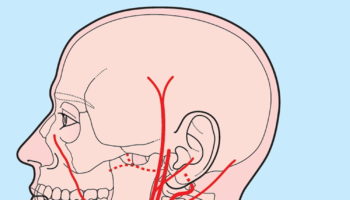
Human heart
Your heart is a strong muscle about the size of the palm of your hand. Your body depends on the heart’s pumping action to deliver oxygen- and nutrient-rich blood to the body’s cells. When the cells are nourished properly, the body can function normally. Just like an engine makes a car go, the heart keeps your body running. The heart has two pumps. The stronger pump uses arteries to send blood with oxygen away from the heart, throughout the body. The other pump uses veins to bring blood back to the heart and sends it to the lungs to get more oxygen. An electrical system in the heart controls the heart’s pumps (the heart beat or pulse).
How the Heart Works
The heart has two sides, separated by an inner wall called the septum. The right side of the heart pumps blood to the lungs to pick up oxygen. The left side of the heart receives the oxygen-rich blood from the lungs and pumps it to the body.
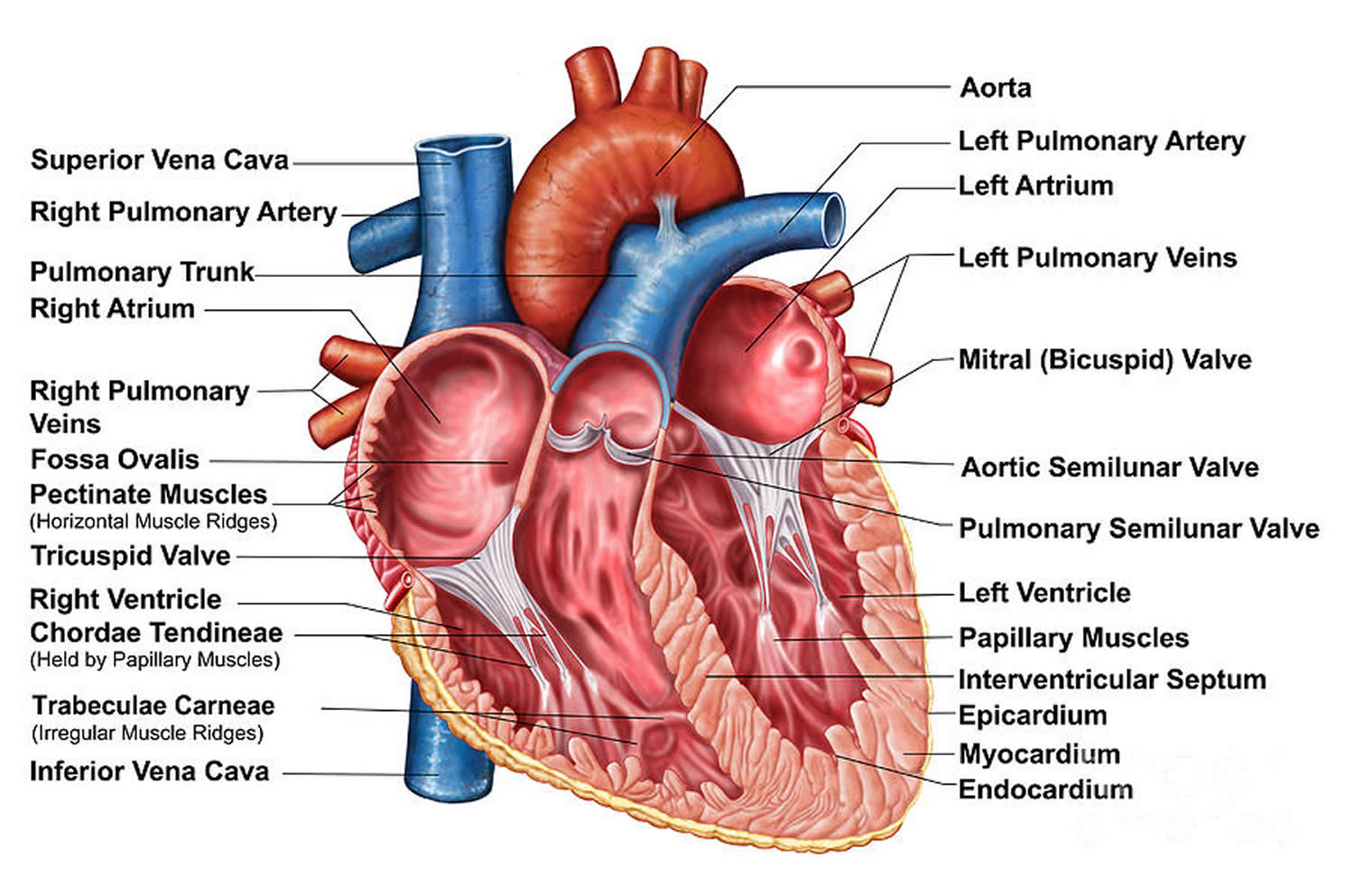
The heart has four chambers 1, two on the right and two on the left:
- Two upper chambers are called atrium (two is called an atria). The atria collect blood as it flows into the heart.
- Two lower chambers are called ventricles. The ventricles pump blood out of the heart to the lungs or other parts of the body.
The heart also has four valves that open and close to let blood flow from the atria to the ventricles and from the ventricles into the two large arteries connected to the heart in only one direction when the heart contracts (beats). The four heart valves are:
- Tricuspid valve, located between the right atrium and right ventricle
- Pulmonary or pulmonic valve, between the right ventricle and the pulmonary artery. This artery carries blood from the heart to the lungs.
- Mitral valve, between the left atrium and left ventricle
- Aortic valve, between the left ventricle and the aorta. This aorta carries blood from the heart to the body.
Each valve has a set of flaps (also called leaflets or cusps). The mitral valve has two flaps; the others have three. Valves are like doors that open and close. They open to allow blood to flow through to the next chamber or to one of the arteries. Then they shut to keep blood from flowing backward. Blood flow occurs only when there’s a difference in pressure across the valves, which causes them to open. Under normal conditions, the valves permit blood to flow in only one direction.
The heart four chambers and four valves and is connected to various blood vessels. Veins are blood vessels that carry blood from the body to the heart. Arteries are blood vessels that carry blood away from the heart to the body.
The heart pumps blood to the lungs and to all the body’s tissues by a sequence of highly organized contractions of the four chambers. For the heart to function properly, the four chambers must beat in an organized way.
When the heart’s valves open and close, they make a “lub-DUB” sound that a doctor can hear using a stethoscope 2.
- The first sound—the “lub”—is made by the mitral and tricuspid valves closing at the beginning of systole. Systole is when the ventricles contract, or squeeze, and pump blood out of the heart.
- The second sound—the “DUB”—is made by the aortic and pulmonary valves closing at the beginning of diastole. Diastole is when the ventricles relax and fill with blood pumped into them by the atria.
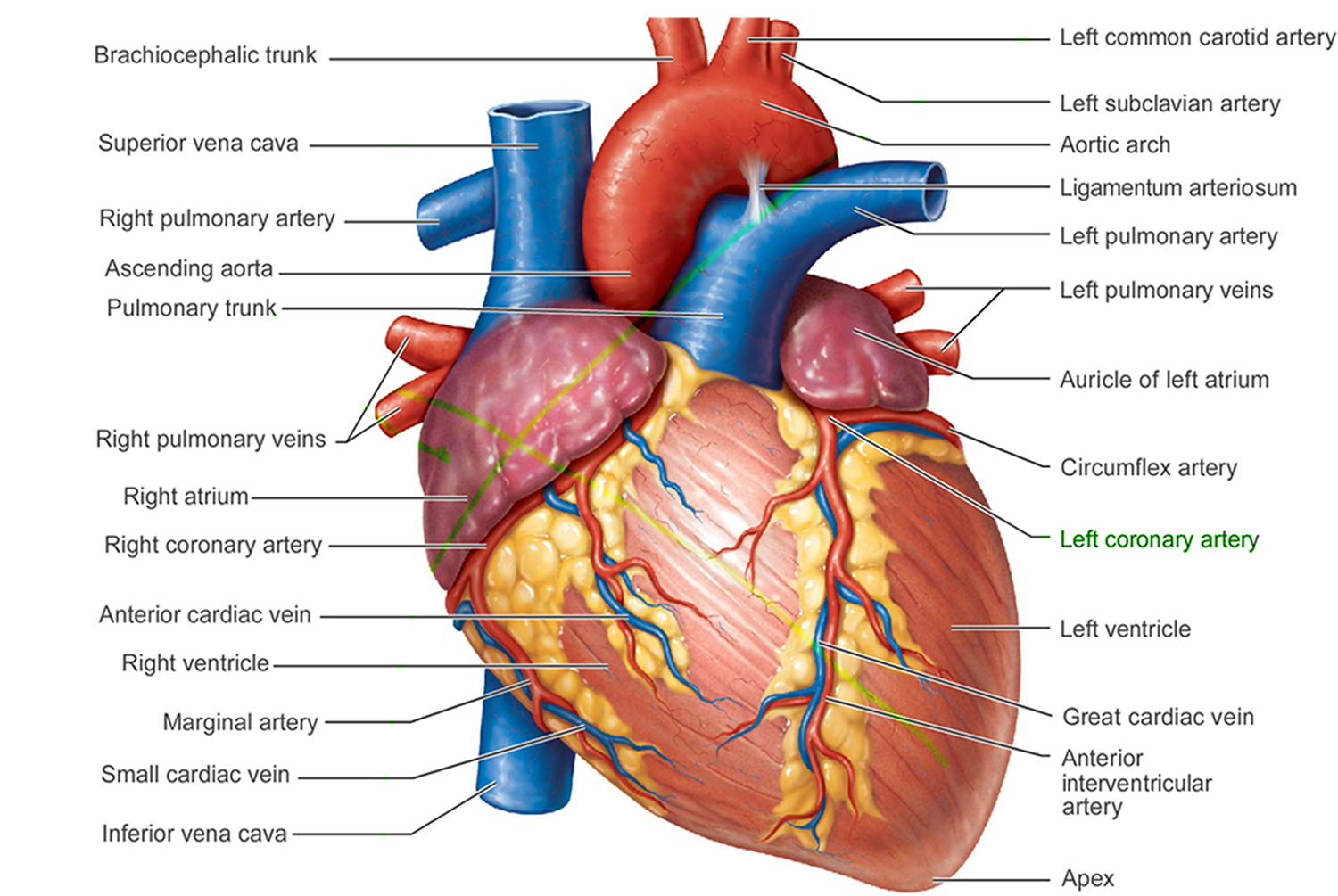
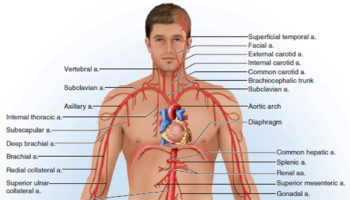
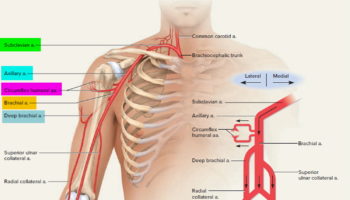
Arteries
The arteries are major blood vessels connected to your heart.
- The pulmonary artery carries blood from the right side of the heart to the lungs to pick up a fresh supply of oxygen.
- The aorta is the main artery that carries oxygen-rich blood from the left side of the heart to the body.
- The coronary arteries are the other important arteries attached to the heart. They carry oxygen-rich blood from the aorta to the heart muscle, which must have its own blood supply to function.
Veins
The veins also are major blood vessels connected to your heart.
- The pulmonary veins carry oxygen-rich blood from the lungs to the left side of the heart so it can be pumped to the body.
- The superior and inferior vena cavae are large veins that carry oxygen-poor blood from the body back to the heart.
Blood Flow
- The Right Side of Your Heart
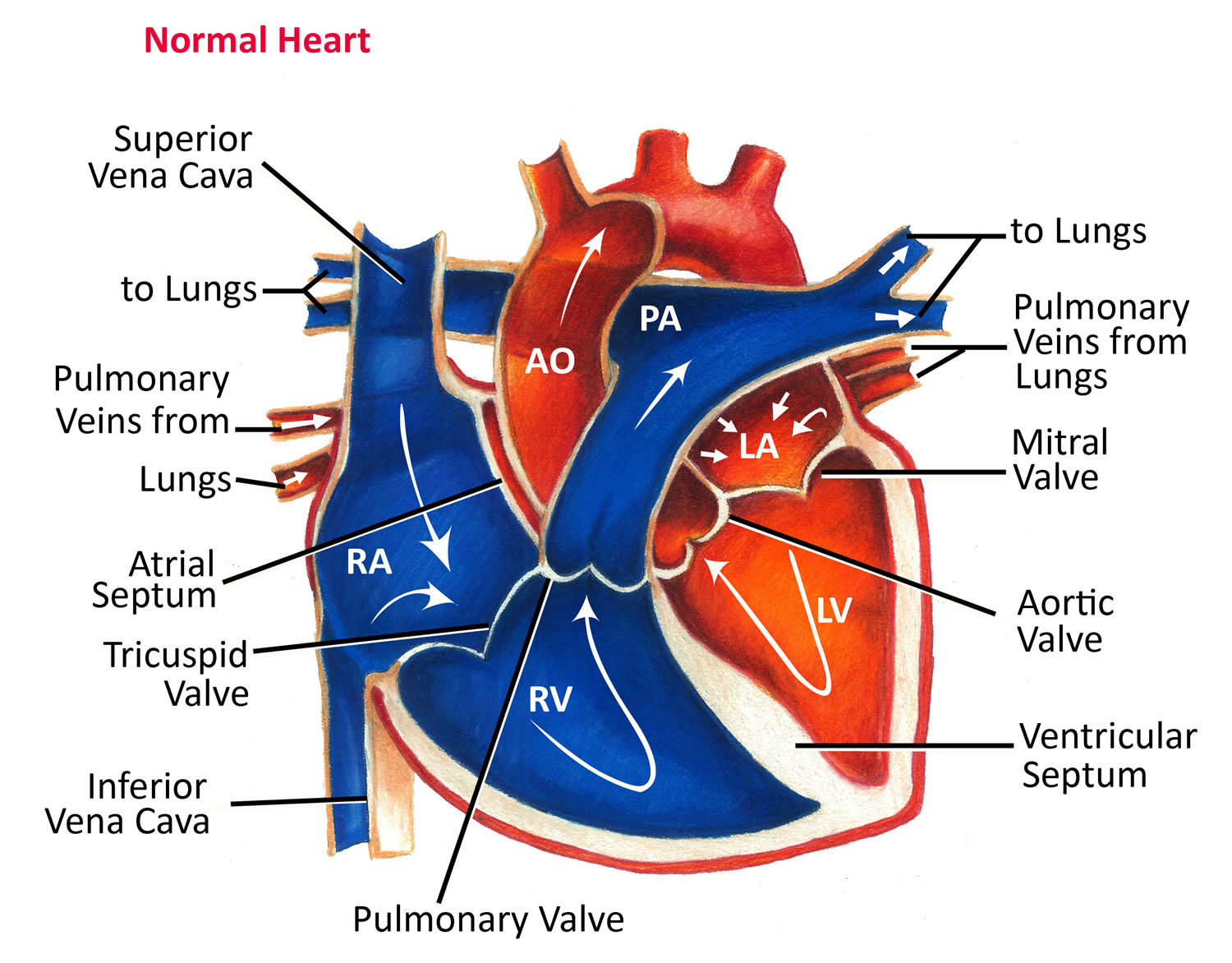
In figure 3 above, the superior and inferior vena cavae are shown in blue to the left of the heart muscle as you look at the picture. These veins are the largest veins in your body.
After your body’s organs and tissues have used the oxygen in your blood, the vena cavae carry the oxygen-poor blood back to the right atrium of your heart.
The superior vena cava carries oxygen-poor blood from the upper parts of your body, including your head, chest, arms, and neck. The inferior vena cava carries oxygen-poor blood from the lower parts of your body.
The oxygen-poor blood from the vena cavae flows into your heart’s right atrium. From the right atrium, blood is pumped into the right ventricle. And then from the right ventricle, blood is pumped to your lungs through the pulmonary arteries (shown in blue in the center of figure 3).
Once in the lungs, the blood travels through many small, thin blood vessels called capillaries. There, the blood picks up more oxygen and transfers carbon dioxide to the lungs—a process called gas exchange.
The oxygen-rich blood passes from your lungs back to your heart through the pulmonary veins (shown in red to the left of the right atrium in figure 3).
- The Left Side of Your Heart
Oxygen-rich blood from your lungs passes through the pulmonary veins (shown in red to the right of the left atrium in figure 3 above). The blood enters the left atrium and is pumped into the left ventricle.
From the left ventricle, the oxygen-rich blood is pumped to the rest of your body through the aorta. The aorta is the main artery that carries oxygen-rich blood to your body.
Like all of your organs, your heart needs oxygen-rich blood. As blood is pumped out of your heart’s left ventricle, some of it flows into the coronary arteries (shown in red in figure 3).
Your coronary arteries are located on your heart’s surface at the beginning of the aorta. They carry oxygen-rich blood to all parts of your heart.
For the heart to work well, your blood must flow in only one direction. Your heart’s valves make this possible. Both of your heart’s ventricles have an “in” (inlet) valve from the atria and an “out” (outlet) valve leading to your arteries.
Healthy valves open and close in exact coordination with the pumping action of your heart’s atria and ventricles. Each valve has a set of flaps called leaflets or cusps that seal or open the valve. This allows blood to pass through the chambers and into your arteries without backing up or flowing backward.
