What is Rocky Mountain spotted fever
Rocky Mountain spotted fever caused by the bacteria Rickettsia rickettsii that is spread through the bite on an infected tick. Most people who get sick with Rocky Mountain spotted fever will have a fever, headache, and rash. Rocky Mountain spotted fever is the most severe rickettsiosis in the United States and can be deadly if not treated early with the right antibiotic.
Rocky Mountain spotted fever is a rapidly progressive disease and without early administration of doxycycline can be fatal within days.
- Treatment with doxycycline antibiotic usually cures the infection. But about 3% of people who get Rocky Mountain spotted fever will die.
Contrary to the name “Rocky Mountain,” most recent cases have been reported in the eastern United States, including North and South Carolina, Virginia, Georgia, Tennessee, and Oklahoma. Most cases occur in the spring and summer and are found in children.
Risk factors include recent hiking or exposure to ticks in an area where the disease is known to occur. The bacteria are unlikely to be transmitted to a person by a tick that has been attached for less than 20 hours. Only about 1 in 1,000 wood and dog ticks carry the bacteria. Bacteria can also infect people who crush ticks they have removed from pets with their bare fingers.
Rocky Mountain spotted fever the most severe spotted fever rickettsiosis in the United States. Similar, but less severe diseases caused by closely related bacteria can be easily confused with Rocky Mountain spotted fever. Other spotted fevers in the United States include:
- Rickettsia parkeri rickettsiosis, caused by parkeri
- Pacific Coast tick fever, caused by Rickettsia species 364D
- Rickettsialpox, caused by Rickettsia akari
These diseases share many signs and symptoms, including fever, headache, and rash, but are typically less severe than Rocky Mountain spotted fever. Patients with these spotted fevers can also show signs of an eschar (dark necrotic scab at the site of the arthropod bite). Eschars are not common in cases of Rocky Mountain spotted fever.
Rocky Mountain spotted fever transmission
Rocky Mountain spotted fever is a serious tickborne illness which can be deadly if not treated early. Rocky Mountain spotted fever is spread by several species of ticks in the United States, including:
- American dog tick (Dermacentor variabilis) (Figure 1), widely distributed east of the Rocky Mountains and in portions of the Pacific Coast.
- Rocky Mountain wood tick (Dermacentor andersoni) (Figure 2), in the Rocky Mountain region.
- Brown dog ticks (Rhipicephalus sanguineus) (Figure 3) can be found worldwide and serves as the primary vector of Rocky Mountain spotted fever in parts of the southwestern United States and Mexico.
Rocky Mountain spotted fever cases occur throughout the United States, but are most commonly reported from North Carolina, Tennessee, Missouri, Arkansas, and Oklahoma.
Blood transfusion or organ transplant
- Transmission of Rickettsia rickettsii through blood transfusion is extremely rare.
- Organ transplant acquired Rocky Mountain spotted fever has not been documented, but is physiologically possible.
Figure 1. Rocky Mountain spotted fever tick – American dog tick (Dermacentor variabilis)
Figure 2. Rocky Mountain spotted fever tick – Rocky Mountain wood tick (Dermacentor andersoni)
Figure 3. Rocky Mountain spotted fever tick – brown dog tick (Rhipicephalus sanguineus)
Rocky Mountain spotted fever prevention
- There is no vaccine to prevent Rocky Mountain spotted fever. Prevent illness by preventing tick bites, preventing ticks on your pets, and preventing ticks in your yard.
- Ticks live in grassy, brushy, or wooded areas, or even on animals, so spending time outside camping, gardening, or hunting will bring you in close contact with ticks. Protect yourself, your family, and your pets. Here’s how:
Before You Go Outdoors
- Know where to expect ticks. Ticks live in grassy, brushy, or wooded areas, or even on animals, so spending time outside camping, gardening, or hunting could bring you in close contact with ticks. Many people get ticks in their own yard or neighborhood.
- Treat clothing and gear with products containing permethrin. Permethrin can be used to treat boots, clothing and camping gear and remain protective through several washings.
