What is trichoepithelioma
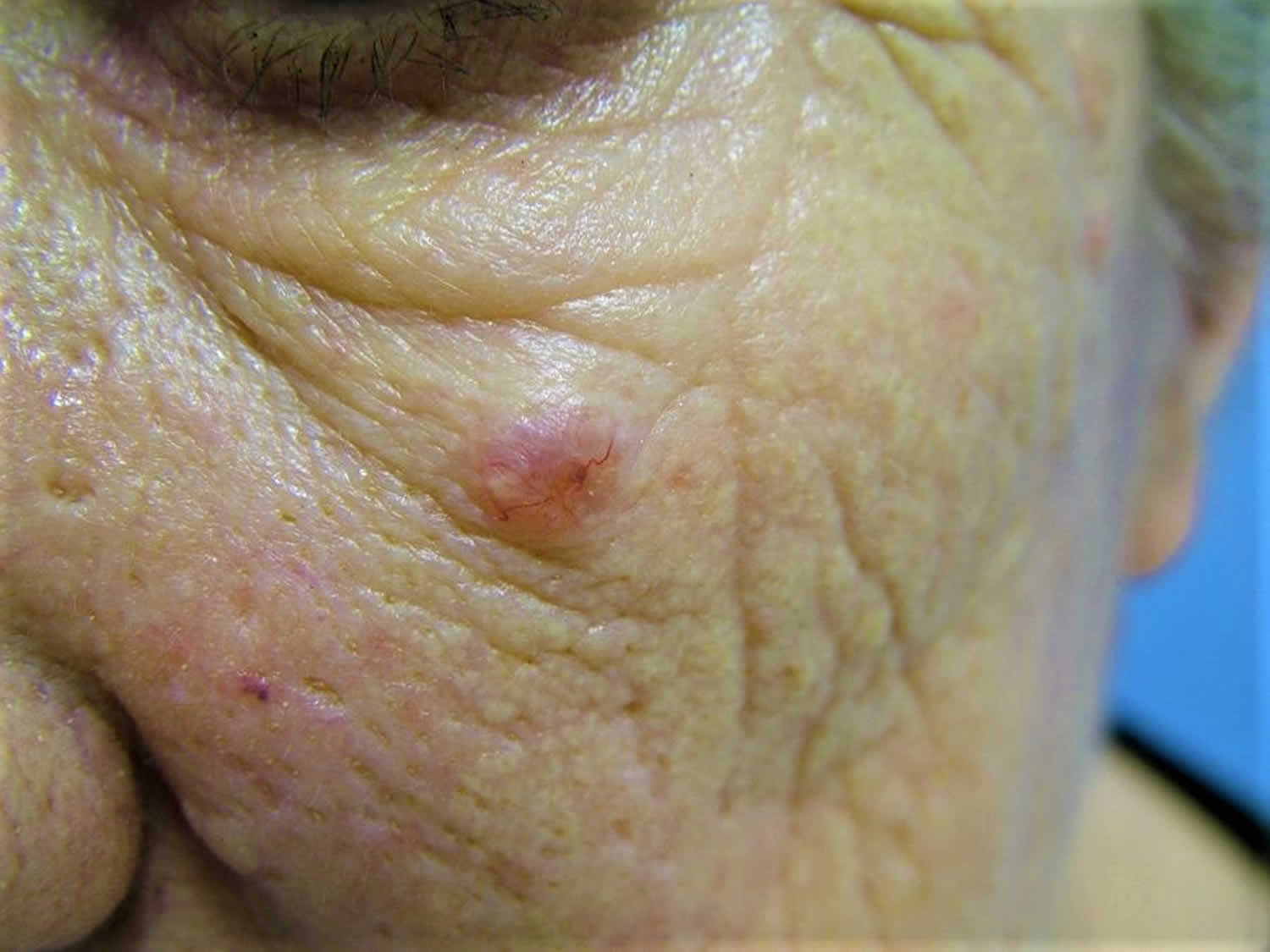
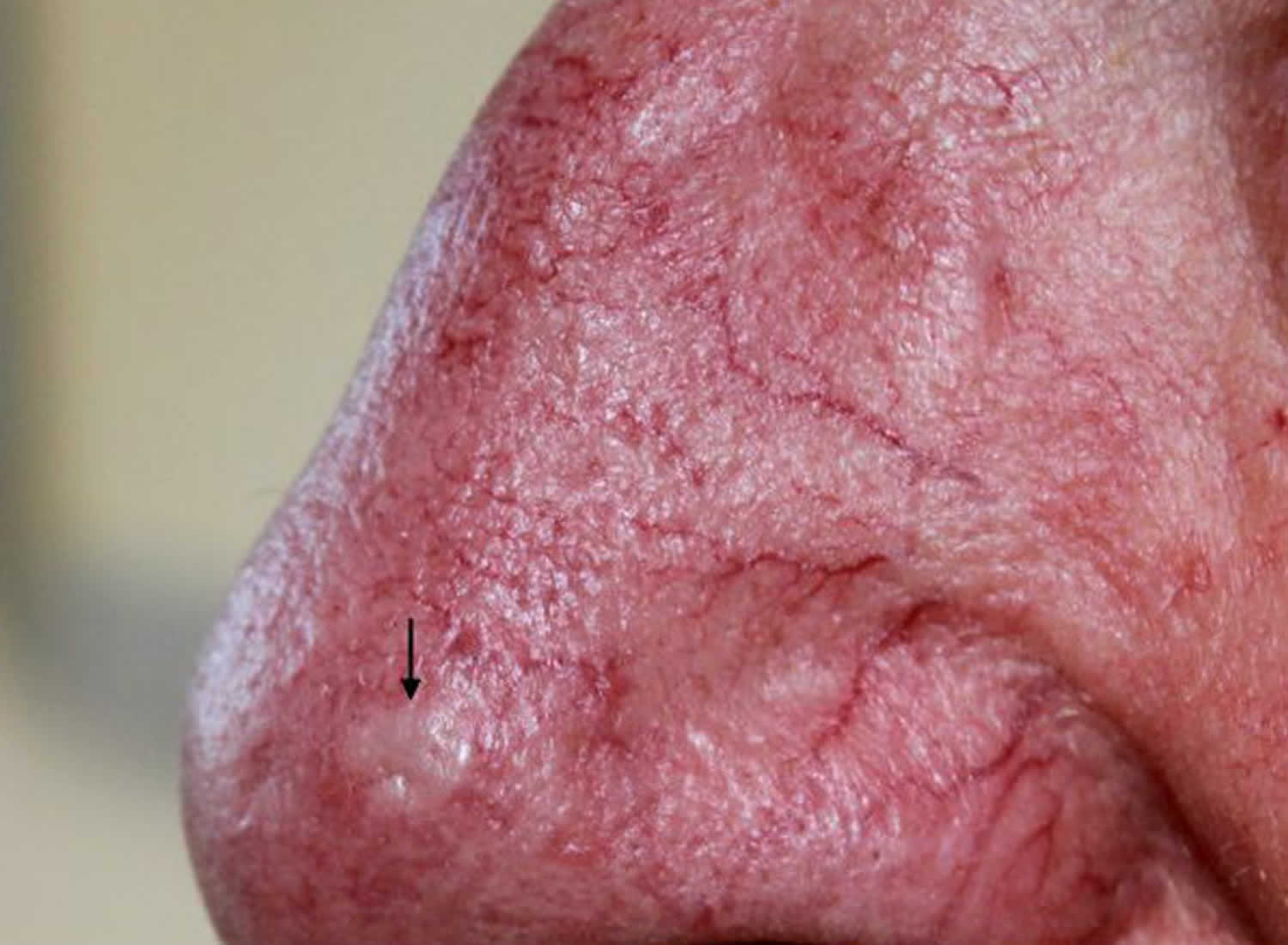
Trichoepitheliomas are benign (harmless) tumors that arise from the walls of the hair follicle on the face after puberty 1. The tumor cells form rudimentary hair follicles but do not form actual hair shafts. Trichoepithelioma are small (usually less than one centimeter), firm, rounded and shiny. Trichoepitheliomas may be yellow, pink, brown or bluish. They usually gradually increase in number with age, occurring on both cheeks, eyelids and around the nose.
Trichoepithelioma typically occurs in young to aging adults; however, the hereditary form may be seen in younger individuals. A single case study has reported a congenital lesion of desmoplastic trichoepithelioma 2.
Trichoepithelioma can be classified into three varieties: solitary, multiple, and desmoplastic 3. Multiple variants are far more common than the solitary ones. Multiple trichoepitheliomas are usually inherited and maybe associated with Spiegler-Brookler syndrome 4. The desmoplastic trichoepithelioma which is a solitary ring-shaped shiny lesion and is usually excised because it can look like a basal cell carcinoma (BCC). Solitary trichoepithelioma does not follow an inheritance pattern and is usually firm, nonulcerated nodule usually <2 cm in diameter. It appears most commonly in middle-aged individuals and most commonly on the face 4.
