What is cryptosporidium
Cryptosporidium is a microscopic parasite that causes the diarrheal disease cryptosporidiosis. Both the parasite and the disease are commonly known as “Crypto.”
There are many species of Cryptosporidium that infect animals, some of which also infect humans. Ingesting the Cryptosporidium parasites can lead to cryptosporidiosis infection. The Cryptosporidium parasites are found in the feces of infected humans or animals. The parasite is one of the most common causes of waterborne disease in humans around the world.
The Cryptosporidium parasite is protected by an outer shell that allows it to survive outside the body for long periods of time and makes it very tolerant to chlorine disinfection. Cryptosporidium parasite now causes over half of the reported waterborne disease outbreaks associated with swimming in chlorinated public swimming pools 1. Cryptosporidium’s chlorine resistance and documented excretion for weeks after resolution of symptoms has led Centers for Disease Control and Prevention (CDC) and The American Academy of Pediatrics 2 to recommend that all persons refrain from swimming until 2 weeks after resolution of symptoms.
While Cryptosporidium parasite can be spread in several different ways, water (drinking water and recreational water) is the most common way to spread the parasite. Cryptosporidium is a leading cause of waterborne disease among humans in the United States.
Although cryptosporidium parasite (Crypto) can affect all people, some groups are likely to develop more serious illness. For people with weakened immune systems, symptoms can be severe and could lead to severe or life-threatening illness. Examples of people with weakened immune systems include those with AIDS; those with inherited diseases that affect the immune system; and cancer and transplant patients who are taking certain immunosuppressive drugs.
Infection with Cryptosporidium species results in a wide range of manifestations, from asymptomatic infections to severe, life-threatening illness; incubation period is an average of 7 days (but can range from 2 to 10 days). Watery diarrhea is the most frequent symptom, and can be accompanied by dehydration, weight loss, abdominal pain, fever, nausea and vomiting. In most healthy people (immunocompetent persons), symptoms are usually short lived (1 to 2 weeks); they can be chronic and more severe (life-threatening) in immunocompromised patients, especially those with CD4 counts < 200/µl. While the small intestine is the site most commonly affected, symptomatic Cryptosporidium infections have also been found in other organs including other digestive tract organs, the lungs, and possibly conjunctiva.
The first signs and symptoms of cryptosporidium infection usually appear within a week after infection and may include:
- Watery diarrhea
- Dehydration
- Lack of appetite
- Weight loss
- Stomach cramps or pain
- Fever
- Nausea
- Vomiting
Symptoms may last for up to two weeks, though they may come and go sporadically for up to a month, even in people with healthy immune systems. Some people with cryptosporidium infection may have no symptoms.
How is cryptosporidiosis spread?
Cryptosporidium lives in the gut of infected humans or animals. An infected person or animal sheds cryptosporidium parasites in their poop. An infected person can shed 10,000,000 to 100,000,000 cryptosporidium parasites in a single bowel movement. Shedding of cryptosporidium parasites in poop begins when symptoms like diarrhea begin and can last for weeks after symptoms stop. Swallowing as few as 10 cryptosporidium parasites can cause infection.
Outbreaks of cryptosporidiosis have been reported in several countries, the most remarkable being a waterborne outbreak in Milwaukee (Wisconsin) in 1993, that affected more than 400,000 people.
Cryptosporidium can be spread by:
- Swallowing recreational water (for example, the water in swimming pools, fountains, lakes, rivers) contaminated with cryptosporidium
- Cryptosporidium’s high tolerance to chlorine enables the parasite to survive for long periods of time in chlorinated drinking and swimming pool water
- Drinking untreated water from a lake or river that is contaminated with cryptosporidium
- Swallowing water, ice, or beverages contaminated with poop from infected humans or animals
- Eating undercooked food or drinking unpasteurized/raw apple cider or milk that gets contaminated with cryptosporidium
- Touching your mouth with contaminated hands
- Hands can become contaminated through a variety of activities, such as touching surfaces or objects (e.g., toys, bathroom fixtures, changing tables, diaper pails) that have been contaminated by poop from an infected person, changing diapers, caring for an infected person, and touching an infected animal
- Exposure to feces from an infected person through oral-anal sexual contact
Cryptosporidium is not spread through contact with blood.
Cryptosporidium life cycle
Many species of Cryptosporidium exist that infect humans and a wide range of animals. Although Cryptosporidium parvum and Cryptosporidium hominis (formerly known as Cryptosporidium parvum anthroponotic genotype or genotype 1) are the most prevalent species causing disease in humans, infections by Cryptosporidium felis, Cryptosporidium meleagridis, Cryptosporidium canis, and Cryptosporidium muris have also been reported.
- Sporulated oocysts, containing 4 sporozoites, are excreted by the infected host through feces and possibly other routes such as respiratory secretions.
- Transmission of Cryptosporidium parvum and Cryptosporidium hominis occurs mainly through contact with contaminated water (e.g., drinking or recreational water). Occasionally food sources, such as chicken salad, may serve as vehicles for transmission. Many outbreaks in the United States have occurred in waterparks, community swimming pools, and day care centers. Zoonotic and anthroponotic transmission of Cryptosporidium parvum and anthroponotic transmission of Cryptosporidium hominis occur through exposure to infected animals or exposure to water contaminated by feces of infected animals.
- Following ingestion (and possibly inhalation) by a suitable host,
- [a] excystation occurs.
- [b] and [c] the sporozoites are released and parasitize epithelial cells of the gastrointestinal tract or other tissues such as the respiratory tract.
- [d], [e] and [f] in these cells, the parasites undergo asexual multiplication (schizogony or merogony) and then
- [g] sexual multiplication (gametogony) producing microgamonts (male) and
- [h] macrogamonts (female).
- [i] upon fertilization of the macrogamonts by the microgametes,
- [j] and [k] oocysts develop that sporulate in the infected host. Two different types of oocysts are produced, the thick-walled, which is commonly excreted from the host [j] and the thin-walled oocyst [k], which is primarily involved in autoinfection. Oocysts are infective upon excretion, thus permitting direct and immediate fecal-oral transmission.
Note: that oocysts of Cyclospora cayetanensis, another important coccidian parasite, are unsporulated at the time of excretion and do not become infective until sporulation is completed.
