What is peripheral neuropathy
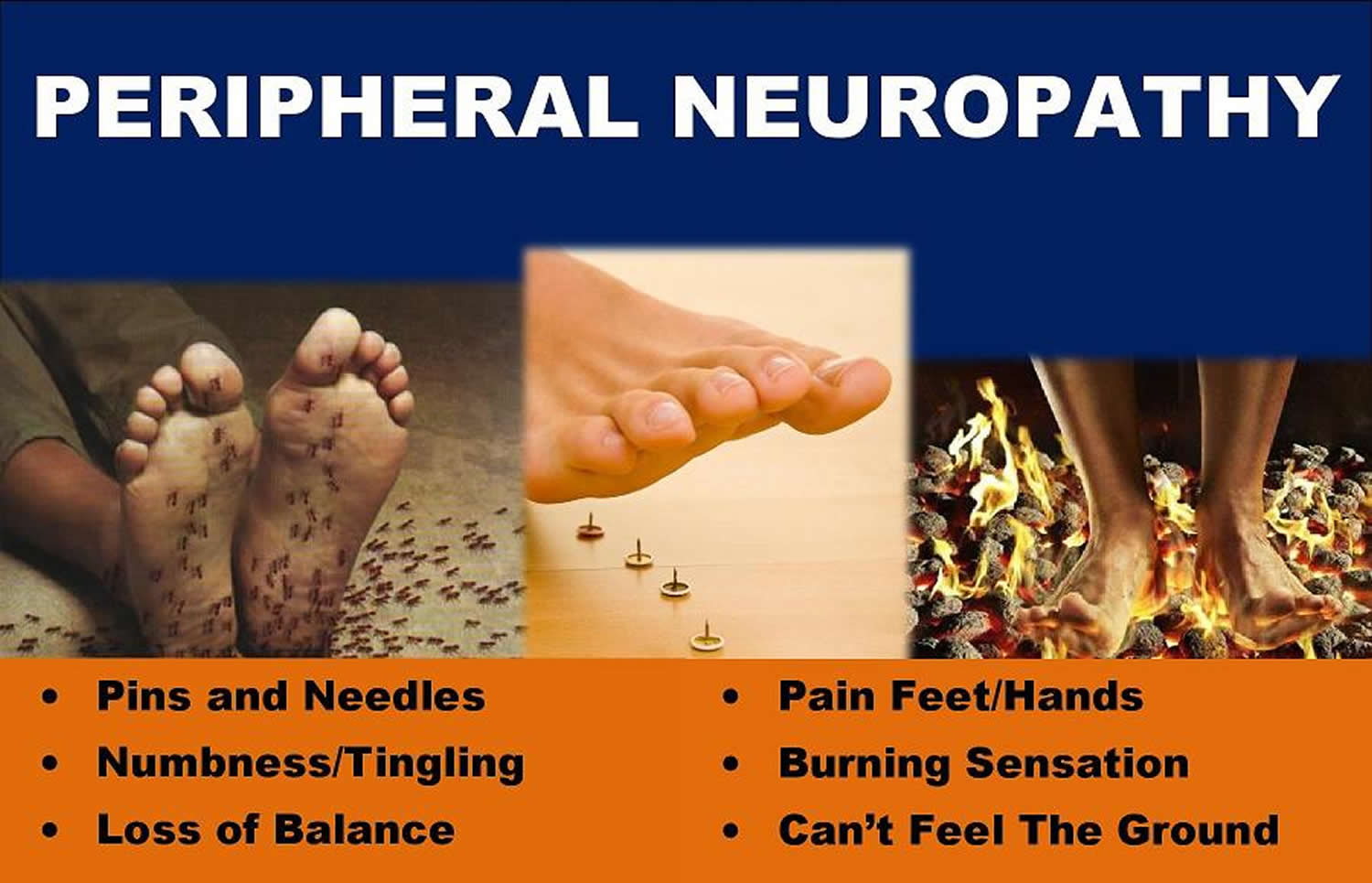
Peripheral neuropathy refers to a diverse group of disease affecting the motor, sensory and autonomic nerves lying outside the central nervous system. Peripheral neuropathy develops when nerves in the body’s extremities – such as the hands, feet and arms – are damaged. This can cause a wide variety of symptoms, such as weakness, numbness, pain or sensitivity to touch at peripheral sites, particularly the hands and feet. Peripheral neuropathy is caused by nerve damage which may result from diabetes (diabetic neuropathy), surgery, injuries, infections or other causes. Worldwide, leprosy is also an important cause.
Peripheral neuropathy is fairly common, but frequency varies with the cause of the condition.
Peripheral neuropathy may affect:
- only one nerve (mononeuropathy)
- several nerves (mononeuritis multiplex)
- all the nerves in the body (polyneuropathy)
Polyneuropathy is the most common type and starts by affecting the longest nerves first, so symptoms typically begin in the feet. Over time it gradually starts to affect shorter nerves so feels as if it’s spreading upwards, later affecting the hands.
In United States, both type 1 and type 2 diabetes is the most common cause of peripheral neuropathy. Up to one half of patients with diabetes mellitus have a neuropathy depending on the criteria used for diagnosis. Over time, the high blood sugar levels associated with diabetes can damage the nerves. This type of nerve damage is known as diabetic polyneuropathy. It is the most common acute polyneuropathy.
Peripheral neuropathy can also have a wide range of other causes. For example, it can be caused by:
- physical injury to the nerves
- a viral infection such as shingles
- a side effect of certain medications or drinking too much alcohol
People who are known to be at an increased risk of peripheral neuropathy may have regular check-ups so their nerve function can be assessed.