Solitary trichoepitheliomas may be confused clinically and pathologically with basal cell carcinoma (BCC), which is more common but usually arises as a solitary tumor. The distinction between BCC and trichoepithelioma is clinically important since a basal cell carcinoma should be excised with a 3-4 mm margin of healthy tissue, while a trichoepithelioma may only require minimal resection 3. Gray and Helwig 5 in their series of 83 patient showed that 35% of the solitary trichoepitheliomas were misdiagnosed as BCC although they found ulceration to be present in only five of their cases. The presence of ulceration makes the clinician to error toward the diagnosis of either a basal cell carcinoma (BCC) or sebaceous carcinoma. The histopathological features that go in favor of a trichoepithelioma include numerous keratinous cysts, lacy pattern of tumor cells, dense stroma, minimal inflammation, absent of minimum of abnormal hair follicles. In contrast, a basal cell carcinoma shows epidermal ulceration, very few keratinous cysts, minimal stroma, dense inflammation, and tumor lobules in adenoid and cystic patterns 6. Simpson et al. 4 presented the largest study (n = 18) of eyelid trichoepitheliomas over a duration of more than 30 years. There was male preponderance (M: F = 2:1) with the mean age at a presentation being 48.6 years (range 3-73 years). The upper lid was found to be twice more predisposed than lower lids. All patients underwent excision; however, two of them recurred after 10 and 12 years, respectively.
Other conditions which can be confused with trichoepithelioma include trichofolliculoma (a solitary tumor arising on the face of the elderly), milia (small epidermal cysts), syringoma (sweat gland tumors most often seen on the eyelids).
