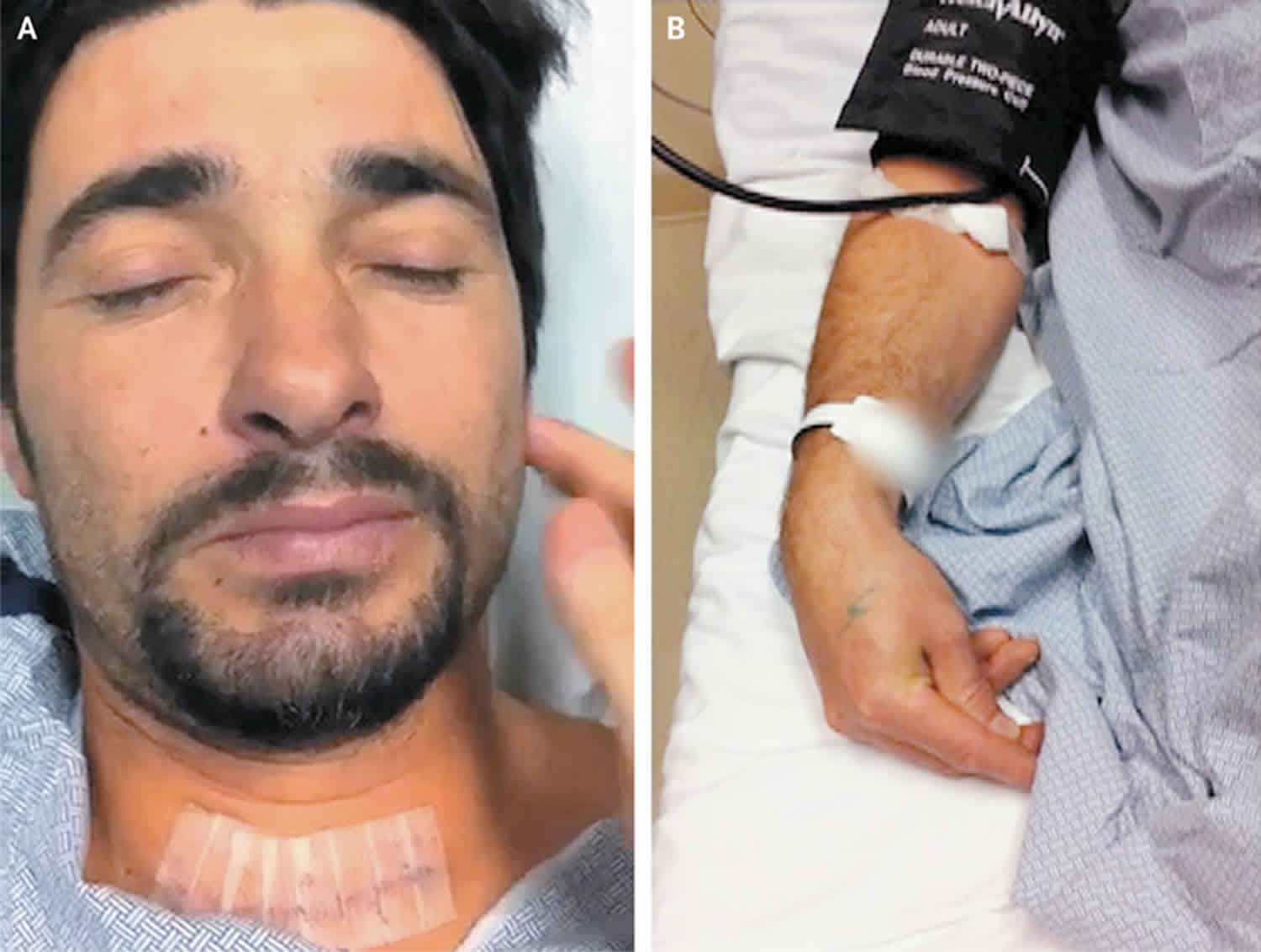
Chvostek’s sign
Chvostek sign is a contraction of ipsilateral facial muscles subsequent to percussion over the facial nerve and is considered a clinical indicator of hypocalcemia 1. Positive Chvostek’s sign represents increased neuromuscular excitability caused by hypocalcaemia. Chvostek’s sign is elicited by tapping on the face at a point just anterior to the ear and just below the zygomatic bone 2. A positive response is represented by twitching of the ipsilateral facial muscles, suggesting neuromuscular excitability caused by hypocalcaemia. Although, classically described with hypocalcaemia due to hypoparathyroidism, it is also elicited in some young healthy children and alkalotic states as during vomiting and hyperventilation 2. Chvostek’s sign is very easy to test in clinical practice compared with Trousseau’s sign and hence its clinical significance. However, up to 10% of the population will have a positive Chvostek sign in the absence of hypocalcemia; thus, this test, while suggestive, is not diagnostic of hypocalcemia 3.