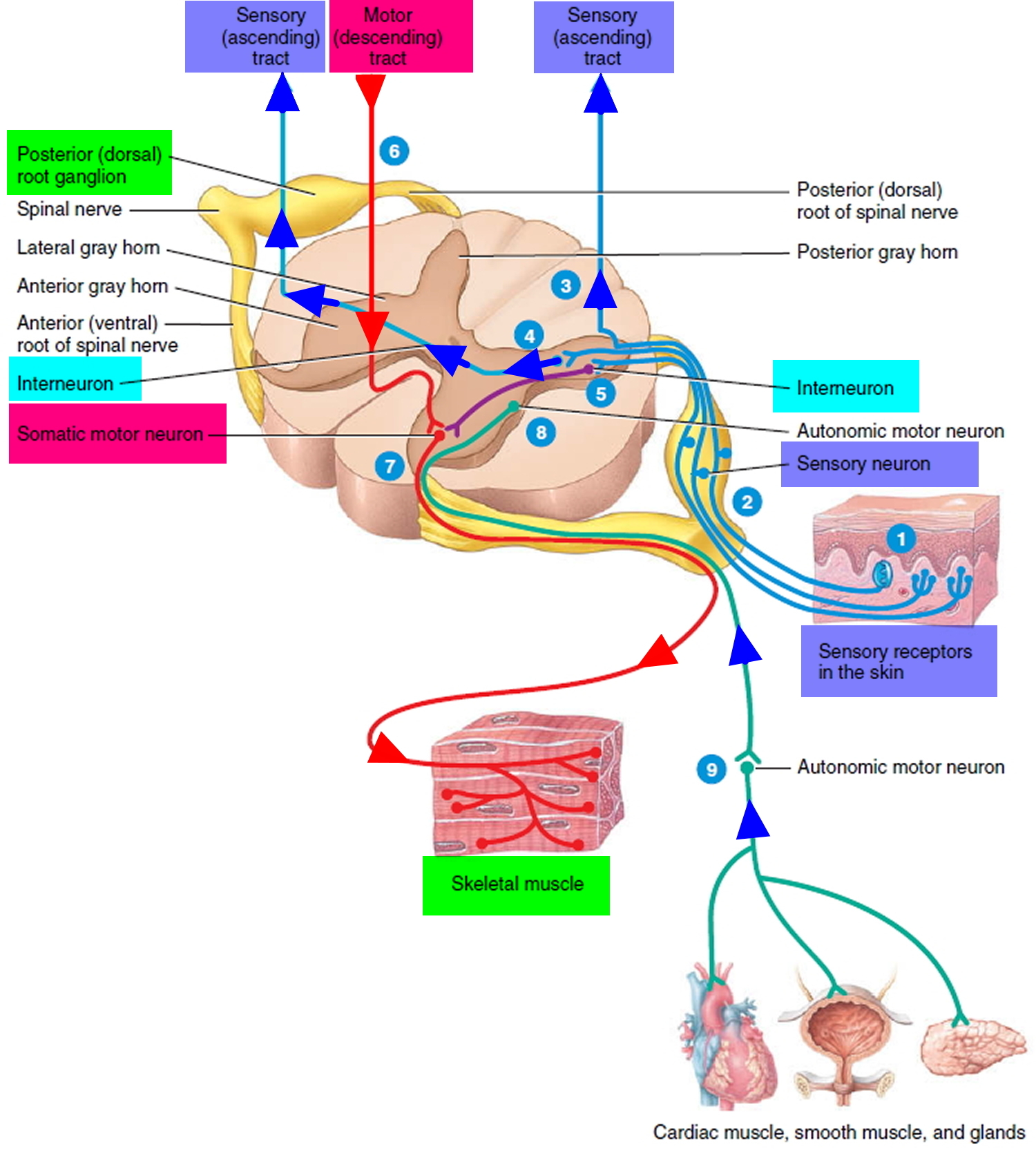
The peripheral nerves make up a vast network that transmit information from/to the brain and spinal cord (the central nervous system) to/from every other part of the body (see Figures 1 and 2). Information for movement is conveyed from the central nervous system via the nerves (motor pathways) and information regarding sensation from the peripheries to the central nervous system (sensory pathways).
Every nerve in your peripheral system has a specific function, so symptoms depend on the type of nerves affected. Nerves are classified into:
- Sensory nerves that receive sensation, such as temperature, pain, vibration or touch, from the skin
- Motor nerves that control muscle movement
- Autonomic nerves that control functions such as blood pressure, heart rate, digestion and bladder
The main symptoms of peripheral neuropathy can include:
- Gradual onset of numbness, prickling or tingling in your feet or hands, which can spread upward into your legs and arms
- Sharp, jabbing, throbbing, freezing, burning pain or shooting pain in affected areas
- Extreme sensitivity to touch
- Loss of balance and lack of co-ordination and falling
- Muscle weakness or paralysis, especially in the feet if motor nerves are affected
If autonomic nerves are affected, signs and symptoms might include:
- Heat intolerance and altered sweating
- Bowel, bladder or digestive problems
- Changes in blood pressure, causing dizziness or lightheadedness
These symptoms are usually constant, but may come and go.
Seek medical care right away if you notice unusual tingling, weakness or pain in your hands or feet. Early diagnosis and treatment offer the best chance for controlling your symptoms and preventing further damage to your peripheral nerves.
Treatment for peripheral neuropathy depends on the symptoms and underlying cause. Only some of the underlying causes of neuropathy can be treated. For example, if you have diabetes it may help to gain better control of your blood sugar level, stop smoking and cut down on alcohol.