Dermoscopy may be helpful. Typically, multiple white clods of variable diameter are seen.
The diagnosis is often only made by pathology after biopsy or after removing the lesion surgically. Individual trichoepithelioma lesions may be removed surgically (excision biopsy) if there is any suspicion of malignant change. Carbon dioxide laser and dermabrasion may improve the appearance but partial destruction of the tumor is usually followed by regrowth.
A 2006 study 7 has suggested that abnormalities in the cylindromatosis oncogene (CYLD), which maps to 16q12-q13, may result in one of 3 syndromes: Brooke-Spiegler syndrome, familial cylindromatosis, and multiple familial trichoepithelioma (MFT1). Furthermore, some cases of patients with multiple trichoepitheliomas appear to be sporadic and not related with familial incidence 8.
The tendency to multiple trichoepitheliomas is inherited in Brooke-Spiegler syndrome, but trichoepithelioma is more common in females. Brooke-Spiegler syndrome is a rare genetic condition resulting in a range of tumors derived from skin appendages (hair follicle tumors and sweat gland tumors). Brooke-Spiegler syndrome includes the limited variants, familial cylindromatosis and multiple familial trichoepitheliomas.
Figure 1. Solitary trichoepithelioma
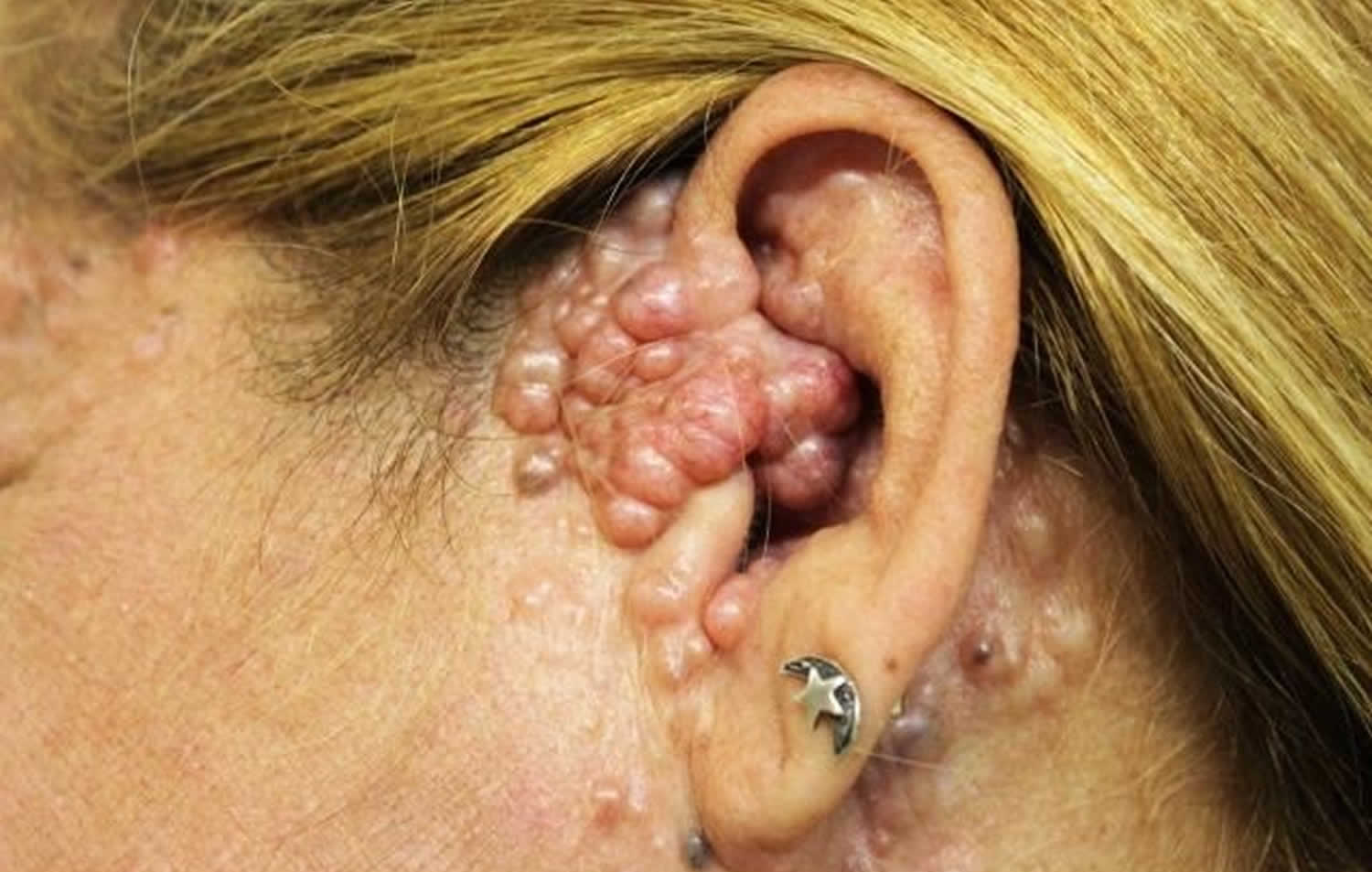
Figure 2. Multiple familial trichoepithelioma
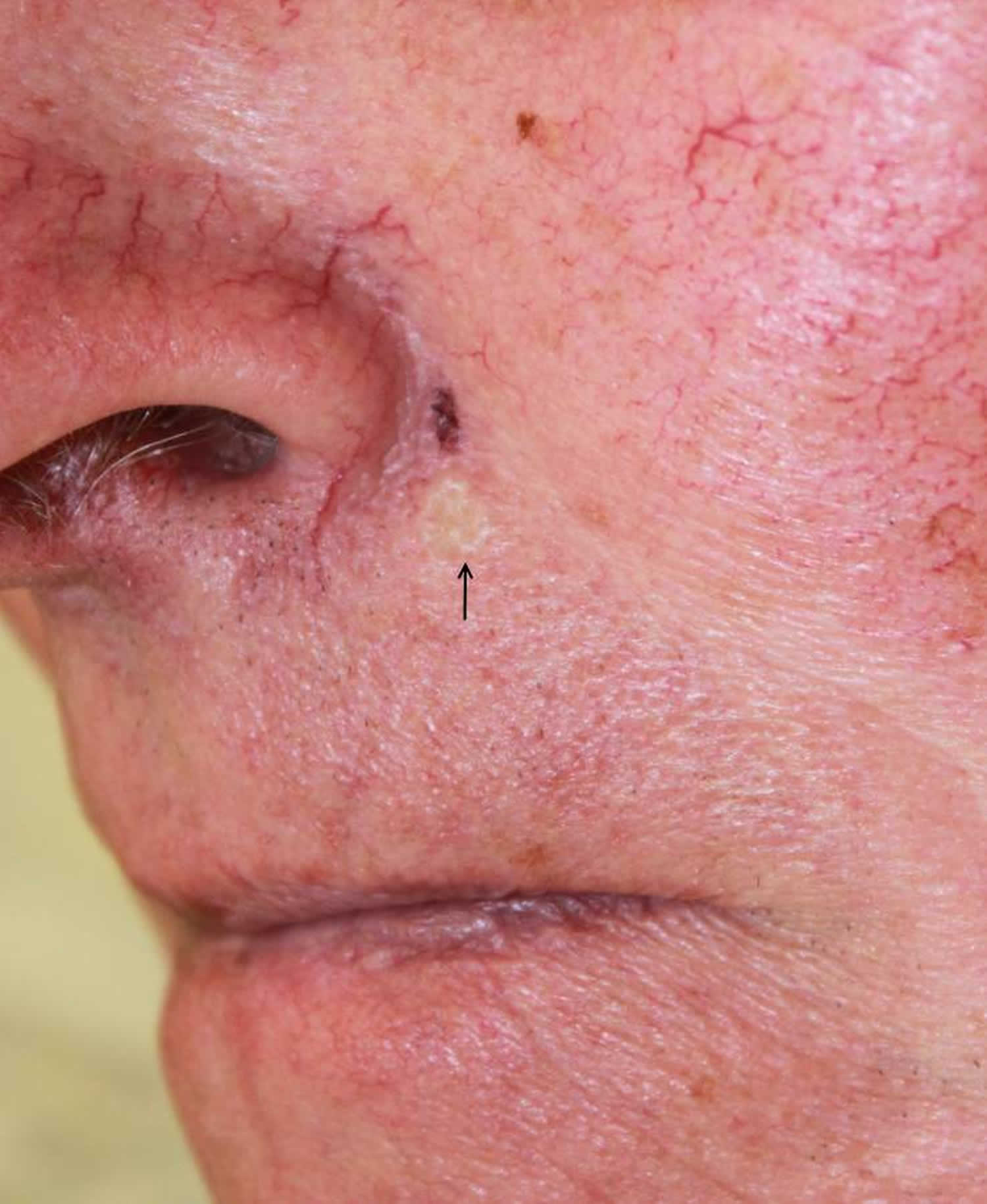
Figure 3. Desmoplastic trichoepithelioma
Is there any way to get rid of trichoepitheliomas? My face is full of them. I have tried different kinds of laser treatments, but the tumors regrow.
