What are shin splints
The term “shin splints” also known as Medial Tibial Stress Syndrome (MTSS) refers to pain along the inner edge of the shinbone (tibia). Shin splints are not a specific medical condition, but rather a generic term describing pain that is experienced between the knee and ankle after physical activity. Shin splints (medial tibial stress syndrome) is an inflammation of the muscles, tendons, and bone tissue around your tibia. Pain typically occurs along the inner border of the tibia, where muscles attach to the bone. Although there are many reasons why pain is felt in this area, shin splints are considered a cumulative stress disorder, as opposed to an acute injury. Shin splints (medial tibial stress syndrome) typically occurs in athletes (e.g. runners/jumpers) and is characterized by localized pain that occurs during exercise at the medial surface of the distal two-thirds of the tibial shaft. Shin splints typically develop when the constant pounding and stresses placed on the bones, muscles and joints overwhelm the body’s natural ability to repair the damage and restore itself. Shin splints can often be described as “too much, too soon”, often affecting long distance runners who build up their mileage too quickly, or seasoned runners who change their workout regime abruptly, for example switching from running on flat surfaces to hills.
Shin splints are commonly seen in athletes, runners, military recruits and even middle-aged weekend warriors, especially at the beginning of the sporting season. Treating them can be as simple as adding extra arch support to redistribute the stresses, or changing to softer running surfaces. “Active rest”, which means that a runner, for example, should take up swimming or biking for awhile, which gives the effected areas time to heal but maintains the cardiovascular benefits of exercise.
Causes of the pain that are characteristic of shin splints generally fall into two areas – muscle or bone. The muscles that connect to the ankle are covered by a tough membrane known as fascia. This fascia holds the muscles together, but it is quite tough and inelastic. When the muscles naturally expand as a result of exertion, they have nowhere to go. This expansion cuts off circulation, and the resulting pressure causes the pain. This form of shin splints, known as exertional compartment syndrome, is common in athletes playing field sports like soccer or those who run a lot on hard surfaces. The second major source of shin splints is related to the bones, ranging from stress reactions to full-blown stress fractures. The constant pounding the skeleton endures during running, for example, can cause many microscopic cracks to appear on the bones of the leg. Normally, with rest, the body easily repairs these cracks. Over time, however, these tiny cracks can coalesce into a complete stress fracture, or even a complete fracture.
Warming before exercise as a preventive measure for injuries such as shin splints remains hotly debated by specialists in the field. Based on a research at the Duke University’s Michael W. Krzyzewski Human Performance Laboratory (K Lab), they recommend a slow warm-up period before beginning the activity. They believe that about 10 minutes of graduated activity is the best way to prepare the body for exertion.
Shin splints signs and symptoms:
- Pain and/or inflammation along the inside of the shin – it may feel razor sharp, dull ache or throbbing
- Pain during exercise that may feel better as you warm up in the initial stages of injury
- Pain after exercise
- Pain at night or first thing in the morning
- Tender to touch inside of shins
Treating shin splints at home
Shin splints can usually be treated at home. The following may help relieve the pain and allow your legs to heal:
- Rest – stop the activity that causes your shin splints for at least two to three weeks; you can then start gradually returning to your normal activities
- Ice – hold an ice pack against your shins (a bag of frozen peas wrapped in a tea towel works, too) for around 10 minutes every few hours for the first few days; this helps with pain and swelling
- Pain relief – take over-the-counter painkillers, such as paracetamol and ibuprofen, to help relieve the pain if you need to
- Switch to low-impact activities – using a cross-trainer, cycling, swimming and yoga are good ways to keep fit without putting too much pressure on your shins while they heal
You can start to return to your usual activities over the following few weeks once the pain has gone. Take care to increase your activity level gradually, building up the time you spend running or doing sports.
Make sure you follow the steps to prevent shin splints outlined below to reduce the risk of the pain coming back.