Nerve pain may be treated with prescribed medications called neuropathic pain agents, as standard painkillers are often ineffective.
If you have other symptoms associated with peripheral neuropathy, these may need to be treated individually. For example, treatment for muscle weakness may involve physiotherapy and the use of walking aids.
If the underlying cause of peripheral neuropathy isn’t treated, you may be at risk of developing potentially serious complications, such as a foot ulcer that becomes infected. This can lead to gangrene (tissue death) if untreated, and in severe cases may mean the affected foot has to be amputated.
Peripheral neuropathy may affect the nerves controlling the automatic functions of the heart and circulation system (cardiovascular autonomic neuropathy). You may need treatment to increase your blood pressure or, in rare cases, a pacemaker.
The nervous system
The nervous system has two major anatomical subdivisions:
- The central nervous system (CNS) consists of the brain and spinal cord, which are enclosed and protected by the cranium and vertebral column. The central nervous system is discussed further in the other posts: Human brain and Spinal cord.
- The peripheral nervous system (PNS) consists of all the rest; it is composed of nerves and ganglia. The peripheral nervous system is the network of nerves that lie outside the central nervous system (the brain and spinal cord). A nerve is a bundle of nerve fibers (axons) wrapped in fibrous connective tissue. Nerves emerge from the central nervous system (CNS) through foramina of the skull and vertebral column and carry signals to and from other organs of the body. A ganglion (plural, ganglia) is a knotlike swelling in a nerve where the cell bodies of peripheral neurons are concentrated.
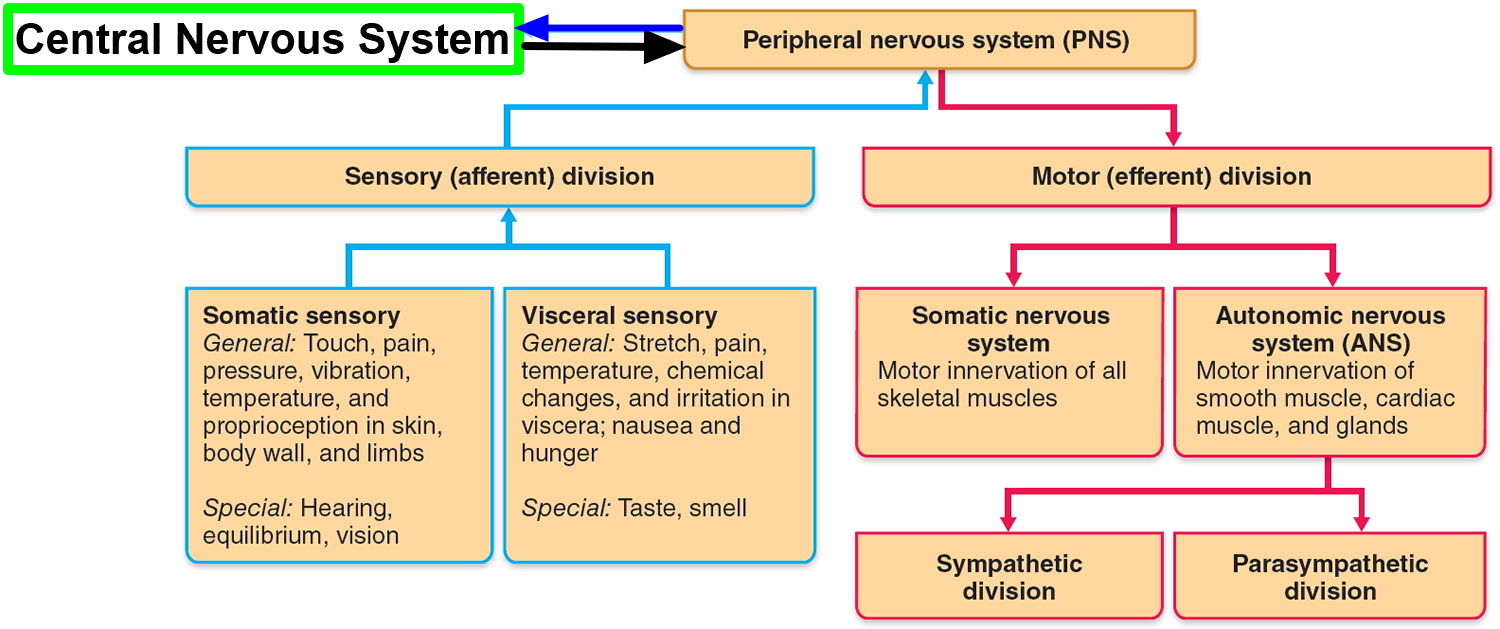
Figure 1. Nervous system and its parts
Peripheral nervous system
The peripheral nervous system includes different types of nerves with their own specific functions, including:
- sensory nerves – responsible for transmitting sensations, such as pain and touch
- motor nerves – responsible for controlling muscles
- autonomic nerves – responsible for regulating automatic functions of the body, such as blood pressure and bladder function
The peripheral nervous system is functionally divided into sensory and motor divisions, and each of these is further divided into somatic and visceral subdivisions.
The sensory (afferent) division carries signals from various receptors (sense organs and simple sensory nerve endings) to the central nervous system (CNS). This pathway informs the central nervous system (CNS) of stimuli within and around the body.
- The somatic sensory division carries signals from receptors in the skin, muscles, bones, and joints.
- The visceral sensory division carries signals mainly from the viscera of the thoracic and abdominal cavities, such as the heart, lungs, stomach, and urinary bladder.
