass: An FNA biopsy is sometimes used as the first test for someone with a newly found lump in the neck. It may show that the lump is a benign (not cancer) lymph node that has grown because of a nearby infection, such as a sinus or tooth infection. In this case, treatment of the infection is all that’s needed. Or the FNA may find a benign, fluid-filled cyst that can be cured by surgery. But even when the FNA results are benign, if other symptoms suggest cancer, more tests (such as pharyngoscopy and panendoscopy) are needed. If the FNA sample has cancer cells, the doctor looking at the biopsy sample can usually tell what type of cancer it is. If the cells look like a squamous cell cancer, more exams will be done to search for the source of the cancer in the mouth and throat. If the FNA shows a different type of cancer, such as lymphoma or a cancer that has spread to a lymph node in the neck from another organ (like the thyroid or lungs) more tests will be done to find it, and treatment for that type of cancer will be given.
- Learning how far a diagnosed cancer has spread: FNA also might be done after oral or oropharyngeal cancer has been diagnosed to find out if the cancer has spread to lymph nodes in the neck. This information will help the doctor decide the best treatment for the cancer.
- Seeing if cancer has come back after treatment: FNA might be used for people whose cancer has been treated by surgery and/or radiation therapy, to find out if a new neck mass in the treated area is scar tissue or cancer that has come back.
Lab tests of biopsy samples
All biopsy samples are sent to a lab to be checked closely by a pathologist, a doctor who is specially trained to diagnose cancer from a biopsy. The doctor can usually tell cancer cells from normal cells, as well as what type of cancer it is, by the way the cells look. In some cases, the doctor may need to test the cells with special stains to help find out what type of cancer it is.
HPV (p16) testing
For cancers of the throat, the biopsy samples are often tested (for the p16 protein) to see if HPV infection is present. This is a key part of staging (finding out if and how much the cancer has spread) and is considered when making treatment decisions for oropharyngeal cancer. This information can also help the doctor predict the probable course of the cancer, because people whose cancers are linked to HPV tend to do better than those whose cancers are not.
Imaging tests
Imaging tests are not used to diagnose oral cavity or oropharyngeal cancers, but they may be done for a number of reasons before and after a cancer diagnosis, including:
- To look at a suspicious area that might be cancer
- To learn how far cancer might have spread
- To help find out if treatment is working
- To look for signs that the cancer has come back (recurred) after treatment
Chest x-ray
An x-ray of your chest might be done after oral cavity or oropharyngeal cancer has been diagnosed to see if the cancer has spread to the lungs. More often though, a CT scan or PET/CT scan of the lungs is done since they tend to give more detailed pictures.
Computed tomography (CT or CAT scan)
A CT scan uses x-rays to make detailed, cross-sectional images of your body. It can help your doctor see the size and location of a tumor, if it’s growing into nearby tissues, if it has spread to lymph nodes in the neck, or to the lungs or other distant organs.
CT-guided needle biopsy: If a lung biopsy is needed to check for cancer spread, this test can also be used to guide a biopsy needle into the mass (lump) to get a tissue sample to check for cancer.
Magnetic resonance imaging (MRI)
Like CT scans, MRI scans show detailed images of soft tissues in the body. But MRI scans use radio waves and strong magnets instead of x-rays. A contrast material called gadolinium may be injected into a vein before the scan to get clear pictures. An MRI scan may be done for oral cavity cancer if there are a lot of dental fillings that might distort the CT pictures or to look closely if the cancer is growing into the bone marrow.
Positron emission tomography (PET) scan
For a PET scan, a slightly radioactive form of sugar (known as FDG) is injected into the blood and collects mainly in cancer cells.
PET/CT scan: Often a PET scan is combined with a CT scan using a special machine that can do both scans at the same time. This lets the doctor compare areas of higher radioactivity on the PET with the more detailed picture on the CT scan.
PET/CT scans can be useful:
- If your doctor thinks the cancer might have spread but doesn’t know where. They can show spread of cancer to the liver, bones, and some other organs.
- In follow up of patients after oral cavity or oropharyngeal cancer treatment.
Bone scan
For a bone scan, a small amount of low-level radioactive material is injected into the blood and collects mainly in abnormal areas of bone. A bone scan can help show if a cancer has spread to the bones. But this test isn’t needed very often because PET scans can usually show if cancer has spread to the bones.
Barium swallow
A barium swallow can be used to see the lining of the upper part of the digestive system, especially the esophagus (the tube that connects the throat to the stomach). In this test, you drink a chalky liquid called barium which coats the walls of your throat and esophagus. A series of x-rays is taken as you swallow. Your doctor may order this test because people with oral and oropharyngeal cancers are at risk for cancer of the esophagus. It’s also useful to see if the cancer is causing problems with swallowing.
Ultrasound
An ultrasound uses sound waves and their echoes to create images of the inside of the body. A small microphone-like instrument called a transducer gives off sound waves and picks up the echoes as they bounce off organs. The echoes are converted by a computer into an image on a screen.
Neck ultrasound: For this exam, a technician moves the transducer along the skin over your neck. This type of ultrasound can be used to look for lymph nodes in the neck to see if they are swollen or if they look abnormal inside which could be signs of cancer. The ultrasound can help guide a needle into the abnormal lymph node for an FNA biopsy. It might also be used after treatment to look for signs of cancer coming back (recurrence).
Pre-treatment tests for oral cavity or oropharyngeal cancer
Other tests might be done as part of a work-up if a patient has been diagnosed with oral cavity or oropharyngeal cancer. These tests are not used to diagnose the cancer, but they may be done for other reasons, such as to see if a person is healthy enough for treatments such as surgery, radiation therapy, or chemotherapy.
Blood tests
No blood test can diagnose cancer in the oral cavity or oropharynx. Still, your doctor may order routine blood tests to get an idea of your overall health, especially before treatment. Such tests can help diagnose poor nutrition and low blood cell counts. A complete blood count (CBC) looks at whether your blood has normal amounts of different types of blood cells. For example, it can show if you are anemic (have a low number of red blood cells). Blood chemistry tests can help determine how well your liver or kidneys are working.
Function tests before surgery
If surgery is planned, you might also have an electrocardiogram (EKG) to make sure your heart is working well. Some people having surgery also may need breathing tests, called pulmonary (lung) function tests.
Dental exam before radiation treatment
If radiation therapy will be part of the treatment, you’ll be asked to see a dentist before starting. The dentist will help with routine dental care and may remove any bad teeth, if needed, before radiation treatment is started. Radiation can damage the saliva (spit) glands and cause dry mouth. This can increase the chance of cavities, infection, and breakdown of the jawbone.
If the cancer is in your jaw or the roof of your mouth, a dentist with special training (called a prosthodontist) might be asked to evaluate you. This dentist can make replacements for missing teeth or other structures of the oral cavity to help restore your appearance; comfort; and ability to chew, swallow, and speak after treatment. If part of the jaw or roof of the mouth (palate) will be removed with the tumor, the prosthodontist will work to ensure that the replacement artificial teeth and the remaining natural teeth fit together correctly. This can be done with dentures, other types of prostheses, or dental implants.
Hearing tests
Cisplatin, the main chemotherapy drug used in treating oral cavity and oropharyngeal cancer can cause hearing loss. Your care team will most likely have your hearing checked (with an audiogram) before starting treatment to compare to later if you happen to have hearing problems from chemo.
Nutrition and speech tests
Often, you will have a nutritionist who will evaluate your nutrition status before, during, and after your treatment to try and keep your weight and protein stores as normal as possible. You might also visit a speech therapist who will test your ability to swallow and speak. They might give you exercises to do during treatment to help strengthen the muscles in the head and neck area so you can eat and talk easily after treatment.
Oral cancer stages
After someone is diagnosed with oral cavity or oropharyngeal cancer, doctors will try to figure out if it has spread, and if so, how far. This process is called staging. The stage of a cancer describes how much cancer is in the body. It helps determine how serious the cancer is and how best to treat it. Doctors also use a cancer’s stage when talking about survival statistics.
The staging system most often used for oral cavity or oropharyngeal cancers is the American Joint Committee on Cancer (AJCC) TNM system, which is based on 3 key pieces of information:
- The extent of the tumor (T): How large is the main (primary) tumor and which, if any, tissues of the oral cavity or oropharynx it has spread to?
- The spread to nearby lymph nodes (N): Has the cancer spread to nearby lymph nodes? If so, how many , are they on the same side where the cancer started, and how large are they?
- The spread (metastasis) to distant sites (M): Has the cancer spread to distant organs such as the lungs?
Numbers or letters after T, N, and M provide more details about each of these factors. Higher numbers mean the cancer is more advanced. Once a person’s T, N, and M categories have been determined, this information is combined in a process called stage grouping to assign an overall stage.
The earliest stage oral cavity or oropharyngeal cancers are called stage 0 (carcinoma in situ). Stages then range from I (1) through IV (4). As a rule, the lower the number, the less the cancer has spread. A higher number, such as stage IV, means cancer has spread more. And within a stage, an earlier letter means a lower stage. Although each person’s cancer experience is unique, cancers with similar stages tend to have a similar outlook and are often treated in much the same way.
The staging system in the table below is based on the most recent AJCC system, effective January 2018. It uses the pathologic stage (also called the surgical stage). Pathological staging or surgical staging means the doctor stages you after examining the tissue that the surgeon removes during an operation. Sometimes, if surgery isn’t possible right away or at all, the cancer will be given a clinical stage instead (which is not shown below). Clinical staging is based on the results of a physical exam, endoscopy exam, biopsy, and imaging tests. The clinical stage will be used to help plan treatment. Sometimes, though, the cancer has spread further than the clinical stage estimates, and it may not predict the patient’s outlook as accurately as a pathologic stage.
Oropharyngeal cancers that contain HPV DNA (called p16-positive) tend to have a better outlook than those without HPV (p16-negative). Because p16-positive cancers have a better prognosis than p16-negative oropharyngeal cancers, separate staging systems are used. Both systems are described below.
Cancer staging can be complex, so ask your doctor to explain it to you in a way you understand.