Figure 1. The anatomy of the heart
Figure 2. The anatomy of the heart chambers
Figure 3. Normal heart blood flow
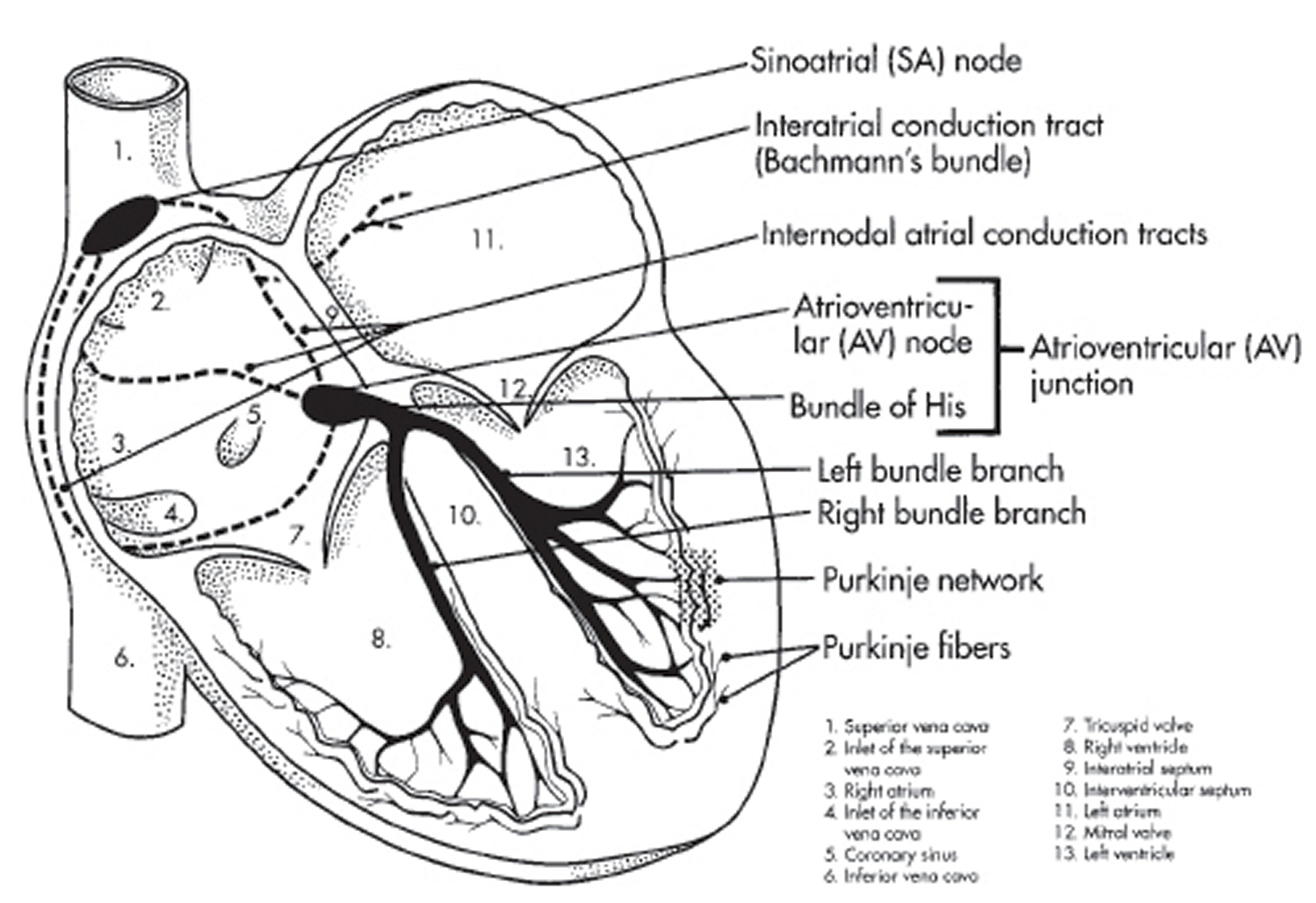
The Heart’s Electrical System
The heart’s electrical system controls the rate and rhythm of the heartbeat.
With each heartbeat, an electrical signal spreads from the top of the heart to the bottom. As the signal travels, it causes the heart to contract and pump blood.
Your heart’s electrical system controls all the events that occur when your heart pumps blood 3. The electrical system also is called the cardiac conduction system. If you’ve ever seen the heart test called an EKG (electrocardiogram), you’ve seen a graphical picture of the heart’s electrical activity.
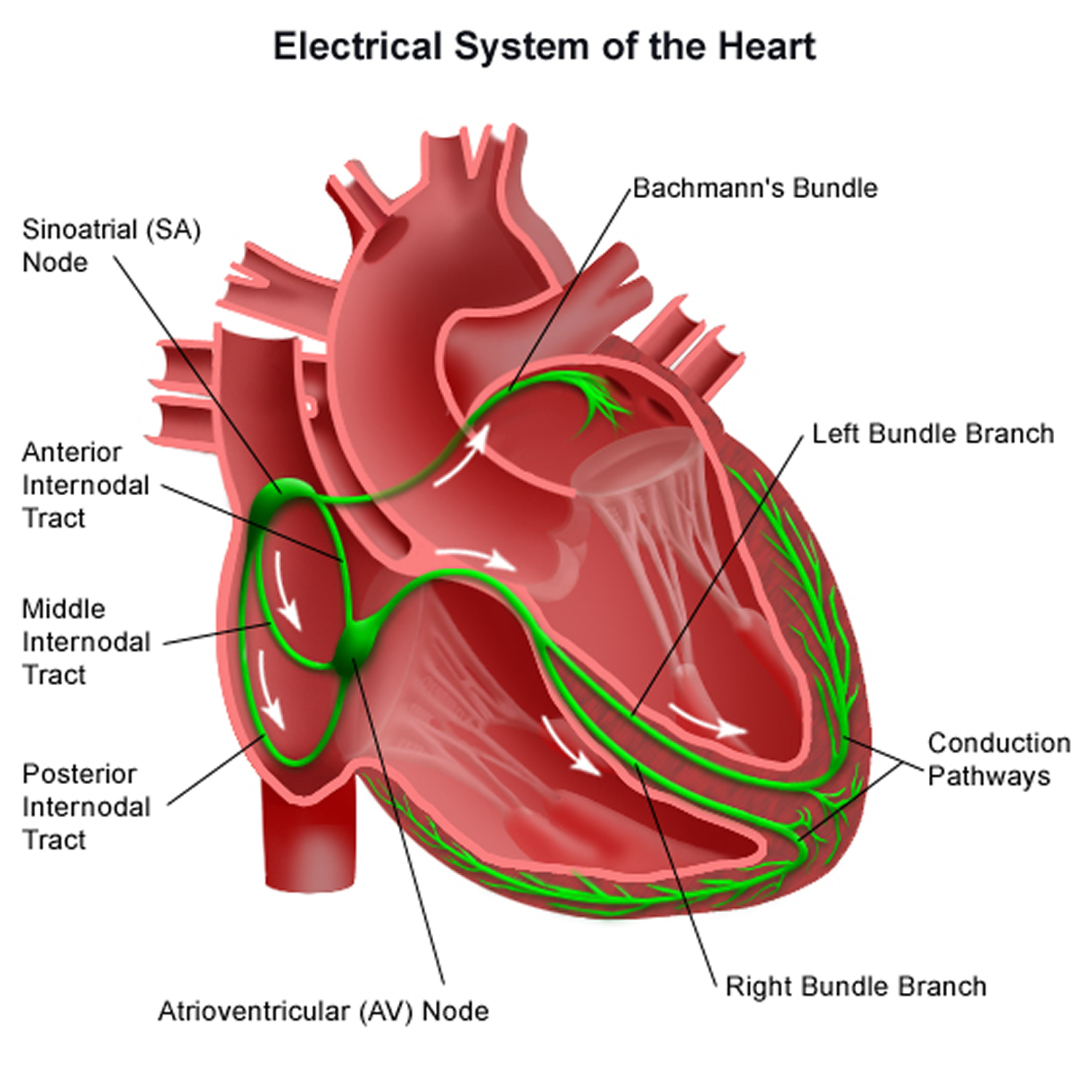
Your heart’s electrical system is made up of three main parts:
- The Sinoatrial (SA) node, located in the right atrium of your heart
- The Atrioventricular (AV) node, located on the interatrial septum close to the tricuspid valve
- The His-Purkinje system, located along the walls of your heart’s ventricles
A heartbeat is a complex series of events. These events take place inside and around your heart. A heartbeat is a single cycle in which your heart’s chambers relax and contract to pump blood. This cycle includes the opening and closing of the inlet and outlet valves of the right and left ventricles of your heart.
Each heartbeat has two basic parts: diastole and systole. During diastole, the atria and ventricles of your heart relax and begin to fill with blood.
At the end of diastole, your heart’s atria contract (atrial systole) and pump blood into the ventricles. The atria then begin to relax. Your heart’s ventricles then contract (ventricular systole), pumping blood out of your heart.
Each electrical signal begins in a group of cells called the sinus node or sinoatrial (SA) node. The SA node is located in the heart’s upper right chamber, the right atrium. In a healthy adult heart at rest, the SA node fires off an electrical signal to begin a new heartbeat 60 to 100 times a minute. In a normal, healthy heart, each beat begins with a signal from the SA node. This is why the SA node sometimes is called your heart’s natural pacemaker. Your pulse, or heart rate, is the number of signals the SA node produces per minute.
The signal is generated as the vena cavae fill your heart’s right atrium with blood from other parts of your body. The signal spreads across the cells of your heart’s right and left atria.
From the SA node, the electrical signal travels through special pathways in the right and left atria. This causes the atria to contract and pump blood through the open valves from the atria into heart’s two lower chambers, the ventricles.
The electrical signal then moves down to a group of cells called the atrioventricular (AV) node, located between the atria and the ventricles. Here, the signal slows down just a little, allowing your heart’s right and left ventricles time to finish filling with blood.
The electrical signal then leaves the AV node and travels along a pathway called the bundle of His. This pathway divides into a right bundle branch and a left bundle branch. The signal goes down these branches to the ventricles, causing them to contract and pump blood to the lungs and the rest of the body.
From the bundle of His, the signal fibers divide into left and right bundle branches through the Purkinje fibers. These fibers connect directly to the cells in the walls of your heart’s left and right ventricles.
The signal spreads across the cells of your ventricle walls, and both ventricles contract. However, this doesn’t happen at exactly the same moment.
The left ventricle contracts an instant before the right ventricle. This pushes blood through the pulmonary valve (for the right ventricle) to your lungs, and through the aortic valve (for the left ventricle) to the rest of your body.
As the signal passes, the walls of the ventricles relax and await the next signal.
This process continues over and over as the atria refill with blood and more electrical signals come from the SA node.
A problem with any part of this process can cause an arrhythmia. For example, in atrial fibrillation, a common type of arrhythmia, electrical signals travel through the atria in a fast and disorganized way. This causes the atria to quiver instead of contract.
Figure 4. The heart’s electrical system
How to keep your heart healthy
Heart disease also called cardiovascular disease, is the number one killer in the U.S. Heart disease is also a major cause of disability. The most common cause of heart disease is narrowing or blockage of your coronary arteries also called coronary artery disease, the coronary arteries are the blood vessels that supply blood to your heart. A buildup of fatty deposits or plaques in your arteries (also known as atherosclerosis) is the most common cause of coronary artery disease. Atherosclerosis is not part of normal aging and can be serious. Unhealthy lifestyle habits, such as a poor diet, lack of exercise, being overweight and smoking, can lead to atherosclerosis. Coronary artery disease happens slowly over time. It’s the major reason people have heart attacks. Other kinds of heart problems may happen to the valves in the heart or the heart may not pump well and cause heart failure. Some people are born with heart disease also known as congenital heart disease.
Heart disease describes a range of conditions that affect your heart. Heart diseases include:
- Blood vessel disease, such as coronary artery disease
- Heart rhythm problems (arrhythmias)
- Heart defects you’re born with (congenital heart defects)
- Heart valve disease
- Disease of the heart muscle
- Heart infection
Many forms of heart disease can be prevented or treated with healthy lifestyle choices.
Risk factors are conditions or habits that increase your risk of developing a disease. The following are risk factors that can increase your chance of developing heart disease and cardiovascular disease:
- High blood cholesterol (hypercholesterolemia). High levels of cholesterol in your blood can increase the risk of plaque formation and atherosclerosis.
- High blood pressure (hypertension). Uncontrolled high blood pressure can result in hardening and thickening of your arteries, narrowing the vessels through which blood flows. Blood pressure is considered high if it stays at or above 140/90 mmHg over time. If you have diabetes or chronic kidney disease, high blood pressure is defined as 130/80 mmHg or higher. (The mmHg is millimeters of mercury—the units used to measure blood pressure.)
- Diabetes. Diabetes increases your risk of heart disease. Both conditions share similar risk factors, such as obesity and high blood pressure.
- Insulin resistance. This condition occurs if the body can’t use its own insulin properly. Insulin is a hormone that helps move blood sugar into cells where it’s used for energy. Insulin resistance may lead to diabetes.
- Obesity or being overweight. Excess weight typically worsens other heart disease risk factors.
- Metabolic syndrome. Metabolic syndrome is the name for a group of risk factors that raises your risk for coronary heart disease and other health problems, such as diabetes and stroke.
- Smoking. Nicotine tightens your blood vessels, and carbon monoxide can damage their inner lining, making them more susceptible to atherosclerosis. Heart attacks are more common in smokers than in nonsmokers.
- Poor diet. A diet that’s high in fat, salt, sugar and cholesterol can contribute to the development of heart disease. A healthy diet can help reduce your risk of developing coronary heart disease and stop you gaining weight, reducing your risk of diabetes and high blood pressure.
- Physical inactivity. Lack of exercise also is associated with many forms of heart disease and some of its other risk factors as well.
- Ethnicity
- Family history. A family history of heart disease increases your risk of coronary artery disease, especially if a parent developed it at an early age (before age 55 for a male relative, such as your brother or father, and 65 for a female relative, such as your mother or sister).
- Air pollution. Air pollution is harmful to your heart and circulation. Research shows that air pollution can affect your heart and circulation by:
- damaging the inside walls of your blood vessels, causing them to become narrower and harder
- restricting the movement of your blood vessels, which can increase your blood pressure and add to the strain on your heart
- making your blood more likely to clot
- affecting the normal electrical functioning of your heart which could cause abnormal heart rhythms
- causing small changes to the structure of your heart like those that are seen in the early stages of heart failure.
- This damage can contribute to the development of new health problems, or put people with existing heart and circulatory conditions at increased risk of events like a heart attack or stroke.
- Poor dental health. It’s important to brush and floss your teeth and gums often, and have regular dental checkups. If your teeth and gums aren’t healthy, germs can enter your bloodstream and travel to your heart, causing endocarditis.
- Stress. Unrelieved stress may damage your arteries and worsen other risk factors for heart disease. Research suggests that an emotionally upsetting event, particularly one involving anger, can serve as a trigger for a heart attack or angina in some people. Stress can contribute to high blood pressure and other heart disease risk factors. Some of the ways people cope with stress—drinking alcohol, using other substances, smoking, or overeating—are not healthy ways to manage stress.
- Drug abuse
- Excessive use of alcohol or caffeine. Heavy drinking can damage the heart muscle and worsen other coronary heart disease risk factors. Men should have no more than two drinks containing alcohol a day. Women should have no more than one drink containing alcohol a day.
- Age. Growing older increases your risk of damaged and narrowed arteries and a weakened or thickened heart muscle. Genetic or lifestyle factors cause plaque to build up in your arteries as you age. In men, the risk for coronary heart disease increases starting at age 45. In women, the risk for coronary heart disease increases starting at age 55.
- Sex. Men are generally at greater risk of heart disease. The risk for women increases after menopause.
- Preeclampsia. Preeclampsia (high blood pressure during pregnancy) can occur during pregnancy. The two main signs of preeclampsia are a rise in blood pressure and excess protein in the urine. Preeclampsia is linked to an increased lifetime risk of heart disease, including coronary heart disease, heart attack, heart failure, and high blood pressure. Preeclampsia (high blood pressure during pregnancy) is a risk factor that you can’t control. However, if you’ve had the condition, you should take extra care to monitor your blood pressure and try to lower other heart disease risk factors.
- Mental health problems. Some common mental health conditions include:
- Depression, which is a long-lasting low mood disorder
- Anxiety disorders such as social anxiety disorder, phobias and post-traumatic stress disorder (PTSD)
- Personality disorders such as paranoia, borderline personality disorder and obsessive-compulsive disorder (OCD)
- Bipolar disorder (BPD), previously called manic depression, which causes extreme and unpredictable mood changes
- Psychosis and schizophrenia, which is when a person experiences an altered state of reality
The good news is many heart and cardiovascular diseases are caused by risk factors that can be controlled, treated or modified.
Complications of heart disease include:
- Heart failure. One of the most common complications of heart disease, heart failure occurs when your heart can’t pump enough blood to meet your body’s needs. Heart failure can result from many forms of heart disease, including heart defects, cardiovascular disease, valvular heart disease, heart infections or cardiomyopathy.
- Heart attack. A blood clot blocking the blood flow through a blood vessel that feeds the heart causes a heart attack, possibly damaging or destroying a part of the heart muscle. Atherosclerosis can cause a heart attack.
- Stroke. The risk factors that lead to cardiovascular disease can also lead to an ischemic stroke, which happens when the arteries to your brain are narrowed or blocked so that too little blood reaches your brain. A stroke is a medical emergency — brain tissue begins to die within just a few minutes of a stroke.
- Aneurysm. A serious complication that can occur anywhere in your body, an aneurysm is a bulge in the wall of your artery. If an aneurysm bursts, you may face life-threatening internal bleeding.
- Peripheral artery disease. When you develop peripheral artery disease, your extremities — usually your legs — don’t receive enough blood flow. This causes symptoms, most notably leg pain when walking (claudication). Atherosclerosis also can lead to peripheral artery disease.
- Sudden cardiac arrest. Sudden cardiac arrest is the sudden, unexpected loss of heart function, breathing and consciousness, often caused by an arrhythmia. Sudden cardiac arrest is a medical emergency. If not treated immediately, it results in sudden cardiac death.
You can help reduce your risk of heart disease by taking steps to control factors that put you at greater risk:
- Control your blood pressure. Ask your doctor for a blood pressure measurement at least every two years. He or she may recommend more frequent measurements if your blood pressure is higher than normal or you have a history of heart disease. Optimal blood pressure is less than 120 systolic and 80 diastolic, as measured in millimeters of mercury (mm Hg).
