What is oxalate
Oxalate in the mammalian body originates from two main sources: endogenous (body in your liver) production and external source via dietary intake. The ratio between liver-generated and absorption-related sources depends on oxalate content in ingested food. Both sources have a potentially important role in increasing oxalate concentrations in plasma and urine. Oxalate is a toxic simple organic acid that is ubiquitous in the plant kingdom and widely consumed in normal human diets as a component of fruits, vegetables, grains and nuts 1. The normal daily intake of oxalate ranges from 70 to 920 mg, but strongly increases in vegetarians 2. The average daily dietary oxalate intake content in the United States is 214 mg in men, 185 mg in older women, and 183 mg in younger women; spinach accounts for > 40% of the oxalate intake 3. Despite the toxicity of oxalate to mammals, it cannot be degraded by mammalian enzymes 4. However, it can be metabolized by many gut bacteria, such as Oxalobacter formigenes and Lactobacillus acidophilus, among others 5.
Figure 1. Oxlate sources
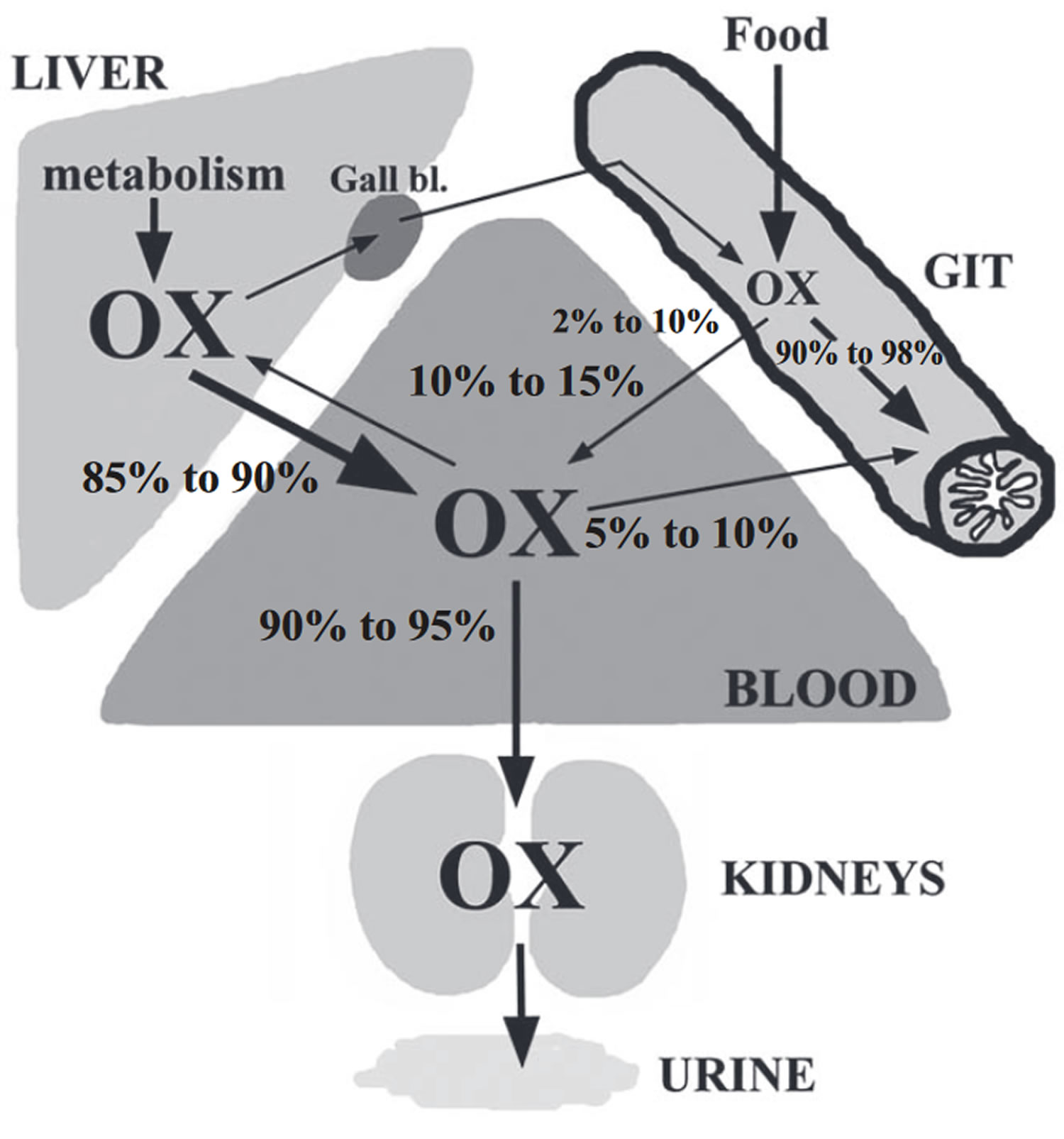
Note: OX= oxalate; Gall bl.= gallbladder; GIT= gastrointestinal tract
[Source 6]Factors leading to high rates of oxalate absorption from the gut include the presence of medical conditions or surgical interventions leading to steatorrhea, low dietary content in calcium and magnesium, both of which bind oxalate in the gastrointestinal tract and decrease its absorption and renal excretion, and the absence from the intestinal flora of certain species of bacteria, in particular, Oxalobacter formigenes, an anaerobic bacterium that metabolizes oxalate. The absence of this bacterium from the gut has been associated with hyperoxaluria, but bacteriotherapies involving oxalate-degrading bacteria have met with mixed results 7. While probiotics containing Oxalobacter formigenes, Lactobacillus spp., Bifidobacterium spp., or Enterococcus spp. effectively reduce urinary oxalate excretion, the bacteria and the oxalate-degrading function are often lost when probiotic use ceases and/or oxalate is removed from the diet 8. In some cases, urinary oxalate remains unchanged despite long-term administration of probiotics and persistence of oxalate-degrading microbes in the gut 9.
