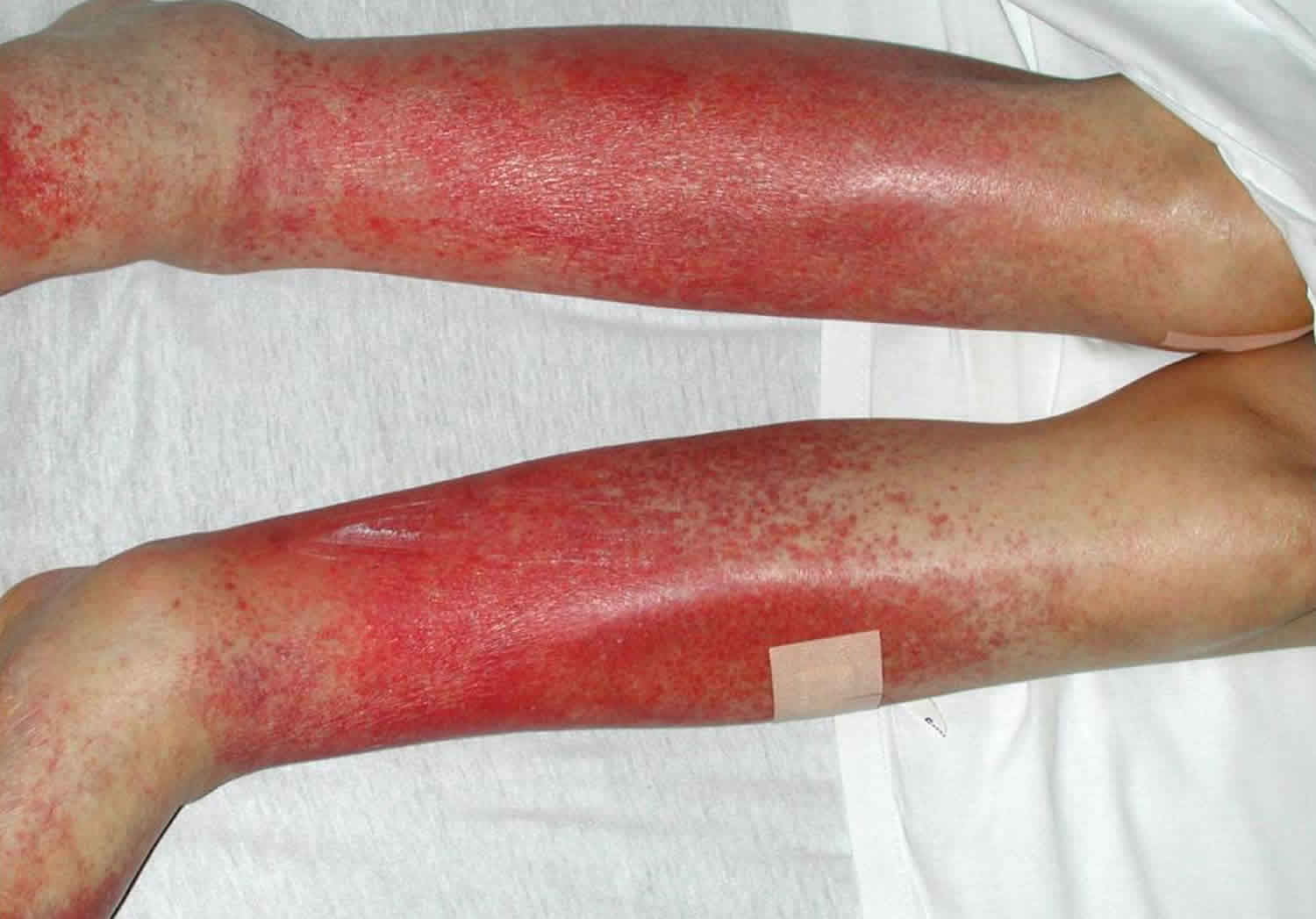
Schamberg disease
Schamberg disease also called progressive pigmented purpuric dermatosis, is a type of pigmented purpuric dermatosis, progressive pigmented purpura or capillaritis that is characterized by red-brown purpuric macules that are known as ‘cayenne pepper’ spots 1. Schamberg disease is a harmless skin condition in which there are reddish-brown patches caused by leaky capillaries. Schamberg disease usually develops insidiously on one or both lower legs and onset occurs on average in the fifth decade of life. However, some authors have suggested that Schamberg disease is relatively common in children, sometimes occurring before puberty 2. Torrelo et al 2 reviewed 13 cases of Schamberg disease that occurred before 10 years of age and found that it predominantly occurred in girls, consistently involved the lower limbs, and was a chronic persistent disease. A case of a 1-year-old infant with Schamberg disease has also been reported 3. Regular or irregular crops of red-brown flat patches with cayenne pepper spots on their borders appear for no apparent reason 4. Although most common on the lower legs, the Schamberg form of capillaritis can arise on any part of the body. It is usually irregularly distributed on both sides with few or many patches. There are no symptoms.
