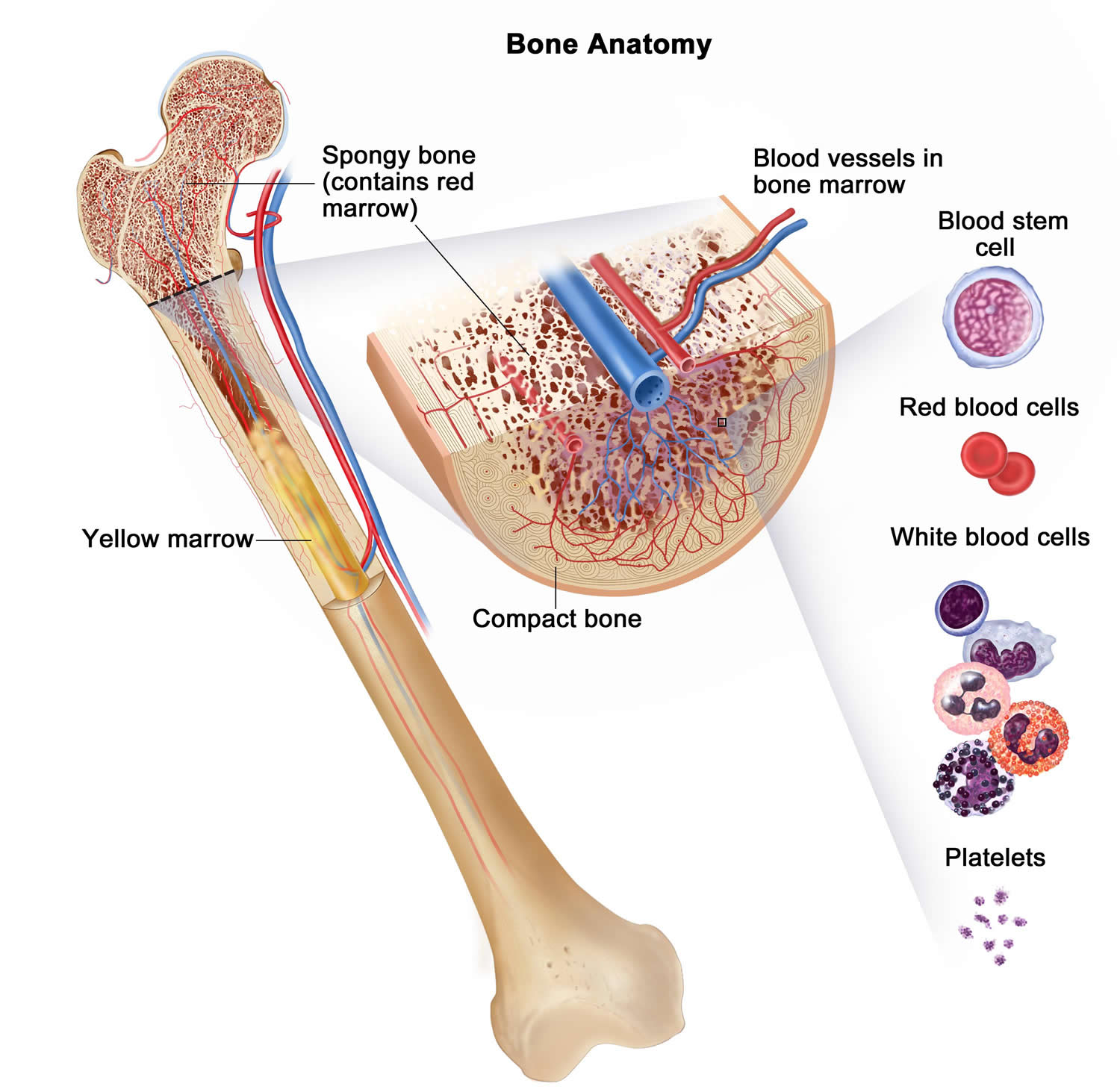
What is myelodysplastic syndrome
Myelodysplastic syndromes (MDS) are conditions that can occur when the blood-forming cells in the bone marrow become abnormal. This leads to low numbers of one or more types of blood cells. Myelodysplastic syndrome is considered a type of cancer.
In a healthy person, bone marrow makes new, immature blood cells that mature over time. Myelodysplastic syndromes occur when something disrupts this process so that the blood cells don’t mature and are abnormal (dysplastic) and the bone marrow have problems making new blood cells. Instead of developing normally, many of the blood cells formed by these bone marrow cells are defective and the blood cells die in the bone marrow or just after entering the bloodstream. Over time, there are more immature, defective cells than healthy ones, leading to problems such as fatigue caused by anemia, infections caused by leukopenia, and bleeding caused by thrombocytopenia. Different cell types can be affected, although the most common finding in myelodysplastic syndrome is a shortage of red blood cells (anemia).
The number of people diagnosed with myelodysplastic syndromes in the United States each year is not known for sure. Some estimates have put this number at about 10,000, while other estimates have been much higher.
Myelodysplastic syndrome is uncommon before age 50, and the risk increases as a person gets older. Myelodysplastic syndromes is most commonly diagnosed in people in their 70s. The number of new cases diagnosed each year is likely increasing as the average age of the US population increases.
There are several different types of myelodysplastic syndrome, based on how many types of blood cells are affected and other factors.
In about 1 in 3 patients, myelodysplastic syndrome can progress to a rapidly growing cancer of bone marrow cells called acute myeloid leukemia (AML). In the past, myelodysplastic syndrome was sometimes referred to as pre-leukemia or smoldering leukemia. Because most patients do not get leukemia, myelodysplastic syndrome used to be classified as a disease of low malignant potential. Now that doctors have learned more about myelodysplastic syndrome, it is considered to be a form of cancer.
Normal bone marrow
Bone marrow is found in the middle of certain bones. It is made up of blood-forming cells, fat cells, and supporting tissues. A small fraction of the blood-forming cells are blood stem cells. Stem cells are needed to make new blood cells.
