What is brain cancer
A brain cancer also called malignant brain tumor, is a mass or growth of abnormal cells in your brain or close to your brain – that have grown out of control 1. A brain cancer (malignant brain tumor) is a fast-growing cancer that spreads to other areas of the brain and spine. The main concerns with brain and spinal cord cancer are how readily they spread through the rest of the brain or spinal cord and whether they can be removed and not come back.
Brain and spinal cord tumors tend to be different in adults and children. They often form in different areas, develop from different cell types, and may have a different outlook and treatment.
Brain cancers can begin in your brain (primary brain tumors), or cancer can begin in other parts of your body and spread to your brain (secondary or metastatic, brain tumors). Most malignant tumors are secondary cancers, which means they started in another part of the body and spread to the brain. Primary brain tumors are those that started in the brain.
The American Cancer Society’s estimates for brain and spinal cord tumors in the United States for 2022 include both adults and children 2:
- About 25,050 malignant tumors of the brain or spinal cord (14,170 in males and 10,880 in females) will be diagnosed. These numbers would be much higher if benign (non-cancer) tumors were also included.
- About 18,280 people (10,710 males and 7,570 females) will die from brain and spinal cord tumors.
Overall, the chance that a person will develop a malignant tumor of the brain or spinal cord in his or her lifetime is less than 1%. The risk for men (about 1 in 140) is slightly higher than that for women (about 1 in 190), although certain types of tumors are more common in women.
Doctors diagnose brain tumors by doing a neurologic exam and tests including an MRI, CT scan, and biopsy.
When diagnosed with a brain tumor, it is important to understand:
- The type and grade of the brain tumor (how aggressive it is)
- Whether it is a primary or a secondary brain tumor
- If it is cancerous (malignant) or benign brain tumor
- Where in the brain the tumor is located
Brain tumor treatment options depend on the type of brain tumor you have, as well as its size and location. Brain tumor treatment options include watchful waiting, surgery, radiation therapy, chemotherapy, and targeted therapy. Targeted therapy uses drugs or other substances that attack cancer cells with less harm to normal cells. Many people get a combination of treatments.
Survival rates for brain and spinal cord tumors vary widely, depending on the type of tumor (and other factors). Rates for some of the more common types of brain and spinal cord tumors are discussed in Survival Rates for Selected Adult Brain and Spinal Cord Tumors.
How quickly a brain tumor grows can vary greatly. The growth rate as well as location of a brain tumor determines how it will affect the function of your nervous system.
Generally, brain cancers (tumors) are graded from 1 to 4, according to their behavior, such as how fast they grow and how likely they are to grow back after treatment. A malignant brain tumor is either grade 3 or 4, whereas grade 1 or 2 tumors are usually classed as benign or non-cancerous.
Brain and spinal cord tumors are the second most common cancers in children (after leukemia). They account for about 1 out of 4 childhood cancers. More than 4,000 central nervous system tumors are diagnosed each year in children and teens. The incidence rate (number of tumors per 100,000 children) has not changed much in recent years.
Boys develop these tumors slightly more often than girls.
About 3 out of 4 children with brain tumors (all types combined) survive at least 5 years after being diagnosed. The outlook can vary a great deal based on the type of tumor, where it is, and other factors.
Survival rates for some of the more common types of brain and spinal cord tumors are discussed towards the bottoms of this article in Survival rates for more common childhood brain and spinal cord tumors.
Human Brain
To understand brain and spinal cord tumors, it helps to know about the normal structure and function of the central nervous system (CNS), which is the medical name for the brain and spinal cord. The human brain is a component of the central nervous system (CNS). The human brain is roughly the size of two clenched fists and weighs about 1.6 kg (3.5 lb) in men and 1.45 kg in women 3. The difference between the sexes is proportional to body size, not intelligence.
The brain is the center of thought, feeling, memory, speech, vision, hearing, movement, breathing, and much more. The spinal cord and special nerves in the head called cranial nerves help carry messages between the brain and the rest of the body. These messages tell our muscles how to move, transmit information gathered by our senses, and help coordinate the functions of our internal organs.
The brain is protected by the skull. Likewise, the spinal cord is protected by the bones (vertebrae) of the spinal column.
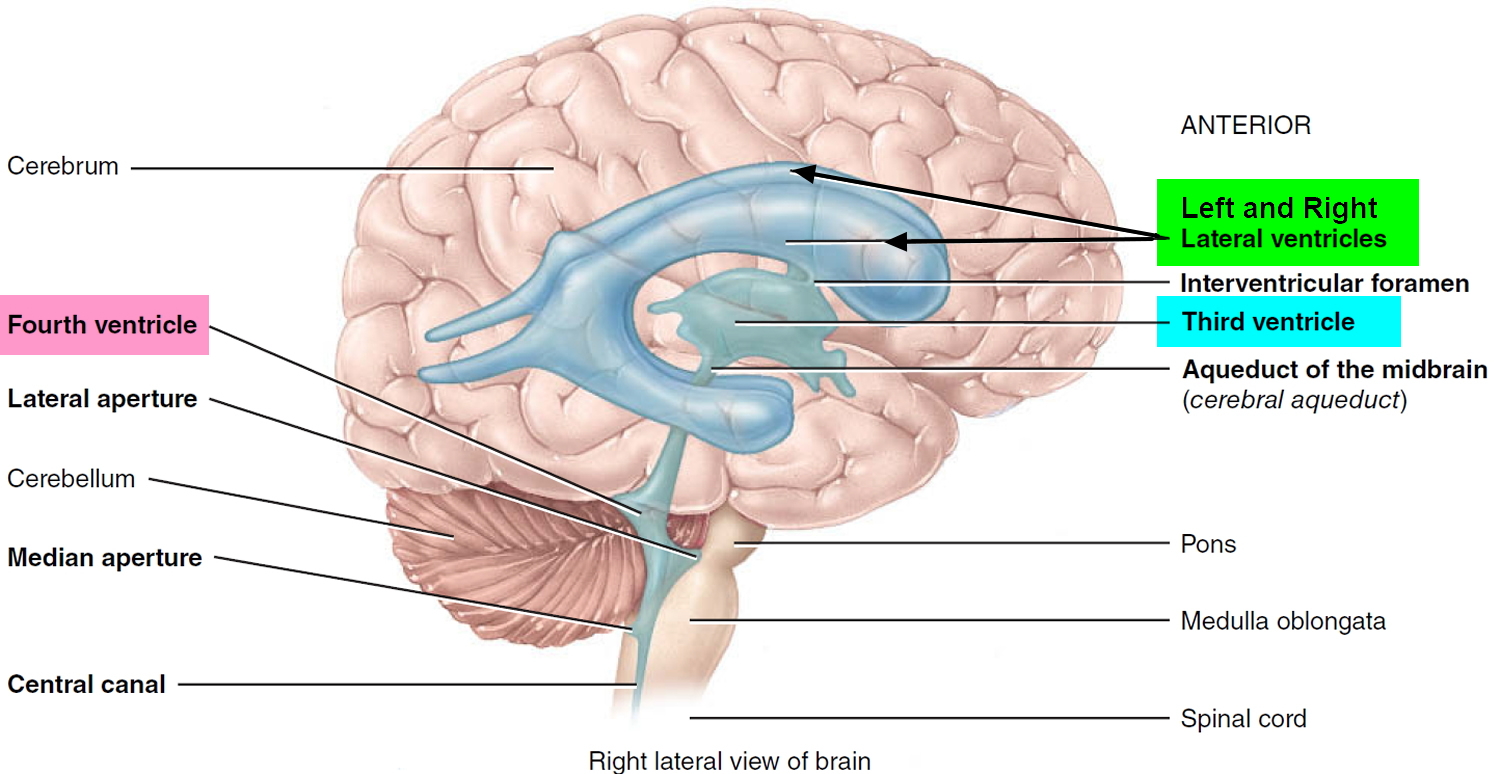
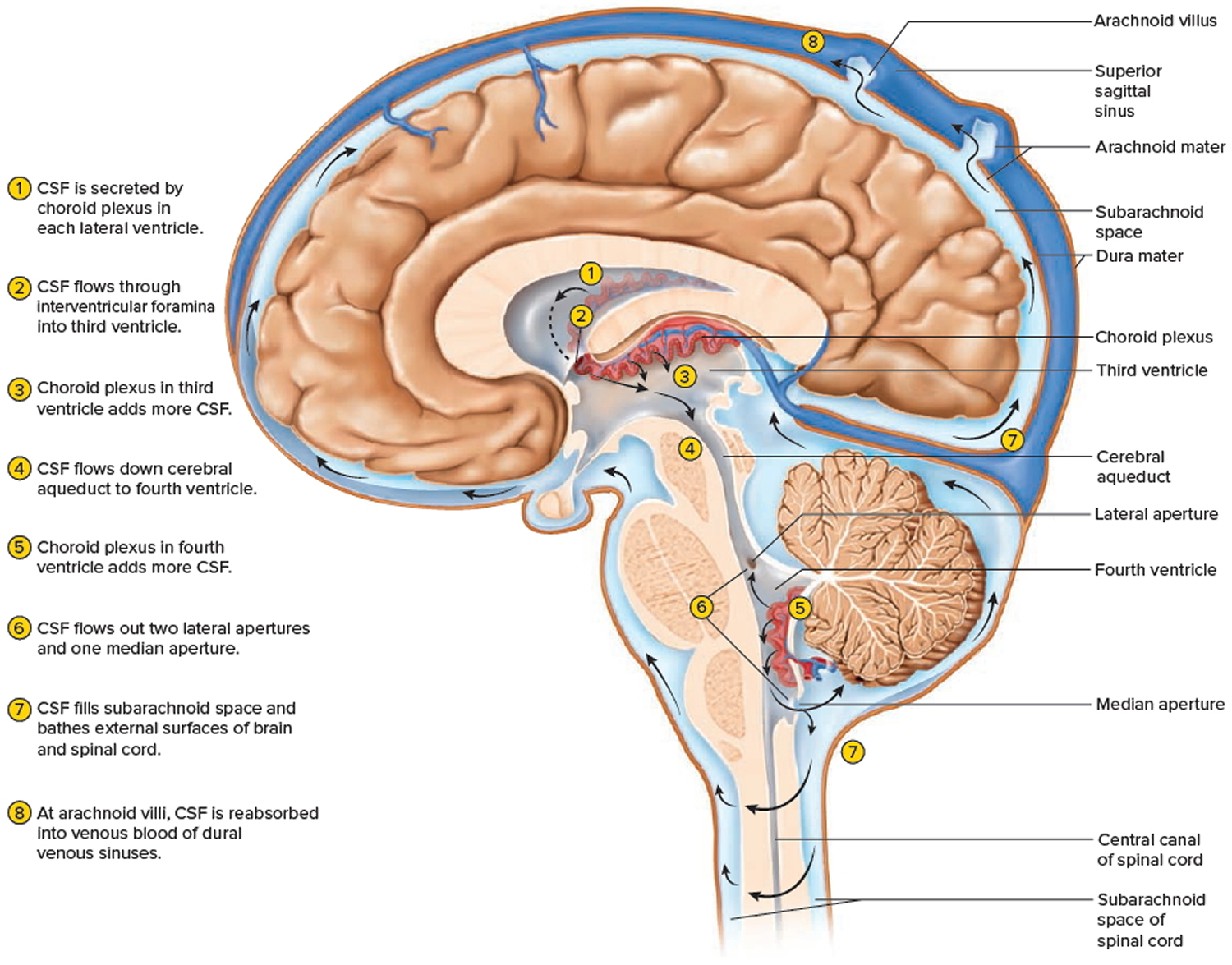
The brain and spinal cord are surrounded and cushioned by a special liquid, called cerebrospinal fluid (CSF). Cerebrospinal fluid is made by the choroid plexus, which is found in spaces within the brain called ventricles. The ventricles and the spaces around the brain and spinal cord are filled with CSF.
Anatomists conceptually divide the brain into four major parts:
- The Cerebrum. The cerebrum controls thinking, learning, problem solving, emotions, speech, reading, writing, and voluntary movement.
- The Diencephalon (thalamus, hypothalamus, and epithalamus).
- The Cerebellum. The cerebellum controls movement, balance, and posture.
- The Brainstem. The brain stem connects the brain to the spinal cord, and controls breathing, heart rate, and the nerves and muscles that we use to see, hear, walk, talk, and eat.
Together, the brain and spinal cord (the central nervous system [CNS]) control the physiological and psychological functions of your body.
The brain, like the spinal cord, is composed of gray and white matter. Gray matter—the seat of the neurosomas, dendrites, and synapses—forms a surface layer called the cortex over the cerebrum and cerebellum, and deeper masses called nuclei surrounded by white matter. White matter lies deep to the cortical gray matter in most of the brain, opposite from the relationship of gray and white matter in the spinal cord. As in the spinal cord, white matter is composed of tracts, or bundles of axons, which here connect one part of the brain to another and to the spinal cord.