Figure 1. Cryptosporidium life cycle
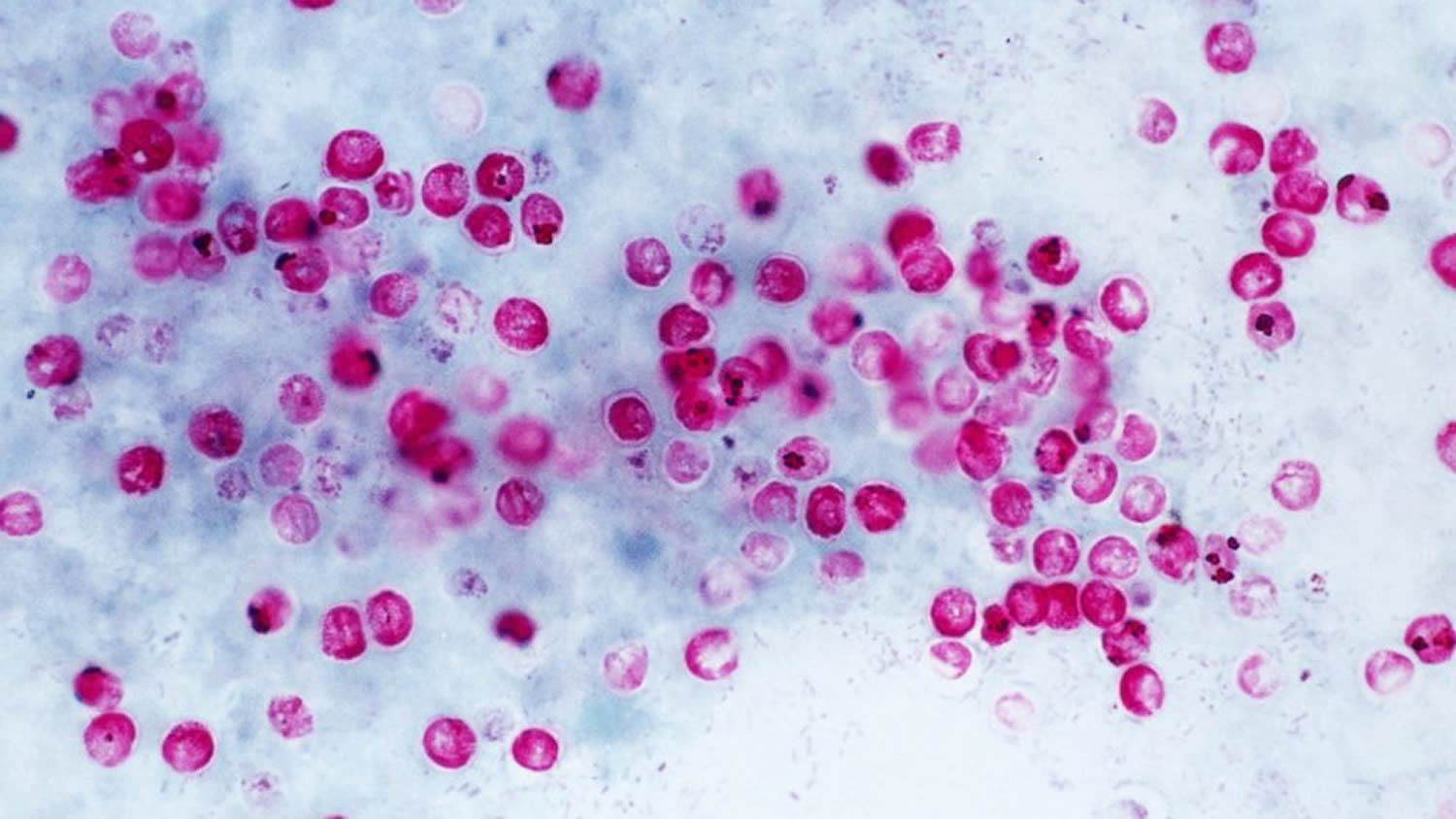
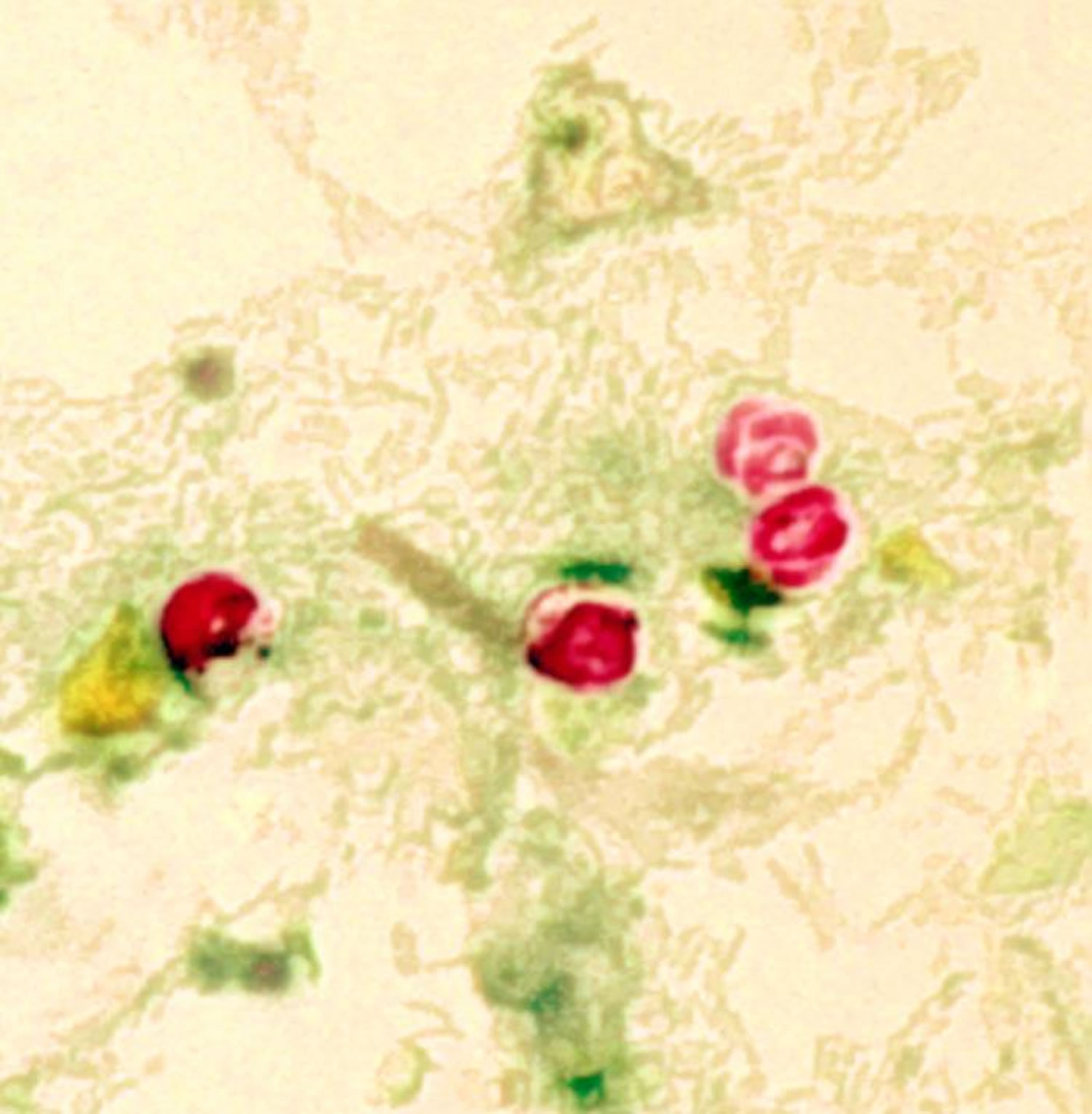
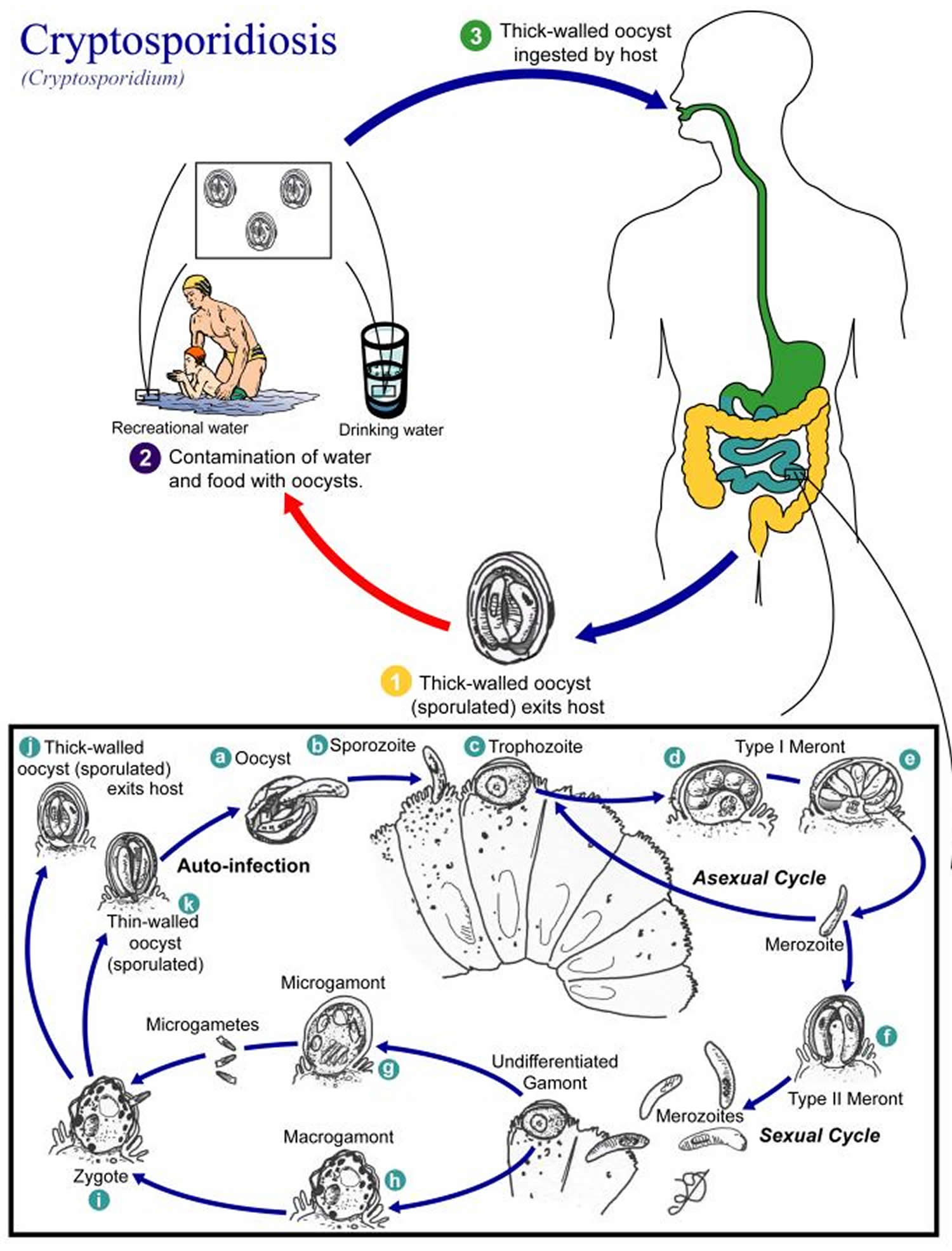 Figure 2. Cryptosporidium parvum oocysts (stained using the modified acid-fast method. These Cryptosporidium parvum oocysts exhibit a bright red coloration when using this staining technique. Note the sporozoites inside the two oocysts on the right)
Figure 2. Cryptosporidium parvum oocysts (stained using the modified acid-fast method. These Cryptosporidium parvum oocysts exhibit a bright red coloration when using this staining technique. Note the sporozoites inside the two oocysts on the right)Cryptosporidium complications
Complications of cryptosporidium infection include:
- Malnutrition resulting from poor absorption of nutrients from your intestinal tract (malabsorption)
- Severe dehydration
- Significant weight loss (wasting)
- Inflammation of a bile duct — the passage between your liver, gallbladder and small intestine
- Inflammation of your gallbladder, liver or pancreas
Cryptosporidium infection itself isn’t life-threatening. However, if you’ve had a transplant or if you have a weakened immune system, developing complications can be dangerous.
Cryptosporidium sources of infection
Cryptosporidium lives in the intestine of infected humans or animals. An infected person or animal sheds cryptosporidium parasites in the stool. Millions of Cryptosporidium parasites can be released in a bowel movement from an infected human or animal. Shedding begins when the symptoms begin and can last for weeks after the symptoms (e.g., diarrhea) stop. You can become infected after accidentally swallowing the parasite. Cryptosporidium may be found in soil, food, water, or surfaces that have been contaminated with the feces from infected humans or animals. Cryptosporidium is not spread by contact with blood.
Cryptosporidium can be spread by:
- Putting something in your mouth or accidentally swallowing something that has come in contact with the stool of a person or animal infected with Cryptosporidium.