Oxalate is also natural chemical in your body. Oxalate is produced by many kinds of cells, including liver cells, kidney, epithelial cells and apocrine cells, among others 10, 11. Most of body oxalate is a metabolic end-product generated largely in the liver and represents 85 % to 90 % of the total oxalate circulating in blood (endogenous oxalate). An unknown proportion of the liver-produced oxalate is removed via bile secretion. The remainder (10 % to 15 %) of blood oxalate (exogenous oxalate) originates from the absorption of food in the gastrointestinal tract. The bulk (90 % to 95 %) of circulating oxalate is ultimately excreted by the kidneys, whereas some 5 % to 10 % of blood oxalate is excreted in the terminal parts of the small intestine and colon. And too much oxalate in your urine can cause serious problems.
Hyperoxaluria is defined as excessive urinary oxalate excretion, which occurs when you have too much oxalate in your urine 12. Too much oxalate in your urine can cause serious problems when the excess oxalate combines with calcium in urine to form the most common type of kidney stone, a calcium oxalate stone and has been associated with acute or chronic kidney injury 13.
Hyperoxaluria develops as a consequence of either excessive endogenous oxalate production (primary hyperoxaluria) or excessive oxalate absorption from the gastrointestinal tract. The later can be associated with enteric hyperoxaluria from fat malabsorption, e.g., in patients with Roux-en-Y gastric bypass surgery 14, jejunoileal bypass surgery 15, Crohn’s disease 16, sprue 17 or taking medications such as orlistat that cause fat malabsorption 18. Other potential culprits for excessive oxalate absorption include either excessive dietary intake of oxalate or its substrate (vitamin C) or dietary deficiency of calcium or magnesium 19.
Although there is substantial variation between individuals, urinary oxalate excretion rises in parallel with dietary oxalate intake when other variables potentially affecting oxaluria are under control 20. Chronic intake of food items with a high content of oxalate may lead to hyperoxaluria with urinary oxalate excretion similar to the degree usually seen in primary hyperoxaluria. The component of urinary oxalate excretion that is derived from gastrointestinal absorption is determined by the oxalate content of the diet and the rate of absorption of oxalate in the intestines. Food items high in oxalate include leafy vegetables, such as spinach, various nuts, e.g., peanuts, and tropical fruits, including Averrhoa carambola (starfruit) and Averrhoa bilimbi (commonly known as bilimbi or cucumber tree) 21.
