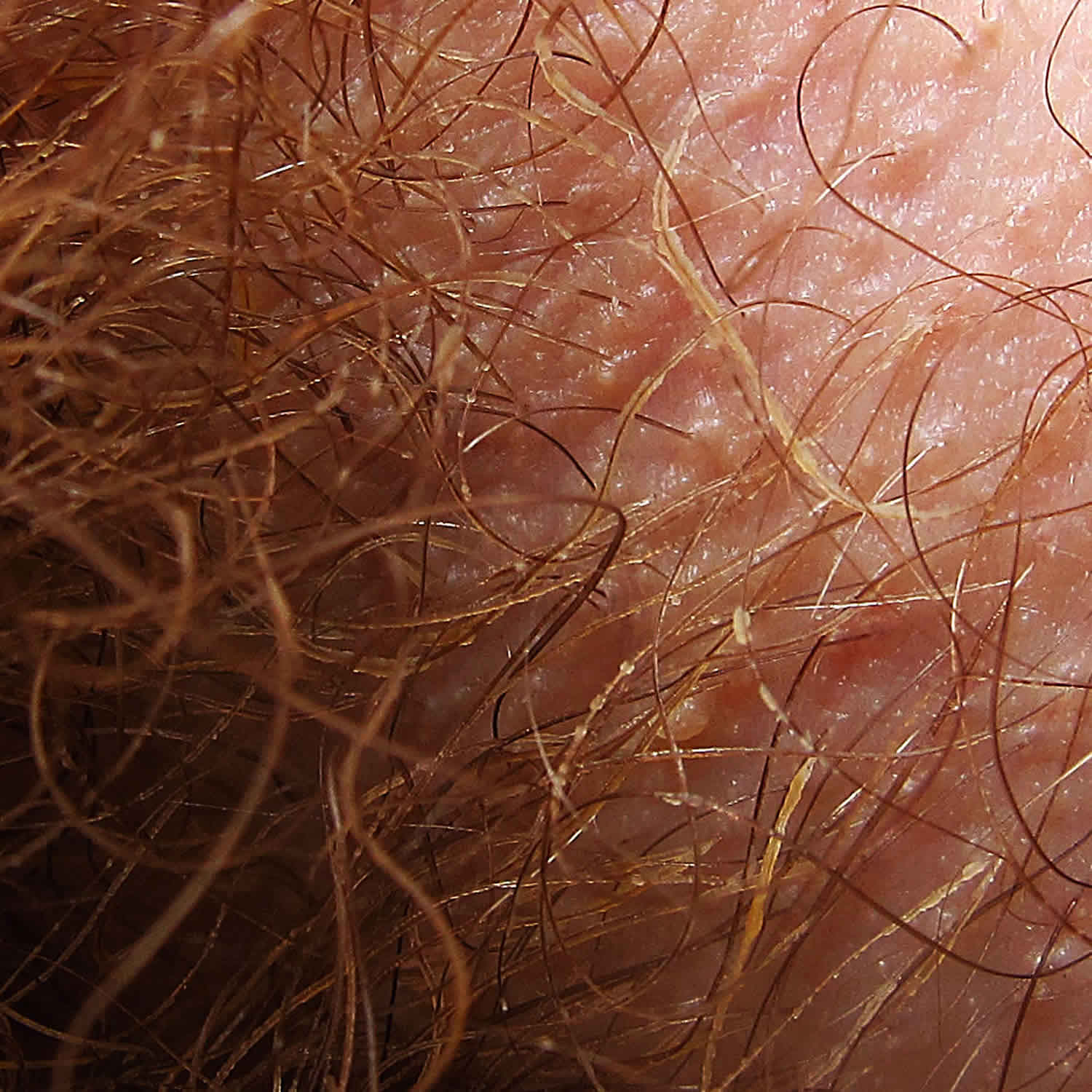
What is trichomycosis axillaris
Trichobacteriosis axillaris is a superficial bacterial infection of the hair shafts in sweat gland bearing areas, such as the armpits and the groin. On rare occasions the pubic hairs when it is called trichomycosis pubis, scrotal and intergluteal hairs may also be affected. The name is misleading because “trichomycosis” is bacterial in origin rather than a fungal infection, so it should be called trichobacteriosis 1. Trichobacteriosis axillaris is a trivial disease of worldwide occurrence that is believed to be caused by the genus Corynebacteria 1. Trichomycosis axillaris is a rare condition and few cases are reported in the literature.
Trichomycosis axillaris is often asymptomatic. Trichomycosis axillaris is characterized by the appearance of concretions (hair-nodules), yellow, black or red granular nodules or concretions that stick to the hair shaft, which grow around the hair shaft 2. However, patients may report sweaty malodorous armpits, and some may be aware of nodules or concretions on the axillary hairs. Similar nodules may present on the pubic hairs (trichomycosis pubis). Discolored axillary sweat may stain clothing. A history of poor hygiene and axillary hyperhidrosis are frequently elicited.
Due to the fact that the condition is asymptomatic and causes practically no discomfort 2, patients generally do not seek medical attention. However, when a careful, deliberate search is performed in the clinical setting, it tends to appear more frequently 3.