- Use Environmental Protection Agency (EPA)-registered insect repellents containing DEET, picaridin, IR3535, Oil of Lemon Eucalyptus, or 2-undecanone. Environmental Protection Agency’s helpful search tool (https://www.epa.gov/insect-repellents/find-repellent-right-you) can help you find the product that best suits your needs. Always follow product instructions.
- Do NOT use insect repellent on babies younger than 2 months old.
- Do NOT use products containing oil of lemon eucalyptus (OLE) or para-menthane-diol (PMD) on children under 3 years old.
- Avoid Contact with Ticks
- Avoid wooded and brushy areas with high grass and leaf litter.
- Walk in the center of trails.
After You Come Indoors
- Check your clothing for ticks. Ticks may be carried into the house on clothing. Any ticks that are found should be removed. Tumble dry clothes in a dryer on high heat for 10 minutes to kill ticks on dry clothing after you come indoors. If the clothes are damp, additional time may be needed. If the clothes require washing first, hot water is recommended. Cold and medium temperature water will not kill ticks effectively.
- Shower soon after being outdoors. Showering within two hours of coming indoors has been shown to reduce your risk of getting Lyme disease. Showering may help wash off unattached ticks and it is a good opportunity to do a tick check.
- Check your body for ticks after being outdoors. Conduct a full body check upon return from potentially tick-infested areas, which even includes your back yard. Use a hand-held or full-length mirror to view all parts of your body. Check these parts of your body and your child’s body for ticks:
- Under the arms
- In and around the ears
- Inside belly button
- Back of the knees
- In and around the hair
- Between the legs
- Around the waist
- Examine gear and pets. Ticks can ride into the home on clothing and pets, then attach to a person later, so carefully examine pets, coats, and daypacks.
What to Do if You Find an Attached Tick
If you find a tick attached to your skin, there’s no need to panic—the key is to remove the tick as soon as possible. There are several tick removal devices on the market, but a plain set of fine-tipped tweezers work very well.
How to remove a tick
- Use fine-tipped tweezers to grasp the tick as close to the skin’s surface as possible.
- Pull upward with steady, even pressure. Don’t twist or jerk the tick; this can cause the mouth-parts to break off and remain in the skin. If this happens, remove the mouth-parts with tweezers. If you are unable to remove the mouth easily with clean tweezers, leave it alone and let the skin heal.
- After removing the tick, thoroughly clean the bite area and your hands with rubbing alcohol or soap and water.
- Never crush a tick with your fingers. Dispose of a live tick by putting it in alcohol, placing it in a sealed bag/container, wrapping it tightly in tape, or flushing it down the toilet.
Avoid folklore remedies such as “painting” the tick with nail polish or petroleum jelly, or using heat to make the tick detach from the skin. Your goal is to remove the tick as quickly as possible–not waiting for it to detach.
Testing of ticks
People who have removed a tick sometimes wonder if they should have it tested for evidence of infection. Although some commercial groups offer testing, in general this is not recommended because:
- Laboratories that conduct tick testing are not required to have the high standards of quality control used by clinical diagnostic laboratories. Results of tick testing should not be used for treatment decisions.
- Positive results showing that the tick contains a disease-causing organism do not necessarily mean that you have been infected.
- Negative results can lead to false assurance. You may have been unknowingly bitten by a different tick that was infected.
- If you have been infected, you will probably develop symptoms before results of the tick test are available. If you do become ill, you should not wait for tick testing results before beginning appropriate treatment.
Follow-up
Watch for signs of illness such as rash or fever in the days and weeks following the bite, and see a health care provider if these develop. Your risk of acquiring a tick-borne illness depends on many factors, including where you live, what type of tick bit you, and how long the tick was attached. If you become ill after a tick bite, see a health care provider.
Reduce Ticks in Your Yard
- Modify your landscape to create Tick-Safe Zones. The Connecticut Tick Management Handbook (http://www.ct.gov/caes/lib/caes/documents/special_features/tickhandbook.pdf) provides valuable advice for preventing blacklegged ticks in the yard. Similar steps may also help reduce other types of ticks in and around the yard. Regularly remove leaf litter and clear tall grasses and brush around homes, and place wood chips or gravel between lawns and wooded areas to keep ticks away from recreational areas, and keep play areas and playground equipment away from away from shrubs, bushes, and other vegetation.