- Lower your cholesterol. Ask your doctor for a baseline cholesterol test when you’re in your 20s and then at least every five years. You may need to start testing earlier if high cholesterol is in your family. If your test results aren’t within desirable ranges, your doctor may recommend more-frequent measurements. Most people should aim for a low-density lipoprotein (LDL or “bad” cholesterol) level below 130 milligrams per deciliter (mg/dL), or 3.4 millimoles per liter (mmol/L). If you have other risk factors for heart disease, you should aim for an LDL level below 100 mg/dL (2.6 mmol/L). If you’re at very high risk of heart disease — if you’ve already had a heart attack or have diabetes, for example — aim for an LDL level below 70 mg/dL (1.8 mmol/L).
- Keep diabetes under control. If you have diabetes, tight blood sugar control can help reduce the risk of heart disease.
- Don’t smoke. Smoking is a major risk factor for heart disease, especially atherosclerosis. One of the best things you can do for your heart is to stop smoking or using smokeless tobacco. Quitting is the best way to reduce your risk of heart disease and its complications. Even if you’re not a smoker, be sure to avoid secondhand smoke. Chemicals in tobacco can damage your heart and blood vessels. Cigarette smoke reduces the oxygen in your blood, which increases your blood pressure and heart rate because your heart has to work harder to supply enough oxygen to your body and brain. There’s good news though. Your risk of heart disease starts to drop in as little as a day after quitting. After a year without cigarettes, your risk of heart disease drops to about half that of a smoker. No matter how long or how much you smoked, you’ll start reaping rewards as soon as you quit.
- Don’t drink or limit your alcohol intake. Alcohol can cause abnormal heart rhythms, high blood pressure, damage to your heart muscle and other diseases such as stroke, liver problems and some cancers. Alcohol is also high in calories so it can lead to weight gain. It also lowers your inhibitions which might mean you find it harder to stick to your healthy eating plans when you have been drinking. If you are trying to lose weight, cut down on alcohol. Drinking more than the recommended amount of alcohol can have a harmful effect on your heart and general health.
- Get enough exercise. Regular, daily physical activity can lower your risk of heart disease. Physical activity helps you achieve and maintain a healthy weight and control diabetes, high cholesterol and high blood pressure — all risk factors for heart disease. If you have a heart arrhythmia or heart defect, there may be some restrictions on the activities you can do, so talk to your doctor. Exercise at least 30 to 60 minutes most days of the week. If you haven’t been active for a while, you may need to slowly work your way up to these goals, but in general, you should aim for at least:
- 150 minutes a week of moderate aerobic exercise, such as walking at a brisk pace
- 75 minutes a week of vigorous aerobic activity, such as running
- Two or more strength training sessions a week
- Even shorter bouts of activity offer heart benefits, so if you can’t meet those guidelines, don’t give up. Just five minutes of moving can help, and activities such as gardening, housekeeping, taking the stairs and walking the dog all count toward your total. You don’t have to exercise strenuously to achieve benefits, but you can see bigger benefits by increasing the intensity, duration and frequency of your workouts.
- Get enough good-quality sleep. Quality sleep is good for your heart. It can be a challenge to make time for good sleep, but it’s important. For two weeks try to get 8 hours of good, quality sleep each night. Yes, each person’s sleep needs vary slightly, but eight is a good number to shoot for.
- Eat healthy foods. A heart-healthy diet based on fruits, vegetables and whole grains — and low in saturated fat, salt (sodium), cholesterol and added sugar — can help you control your weight, blood pressure and cholesterol.
- Maintain a healthy weight. Being overweight increases your risk of heart disease. A body mass index (BMI) of less than 25 and a waist circumference of 35 inches (88.9 centimeters) or less is the goal for preventing and treating heart disease.
- Reduce and manage stress. Reduce stress as much as possible. Practice techniques for managing stress, such as muscle relaxation and deep breathing.
- Get treatment for depression. Being depressed can increase your risk of heart disease significantly. Talk to your doctor if you feel hopeless or uninterested in your life.
- Practice good hygiene. Regularly wash your hands and brush and floss your teeth to keep yourself well.
- Get regular medical checkups. Early detection and treatment can set the stage for a lifetime of better heart health.
Lifestyle factors for healthy heart
Following a healthy lifestyle can help you and your children prevent or control many coronary heart disease risk factors. Because many lifestyle habits begin during childhood, parents and families should encourage their children to make heart healthy choices. For example, you and your children can lower your risk of coronary heart disease if you maintain a healthy weight, follow a healthy diet, do physical activity regularly, and don’t smoke.
Strong studies make it possible to link reductions in risk to these habits. Following a healthy lifestyle may prevent over 80% of cases of coronary artery disease 4, 5, 50% of ischemic strokes 6, 80% of sudden cardiac deaths 7 and 72% of premature deaths related to heart disease 8. In other words, a healthy lifestyle is a good investment in a longer, healthier life.
Table 1. Lifestyle factors for healthy heart
| Goal/Metric | Ideal Heart Health Condition |
| Current smoking | |
| Adults >20 years of age | Never or quit >12 months ago |
| Children 12–19 y of age | Never tried; never smoked whole cigarette |
| Body mass index (BMI) | |
| Adults >20 years of age | <25 kg/m² |
| Children 2–19 years of age | <85th Percentile |
| Physical activity | |
| Adults >20 years of age | ≥150 minutes/week moderate intensity or ≥75 minutes/week vigorous intensity or combination |
| Children 12–19 years of age | ≥60 min of moderate- or vigorous-intensity activity every day |
| Healthy diet score* | |
| Adults >20 years of age | 4–5 Components* |
| Children 5–19 years of age | 4–5 Components* |
| Total cholesterol | |
| Adults >20 years of age | <200 mg/dL† |
| Children 6–19 years of age | <170 mg/dL† |
| Blood pressure | |
| Adults >20 years of age | <120/<80 mm Hg† |
| Children 8–19 years of age | <90th Percentile† |
| Fasting plasma glucose | |
| Adults >20 years of age | <100 mg/dL† |
| Children 12–19 years of age | <100 mg/dL† |
Footnotes:
*The Strategic Planning Task Force of the American Heart Association committee selected 5 aspects of diet to define a healthy dietary score. The score is not intended to be comprehensive. Rather, it is a practical approach that provides individuals with a set of potential concrete actions. A comprehensive rationale is set forth in the text of this document, and a comprehensive set of nutrition recommendations is provided in the 2006 Nutrition Guidelines 9, 10, 11.
†Untreated values.
[Source 12]Changes to Your Heart With Age
Aging can cause changes in the heart and blood vessels. For example, as you get older, your heart can’t beat as fast during physical activity or stress as when you were younger. However, the number of heart beats per minute (heart rate) at rest does not change as you age 13.
Many of the problems older people have with their heart and blood vessels are really caused by disease, not by aging. For example, an older heart can normally pump blood as strong as a younger heart; less ability to pump blood is caused by disease. But, changes that happen with age may increase a person’s risk of heart disease. The good news is there are things you can do to delay, lower, or possibly avoid or reverse your risk.
A common problem related to aging is “hardening of the arteries,” called arteriosclerosis. This problem is why blood pressure goes up with age.
Age can cause other changes to the heart 13. For example:
- Blood vessels can become stiffer, and some parts of the heart wall will thicken to help with blood flow.
- Your heart valves may become thicker and stiffer, causing leaks or problems with pumping blood out of the heart.
- The size of the sections of your heart may increase.
Other factors, such as thyroid disease or chemotherapy, may weaken the heart muscle. Things you can’t control, like your family history, might also increase your risk of heart disease. But even so, leading a heart-healthy lifestyle might help you avoid or delay serious illness 14.
Blood Pressure
As you get older, it is important for you to have your blood pressure checked regularly, even if you are healthy. You may feel fine, but if not treated, high blood pressure can lead to stroke and problems with your heart, eyes, and kidneys. Exercise and reducing salt in your diet can help, but often medication is needed to manage high blood pressure and the related problems.
Normal Blood Pressure
Blood pressure is the force of blood pushing against the walls of the arteries as the heart pumps blood 15. Your blood pressure is determined both by the amount of blood your heart pumps and the amount of resistance to blood flow in your arteries. The more blood your heart pumps and the narrower your arteries, the higher your blood pressure. High blood pressure, sometimes called hypertension, happens when this force is too high. A blood pressure reading is given in millimeters of mercury (mm Hg). Mercury was used in the first accurate pressure gauges and is still used in medicine today as the standard unit of measurement for pressure. Health care workers check blood pressure readings the same way for children, teens, and adults. They use a gauge, stethoscope or electronic sensor, and a blood pressure cuff. With this equipment, they measure:
- Systolic Pressure (top number): blood pressure when the heart beats while pumping blood.
- Diastolic Pressure (bottom number): blood pressure when the heart is at rest between beats.
Normal blood pressure for adults is defined as a systolic pressure below 120 mmHg and a diastolic pressure below 80 mmHg. It is normal for blood pressures to change when you sleep, wake up, or are excited or nervous. When you are active, it is normal for your blood pressure to increase. However, once the activity stops, your blood pressure returns to your normal baseline range.
Typically, more attention is given to systolic blood pressure (the first number) as a major risk factor for cardiovascular disease for people over 50. In most people, systolic blood pressure rises steadily with age due to the increasing stiffness of large arteries, long-term buildup of plaque and an increased incidence of cardiac and vascular disease. However, either an elevated systolic or an elevated diastolic blood pressure reading may be used to make a diagnosis of high blood pressure. According to recent studies, the risk of death from ischemic heart disease and stroke doubles with every 20 mm Hg systolic or 10 mm Hg diastolic increase among people from age 40 to 89.
Blood pressure normally rises with age and body size. Newborn babies often have very low blood pressure numbers that are considered normal for babies, while older teens have numbers similar to adults.
Abnormal Blood Pressure
Abnormal increases in blood pressure are defined as having blood pressures higher than 120/80 mmHg. You can have high blood pressure for years without any symptoms. Uncontrolled high blood pressure increases your risk of serious health problems, including heart attack and stroke. Fortunately, high blood pressure can be easily detected. And once you know you have high blood pressure, you can work with your doctor to control it.
The following table outlines and defines high blood pressure severity levels. The ranges in the table are blood pressure guides for adults who do not have any short-term serious illnesses. People with diabetes or chronic kidney disease should keep their blood pressure below 130/80 mmHg.
Although blood pressure increases seen in prehypertension are less than those used to diagnose high blood pressure, prehypertension can progress to high blood pressure and should be taken seriously. Over time, consistently high blood pressure weakens and damages your blood vessels, which can lead to complications.
Table 3. Stages of High Blood Pressure in Adults
| Stages | Systolic (top number) | Diastolic (bottom number) | |
| NORMAL | Less than 120 | AND | Less than 80 |
| ELEVATED | 120–129 | AND | Less than 80 |
| High blood pressure (HYPERTENSION) Stage 1 | 130–139 | OR | 80–89 |
| High blood pressure (HYPERTENSION) Stage 2 | 140 or HIGHER | OR | 90 or HIGHER |
| HYPERTENSIVE CRISIS (you should call your local emergency services number and see a doctor immediately) | HIGHER than 180 | AND/OR | HIGHER than 120 |
Footnote: Healthy and unhealthy blood pressure ranges. A hypertensive crisis (high blood pressure crisis) is when blood pressure rises quickly and severely with readings of 180/120 or greater.
The consequences of uncontrolled blood pressure in this range can be severe and include:
- Stroke
- Loss of consciousness
- Memory loss
- Heart attack
- Damage to the eyes and kidneys
- Loss of kidney function
- Aortic dissection
- Angina (unstable chest pain)
- Pulmonary edema (fluid backup in the lungs)
- Eclampsia
An elevated reading may or may not be accompanied by one or more of the following symptoms:
- Severe headache
- Shortness of breath
- Nosebleeds
- Severe anxiety
High blood pressure Prevention
High blood pressure can often be prevented or reduced by eating healthily, maintaining a healthy weight, taking regular exercise, drinking alcohol in moderation and not smoking.
Healthy diet
Cut down on the amount of salt in your food and eat plenty of fruit and vegetables. The Healthy Eating highlights the different types of food that make up our diet, and shows the proportions we should eat them in to have a well-balanced and healthy diet.
Salt raises your blood pressure. The more salt you eat, the higher your blood pressure. Aim to eat less than 1.5 g (1500 mg) of salt a day, which is about half a teaspoonful. A lower sodium level — 1,500 milligrams (mg) a day — is appropriate for people 51 years of age or older, and individuals of any age who are black or who have hypertension, diabetes or chronic kidney disease.
Otherwise healthy people can aim for 2,300 mg a day or less. While you can reduce the amount of salt you eat by putting down the saltshaker, you generally should also pay attention to the amount of salt that’s in the processed foods you eat, such as canned soups or frozen dinners.
Eating a low-fat diet that includes lots of fiber – such as wholegrain rice, bread and pasta – and plenty of fruit and vegetables also helps lower blood pressure. Aim to eat five portions of fruit and vegetables every day.
Tips for a lower-salt diet
Too much salt can raise your blood pressure, which puts you at increased risk of health problems such as heart disease and stroke. But a few simple steps can help you to cut your salt intake.
Salt (Sodium) Equivalents
Sodium chloride or table salt is approximately 40 percent sodium. It’s important to understand just how much sodium is in salt so you can take measures to control your intake. These amounts are approximate.
- 1/4 teaspoon salt = 575 mg sodium
- 1/2 teaspoon salt = 1,150 mg sodium
- 3/4 teaspoon salt = 1,725 mg sodium
- 1 teaspoon salt = 2,300 mg sodium
Sodium Sources
Sodium can be sneaky. Taking control of your sodium means checking labels and reducing preservatives. Other foods to be aware of include:
- Processed foods
- Natural foods with a higher-than-average sodium content, including cheese, seafood, olives and some legumes
- Table salt, sea salt and kosher salt (sodium chloride)
- Some over-the-counter drugs
- Some prescription medications
You don’t have to add salt to food to be eating too much – 75% of the salt we eat is already in everyday foods such as bread, breakfast cereal and ready meals.
A diet that is high in salt can cause raised blood pressure, which currently affects more than one third of adults in the US.
High blood pressure often has no symptoms, and it is estimated that in America about one in every three people who have high blood pressure don’t know it. But if you have it, you are more likely to develop heart disease or have a stroke.
Heart rate
Your heart rate, or pulse, is the number of times your heart beats per minute. Normal heart rate varies from person to person. Knowing yours can be an important heart-health gauge.
According to the National Institute of Health, the average resting heart rate:
- for children 10 years and older, and adults (including seniors) is 60 – 100 beats per minute
- for well-trained athletes is 40 – 60 beats per minute.
As you age, changes in the rate and regularity of your pulse can change and may signify a heart condition or other condition that needs to be addressed.