Table 1. Lip, oral cavity, and p16 (HPV)-negative oropharynx cancer stages
| American Joint Committee on Cancer (AJCC) stage | Stage grouping | Lip, oral cavity and p16 (HPV)-negative oropharynx cancer stage description* (2 cm = about ¾ inch; 3 cm = about 1¼ ; 4 cm = about 1½) |
|---|---|---|
| 0 | Tis N0 M0 | The cancer is still within the epithelium (the top layer of cells lining the oral cavity and oropharynx) and has not yet grown into deeper layers. It has not spread to nearby lymph nodes (N0) or distant sites (M0). This stage is also known as carcinoma in situ (Tis). |
| 1 | T1 N0 M0 | The cancer is 2 cm or smaller. It’s not growing into nearby tissues (T1). It has not spread to nearby lymph nodes (N0) or to distant sites (M0). |
| 2 | T2 N0 M0 | The cancer is larger than 2 cm but no larger than 4 cm . It’s not growing into nearby tissues (T2). It has not spread to nearby lymph nodes (N0) or to distant sites (M0). |
| 3 | T3 N0 M0 | The cancer is larger than 4 cm (T3). For cancers of the oropharynx, T3 also includes tumors that are growing into the epiglottis (the base of the tongue). It has not spread to nearby lymph nodes (N0) or to distant sites (M0). |
| OR | ||
| T1, T2, T3 N1 M0 | The cancer is any size and may have grown into nearby structures if oropharynx cancer(T1-T3) AND has spread to 1 lymph node on the same side as the primary tumor. The cancer has not grown outside of the lymph node and the lymph node is no larger than 3 cm (N1). It has not spread to distant sites (M0). | |
| 4A | T4a N0 or N1 M0 | The cancer is any size and is growing into nearby structures such as: For lip cancers: nearby bone, the inferior alveolar nerve (the nerve to the jawbone), the floor of the mouth, or the skin of the chin or nose (T4a) For oral cavity cancers: the bones of the jaw or face, deep muscle of the tongue, skin of the face, or the maxillary sinus (T4a) For oropharyngeal cancers: the larynx (voice box), the tongue muscle, or bones such as the medial pterygoid, the hard palate, or the jaw (T4a). This is known as moderately advanced local disease (T4a). AND either of the following: It has not spread to nearby lymph nodes (N0) It has spread to 1 lymph node on the same side as the primary tumor, but has not grown outside of the lymph node and the lymph node is no larger than 3 cm (N1). It has not spread to distant sites (M0). |
| OR | ||
| T1, T2, T3 or T4a N2 M0 | The cancer is any size and may have grown into nearby structures (T0-T4a). It has not spread to distant organs (M0). It has spread to one of the following: One lymph node on the same side as the primary tumor, but it has not grown outside of the lymph node and the lymph node is larger than 3 cm but not larger than 6 cm (about 2½ inches) (N2a) OR It has spread to more than 1 lymph node on the same side as the primary tumor, but it has not grown outside any of the lymph nodes and none are larger than 6 cm (N2b) OR It has spread to 1 or more lymph nodes either on the opposite side of the primary tumor or on both sides of the neck, but has not grown outside any of the lymph nodes and none are larger than 6 cm (N2c). | |
| 4B | Any T N3 M0 | The cancer is any size and may have grown into nearby soft tissues or structures (Any T) AND any of the following: It has spread to 1 lymph node that’s larger than 6 cm but has not grown outside of the lymph node (N3a) OR It has spread to 1 lymph node that’s larger than 3 cm and has clearly grown outside the lymph node (N3b) OR It has spread to more than 1 lymph node on the same side, the opposite side, or both sides of the primary cancer with growth outside of the lymph node(s) (N3b) OR It has spread to 1 lymph node on the opposite side of the primary cancer that’s 3 cm or smaller and has grown outside of the lymph node (N3b). It has not spread to distant organs (M0). |
| OR | ||
| T4b Any N M0 | The cancer is any size and is growing into nearby structures such as the base of the skull or other bones nearby, or it surrounds the carotid artery. This is known as very advanced local disease (T4b). It might or might not have spread to nearby lymph nodes (Any N). It has not spread to distant organs (M0). | |
| 4C | Any T Any N M1 | The cancer is any size and may have grown into nearby soft tissues or structures (Any T) AND it might or might not have spread to nearby lymph nodes (Any N). It has spread to distant sites such as the lungs (M1). |
Footnotes: * The following additional categories are not described in the table above:
- TX: Main tumor cannot be assessed due to lack of information.
- T0: No evidence of a primary tumor.
- NX: Regional lymph nodes cannot be assessed due to lack of information.
Table 2. p16 (HPV)-positive oropharynx cancer stages
| American Joint Committee on Cancer (AJCC) stage | Stage grouping | p16 (HPV)-positive oropharynx cancer stage description* (2 cm = about ¾ inch; 4 cm = about 1½; 6 cm = about 2½ inches) |
|---|---|---|
| 1 | T0, T1 or T2 N0 or N1 M0 | The cancer is no larger than 4 cm (T0 to T2) AND any of the following: It has not spread to nearby lymph nodes (N0) OR It has spread to 1 or more lymph nodes on the same side as the primary cancer, and none are larger than 6 cm (N1). It has not spread to distant sites (M0). |
| 2 | T0, T1 or T2 N2 M0 | The cancer is no larger than 4 cm (T0 to T2) AND it has spread to 1 or more lymph nodes on the opposite side of the primary cancer or both sides of the neck, and none are larger than 6 cm (N2). It has not spread to distant sites (M0). |
| OR | ||
| T3 or T4 N0 or N1 M0 | The cancer is larger than 4 cm (T3) OR is growing into the epiglottis (the base of the tongue) (T3) OR is growing into the larynx (voice box), the tongue muscle, or bones such as the medial pterygoid plate, the hard palate, or the jaw (T4) AND any of the following: It has not spread to nearby lymph nodes (N0) OR It has spread to 1 or more lymph nodes on the same side as the primary cancer, and none are larger than 6 cm (N1). It has not spread to distant sites (M0). | |
| 3 | T3 or T4 N2 M0 | The cancer is larger than 4 cm (T3) OR is growing into the epiglottis (the base of the tongue) (T3) OR is growing into the larynx (voice box), the tongue muscle, or bones such as the medial pterygoid plate, the hard palate, or the jaw (T4) AND it has spread to 1 or more lymph nodes on the opposite side of the primary cancer or both sides of the neck, and none are larger than 6 cm (N2). It has not spread to distant sites (M0). |
| 4 | Any T Any N M1 | The cancer is any size and may have grown into nearby structures (Any T) AND it might or might not have spread to nearby lymph nodes (Any N). It has spread to distant sites such as the lungs or bones (M1). |
Footnotes: * The following additional categories are not described in the table above:
- TX: Main tumor cannot be assessed due to lack of information.
- T0: No evidence of a primary tumor.
- NX: Regional lymph nodes cannot be assessed due to lack of information.
Stage 0 or carcinoma in situ (CIS)
Stage 0 cancer or carcinoma in situ (CIS) means your cancer is at a very early stage. Some doctors prefer to call this pre cancer. There are cancer cells but they are all contained within the lining of the mouth. The cancer cells have not spread.
If the pre cancer is not treated, there is a high risk the condition will develop into an invasive cancer.
Stage 1 oral cancer
Stage 1 oral cancer is the earliest stage of invasive cancer. Stage 1 mouth cancer means the cancer is 2cm or smaller and it is 5mm deep or less. It has not spread to nearby tissues, lymph nodes or other organs.
In the TNM staging system stage 1 mouth cancer is the same as T1, N0, M0.
Stage 2 oral cancer
Stage 2 oral cancer can mean different things including:
- the cancer is 2 cm or smaller, and it is deeper than 5 mm but no deeper than 10 mm
- the cancer is larger than 2 cm but no larger than 4 cm, and it is 10 mm deep or less
Stage 2 oral cancer has not spread to nearby lymph nodes or other organs.
In the TNM staging system stage 2 mouth cancer is the same as T2, N0, M0
Stage 3 oral cancer
Stage 3 oral cancer means one of the following;
- the cancer is larger than 2 cm but no larger than 4cm and deeper than 10mm and it has not spread to any lymph nodes or other parts of the body
- or the cancer is larger than 4cm, but no deeper than 10mm, and has not spread to any lymph nodes or to other parts of the body
- the cancer is any size but one lymph node contains cancer cells on the same side of the neck as the cancer, and the lymph node is no more than 3cm across
In the TNM staging system stage 3 mouth cancer is the same as one of the following:
- T3, N0, M0
- T1,2 or 3, N1, M0
Stage 4 oral cancer
Stage 4 oral cancer means the cancer is advanced. It is further divided into 3 stages – 4A, 4B and 4C.
Stage 4A mouth cancer can mean different things:
- It can mean that the cancer has grown further than the mouth into surrounding structures. It may also have spread into 1 lymph node which is no larger than 3cm.
- Or, it can mean that the cancer is any size. But it has spread into one or more lymph nodes on either side of the neck. The lymph nodes are between 3 and 6cm in size.
Stage 4B mouth cancer can mean different things, including:
- cancer has spread into nearby areas such as the space behind the jaw, the base of the skull, or the area of neck surrounding the arteries (carotid arteries)
- a lymph node containing cancer is larger than 6cm
- cancer has spread into tissues surrounding the lymph node
In the TNM staging system stage 4b mouth cancer is the same as one of the following:
- any T, N3, M0
- T4b, any N, M0
Stage 4C mouth cancer means the cancer has spread to other parts of the body such as the lungs or bones. In the TNM staging system stage 4c mouth cancer means any T, any N, M1.
Recurrent oral cancer
Recurrent oral cancer means that the cancer has come back after it has been treated. If it comes back in the same place that the cancer first started, it’s called local recurrence. If it comes back in tissues or lymph nodes close to where it first started, it’s called regional recurrence. It can also recur in another part of the body. This is called distant metastasis or distant recurrence.