- Consider using a chemical control agent. Effective tick control chemicals are available for use by the homeowner, or they can be applied by a professional pest control expert, and even limited applications can greatly reduce the number of ticks. A single springtime application of acaricide can reduce the population of ticks that cause Lyme disease by 68–100%.
- Discourage deer. Removing plants that attract deer and constructing physical barriers may help discourage deer from entering your yard and bringing backlegged ticks with them.
Prevent Ticks on Animals
Use tick control products to prevent family pets from bringing ticks into the home. Tick collars, sprays, shampoos, oral medications, or “top spot” medications should be used regularly to protect your animals and your family from ticks. Consult your veterinarian and be sure to use these products according to the package instructions.
Rocky Mountain spotted fever symptoms
Signs and symptoms of Rocky Mountain spotted fever begin 3-12 days after the bite of an infected tick. However, because tick bites are not painful, many people do not remember being bitten. Illness generally begins with sudden onset of fever and headache and most people visit a healthcare provider during the first few days of symptoms.
Early signs and symptoms are not specific to Rocky Mountain spotted fever (including fever and headache). However, the disease can rapidly progress to a serious and life-threatening illness. See your health care provider if you become ill after having been bitten by a tick or having been in the woods or in areas with high brush where ticks commonly live.
Signs and symptoms can include:
- Fever
- Headache
- Rash
- Nausea
- Vomiting
- Stomach pain
- Muscle pain
- Lack of appetite
Early illness (days 1-4)
- Fever
- Headache
- Gastrointestinal symptoms (nausea, vomiting, anorexia)
- Abdominal pain (may mimic appendicitis or other causes of acute abdominal pain)
- Myalgia
- Rash (typically occurs 2-4 days after the onset of fever)
- Edema around the eyes and on the back of hands
Late illness (day 5 or later)
- Altered mental status, coma, cerebral edema
- Respiratory compromise (pulmonary edema, acute respiratory distress syndrome)
- Necrosis, often requiring amputation
- Multiorgan system damage (CNS, renal failure)
Risk factors for severe illness
- Delayed treatment
- Children < 10 years
- Persons with glucose-6-phosphate dehydrogenase (G6PD) deficiency
