Pemphigoid gestationis
Pemphigoid gestationis was previously called herpes gestationis although it has no association with the herpes virus, is a rare pregnancy-associated autoimmune skin disease that is characterized by an itchy rash that develops into blisters 1. Pemphigoid gestationis is a bullous autoimmune, sub-epidermal dermatosis clinically and pathogenetically similar to bullous pemphigoid 2. Pemphigoid gestationis is most common during the third trimester and less commonly in the second trimester or even after delivery, but it can manifest in principle during all three trimesters. Pemphigoid gestationis manifests with inflammatory skin lesions and severe pruritus. It recurs in subsequent pregnancies earlier and as a more serious course.
The incidence of pemphigoid gestationis has been variably estimated, one case per 2000 up to 60,000 pregnancies. It is more frequent in persons with fair skin than dark skin. pemphigoid gestationis mainly occurs late in pregnancy with 60% of cases occurring between the 28th and the 32nd week of amenorrhea. Multigravidae are more susceptible to develop pemphigoid gestationis than primigravidae with an earlier onset of symptoms.
Pemphigoid gestationis usually resolves within 2 months after delivery. Nonetheless, it may persist or exacerbate after pregnancy due to a sudden increase in the level of antibodies. Recurrence may occur with subsequent pregnancies, menstruations or treatment with estrogens and progesterone-containing oral contraceptives. Fetal risks observed in pemphigoid gestationis are low birth weight baby, prematurity, and temporary skin lesions which resolve several weeks after the birth, but there is no increased risk of stillbirth and abortion. This risk may be correlated with disease severity. A postpartum flare-up has been observed.
The association of this disease with hydatidiform mole and choriocarcinoma must not be forgotten.
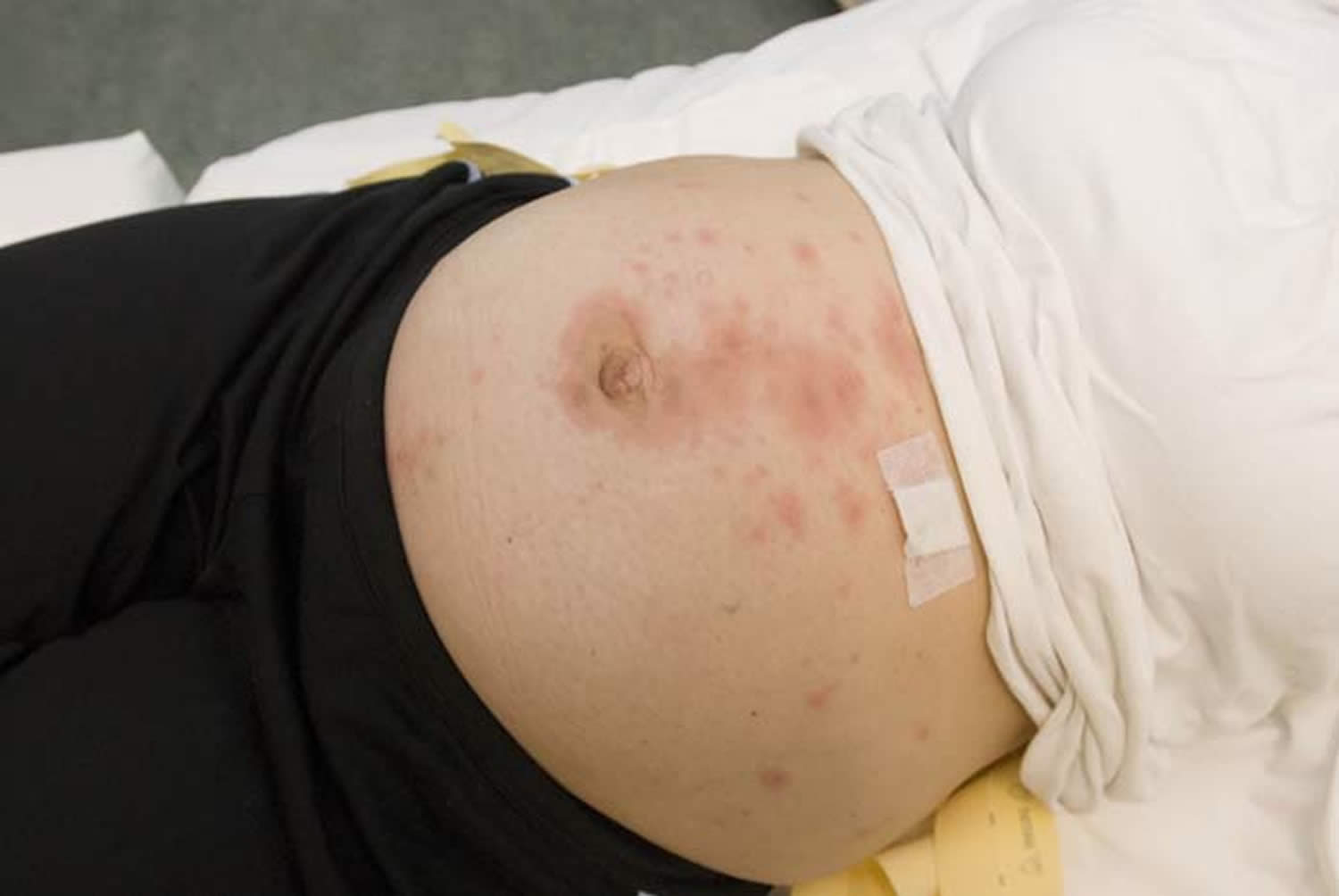
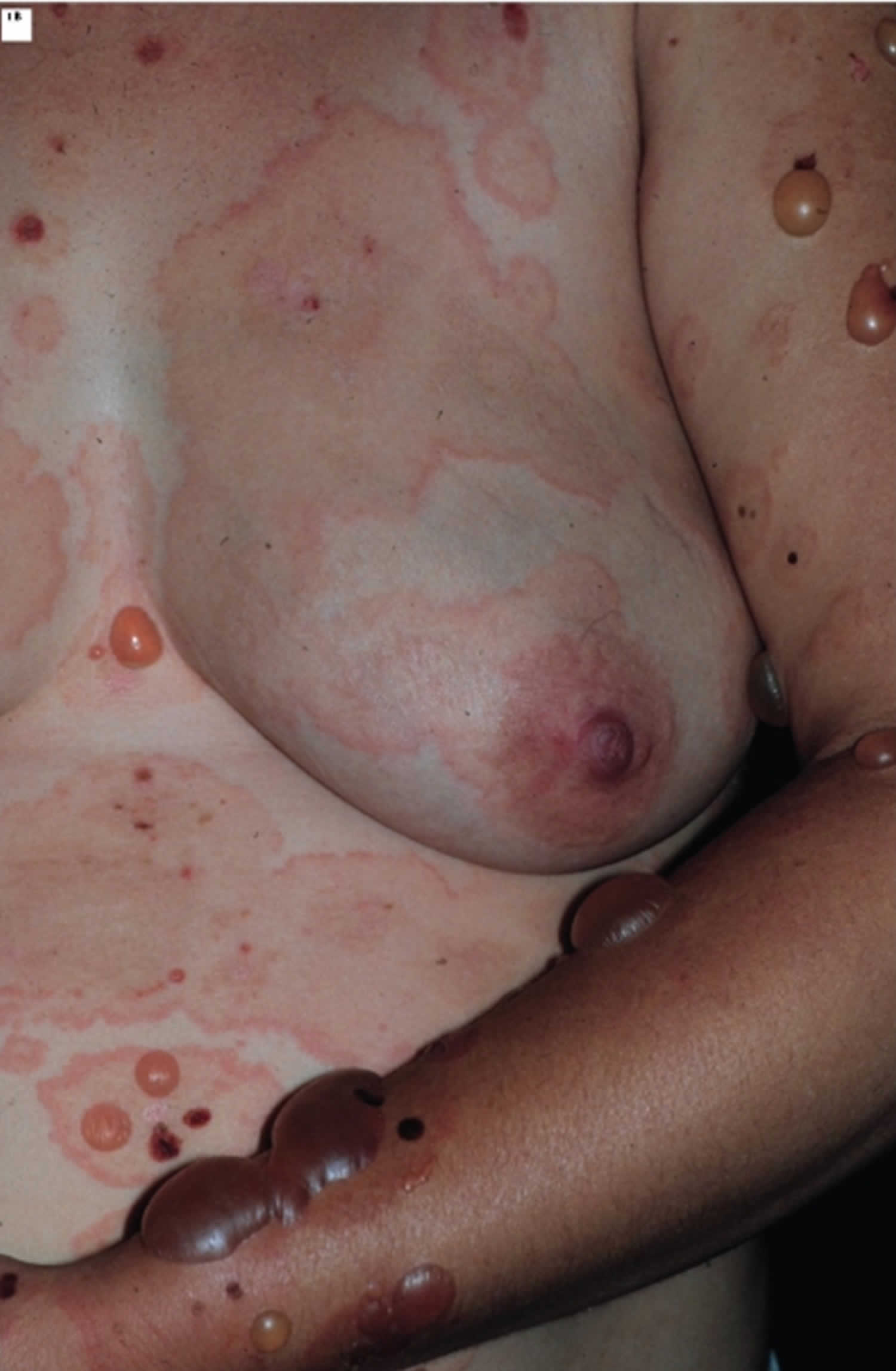
Figure 1. Pemphigoid gestationis
Footnote: Pemphigoid Gestationis: Pruritic urticarial lesions and tense blisters on the trunk.