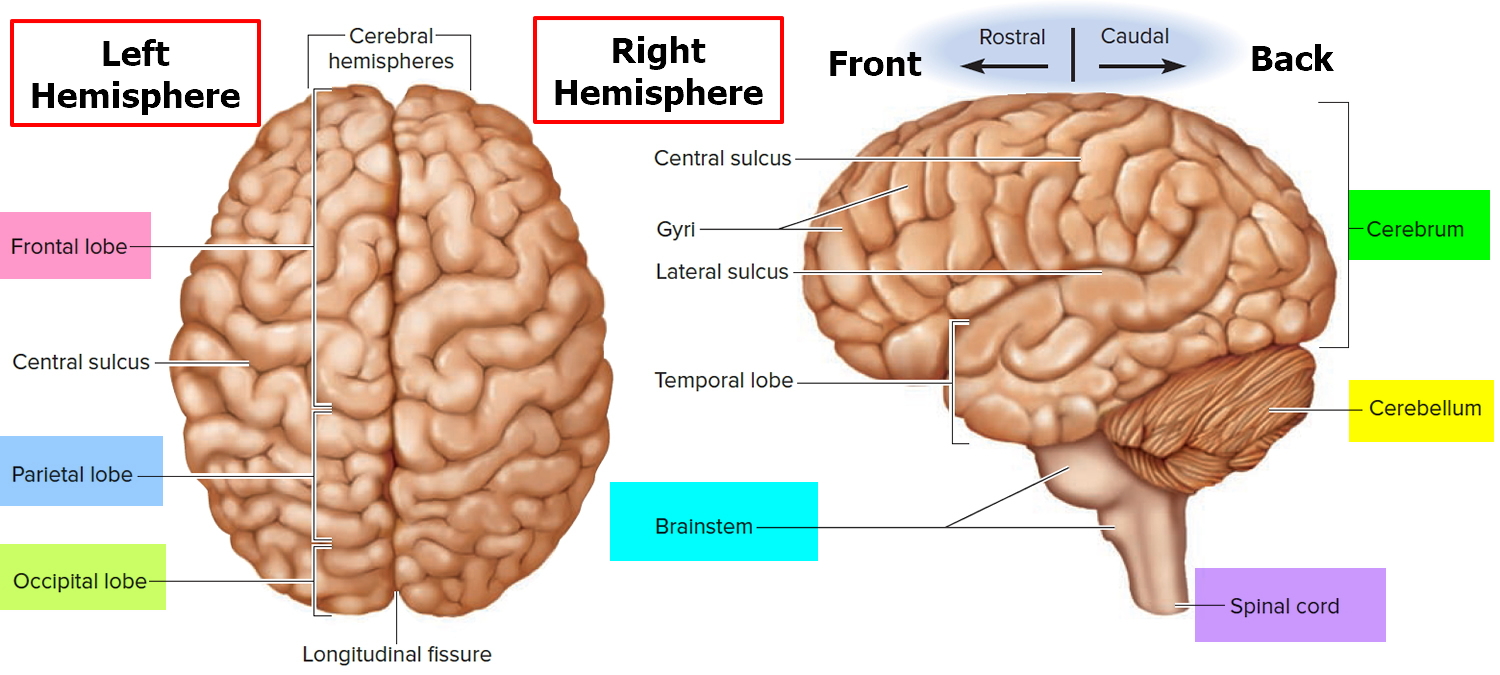
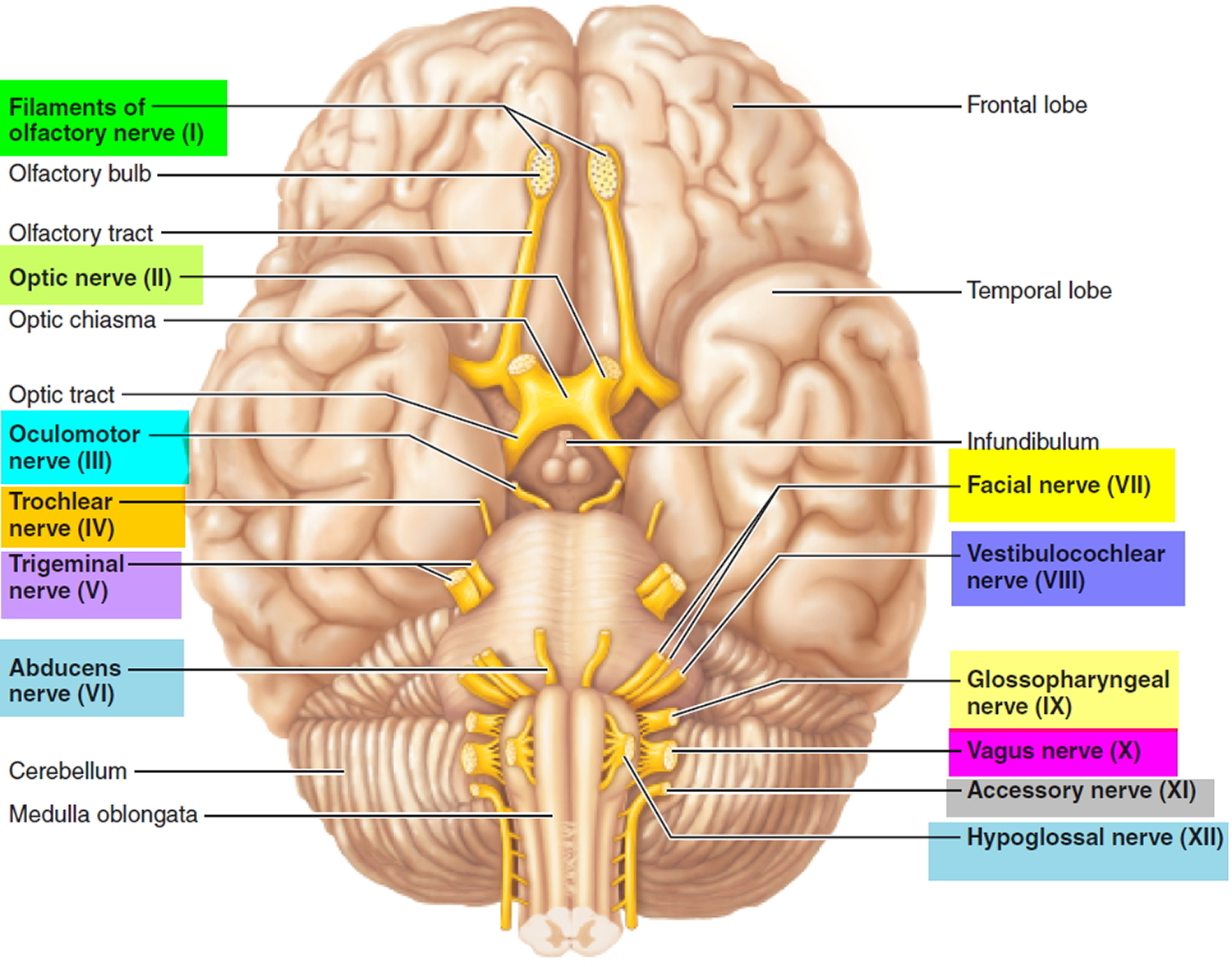
Figure 1. Human brain
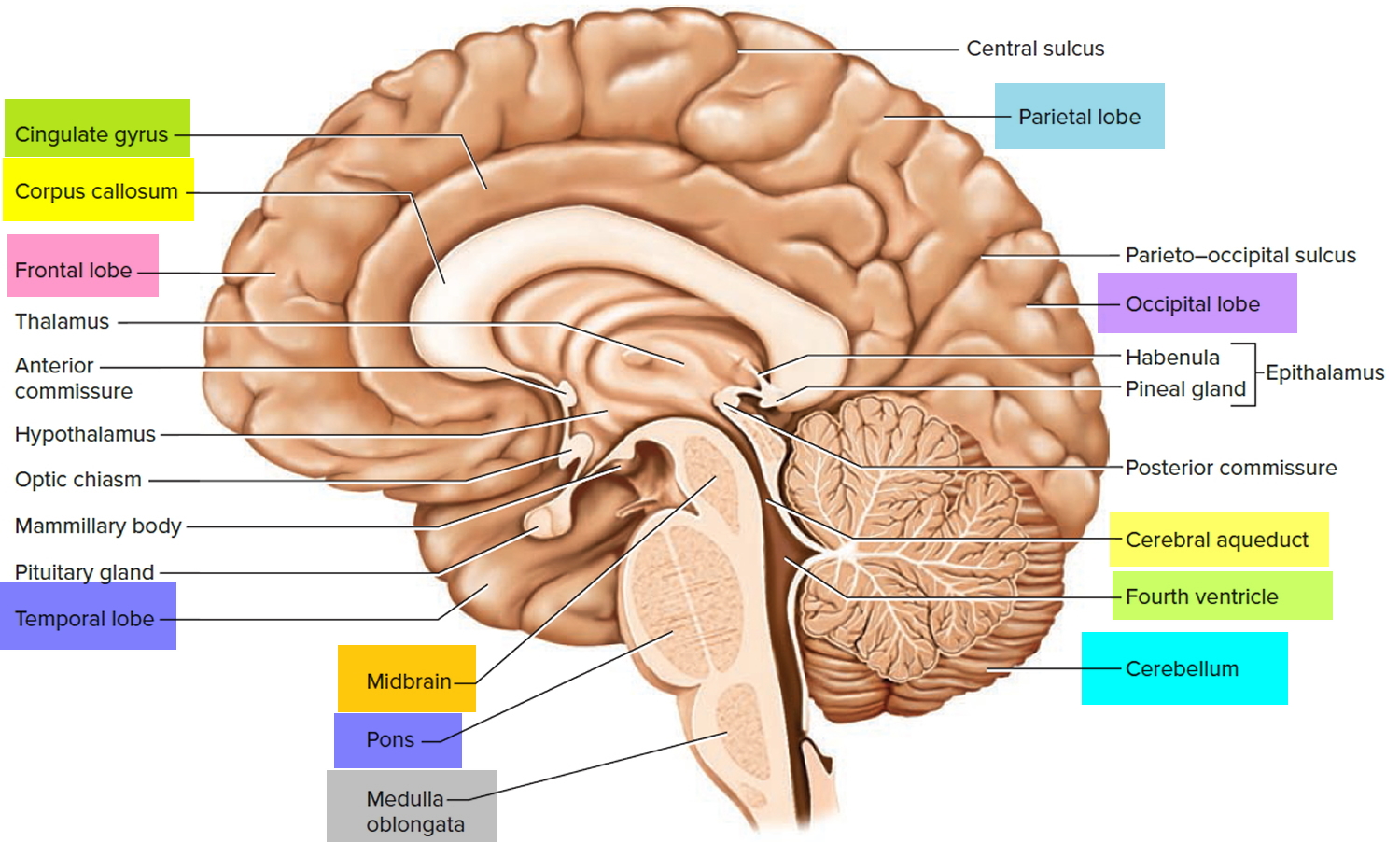
Figure 2. Medial aspect of the human brain
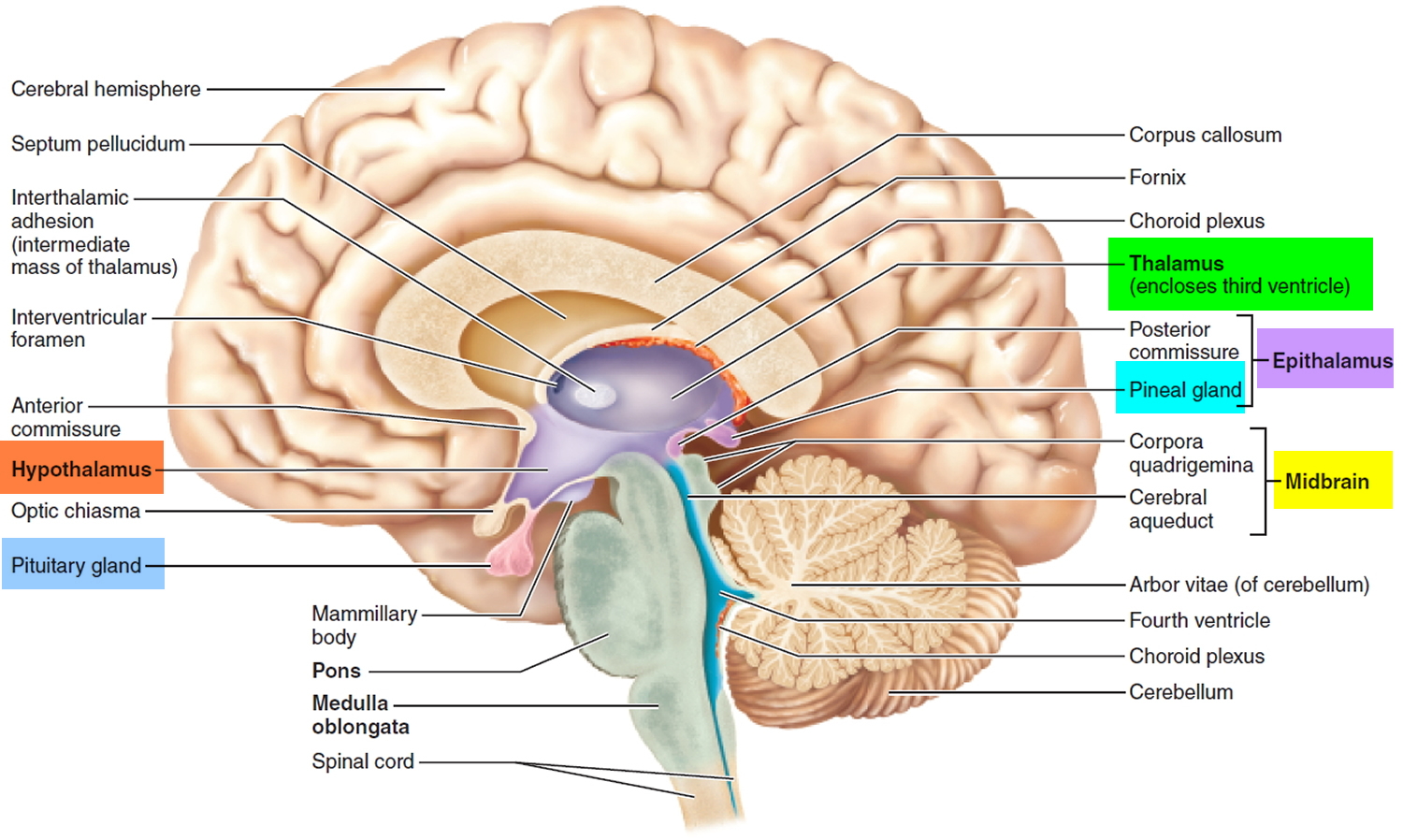
Figure 3. Diencephalon of the human brain
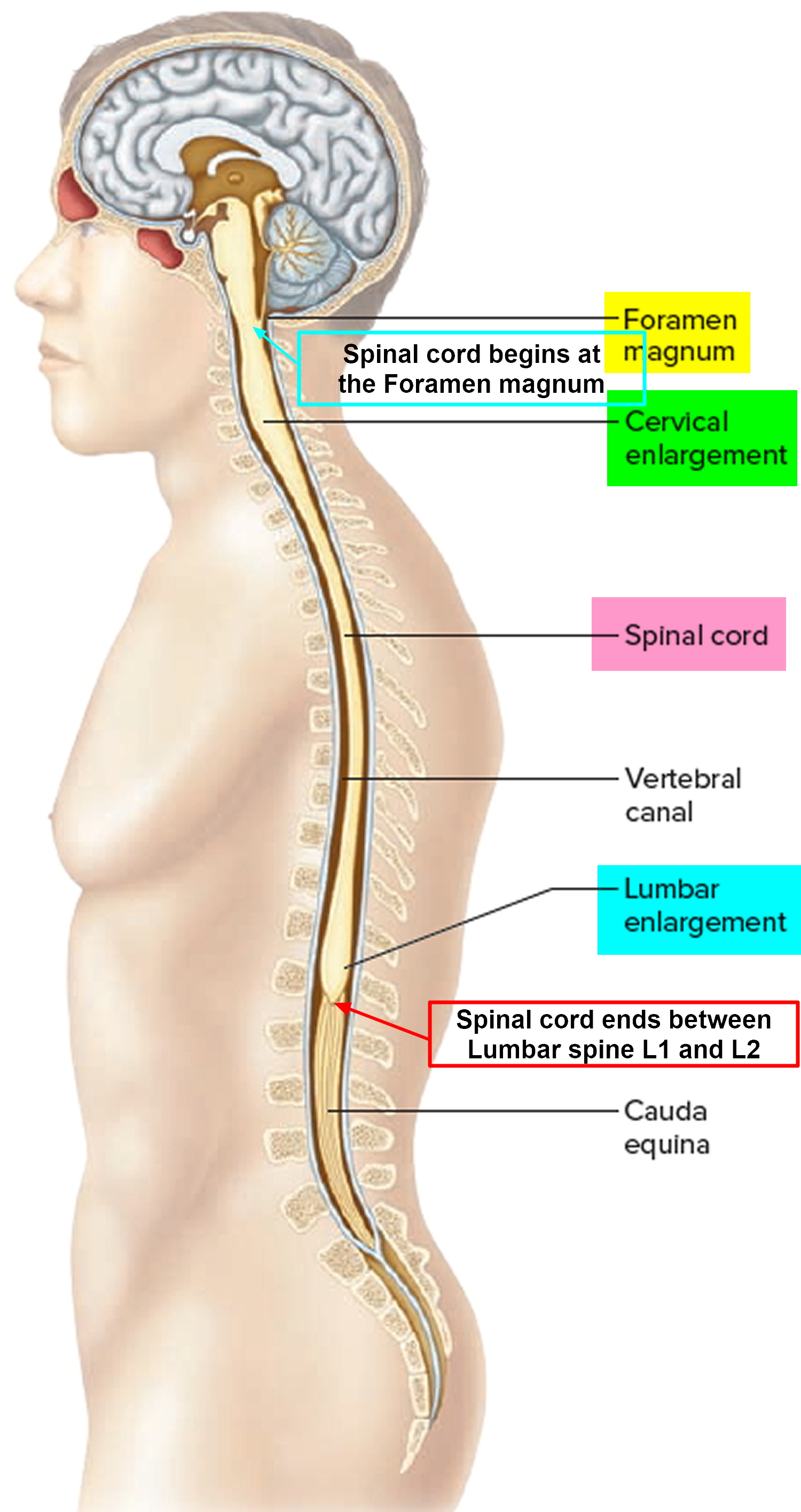
Figure 4. Spinal cord
Figure 6. Ventricles of the brain
Figure 7. Cerebrospinal fluid (CSF) formation, absorption and circulation around and within the brain
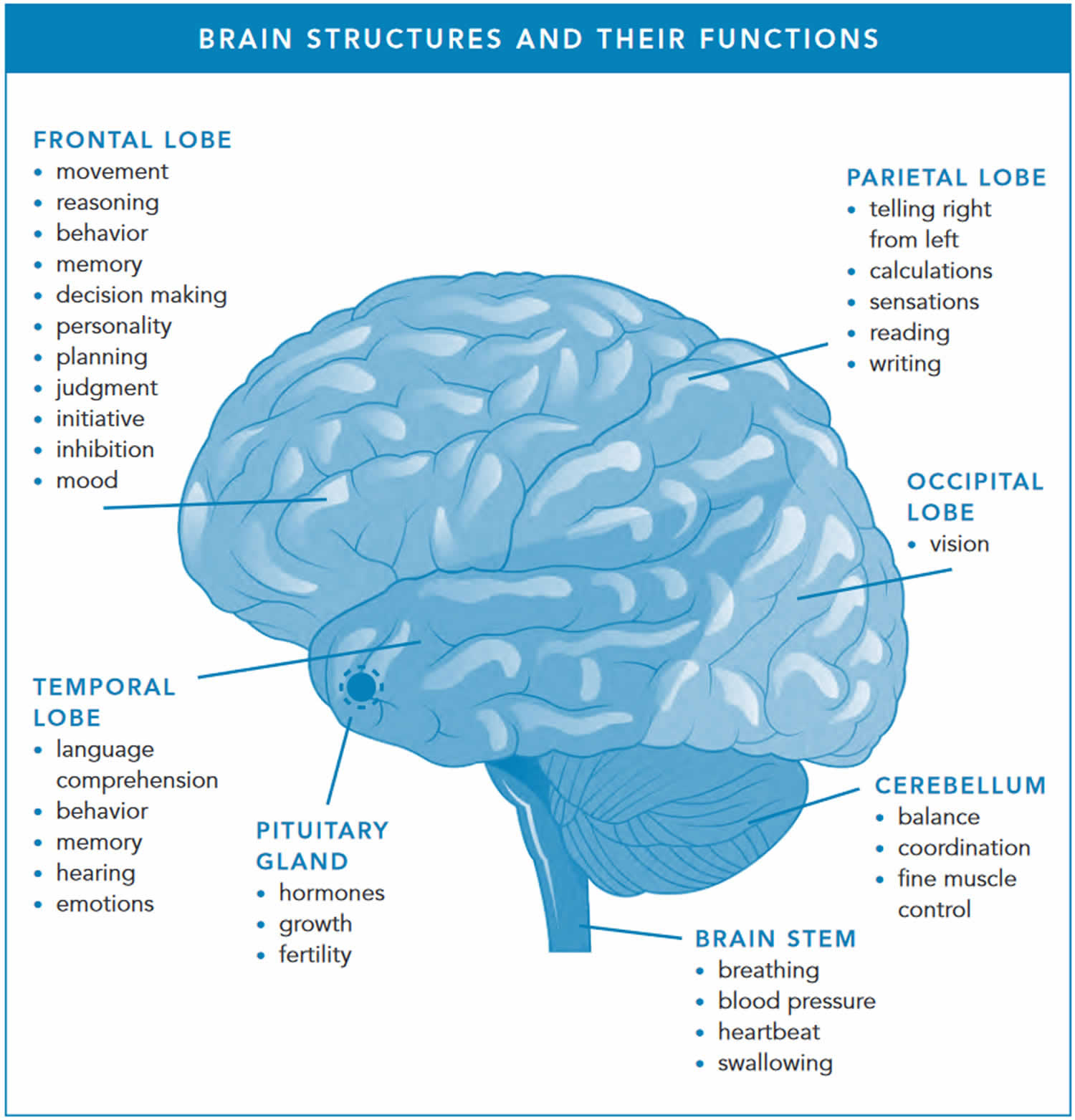
Figure 8. Brain structures and brain functions
Parts of the brain
Anatomists conceptually divide the brain into four major parts. Each part has a special function.
- The Cerebrum.
- The Diencephalon (thalamus, hypothalamus, and epithalamus).
- The Cerebellum.
- The Brain stem.
Cerebrum
The cerebrum is the large, outer part of the brain. The cerebrum is about 83% of the brain’s volume and consists of a pair of half globes called the cerebral hemispheres (left and right hemispheres). Each hemisphere is marked by thick folds called gyri (singular, gyrus) separated by shallow grooves called sulci (singular, sulcus). A very deep median groove, the longitudinal fissure, separates the right and left hemispheres from each other. At the bottom of this fissure, the hemispheres are connected by a thick bundle of nerve fibers called the corpus callosum—a prominent landmark for anatomical description with a distinctive C shape in sagittal section.
The cerebral hemispheres control reasoning, thought, emotion, and language. It is also responsible for planned (voluntary) muscle movements (throwing a ball, walking, chewing, etc.) and for taking in and interpreting sensory information such as vision, hearing, smell, touch, and pain.
The symptoms caused by a tumor in a cerebral hemisphere depend on where the tumor is. Common symptoms include:
- Seizures
- Trouble speaking
- A change of mood such as depression
- A change in personality
- Weakness or paralysis in part of the body
- Changes in vision, hearing, or other senses
Cerebellum
The cerebellum occupies the posterior cranial fossa inferior to the cerebrum, separated from it by the transverse cerebral fissure. It is also marked by fissures, sulci, and gyri (called folia in the cerebellum). The cerebellum is the second-largest region of the brain, constituting about 10% of its volume but containing over 50% of its neurons.
The cerebellum lies under the cerebrum at the back part of the brain. It helps coordinate movement. Tumors of the cerebellum can cause problems with coordination in walking, trouble with precise movements of hands, arms, feet, and legs, problems swallowing or synchronizing eye movements, and changes in speech rhythm.
Brain stem
The brain stem is the lower part of the brain that connects to the spinal cord. It contains bundles of very long nerve fibers that carry signals controlling muscles and sensation or feeling between the cerebrum and the rest the body. Special centers in the brain stem also help control breathing and the beating of the heart. Also, most cranial nerves (see Figures 1 and 2) start in the brain stem.
The brainstem is defined all of the brain except the cerebrum and cerebellum. The brain stem is divided into 3 main parts, from rostral (front towards the nose) to caudal (back end), are the midbrain, pons, and medulla oblongata. In a living person, the brainstem is oriented like a vertical stalk with the cerebrum perched on top like a mushroom cap. Postmortem changes give it a more oblique angle in the cadaver and consequently, in many medical illustrations. Towards the back end, the brainstem ends at the foramen magnum of the skull, and the central nervous system (CNS) continues below this as the spinal cord.
Tumors in this critical area of the brain can cause weakness, stiff muscles, or problems with sensation, facial or eye movement, hearing, or swallowing. Double vision is a common early symptom of brain stem tumors, as are problems with coordination in walking. Because the brain stem is a small area that is so essential for life, it might not be possible to surgically remove tumors in this area.
The Diencephalon (thalamus, hypothalamus, and epithalamus)
Deep in the core area of the brain, just above the top of the brainstem, is the diencephalon that consists largely of three paired structures—the thalamus, the hypothalamus and the epithalamus. The diencephalon are structures that have a great deal to do with perception, movement, and the body’s vital functions.
The thalamus consists of two oval masses that contain about a dozen major nuclei, each of which sends axons to a particular portion of the cerebral cortex (Figure 3). The thalamic masses contain nerve cell bodies that sort information from four of the senses—sight, hearing, taste, and touch—and relay it to the cerebral cortex. (Only the sense of smell sends signals directly to the cortex, bypassing the thalamus.) Sensations of pain, temperature, and pressure are also relayed through the thalamus, as are the nerve impulses from the cerebral hemispheres that initiate voluntary movement.
Sensory inputs are not the only type of information relayed through the thalamus. Every part of the brain that communicates with the cerebral cortex must relay its signals through a nucleus of the thalamus. The thalamus can therefore be thought of as the “gateway” to the cerebral cortex.
The thalamus not only relays information to the cerebral cortex but also processes the information as it passes through.
The thalamic nuclei organize and then either amplify or “tone down” the signals headed for the cerebral cortex. This is why, for example, you can focus on a conversation with a single person in large, noisy cafeteria.
The hypothalamus (“below the thalamus”) is the inferior portion of the diencephalon. Projecting inferiorly from the hypothalamus is the pituitary gland (Figure 1) and the hypothalamus occupies approximately 2 per cent of the brain volume. The hypothalamus is situated in a strategic position at the crossroad of four systems, neurovegetative, neuroendocrine, limbic, and optic 4.