- Swallowing recreational water contaminated with Cryptosporidium. Recreational water can be contaminated with sewage or feces from humans or animals.
- Swallowing water or beverages contaminated by stool from infected humans or animals.
- Eating uncooked food contaminated with Cryptosporidium. All fruits and vegetables you plan to eat raw should be thoroughly washed with uncontaminated water.
- Touching your mouth with contaminated hands. Hands can become contaminated through a variety of activities, such as:
- touching surfaces (e.g., toys, bathroom fixtures, changing tables, diaper pails) that have been contaminated by stool from an infected person,
- changing diapers,
- caring for an infected person, and
- handling an infected animal such as a cow or calf.
People with greater exposure to contaminated materials are more at risk for infection, such as:
- Children who attend childcare centers, including diaper-aged children
- Childcare workers
- Parents of infected children
- People who take care of other people with cryptosporidiosis
- International travelers
- Backpackers, hikers, and campers who drink unfiltered, untreated water
- People who drink from untreated shallow, unprotected wells
- People, including swimmers, who swallow water from contaminated sources
- People who handle infected cattle
- People exposed to human feces through sexual contact
Contaminated water may include water that has not been boiled or filtered, as well as contaminated recreational water sources. Several community-wide outbreaks of cryptosporidiosis have been linked to drinking municipal water or recreational water contaminated with cryptosporidium.
Cryptosporidium parasites are found in every region of the United States and throughout the world. Travelers to developing countries may be at greater risk for infection because of poorer water treatment and food sanitation, but cryptosporidiosis occurs worldwide. In the United States, an estimated 748,000 cases of cryptosporidiosis occur each year 3.