Mouth cancer grades
Grading describes how the cancer cells look compared to normal, healthy cells. Knowing the grade gives your healthcare team an idea of how quickly the cancer may be growing and how likely it is to spread. To find out the grade of oral cancer, a pathologist looks at a tissue sample from the mouth under a microscope. They look at how different the cells look from normal cells (called differentiation) and other features of the tumour such as the size and shape of the cells and how the cells are arranged. They can usually tell how fast a tumour is growing by looking at how many cells are dividing.
The pathologist gives oral cancer a grade from 1 to 3. A lower number means the cancer is a lower grade.
There are 3 grades of mouth cancer:
- Grade 1 (low grade) means cancer cells look like normal mouth cells
- Grade 2 (intermediate grade) look slightly different to normal mouth cells
- Grade 3 (high grade) look very abnormal and not much like normal mouth cells
Your cancer might be graded as Gx. This means that the grade cannot be assessed.
Differentiation
Differentiation means how developed or mature a cell is. Doctors might describe cancer as poorly or well differentiated.
Doctors might describe:
- Grade 1 cancer as well differentiated
- Grade 2 cancer cells are moderately differentiated
- Grade 3 cancer cells are poorly differentiated
Oral cancer treatment
If you have oral cancer, your healthcare team will create a treatment plan just for you. It will be based on your health and specific information about the cancer. When deciding which treatments to offer for oral cancer, your healthcare team will consider:
- the size of the cancer
- the stage of the cancer
- the location of the cancer
- your overall health and ability to recover from surgery, radiation therapy or chemotherapy
- how a treatment will affect appearance and function (such as your speech and ability to swallow and chew)
- your personal preferences
The main treatment options for people with oral cavity and oropharyngeal cancers are:
- Surgery
- Radiation Therapy
- Chemotherapy
- Targeted Therapy
- Immunotherapy
- Palliative care
Your healthcare team may include a number of healthcare professionals with special training in treating people with oral cancer, including:
- head and neck surgeon (also called an otolaryngologist or ear, nose and throat (ENT) doctor) (specializes in surgery of the mouth, jaw, face and neck)
- head and neck reconstructive surgeon (specializes in reconstruction around the head and neck and facial plastic surgery)
- oral and maxillofacial surgeon (specializes in surgery of the mouth, jaw and face)
- medical oncologist (specializes in treating cancer with drugs)
- radiation oncologist (specializes in treating cancer with radiation therapy)
- maxillofacial prosthodontist (specializes in replacing lost head and neck tissues and teeth with prosthetics)
- dentist
- speech therapist (speech-language pathologist)
- registered dietitian
- social worker
Oral cancer can make it difficult to eat, so you may not eat enough and you may lose weight. Before you start treatment, a dietitian may do a nutritional assessment to see how oral cancer has affected your nutrition. If you aren’t getting good enough nutrition, you may need to have a feeding tube placed before you start treatment. This is to make sure you get enough nutrition to maintain your weight and strength during treatment.
It is important to assess if and how oral cancer has affected your speech. You will often see a speech therapist when you are first diagnosed and throughout your treatment to help manage any speech problems you may have as a result of oral cancer or its treatment.
It is also important to have a complete dental exam as you may need dental work done before treatment can start.
If you are a smoker, your healthcare team will talk to you about how they can help you quit. Smoking can limit how well your cancer treatment works, so it is important to quit before you start treatment.
Oral cancer is usually treated with surgery first. Surgery may be followed with radiation therapy or sometimes radiation therapy and chemotherapy. Reconstruction may be needed to repair structures in the mouth and jaw or to help with speech and swallowing. Reconstruction is planned at the same time as treatment. It is important for the healthcare team involved in reconstruction to assess and talk to you about what your expectations are before any surgery or other treatments are done.
Surgery for oral cavity and oropharyngeal cancer
Surgery is often the first treatment used for these cancers. Several types of operations can be done to treat oral cavity and oropharyngeal cancers, depending on where the cancer is located and its stage. It’s most commonly used for small, early-stage cancers that haven’t spread.
After the cancer is removed, reconstructive surgery might be done to help restore the appearance and function of the areas affected by the cancer or cancer treatment.
Studies have shown that people with head and neck cancer who are treated at facilities that perform a lot of head and neck cancer surgeries, tend to live longer. Because of this and the complex nature of these operations, it’s very important to have a surgeon and cancer center who has experience treating these cancers.
Tumor resection
In a tumor resection, the entire tumor and a margin (edge) of normal-looking tissue around it is removed (resected). The margin of normal tissue is taken out to reduce the chance of any cancer cells being left behind.
The main (primary) tumor is removed using a method based on its size and location. For example, if a tumor is in the front of the mouth, it might be relatively easy to remove it through the mouth. But a larger tumor (especially when it has grown into the oropharynx) may need to be removed through an incision (cut) in the neck or by cutting the jaw bone with a special saw to get to the tumor. This is called a mandibulotomy.
Based on the location and size of the tumor, one of the operations listed here may be done to remove it:
Mohs micrographic surgery (for some cancers of the lip)
Some cancers of the lip, such as those at the very edge of the lip, may be removed by Mohs surgery, also known as micrographic surgery. The tumor is removed in very thin slices. Each slice is looked at right away under the microscope to see if it has cancer cells. Slices are removed and examined until no cancer cells are seen.
With this method, the amount of normal tissue removed with the tumor is reduced and the change in appearance caused by the surgery is limited. It requires a surgeon trained in the technique and may take more time than a standard tumor resection.
Glossectomy (removal of the tongue)
Glossectomy may be needed to treat cancer of the tongue. For smaller cancers, only part of the tongue (less than 1/3) may need to be removed (partial glossectomy). For larger cancers, the entire tongue may need to be removed (total glossectomy).
Mandibulectomy (removal of the jaw bone)
For a mandibulectomy (or mandibular resection), the surgeon removes all or part of the jaw bone (mandible). This operation might be needed if the tumor has grown into the jaw bone. If a tumor near the jaw is hard to move when the doctor examines it, it often means that the cancer has grown into the jaw bone.
If the jaw bone looks normal on imaging tests and there’s no evidence the cancer has spread there, the bone may not need to be cut all the way through. In this operation, also known as a partial-thickness mandibular resection or marginal mandibulectomy, the surgeon removes only part or a piece of jaw bone.
If the x-ray shows the tumor has grown into the jaw bone, a large part of the jaw will need to be removed in an operation called a segmental mandibulectomy. The removed piece of the mandible can then be replaced with a piece of bone from another part of the body, such as the lower leg, hip bone, or the shoulder blade. A metal plate or a piece of bone from a deceased donor may also be used to repair the bone.
Maxillectomy
If cancer has grown into the hard palate (front part of the roof of the mouth), all or part of the involved bone (maxilla) will need to be removed. This operation is called a maxillectomy or partial maxillectomy.
This operation makes a hole in the roof of the mouth which can be filled with a special denture called a prosthesis. This is created by a prosthodontist, a dentist with special training. Other options to close this gap include a skin graft or a piece of muscle from the forearm or thigh.
Robotic surgery
More and more, trans-oral robotic surgery (TORS) is being used to remove cancers of the back of the throat and mouth that might otherwise need a mandibulectomy for the surgeon to reach the tumor. The surgeon sits at a control panel in the operating room and with the help of an attached camera moves robotic arms with small tools on them to cut out the tumor.
Because the more standard, open surgeries for throat cancer can result in more extensive operations, newer robotic surgeries may allow surgeons to completely remove throat cancers with fewer side effects. Since these procedures are newer, it’s important to have them done by surgeons and at treatment centers that are experienced in this approach.
Laryngectomy (removal of the voice box)
Very rarely, surgery to remove large tumors at the base of the tongue or oropharynx may require removing tissue that a person needs to swallow normally. As a result, food may enter the windpipe (trachea) and reach the lungs, where it can cause pneumonia. When there’s a high risk of this, the voice box (larynx) may also be removed during the same operation as the one to remove the cancer. Removal of the larynx is called a laryngectomy.
When the voice box is removed, the windpipe is attached to a hole (stoma) made in the skin in the front of the neck. You breathe and cough through this stoma (instead of breathing through the mouth or nose). This is called a tracheostomy or trach.
Losing your voice box will mean that normal speech is no longer possible, but people can learn other ways to speak.
Neck dissection
Cancers of the oral cavity and oropharynx often spread to the lymph nodes in the neck. Removing these lymph nodes (and other nearby tissues) is called a neck dissection or lymph node dissection and is done at the same time as the surgery to remove the main tumor. The goal is to remove lymph nodes proven to contain cancer. Sometimes doctors recommend an elective lymph node dissection. This may be done if there’s no proof that the cancer has spread to the lymph nodes, but there’s a high chance that it has based on tumor size.
In some early-stage mouth and lip cancers, a sentinel lymph node biopsy might be done to test the lymph nodes for cancer before removing them. This should only be done at treatment centers by doctors with a lot of experience in the technique.
There are several types of neck dissection procedures, and they differ in how much tissue is removed from the neck. The amount of tissue removed depends on the primary cancer’s size and how much it has spread to lymph nodes.
In a partial or selective neck dissection only a few lymph nodes are removed.
For a modified radical neck dissection, most lymph nodes on one side of the neck between the jaw bone and collarbone are removed, as well as some muscle and nerve tissue.
In a radical neck dissection, nearly all nodes on one side, as well as even more muscles, nerves, and veins are removed.
The most common side effects of any neck dissection are numbness of the ear, weakness when raising the arm above the head, and weakness of the lower lip. These side effects are caused when nerves that supply these areas are damaged during the operation. After a selective neck dissection, the nerve might only be injured and can heal over time. Nerves heal slowly, but in this case, the weakness of the shoulder and lower lip may go away after a few months. If a nerve is removed as part of a radical neck dissection or because of involvement with tumor, the weakness will be permanent.
After any neck dissection procedure, physical therapy can help improve neck and shoulder movement.
Reconstructive surgery
Operations may be needed to help restore the structure of areas affected by more extensive surgeries to remove the cancer.
For small tumors, the narrow edge of normal tissue removed along with the tumor is usually small enough that reconstructive surgery isn’t needed. But removing larger tumors may cause defects in the mouth, throat, or neck that will need to be repaired. Sometimes a thin slice of skin, taken from the thigh or other area, can be used to repair a small defect. This is called a skin graft.