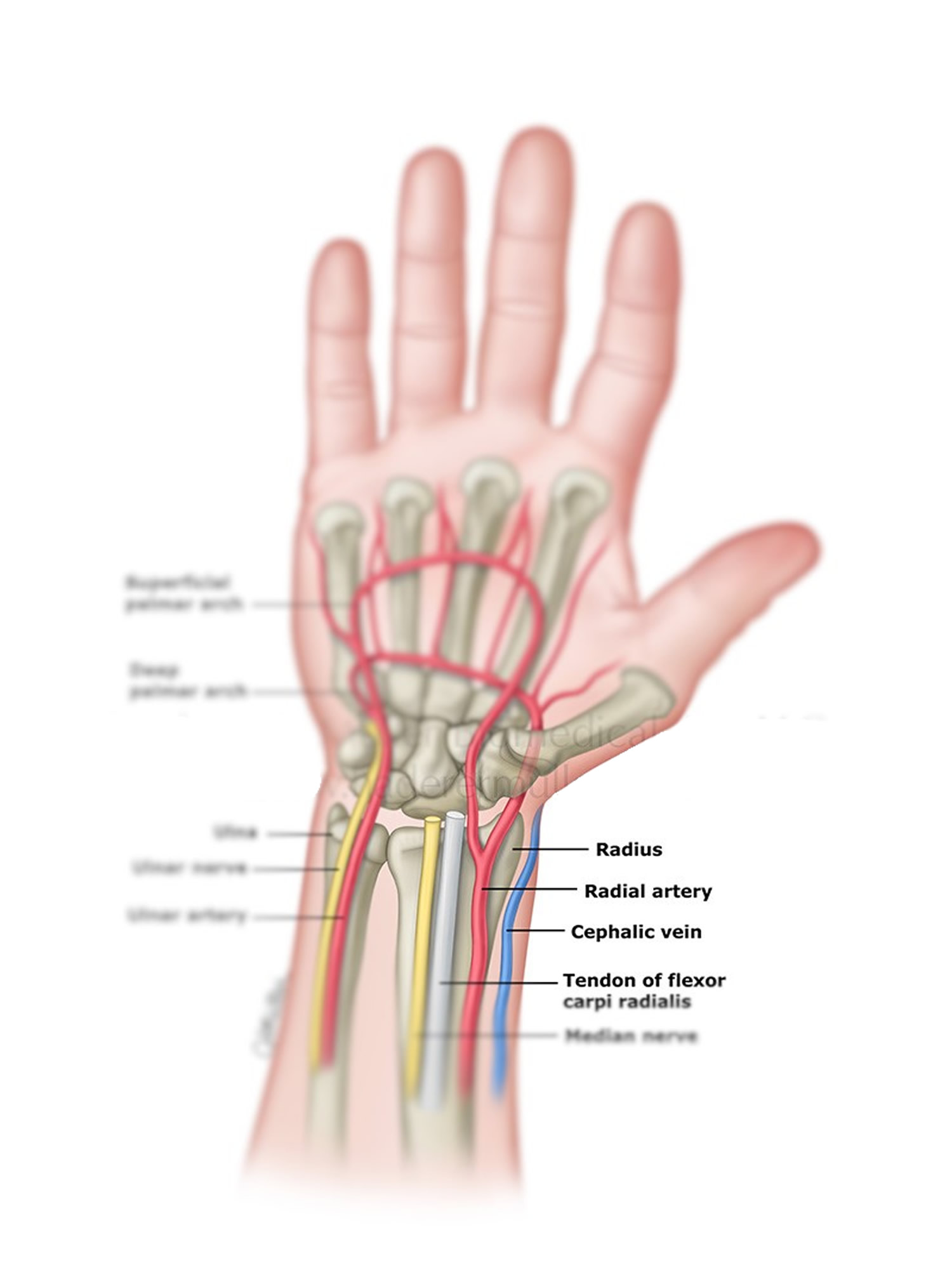
The best places to find your pulse are the:
- wrists
- inside of your elbow
- side of your neck
- top of the foot
Figure 5. Radial artery at the wrist and taking a radial pulse
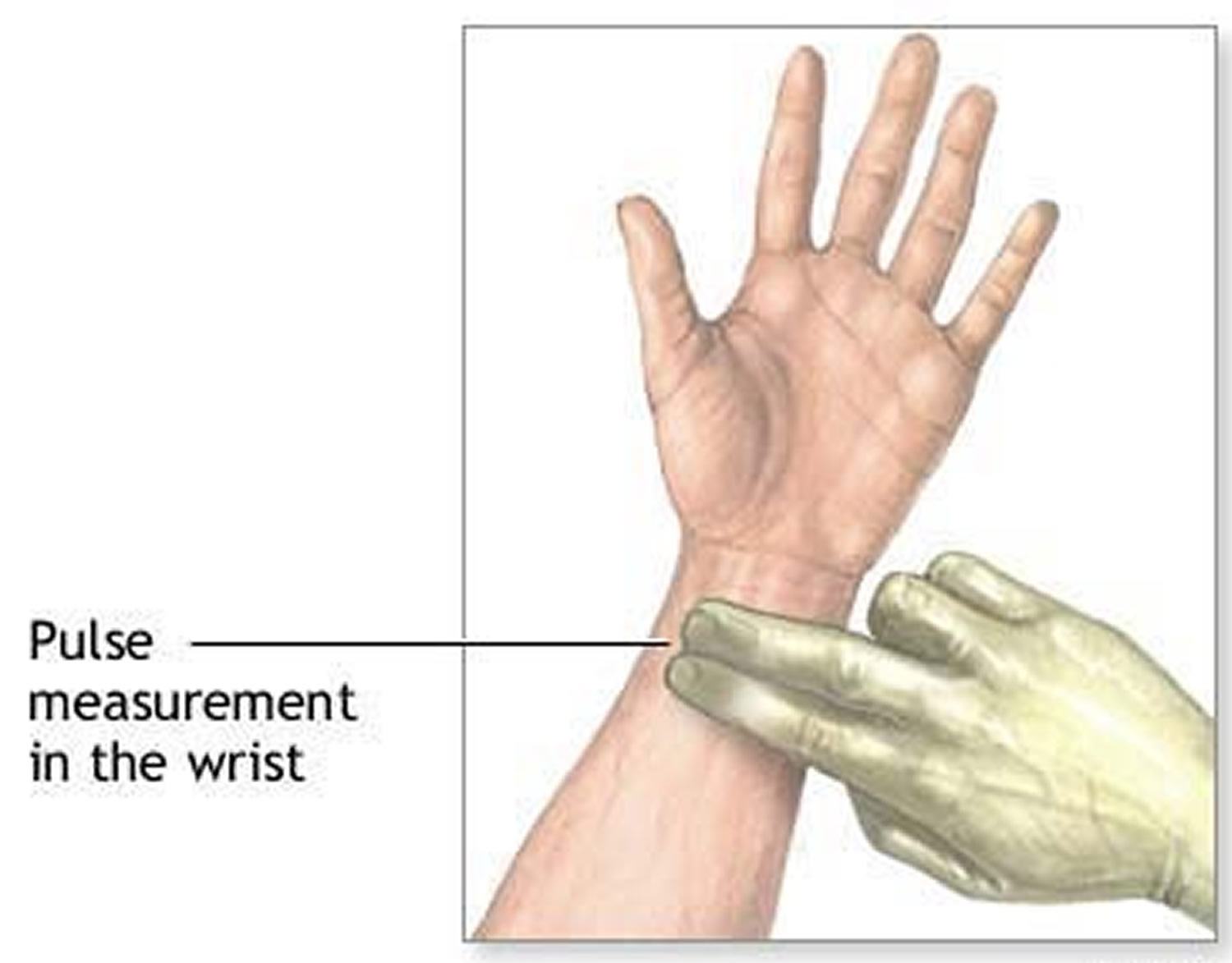
To get the most accurate reading, put your finger over your pulse and count the number of beats in 60 seconds.
How to take your pulse at the wrist:
- Take your pulse on the inside of your wrist, on the thumb side.
- Use the tips of your first two fingers (not your thumb) to press lightly over the blood vessels on your wrist.
- Count your pulse for 10 seconds and multiply by 6 to find your beats per minute.
Your resting heart rate is the heart pumping the lowest amount of blood you need because you’re not exercising. If you’re sitting or lying and you’re calm, relaxed and aren’t ill, your heart rate is normally between 60 (beats per minute) and 100 (beats per minute).
But a heart rate lower than 60 doesn’t necessarily signal a medical problem. It could be the result of taking a drug such as a beta blocker. A lower heart rate is also common for people who get a lot of physical activity or are very athletic. Active people often have lower heart rates because their heart muscle is in better condition and doesn’t need to work as hard to maintain a steady beat.
Moderate physical activity doesn’t usually change the resting pulse much. If you’re very fit, it could change to 40 beats per minute. A less active person might have a heart rate between 60 and 100 beats per minute. That’s because the heart muscle has to work harder to maintain bodily functions, making it higher.
How Other Factors Affect Heart Rate
- Air temperature: When temperatures (and the humidity) soar, the heart pumps a little more blood, so your pulse rate may increase, but usually no more than five to 10 beats a minute.
- Body position: Resting, sitting or standing, your pulse is usually the same. Sometimes as you stand for the first 15 to 20 seconds, your pulse may go up a little bit, but after a couple of minutes it should settle down.
- Emotions: If you’re stressed, anxious or “extraordinarily happy or sad” your emotions can raise your pulse.
- Body size: Body size usually doesn’t change pulse. If you’re very obese, you might see a higher resting pulse than normal, but usually not more than 100.
- Medication use: Medications that block your adrenaline (beta blockers) tend to slow your pulse, while too much thyroid medication or too high of a dosage will raise it.
- Energy drinks.
- Caffeine in beverages and foods.
How do you get your heart rate on target during exercise ?
When you work out, are you doing too much or not enough ?
There’s a simple way to know: Your target heart rate helps you hit the bull’s eye.
This table shows estimated target heart rates for different ages.
- Your maximum heart rate is about 220 minus your age.
In the age category closest to yours, read across to find your target heart rate. Heart rate during moderately intense activities is about 50-69% of your maximum heart rate, whereas heart rate during hard physical activity is about 70% to less than 90% of the maximum heart rate.
The figures are averages, so use them as general guidelines.
Important Note: A few high blood pressure medications lower the maximum heart rate and thus the target zone rate. If you’re taking such medicine, call your physician to find out if you need to use a lower target heart rate.
If your heart rate is too high, you’re straining. So slow down. If it’s too low, and the intensity feels “light” or “moderate/brisk,” you may want to push yourself to exercise a little harder.
During the first few weeks of working out, aim for the lower ranger of your target zone (50 percent) and gradually build up to the higher range (85 percent). After six months or more, you may be able to exercise comfortably at up to 85 percent of your maximum heart rate.
Table 2. Target heart rate during exercise
| Age | Target heart rate Zone 50-85% | Average Maximum Heart Rate, 100% |
| 20 years | 100-170 beats per minute | 200 beats per minute |
| 30 years | 95-162 beats per minute | 190 beats per minute |
| 35 years | 93-157 beats per minute | 185 beats per minute |
| 40 years | 90-153 beats per minute | 180 beats per minute |
| 45 years | 88-149 beats per minute | 175 beats per minute |
| 50 years | 85-145 beats per minute | 170 beats per minute |
| 55 years | 83-140 beats per minute | 165 beats per minute |
| 60 years | 80-136 beats per minute | 160 beats per minute |
| 65 years | 78-132 beats per minute | 155 beats per minute |
| 70 years | 75-128 beats per minute | 150 beats per minute |
Best foods for heart health
A healthy diet can help protect your heart, improve your blood pressure and cholesterol, and reduce your risk of type 2 diabetes. A heart-healthy eating plan includes:
- Vegetables and fruits
- Beans or other legumes
- Lean meats and fish
- Low-fat or fat-free dairy foods
- Whole grains
- Healthy fats, such as olive oil
The following foods are the foundation of a heart-healthy eating plan:
- Vegetables such as leafy greens (spinach, collard greens, kale, cabbage), broccoli, and carrots
- Fruits such as apples, bananas, oranges, pears, grapes, and prunes
- Whole grains such as plain oatmeal, brown rice, and whole-grain bread or tortillas
- Fat-free or low-fat dairy foods such as milk, cheese, or yogurt
- Protein-rich foods:
- Fish high in omega-3 fatty acids (salmon, tuna, and trout)
- Lean meats such as 95% lean ground beef or pork tenderloin or skinless chicken or turkey
- Eggs
- Nuts, seeds, and soy products (tofu)
- Legumes such as kidney beans, lentils, chickpeas, black-eyed peas, and lima beans
- Oils and foods high in monounsaturated and polyunsaturated fats:
- Canola, corn, olive, safflower, sesame, sunflower, and soybean oils (not coconut or palm oil)
- Nuts such as walnuts, almonds, and pine nuts
- Nut and seed butters
- Salmon and trout
- Seeds (sesame, sunflower, pumpkin, or flax)
- Avocados
- Tofu
Research shows that the best foods that protect your heart and blood vessels, include the following:
- Fruits and Vegetables. Current World Health Organization (WHO) recommendations for fruit intake combined with vegetable intake are a minimum 400 g/day 18. A recent meta-analysis indicated that the intake of 800 g/day of fruit was associated with a 27% reductions in relative risk of cardiovascular disease 19.
- Fatty fish (Omega-3 fatty acids). Omega-3 fatty acid is a polyunsaturated fatty acid that must be obtained through dietary intake from fish as well as other types of seafood as it is not produced naturally in the human body 20. Eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA) are essential fatty acids present in omega-3 21. Fatty fish such as salmon, sardines and mackerel are abundant sources of omega-3 fatty acids, healthy unsaturated fats that have been linked to lower blood levels of beta-amyloid—the protein that forms damaging clumps in the brains of people with Alzheimer’s disease. Omega-3 fatty acids are thought to help keep your blood vessels healthy and to help to reduce blood pressure. Research into this style of eating has shown a reduced risk of developing problems such as type 2 diabetes, high blood pressure and raised cholesterol, which are all risk factors for heart disease 22. The American Heart Association recommends eating 2 servings of fish (particularly fatty fish) per week. A serving is 3.5 ounce cooked, or about ¾ cup of flaked fish. Fatty fish like salmon, mackerel, herring, lake trout, sardines and albacore tuna are high in omega-3 fatty acids 23. Eating oily fish is a nutritious choice which can form part of the Mediterranean diet (more bread, fruit, vegetables, fish and less meat, and replacing butter with unsaturated fat spreads). Researchers have also found that people who closely follow a traditional Mediterranean style diet are more likely to live a longer life and also are less likely to become obese. Try to eat fish at least twice a week, but choose varieties that are low in mercury, such as salmon, cod, canned light tuna, and pollack. If you’re not a fan of fish, ask your doctor about taking an omega-3 supplement, or choose terrestrial omega-3 sources such as flaxseeds, avocados, and walnuts. Plant sources of omega-3 fatty acids include flaxseed, oils (olive, canola, flaxseed, soybean), nuts and other seeds (walnuts, butternut squash and sunflower). Replacements for vegans/vegetarians exist that are not supplements, but the evidence is not as robust for plant sources of omega-3 fatty acids.
- Berries. Researchers credit the high levels of flavonoids in berries with the benefit 24. Flavonoids, the natural plant pigments that give berries their brilliant hues, also help improve memory, research shows. Berries contain a particularly high amount of flavonoids called anthocyanidins that are capable of crossing the blood brain barrier and localizing themselves in the hippocampus, an area of the brain known for memory and learning. Epidemiological evidence has established strong inverse associations between flavonoid-rich fruit (e.g. strawberries, grapefruit) and coronary heart disease mortality in cardiovascular disease-free postmenopausal women after multivariate adjustment 25. In a 20-year study of over 16,000 older adult women (aged ≥70 years), those who ate the most blueberries and strawberries had the slowest rates of cognitive decline by up to two-and-a-half years 24.
- Walnuts. Nuts are excellent sources of protein, fat-soluble vitamin E and healthy fats, and one type of nut in particular might also improve memory. A 2015 study from UCLA linked higher walnut consumption to improved cognitive test scores. Walnuts are high in a type of omega-3 fatty acid called alpha-linolenic acid (ALA). Diets rich in alpha-linolenic acid and other omega-3 fatty acids have been linked to lower blood pressure and cleaner arteries. That’s good for both the heart and brain.
- Meat-free meals. Heart-healthy eating encourages consuming meat sparingly. Beans, lentils and soybeans, which pack protein and fiber, make a worthy substitute. They’ll keep you full and are rich in B vitamins, which are important for brain health. In one study analyzing the diets of older adults, those who had the lowest intakes of legumes had greater cognitive decline than those who ate more.
The American Heart Association suggests these daily amounts:
- Vegetables – canned, dried, fresh and frozen vegetables; 5 servings
- Fruits – canned, dried, fresh and frozen fruits; 4 servings
- Whole grains – barley, brown rice, millet, oatmeal, popcorn and whole wheat bread, crackers and pasta; 3-6 servings
- Dairy – low fat (1%) and fat-free dairy products; 3 servings
- Proteins – eggs, fish, lean meat, legumes, nuts, poultry and seeds; 1-2 servings. Eat a variety of fish at least twice a week, especially fish containing omega-3 fatty acids (for example, salmon, trout and herring).
- Oils – polyunsaturated and monounsaturated canola, olive, peanut, safflower and sesame oil; 3 tablespoons
- Limit – sugary drinks, sweets, fatty meats, and salty or highly processed foods
- Choose foods with less salt (sodium) and prepare foods with little or no salt. To lower blood pressure, aim to eat no more than 2,300 milligrams of sodium per day. Reducing daily intake to 1,500 mg is desirable because it can lower blood pressure even further.
- Limit saturated fat and trans fat and replace them with the better fats, monounsaturated and polyunsaturated. If you need to lower your blood cholesterol, reduce saturated fat to no more than 5 to 6 percent of total calories. For someone eating 2,000 calories a day, that’s about 13 grams of saturated fat.
- Avoid – partially hydrogenated oils, tropical oils, and excessive calories
- Replace – highly processed foods with homemade or less-processed options
- If you drink alcohol, drink in moderation. That means no more than one drink per day if you’re a woman and no more than two drinks per day if you’re a man.
Carbohydrate
Carbohydrate (starch) is the body’s main energy (fuel) source. Starch is broken down to produce glucose which is used by your body for energy.
Starchy foods are an important part of the healthy diet. They should make up about a third of all the food that you eat. You don’t have to avoid or restrict them because they are ‘fattening’. Instead, be aware of the total amount of starch that you eat. Cutting out one food group, such as carbohydrate can cause dietary imbalance. Starchy foods include bread, potatoes, rice and pasta. Wholegrain options are healthier choices.
Fiber rich foods help your gut to function properly and have many other health benefits. Studies have shown that people who are overweight or obese tend to lose weight if they include plenty of high fiber, starchy carbohydrate in their diets.
Sugar
Sugar is a type of carbohydrate. Like starch, it breaks down into glucose, to provide energy for your body. ‘Free’ sugars are often added to foods during manufacture and include refined sugars such as sucrose (table sugar). This kind of sugar is also found naturally, in unsweetened fruit juices, and in syrups and honey.
Excess consumption of free sugars is linked to the risk of obesity, type 2 diabetes and tooth decay. Many of the free sugars that you consume, are in sugary drinks. A regular can of cola for instance, can contain the equivalent of seven teaspoons of sugar (35g). The guidance about free sugar consumption suggests a daily limit of 30g. This is equivalent to six teaspoons.
The natural sugars found in milk and in whole fruits and vegetables are not free sugars and do not need to be restricted in the same way.
Fruit and vegetables
Fruit and vegetables contain high levels of ‘micronutrients’. These include vitamins, minerals and antioxidants. Micronutrients are essential to the body’s many biochemical processes.
Fruit and vegetables are often high in fiber. They are generally low in calorie and they taste good. The current Dietary Guidelines for Americans recommends at least five portions of different fruit and vegetable per day 26. Like carbohydrate, fruit and vegetable should account for about one third of what you eat, per day. Dried, frozen, tinned, as well as fresh, fruit and veg are all included. One portion of pulses (baked beans, lentils, dried peas) can also count towards your five a day.
Dietary fiber
Fiber comes from plant-based foods, including fruits, vegetables and wholegrains. Dietary fiber is the part of plants that you eat but which doesn’t get digested in your small intestine. Instead, it is completely or partially broken down (fermented) by bacteria in your large intestine. Once broken down in your large intestine, it has been suggested that dietary fibers increase the beneficial bacteria in your gut. This improves your immune system. Fibre includes carbohydrates called polysaccharides and resistant oligosaccharides. Recent research suggests that fiber should be categorized by its physical characteristics; how well it dissolves (solubility), how thick it is (viscosity) and how well it breaks down (fermentability). Some commonly known terms are described below:
- Soluble fiber including pectins and beta glucans is found in foods like fruit and oats.
- Insoluble fiber including cellulose is found in wheat bran and nuts.
- Resistant starch is a soluble fiber that is highly fermentable in the gut. It gets broken down by good bacteria to produce short chain fatty acids (SCFAs). Resistant starch is naturally present in some foods such as bananas, potatoes, grains and pulses.
- Prebiotics are types of carbohydrate that only our gut bacteria can feed upon. Some examples are onions, garlic, asparagus and banana
Fibre is essential for your gut to work normally. It increases good bacteria which supports your immunity against inflammatory disorders and allergies. A high fiber diet seems to reduce the risk of chronic diseases such as heart disease, type 2 diabetes and bowel cancer.
