What is a bunion
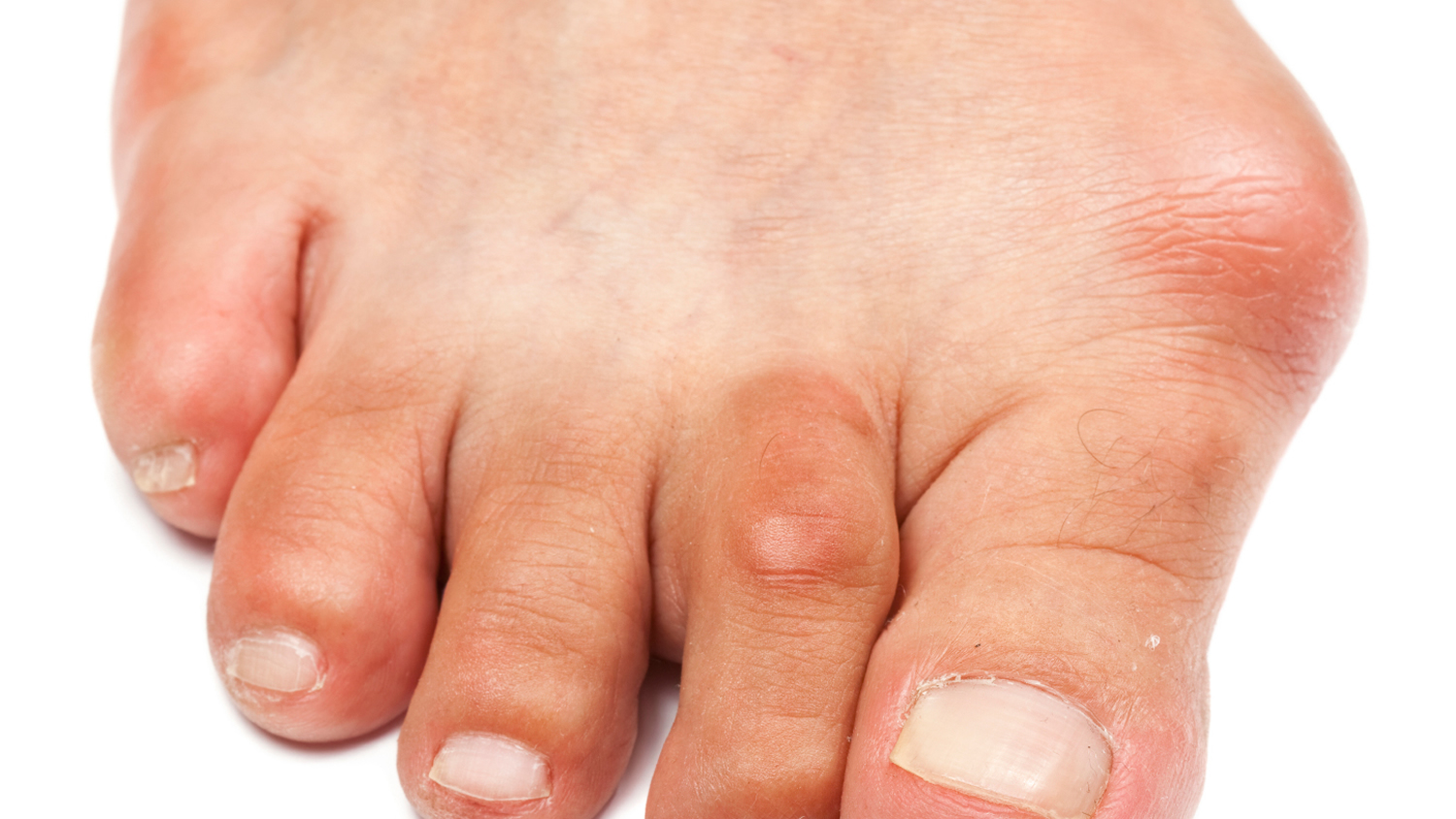
A bunion forms when your big toe points (angulates) toward the second toe 1. Bunion forms when your big toe pushes against your next toe, forcing the joint of your big toe to get bigger and stick out. This causes a bump to appear on the inside edge of your toe. The skin over the bunion might be red and sore.
- Hallux valgus (where the great toe moves towards the second toe) is found in at least 2% of children aged 9 to 10 years and almost half of adults, with greater prevalence in women 2.
Wearing tight, narrow shoes might cause bunions or make them worse. Bunions also can develop as a result of an inherited structural defect, stress on your foot or a medical condition, such as arthritis.
Smaller bunions (bunionettes) can develop on the joint of your little toe.