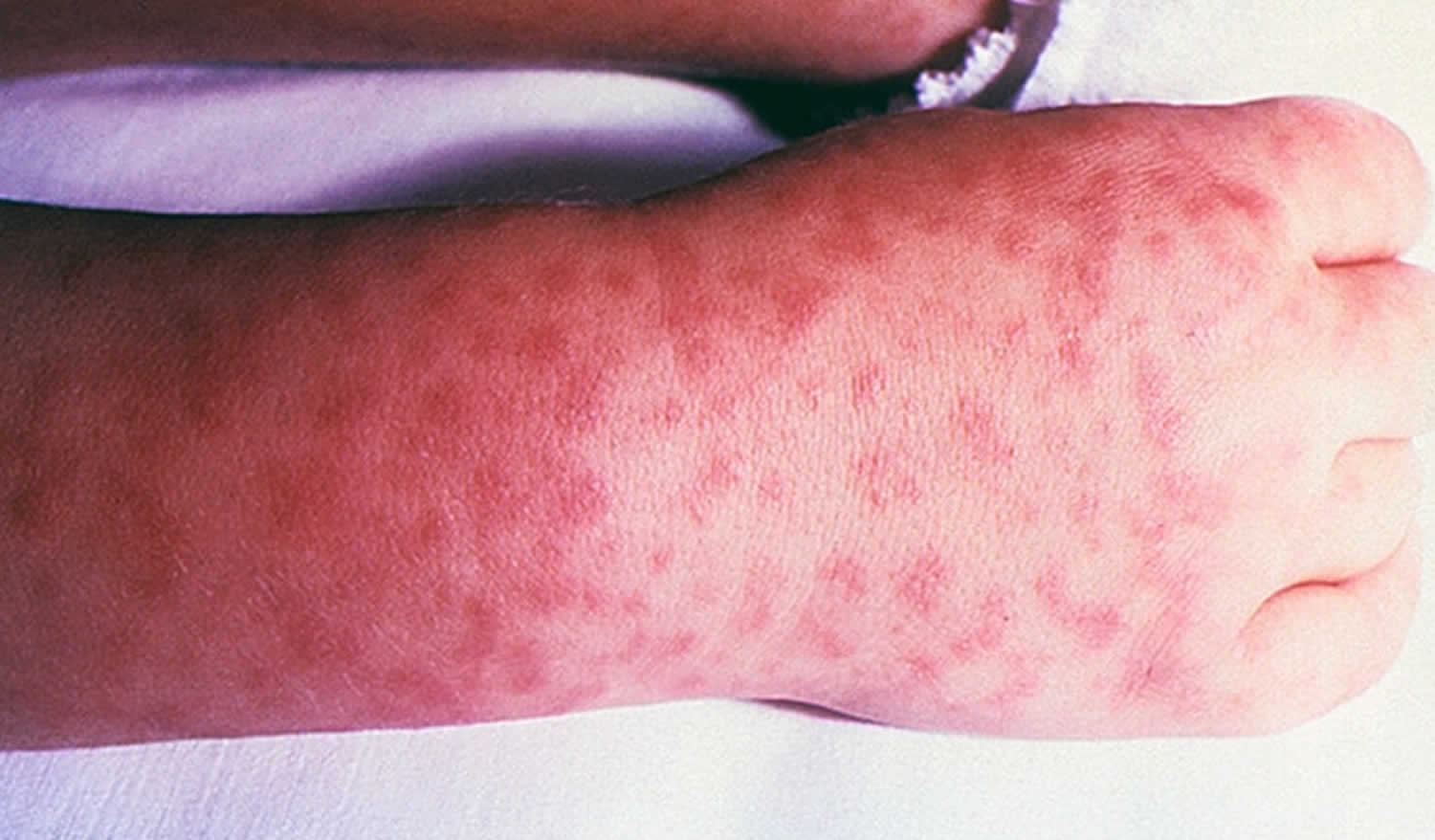
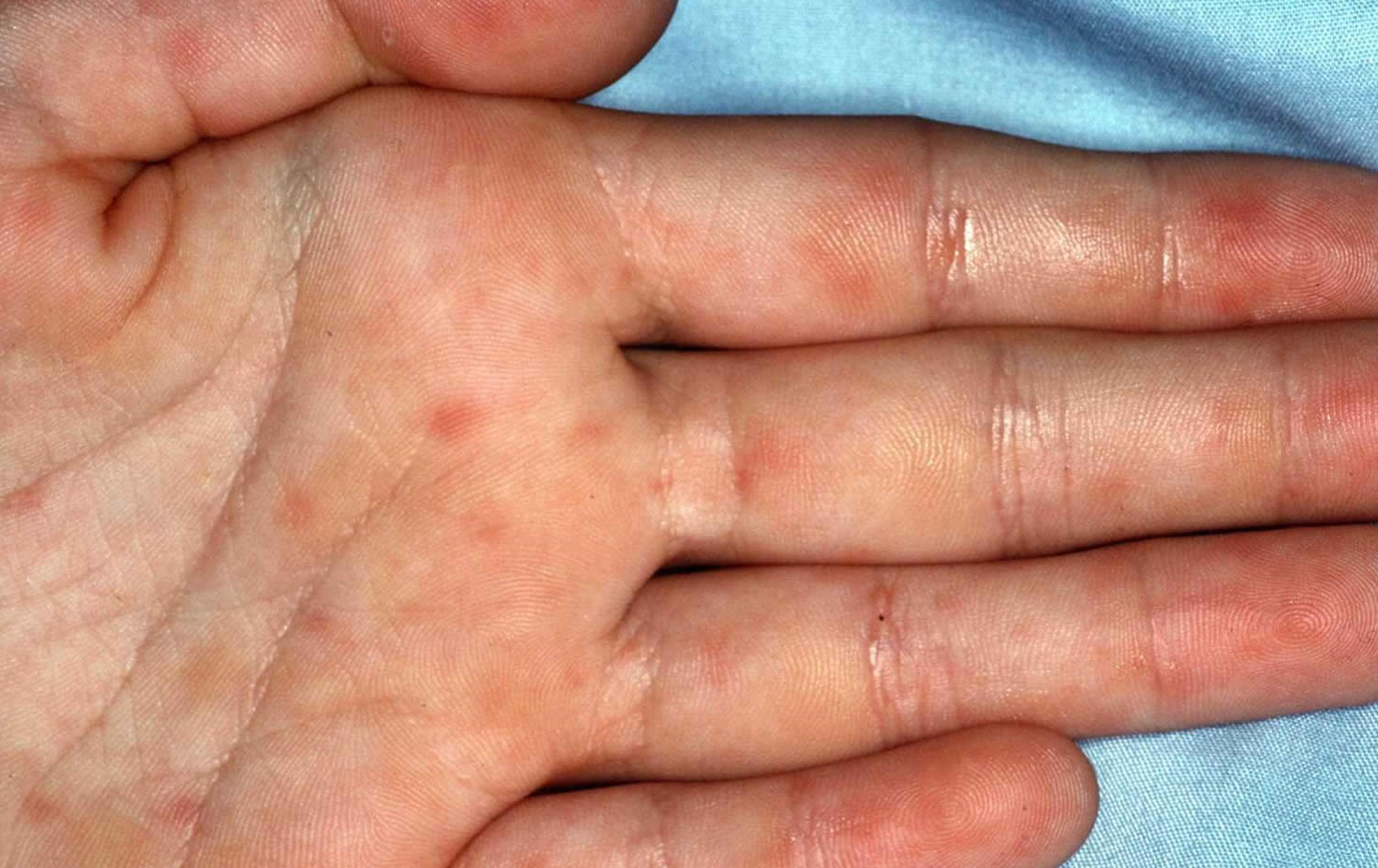
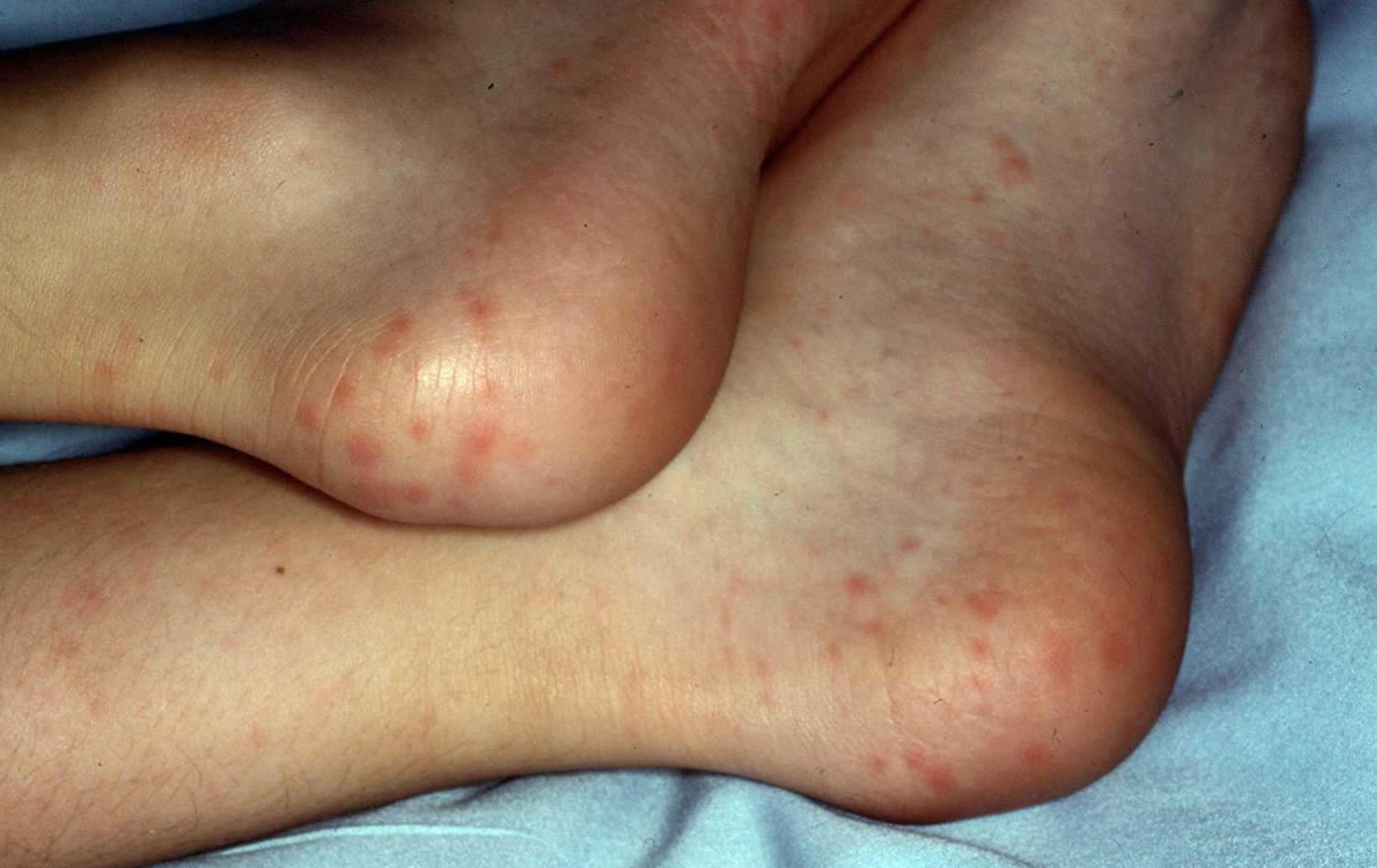
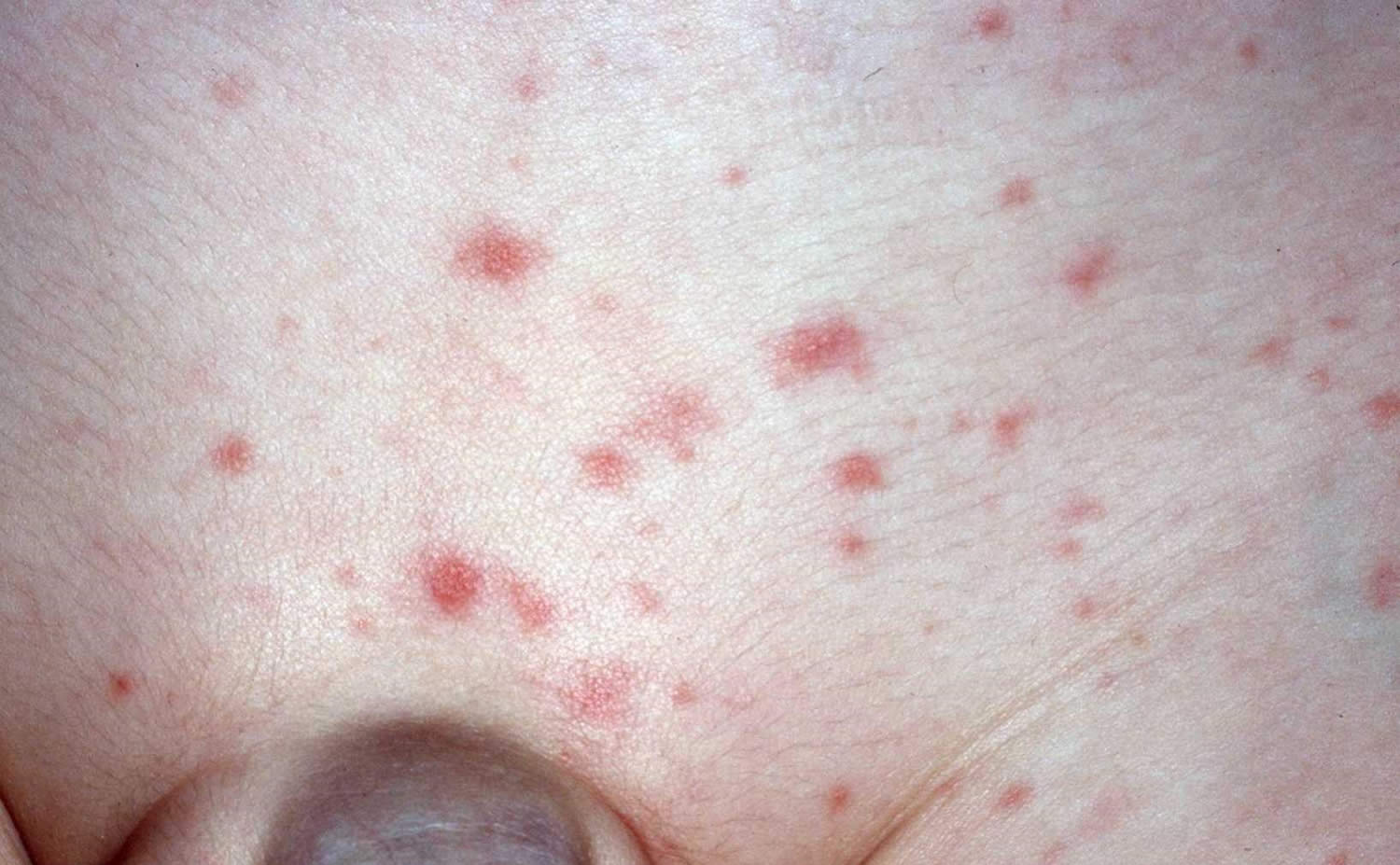
Rocky Mountain spotted fever rash
Rash is a common sign in people who are sick with Rocky Mountain spotted fever. Rash usually develops 2-4 days after fever begins. The look of the rash can vary widely over the course of illness. Some rashes can look like red splotches and some look like pinpoint dots. While almost all patients with Rocky Mountain spotted fever will develop a rash, it often does not appear early in illness, which can make Rocky Mountain spotted fever difficult to diagnose.
Early Rash
- A classic case of Rocky Mountain spotted fever involves a rash that appears 2-4 days after the onset of fever as small, flat, pink, macules on the wrists, forearms, and ankles and spreads to include the trunk and sometimes the palms of hands and soles of feet.
- Rash can be highly variable and people who fail to develop a rash, or develop an atypical rash, are at increased risk of being misdiagnosed.
Late Rash
- The petechial rash of Rocky Mountain spotted fever does not typically appear until day 5-6 of illness.