To repair a larger defect, more tissue may be needed. A piece of muscle with or without skin may be rotated from an area close by, such as the chest (pectoralis major pedicle flap) or upper part of the back (trapezius pedicle flap).
Thanks to advances in microvascular surgery (sewing together small blood vessels under a microscope), there are many more options for reconstructing the oral cavity and oropharynx. Tissue from other areas of the body, such as the intestine, arm muscle, abdominal (belly) muscle, or lower leg bone, may be used to replace parts of the mouth, throat, or jaw bone.
Before you have extensive head and neck surgery, talk to the surgeon about your options for reconstructive surgery.
Surgery to save or restore body function
Tracheostomy
A tracheostomy or trach is a stoma (hole) made through the skin in the front of the neck and attached to the trachea (windpipe). It’s done to help a person breathe. If a lot of swelling is expected in the airway after the cancer is removed, the doctor may want to do a short-term tracheotomy (using a small plastic tube) to allow the person to breathe more easily until the swelling goes down. It stays in place for a short time, and is then removed (or reversed) when it’s no longer needed.
If the cancer is blocking the throat and is too big to remove completely, an opening may be made to connect a lower part of the windpipe to a stoma (hole) in the front of the neck. This is done to bypass the tumor and allow the person to breathe more comfortably. This is called a permanent tracheostomy.
A permanent tracheostomy is also needed after a total laryngectomy.
Feeding tubes
Cancers in the oral cavity and oropharynx may keep you from swallowing enough food to stay well nourished. This can make you weak and make it harder to complete treatment. Sometimes the treatment itself can make it hard to eat enough.
A gastrostomy tube (G-tube) is a feeding tube that’s put through the skin and muscle of your abdomen (belly) and right into your stomach. Sometimes this tube is placed during an operation, but often it’s put in endoscopically. While you are sedated (using drugs to put you in a deep sleep), the doctor puts a long, thin, flexible tube with a camera on the end (an endoscope) down the throat to see inside the stomach. The feeding tube is then guided through the endoscope and to the outside of the body. When the feeding tube is placed through endoscopy, it’s called a percutaneous endoscopic gastrostomy, or PEG tube. Once in place, it can be used to put liquid nutrition right into the stomach. As long as they can still swallow normally, people with these tubes can eat normal food, too.
Percutaneous endoscopic gastrostomy (PEG) tube can be used for as long as needed. Sometimes these tubes are used for a short time to help keep you healthy and fed during treatment. They can be removed when you can eat normally.
If the swallowing problem is likely to be only short-term, another option is to place a nasogastric feeding tube (NG tube). This tube goes in through the nose, down the esophagus, and into the stomach. Again, special liquid nutrients are put in through the tube. Some people dislike having a tube coming out of their nose, and prefer a PEG tube.
In any case, the patient and family are taught how to use the tube. After you go home, home health nurses may visit to make sure you are comfortable with tube feedings.
Dental extraction and implants
When radiation treatment is planned, a dental evaluation must be done. Depending on the radiation plan and condition of your teeth, some or even all of the teeth may need to be removed before radiation can start. The teeth may be removed either by the head and neck surgeon or an oral surgeon. If left in and exposed to radiation, teeth that are broken or infected (abscessed) are very likely to cause problems such as infections and areas of necrosis (bone death) in the jaw.
If part of the jaw bone (mandible) is removed and reconstructed with bone from another part of the body, the surgeon might place dental implants (hardware to which prosthetic teeth can be attached) in the bone. This can be done either at the same time the mandible is reconstructed or at a later date.
Surgery risks and side effects
All surgery carries risk, including blood clots, infections, complications from anesthesia, and pneumonia. These risks are generally low but are higher with more complex operations.
If the surgery is not too complex, the main side effect may be some pain afterward, which can be treated with medicines.
Surgery for cancers that are large or hard to reach may be very complicated, in which case side effects may include infection; wound breakdown; problems with eating, breathing, and speaking; or on very rare occasions death during or shortly after the procedure. Surgery also can be disfiguring, especially if bones in the face or jaw need to be removed. The surgeon’s skill is very important in minimizing these side effects, while removing all of the cancer, so it’s important to choose a surgeon with a lot of experience in these types of cancer.
- Impact of glossectomy: Most people can still speak if only part of the tongue is removed, but they often notice that their speech isn’t as clear as it once was. The tongue is important in swallowing, so this may also be affected. Speech therapy can often help with these problems. When the entire tongue is removed, patients lose the ability to speak and swallow. With reconstructive surgery and a good rehabilitation program including speech therapy, some people may regain the ability to swallow and speak well enough to be understood.
- Impact of laryngectomy: Laryngectomy, the surgery that removes the voice box, leaves a person without the normal means of speech. There are several ways to restore one’s voice. After a laryngectomy, the person breathes through a stoma (tracheostomy) placed in the front of the lower neck. Having a stoma means that the air you breathe in and out will no longer pass through your nose or mouth, which would normally help moisten, warm, and filter the air (removing dust and other particles). The air reaching the lungs will be dryer and cooler. This can irritate the lining of the breathing tubes and cause thick or crusty mucus to build up. It’s important to learn how to take care of your stoma. You will need to use a humidifier over the stoma as much as possible, especially right after the operation, until the airway lining has a chance to adjust to the drier air now reaching it. You will also need to learn how to suction out and clean your stoma to help keep your airway open. Your doctors, nurses, and other health care professionals can teach you how to care for and protect your stoma, which includes precautions to keep water from entering the windpipe while showering or bathing, as well as keeping small particles out of the windpipe.
- Impact of facial bone removal: Some cancers of the head and neck are treated with operations that remove part of the facial bone structure. Because the changes that result are so visible, they can have a major effect on how people view themselves. They can also affect speech and swallowing. It’s important to talk with your doctor about these changes before the surgery. This can help you prepare for them. You can also get an idea about what options might be available afterward. Recent advances in facial prostheses (man-made replacements) and in reconstructive surgery now give many people a more normal look and clearer speech. These things can be a great help to a person’s self-esteem.
Radiation therapy for oral cavity and oropharyngeal cancer
Radiation therapy also called radiotherapy uses high energy waves similar to x-rays to kill cancer cells. You have external beam radiothearpy for mouth and oropharyngeal cancer. External radiotherapy uses a machine outside the body to direct radiation beams at the cancer.
Studies have shown that people who are treated at centers that treat a lot of head and neck cancers with radiation, tend to live longer. And because of the complicated types of surgeries, along with the need for coordination between cancer specialists to make a complete treatment plan, it’s very important to have treatment at cancer centers by radiation oncologists who have experience in treating these cancers.
Depending on the stage of the oral cavity or oropharyngeal cancer and other factors, radiation therapy might be used:
- Alone as the main treatment for small cancers or for people who can’t have surgery.
- After surgery (adjuvant therapy), either alone or with chemotherapy (chemoradiation), to try to kill any cancer cells that might have been left behind because they were too small to be seen with the naked eye during surgery. Radiation after surgery can also help lower the chance the cancer will come back in the same spot.
- Before surgery (neoadjuvant therapy) with chemotherapy (chemoradiation) or after chemotherapy to try to shrink some larger cancers. In some cases, this might make it possible to use less extensive surgery and remove less tissue.
- With a targeted drug for larger cancers, if chemotherapy is not an option.
- To help ease symptoms of advanced cancer, such as pain, bleeding, trouble swallowing, and problems caused by cancer spread to lungs or bones.
- To treat cancer that has come back after treatment (recurrence).
Chemoradiation (radiation given at the same time as chemotherapy) often works better than radiation alone, but it also has more side effects.
Radiation to this part of your body can cause problems for your teeth and gums, so it’s important to see a dentist before starting treatment. A dentist can make sure your mouth is healthy before treatment. They might recommend that certain bad teeth be removed before you start radiation because this can increase your chance of infection. During and after treatment your dentist can help check for and treat any problems that may come up, such as infection or tooth and bone damage.
External beam radiation used for oral and oropharyngeal cancers
External beam radiation therapy (EBRT) is the type of radiation therapy most often used to treat oral cavity or oropharyngeal cancer or its spread to other organs. It focuses radiation from a source outside the body onto the cancer.
Before EBRT, a somewhat flexible but sturdy mesh head and neck mask might be made to hold your head, neck, and shoulders in the exact same position for each treatment. Some people might feel a bit confined while this mask is on and might need to ask for medicine to help them relax during the treatment. Sometimes, the mask can be adjusted so that it is not too constricting. Discuss your options with your radiation oncologist. You might also be fitted for a bite block that you hold in your mouth during treatment
Treatment is much like getting an x-ray, but the radiation dose is stronger. The procedure itself is without pain and each treatment lasts only a few minutes. The setup time (getting you into place for treatment) often takes longer.
Different types of external beam radiation therapy (EBRT)
There are also more advanced EBRT techniques that help doctors focus the radiation more precisely.
- Three-dimensional conformal radiation therapy (3D-CRT) uses special computers to precisely map the location of the tumor. Several radiation beams are then shaped and aimed at the tumor from different directions, which makes it less likely to damage normal tissues.
- Intensity modulated radiation therapy (IMRT) is a form of 3D-CRT. It uses a computer-driven machine that actually moves around the patient as it delivers radiation. Along with shaping the beams and aiming them at the tumor from several angles, the intensity (strength) of the beams can be adjusted to limit the dose reaching nearby normal tissues. This may let the doctor deliver a higher dose to the tumor.
- Proton beam radiation therapy focuses beams of protons instead of x-rays on the cancer. Unlike x-rays, which go through the patient and release radiation both before and after they hit the tumor, protons only travel a certain distance, so the tissues behind the tumor are exposed to very little radiation. Even the tissues in front of the tumor see less radiation than the tumor itself. This means that proton beam radiation can deliver radiation to the cancer while doing less damage to nearby normal tissues. Because there are so many critical structures close by, proton beam radiation can be used to treat certain tumors of the oral cavity or oropharynx. Proton therapy can be a safe option in certain cases when using x-rays is not. Proton therapy is not widely available in the United States. The machines needed to make protons are very expensive. Proton therapy might also not be covered by all insurance companies at this time.
