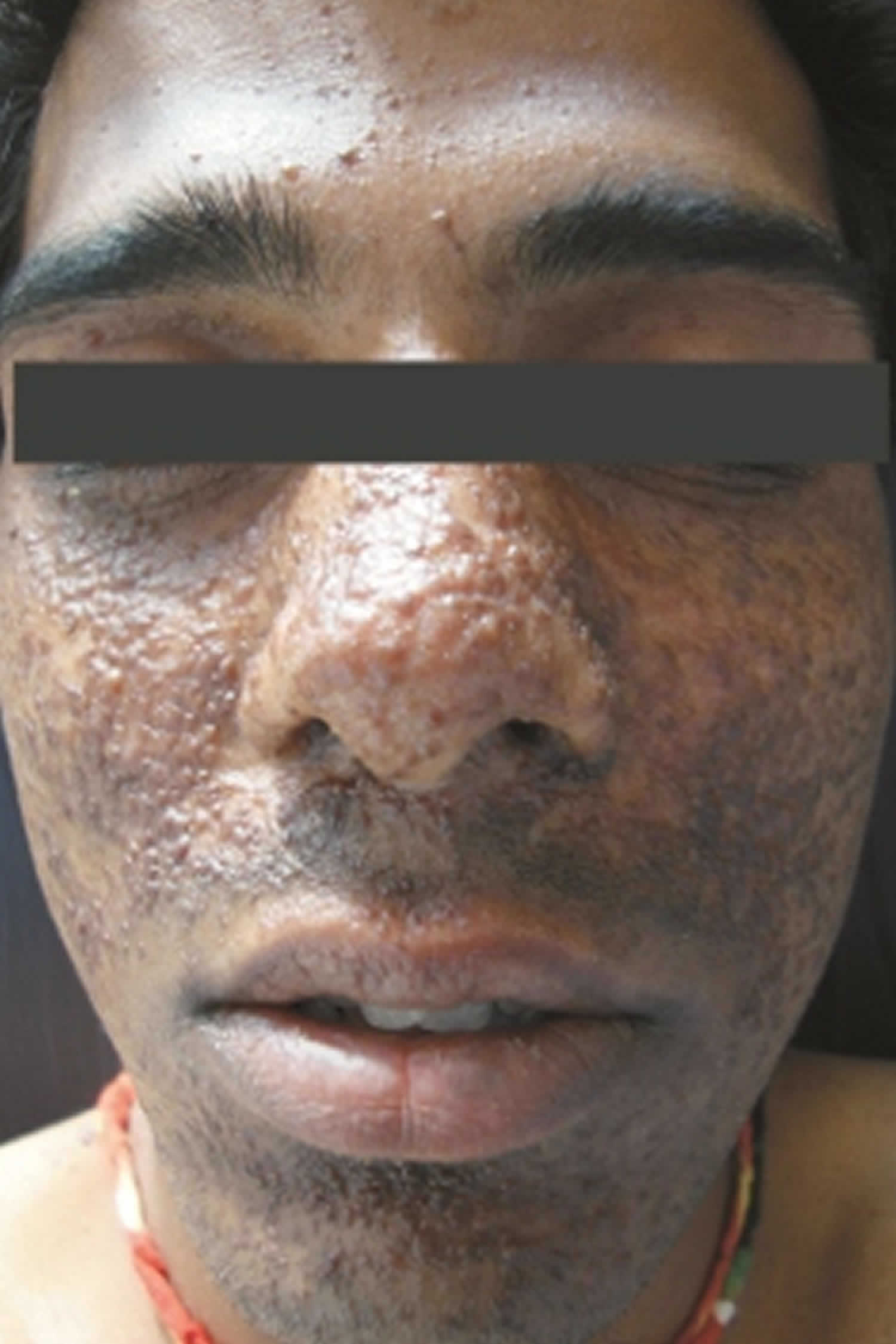
Adenoma sebaceum
Adenoma sebaceum also called facial angiofibromas, is facial rash that appears as a spread of small pink or red spots across the cheeks and nose in a butterfly distribution. Its presence is one of the major diagnostic criteria for establishing the diagnosis of tuberous sclerosis 1. Adenoma sebaceum are usually symmetrical and most commonly occur in the nasolabial folds 2. The upper lip is usually spared 2. Adenoma sebaceum or cutaneous angiofibromas are benign fibrous neoplasms comprised of a proliferation of stellate and spindled cells, thin-walled blood vessels with dilated lumina in the dermis, and concentric collagen bundles 3. Cutaneous angiofibromas can be located on different areas of the body including the face where they are commonly called adenoma sebaceum or fibrous papules. On the penis where angiofibromas are called pearly penile papules, underneath the nail where they are called periungual angiofibromas or Koenen tumors, and in the mouth where they are called oral fibromas 3. Pearly penile papules are chronic, asymptomatic, papules found on the coronal margin and sulcus of the penis. They are more common in uncircumcised men 4.