Once infected, people with decreased immunity are most at risk for severe disease. The risk of developing severe disease may differ depending on each person’s degree of immune suppression.
Cryptosporidium infection causes
Cryptosporidium infection begins when you ingest the one-celled cryptosporidium parasite. Some strains of cryptosporidium may cause more serious disease.
These parasites then travel to your intestinal tract, where they settle into the walls of your intestines. Eventually, more cells are produced and shed in massive quantities into your feces, where they are highly contagious.
You can become infected with cryptosporidia by touching anything that has come in contact with contaminated feces. Methods of infection include:
- Drinking contaminated water that contains cryptosporidium parasites
- Swimming in contaminated water that contains cryptosporidium parasites and accidentally swallowing some of it
- Eating uncooked, contaminated food that contains cryptosporidia
- Touching your hand to your mouth if your hand has been in contact with a contaminated surface or object
- Having close contact with other infected people or animals — especially their feces — which can allow the parasite to be transmitted from your hands to your mouth
If you have a compromised immune system from HIV/AIDS, you’re more susceptible to illness from cryptosporidium parasites than is a person with a healthy immune system. People with HIV/AIDS can develop severe symptoms and a chronic, persistent form of disease that may be difficult to treat.
Hardy cryptosporidium parasites
Cryptosporidium parasites are one of the more common causes of infectious diarrhea in humans. This parasite is difficult to eradicate because it’s resistant to many chlorine-based disinfectants and can’t be effectively removed by many filters. Cryptosporidia can also survive in the environment for many months at varying temperatures, though the parasite can be destroyed by freezing or boiling.
Risk factors for cryptosporidium
People who are at increased risk of developing cryptosporidiosis include:
- Those who are exposed to contaminated water
- Children, particularly those wearing diapers, who attend child care centers
- Parents of infected children
- Child care workers
- Animal handlers
- Those who engage in oral-to-anal sexual activity
- International travelers, especially those traveling to developing countries
- Backpackers, hikers and campers who drink untreated, unfiltered water
- Swimmers who swallow water in pools, lakes and rivers
- People who drink water from shallow, unprotected wells
Cryptosporidium prevention
The following recommendations are intended to help prevent and control cryptosporidiosis in members of the general public.
Practice Good Hygiene
- Wet hands with clean, running water and apply soap. Lather all surfaces of hands and scrub for at least 20 seconds. Rinse with clean, running water and dry with a clean towel or air
- before preparing or eating food,
- after using the toilet,
- after changing diapers or cleaning up a child who has used the toilet,
- before and after caring for someone who is ill with diarrhea,
- after handling an animal, particularly young livestock, or its stool,
- after gardening, even if wearing gloves.
Note: Alcohol-based hand sanitizers do NOT effectively kill Cryptosporidium.
At child care facilities
Exclude children who are ill with diarrhea from child care settings until the diarrhea has stopped.
- Children who are infected with the parasite but who do not have diarrhea may be allowed to return.
- Recently returning children can be grouped together in one classroom to minimize exposing uninfected children to the parasite.
- Move adults with diarrhea to jobs that minimize opportunities for spreading infection (for example, administrative work instead of food preparation).
Establish, implement, and enforce policies on water-play and swimming that:
- Exclude children ill with diarrhea from water-play and swimming activities.
- Exclude children diagnosed with cryptosporidium from water-play and swimming activities for an additional 2 weeks after their diarrhea has resolved.
- Discourage children from getting the water in their mouths and swallowing it.
- Have children and staff wash their hands before using water tables.
- Have children and staff shower with soap before swimming in the water.
- If a child is too young to shower independently, have staff wash the child, particularly the rear end, with soap and water.
- Take frequent bathroom breaks or check their diapers often.
- Change children’s diapers in a diaper-changing area or bathroom and not by the water.
- Prohibit the use of temporary inflatable or rigid fill-and-drain swimming pools and slides because they can spread germs in child-care facilities.
Practice good hygiene.
Good handwashing means:
- Wet your hands with clean, running water (warm or cold), turn off the tap, and apply soap.
- Lather your hands by rubbing them together with the soap. Be sure to lather the backs of your hands, between your fingers, and under your nails.
- Scrub your hands for at least 20 seconds. Need a timer? Hum the “Happy Birthday” song from beginning to end twice.
- Rinse your hands well under clean, running water.
- Dry your hands using a clean towel or air dry them.
For children:
- Observe handwashing or assist when needed.
- Wash children’s hands when they first arrive at the childcare facility, after they use the toilet, after having their diapers changed, and before eating snacks or meals.
For adults:
- Wash hands after using the toilet, after helping a child use the toilet, after diapering a child, and before handling or eating food. Note: Where staffing permits, people who change diapers should not prepare or serve food.
Reinforce good diapering practices.
- Separate diaper-changing areas from children’s play and food preparation areas.
- Use disposable gloves and change them after each diaper change.
- Use disposable paper over diaper-changing surfaces and change it after each diaper change.
- Ensure children wear clothing over their diapers to reduce the opportunity for leakage.
- Wash hands: both yours and the child’s after each diaper change.
Disinfect surfaces and objects, including but not limited to bathrooms, diaper-changing areas, food-preparation areas, tabletops, high chairs, and toys.
Notify the state or local health department about an excessive level of diarrhea or any cryptosporidium cases in the childcare facility. Cryptosporidium is a nationally reportable disease.
At the swimming pool
- Protect others by not swimming if ill with diarrhea.
- If cryptosporidiosis is diagnosed, do not swim for at least 2 weeks after diarrhea stops.
- Do not swallow the water.
- Take young children on bathroom breaks every 60 minutes or check their diapers every 30—60 minutes.
Avoid Water That Might Be Contaminated
- Do not drink untreated water from lakes, rivers, springs, ponds, streams, or shallow wells.
- Follow advice given during local drinking water advisories.
- If the safety of drinking water is in doubt (e.g., during an outbreak, or if water treatment is unknown) use at least one of the following:
- Commercially bottled water,
- Water that has been previously boiled for 1 minute and left to cool. At elevations above 6,500 feet (1,981 meters), boil for 3 minutes.
- Use a filter designed to remove Cryptosporidium.
- The label might read ‘NSF 53’ or ‘NSF 58’.
- Filter labels that read “absolute pore size of 1 micron or smaller” are also effective.
- If the safety of drinking water is in doubt, (e.g., during an outbreak or if water treatment is unknown), use bottled, boiled, or filtered water to wash fruits and vegetables that will be eaten raw.
Practice Extra Caution While Traveling
- Do not use or drink inadequately treated water or use ice when traveling in countries where the water might be unsafe.
- Avoid eating uncooked foods when traveling in countries where the food supply might be unsafe.
Prevent Contact and Contamination With Feces During Sex
- Use barriers (e.g., condoms, natural rubber latex sheets, dental dams, or cut-open non-lubricated condoms) between the mouth and a partner’s genitals or rectum.