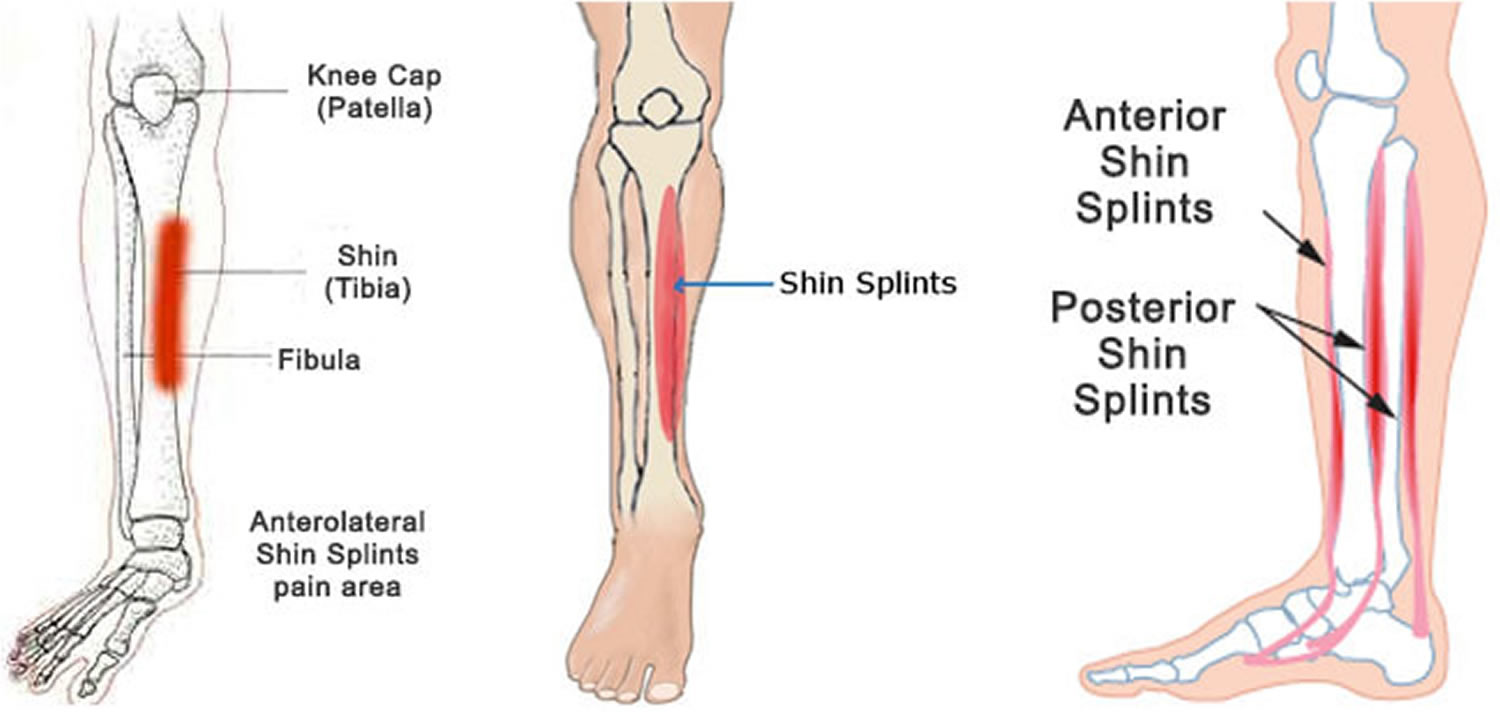
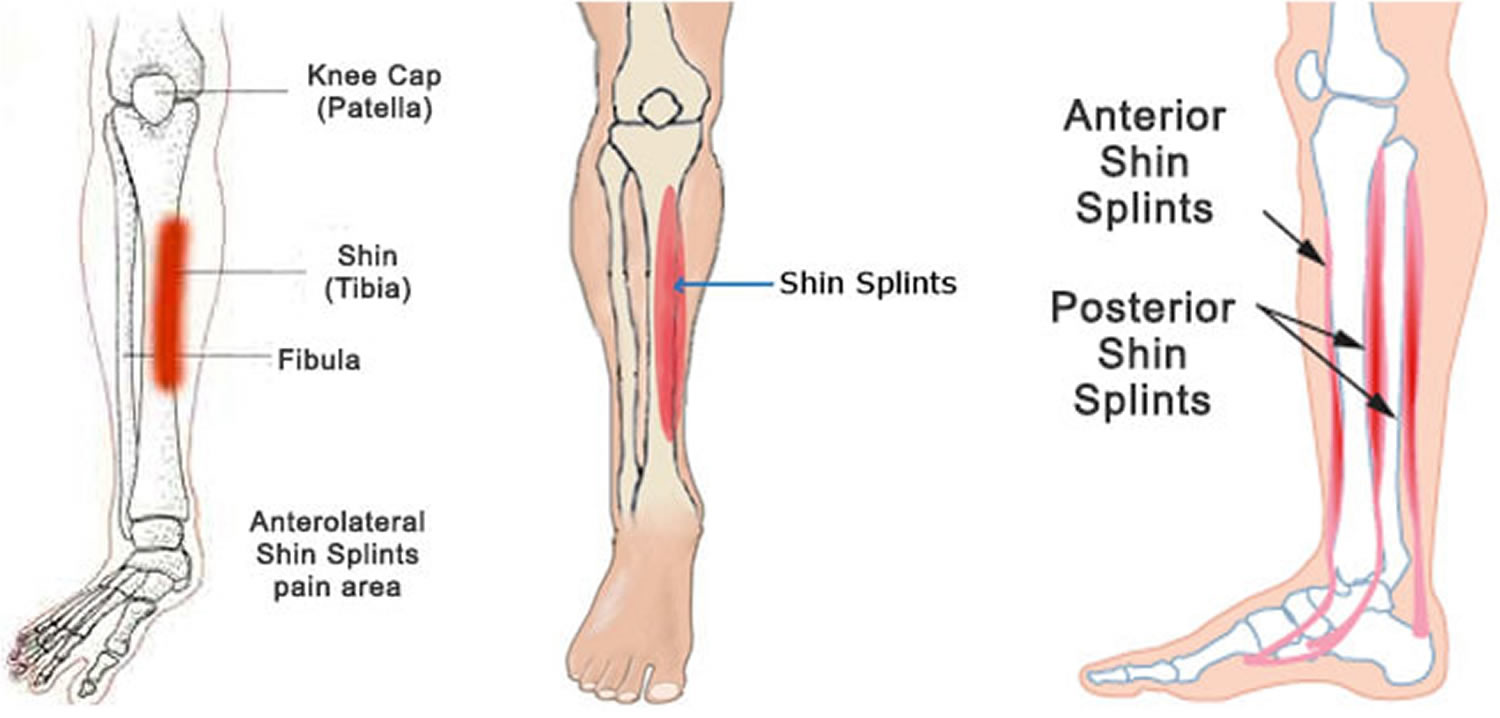
Figure 1. Shin splints
Figure 2. Shin splints
It’s a good idea to see your doctor if your pain doesn’t improve despite the treatments mentioned above.