The hypothalamus forms the inferolateral walls of the third ventricle. On the underside of the brain, the hypothalamus lies between the optic chiasma (point of crossover of cranial nerves II, the optic nerves) and the posterior border of the mammillary bodies, rounded bumps that bulge from the hypothalamic floor (mammillary = “little breast”).
The hypothalamus, like the thalamus, contains about a dozen brain nuclei of gray matter. Despite its relatively small size (roughly that of a thumbnail or an almond), functionally, the hypothalamus is the main visceral control center of the body, regulating many activities of the visceral organs.
The hypothalamus is the main point of interaction for the body’s two physical control systems: the nervous system, which transmits information in the form of minute electrical impulses, and the endocrine system, which brings about changes of state through the release of chemical factors. It is the hypothalamus that first detects crucial changes in the body and responds by stimulating various glands and organs to release hormones.
Cranial nerves
The cranial nerves extend directly out of the base of the brain (as opposed to coming out of the spinal cord). These nerves carry signals directly between the brain and the face, eyes, ears, tongue, mouth, and some other areas.
Tumors starting in cranial nerves can cause vision problems, trouble swallowing, hearing loss in one or both ears, or facial paralysis, numbness, or pain.
Spinal cord
The spinal cord has bundles of very long nerve fibers that carry signals that control muscles, sensation or feeling, and bladder and bowel control.
Spinal cord tumors can cause weakness, paralysis, or numbness. The spinal cord is a narrow structure, so tumors within it usually cause symptoms on both sides of the body (for example, weakness or numbness of both legs). This is different from most brain tumors, which often affect only one side of the body.
The nerves that reach the arms begin in the spinal cord at the level of the neck (cervical spine). Nerves that branch off the spinal cord to the legs, bowel, and bladder arise in the back (thoracic and lumbar spine). Most tumors of the spinal cord start in the neck and can cause symptoms in the arms and legs, as well as affect bowel and bladder function. Spinal cord tumors below the neck only affect the legs and bowel and bladder function.
Blood-brain barrier
The inner lining of the small blood vessels (capillaries) in the brain and spinal cord creates a very selective barrier between the blood and the tissues of the central nervous system. This barrier normally helps maintain the brain’s metabolic balance and keeps harmful toxins from getting into the brain. Unfortunately, it also keeps out most chemotherapy drugs that are used to kill cancer cells, which in some cases limits their usefulness.
Choroid plexus
The choroid plexus is the area of the brain within the ventricles that makes CSF, which nourishes and protects the brain.
Pineal gland
The pineal gland is not really part of the brain. The pineal gland is a small endocrine gland that sits between the cerebral hemispheres. It makes melatonin, a hormone that regulates sleep, in response to changes in light. The most common tumors of the pineal gland are called pineoblastomas.
Types of cells and body tissues in the brain and spinal cord
The brain and spinal cord have many kinds of tissues and cells, which can develop into different types of tumors.
Neurons (nerve cells): These are the cells in the brain that help determine thought, memory, emotion, speech, muscle movement, sensation, and just about everything else that the brain and spinal cord do. They do this by transmitting chemical and electrical signals through their nerve fibers (axons). Axons in the brain tend to be short, while those in the spinal cord can be as long as several feet.
Unlike many other types of cells that can grow and divide to repair damage from injury or disease, neurons in the brain and spinal cord largely stop dividing about a year after birth (with a few exceptions). Neurons do not usually form tumors, but they are often damaged by tumors that start nearby.
Glial cells: Glial cells are the supporting cells of the brain. Most brain and spinal cord tumors develop from glial cells. These tumors are sometimes referred to as gliomas.
There are 3 types of glial cells – astrocytes, oligodendrocytes, and ependymal cells. A fourth cell type called microglia is part of the immune system and is not truly a glial cell.
- Astrocytes help support and nourish neurons. When the brain is injured, astrocytes form scar tissue that helps repair the damage. The main tumors starting in these cells are called astrocytomas or glioblastomas.
- Oligodendrocytes make myelin, a fatty substance that surrounds and insulates the nerve cell axons of the brain and spinal cord. This helps neurons send electric signals through the axons. Tumors starting in these cells are called oligodendrogliomas.
- Ependymal cells line the ventricles (fluid-filled areas) within the brain and form part of the pathway through which CSF flows. Tumors starting in these cells are called ependymomas.
- Microglia are the immune (infection-fighting) cells of the central nervous system.
Neuroectodermal cells: These are very early forms of nervous system cells that are probably involved in brain cell development. They are found throughout the brain, although they are not often seen in the adult central nervous system. The most common tumors that come from these cells develop in the cerebellum and are called medulloblastomas.
Meninges: These are layers of tissue that line and protect the brain and spinal cord. CSF travels through spaces formed by the meninges. The most common tumors that start in these tissues are called meningiomas.
Choroid plexus: The choroid plexus is the area of the brain within the ventricles that makes CSF, which nourishes and protects the brain.
Pituitary gland and hypothalamus: The pituitary is a small gland at the base of the brain. It is connected to a part of the brain called the hypothalamus. Both make hormones that help regulate the activity of several other glands in the body. For example, they control the amount of thyroid hormone made by the thyroid gland, breast milk production and release, and the amount of male or female hormones made by the testicles or ovaries. They also make growth hormone, which stimulates body growth, and vasopressin, which regulates water balance by the kidneys.
The growth of tumors in or near the pituitary or hypothalamus, as well as surgery and/or radiation therapy in this area, can affect these functions. For example, tumors starting in the pituitary gland sometimes make too much of a certain hormone, which can cause problems. On the other hand, a person may have low levels of one or more hormones after treatment and may need to take hormones to make up for this.
Pineal gland: The pineal gland is not really part of the brain. It is a small endocrine gland that sits between the cerebral hemispheres. It makes melatonin, a hormone that regulates sleep, in response to changes in light. The most common tumors of the pineal gland are called pineoblastomas.
Blood-brain barrier: The inner lining of the small blood vessels (capillaries) in the brain and spinal cord creates a very selective barrier between the blood and the tissues of the central nervous system. This barrier normally helps maintain the brain’s metabolic balance and keeps harmful toxins from getting into the brain. Unfortunately, it also keeps out most chemotherapy drugs that are used to kill cancer cells, which in some cases limits their usefulness.
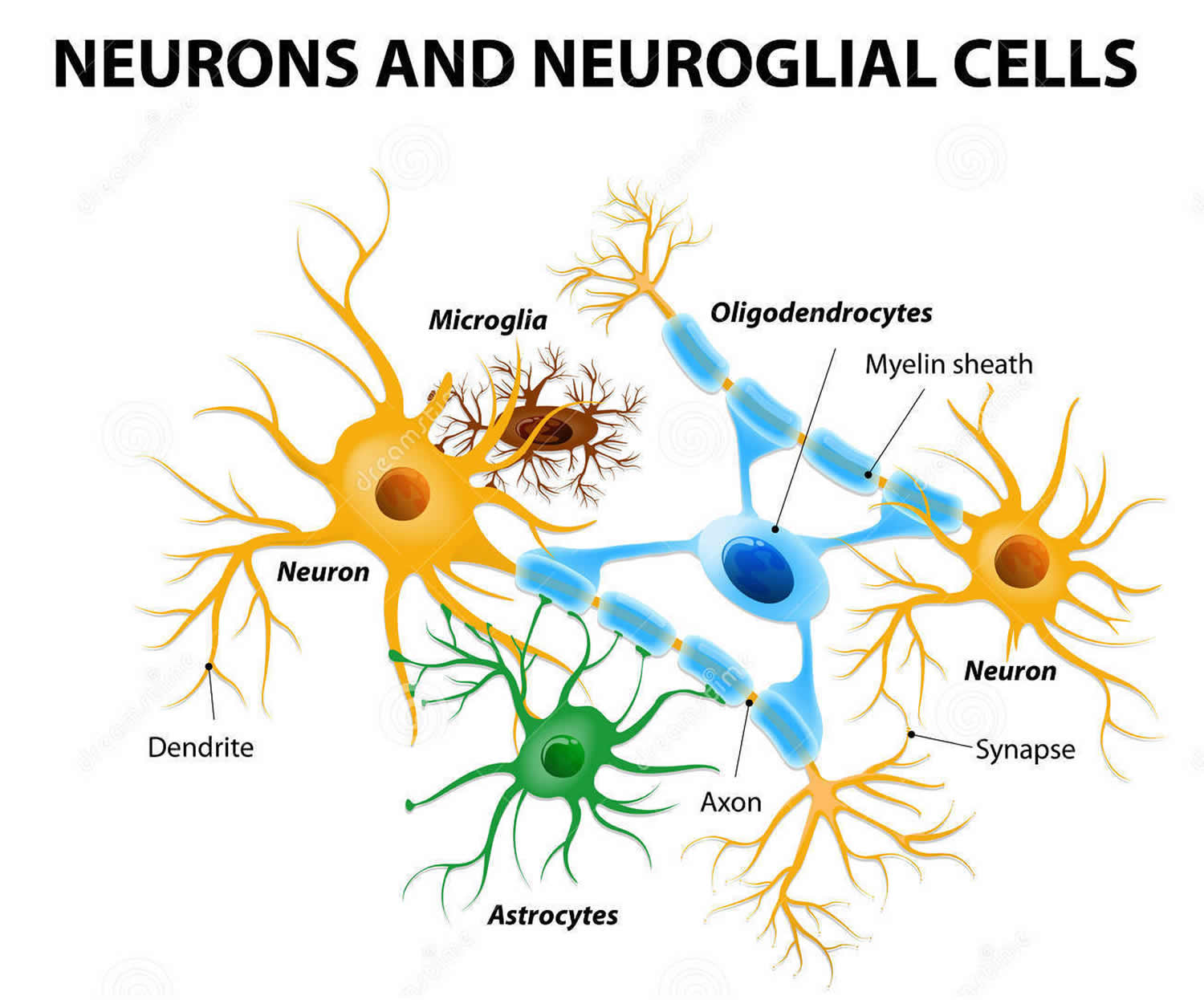
Figure 9. Glial (neuroglial) cells in the brain (astrocytes, oligodendrocytes, and microglial cells)
Footnote: Glial (Neuroglial) cells do not conduct nerve impulses, but, instead, support, nourish, and protect the neurons. Glial cells (glia) are far more numerous than neurons and, unlike neurons, are capable of mitosis. Glial roles that are well-established include maintaining the ionic milieu of nerve cells, modulating the rate of nerve signal propagation, modulating synaptic action by controlling the uptake of neurotransmitters, providing a scaffold for some aspects of neural development, and aiding in (or preventing, in some instances) recovery from neural injury 5.
Brain cancer survival rate
Survival rates are a way to get a general idea of the outlook (prognosis) for people with a certain type of tumor. They tell you what portion of people with the same type of tumor are still alive a certain amount of time (usually 5 years) after they were diagnosed. They can’t tell you how long you will live, but they may help give you a better understanding about how likely it is that your treatment will be successful.
The 5-year survival rate is the percentage of people who live at least 5 years after being diagnosed. For example, a 5-year survival rate of 70% means that an estimated 70 out of 100 people who have that type of tumor are still alive 5 years after being diagnosed. Keep in mind, however, that many of these people live much longer than 5 years.
Relative survival rates (like the numbers below) are a more accurate way to estimate the effect of cancer on survival. These rates compare people with cancer to people in the overall population. For example, if the 5-year relative survival rate for a specific type of tumor is 70%, it would mean that people who have that type of tumor are, on average, about 70% as likely as people who don’t have that tumor to live for at least 5 years after being diagnosed.
But remember, the 5-year relative survival rates are estimates – your outlook can vary based on a number of factors specific to you.
Survival rates don’t tell the whole story
Survival rates are often based on previous outcomes of large numbers of people who had the disease, but they can’t predict what will happen in any particular person’s case. There are some limitations to remember:
These numbers are among the most current available. But to get 5-year survival rates, doctors have to look at people who were treated at least 5 years ago. As treatments are improving over time, people who are now being diagnosed with brain or spinal cord tumors may have a better outlook than these statistics show.
The outlook for people with brain or spinal cord tumors varies by the type of tumor and the person’s age. But many other factors can also affect a person’s outlook, such as their age and overall health, where the tumor is located, and how well the tumor responds to treatment. The outlook for each person is specific to their circumstances.
Your doctor can tell you how these numbers may apply to you, as he or she is familiar with your situation.
Survival rates for more common adult brain and spinal cord tumors
The numbers in the table below come from the Central Brain Tumor Registry of the United States (https://cbtrus.org) and are based on people who were treated between 2001 and 2015. As can be seen below, survival rates for some types of brain and spinal cord tumors can vary widely by age, with younger people tending to have better outlooks than older people. The survival rates for those 65 or older are generally lower than the rates for the ages listed below.
These numbers are for some of the more common types of brain and spinal cord tumors. Accurate numbers are not readily available for all types of tumors, often because they are rare or are hard to classify.
Survival rates can give you an idea of what percentage of people with the same type of brain or spinal cord tumor are still alive a certain amount of time (such as 5 years) after they were diagnosed. They can’t tell you how long you will live, but they may help give you a better understanding of how likely it is that your treatment will be successful.
Keep in mind that survival rates are estimates and are often based on previous outcomes of large numbers of people who had a specific type of tumor, but they can’t predict what will happen in any particular person’s case. These statistics can be confusing and may lead you to have more questions. Your doctor is familiar with your situation; ask how these numbers may apply to you.
A relative survival rate compares people with the same type of tumor to people in the overall population. For example, if the 5-year relative survival rate for a specific type of brain tumor is 70%, it means that people who have that tumor are, on average, about 70% as likely as people who don’t have that tumor to live for at least 5 years after being diagnosed.
Remember, these survival rates are only estimates – they can’t predict what will happen to any individual. If you find these statistics are confusing and you have more questions, talk to your doctor to better understand your specific situation.
Table 1. Survival rates for common adult brain and spinal cord tumors
| Type of Brain Tumor | 5-Year Relative Survival Rate | ||
|---|---|---|---|
| Age | |||
| 20-44 | 45-54 | 55-64 | |
| Low-grade (diffuse) astrocytoma | 73% | 46% | 26% |
| Anaplastic astrocytoma | 58% | 29% | 15% |
| Glioblastoma | 22% | 9% | 6% |
| Oligodendroglioma | 90% | 82.00% | 69% |
| Anaplastic oligodendroglioma | 76% | 67% | 45% |
| Ependymoma/anaplastic ependymoma | 92% | 90% | 87% |
| Meningioma | 84% | 79% | 74% |
Footnotes:
- These numbers don’t take everything into account. Survival rates are grouped here based on tumor type and a person’s age. But other factors, such as the location of the tumor, whether it can be removed (or destroyed) completely, and if the tumor cells have certain gene or chromosome changes, can also affect your outlook.
- People now being diagnosed with brain or spinal cord tumors may have a better outlook than these numbers show. Treatments improve over time, and these numbers are based on people who were diagnosed and treated at least five years earlier.
- Remember, these survival rates can’t predict what will happen to any individual person. If you find these statistics are confusing and you have more questions, talk to your doctor to better understand your specific situation.
Prognostic Factors for brain and spinal cord cancers
For most types of cancer, the stage of the cancer — a measure of how far it has spread — is one of the most important factors in selecting treatment options and in determining a person’s outlook (prognosis).
But tumors of the brain and spinal cord differ in some important ways from cancers in other parts of the body. One of the main reasons other cancers are dangerous is that they can spread throughout the body. Tumors starting in the brain or spinal cord can spread to other parts of the central nervous system, but they almost never spread to other organs. These tumors are dangerous because they can interfere with essential brain functions.
Because tumors in the brain or spinal cord almost never spread to other parts of the body, they do not have a formal staging system like most other cancers. Some of the important factors that help determine a person’s outlook include:
- Their age
- Their functional level (whether the tumor is affecting normal brain functions and everyday activity)
- The type of tumor (such as astrocytoma, ependymoma, etc.)
- The grade of the tumor (how quickly the tumor is likely to grow, based on how the cells look under a microscope)
- If the tumor cells have certain gene mutations or other changes (For example, tumors with a mutation in the IDH1 or IDH2 gene, known as “IDH-mutant” tumors, tend to grow more slowly and have a better outlook than tumors without these mutations.)
- The location and size of the tumor
- How much of the tumor can be removed by surgery (if it can be done)
- Whether or not the tumor has spread through the cerebrospinal fluid to other parts of the brain or spinal cord
- Whether or not tumor cells have spread beyond the central nervous system
If you have a brain or spinal cord tumor, talk to your doctor to learn more about how these and other factors might affect your outlook and treatment options.
Types of brain cancer and spinal cord tumors in Adults
Tumors that start in the brain (primary brain tumors) are not the same as tumors that start in other organs, such as the lung or breast, and then spread to the brain (metastatic or secondary brain tumors). In adults, metastatic tumors to the brain are actually more common than primary brain tumors. These tumors are not treated the same way. For example, breast or lung cancers that spread to the brain are treated differently from tumors that start in the brain.
Unlike cancers that start in other parts of the body, tumors that start in the brain or spinal cord rarely spread to distant organs. Even so, brain or spinal cord tumors are rarely considered benign (non-cancerous). They can still cause damage by growing and spreading into nearby areas, where they can destroy normal brain tissue. And unless they are completely removed or destroyed, most brain or spinal cord tumors will continue to grow and eventually be life-threatening.
Primary brain tumors can start in almost any type of tissue or cell in the brain or spinal cord. Some tumors have mixed cell types. Tumors in different areas of the central nervous system (CNS) may be treated differently and have a different prognosis (outlook).
Brain and spinal cord tumor grades
Some brain and spinal cord tumors are more likely to grow into nearby tissues (and to grow quickly) than are other tumors. The World Health Organization (WHO) divides brain and spinal cord tumors into 4 grades (using Roman numerals I to IV), based largely on how the cells look under the microscope:
- Grade I: These tumors typically grow slowly and do not grow into (invade or infiltrate) nearby tissues. They can often be cured with surgery.
- Grade II: These tumors also tend to grow slowly but they can grow into nearby brain tissue. They are more likely to come back after surgery than grade I tumors. They are also more likely to become faster-growing tumors over time.
- Grade III: These tumors look more abnormal under the microscope. They can grow into nearby brain tissue and are more likely to need other treatments in addition to surgery.
- Grade IV: These are the fastest growing tumors. They generally require the most aggressive treatment.
Gliomas
Gliomas are brain tumor that start in glial cells. These are the supporting cells of the brain and the spinal cord. There are different types of gliomas.
There are 3 types of glial cells:
- Astrocytes – tumor that start in these cells are called astrocytoma or glioblastoma
- Oligodendrocytes – tumor that start in these cells are called oligodendrogliomas
- Ependymal cells – tumor that start in these cells are called ependymomas
About 3 out of 10 of all brain tumors are gliomas. Most fast-growing brain tumors are gliomas. The most common type is called astrocytoma.
Astrocytomas
Astrocytomas are tumors that start in glial cells called astrocytes. Astrocytes are star shaped cells. They support the nerve cells (neurones) in the brain. Astrocytomas are the most common type of brain tumors in both adults and children. About 2 out of 10 brain tumors are astrocytomas. Symptoms of astrocytoma depend on where the tumor is in the brain. Common symptoms include headaches and seizures (fits).
Most astrocytomas can spread widely throughout the brain and blend with the normal brain tissue, which can make them very hard to remove with surgery. Sometimes they spread along the cerebrospinal fluid (CSF) pathways. It is very rare for them to spread outside of the brain or spinal cord.
As with other types of brain tumors, astrocytomas are often grouped by grade (according to how quickly they are likely to grow).
- Low-grade (grade 1 or 2) astrocytomas tend to grow slowly. These include:
- Non-infiltrating (grade 1) astrocytomas, which do not usually grow into nearby tissues and tend to have a good prognosis. Examples include pilocytic astrocytomas and subependymal giant cell astrocytomas (SEGAs). These are more common in children than in adults.