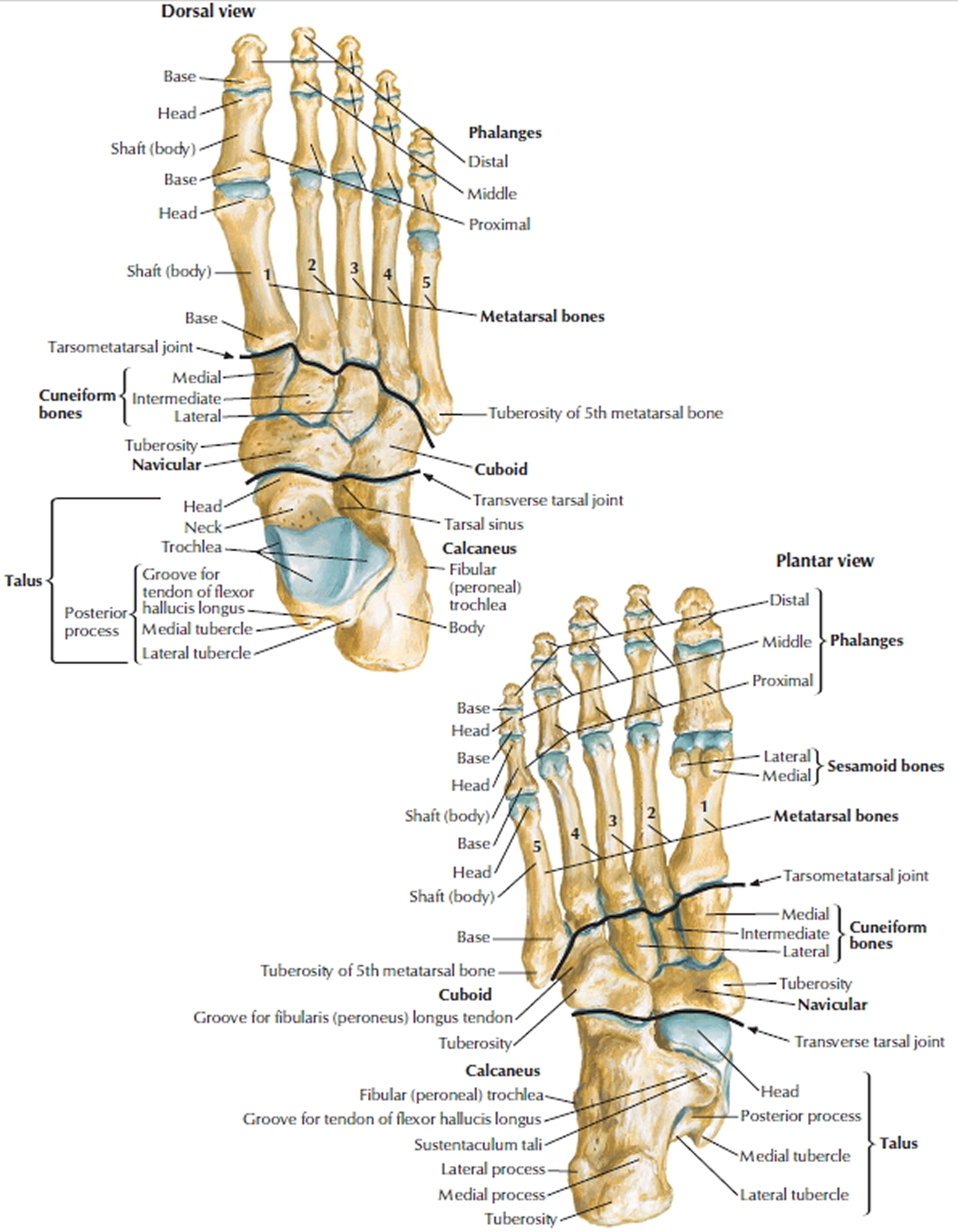
Figure 1. Normal foot bones
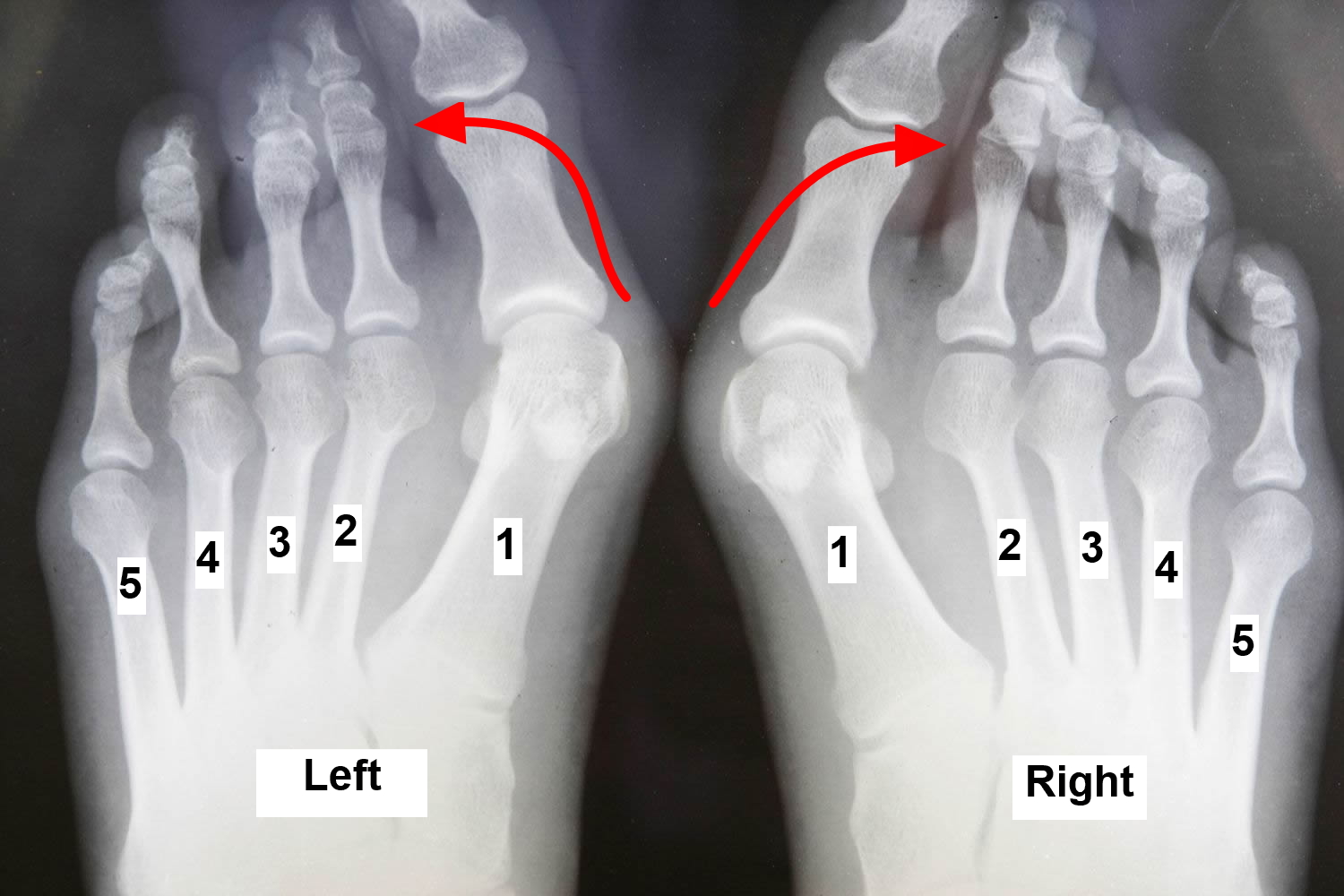
Figure 2. Bunion (X-ray of big toe bone angulating away from the midline of the body)
Symptoms of bunion
The signs and symptoms of a bunion include:
- Big toe turned toward the other toes and may cross over the second toe.
- A bony bump at the first toe joint, with decreased movement in the toe site.
- Pain over the joint, which pressure from shoes makes worse.
- Swelling, redness or soreness around your big toe joint
- Corns or calluses — these often develop where the first and second toes overlap
- Persistent or intermittent pain
- Restricted movement of your big toe if arthritis affects the toe
- Red, thickened skin along the inside edge at the base of the big toe.
- Difficulty wearing regular shoes.
You may have problems finding shoes that fit or that do not cause pain.
When to see a doctor
Although bunions often require no medical treatment, see your doctor or a doctor who specializes in treating foot disorders (podiatrist or orthopedic foot specialist) if you have:
- Persistent big toe or foot pain
- A visible bump on your big toe joint
- Decreased movement of your big toe or foot
- Difficulty finding shoes that fit properly because of a bunion
Causes of bunions
There are many theories about how bunions develop, but the exact cause is unknown. Factors likely include:
- Inherited foot type
- Foot injuries
- Deformities present at birth (congenital)
Experts disagree on whether tight, high-heeled or too-narrow shoes cause bunions or whether footwear simply contributes to bunion development.
Bunions might be associated with certain types of arthritis, particularly inflammatory types, such as rheumatoid arthritis.
Risk factors for bunions
These factors might increase your risk of bunions:
- High heels. Wearing high heels forces your toes into the front of your shoes, often crowding your toes.
- Ill-fitting shoes. People who wear shoes that are too tight, too narrow or too pointed are more susceptible to bunions.