The motor (efferent) division carries signals from the CNS (the brain and the spinal cord) mainly to gland and muscle cells that carry out the body’s responses. Cells and organs that respond to these signals are called effectors.
- The somatic motor division carries signals to the skeletal muscles. This produces voluntary muscle contractions as well as involuntary somatic reflexes.
- The visceral motor division (autonomic nervous system) carries signals to glands, cardiac muscle, and smooth muscle. We usually have no voluntary control over these effectors, and the autonomic nervous system operates at an unconscious level. The responses of the autonomic nervous system and its effectors are visceral reflexes. The autonomic nervous system has two further divisions:
- The sympathetic division tends to arouse the body for action—for example, by accelerating the heartbeat and increasing respiratory airflow—but it inhibits digestion.
- The parasympathetic division tends to have a calming effect—slowing the heartbeat, for example—but it stimulates digestion.
Figure 2. Functional classes of neurons
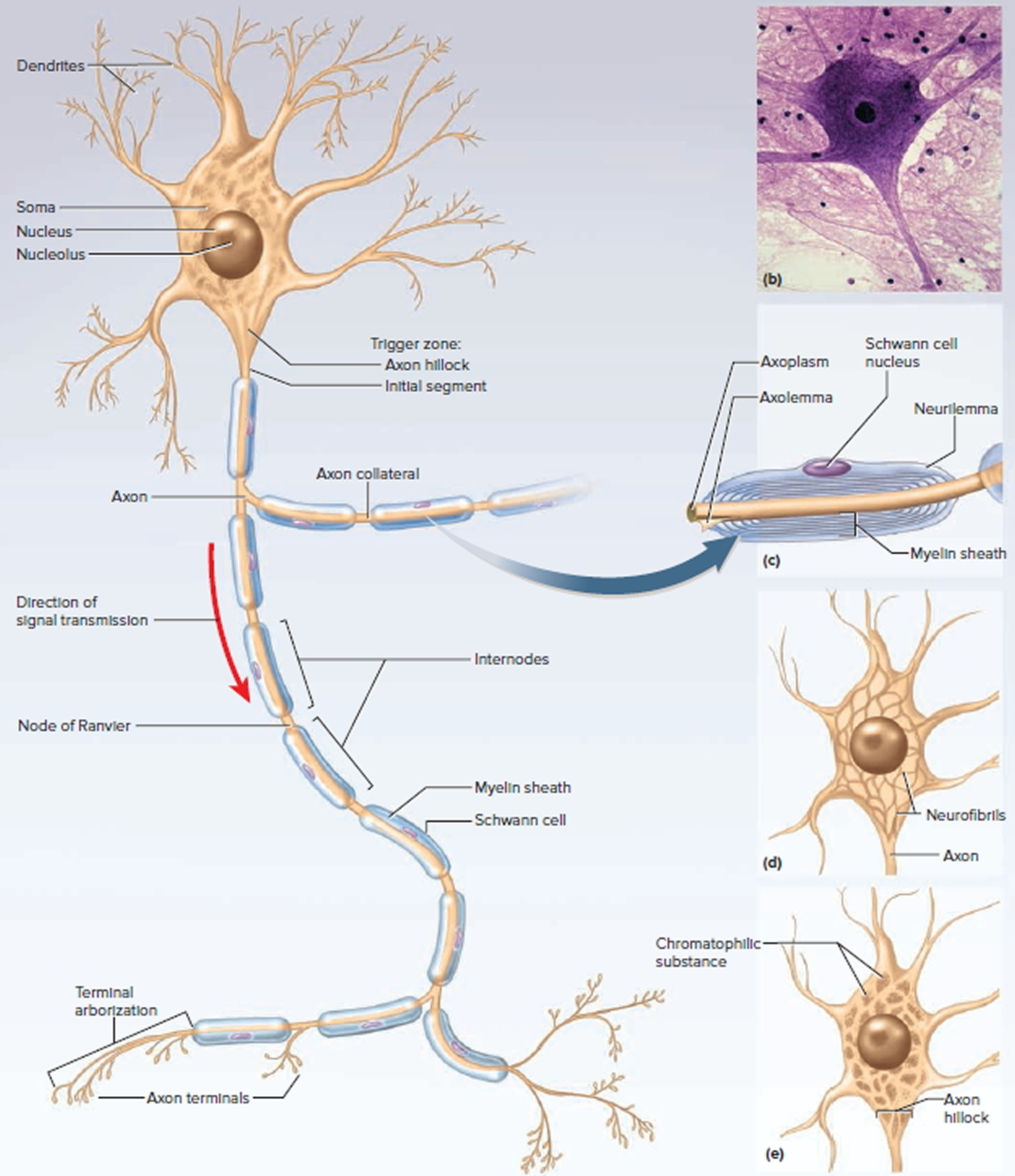
Figure 3. General structure of a neuron
Peripheral neuropathy prognosis
Recovery from peripheral neuropathy is usually slow. The course of the peripheral neuropathy will depend on the type of peripheral neuropathy, the type of nerves that have been damaged and on the underlying cause. Patient may fully recover without residual effects or may partially recover and have sensory, motor, and vasomotor (blood vessel) deficits. If severely affected, the damage may be permanent or may get gradually worse with time and the patient may develop chronic muscle wasting.
In acute neuropathies, such as Guillain-Barre syndrome where there is an immune attack on the nerves following an infection, symptoms appear suddenly, progress rapidly, and resolve slowly as damaged nerves heal.
In chronic forms, symptoms begin subtly and progress slowly. Some people may have periods of relief followed by relapse. Others may reach a plateau stage where symptoms stay the same for many months or years. Some chronic neuropathies worsen over time, but very few forms prove fatal unless complicated by other diseases. Occasionally the neuropathy is a symptom of another disorder.
