Onychauxis
Onychauxis is medical term for an abnormally thick nail due to psoriasis, trauma, fungal nail infection (onychomycosis) or nonsyndromic congenital nail disorder 10. Onychauxis is characterized by localized hypertrophy of the nail plate, which manifests as hyperkeratosis, discoloration, and loss of translucency of the nail plate, with or without subungual hyperkeratosis 1. Cutting the nail becomes very difficult and pressure from shoes can cause this condition to become painful. Left untreated the thickened nails can increase the pressure under the nail causing bruising or even ulceration especially whilst wearing footwear, they may also start to curl and can turn a yellowy, brown color. A professional opinion from a podiatrist should be sought to ensure that there are no underlying problems which have caused your nails to thicken.
Nonsyndromic congenital nail disorder 10 is a condition that affects the fingernails and toenails. Affected individuals have extremely thick nails (onychauxis) that separate from the underlying nail bed (onycholysis) and can appear claw-like. Some fingers and toes may be missing part of the nail (hyponychia). In affected individuals, the nails are often abnormal from birth. However, the abnormalities may not be noticeable until later in childhood because the nails tend to grow more slowly than normal. Individuals with nonsyndromic congenital nail disorder 10 do not have any other health problems related to the condition. Nonsyndromic congenital nail disorder 10 is likely a rare disorder. At least 14 affected individuals have been described in the scientific literature 2.
Patients with onychauxis nails should be advised to trim their nails frequently. If the nails have grown long enough that nail-clipping becomes difficult, patients may soak their nails in water—such as during bathing or showering—for at least 5 min (or up to 30 min)—to allow for straightening and softening of the nail before clipping 3.