- Wash hands immediately after handling a condom or other barrier used during anal sex and after touching the anus or rectal area.
Immunocompromised Persons Prevention and Control
The following recommendations are intended to help prevent and control cryptosporidiosis in immunocompromised persons.
Wash Your Hands
Washing your hands often with soap and water is probably the single most important step you can take to prevent cryptosporidium and many other illnesses. Always wash your hands before eating and preparing food. Wash your hands well after touching children in diapers; after touching clothing, bedding, toilets, or bed pans soiled by someone who has diarrhea; after gardening; any time you touch pets or other animals; and after touching anything that might have had contact with even the smallest amounts of human or animal stool, including dirt in your garden and other places. Even if you wear gloves when you do these activities you should still wash well when you finish. Children should be supervised by adults to make sure they wash their hands well.
Note: Alcohol-based hand sanitizers do NOT effectively kill Cryptosporidium.
Practice safer sex
Infected people may have cryptosporidium on their skin in the anal and genital areas, including the thighs and buttocks. However, since you cannot tell if someone has cryptosporidium, you may want to take these precautions with any sex partner. Avoid sexual practices that might result in oral exposure to stool (e.g., oral-anal contact). To reduce the risk for exposure to stool, consider using dental dams or similar barrier methods for oral-anal and oral-genital contact, wearing latex gloves during digital-anal contact, and changing condoms after anal intercourse. Frequent washing of hands and genitals with warm soapy water during and after activities that might bring these body parts in contact with stool might further reduce the risk for infection with cryptosporidium. This advice is good not only for preventing infection with cryptosporidium but also preventing infection with other gastrointestinal germs, such as Giardia, hepatitis A, Salmonella, Shigella, and amebas.
Avoid touching farm animals
If you touch a farm animal, particularly a calf, lamb, or other young animal, or visit a farm where animals are raised, wash your hands well with soap and water before preparing food or putting anything in your mouth. Do not touch the stool of any animal. After you visit a farm or other area with animals, have someone who is not immunocompromised clean your shoes, or wear disposable gloves if you clean them yourself. Wash your hands well with soap and water after taking off the gloves.
Avoid touching the stool of pets
Most pets are safe to own. However, someone who is not immunocompromised should clean their litter boxes or cages, and dispose of the stool. If you must clean up after a pet, use disposable gloves. Wash your hands well with soap and water afterwards. The risk of getting cryptosporidium is greatest from pets that are less than 6 months old, animals that have diarrhea, and stray animals. Older animals can also have cryptosporidium, but they are less likely to have it than younger animals. If you get a puppy or kitten that is less than 6 months old, have the animal tested for cryptosporidium before bringing it home. If any pet gets diarrhea, have it tested for cryptosporidium.
Avoid swallowing water when swimming in the ocean, lakes, rivers, or pools, and when using hot tubs
When swimming in lakes, rivers, or pools, and when using hot tubs, avoid swallowing water. Many outbreaks of cryptosporidium have been traced to swallowing contaminated water while swimming. Cryptosporidium is extremely chlorine tolerant so it can live in chlorinated swimming pools and water parks for days. Cryptosporidium also can remain alive in salt water for several days, so swimming in polluted ocean water may also be unsafe.
Wash and/or cook your food
Fresh vegetables and fruits may be contaminated with Crypto. Therefore, wash well all vegetables or fruit you will eat uncooked. If you take extra steps to make your water safe (see below for ways to do so), use this safe water to wash your fruits and vegetables. When you can, peel fruit that you will eat raw, after washing it. Do not eat or drink unpasteurized milk or dairy products. Cooking kills cryptosporidium. Therefore, cooked food and heat-processed foods are probably safe if, after cooking or processing, they are not handled by someone infected with cryptosporidium, or exposed to contaminated water.
Drink safe water
Do not drink water directly from shallow wells, lakes, rivers, springs, ponds, and streams. Because you cannot be sure if your tap water contains Cryptosporidium, you may wish to avoid drinking tap water, including water and ice from a refrigerator and drinks made at a fountain, which are usually made with tap water. Because public water quality and treatment vary throughout the United States, always check with the local health department and water utility to see if they have issued any special notices about the use of tap water by immunocompromised persons. You may also wish to take some additional measures: drinking certain commercially-bottled water, boiling your water, or filtering your water with certain home filters. Processed carbonated (bubbly) drinks in cans or bottles are probably safe, but drinks made at a fountain might not be because they are made with tap water. If you choose to take these extra measures, use them all the time, not just at home. If the public health department advises boiling the water, do not drink tap water unless you boil it.
A. Safe, commercially-bottled water.
Water labeled with any of the four messages below has been processed by a method effective against cryptosporidium
- Reverse osmosis treated
- Distilled
- Filtered through an absolute 1 micron or smaller filter
- “One micron absolute”
Drinks that ARE safe
- Carbonated (bubbly) drinks in cans or bottles
- Commercially-prepared fruit drinks in cans or bottles
- Steaming hot (175 °F [79.5 °C] or hotter) tea or coffee
- Pasteurized drinks
Juices made from fresh fruit can also be contaminated with cryptosporidium. For example, an outbreak of cryptosporidiosis occurred in Ohio resulting in people becoming ill after drinking apple cider made from apples contaminated with cryptosporidium. You may wish to avoid unpasteurized juices or fresh juices if you do not know how they were prepared.
Water labeled with the messages below MAY NOT have been processed by a method effective against cryptosporidium
- Filtered
- Micro-filtered
- Carbon-filtered
- Particle-filtered
- Multimedia-filtered
- Ozonated
- Ozone-treated
- Ultraviolet light-treated
- Activated carbon-treated
- Carbon dioxide-treated
- Ion exchange-treated
- Deionized
- Purified
- Chlorinated
B. Boiling water: Boiling is the best extra measure to ensure that your water is free of Cryptosporidium and other germs. Heating water at a rolling boil for 1 minute kills Cryptosporidium. After the boiled water cools, put it in a clean bottle or pitcher with a lid and store it in the refrigerator. Use the water for drinking, cooking, or making ice. Water bottles and ice trays should be cleaned with soap and water before use. Do not touch the inside of them after cleaning. If you can, clean water bottles and ice trays yourself.
C. Filtering tap water: Many but not all available home water filters remove Cryptosporidium. Filters that have the words “reverse osmosis” on the label protect against Cryptosporidium. Some other types of filters that function by micro-straining also work, but not all filters that are supposed to remove objects 1 micron or larger from water are the same. Look for the words “absolute 1 micron.” Some “1 micron” and most “nominal 1 micron” filters will not work against Cryptosporidium. Also look for the words like “Standard 53” or “Standard 58” and the words “cyst reduction” or “cyst removal” for a tested filter that works against Cryptosporidium. The wording should indicate that the filter is listed and labeled to NSF/ANSI standard 53 or 58 by an ANSI accredited certification organization.