Several therapies have been used to treat multiple trichoepitheliomas, with variable to poor results. A single trichoepithelioma may be treated with surgery. Cryosurgery or laser surgery may be used to remove multiple trichoepitheliomas 9. Imiquimod cream has also been used as a treatment for trichoepitheliomas, with some improvement in symptoms 10. Other treatments have included dermabrasion, photodynamic therapy, and other medications 11. However, in most cases, multiple trichoepitheliomas eventually regrow following treatment 12.
Desmoplastic trichoepithelioma
Desmoplastic trichoepithelioma is a harmless facial skin lesion. It is an uncommon form of trichoepithelioma, with a reported incidence of 1 in 5000 skin biopsies in a cohort of British adults. It has also been called ‘sclerosing epithelial hamartoma’.
Desmoplastic trichoepithelioma grows from cells lining the hair follicle. It is classified as a benign adnexal or hair follicle tumor.
Desmoplastic trichoepithelioma is most often identified in middle-aged females, although it may also occur at other ages and in males. A lesion may have been present for many years before being brought to medical attention.
Desmoplastic trichoepithelioma typically present as a firm skin-colored to red, annular (ring-shaped) plaque with a central dimple. It is usually found on the upper cheek. Desmoplastic trichoepithelioma is stable or may slowly grow up to 1 cm in diameter. Multiple lesions are quite rare.