Schamberg disease was first described in 1901 5. The rash, which corresponds to extravasation of erythrocytes, usually appears on the lower legs but may spread to involve the thighs, abdomen and occasionally the arms. Although the exact pathogenesis of Schamberg disease is unknown, the capillary damage and consequent erythrocyte extravasation appear to be the result of a localized cell-mediated immune injury induced by a skin-specific subset of helper T lymphocytes 6. Histology shows superficial subepithelial and perivascular infiltration of lymphocytes and rarely macrophages without overt vasculitis 7. The cardinal feature differentiating Schamberg disease from other purpuric eruptions is the characteristic nonpalpable punctate purpura and orange-brown pigmentation resulting from extravasation of erythrocytes and hemosiderin deposition in the superficial dermis 7.
Drugs are important precipitating factors for Schamberg disease, with acetaminophen the most commonly implicated drug 8. Unlike the idiopathic form of Schamberg disease, most drug-induced cases resolve quickly after the offending drug is stopped 8.
Schamberg disease causes
The cause of Schamberg disease has yet to be elucidated, but current evidence suggests the involvement of cytokine and cell-mediated immunity 9. Familial presentation is very rare; however, there have been case reports documenting a possible autosomal-dominant inheritance pattern 10. A number of precipitating factors have been reported: venous hypertension; exercise and gravitational dependency; capillary fragility; allergy to dyes, clothing, or alcohol; focal infections; and drug exposure 9. Medications that are commonly linked with Schamberg disease are listed below. Pigmented purpuric dermatoses have also been associated with other medical conditions, including hepatic disease, malignancies, diabetes mellitus, hyperlipidemia, rheumatoid arthritis, lupus erythematous, thyroid dysfunction, hereditary spherocytosis, hematological disorders, and porphyrias 9.
Drugs associated with Schamberg disease or progressive pigmented purpuric dermatosis 11:
- Acetaminophen
- Acetylsalicylic acid
- Carbromal
- Chlordiazepoxide
- Glipizide
- Glybuzole
- Hydralazine HCl
- Meprobamate
- Dipyridamole
- Reserpine
- Thiamine
- Interferon alfa
- Medroxyprogesterone acetate
Drugs are important precipitating factors for Schamberg disease, with acetaminophen the most commonly implicated drug 8. Unlike the idiopathic form of Schamberg disease, most drug-induced cases resolve quickly after the offending drug is stopped 8.
Schamberg disease diagnosis
There are currently no established guidelines for the investigation of Schamberg disease. When diagnosis is unclear, complete blood count, peripheral blood smear, platelet count and function, prothrombin time, partial thromboplastin time, erythrocyte sedimentation rate, antinuclear antibody, and rheumatoid factor should be considered to exclude other causes of purpura 11. A skin biopsy is useful to confirm the clinical diagnosis and to rule out other potentially serious conditions that can mimic Schamberg disease.
Schamberg disease differential diagnosis
The differential diagnosis of Schamberg disease includes stasis dermatitis, leukocytoclastic vasculitis, purpuric contact dermatitis, and early mycosis fungoides (Table 1).
Stasis dermatitis is a complication of long-standing venous insufficiency and is commonly associated with hyperpigmentation, varicose veins, and dependent edema. Scaling, crusting, and ulcerations might be present, but the characteristic punctate petechiae of Schamberg disease are not observed.
Leukocytoclastic vasculitis, also known as hypersensitivity vasculitis, is a small-vessel vasculitis named after its diagnostic histopathology on skin biopsy. It might localize to the skin or be accompanied by systemic manifestations. Cutaneous vasculitis presents as painful palpable purpura on the lower extremities, which can occasionally ulcerate 12. Evidence of autoimmune diseases, acute or chronic illnesses, and ingestion of drugs with known causative associations might be suggestive of this disorder. Skin biopsy confirms the diagnosis.
Purpuric contact dermatitis, an allergic or toxic reaction to textile dyes and resins, can produce purpuric macules, papules, patches, and nodules 13. Diagnosis is usually prompted by the distribution and appearance of the lesions along with a history of exposure. Patch testing can be helpful for confirmation; however, avoidance of the suspected textile can be both diagnostic and therapeutic 13.