- Grade 2 astrocytomas, such as diffuse astrocytomas and pleomorphic xanthoastrocytomas (PXAs). These tumors tend to be slow growing, but they can grow into nearby areas, which can make them harder to remove with surgery. These tumors can become more aggressive and faster growing over time.
- High-grade (grade 3 or 4) astrocytomas tend to grow quickly and spread into the surrounding normal brain tissue. These include:
- Anaplastic (grade 3) astrocytomas
- Glioblastomas (grade 4) are also called glioblastoma multiforme (GBM), which are the fastest growing. These tumors make up more than half of all gliomas and are the most common malignant brain tumors in adults.
Oligodendrogliomas
Oligodendrogliomas start in brain glial cells called oligodendrocytes. Oligodendroglioma is a rare type of brain tumor. Only about 1% to 2% of brain tumors are oligodendrogliomas. Oligodendrogliomas are more common in adults but can also start in young children. Symptoms of oligodendroglioma depend on where the tumor is in the brain. Common symptoms include headaches and seizures (fits).
Oligodendrogliomas are grade 2 tumors that tend to grow slowly, but most of them can grow into (infiltrate) nearby brain tissue and can’t be removed completely by surgery. Oligodendrogliomas sometimes spread along the cerebrospinal fluid (CSF) pathways but rarely spread outside the brain or spinal cord. As with astrocytomas, they can become more aggressive over time. Very aggressive (grade 3) forms of these tumors are known as anaplastic oligodendrogliomas.
Treatment depends on whether the oligodendroglioma is low grade (slow growing) or high grade (fast growing). It also depends on whether you have changes (mutations) in certain genes.
- Treatment for low grade oligodendroglioma
- Surgery. Surgery is usually the first treatment you have. The exact type of surgery you have depends on where the tumor is. A highly specialist doctor (neurosurgeon) removes as much of the tumor as possible. Oligodendrogliomas tend to grow into the brain tissue surrounding the tumor. This means that they don’t have a clear border between the tumor and the normal brain tissue. Not having a clear border can make it difficult to remove the tumor completely.
- Active monitoring. Your doctor might monitor you with regular MRI scans. This is called active monitoring. You may have active monitoring if you have a very slow growing oligodendroglioma.
- Radiation therapy. You might have radiotherapy after surgery. Radiotherapy uses high energy x-rays to destroy cancer cells. You may have radiotherapy after surgery if:
- you have a gene change called a 1p/19q co-deletion
- you are over 40 years old
- doctors can see tumor left behind after surgery
- Chemotherapy. You might have chemotherapy before or after radiotherapy. Chemotherapy uses cytotoxic drugs to destroy cancer cells. You usually have a combination of chemotherapy drugs called PCV. It includes the drugs:
- procarbazine
- lomustine (CCNU)
- vincristine
- Treatment for high grade oligodendroglioma
- Surgery. Surgery is the main treatment for high grade oligodendroglioma. A specialist doctor called neurosurgeon removes as much of the tumor as possible. This is called debulking. It is not usually possible to remove all of the tumor. Your doctor might recommend you have radiotherapy and chemotherapy afterwards.
- Radiation therapy. Radiotherapy uses high energy x-rays to destroy cancer cells. You might have radiotherapy after surgery if you are well overall and able to care for yourself.
- Chemotherapy uses cytotoxic drugs to destroy cancer cells. You might have a combination of chemotherapy drugs called PCV before or after radiotherapy. PCV includes the
- drugs:procarbazine
- lomustine (CCNU)
- vincristine
Ependymomas
Ependymomas start in ependymal cells, and typically grow in the ventricles or spinal cord in adults. Ependymomas can range from fairly low-grade (grade 2) tumors to higher grade (grade 3) tumors, which are called anaplastic ependymomas. Ependymomas are rare tumors. Only about 2% of brain tumors are ependymomas.
Ependymomas are more common in children and young adults but can also happen in older people. In older people, ependymomas tend to start in the lower part of the spinal cord.
Ependymomas are more likely to spread along the cerebrospinal fluid (CSF) pathways than other gliomas but do not spread outside the brain or spinal cord. Ependymomas may block the flow of CSF from the ventricles, causing the ventricles to become very large – a condition called hydrocephalus.
Unlike astrocytomas and oligodendrogliomas, ependymomas usually do not grow into normal brain tissue. As a result, some (but not all) ependymomas can be removed completely and cured by surgery. But because they can spread along ependymal surfaces and CSF pathways, treating them can sometimes be difficult. Spinal cord ependymomas have the greatest chance of being cured with surgery, but treatment can cause side effects related to nerve damage.
Brain stem glioma
Glioma in the brain stem is very rare. The brain stem is the lowest part of the brain, that connects with the spinal cord. It controls body functions that you don’t usually think about such as your breathing.
Brain stem gliomas are more common in children than in adults. For some children, they grow rapidly and spread to other parts of the brain. Brain stem gliomas in children are also called diffuse intrinsic pontine glioma.
For a brain stem glioma, you usually have surgery to remove part of the tumor. After surgery, you might have radiotherapy and chemotherapy, or chemotherapy on its own.
Meningiomas
Meningiomas begin in the meninges, the layers of tissue that surround the outer part of the brain and spinal cord. The meninges are membranes that support and protect the brain and spinal cord. A clear fluid called cerebrospinal fluid (CSF) travels in the spaces formed by the meninges. Meningiomas account for about 1 out of 3 primary brain and spinal cord tumors. They are the most common primary brain tumors in adults (although strictly speaking, they are not actually brain tumors). Meningiomas can start anywhere in the brain and spinal cord. But they are more common in the cerebrum and cerebellum.
The risk of these tumors increases with age. They occur about twice as often in women. Sometimes these tumors run in families, especially in those with neurofibromatosis, a syndrome in which people develop many benign tumors of nerve tissue.
Meningiomas are often assigned a grade, based on how the cells look under the microscope:
- Grade 1 (benign) meningiomas have cells that look the most like normal cells. These are the most common type of meningioma. Most of these tumors can be cured by surgery, but some grow very close to vital structures in the brain or cranial nerves and cannot be cured by surgery alone.
- Grade 2 (atypical or invasive) meningiomas usually have cells that look slightly more abnormal. They can grow directly into nearby brain tissue and bone and are more likely to come back (recur) after surgery.
- Grade 3 (anaplastic or malignant) meningiomas have cells that look the most abnormal. These are the least common type of meningiomas. They tend to grow quickly, can grow into nearby brain tissue and bone, and are the most likely to come back after treatment. Some may even spread to other parts of the body.
Symptoms of meningioma depend on where the tumor is in the brain. Symptoms include:
- seizures (fits)
- weakness
- loss of eyesight
- hearing loss
Meningiomas treatment depends on whether the meningioma is low grade (slow growing) or high grade (fast growing). It also depends on where the tumor is.
- Active monitoring. For a low grade meningioma, your doctor might monitor you with regular MRI scans. This is called active monitoring. You then have treatment if there are signs that the tumor is growing.
- Surgery. A highly specialized doctor (neurosurgeon) removes as much of the tumor as possible. Sometimes this is the only treatment you need. The exact type of surgery you have depends on where the tumor is. It isn’t always possible to completely remove the tumor during the operation. Especially if the tumor is growing around important nerves or blood vessels. You might have more surgery if doctors couldn’t remove all of the tumor. Or your doctor might suggest that you have radiotherapy.
- Radiation therapy. Radiotherapy uses high energy x-rays to kill tumor cells. You might have radiotherapy:
- to reduce the risk of the meningioma coming back, especially if the tumor is fast growing
- if the tumor is in an area that is too difficult to operate (for example, the base of the skull)
- if you can’t have surgery for any reason
- if the meningioma comes back
- You may have a type of radiotherapy called stereotactic radiotherapy. It targets high doses of radiotherapy to the tumor.
Medulloblastomas
Medulloblastomas develop from neuroectodermal cells (early forms of nerve cells) in the cerebellum. Medulloblastomas are part of a class of tumors called embryonal tumors that can also start in other parts of the central nervous system. Medulloblastomas are fast-growing (grade 4) tumors and often spread throughout the CSF pathways. Between 33 to 35 out of 100 children (33 – 35%) have medulloblastoma that has spread when they are first diagnosed, but they can be treated by surgery, radiation therapy, and chemotherapy.
Medulloblastomas occur much more often in children than in adults. Medulloblastoma is the second most common brain tumor in children. But it is the most common malignant (high grade) children’s brain tumor.
Medulloblastoma is most commonly diagnosed in children between 3 and 4 and between 8 and 10 years old. And it’s slightly more common in boys than girls.
Around 5 out of every 100 cases of medulloblastoma (around 5%) are linked with either:
- Familial Adenomatous Polyposis (FAP) – sometimes known as Turcot syndrome
- Nevoid basal cell carcinoma syndrome (NBCCS) – also known as Gorlin syndrome
Researchers are learning more about medulloblastoma all the time. At the moment, medulloblastoma is grouped by what the cells look like under the microscope. Your child’s doctors need a sample of the tumor to work out which type it is. This means they won’t be able to tell you straight away about what type or group it is.
There are 4 groups of medulloblastoma:
- Classical medulloblastoma – around 8 out of 10 children (around 80%) have classical medulloblastoma
- Anaplastic or large cell medulloblastoma
- Nodular or desmoplastic medulloblastoma – this type is most common in infants
- Medulloblastoma with extensive nodularity (MBEN)
Using new techniques, scientists can also look at the genes and proteins inside the medulloblastoma cells. This means doctors can now group medulloblastoma into 4 further subtypes. These are:
- Subtype 1 – wingless (WNT) medulloblastoma
- Subtype 2 – sonic hedgehog (SHH) medulloblastoma
- Subtype 3 – group 3 medulloblastoma
- Subtype 4 – group 4 medulloblastoma
Researchers are interested in learning more about these differences in medulloblastoma. They hope to make treatments targeted to these gene changes in the future.
Your child might have symptoms for a few weeks or months before they are diagnosed with medulloblastoma. Many of the symptoms are general and non specific. Some are similar to less serious childhood illnesses. Symptoms include:
- headaches in the morning
- feeling or being sick – being sick often makes the headaches feel better
- double vision
- finding it hard to sit or stand unsupported – your child might often fall backwards
- being more fractious or irritable – it might be taking longer than usual to get your young child to settle
- loss of appetite
- behavior changes – they might be interacting with you or their siblings less
A symptom that is sometimes found during a young infants routine development check up is an increasing head size (head circumference). Or the soft spot on top of the skull (fontanelle) might be swollen.
The main treatments for medulloblastoma are:
- surgery
- radiotherapy
- chemotherapy
Each child has their own treatment plan. Surgery is usually the first treatment your child will have. Less commonly your child might have chemotherapy first to shrink the tumour before surgery.
Your child’s specialist team decides on the best treatment for your child. Both you and your child will be involved in decisions about treatment and care.
Gangliogliomas
Gangliogliomas contain both neurons and glial cells. These tumors are very uncommon in adults. They are typically slow growing (grade I) tumors and can usually be cured by surgery alone or surgery combined with radiation therapy.
Schwannomas (neurilemmomas)
Schwannomas develop from Schwann cells also called the nerve sheath (the tissue that covers nerves), which surround and insulate cranial nerves and other nerves. Schwannomas make up about 8% of all central nervous system (CNS) tumors.
Schwannomas are almost always benign (grade 1) tumors. They can arise from any cranial nerve. When they form on the cranial nerve responsible for hearing and balance near the cerebellum, they are called vestibular schwannomas or acoustic neuromas. Neurofibromatosis Type 2 (NF2) is a rare inherited condition which can make you more likely to develop vestibular schwannomas in both ears.
Schwannomas can also start on spinal nerves after the point where they have left the spinal cord. When this happens, they can press on the spinal cord, causing weakness, sensory loss, and bowel and bladder problems.
When schwannomas are cancerous they are called malignant schwannomas. Malignant schwannomas are also called malignant peripheral nerve sheath tumors (MPNSTs) or neurofibrosarcomas. Malignant schwannomas can start anywhere in the body. But the most common area is the major nerve of the leg (the sciatic nerve).
Treatment of Schwannomas depends on where the tumor is in your body and whether it is non cancerous (benign) or cancerous (malignant). Your specialist may monitor you carefully at first rather than suggest treatment. They will see you regularly and monitor any symptoms you have. This is because the treatment can cause a lot of side effects.
- Surgery. The main treatment for schwannoma is surgery to remove the tumor. The type of surgery you have depends on where in the body the tumor is.
- Targeted radiotherapy. For small vestibular schwannomas, you may have stereotactic radiotherapy or radiosurgery. Both treatments target high doses of radiotherapy to the tumor. You might have targeted radiotherapy alone, or after surgery if the surgeon was unable to completely remove the tumor.
- Treatment for malignant schwannoma. You might also have radiotherapy and chemotherapy if you have a malignant tumor.
Craniopharyngiomas
Craniopharyngiomas are slow-growing (grade 1) tumors start above the pituitary gland but below the brain itself. Craniopharyngiomas may press on the pituitary gland and the hypothalamus, causing hormone problems. Because they start very close to the optic nerves, they can also cause vision problems. Their tendency to stick to these important structures can make them hard to remove completely without damaging vision or hormone balance. Craniopharyngiomas are more common in children, but they are sometimes seen in adults.
Other tumors that can start in or near the brain
Chordomas
Chordomas are rare tumors start in the bone at the base of the skull or at the lower end of the spine. Chordomas don’t start in the central nervous system, but they can injure the nearby brain or spinal cord by pressing on it.
These tumors are treated with surgery if possible, often followed by radiation therapy, but they tend to come back in the same area after treatment, causing more damage. Chordomas usually do not spread to other organs.
Non-Hodgkin lymphomas
Lymphomas are cancers that start in white blood cells called lymphocytes (one of the main cell types of the immune system). Most lymphomas start in other parts of the body, but some start in the CNS, and are called primary CNS lymphomas.
Non-Hodgkin lymphomas (NHL) are more common in people with immune system problems, such as those infected with HIV, the virus that causes AIDS. Because of new treatments for AIDS, primary CNS lymphomas have become less common in recent years. They account for about 2% of primary brain tumors.
Non-Hodgkin lymphomas (NHL) often grow quickly and can be hard to treat. Recent advances in chemotherapy, however, have improved the outlook for people with these cancers.
Pituitary tumors
Pituitary tumors are tumors that start in the pituitary gland and they are almost always benign (non-cancerous). But they can still cause problems if they grow large enough to press on nearby structures or if they make too much of any kind of hormone.
Hemangioblastomas
Hemangioblastomas are rare benign brain tumors that start in the cells that line the blood vessels in the brain, spinal cord and brain stem. Hemangioblastomas usually grow slowly over some years. Most hemangioblastomas start in the back of the brain (cerebellum).
Hemangioblastomas are rare tumors. About 2 out of every 100 brain tumors (2%) diagnosed are hemangioblastomas.
Hemangioblastomas don’t usually spread to other parts of the brain. The symptoms you have depend on where the tumor is in the brain. Symptoms might include:
- problems with walking, balance, speech and coordination
- a build up of brain fluid (cerebrospinal fluid) which can cause headaches and feeling sick
Some hemangioblastomas happen because of a rare inherited syndrome called von Hippel-Lindau syndrome. People with this syndrome have a higher risk of developing different types of tumors, including hemangioblastomas.
Hemangioblastomas treatment depends on:
- the size of the tumor
- the symptoms you have
- your age
- your quality of life
Treatment might be monitoring, surgery or radiotherapy. The team caring for you will talk to you about your treatment.
- Active monitoring or watchful waiting. You might not need treatment straight away if you have a very small hemangioblastoma and you don’t have symptoms. If this is the case, your doctors may recommend monitoring the tumor with regular MRI scans.
- Surgery. Surgery is the main treatment for hemangioblastoma. A brain specialist surgeon (neurosurgeon) removes all the tumor or just a part. This depends on where the tumor is. You might have side effects after the operation. The side effects include:
- bleeding in the brain
- infection in the membranes that surround the brain (meningitis)
- Radiotherapy. You might have radiotherapy if:
- you can’t have surgery for any reason
- your hemangioblastoma has come back after surgery
- doctors couldn’t remove all the tumor during the operation
- You might have a type of radiotherapy called stereotactic radiotherapy or radiosurgery. Both treatments target high doses of radiotherapy to the tumor.
What causes brain cancer in Adults
The cause of most brain and spinal cord tumors is not fully understood, and there are very few well-established risk factors. But researchers have found some of the changes that occur in normal brain cells that may lead them to form brain tumors.
Normal human cells grow and function based mainly on the information contained in each cell’s DNA. Brain and spinal cord tumors, like other tumors, are caused by changes in the DNA inside cells. DNA is the chemical that makes up our genes, which control how our cells function. We usually look like our parents because they are the source of our DNA. But DNA affects more than how we look.
Some genes control when our cells grow, divide into new cells, and die:
- Certain genes that help cells grow, divide, and stay alive are called oncogenes.
- Genes that help keep cell division under control, or make cells die at the right time, are called tumor suppressor genes.
Cancers can be caused by DNA changes that turn on oncogenes or turn off tumor suppressor genes. These gene changes can be inherited from a parent, but more often they happen during a person’s lifetime.
Inherited gene changes
Researchers have found gene changes that cause some rare inherited syndromes (like neurofibromatosis, tuberous sclerosis, Li-Fraumeni syndrome, and von Hippel-Lindau syndrome) and increase the risk of developing some brain and spinal cord tumors. For example, the Li-Fraumeni syndrome is caused by changes in the TP53 tumor suppressor gene. Normally, this gene prevents cells with damaged DNA from growing. Changes in this gene increase the risk of developing brain tumors (particularly gliomas), as well as some other cancers.
Gene changes acquired during a person’s lifetime
Most often, it’s not known why people without inherited syndromes develop brain or spinal cord tumors. Most exposures that cause cancer somehow damage DNA. For example, tobacco smoke is a risk factor for lung cancer and several other cancers because it contains chemicals that can damage the genes inside cells. The brain is relatively protected from tobacco smoke and other cancer-causing chemicals that we might breathe in or eat, so these factors are not likely to play a major role in these cancers.
Several different gene changes usually occur in normal cells before they become cancerous. There are many kinds of brain tumors, each of which may have different sets of gene changes. A number of gene changes have been found in different brain tumor types, but there are probably many others that have not yet been found.
Researchers now understand some of the gene changes that occur in different types of brain tumors, but it’s still not clear what causes most of these changes. Some gene changes might be inherited, but most brain and spinal cord tumors are not the result of known inherited syndromes. Other than radiation, no known lifestyle-related or environmental factors are clearly linked to brain tumors. Most gene changes are probably just random events that sometimes happen inside a cell, without having an outside cause.
Risk Factors for Brain and Spinal Cord Tumors in Adults
A risk factor is anything that affects your chance of getting a disease such as a brain or spinal cord tumor. Different types of cancer have different risk factors. Some risk factors, like smoking, you can change. Others, like your age or family history, can’t be changed.
But having a risk factor, or even several, does not always mean that a person will get the disease, and many people get tumors without having any known risk factors.
Most brain tumors are not linked with any known risk factors and have no obvious cause. But there are a few factors that can raise the risk of brain tumors.
Radiation exposure
The best known environmental risk factor for brain tumors is radiation exposure, most often from radiation therapy to treat some other condition. For example, before the risks of radiation were known, children with ringworm of the scalp (a fungal infection) were sometimes treated with low-dose radiation therapy, which was later found to increase their risk of brain tumors as they got older.
Today, most radiation-induced brain tumors are caused by radiation to the head given to treat other cancers. They occur most often in people who received radiation to the brain as children as part of their treatment for leukemia. These brain tumors usually develop around 10 to 15 years after the radiation.
Radiation-induced tumors are still fairly rare, but because of the increased risk (as well as the other side effects), radiation therapy is only given to the head after carefully weighing the possible benefits and risks. For most patients with other cancers involving the brain or head, the benefits of radiation therapy far outweigh the risk of developing a brain tumor years later.