Eating a range of dietary fiber can:
- Improve the diversity of your microbiota
- Improve constipation and lactose intolerance
- Enhance immunity
- Reduce inflammation in your gut
For example, high quality randomized controlled trials have shown that eating oat bran leads to lower blood pressure and lower total cholesterol.
Benefits of a high-fiber diet:
- Normalizes bowel movements. Dietary fiber increases the weight and size of your stool and softens it. A bulky stool is easier to pass, decreasing your chance of constipation. If you have loose, watery stools, fiber may help to solidify the stool because it absorbs water and adds bulk to stool.
- Helps maintain bowel health. A high-fiber diet may lower your risk of developing hemorrhoids and small pouches in your colon (diverticular disease). Studies have also found that a high-fiber diet likely lowers the risk of colorectal cancer. Some fiber is fermented in the colon. Researchers are looking at how this may play a role in preventing diseases of the colon.
- Lowers cholesterol levels. Soluble fiber found in beans, oats, flaxseed and oat bran may help lower total blood cholesterol levels by lowering low-density lipoprotein, or “bad,” cholesterol levels. Studies also have shown that high-fiber foods may have other heart-health benefits, such as reducing blood pressure and inflammation.
- Helps control blood sugar levels. In people with diabetes, fiber — particularly soluble fiber — can slow the absorption of sugar and help improve blood sugar levels. A healthy diet that includes insoluble fiber may also reduce the risk of developing type 2 diabetes.
- Aids in achieving healthy weight. High-fiber foods tend to be more filling than low-fiber foods, so you’re likely to eat less and stay satisfied longer. And high-fiber foods tend to take longer to eat and to be less “energy dense,” which means they have fewer calories for the same volume of food.
- Helps you live longer. Studies suggest that increasing your dietary fiber intake — especially cereal fiber — is associated with a reduced risk of dying from cardiovascular disease and all cancers.
Good sources of dietary fiber include:
- Pulses (like lentils and peas) and beans and legumes (think navy beans, small white beans, split peas, chickpeas, lentils, pinto beans)
- Fruits and vegetables, vegetables such as carrots, broccoli, green peas, and collard greens; fruits especially those with edible skin (like pears and apples with the skin on) and those with edible seeds (like berries)
- Nuts—try different kinds (pumpkin seeds, almonds, sunflower seeds, pistachios and peanuts are a good source of fiber and healthy fats, but be mindful of portion sizes, because they also contain a lot of calories in a small amount!)
- Whole grains such as:
- Quinoa, barley, bulgur, oats, brown rice and farro
- Whole wheat pasta
- Whole grain cereals, including those made from whole wheat, wheat bran and oats
Choose fiber rich foods from a variety of sources including wholegrains, fruit and vegetable, nuts and seeds, beans and pulses. When you read food labels check for the grams of fiber per serving or per 100g. Foods that are naturally high in fiber and contain at least 3 grams per 100 gram are often labeled as a “good source,” and foods labeled as “excellent source” contain more than 5 grams of fiber per serving.
Depending on your age and sex, adults should get 25 to 31 grams of fiber a day 27. Older adults sometimes don’t get enough fiber because they may lose interest in food.
- Men over the age of 50 should get at least 38 grams of fiber per day.
- Women over the age of 50 should get 25 grams per day.
- Children ages 1 to 3 should get 19 grams of fiber per day.
- Children between 4 and 8 years old should get 25 grams per day.
- Girls between 9 and 18 should get 26 grams of fiber each day. Boys of the same age range should get between 31 and 38 grams of fiber per day.
You may wish to see a dietitian if you:
- are unsure about how much and/or what types of fiber you currently have in your diet
- suffer with constipation or diarrhea (e.g. irritable bowel syndrome [IBS])
- have a condition which can restrict your fiber intake (e.g. inflammatory bowel disease)
Keep in mind that if you haven’t been eating a lot of foods high in fiber on a daily basis, it’s important to increase your intake slowly to allow your body to adjust. A sudden increase in eating foods high in fiber (especially foods with added fiber or when using supplements) can cause gas, bloating or constipation. Be sure you are drinking enough water too, because fiber needs water to move through your body.
Protein
Protein is vital. It is your body’s main building block. Animal products such as meat, fish, eggs and dairy are good sources of dietary protein. Meat and fish also provide your body with a form of iron (heme), which is easy to absorb. Fish also contains essential fatty acids (e.g, Omega-3).
Protein also comes from foods of plant origin. Pulses, nuts, and seeds are all high in protein. Pulses are a very good meat alternative, whether or not you are vegetarian or vegan.
Cutting back on consumption of red meat (beef, lamb, goat, pork) especially, is better for your health and for the environment: current advice is to have no more than 300g of red meat per week. Try to avoid processed meats such as bacon, salami, hot dogs, ham. Consumption of these cured meat products has been linked to a much higher risk of certain gut cancers.
Dairy
Dairy products and calcium-fortified alternatives are your body’s main source of calcium, which is necessary for the growth, development and maintenance of healthy bones and teeth. Dairy products and alternatives are also a source of protein. Milk, cheese, cream and milk-based sauces and yogurts can have a high saturated fat content. Fat reduced options are recommended, and small quantities.
Fats
Fats also known as lipids, is an essential nutrient (a primary storage form of energy, a kilojoule-dense nutrient) your body need for energy and to help your gut absorb vitamins A, D, E and K from foods. Fat has twice as many calories as proteins or carbohydrates. There are nine calories (37kJ) in every gram of fat, regardless of what type of fat it is. Fats are more energy-dense than carbohydrates and proteins, which provide four calories (17kJ) per gram. Dietary fat also plays a major role in your cholesterol levels. You need some fat in your diet but not too much. There are different types of fats, some are “good” and some are “bad”, however, you should try to avoid “bad” fats. When it comes to dietary fat, what matters most is the type of fat you eat. Contrary to past dietary advice promoting low-fat diets, newer research shows that healthy fats are necessary and beneficial for health.
Healthy fats are unsaturated. They keep cholesterol levels within a healthy range, reduce your risk of heart problems and may be good for the skin, eyes and brain. Unsaturated fats are the best choice for a healthy diet.
Unhealthy fats are saturated and trans fats, which can raise levels of ‘bad’ cholesterol and increase the risk of heart disease. Multiple studies have linked high levels of saturated fat with cognitive decline. A diet that is higher in unsaturated fats and lower in saturated fats is linked to better cognition.
- Saturated fats such as butter, solid shortening, and lard. Eating foods that contain saturated fats raises the level of cholesterol in your blood. High levels of LDL cholesterol (low-density lipoprotein or “bad” cholesterol) in your blood increase your risk of heart disease and stroke. The American Heart Association recommends aiming for a dietary pattern that achieves 5% to 6% of calories from saturated fat. For example, if you need about 2,000 calories a day, no more than 120 of them should come from saturated fat. That’s about 13 grams of saturated fat per day 28.
- Trans fats also known as trans fatty acids or “partially hydrogenated oils”. These are found in vegetable shortenings, some margarines, crackers, cookies, snack foods, and other foods made with or fried in partially hydrogenated oils. By 2018, most U.S. companies will not be allowed to add partially hydrogenated oils to food.
“Bad” fats, such as artificial trans fats and saturated fats, are guilty of the unhealthy things all fats have been blamed for—weight gain, clogged arteries, an increased risk of certain diseases, and so forth. Large studies have found that replacing saturated fats in your diet with unsaturated fats and omega-3 fatty acids can reduce your risk of heart disease by about the same amount as cholesterol-lowering drugs. Since fat is an important part of a healthy diet, rather than adopting a low-fat diet, it’s more important to focus on eating more beneficial “good” fats and limiting harmful “bad” fats. For good health, the majority of the fats that you eat should be monounsaturated or polyunsaturated. Eat foods containing monounsaturated fats and/or polyunsaturated fats such as canola oil, olive oil, safflower oil, sesame oil or sunflower oil instead of foods that contain saturated fats and/or trans fats.
For years you’ve been told that eating fat will add inches to your waistline, raise cholesterol, and cause a myriad of health problems. When food manufacturers reduce fat, they often replace it with carbohydrates from sugar, refined grains, or other starches. Your body digests these refined carbohydrates and starches very quickly, affecting your blood sugar and insulin levels and possibly resulting in weight gain and disease 29. But now scientists know that not all fat is the same. Research has shown that unsaturated fats are good for you. Healthy fats play a huge role in helping you manage your moods, stay on top of your mental game, fight fatigue, and even control your weight. These fats come mostly from plant sources. Cooking oils that are liquid at room temperature, such as canola, peanut, safflower, soybean, and olive oil, contain mostly unsaturated fat. Nuts, seeds, and avocados are also good sources. Fatty fish—such as salmon, sardines, and herring—are rich in unsaturated fats, too. You should actively make unsaturated fats a part of your diet. Of course, eating too much fat will put on the pounds too. Note also that by swapping animal fats for refined carbohydrates—such as replacing your breakfast bacon with a bagel or pastry—won’t have the same benefits. In fact eating refined carbohydrates or sugary foods can have a similar negative effect on your cholesterol levels, your risk for heart disease, and your weight. Limiting your intake of saturated fat can still help improve your health—as long as you take care to replace it with good fat rather than refined carbs. In other words, don’t go no fat, go good fat.
Healthy-eating tips:
- Use olive oil in cooking.
- Replace saturated fats with unsaturated fats; for example, use avocado, tahini, nut or seed butter instead of dairy butter.
- Eat fish, especially oily fish, twice a week.
- Consume legume- or bean-based meals twice a week.
- Snack on nuts or add them to your cooking.
- Throw avocado in salads.
- Choose lean meats and trim any fat you can see (including chicken skin).
- Use table spreads that have less than 0.1g of trans fats per 100g.
Saturated fats
Saturated fats are fat molecules that are “saturated” with hydrogen molecules. Saturated fats are normally solid at room temperature. Saturated fats occur naturally in many foods — primarily meat and dairy foods (butter, cream, full-fat milk and cheese). Beef, lamb, pork on poultry (with the skin on) contain saturated fats, as do butter, cream and cheese made from whole or 2% milk. Plant-based foods that contain saturated fats include coconut, coconut oil, coconut milk and coconut cream, cooking margarine, and cocoa butter, as well as palm oil and palm kernel oil (often called tropical oils). Saturated fats are also found in snacks like chips, cakes, biscuits and pastries, and takeaway foods. Consuming more than the recommended amount of saturated fat is linked to heart disease and high cholesterol.
The American Dietary Guidelines recommend that:
- men should not eat more than 30g of saturated fat a day
- women should not eat more than 20g of saturated fat a day
- children should have less
For people who need to lower their cholesterol, the American Heart Association recommends reducing saturated fat to less than 6% of total daily calories. For someone eating 2,000 calories a day, that’s about 11 to 13 grams of saturated fat 28.
Examples of foods with saturated fat are:
- fatty beef,
- lamb,
- pork,
- poultry with skin,
- beef fat (tallow),
- meat products including sausages and pies,
- lard and cream,
- butter and ghee,
- cheese especially hard cheese like cheddar,
- other dairy products made from whole or reduced-fat (2 percent) milk,
- cream, soured cream and ice cream,
- some savory snacks, like cheese crackers and some popcorns,
- chocolate confectionery,
- biscuits, cakes, and pastries
In addition, many baked goods and fried foods can contain high levels of saturated fats. Some plant-based oils, such as palm oil, palm kernel oil, coconut oil and coconut cream, also contain primarily saturated fats, but do not contain cholesterol.
Unsaturated Fats
If you want to reduce your risk of heart disease, it’s best to reduce your overall fat intake and swap saturated fats for unsaturated fats. Unsaturated fats are in fish, such as salmon, trout and herring, and plant-based foods such as avocados, olives and walnuts. Liquid vegetable oils, such as soybean, corn, safflower, canola, olive and sunflower, also contain unsaturated fats.
There are 2 types of unsaturated fats: monounsaturated and polyunsaturated. Unsaturated fats help reduce your risk of heart disease and lower your cholesterol levels.
- Polyunsaturated fats such as omega-3 and omega-6 fats are found in fish, nuts, and safflower and soybean oil.
- Monounsaturated fats are found in olive and canola oil, avocado, cashews and almonds.
Monounsaturated fats have one (“mono”) unsaturated carbon bond in the molecule. Polyunsaturated fats have more than one (“poly,” for many) unsaturated carbon bonds. Both of these unsaturated fats are typically liquid at room temperature.
Eaten in moderation, both kinds of unsaturated fats may help improve your blood cholesterol when used in place of saturated and trans fats.
Polyunsaturated fats
Polyunsaturated fats are simply fat molecules that have more than one unsaturated carbon bond in the molecule, this is also called a double bond. Oils that contain polyunsaturated fats are typically liquid at room temperature but start to turn solid when chilled. Olive oil is an example of a type of oil that contains polyunsaturated fats.
There are 2 main types of polyunsaturated fats: omega-3 and omega-6. Oils rich in polyunsaturated fats also provide essential fats that your body needs but can’t produce itself – such as omega-6 and omega-3 fatty acids. You must get essential fats through food. Omega-6 and omega-3 fatty acids are important for many functions in the body. A deficiency of essential fatty acids—either omega-3s or omega-6s—can cause rough, scaly skin and dermatitis 30.
Polyunsaturated fats can help reduce bad cholesterol levels in your blood which can lower your risk of heart disease and stroke. Polyunsaturated fats also provide nutrients to help develop and maintain your body’s cells. Oils rich in polyunsaturated fats also contribute vitamin E to the diet, an antioxidant vitamin most Americans need more of.
Foods high in polyunsaturated fat include a number of plant-based oils, including:
- soybean oil
- corn oil
- sunflower oil
Other sources include some nuts and seeds such as walnuts and sunflower seeds, tofu and soybeans.
Omega-6 fats are found in vegetable oils, such as:
- rapeseed
- corn
- sunflower
- some nuts
Omega-3 fats are found in oily fish, such as:
- kippers
- herring
- trout
- sardines
- salmon
- mackerel
The American Heart Association also recommends eating tofu and other forms of soybeans, canola, walnut and flaxseed, and their oils. These foods contain alpha-linolenic acid (ALA), another omega-3 fatty acid.
Polyunsaturated fats (PUFAs) are frequently designated by their number of carbon atoms and double bonds. Alpha-linolenic acid (ALA), for example, is known as C18:3n-3 because it has 18 carbons and 3 double bonds and is an omega-3 fatty acid. Similarly, eicosapentaenoic acid (EPA) is known as C20:5n-3 and docosahexaenoic acid (DHA) as C22:6n-3. Omega-6 fatty acids (omega-6s) have a carbon–carbon double bond that is six carbons away from the methyl end of the fatty acid chain. Linoleic acid (LA) known as C18:2n-6 and arachidonic acid (AA) known as C20:4n-6 are two of the major omega-6s.
The human body can only form carbon–carbon double bonds after the 9th carbon from the methyl end of a fatty acid 31. Therefore, alpha-linolenic acid (ALA) and linoleic acid (LA) are considered essential fatty acids, meaning that they must be obtained from the diet 32. Alpha-linolenic acid (ALA) can be converted into eicosapentaenoic acid (EPA) and then to docosahexaenoic acid (DHA), but the conversion (which occurs primarily in the liver) is very limited, with reported rates of less than 15% 33. Therefore, consuming EPA and DHA directly from foods and/or dietary supplements is the only practical way to increase levels of these fatty acids in the body.
Alpha-linolenic acid (ALA) is present in plant oils, such as flaxseed, soybean, and canola oils 33. Docosahexaenoic acid (DHA) and eicosapentaenoic acid (EPA) are present in fish, fish oils, and krill oils, but they are originally synthesized by microalgae, not by the fish. When fish consume phytoplankton that consumed microalgae, they accumulate the omega-3s in their tissues 33.
Some researchers propose that the relative intakes of omega-6s and omega-3s—the omega-6/omega-3 ratio—may have important implications for the pathogenesis of many chronic diseases, such as cardiovascular disease and cancer 34, but the optimal ratio—if any—has not been defined 35. Others have concluded that such ratios are too non-specific and are insensitive to individual fatty acid levels 36. Most agree that raising eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA) blood levels is far more important than lowering linoleic acid (LA) or arachidonic acid levels.
Currently, most clinicians do not assess omega-3 status, but it can be done by measuring individual omega-3s in plasma or serum phospholipids and expressing them as the percentage of total phospholipid fatty acids by weight 37. Experts have not established normal ranges, but mean values for serum or plasma phospholipid eicosapentaenoic acid (EPA) plus docosahexaenoic acid (DHA) among U.S. adults not taking omega-3 supplements are about 3%–4% 37. Plasma and serum fatty acid values, however, can vary substantially based on an individual’s most recent meal, so they do not reflect long-term dietary consumption 38.
It is also possible to assess omega-3 status via analysis of erythrocyte fatty acids, a measurement that reflects longer-term intakes over approximately the previous 120 days 39. The “omega-3 index” proposed by Harris and von Schacky reflects the content of eicosapentaenoic acid (EPA) plus docosahexaenoic acid (DHA) in erythrocyte membranes expressed as a percentage of total erythrocyte fatty acids 40. This index can be used as a surrogate for assessing tissue levels of eicosapentaenoic acid (EPA) plus docosahexaenoic acid (DHA) 41. Eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA) typically comprise about 3%–5% of erythrocyte fatty acids in Western populations with low fish intakes. In Japan, where fish consumption is high, erythrocyte eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA) levels are about twice those of Western populations 33.