Your doctor may:
- ask about your symptoms and examine your legs to try to work out what’s causing your pain
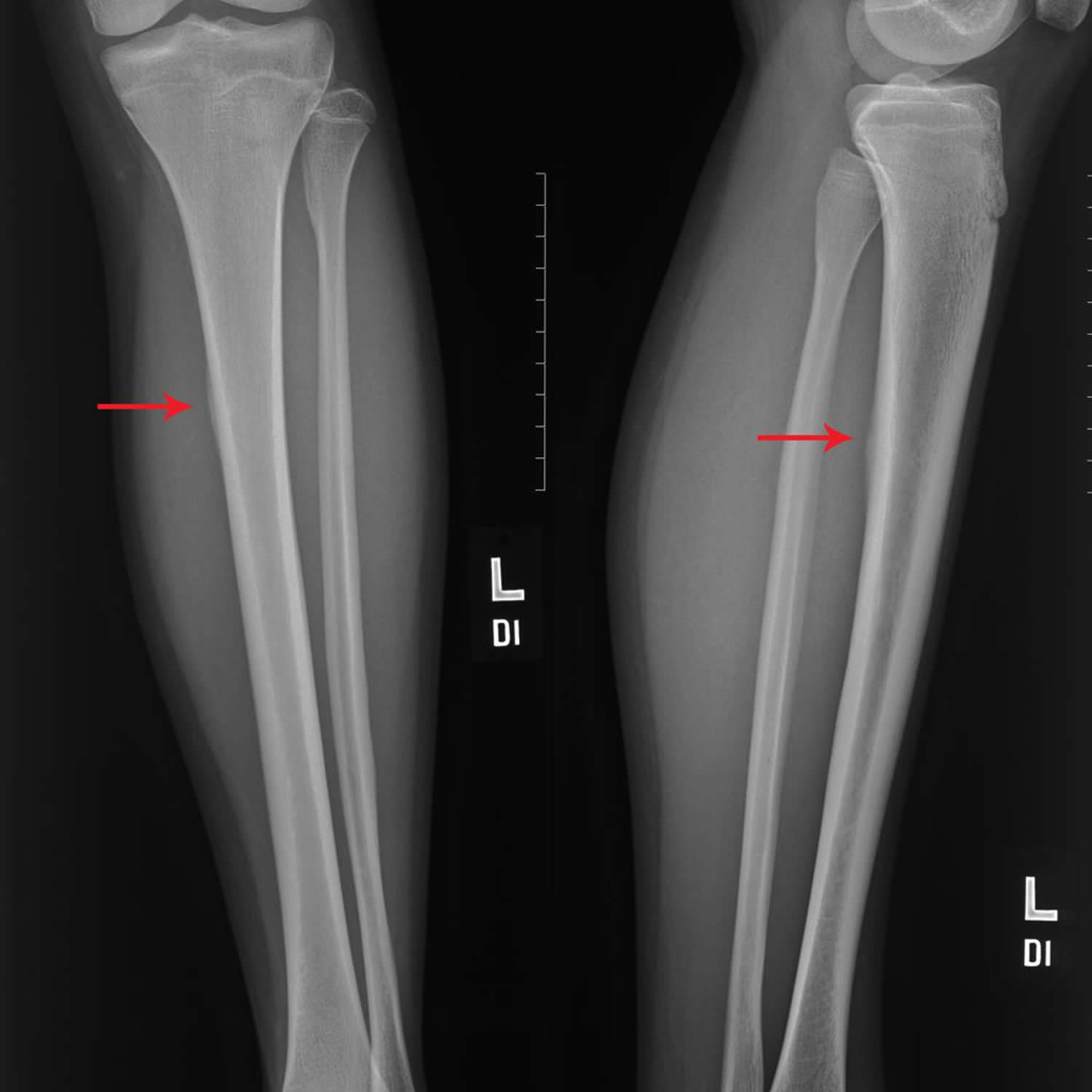
- refer you for an X-ray or special scan of your legs – an X-ray may be normal, so a more detailed scan may be needed to help with diagnosis or identify other causes of lower leg pain
- refer you to a physiotherapist – they can assess your injury, show you some exercises, and recommend a suitable programme of activity
- refer you to an orthopedic surgeon or a consultant in sport and exercise medicine
Fredericson MRI classification of shin splints
In 1995, Fredericson and associates 1 reviewed the MRI findings of 14 athletes with 18 tibial stress injuries and developed a classification system for stress injuries based on the presence of periosteal edema, bone marrow edema, and intracortical signal abnormality. The rationale behind the classification system was to create a standardized method to assess the severity of stress injuries that could assist clinicians in prescribing appropriate rehabilitation for patients with varying levels of injury 1.