Filters designed to remove cryptosporidium (any of the four messages below on a package label indicate that the filter should be able to remove cryptosporidium)
- Reverse osmosis (with or without NSF 53 or NSF 58 labeling)
- Absolute pore size of 1 micron or smaller (with or without NSF 53 or NSF 58 labeling)
- Tested and certified to NSF/ANSI Standard 53 or NSF/ANSI Standard 58 for cyst removal
- Tested and certified to NSF/ANSI Standard 53 or NSF/ANSI Standard 58 for cyst reduction
Because filter testing is expensive, some filters that may work against Cryptosporidium may not have been tested. Reverse-osmosis filters work against Cryptosporidium whether they have been tested or not. Other filters that may not have been tested also may work if they have an absolute pore size of 1 micron or smaller.
Filters labeled only with these words may NOT be designed to remove cryptosporidium
- Nominal pore size of 1 micron or smaller
- One micron filter
- Effective against Giardia
- Effective against parasites
- Carbon filter
- Water purifier
- EPA approved (Caution: EPA does not approve or test filters)
- EPA registered (Caution: EPA does not register filters based on their ability to remove Cryptosporidium)
- Activated carbon
- Removes chlorine
- Ultraviolet light
- Pentiodide resins
- Water softener
- Chlorinated
Filters collect germs from your water, so someone who is not immunocompromised should change the filter cartridges for you; if you do it yourself, wear gloves and wash your hands well with soap and water afterwards. Filters may not remove Cryptosporidium as well as boiling does because even good brands of filters may sometimes have manufacturing flaws that allow small numbers of Cryptosporidium parasites to get past the filter. Also, poor filter maintenance or failure to replace filter cartridges as recommended by the manufacturer can cause your filter to fail.
D. Home distillers: You can remove Cryptosporidium and other germs from your water with a home distiller. If you use one, you need to carefully store your water. After purification, put the water in a clean bottle or pitcher with a lid and store it in the refrigerator. Water bottles and ice trays should be cleaned with soap and water before use. Do not touch the inside of them after cleaning.
Take extra care when traveling
If you travel, particularly to developing nations, you may be at a greater risk for cryptosporidium because of poorer water treatment and food sanitation. Warnings about food, drinks, and swimming are especially important in such settings. Foods and beverages, in particular raw fruits and vegetables, tap water, ice made from tap water, unpasteurized milk or dairy products, and items purchased from street vendors might be contaminated. Steaming-hot foods, fruits you peel yourself, bottled and canned processed drinks, and hot coffee or hot tea are probably safe. Talk with your health care provider about other guidelines for travel abroad.
Cryptosporidium symptoms
Symptoms of cryptosporidiosis generally begin 2 to 10 days (average 7 days) after becoming infected with the cryptosporidium parasite. The most common symptom of cryptosporidiosis is watery diarrhea.
Symptoms include:
- Watery diarrhea
- Stomach cramps or pain
- Dehydration
- Nausea
- Vomiting
- Fever
- Weight loss
Some people with cryptosporidium will have no symptoms at all.
Symptoms usually last about 1 to 2 weeks (with a range of a few days to 4 or more weeks) in persons with healthy immune systems. Occasionally, people may experience a recurrence of symptoms after a brief period of recovery before the illness ends. Symptoms can come and go for up to 30 days.
While the small intestine is the site most commonly affected, in immunocompromised persons Cryptosporidium infections could possibly affect other areas of the digestive tract or the respiratory tract.
People with weakened immune systems may develop serious, chronic, and sometimes fatal illness. Examples of people with weakened immune systems include:
- people with AIDS;
- those with inherited diseases that affect the immune system; and
- cancer and transplant patients who are taking certain immunosuppressive drugs.
The risk of developing severe cryptosporidium disease may differ depending on each person’s degree of immune suppression.
Cryptosporidium diagnosis
Diagnosis of cryptosporidiosis is made by examination of stool samples. Because detection of Cryptosporidium can be difficult, patients may be asked to submit several stool samples over several days. Most often, stool specimens are examined microscopically using different techniques (e.g., acid-fast staining, direct fluorescent antibody [DFA] , and/or enzyme immunoassays for detection of Cryptosporidium sp. antigens).
Acid-fast staining methods, with or without stool concentration, are most frequently used in clinical laboratories. For greatest sensitivity and specificity, immunofluorescence microscopy is the method of choice (followed closely by enzyme immunoassays). Molecular methods are mainly a research tool.
Molecular methods (e.g., polymerase chain reaction – PCR) are increasingly used in reference diagnostic labs, since they can be used to identify Cryptosporidium at the species level. Tests for Cryptosporidium are not routinely done in most laboratories; therefore, healthcare providers should specifically request testing for this parasite.
Acid-fast staining test
The simplest way to diagnose cryptosporidium infection is a method called an acid-staining test, which identifies cryptosporidium under a microscope. To obtain cells for the analysis, your doctor might ask for a stool sample, or in more extreme cases, take a tissue sample (biopsy) from your intestine for the test.
Enzyme Immunoassays
At least four commercial EIA tests (see Table 1 below) have been introduced for the detection of cryptosporidial antigens in stool samples. These kits are reportedly superior to conventional microscopic examination (especially acid-fast staining methods) and show good correlation with the monoclonal antibody-based immunofluorescence assays. Kit sensitivities and specificities ranged from 66.3% to 100% and 93% to 100%, respectively ( Table 1).
Table 1. Commercially available diagnostic kits for detection of Cryptosporidium species (primarily in clinical specimens; partial list)
| Kit Name (Clinical specimens) | Manufacturer/distributor | Type of test1 | Sensitivity2 | Specificity2 | Comparison test | Reference |
|---|---|---|---|---|---|---|
| ProSpecT/ Cryptosporidium | Alexon, Inc. | EIA-plate | 97 98 96 94 (97) | 98 98 99.5 99 (98) | acid-fast stain, IIF3 acid-fast stain M-DIF4 M-DIF4, acid-fast, Color Vue | 4 5 6 7 |
| IDEIA Cryptosporidium | Dako Corp. | EIA-plate | 100 (93.1) | 100 (98.7) | auramine stain, N-DIF5 | 8 |
| MeriFluor™ Cryptosporidium/Giardia | Meridian Diagnostics, Inc. | DFA, IgG | 100 96 (100) | 100 100 (100) | acid-fast stain acid-fast, ProSpecT, Color Vue | 9 7 |
| Color Vue Cryptosporidium | Seradyn, Inc. | EIA-plate | 93 76 94 (92) | 93 100 100 (100) | IIF3 M-DIF4 M-DIF4, acid-fast, ProSpecT | 10 6 7 |
| Cryptosporidium Antigen Detection Microwell ELISA | LMD Laboratories | EIA-plate | 66.3 93 | 99.8 99 | acid-fast, auramine IIF3 |
- 1 EIA = enzyme immunoassay; DFA = direct immunofluorescence assay, IIF = indirect immunofluorescence assay, NA = not available
- 2 Percent specificity or specificity compared to conventional methods, numbers in parentheses indicate values reported by the manufacturer
- 3 IIF = indirect immunofluorescence (MeriFluor Cryptosporidium/Giardia assay)
- 4 M-DIF = direct immunofluorescence (MeriFluor Cryptosporidium/Giardia assay)
- 5 N-DIF = direct immunofluorescence (DetectIF Cryptosporidium, Shield Diagnostics, Ltd.)