Is trichomycosis axillaris an STD?
No. Trichomycosis axillaris is a benign condition that does not have any complications.
Trichomycosis axillaris causes
Trichomycosis axillaris is caused by the overgrowth of Corynebacterium (Corynebacterium tenuis, Corynebacterium propinguum, Corynebacterium flavescens) and Serratia marcescens. The concretions consist of tightly packed bacteria. The bacteria proliferate in moist areas of the body, thus mainly affect underarm hairs, and to a lesser extent, pubic hair.
The bacteria cause malodour due to the metabolisation of testosterone in sweat into smelly compounds.
Trichomycosis infection begins when the causative agent comes in contact with the hair shaft, and the bacteria adhere to the surface, or the cuticle, of the hair, using a cement-like substance, the chemical composition of which is not yet known, that is insoluble in water as well as in the other principal solvents (i.e., acetone, ethanol) 1. Electron microscopy studies have clearly shown that the microorganism does not penetrate to the medulla’s cortex of the hair; instead, it only adheres strongly to the surface of the hair and develops slowly until it forms concretions around the hair shaft 4. Levit 5 has suggested that the adhesive substance is synthesized by both the apocrine glands of the human host and by the microorganism, which would explain why the disease develops in the areas of the body where it does (i.e., axillary, pubic and inter-gluteal hairs) 6.
Who gets trichomycosis axillaris?
Trichomycosis axillaris occurs in males and females of all races in temperate and tropical climates. It appears to be more common in men than women but this is because many women shave their underarm hair.
Contributing factors include:
- Humidity and warmth
- Crowded conditions
- Poor hygiene
- Hyperhidrosis
- Obesity
Trichomycosis axillaris symptoms
Trichomycosis axillaris is often symptomless and often ignored.
Trichomycosis axillaris signs include:
- Sweaty, smelly armpits
- 1–2 mm yellow, red or black concretions encircling the hair shaft, which make the hair appear beaded or thicker. Yellow concretions are the most common, whilst red and black are found in tropical climates
- Sweat is also discolored yellow, red or black, and may stain clothing
- Hair loss is rare, and is due to bacteria invadind and destroying the hair shaft
- The corynebacterial triad is the occurrence of erythrasma, trichomycosis axillaris, and pitted keratolysis in a single individual.
Trichomycosis axillaris diagnosis
- Trichomycosis axillaris is mostly diagnosed by its clinical appearance.
- Wood lamp examination shows pale-yellow fluorescence.
- Potassium hydroxide preparation and Gram staining can identify the bacteria.
Trichomycosis axillaris may resemble pubic lice (pediculosis) and Trichosporon aselie infections.
Trichomycosis axillaris treatment
The fastest way to get rid of trichomycosis axillaris is to clip the affected hairs or shave the area for a period of 2-3 weeks. Those patients who shave the affected area only once will generally experience a recurrence of the infection, since, the bacteria begin to develop the concretions once again as the hair grows back. Effective topical antibacterial preparations include clindamycin, erythromycin and fusidic acid. Topical treatments containing any of the following: 3% sulfur, 2% formalin, 1% mercury chloride (or mercuric chloride) or 2% sodium hypochlorite, as well as topical antibiotics with fusidic acid, erythromycin and clindamycin, may also be used 7. Anti fungal agents like naftifine and some azole derivatives (e.g., Clotrimazole powder) are effective as well and also curative 8.
Recurrences of trichomycosis axillaris are prevented by keeping the underarm dry and clean.
- Antiperspirants with aluminium chloride reduce sweating
- Antiseptics such as benzoyl peroxide gel or wash reduce bacterial colonization.
- Bonifaz A, Váquez-González D, Fierro L, Araiza J, Ponce RM. Trichomycosis (trichobacteriosis): clinical and microbiological experience with 56 cases. Int J Trichology. 2013;5(1):12–16. doi:10.4103/0974-7753.114704 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3746219
- Bargman H. Trichomycosis of the scrotal hair. Arch Dermatol. 1984;120:299.
- McBride ME, Duncan WC. Trichomycosis axillaris. Arch Dermatol. 1972;105:459–60.
- Shelley WB, Miller MA. Electron microscopy, histochemistry, and microbiology of bacterial adhesion in trichomycosis axillaris. J Am Acad Dermatol. 1984;10:1005–14.
- Levit F. Trichomycosis axillaris: A different view. J Am Acad Dermatol. 1988;18:778–9
- Lestringant GG, Qayed KI, Fletcher S. Is the incidence of trichomycosis of genital hair underestimated? J Am Acad Dermatol. 1991;24:297–8
- Rho NK, Kim BJ. A corynebacterial triad: Prevalence of erythrasma and trichomycosis axillaris in soldiers with pitted keratolysis. J Am Acad Dermatol. 2008;58:S57–8.
- Bonifaz A, Gómez-Daza F, Paredes V, Ponce RM. Tinea versicolor, tinea nigra, white piedra, and black piedra. Clin Dermatol. 2010;28:140–5.