Adenoma sebaceum are solitary, dome-shaped, skin-colored to red papules located on the central face, usually around the nose and on the malar eminences. They can have tiny telangiectatic vessels located on the surface of the papule. In tuberous sclerosis, angiofibromas typically arise symmetrically on the cheeks, nasolabial folds, nose, and chin. They can start off as erythematous macules that form into the red to red-brown papules that can coalesce into plaques.
Facial angiofibromas are considered one of the most obvious clinical presentations of tuberous sclerosis or tuberous sclerosis complex (TSC). Multiple facial angiofibromas are also found in multiple endocrine neoplasia type 1 (MEN-1) and Birt-Hogg-Dube syndrome.
Adenoma sebaceum skin lesions are found in 60-70% of cases of tuberous sclerosis or tuberous sclerosis complex. Tuberous sclerosis or tuberous sclerosis complex (TSC) is a rare genetic disease that causes benign tumors (hamartomas) to grow in the brain and on other vital organs such as the kidneys, heart, eyes, lungs, and skin. Tuberous sclerosis usually affects the central nervous system (brain and spinal cord). In addition to the benign tumors that frequently occur in tuberous sclerosis complex, other common symptoms include seizures, impaired intellectual development, developmental delay, behavior problems, and skin abnormalities. However, individuals with the condition may be affected in many different ways and with differing degrees of severity. Some patients may have very few, or no symptoms at all, while others may be severely affected with a multitude of symptoms. Tuberous sclerosis may be present at birth, but signs of the disorder can be subtle and full symptoms may take some time to develop. Three types of brain tumors are associated with tuberous sclerosis: cortical tubers, which generally form on the surface of the brain; subependymal nodules, which form in the walls of the ventricles (the fluid-filled cavities of the brain); and giant-cell astrocytomas, a type of tumor that can block the flow of fluids within the brain.
With tuberous sclerosis, angiofibromas typically arise on the face in childhood and early adulthood. Both facial angiofibromas (greater than or equal to 3 needed) and periungual angiofibroma (greater than or equal to 2 needed) are 2 of the major criteria for tuberous sclerosis 3.
Adenoma sebaceum are benign and do not always require removal. Options for treatment of angiofibromas include:
- Excision
- Dermabrasion
- Using lasers, electrical, and radiofrequency devices
- Cryotherapy
- Topical podophyllotoxin
- Topical rapamycin
- Topical beta-blocker (eg, timolol) 5.
Multiple treatments are often necessary 3.
Figure 1. Adenoma sebaceum
Adenoma sebaceum causes
Adenoma sebaceum or cutaneous angiofibromas are caused by a local overgrowth of collagen, fibroblasts, and blood vessels.
- Tuberous sclerosis is caused by mutations in the genes tuberous sclerosis complex 1 (TSC 1) that encodes the protein hamartin and tuberous sclerosis complex 2 (TSC 2) that encodes the protein tuberin. These proteins normally suppress the activation of mammalian target of rapamycin (mTOR), however, when mutated, they cause unregulated proliferation of cell growth forming multi-organ hamartomas. mTOR is activated in the proliferating fibroblast-like cells within facial angiofibromas. The cells produce an epidermal growth factor called epiregulin, which stimulates epidermal cell proliferation so that they are produced at a faster rate. Angiofibromas of tuberous sclerosis also have vascular proliferation from increased expression of angiogenic factors such as vascular endothelial growth factor (VEGF). VEGF stimulates mTOR 6.