There are 3 main types of blood cells: red blood cells, white blood cells, and platelets.
Red blood cells pick up oxygen in the lungs and carry it to the rest of the body. These cells also bring carbon dioxide back to the lungs. Having too few red blood cells is called anemia. It can make a person feel tired and weak and look pale. Severe anemia can cause shortness of breath.
White blood cells (also known as leukocytes) are important in defending the body against infection. There are different types of white blood cells:
- Granulocytes are white blood cells that have granules that can be seen under the microscope. In the bone marrow, granulocytes develop from young cells called myeloblasts. The most common type of granulocyte is the neutrophil. When the number of neutrophils in the blood is low, the condition is called neutropenia. This can lead to severe infections.
- Monocytes are also important in protecting the body against germs. The cells in the bone marrow that turn into monocytes are called monoblasts.
- Lymphocytes make proteins called antibodies that help the body fight germs. They can also directly kill invading germs. Lymphocytes are not usually abnormal in myelodysplastic syndrome.
Platelets are thought of as a type of blood cell, but they are actually small pieces of a cell. They start as a large cell in the bone marrow called the megakaryocyte. Pieces of this cell break off and enter the bloodstream as platelets. You need platelets for your blood to clot. They plug up damaged areas of blood vessels caused by cuts or bruises. A shortage of platelets, called thrombocytopenia, can result in abnormal bleeding or bruising.
Figure 1. Bone marrow anatomy
Myelodysplastic Syndromes Types
Myelodysplastic syndromes (MDS) are classified using the World Health Organization (WHO) classification system, which was most recently updated in 2016. It divides MDS into types based mainly on how the cells in the bone marrow look under the microscope, as well as some other factors:
- How many early forms of cell types in the bone marrow (red blood cells, white blood cells, or platelets) show dysplasia (look abnormal under the microscope).
- How many types of low blood cell counts (cytopenias) a person has.
- What portion of early red blood cells are ring sideroblasts (cells that contain rings of iron deposits around the nucleus).
- The portion of blasts (very early forms of blood cells) in the bone marrow or blood.
- Certain chromosome changes in the bone marrow cells.
Based on these factors, the WHO system recognizes 6 main types of myelodysplastic syndrome:
- Myelodysplastic syndrome with multilineage dysplasia (MDS-MLD)
- Myelodysplastic syndrome with single lineage dysplasia (MDS-SLD)
- Myelodysplastic syndrome with ring sideroblasts (MDS-RS)
- Myelodysplastic syndrome with excess blasts (MDS-EB)
- Myelodysplastic syndrome with isolated del(5q)
- Myelodysplastic syndrome unclassifiable (MDS-U)
Because small differences in the way the cells look can change the diagnosis, doctors may sometimes disagree on a patient’s exact type of myelodysplastic syndrome.
Myelodysplastic syndrome with multilineage dysplasia
In myelodysplastic syndrome with multilineage dysplasia:
- Dysplasia is seen in at least 10% of the early cells of 2 or 3 cell types (red blood cells, white blood cells, and/or megakaryocytes [the cells that make platelets]) in the bone marrow.
- The person has low numbers of at least 1 type of blood cell.
- There is a normal number (less than 5%) of very early cells called blasts in the bone marrow, and blasts are rare (or absent) in the blood.
This is the most common type of myelodysplastic syndrome. In the past, it was referred to as refractory cytopenia with multilineage dysplasia.
Myelodysplastic syndrome with single lineage dysplasia
In myelodysplastic syndrome with single lineage dysplasia:
- Dysplasia is seen in at least 10% of the early cells of 1 cell type (either red blood cells, white blood cells, or megakaryocytes [the cells that make platelets]) in the bone marrow.
- The person has low numbers of 1 or 2 types of blood cells, but normal numbers of the other type(s).
- There is a normal number (less than 5%) of very early cells called blasts in the bone marrow, and blasts are rare (or absent) in the blood.
This type of myelodysplastic syndrome is not common. It seldom, if ever, progresses to acute myeloid leukemia (AML). Patients with this type of myelodysplastic syndrome can often live a long time, even without treatment.
This was referred to as refractory cytopenia with unilineage dysplasia in the previous classification system. It includes refractory anemia, refractory neutropenia, and refractory thrombocytopenia, depending on which cell type is affected.
Myelodysplastic syndrome with ring sideroblasts
In this type of myelodysplastic syndrome, many of the early red blood cells are ring sideroblasts. For this diagnosis, at least 15% of the early red blood cells must be ring sideroblasts (or at least 5% if the cells also have a mutation in the SF3B1 gene).
This condition is further divided into 2 types, based on how many of the cell types in the bone marrow are affected by dysplasia:
- Myelodysplastic syndrome with ring sideroblasts with single lineage dysplasia: dysplasia in only one cell type
- Myelodysplastic syndrome with ring sideroblasts with multilineage dysplasia: dysplasia in more than one cell type
This type of myelodysplastic syndrome is not common. It rarely turns into AML, and the outcome for people with this type is generally better than for some other types of myelodysplastic syndrome. This was previously referred to as refractory anemia with ring sideroblasts.
Myelodysplastic syndrome with excess blasts
In this type of myelodysplastic syndrome, there are more blasts than normal in the bone marrow and/or blood. The person also has low numbers of at least one type of blood cell. There may or may not be severe dysplasia in the bone marrow.
This condition is further divided into 2 types, based on how many of the cells in the bone marrow or blood are blasts:
- Myelodysplastic syndrome with excess blasts 1: blasts make up 5% to 9% of the cells in the bone marrow, or 2% to 4% of the cells in the blood
- Myelodysplastic syndrome with excess blasts 2: blasts make up 10% to 19% of the cells in the bone marrow, or 5% to 19% of the cells in the blood
This type accounts for about 1 in 4 cases of myelodysplastic syndrome. It is one of the types most likely to turn into AML, with the risk being higher for myelodysplastic syndrome with excess blasts 2 than for myelodysplastic syndrome with excess blasts 1. This was previously referred to as refractory anemia with excess blasts.