Desmoplastic trichoepithelioma treatment
True desmoplastic trichoepithelioma is a benign tumor with no malignant potential, so there is no need to remove them. However, it is best to keep the lesion under observation in case the diagnosis is incorrect, as basal cell carcinoma may look very similar.
Treatment options include:
- Curettage and electrodesiccation
- Surgical excision
- Mohs micrographic surgery, which ensures clear margins.
Multiple familial trichoepithelioma
Multiple familial trichoepithelioma is a genetic disorder characterized by multiple smooth, round, firm, skin-colored tumors (trichoepitheliomas) that usually occur on the face, but may also occur on the scalp, neck, and trunk 13. The tumors are from immature hair follicles 14. They usually first develop during childhood or adolescence and may grow larger and increase in number over time 9. The genetic disorder can be caused by mutations in the CYLD gene or by mutations in other genes which are still unknown. The condition may be divided in two subtypes, multiple familial trichoepithelioma type 1 and multiple familial trichoepithelioma type 2. Susceptibility to multiple familial trichoepithelioma is inherited in an autosomal dominant fashion, which means one copy of the mutated gene in each cell increases the risk of developing this disorder. However, a second, non-inherited (acquired) mutation is required for the tumors to develop in this disorder.
People with multiple familial trichoepithelioma typically develop large numbers of smooth, round, firm skin-colored tumors called trichoepitheliomas, which arise from hair follicles 14. These benign (noncancerous) tumors may occasionally transform into a type of skin cancer called basal cell carcinoma 15. Occasionally, other types of tumors, including growths called spiradenomas (which originate in sweat glands) and cylindromas (which likely originate in hair follicles) also develop. Affected people are also at risk of developing tumors in other tissues, particularly benign tumors of the salivary glands 13.
The tumors in multiple familial trichoepithelioma typically first appear during childhood or adolescence. They appear most often around the nose, forehead, and upper lip. Occasionally they occur on the scalp, neck, and upper trunk. They may grow larger and increase in number over time 13. In rare cases, the tumors may get in the way of the eyes, ears, nose, or mouth and affect vision or hearing. The growths can be disfiguring and may cause depression or other psychological problems. For reasons that remain unknown, females are often more severely affected than males 13.
Treatment often involves surgery to remove a single lesion and cryosurgery or laser surgery for multiple ones 16.
Multiple familial trichoepithelioma cause
Multiple familial trichoepithelioma can be caused by mutations in the CYLD gene which is found on chromosome 16 17. It is thought to be inherited in an autosomal dominant fashion with reduced penetrance. Autosomal dominant means that a single mutation in one copy of a gene is sufficient to cause the condition. Reduced penetrance means that not everyone with the gene mutation will develop symptoms of the condition 9.
Susceptibility to multiple familial trichoepithelioma has an autosomal dominant pattern of inheritance. This means that one mutated copy of the CYLD gene in each cell increases the risk that a person will develop the multiple familial trichoepithelioma. However, a second, non-inherited (acquired) mutation is needed for development of the skin tumors characteristic of this condition 13.
Do people with multiple familial trichoepithelioma always have affected family members?
Multiple familial trichoepithelioma is thought to be due to a single mutation in the CYLD gene or in another gene which has yet to be identified. A number of case reports of families with multiple familial trichoepithelioma demonstrating an autosomal dominant pattern of inheritance have been reported in the medical literature. Still, as with other autosomal dominant conditions, it is possible for a new mutation to occur for the first time in a family in an affected individual. For example a CYLD gene mutation may occur spontaneously for the first time in an egg or sperm or in the fertilized egg sometime after conception. This phenomenon is called a de novo or “new” mutation. A person with a new mutation would not be expected to have other affected family members.
In addition, some literature suggests that mutations that cause multiple familial trichoepithelioma may have reduced penetrance. This means that a person may inherit the disease causing mutation, yet never develop symptoms of the condition. As a result it is possible for a person with multiple familial trichoepithelioma to have a parent or other relative with the disease causing mutation, but with no symptoms of the condition.
If you have concerns about if and how multiple familial trichoepithelioma may be running in your family, we recommend that you speak with a genetics professional.
To find a medical professional who specializes in genetics, you can ask your doctor for a referral or you can search for one yourself. Online directories are provided by the American College of Medical Genetics (https://www.acmg.net/) and the National Society of Genetic Counselors (https://www.findageneticcounselor.com/).
Multiple familial trichoepithelioma diagnosis
A diagnosis of multiple familial trichoepithelioma is made based on the symptoms in the patient, the patient’s family history, and the appearance of the trichoepithelioma cells under a microscope (histology) 14. Multiple familial trichoepithelioma must be distinguished from basal cell carcinoma (cancerous tumor) and other rare genetic syndromes such as Cowden syndrome.
Multiple familial trichoepithelioma treatment
Several therapies have been used to treat multiple trichoepitheliomas, with variable to poor results. A single trichoepithelioma may be treated with surgery. Cryosurgery or laser surgery may be used to remove multiple trichoepitheliomas 9. Imiquimod cream has also been used as a treatment for trichoepitheliomas, with some improvement in symptoms 10. Other treatments have included dermabrasion, photodynamic therapy, and other medications 18. However, in most cases, multiple trichoepitheliomas eventually regrow following treatment 11.
Trichoepithelioma causes
The gene involved in basal cell carcinoma (PTCH, human patched gene located on band 9q22.3) appears to participate in the pathogenesis of trichoepithelioma 19. Since trichoepithelioma is inherited in an autosomal dominant fashion, males and females receive the gene equally, but because of lessened expressivity and penetrance in men, most patients are women.