- Birt-Hogg-Dubé syndrome is caused by a mutation in the FLCN gene, which encodes the protein folliculin 7.
- Multiple endocrine neoplasia type 1 (MEN-1) results from a mutation in the MEN1 gene which produces the protein menin 3.
Genetic mosaicism for these genetic conditions must also be considered 8. What specifically triggers the development of angiofibroma is unknown.
People with specific questions about genetic risks or genetic testing for themselves or family members should speak with a genetics professional.
Resources for locating a genetics professional in your community are available online:
- The National Society of Genetic Counselors (https://www.findageneticcounselor.com/) offers a searchable directory of genetic counselors in the United States and Canada. You can search by location, name, area of practice/specialization, and/or ZIP Code.
- The American Board of Genetic Counseling (https://www.abgc.net/about-genetic-counseling/find-a-certified-counselor/) provides a searchable directory of certified genetic counselors worldwide. You can search by practice area, name, organization, or location.
- The Canadian Association of Genetic Counselors (https://www.cagc-accg.ca/index.php?page=225) has a searchable directory of genetic counselors in Canada. You can search by name, distance from an address, province, or services.
- The American College of Medical Genetics and Genomics (http://www.acmg.net/ACMG/Genetic_Services_Directory_Search.aspx) has a searchable database of medical genetics clinic services in the United States.
Adenoma sebaceum differential diagnosis
The differential diagnosis for angiofibroma depends on its location 3.
Differential diagnoses for facial lesions that can resemble angiofibromas can include:
- Intradermal melanocytic nevus
- Acne
- Basal cell carcinoma
- Adnexal tumors
Differential diagnoses for periungual lesions that can resemble angiofibroma can include:
- Viral warts
- Subungual exostosis.
Differential diagnoses for penile lesions that can resemble angiofibroma can include:
- Molluscum contagiosum
- Anogenital warts.
Adenoma sebaceum signs and symptoms
Adenoma sebaceum or an angiofibroma is a firm, flesh-colored dome-shaped papule less than 5 mm in diameter. Small capillaries may be visible on the surface of the lesion. Facial angiomas associated with a genetic syndrome are commonly found in clusters in the butterfly region of the face. Adenoma sebaceum or angiofibromas may be itchy and may also bleed. Those associated with genetic syndromes result in facial disfigurement and stigmatisation 3.
Tuberous sclerosis is a rare genetic disease that causes benign tumors to grow in the brain and other organs. Symptoms vary, depending on where the tumors grow. They could include
- Skin problems, such as light patches and thickened skin
- Seizures
- Behavior problems
- Intellectual disabilities
- Kidney problems
Some people have signs of tuberous sclerosis at birth. In others it can take time for the symptoms to develop. The disease can be mild, or it can cause severe disabilities. In rare cases, tumors in vital organs or other symptoms can be life-threatening.
Seventy-five percent of individuals with tuberous sclerosis will eventually develop adenoma sebaceum (angiofibromas). Periungual angiofibromas are less common in children, but the incidence increases to 40% in adults. In tuberous sclerosis, periungual angiofibromas occur in 30% to 60% of patients. Oral fibromas can occur in 30% to 70% of patients with tuberous sclerosis and occur more in adults than in children. Pearly penile papules occur in about 30% of post-pubertal males.
Adenoma sebaceum diagnosis
The diagnosis of adenoma sebaceum or angiofibroma may be made clinically or after a skin biopsy. The histopathology of adenoma sebaceum or angiofibroma shows an ‘onion skin’ pattern around vessels and follicles, hyperkeratosis, and vascular proliferation 9. All cutaneous angiofibromas are composed of a dermal proliferation of fibroblasts in a collagenous stroma with an increase in the number of thin-walled, dilated blood vessels. Collagen fibers are concentrically arranged around hair follicles and blood vessels. Elastic fibers can be decreased, and the epidermis can be atrophic. Fibroblasts can be stellate in shape and can be multinucleated. Immunohistochemistry for these cells will show positivity for factor XIIa and negative for S100 protein.