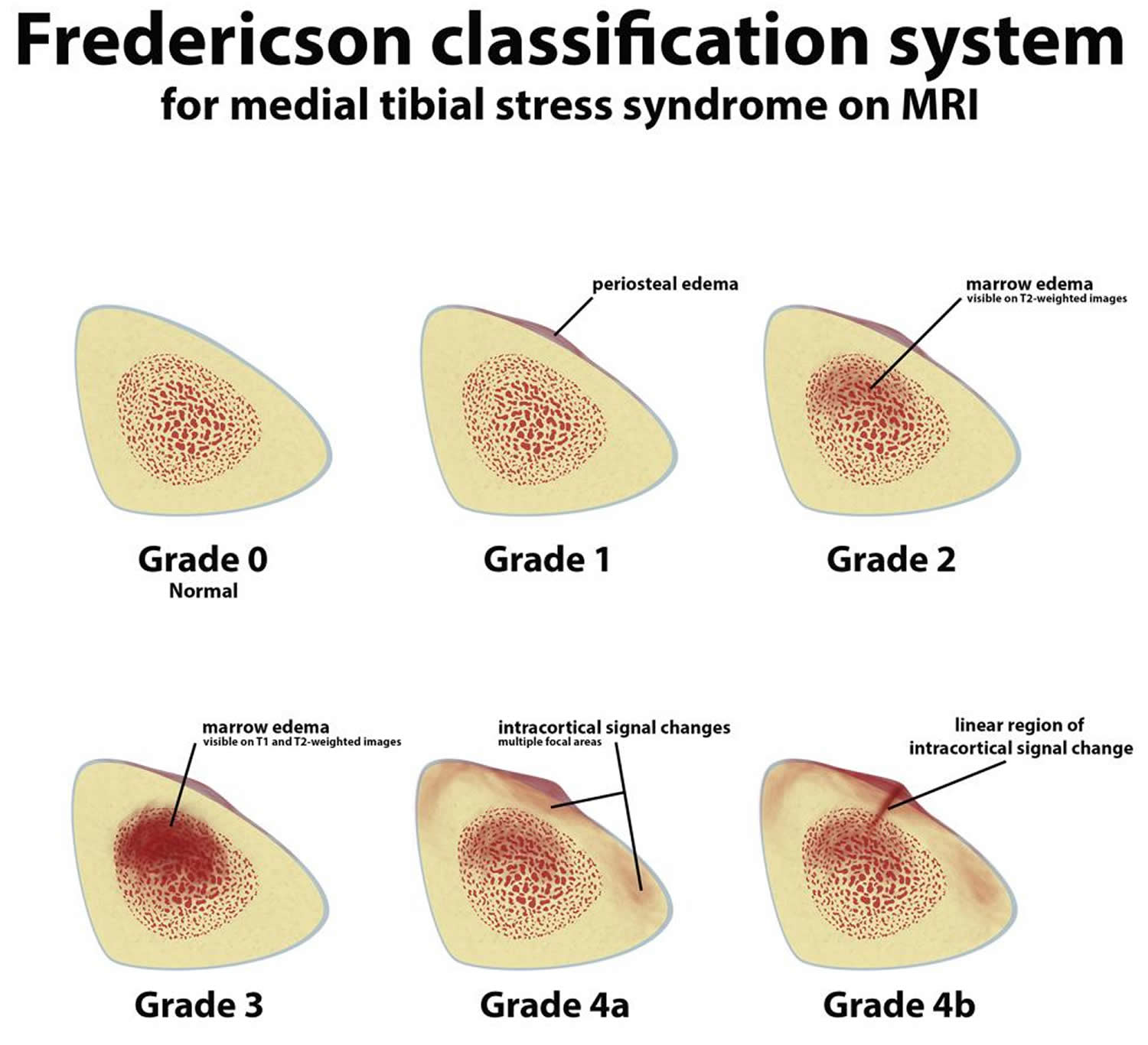
The Fredericson Medial Tibial Stress Syndrome (shin splints) classification follows a progression related to the extent of injury. This begins with periosteal edema (Grade 1), followed by progressive marrow involvement (Grades 2 and 3), and eventually cortical stress fracture (Grades 4a and 4b).
