What is mesothelioma
Mesothelioma is a type of cancer that starts in the mesothelium lining that covers the outer surface of some of the body’s organs, especially in the linings of the chest or abdomen. Mesothelioma is an aggressive and deadly form of cancer. Mesothelioma treatments are available, but for many people with mesothelioma, a cure is not possible. Mesothelioma doesn’t include a form of noncancerous (benign) tumor that occurs in the chest and is sometimes called benign mesothelioma or solitary fibrous tumor.
The only known cause of mesothelioma is exposure to asbestos. Most people who get mesothelioma have worked on jobs where they inhaled asbestos particles. It can take just a tiny amount of asbestos to cause mesothelioma, and the disease may take 20 to 60 years to develop. Most cases of mesothelioma result from exposure to asbestos at work. There is also an increased risk of mesothelioma among family members of workers and people living in neighborhoods near asbestos factories and mines. Although the risk of mesothelioma increases with the amount of asbestos exposure, there is no clear safe level of asbestos exposure in terms of mesothelioma risk. Unfortunately, the risk of mesothelioma does not drop with time after exposure to asbestos. The risk appears to be lifelong. Unlike lung cancer, mesothelioma risk is not increased among smokers.
Mesothelioma mainly affects the lining of the lungs (pleural mesothelioma), although it can also affect the lining of the abdomen (peritoneal mesothelioma), heart or testicles.
Most mesothelioma cancer cases are diagnosed in people aged 60-80 and men are affected more commonly than women.
Sometimes it is hard to tell the difference between malignant mesothelioma and lung cancer. Your doctor uses imaging tests and a biopsy to make the diagnosis. Malignant mesothelioma is often found when it is advanced. This makes it harder to treat.
Unfortunately, there is no cure for mesothelioma and it is often not diagnosed until it is quite advanced. Treatment is designed to reduce symptoms and improve quality of life.
Depending on how advanced the mesothelioma is, you might have chemotherapy or radiotherapy to destroy the cancer cells, or surgery to remove the tumor, the pleura and sometimes the diaphragm and part of the lining of the heart.
To control breathlessness and pain, a surgical procedure called VATS pleurodesis is done to drain fluid from the lungs, or from the abdomen. Some people have a drain (a small tube) inserted so that fluid can be removed regularly.
Mesothelioma is fairly rare in the United States, with about 3,000 new cases being diagnosed each year 1.
The rate of mesotheliomas in the United States increased from the 1970s to the early 1990s, but since then it has leveled off and even gone down slightly. These changes have largely been seen in men, and are probably related to changes over time in workplace exposures to asbestos. The rate of mesothelioma is lower in women and has been fairly steady for some time. In many other countries, the rate of mesothelioma is still increasing.
Mesothelioma is more common in whites and Hispanics/Latinos than in African Americans or Asian Americans.
Mesotheliomas are much more common in older people than younger people. The average age at the time of diagnosis for pleural mesothelioma (mesothelioma in the chest) is 69.
Living with mesothelioma
There is no cure for mesothelioma. If you have mesothelioma, you might have periods when you are quite healthy; at other times, you will need treatment to control symptoms.
The mesothelium
A layer of specialized cells called mesothelial cells lines the inside of the chest, the abdomen, and the space around your heart. These cells also cover the outer surface of most of your internal organs. The lining formed by these cells is called the mesothelium (also called the serosa or serous membrane). The mesothelium (serous membranes) produce watery serous fluid, which arises from the blood and derives its name from the fact that it is similar to blood serum in composition.
The mesothelium helps protect your organs by making a special lubricating fluid that allows organs to move against each other. For example, this fluid makes it easier for your lungs to move (expand and contract) inside the chest when you breathe. The mesothelium has different names in different parts of the body:
- The pleura coats the lungs and the space in the chest containing the lungs.
- The peritoneum lines the inside of the abdomen and many of the organs in the abdomen.
- The pericardium covers the heart and creates the space that holds the heart in the chest.
- The tunica vaginalis lines the testicles.
Mesothelial tumors can start in any of these linings. These tumors can be non-cancerous (benign) or cancerous (malignant).
What is asbestos?
Asbestos is a group of minerals that occur naturally as bundles of fibers. These fibers are found in soil and rocks in many parts of the world. They are made mainly of silicon and oxygen, but they also contain other elements. There are 2 main types of asbestos:
- Chrysotile asbestos, also known as white asbestos, is the most common type of asbestos in industrial applications. When looked at under the microscope, chrysotile asbestos fibers wrap around themselves in a spiral, which is why this form of asbestos is also called serpentine or curly asbestos.
- Amphibole asbestos fibers are straight and needle-like. There are several types of amphibole fibers, including amosite (brown asbestos), crocidolite (blue asbestos), tremolite, actinolite, and anthophyllite.
Both types of asbestos have been linked with cancer. All forms of asbestos have been linked to mesothelioma, although amphibole asbestos appears to cause this cancer at lower levels of exposure than chrysotile asbestos.
Evidence from studies in both people and lab animals has shown that asbestos can increase the risk for some types of cancer. When asbestos fibers in the air are inhaled, they can stick to mucus in the throat, trachea (windpipe), or bronchi (large breathing tubes of the lungs) and might be cleared by being coughed up or swallowed. But some fibers reach the ends of the small airways in the lungs or penetrate into the outer lining of the lung and chest wall (known as the pleura). These fibers can irritate the cells in the lung or pleura and eventually cause lung cancer or mesothelioma.
Asbestos fibers can be useful because they are strong, resistant to heat and to many chemicals, and do not conduct electricity. As a result, asbestos has been used as an insulating material since ancient times. Since the industrial revolution, asbestos has been used to insulate factories, schools, homes, and ships, and to make automobile brake and clutch parts, roofing shingles, ceiling and floor tiles, cement, textiles, and hundreds of other products.
During the first half of the 20th century, growing evidence showed that breathing in asbestos caused scarring of the lungs. Exposure to asbestos dust in the workplace was not controlled at that time. Beginning in England in the 1930s, steps were taken to protect workers in the asbestos industry by installing ventilation and exhaust systems. However, in the huge shipbuilding effort during World War II, large numbers of workers were exposed to high levels of asbestos.
As asbestos-related cancers became better recognized in the second half of the 20th century, measures were taken to reduce exposure, including establishing exposure standards and laws that banned the use of asbestos in construction materials. There has been a dramatic decrease in importing and using asbestos in the United States since the mid-1970s, and alternative insulating materials have been developed. As a result, asbestos exposure has dropped dramatically. However, it’s still used in some products, and it’s still possible to be exposed to asbestos in older buildings, water pipes, and other settings. Asbestos use has been banned in the European Union since 2005, although the ban did not require removal of asbestos that was already in place. Still, heavy asbestos use continues in some countries.
Other types of cancer
Studies have also found clear links between workplace exposure to asbestos and cancers of the larynx (voice box) and ovaries.
Some studies have also suggested that workplace asbestos exposure may be linked to other cancers, including cancers of the pharynx (throat), stomach, colon, and rectum. However, the link between these cancers and asbestos is not as clear as it is for the other cancers discussed here. For cancer of the throat, the link is strongest for the hypopharynx, the part of the throat closest to the larynx (voice box). It’s not clear exactly how asbestos might affect risk for these cancers, but swallowed asbestos fibers might somehow contribute to the risk.