If an underlying genetic condition is suspected, appropriate genetic screening and evaluation are required 3.
Adenoma sebaceum treatment
Current treatments for adenoma sebaceum include shave excision, cryotherapy, electrodessication, radiofrequency ablation, dermabrasion, lasers such as ablative fractional laser resurfacing and pulsed dye laser (PDL), and topical podophyllotoxin. Although these treatments have proven to be successful, they can result in scarring, post-inflammatory hyperpigmentation, and pain. The recurrence rate can be up to 80%, necessitating follow-up treatments. Topical rapamycin, a mTOR inhibitor, seems to be a safe and effective treatment for angiofibromas however long-term studies still need to be conducted. Combination treatments, such as fractional laser resurfacing and PDL laser, can be employed with topical medications, such as timolol or rapamycin, to effectively treat these lesions 10.
Rapamycin has recently gained popularity in the treatment of angiofibromas. After binding to mTOR, it inhibits its activity which downregulates cell proliferation. It also decreases VEGF production by downregulating VEGF- stimulated endothelial cell proliferation. Several case series, case reports, and one randomized controlled trial have been published verifying the effectiveness of topical rapamycin used as 0.1% once or twice daily, as well as 0.2%, used 5 times a week and 0.4% used 3 times a week 11, 12. The angiofibromas cleared as long as the medication was being used. The longest reported follow up has been 3 years. Many have used crushed rapamycin tablets and mixed them in Vaseline to obtain the desired concentration which was not a standardized dose. DeKlotz et al. 13 proposed a standardized formulation on how to make 0.1% topical rapamycin in 2011. Few if any side effects occur from the topical medication including mild irritation and erythema. Park et al. 14 showed that topical rapamycin was enough to treat the lesions when they were small in size, that is less than 4 mm. However, if they were larger than 4 mm, ablative laser resurfacing was needed in conjunction with rapamycin. It can also be costly to use topical rapamycin in the treatment of angiofibromas due to the length of treatment that is necessary to obtain sufficient results costing several hundred to several thousand dollars out of pocket.
Beta-blockers have been used for many years now in the treatment of vascular lesions. Oral propranolol has been successful in the treatment of hemangiomas in the pediatric population. However, side effects such as hypoglycemia limit its use in certain patients. Topical timolol 0.5% solution or gel used 2 or 3 times a day has proven to be very successful in the treatment of superficial hemangiomas. The mechanism of action of beta-blockers is thought to be due to its role in blocking the formation of renin to angiotensin II. In doing so, angiotensin II does not form VEGF, which converts endothelial stem cells to endothelial cells, leading to decreased capillary development. Matrix metalloproteinase-9 is involved in angiogenesis, and its activity is thought to be inhibited by beta blockers. One other way beta- blockers work to decrease angiogenesis is by producing osteoprotegerin. This causes tumor necrosis factor apoptosis of mesenchymal and endothelial cells 15.
There is no cure for tuberous sclerosis, although treatment is available for a number of the symptoms. Rapamycin and related drugs are not yet approved by the U.S. Food and Drug Administration (FDA) for any purpose in individuals with tuberous sclerosis. The FDA has approved the drug everolimus (Afinitor®) to treat subependymal giant cell astrocytomas (SEGA brain tumors) and angiomyolipoma kidney tumors. Antiepileptic drugs such as vigabatrin may be used to control seizures and medications may be prescribed for behavior problems. Intervention programs, including special schooling and occupational therapy, may benefit individuals with special needs and developmental issues. Surgery, including dermabrasion and laser treatment, may be useful for treatment of skin lesions. Because tuberous sclerosis is a lifelong condition, individuals need to be regularly monitored by a doctor. Due to the many varied symptoms of tuberous sclerosis, care by a clinician experienced with the disorder is recommended.