Myelodysplastic syndrome with isolated del(5q)
In this type of myelodysplastic syndrome, the chromosomes of the bone marrow cells are missing part of chromosome number 5. (There may also be one other chromosome abnormality, as long as it isn’t a loss of part or all of chromosome 7.) The person also has low numbers of 1 or 2 types of blood cells (usually red blood cells), and there is dysplasia in at least 1 cell type in the bone marrow.
This type of myelodysplastic syndrome is not common. It occurs most often in older women. For reasons that aren’t clear, patients with this type of myelodysplastic syndrome tend to have a good prognosis (outlook). They often live a long time and rarely go on to develop AML.
Myelodysplastic syndrome unclassifiable
This type of myelodysplastic syndrome is uncommon. For myelodysplastic syndrome unclassifiable, the findings in the blood and bone marrow don’t fit any other type of myelodysplastic syndrome. For example, the numbers of any one of the cell types may be low in the blood, but less than 10% of that type of cell looks abnormal in the bone marrow. Or the cells in the bone marrow have at least one certain chromosome abnormality that is only seen in myelodysplastic syndrome or leukemia.
This type is rare, so it has not been studied well enough to predict prognosis (outlook).
Clinical classification of myelodysplastic syndrome
Along with the WHO classification, myelodysplastic syndrome can also be classified based on the underlying cause. This is known as a clinical classification.
- If no cause can be identified, it’s called primary myelodysplastic syndrome. (This type is more common.)
- When the cause of the disease is known, it’s called secondary myelodysplastic syndrome.
Secondary myelodysplastic syndrome is often related to prior cancer treatment, or it develops in someone who already had a different bone marrow disease. This is discussed further in Risk Factors for Myelodysplastic Syndrome.
Identifying myelodysplastic syndrome as primary or secondary is important because the secondary type is much less likely to respond to treatment.
Myelodysplastic syndrome complications
Complications of myelodysplastic syndromes include:
- Anemia. Reduced numbers of red blood cells can cause anemia, which can make you feel tired.
- Recurrent infections. Having too few white blood cells increases your risk of serious infections.
- Bleeding that won’t stop. Lacking platelets in your blood to stop bleeding can lead to excessive bleeding.
- Increased risk of cancer. Some people with myelodysplastic syndromes might eventually develop a cancer of the blood cells (leukemia).
Myelodysplastic syndrome prognosis
Myelodysplastic Syndrome Prognostic Scores
Myelodysplastic syndromes are diseases of the bone marrow. The outlook for these cancers isn’t based on the size of a tumor or whether the cancer has spread. Because of this, doctors use other factors to predict outlook and decide when to treat. Some of these factors have been combined to develop scoring systems.
Revised International Prognostic Scoring System
The revised International Prognostic Scoring System is based on 5 factors:
- The percentage of blasts (very early forms of blood cells) in the bone marrow
- The type and number of chromosome abnormalities in the cells
- The level of red blood cells (measured as hemoglobin) in the patient’s blood
- The level of platelets in the patient’s blood
- The level of neutrophils (a type of white blood cell) in the patient’s blood
Each factor is given a score, with the lowest scores having the best outlook. Then the scores for the factors are added up to put people with myelodysplastic syndrome into 5 risk groups:
- Very low risk
- Low risk
- Intermediate risk
- High risk
- Very high risk
These risk groups can be used to help predict a person’s outlook. This can be helpful when trying to determine the best treatment options.
This system has some important limitations. For example, it was developed before many of the current treatments for myelodysplastic syndrome were available, so it only took into account people who were not treated for their myelodysplastic syndrome. It also did not include people who have myelodysplastic syndrome as a result of getting chemotherapy (secondary myelodysplastic syndrome). But this system can still be helpful and is still widely used.
WHO Prognostic Scoring System
The World Health Organization (WHO) scoring system is based on 3 factors:
- The type of myelodysplastic syndrome based on the WHO classification (For example, myelodysplastic syndrome-unclassifiable, myelodysplastic syndrome with ring sideroblasts single lineage dysplasia, and myelodysplastic syndrome-del(5q) tend to have the best outlook, whereas myelodysplastic syndrome with excess blasts tends to have the worst.)
- Chromosome abnormalities (grouped as good, intermediate, or poor)
- Whether or not the patient needs regular blood transfusions
Each factor is given a score, with the lowest scores having the best outlook. Then the scores are added up to put people with myelodysplastic syndrome into 5 risk groups:
- Very low risk
- Low risk
- Intermediate risk
- High risk
- Very high risk
These risk groups can be used to help predict a person’s outlook, as well as how likely the myelodysplastic syndrome is to transform into acute myeloid leukemia (AML). This can be helpful when trying to determine the best treatment options. But as with the Revised International Prognostic Scoring System, this system has some important limitations. For example, it does not include people who have myelodysplastic syndrome as a result of getting chemotherapy (known as secondary myelodysplastic syndrome).
Both the Revised International Prognostic Scoring System and the WHO Prognostic Scoring System can be complex, and different doctors might use different systems. If you have myelodysplastic syndrome, talk to your doctor about which system they use, which risk group you are in, and what it might mean for your treatment and outlook.
Other prognostic factors
Along with the factors used in these scoring systems, doctors have found other factors that can also help predict a person’s outlook. These include:
- A person’s age
- A person’s performance status (how well they’re able to do normal daily activities)
- The severity of low blood cell counts
- The results of certain blood tests, such as the serum ferritin level
- Certain gene or chromosome changes that are not accounted for in the scoring systems.