Table 1. Alpha-linolenic acid (ALA), eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA) content of selected foods
| Food | Grams per serving | ||
| ALA | DHA | EPA | |
| Flaxseed oil, 1 tbsp | 7.26 | ||
| Chia seeds, 1 ounce | 5.06 | ||
| English walnuts, 1 ounce | 2.57 | ||
| Flaxseed, whole, 1 tbsp | 2.35 | ||
| Salmon, Atlantic, farmed cooked, 3 ounces | 1.24 | 0.59 | |
| Salmon, Atlantic, wild, cooked, 3 ounces | 1.22 | 0.35 | |
| Herring, Atlantic, cooked, 3 ounces* | 0.94 | 0.77 | |
| Canola oil, 1 tbsp | 1.28 | ||
| Sardines, canned in tomato sauce, drained, 3 ounces* | 0.74 | 0.45 | |
| Mackerel, Atlantic, cooked, 3 ounces* | 0.59 | 0.43 | |
| Salmon, pink, canned, drained, 3 ounces* | 0.04 | 0.63 | 0.28 |
| Soybean oil, 1 tbsp | 0.92 | ||
| Trout, rainbow, wild, cooked, 3 ounces | 0.44 | 0.4 | |
| Black walnuts, 1 ounce | 0.76 | ||
| Mayonnaise, 1 tbsp | 0.74 | ||
| Oysters, eastern, wild, cooked, 3 ounces | 0.14 | 0.23 | 0.3 |
| Sea bass, cooked, 3 ounces* | 0.47 | 0.18 | |
| Edamame, frozen, prepared, ½ cup | 0.28 | ||
| Shrimp, cooked, 3 ounces* | 0.12 | 0.12 | |
| Refried beans, canned, vegetarian, ½ cup | 0.21 | ||
| Lobster, cooked, 3 ounces* | 0.04 | 0.07 | 0.1 |
| Tuna, light, canned in water, drained, 3 ounces* | 0.17 | 0.02 | |
| Tilapia, cooked, 3 ounces* | 0.04 | 0.11 | |
| Scallops, cooked, 3 ounces* | 0.09 | 0.06 | |
| Cod, Pacific, cooked, 3 ounces* | 0.1 | 0.04 | |
| Tuna, yellowfin, cooked 3 ounces* | 0.09 | 0.01 | |
| Kidney beans, canned ½ cup | 0.1 | ||
| Baked beans, canned, vegetarian, ½ cup | 0.07 | ||
| Ground beef, 85% lean, cooked, 3 ounces** | 0.04 | ||
| Bread, whole wheat, 1 slice | 0.04 | ||
| Egg, cooked, 1 egg | 0.03 | ||
| Chicken, breast, roasted, 3 ounces | 0.02 | 0.01 | |
| Milk, low-fat (1%), 1 cup | 0.01 | ||
Footnotes: *Except as noted, the U.S. Department of Agriculture (USDA) database does not specify whether fish are farmed or wild caught. **The USDA database does not specify whether beef is grass fed or grain fed.
Essential Fatty Acids
Essential Fatty Acids such as omega-3 oils are ‘essential’ because your body can’t make them and you have to obtain them from your food. Essential Fatty Acids are found in the skin of white fish but also in the flesh of oily fish such as fresh and tinned salmon, mackerel, sardines and fresh tuna. Advice for fish eaters is to have one portion of oily fish, and one portion of white fish per week.
Essential Fatty Acids can also be found in some plant oils such as flaxseed, rapeseed and soya but there is not as much in these oils as there is in fish and seafood.
Omega-3 fatty acids
Omega-3 fatty acids (omega-3s) are a type of polyunsaturated fat and have a carbon–carbon double bond located three carbons from the methyl end of the chain (see Figure 6). Omega-3 fatty acids, sometimes referred to as “n-3s,” are present in certain foods such as flaxseed and fish, as well as dietary supplements such as fish oil. Omega-3 fatty acids are especially beneficial to your health. Omega-3s play important roles in the body as components of the phospholipids that form the structures of cell membranes 30. There are different types of omega-3s: eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA) are found in fish and algae and have the most health benefits, while alpha-linolenic acid (ALA) comes from plants and is a less potent form of omega-3, although the body does convert ALA to EPA and DHA at low rates. Alpha-linolenic acid (ALA) contains 18 carbon atoms, whereas eicosapentaenoic acid (EPA), and docosahexaenoic acid (DHA) are considered “long-chain” omega-3s because EPA contains 20 carbons and DHA contains 22 41.
Docosahexaenoic acid (DHA), in particular, is especially high in the retina, brain, and sperm 33. In addition to their structural role in cell membranes, omega-3s (along with omega-6s) provide energy for the body and are used to form eicosanoids. Eicosanoids are signaling molecules that have similar chemical structures to the fatty acids from which they are derived; they have wide-ranging functions in the body’s cardiovascular, pulmonary, immune, and endocrine systems 31. Higher concentrations of EPA and DHA than arachidonic acid tip the eicosanoid balance toward less inflammatory activity 42.
Research has shown that a diet rich in omega-3 fatty acids may help to:
- Prevent and reduce symptoms of depression, ADHD, and bipolar disorder.
- Protect against memory loss and dementia.
- Reduce the risk of heart disease, stroke, and cancer.
- Ease arthritis, joint pain, and inflammatory skin conditions.
- Support a healthy pregnancy.
- Battle fatigue, sharpen your memory, and balance your mood.
Fish the best source of omega-3 (high in EPA and DHA):
- Anchovies
- Herring
- Salmon
- Mackerel
- Sardines
- Trout
- Tuna
- Mussels
- Oysters
- Halibut
Vegetarian sources of omega-3s (high in ALA):
- Algae such as seaweed (high in EPA and DHA)
- Eggs (small amounts of DHA)
- Flaxseeds and flaxseed oil
- Chia seeds
- Canola and soybean oil
- Walnuts
- Mayonnaise
- Edamame
- Beans (refried, kidney, etc.)
- Brussels sprouts
- Kale
- Spinach
Fish is a good source of protein and omega-3 fatty acids, which are good for your heart. Research has shown that omega-3 fatty acids can reduce your risk of heart disease and stroke. A 2020 Cochrane review 43 of 86 randomized controlled trials published between 1968 and 2019 found that 0.5 g/day to more than 5 g/day omega-3 fatty acids for 12 to 88 months in a total of 162,796 participants reduced serum triglyceride levels by about 15% and slightly decreased rates of cardiovascular mortality and coronary heart disease events. However, the omega-3 fatty acids supplements did not affect all-cause mortality, cardiovascular events, stroke, or arrhythmia. The authors of several earlier meta-analyses and systematic reviews, as well as a 2016 report from the Agency for Healthcare Research and Quality, concluded that omega-3 fatty acids supplements do not appear to significantly reduce the risk of most cardiovascular events 44. Many of these analyses 45, however, but not all 46, did find that omega-3s reduce the risk of cardiac death.
The American Heart Association recommends eating 2 servings of fish (particularly fatty fish) per week. A serving is 3.5 ounce (100 g) cooked, or about ¾ cup of flaked fish. Fatty fish like salmon, mackerel, herring, lake trout, sardines and albacore tuna are high in omega-3 fatty acids. For people with existing coronary heart disease, such as a recent heart attack (myocardial infarction), the American Heart Association recommends approximately 1 gram/day EPA plus DHA, preferably from oily fish; however, supplements could also be considered under the direction of a physician 47. The American Heart Association does not recommend omega-3 supplements for people who do not have a high cardiovascular disease risk.
While omega-3s are best obtained through food, there are many omega-3 and fish oil supplements available. A typical fish oil supplement provides about 1,000 mg fish oil, containing 180 mg EPA and 120 mg DHA, but doses vary widely 48. If you need to substantially lower your triglycerides, your doctor may recommend prescription fish oil, which has been concentrated to contain about 900 mg of EPA plus DHA per capsule. Cod liver oil supplements provide vitamin A and vitamin D in addition to omega-3s. For strict vegetarians or vegans, as well as obtaining ALA from food sources, look for capsules containing DHA and EPA extracted from algae, the original source of omega-3s for fish. Although seafood contains varying levels of methyl mercury (a toxic heavy metal) 49, omega-3 supplements have not been found to contain this contaminant because it is removed during processing and purification 50.
Some types of fish may contain high levels of mercury, PCBs (polychlorinated biphenyls), dioxins and other environmental contaminants. Levels of these substances are generally highest in older, larger, predatory fish and marine mammals.
The benefits and risks of eating fish vary depending on a person’s stage of life.
Children and pregnant women are advised by the U.S. Food and Drug Administration (FDA) to:
- Avoid eating those fish with the potential for the highest level of mercury contamination (such as shark, swordfish, king mackerel or tilefish).
- Eat a variety of fish and shellfish that are lower in mercury (such as canned light tuna, salmon, pollock, catfish).
- Check local advisories about the safety of fish caught by family and friends in local lakes, rivers and coastal areas.
For middle-aged and older men and postmenopausal women, the benefits far outweigh the potential risks when the amount of fish eaten is within the recommendations established by the FDA and Environmental Protection Agency.
Eating a variety of fish will help minimize any potentially adverse effects due to environmental pollutants. Five of the most commonly eaten fish or shellfish that are low in mercury are shrimp, canned light tuna, salmon, pollock, and catfish. Avoid eating shark, swordfish, king Mackerel, or tilefish because they contain high levels of mercury.
Cholesterol
Dietary fat plays a major role in your cholesterol levels. Cholesterol is a type of fat, a wax-like substance that your body needs to function properly that comes from foods such as eggs and is also found in your blood mostly made by your body in your liver. In and of itself, cholesterol isn’t bad. But when you get too much of it, it can have a negative impact on your health. The 2 main types of cholesterol are:
- “Good” cholesterol or HDL (high-density lipoprotein) cholesterol. “Good” HDL cholesterol has a positive effect by taking cholesterol from parts of the body where there’s too much of it to the liver, where it’s disposed of.
- “Bad” cholesterol or LDL (low-density lipoprotein) cholesterol.
High levels of LDL cholesterol (low-density lipoprotein or “bad” cholesterol) can increase your risk of heart disease. The key is to keep your LDL levels low and HDL high, which may protect against heart disease and stroke. High levels of LDL cholesterol (low-density lipoprotein or “bad” cholesterol) can clog arteries and low HDL (high-density lipoprotein or “good” cholesterol) can be a marker for increased cardiovascular risk. However, eating foods that contain any type of cholesterol won’t actually raise your body’s cholesterol levels. Rather than the amount of cholesterol you eat, the biggest influence on your cholesterol levels is the type of fats you consume. Eating saturated or trans fats is far more likely to give you high cholesterol. So instead of counting cholesterol, it’s important to focus on replacing bad fats with good fats.
LDL (bad) cholesterol
LDL (low-density lipoprotein) cholesterol is considered the “bad” cholesterol, because it contributes to fatty buildups in arteries (atherosclerosis). This narrows the arteries and increases the risk for heart attack, stroke and peripheral artery disease. Your body naturally produces all the LDL cholesterol you need. Eating foods containing saturated fats and trans fats causes your body to produce even more LDL — raising the level of “bad” cholesterol in your blood.
HDL (good) cholesterol
HDL (high-density lipoprotein) cholesterol can be thought of as the “good” cholesterol because a healthy level may protect against heart attack and stroke. HDL carries LDL (bad) cholesterol away from the arteries and back to the liver, where the LDL is broken down and passed from the body. But HDL cholesterol doesn’t completely eliminate LDL cholesterol. Only one-third to one-fourth of blood cholesterol is carried by HDL.
Trans fats
Avoid trans fat. Trans fats also known as trans fatty acids or “partially hydrogenated oils”, are created in an industrial process that adds hydrogen to liquid vegetable oils to make them more solid, so they ‘behave’ like a saturated fat. There are two broad types of trans fats found in foods: naturally-occurring and artificial trans fats. Naturally-occurring trans fats are produced in the gut of some animals and foods made from these animals (e.g., milk and meat products) may contain small quantities of these fats. Artificial trans fats (or trans fatty acids) are created in an industrial process that adds hydrogen to liquid vegetable oils to make them more solid.
Trans fats increase the levels of ‘bad’ LDL cholesterol and decreases the levels of ‘good’ HDL cholesterol in your body, which increases your risk of developing heart disease and stroke. Trans fats is also associated with a higher risk of developing type 2 diabetes. Trans fats can be found in many foods such as in butter, margarine (in small amounts), deep-fried and processed foods like doughnuts, cakes and pastries. Baked goods, such as pastries, pizza dough, frozen pizza, pie crust, cookies, biscuits, and crackers also can contain trans fats.
Since 2006, the FDA has required trans fat content to be listed on the Nutrition Facts panel of packaged foods. In recent years, many major national fast-food chains and casual-dining restaurant chains have announced they will no longer use trans fats to fry or deep-fry foods.
The American Heart Association recommends that adults who would benefit from lowering LDL cholesterol eliminate trans fat from their diet.
To find the amount of trans fats in a particular packaged food, look at the Nutrition Facts panel. Companies must list any measurable amount of trans fat (0.5 grams or more per serving) in a separate line in the “Total Fat” section of the panel, directly beneath the line for “Saturated Fat.” This means if a food package states 0 grams of trans fats, it might still have some trans fats if the amount per serving is less than 0.5 g. You can also spot trans fats by reading ingredient lists and looking for the ingredients referred to as “partially hydrogenated oils.”
Salt
Salt or sodium is a mineral that’s essential for life. Table salt is a combination of two minerals — about 40% sodium and 60% chloride. Salt or sodium is regulated by your kidneys, and it helps control your body’s fluid balance. It also helps send nerve impulses and affects muscle function. High levels of salt in your diet can increase blood pressure. High blood pressure is known as the “silent killer” because its symptoms are not always obvious. It’s one of the major risk factors for heart disease, the No. 1 killer worldwide. Ninety percent of American adults are expected to develop high blood pressure over their lifetimes. Because high blood pressure is an important risk factor for stroke, and strokes are detrimental to cognitive health, excessive salt intake is harmful for your brain health. There is a well-established relationship between consuming high levels of sodium and risk of stroke. In Japan, a public health education intervention in the 1960s showed the effectiveness of dietary interventions to reduce sodium intake. A 50% reduction in salt in the diet was associated with an 85% reduction in mortality caused by stroke.
Most of the salt that you eat is added to processed foods. More than 70% of the sodium you consume comes from packaged, prepared and restaurant foods. The rest of the sodium in the diet occurs naturally in food (about 15 percent) or is added when we’re cooking food or sitting down to eat (about 11 percent). Current recommendations from the Dietary Guidelines for Americans are to limit sodium intake to 2,300 milligrams (mg) a day, which amounts to about one teaspoon of salt. The American Heart Association recommends an ideal limit of no more than 1,500 mg per day for most adults. On average, Americans eat more than 3,400 milligrams of sodium each day — much more than the American Heart Association and other health organizations recommend. Because the average American eats so much excess sodium, even cutting back by 1,000 milligrams a day can significantly improve blood pressure and heart health. One estimate suggested that if the U.S. population dropped its sodium intake to 1,500 mg/day (1/2 teaspoon salt), overall blood pressure could decrease by 25.6%, with an estimated $26.2 billion in health care savings. Another estimate projected that achieving this goal would reduce cardiovascular disease deaths by anywhere from 500,000 to nearly 1.2 million over the next decade.
Here are the approximate amounts of sodium in a given amount of salt:
- 1/4 teaspoon salt = 575 mg sodium
- 1/2 teaspoon salt = 1,150 mg sodium
- 3/4 teaspoon salt = 1,725 mg sodium
- 1 teaspoon salt = 2,300 mg sodium
The body needs only a small amount of sodium (less than 500 milligrams per day) to function properly. That’s a mere smidgen — the amount in less than ¼ teaspoon. Very few people come close to eating less than that amount. Plus, healthy kidneys are great at retaining the sodium that your body needs.
Best heart healthy diet
The typical, contemporary Western diet (high in salt, sugar, excess calories, and saturated fats) is not good for the heart. Eating a heart-healthy diet benefits both your body and your heart. In general, best diet for your heart and arteries is lower in saturated fats. Research in the area of the relationship between diet and your heart point to the benefits of two diets in particular: the DASH (Dietary Approaches to Stop Hypertension) diet and the Mediterranean diet. A plant-based diet that is rich in a variety of fruits and vegetables, particularly green-leafy vegetables and berries, is associated with better heart health. Specific foods (such as olive oil), and particular nutritional supplements (including phenolic compounds like curcumin and quercetin) that may also prove effective for Alzheimer’s disease prevention. These diets can help reduce heart disease and may also be able to reduce risk of dementia.
- Dietary Approaches to Stop Hypertension (DASH) diet
- The DASH diet aims to reduce blood pressure by:
- Eating foods that are low in saturated fat, total fat and cholesterol, and high in fruits, vegetables and low-fat dairy.
- Consuming whole grains, poultry, fish and nuts.
- Decreasing your intake of saturated fats, red meats, sweets, sugared beverages and sodium.
- The DASH diet aims to reduce blood pressure by:
- Mediterranean diet
- The Mediterranean diet incorporates different principles of healthy eating that are typically found in the areas bordering the Mediterranean Sea.
- Focusing on fruit, vegetables, nuts and grains.
- Replacing butter with healthy fats, like olive oil.
- Limiting red meat.
- Using herbs to flavor food rather than salt.
- Eating fish and poultry at least twice a week.
- The Mediterranean diet incorporates different principles of healthy eating that are typically found in the areas bordering the Mediterranean Sea.
Mediterranean diet
“Mediterranean diet” is a generic term based on the traditional eating habits in the countries bordering the Mediterranean Sea 51. There’s not one standard Mediterranean diet. At least 16 countries border the Mediterranean. Eating styles vary among these countries and even among regions within each country because of differences in culture, ethnic background, religion, economy, geography and agricultural production 52. However, there are some common factors. Mediterranean diet is low in saturated fat and high in fiber 53.
A Mediterranean-style diet typically includes:
- plenty of fruits, vegetables, bread and other grains, potatoes, beans, nuts and seeds are eaten daily and make up the majority of food consumed;
- olive oil as a primary fat source, may account for up to 40% of daily calories; and
- small portions of cheese or yogurt are usually eaten each day, along with a serving of fish, poultry, or eggs.
Fish and poultry are more common than red meat in the Mediterranean diet. The Mediterranean diet also centers on minimally processed, plant-based foods. Wine may be consumed in low to moderate amounts, usually with meals. Fruit is a common dessert instead of sweets.