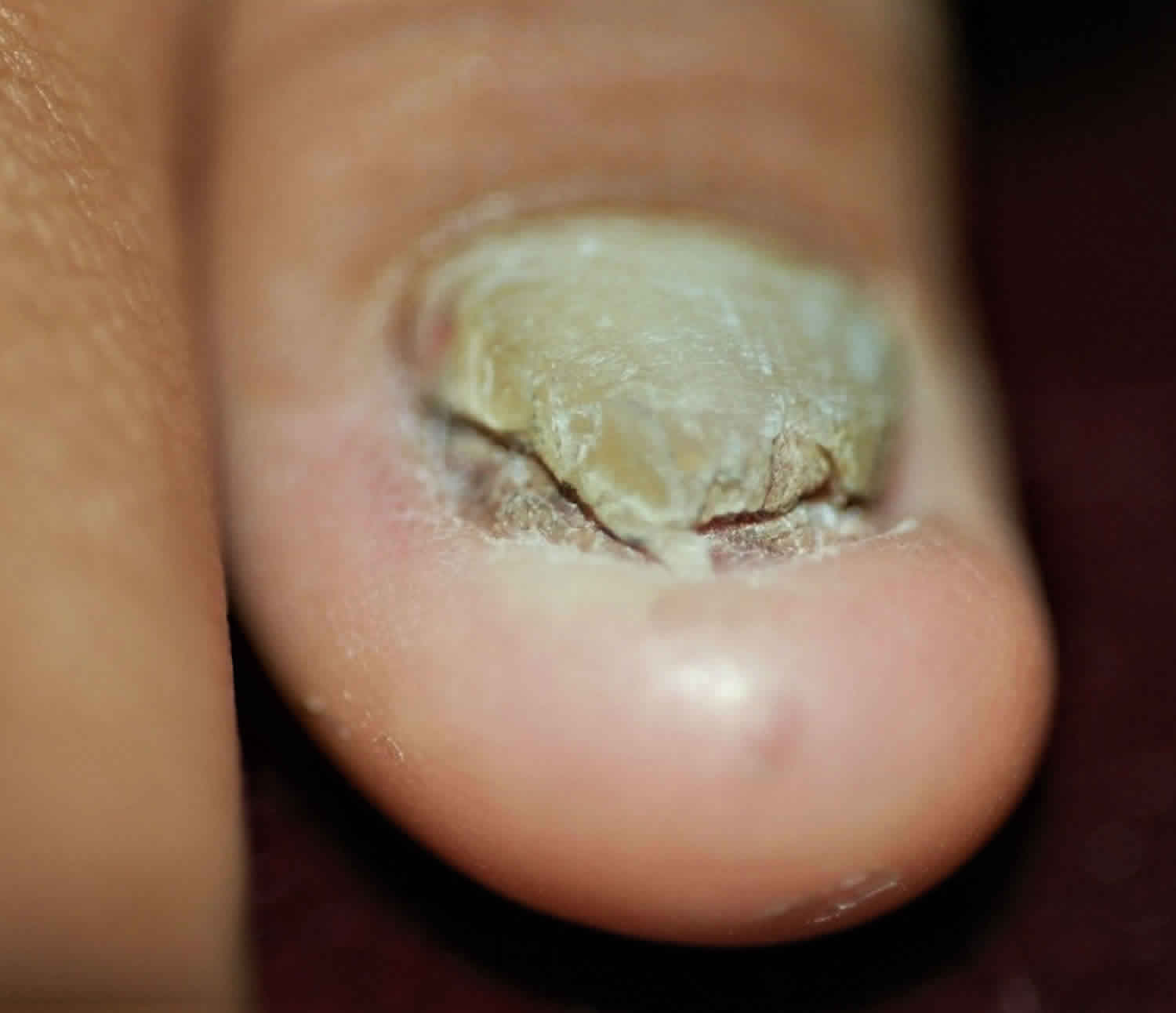
Figure 1. Onychauxis (due to fungal nail infection or onychomycosis)
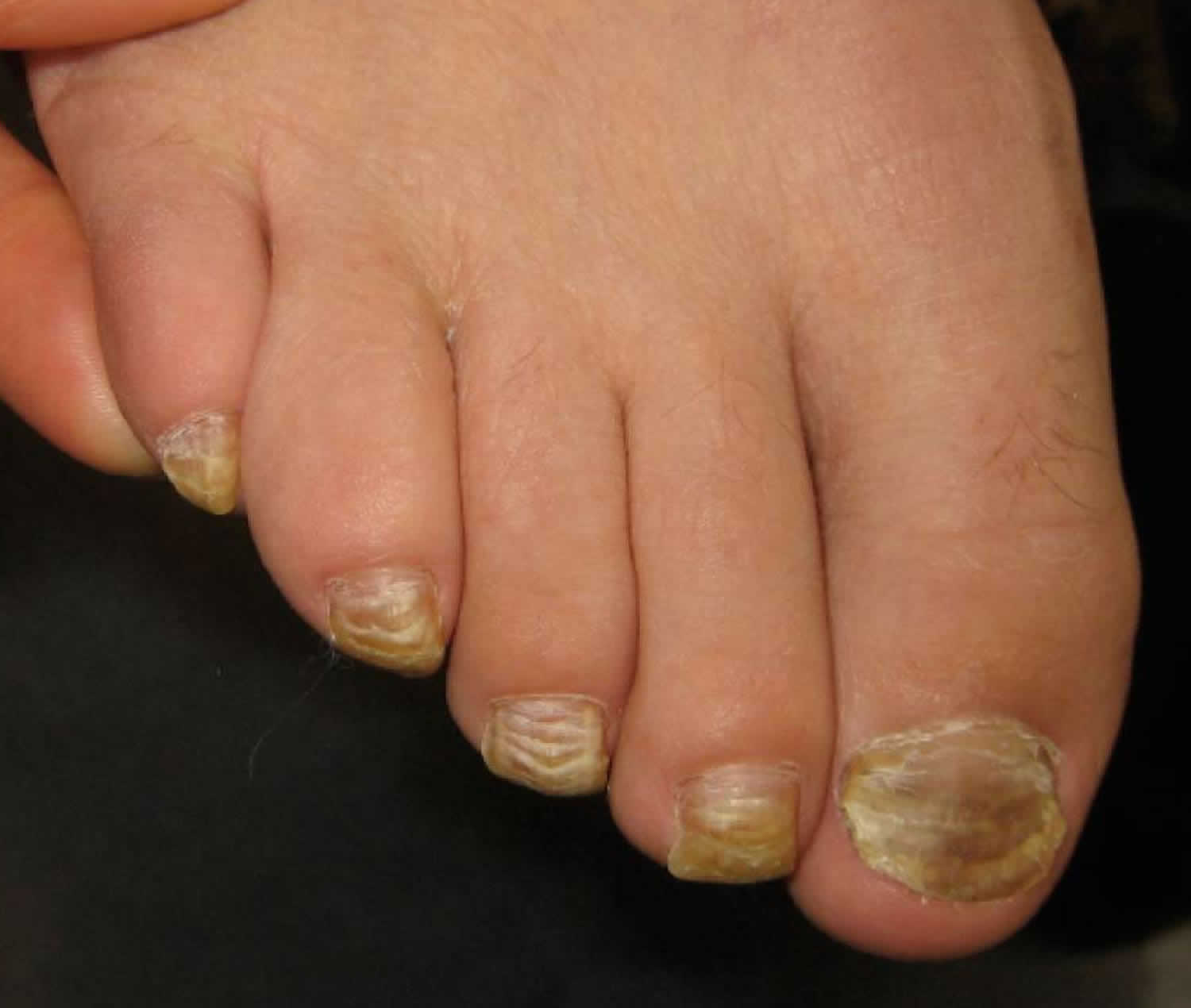
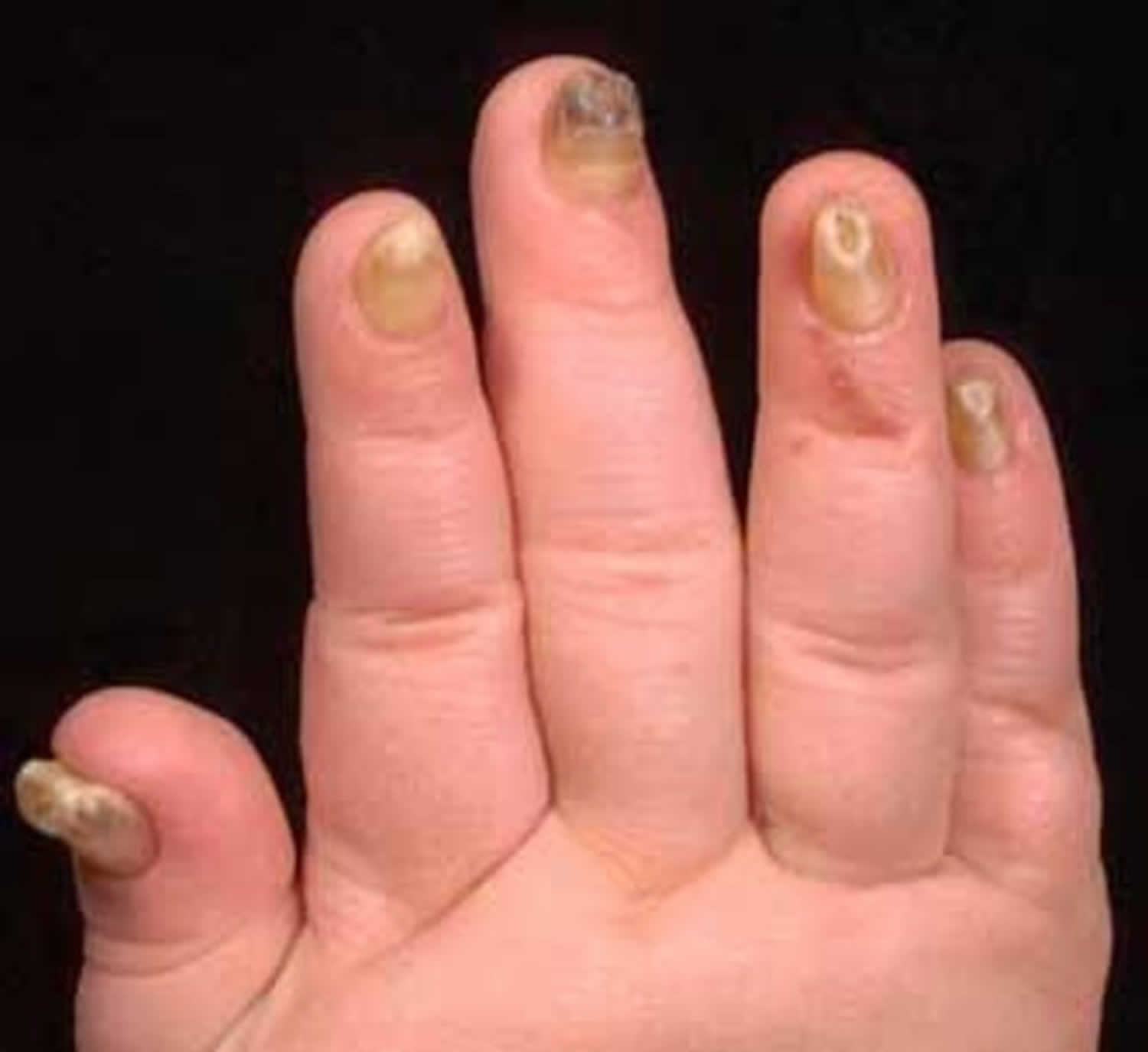
Figure 2. Onychauxis nails (due to nonsyndromic congenital nail disorder 10)
Onychauxis causes
Onychauxis causes include:
- A major trauma or repeated pressure from shoes on long nails.
- Fungal infection of the nails or skin diseases. Onychomycosis is a fungal infection of the nail unit. Approximately 90% of toenail and 75% of fingernail onychomycosis are caused by dermatophytes, notably Trichophyton mentagrophytes and Trichophyton rubrum 4.
- Poor circulation (peripheral arterial disease), particularly in elderly people 5.
- Psoriasis, eczema and a number of other systematic diseases can affect the toenails.
- Nonsyndromic congenital nail disorder 10.