Figure 3. Shin splints (Medial Tibial Stress Syndrome) Fredericson MRI Classification
[Source 1]Figure 4. Shin splints – Grade of Stress Injury
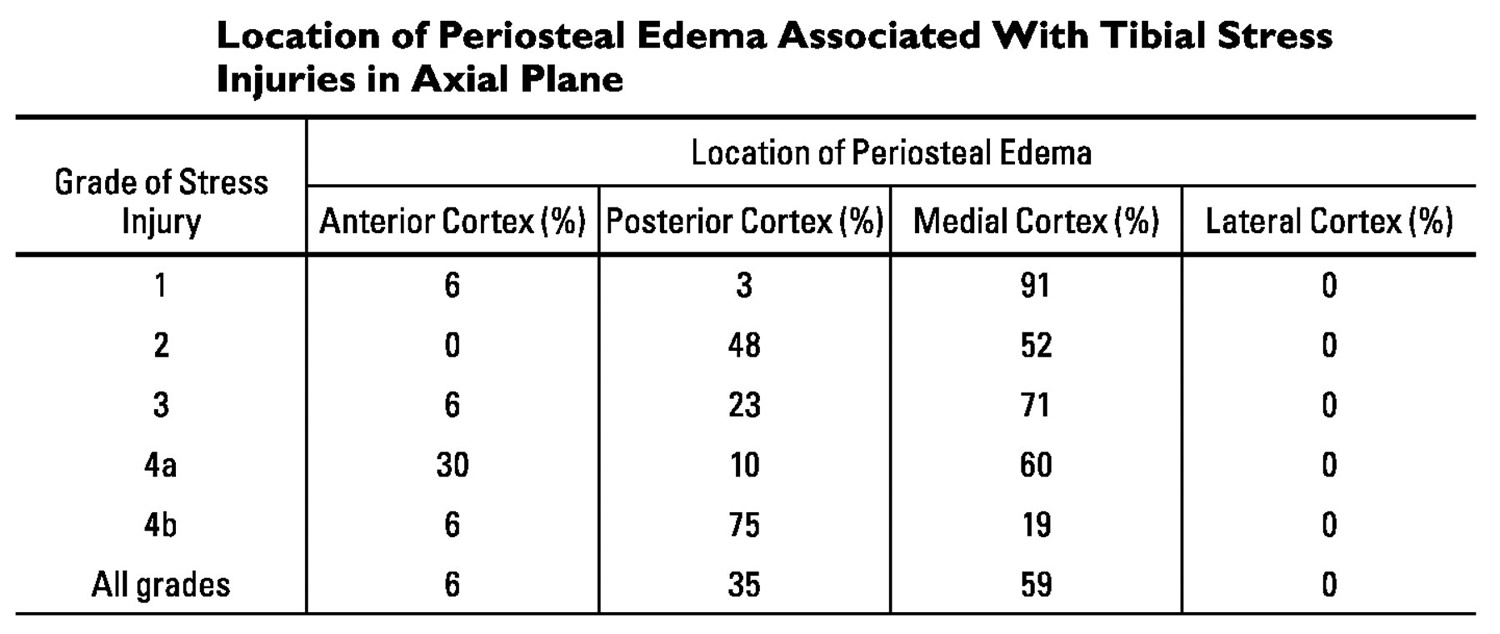 [Source 2]
[Source 2]Fredericson MRI classification of shin splints is an accurate way to correlate the extent of bone involvement with clinical symptoms, which leads to more accurate recommendations for rehab and return to sports activity.