Main meals consumed daily should be a combination of three elements: cereals, vegetables and fruits, and a small quantity of legumes, beans or other (though not in every meal). Cereals in the form of bread, pasta, rice, couscous or bulgur (cracked wheat) should be consumed as one–two servings per meal, preferably using whole or partly refined grains. Vegetable consumption should amount to two or more servings per day, in raw form for at least one of the two main meals (lunch and dinner). Fruit should be considered as the primary form of dessert, with one–two servings per meal. Consuming a variety of colors of both vegetables and fruit is strongly recommended to help ensure intake of a broad range of micronutrients and phytochemicals. The less these foods are cooked, the higher the retention of vitamins and the lower use of fuel, thus minimizing environmental impact.
The Mediterranean Diet is associated with a lower incidence of mortality from all-causes 54 and is also related to lower incidence of cardiovascular diseases 55, type 2 diabetes 56, certain types of cancer 57, and neurodegenerative diseases 58. The Mediterranean diet is now recognized as one of the most healthy food patterns in the world.
Year after year, the Mediterranean diet comes out on top in the U.S. News and World Report annual ranking of best diets. The Mediterranean diet is also touted as one of the healthiest by many health organizations and dietitians 59.
A Mediterranean-style diet is a healthy dietary pattern that:
- emphasizes vegetables, fruits, whole grains, beans and legumes;
- includes low-fat or fat-free dairy products, fish, poultry, non-tropical vegetable oils and nuts; and
- limits added sugars, sugary beverages, sodium, highly processed foods, refined carbohydrates, saturated fats, and fatty or processed meats.
This style of eating can play a big role in preventing heart disease and stroke and reducing risk factors such as obesity, diabetes, high cholesterol and high blood pressure. There is some evidence that a Mediterranean diet rich in virgin olive oil may help the body remove excess cholesterol from arteries and keep blood vessels open.
The Mediterranean Diet is characterized by 60:
- An abundance of plant food (fruit, vegetables, breads, cereals, potatoes, beans, nuts, and seeds);
- Minimally processed, seasonally fresh, locally grown foods;
- Desserts comprised typically of fresh fruit daily and occasional sweets containing refined sugars or honey;
- Olive oil (high in polyunsaturated fat) as the principal source of fat;
- Daily dairy products (mainly cheese and yogurt) in low to moderate amounts;
- Fish and poultry in low to moderate amounts;
- Up to four eggs weekly;
- Red meat rarely; and
- Wine in low to moderate amounts with meals.
Here are some things you can do to switch from a traditional Western-style diet to a more Mediterranean way of eating.
- Dip bread in a mix of olive oil and fresh herbs instead of using butter.
- Add avocado slices to your sandwich instead of bacon.
- Have fish for lunch or dinner instead of red meat. Brush it with olive oil, and broil or grill it.
- Sprinkle your salad with seeds or nuts instead of cheese.
- Cook with olive or canola oil instead of butter or oils that are high in saturated fat.
- Choose whole-grain bread, pasta, rice, and flour instead of foods made with white flour.
- Add ground flaxseed to cereal, low-fat yogurt, and soups.
- Cut back on meat in meals. Instead of having pasta with meat sauce, try pasta tossed with olive oil and topped with pine nuts and a sprinkle of Parmesan cheese.
- Dip raw vegetables in a vinaigrette dressing or hummus instead of dips made from mayonnaise or sour cream.
- Have a piece of fruit for dessert instead of a piece of cake.
- Use herbs and spices instead of salt to add flavor to foods.

DASH diet
DASH stands for Dietary Approaches to Stop Hypertension is similar to a Mediterranean-type diet 61. DASH diet is an eating plan that is based on research studies sponsored by the National Heart, Lung, and Blood Institute 62. The DASH diet is a lifelong approach to healthy eating that’s designed to help treat or prevent high blood pressure (hypertension). The DASH diet encourages you to reduce the sodium in your diet and eat a variety of foods rich in nutrients that help lower blood pressure, such as potassium, calcium and magnesium and eating foods that are low in saturated fat, total fat, and cholesterol, and high in fruits, vegetables, and low fat dairy foods 63.
DASH Diet is a flexible and balanced eating plan that helps you create a heart-healthy eating style for life.
The DASH diet eating plan requires no special foods and has no hard-to-follow recipes. It simply calls for a certain number of daily servings from various food groups to provide your daily and weekly nutritional goals. The Dietary Approaches to Stop Hypertension (DASH) diet recommends 64:
- Grains and grain products: 7–8 servings per day, more than half of which are whole-grain foods
- Fruits: 4–5 servings per day
- Vegetables: 4–5 servings per day
- Low-fat or non-fat dairy foods: 2–3 servings per day
- Lean meats, fish, poultry: 6 or less servings or fewer per day
- Nuts, seeds, and legumes: 4–5 servings per week
- Added fats and oils: 2–3 servings per day
- Sweets: 5 or less servings per week
- Salt (sodium): 1,500 milligrams (mg) sodium lowers blood pressure even further than 2,300 mg sodium daily.
- Limiting foods that are high in saturated fat, such as fatty meats, full-fat dairy products, and tropical oils such as coconut, palm kernel and palm oils
- Limiting sugar-sweetened beverages and sweets.
The DASH diet eating plan includes vegetables, whole grains, poultry, fish, and nuts, and has low amounts of fats, red meats, sweets, and sugared beverages. It is also high in potassium, calcium and magnesium, as well as protein and fiber. The number of servings depends on the number of calories you’re allowed each day. Your calorie level depends on your age, sex, the amount of lean body mass (muscular, athletic, average or overweight), height and, especially, how active you are. Think of this as an energy balance system—if you want to maintain your current weight, you should take in only as many calories as you burn by being physically active. If you need to lose weight, eat fewer calories than you burn or increase your activity level to burn more calories than you eat.
The DASH dietary approach has been shown to lower blood pressure, but little has been published regarding weight loss 61. In fact, a systematic review and meta-analysis on observational prospective studies on the effects of Dietary Approaches to Stop Hypertension (DASH)-style diet, showed that the DASH diet can significantly protect against cardiovascular diseases, coronary heart disease, stroke, and heart failure risk by 20%, 21%, 19% and 29%, respectively 65, 66.
Blood pressure is usually measured in millimeters of mercury (mmHg) and is recorded as two numbers—systolic pressure (as the heart beats) “over” diastolic pressure (as the heart relaxes between beats)—for example, 120/80 mmHg. Both numbers in a blood pressure test are important, but for people who are age 50 or older, systolic pressure gives the most accurate diagnosis of high blood pressure. Systolic pressure is the top number in a blood pressure reading. It is high if it is 140 mmHg or above 67.
High blood pressure is blood pressure higher than 140/90 mmHg and prehypertension is blood pressure between 120/80 and 139/89 mmHg. Prehypertension means that you don’t have high blood pressure now, but are likely to develop it in the future unless you adopt the healthy lifestyle. High blood pressure is dangerous because it makes your heart work too hard, hardens the walls of your arteries, and can cause the brain to hemorrhage or the kidneys to function poorly or not at all. If not controlled, high blood pressure can lead to heart and kidney disease, stroke and blindness.
Being overweight or obese increases your risk of developing high blood pressure. In fact, your blood pressure rises as your body weight increases. Losing even 10 pounds can lower your blood pressure and losing weight has the biggest effect on those who are overweight and already have hypertension. Overweight and obesity are also risk factors for heart disease. And being overweight or obese increases your chances of developing high blood cholesterol and diabetes—two
more risk factors for heart disease.
The original DASH trial 68 consisted of 459 subjects with systolic blood pressures <160 mm Hg and diastolic blood pressures between 80 and 95 mm Hg. For three weeks, all participants were fed a control diet low in fruits, vegetables, and dairy products, and with a fat content typical of an American diet (37% of daily caloric intake). During the following eight weeks, the participants were randomized to one of three diets: the control diet, a diet rich in fruits and vegetables, or the DASH Diet.
The DASH Diet was not low in sodium (salt), but still reduced blood pressure. A meta-analysis of 56 randomized, controlled trials that included over 3,500 participants did not support universal sodium restriction, but instead only recommended dietary sodium restriction in the elderly 69.
The DASH Diet reduced systolic blood pressure by 5.5 mm Hg and diastolic blood pressure by 3.3 mm Hg, as compared with controls. Subgroup analysis showed that African Americans and those with hypertension had the greatest reduction in blood pressure 68 . The DASH diet results might be applied to a larger group due to the heterogeneous population: half of the participants were women, 60% were African American, and 37% had household incomes of <$30,000 per year. One limitation of applying the DASH Diet to the general population is that the study was carried out in a very controlled setting, where all the meals were prepared for the subjects, and thus no comments may be made regarding attrition rates for the diet.
By following the DASH diet, you may be able to reduce your blood pressure by a few points in just two weeks. Over time, your systolic blood pressure could drop by eight to 14 points, which can make a significant difference in your health risks.
Salt or sodium is a mineral that’s essential for life. Table salt is a combination of two minerals — about 40% sodium and 60% chloride. Salt or sodium is regulated by your kidneys, and it helps control your body’s fluid balance. It also helps send nerve impulses and affects muscle function. High levels of salt in your diet can increase blood pressure. High blood pressure is known as the “silent killer” because its symptoms are not always obvious. It’s one of the major risk factors for heart disease, the No. 1 killer worldwide. Ninety percent of American adults are expected to develop high blood pressure over their lifetimes. Because high blood pressure is an important risk factor for stroke, and strokes are detrimental to cognitive health, excessive salt intake is harmful for your brain health. Most of the salt that you eat is added to processed foods. More than 70% of the sodium you consume comes from packaged, prepared and restaurant foods. The rest of the sodium in the diet occurs naturally in food (about 15 percent) or is added when we’re cooking food or sitting down to eat (about 11 percent). The American Heart Association recommends no more than 2,300 milligrams (mg) a day and moving toward an ideal limit of no more than 1,500 mg per day for most adults. On average, Americans eat more than 3,400 milligrams of sodium each day — much more than the American Heart Association and other health organizations recommend. Because the average American eats so much excess sodium, even cutting back by 1,000 milligrams a day can significantly improve blood pressure and heart health. One estimate suggested that if the U.S. population dropped its sodium intake to 1,500 mg/day (1/2 teaspoon salt), overall blood pressure could decrease by 25.6%, with an estimated $26.2 billion in health care savings. Another estimate projected that achieving this goal would reduce cardiovascular disease deaths by anywhere from 500,000 to nearly 1.2 million over the next decade.
Here are the approximate amounts of sodium in a given amount of salt:
- 1/4 teaspoon salt = 575 mg sodium
- 1/2 teaspoon salt = 1,150 mg sodium
- 3/4 teaspoon salt = 1,725 mg sodium
- 1 teaspoon salt = 2,300 mg sodium
The body needs only a small amount of sodium (less than 500 milligrams per day) to function properly. That’s a mere smidgen — the amount in less than ¼ teaspoon. Very few people come close to eating less than that amount. Plus, healthy kidneys are great at retaining the sodium that your body needs.
Table 2. Daily Nutrient Goals Used in the DASH Studies (for a 2,100 Calorie Eating Plan)
| Total fat: 27% of calories | Sodium: 2,300 mg* |
| Saturated fat: 6% of calories | Potassium: 4,700 mg |
| Protein: 18% of calories | Calcium: 1,250 mg |
| Carbohydrate: 55% of calories | Magnesium: 500 mg |
| Cholesterol: 150 mg | Fiber: 30 g |
Footnote: 1,500 mg sodium* was a lower goal tested and found to be even better for lowering blood pressure. It was particularly effective for middle-aged and older individuals, African Americans, and those who already had high blood pressure. The American Heart Association recommends no more than 2,300 milligrams (mg) a day and moving toward an ideal limit of no more than 1,500 mg per day for most adults. On average, Americans eat more than 3,400 milligrams of sodium each day — much more than the American Heart Association and other health organizations recommend. Because the average American eats so much excess sodium, even cutting back by 1,000 milligrams a day can significantly improve blood pressure and heart health.
Abbreviations: g = grams; mg = milligrams
[Source 70 ]Exercise and Physical Activity
Exercise and physical activity are good for just about everyone. The American Heart Association recommends adults get at least 150 minutes per week of moderate-intensity aerobic activity or 75 minutes per week of vigorous aerobic activity (or a combination of both), preferably spread throughout the week. Any activity is better than none. Even light-intensity activity can offset the serious health risks of being sedentary. Moderate to vigorous aerobic exercise is best. Your heart will beat faster, and you’ll breathe harder than normal. As you get used to being more active, increase your time and/or intensity to get more benefits. Include moderate- to high-intensity muscle-strengthening activity (like resistance or weight training) at least twice a week.
Staying active can help you:
- Keep and improve your strength so you can stay independent
- Have more energy to do the things you want to do and reduce fatigue
- Improve your balance and lower risk of falls and injuries from falls
- Manage and prevent some diseases like arthritis, heart disease, stroke, type 2 diabetes, osteoporosis, and 8 types of cancer, including breast and colon cancer
- Sleep better at home
- Reduce levels of stress and anxiety
- Reach or maintain a healthy weight and reduce risk of excessive weight gain
- Control your blood pressure
- Possibly improve or maintain some aspects of cognitive function, such as your ability to shift quickly between tasks or plan an activity
- Perk up your mood and reduce feelings of depression
Research has shown that exercise is not only good for your physical health, it also supports emotional and mental health. You can exercise with a friend and get the added benefit of emotional support. So, next time you’re feeling down, anxious, or stressed, try to get up and start moving.
Physical activity can help:
- Reduce feelings of depression and stress, while improving your mood and overall emotional well-being
- Increase your energy level
- Improve sleep
- Empower you to feel more in control
In addition, exercise and physical activity may possibly improve or maintain some aspects of cognitive function, such as your ability to shift quickly between tasks, plan an activity, and ignore irrelevant information.
Most people tend to focus on one type of exercise or activity and think they’re doing enough. Research has shown that it’s important to get all 4 types of exercise:
- Endurance
- Strength
- Balance
- Flexibility.
Each one has different benefits. Doing one kind also can improve your ability to do the others, and variety helps reduce boredom and risk of injury. No matter your age, you can find activities that meet your fitness level and needs.
The Department of Health and Human Services recommends these exercise guidelines for most healthy adults:
- AEROBIC activity. Get at least 150 minutes a week of moderate aerobic activity — such as brisk walking, swimming or mowing the lawn — or 75 minutes a week of vigorous aerobic activity — such as running or aerobic dancing. You can also do a combination of moderate and vigorous activity. It’s best to do this over the course of a week.
- STRENGTH training. Strength train at least twice a week. Consider free weights, weight machines or activities that use your own body weight — such as rock climbing or heavy gardening. The amount of time for each session is up to you.
Endurance exercises
Endurance activities, often referred to as aerobic, increase your breathing and heart rates. These activities help keep you healthy, improve your fitness, and help you perform the tasks you need to do every day. Endurance exercises improve the health of your heart, lungs, and circulatory system. They also can delay or prevent many diseases that are common in older adults such as diabetes, colon and breast cancers, heart disease, and others.
Physical activities that build endurance include:
- Brisk walking or jogging
- Yard work (mowing, raking)
- Dancing
- Swimming
- Biking
- Climbing stairs or hills
- Playing tennis or basketball
Increase your endurance or “staying power” to help keep up with your grandchildren during a trip to the park, dance to your favorite songs at a family wedding, and rake the yard and bag up leaves. Build up to at least 150 minutes of activity a week that makes you breathe hard. Try to be active throughout your day to reach this goal and avoid sitting for long periods of time.
Safety tips
- Do a little light activity, such as easy walking, before and after your endurance activities to warm up and cool down.
- Listen to your body: endurance activities should not cause dizziness, chest pain or pressure, or a feeling like heartburn.
- Be sure to drink liquids when doing any activity that makes you sweat. If your doctor has told you to limit your fluids, be sure to check before increasing the amount of fluid you drink while exercising.
- If you are going to be exercising outdoors, be aware of your surroundings.
- Dress in layers so you can add or remove clothes as needed for hot and cold weather.
- To prevent injuries, use safety equipment, such as a helmet when bicycling.
Strength exercises
Some people call using weight to improve your muscle strength “strength training” or “resistance training.” Your muscular strength can make a big difference. Strong muscles help you stay independent and make everyday activities feel easier, like getting up from a chair, climbing stairs, and carrying groceries. Keeping your muscles strong can help with your balance and prevent falls and fall-related injuries. You are less likely to fall when your leg and hip muscles are strong.
Some people choose to use weights to help improve their strength. If you do, start by using light weights at first, then gradually add more. Other people use resistance bands, stretchy elastic bands that come in varying strengths. If you are a beginner, try exercising without the band or use a light band until you are comfortable. Add a band or move on to a stronger band (or more weight) when you can do two sets of 10 to 15 repetitions easily. Try to do strength exercises for all of your major muscle groups at least 2 days per week, but don’t exercise the same muscle group on any 2 days in a row. Below are a few examples of strength exercises:
- Lifting weights
- Carrying groceries
- Gripping a tennis ball
- Overhead arm curl
- Arm curls
- Wall push-ups
- Lifting your body weight
- Using a resistance band
Safety tips:
- Don’t hold your breath during strength exercises and breathe regularly.
- Breathe out as you lift or push, and breathe in as you relax.
- Talk with your doctor if you are unsure about doing a particular exercise.
Balance exercises
Balance exercises help prevent falls, a common problem in older adults that can have serious consequences. Many lower-body strength exercises also will improve your balance. Balance exercises include:
- Tai Chi, a “moving meditation” that involves shifting the body slowly, gently, and precisely, while breathing deeply.
- Standing on one foot.
- The heel-to-toe walk.
- The balance walk.
- Standing from a seated position.
Safety tips:
- Have a sturdy chair or a person nearby to hold on to if you feel unsteady.
- Talk with your doctor if you are unsure about a particular exercise.
Flexibility exercises
Stretching can improve your flexibility. Moving more freely will make it easier for you to reach down to tie your shoes or look over your shoulder when you back your car out of the driveway. Flexibility exercises include:
- The back stretch exercise
- The inner thigh stretch
- The ankle stretch
- The back of leg stretch
Safety tips:
- Stretch when your muscles are warmed up.
- Stretch after endurance or strength exercises.
- Don’t stretch so far that it hurts.
- Always remember to breathe normally while holding a stretch.
- Talk with your doctor if you are unsure about a particular exercise.