The proportion of urinary oxalate that is derived from dietary oxalate is estimated to range from 10 to 50% 22. In addition to oxalate intake, intake of oxalate precursors may cause hyperoxaluria. Vitamin C (ascorbic acid), pyridoxylate, which is a combination of glyoxylic acid and pyridoxine, and hydroxyproline are potential sources of oxalate that have caused hyperoxaluric renal disease in clinical and experimental studies. Furthermore, hyperoxaluria and oxalate nephropathy may develop as a result of the oxalate salts of parenteral medications. It is well established that a large proportion of urinary oxalate is derived from the endogenous metabolism of glycine, glycolate, hydroxyproline, and dietary vitamin C 23. A recent metabolic study compared a controlled diet with 25% of protein from gelatin (2.75 g of hydroxyproline) with the same diet except with 25% of protein from whey (containing no hydroxyproline) 24. The diet that was high in hydroxyproline increased urinary oxalate excretion by 42%. Another metabolic trial demonstrated that 1000 mg of supplemental vitamin C consumed twice daily increased urinary oxalate excretion by 20 to 33% 25.
A review of oxalate load studies indicates that a peak in urinary oxalate excretion normally occurs two to four hours after the oxalate ingestion 26. Thus, it is quite possible that such transient oxalate loads on the kidney result in a transient hyperoxaluria. Interestingly, Gambaro et al have noted that the fractional excretion of oxalate was 70% higher in stone formers compared with normal individuals 27. It is plausible that a transient renal oxalate load on the kidney associated with an oxalate-rich meal might lead to renal cell injury, most likely in the proximal tubule. This may be amplified in stone formers due to an enhanced oxalate secretion and an elevated intestinal absorption 28. It has been established that oxalate can affect renal cells by either stimulating cellular proliferation or by inducing cell injury 29.
Calcium stones, including calcium oxalate stones ~ 70% and calcium phosphate stones ~ 15%, are the most common types of kidney stones. Calcium oxalate is also associated with benign breast tissue calcifications 30. Furthermore, a low-calcium diet was shown to be a significant risk factor for the kidney stones (calcium oxalate stones) disease 31. The explanation for the role of dietary calcium was that it complexed intestinal oxalate and limited its availability for absorption 31. In a study 32, a 34% increase in urinary oxalate excretion accompanied the decrease in calcium intake from 1002 mg to 391 mg per day, which is consistent with this theory. The studies of Liebman and Chai also support this role for dietary calcium in showing that supplemental calcium decreased the absorption of an oxalate load by more than 50% 31. Other observational studies have shown an inverse relation between dietary calcium and the risk for incident kidney stones 33, 34 suggested that dietary calcium may bind to oxalate in the gut, thereby limiting intestinal oxalate absorption (and subsequent urinary oxalate excretion). Indeed, the inhibitory effect of calcium ingestion on urinary oxalate excretion has been demonstrated in oxalate loading studies 35. Magnesium intake may also decrease urinary oxalate in a similar manner 36, 37.
Moreover, there is nearly universal agreement in studies of normal and stone-forming populations that the mean calcium excretion of the stone forming population is higher than that of the normal population, that the incidence of hypercalciuria (high urine calcium concentration) in the stone-forming population is 5 to 10 times above that in a normal population, and that the relative supersaturation of the urine is higher in hypercalciuric individuals than in normocalciuric individuals 38, 39. Differences in oxalate excretion are less pronounced, suggesting that if oxalate plays a role it may in part be due to effects other than by affecting relative supersaturation alone.
Currently, there are no established therapies that decrease urinary oxalate excretion in individuals with idiopathic calcium oxalate kidney stones disease. They are often advised, without substantial data to support the efficacy of this dietary recommendation, to avoid oxalate-rich foods 20.
Foods high in oxalate
Dietary hyperoxaluria has been reported after ingestion of large amounts of food products with high oxalate content for medicinal, cosmetic or weight loss purposes. Most commonly implicated vegetables and fruits are peanuts 40, Averrhoa bilimbi (commonly known as bilimbi or cucumber tree) 21, celery, carrots, parsley, beets, and spinach 41.
Even though those food products are ubiquitous in many diets, there have been few reports of renal parenchymal disease secondary to dietary hyperoxaluria 42. Bakul et al have described a case series of 10 patients who developed acute renal failure after consumption of A. bilimbi fruit juice 21. Seven patients required hemodialysis while 3 cases recovered kidney function with conservative management. While their serum creatinine values at time of diagnosis ranged from 5.5 to 12.3 mg/dL, all 10 patients recovered within 2 to 6 weeks.