Myelodysplastic syndrome life expectancy
Survival stats are often based on previous outcomes of large numbers of people who had the disease, but they can’t predict what will happen in any particular person’s case. There are some limitations to remember:
- The numbers below are based on patients diagnosed with a myelodysplastic syndrome (myelodysplastic syndrome) some time ago. Improvements in treatment since these numbers were gathered may result in a better outlook for people now being diagnosed with myelodysplastic syndrome.
- These numbers are based on prognostic scores that take into account certain factors, such as the type of myelodysplastic syndrome, the results of certain blood tests, and whether the abnormal cells have certain chromosome changes. But other factors might also affect a person’s outlook, such as the patient’s age and health, and how well the disease responds to treatment.
Your doctor can tell you how the numbers below apply to you, as he or she is familiar with your particular situation.
Survival statistics for myelodysplastic syndrome
Remember, these survival statistics are only estimates – they can’t predict what will happen to any individual person. Many other factors can also affect a person’s outlook. We understand that these statistics can be confusing and may lead you to have more questions. Talk to your doctor to better understand your specific situation.
The following survival statistics are based on the Revised International Prognostic Scoring System risk groups. It’s important to note that this system is based largely on people who were diagnosed many years ago and who did not get treatments such as chemotherapy for their myelodysplastic syndrome.
Table 1. Myelodysplastic syndrome life expectancy – Revised International Prognostic Scoring System risk groups
| Revised International Prognostic Scoring System Risk Group | Median survival |
| Very low | 8.8 years |
| Low | 5.3 years |
| Intermediate | 3 years |
| High | 1.6 years |
| Very high | 0.8 years |
The WHO Prognostic Scoring System risk groups can also be used to predict outcome – both median survival and the chance that the myelodysplastic syndrome will transform into acute myeloid leukemia (AML) within 5 years. These statistics were published in 2007 based on patients diagnosed between 1982 and 2004.
Table 2. Myelodysplastic syndrome life expectancy – WHO Prognostic Scoring System risk groups
| WHO Prognostic Scoring System Risk Group | Median Survival | Risk of AML (within 5 years) |
| Very low | 11.8 years | 3% |
| Low | 5.5 years | 14% |
| Intermediate | 4 years | 33% |
| High | 2.2 years | 54% |
| Very high | 9 months | 84% |
Myelodysplastic syndrome causes
Some cases of myelodysplastic syndrome are linked to known risk factors, but most often, the cause is unknown.
Scientists have made great progress in understanding how certain changes in the DNA in bone marrow cells may cause myelodysplastic syndrome to develop. DNA is the chemical that makes up your genes, which control how your cells function. You usually look like your parents because they are the source of your DNA. But DNA affects more than the way you look.
Some genes control when our cells grow, divide into new cells, and die:
- Certain genes that help cells grow, divide, and stay alive are called oncogenes.
- Genes that help keep cell division under control, or cause cells to die at the right time are called tumor suppressor genes.
Cancers can be caused by gene mutations (defects) that turn on oncogenes or turn off tumor suppressor genes.
Usually mutations in several different genes inside bone marrow cells are needed before a person develops myelodysplastic syndrome. Some of the mutations most often seen in myelodysplastic syndrome cells include those in the DNMT3A, TET2, ASXL1, TP53, RUNX1, SRSF2, and SF3B1 genes. Some of these gene changes can be inherited from a parent, but more often they happen during a person’s lifetime.
Inherited gene changes
Researchers have found the gene changes that cause some rare inherited syndromes (like familial platelet disorder with a propensity to myeloid malignancy) linked to an increased risk of developing myelodysplastic syndrome. This syndrome is caused by inherited changes in the RUNX1 gene. Normally, this gene helps control the development of blood cells. Changes in this gene can lead to blood cells not maturing like they normally would, which can increase the risk of developing myelodysplastic syndrome.
Gene changes acquired during a person’s lifetime
Often, it’s not known why people without inherited syndromes develop myelodysplastic syndrome.
Some outside exposures can lead to myelodysplastic syndrome by damaging the DNA inside bone marrow cells. For example, tobacco smoke contains chemicals that can damage genes. Exposure to radiation or certain chemicals such as benzene or some chemotherapy drugs can also cause mutations that lead to myelodysplastic syndrome.
But sometimes the gene changes that lead to myelodysplastic syndrome seem to occur for no apparent reason. Many of these gene changes are probably just random events that sometimes happen inside a cell, without having an outside cause.
Gene changes inside cells can build up over a person’s lifetime, which might help explain why myelodysplastic syndrome largely affects older people.
Risk Factors for Myelodysplastic Syndromes
A risk factor is anything that changes your chance of getting a disease such as cancer. Different cancers have different risk factors. Some risk factors, like smoking, you can change. Others, like your age or family history, can’t be changed.
But having a risk factor, or even several, does not always mean that a person will get the disease, and many people get cancer without having any known risk factors.
There are several known risk factors for myelodysplastic syndromes.
Older age
Older age is one of the most important risk factors for myelodysplastic syndrome. Myelodysplastic syndrome is uncommon in people younger than 50, and most cases are found in people in their 70s or 80s.
Sex
Myelodysplastic syndrome is more common in men than in women. The reason for this is not clear, although it might have to do with men having been more likely to smoke or to be exposed to certain chemicals in the workplace in the past.
Cancer treatment
Prior treatment with chemotherapy (chemo) is another important risk factor for myelodysplastic syndrome. Patients who have been treated with certain chemo drugs for cancer are more likely to develop myelodysplastic syndrome later on. When myelodysplastic syndrome is caused by cancer treatment it is called secondary myelodysplastic syndrome or treatment-related myelodysplastic syndrome.
Some of the drugs that can lead to myelodysplastic syndrome include:
- Mechlorethamine (nitrogen mustard)
- Procarbazine
- Chlorambucil
- Cyclophosphamide
- Ifosfamide
- Etoposide
- Teniposide
- Doxorubicin
The risk of secondary myelodysplastic syndrome varies based on the type and doses of drugs. It might also be affected by the type of cancer the chemo is treating. Combining these drugs with radiation therapy increases the risk further. People who have had stem cell transplants (bone marrow transplants) can also develop myelodysplastic syndrome because of the very high doses of chemo they received. Still, only a small percentage of people who are treated with these medicines will eventually develop myelodysplastic syndrome.