- Leprosy 6
- Congenital syphilis 7
Nonsyndromic congenital nail disorder 10 is caused by mutations in the FZD6 gene, which provides instructions for making a protein called frizzled-6. This protein is embedded in the outer membrane of many types of cells, where it is involved in transmitting chemical signals from outside the cell to the cell’s nucleus. The frizzled-6 protein plays an especially critical role in the growth and development of nails, particularly the attachment of the nail to the nail bed.
FZD6 gene mutations that cause nonsyndromic congenital nail disorder 10 lead to the production of a frizzled-6 protein that cannot get to the cell membrane where it is needed or that cannot transmit signals into the cell. As a result, the growth and development of nails is poorly regulated, which leads to onycholysis and other abnormalities of the fingernails and toenails.
Nonsyndromic congenital nail disorder 10 is inherited in an autosomal recessive pattern, which means both copies of the gene in each cell have mutations. The parents of an individual with an autosomal recessive condition each carry one copy of the mutated gene, but they typically do not show signs and symptoms of the condition.
Onychauxis treatment
Onychauxis treatment involves treating the underlying health cause and most people will start growing normal nails again once the underlying condition is managed or cured. In the meantime, patients with onychauxis can help ease discomfort by wearing comfortable shoes with wide toe boxes and engaging in exercise to help boost blood circulation. A podiatrist can reduce the thickness of the nails and keep them to a reasonable length. Periodic partial or total debridement of the thickened nail should be done with the help of electric drills or burrs 8. Chemical (40% urea paste) or surgical avulsion may be needed. Permanent ablation with chemical (phenol) or surgical matricectomy may be required for recurrent and troublesome onychauxis, can be employed in persons with a good vascular supply 9.
Mild fungal nail infections (onychomycosis) affecting less than 50% of one or two nails may respond to topical antifungal medications, but cure usually requires an oral antifungal medication for several months.
Recently, non-drug treatment has been developed to treat onychomycosis thus avoiding the side effects and risks of oral antifungal drugs.
Lasers emitting infrared radiation are thought to kill fungi by the production of heat within the infected tissue. Laser treatment is reported to safely eradicate nail fungi with one to three, almost painless, sessions. Several lasers have been approved for this purpose by the FDA and other regulatory authorities. However, high-quality studies of efficacy are lacking, and existing studies indicate that laser treatment is less medically effective than topical or oral antifungal agents.
- Nd:YAG (neodymium-doped yttrium aluminium garnet) continuous, long or short-pulsed lasers
- Ti:Sapphire modelocked laser
- Diode laser
Photodynamic therapy using the application of 5-aminolevulinic acid or methyl aminolevulinate followed by exposure to red light has also been reported to be successful in small numbers of patients, whose nails were presoftened or medically avulsed using 40% urea ointment for a week or so.
Iontophoresis and ultrasound are under investigation as devices used to enhance the delivery of antifungal drugs to the nail plate.
References- Cohen PR, Scher RK. Aging. In: Hordinsky MK, Sawaya ME, Scher RK, editors. Atlas of hair and nails. Philadelphia: Churchill Livingstone; 2000. p. 213-25.
- Nonsyndromic congenital nail disorder 10. https://medlineplus.gov/genetics/condition/nonsyndromic-congenital-nail-disorder-10
- Chen SX, Cohen PR. Parrot Beak Nails Revisited: Case Series and Comprehensive Review. Dermatol Ther (Heidelb). 2018;8(1):147-155. doi:10.1007/s13555-017-0217-y
- Leung AKC, Lam JM, Leong KF, et al. Onychomycosis: An Updated Review. Recent Pat Inflamm Allergy Drug Discov. 2020;14(1):32-45. doi:10.2174/1872213X13666191026090713
- Cabete J, Galhardas C, Apetato M, Lestre S. Onychomycosis in patients with chronic leg ulcer and toenail abnormalities. An Bras Dermatol. 2015;90(1):136-139. doi:10.1590/abd1806-4841.20152940
- Rajput CD, Nikam BP, Gore SB, Malani SS. Nail changes in leprosy: An observational study of 125 patients. Indian Dermatol Online J 2020;11:195-201. https://www.idoj.in/text.asp?2020/11/2/195/276551
- Leung AKC, Leong KF, Lam JM. A Case of Congenital Syphilis Presenting with Unusual Skin Eruptions. Case Rep Pediatr. 2018;2018:1761454. Published 2018 Mar 25. doi:10.1155/2018/1761454
- Singh G, Haneef NS, Uday. Nail changes and disorders among the elderly. Indian J Dermatol Venereol Leprol 2005;71:386-92 https://www.ijdvl.com/text.asp?2005/71/6/386/18941
- Cohen PR, Scher RK. Geriatric nail disorders: diagnosis and treatment. J Am Acad Dermatol 1992;26:521-31.