- NOTE: Petechiae are a sign of severe disease. Every attempt should be made to treat before petechiae develop.
Figure 4. Rocky Mountain spotted fever rash
Rocky Mountain spotted fever long term effects
Rocky Mountain spotted fever does not result in chronic or persistent infections.
Rickettsia rickettsii bacteria infects the endothelial cells that line the blood vessels causing vasculitis. As infection continues, bleeding or clotting in the brain or other vital organs may occur.
Some patients who recover from severe Rocky Mountain spotted fever may be left with permanent damage, including amputation of arms, legs, fingers, or toes (from damage to blood vessels in these areas); hearing loss; paralysis; or mental disability. Any permanent damage is caused by the acute illness and does not result from a chronic infection.
Patients who had severe Rocky Mountain spotted fever requiring prolonged hospitalization may have long-term health problems caused by disease:
- Neurological deficits
- Damage to internal organs
- Vascular damage requiring amputation:
- Loss of fluid from damaged vessels can result in loss of circulation to the extremities, fingers, toes or even limbs. Irreversible injury by ischemic damage may result in amputation of damaged tissue or digits.
Those who do not have this kind of vascular damage in the initial stages of the disease typically experience a full recovery.
Rocky Mountain spotted fever diagnosis
The health care provider will perform a physical examination and ask about the symptoms.
Rocky Mountain spotted fever can be difficult to diagnose because the early signs and symptoms are similar to those caused by many other diseases.
Laboratory tests can check a blood sample, rash specimen or the tick itself for evidence of the organism that causes the infection. Because early treatment with antibiotics is so important, doctors don’t wait for these test results before starting treatment if Rocky Mountain fever is strongly suspected.
- The signs and symptoms of Rocky Mountain spotted fever are similar to those of many other diseases. See your health care provider if you develop any of the signs or symptoms of Rocky Mountain spotted fever.
- Be sure to tell your health care provider if you become ill and have recently been bitten by a tick or have spent time in areas where ticks may be found.
- Your health care provider may order certain blood tests to look for evidence of Rocky Mountain spotted fever.