Genetic syndromes
People with certain inherited syndromes are more likely to develop myelodysplastic syndrome. These syndromes are caused by abnormal (mutated) genes that have been passed on from one or both parents. Examples include:
- Fanconi anemia
- Shwachman-Diamond syndrome
- Diamond Blackfan anemia
- Familial platelet disorder with a propensity to myeloid malignancy
- Severe congenital neutropenia
- Dyskeratosis congenita
Familial myelodysplastic syndrome
In some families, myelodysplastic syndrome occurs more often than would be expected. Sometimes this is due to a known gene mutation that runs in the family, but in other cases the cause isn’t clear.
Smoking
Smoking increases the risk of myelodysplastic syndrome. Many people know that smoking can cause cancer of the lungs, but it can also cause cancer in other parts of the body that don’t come into direct contact with smoke. Cancer-causing substances in tobacco smoke are absorbed into the blood as it passes through the lungs. Once in the bloodstream, these substances spread to many parts of the body.
Environmental exposures
Some environmental exposures have been linked to myelodysplastic syndrome:
- High-dose radiation exposure (such as surviving an atomic bomb blast or nuclear reactor accident) increases the risk of developing myelodysplastic syndrome.
- Long-term workplace exposure to benzene and certain chemicals used in the petroleum and rubber industries can also increase the risk of developing myelodysplastic syndrome.
Myelodysplastic syndromes prevention
There is no sure way to prevent myelodysplastic syndromes. But there are things you can do that might lower your risk.
Not smoking
Since smoking is linked to an increased risk of myelodysplastic syndrome, not smoking can lower the risk. Of course, nonsmokers are also less likely than smokers to develop many other types of cancers, as well as heart disease, stroke, and other diseases.
Avoiding exposure to radiation or certain chemicals
Avoiding known cancer-causing industrial chemicals, such as benzene, might lower your risk of developing myelodysplastic syndrome.
Treating cancer with radiation and certain chemotherapy drugs can increase the risk of myelodysplastic syndrome. Doctors are studying ways to limit the risk of myelodysplastic syndrome in patients who get these treatments. For some cancers, doctors may try to avoid using the chemotherapy drugs that are more likely to lead to myelodysplastic syndrome. Some people, however, may need these specific drugs. Often, the obvious benefits of treating life-threatening cancers with chemo and radiation therapy must be balanced against the small chance of developing myelodysplastic syndrome several years later.
Myelodysplastic syndrome symptoms
Myelodysplastic syndrome is sometimes found when a person sees a doctor because of signs or symptoms they are having. These signs and symptoms often do not show up in the early stages of myelodysplastic syndrome. But sometimes myelodysplastic syndrome is found before it causes symptoms because of an abnormal result on a blood test that was done as part of a routine exam or for some other health reason. Myelodysplastic syndrome that is found early does not always need to be treated right away, but it should be watched closely for signs that it’s progressing.
A main feature of myelodysplastic syndromes is that they cause low blood cell counts. In other cases, symptoms related to shortages of one or more types of blood cells (cytopenias) are the first sign of myelodysplastic syndrome:
- Having too few red blood cells (anemia) can lead to feeling tired, dizzy, or weak, as well as shortness of breath and pale skin.
- Not having enough normal white blood cells (leukopenia), especially cells called neutrophils (neutropenia), can lead to frequent or severe infections.
- Having too few blood platelets (thrombocytopenia) can lead to easy bruising and bleeding. Some people have frequent or severe nosebleeds or bleeding from the gums.
Other symptoms can include:
- Fatigue
- Weight loss
- Fever
- Bone pain
- Loss of appetite
- Unusual paleness (pallor) which occurs due to a low red blood cell count (anemia)
- Pinpoint-sized red spots just beneath your skin caused by bleeding (petechiae)
These symptoms are more likely to be caused by something other than myelodysplastic syndrome. Still, if you have any of these symptoms, especially if they don’t go away or get worse over time, see your doctor so that the cause can be found and treated, if needed.
Myelodysplastic syndrome diagnosis
A physical exam, medical history and tests might be used if your doctor suspects you have a myelodysplastic syndrome.
Tests might include:
- Blood tests. Your doctor might order a number of blood tests to determine the number of red cells, white cells and platelets and look for unusual changes in the size, shape and appearance of various blood cells. The complete blood count (CBC) is a test that measures the levels of red blood cells, white blood cells, and platelets in your blood. The CBC is often done with a differential count, which is a count of the different types of white blood cells in the blood sample. In a blood smear, some of the blood is put on a slide to see how the cells look under the microscope. The doctor may also order tests to check for other possible causes of low blood counts. For example, low levels of iron, vitamin B12, or folate can cause anemia. If one of these is found to be abnormal, a diagnosis of myelodysplastic syndrome is much less likely. Blood abnormalities may suggest myelodysplastic syndrome, but the doctor cannot make an exact diagnosis without examining a sample of your bone marrow cells.
- Removing bone marrow for testing. During a bone marrow biopsy and aspiration, a thin needle is used to withdraw (aspirate) a small amount of liquid bone marrow, usually from a spot on the back of your hipbone. Then a small piece of bone with its marrow is removed (biopsy). The samples are examined in a laboratory to look for abnormalities. The doctors will look at the size, shape, and other features of the cells. The percentage of cells in the bone marrow or blood that are blasts (very early forms of blood cells) is particularly important. In myelodysplastic syndrome, the blasts do not mature properly, so there may be too many blasts and not enough mature cells.
- For a diagnosis of myelodysplastic syndrome, a patient must have less than 20% blasts in the bone marrow and blood. A patient who has more than 20% blasts is considered to have acute myeloid leukemia (AML).