How are people exposed to asbestos?
People can be exposed to asbestos in different ways:
- Inhaling asbestos: Most exposures come from inhaling asbestos fibers in the air. This can occur during the mining and processing of asbestos, when making asbestos-containing products, or when installing asbestos insulation. It can also occur when older buildings are demolished or renovated, or when older asbestos-containing materials begin to break down. In any of these situations, asbestos fibers tend to create a dust made of tiny particles that can float in the air.
- Swallowing asbestos: Asbestos fibers can also be swallowed. This can happen when people consume contaminated food or liquids (such as water that flows through asbestos cement pipes). It can also occur when people cough up asbestos they have inhaled, and then swallow their saliva.
Many people are exposed to very low levels of naturally occurring asbestos in outdoor air as a result of erosion of asbestos-containing rocks. The risk of this is higher in areas where rocks have higher asbestos content. In some areas, asbestos can be detected in the water supply as well as in the air. It can get into the water through several sources, such as rock or soil erosion, corrosion of asbestos cement pipes, or the breakdown of roofing materials containing asbestos that then enter the sewers after it rains.
However, the people with the heaviest exposure are those who worked in asbestos industries, such as shipbuilding and insulation. Many of these people recall working in thick clouds of asbestos dust, day after day.
Family members of asbestos workers can also be exposed to high levels of asbestos because the fibers can be carried home on the workers’ clothing, and can then be inhaled by others in the household.
Asbestos exposure is also a concern in older buildings. If building materials that contain asbestos (like older insulation and ceiling and floor tiles) begin to decompose over time, asbestos fibers can be found in indoor air and may pose a health threat. There is no health risk if the asbestos is bonded into intact finished products, such as walls and tiles. As long as the material is not damaged or disturbed (for example, by drilling or remodeling), the fibers are not released into the air. Maintenance workers who sweep up and dispose of the asbestos dust or handle damaged asbestos-containing materials are often exposed to higher levels than other people in these buildings. Removing asbestos from homes and other buildings can also cause some exposure, although modern asbestos abatement workers are trained to use proper protective equipment to minimize exposure.
Although use of asbestos has declined in the United States, people can still be exposed to asbestos in the workplace. In recent years, the US Occupational Health and Safety Administration (OSHA) has estimated that over a million American employees in construction and general industries face significant asbestos exposure on the job.
The mining and use of asbestos is also still a health hazard in some other parts of the world. Mining in the Russian Federation, China, Kazakhstan, Brazil, Canada, and Zimbabwe accounts for almost all of the world production of asbestos. Much of what is produced is used in the Russian Federation (and other countries in the former Soviet Union) and Asia, and its use is on the rise in some areas. In 2005, the World Health Organization estimated that about 125 million people worldwide were exposed to asbestos at work, despite the known links to cancer and other lung diseases for more than 60 years.
Does asbestos cause any other health problems?
The major health problem caused by asbestos exposure, aside from cancer, is a lung disease called asbestosis. When a person breathes high levels of asbestos over time, some of the fibers lodge deep in the lungs. Irritation caused by the fibers can eventually lead to scarring (fibrosis) in the lungs. This can make it hard to breathe. The main symptoms of asbestosis are shortness of breath and a chronic cough.
When asbestosis occurs, it is typically 10 to 20 years after the initial exposure to asbestos. The disease can get worse over time. While some people may not have serious symptoms, others may be seriously disabled by breathing problems. Unfortunately there is no effective treatment for this disease.
Asbestos can also reach the outer lining of the lungs (pleura), where it can cause pleural plaques (areas of hard, scar-like tissue in the pleura), pleural thickening, and pleural effusions (buildup of fluid between the lungs and the pleura). All of these conditions can make it harder to breathe.
What should I do if I’ve been exposed to asbestos?
If you’ve been exposed to asbestos, it’s important to assess the amount of your exposure. If you were exposed only very briefly, or only at very low levels, your risk of a resulting disease is probably low. However, it you were exposed at high levels or for long periods of time, you may be at increased risk of certain cancers or the other diseases discussed above. You can help protect your health in several ways:
- If you are a smoker, it’s very important that you try to stop smoking. Evidence suggests that asbestos-exposed workers who quit smoking can significantly reduce their risk of developing lung cancer.
- Talk to your doctor about whether you should get regular health checkups to look for signs of asbestos-related diseases. This is especially important if you are a smoker. You may want to ask about seeing a doctor experienced with asbestos-related diseases. Some doctors recommend that people with heavy asbestos exposure get regular chest x-rays or CT scans and lung function tests. These tests can’t detect asbestos fibers themselves, but they can sometimes find problems, including some cancers, that could be caused by the fibers. In fact, some expert groups advise that asbestos exposure alone is enough to consider getting regular CT scans to screen for lung cancer, regardless of a person’s smoking history.
- Tell your doctor if you start to have symptoms that might be related to asbestos exposure such as shortness of breath, a new or worsening cough, coughing up blood, pain or tightness in the chest, trouble swallowing, or unintended weight loss. See your doctor promptly for any respiratory illness.
- Ask your doctor about getting vaccines against flu and pneumonia.
If you’ve already been diagnosed with an asbestos-related disease, there are some places you may be able to go for financial help with treatment. Some people with asbestos-related illness may be eligible for Medicare coverage. Some people also may qualify for help, including medical payments, under different workers’ compensation programs. These can include state workers compensation programs, the Federal Employees’ Compensation Program, and the Longshore and Harbor Workers’ Compensation Program. Eligible veterans may receive health care at a Department of Veterans Affairs (VA) Medical Center for asbestos-related diseases.