- American Heart Association. About Arrhythmia. http://www.heart.org/HEARTORG/Conditions/Arrhythmia/AboutArrhythmia/About-Arrhythmia_UCM_002010_Article.jsp
- Centers for Disease Control and Prevention. Division of Birth Defects and Developmental Disabilities. Congenital Heart Defects (CHDs). https://www.cdc.gov/ncbddd/heartdefects/index.html
- National Institutes of Health. National Heart, Lung and Blood Institute. Your Heart’s Electrical System. https://www.nhlbi.nih.gov/health/health-topics/topics/hhw/electrical
- Dowse GK, Gareebo H, Alberti KG, Zimmet P, Tuomilehto J, Purran A, Fareed D, Chitson P, Collins VR. Changes in population cholesterol concentrations and other cardiovascular risk factor levels after five years of the Non-communicable Disease Intervention Programme in Mauritius. BMJ. 1995; 311: 1255–1259. http://www.bmj.com/content/311/7015/1255
- http://www.bmj.com/content/313/7064/1044
- Chiuve SE, Rexrode KM, D. S, Logroscino G, Manson JE, Rimm EB. Primary prevention of stroke by healthy lifestyle. Circulation. 2008;118:947-54. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2730914/
- Chiuve SE, Fung TT, Rexrode KM, et al. Adherence to a low-risk, healthy lifestyle and risk of sudden cardiac death among women. JAMA. 2011;306:62-9. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3210472/
- van Dam RM, Li T, Spiegelman D, Franco OH, Hu FB. Combined impact of lifestyle factors on mortality: prospective cohort study in US women. BMJ. 2008;337:a1440. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2658866/
- Stamler R. Implications of the INTERSALT study. Hypertension. 1991; 17 (suppl): I16–I20. https://www.ncbi.nlm.nih.gov/pubmed/1986996
- US Department of Health and Human Services and US Department of Agriculture. Dietary Guidelines for Americans, 2005. 6th ed. Washington, DC: US Government Printing Office; 2005.
- Johnson RK, Appel LJ, Brands M, Howard BV, Lefevre M, Lustig RH, Sacks F, Steffen LM, Wylie-Rosett J; on behalf of the American Heart Association Nutrition Committee of the Council on Nutrition, Physical Activity, and Metabolism and the Council on Epidemiology and Prevention. Dietary sugars intake and cardiovascular health: a scientific statement from the American Heart Association. Circulation. 2009; 120: 1011–1020. http://circ.ahajournals.org/content/120/11/1011
- Lloyd-Jones DM, Hong Y, Labarthe D, et al. Defining and setting national goals for cardiovascular health promotion and disease reduction: the American Heart Association’s strategic Impact Goal through 2020 and beyond. Circulation. 2010;121:586-613. http://circ.ahajournals.org/content/121/4/586.long
- National Institutes of Health. National Institute of Aging. Heart Health. https://www.nia.nih.gov/health/heart-health
- National Institutes of Health. National Institute of Aging. Heart Health. https://www.nia.nih.gov/health/heart-health
- National Institutes of Health. High Blood Pressure. https://www.nhlbi.nih.gov/health/health-topics/topics/hbp/
- Understanding Blood Pressure Readings. https://www.heart.org/en/health-topics/high-blood-pressure/understanding-blood-pressure-readings
- American Heart Association. Target Heart Rates. http://www.heart.org/HEARTORG/HealthyLiving/PhysicalActivity/FitnessBasics/Target-Heart-Rates_UCM_434341_Article.jsp
- WHO. Diet, nutrition and the prevention of chronic diseases. Report of a Joint FAO, WHO Expert Consultation. WHO Technical Report Series. Geneva: World Helath Organization; 2003.
- Aune D, Giovannucci E, Boffetta P, Fadnes LT, Keum N, Norat T, Greenwood DC, Riboli E, Vatten LJ, Tonstad S. Fruit and vegetable intake and the risk of cardiovascular disease, total cancer and all-cause mortality—a systematic review and dose-response meta-analysis of prospective studies. Int J Epidemiol. 2017;46(3):1029–1056. doi: 10.1093/ije/dyw319
- Davis B.A., Prall B.C. The challenges of incorporation of omega-3 fatty acids into ration components and their prevalence in garrison feeding. Military medicine. 2014;179:162–167. doi: 10.7205/MILMED-D-14-00172
- Bailes J.E., Patel V. The potential for DHA to mitigate mild traumatic brain injury. Mil. Med. 2014;179:112–116. doi: 10.7205/MILMED-D-14-00139
- Michael I McBurney, Nathan L Tintle, Ramachandran S Vasan, Aleix Sala-Vila, William S Harris, Using an erythrocyte fatty acid fingerprint to predict risk of all-cause mortality: the Framingham Offspring Cohort, The American Journal of Clinical Nutrition, 2021;, nqab195, https://doi.org/10.1093/ajcn/nqab195
- Fish and Omega-3 Fatty Acids. https://www.heart.org/en/healthy-living/healthy-eating/eat-smart/fats/fish-and-omega-3-fatty-acids
- Devore, E. E., Kang, J. H., Breteler, M. M., & Grodstein, F. (2012). Dietary intakes of berries and flavonoids in relation to cognitive decline. Annals of neurology, 72(1), 135–143. https://doi.org/10.1002/ana.23594
- Mink PJ, Scrafford CG, Barraj LM, Harnack L, Hong CP, Nettleton JA, Jacobs DR., Jr Flavonoid intake and cardiovascular disease mortality: a prospective study in postmenopausal women. Am J Clin Nutr. 2007;85(3):895–909. doi: 10.1093/ajcn/85.3.895
- https://www.dietaryguidelines.gov/sites/default/files/2020-12/Dietary_Guidelines_for_Americans_2020-2025.pdf
- U.S. Department of Agriculture and U.S. Department of Health and Human Services. Dietary Guidelines for Americans, 2015-2020. https://health.gov/sites/default/files/2019-09/2015-2020_Dietary_Guidelines.pdf
- The Skinny on Fats. https://www.heart.org/en/health-topics/cholesterol/prevention-and-treatment-of-high-cholesterol-hyperlipidemia/the-skinny-on-fats
- Jakobsen, M.U., et al., Intake of carbohydrates compared with intake of saturated fatty acids and risk of myocardial infarction: importance of the glycemic index. Am J Clin Nutr, 2010. 91(6): p. 1764-8.
- Institute of Medicine, Food and Nutrition Board. Dietary reference intakes for energy, carbohydrate, fiber, fat, fatty acids, cholesterol, protein, and amino acids (macronutrients). Washington, DC: National Academy Press; 2005.
- Jones PJH, Rideout T. Lipids, sterols, and their metabolites. In: Ross AC, Caballero B, Cousins RJ, Tucker KL, Ziegler TR, eds. Modern Nutrition in Health and Disease. 11th ed. Baltimore, MD: Lippincott Williams & Wilkins; 2014.
- Jones PJH, Papamandjaris AA. Lipids: cellular metabolism. In: Erdman JW, Macdonald IA, Zeisel SH, eds. Present Knowledge in Nutrition. 10th ed. Washington, DC: Wiley-Blackwell; 2012:132-48.
- Harris WS. Omega-3 fatty acids. In: Coates PM, Betz JM, Blackman MR, et al., eds. Encyclopedia of Dietary Supplements. 2nd ed. London and New York: Informa Healthcare; 2010:577-86.
- Simopoulos AP. The importance of the omega-6/omega-3 fatty acid ratio in cardiovascular disease and other chronic diseases. Exp Biol Med (Maywood). 2008 Jun;233(6):674-88. doi: 10.3181/0711-MR-311
- Wang C, Chung M, Lichtenstein A, Balk E, Kupelnick B, DeVine D, et al. Effects of omega-3 fatty acids on cardiovascular disease. Summary, evidence report/technology assessment no. 94. (Prepared by the Tufts New England Medical Center Evidence-based Practice Center, Boston, MA.) AHRQ Publication No. 04-E009-1. Agency for Healthcare Research and Quality, 2004. https://archive.ahrq.gov/downloads/pub/evidence/pdf/o3cardio/o3cardio.pdf
- Harris WS, Davidson MH. RE: Plasma phospholipid fatty acids and prostate cancer risk in the SELECT trial. J Natl Cancer Inst. 2014 Apr;106(4):dju019. doi: 10.1093/jnci/dju019
- Brasky TM, Darke AK, Song X, Tangen CM, Goodman PJ, Thompson IM, Meyskens FL Jr, Goodman GE, Minasian LM, Parnes HL, Klein EA, Kristal AR. Plasma phospholipid fatty acids and prostate cancer risk in the SELECT trial. J Natl Cancer Inst. 2013 Aug 7;105(15):1132-41. doi: 10.1093/jnci/djt174
- Harris WS. Are n-3 fatty acids still cardioprotective? Curr Opin Clin Nutr Metab Care. 2013 Mar;16(2):141-9. doi: 10.1097/MCO.0b013e32835bf380
- Agency for Healthcare Research and Quality. Omega-3 fatty acids and cardiovascular disease – 2015. https://effectivehealthcare.ahrq.gov/products/fatty-acids-cardiovascular-disease/research-protocol
- Harris WS. The omega-3 index as a risk factor for coronary heart disease. Am J Clin Nutr. 2008 Jun;87(6):1997S-2002S. doi: 10.1093/ajcn/87.6.1997S
- Metcalf RG, Cleland LG, Gibson RA, Roberts-Thomson KC, Edwards JR, Sanders P, Stuklis R, James MJ, Young GD. Relation between blood and atrial fatty acids in patients undergoing cardiac bypass surgery. Am J Clin Nutr. 2010 Mar;91(3):528-34. doi: 10.3945/ajcn.2009.28302
- James M, Proudman S, Cleland L. Fish oil and rheumatoid arthritis: past, present and future. Proc Nutr Soc. 2010 Aug;69(3):316-23. doi: 10.1017/S0029665110001564
- Abdelhamid AS, Brown TJ, Brainard JS, Biswas P, Thorpe GC, Moore HJ, Deane KH, Summerbell CD, Worthington HV, Song F, Hooper L. Omega-3 fatty acids for the primary and secondary prevention of cardiovascular disease. Cochrane Database Syst Rev. 2020 Feb 29;3(2):CD003177. doi: 10.1002/14651858.CD003177.pub5
- Weylandt KH, Serini S, Chen YQ, Su HM, Lim K, Cittadini A, Calviello G. Omega-3 Polyunsaturated Fatty Acids: The Way Forward in Times of Mixed Evidence. Biomed Res Int. 2015;2015:143109. doi: 10.1155/2015/143109
- Casula M, Soranna D, Catapano AL, Corrao G. Long-term effect of high dose omega-3 fatty acid supplementation for secondary prevention of cardiovascular outcomes: A meta-analysis of randomized, placebo controlled trials [corrected]. Atheroscler Suppl. 2013 Aug;14(2):243-51. doi: 10.1016/S1567-5688(13)70005-9. Erratum in: Atheroscler Suppl. 2014 Mar;233(1):122.
- Agency for Healthcare Research and Quality. Omega-3 fatty acids and cardiovascular disease: an updated systematic review. 2016. https://effectivehealthcare.ahrq.gov/products/fatty-acids-cardiovascular-disease/research
- Siscovick DS, Barringer TA, Fretts AM, Wu JH, Lichtenstein AH, Costello RB, Kris-Etherton PM, Jacobson TA, Engler MB, Alger HM, Appel LJ, Mozaffarian D; American Heart Association Nutrition Committee of the Council on Lifestyle and Cardiometabolic Health; Council on Epidemiology and Prevention; Council on Cardiovascular Disease in the Young; Council on Cardiovascular and Stroke Nursing; and Council on Clinical Cardiology. Omega-3 Polyunsaturated Fatty Acid (Fish Oil) Supplementation and the Prevention of Clinical Cardiovascular Disease: A Science Advisory From the American Heart Association. Circulation. 2017 Apr 11;135(15):e867-e884. doi: 10.1161/CIR.0000000000000482
- National Institutes of Health. Dietary Supplement Label Database. 2015.
- U.S. Food and Drug Administration. Fish: what pregnant women and parents should know. 2014. https://www.fda.gov/food/consumers/advice-about-eating-fish
- ConsumerLab.com. Product review: fish oil and omega-3 fatty acid supplements review (including krill, algae, calamari, green-lipped mussel oil). 2021. https://www.consumerlab.com/reviews/fish-oil-supplements-review/omega3
- Altomare, R., Cacciabaudo, F., Damiano, G., Palumbo, V. D., Gioviale, M. C., Bellavia, M., Tomasello, G., & Lo Monte, A. I. (2013). The mediterranean diet: a history of health. Iranian journal of public health, 42(5), 449–457. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3684452
- Castro-Quezada, I., Román-Viñas, B., & Serra-Majem, L. (2014). The Mediterranean diet and nutritional adequacy: a review. Nutrients, 6(1), 231–248. https://doi.org/10.3390/nu6010231
- Serra-Majem, L., Tomaino, L., Dernini, S., Berry, E. M., Lairon, D., Ngo de la Cruz, J., Bach-Faig, A., Donini, L. M., Medina, F. X., Belahsen, R., Piscopo, S., Capone, R., Aranceta-Bartrina, J., La Vecchia, C., & Trichopoulou, A. (2020). Updating the Mediterranean Diet Pyramid towards Sustainability: Focus on Environmental Concerns. International journal of environmental research and public health, 17(23), 8758. https://doi.org/10.3390/ijerph17238758
- Sofi F., Macchi C., Abbate R., Gensini G.F., Casini A. Mediterranean diet and health. Biofactors. 2013;39:335–342. doi: 10.1002/biof.1096
- Estruch R., Ros E., Salas-Salvadó J., Covas M.I., Corella D., Arós F., Gómez-Gracia E., Ruiz-Gutiérrez V., Fiol M., Lapetra J., et al. Primary prevention of cardiovascular disease with a Mediterranean diet. N. Engl. J. Med. 2013;368:1279–1290. doi: 10.1056/NEJMoa1200303
- Mitrou P.N., Kipnis V., Thiébaut A.C., Reedy J., Subar A.F., Wirfält E., Flood A., Mouw T., Hollenbeck A.R., Leitzmann M.F., et al. Mediterranean dietary pattern and prediction of all-cause mortality in a US population: Results from the NIH-AARP Diet and Health Study. Arch. Intern. Med. 2007;167:2461–2468. doi: 10.1001/archinte.167.22.2461
- Couto E., Boffetta P., Lagiou P., Ferrari P., Buckland G., Overvad K., Dahm C.C., Tjønneland A., Olsen A., Clavel-Chapelon F., et al. Mediterranean dietary pattern and cancer risk in the EPIC cohort. Br. J. Cancer. 2011;104:1493–1499. doi: 10.1038/bjc.2011.106
- Sofi F., Abbate R., Gensini G.F., Casini A. Accruing evidence on benefits of adherence to the Mediterranean diet on health: An updated systematic review and meta-analysis. Am. J. Clin. Nutr. 2010;92:1189–1196. doi: 10.3945/ajcn.2010.29673
- Widmer, R. J., Flammer, A. J., Lerman, L. O., & Lerman, A. (2015). The Mediterranean diet, its components, and cardiovascular disease. The American journal of medicine, 128(3), 229–238. https://doi.org/10.1016/j.amjmed.2014.10.014
- F.B. Hu. The Mediterranean Diet and mortality—olive oil and beyond. N Engl J Med, 348 (2003), pp. 2595-2596
- Journal of the American College of Cardiology Volume 45, Issue 9, 3 May 2005, Pages 1379-1387. Diets and Cardiovascular Disease: An Evidence-Based Assessment. http://www.sciencedirect.com/science/article/pii/S0735109705003670
- National Institutes of Health. National Heart, Blood and Lung Institute. Description of the DASH Eating Plan. https://www.nhlbi.nih.gov/health/health-topics/topics/dash
- National Institutes of Health. National Heart, Blood and Lung Institute. Your Guide To Lowering Your Blood Pressure With DASH. https://www.nhlbi.nih.gov/files/docs/public/heart/dash_brief.pdf
- Sacks FM, Svetkey LP, Vollmer WM, Appel LJ, Bray GA, Harsha D, Obarzanek E, Conlin PR, Miller ER 3rd, Simons-Morton DG, Karanja N, Lin PH; DASH-Sodium Collaborative Research Group. Effects on blood pressure of reduced dietary sodium and the Dietary Approaches to Stop Hypertension (DASH) diet. DASH-Sodium Collaborative Research Group. N Engl J Med. 2001 Jan 4;344(1):3-10. doi: 10.1056/NEJM200101043440101
- Salehi-Abargouei A, Maghsoudi Z, Shirani F, Azadbakht L. Nutrition. 2013 Apr;29(4):611-8. doi: 10.1016/j.nut.2012.12.018. Effects of Dietary Approaches to Stop Hypertension (DASH)-style diet on fatal or nonfatal cardiovascular diseases–incidence: a systematic review and meta-analysis on observational prospective studies. http://www.nutritionjrnl.com/article/S0899-9007(13)00007-5/fulltext
- Fung TT, Chiuve SE, McCullough ML, Rexrode KM, Logroscino G, Hu FB. Adherence to a DASH-style diet and risk of coronary heart disease and stroke in women. Arch Intern Med. 2008 Apr 14;168(7):713-20. PMID: 18413553. http://jamanetwork.com/journals/jamainternalmedicine/fullarticle/414155
- National Institutes of Health. National Heart, Blood and Lung Institute. Your Guide to Lowering Blood Pressure. https://www.nhlbi.nih.gov/files/docs/public/heart/hbp_low.pdf
- L.J. Appel, T.J. Moore, E. Obarzenek, et al.A clinical trial of the effects of dietary patterns on blood pressure. N Engl J Med, 336 (1997), pp. 1117-1124
- J.P. Midgley, A.G. Matthew, C.M. Greenwood, A.G. Logan. Effect of reduced dietary sodium on blood pressure: a meta-analysis of randomized controlled trials. JAMA, 275 (1996), pp. 1590-1597
- National Institutes of Health. National Heart, Blood and Lung Institute. Your Guide to Lowering Blood Pressure with DASH. https://www.nhlbi.nih.gov/files/docs/public/heart/new_dash.pdf