- Other types of lab tests can also be done on the bone marrow or blood samples to helpdiagnose myelodysplastic syndrome:
- Flow cytometry and immunocytochemistry: For both flow cytometry and immunocytochemistry, samples of cells are treated with antibodies, which are proteins that stick only to certain other proteins on cells. For immunocytochemistry, the cells are then looked at under a microscope to see if the antibodies stuck to them (meaning they have these proteins), while for flow cytometry a special machine is used. These tests can be helpful in distinguishing different types of myelodysplastic syndrome or leukemia from one another and from other diseases.
- Chromosome tests: These tests look at the chromosomes (long strands of DNA) inside the cells. Each cell should have 46 chromosomes (23 pairs). Abnormal chromosomes are common in myelodysplastic syndrome.
- Cytogenetics: In this test, the cells are looked at under a microscope to see if the chromosomes have any abnormalities. A drawback of this test is that it usually takes about 2 to 3 weeks because the cells must grow in lab dishes for a couple of weeks before their chromosomes can be viewed. The results of cytogenetic testing are written in a shorthand form that describes which chromosome changes are present. For example:
- A minus sign (-) or the abbreviation “del” is used to mean a deletion. For example, if a copy of chromosome 7 is missing, it can be written as -7 or del(7). Often, only a part of the chromosome is lost. There are 2 parts to a chromosome, called p and q. The loss of the q part of chromosome 5 is written 5q- or del(5q).
- A plus sign is used when there is an addition (an extra copy of all or part of a chromosome). +8, for example, means that chromosome 8 has been duplicated, and there are too many copies of it within the cell.
- The letter t is used to indicate a translocation, in which parts of two chromosomes have traded places with each other. For example, if chromosomes 8 and 21 have swapped pieces, it would be written as t(8;21)
- Certain chromosome changes in myelodysplastic syndrome cells can help predict the likely course of myelodysplastic syndrome. For example, a deletion of a part of chromosome 5, or del(5q), usually predicts a better outcome (as long as there is no more than one other chromosome change, and it isn’t a loss of part of chromosome 7). Changes in 3 or more chromosomes or the deletion of chromosome 7 tend to have a poorer outlook.
- Fluorescent in situ hybridization (FISH): This test looks more closely at cell DNA using fluorescent dyes that only attach to specific gene or chromosome changes. An advantage of FISH is that it doesn’t require actively dividing cells, so it can usually provide results within a couple of days. FISH is very good for finding translocations – it can even find some that may be too small to be seen with usual cytogenetic testing.
- Polymerase chain reaction (PCR): This is a very sensitive DNA test that can also find some chromosome changes too small to be seen under a microscope, even if there are very few abnormal cells in a sample.
- Cytogenetics: In this test, the cells are looked at under a microscope to see if the chromosomes have any abnormalities. A drawback of this test is that it usually takes about 2 to 3 weeks because the cells must grow in lab dishes for a couple of weeks before their chromosomes can be viewed. The results of cytogenetic testing are written in a shorthand form that describes which chromosome changes are present. For example:
Myelodysplastic syndrome treatment
Treatment for myelodysplastic syndromes most often targets slowing disease progression, managing symptoms, such as fatigue, and preventing bleeding and infections.
If you have no symptoms, your doctor might recommend watchful waiting with regular exams and lab tests to see if the disease progresses.
Research on myelodysplastic syndromes is ongoing. Ask your doctor about clinical trials for which you might be eligible.
Supportive Therapy
Supportive therapies are treatments that help treat (or prevent) the symptoms or complications of myelodysplastic syndromes, as opposed to treating the myelodysplastic syndrome directly. Supportive therapy might be used alone or along with other treatments for myelodysplastic syndrome.
For example, for many patients with myelodysplastic syndrome, one of the main goals of treatment is to prevent the problems caused by low blood cell counts.
Treating low red blood cell counts (anemia)
Low red blood cell counts (anemia) can cause severe fatigue and other symptoms. Patients with myelodysplastic syndrome and anemia that’s causing symptoms might benefit from getting injections of a manmade version of the growth factor erythropoietin, which can sometimes help the bone marrow make new red blood cells.
If this isn’t helpful, red blood cell transfusions might be needed. Some people are concerned about a slight risk of infections (such as hepatitis or HIV) spread by blood transfusion, but this possibility is very unlikely, and the benefits of the transfused cells greatly outweigh this risk.
Treating iron build up from blood transfusions
Blood transfusions can cause excess iron to build up in the body. The iron can build up over time in the liver, heart, and other organs, affecting how they function. This is usually seen only in people who receive many transfusions over a period of years. Patients at risk for iron overload are often advised to avoid taking iron supplements or multivitamins that contain iron.
Drugs called chelating agents, which bind with the iron so that the body can get rid of it, can be used in patients who develop iron overload from red blood cell transfusions (unless they have poor kidney function).
- Deferoxamine (Desferal) is usually given as an infusion under the skin, using a small, portable pump. This can be inconvenient because the infusion must be done slowly (over at least 8 hours) each day or on most days of the week.
- Deferasirox (Exjade, Jadenu) is a newer drug that is taken by mouth (as a tablet, dissolved in juice or water, or sprinkled on food) once a day.
Treating low platelet counts
Myelodysplastic syndrome patients with low platelet counts might have problems with bleeding or bruising easily. The options for treating a shortage of platelets might include platelet transfusions or treatment with certain growth factor drugs. If bleeding is not helped by these treatments, another option might be treatment with a drug called an antifibrinolytic agent, such as aminocaproic acid (Amicar).
Treating low white blood cell counts
Patients with low white blood cell counts are more likely to get infections, and the infections are more likely to be serious. It’s important to avoid cuts and scrapes, and take care of them right away if they do happen. Patients should tell their doctors right away about any possible signs of infection, such as fever, signs of pneumonia (cough, shortness of breath), or urinary infection (burning when urinating).