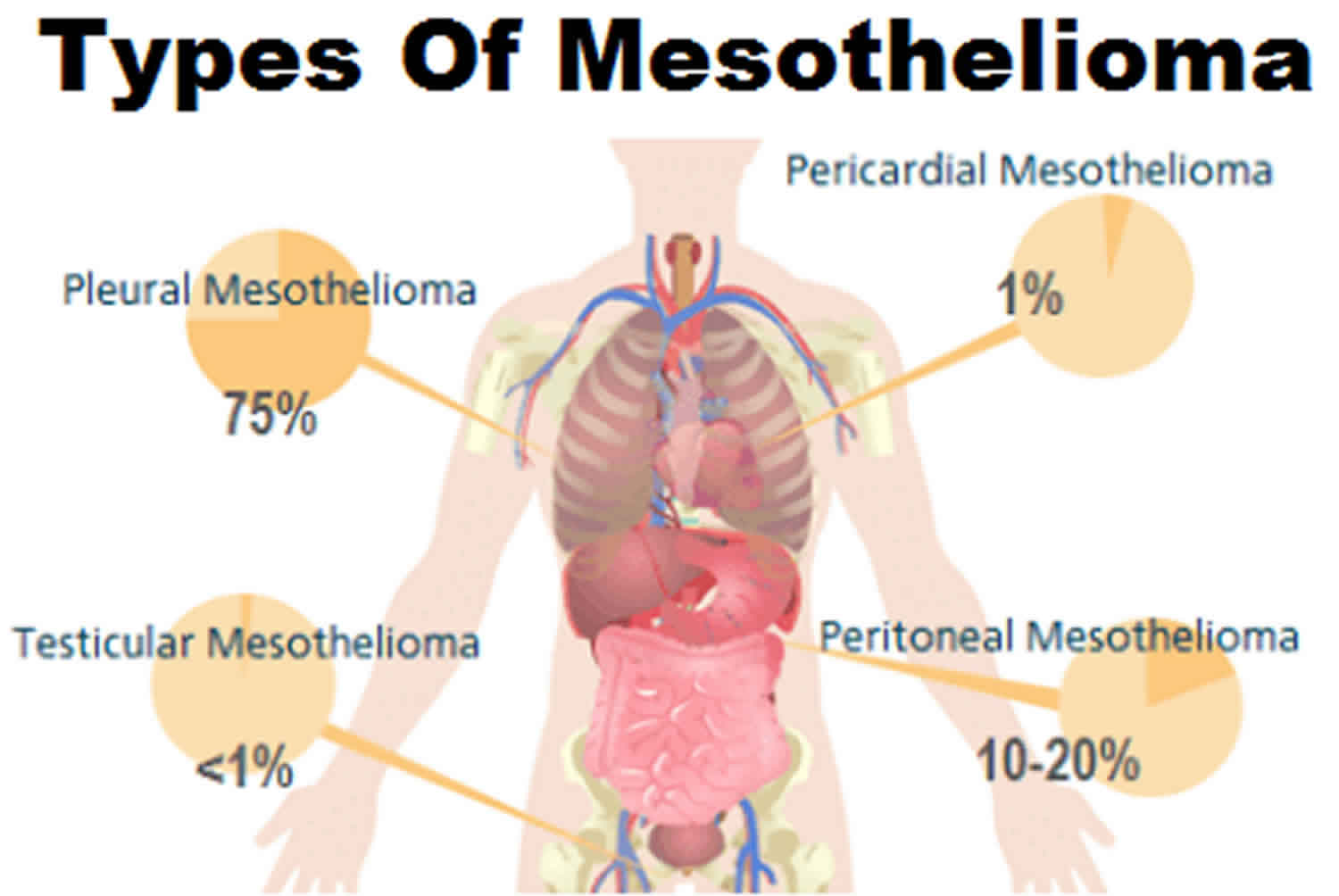
Types of mesothelioma
Mesothelioma grows in the mesothelial cells (epithelial cells of the serous membrane), which are found in the membranes that surround most organs in the body.
There are 2 main types of mesothelioma are:
- Pleural mesothelioma: This type develops in the lining of the lungs, called the pleura. It is the most common form of mesothelioma, accounting for about 9 out of 10 cases. It is different from lung cancer.
- Peritoneal mesothelioma: This develops in the lining of the abdomen (tummy).
Sometimes, mesothelioma can develop in the lining of the heart (pericardial mesothelioma) or in the membrane around the testicles (mesothelioma of the tunica vaginalis).
Malignant mesothelioma
A cancerous tumor of the mesothelium is called a malignant mesothelioma, although this is often shortened to just mesothelioma. Mesotheliomas can start in 4 main areas in the body.
- Pleural mesotheliomas start in the chest. About 3 out of 4 mesotheliomas are pleural mesotheliomas.
- Peritoneal mesotheliomas begin in the abdomen. They make up most of the remaining cases.
- Pericardial mesotheliomas start in the covering around the heart and are very rare.
- Mesotheliomas of the tunica vaginalis are very rare tumors that start in the covering layer of the testicles.
Malignant mesotheliomas can also be classified into 3 main types based on how the cancer cells are arranged:
- About half of mesotheliomas are epithelioid. This type tends to have a better outlook (prognosis) than the other types.
- About 10% of mesotheliomas are sarcomatoid (fibrous).
- Mixed (biphasic) mesotheliomas have both epithelioid and sarcomatoid areas. They make up the remaining 30% to 40% of mesotheliomas.
Benign tumors of the mesothelium
Benign (non-cancerous) tumors can also start in the mesothelium. These tumors are typically removed by surgery, and there is often no need for additional treatment.
Note: Mesothelioma doesn’t include benign mesothelioma or solitary fibrous tumor.
Localized fibrous tumor of the pleura
This type of benign tumor can form in the pleura surrounding the lungs. It used to be called benign fibrous mesothelioma, but doctors now know that this tumor actually does not start in mesothelial cells. This disease is usually benign, but about 1 in 10 are cancerous. A similar condition that starts in the peritoneum is called solitary fibrous tumor of the peritoneum.
Adenomatoid mesothelioma
This benign tumor can develop in the mesothelium of certain reproductive organs. In men, it often starts in the epididymis (ducts that carry sperm cells out of the testicle). In women, this tumor can begin in the fallopian tubes (tubes that carry eggs from the ovaries to the uterus).
Benign cystic mesothelioma
This rare non-cancerous tumor often begins in the peritoneum.
Mesothelioma causes
Researchers have found several factors that increase a person’s risk of mesothelioma, but it’s not yet clear exactly how all of these factors might cause this cancer.
Cancers, including mesotheliomas, occur when cells in the body suffer damage to their DNA. DNA is the chemical in each of our cells that makes up our genes – the instructions for how our cells function. We usually look like our parents because they are the source of our DNA. But DNA affects more than how we look. Some genes control when cells in the body grow, divide into new cells, and die at the right time. Changes in these genes may cause cells to grow out of control, which can lead to cancer.
Asbestos exposure is the main cause of pleural mesothelioma. When asbestos fibers are breathed in, they travel to the ends of small air passages and reach the pleura, where they can cause inflammation and scarring. This may damage cells’ DNA and cause changes that result in uncontrolled cell growth. If swallowed, these fibers can reach the abdominal lining, where they can have a role in causing peritoneal mesothelioma.
But most people exposed to asbestos, even in large amounts, do not get mesothelioma. Other factors, such as a person’s genes, may make them more likely to develop mesothelioma when exposed to asbestos. For example, researchers have found that some people who seem to be at high risk have changes in BAP1, a gene that normally helps keep cell growth under control. Other genes are probably important as well.
Radiation treatments for other cancers have been linked to mesothelioma in some studies. Radiation can damage the cells’ DNA, leading to out-of-control cell growth.
It is still not known if infection with the SV40 virus increases the risk of mesothelioma, or exactly how it might do so. In lab studies, researchers have found that the virus can affect certain genes that have been linked with cancer, but further research in this area is needed.
Risk factors for malignant mesothelioma
A risk factor is anything that affects your chance of getting a disease such as cancer. Different cancers have different risk factors. Some risk factors, like smoking, can be changed. Others, like a person’s age or family history, can’t be changed.
But having a known risk factor, or even several, does not mean that you will get the disease. And some people who get the disease may have few or no known risk factors.
Researchers have found some factors that increase a person’s risk of mesothelioma.
Asbestos
The main risk factor for pleural mesothelioma is exposure to asbestos. In fact, most cases of pleural mesothelioma have been linked to asbestos exposure, usually from high levels of exposure in the workplace.
Asbestos is a group of minerals that occur naturally as bundles of tiny fibers. These fibers are found in soil and rocks in many parts of the world.
When asbestos fibers in the air are inhaled, they can get into the lungs. Fibers that stay in the lungs can travel to the ends of the small airways and enter the pleural lining of the lung and chest wall. These fibers can then injure the cells of the pleura, and eventually cause mesothelioma. Asbestos fibers can also damage cells of the lung and result in asbestosis (scar tissue in the lung) and/or lung cancer.
Peritoneal mesothelioma, which forms in the abdomen, can result from coughing up and swallowing inhaled asbestos fibers.