Multiple familial trichoepithelioma can be caused by mutations in the CYLD gene 13. This gene provides instructions for making a protein that helps regulate nuclear factor-kappa-B. Nuclear factor-kappa-B is a group of related proteins that help protect cells from self-destruction (apoptosis) in response to certain signals. In regulating the action of nuclear factor-kappa-B, the CYLD protein allows cells to respond properly to signals to self-destruct when appropriate, such as when the cells become abnormal. By this mechanism, the CYLD protein acts as a tumor suppressor, which means that it helps prevent cells from growing and dividing too fast or in an uncontrolled way.
People with CYLD-related multiple familial trichoepithelioma are born with a mutation in one of the two copies of the CYLD gene in each cell. This mutation prevents the cell from making functional CYLD protein from the altered copy of the gene. However, enough protein is usually produced from the other, normal copy of the gene to regulate cell growth effectively. For tumors to develop, a second mutation or deletion of genetic material involving the other copy of the CYLD gene must occur in certain cells during a person’s lifetime.
When both copies of the CYLD gene are mutated in a particular cell, that cell cannot produce any functional CYLD protein. The loss of this protein allows the cell to grow and divide in an uncontrolled way to form a tumor. In people with multiple familial trichoepithelioma, a second CYLD mutation typically occurs in multiple cells over an affected person’s lifetime. The loss of CYLD protein in these cells leads to the growth of skin appendage tumors.
Some researchers consider multiple familial trichoepithelioma and two related conditions called familial cylindromatosis and Brooke-Spiegler syndrome, which are also caused by CYLD gene mutations, to be different forms of the same disorder. It is unclear why mutations in the CYLD gene cause different patterns of skin appendage tumors in each of these conditions, or why the tumors are generally confined to the skin in these disorders.
Some people with multiple familial trichoepithelioma do not have mutations in the CYLD gene. Scientists are working to identify the genetic cause of the disorder in these individuals. Susceptibility to multiple familial trichoepithelioma has an autosomal dominant pattern of inheritance, which means one copy of the altered gene in each cell increases the risk of developing this condition. However, a second, non-inherited mutation is required for development of skin appendage tumors in this disorder.
Brooke-Spiegler syndrome patients have a high incidence of multiple skin appendage tumors such as cylindroma, trichoepithelioma, and spiradenoma. These patients may show mutations of the CYLD gene (cylindromatosis gene) that map to 16q12-q13 20.
Studies have indicated that CYLD encodes a deubiquitinating enzyme that negatively regulates the nuclear factor (NF)–kappaB and c-Jun N-terminal kinase (JNK) pathways 21. Due to the presence of significant numbers of Merkel cells within the tumor nest and the detection of a sheath of CD34-positive dendrocytes around the tumor nests, it appears that trichoepithelioma differentiates toward or derives from hair structures, particularly the hair bulge. Rare instances of tumors resembling trichoepithelioma have been reported in animals 22.
Trichoepithelioma histology
As many as 30% of trichoepitheliomas connect with the overlying epidermis, but in general they are circumscribed, dermal nodules. In the upper dermis, multiple nodules are composed of uniform, basaloid cells, frequently with central, keratin-filled cysts.
Scanning power view reveals a tumor comprised of multiple nodules situated within the dermis. Small horn cysts, abortive hair follicles and calcification are frequently seen. The stroma is denser and more cellular than with basal cell carcinoma, and there is often focal stromal cracking. Often pronounced bulbar differentiation may be seen, emulating the follicular bulb and papilla; these structures have been referred to as papillary mesenchymal bodies.
Desmoplastic trichoepithelioma
Scanning power view demonstrates an infiltrating tumor which appears to be arising from the epidermis. The tumor is comprised of small islands of basaloid epithelium superficially which form cords and strands towards the base and periphery. Horn cysts, frequently many, calcification and foreign body granulomas can be seen. The cells are bland and mitotic activity is usually very low, however the infiltrative sclerosing growth pattern can cause difficulty in discriminating this lesion from syringoma or sometimes microcystic adnexal carcinoma. Trichoblastoma is a deeper form of trichoepithelioma.
Trichoepithelioma signs and symptoms
Slow-growing, single or multiple rounded papules or nodules (2-8 mm in diameter) that are skin-colored are typically observed on the face. The lesions are located mainly on the nasolabial folds, the nose, the forehead, the upper lip, and the scalp; 50% of lesions occur on the face and the scalp. Occasionally, lesions also occur on the neck and the upper part of the trunk. Heller et al report a rare case of trichoepithelioma of the vulva 23. Ulceration is rare.
The occurrence of multiple trichoepitheliomas (multiple familial trichoepithelioma) is transmitted as an autosomal dominant trait. People with multiple familial trichoepithelioma typically develop large numbers of smooth, round tumors called trichoepitheliomas, which arise from hair follicles. Trichoepitheliomas are generally noncancerous (benign) but occasionally develop into a type of skin cancer called basal cell carcinoma. Individuals with multiple familial trichoepithelioma occasionally also develop other types of tumors, including growths called spiradenomas and cylindromas. Spiradenomas develop in sweat glands. The origin of cylindromas has been unclear; while previously thought to derive from sweat glands, they are now generally believed to begin in hair follicles. Affected individuals are also at increased risk of developing tumors in tissues other than skin appendages, particularly benign or malignant tumors of the salivary glands.