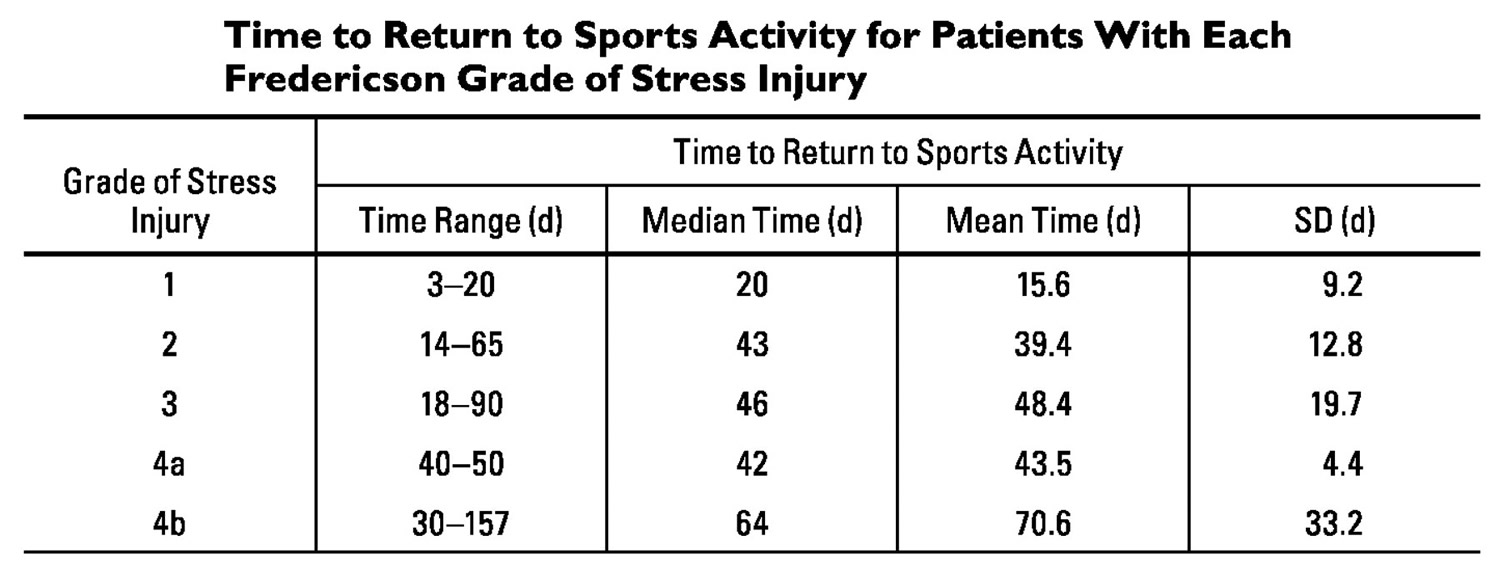
The estimated delay in returning to impact activity based on this classification is 3:
- Grade 1: 2-3 weeks
- Grades 2-4a: 6-7 weeks
- Grade 4b: 9-10 weeks or more
Figure 5. Shin splints time to return to sports activity
Shin splints causes
What causes shin splints
Unfortunately, a consensus hasn’t been reached among health professionals. In general, shin splints develop when the muscle and bone tissue (periosteum) in the leg become overworked by repetitive activity. Shin splints are usually brought on by running or repetitive weight bearing on the legs (e.g. tennis, basketball). It’s thought this leads to swelling (inflammation) of the tissue around the shin bone.
Shin splints often occur after sudden changes in physical activity. These can be changes in frequency, such as increasing the number of days you exercise each week. Changes in duration and intensity, such as running longer distances or on hills, can also cause shin splints.
Several things can increase your chances of getting shin splints, including:
- Having flat feet or abnormally rigid arches
- Exercising with improper or worn-out footwear that don’t cushion and support your feet properly
- A sudden change in your activity level – such as starting a new exercise plan or suddenly increasing the distance or pace you run
- Running on hard or uneven surfaces
- Being overweight
- Having feet that roll inwards (known as over-pronation)
- Having tight calf muscles, weak ankles, or a tight Achilles tendon (the band of tissue connecting the heel to the calf muscle)
Runners are at highest risk for developing shin splints. Dancers and military recruits are two other groups frequently diagnosed with the condition.
Probable causes of shin splints include:
- small tears in the muscle that’s pulled off the bone
- an inflammation of the sheath of the tissue that wraps around the tibia (periosteum)
- an inflammation of the muscle
– or a combination of these
Luckily, they’re all treated similarly!
Other causes of lower leg pain
Pain in the lower legs and shins can also be caused by:
- stress fractures (tiny cracks in the bone) – the pain often affects one leg, but can affect both, and is usually focused in a small area; there may also be some swelling
- a sprain or strain – this can cause swelling, bruising and pain that continues during rest
- a tendon injury – symptoms include pain, stiffness, weakness and a grating or crackling sensation when moving the affected area
- reduced blood supply to the legs (peripheral arterial disease) – this causes an aching pain triggered by physical activity that fades after a few minutes of rest
- swelling of the leg muscle (compartment syndrome) – this can cause cramping pain in the muscles that develops gradually during exercise and fades quickly at rest
Risk factors for shin splints
You’re more at risk of shin splints if:
- You’re a runner, especially one beginning a running program
- You suddenly increase the duration, frequency or intensity of exercise
- You run on uneven terrain, such as hills, or hard surfaces, such as concrete
- You’re in military training
- You have flat feet or high arches
Shin splints prevention
How to prevent shin splints
There are things you can do to prevent shin splints.