Different treatment schedules for external beam radiation therapy (EBRT)
Standard external beam radiation therapy (EBRT) for oral cavity or oropharyngeal cancers is usually given in daily fractions (doses) 5 days a week for about 7 weeks. But sometimes other schedules might be used:
- Hyperfractionation radiation is a slightly lower radiation dose given more than once a day (for example, twice a day for 7 weeks).
- Accelerated fractionation radiation is the standard dose of radiation given each day but over a shorter time (5 to 6 weeks) instead of the usual 7 weeks (for example, radiation is given 6 days a week over 5 weeks instead of the standard 5 days a week for 7 weeks).
- Hypofractionation radiation is a slightly higher radiation dose given each day to lessen the number of treatments (for example, a higher radiation dose is given each day for 6 weeks, not the standard 7 weeks).
Hyperfractionation and accelerated fractionation schedules may reduce the risk of cancer coming back in or near the place it started (called local recurrence) and might help some people live longer compared to standard EBRT. The drawback is that treatments given on these schedules also tend to have more severe side effects. Adding chemotherapy to these treatment schedules (chemoradiation) doesn’t appear to improve outcomes more.
Brachytherapy for oral and oropharyngeal cancers
Brachytherapy is rarely used to treat oral cavity or oropharyngeal cancers as a first treatment, but it might be used if the cancer recurs (comes back).
Side effects of radiation therapy for oral cavity or oropharyngeal cancer
If you are going to get radiation therapy, it’s important to ask your doctor about the possible side effects so you know what to expect.
Radiation to the mouth and throat area can cause several short-term side effects depending on where the radiation is aimed and can include:
- Skin changes like a sunburn or suntan in the treated area
- Hoarseness
- Loss of taste
- Redness, soreness, or even pain in the mouth and throat
- Dry mouth
- Trouble swallowing
- Feeling tired
- Open sores in the mouth and throat
Long-lasting or permanent side effects of radiation therapy
- Poor nutrition and trouble swallowing: Many people treated with radiation to the oral cavity and throat area have painful sores in the mouth and throat that can make it very hard to eat and drink. This can lead to weight loss and poor nutrition. The sores heal with time after the radiation ends, but some people continue to have problems swallowing long after treatment ends because of the tightening of the muscles caused by radiation. Ask your speech pathologist about swallowing exercises you can do to help keep those muscles working and increase your chance of eating normally after treatment. Liquid feeding through a tube placed into the stomach might be needed.
- Dry mouth: Damage to the salivary (spit) glands from radiation can cause a dry mouth that doesn’t get better with time. This can lead to discomfort and problems eating and swallowing, as well as damage to the jaw bone. The lack of saliva can also lead to tooth decay (cavities). People treated with radiation to the mouth or neck need to practice careful oral hygiene to help prevent this problem and see their dentist regularly. Fluoride treatments may also help.
- Damage to the jaw bone: This problem, known as osteoradionecrosis of the jaw, can be a serious side effect of radiation treatment. This is more common after tooth infection, extraction, or trauma, and it can be hard to treat. The main symptom is pain in the jaw. In some cases, the bone actually breaks. Sometimes the fractured bone heals by itself, but often the damaged bone will have to be repaired with surgery. To help prevent this problem, people getting radiation to the mouth or throat area need to see a dentist to have any problems with their teeth treated before radiation is started. In some cases, teeth may need to be removed.
- Thyroid problems: Radiation might damage your thyroid gland. Your doctor will do blood tests regularly to see how well your thyroid is working. You may need treatment if it’s been damaged and is not working well.
- Lymphedema: Some people treated with radiation therapy might be at risk of developing lymphedema in the head and neck areas that were treated. These areas can become swollen and firm. This can be worse if the person also had surgery. Sometimes, medicines, physical therapy, or massage therapy might be helpful.
- Damage to the carotid artery: Radiation to the neck area might increase a person’s risk of stroke many years after treatment. This might be because of health problems that were already present before radiation such as narrowing of the artery or an increase in plaques which can both decrease blood flow. People who smoke are also damaging their arteries. Because of this some doctors might order regular ultrasounds for you after treatment, to keep an eye on the arteries.
Chemotherapy for oral cavity and oropharyngeal cancer
Chemotherapy (chemo) is treatment with anti-cancer drugs that are injected into a vein or taken by mouth, which allows them to enter the blood and reach most parts of the body.
Chemo might be used at different times in the treatment process for treatment of oral cavity or oropharyngeal cancers:
- Adjuvant chemotherapy is given after surgery and is sometimes combined with radiation therapy. The goal is to kill cancer cells that might have been left behind at surgery because they were too small to see. This helps lower the chance that the cancer will come back.
- Neoadjuvant or induction chemotherapy is given before surgery. Sometimes the chemo is given first followed by radiation. Other times, it is given at the same time as radiation. The goal is to shrink some larger cancers to make surgery easier and remove less tissue. This can lead to fewer serious side effects and problems from surgery.
- For advanced cancer, chemo (with or without radiation therapy) can be used to treat cancers that are too large or have spread too far to be removed by surgery. The goal is to slow the growth of the cancer for as long as possible and to help relieve any symptoms the cancer is causing.
Chemo drugs for oral cavity or oropharyngeal cancer are usually given by mouth or into a vein (IV) as an infusion over a certain period of time. This can be done in a doctor’s office, infusion center, or in a hospital setting.
Often, a slightly larger and sturdier IV is required in the vein system for chemo. These IVs are known as central venous catheters (CVCs) , central venous access devices (CVADs), or central lines. They are used to put medicines, blood products, nutrients, or fluids right into your blood. They can also be used to take blood for tests. There are many different kinds of CVCs. The most common types are the port and the PICC line.
Chemotherapy is given in cycles: one drug or a combination of drugs given on a set schedule, followed by a rest period. Common schedules of chemo cycles can be once a week, once every 3 weeks, or once every 4 weeks. The schedule depends on the drugs used. The chemo schedule repeats to start the next cycle.
Adjuvant or neoadjuvant chemo is often given for a total of 3 to 6 months, depending on the drugs used. The length of treatment depends on how well it is working and what side effects you might have.
The chemo drugs used most often for cancers of the oral cavity and oropharynx that can be given with or without radiation include:
- Cisplatin
- Carboplatin
- 5-fluorouracil (5-FU)
- Paclitaxel (Taxol)
- Docetaxel (Taxotere)
- Hydroxyurea
Other drugs that are used less often include:
- Methotrexate
- Capecitabine
A chemo drug may be used alone or combined with other drugs. Combining drugs can often shrink tumors better, but tend to cause more side effects. A commonly used combination is carboplatin and 5-FU. This combination works better than either drug alone in shrinking cancers of the oral cavity and oropharynx. Another combination often used is cisplatin, 5-FU, plus docetaxel. In certain cases, chemo might be given along with a targeted drug or immunotherapy.
Chemoradiation
Chemoradiation is chemotherapy given at the same time as radiation. It has been shown to shrink oral cavity and oropharyngeal tumors more than either treatment alone and is helpful for people whose cancers are not widespread, but are too advanced for surgery. But this combined approach can be hard to tolerate, especially for people in poor health.
A preferred schedule is to give a dose of cisplatin every 3 weeks (for a total of 2 to 3 doses) during radiation. For people who cannot tolerate chemo, the targeted drug cetuximab might be used with radiation instead. See below for more chemo drugs that might be used with radiation.
Side effects of chemotherapy
Chemo drugs attack cells that are dividing quickly, which is why they work against cancer cells. But other cells in the body, such as those in the bone marrow, the lining of the mouth and intestines, and the hair follicles also divide quickly and are affected. This can lead to side effects.
The side effects of chemo depend on the type and dose of drugs given and how long they are taken. Common side effects can include:
- Hair loss
- Mouth sores
- Loss of appetite or weight loss
- Nausea and vomiting
- Diarrhea
- Nail changes
- Skin changes
Chemo can affect the blood-producing cells of the bone marrow, which can lead to:
- Increased chance of infections (from low white blood cell counts)
- Easy bruising or bleeding (from low blood platelet counts)
- Fatigue (from low red blood cell counts)
Along with the risks above, some side effects are seen more often with certain chemo drugs. For example, 5-FU often causes diarrhea. This might need to be treated with drugs like loperamide. Cisplatin, docetaxel, and paclitaxel can cause nerve damage (called neuropathy). This can lead to numbness and tingling in the hands and feet. This often improves once treatment is stopped, but for some people it can last a long time. Cisplatin can also cause kidney damage. To help prevent this, intravenous (IV) fluid is given before and after each dose.
Most side effects tend to get better over time once treatment is stopped. Some, such as neuropathy can last a long time or even be permanent. If your doctor plans treatment with chemo be sure to discuss the drugs that will be used and the possible side effects. Once chemo is started, tell your health care team if you notice any changes or have any side effects. There are ways to prevent or treat many of the side effects of chemo. For example, many drugs are available to help prevent or treat nausea and vomiting. In some cases, the doses of the chemo drugs may need to be reduced or treatment may need to be delayed or stopped to help keep the problem from getting worse.
Targeted therapy for oral cavity and oropharyngeal cancer
Targeted drug therapy is the use of medicines that target or are directed at proteins on cancer cells that help them grow, spread, and live longer. Targeted drug therapy can be used to treat oral cavity and oropharyngeal cancers by destroying cancer cells or slowing their growth. Their side effects are different from chemotherapy (sometimes less severe) and many are taken as a pill.
Some targeted drugs, for example, monoclonal antibodies, work in more than one way to control cancer cells and may also be considered immunotherapy because they boost the immune system.
Epidermal growth factor receptor (EGFR) is a protein that helps cancer cells grow. Drugs that target EGFR can be used to treat some oral cavity or oropharyngeal cancers.
Cetuximab
Cetuximab (Erbitux) is a monoclonal antibody, which is a man-made version of an immune system protein. It targets the epidermal growth factor receptor (EGFR) protein on the surface of certain cells that helps cells grow and divide. Oral cavity and oropharyngeal cancer cells often have higher than normal amounts of EGFR. By blocking EGFR, cetuximab can help slow or stop cancer cell growth.