People with multiple familial trichoepithelioma typically begin developing tumors during childhood or adolescence. The tumors mostly appear on the face, especially in the folds in the skin between the nose and lips (nasolabial folds, sometimes called smile lines), but may also occur on the neck, scalp, or trunk. They may grow larger and increase in number over time.
In severe cases, the tumors may get in the way of the eyes, ears, nose, or mouth and affect vision, hearing, or other functions. The growths can be disfiguring and may contribute to depression or other psychological problems. For reasons that are unclear, females with multiple familial trichoepithelioma are often more severely affected than males.
An association may exist with other cutaneous tumors (eg, cylindroma or Brooke-Spiegler syndrome, spiradenoma, basal cell carcinoma, ungual fibromas) or dystrophia unguis congenita.
Trichoepithelioma may be part of the Rombo syndrome (ie, vermiculate atrophoderma, milia, hypotrichosis, trichoepithelioma, basal cell carcinoma, peripheral vasodilatation).
Solitary giant trichoepithelioma presents as a large, polypoid lesion, usually in the lower part of the trunk or in the gluteal area.
Trichoepithelioma diagnosis
Trichoepithelioma is diagnosed on full-thickness skin biopsy to allow a histologic diagnosis as sclerosing basal cell carcinoma and microcystic adnexal carcinoma may appear similar. Ensure that the biopsy sample is sufficiently deep to allow the dermatopathologist to study most of the lesion in cases of a solitary trichoepithelioma. In particular, a shave biopsy of a plaquelike lesion on the lip may result in identifying the superficial portion of a microcystic adnexal carcinoma (an aggressive adnexal neoplasm) as a trichoepithelioma. Some adnexal carcinomas may show a very limited degree of cytologic atypia. In such cases, only by examining the periphery of the lesion with the characteristic infiltrative pattern allows correct diagnosis. Resampling or re-excision may be necessary for the definitive diagnosis or complete eradication in uncertain cases.
In vivo studies such as high-definition optical coherence tomography have been applied to distinguish trichoepithelioma from other cutaneous tumors 24. If necessary, genetic studies may be used to detect the abnormalities in band 9p21 in trichoepithelioma patients.
Trichoepithelioma treatment
Treatment of the trichoepithelioma lesion is primarily surgical. Laser and radiofrequency have been used with diverse results. A Brazilian study 25 of several types of cutaneous tumors reported only a partial response for trichoepithelioma to 5% imiquimod cream. Other studies suggest the possibility of targeted therapies, such as antitumor necrosis factor-alpha 26 or targeting mammalian target of rapamycin (mTOR) and hypoxia signaling pathways 27.
Trichoepithelioma surgery
Solitary lesions can be excised. In the case of multiple tumors, this surgical approach may not be feasible.
Split-thickness skin grafting, dermabrasion, and laser surgery have been proposed, but the results of these procedures vary 28.
Management of either form (ie, solitary, multiple/hereditary) by superficial biopsy is usually adequate.
Recurrence of solitary trichoepithelioma is uncommon. When the multiple facial lesions are surgically flattened by dermabrasion or laser therapy, they tend to regrow into elevated papules or nodules. This regrowth may occur rapidly within months, or it may take several years. Some patients find a prolonged cosmetic improvement to be worthwhile even if repeated procedures are necessary.
Ensure that the patient is informed about the possibility of scarring. As with many benign skin neoplasms, the patient is mainly concerned about the aesthetic appearance of the lesion. Scarring may result from all available methods for tumor removal. In patients with multiple lesions, treating 1 or 2 of the lesions and showing the patient the final result may be helpful before embarking on extensive aggressive therapy.
Complications
The persistence or recurrence of trichoepitheliomas is a complication, and scarring may occur after treatment.
Trichoepithelioma prognosis
Slow growth is characteristic of trichoepithelioma. Partial removal may result in persistence or recurrence. Although rare, trichoepitheliomas can develop high-grade carcinomas and mixed (epithelial/sarcomatous) tumors 29. Familial trichoepithelioma has shown an aggressive, recurrent behavior in rare cases.
In cases of multiple trichoepitheliomas, the lesions may cause disfigurement because of involvement of the face. The rare cases of trichoepithelioma described as having aggressive behavior (ie, ulceration, recurrence) are probably follicular tumors within the basal cell nevus syndrome and not trichoepithelioma.