Recovery from peripheral neuropathy is usually slow. Depending on the type of peripheral neuropathy, the patient may fully recover without residual effects or may partially recover and have sensory, motor, and vasomotor (blood vessel) deficits. If severely affected, the patient may develop chronic muscular wasting.
How bad can peripheral neuropathy get?
Peripheral neuropathy can sometimes cause other medical problems, such as foot ulcers and heart rhythm changes, and blood circulation problems.
These complications vary depending on the underlying cause of the condition.
Diabetic foot ulcer
A diabetic foot ulcer is an open wound or sore on the skin that’s slow to heal. These are common in people with diabetic polyneuropathy.
If you have numb feet, it’s easy to cut your foot by stepping on something sharp.
An ulcer can also occur if you unknowingly develop a blister caused by badly fitting shoes. If you don’t feel any pain, you may continue walking without protecting the blister. If the cut or blister gets worse, it may develop into an ulcer.
High blood sugar can damage your blood vessels, causing the blood supply to your feet to become restricted. A reduced blood supply to the skin on your feet means it receives a lower number of infection-fighting cells, which can mean wounds take longer to heal and can lead to gangrene.
Gangrene
If you do develop a wound infection in one of your feet as a result of peripheral neuropathy, there’s a risk this could lead to gangrene (death of part of the skin or underlying tissues).
If gangrene does develop, you may need surgery to remove the damaged tissue (known as debridement) and antibiotics to treat any underlying infection. In severe cases your toe or foot may need to be amputated.
If you have diabetes, you should take extra care of your feet. Get your feet checked regularly by a podiatrist (a medical professional, also known as a chiropodist, who specializes in foot care).
Cardiovascular autonomic neuropathy
Cardiovascular autonomic neuropathy is another potentially serious problem that’s common in people with diabetic polyneuropathy.
Cardiovascular autonomic neuropathy occurs when damage to the peripheral nerves disrupts the automatic functions that control your blood circulation and heartbeat.
The two main noticeable symptoms of cardiovascular autonomic neuropathy are:
- an inability to exercise for more than a very short period of time
- orthostatic hypotension – a type of low blood pressure that can make you feel dizzy or faint when you stand up
Treating cardiovascular autonomic neuropathy
You may be able to control the symptoms of orthostatic hypotension by using a number of self care techniques, such as:
- standing or sitting up slowly and gradually
- drinking plenty of fluids to increase the volume of your blood and raise your blood pressure
- wearing compression stockings to help prevent blood falling back down into your legs
- tilting your bed by raising it at the head end
In some cases, medication may be required to treat orthostatic hypotension.
Two widely used medications are:
- fludrocortisone – which works by increasing the volume of your blood
- midodrine – which works by tightening your blood vessels
A more serious concern with cardiovascular autonomic neuropathy is that your heart may suddenly develop an abnormal pattern of beating (arrhythmia), which could lead to a cardiac arrest, where your heart stops beating altogether.
To prevent this, you may be prescribed medication to help regulate the beating of your heart, such as flecainide, beta-blockers or amiodarone.
If you have cardiovascular autonomic neuropathy, you’ll probably need to have regular check-ups so your heart function can be monitored.
Peripheral neuropathy complications
Complications of peripheral neuropathy can include:
- Burns and skin trauma. You might not feel temperature changes or pain on parts of your body that are numb.
- Infection. Your feet and other areas lacking sensation can become injured without your knowing. Check these areas regularly and treat minor injuries before they become infected, especially if you have diabetes mellitus.
- Falls. Weakness and loss of sensation may be associated with lack of balance and falling.
Peripheral neuropathy causes
What causes peripheral neuropathy
Diabetes is the most common cause of peripheral neuropathy in the US.
Peripheral neuropathy can also be caused by other health conditions and certain medications. In some cases, no cause can be identified and this is termed idiopathic peripheral neuropathy.
Diabetes
Peripheral neuropathy caused by either type 1 diabetes or type 2 diabetes is called diabetic polyneuropathy. It’s probably caused by high levels of glucose in your blood damaging the tiny blood vessels that supply your nerves.
Peripheral neuropathy becomes more likely the longer you’ve had diabetes. Up to one in every four people with the condition experience some pain caused by nerve damage.
If you have diabetes, your risk of polyneuropathy is higher if your blood sugar is poorly controlled or you:
- smoke
- regularly consume large amounts of alcohol
- are over 40 years old
If you have diabetes, you should examine your own feet regularly to check for ulcers (open wounds or sores) or chilblains.
Other causes
As well as diabetes, there are many other possible causes of peripheral neuropathy.
Health conditions
Some of the health conditions that can cause peripheral neuropathy include:
- Excessive alcohol drinking for years
- Low levels of vitamin B12 or other vitamins including B-1 (Thiamin), B-6 (Pyridoxine), B-3 (Niacin) and vitamin E are crucial to nerve health.
- Physical damage to the nerves – such as from an injury or during surgery. Traumas, such as from motor vehicle accidents, falls or sports injuries, can sever or damage peripheral nerves. Nerve pressure can result from having a cast or using crutches or repeating a motion such as typing many times.