Many people are exposed to very low levels of naturally occurring asbestos in outdoor air in dust that comes from rocks and soil containing asbestos. This is more likely to happen in areas where rocks have higher asbestos content. In some areas, asbestos can be found in the water supply as well as in the air.
In the past, asbestos was used in many products because of its heat and fire-resistant properties. The link between asbestos and mesothelioma is now well known, so its use in the United States has gone down dramatically. Most use stopped several decades ago, but it is still used in some products.
Still, millions of Americans may already have been exposed to asbestos. People at risk for asbestos exposure in the workplace include some miners, factory workers, insulation manufacturers and installers, railroad and automotive workers, ship builders, gas mask manufacturers, plumbers, and construction workers. Family members of people exposed to asbestos at work can also be exposed because the workers can carry home asbestos fibers on their clothes.
Asbestos was also used to insulate many older homes, as well as commercial and public buildings around the country, including some schools. Because these particles are contained within the building materials, they are not likely to be found in the air in large numbers. The risk of exposure is likely to be very low unless the particles somehow escape into the air, such as when building materials begin to decompose over time, or during remodeling or removal.
The risk of developing mesothelioma is loosely related to how much asbestos a person is exposed to and how long this lasts. People exposed at an early age, for a long time, and at higher levels are more likely to develop this cancer. Still, most people exposed to asbestos, even in large amounts, do not get mesothelioma. Other factors, such as a person’s genes, may make them more likely to develop mesothelioma when exposed to asbestos.
Mesotheliomas related to asbestos exposure take a long time to develop. The time between first exposure to asbestos and diagnosis of mesothelioma is usually between 20 and 50 years. Unfortunately, the risk of mesothelioma does not go down over time after the exposure to asbestos stops. The risk appears to be lifelong.
Zeolites
Zeolites are minerals chemically related to asbestos. An example is erionite, which is common in the rocks and soil in parts of Turkey. High mesothelioma rates in these areas are believed to be caused by exposure to this mineral.
Radiation
There have been a few published reports of mesotheliomas that developed after people were exposed to high doses of radiation to the chest or abdomen as treatment for another cancer. Although the risk of mesothelioma is higher in patients who have been treated with radiation, this cancer is still rare in these patients.
There have also been reports linking mesothelioma to injections of thorium dioxide (Thorotrast). This radioactive material was used by doctors for certain x-ray tests until the 1950s. Thorotrast was found to cause cancers, so it has not been used for many decades.
SV40 virus
Some studies have raised the possibility that infection with simian virus 40 (SV40) might increase the risk of developing mesothelioma. Some injectable polio vaccines given between 1955 and 1963 were contaminated with SV40. As many as 30 million people in the United States may have been exposed to this virus.
Some lab studies have suggested that SV40 infection might cause mesothelioma. For example, infecting some lab animals like hamsters with SV40 causes mesotheliomas to develop. Researchers also have noticed that SV40 can cause mouse cells grown in lab dishes to become cancerous, and that asbestos increases the cancer-causing effect of SV40 on these cells. Other researchers have found SV40 DNA in some biopsy specimens of human mesotheliomas. But fragments of SV40 DNA can also be found in some non-cancerous human tissues.
So far, the largest studies looking at this issue in humans have not found an increased risk for mesothelioma or other cancers among people who received the contaminated vaccines as children. But the peak age range for diagnosis of mesothelioma is 50 to 70 years. Some researchers have pointed out that this issue may remain unresolved until more of the people accidentally exposed to SV40 between 1955 and 1963 reach that age range.
Most experts have concluded that at this time we still don’t know if SV40 is responsible for some mesotheliomas. This important topic is still being researched.
Age
The risk of mesothelioma increases with age. Mesothelioma can occur in young people (even children), but it is rare in people under age 45. About 2 out of 3 people with mesothelioma of the chest are 65 or older.
Gender
Mesothelioma is much more common in men than in women. This is probably because men have been more likely to work in jobs with heavy exposure to asbestos.
Can mesothelioma be prevented?
Being exposed to asbestos is by far the biggest risk factor for mesothelioma, so the best way to reduce your risk is to limit your exposure to asbestos at home, in public buildings, and at work.
People who might be exposed to high levels of asbestos at work include some miners, factory workers, insulation manufacturers and installers, railroad and automotive workers, ship builders, gas mask manufacturers, plumbers, and construction workers. If there is a chance of on-the-job exposure, such as during the renovation of old buildings, you should use all protective equipment and safety procedures designed for working around asbestos.
Older homes may have insulation containing asbestos or other materials. A knowledgeable expert can check your home to find out if there is any asbestos and whether it poses any risk of exposure. This may mean testing the air for asbestos levels. Just because asbestos exists in a home does not necessarily mean that it needs to be removed. As long as the material is not damaged or disturbed, for example by drilling or remodeling, the fibers will not be released into the air. If asbestos needs to be removed from your home, you should hire a qualified contractor to do this to avoid contaminating your home or causing any exposure to your family or to the workers. You should not attempt to remove asbestos-containing material yourself.
Asbestos can also be found in some commercial and public buildings (including some schools), where the same basic principles apply. Intact, undisturbed materials containing asbestos generally do not pose a health risk. They may pose a risk if they are damaged, are disturbed in some way, or deteriorate over time and release asbestos fibers into the air. By federal law, all schools are required to inspect materials with asbestos regularly and to have a plan in place for managing them.
Mesothelioma symptoms
Many of the early symptoms of mesothelioma are more likely to be caused by other conditions, so at first people may ignore them or mistake them for common, minor ailments. Most people with mesothelioma have symptoms for at least a few months before they are diagnosed.
Pleural mesothelioma (mesothelioma of the chest) has symptoms that include:
- Shortness of breath (worse when active or lying down)
- Chest pain, or pain in the side of the chest or lower back
- Pain in the shoulder or upper arm
- A cough that doesn’t go away
- Night sweats
- Fever
- Excessive sweating
- Fatigue
- Weight loss (without trying)
- Trouble swallowing (feeling like food gets stuck)
- Hoarseness
- Swelling of the face and arms
Peritoneal mesothelioma has symptoms that include:
- Swelling or fluid in the abdomen
- Pain in the tummy
- Not feeling hungry
- Feeling nauseous
- Fever
- Problems with urinating or bowel movements (pooing)
- Weight loss (without trying)
- Nausea and vomiting
- Constipation
Mesothelioma can cause fluid to build up around the pleura (called pleural effusion) or in the tummy (called peritoneal effusion), which causes swelling and pain.
These symptoms can be caused by mesothelioma, but more often they are caused by other conditions. Still, if you have any of these problems (especially if you have been exposed to asbestos), it’s important to see your doctor right away so the cause can be found and treated, if needed.
Mesothelioma diagnosis
Mesothelioma can be quite hard to diagnose because it can look like other types of cancer. If your doctor suspects mesothelioma, they will order a range of tests and combine all the information to make a firm diagnosis.
Mesothelioma is most often diagnosed after a person goes to a doctor because of symptoms they are having. If there is a reason to suspect you might have mesothelioma, your doctor will examine you and use one or more tests to find out. Symptoms might suggest that the problem could be mesothelioma, but tests will be needed to confirm the diagnosis.
Medical history and physical exam
If you have any signs or symptoms that suggest you might have mesothelioma, your doctor will want to get your medical history to learn about your symptoms and possible risk factors, especially asbestos exposure.