Cetuximab can be combined with radiation therapy for some earlier stage cancers. For more advanced cancers, it may be combined with standard chemo drugs such as cisplatin, or it may be used by itself.
Cetuximab is given by infusion into a vein (IV), either once a week or every other week.
Side effects of targeted drug therapy
Many people develop skin problems such as an acne-like rash on the face and chest during treatment, which in some cases can lead to infections. Cetuximab can make your skin very sensitive to the sun, so you’ll need to protect your skin while getting treatment and for at least months after treatment. Other side effects may include headache, tiredness, fever, and diarrhea.
A rare but serious side effect of cetuximab is an allergic reaction during the first infusion, which could cause problems with breathing and low blood pressure. You may be given medicine before treatment to help prevent this.
Immunotherapy for oral cavity and oropharyngeal cancer
Immunotherapy can be used to treat oral cavity and oropharyngeal cancers. Immunotherapy is the use of medicines to help boost a person’s own immune system to find and destroy cancer cells more effectively. It typically works on specific proteins involved in the immune system to enhance the immune response. It has different (sometimes less severe) side effects than chemotherapy.
Some immunotherapy drugs, for example, monoclonal antibodies, work in more than one way to control cancer cells and may also be considered targeted drug therapy because they block a specific protein on the cancer cell to keep it from growing.
Immune checkpoint inhibitors
An important part of the immune system is its ability to keep itself from attacking normal cells in the body. To do this, it uses “checkpoints,” proteins on immune cells that need to be turned on (or off) to start an immune response. Cancer cells sometimes use these checkpoints to avoid being attacked by the immune system. Drugs that target these checkpoints are called checkpoint inhibitors, can be used to treat some people with oral cavity or oropharyngeal cancer.
PD-1 inhibitors
Pembrolizumab (Keytruda) and nivolumab (Opdivo) are drugs that target PD-1, a protein on T cells in the immune system. PD-1 normally helps keep T cells from attacking other cells . By blocking PD-1, these drugs boost the immune response against cancer cells. This can shrink some tumors or slow their growth.
These drugs can be used after chemotherapy stops working in people with oral cavity or oropharyngeal cancer that has returned after treatment (recurrent) or that has spread to other parts of the body (metastatic). Nivolumab is given as an intravenous (IV) infusion every 2 or 4 weeks. Pembrolizumab is given as an IV infusion every 3 or 6 weeks.
Pembrolizumab, alone or with chemotherapy, is also an option as the first treatment in some people whose cancer has recurred, is metastatic, or cannot be removed with surgery. It is given as an IV infusion every 3 or 6 weeks.
Side effects of these drugs can include fatigue, cough, nausea, diarrhea, skin rash, loss of appetite, constipation, joint pain, and itching.
Other, more serious side effects occur less often.
- Infusion reactions: Some people might have an infusion reaction while getting these drugs. This is like an allergic reaction, and can cause fever, chills, flushing of the face, rash, itchy skin, feeling dizzy, wheezing, and trouble breathing. It’s important to tell your doctor or nurse right away if you have any of these symptoms while getting these drugs.
- Autoimmune reactions: These drugs work by removing one of the safeguards of the body’s immune system. Sometimes the immune system starts attacking other parts of the body, which can cause serious or even life-threatening problems in the lungs, intestines, liver, hormone-making glands, kidneys, nerves, skin, or other organs.
It’s very important to report any new side effects during or after treatment with any of these drugs to your health care team promptly. If serious side effects do occur, you might need to stop treatment and take high doses of corticosteroids to suppress your immune system.
Follow up for mouth and oropharyngeal cancer
After treatment for mouth and oropharyngeal cancer, you have regular check ups at the hospital. You might also have tests including blood tests, x-rays and scans. Over time, these appointments become less frequent.
You usually have follow up appointments every few months to check how you are and see whether you have any problems or worries. The appointments also give you the chance to raise any concerns you have about your progress.
Palliative care
Palliative care can help ease physical symptoms from the cancer or its treatment, can help people cope with feelings they might have related to the diagnosis, and can also support caregivers. Palliative care works best if it is added to a person’s care early on in their diagnosis, especially for those people with advanced cancer. Some studies show it may even help people live longer.
Pain management and oral cavity and oropharyngeal cancer
Pain is a significant concern for many people with cancer. It can almost always be treated with milder drugs like ibuprofen or acetaminophen or, if needed, with stronger medicines like morphine or drugs like it (known as opioids). Sometimes, procedures like surgery, a nerve block, or radiation might be options to lessen pain.
Nutrition and oral cavity and oropharyngeal cancer
Keeping healthy through nutrition is another important concern for people with oral cavity or oropharyngeal cancers. Both the cancer and its treatment can make it hard to swallow and to eat or drink. If this is the case, a feeding tube may be needed. This tube will most likely be needed during treatment, but in some cases it might need to be left in longer.
There are many other ways your cancer care team can help you maintain your quality of life and help control your symptoms. But you have to tell your team how you’re feeling and what symptoms you’re having. Some people don’t like to disappoint their doctors by telling them they’re not feeling well. Others just don’t want to complain. This is not helpful to you or your treatment goals. Tell your doctor how you really feel. Talking about the symptoms you’re having lets your doctor give treatments or medicines that can help relieve them which can help you handle treatment better. You will probably feel better and be able to focus on the things that are important to you.
Treatment options for oral cavity cancer by stage
Treatment for oral cavity cancer is based largely on the stage (extent) of the cancer, but other factors can also be important.
Stage 0 (carcinoma in situ) oral cavity cancer treatment
Although cancer in this stage is on the surface layer and has not started to grow into deeper layers of tissue, it can do so if not treated. The usual treatment is surgery (usually Mohs surgery, surgical stripping, or thin resection) to remove the top layers of tissue along with a small margin (edge) of normal tissue. Follow-up is important to watch for any signs that the cancer has come back. Carcinoma in situ that keeps coming back after surgery may also need to be treated with radiation therapy.
Nearly all people with stage 0 (carcinoma in situ) survive a long time without the need for more treatment.
Stages 1 and 2 oral cavity cancer treatment
Most patients with stage 1 or stage 2 oral cavity cancers do well when treated with surgery and/or radiation therapy. Chemotherapy (chemo) given along with radiation (called chemoradiation) is another option. Both surgery and radiation work equally well in treating these cancers. The choice depends on your preferences and the expected side effects, including how the treatment might affect how you look and how you swallow and speak.
Lip
Surgery is preferred for small cancers that can be removed. Radiation alone may also be used as the first treatment.
Large or deep cancers often require surgery. If needed, reconstructive surgery can help correct the defect in the lip.
If the tumor is thick, it increases the possibility that the cancer might have spread to lymph nodes in the neck. If abnormal lymph nodes are felt or seen on an imaging test, the surgeon might remove them (called lymph node dissection) so they can be checked for cancer spread.
Oral cavity
For cancers of the floor of the mouth, front of the tongue, inside of the cheek, gums, and hard palate, surgery is the main treatment. Lymph nodes in the neck might be removed (called lymph node dissection) to check them for cancer spread. If it looks like surgery hasn’t completely removed the cancer or if there is a high chance of it coming back, radiation alone or chemoradiation might be added.
Radiation can be used instead of surgery as the main treatment for some people. This is most often done for people who can’t have surgery because of other medical problems.
Stages 3 and 4A oral cavity cancer treatment
These cancers in the floor of the mouth, front of the tongue, inside of the cheek, gums, and hard palate include bigger cancers, those that have grown into nearby tissues, and/or those that have spread to nearby lymph nodes in the neck. Surgery is usually done first and includes taking out some of the neck lymph nodes (lymph node dissection). Surgery is most often followed by radiation alone or chemoradiation.
Stages 4B and 4C oral cavity cancer treatment
Stage 4B cancers have already spread into nearby tissues, structures, and maybe lymph nodes. Stage 4C cancers have spread to other parts of the body, such as the lungs.
People with stage 4B cancers that cannot be removed by surgery or who are too weak for surgery might be treated with radiation alone. Depending on a person’s overall health, chemoradiation or chemotherapy first followed by radiation might be options. Chemotherapy alone may also be recommended.
Stage 4C cancers are usually treated with chemo, cetuximab, or both. Immunotherapy, alone or with chemo, might be another option. Treatments such as radiation can also be used to help relieve symptoms from the cancer or to help prevent new problems.
Recurrent oral cavity cancer
When cancer comes backs after treatment, it’s called recurrent cancer. It can come back in or near the same place the cancer first started (local), in nearby lymph nodes (regional), or it can spread to other organs such as the lungs or bone (distant). Treatment options for recurrent cancers depend on the location and size of the cancer, what treatments have already been used, and the person’s general health. Because these cancers can be hard to treat, clinical trials of newer treatments may be a good option for some people.
If the cancer comes back in the same area and radiation therapy was used as the first treatment, surgery is often the next treatment, if the cancer can be removed completely and the patient is healthy enough for surgery. Usually, external beam radiation therapy cannot be repeated in the same site except in certain cases. But internal radiation (brachytherapy) can often be used to control the cancer if it has come back in the place it started. If surgery was used first, more surgery, radiation therapy, chemo, cetuximab, immunotherapy, or a combination of these may be options.
If the cancer comes back in the lymph nodes in the neck, the nodes are often removed with surgery (lymph node dissection). This may be followed by radiation or chemoradiation.
If the cancer comes back in a distant area, chemo (and/or cetuximab) is often used. Immunotherapy with or without chemo might be an option as well. These treatments may shrink or slow the growth of some cancers for a while and help relieve symptoms, but these cancers are very hard to cure.
If further treatment is recommended, it’s important to talk to your doctor so that you understand what the goal of treatment is — whether it’s to try to cure the cancer or to keep it under control for as long as possible and to relieve symptoms. This can help you weigh the risks and benefits of each treatment.
Oral cancer prognosis
If you have oral cancer, you may have questions about your prognosis. A prognosis is the doctor’s best estimate of how cancer will affect someone and how it will respond to treatment. Prognosis and survival depend on many factors. Only a doctor familiar with your medical history, the type and stage and other features of the cancer, the treatments chosen and the response to treatment can put all of this information together with survival statistics to arrive at a prognosis.