- Gupta A, Ali MJ, Mishra DK, Naik MN. Solitary trichoepithelioma of the eyelid: A clinico-pathological correlation. Int J Trichol 2015;7:80-1[↩]
- Carter JJ, Kaur MR, Hargitai B, Brown R, Slator R, Abdullah A. Congenital desmoplastic trichoepithelioma. Clin Exp Dermatol. 2007 Sep. 32(5):522-4.[↩]
- Sugano DM, Lucci LM, Avila MP, Rehder JR, Pettinati J. Eyelid trichoepithelioma – Report of 2 cases. Arq Bras Oftalmol 2005;68:136-9.[↩][↩]
- Simpson W, Garner A, Collin JR. Benign hair-follicle derived tumours in the differential diagnosis of basal-cell carcinoma of the eyelids: A clinicopathological comparison. Br J Ophthalmol 1989;73:347-53.[↩][↩][↩]
- Gray HR, Helwig EB. Epithelioma adenoides cysticum and solitary trichoepithelioma. Arch Dermatol 1963;87:102-14.[↩]
- Kuo DS, Nyong’o OL. Congenital solitary eyelid trichoepithelioma. J AAPOS 2010;14:277-9.[↩]
- Young AL, Kellermayer R, Szigeti R, Teszas A, Azmi S, Celebi JT. CYLD mutations underlie Brooke-Spiegler, familial cylindromatosis, and multiple familial trichoepithelioma syndromes. Clin Genet. 2006 Sep. 70(3):246-9.[↩]
- Sehrawat M, Jairath V, Jain VK. Nonfamilial Multiple Trichoepithelioma: Few and Far Between. Indian J Dermatol. 2016 Jan-Feb. 61 (1):78-80.[↩]
- Neff AG, Carter KD. Benign Eyelid Lesions. In: Yanoff & Duker. Ophthalmology, 3rd ed. Philadelphia, PA: Mosby; 2008[↩][↩][↩][↩]
- Alessi SS, Sanches JA, Oliveira WR, Messina MC, Pimentel ER, Festa Neto C. Treatment of cutaneous tumors with topical 5% imiquimod cream. Clinics. 2009; 64(10):961-966.[↩][↩]
- Trichoepithelioma. https://emedicine.medscape.com/article/1060049-overview[↩][↩]
- Trichoepithelioma. https://www.dermnetnz.org/topics/trichoepithelioma/[↩]
- Multiple familial trichoepithelioma. https://ghr.nlm.nih.gov/condition/multiple-familial-trichoepithelioma[↩][↩][↩][↩][↩][↩]
- Morelli JG. Tumors of the Skin. In: Kliegman eds. Nelson Textbook of Pediatrics, 18th ed. Philadelphia, PA: Saunders; 2007[↩][↩][↩]
- Multiple Familial Trichoepitheliomas. https://www.orpha.net/data/patho/GB/uk-Trichoepithelioma.pdf[↩]
- Nagy N, Farkas K, Kemény L & Széll M. Phenotype-genotype correlations for clinical variants caused by CYLD mutations. Eur J Med Genet. 2015 May;. May, 2015; 58(5):271-8.[↩]
- TRICHOEPITHELIOMA, MULTIPLE FAMILIAL, 1 https://omim.org/entry/601606[↩]
- Trichoepithelioma. https://www.dermnetnz.org/topics/trichoepithelioma[↩]
- Matt D, Xin H, Vortmeyer AO, Zhuang Z, Burg G, Boni R. Sporadic trichoepithelioma demonstrates deletions at 9q22.3. Arch Dermatol. 2000 May. 136(5):657-60.[↩]
- Espana A, Garcia-Amigot F, Aguado L, Garcia-Foncillas J. A novel missense mutation in the CYLD gene in a Spanish family with multiple familial trichoepithelioma. Arch Dermatol. 2007 Sep. 143(9):1209-10.[↩]
- Blake PW, Toro JR. Update of cylindromatosis gene (CYLD) mutations in Brooke-Spiegler syndrome: novel insights into the role of deubiquitination in cell signaling. Hum Mutat. 2009 Jul. 30(7):1025-36.[↩]
- Martín de Las Mulas J, Molina AM, Millan Y, Carrasco L, Moyano R, Mozos E. Spontaneous trichoepithelioma in a laboratory mouse: gross, microscopic and immunohistochemical findings. Lab Anim. 2007 Jan. 41(1):136-40.[↩]
- Heller J, Roche N, Hameed M. Trichoepithelioma of the vulva: report of a case and review of the literature. J Low Genit Tract Dis. 2009 Jul. 13(3):186-7.[↩]
- Oliveira A, Arzberger E, Zalaudek I, Hofmann-Wellenhof R. Imaging of desmoplastic trichoepithelioma by high-definition optical coherence tomography. Dermatol Surg. 2015 Apr. 41 (4):522-5.[↩]
- Alessi SS, Sanches JA, de Oliveira WR, Messina MC, Pimentel ER, Festa Neto C. Treatment of cutaneous tumors with topical 5% imiquimod cream. Clinics (Sao Paulo). 2009. 64(10):961-6.[↩]
- Fisher GH, Geronemus RG. Treatment of multiple familial trichoepitheliomas with a combination of aspirin and a neutralizing antibody to tumor necrosis factor alpha: A case report and hypothesis of mechanism. Arch Dermatol. 2006 Jun. 142 (6):782-3.[↩]
- Brinkhuizen T, Weijzen CA, Eben J, Thissen MR, van Marion AM, Lohman BG, et al. Immunohistochemical analysis of the mechanistic target of rapamycin and hypoxia signalling pathways in basal cell carcinoma and trichoepithelioma. PLoS One. 2014. 9 (9):e106427.[↩]
- Richard A, Chevalier JM, Verneuil L, Sergent B, Tesnière A, Dolfus C, et al. [CO2 laser treatment of skin cylindromas in Brooke-Spiegler syndrome]. Ann Dermatol Venereol. 2014 May. 141(5):346-53.[↩]
- Rosso R, Lucioni M, Savio T, Borroni G. Trichoblastic sarcoma: a high-grade stromal tumor arising in trichoblastoma. Am J Dermatopathol. 2007 Feb. 29(1):79-83.[↩]