The possible risk from exposure to imaging tests that use radiation, such as x-rays or CT scans, is not known for sure. These tests use much lower levels of radiation than those used in radiation treatments, so if there is any increase in risk, it is likely to be very small. But to be safe, most doctors recommend that people (especially children and pregnant women) not get these tests unless they are clearly needed.
Family history
Most people with brain tumors do not have a family history of the disease, but in rare cases brain and spinal cord cancers run in families. In general, patients with familial cancer syndromes tend to have many tumors that first occur when they are young. Some of these families have well-defined disorders, such as:
Neurofibromatosis type 1 (NF1)
This genetic disorder, also known as von Recklinghausen disease, is the most common syndrome linked to brain or spinal cord tumors. People with this condition have higher risks of schwannomas, meningiomas, and certain types of gliomas, as well as neurofibromas (benign tumors of peripheral nerves). Changes in the NF1 gene cause this disorder. These changes are inherited from a parent in about half of all cases. In the other half, the NF1 gene changes occur before birth in people whose parents did not have this condition.
Neurofibromatosis type 2 (NF2)
This condition, which is much less common than NF1, is associated with vestibular schwannomas (acoustic neuromas), which almost always occur on both sides of the head. It is also linked with an increased risk of meningiomas or spinal cord ependymomas. Changes in the NF2 gene are usually responsible for neurofibromatosis type 2. Like NF1, the gene changes are inherited in about half of cases. In the other half, they occur before birth in children without a family history.
Tuberous sclerosis
People with this condition may have subependymal giant cell astrocytomas (SEGAs), which are low-grade astrocytomas that develop beneath the ependymal cells of the ventricles. They may also have other benign tumors of the brain, skin, heart, kidneys, and other organs. This condition is caused by changes in either the TSC1 or the TSC2 gene. These gene changes can be inherited from a parent, but most often they develop in people without a family history.
Von Hippel-Lindau disease
Von Hippel-Lindau syndrome (VHL) also called VHL disease, VHL syndrome or von Hippel-Lindau disease, is a rare, inherited disorder that causes tumors and cysts to grow in certain parts of the body, including the brain, spinal cord, eyes, inner ear, adrenal glands, pancreas, kidney, and reproductive tract. The tumors are usually benign (not cancer), but some may be malignant (cancer). Patients with von Hippel-Lindau syndrome have an increased risk of certain types of cancer, especially kidney cancer and pancreatic cancer. The signs and symptoms of von Hippel-Lindau syndrome usually do not appear until young adulthood. Von Hippel-Lindau syndrome is caused by a mutation (change) in the VHL gene. Most often the gene changes are inherited, but in some cases the changes happen before birth in people whose parents don’t have them.
Li-Fraumeni syndrome
People with this condition are at higher risk for developing gliomas, along with breast cancer, soft tissue sarcomas, leukemia, adrenal gland cancer, and certain other types of cancer. It is caused by changes in the TP53 gene.
Other syndromes
Other inherited conditions are also linked with increased risks of certain types of brain and spinal cord tumors, including:
- Gorlin syndrome also called basal cell nevus syndrome, BCNS, NBCCS or nevoid basal cell carcinoma syndrome. Gorlin syndrome is a rare, inherited disorder that affects many organs and tissues in the body. People with Gorlin syndrome have a very high risk of developing basal cell skin cancer during adolescence or early adulthood. They are also at risk of developing medulloblastoma (a type of brain cancer) and other types of cancer. Gorlin syndrome may also cause benign (not cancer) tumors in the jaw, heart, or ovaries. Other signs and symptoms include a large head and unusual facial features; small pits in the skin on the hands and feet; abnormalities of the spine, ribs, or skull; eye problems; and developmental problems. Gorlin syndrome is caused by a mutation (change) in the PTCH1 gene.
- Turcot syndrome. Turcot syndrome also known as brain tumor-polyposis syndrome, describes people who have many colon polyps and an increased risk of colorectal cancer, as well as an increased risk for certain types of brain tumors. But this syndrome is actually made up of two different hereditary conditions:
- When linked with familial adenomatous polyposis (FAP), there is a mutation in the APC gene. In people with this gene mutation, brain tumors are typically medulloblastomas.
- When linked with Lynch syndrome (also known as hereditary non-polyposis colorectal cancer or HNPCC), the mutation is in one of the mismatch repair genes, such as MLH1 or PMS2. In people with one of these gene mutations, brain tumors are usually gliomas.
- Cowden syndrome also called Cowden disease or multiple hamartoma syndrome, is a rare inherited disorder marked by the presence of many benign (not cancer) growths called hamartomas and an increased risk of developing certain cancers. Hamartomas form in different parts of the body, especially the skin, mouth, and gastrointestinal tract. Other benign tumors may also occur in the thyroid, breast, uterus, soft tissue, and brain. Other signs and symptoms include a larger-than-average head, abnormal skin changes, blood vessel problems, autism spectrum disorder, and learning and developmental delays. People with Cowden syndrome have an increased risk of developing certain types of cancer, including melanoma and cancers of the breast, thyroid, endometrium, kidney, colon, and rectum. Cowden syndrome is usually caused by mutations (changes) in the PTEN gene.
- Turner syndrome. Turner syndrome (45X) is a genetic condition that occurs in females who have a missing or abnormal X chromosome (sex chromosome). Turner syndrome is marked by a shorter-than-average height, ovaries that do not function normally, and infertility. Other signs and symptoms may include extra folds of skin on the neck, a low hairline at the back of the neck, swelling of the hands and feet, and heart, kidney, bone, and hearing problems. Turner syndrome is present at birth but its signs and symptoms may occur slowly over time. Having Turner syndrome increases the risk of germ cell tumors in the ovaries.
Some families may have genetic disorders that are not well recognized or that may even be unique to a particular family.
Having a weakened immune system
People with weakened immune systems have an increased risk of developing lymphomas of the brain or spinal cord (known as primary CNS lymphomas). Lymphomas are cancers of lymphocytes, a type of white blood cell that fights disease. Primary CNS lymphoma is less common than lymphoma that develops outside the brain.
A weakened immune system can be congenital (present at birth), or it can be caused by treatments for other cancers, treatment to prevent rejection of transplanted organs, or diseases such as acquired immunodeficiency syndrome (AIDS).
Factors with uncertain, controversial, or unproven effects on brain tumor risk
Cell phone use
Cell phones give off radiofrequency (RF) rays, a form of energy on the electromagnetic spectrum between FM radio waves and those used in microwave ovens, radar, and satellite stations. Cell phones do not give off ionizing radiation, the type that can cause cancer by damaging the DNA inside cells. Still, there have been concerns that the phones, whose antennae are built-in and therefore are placed close to the head when being used, might somehow raise the risk of brain tumors.
Some studies have suggested a possible increased risk of brain tumors or of vestibular schwannomas (acoustic neuromas) with cell phone use, but most of the larger studies done so far have not found an increased risk, either overall or among specific types of tumors. Still, there are very few studies of long-term use (10 years or more), and cell phones haven’t been around long enough to determine the possible risks of lifetime use. The same is true of any possible higher risks in children, who are increasingly using cell phones. Cell phone technology also continues to change, and it’s not clear how this might affect any risk.
These risks are being studied, but it will probably be many years before firm conclusions can be made. In the meantime, for people concerned about the possible risks, there are ways to lower your exposure, such as using the phone’s speaker or an earpiece to move the phone itself away from the head.
Other factors
Other environmental factors such as exposure to vinyl chloride (a chemical used to manufacture plastics), petroleum products, and certain other chemicals have been linked with an increased risk of brain tumors in some studies but not in others.
Exposure to aspartame (a sugar substitute), exposure to electromagnetic fields from power lines and transformers, and infection with certain viruses have been suggested as possible risk factors, but most researchers agree that there is no convincing evidence to link these factors to brain tumors. Research on these and other possible risk factors continues.
Signs and Symptoms of Adult Brain and Spinal Cord Tumors
The signs and symptoms of brain tumors differ from person to person. Some people may have symptoms that suggest there is a brain tumor, others have no obvious symptoms. Signs and symptoms depend on where the tumor forms in the brain, what the affected part of the brain controls, and the size of the tumor.
Commonly, people with brain tumor experience long-term headaches, seizures or convulsions, difficulty thinking and speaking/finding words, personality changes, tingling or stiffness in one side of the body, a loss of balance, vision changes, nausea, and/or disorientation.
Consult with your doctor if you have any of the following symptoms:
- Headaches that are new or worsening, especially in the morning or when lying down (these are often the first symptom of a brain tumor)
- Frequent nausea or vomiting
- Dizziness, loss of balance and coordination or room spinning
- Vision, hearing, and speech problems
- Difficulty with balance and trouble walking
- Weakness on one side or part of the body
- Unusual sleepiness or change in activity level
- Changes in personality or mood, such as anger, irritability or emotional withdrawal
- Changes to how you think
- Inability to focus or vision loss
- Confusion
- Seizures
- Loss of consciousness
- Impaired sense of smell or taste
- Drowsiness and fatigue
- Endocrine dysfunction (hormone/gland changes)
You may notice other signs, like memory problems or difficulty speaking or remembering words.
Having one or more of the symptoms above does not necessarily mean that you have a brain or spinal cord tumor. All of these symptoms can have other causes. Still, if you have any of these symptoms, especially if they don’t go away or get worse over time, see your doctor so the cause can be found and treated, if needed.
General symptoms
Tumors in any part of the brain might increase the pressure inside the skull (known as intracranial pressure). This can be caused by growth of the tumor itself, swelling in the brain, or blockage of the flow of cerebrospinal fluid. Increased pressure can lead to general symptoms such as:
- Headache
- Nausea
- Vomiting
- Blurred vision
- Balance problems
- Personality or behavior changes
- Seizures
- Drowsiness or even coma
Headaches that tend to get worse over time are a common symptom of brain tumors, occurring in about half of patients. (Of course, most headaches are not caused by tumors.)
As many as half of people with brain tumors will have seizures at some point. The type of seizure may depend on where the tumor is. Sometimes this is the first sign of a brain tumor, but fewer than 1 in 10 first seizures are caused by brain tumors.
Symptoms of tumors in different parts of the central nervous system
Brain and spinal cord tumors often cause problems with the specific functions of the region they develop in. But these symptoms can be caused by any disease in that particular location — they do not always mean a person has a brain or spinal cord tumor.
- Tumors in the parts of the cerebrum (the large, outer part of the brain) that control movement or sensation can cause weakness or numbness of part of the body, often on just one side.
- Tumors in or near the parts of the cerebrum responsible for language can cause problems with speech or even understanding words.
- Tumors in the front part of the cerebrum can sometimes affect thinking, personality, and language.
- If the tumor is in the cerebellum (the lower, back part of the brain that controls coordination), a person might have trouble walking, trouble with precise movements of hands, arms, feet, and legs, problems swallowing or synchronizing eye movements, and changes in speech rhythm.
- Tumors in the back part of the cerebrum, or around the pituitary gland, the optic nerve, or certain other cranial nerves can cause vision problems.
- Tumors in or near other cranial nerves might lead to hearing loss (in one or both ears), balance problems, weakness of some facial muscles, facial numbness or pain, or trouble swallowing.
- Spinal cord tumors can cause numbness, weakness, or lack of coordination in the arms and/or legs (usually on both sides of the body), as well as bladder or bowel problems.
The brain also controls functions of some other organs, including hormone production, so brain tumors can also cause many other symptoms not listed here.
Having one or more of the symptoms above does not necessarily mean that you have a brain or spinal cord tumor. All of these symptoms can have other causes. Still, if you have any of these symptoms, especially if they don’t go away or get worse over time, see your doctor so the cause can be found and treated, if needed.
How is Brain and Spinal Cord Cancers Diagnosed – Adults
Brain and spinal cord tumors are usually found because of signs or symptoms a person is having. If a tumor is suspected, tests will be needed to confirm the diagnosis.
Medical history and physical exam
If signs or symptoms suggest you might have a brain or spinal cord tumor, your doctor will get a complete medical history, focusing on your symptoms and when they began. The doctor will also do a neurologic exam to check your brain and spinal cord function. This exam tests reflexes, muscle strength, vision, eye and mouth movement, coordination, balance, alertness, and other functions.
If the results of the exam are abnormal, your doctor may refer you to a neurologist (a doctor who specializes in medical treatment of nervous system diseases) or a neurosurgeon (a doctor who specializes in surgical treatment of nervous system diseases), who will do a more detailed neurologic exam or other tests.
Imaging tests
Your doctor may order one or more imaging tests. These tests use x-rays, strong magnets, or radioactive substances to create pictures of the brain and spinal cord. The pictures may be looked at by doctors specializing in this field (neurosurgeons, neurologists, and neuroradiologists) as well as by your primary doctor.
Magnetic resonance imaging (MRI) and computed tomography (CT) scans are used most often to look for brain diseases. These scans will show a brain tumor, if one is present, in almost all cases. Doctors can often also get an idea about what type of tumor it might be, based on how it looks on the scan and where it is in the brain.
Magnetic resonance imaging (MRI) scan
MRI scans are very good for looking at the brain and spinal cord and are considered the best way to look for tumors in these areas. The images they provide are usually more detailed than those from CT scans (described below). But they do not image the bones of the skull as well as CT scans and therefore may not show the effects of tumors on the skull.
MRI scans use radio waves and strong magnets (instead of x-rays) to make pictures. A contrast material called gadolinium may be injected into a vein before the scan to help see details better.
Special types of MRI can be useful in some situations:
Magnetic resonance angiography (MRA) and magnetic resonance venography (MRV): These special types of MRI may be used to look at the blood vessels in the brain. This can be very useful before surgery to help the surgeon plan an operation.
Magnetic resonance spectroscopy (MRS): This test can be done as part of an MRI. It measures biochemical changes in an area of the brain (displayed in graph-like results called spectra, although basic images can also be created). By comparing the results for a tumor to that of normal brain tissue, it can sometimes help determine the type of tumor (or how quickly it is likely to grow), although a biopsy of the tumor is often still needed to get an accurate diagnosis. MRS can also be used after treatment to help determine if an area that still looks abnormal on another test is remaining tumor or if it is more likely to be scar tissue.
Magnetic resonance perfusion: For this test, also known as perfusion MRI, a contrast dye is injected quickly into a vein. A special type of MR image is then obtained to look at the amount of blood going through different parts of the brain and tumor. Tumors often have a bigger blood supply than normal areas of the brain. A faster growing tumor may need more blood.
Perfusion MRI can give doctors an idea of the best place to take a biopsy. It can also be used after treatment to help determine if an area that still looks abnormal is remaining tumor or if it is more likely to be scar tissue.
Functional MRI (fMRI): This test looks for tiny blood flow changes in an active part of the brain. It can be used to determine what part of the brain handles a function such as speech, thought, sensation, or movement. Doctors can use this to help determine which parts of the brain to avoid when planning surgery or radiation therapy.
This test is similar to a standard MRI, except that you will be asked to do specific tasks (such as answering simple questions or moving your fingers) while the scans are being done.
Computed tomography (CT) scan
A CT scan uses x-rays to make detailed cross-sectional images of your brain and spinal cord (or other parts of the body). Unlike a regular x-ray, a CT scan creates detailed images of the soft tissues in the body.
CT scans are not used as often as MRI scans when looking at brain or spinal cord tumors, but they can be useful in some cases. They may be used if MRI is not an option (such as in people who are very overweight or people who have a fear of enclosed spaces).CT scans also show greater detail of the bone structures near the tumor.
As with MRI, you may get an injection of a contrast dye through an IV (intravenous) line before the scan (although a different dye is used for CT scans). This helps better outline any tumors that are present.
CT angiography (CTA): For this test, you are injected with a contrast material through an IV line while you are in the CT scanner. The scan creates detailed images of the blood vessels in the brain, which can help doctors plan surgery. CT angiography can provide better details of the blood vessels in and around a tumor than MR angiography in some cases.
Positron emission tomography (PET) scan
For a PET scan, you are injected with a slightly radioactive substance (usually a type of sugar known as FDG) which collects mainly in tumor cells. A special camera is then used to create a picture of areas of radioactivity in the body. The picture is not as detailed as a CT or MRI scan, but it can provide helpful information about whether abnormal areas seen on other tests (such as MRIs) are likely to be tumors or not. This test is more likely to be helpful for fast-growing (high-grade tumors) than for slower-growing tumors.
This test is also useful after treatment to help determine if an area that still looks abnormal on an MRI scan is remaining tumor or if it is more likely to be scar tissue. Remaining tumor might show up on the PET scan, while scar tissue will not.
Chest x-ray
A chest x-ray might be done to look for tumors in the lungs if a tumor is found in the brain. This is because in adults, most tumors in the brain actually have started in another organ (most often the lung) and then spread to the brain. This test can be done in a doctor’s office, in an outpatient radiology center, or in a hospital.
Brain or spinal cord tumor biopsy
Imaging tests such as MRI and CT scans may show an abnormal area that is likely to be a brain or spinal cord tumor. But often these scans can’t tell exactly what type of tumor it is. This can only be done by removing some of the tumor tissue in a procedure called a biopsy. A biopsy may be done as a procedure on its own, or it may be part of surgery to treat the tumor.
Sometimes, a tumor may look so much like an astrocytoma on an MRI scan that a biopsy is not needed, especially if the tumor is in a part of the brain that would make it hard to biopsy (such as the brain stem). In rare cases a PET scan or MR spectroscopy may give enough information so that a biopsy is not needed.
The 2 main types of biopsies for brain tumors are:
Stereotactic (needle) biopsy
This type of biopsy may be used if, based on imaging tests, the risks of surgery to remove the tumor might be too high (such as with some tumors in vital areas, those deep within the brain, or other tumors that probably can’t be treated with surgery) but a sample is still needed to make a diagnosis.
The patient may be asleep (under general anesthesia) or awake during the biopsy. If the patient is awake, the neurosurgeon injects a local anesthetic into areas of skin above the skull to numb them. (The skull and brain do not feel pain.)
The biopsy itself can be done in two main ways:
- One approach is to get an MRI or CT, and then use either markers (each about the size of a nickel) placed on different parts of the scalp, or facial and scalp contours, to create a map of the inside of the head. An incision (cut) is then made in the scalp, and a small hole is drilled in the skull. An image-guidance system is then used to direct a hollow needle into the tumor to remove small pieces of tissue.
- In an approach that’s being used less often, a rigid frame is attached to the head. An MRI or CT scan is often used along with the frame to help the neurosurgeon guide a hollow needle into the tumor. This also requires an incision in the scalp and a small hole in the skull.
The removed tissue is sent to a pathologist (a doctor specializing in diagnosis of diseases by lab tests). Sometimes it might need to be looked at by a neuropathologist, a pathologist who specializes in nervous system diseases. The pathologist looks at it under a microscope (and might do other lab tests) to determine if the tumor is benign or malignant (cancerous) and exactly what type of tumor it is. This is very important in determining a person’s prognosis (outlook) and the best course of treatment. A preliminary diagnosis might be available the same day, although it often takes at least a few days to get a final diagnosis.
Surgical or open biopsy (craniotomy)
If imaging tests show the tumor can likely be treated with surgery, the neurosurgeon may not do a needle biopsy. Instead, he or she may do an operation called a craniotomy to remove all or most of the tumor. (Removing most of the tumor is known as debulking.)
For a preliminary diagnosis, small samples of the tumor are looked at right away by the pathologist while the patient is still in the operating room. This can help guide treatment, including whether further surgery should be done at that time. A final diagnosis is made within a few days in most cases.
Lab tests of biopsy specimens
Finding out which type of tumor someone has is very important in helping to determine their outlook (prognosis) and treatment options. But in recent years, doctors have found that changes in certain genes, chromosomes, or proteins within the cancer cells can also be important. Some tumors are now tested for these types of changes. For example:
- Gliomas that are found to have IDH1 or IDH2 gene mutations tend to have a better outlook than gliomas without these gene mutations.
- Oligodendrogliomas whose cells are missing parts of certain chromosomes (known as a 1p19q co-deletion) are much more likely to be helped by chemotherapy than tumors that do not.