A physical exam can provide information about possible signs of mesothelioma and other health problems. Pleural mesothelioma can cause fluid to build up around the lungs in the chest (called a pleural effusion). In cases of peritoneal mesothelioma, fluid can build up in the abdomen (called ascites). In pericardial mesothelioma, fluid builds up in the sac around the heart (called a pericardial effusion). Rarely, mesothelioma can develop in the groin and look like a hernia. All of these might be found during a physical exam, such as when the doctor listens to these areas with a stethoscope or taps on the chest or abdomen.
If mesothelioma is a possibility, tests will be needed to make sure. These might include imaging tests, blood tests, and other procedures.
Imaging tests
Imaging tests use x-rays, radioactive particles, sound waves, or magnetic fields to create pictures of the inside of your body. Imaging tests might be done for a number of reasons, such as:
- To look at suspicious areas that might be cancer
- To learn how far cancer has spread
- To help determine if treatment is working
People thought to have mesothelioma may have one or more of these tests.
Chest x-ray
This is often the first test done if someone has symptoms such as a constant cough or shortness of breath. Findings that might suggest mesothelioma include an abnormal thickening of the pleura, calcium deposits on the pleura, fluid in the space between the lungs and the chest wall, or changes in the lungs themselves as a result of asbestos exposure.
Computed tomography (CT) scan
The CT scan uses x-rays to make detailed cross-sectional images of your body. Instead of taking one picture, like a regular x-ray, a CT scanner takes many pictures as it rotates around you while you are lying on a narrow table. A computer then combines these into images of slices of the body.
CT scans are often used to help look for mesothelioma and to determine the exact location of the cancer. They can also help determine the stage (extent) of the cancer. For example, they can show if the cancer has spread to other organs. This can help determine if surgery might be a treatment option. Finally, CT scans can also be used to learn if treatment such as chemotherapy is shrinking or slowing the growth of the cancer.
A CT scanner has been described as a large donut, with a narrow table that slides in and out of the middle opening. You will need to lie still on the table while the scan is being done. CT scans take longer than regular x-rays, and you might feel a bit confined by the ring while the pictures are being taken.
Before the test, you might have to drink a liquid called oral contrast. This helps outline the intestine so that certain areas are not mistaken for tumors. You might also need an IV (intravenous) line through which a different kind of contrast is injected. This helps better outline structures in your body. The injection can cause some flushing (redness and warm feeling). Some people are allergic and get hives or, rarely, more serious reactions like trouble breathing and low blood pressure. Be sure to tell the doctor if you have any allergies (especially to iodine or shellfish) or have ever had a reaction to any contrast material used for x-rays.
Echocardiogram
This test uses sound waves to look at the heart. It may be done if your doctor suspects that you have fluid around your heart (a pericardial effusion). This test can also tell how well the heart is working. For the most common version of this test, you lie on a table while a technician moves an instrument called a transducer over the skin on your chest. A gel is often put on the skin first.
Positron emission tomography (PET) scan
For a PET scan, a radioactive substance (usually a type of sugar related to glucose, known as FDG) is injected into the blood. The amount of radioactivity used is very low. Because cancer cells grow quickly, they absorb more of the sugar than most other cells. After waiting about an hour, you lie on a table in the PET scanner for about 30 minutes while a special camera creates a picture of areas of radioactivity in the body.
The picture from a PET scan is not as detailed as a CT or MRI scan, but it can provide helpful information about whether abnormal areas seen on these tests are likely to be cancerous or not. For example, it can give the doctor a better idea of whether a thickening of the pleura or peritoneum seen on a CT scan is more likely cancer or merely scar tissue. If you have been diagnosed with mesothelioma, your doctor may use this test to see if the cancer has spread to lymph nodes or other parts of the body. A PET scan can also be useful if your doctor thinks the cancer may have spread but doesn’t know where.
Some machines can do both a PET and CT scan at the same time (PET/CT scan). This lets the doctor compare areas of higher radioactivity on the PET scan with the more detailed appearance of that area on the CT.
Magnetic resonance imaging (MRI) scan
Like CT scans, MRI scans make detailed images of the body’s soft tissues. But MRI scans use radio waves and strong magnets instead of x-rays. A contrast material called gadolinium is often injected into a vein before the scan to better show details. This contrast is different than the one used for CT scans, so being allergic to one doesn’t mean you are allergic to the other.
MRI scans can sometimes help show the exact location and extent of a tumor since they provide very detailed images of soft tissues. For mesotheliomas, they may be useful in looking at the diaphragm (the thin band of muscle below the lungs that helps us breathe), a possible site of cancer spread.
MRI scans take longer than CT scans – often up to an hour. You may have to lie inside a narrow tube, which can upset people with a fear of enclosed spaces. Special, more open MRI machines may be an option in some cases. The MRI machine makes buzzing and clicking noises that you might find disturbing. Some places will give you earplugs to help block this out.
Blood tests
Blood levels of certain substances are often higher in people with mesothelioma:
- Osteopontin
- Soluble mesothelin-related peptides (SMRPs), detected with the MesoMark® test
Mesothelioma can’t be diagnosed with these blood tests alone, but high levels of these substances can make the diagnosis more likely. These tests are not routinely used in most doctors’ offices because of their limited value.
Tests of fluid and tissue samples
Symptoms and test results may strongly suggest that a person has mesothelioma, but the actual diagnosis is made by removing cells from an abnormal area and looking at them under a microscope. This is known as a biopsy. It can be done in different ways, depending on the situation.
Removing fluid for testing
If there is a buildup of fluid in part of the body that might be due to mesothelioma, a sample of this fluid can be removed by inserting a thin, hollow needle through the skin and into the fluid. Numbing medicine is used on the skin before the needle is inserted. This may be done in a doctor’s office or in the hospital. Sometimes ultrasound (or an echocardiogram) is used to guide the needle. These tests use sound waves to see inside the body.
This procedure has different names depending on where the fluid is:
- Thoracentesis removes fluid from the chest.
- Paracentesis removes fluid from the abdomen.
- Pericardiocentesis removes fluid from the sac around the heart.
The fluid is then tested for its chemical makeup and is looked at under a microscope to see if it contains cancer cells. If cancer cells are found, special tests might be done to see if the cancer is a mesothelioma, a lung cancer, or another type of cancer.
Even if no cancer cells are found in the fluid, a person might still have cancer. In many cases, doctors need to get an actual sample of the mesothelium (the pleura, peritoneum, or pericardium) to determine if a person has mesothelioma.
Needle biopsies
Suspected tumors in the chest are sometimes sampled by needle biopsy. A long, hollow needle is passed through the skin in the chest between the ribs and into the pleura. Imaging tests such as CT scans are used to guide the needle into the tumor so that small samples can be removed to be looked at under the microscope. This is often done using just numbing medicine.
Needle biopsy can also be used to get samples of the lymph nodes in the space between the lungs to see if the cancer has spread there.
Needle biopsies do not require a surgical incision or overnight hospital stay. But the downside is that sometimes the samples removed are not big enough to make an accurate diagnosis. This is especially true for mesothelioma. A more invasive biopsy method may be needed.