- An underactive thyroid gland (hypothyroidism)
- Certain infections – such as shingles, Lyme disease, diphtheria, botulism, Epstein-Barr virus, hepatitis C, leprosy, diphtheria and HIV
- Inflammation of the blood vessels (vasculitis)
- Chronic liver disease or chronic kidney disease
- Monoclonal gammopathy of undetermined significance – the presence of an abnormal protein in the blood
- Certain types of cancer, such as lymphoma (a cancer of the lymphatic system) and multiple myeloma (a type of bone marrow cancer). Growths, cancerous (malignant) and noncancerous (benign), can develop on the nerves or press nerves. Also, polyneuropathy can arise as a result of some cancers related to the body’s immune response. These are a form of paraneoplastic syndrome.
- Charcot-Marie-Tooth disease and other types of hereditary motor sensory neuropathy – genetic conditions that cause nerve damage, particularly in the feet
- Having high levels of toxins in your body, such as arsenic, lead or mercury
- Guillain-Barré syndrome – a rare condition that causes rapid onset of paralysis within days
- Amyloidosis – a group of rare but serious conditions caused by deposits of abnormal protein called amyloid in tissues and organs throughout the body
- Conditions caused by overactivity of the immune system – such as rheumatoid arthritis, lupus, chronic inflammatory demyelinating polyneuropathy, necrotizing vasculitis or Sjogren’s syndrome
Medication
A few medications may sometimes cause peripheral neuropathy as a side effect in some people. These include:
- some types of chemotherapy for cancer – especially for bowel cancer, lymphoma or myeloma
- some antibiotics, if taken for months – such as metronidazole or nitrofurantoin
- phenytoin – used to treat epilepsy – if taken for a long time
- amiodarone and thalidomide
Risk Factors for peripheral neuropathies
Peripheral neuropathy may be either inherited or acquired.
Peripheral neuropathy risk factors include:
- Diabetes mellitus, especially if your sugar levels are poorly controlled
- Alcohol
- Nutritional deficiencies (vitamin B1, B3, B6, B12 and vitamin E)
- Toxins (carbon disulfide, acrylamide)
- Endocrine causes (diabetes, thyroid disease)
- Metabolic causes (renal failure)
- Liver or thyroid disorders
- Infections (HIV, Lyme disease, Leprosy, Epstein-Barr virus, hepatitis C and shingles)
- Connective tissue disease (scleroderma, SLE, sarcoidosis)
- Immune disorders (Guillain-Barre syndrome, chronic inflammatory demyelinating neuropathy)
- Cancer
- Medications/Drugs
- Repetitive motion, such as those performed for certain jobs
- Family history of neuropathy
- Inherited conditions (Charcot-Marie-Tooth disease)
Peripheral neuropathy prevention
Manage underlying conditions
The best way to prevent peripheral neuropathy is to manage medical conditions that put you at risk, such as diabetes, alcoholism or rheumatoid arthritis.
Make healthy lifestyle choices
- Eat a diet rich in fruits, vegetables, whole grains and lean protein to keep nerves healthy. Protect against vitamin B-12 deficiency by eating meats, fish, eggs, low-fat dairy foods and fortified cereals. If you’re vegetarian or vegan, fortified cereals are a good source of vitamin B-12, but talk to your doctor about B-12 supplements.
- Exercise regularly. With your doctor’s okay, try to get at least 30 minutes to one hour of exercise at least three times a week.
- Avoid factors that may cause nerve damage, including repetitive motions, cramped positions, exposure to toxic chemicals, smoking and overindulging in alcohol.
Peripheral neuropathy symptoms
Symptoms vary according to the type of peripheral neuropathy and may develop quickly or slowly.
The main types of peripheral neuropathy include:
- sensory neuropathy – damage to the nerves that carry messages of touch, temperature, pain and other sensations to the brain
- motor neuropathy – damage to the nerves that control movement
- autonomic neuropathy – damage to the nerves that control involuntary bodily processes, such as digestion, bladder function and control of blood pressure
- mononeuropathy – damage to a single nerve outside of the central nervous system
In many cases, someone with peripheral neuropathy may have more than one of these types at the same time.
A combination of sensory and motor neuropathy is particularly common (sensorimotor polyneuropathy).
The symptoms of the main types of peripheral neuropathy are now described.
Sensory peripheral neuropathy
Symptoms of sensory neuropathy can include:
- prickling and tingling sensation in the affected body part (pins and needles)
- numbness and less of an ability to feel pain or changes in temperature, particularly in your feet
- a burning or sharp pain, usually in the feet
- feeling pain from something that should not be painful at all, such as a very light touch (allodynia)
- loss of balance or co-ordination caused by less ability to tell the position of the feet or hands (sensory ataxia)
Motor peripheral neuropathy
Symptoms of motor neuropathy can include:
- twitching and muscle cramps
- muscle weakness or paralysis affecting one or more muscles
- thinning (wasting) of muscles
- foot drop – difficulty lifting up the front part of your foot and toes, particularly noticeable when walking
Autonomic peripheral neuropathy
Damage to the autonomic nerves can result in a wide range of symptoms depending on where in the body the damage occurs.
Symptoms of autonomic neuropathy can include:
- constipation or diarrhea, particularly at night
- feeling sick, bloating and belching
- low blood pressure (postural or orthostatic hypotension), which can make you feel faint or dizzy when standing up
- rapid heartbeat (tachycardia)
- heat intolerance and excessive sweating or a lack of sweating
- problems with sexual function, such as erectile dysfunction in men
- difficulty fully emptying your bladder of urine
- bowel incontinence (loss of bowel control)
Peripheral mononeuropathy
Depending on the specific nerve affected, symptoms of mononeuropathy can include:
- altered sensation or weakness in the fingers
- double vision or other problems with focusing your eyes, sometimes with eye pain
- weakness of one side of your face (Bell’s palsy)
- foot or shin pain, weakness or altered sensation
The most common type of peripheral mononeuropathy is carpal tunnel syndrome. The carpal tunnel is a small tunnel in your wrist.