The correlation of hypocalcemia and Chvostek sign has long had acceptance in the medical community, despite there being very little literature to support this claim 4. A population-based study performed by Dr. Hujoel 1 found that there was no correlation of Chvostek sign and hypocalcemia, and furthermore, for every 1 mg/dl increase in calcium, there was a 4% higher chance of a positive Chvostek sign. It was, in turn, concluded that hypercalcemia had a more significant correlation with facial nerve tetany upon stimulation. Further studies have shown that a positive Chvostek sign can be elicited in 25% of healthy individuals, and 29% of those with hypocalcemia did not produce a positive sign 5.
Hypocalcemia is defined as a total serum calcium concentration less than 8.8 mg/dL (< 2.20 mmol/L) in the presence of normal plasma protein concentrations or as a serum ionized calcium concentration < 4.7 mg/dL (< 1.17 mmol/L) 6. Note that reference ranges for serum calcium vary by age and sex.
Hypocalcemia may be acquired or hereditary. Acquired causes include a variety of illnesses (eg, hypoparathyroidism, hepatic disease, kidney disease), diet, medication, and surgery.
Calcium is an essential electrolyte in the body. Calcium is associated with many functions, and of significance; muscle contractions and propagation of nerve impulses. Deficiencies in calcium may lead to seizures, cardiomyopathy, QT prolongation (can precipitate deadly arrhythmias), and congestive heart failure 7. Ventricular arrhythmias are among the most critical and can lead to cardiac arrest 8. Secondary to this; patients often receive replacement therapy in the hospital setting. One common cause of hypocalcemia is a complication during thyroidectomies 9. According to Rio Del, et al. 9 there is a 13.8% incidence of hypocalcemia status post a thyroid lobectomy, and a 38.8% incidence status post total thyroidectomy. Supplementation with calcium carbonate in a patient who has undergone thyroid surgery has become common practice because of the potential for hypocalcemia. Patients receiving calcium supplementation should avoid proton pump inhibitors because they are well known to cause worsening of hypocalcemia 10. As discussed above, there is a minimal correlation with calcium levels and Chvostek sign; although this may be true, if tetany presents with stimulation of the facial nerve, it may be beneficial to check the serum calcium level.
Resolution of Chvostek’s sign occurs with effective treatment of hypoparathyroidism with calcium and active vitamin D.
The parathyroid gland is located on the posterior surface of the thyroid gland, and during the procedure, a lobe of the gland may get resected. The parathyroid gland produces parathyroid hormone (PTH), and resection can lead to a decrease in PTH levels 11. Parathyroid hormone regulates calcium levels in the body; hence, a reduction in its serum level will lead to hypocalcemia.
The presentation of hypocalcemia varies widely, from asymptomatic to life-threatening. Hypocalcemia is frequently encountered in patients who are hospitalized. Depending on the cause, unrecognized or poorly treated hypocalcemic emergencies can lead to significant morbidity or death 12. Symptomatic patients with classic clinical findings of acute hypocalcemia require immediate resuscitation and evaluation. However, most cases of hypocalcemia are discovered by clinical suspicion and appropriate laboratory testing.