A prognostic factor is an aspect of the cancer or a characteristic of the person (such as whether they smoke) that the doctor will consider when making a prognosis. A predictive factor influences how a cancer will respond to a certain treatment. Prognostic and predictive factors are often discussed together. They both play a part in deciding on a treatment plan and a prognosis.
The following are prognostic factors for oral cancer:
- Stage. The stage of oral cancer is an important prognostic factor. The lower the stage, the better the prognosis.
- Tumor thickness. Tumor thickness is also an important prognostic factor. A thin tumor has a better prognosis. A thicker tumor has a higher risk of coming back (recurring) in the same place (local recurrence). Thicker tumours are also more likely to have spread to the lymph nodes.
- Margin status. The margin is the area of healthy tissue around a tumor that is removed along with the tumor during surgery. If cancer cells are found in the margin, it is called a positive surgical margin. If cancer cells are not found in the margin, it is called a negative margin. Tumours with negative surgical margins have a better prognosis.
- Spread to nerves. When oral cancer has grown into, around or along a nerve (called perineural invasion) the prognosis may be poorer.
- Spread to blood vessels. When oral cancer has spread to blood vessels (called vascular invasion) it may increase the risk of spread throughout the body. Cancer that has spread throughout the body has a poorer prognosis.
- Spread to lymph nodes. Oral cancer that has spread to the lymph nodes has a poorer prognosis. The more lymph nodes the cancer reaches, the higher the risk of distant spread or metastasis. If cancer grows beyond the wall of a lymph node (called extracapsular extension), the prognosis is also poorer.
- Location. Prognosis can also depend on the location of the oral cancer.
The National Cancer Institute’s Surveillance, Epidemiology and End Results (SEER) database tracks 5-year relative survival rates for oral cavity and oropharyngeal cancers in the United States, based on how far the cancer has spread. The SEER database, however, does not group cancers by AJCC TNM stages (stage 1, stage 2, stage 3, etc.). Instead, it groups cancers into localized, regional, and distant stages:
- Localized: There is no sign the cancer has spread outside the organ where it started (for example, the lip, tongue, or floor of mouth).
- Regional: The cancer has spread to nearby structures or lymph nodes.
- Distant: The cancer has spread to distant parts of the body such as the lungs.
Oral cancer and and oropharyngeal cancers 5-year Relative Survival rates
[Source 8 ]Oral cavity cancer survival by stage
There are no US statistics available for different stages of mouth cancer or particular treatments. The following statistics are from the National Cancer Intelligence Network for people diagnosed with mouth (oral cavity) cancer in England and Wales, between 2004 and 2011 37. The figures are for 1 and 3 year survival. At the moment there are no statistics available for 5 year survival.
For men diagnosed with stage 1 and 2 mouth (oral cavity) cancer:
- more than 90 out of 100 (more than 90%) survive their cancer for 1 year or more
- around 80 out of 100 (around 80%) survive their cancer for 3 years or more
For women diagnosed with stage 1 and 2 mouth cancer:
- around 95 out of 100 (around 95%) survive their cancer for 1 year or more
- more than 80 out of 100 (more than 80%) survive their cancer for 3 years or more
For men diagnosed with stage 3 and 4 mouth cancer:
- almost 70 out of 100 (almost 70%) survive their cancer for a year or more
- almost 50 out of 100 (almost 50%) survive their cancer for 3 years or more
For women diagnosed with stage 3 or 4 cancer:
- around 65 out of 100 (around 65%) survive their cancer for a year or more
- almost 50 out of 100 (almost 50%) survive their cancer for 3 years or more
Oral cavity cancer survival by site of tumor
Survival for mouth and oropharyngeal cancer depends on where the cancer is. These statistics are for people diagnosed in England between 2009 and 2013 38.
For mouth (oral cavity) cancer:
- almost 80 out of 100 people (almost 80%) survive their cancer for 1 year or more after they are diagnosed
- around 55 out of 100 people (around 55%) survive their cancer for 5 years or more after diagnosis
- 45 out of 100 people (45%) survive their cancer for 10 years or more after diagnosis
For oropharyngeal cancer
- around 85 out of 100 (around 85%) survive their cancer for a year or more after diagnosis
- around 65 out of 100 (around 65%) survive their cancer for 5 years or more after diagnosis
- almost 60 out of 100 (almost 60%) survive their cancer for 10 years or more after diagnosis
The oropharynx is the part of the throat just behind your mouth
For tongue cancer:
- around 80 out of 100 (around 80%) survive their cancer for a year or more after diagnosis
- 60 out of 100 (60%) survive their cancer for 5 years or more after diagnosis
- around 50 out of 100 (around 50%) survive their cancer for 10 years or more after diagnosis
Oral cancer survival rates
Survival rates can give you an idea of what percentage of people with the same type and stage of cancer are still alive a certain amount of time (usually 5 years) after they were diagnosed. They can’t tell you how long you will live, but they may help give you a better understanding of how likely it is that your treatment will be successful.
Keep in mind that survival rates are estimates and are often based on previous outcomes of large numbers of people who had a specific cancer, but they can’t predict what will happen in any particular person’s case. These statistics can be confusing and may lead you to have more questions. Your doctor is familiar with your situation; ask how these numbers may apply to you.
A relative survival rate compares people with the same type and stage of cancer to people in the overall population. For example, if the 5-year relative survival rate for localized oral cavity and pharynx cancer is 86.3%, it means that people who have localized oral cavity and pharynx cancer are, on average, about 86.3% as likely as people who don’t have that cancer to live for at least 5 years after being diagnosed.
The National Cancer Institute’s Surveillance, Epidemiology and End Results (SEER) database tracks 5-year relative survival rates for oral cavity and oropharyngeal cancers in the United States, based on how far the cancer has spread. The SEER database, however, does not group cancers by AJCC TNM stages (stage 1, stage 2, stage 3, etc.). Instead, it groups cancers into localized, regional, and distant stages:
- Localized: There is no sign the cancer has spread outside the organ where it started (for example, the lip, tongue, or floor of mouth).
- Regional: The cancer has spread to nearby structures or lymph nodes.
- Distant: The cancer has spread to distant parts of the body such as the lungs.
Table 3. 5-year relative survival rates for Lip cancers
| SEER Stage | 5-Year Relative Survival Rate |
|---|---|
| Localized | 93% |
| Regional | 65% |
| Distant | 33% |
| All SEER stages combined | 91% |
Footnotes:
- These numbers are based on people diagnosed with oral cavity or oropharyngeal cancer between 2011 and 2017.
- These numbers apply only to the stage of the cancer when it is first diagnosed. They do not apply later on if the cancer grows, spreads, or comes back after treatment.
- These numbers don’t take everything into account. Survival rates are grouped based on how far the cancer has spread, but your age, overall health, how well the cancer responds to treatment, and other factors will also affect your outlook. Currently, these survival rates are not based on the p16 (HPV) status of the cancer.
- People now being diagnosed with oral cavity or oropharyngeal cancer may have a better outlook than these numbers show. Treatments improve over time, and these numbers are based on people who were diagnosed and treated at least five years earlier.
Table 4. 5-year relative survival rates for Tongue cancers
| SEER Stage | 5-Year Relative Survival Rate |
|---|---|
| Localized | 83% |
| Regional | 69% |
| Distant | 41% |
| All SEER stages combined | 68% |
Footnotes:
- These numbers are based on people diagnosed with oral cavity or oropharyngeal cancer between 2011 and 2017.
- These numbers apply only to the stage of the cancer when it is first diagnosed. They do not apply later on if the cancer grows, spreads, or comes back after treatment.
- These numbers don’t take everything into account. Survival rates are grouped based on how far the cancer has spread, but your age, overall health, how well the cancer responds to treatment, and other factors will also affect your outlook. Currently, these survival rates are not based on the p16 (HPV) status of the cancer.
- People now being diagnosed with oral cavity or oropharyngeal cancer may have a better outlook than these numbers show. Treatments improve over time, and these numbers are based on people who were diagnosed and treated at least five years earlier.
Table 5. 5-year relative survival rates for Floor of the mouth cancers
| SEER Stage | 5-Year Relative Survival Rate |
|---|---|
| Localized | 73% |
| Regional | 41% |
| Distant | 23% |
| All SEER stages combined | 52% |
Footnotes:
- These numbers are based on people diagnosed with oral cavity or oropharyngeal cancer between 2011 and 2017.
- These numbers apply only to the stage of the cancer when it is first diagnosed. They do not apply later on if the cancer grows, spreads, or comes back after treatment.
- These numbers don’t take everything into account. Survival rates are grouped based on how far the cancer has spread, but your age, overall health, how well the cancer responds to treatment, and other factors will also affect your outlook. Currently, these survival rates are not based on the p16 (HPV) status of the cancer.
- People now being diagnosed with oral cavity or oropharyngeal cancer may have a better outlook than these numbers show. Treatments improve over time, and these numbers are based on people who were diagnosed and treated at least five years earlier.
Table 6. 5-year relative survival rates for Oropharynx cancers
| SEER Stage | 5-year Relative Survival Rate |
|---|---|
| Localized | 59% |
| Regional | 59% |
| Distant | 28% |
| All SEER stages combined | 50% |
Footnotes:
- These numbers are based on people diagnosed with oral cavity or oropharyngeal cancer between 2011 and 2017.
- These numbers apply only to the stage of the cancer when it is first diagnosed. They do not apply later on if the cancer grows, spreads, or comes back after treatment.
- These numbers don’t take everything into account. Survival rates are grouped based on how far the cancer has spread, but your age, overall health, how well the cancer responds to treatment, and other factors will also affect your outlook. Currently, these survival rates are not based on the p16 (HPV) status of the cancer.
- People now being diagnosed with oral cavity or oropharyngeal cancer may have a better outlook than these numbers show. Treatments improve over time, and these numbers are based on people who were diagnosed and treated at least five years earlier.