- In high-grade gliomas, MGMT promoter methylation is linked with better outcomes and a higher likelihood of responding to chemotherapy, so it can sometimes be used to help guide treatment.
Lumbar puncture (spinal tap)
This test is used mainly to look for cancer cells in the cerebrospinal fluid (CSF), the liquid that surrounds the brain and spinal cord. For this test, you lie on your side on a bed or exam table with your knees up near your chest. The doctor first numbs an area in the lower part of the back near the spine. A small, hollow needle is then placed between the bones of the spine to withdraw some of the fluid.
This fluid is sent to a lab to be looked at for cancer cells. Other tests may be done on the fluid as well.
Lumbar punctures are usually very safe, but doctors have to make sure the test does not result in a large drop in pressure in the fluid, which could possibly cause serious problems. For this reason, imaging tests such as CT or MRI scans are done first.
Lumbar punctures usually aren’t done to diagnose brain tumors, but they may be done to help determine the extent of a tumor by looking for cancer cells in the CSF. They are often used if a tumor has already been diagnosed as a type that can commonly spread through the CSF, such as an ependymoma. Lumbar punctures are particularly important in people with suspected brain lymphomas because often the lymphoma cells spread into the CSF.
Blood and urine tests
These lab tests rarely are part of the actual diagnosis of brain and spinal cord tumors, but they may be done to check how well the liver, kidneys, and some other organs are working. This is especially important before any planned surgery. If you are getting chemotherapy, blood tests will be done routinely to check blood counts and to see if the treatment is affecting other parts of your body.
Brain cancer treatment in Adults
If you have a brain tumor, your treatment will depend on:
- the type of tumor
- where it is in your brain
- how big it is and how far it’s spread
- how abnormal the cells are
- your overall health and fitness
Several types of treatment can be used to treat brain and spinal cord tumors, including:
- steroids
- medicines to help with symptoms
- surgery
- radiotherapy
- chemotherapy
- targeted drug therapy
- alternating electric field therapy
Treatment is based on the type of tumor and other factors, and often more than one type of treatment is used. Typically a team of doctors plan each person’s treatment individually to give them the best chance of treating the tumor while limiting the side effects as much as possible.
After being diagnosed with a brain tumor, steroids may be prescribed to help reduce swelling around the tumor. Other medicines can be used to help with other symptoms of brain tumors, such as anti-epileptic medicines for seizures and painkillers for headaches.
Surgery is often used to remove brain tumors. The aim is to remove as much abnormal tissue as safely as possible.
It’s not always possible to remove all of a tumor, so further treatment with radiotherapy or chemotherapy may be needed to treat any abnormal cells left behind.
Sometimes there’s a small chance the tumor could return, so you may need regular follow-up appointments to monitor this.
Which doctors treat brain and spinal cord tumors?
Brain and spinal cord tumors can often be hard to treat and require care from a team of different types of doctors. This team is often led by a neurosurgeon, a doctor who operates on brain and nervous system tumors. Other doctors on the team might include:
- Neurologist: a doctor who diagnoses brain and nervous system diseases and treats them with medicines
- Radiation oncologist: a doctor who uses radiation to treat cancer
- Medical oncologist: a doctor who uses chemotherapy and other medicines to treat cancers
- Endocrinologist: a doctor who treats diseases in glands that secrete hormones
You might have many other specialists on your treatment team as well, including physician assistants, nurse practitioners, nurses, psychologists, social workers, rehabilitation specialists, and other health professionals. See Health Professionals Associated With Cancer Care for more on this.
Making treatment decisions
It’s important to discuss all of your treatment options, including their goals and possible side effects, with your treatment team to help make the decision that best fits your needs. Some important things to consider include:
- Your age and overall health
- The type and location of your tumor
- The likelihood that treatment will cure your tumor (or help in some other way)
- Your feelings about the possible side effects from treatment
You may feel that you need to decide quickly, but it’s important to give yourself time to think about the information you have learned. It’s also very important to ask questions if there is anything you’re not sure about.
Getting a second opinion
If time permits, getting a second opinion from a doctor experienced with your type of tumor is often a good idea. This can give you more information and help you feel more confident about the treatment plan you choose. If you aren’t sure where to go for a second opinion, ask your doctor for help.
Thinking about taking part in a clinical trial
Clinical trials are carefully controlled research studies that are done to get a closer look at promising new treatments or procedures. Clinical trials are one way to get state-of-the art cancer treatment. Sometimes they may be the only way to get access to newer treatments. They are also the best way for doctors to learn better methods to treat brain and spinal cord tumors. Still, they are not right for everyone.
If you would like to learn more about clinical trials that might be right for you, start by asking your doctor if your clinic or hospital conducts clinical trials.
Considering complementary and alternative methods
You may hear about alternative or complementary methods that your doctor hasn’t mentioned to treat your cancer or relieve symptoms. These methods can include vitamins, herbs, and special diets, or other methods such as acupuncture or massage, to name a few.
Complementary methods refer to treatments that are used along with your regular medical care. Alternative treatments are used instead of a doctor’s medical treatment. Although some of these methods might be helpful in relieving symptoms or helping you feel better, many have not been proven to work. Some might even be dangerous.
Be sure to talk to your treatment team about any method you are thinking about using. They can help you learn what is known (or not known) about the method, which can help you make an informed decision.
Help getting through treatment
Your treatment team will be your first source of information and support, but there are other resources for help when you need it. Hospital- or clinic-based support services are an important part of your care. These might include nursing or social work services, financial aid, nutritional advice, rehab, or spiritual help.
Choosing to stop treatment or choosing no treatment at all
For some people, when treatments have been tried and are no longer controlling the tumor, it could be time to weigh the benefits and risks of continuing to try new treatments. Whether or not you continue treatment, there are still things you can do to help maintain or improve your quality of life.
Some people, especially if the tumor is advanced, might not want to be treated at all. There are many reasons you might decide not to get treatment, but it’s important to talk this through with your doctors before you make this decision. Remember that even if you choose not to treat the tumor, you can still get supportive care to help with pain or other symptoms.
Corticosteroids
Corticosteroid drugs such as dexamethasone (Decadron) are often given to reduce swelling around brain tumors. This may help relieve headaches and other symptoms.
Medicines to help with symptoms
Some drugs commonly used in people with brain or spinal cord tumors do not treat the tumors directly, but they may help lessen symptoms caused by the tumor or its treatment.
Anti-seizure drugs (anticonvulsants)
Drugs may also be given to lower the chance of seizures in people with brain tumors. Different anti-seizure drugs can be used. Because many of these drugs can affect how other drugs such as chemotherapy work in the body, they are not usually given unless the tumor has caused seizures.
Hormones
The pituitary gland helps control the levels of many different hormones in the body. If the pituitary gland is damaged by the tumor itself or by tumor treatments (such as surgery or radiation therapy), you may need to take pituitary hormones or other hormones to replace those missing.
Brain tumor surgery
Surgery on brain and spinal cord tumors may be done to:
- Get a biopsy sample to determine the type of tumor
- Remove the tumor (or as much of it as possible)
- Help prevent or treat symptoms or possible complications from the tumor
Before surgery, be sure you understand the goal of the surgery, as well as its possible benefits and risks.
Surgery on the brain or spinal cord is a serious operation, and surgeons are very careful to try to limit any problems either during or after surgery. Complications during or after any type of surgery can include bleeding, infections, or reactions to anesthesia, although these are not common.
A major concern after surgery is swelling in the brain. Drugs called corticosteroids are typically given before and for several days after surgery to help lessen this risk.
Seizures are also possible after brain surgery. Anti-seizure medicines can help lower this risk, although they might not prevent them completely.
One of the biggest concerns when removing brain tumors is the possible loss of brain function afterward, which is why doctors are very careful to remove only as much tissue as is safely possible. If problems do arise, it could be right after surgery, or it could be days or even weeks later, so close monitoring for any changes is very important.
Surgery to remove the tumor
Most often, the first step in brain or spinal cord tumor treatment is for the neurosurgeon to remove as much of the tumor as is safe without affecting normal brain function. Surgery alone or combined with radiation therapy may control or cure many types of tumors, including some low-grade astrocytomas, ependymomas, craniopharyngiomas, gangliogliomas, and meningiomas.
Tumors that tend to spread widely into nearby brain or spinal cord tissue, such as anaplastic astrocytomas or glioblastomas, typically cannot be cured by surgery. But surgery is often done first to reduce the amount of tumor that needs to be treated by radiation or chemotherapy, which might help these treatments work better. This could help prolong the person’s life, even if all of the tumor can’t be removed.
Surgery can also be done to help relieve some of the symptoms caused by brain tumors, particularly those caused by a buildup of pressure within the skull. These can include headaches, nausea, vomiting, and blurred vision. Surgery may also make seizures easier to control with medicines.
Surgery to remove the tumor may not be a good option in some situations, such as if the tumor is deep within the brain, if it’s in a part of the brain that can’t be removed, such as the brain stem, or if a person can’t have a major operation for other health reasons.
Surgery is not very effective against some types of brain tumors, such as lymphomas, although it may be used to get a biopsy sample for diagnosis.
Craniotomy
A craniotomy is a surgical opening made in the skull. This is the most common approach for surgery to treat brain tumors. The person may either be under general anesthesia (in a deep sleep) or may be awake for at least part of the procedure (with the surgical area numbed) if brain function needs to be assessed during the operation.
Part of the head might be shaved before surgery. The neurosurgeon first makes a cut in the scalp over the skull near the tumor, and folds back the skin. A special type of drill is used to remove the piece of the skull over the tumor.
The opening is typically large enough for the surgeon to insert several instruments and see the parts of the brain needed to operate safely. The surgeon may need to cut into the brain itself to reach the tumor. The surgeon might use MRI or CT scans taken before the surgery (or may use ultrasound once the skull has been opened) to help locate the tumor and its edges.
The surgeon can remove the tumor in different ways depending on how hard or soft it is, and whether it has many or just a few blood vessels:
- Many tumors can be cut out with a scalpel or special scissors.
- Some tumors are soft and can be removed with suction devices.
- In other cases, a handheld ultrasonic aspirator can be placed into the tumor to break it up and suck it out.
Many devices can help the surgeon see the tumor and surrounding brain tissue. The surgeon often operates while looking at the brain through a special microscope. MRI or CT scans can be done before surgery (or ultrasound can be used once the skull has been opened) to map the area of tumors deep in the brain. In some cases, the surgeon uses intraoperative imaging, in which MRI (or other) images are taken at different times during the operation to show the location of any remaining tumor. This may allow some brain tumors to be resected more safely and extensively.
As much of the tumor is removed as possible while trying not to affect brain functions. The surgeon can use different techniques to lower the risk of removing vital parts of the brain, such as:
- Intraoperative cortical stimulation (cortical mapping): In this approach, the surgeon electrically stimulates parts of the brain in and around the tumor during the operation and monitors the response. This can show if these areas control an important function (and therefore should be avoided).
- Functional MRI: This type of imaging test can be done before surgery to locate a particular function of the brain. This information can be used to identify and preserve that region during the operation.
- Fluorescence-guided surgery: For some types of tumors, such as glioblastomas, the patient can be given a special fluorescent dye before surgery. The dye is taken up by the tumor, which then glows when the surgeon looks at it under fluorescent lighting from the operating microscope. This lets the surgeon better separate tumor from normal brain tissue.
- Newer techniques: Newer types of MRI, as well as newer surgical approaches, might be helpful in some situations.
Once the surgery is complete, the piece of the skull bone is put back in place and fastened with metal screws and plates, wires, or special stitches. Usually any metal pieces are made from titanium, which allows a person to get follow-up MRIs [and will not set off metal detectors].
You might have small tube (called a drain) coming out of the incision that allows excess cerebrospinal fluid (CSF) to leave the skull. Other drains may be in place to allow blood that builds up after surgery to drain from under the scalp. These drains are usually removed after a few days. An imaging test such as an MRI or CT scan is typically done 1 to 3 days after the operation to confirm how much of the tumor has been removed. Recovery time in the hospital is usually 4 to 6 days, although this depends on the size and location of the tumor, the patient’s general health, and whether other treatments are given. Healing around the surgery site usually takes several weeks.
Surgery to help with CSF flow blockage
If a tumor blocks the flow of cerebrospinal fluid (CSF), it can increase pressure inside the skull (known as increased intracranial pressure, or ICP). This can cause symptoms like headaches, nausea, and drowsiness, and may even be life-threatening. Surgery to remove the tumor can often help with this, but there are also other ways to drain away excess CSF and lower the pressure if needed.
For example, the neurosurgeon may put in a silicone tube called a shunt (also called a ventriculoperitoneal shunt or VP shunt). One end of the shunt is placed in a ventricle of the brain (an area filled with CSF) and the other end is placed in the abdomen or, less often, the heart (and would then be referred to as a ventriculoatrial shunt). The tube runs under the skin of the neck and chest. The flow of CSF is controlled by a valve placed along the tubing.
Shunts can be temporary or permanent. They can be placed before or after the surgery to remove the tumor. Placing a shunt normally takes about an hour. As with any operation, complications might develop, such as bleeding or infection. Strokes are possible as well. Sometimes shunts get clogged and need to be replaced. The hospital stay after shunt procedures is typically 1 to 3 days, depending on the reason it is placed and the patient’s general health.
Another option to treat increased pressure in the skull in some cases is an endoscopic third ventriculostomy (ETV). In this operation, an opening is made in the floor of the third ventricle at the base of the brain to allow the CSF to flow again. This operation is done through a small hole in the front of the skull. An advantage of this approach is that it does not require a shunt. But there is also a chance that the opening made in the ventricle might close up again, which is more likely in people with brain tumors.
If the pressure inside the head needs to be relieved for a short time, an external ventricular drain (EVD) might be put in place to allow the excess CSF to drain out. The drain is a small tube. One end is put into a ventricle, and the other end is attached to a collection bag outside the body. Along with collecting the excess CSF, the drain can also be used to measure the pressure inside the skull, as well as to look for tumor cells, blood, or signs of infection in the CSF.
The drain can be placed either during surgery or during a procedure at the patient’s bedside. It can be put in place to relieve the pressure in the days before surgery, or to help drain the fluid that collects after an operation. If the pressure inside the skull needs to be lowered for more than a few days, the doctor might need to change this to a VP shunt.
Surgery to put in a ventricular access catheter
Surgery may also be used to insert a ventricular access catheter, such as an Ommaya reservoir, to help deliver chemotherapy directly into the CSF. A small incision is made in the scalp, and a small hole is drilled in the skull. A flexible tube is then threaded through the hole until the open end of the tube is in a ventricle, where it reaches the CSF. The other end, which has a dome-shaped reservoir, stays just under the scalp. After the operation, doctors and nurses can use a thin needle to give chemotherapy drugs through the reservoir or to remove CSF from the ventricle for testing.
Radiation therapy
Radiation therapy uses high-energy beams, such as X-rays or protons, to kill tumor cells. Radiation therapy can come from a machine outside your body (external beam radiation), or, very rarely, radiation can be placed inside your body close to your brain tumor (brachytherapy).
External beam radiation can focus just on the area of your brain where the tumor is located, or it can be applied to your entire brain (whole-brain radiation). Whole-brain radiation is most often used to treat cancer that spreads to the brain from some other part of the body and forms multiple tumors in the brain.
Traditionally, radiation therapy uses X-rays, but a newer form of this treatment uses proton beams. Proton beam therapy allows doctors to control the radiation more precisely. It may be helpful for treating brain tumors in children and tumors that are very close to sensitive areas of the brain. Proton beam therapy isn’t as widely available as traditional X-ray radiation therapy.
Before your treatments start, the radiation team will determine the correct angles for aiming the radiation beams and the proper dose of radiation. This planning session, called simulation, usually includes getting imaging tests such as CT or MRI scans.
In most cases, the total dose of radiation is divided into daily amounts (usually given Monday through Friday) over several weeks. At each treatment session, you lie on a special table while a machine delivers the radiation from precise angles. The treatment is not painful. Each session lasts about 15 to 30 minutes, and much of that time is spent making sure the radiation is aimed correctly. The actual treatment time each day is much shorter.
High doses of radiation therapy can damage normal brain tissue, so doctors try to deliver the radiation to the tumor while giving the lowest possible dose to normal surrounding brain areas. Several techniques can help doctors focus the radiation more precisely:
- Three-dimensional conformal radiation therapy (3D-CRT): 3D-CRT uses the results of imaging tests such as MRI and special computers to map the location of the tumor precisely. Several radiation beams are then shaped and aimed at the tumor from different directions. Each beam alone is fairly weak, which makes it less likely to damage normal tissues, but the beams converge at the tumor to give a higher dose of radiation there.
- Intensity modulated radiation therapy (IMRT): Intensity modulated radiation therapy (IMRT): is an advanced form of 3D therapy. It uses a computer-driven machine that moves around the patient as it delivers radiation. Along with shaping the beams and aiming them at the tumor from several angles, the intensity (strength) of the beams can be adjusted to limit the dose reaching the most sensitive normal tissues. This may let the doctor deliver a higher dose to the tumor. Many major hospitals and cancer centers now use IMRT.
- Volumetric modulated arc therapy (VMAT): This newer technique is similar to IMRT. For this treatment, the patient lies on a table, which passes through the machine delivering the radiation. The source of the radiation (the linear accelerator) rotates around the table in an arc, delivering the beams from different angles. A computer controls the intensity of the beams to help keep the radiation focused on the tumor. It’s not yet clear if this approach results in better outcomes than IMRT, although it does allow the radiation to be given over less time in each treatment session.
- Conformal proton beam radiation therapy: Proton beam therapy uses an approach similar to 3D-CRT. But instead of using x-rays, it focuses proton beams on the tumor. Protons are positive parts of atoms. Unlike x-rays, which release energy both before and after they hit their target, protons cause little damage to tissues they pass through and then release their energy after traveling a certain distance. This lets doctors deliver more radiation to the tumor and do less damage to nearby normal tissues. This approach may be more helpful for brain tumors that have distinct edges (such as chordomas), but it is not clear if it will be useful for tumors that typically grow into or mix with normal brain tissue (such as astrocytomas or glioblastomas). There are a limited number of proton beam centers in the United States at this time.
- Stereotactic radiosurgery (SRS)/stereotactic radiotherapy (SRT): Stereotactic radiosurgery is not a form of surgery in the traditional sense. (There is no actual surgery in this treatment.) Instead, radiosurgery uses multiple beams of radiation to give a highly focused form of radiation treatment to kill the tumor cells in a very small area. Each beam of radiation isn’t particularly powerful, but the point where all the beams meet — at the brain tumor — receives a very large dose of radiation to kill the tumor cells. Stereotactic radiosurgery (SRS)/stereotactic radiotherapy (SRT) delivers a large, precise radiation dose to the tumor area in a single session (stereotactic radiosurgery [SRS]) or in a few sessions (stereotactic radiotherapy [SRT]). It may be used for some tumors in parts of the brain or spinal cord that can’t be treated with surgery or when a patient isn’t healthy enough for surgery. A head frame might be attached to the skull to help aim the radiation beams. (Sometimes a face mask is used to hold the head in place instead.) Once the exact location of the tumor is known from CT or MRI scans, radiation is focused at the tumor from many different angles. This can be done in 2 ways:
- In one approach, thin radiation beams are focused at the tumor from hundreds of different angles for a short period of time. Each beam alone is weak, but they all converge at the tumor to give a higher dose of radiation. An example of a machine that uses this technique is the Gamma Knife.
- Another approach uses a movable linear accelerator (a machine that creates radiation) that is controlled by a computer. Instead of delivering many beams at once, this machine moves around the head to deliver radiation to the tumor from many different angles. Several machines with names such as X-Knife, CyberKnife, and Clinac deliver stereotactic radiosurgery in this way.
- Stereotactic radiosurgery (SRS) typically delivers the whole radiation dose in a single session, though it may be repeated if needed.
- For stereotactic radiotherapy (SRT) (also called fractionated radiosurgery), doctors give the radiation in several treatments to deliver the same or a slightly higher dose. Frameless techniques are now available to make this more comfortable.