- The results of these tests can take weeks. If your health care provider thinks your illness might be Rocky Mountain spotted fever, he or she should recommend antibiotic treatment before test results are available.
Tests that may be done include:
- Antibody titer by complement fixation or immunofluorescence
- Complete blood count (CBC)
- Kidney function tests
- Partial thromboplastin time (PTT)
- Prothrombin time (PT)
- Skin biopsy taken from the rash to check for Rickettsia rickettsii
- Urinalysis to check for blood or protein in the urine
Rocky Mountain spotted fever treatment
Rocky Mountain spotted fever can be life-threatening. People who develop Rocky Mountain spotted fever are much more likely to avoid complications if treated within five days of developing symptoms. That’s why your doctor will probably have you begin antibiotic therapy before receiving conclusive test results.
Early treatment with the antibiotic doxycycline (e.g., Monodox, Vibramycin, others) can prevent death and severe illness.
Doxycycline is the recommended antibiotic treatment for Rocky Mountain spotted fever in adults and children of all ages, but doxycycline is not a good choice if you’re pregnant. In that case, your doctor may prescribe chloramphenicol as an alternative.
Treatment duration
- When treated with doxycycline, fever generally subsides within 24–48 hours.
- Severely ill patients may require longer periods of treatment before fever will resolve, especially if they have experienced damage to organ systems.
- Resistance to doxycycline or relapses in symptoms after the completion of the recommended course has not been documented.
Recommended Treatment and Dosage for Rocky Mountain spotted fever
- Doxycycline is the first-line treatment for adults and children of all ages:
- Adults: 100 mg every 12 hours
- Children under 45 kg (100 lbs): 2.2 mg/kg body weight given twice a day
Patients with suspected Rocky Mountain spotted fever should be treated with doxycycline for at least 3 days after the fever subsides and there is evidence of clinical improvement. Minimum course of treatment is 5-7 days.
Treating Children and Pregnant Women
- Doxycycline is the drug of choice recommended by both Centers for Disease Control and Prevention (CDC) and the American Academy of Pediatrics Committee on Infectious Diseases to treat suspected rickettsial disease in children.
- A recent study found that short courses of doxycycline (5–10 days) did not result in staining of permanent teeth or enamel hypoplasia. Use doxycycline as the first-line treatment for suspected Rocky Mountain spotted fever in patients of all ages.
- Use of antibiotics other than doxycycline increases the risk of severe illness and death.
Other Treatments
- Doxycycline should be used whenever possible.
- In cases of severe doxycycline allergy, rapid desensitization procedures in an inpatient setting may be considered. Physicians should carefully weigh the benefits of doxycycline use and the risks of adverse effects on a case-by-case basis with an infectious disease or other specialist.
- Chloramphenicol is the only alternative drug used to treat Rocky Mountain spotted fever; however, epidemiologic studies suggest that Rocky Mountain spotted fever patients treated with chloramphenicol are at higher risk for death than people who received a tetracycline-class antibiotic.
- Oral formulations of chloramphenicol are not available in the United States, and use of this drug carries the potential for other adverse risks, such as aplastic anemia and Grey baby syndrome.
- The use of sulfa-containing drugs may worsen clinical course and increase the likelihood of death from Rocky Mountain spotted fever.
- Other antibiotics, including almost all other classes of broad- spectrum antibiotics, are not effective in treating Rocky Mountain spotted fever.
- The most current evidence-based information indicate that the use of doxycycline during pregnancy is unlikely to pose substantial teratogenic effects; nonetheless, it is still not possible to conclude that no risk exists. Pregnant patients should be counseled on the potential risks versus benefits when making a treatment decision.
- Healthcare providers should be cautious when exploring treatments other than doxycycline, which is highly effective in treating multiple tickborne diseases including anaplasmosis, ehrlichiosis, Lyme disease, and other spotted fever group rickettsioses (spotted fevers).
Antibiotics as Prophylaxis
- Post-tick bite antibiotic prophylaxis is not recommended to prevent Rocky Mountain spotted fever.
- People who were bitten by a tick should be advised to watch for signs and symptoms and see their healthcare provider if fever, rash, or other symptoms develop within two weeks of tick bite.
- Treatment for asymptomatic individuals is not currently recommended.