There is a slight chance that the needle could put a small hole in the lung during the biopsy. This can cause air to build up in the space between the lung and the chest wall (known as a pneumothorax). A small pneumothorax might not cause any symptoms. It may only be seen on an x-ray done after the biopsy, and it will often go away on its own. But a larger pneumothorax can make part of a lung collapse and might need to be treated. The treatment is placement of a small tube (a catheter) through the skin and into the space between the lungs. The tube is used to suck the air out in order to re-expand the lung and is left in place for a short time.
Endoscopic biopsies
Endoscopic biopsy is commonly used to diagnose mesothelioma. An endoscope is a thin, tube-like instrument used to look inside the body. It has a light and a lens (or tiny video camera) on the end for viewing and often has a tool to remove tissue samples. Endoscopes have different names depending on the part of the body where they’re used.
Thoracoscopy: This procedure uses an endoscope called a thoracoscope to look at areas inside the chest. It can be used to look at the pleura and take tissue samples for biopsies.
Thoracoscopy is done in the operating room while you are under general anesthesia (in a deep sleep). The doctor inserts the thoracoscope through one or more small cuts made in the chest wall to look at the space between the lungs and the chest wall. This lets the doctor see possible areas of cancer and remove small pieces of tissue to look at under the microscope. The doctor can also sample lymph nodes and fluid and see if a tumor is growing into nearby tissues or organs.
Thoracoscopy can also be used as part of a procedure to keep fluid from building up in the chest. This is called pleurodesis and is discussed in Palliative Procedures Used for Malignant Mesothelioma.
Laparoscopy: For this test, the doctor uses an endoscope called a laparoscope to look inside the abdomen and biopsy any peritoneal tumors. This is done in the operating room while you are under general anesthesia (in a deep sleep). The laparoscope is inserted into the abdomen through small cuts on the front of the abdomen.
Mediastinoscopy: If imaging tests such as a CT scan suggest that the cancer might have spread to the lymph nodes between the lungs, the doctor may want to sample some of them to see if they really contain cancer. The area between the lungs is called the mediastinum, and looking at it with an endoscope is called mediastinoscopy. This is done in an operating room while you are under general anesthesia (in a deep sleep).
A small cut is made in the front of the neck above the breastbone (sternum) and a thin, hollow, lighted tube (called a mediastinoscope) is inserted behind the sternum. Special instruments can be passed through this tube to take tissue samples from the lymph nodes along the windpipe and the major bronchial tube areas.
Lung cancers often spread to lymph nodes, but mesotheliomas do this less often. Testing the lymph nodes can help show whether a cancer is still localized or if it has started to spread, which might affect treatment options. It can also sometimes help tell lung cancers from mesotheliomas.Patients with mesothelioma don’t need to have bronchoscopy to see if tumors are in their airways (because that isn’t where tumors from mesothelioma are found). Instead, bronchoscopy may be used to biopsy lymph nodes near the lungs (instead of using mediastinoscopy).
Endobronchial ultrasound needle biopsy: For this test, a bronchoscope (a long, thin, flexible, fiber-optic tube) with an ultrasound device at its tip is passed down the throat and into the windpipe. The ultrasound lets the doctor see the nearby lymph nodes. A hollow needle is then passed down the bronchoscope and through the airway wall into the nodes to take biopsy samples. This procedure may be done with either general anesthesia (where you are asleep), or with numbing medicine (local anesthesia) and light sedation.
Open surgical biopsy
Sometimes, endoscopic biopsies aren’t enough to make a diagnosis, so more invasive procedures are needed. By making an incision in the chest (thoracotomy) or an incision in the abdomen (laparotomy) the surgeon can remove a larger sample of tumor or, sometimes, remove the entire tumor.
Testing the samples in the lab
No matter how they’re obtained, all biopsy and fluid samples are sent to the pathology lab. There, a doctor will look at them under a microscope and test them to find out if they contain cancer cells (and if so, what type of cancer it is).
It’s often hard to diagnose mesothelioma by looking at cells from fluid samples. It can even be hard to diagnose mesothelioma with tissue from small needle biopsies. Under the microscope, mesothelioma can often look like other types of cancer. For example, pleural mesothelioma can resemble some types of lung cancer, and peritoneal mesothelioma in women may look like some cancers of the ovaries.
For this reason, special lab tests are often done to help tell mesothelioma from some other cancers. To learn about some of the tests that might be done on tissue samples, see Testing Biopsy and Cytology Specimens for Cancer.
If mesothelioma is diagnosed, the doctor will also determine what type of mesothelioma it is, based on the patterns of cells seen in the microscope. Most mesotheliomas are classified as either epithelioid, sarcomatoid, or mixed/biphasic.
Pulmonary function tests
If mesothelioma has been diagnosed, pulmonary function tests (PFTs) may be done to see how well your lungs are working. This is especially important if surgery might be an option to treat the cancer. Surgery often requires removing part or all of a lung, so it’s important to know how well the lungs are working to start with. These tests can give the surgeon an idea of whether surgery may be an option, and if so, how much lung can safely be removed safely.
There are a few different types of PFTs, but they all basically have you breathe in and out through a tube connected to a machine that measures your lung function.
Can mesothelioma be found early?
Mesothelioma is uncommon, and there are no widely recommended screening tests for this cancer in people who are not at increased risk. (Screening is testing for cancer in people who don’t have any symptoms.)
For people with known exposure to asbestos, some doctors recommend imaging tests such as chest x-rays or computed tomography (CT) scans to look for changes in the lungs that might be signs of mesothelioma or lung cancer. But it is not clear how useful these tests are in finding mesotheliomas early.
In recent years, doctors have found that people with mesothelioma often have high levels of certain substances in their blood, including osteopontin and soluble mesothelin-related peptides (SMRPs). Blood tests for these substances may one day be useful in finding mesotheliomas early, as well as for monitoring the course of the disease in people who have mesothelioma.
Most mesotheliomas are found when a person goes to a doctor because of symptoms. People who have been exposed to asbestos should know the possible signs and symptoms of mesothelioma. Many of these symptoms are more likely to be caused by something other than mesothelioma, but it’s important to report any new symptoms to your doctor right away so that the cause can be found and treated, if needed.
Mesothelioma stages
After someone is diagnosed with malignant mesothelioma, doctors will try to figure out if it has spread, and if so, how far. This process is called staging. The stage of a cancer describes how much cancer is in the body. It helps determine how serious the cancer is and how best to treat it. Doctors also use a cancer’s stage when talking about survival statistics.
The stages of mesothelioma range from I (1) through IV (4). As a rule, the lower the number, the less the cancer has spread. A higher number, such as stage IV, means cancer has spread more. And within a stage, an earlier letter means a lower stage. Although each person’s cancer experience is unique, cancers with similar stages tend to have a similar outlook and are often treated in much the same way.
How is the stage determined?
Malignant pleural mesothelioma (MPM), the most common type, is the only mesothelioma for which a formal staging system exists. These mesotheliomas start in the pleura, which includes the lining of the lungs and the inner lining of the chest wall.
The staging system most often used for MPM is the American Joint Committee on Cancer (AJCC) TNM system, which is based on 3 key pieces of information:
- The extent (size) of the main tumor (T): Has the cancer grown into nearby structures or organs? Is it possible to remove it with surgery?
- The spread to nearby lymph nodes (N): Has the cancer spread to nearby lymph nodes?
- The spread (metastasis) to distant sites (M): Has the cancer spread to distant organs such as the bones, the liver, the lung or pleura (lining of the lung) on the other side of the body, or the peritoneum (the lining of the abdomen)?