- Image-guided radiation therapy (IGRT): For image-guided radiation therapy (IGRT), an imaging test such as a CT scan is done just before each treatment to help better guide the radiation to its target. Image-guided radiation therapy (IGRT) is typically used along with some of the more precise techniques for delivering radiation described above. It is most useful when the radiation needs to be delivered very precisely, such as when a tumor is very close to vital structures.
- Brachytherapy (internal radiation therapy): Unlike the external radiation approaches above, brachytherapy involves inserting radioactive material directly into or near the tumor. The radiation it gives off travels a very short distance, so it affects only the tumor. This technique is most often used along with external radiation. It provides a high dose of radiation at the tumor site, while the external radiation treats nearby areas with a lower dose.
- Whole brain and spinal cord radiation therapy (craniospinal radiation): If tests like an MRI scan or lumbar puncture find the tumor has spread along the covering of the spinal cord (meninges) or into the surrounding cerebrospinal fluid, radiation may be given to the whole brain and spinal cord. Some tumors such as ependymomas and medulloblastomas are more likely to spread this way and often require craniospinal radiation.
Radiation is more harmful to tumor cells than it is to normal cells. Still, radiation can also damage normal brain tissue, which can lead to side effects. Side effects of radiation therapy depend on the type and dose of radiation you receive. Common side effects during or immediately following radiation include fatigue, headaches, memory loss, scalp irritation and hair loss.
- Side effects during or soon after treatment: Some people become irritable and tired during the course of radiation therapy. Nausea, vomiting, and headaches are also possible side effects but are uncommon. Sometimes dexamethasone (a corticosteroid) or other drugs can help relieve these symptoms. Some people might have hair loss in areas of the scalp that get radiation. Other side effects are also possible, depending on where the radiation is aimed.
- Problems with thinking and memory: A person may lose some brain function if large areas of the brain get radiation. Problems can include memory loss, personality changes, and trouble concentrating. There may also be other symptoms depending on the area of brain treated and how much radiation was given. These risks must be balanced against the risks of not using radiation and having less control of the tumor.
- Radiation necrosis: Rarely after radiation therapy, a mass of dead (necrotic) tissue forms at the site of the tumor in the months or years after radiation treatment. This can often be controlled with corticosteroid drugs, but surgery may be needed to remove the necrotic tissue in some instances.
- Increased risk of another tumor: Radiation can damage genes in normal cells. As a result, there is a small risk of developing a second cancer in an area that got radiation — for example, a meningioma of the coverings of the brain, another brain tumor, or less likely a bone cancer in the skull. If this develops, it’s usually many years after the radiation is given. This small risk should not prevent those who need radiation from getting treatment.
Chemotherapy
Chemotherapy (chemo) uses anti-cancer drugs to kill tumor cells. Chemotherapy drugs can be taken orally in pill form or injected into a vein (intravenously). However, many chemo drugs aren’t able to enter the brain and reach tumor cells. For some brain tumors, drugs can be given directly into the cerebrospinal fluid (CSF, the fluid that bathes the brain and spinal cord), either in the brain or into the spinal canal below the spinal cord. To help with this, a thin tube known as a ventricular access catheter may be inserted through a small hole in the skull and into a ventricle of the brain during a minor operation.
In general, chemo is used for faster-growing brain tumors. Some types of brain tumors, such as medulloblastoma and lymphoma, tend to respond better to chemo than others. Chemo is not as helpful for treating some other types of tumors, such as spinal cord tumors, so it is used less often for these tumors.
Chemo is most often used along with other treatments such as surgery and/or radiation therapy. Chemo can also be used by itself, especially for more advanced tumors or for tumors that have come back after other types of treatment.
Some of the chemo drugs used to treat brain and spinal cord tumors include:
- Carboplatin
- Carmustine (BCNU)
- Cisplatin
- Cyclophosphamide
- Etoposide
- Irinotecan
- Lomustine (CCNU)
- Methotrexate
- Procarbazine
- Temozolomide (Temodar)
- Vincristine
These drugs can be used alone or in combinations, depending on the type of brain tumor. Tests of your brain tumor cells can determine whether chemotherapy will be helpful for you. The type of brain tumor you have also is helpful in determining whether to recommend chemotherapy.
Chemotherapy is given in cycles, with each period of treatment followed by a rest period to give the body time to recover. Each cycle typically lasts for a few weeks.
Carmustine (Gliadel) wafers: These dissolvable wafers contain the chemo drug carmustine (BCNU). After the surgeon removes as much of the brain tumor as is safe during a craniotomy, the wafers can be placed directly on or next to the parts of the tumor that can’t be removed. Unlike IV or oral chemo that reaches all areas of the body, this type of therapy concentrates the drug at the tumor site, producing few side effects in other parts of the body.
Chemo drugs can cause side effects and the side effects depend on the type and dose of drugs you receive including and how long treatment lasts.
Common chemo side effects can include:
- Hair loss
- Mouth sores
- Loss of appetite
- Nausea and vomiting
- Diarrhea
- Increased chance of infections (from having too few white blood cells)
- Easy bruising or bleeding (from having too few blood platelets)
- Fatigue (from having too few red blood cells, changes in metabolism, or other factors)
Some of the most effective drugs against brain tumors tend to have fewer of these side effects than other common chemo drugs. Most side effects usually go away after treatment is finished. There are often ways to lessen these side effects. For example, drugs can often help prevent or reduce nausea and vomiting.
Some chemo drugs can also cause other, less common side effects. For example, cisplatin and carboplatin can also cause kidney damage and hearing loss. Your doctor will check your kidney function and hearing if you are getting these drugs. Some of these side effects might last after treatment is stopped.
Be sure to report any side effects to your medical team while getting chemo, so you can be treated promptly. Sometimes, the doses of the drugs may need to be reduced or treatment may need to be delayed or stopped to prevent the effects from getting worse.
Targeted drug therapy
Targeted drug treatments focus on specific abnormalities present within cancer cells. By blocking these abnormalities, targeted drug treatments can cause cancer cells to die. Targeted therapy drugs are available for certain types of brain tumors, and many more are being studied in clinical trials. Targeted drugs don’t yet play a large role in treating brain or spinal cord tumors, but some of them might be helpful for certain types of tumors. Your doctor may have your tumor cells tested to see whether targeted therapy is likely to be an effective treatment for your brain tumor.
Bevacizumab (Avastin, Mvasi, Zirabev)
Bevacizumab is a man-made version of an immune system protein called a monoclonal antibody. This antibody targets vascular endothelial growth factor (VEGF), a protein that helps tumors form new blood vessels (a process known as angiogenesis), which they need in order to grow.
This drug is used mainly to treat some types of gliomas (especially fast-growing ones such as glioblastomas) that come back after initial treatment. It might also be useful in treating recurrent meningiomas.
When used alone or added to chemotherapy, this drug can help shrink some tumors or extend the time until they start growing again, although it does not seem to help people live longer. It can also help lower the dose of the steroid drug dexamethasone needed to help reduce swelling in the brain, which is especially important for patients sensitive to steroid side effects.
Bevacizumab is given by intravenous (IV) infusion, usually once every 2 weeks.
Common side effects include high blood pressure, tiredness, bleeding, low white blood cell counts, headaches, mouth sores, loss of appetite, and diarrhea. Less common but possibly serious side effects include blood clots, internal bleeding, heart problems, and holes (perforations) in the intestines. This drug can also slow wound healing, so usually it can’t be given within a few weeks of surgery.
Everolimus (Afinitor)
Everolimus works by blocking a cell protein known as mTOR, which normally helps cells grow and divide into new cells. For subependymal giant cell astrocytomas (SEGAs) that can’t be removed completely by surgery, This drug may shrink the tumor or slow its growth for some time, although it’s not clear if it can help people with these tumors live longer.
Everolimus is a pill taken once a day. Common side effects include mouth sores, increased risk of infections, nausea, loss of appetite, diarrhea, skin rash, feeling tired or weak, fluid buildup (usually in the legs), and increases in blood sugar and cholesterol levels. A less common but serious side effect is damage to the lungs, which can cause shortness of breath or other problems.
Alternating electric field therapy
Researchers have found that exposing some types of tumor cells to alternating electric fields also known as tumor treating fields, can interfere with the cells’ ability to grow and spread. A wearable device known as Optune, which generates such electric fields, is now an option to help treat some people with glioblastomas. For this treatment, the head is shaved, and 4 sets of electrodes are placed on the scalp. The electrodes are attached to a battery pack (kept in a backpack) and are worn for most of the day. They generate mild electric currents that are thought to affect tumor cells in the brain more than normal cells.
Optune can be used:
- Along with chemotherapy in people with newly diagnosed glioblastoma after treatment with surgery and radiation therapy. It may help people live longer than if they just get chemotherapy alone.
- Instead of chemotherapy in people whose glioblastoma has come back after initial treatment. It hasn’t been shown to help people live longer than chemotherapy in this situation, but it tends to have much milder side effects.
Side effects of the device tend to be minor, and can include skin irritation at the electrode sites, trouble sleeping, mood changes, and a slightly increased risk of headaches and seizures.
Alternative medicine
Little research has been done on complementary and alternative brain tumor treatments. So far, no dietary supplements (including vitamins, minerals, and herbal products) have been shown to clearly help lower the risk of brain or spinal cord tumors progressing or coming back. No alternative treatments have been proved to cure brain tumors. This doesn’t mean that no supplements will help, but it’s important to know that none have been proven to do so. However, complementary treatments may help you cope with the stress of a brain tumor diagnosis.
Some complementary treatments that may help you cope include:
- Acupuncture
- Art therapy
- Exercise
- Meditation
- Music therapy
- Relaxation exercises
Talk with your doctor about your options.
Rehabilitation after treatment
Because brain tumors can develop in parts of the brain that control motor skills, speech, vision and thinking, rehabilitation may be a necessary part of recovery. Depending on your needs, your doctor may refer you to:
- Physical therapy to help you regain lost motor skills or muscle strength
- Occupational therapy to help you get back to your normal daily activities, including work, after a brain tumor or other illness
- Speech therapy with specialists in speech difficulties (speech pathologists) to help if you have difficulty speaking
- Tutoring for school-age children to help kids cope with changes in their memory and thinking after a brain tumor
Types of brain cancer in Children
Tumors can form in almost any type of tissue or cell in the brain or spinal cord. Some tumors have a mixture of cell types. Tumors in different areas of the central nervous system may be treated differently and have a different prognosis (outlook).
Brain tumors in children are more likely to start in the lower parts of the brain, such as the cerebellum and brain stem, than they are in adults. But they can start in the upper parts of the brain as well.
Gliomas
Gliomas are not a specific type of tumor. Glioma is a general term for a group of tumors that start in glial cells. A number of tumors can be considered gliomas, including glioblastoma (also known as glioblastoma multiforme), anaplastic astrocytoma, astrocytoma, oligodendroglioma, ependymoma, brain stem glioma, and optic glioma. About half of all brain and spinal cord tumors in children are gliomas.
Astrocytomas
- Astrocytomas are tumors that start in cells called astrocytes, a kind of glial cell.
- Most astrocytomas can spread widely throughout the brain and blend with the normal brain tissue, which can make them very hard to remove by surgery. Sometimes they spread along the cerebrospinal fluid (CSF) pathways. It is very rare for them to spread outside of the brain or spinal cord.
- Astrocytomas are often grouped as high grade, intermediate grade, or low grade, based largely on how the cells look under the microscope.
Intermediate- and high-grade astrocytomas: These tumors tend to grow quickly and spread into the surrounding normal brain tissue. The highest-grade astrocytoma, known as glioblastoma, is the fastest growing. Anaplastic astrocytomas are also in this group.
Low-grade astrocytomas: These tumors tend to grow slowly and are the most common type in children. Some special types, known as non-infiltrating astrocytomas, tend to grow very slowly and do not grow into (infiltrate) nearby tissues, so they often have a good prognosis.
- Pilocytic astrocytomas are slow growing and rarely infiltrate nearby tissues. They most commonly occur in the cerebellum but can also begin in the optic nerve, hypothalamus, brain stem, or other areas. They account for nearly 1 out of 5 brain tumors in children.
- Subependymal giant cell astrocytomas (SEGAs) occur in the ventricles. They are also slow growing and rarely infiltrate nearby tissues. These tumors are almost always linked with an inherited condition called tuberous sclerosis.
- Fibrillary (diffuse) astrocytomas are also slow-growing tumors, but with the important characteristic of growing into nearby tissues, which makes them hard to remove with surgery. Though these tumors are thought of as low grade, they tend to become more aggressive and fast growing over time.
- Optic gliomas are low-grade astrocytomas that start in the optic nerves (the nerves leading from the eyes to the brain). They are often linked with an inherited condition called neurofibromatosis type 1. These tumors are rarely fatal, but they may cause vision loss and injury to nearby brain tissue.
Oligodendrogliomas
These tumors start in brain glial cells called oligodendrocytes. These tumors tend to grow slowly, but like astrocytomas, most of them can grow into nearby brain tissue and can’t be removed completely by surgery. Oligodendrogliomas rarely spread along the CSF pathways and even less frequently spread outside the brain or spinal cord. Only about 1% of brain tumors in children are oligodendrogliomas. As with astrocytomas, they can become more aggressive over time.
Ependymomas
- About 5% of brain tumors in children are ependymomas. These tumors start in the ependymal cells that line the ventricles or central canal of the spinal cord. They can range from fairly low-grade (slow growing) tumors to higher grade ones, which are called anaplastic ependymomas.
- Ependymomas may spread along the CSF pathways but do not spread outside the brain or spinal cord. These tumors can block the flow of CSF out of the ventricles, causing the ventricles to become very large – a condition called hydrocephalus.
- Unlike astrocytomas and oligodendrogliomas, ependymomas usually do not grow into normal brain tissue. As a result, some (but not all) ependymomas can be removed and cured by surgery. But because they can spread along ependymal surfaces and CSF pathways, treating them can sometimes be difficult.
Mixed gliomas
These tumors contain more than one cell type. For example, oligoastrocytomas have some of the same types of cells as both oligodendrogliomas and astrocytomas. Treatment is typically based on the fastest-growing component of the tumor.
Brain stem gliomas
This term refers to the location of the tumor, rather than the type of cell it starts in. A small number of brain stem gliomas occur as a tumor with very distinct edges (called a focal brain stem glioma). More often, brain stem gliomas grow diffusely throughout the brain stem, rather than growing as a focal tumor. These tumors often start in the pons, where they are called diffuse intrinsic pontine gliomas (DIPGs).
About 10% to 20% of brain tumors in children are brain stem gliomas. Nearly all of these tumors are some type of astrocytoma.
Primitive neuroectodermal tumors (PNETs)
These tumors start in primitive (immature) cells of the central nervous system called neuroectodermal cells. About 1 out of 5 brain tumors in children are PNETs. They are more common in younger children than older ones, and are rare in adults. PNETs tend to grow quickly and often spread throughout the CSF pathways.
- Medulloblastomas: PNETs that start in the cerebellum are called medulloblastomas. Most PNETs in children are medulloblastomas. These tumors can often be treated effectively and tend to have a better outlook than PNETs in other parts of the brain.
- Pineoblastomas: PNETs that occur in the pineal gland are called pineoblastomas. These tumors are usually harder to treat than medulloblastomas.
- Other PNETs: Other, less common types of central nervous system PNETs include medulloepitheliomas, ependymoblastomas, and neuroblastomas that start in the brain or spinal cord.
Craniopharyngiomas
These slow-growing tumors start above the pituitary gland but below the brain itself. They account for about 4% of brain tumors in children. These tumors may press on the pituitary gland and the hypothalamus, causing hormone problems. Because craniopharyngiomas start very close to the optic nerves, they can also cause vision problems. This makes them hard to remove completely without damaging the child’s vision or hormone balance.
Mixed glial and neuronal tumors
Certain tumors that develop in children and young adults (and rarely in older adults) have both glial and neuronal cell components. They tend to have a fairly good prognosis.
- Pleomorphic xanthoastrocytoma (PXA) and dysembryoplastic neuroepithelial tumors (DNETs) look as if they could grow quickly when seen under the microscope, but these tumors tend to be fairly benign, and most are cured by surgery alone.
- Ganglioglioma is a type of tumor that has both mature neurons and glial cells. Most can be cured by surgery alone or surgery combined with radiation therapy.
Choroid plexus tumors
These rare tumors start in the choroid plexus within the ventricles of the brain. Most are benign (choroid plexus papillomas) and are cured by surgery. However, some are malignant (choroid plexus carcinomas).
Schwannomas (neurilemmomas)
This type of tumor starts in Schwann cells that surround and insulate cranial nerves and other nerves. Schwannomas are usually benign tumors. They often form near the cerebellum on the cranial nerve responsible for hearing and balance, in which case they are called vestibular schwannomas or acoustic neuromas. They may also develop on spinal nerves past the point where the nerves have left the spinal cord. When this is the case, the tumor can press on the spinal cord, causing weakness, sensory loss, and bowel and bladder problems.
These tumors are rare in children. When schwannomas are found in a child, particularly if there are tumors on both sides of the head, it often means the child has an inherited tumor syndrome such as neurofibromatosis type 2.
Other tumors that start in or near the brain
Meningiomas
These tumors begin in the meninges, the layers of tissue that surround the outer part of the brain and spinal cord. Meningiomas cause symptoms by pressing on the brain or spinal cord. They are much less common in children than in adults.
Meningiomas are almost always benign and are usually cured by surgery. Some, however, are located very close to vital structures in the brain and can’t be cured by surgery alone.
Meningiomas are often assigned a grade based on how the tumor cells look.
- Grade I tumors, which look most like normal cells, make up about 80% to 90% of meningiomas.
- Grade II (atypical) meningiomas look slightly more abnormal.
- Grade III (anaplastic) meningiomas, which look the most abnormal, make up only about 1% to 3% of meningiomas.
Higher-grade meningiomas are more likely to come back after treatment, and some grade III meningiomas can spread to other parts of the body.
Chordomas
These tumors start in the bone at the base of the skull or at the lower end of the spine. These tumors don’t start in the central nervous system, but they can injure nearby parts of the brain or spinal cord by pressing on them. Chordomas tend to come back after treatment, if they are not removed completely, causing more damage. They usually do not spread to other organs. Chordomas are much more common in adults than in children.
Germ cell tumors
These rare tumors develop from germ cells, which normally form eggs in women and sperm in men. During normal development before birth, germ cells travel to the ovaries or testicles and develop into eggs or sperm cells. But sometimes some germ cells don’t move where they should and end up in abnormal locations such as the brain. They may then develop into germ cell tumors, similar to those that can form in the ovaries or testicles.
Germ cell tumors of the nervous system usually occur in children, most often in the pineal gland or above the pituitary gland. These tumors can sometimes be diagnosed without a biopsy by measuring certain chemicals in the cerebrospinal fluid (CSF) or blood.
The most common germ cell tumor of the nervous system is the germinoma. Other tumors that start in germ cells include choriocarcinomas, embryonal carcinomas, teratomas, and yolk sac tumors (endodermal sinus tumors).
Neuroblastomas
These nerve cell tumors are the third most common cancer in children. Neuroblastomas rarely develop in the brain or spinal cord; most develop from nerve cells inside the abdomen or chest. This type of cancer is most common during early infancy.
Lymphomas
Lymphomas are cancers that start in cells called lymphocytes (one of the main cell types of the immune system). Most lymphomas start in other parts of the body, but a small portion start in the central nervous system (CNS). CNS lymphomas are rare in children. For more on childhood lymphomas, see Non-Hodgkin Lymphoma.
Pituitary tumors
Tumors that start in the pituitary gland are almost always benign (non-cancerous). But they can still cause problems if they grow large enough to press on nearby structures or if they make too much of any kind of hormone. These tumors are more common in teens than in younger children.
Cancers that spread to the brain from other sites
Sometimes brain tumors are found not to have started in the brain but rather to have metastasized (spread) there from some other part of the body. Tumors that start in other organs and then spread to the brain are called metastatic or secondary brain tumors (as opposed to primary brain tumors, which start in the brain). This is important because metastatic and primary brain tumors are often treated differently.