Doctors typically treat known or suspected bacterial infections with antibiotics. For serious infections, a white blood cell growth factor may also be used. This drug can raise the white blood cell count to help fight the infection.
Blood transfusions
Blood transfusions can be used to replace red blood cells, white blood cells or platelets in people with myelodysplastic syndromes.
Medications
Treatment for myelodysplastic syndromes might include medications that:
- Increase the number of blood cells your body makes. Called growth factors, these medications are artificial versions of substances found naturally in your bone marrow. Some growth factors, such as epoetin alfa (Epogen, Procrit) or darbepoetin alfa (Aranesp), reduce the need for blood transfusions by increasing red blood cells. Others, such as filgrastim (Neupogen, Zarxio) might help prevent infections by increasing white blood cells in people with certain myelodysplastic syndromes.
- Red blood cell growth factors:
- Epoetin (Epogen or Procrit) is a manmade version of the growth factor erythropoietin, which promotes red blood cell production. It can help some patients avoid red blood cell transfusions. Giving some patients both epoetin and G-CSF.
- Darbepoetin alfa (Aranesp) is a long-acting form of erythropoietin. It works in the same way but was designed to be given less often.
- White blood cell growth factors:
- Granulocyte colony stimulating factor ( G-CSF, fligrastim, or Neupogen) and granulocyte macrophage-colony stimulating factor (GM-CSF, sargramostim, or Leukine) can improve white blood cell production. These are not used routinely to prevent infections, but they can help some MDS patients whose main problem is a shortage of white blood cells and who have frequent infections.
- Pegfilgrastim (Neulasta) is a long-acting form of G-CSF. It works in the same way but can be given less often.
- Platelet growth factors:
- Drugs called thrombopoietin-receptor agonists, such as romiplostim (Nplate) and eltrombopag (Promacta) might help some people with MDS who have very low platelet levels, although this is still being studied.
- A drug called oprelvekin (interleukin-11, IL-11, or Neumega) can be used to raise platelet counts after chemotherapy and in some other diseases. But for most MDS patients, this drug has not been found to be very helpful.
- Stimulate blood cells to mature. Medications such as azacitidine (Vidaza) and decitabine (Dacogen) might improve the quality of life of people with certain myelodysplastic syndromes and reduce the risk of acute myelogenous leukemia.
- Suppress your immune system. These types of medications are used in certain myelodysplastic syndromes, and might lessen the need for red blood cell transfusions.
- Help people with a certain genetic abnormality. If your myelodysplastic syndrome is associated with a gene mutation called isolated del(5q), your doctor might recommend lenalidomide (Revlimid).
- Treat infections. If your condition causes you to have infections, you’ll be treated with antibiotics.
Bone marrow transplant
During a bone marrow transplant, also known as a stem cell transplant, high doses of chemotherapy drugs are used to clear out the defective blood cells from your bone marrow. Then the abnormal bone marrow stem cells are replaced with healthy, donated cells (allogeneic transplant).
There are 2 main types of stem cell transplant:
- For an allogeneic stem cell transplant, after the bone marrow is destroyed, the patient receives blood-forming stem cells from another person — the donor. This is the type of transplant typically used for myelodysplastic syndrome. The results of this treatment tend to be best when when the donor’s cell type (also known as the HLA type) is closely matched to the patient’s cell type and the donor is closely related to the patient, such as a brother or sister. Less often, the donor is matched to the patient, but is not related.
- In an autologous stem cell transplant, the patient gets back their own stem cells (which were removed before treatment). This type of transplant is not typically used for patients with myelodysplastic syndrome because the patient’s bone marrow contains abnormal stem cells.
Allogeneic stem cell transplants can have serious, even life-threatening, side effects, so they are typically done in younger patients who are in relatively good health. Patients in their 60s or even 70s have been transplanted successfully, but in older patients the stem cell transplant is generally done using less intensive (reduced intensity) chemotherapy and/or radiation. The lower doses may not kill all the bone marrow cells, but they are just enough to allow the donor cells to take hold and grow in the bone marrow. The lower doses also cause fewer side effects, which makes this type of transplant easier for older patients to tolerate. Still, some serious side effects are still possible.
Side effects of a stem cell transplant
The early side effects from a stem cell transplant are similar to the side effects expected from chemotherapy and radiation, only more severe. One of the most serious side effects is low blood counts, which can lead to risks of serious infections and bleeding.
Another possible serious side effect from allogeneic transplants is graft-versus-host disease (GVHD). This occurs when the new immune cells (from the donor) see the patient’s tissues as foreign and attack them. GVHD can affect any part of the body and can be life threatening.
Although allogeneic stem cell transplant is currently the only treatment that can cure some people with myelodysplastic syndrome, not everyone who gets a transplant is cured. In addition, some people may die from complications of this treatment. Your chance for cure is higher if you are young and your myelodysplastic syndrome hasn’t begun to transform into leukemia. Still, doctors often recommend waiting until the myelodysplastic syndrome develops into a more advanced stage before considering a stem cell transplant.
Newer techniques use less-toxic chemotherapy before the transplant than did older ones. However, bone marrow transplants carry a significant risk of side effects. For this reason, few people with myelodysplastic syndromes are candidates for bone marrow stem cell transplant.
Chemotherapy
Chemotherapy (chemo) is the use of drugs for treating a disease such as cancer. Some chemo drugs can be swallowed as pills, while others are injected by needle into a vein or muscle. These drugs are considered systemic treatment because they enter the bloodstream and reach most areas of the body. This type of treatment is useful for diseases such as myelodysplastic syndrome (myelodysplastic syndrome) that are not only in one part of the body. The purpose of the chemo is to kill the abnormal stem cells and allow normal ones to grow back.