Numbers or letters after T, N, and M provide more details about each of these factors. Higher numbers mean the cancer is more advanced. Once a person’s T, N, and M categories have been determined, this information is combined in a process called stage grouping to assign an overall stage.
The system described below is the most recent AJCC system, effective as of January 2018. It is used only for malignant pleural mesotheliomas. Mesotheliomas starting in other places are less common and do not have formal staging systems.
Mesothelioma cancer is typically given a clinical stage based on the results of a physical exam, biopsy, and imaging tests. If surgery is done, the pathologic stage (also called the surgical stage) is determined by examining tissue removed during the operation.
Cancer staging can be complex, so ask your doctor to explain it to you in a way you understand.
Table 1. Stages of malignant pleural mesothelioma
| AJCC Stage | Stage grouping | Stage description* |
| IA | T1 N0 M0 | Mesothelioma is in the pleura lining the chest wall on one side of the chest. It may or may not also affect the pleura lining the diaphragm (the thin breathing muscle below the lungs), the mediastinum (the space between the lungs), or the pleura covering the lung (T1). It has not spread to nearby lymph nodes (N0) or to distant sites (M0). |
|
IB | T2 N0 M0 | Mesothelioma is in the pleura lining the chest wall on one side of the chest, as well as in the pleura coating the diaphragm, the mediastinum, and the lung. It also has grown into the diaphragm or the lung itself (T2). It has not spread to nearby lymph nodes (N0) or to distant sites (M0). |
| OR | ||
| T3 N0 M0 | The mesothelioma has grown into nearby structures but may still possibly be removed (resected) with surgery (T3). The tumor is in the pleura lining the chest wall on one side of the chest, as well as the pleura coating the lung, the diaphragm, and the mediastinum on the same side. It also has grown into at least one of the following:
The cancer has not spread to nearby lymph nodes (N0) or to distant sites (M0). | |
| II | T1 or T2 N1 M0 | Mesothelioma is in the pleura lining the chest wall on one side of the chest (T1), and it may have grown into the diaphragm or the lung itself (T2). The cancer has spread to nearby lymph nodes on the same side of the body as the main tumor (N1). It has not spread to distant sites (M0). |
|
IIIA | T3 N1 M0 | The mesothelioma has grown into nearby structures but may still possibly be removed (resected) with surgery (T3). The tumor is in the pleura lining the chest wall on one side of the chest, as well as the pleura coating the lung, the diaphragm, and the mediastinum on the same side. It also has grown into at least one of the following:
The cancer has spread to nearby lymph nodes on the same side of the body as the main tumor (N1). It has not spread to distant sites (M0). |
|
IIIB
| T1-T3 N2 M0 | The mesothelioma may or may not have grown into nearby structures, but it may still possibly be removed (resected) with surgery (T1 to T3). The cancer has spread to nearby lymph nodes on the other side of the body, or to lymph nodes above the collarbone (supraclavicular lymph nodes) on either side (N2). It has not spread to distant sites (M0). |
| OR | ||
|
T4 Any N M0 | The mesothelioma has grown too far to be removed completely with surgery (T4). The tumor is in the pleura lining the chest wall on one side of the chest, as well as the pleura coating the lung, diaphragm, and mediastinum on the same side. The tumor also has grown into at least one of the following:
The cancer may or may not have spread to nearby lymph nodes (any N). It has not spread to distant sites (M0). | |
| IV | Any T Any N M1 | The mesothelioma may or may not have grown into nearby structures (any T). It may or may not have spread to nearby lymph nodes (any N). It has spread to distant organs such as the bones, the liver, the lung or pleura on the other side of the body, or the peritoneum (the lining of the abdomen) (M1). |
Footnotes: * The following additional categories are not listed on the table above:
TX: Main tumor cannot be assessed due to lack of information.
T0: There is no evidence of a primary tumor.
NX: Nearby lymph nodes cannot be assessed due to lack of information.
Resectable versus unresectable cancer
The TNM system groups mesotheliomas into several stages that help give doctors an idea about a person’s prognosis (outlook). But for treatment purposes, doctors often use a simpler system, based on whether the cancer is likely to be resectable (where all visible tumor can be removed by surgery) or unresectable.
In general, most stage I and II mesotheliomas, as well as some stage III mesotheliomas, are potentially resectable, but there are exceptions. Whether the cancer can be removed depends not only on how far the tumor has grown, but also on its subtype (most doctors believe only epithelioid and mixed/biphasic tumors are potentially resectable), where it’s located, and if the patient is healthy enough to have surgery.
Even for resectable mesotheliomas, in most cases cancer cells that can’t be seen are left behind after surgery. For this reason, many doctors use other treatments (radiation therapy and/or chemotherapy) along with surgery when possible.
Other prognostic factors
Stage is an important factor in predicting a person’s prognosis (outlook), but other factors also play a role. Some factors linked to longer survival times include:
- Still being able to carry out normal daily tasks
- Being younger
- Being female
- Having the epthelioid subtype of mesothelioma
- Having normal levels of LDH in the blood
- Having normal levels of red blood cells, white blood cells, and platelets
Mesothelioma prognosis
Malignant mesothelioma is only very rarely curable, either by surgery, radiotherapy or chemotherapy. The median survival from time of diagnosis is only one year. Outcomes are worse for male patients, and for patients with extensive disease at diagnosis.
Mesothelioma survival rates
Survival rates tell you what portion of people with the same type and stage of cancer are still alive a certain amount of time (such as 5 years) after they were diagnosed. They can’t tell you how long you will live, but they may help give you a better understanding about how likely it is that your treatment will be successful.
Cancer survival rates don’t tell the whole story
Survival rates are often based on previous outcomes of large numbers of people who had the disease, but they can’t predict what will happen in any particular person’s case. There are a number of limitations to remember:
- The numbers below are among the most current available. But to get 2-year and 5-year survival rates, doctors have to look at people who were treated at least several years ago. As treatments are improving over time, people who are now being diagnosed with mesothelioma may have a better outlook than these statistics show.
- These statistics are based on the stage of the cancer when it was first diagnosed. They do not apply to cancers that later come back or spread, for example.
- The outlook for people with mesothelioma varies by the stage (extent) of the cancer – in general, the survival rates are higher for people with earlier stage cancers. But many other factors can also affect a person’s outlook, such as a person’s age and overall health, where the cancer is in the body, what type of mesothelioma it is, and how well the cancer responds to treatment. The outlook for each person is specific to their circumstances.
Your doctor can tell you how these numbers may apply to you, as he or she is familiar with your particular situation.
Survival rates for malignant pleural mesothelioma
The numbers below come from thousands of people from all over the world who were diagnosed with malignant pleural mesothelioma, mainly between the years 2000 and 2013. These numbers are only for mesotheliomas that start in the inner lining of the chest (the pleura), which is the most common place for mesothelioma to start.
Here are the 2-year and 5-year survival rates, by stage, for malignant pleural mesothelioma 3:
- For stage IA cancers, the 2-year survival rate is about 46%, and the 5-year survival rate is about 16%.
- For stage IB cancers, the 2-year survival rate is about 41%, and the 5-year survival rate is about 13%.
- For stage II cancers, the 2-year survival rate is about 38%, and the 5-year survival rate is about 10%.