Mycosis fungoides is a cutaneous T-cell lymphoma with a potential for lymphatic and hemopoietic involvement 14. It initially presents as erythematous patches affecting the lower trunk and buttocks, and progresses to infiltrated plaques and tumors 14. Diagnosis is confirmed by skin biopsy.
Table 1. Differential diagnoses for Schamberg disease
| DIAGNOSIS | CLINICAL CHARACTERISTICS | CONFIRMATION |
|---|---|---|
| Progressive pigmentary dermatoses | Nonpalpable cayenne pepper–like purpura on an orange-brown macular base | Biopsy only if clinical diagnosis is in question |
| Stasis dermatitis | Hyperpigmentation, varicose veins, dependent edema; scaling, crusting, and ulcerations might be present | Underlying venous insufficiency |
| Leukocytoclastic vasculitis | Painful palpable purpura on lower extremities, which might ulcerate | Skin biopsy |
| Purpuric contact dermatitis | Purpuric macules, papules, patches, and nodules following textile distribution | Avoidance of suspected contactant |
| Early mycosis fungoides | Initial erythematous patches affecting lower trunk and buttocks, progressing to infiltrated plaques and tumors | Skin biopsy |
Schamberg disease treatment
Although diagnosis is quite straightforward, Schamberg disease are slow to resolve and rather resistant to treatment. As Schamberg disease can be quite distressing, it is important for doctors to reassure patients that Schamberg disease are benign disorders with no systemic complications 11. There is no current medical intervention shown to be beneficial; however, topical corticosteroids and antihistamines might alleviate pruritus, and the use of compression stockings is recommended 9. Individual case reports have documented success with immunomodulating therapies such as psoralen photochemotherapy, griseofulvin, pentoxifylline, and cyclosporine 9. Current recommendations suggest discontinuing suspected provoking factors and beginning a trial of topical corticosteroids for 4 to 6 weeks 9.
- Park JH, Kang HY. Generalized schamberg disease in a child. Ann Dermatol. 2013;25(4):524–525. doi:10.5021/ad.2013.25.4.524 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3870235[↩]
- Torrelo A, Requena C, Mediero IG, Zambrano A. Schamberg’s purpura in children: a review of 13 cases. J Am Acad Dermatol. 2003;48:31–33.[↩][↩]
- Zvulunov A, Avinoach I, Hatskelzon L, Halevy S. Pigmented purpuric dermatosis (Schamberg’s purpura) in an infant. Dermatol Online J. 1999;5:2.[↩]
- Capillaritis. https://dermnetnz.org/topics/capillaritis/[↩]
- Chatterjee S. Schamberg disease: uncommon reaction to a common drug. CMAJ. 2009;181(12):E275. doi:10.1503/cmaj.081929 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2789147[↩]
- Smoller BR, Kamel OW. Pigmented purpuric eruptions: immunopathologic studies supportive of a common immunophenotype. J Cutan Pathol. 1991;18:423–7.[↩]
- Sardana K, Sarkar R, Sehgal VN. Pigmented purpuric dermatoses: an overview. Int J Dermatol. 2004;43:482–8.[↩][↩]
- Schroeder-Devere T. Pigmented purpuric dermatoses. In: Wolff K, Goldsmith LA, Katz SI, et al., editors. Fitzpatrick’s dermatology in general medicine. 7th ed. New York (NY): McGraw-Hill; 2008. pp. 1633–7.[↩][↩][↩][↩]
- Sardana K, Sarkar R, Sehgal VN. Pigmented purpuric dermatoses: an overview. Int J Dermatol. 2004;43(7):482–8.[↩][↩][↩][↩][↩][↩]
- Sethuraman G, Sugandhan S, Bansal A, Das AK, Sharma VK. Familial pigmented purpuric dermatoses. J Dermatol. 2006;33(9):639–41.[↩]
- Ho C, Yan P, Mistry N, Hong CH. Answer: Can you identify this condition?. Can Fam Physician. 2010;56(10):1024–1025. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2954085[↩][↩][↩]
- Gonzalez-Gay MA, Garcia-Porrua C, Pujol RM. Clinical approach to cutaneous vasculitis. Curr Opin Rheumatol. 2005;17(1):56–61.[↩]
- Lazarov A, Cordoba M. Purpuric contact dermatitis in patients with allergic reaction to textile dyes and resins. J Eur Acad Dermatol Venereol. 2000;14(2):101–5.[↩][↩]
- Lenane P, Powell FC, O’Keane C, Dervan P, O’Sullivan D, Bourke E, et al. Mycosis fungoides—a review of the management of 28 patients and of the recent literature. Int J Dermatol. 2007;46(1):19–26.[↩][↩]