- Rheumatoid arthritis. Having this inflammatory condition can make you more susceptible to bunions.
- Heredity. The tendency to develop bunions might be because of an inherited structural foot defect.
Complications of bunions
Although they don’t always cause problems, bunions are permanent unless surgically corrected. Possible complications include:
- Bursitis. This painful condition occurs when the small fluid-filled pads (bursae) that cushion bones, tendons and muscles near your joints become inflamed.
- Hammertoe. An abnormal bend that occurs in the middle joint of a toe, usually the toe next to your big toe, can cause pain and pressure.
- Metatarsalgia. This condition causes pain and inflammation in the ball of your foot.
Prevention of bunions
To help prevent bunions:
- Choose shoes carefully. They should have a wide toe box — no pointy toes — and there should be space between the tip of your longest toe and the end of the shoe.
- Your shoes should conform to the shape of your feet without squeezing or pressing any part of your foot.
Diagnosis of bunion
Your doctor can identify a bunion by examining your foot. After the physical exam, an X-ray of your foot can help your doctor identify the cause of the bunion and rate its severity.
Treatment of bunions
Treatment options vary depending on the severity of your bunion and the amount of pain it causes.
Conservative treatment
Nonsurgical treatments that may relieve the pain and pressure of a bunion include:
- Changing shoes. Wear roomy, comfortable shoes that provide plenty of space for your toes.
- Padding and taping or splinting. Use over-the-counter, nonmedicated bunion pads. Also, your doctor can help you tape your foot in a normal position. This can reduce stress on the bunion and alleviate your pain.
- Medications. Acetaminophen (Tylenol, others), ibuprofen (Advil, Motrin IB, others) or naproxen sodium (Aleve) can help you control the pain of a bunion.
- Cortisone injections also might help.
- Shoe inserts. Padded shoe inserts can help distribute pressure evenly when you move your feet, reducing your symptoms and preventing your bunion from getting worse. Over-the-counter arch supports can provide relief for some people; others require prescription orthotic devices.
- Applying ice. Icing your bunion after you’ve been on your feet too long or if it becomes inflamed can help relieve soreness and inflammation.
Bunion surgery
If conservative treatment doesn’t provide relief from your symptoms, you might need surgery. However, surgery isn’t recommended unless a bunion causes you frequent pain or interferes with your daily activities.
There are numerous surgical procedures for bunions, and no one technique is best for every problem.
Surgical procedures for bunions might involve:
- Removing the swollen tissue from around your big toe joint
- Straightening your big toe by removing part of the bone
- Realigning the long bone between the back part of your foot and your big toe, to straighten out the abnormal angle in your big toe joint
- Joining the bones of your affected joint permanently
It’s possible that you’ll be able to walk on your foot immediately after a bunion procedure. However, full recovery can take weeks to months.
To prevent a recurrence, you’ll need to wear proper shoes after recovery. For most people, it’s unrealistic to expect to wear narrower shoes after surgery.
Talk to your doctor about what you can expect after bunion surgery.
Bunion removal surgery
Bunion removal is surgery to treat deformed bones of the big toe and foot. A bunion occurs when the big toe points toward the second toe, forming a bump on the inner side of the foot.
Description:
You will be given anesthesia (numbing medicine) so that you won’t feel pain.
- Local anesthesia. Your foot may be numbed with pain medicine. You may also be given medicines that relax you. You will stay awake.
- Spinal anesthesia. This is also called regional anesthesia. The pain medicine is injected into a space in your spine. You will be awake but will not be able to feel anything below your waist.
- General anesthesia. You will be asleep and pain-free.
The surgeon makes a cut around the toe joint and bones. The deformed joint and bones are repaired using pins, screws, plates, or a cast to keep the bones in place.
The surgeon may repair the bunion by:
- Making certain tendons or ligaments shorter or longer.
- Taking out the damaged part of the joints and then using screws, wires, or a plate to hold the joint together so that they can fuse.
- Shaving off the bump on the toe joint.
- Removing the damaged part of the joint.
- Cutting parts of the bones on each side of the toe joint, and then putting them in their proper position.
Risks associated with bunion surgery
Risks for anesthesia and surgery in general include:
- Allergic reactions to medicines
- Breathing problems
- Bleeding, blood clots, or infection
Risks for bunion surgery include:
- Numbness in the big toe
- The wound does not heal well
- The surgery does not correct the problem
- Nerve damage
- Persistent pain
- Stiffness in the toe
- Arthritis in the toe
Prognosis after bunion surgery
You should have less pain after your bunion is removed and your foot has healed. You should also be able to walk and wear shoes more easily. This surgery does repair some of the deformity of your foot, but it will not give you a perfect-looking foot.
Full recovery may take 3 to 5 months.
References