In carpal tunnel syndrome, the median nerve becomes compressed where it passes through this tunnel, which may cause tingling, pain or numbness in the fingers.
Peripheral neuropathy diagnosis
A number of tests may be used to diagnose peripheral neuropathy and its underlying cause.
When you see your doctor, they’ll ask about your symptoms and examine the affected area of your body. This may involve testing sensation, strength and reflexes.
Your doctor may also arrange blood tests, especially to check for causes such as diabetes or vitamin B12 deficiency.
Confirming if you have a peripheral neuropathy
Some people may need to see a neurologist (a specialist in conditions affecting the nervous system) in hospital for further tests such as:
- a nerve conduction test – where small metal wires called electrodes are placed on your skin which release tiny electric shocks that stimulate your nerves; the speed and strength of the nerve signal is measured
- electromyography (EMG) – where a small needle is inserted through your skin into your muscle and used to measure the electrical activity of your muscles
Nerve conduction test and electromyography are usually carried out at the same time.
Identifying the cause of a neuropathy
Your doctor can usually identify the underlying cause of a peripheral neuropathy.
If diabetes is suspected, your doctor can usually make a confident diagnosis based on your symptoms, a physical examination and checking the levels of glucose in your blood and urine.
If you’re taking a medication known to cause peripheral neuropathy, your doctor may temporarily stop or reduce your dose to see whether your symptoms improve.
If the cause is uncertain, you may be referred to a neurologist for more extensive blood tests to check:
- whether you have a rare acquired cause that may be responsible
- whether you have a genetic abnormality, such as Charcot-Marie-Tooth disease
You may need a lumbar puncture to test the cerebrospinal fluid (a clear, colorless fluid that surrounds and supports the brain and spinal cord) for inflammation.
Further tests
Occasionally, a nerve biopsy may be carried out as part of your diagnosis. This is a minor surgical procedure where a small sample of a peripheral nerve is removed from near your ankle so it can be examined under a microscope.
It’s then checked for changes that could be a sign of certain types of peripheral neuropathy. However, nerve biopsies are rarely needed.
You may also need a scan and blood tests to look for any underlying cause of your peripheral neuropathy, such as:
- Chest x-ray
- Computerised tomography (CT) scan
- Magnetic resonance imaging (MRI) scan
- Genetic testing is available for the evaluation of specific types of hereditary sensorimotor neuropathies.
- Blood tests measuring haemoglobin, inflammatory markers, vitamin levels, blood sugar and thyroid function, infection markers and antibody levels
Urinalysis
Peripheral neuropathy treatment
Any underlying condition is treated first, followed by symptomatic treatment. Symptoms often can be controlled, and eliminating the causes of specific forms of peripheral neuropathy often can prevent new damage. Systemic diseases frequently require more complex treatments.
In general, adopting healthy habits, such as maintaining optimal weight, avoiding exposure to toxins, following a physiotherapist supervised exercise program, eating a balanced diet, correcting vitamin deficiencies, and limiting or avoiding alcohol consumption can reduce the physical and emotional effects of peripheral neuropathy.
Quitting smoking is particularly important because smoking constricts the blood vessels that supply nutrients to the peripheral nerves and can worsen neuropathic symptoms.
Treatment may be more successful for certain underlying causes. For example, ensuring diabetes is well controlled may help improve neuropathy or at least stop it getting worse. Strict control of blood glucose levels has been shown to reduce neuropathic symptoms and help people with diabetic neuropathy avoid further nerve damage. Inflammatory and autoimmune conditions leading to neuropathy can be controlled with steroids or immunosupressive medications.
If you have neuropathies caused by pressure on nerves, such as pressure from tumors, you might need surgery to reduce the pressure.
Treating the underlying cause
There are many different possible causes of peripheral neuropathy, some of which can be treated in different ways. For example:
- diabetes can sometimes be controlled by lifestyle changes, such as stopping smoking, cutting down on alcohol, maintaining a healthy weight and exercising regularly
- vitamin B12 deficiency can be treated with B12 injections or tablets
- peripheral neuropathy caused by a medication you’re taking may improve if the medication is stopped
Some less common types of peripheral neuropathy may be treated with medication, such as:
- Corticosteroids – powerful anti-inflammatory medication
- Immunosuppressants – medications that reduce the activity of the immune system
- Plasma exchange and intravenous immune globulin. These procedures, which help suppress immune system activity, might benefit people with certain inflammatory conditions. Plasma exchange involves removing your blood, then removing antibodies and other proteins from the blood and returning the blood to your body. In immune globulin therapy, you receive high levels of proteins that work as antibodies (immunoglobulins).
However, the underlying cause may not always be treatable.
Relieving nerve pain
You may also require medication to treat any nerve pain (neuropathic pain) you’re experiencing.
Unlike most other types of pain, neuropathic pain doesn’t usually get better with common painkillers, such as paracetamol and ibuprofen.
For more-severe symptoms, your doctor might prescribe painkillers. Medications containing opioids, such as tramadol (Conzip, Ultram) or oxycodone (Oxycontin, Roxicodone, others), can lead to dependence and addiction, so these drugs generally are prescribed only when other treatments fail.
These should usually be started at the minimum dose, with the dose gradually increased until you notice an effect, because the ideal dose for each person is unpredictable. Higher doses may be better at managing the pain, but are also more likely to cause side effects.
The most common side effects are tiredness, dizziness or feeling “drunk”. If you get these, it may be necessary to reduce your dose. Don’t drive or operate machinery if you experience drowsiness or blurred vision. You also may become more sensitive to the effects of alcohol.