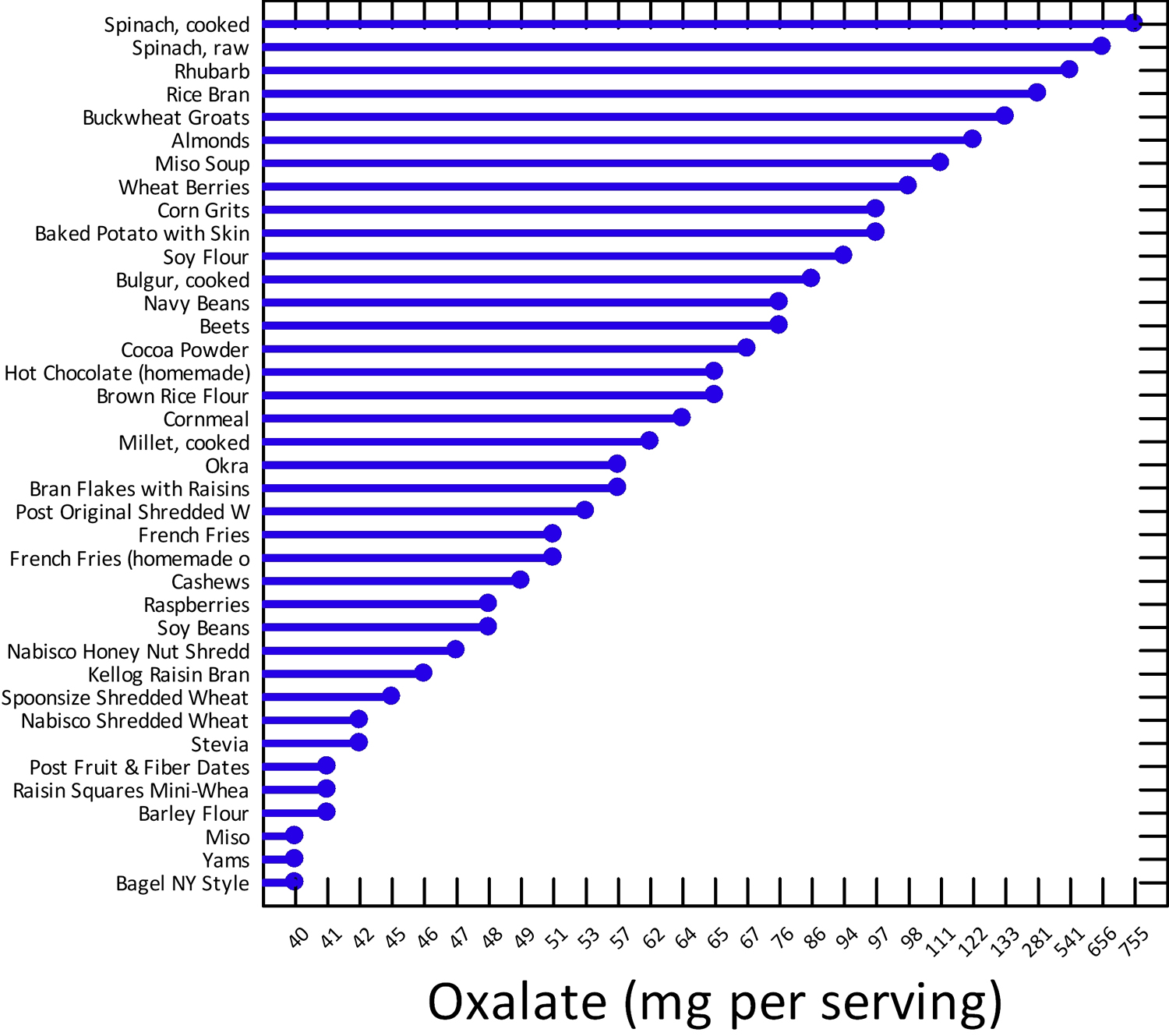
Figure 2. Oxalate rich foods
Table 1. Foods that contribute to oxalate
| Food | % | Food | % | Food | % |
|---|---|---|---|---|---|
| Cooked spinach | 23.1 | Cooked spinach | 25.8 | Cooked spinach | 22.0 |
| Raw spinach | 17.3 | Raw spinach | 18.4 | Raw spinach | 20.3 |
| Potatoes (whole) | 10.2 | Potatoes (whole) | 11.1 | Potatoes (whole) | 9.9 |
| Cold cereal | 4.4 | Cold cereal | 4.3 | Cold cereal | 3.8 |
| Oranges | 2.9 | Oranges | 2.5 | French fries | 2.5 |
| French fries | 1.9 | Coffee | 1.7 | Oranges | 2.0 |
| Mixed nuts | 1.7 | Cooked carrots | 1.7 | Pasta | 2.0 |
| Navy beans (canned) | 1.7 | Tea | 1.6 | Pasta sauce | 1.9 |
| Cookies | 1.6 | Cookies | 1.5 | English muffins | 1.7 |
| Peanuts | 1.6 | Pasta sauce | 1.4 | Coffee | 1.7 |
Note 43: Spinach has 794 mg oxalate/100 g; Potato has 24.7 mg oxalate/100 g;
[Source 44]Table 2. Oxalate content of foods
| Food Item | Serving size | Oxalate Category | Oxalate Value | ||
| Spinach, cooked | 1/2 cup | Very High | 755 | ||
| Spinach, raw | 1 cup | Very High | 656 | ||
| Rhubarb | 1/2 cup | Very High | 541 | ||
| Rice Bran | 1 cup | Very High | 281 | ||
| Buckwheat Groats | 1 cup cooked | Very High | 133 | ||
| Almonds | 1 oz or 22 kernels | Very High | 122 | ||
| Miso Soup | 1 cup | Very High | 111 | ||
| Wheat Berries | 1 cup cooked | Very High | 98 | ||
| Corn Grits | 1 cup | Very High | 97 | ||
| Corn Grits | 1 cup | Very High | 97 | ||
| Baked Potato with Skin | 1 medium | Very High | 97 | ||
| Soy Flour | 1 cup | Very High | 94 | ||
| Bulgur, cooked | 1 cup | Very High | 86 | ||
| Navy Beans | 1/2 cup | Very High | 76 | ||
| Beets | 1/2 cup | Very High | 76 | ||