[Source 3 ]Pemphigoid gestationis vs PUPPP
PUPPP is short for Pruritic Urticarial Papules and Plaques of Pregnancy also called polymorphic eruption of pregnancy, is an itchy, bumpy rash that starts in the stretch marks of the abdomen in the last 3 months of pregnancy then clears with delivery.
PUPPP occurs in about 1 in 160 pregnancies.
- It is more common in a first pregnancy than subsequent pregnancies.
- It is more commonly reported in women with white skin than in women with black skin.
- The risk is greater with excessive weight gain, including multiple births (eg twins or triplets).
- A male fetus is a greater risk than a female fetus.
Does PUPPP affect the baby?
Rarely, the baby can be born with a mild form of polymorphic eruption of pregnancy rash but this soon fades. Polymorphic eruption of pregnancy does not cause any other problem for the baby.
How long does PUPPP last?
Polymorphic eruption of pregnancy continues until delivery then usually resolves within 4–6 weeks. Rarely, it may persist for longer. In some cases, this relates to retained placental products.
Can PUPPP recur with future pregnancies?
It is very uncommon for polymorphic eruption of pregnancy to recur. If it occurs, it is likely to be milder.
What causes PUPPP?
Polymorphic eruption of pregnancy is thought to be related to stretching of the skin on the abdomen. The stretching elicits an immune response due to connective tissue damage. Supporting the stretch mark theory are the following observations:
- Most cases begin in the last 3 months, especially the last 5 weeks, when the stretching is greatest.
- The rash usually starts around the umbilicus where stretching of the abdomen is greatest.
- Triplet pregnancies have a higher risk (14%) than twin pregnancies (2.9%).
Another theory considers low-level traffic of fetal cells within the mother’s circulation, which appears increased in women with polymorphic eruption of pregnancy, and may persist for some time after the baby has been born.
PUPPP signs and symptoms
The rash usually begins during the third trimester, in the last few weeks of pregnancy. About 15% of women with polymorphic eruption of pregnancy report that it actually began immediately after delivery.
Small pink papules appear first in the stretch marks around the umbilicus, often with a pale halo around each papule. The papules coalesce to form large, red, urticated (hive-like) plaques, and occasionally small vesicles are present. The rash spreads from the abdomen to involve the buttocks and thighs, and sometimes the arms and legs. Lesions on or above the breasts are rare.
Polymorphic eruption of pregnancy is very itchy (pruritic) and patients find it difficult to sleep at night.
How is PUPPP diagnosed?
The history and clinical findings are usually typical. There are no specific tests. Skin biopsy findings are nonspecific.
PUPPP treatment
There is no curative treatment for polymorphic eruption of pregnancy (apart from delivery!). Symptoms can be controlled using:
- Emollients (moisturizers) applied liberally and frequently as required.
- Topical steroids applied thinly once or twice daily to the red itchy patches.
- A short course of systemic steroids (eg, prednisone), in severe polymorphic eruption of pregnancy.
- Antihistamines – antihistamine tablets appear safe in late pregnancy (though they may make the baby drowsy on delivery).
What causes pemphigoid gestationis?
Pemphigoid gestationis is an autoimmune blistering disease, which basically means that an individual’s immune system starts reacting against his or her own tissue. Immunoglobulin type G (IgG) anti-basement membrane zone auto-antibodies (known as the PG factor) cause the damage.
In pemphigoid gestationis, the target is a protein known as BPAG2 (also called BP 180), found within the basement membrane, which is the zone between the epidermis and the dermis (the top and middle layers of skin). BPAG2 is within the hemidesmosome, the cell component that sticks the epidermal keratinocyte cells to the dermis.
The antibody attack results in inflammation and separation of the epidermis from the dermis allowing fluid to build up and create a blister.
Pemphigoid gestationis is strongly associated with the maternal HLA-DRs DRB1*0301 (HLA-DR3) and DRB1*0401/040X (HLA-DR4) 2. This strong association indicates the important role of MHC class II in the pathogenesis of pemphigoid gestationis.