The side effects should improve after a week or two as your body gets used to the medication. However, if your side effects continue, tell your GP as it may be possible to change to a different medication that suits you better.
Even if the first medication tried doesn’t help, others may.
Peripheral neuropathy medications
Many of these medications may also be used for treating other conditions, such as depression, epilepsy, anxiety or headaches. If you’re given an antidepressant, this may treat pain even if you’re not depressed. This doesn’t mean your doctor suspects you’re depressed.
Medications used to relieve peripheral neuropathy pain include:
- Duloxetine – also used for treatment of bladder problems and depression
- Pregabalin and gabapentin – also used to treat epilepsy, headaches or anxiety. Side effects can include drowsiness and dizziness.
- Antidepressants. Certain tricyclic antidepressants, such as amitriptyline, doxepin and nortriptyline (Pamelor), have been found to help relieve pain by interfering with chemical processes in your brain and spinal cord that cause you to feel pain. Amitriptyline – also used for treatment of headaches and depression. The serotonin and norepinephrine reuptake inhibitor duloxetine (Cymbalta) and the extended-release antidepressant venlafaxine (Effexor XR) also might ease the pain of peripheral neuropathy caused by diabetes. Side effects may include dry mouth, nausea, drowsiness, dizziness, decreased appetite and constipation.
There are also some additional medications that can be used to relieve pain in a specific area of the body or to relieve particularly severe pain for short periods. These are described below.
Capsaicin cream
If your pain is confined to a particular area of your body and you can’t, or would prefer not to, take the medications above, you may benefit from using capsaicin cream.
Capsaicin is the substance that makes chilli peppers hot and is thought to work in neuropathic pain by stopping the nerves sending pain messages to the brain.
A pea-sized amount of capsaicin cream is rubbed on the painful area of skin three or four times a day.
Side effects of capsaicin cream can include skin irritation and a burning sensation in the treated area when you first start treatment.
Don’t use capsaicin cream on broken or inflamed skin and always wash your hands after applying it.
Tramadol
Tramadol is a powerful painkiller related to morphine that can be used to treat neuropathic pain that doesn’t respond to other treatments your GP can prescribe.
Like all opioids, tramadol can be addictive if it’s taken for a long time. It will usually only be prescribed for a short time. Tramadol can be useful to take at times when your pain is worse.
Common side effects of tramadol include:
- feeling sick or vomiting
- dizziness
- constipation
Treating other symptoms
In addition to treating pain, you may also require treatment to help you manage other symptoms you’re experiencing as a result of peripheral neuropathy.
For example, if you have muscle weakness, you may need physiotherapy to learn exercises to improve your muscle strength. You may also need to wear splints to support weak ankles or use walking aids to help you get around.
Other problems associated with peripheral neuropathy may be treatable with medication, such as:
- erectile dysfunction
- constipation
- the slow movement of food through your stomach (gastroparesis)
In some cases, you may need more invasive treatment, such as botulinum toxin injections for hyperhidrosis or urinary catheterisation if you have problems emptying your bladder.
Peripheral neuropathy natural treatment
As peripheral neuropathy can be a very painful and troublesome condition that may only partly be relieved by medication, some people may be tempted to try other treatments, such as:
- Acupuncture. Inserting thin needles into various points on your body might reduce peripheral neuropathy symptoms. You might need multiple sessions before you notice improvement. Acupuncture is generally considered safe when performed by a certified practitioner using sterile needles.
- Transcutaneous electrical nerve stimulation (TENS). Electrodes placed on the skin deliver a gentle electric current at varying frequencies. TENS should be applied for 30 minutes daily for about a month.
- Herbal medicine. Certain herbs, such as evening primrose oil, might help reduce neuropathy pain in people with diabetes. Some herbs interact with medications, so discuss herbs you’re considering with your doctor.
- Physical therapy. If you have muscle weakness, physical therapy can help improve your movements. You may also need hand or foot braces, a cane, a walker, or a wheelchair.
- Benfotiamine (a form of vitamin B1) supplements
- Alpha-lipoic acid (an antioxidant) supplements. This has been used as a treatment for peripheral neuropathy in Europe for years. Discuss using alpha-lipoic acid with your doctor because it can affect blood sugar levels. Other side effects can include stomach upset and skin rash.
- Amino acids. Amino acids, such as acetyl-L-carnitine, might benefit people who have undergone chemotherapy and people with diabetes. Side effects might include nausea and vomiting.
However, while some people may find these helpful, the evidence for them isn’t always clear. It’s advisable to speak to your doctor before trying these treatments in case they could interfere with your ongoing treatment.
Home remedies
To help you manage peripheral neuropathy:
- Take care of your feet, especially if you have diabetes. Check daily for blisters, cuts or calluses. Wear soft, loose cotton socks and padded shoes. You can use a semicircular hoop, which is available in medical supply stores, to keep bedcovers off hot or sensitive feet.
- Exercise. Regular exercise, such as walking three times a week, can reduce neuropathy pain, improve muscle strength and help control blood sugar levels. Gentle routines such as yoga and tai chi might also help.
- Quit smoking. Cigarette smoking can affect circulation, increasing the risk of foot problems and other neuropathy complications.
- Eat healthy meals. Good nutrition is especially important to ensure that you get essential vitamins and minerals. Include fruits, vegetables, whole grains and lean protein in your diet.
- Avoid excessive alcohol. Alcohol can worsen peripheral neuropathy.
- Monitor your blood glucose levels. If you have diabetes, this will help keep your blood glucose under control and might help improve your neuropathy.