- Wear a proper fitting athletic shoe. To get the right fit, determine the shape of your foot using the “wet test.” Step out of the shower onto a surface that will show your footprint, like a brown paper bag. If you have a flat foot, you will see an impression of your whole foot on the paper. If you have a high arch, you will only see the ball and heel of your foot. When shopping, look for athletic shoes that match your particular foot pattern. In addition, make sure you wear shoes designed for your sport. Running long distances in court-type sneakers can contribute to shin splints.
- Run and train on flat, soft surfaces, such as a recreation ground or playing field, whenever possible
- Slowly build your fitness level. Increase the duration, intensity, and frequency of your exercise regimen gradually.
- Cross train. Alternate jogging with lower impact sports like swimming or cycling.
- Barefoot running. In recent years, barefoot running has gained in popularity. Many people claim it has helped to resolve shin splints. Some research indicates that barefoot running spreads out impact stresses among muscles, so that no area is overloaded. However, there is no clear evidence that barefoot running reduces the risk for any injury. Like any significant change in your fitness regimen, a barefoot running program should be started very gradually.
- Begin with short distances to give your muscles and your feet time to adjust. Pushing too far, too fast can put you at risk for stress injuries. In addition, barefoot runners are at increased risk for cuts and bruises on their feet. Several brands of minimalist shoes with “toes” are available and these also require a slow working in period as your body adjusts to this different activity.
- Consider arch supports. Arch supports can help prevent the pain of shin splints, especially if you have flat arches.
- Lose weight if you’re overweight
- Improve your overall strength and flexibility
- Warm up before exercising and stretch after exercising – in particular, stretching your calves and the front of your legs may help
- Analyze your movement. A formal video analysis of your running technique can help to identify movement patterns that can contribute to shin splints. In many cases, a slight change in your running can help decrease your risk.
If your shin splints do not improve after rest and other methods described above, be sure to see a doctor to determine whether something else is causing your leg pain.
Speak to a foot specialist called a podiatrist if you have flat feet or your feet roll inwards. They may recommend supportive inserts for your shoes (orthotics) to reduce the pressure on your shins.
Shin splints symptoms
The most common symptom of shin splints is pain along the border of the shin bones (tibia), which run down the front of your lower legs. Mild swelling in the area may also occur.
Shin splints (medial tibial stress syndrome) causes pain and tenderness along the inside of the lower leg. The pain is usually associated with running, and persists for a period of time after the activity ceases. The pain may improve during the run, but recur towards the end or after the activity finishes. The same process can also occur on the outside edge of the tibia, which is why the problem is sometimes referred to as tenoperiostitis. The area along the edge of the bone, where the muscle attaches to the tibia, will be tender.
The shin splints tends to:
- begin soon after starting exercise
- gradually improve when resting – sometimes the pain may fade while you’re still exercising, but it can eventually become constant and continue even when resting
- be sharp and razor-like or dull and achy to begin with, but may become increasingly sharp or severe and stop you exercising
- affect both shins
- be felt over a large part of the shin (an area over 5cm across) – pain in a small area may be caused by a stress fracture instead
- be aggravated by touching the sore spot
- occur both during and after exercise
Sometimes there may also be some swelling.
Stress Fracture
Stress fracture usually causes localized pain situated at the junction of the upper and middle third of the tibia or the middle and lower third of the bone. The pain in this situation is always with activity and the pain will become progressively worse during a run, and with successive runs. Pain will persist for hours to days afterwards. The bone itself will be tender in this condition.
If your shin splints are not responsive to treatment, your doctor may want to make sure you do not have a stress fracture. A stress fracture is a small crack(s) in the tibia caused by stress and overuse.
Imaging tests that create pictures of anatomy help to diagnose conditions. A bone scan and magnetic resonance imaging (MRI) study will often show stress fractures in the tibia.
Tendinitis
Tendons attach muscles to bones. Tendinitis occurs when tendons become inflamed. This can be painful like shin splints, especially if there is a partial tear of the involved tendon. An MRI can help diagnose tendinitis.
Chronic Exertional Compartment Syndrome
An uncommon condition called chronic exertional compartment syndrome causes symptoms like shin splints. Chronic exertional compartment syndrome is a painful condition that occurs when pressure within the leg muscles builds to dangerous levels that is brought on by exercise. Symptoms of compartment syndrome are leg pain, tightness or burning, with sensations such as tingling or pins and needles. The pain will build up during a run, to the point where the person has to stop. On stopping exercise, the severe pain goes away within a few minutes, but a residual ache persists.
The tests used to diagnose this condition involve measuring the pressure within the leg compartments before and after exercise.
Shin splints diagnosis
After discussing your symptoms and medical history, your doctor will examine your lower leg. An accurate diagnosis is very important. Sometimes, other problems may exist that can have an impact on healing.