Molecular Methods
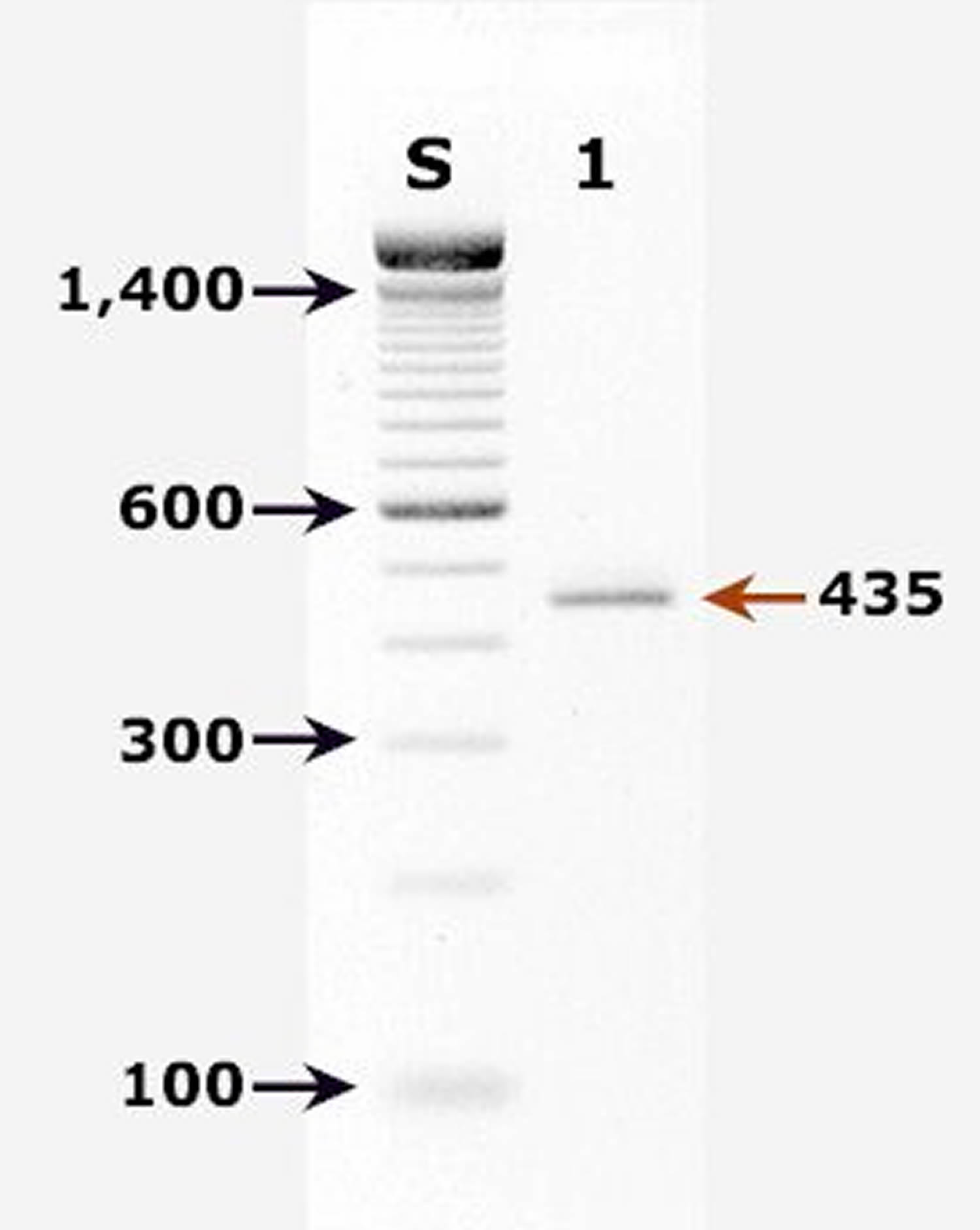
Agarose gel (2%) analysis of a PCR diagnostic test for detection of Cryptosporidium parvum DNA. PCR was performed using primers CPBDIAGF and CPBDIAGR 12.
- Lane S: Molecular base pair standard (100-bp ladder). Black arrows show the size of standard bands.
- Lane 1: C. parvum positive fecal specimen. The red arrow shows the diagnostic band of 435 bp for zoonotic Cryptosporidium parvum.
Figure 3. Cryptosporidium parvum DNA
Real-Time PCR
A TaqMan-based real-time PCR assay for detection and identification of Cryptosporidium parvum (bovine genotype) and Cryptosporidium hominis (human genotype) has been developed and validated at CDC. The assay combines the detection of two genomic targets: the 18S rRNA gene to achieve a sensitive detection of Cryptosporidium spp. and a gene with unknown function to provide species differentiation. Each DNA sample is run in two parallel reactions. The first consists of the highly sensitive detection of the Cryptosporidium 18S rRNA gene and the species-specific detection of Cryptosporidium parvum in a duplex format. The other reaction detects Cryptosporidium hominis on the species level.
Antibody detection
There are currently no commercially available serologic assays for the detection of Cryptosporidium-specific antibodies. However, immunoblots for detecting the 17 and 27 kDa sporozoite antigens associated with recent infection may be useful for epidemiologic investigations.
Cryptosporidium treatment
Most people who have healthy immune systems will recover without treatment. Diarrhea can be managed by drinking plenty of fluids to prevent dehydration. People who are in poor health or who have weakened immune systems are at higher risk for more severe and prolonged illness. Young children and pregnant women may be more susceptible to dehydration resulting from diarrhea and should drink plenty of fluids while ill. Rapid loss of fluids from diarrhea may be especially life threatening to babies. Therefore, parents should talk to their healthcare providers about fluid replacement therapy options for infants.
Anti-diarrheal medicine may help slow down diarrhea, but a healthcare provider should be consulted before such medicine is taken. Nitazoxanide has been FDA-approved for treatment of diarrhea caused by Cryptosporidium in people with healthy immune systems and is available by prescription. However, the effectiveness of nitazoxanide in immunosuppressed individuals is unclear.
FDA licensed nitazoxanide (Alinia®, Romark Laboratories, Tampa, FL, USA) for treatment of cryptosporidiosis in children aged 1-11 years in November 2002. In June 2004, nitazoxanide was also licensed for older children and adults. It can now be prescribed for all patients ≥ 1 year of age 13. Clinical cure (resolution of diarrhea) rates range from 72-88% 13. Parasitologic cure (no Cryptosporidium detected in stool) rates range from 60-75% 13. Parasitologic cure rate was a key consideration in developing prevention recommendations that ask people to refrain from swimming for 2 weeks after resolution of symptoms. Retesting of treated persons is not considered necessary.