- Abati, S.; Bramati, C.; Bondi, S.; Lissoni, A.; Trimarchi, M. Oral Cancer and Precancer: A Narrative Review on the Relevance of Early Diagnosis. Int. J. Environ. Res. Public Health 2020, 17, 9160. https://doi.org/10.3390/ijerph17249160[↩]
- Warnakulasuriya S. Global epidemiology of oral and oropharyngeal cancer. Oral Oncol. 2009 Apr-May;45(4-5):309-16. doi: 10.1016/j.oraloncology.2008.06.002[↩]
- Dhanuthai, K., Rojanawatsirivej, S., Thosaporn, W., Kintarak, S., Subarnbhesaj, A., Darling, M., Kryshtalskyj, E., Chiang, C. P., Shin, H. I., Choi, S. Y., Lee, S. S., & Aminishakib, P. (2018). Oral cancer: A multicenter study. Medicina oral, patologia oral y cirugia bucal, 23(1), e23–e29. https://doi.org/10.4317/medoral.21999[↩]
- Key Statistics for Oral Cavity and Oropharyngeal Cancers. https://www.cancer.org/cancer/oral-cavity-and-oropharyngeal-cancer/about/key-statistics.html[↩][↩][↩]
- Oral Cavity Cancer: Professional Version. https://www.ahns.info/resources/oral-cavity-cancer/2/[↩]
- Goldstein, B. Y., Chang, S. C., Hashibe, M., La Vecchia, C., & Zhang, Z. F. (2010). Alcohol consumption and cancers of the oral cavity and pharynx from 1988 to 2009: an update. European journal of cancer prevention : the official journal of the European Cancer Prevention Organisation (ECP), 19(6), 431–465. https://doi.org/10.1097/CEJ.0b013e32833d936d[↩]
- Khan, Z., Tönnies, J., & Müller, S. (2014). Smokeless tobacco and oral cancer in South Asia: a systematic review with meta-analysis. Journal of cancer epidemiology, 2014, 394696. https://doi.org/10.1155/2014/394696[↩]
- Oral Cavity and Pharynx Cancer — Cancer Stat Facts. https://seer.cancer.gov/statfacts/html/oralcav.html[↩][↩]
- Machiels JP, René Leemans C, Golusinski W, Grau C, Licitra L, Gregoire V; EHNS Executive Board, ESMO Guidelines Committee, ESTRO Executive Board. Reprint of “Squamous cell carcinoma of the oral cavity, larynx, oropharynx and hypopharynx: EHNS-ESMO-ESTRO Clinical Practice Guidelines for diagnosis, treatment and follow-up”. Oral Oncol. 2021 Feb;113:105042. doi: 10.1016/j.oraloncology.2020.105042[↩]
- Mehanna, H., Evans, M., Beasley, M., Chatterjee, S., Dilkes, M., Homer, J., O’Hara, J., Robinson, M., Shaw, R., & Sloan, P. (2016). Oropharyngeal cancer: United Kingdom National Multidisciplinary Guidelines. The Journal of laryngology and otology, 130(S2), S90–S96. https://doi.org/10.1017/S0022215116000505[↩]
- Wong, T.S.C., Wiesenfeld, D. (2018) Oral Cancer. Australian Dental Journal, 63: S1 S91– S99. https://doi.org/10.1111/adj.12594[↩][↩]
- Swerdlow, S. H., Campo, E., Pileri, S. A., Harris, N. L., Stein, H., Siebert, R., Advani, R., Ghielmini, M., Salles, G. A., Zelenetz, A. D., & Jaffe, E. S. (2016). The 2016 revision of the World Health Organization classification of lymphoid neoplasms. Blood, 127(20), 2375–2390. https://doi.org/10.1182/blood-2016-01-643569[↩]
- National Institutes of Health, National Cancer Institute. Surveillance, epidemiology, and end results program cancer stat facts: Hodgkin lymphoma. https://seer.cancer.gov/statfacts/html/hodg.html[↩]
- National Institutes of Health, National Cancer Institute. Surveillance, epidemiology, and end results program cancer stat facts: Non-Hodgkin Lymphoma. https://seer.cancer.gov/statfacts/html/nhl.html[↩]
- Neville, B.W. and Day, T.A. (2002), Oral Cancer and Precancerous Lesions. CA: A Cancer Journal for Clinicians, 52: 195-215. https://doi.org/10.3322/canjclin.52.4.195[↩][↩]
- Kramer IR, Lucas RB, Pindborg JJ, Sobin LH. Definition of leukoplakia and related lesions: an aid to studies on oral precancer. Oral Surg Oral Med Oral Pathol. 1978 Oct;46(4):518-39.[↩]
- Scheifele C, Reichart PA, Dietrich T. Low prevalence of oral leukoplakia in a representative sample of the US population. Oral Oncol. 2003 Sep;39(6):619-25. doi: 10.1016/s1368-8375(03)00050-2[↩]
- Shafer WG, Waldron CA. Erythroplakia of the oral cavity. Cancer. 1975 Sep;36(3):1021-8. doi: 10.1002/1097-0142(197509)36:3<1021::aid-cncr2820360327>3.0.co;2-w[↩]
- Oral leukoplakia. https://dermnetnz.org/topics/oral-leukoplakia[↩]
- Management update of potentially premalignant oral epithelial lesions. Oral Surg Oral Med Oral Pathol Oral Radiol 2018; 125(6)628–636. doi:10.1016/j.oooo.2018.03.010[↩]
- Awadallah M, Idle M, Patel K, Kademani D. Management update of potentially premalignant oral epithelial lesions. Oral Surg Oral Med Oral Pathol Oral Radiol. 2018 Jun;125(6):628-636. doi: 10.1016/j.oooo.2018.03.010[↩][↩]
- Speight PM, Khurram SA, Kujan O. Oral potentially malignant disorders: risk of progression to malignancy. Oral Surg Oral Med Oral Pathol Oral Radiol. 2018 Jun;125(6):612-627. doi: 10.1016/j.oooo.2017.12.011[↩]
- Mangold AR, Torgerson RR, Rogers RS 3rd. Diseases of the tongue. Clin Dermatol. 2016 Jul-Aug;34(4):458-69. doi: 10.1016/j.clindermatol.2016.02.018[↩][↩]
- van der Waal, I. Oral Leukoplakia: Present Views on Diagnosis, Management, Communication with Patients, and Research. Curr Oral Health Rep 6, 9–13 (2019). https://doi.org/10.1007/s40496-019-0204-8[↩][↩][↩][↩][↩][↩]
- Ohta K, Yoshimura H. Leukoplakia of the tongue. Cleve Clin J Med. 2020 Mar;87(3):133-134. https://doi.org/10.3949/ccjm.87a.19087[↩][↩]
- Lodi, G., Franchini, R., Warnakulasuriya, S., Varoni, E. M., Sardella, A., Kerr, A. R., Carrassi, A., MacDonald, L. C., & Worthington, H. V. (2016). Interventions for treating oral leukoplakia to prevent oral cancer. The Cochrane database of systematic reviews, 7(7), CD001829. https://doi.org/10.1002/14651858.CD001829.pub4[↩]
- Wright JM. A review and update of oral precancerous lesions. Tex Dent J. 1998;115:15–9.[↩]
- Villa A, Villa C, Abati S. Oral cancer and oral erythroplakia: an update and implication for clinicians. Aust Dent J. 2011;56:253–6. doi: 10.1111/j.1834-7819.2011.01337.x[↩]
- Blot WJ, McLaughlin JK, Winn DM, Austin DF, Greenberg RS, Preston-Martin S, Bernstein L, Schoenberg JB, Stemhagen A, Fraumeni JF Jr. Smoking and drinking in relation to oral and pharyngeal cancer. Cancer Res. 1988 Jun 1;48(11):3282-7[↩]
- Koo K, Barrowman R, McCullough M, Iseli T, Wiesenfeld D. Non-smoking non-drinking elderly females: a clinically distinct subgroup of oral squamous cell carcinoma patients. Int J Oral Maxillofac Surg. 2013 Aug;42(8):929-33. doi: 10.1016/j.ijom.2013.04.010[↩]
- Gandini, S., Botteri, E., Iodice, S., Boniol, M., Lowenfels, A.B., Maisonneuve, P. and Boyle, P. (2008), Tobacco smoking and cancer: A meta-analysis. Int. J. Cancer, 122: 155-164. https://doi.org/10.1002/ijc.23033[↩][↩]
- Lee, Y. C., Marron, M., et al (2009). Active and involuntary tobacco smoking and upper aerodigestive tract cancer risks in a multicenter case-control study. Cancer epidemiology, biomarkers & prevention : a publication of the American Association for Cancer Research, cosponsored by the American Society of Preventive Oncology, 18(12), 3353–3361. https://doi.org/10.1158/1055-9965.EPI-09-0910[↩]
- Kumar M, Nanavati R, Modi TG, Dobariya C. Oral cancer: Etiology and risk factors: A review. J Cancer Res Ther. 2016 Apr-Jun;12(2):458-63. https://www.cancerjournal.net/text.asp?2016/12/2/458/186696[↩][↩]
- Kruse, A. L., & Grätz, K. W. (2009). Oral carcinoma after hematopoietic stem cell transplantation–a new classification based on a literature review over 30 years. Head & neck oncology, 1, 29. https://doi.org/10.1186/1758-3284-1-29[↩][↩]
- Can Oral Cavity and Oropharyngeal Cancers Be Found Early? https://www.cancer.org/cancer/oral-cavity-and-oropharyngeal-cancer/detection-diagnosis-staging/detection.html[↩]
- Oral Cavity and Oropharyngeal Cancer Stages. https://www.cancer.org/cancer/oral-cavity-and-oropharyngeal-cancer/detection-diagnosis-staging/staging.html[↩][↩]
- https://csg.lshtm.ac.uk/wp-content/uploads/2016/07/Muller-et-al_Rare-and-common-cancers_net-survival_25Jul17.pdf[↩]
- Survival for mouth and oropharyngeal cancer. https://www.cancerresearchuk.org/about-cancer/mouth-cancer/survival[↩]
- Survival Rates for Oral Cavity and Oropharyngeal Cancer. https://www.cancer.org/cancer/oral-cavity-and-oropharyngeal-cancer/detection-diagnosis-staging/survival-rates.html[↩][↩][↩][↩]