- For stage IIIA cancers, the 2-year survival rate is about 30%, and the 5-year survival rate is about 8%.
- For stage IIIB cancers, the 2-year survival rate is about 26%, and the 5-year survival rate is about 5%.
- For stage IV cancers, the 2-year survival rate is about 17%, and the 5-year survival rate is less than 1%.
Along with the stage of the cancer, the outlook for people with malignant pleural mesothelioma can also be affected by other factors. For example, the type of mesothelioma, based on how the cancer cells are arranged when seen in the lab, is important. The epithelioid type tends to have a better outlook than the other types, such as sarcomatoid or mixed (biphasic) malignant pleural mesothelioma. Other factors can be important as well.
Remember, these survival rates are only estimates – they can’t predict what will happen to any individual person. These statistics can be confusing and may lead you to have more questions. Talk to your doctor to better understand your specific situation.
Mesothelioma treatment
What treatment you undergo for mesothelioma depends on your health and certain aspects of your cancer, such as its stage and location.
Unfortunately, mesothelioma often is an aggressive disease and for most people a cure isn’t possible. Mesothelioma is usually diagnosed at an advanced stage — when it isn’t possible to remove the cancer through an operation. Instead, your doctor may work to control your cancer to make you more comfortable.
Discuss treatment goals with your doctor. Some people want to do everything they can to treat their cancer, even if that means enduring side effects for a small chance of an improvement. Others prefer treatments that make them comfortable so that they can live their remaining time as symptom-free as possible.
Surgery
Surgeons work to remove mesothelioma when it’s diagnosed at an early stage. In some cases this may cure the cancer.
Sometimes it isn’t possible to remove all of the cancer. In those cases, surgery may help to reduce the signs and symptoms caused by mesothelioma spreading in your body.
Surgical options may include:
- Surgery to decrease fluid buildup. Pleural mesothelioma may cause fluid to build up in your chest, causing difficulty breathing. Surgeons insert a tube or catheter into your chest to drain the fluid. Doctors may also inject medicine into your chest to prevent fluid from returning (pleurodesis).
- Surgery to remove the tissue around the lungs or abdomen. Surgeons may remove the tissue lining the ribs and the lungs (pleurectomy) or the tissue lining the abdominal cavity (peritonectomy). This procedure won’t cure mesothelioma, but may relieve signs and symptoms.
- Surgery to remove as much of the cancer as possible (debulking). If all of the cancer can’t be removed, surgeons may attempt to remove as much as possible. Debulking allows doctors to more accurately direct radiation treatments to relieve pain and fluid buildup caused by mesothelioma.
- Surgery to remove a lung and the surrounding tissue. Removing the affected lung and the tissue that surrounds it may relieve signs and symptoms of pleural mesothelioma. If you’ll be receiving radiation therapy to the chest after surgery, this procedure also allows doctors to use higher doses, since they won’t need to worry about protecting your lung from damaging radiation.
Chemotherapy
Chemotherapy uses chemicals to kill cancer cells. Systemic chemotherapy travels throughout the body and may shrink or slow the growth of a mesothelioma that can’t be removed using surgery. Chemotherapy may also be used before surgery (neoadjuvant chemotherapy) to make an operation easier or after surgery (adjuvant chemotherapy) to reduce the chance that cancer will return.
Chemotherapy drugs may also be heated and administered directly into the abdominal cavity (intraperitoneal chemotherapy), in the case of peritoneal mesothelioma. Using this strategy, chemotherapy drugs can reach the mesothelioma directly without injuring healthy cells in other parts of the body. This allows doctors to administer higher doses of chemotherapy drugs.
Radiation therapy
Radiation therapy focuses high-energy beams from sources such as X-rays and protons to a specific spot or spots on your body. Radiation may be used after surgery to kill any remaining cancer cells. It may also help reduce signs and symptoms of advanced cancer in situations where surgery isn’t an option.
Clinical trials
Clinical trials are studies of new mesothelioma treatment methods. People with mesothelioma may opt for a clinical trial for a chance to try new types of treatment. However, a cure isn’t guaranteed. Carefully consider your treatment options and talk to your doctor about what clinical trials are open to you. Your participation in a clinical trial may help doctors better understand how to treat mesothelioma in the future.
Clinical trials are currently investigating a number of new approaches to mesothelioma treatment, including:
- Targeted therapy, which involves using drugs that attack specific abnormalities within cancer cells.
- Biological therapy, which uses your body’s immune system to fight cancer.
- Gene therapy, which involves altering the genes inside the cancer cells in order to stop disease.
Treatment for other types of mesothelioma
Pericardial mesothelioma and mesothelioma of tunica vaginalis are very rare. Early-stage cancer may be removed through surgery. Doctors have yet to determine the best way to treat later-stage cancers, though. Your doctor may recommend other treatments to improve your quality of life.
Alternative medicine
No alternative medicine treatments have proved helpful in treating mesothelioma. But complementary and alternative treatments may help control mesothelioma signs and symptoms. Discuss options with your doctor.
Mesothelioma can cause pressure within your chest that can make you feel as if you’re always short of breath. Breathlessness can be distressing. Your doctor may recommend using supplemental oxygen or taking medications to make you more comfortable, but often these aren’t enough. Combining your doctor’s recommended treatments with complementary and alternative approaches may help you feel better.
Alternative treatments that have shown some promise in helping people cope with breathlessness include:
- Acupuncture. Acupuncture uses thin needles inserted at precise points into your skin.
- Breath training. A nurse or physical therapist can teach you breathing techniques to use when you feel breathless. Sometimes you may feel breathless and begin to panic. Using these techniques may help you feel more in control of your breathing.
- Relaxation exercises. Slowly tensing and relaxing different muscle groups may help you feel more at ease and breathe easier. Your doctor may refer you to a therapist who can teach you relaxation exercises so that you can do them on your own.
- Sitting near a fan. Directing a fan to your face may help ease the sensation of breathlessness.
Coping and support
A diagnosis of mesothelioma can be devastating not only to you but also to your family and friends. In order to regain a sense of control, try to:
- Learn enough about mesothelioma to make decisions about your care. Write down questions to ask your doctor. Ask your health care team for information to help you better understand your disease. Good places to start looking for more information include the National Cancer Institute (https://www.cancer.gov/) and the American Cancer Society (https://www.cancer.org/).
- Surround yourself with a support network. Close friends or family can help you with everyday tasks, such as getting you to appointments or treatment. If you have trouble asking for help, learn to be honest with yourself and accept help when you need it.
- Seek out other people with cancer. Ask your health care team about cancer support groups in your community. Sometimes there are questions that can only be answered by other people with cancer. Support groups offer a chance to ask these questions and receive support from people who understand your situation. Online support message boards, such as the American Cancer Society’s Cancer Survivors Network, can offer similar benefits while allowing you to remain anonymous.
- Plan ahead. Ask your health care team about advance directives that give your family guidance on your medical wishes in case you can no longer speak for yourself.
- What Are the Key Statistics About Malignant Mesothelioma? https://www.cancer.org/cancer/malignant-mesothelioma/about/key-statistics.html
- Malignant Mesothelioma Stages. https://www.cancer.org/cancer/malignant-mesothelioma/detection-diagnosis-staging/staging.html
- Survival Statistics for Mesothelioma. https://www.cancer.org/cancer/malignant-mesothelioma/detection-diagnosis-staging/survival-statistics.html