HIV-positive individuals who suspect they have cryptosporidiosis should contact their healthcare provider. For those persons with AIDS, anti-retroviral therapy that improves the immune status will also decrease or eliminate symptoms of cryptosporidiosis. However, even if symptoms disappear, cryptosporidiosis is often not curable and the symptoms may return if the immune status worsens.
Table 2. Nitazoxanide dosage
| Immunocompetent Persons 14 | |
|---|---|
| Adult dosage | 500 mg twice daily x 3 days |
| Pediatric dosage | 1-3 years: 100 mg twice daily x 3 days |
| 4-11 years: 200 mg twice daily x 3 days | |
Nitazoxanide oral suspension (100 mg/5ml; patients ≥ 1 year of age) and Nitazoxanide tablets (500 mg; patients ≥ 12 years of age) are indicated for the treatment of diarrhea caused by Cryptosporidium.
How rapidly does the drug nitazoxanide work?
It may take up to 5 days for diarrhea to resolve in approximately 80% of patients 4. Because of this and the lower parasitologic cure rate, CDC still recommends that all infected persons, including those who have completed treatment, do not swim for 2 weeks after resolution of symptoms. It is critical that this recommendation is followed to prevent the spread of this chlorine-resistant parasite through public swimming pools and other aquatics venues.
Should patients be re-tested after treatment with nitazoxanide and, if so, when?
Healthcare professionals might consider re-testing stool at least 1 week after the last dose of nitazoxanide only if symptoms do not resolve. In such cases, longer courses of treatment might be needed. Persistent symptoms may also represent re-infection or other causes of illness besides cryptosporidiosis.
I’m still ill after treatment. What other treatment regimens have been tried?
Nitazoxanide appears to be well tolerated and different treatment regimens have been used for a variety of infections. Immunocompetent persons with cryptosporidiosis have been treated with multiple 3-day courses of nitazoxanide 15. Seven-day courses have also been used in early studies for cryptosporidiosis and other parasitic infections 16. AIDS patients with Cryptosporidium-associated diarrhea received the drug for 28 days 17. However, Nitazoxanide is presently not approved to treat immunodeficient persons because nitazoxanide oral suspension and nitazoxanide tablets have not been shown to be superior to placebo for the treatment of diarrhea caused by Cryptosporidium in HIV-infected or immunodeficient patients 13.
What about patients who are immunocompromised?
Nitazoxanide has been approved for treatment of diarrhea caused by Cryptosporidium in people with healthy immune systems. It is presently not approved to treat immunodeficient persons because nitazoxanide oral suspension and nitazoxanide tablets have not been shown to be superior to placebo for the treatment of diarrhea caused by Cryptosporidium in HIV-infected or immunodeficient patients 13.
If you have HIV/AIDS, highly active antiretroviral therapy (HAART) can reduce the viral load in your body and boost your immune response. Restoring your immune system to a certain level may completely resolve symptoms of cryptosporidiosis.
- Dziuban EJ, Liang JL, Craun GF, Hill V, Yu PA, Painter J, Moore MR, Calderon RL, Roy SL, Beach MJ; Centers for Disease Control and Prevention (CDC). Surveillance for waterborne disease and outbreaks associated with recreational water–United States, 2003-2004. MMWR Surveill Summ. 2006 55(12):1-30.[↩]
- The American Academy of Pediatrics. In: Pickering LK, Baker CJ, Long SS, McMillan JA, eds. Red Book: 2006 Report of the Committee on Infectious Diseases. 27th ed. Elk Grove Village IL.[↩]
- Scallan E, Hoekstra RM, Angulo FJ, Tauxe RV, Widdowson MA, Roy SL, Jones JL, Griffin PM. Foodborne illness acquired in the United States–major pathogens. Emerg Infect Dis. 2011;17(1):7-15.[↩]
- Xia Z, Sonnad S, Turner S, Marasigan M. Evaluation of a microtiter assay for detection of Cryptosporidium antigen in stool. 92nd Annual Meeting of the American Society for Microbiology, New Orleans, LA. 1992. p. 106.[↩]
- Dagan R, Fraser D, El-On J, Kassis I, Deckelbaum R, Turner S. Evaluation of an enzyme immunoassay for the detection of Cryptosporidium spp. in stool specimens from infants and young children in field studies. Am J Trop Med Hyg 1995;52:134.[↩]
- Aarnaes SL, Blanding J, Speier S, Forthal D, de la Maza LM, Peterson EM. Comparison of the ProSpecT and Color Vue enzyme-linked immunoassays for the detection of Cryptosporidium in stool specimens. Diagn Microbiol Infect Dis 1994;19:221.[↩][↩]
- Kehl KSC, Cicirello H, Havens PL. Comparison of four different methods for detection of Cryptosporidium species. J. Clin Microbiol 1995;33:416.[↩][↩][↩]
- Siddons CA, Chapman PA, Rush BA. Evaluation of an enzyme immunoassay kit for detecting Cryptosporidium in faeces and environmental samples. J Clin Pathol 1992;45:479.[↩]
- Garcia LS, Shum AC, Bruckner DA. Evaluation of a new monoclonal antibody combination reagent for the direct fluorescent detection of Giardia cysts and Cryptosporidium oocysts in human fecal specimens. J Clin Microbiol 1992;30:3255.[↩]
- Sloan LM, Rosenblatt JE. Evaluation of an immunoassay for the detection of Cryptosporidium stool specimens. 91st Annual Meeting of the American Society for Microbiology, Dallas, TX. 1991. p. 22.[↩]
- Cryptosporidiosis Laboratory Diagnosis. https://www.cdc.gov/dpdx/cryptosporidiosis/dx.html[↩]
- Johnson DW, Pieniazek NJ, Griffin DW, Misener L, Rose JB. Development of a PCR protocol for sensitive detection of Cryptosporidium oocysts in water samples. Appl Environ Microbiol 1995;61:3849-55.[↩]
- Fox LM, Saravolatz LD. Nitazoxanide: a new thiazolide antiparasitic agent. Clin Infect Dis. 2005 40(8):1173-80.[↩][↩][↩][↩][↩]
- The Medical Letter, Drugs for Parasitic Infections. 2007. https://www.accessdata.fda.gov/drugsatfda_docs/label/2005/021818lbl.pdf[↩]
- Diaz E, Mondragon J, Ramirez E, Bernal R. Epidemiology and control of intestinal parasites with nitazoxanide in children in Mexico. Am J Trop Med Hyg. 2003 68(4):384-5.[↩]
- Favennec L, Jave Ortiz J, Gargala G, Lopez Chegne N, Ayoub A, Rossignol JF. Double-blind, randomized, placebo-controlled study of nitazoxanide in the treatment of fascioliasis in adults and children from northern Peru. Aliment Pharmacol Ther. 2003 17(2):265-70.[↩]
- Rossignol JF, Hidalgo H, Feregrino M, Higuera F, Gomez WH, Romero JL, Padierna J, Geyne A, Ayers MS. A double-‘blind’ placebo-controlled study of nitazoxanide in the treatment of cryptosporidial diarrhea in AIDS patients in Mexico. Trans R Soc Trop Med Hyg. 1998 92(6):663-6.[↩]