Adenoma sebaceum prognosis
Although angiofibromas are benign, they are persistent and do not spontaneous improve and, when multiple, can cause significant disfigurement, bleeding, pruritus, and erythema emanating the need for an effective treatment. Angiofibromas can be removed for cosmetic or pain-related reasons. The recurrence rate for angiofibromas associated with tuberous sclerosis may be as high as 80% 3.
References- Goodrick S. The road to Vogt’s triad. Lancet Neurol. 2015;14:690.
- Osborne JP. Diagnosis of tuberous sclerosis. Arch Dis Child. 1988;63:1423–5.
- Macri A, Kwan E, Tanner LS. Cutaneous Angiofibroma. [Updated 2020 Sep 15]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK482470
- Bakić M, Ratković M, Gledović B, Vujović B, Radunović D, Babić V, Prelević V. Cutaneous Manifestations of Tuberous Sclerosis. Acta Dermatovenerol Croat. 2018 Apr;26(1):73-74.
- Krakowski AC, Nguyen TA. Inhibition of angiofibromas in a tuberous sclerosis patient using topical timolol 0.5% Gel. Pediatrics. 2015;136(3):e709-13. doi:10.1542/peds.2015-0025
- Garcia NG, de Carli ML, Oliveira DT, Soares CT, Ribeiro Júnior NV, Sperandio FF, Hanemann JA. Tuberous Sclerosis with Severe Cutaneous Manifestation and Multiples Facial Angiofibromas. Head Neck Pathol. 2016 Dec;10(4):542-546.
- Schaffer JV, Gohara MA, McNiff JM, Aasi SZ, Dvoretzky I. Multiple facial angiofibromas: a cutaneous manifestation of Birt-Hogg-Dubé syndrome. J Am Acad Dermatol. 2005;53(2 Suppl 1):S108-11. doi:10.1016/j.jaad.2004.11.021
- Cohen BA. Nodules and tumors. In: Pediatric Dermatology: Fourth Edition. Elsevier Inc.; 2013: 126–47. doi: 10.1016/B978-0-7234-3655-3.00005-9
- Johnston RB. Fibrous tumors and tumor-like proliferations. In: Weedon’s Skin Pathology Essentials. Elsevier; 2017: 612–39. doi:10.1016/b978-0-7020-6830-0.50034-7
- Wataya-Kaneda M, Tanaka M, Yang L, Yang F, Tsuruta D, Nakamura A, Matsumoto S, Hamasaki T, Tanemura A, Katayama I. Clinical and Histologic Analysis of the Efficacy of Topical Rapamycin Therapy Against Hypomelanotic Macules in Tuberous Sclerosis Complex. JAMA Dermatol. 2015 Jul;151(7):722-30.
- SMALL CASE SERIESTopical rapamycin for angiofibromas in paediatricpatients with tuberous sclerosis: Follow up of a pilotstudy and promising future directions. Australasian Journal of Dermatology(2014)55,63–69 doi: 10.1111/ajd.12125 https://onlinelibrary.wiley.com/doi/pdf/10.1111/ajd.12125
- Bouguéon G, Lagarce F, Martin L, Pailhoriès H, Bastiat G, Vrignaud S. Formulation and characterization of a 0.1% rapamycin cream for the treatment of Tuberous Sclerosis Complex-related angiofibromas. Int J Pharm. 2016 Jul 25;509(1-2):279-284.
- DeKlotz CM, Ogram AE, Singh S, Dronavalli S, MacGregor JL. Dramatic improvement of facial angiofibromas in tuberous sclerosis with topical rapamycin: Optimizing a treatment protocol. Arch Dermatol. 2011;147:1116–7.
- Park J, Yun SK, Cho YS, Song KH, Kim HU. Treatment of angiofibromas in tuberous sclerosis complex: the effect of topical rapamycin and concomitant laser therapy. Dermatology. 2014;228(1):37-41.
- Patel AM, Chou EL, Findeiss L, Kelly KM. The horizon for treating cutaneous vascular lesions. Semin Cutan Med Surg. 2012 Jun;31(2):98-104.