Hypomethylating agents
These types of chemo drugs affect the way certain genes inside a cell are controlled. These drugs activate some genes that help cell mature. They also kill cells that are dividing rapidly. Examples of this type of drug include:
- Azacitidine (Vidaza)
- Decitabine (Dacogen)
In some myelodysplastic syndrome patients, using one of these drugs can often improve blood counts (sometimes enough so that blood transfusions aren’t needed), improve quality of life, lower the chance of getting leukemia, and even help a person live longer.
Azacitidine can be injected under the skin or into a vein (IV), often for 7 days in a row each month. Decitabine is often injected into a vein (IV) over 3 hours every 8 hours for 3 days. This is repeated every 6 weeks. Decitabine can also be given by IV over an hour, each day for 5 days in a row, and repeated every 4 weeks.
These drugs can have some of the same side effects as standard chemo drugs (see below), but these side effects are usually milder. A major side effect of these drugs is usually an early drop in blood cell counts, which tends to get better as the drug begins to work. Other side effects can include:
- Fever
- Nausea/vomiting
- Diarrhea or constipation
- Fatigue and weakness
Standard chemotherapy drugs
Standard chemo drugs are less useful for myelodysplastic syndrome than the hypomethylating agents, so they are not used often. But higher-risk myelodysplastic syndrome is more likely to progress to acute myeloid leukemia (AML), so some patients with these types of myelodysplastic syndrome may receive the same chemotherapy treatment as AML patients.
The chemo drug most often used for myelodysplastic syndrome is called cytarabine (ara-C). It can be given by itself at a low-dose, which can often help control the disease, but doesn’t often put it into remission.
Another option is to give the same, intense type of chemo that is used for younger patients with AML. This means giving cytarabine at a higher dose along with other chemo drugs. This is more often used in younger, healthier patients with higher-risk forms of myelodysplastic syndrome (like myelodysplastic syndrome with excess blasts). Some of the chemo drugs that can be combined with cytarabine are:
- Idarubicin
- Daunorubicin
Other chemo drugs might be used as well.
Patients who get the higher dose treatment are more likely to go into remission, but they can also have more severe, even life-threatening side effects, so this treatment is typically given in the hostpital. Still, this treatment may be an option for some patients with advanced myelodysplastic syndrome.
Chemo drugs can cause many side effects. These depend on the type and dose of the drugs that are given and how long they are taken. Common side effects include:
- Hair loss
- Mouth sores
- Loss of appetite
- Nausea and vomiting
- Low blood counts
Myelodysplastic syndrome patients already have low blood counts, which often become even worse for a time before they get better.
- Low white blood cell counts lead to an increased risk of serious infections.
- Low platelet counts can lead to problems with easy bruising and can have serious bleeding, including bleeding into the brain or the intestine.
- Low red blood cell counts (or anemia) can lead to fatigue and shortness of breath. In people with heart problems, severe anemia can lead to a heart attack.
If a patient’s blood cell counts become too low, they may need supportive therapy (including transfusions) or growth factors to help prevent or treat serious side effects.
Most side effects from chemo will go away after treatment is finished. Your health care team can often suggest ways to lessen side effects. For example, drugs can be given to help prevent or reduce nausea and vomiting.
Chemo drugs can also affect other organs. For example:
- Idarubicin and daunorubicin can damage the heart, so they are often not given to patients who already have heart problems.
- Cytarabine can affect the brain and cause balance problems, sleepiness, and confusion. This is more common with higher doses.
If serious side effects occur, the chemo treatments may have to be reduced or stopped, at least temporarily. It’s important to carefully monitor and adjust drug doses, because some of these side effects can be permanent.
Immune treatments
Immunomodulating drugs
Lenalidomide (Revlimid) belongs to a class of drugs known as immunomodulating drugs (IMiDs). It seems to work well in low-grade myelodysplastic syndrome, often eliminating the need for blood transfusions, at least for a time. The drug seems to work best in people whose myelodysplastic syndrome cells are missing a part of chromosome 5 (myelodysplastic syndrome-del(5q)). But it can also help some myelodysplastic syndrome patients that do not have this abnormal chromosome.
Side effects can include:
- Lowered blood counts (most often the white cell count and platelet count)
- Diarrhea or constipation
- Fatigue and weakness
This drug can also increase the risk of serious blood clots that start in the veins in the legs (called a deep vein thrombosis, or DVT). Sometimes, part of a DVT can break off and travel to the lungs (called a pulmonary embolus or PE), where it can cause breathing problems or even death.
This drug might also cause serious birth defects if given to pregnant women. Because of this, it’s only available through a special program by the drug company.
Immune system suppression
Drugs that suppress the immune system can help some patients with lower-risk myelodysplastic syndrome. These drugs are most helpful for people with low numbers of cells in the bone marrow (called hypocellular bone marrow).
Anti-thymocyte globulin (ATG) is an antibody against a type of white blood cell called the T-lymphocyte, which helps control immune reactions. For some patients with myelodysplastic syndrome, T-lymphocytes interfere with normal blood cell production, so ATG can be helpful. ATG is given as an infusion through a vein. It must be given in the hospital because it can sometimes cause severe allergic reactions leading to low blood pressure and problems breathing.
Cyclosporine is another drug that can suppress the immune system. It can be used along with ATG to help some patients with myelodysplastic syndrome. Side effects of cyclosporine can include loss of appetite and kidney damage.
Home remedies
Because people with certain myelodysplastic syndromes have low white blood cell counts, they’re subject to recurrent, and often serious, infections.
To reduce your risk of infections:
- Wash your hands. Wash hands frequently and thoroughly with warm, soapy water, especially before eating or preparing food. Carry an alcohol-based hand sanitizer for times when water isn’t available.
- Take care with food. Thoroughly cook all meat and fish. Avoid fruits and vegetables you can’t peel, especially lettuce, and wash all produce you do use before peeling. To increase safety, you might want to avoid all raw foods.
- Avoid people who are ill. Try to avoid close contact with anyone who is sick, including family members and co-workers.