In children, metastatic brain tumors are much less common than primary brain tumors. Childhood leukemias can sometimes spread to the CSF around the brain and spinal cord. When this happens, the cancer is still considered a leukemia (the cancer cells in the CSF are leukemia cells), so doctors use treatments directed at the leukemia.
Survival rates for more common childhood brain and spinal cord tumors
The numbers below come from the Central Brain Tumor Registry of the United States 7 and are based on children aged 19 or younger who were treated between 1995 and 2010. There are some important points to note about these numbers:
- These numbers are for some of the more common types of tumors. Numbers are not readily available for all types of tumors that occur in children, often because they are rare or are hard to classify.
- In some cases, the numbers include a wide range of different types of tumors that can have different outlooks. For example, the survival rate for primitive neuroectodermal tumors (PNETs) below includes medulloblastomas, pineoblastomas, and primitive neuroectodermal tumors (PNETs) in other parts of the brain. Medulloblastomas tend to have a better outlook than the other primitive neuroectodermal tumors (PNETs). Therefore the actual survival rate for medulloblastomas would be expected to be higher than the number below, while the number for other primitive neuroectodermal tumors (PNETs) would likely be lower.
Survival rates are often based on previous outcomes of large numbers of children who had the disease, but they can’t predict what will happen in any particular child’s case. Knowing the type of a child’s brain tumor is important in estimating their outlook. But many other factors can also affect a child’s outlook, such as the location and extent of the tumor and how well it responds to treatment. Even taking these other factors into account, survival rates are at best rough estimates. Your child’s doctor knows your child’s situation and is your best source of information on this topic.
Table 2. Survival rates for more common childhood brain and spinal cord tumors
| Type of Tumor | 5-Year Survival Rate |
|---|---|
| Pilocytic astrocytoma | About 95% |
| Fibrillary (diffuse) astrocytoma | About 80% to 85% |
| Anaplastic astrocytoma | About 30% |
| Glioblastoma | About 20% |
| Oligodendroglioma | About 90% to 95% |
| Ependymoma/anaplastic ependymoma | About 75% |
| PNETs (includes medulloblastoma and pineoblastoma) | About 60% to 65% |
What causes brain cancer in Children
The cause of most brain and spinal cord tumors is not fully understood. But researchers have found some of the changes that occur in normal brain cells that may lead them to form tumors.
Normal human cells grow and function based mainly on the information contained in each cell’s chromosomes. Chromosomes are long strands of DNA in each cell. Brain and spinal cord tumors, like other tumors, are usually caused by changes (mutations) in the DNA inside cells. DNA is the chemical that makes up our genes – the instructions for how our cells function. We usually look like our parents because they are the source of our DNA. But DNA affects more than how we look.
Some genes control when our cells grow, divide into new cells, and die. Certain genes that help cells grow, divide, and stay alive are called oncogenes. Others that slow down cell division, or cause cells to die at the right time, are called tumor suppressor genes. Cancers can be caused by DNA changes that turn on oncogenes or turn off tumor suppressor genes. These gene changes can be inherited from a parent (as is sometimes the case with childhood cancers), but more often they happen spontaneously during a person’s lifetime.
In recent years, researchers have found the gene changes that cause some rare inherited syndromes (like neurofibromatosis, tuberous sclerosis, Li-Fraumeni syndrome, and von Hippel-Lindau syndrome) and increase the risk of developing some brain and spinal cord tumors. For example, the Li-Fraumeni syndrome is caused by changes in the TP53 tumor suppressor gene. Normally, this gene prevents cells with damaged DNA from growing. Changes in this gene increase the risk of developing brain tumors (particularly gliomas), as well as some other cancers.
In most cases, it is not known why people without inherited syndromes develop brain or spinal cord tumors. Most risk factors for cancer somehow damage genes. For example, tobacco smoke is a risk factor for lung cancer and several other cancers because it contains chemicals that can damage genes. The brain is relatively protected from tobacco smoke and other cancer-causing chemicals that we might breathe in or eat, so these factors are not likely to play a major role in these cancers.
Several different gene changes must usually occur in normal cells before they become cancerous. There are many kinds of brain tumors, each of which may have different sets of gene changes. A number of gene or chromosome changes have been found in different brain tumor types, but there are probably many others that have not yet been found.
Researchers now understand some of the gene changes that occur in different types of brain tumors, but it’s still not clear what causes these changes. Some gene changes might be inherited, but most brain and spinal cord tumors in children are not the result of known inherited syndromes. Most gene changes are probably just random events that sometimes happen inside a cell, without having an outside cause.
Other than radiation, there are no known lifestyle-related or environmental causes of childhood brain tumors, so it is important to remember that there is nothing these children or their parents could have done to prevent these cancers.
Risk Factors for Brain and Spinal Cord Tumors in Children
A risk factor is anything that affects a person’s chance of getting a disease such as a brain or spinal cord tumor. Different types of cancer have different risk factors.
Lifestyle-related risk factors such as diet, body weight, physical activity, and tobacco use play a major role in many adult cancers. But these factors usually take many years to influence cancer risk, and they are not thought to play much of a role in childhood cancers, including brain tumors.
Very few risk factors have been found for brain and spinal cord tumors. There is no clear cause for most of these tumors.
Radiation exposure
The only well-established environmental risk factor for brain tumors is radiation exposure to the head, which most often comes from the treatment of other conditions.
For example, before the risks of radiation were well known (more than 50 years ago), children with ringworm of the scalp (a fungal infection) often received low-dose radiation therapy. This was later found to increase their risk of brain tumors as they got older.
Today, most radiation-induced brain tumors are caused by radiation given to the head to treat other cancers, such as leukemia. These brain tumors usually develop around 10 to 15 years after the radiation.
Radiation-induced tumors are still fairly rare, but because of the increased risk (as well as the other side effects), radiation therapy is only given to the head after carefully weighing the possible benefits and risks. For most patients with cancer in or near the brain, the benefits of getting radiation therapy as part of their treatment far outweigh the small risk of developing a brain tumor years later.
The possible risk from fetal or childhood exposure to imaging tests that use radiation, such as x-rays or CT scans, is not known for sure. These tests use much lower levels of radiation than those used in radiation treatments, so if there is any increase in risk, it is likely to be very small. But to be safe, most doctors recommend that pregnant women and children not get these tests unless they are absolutely needed.
Inherited and genetic conditions
In rare cases (less than 5% of brain tumors), children have inherited abnormal genes from a parent that put them at increased risk for certain types of brain tumors. In other cases, these abnormal genes are not inherited but occur as a result of changes (mutations) in the gene before birth.
People with inherited tumor syndromes often have many tumors that start when they are young. Some of the more well-known syndromes include:
Neurofibromatosis type 1 (von Recklinghausen disease)
This is the most common syndrome linked to brain or spinal cord tumors. It is often inherited from a parent, but it can also start in some children whose parents don’t have it. Children with this syndrome may have optic gliomas or other gliomas of the brain or spinal cord, or neurofibromas (benign tumors of peripheral nerves). Changes in the NF1 gene cause this disorder.
Neurofibromatosis type 2
Less common than von Recklinghausen disease, this condition can also either be inherited or may start in children without a family history. It is associated with cranial or spinal nerve schwannomas, especially vestibular schwannomas (acoustic neuromas), which almost always occur on both sides of the head. It is also linked to an increased risk of meningiomas, as well as spinal cord gliomas or ependymomas. Changes in the NF2 gene are responsible for neurofibromatosis type 2.
Tuberous sclerosis
Children with this condition may develop subependymal giant cell astrocytomas (SEGAs), as well as other benign tumors of the brain, skin, heart, kidneys, or other organs. This condition is caused by changes in either the TSC1 or the TSC2 gene.
Von Hippel-Lindau disease
Children with this disease tend to develop blood vessel tumors (hemangioblastomas) of the cerebellum, spinal cord, or retina, as well as tumors in the kidney, pancreas, and some other parts of the body. It is caused by changes in the VHL gene.
Li-Fraumeni syndrome
People with this syndrome have an increased risk of gliomas, as well as breast cancer, soft tissue sarcomas, leukemia, adrenal gland cancer, and some other types of cancer. It is caused by changes in the TP53 gene.
Other syndromes
Other inherited conditions linked with increased risks of certain types of brain and spinal cord tumors include:
- Gorlin syndrome (basal cell nevus syndrome)
- Turcot syndrome
- Cowden syndrome
- Hereditary retinoblastoma
- Rubinstein-Taybi syndrome
Some families may have genetic disorders that are not well recognized or that could even be unique to a particular family.
Factors with uncertain, controversial, or unproven effects on brain tumor risk
Cell phone use
Cell phones give off radiofrequency (RF) rays, a form of electromagnetic energy on the spectrum between FM radio waves and those used in microwave ovens, radar, and satellite stations. Cell phones do not give off ionizing radiation, the type that can cause cancer by damaging the DNA inside cells. Still, there have been concerns that the phones, whose antennae are built-in and therefore are placed close to the head when being used, might somehow raise the risk of brain tumors.
Some studies have suggested a possible increased risk of brain tumors or of vestibular schwannomas in adults with cell phone use, but most of the larger studies done so far have not found an increased risk, either overall or among specific types of tumors. Still, there are very few studies of long-term use (10 years or more), and cell phones haven’t been around long enough to determine the possible risks of lifetime use. The same is true of any possible higher risks in children, who are increasingly using cell phones. Cell phone technology also continues to change, and it’s not clear how this might affect any risk.
These risks are being studied, but it will likely be many years before firm conclusions can be made. In the meantime, for people concerned about the possible risks, there are ways to lower their (and their children’s) exposure, such as using the speaker function or an earpiece to move the phone itself away from the head when used.
Other factors
Exposure to aspartame (a sugar substitute), exposure to electromagnetic fields from power lines and transformers, and infection with certain viruses have been suggested as possible risk factors, but most researchers agree that there is no convincing evidence to link these factors to brain tumors. Research on these and other potential risk factors continues.
Signs and Symptoms of Brain and Spinal Cord Tumors in Children
Signs and symptoms from brain and spinal cord tumors might occur gradually and become worse over time, or they can happen suddenly, such as with a seizure.
General symptoms
Tumors in any part of the brain might raise the pressure inside the skull (known as intracranial pressure). This can be caused by growth of the tumor, swelling in the brain, or blocked flow of cerebrospinal fluid. Increased pressure can lead to general symptoms such as:
- Headache
- Nausea
- Vomiting
- Crossed eyes or blurred vision
- Balance problems
- Behavior changes
- Seizures
- Drowsiness or even coma
Headaches that get worse over time are a common symptom of brain tumors. But not all brain tumors cause headaches, and most headaches are not caused by tumors.
In some children, seizures are the first symptom of a brain tumor. Most seizures in children are not caused by brain tumors, but if your child has a seizure, your child’s doctor may refer you to a neurologist (a doctor who specializes in brain and nervous system problems) to make sure it wasn’t caused by a brain tumor or other serious disease.
In the first few years of life, other symptoms of tumors can include irritability, loss of appetite, developmental delay, and a drop in intellectual and physical abilities. In very young children who can’t complain of symptoms, a parent may notice an increase in head size, sometimes along with bulging of the soft spots of the skull (fontanelles). This happens because the bones of the skull haven’t grown together yet, and increased pressure from a tumor can push them apart.
In the school-aged child, other general symptoms of tumors can include poor school performance, fatigue, and personality changes.
If the child can cooperate, the doctor can sometimes tell if pressure inside the skull is increased by looking inside the child’s eyes for swelling of the optic nerve (known as papilledema).
Symptoms of tumors in different parts of the central nervous system
Tumors in different parts of the brain or spinal cord can cause different symptoms. But these symptoms can be caused by any disease in that particular location – they don’t always mean a child has a brain or spinal cord tumor.
Brain and spinal cord tumors often cause problems with the specific functions of the region they develop in. For example:
- Tumors in the parts of the cerebrum (the large, outer part of the brain) that control movement or sensation can cause weakness or numbness in a part of the body, often on just one side.
- Tumors in or near the parts of the cerebrum responsible for language can cause problems with speech or even understanding words.
- Tumors in the front part of the cerebrum can sometimes affect thinking, personality, and language skills.
- Tumors in an area of the brain called the basal ganglia typically cause abnormal movements and body positions.
- Tumors in the cerebellum, which controls coordination, can cause trouble walking or with other normal functions, even eating.
- Tumors in the back part of the cerebrum, or around the pituitary gland, the optic nerves, or certain other cranial nerves can cause vision problems.
- Tumors in or near other cranial nerves might lead to loss of hearing, balance problems, weakness of some facial muscles, or trouble swallowing.
- Spinal cord tumors may cause numbness, weakness, or lack of coordination in the arms and/or legs (usually on both sides of the body), as well as bladder or bowel problems.
Having one or more of the symptoms above does not mean that your child definitely has a brain or spinal cord tumor. All of these symptoms can have other causes. Still, if your child has any of these symptoms, especially if they don’t go away or get worse over time, see your child’s doctor so that the cause can be found and treated, if needed.
How Are Brain and Spinal Cord Tumors Diagnosed in Children?
See diagnosis of brain and spinal cord tumors diganosis in adults above.
How Are Brain and Spinal Cord Tumors in Children Staged?
The stage of a cancer is a measure of how far it has spread. The extent of spread is based on the results of imaging tests (see How are brain and spinal cord tumors in children diagnosed?) and any other tests that have been done.
For most types of cancer, the stage is one of the most important factors in selecting treatment options and in determining the outlook (prognosis). But tumors of the brain and spinal cord differ in some important ways from cancers in other parts of the body. One of the main reasons other cancers are dangerous is that they can spread throughout the body. Tumors starting in the brain or spinal cord can spread to other parts of the central nervous system, but they almost never spread to other organs. These tumors are dangerous because when they grow, it can interfere with essential functions of the brain.
Because most tumors in the brain or spinal cord do not usually spread, they are not formally staged. Some of the most important factors that determine your child’s prognosis include:
- The type of tumor (such as astrocytoma, ependymoma, etc.)
- The grade of the tumor (how quickly the tumor is likely to grow, based on how the cells look under a microscope)
- The location and size of the tumor
- How much of the tumor can be removed by surgery (if it can be done)
- Your child’s age
- Your child’s functional level (whether the tumor is affecting normal brain functions and everyday activities)
- Whether or not the tumor has spread through the cerebrospinal fluid (CSF) to other parts of the brain or spinal cord
- Whether or not tumor cells have spread beyond the central nervous system
Medulloblastoma risk groups
A staging system is a standard way for the cancer care team to describe the extent of tumor spread. Formal staging systems have been proposed for some childhood brain tumors.
For example, many clinical trials for treating medulloblastoma use a system that places children into either standard-risk or high-risk groups. Children are placed in the high-risk group if any of these apply:
- The child is younger than 3
- A lot of the tumor can’t be removed during surgery
- Tumor cells are in the CSF or have spread to other parts of the brain or elsewhere
Doctors are still refining this system to make it as accurate as possible.
- Recent research has shown that medulloblastomas can be divided into 4 types, based on the major gene changes found in the cancer cells. Each type of medulloblastoma has a different outlook, so doctors may be able to use this to better tailor the treatment each child gets.
Brain cancer treatment in Children
Children and teens with brain and spinal cord tumors and their families have special needs that can be met best by cancer centers for children and teens, working closely with the child’s primary care doctor. These centers offer the advantage of being treated by teams of specialists who know the differences between cancers in adults and those in children and teens, as well as the unique needs of younger people with cancer.
For childhood brain and spinal cord tumors, this team is often led by a pediatric neurosurgeon, a doctor who uses surgery to treat brain and nervous system tumors in children. Other doctors on the team may include:
- Pediatric neurologist: a doctor who treats brain and nervous system diseases in children
- Radiation oncologist: a doctor who uses radiation to treat cancer
- Pediatric oncologist: a doctor who uses chemotherapy and other medicines to treat children’s cancers
- Endocrinologist: a doctor who treats diseases in glands that secrete hormones
Many other specialists may be involved in your child’s care as well, including physician assistants (PAs), nurse practitioners (NPs), nurses, psychologists, social workers, rehabilitation specialists, and other health professionals.
Going through cancer treatment with a child often means meeting lots of specialists and learning about parts of the medical system you probably haven’t had contact with before.
Before treatment, the doctors and other members of the team will help you, as a parent, understand the tests that will need to be done. The team’s social worker will also counsel you about the problems you and your child might have during and after treatments such as surgery, and might be able to help you find housing and financial aid if needed.
Other team members, such as a psychologist and specialists in rehabilitation, may also see your child before treatment begins. For example, if the tumor is slow growing and your child’s condition is stable, he or she may be seen by a psychologist before treatment to assess any damage the tumor may have caused. Most of the work of these specialists takes place after treatment.
The main treatments for children with brain and spinal cord tumors are:
- Surgery
- Radiation therapy
- Chemotherapy
- Targeted therapy
- Other drug treatments
In many cases children will get some combination of these treatments. Treatment is based on the type of tumor and other factors. Doctors plan each child’s treatment individually to give them the best chance of a cure while limiting side effects as much as possible.
It’s important to discuss your child’s treatment options as well as their possible side effects with the treatment team to help make the decision that’s the best fit for your child. If there is anything you don’t understand, ask to have it explained.
If time allows, getting a second opinion from another doctor experienced with your child’s type of tumor is often a good idea. It can give you more information and help you feel more confident about the treatment plan you choose.
Taking part in a clinical trial
Clinical trials are carefully controlled research studies that are done to get a closer look at promising new treatments or procedures. Clinical trials are one way to get state-of-the art cancer treatment. In some cases they may be the only way to get access to newer treatments. They are also the best way for doctors to learn better methods to treat cancer. Still, they are not right for everyone.
If you would like to learn more about clinical trials that might be right for you, start by asking your doctor if your clinic or hospital conducts clinical trials.
Considering complementary and alternative methods
You may hear about alternative or complementary methods that your doctor hasn’t mentioned to treat your cancer or relieve symptoms. These methods can include vitamins, herbs, and special diets, or other methods such as acupuncture or massage, to name a few.
Complementary methods refer to treatments that are used along with your regular medical care. Alternative treatments are used instead of a doctor’s medical treatment. Although some of these methods might be helpful in relieving symptoms or helping you feel better, many have not been proven to work. Some might even be dangerous.
Be sure to talk to your cancer care team about any method you are thinking about using. They can help you learn what is known (or not known) about the method, which can help you make an informed decision.
Help getting through cancer treatment
Your cancer care team will be your first source of information and support, but there are other resources for help when you need it. Hospital- or clinic-based support services are an important part of your care. These might include nursing or social work services, financial aid, nutritional advice, rehab, or spiritual help.
References- What Are Adult Brain and Spinal Cord Tumors? https://www.cancer.org/cancer/brain-spinal-cord-tumors-adults/about/what-are-brain-spinal-tumors.html
- Key Statistics for Brain and Spinal Cord Tumors. https://www.cancer.org/cancer/brain-spinal-cord-tumors-adults/about/key-statistics.html
- National Center for Biotechnology Information, U.S. National Library of Medicine. Hypothalamus. https://www.ncbi.nlm.nih.gov/pubmedhealth/PMHT0022790/
- Lemaire J-J, Nezzar H, Sakka L, et al. Maps of the adult human hypothalamus. Surgical Neurology International. 2013;4(Suppl 3):S156-S163. doi:10.4103/2152-7806.110667. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3654779/
- Purves D, Augustine GJ, Fitzpatrick D, et al., editors. Neuroscience. 2nd edition. Sunderland (MA): Sinauer Associates; 2001. Neuroglial Cells. Available from: https://www.ncbi.nlm.nih.gov/books/NBK10869/
- Survival Rates for Selected Adult Brain and Spinal Cord Tumors. https://www.cancer.org/cancer/brain-spinal-cord-tumors-adults/detection-diagnosis-staging/survival-rates.html
- Central Brain Tumor Registry of the United States. http://www.cbtrus.org/