Pemphigoid gestationis symptoms
Most patients present with an intensely itchy hive-like rash during mid to late pregnancy (13 to 40 weeks gestation).
- Initially, there are itchy red bumps around the belly button
- Within days to weeks, the rash spreads to other parts of the body including the trunk, back, buttock, and arms. The face, scalp, palms, soles and mucous membranes are usually not affected.
- After 2-4 weeks, large, tense fluid-filled blisters form
- Some patients may have no blisters but instead, have plaques (large raised patches)
In some cases, pemphigoid gestationis occurs throughout pregnancy. Symptoms may lessen or spontaneously resolve towards the end of the pregnancy but this is short-lived, as 75-80% of women will experience a flare-up around delivery. In most cases, symptoms resolve days later after giving birth, however, in some, the disease remains active for months or years. Commencement of menstrual periods, use of oral contraceptives or further pregnancies may cause flare-ups.
How is pemphigoid gestationis diagnosed?
Pemphigoid gestationis diagnosis generally requires a skin biopsy, which shows typical features of subepidermal blistering, similar in microscopic appearance to bullous pemphigoid or epidermolysis bullosa acquisita. Pemphigoid gestationis is confirmed by direct immunofluorescence staining of the biopsy to reveal antibodies. It can be distinguished from bullous pemphigoid and epidermolysis bullosa acquisita using salt-split samples of skin. In some cases, circulating antibodies can be detected by a blood test (indirect immunofluorescence test).
Pemphigoid gestationis treatment
Treatment of pemphigoid gestationis depends on the severity and the stage of the skin lesions. The main goal is to relieve itching, to prevent the formation of new blisters and treat secondary infections. Topical corticosteroids are used in mild disease whilst oral corticosteroids are necessary in more extensive cases. Minimum effective doses should be used to reduce the risk of side effects to both mother and fetus.
Pemphigoid gestationis is often treated with topical corticosteroids and oral antihistaminics especially in localized disease with minimal blistering. Patients that are resistant to topical treatment or have a severe form exceeding 10% of the body surface area require systemic corticosteroids. Treatment includes 0.3 mg/kg to 0.5 mg/kg (20 mg to 40 mg/day) of prednisolone, and in some cases, the addition of immunosuppressant agents such as cyclosporine or azathioprine for disease control.
- Oral antihistamines may be used to relieve itching.
- Isolated cases of pemphigoid gestationis have been treated successfully with dapsone or sulfapyridine.
- Immunosuppressive medications such as azathioprine or ciclosporin may also be used successfully but their safety in pregnancy or during breastfeeding must be carefully considered.
- Intravenous immunoglobulins (IVIG) have been utilized successfully in some cases. In one case of chronic gestational pemphigoid resistant to numerous treatments (corticosteroids, dapsone, azathioprine, IVIG), the disease has been controlled successfully with rituximab-anti-CD20 antibodies.
In most cases, pemphigoid gestationis resolves spontaneously within days after delivery so treatment can be tapered off and stopped. Complications are rare but may include:
- Premature delivery
- Transient blistering on the infant that resolves with the clearance of maternal antibodies (about 3-4 months)
- Secondary infection, which may leave scarring
Pemphigoid gestationis prognosis
Pemphigoid gestationis typically regresses without scarring within weeks to months after delivery. Pemphigoid gestationis may recur in subsequent pregnancies and may be precipitated by menses and the use of oral contraceptives.
Mortality/morbidity
No increase in fetal or maternal mortality has been demonstrated. A greater prevalence of premature and small-for-gestational-age babies is associated with pemphigoid gestationis. Of infants, 5-10% born to affected mothers may present with transient cutaneous involvement that resolves as maternal autoantibodies are cleared.
Patients with pemphigoid gestationis have a higher relative prevalence of other autoimmune diseases, including Hashimoto thyroiditis, Graves disease, and pernicious anemia, which are also associated with HLA-DR3 and DR-4 haplotypes.
- Pemphigoid gestationis. https://www.dermnetnz.org/topics/pemphigoid-gestationis/[↩]
- Gossman W, Gandhi GR, Gharbi A, et al. Pemphigoid Gestationis. [Updated 2019 Jul 11]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2019 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK470287[↩][↩]
- Cobo MF, Santi CG, Maruta CW, Aoki V. Pemphigoid gestationis: clinical and laboratory evaluation. Clinics (Sao Paulo). 2009;64(11):1043–1047. doi:10.1590/S1807-59322009001100002 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2780519[↩]