A “one-leg hop test” is a functional test, that can be used to distinguish between shin splints and a stress fracture: a patient with shin splints can hop at least 10 times on the affected leg where a patient with a stress fracture cannot hop without severe pain.
Your doctor may order additional imaging tests to rule out other shin problems. Several conditions can cause shin pain, including stress fractures, tendinitis, and chronic exertional compartment syndrome.
MRI scan is the most sensitive radiological examination (~88%) 4. It may demonstrate a spectrum of findings ranging from normal to periosteal fluid to marrow edema to actual stress fracture 5. The anterior cortex (+/- posterior cortex) is most commonly affected 4.
These findings are graded using the Fredericson classification system as follows 6:
- Grade 1: Periosteal edema only
- Grade 2: bone marrow edema appreciated only on T2-weighted sequences
- Grade 3: bone marrow edema appreciated on both T1 and T2-weighted sequences
- Grade 4:
- 4a: multiple discrete areas of intracortical signal changes
- 4b: linear area(s) of intracortical signal change correlating with a frank stress fracture
Bone scintigraphy is relatively sensitive (~74%) 4 and may demonstrate high uptake in the affected region, characteristically along the posterior tibial aspect on lateral views.
Shin splints treatment
How to get rid of shin splints
Nonsurgical Treatment
- Rest. Because shin splints are typically caused by overuse, standard treatment includes several weeks of rest from the activity that caused the pain. Lower impact types of aerobic activity can be substituted during your recovery, such as swimming, using a stationary bike, or an elliptical trainer.
- Non-steroidal anti-inflammatory medicines. Drugs like ibuprofen, aspirin, and naproxen reduce pain and swelling.
- Ice. Use cold packs for 20 minutes at a time, several times a day. Do not apply ice directly to the skin.
- Compression. Wearing an elastic compression bandage may prevent additional swelling.
- Flexibility exercises. Stretching your lower leg muscles may make your shins feel better.
- Supportive shoes. Wearing shoes with good cushioning during daily activities will help reduce stress in your shins.
- Orthotics. People who have flat feet or recurrent problems with shin splints may benefit from orthotics. Shoe inserts can help align and stablize your foot and ankle, taking stress off of your lower leg. Orthotics can be custom-made for your foot, or purchased “off the shelf.”
- Return to exercise. Shin splints usually resolve with rest and the simple treatments described above. Before returning to exercise, you should be pain-free for at least 2 weeks. Keep in mind that when you return to exercise, it must be at a lower level of intensity. You should not be exercising as often as you did before, or for the same length of time.
Be sure to warm up and stretch thoroughly before you exercise. Increase training slowly. If you start to feel the same pain, stop exercising immediately. Use a cold pack and rest for a day or two. Return to training again at a lower level of intensity. Increase training even more slowly than before.
Surgical Treatment
Very few people need surgery for shin splints. Surgery has been done in very severe cases that do not respond to nonsurgical treatment. However, it is not clear how effective surgery is.
References- Fredericson M, Bergman AG, Hoffman KL, Dillingham MS. Tibial stress reaction in runners: correlation of clinical symptoms and scintigraphy with a new magnetic resonance imaging grading system. Am J Sports Med 1995; 23:472–481 http://journals.sagepub.com/doi/pdf/10.1177/036354659502300418
- Kijowski R, Choi J, Shinki K et-al. Validation of MRI classification system for tibial stress injuries. AJR Am J Roentgenol. 2012;198 (4): 878-84. AJR Am J Roentgenol – doi:10.2214/AJR.11.6826 https://www.ajronline.org/doi/full/10.2214/AJR.11.6826
- Kijowski R, Choi J, Shinki K et-al. Validation of MRI classification system for tibial stress injuries. AJR Am J Roentgenol. 2012;198 (4): 878-84. AJR Am J Roentgenol. doi:10.2214/AJR.11.6826 https://www.ajronline.org/doi/full/10.2214/AJR.11.6826
- Gaeta M, Minutoli F, Scribano E et-al. CT and MR imaging findings in athletes with early tibial stress injuries: comparison with bone scintigraphy findings and emphasis on cortical abnormalities. Radiology. 2005;235 (2): 553-61. doi:10.1148/radiol.2352040406 https://www.ncbi.nlm.nih.gov/pubmed/15858094
- Anderson MW, Ugalde V, Batt M et-al. Shin splints: MR appearance in a preliminary study. Radiology. 1997;204 (1): 177-80. https://www.ncbi.nlm.nih.gov/pubmed/9205242
- Kijowski R, Choi J, Shinki K et-al. Validation of MRI classification system for tibial stress injuries. AJR Am J Roentgenol. 2012;198 (4): 878-84. doi:10.2214/AJR.11.6826 https://www.ajronline.org/doi/full/10.2214/AJR.11.6826