The treatment of hypocalcemia depends on the cause, the severity, the presence of symptoms, and how rapidly the hypocalcemia developed. Most cases of hypocalcemia are clinically mild and require only supportive treatment and further laboratory evaluation. Oral calcium repletion may be indicated for outpatient treatment of mild cases. On occasion, severe hypocalcemia may result in seizures, tetany, refractory hypotension, or arrhythmias that require a more aggressive approach, including intravenous infusions of calcium.
Trousseau’s sign
Trousseau’s sign is a carpopedal spasm induced by ischemia through inflation of a sphygmomanometer cuff to a suprasystolic blood pressure. Trousseau’s sign emerged at 25 seconds after the start of cuff inflation, with a maximal spasm at 60 seconds. Trousseau sign reported sensitivity and specificity for hypocalcemia are 94% and 99%, respectively 13.
Test for the Trousseau sign by placing a blood pressure cuff on the patient’s arm and inflating to 20 mm Hg above systolic blood pressure for 3-5 minutes. This increases the irritability of the nerves, and a flexion of the wrist and metacarpal phalangeal joints can be observed with extension of the interphalangeal joints and adduction of the thumb (carpal spasm). The Trousseau sign is more specific than the Chvostek sign but has incomplete sensitivity.
References- Hujoel IA. The association between serum calcium levels and Chvostek sign: A population-based study. Neurol Clin Pract. 2016;6(4):321–328. doi:10.1212/CPJ.0000000000000270 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5727700
- Kamalanathan S, Balachandran K, Parthan G, et al. Chvostek’s sign: a video demonstration Case Reports 2012;2012:bcr2012007098 http://dx.doi.org/10.1136/bcr-2012-007098
- What is the Chvostek sign in patients with hypocalcemia? https://www.medscape.com/answers/241893-20150/what-is-the-chvostek-sign-in-patients-with-hypocalcemia
- Hujoel IA. The association between serum calcium levels and Chvostek sign: A population-based study. Neurol Clin Pract. 2016 Aug;6(4):321-328.
- Méneret A, Guey S, Degos B. Chvostek sign, frequently found in healthy subjects, is not a useful clinical sign. Neurology. 2013 Mar 12;80(11):1067.
- Hypocalcemia. https://emedicine.medscape.com/article/241893-overview
- Humphrey E, Clardy C. A Framework for Approaching Refractory Hypocalcemia in Children. Pediatr Ann. 2019 May 01;48(5):e208-e211
- Ashwin Reddy S. Ventricular Arrhythmia Precipitated by Severe Hypocalcaemia Secondary to Primary Hypoparathyroidism. Case Rep Cardiol. 2019;2019:4851073.
- Del Rio P, Rossini M, Montana CM, Viani L, Pedrazzi G, Loderer T, Cozzani F. Postoperative hypocalcemia: analysis of factors influencing early hypocalcemia development following thyroid surgery. BMC Surg. 2019 Apr 24;18(Suppl 1):25.
- Milman S, Epstein EJ. Proton pump inhibitor-induced hypocalcemic seizure in a patient with hypoparathyroidism. Endocr Pract. 2011 Jan-Feb;17(1):104-7.
- Philips R, Nulty P, Seim N, Tan Y, Brock G, Essig G. Predicting transient hypocalcemia in patients with unplanned parathyroidectomy after thyroidectomy. Am J Otolaryngol. 2019 Jul – Aug;40(4):504-508.
- Goyal A, Singh S. Hypocalcemia. [Updated 2019 Jan 21]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK430912
- Jesus JE, Landry A. Images in clinical medicine. Chvostek’s and Trousseau’s signs. N Engl J Med 2012;367:e15. doi:10.1056/NEJMicm1110569