| Cocoa Powder | 4 tsp | Very High | 67 | ||
| Hot Chocolate (homemade) | 1 cup | Very High | 65 | ||
| Brown Rice Flour | 1 cup | Very High | 65 | ||
| Brown Rice Flour | 1 cup | Very High | 65 | ||
| Cornmeal | 1 cup | Very High | 64 | ||
| Cornmeal | 1 cup | Very High | 64 | ||
| Millet, cooked | 1 cup | Very High | 62 | ||
| Okra | 1/2 cup | Very High | 57 | ||
| Bran Flakes with Raisins, Single Brand | 1 cup | Very High | 57 | ||
| Post Original Shredded Wheat & Bran | 1 1/4 cup | Very High | 53 | ||
| French Fries | 4 oz | Very High | 51 | ||
| French Fries (homemade or fast food) | 4 oz or 1/2 cup | Very High | 51 | ||
| Cashews | 1 oz or 18 kernels | Very High | 49 | ||
| Raspberries | 1 cup | Very High | 48 | ||
| Soy Beans | 1/2 Cup | Very High | *** | 48 | |
| Nabisco Honey Nut Shredded Wheat Bite Size | 1 cup | Very High | 47 | ||
| Kellog Raisin Bran | 1 cup | Very High | 46 | ||
| Spoonsize Shredded Wheat | 1 cup | Very High | 45 | ||
| Nabisco Shredded Wheat | 2 biscuits | Very High | 42 | ||
| Stevia | 1 tsp | Very High | *** | 42 | |
| Post Fruit & Fiber Dates, Raisins & Walnuts | 1 cup | Very High | 41 | ||
| Raisin Squares Mini-Wheats | 3/4 cup | Very High | 41 | ||
| Barley Flour | 1/2 Cup | Very High | *** | 41 | |
| Miso | 1 cup | Very High | 40 | ||
| Miso | 1 cup | Very High | 40 | ||
| Yams | 1/2 cup, cubed | Very High | 40 | ||
| Bagel NY Style | 1 Bagel | Very High | *** | 40 | |
| Lentil Soup | 1 cup | Very High | 39 | ||
| Mixed Nuts (with Peanuts) | 1 oz | Very High | 39 | ||
| Chocolate Syrup | 2 Tbs | Very High | 38 | ||
| Chocolate Syrup | 2 Tbs | Very High | 38 | ||
| Candies with Nuts (ex Snickers) | 2 oz | Very High | 38 | ||
| Candies with Nuts (ex Snickers) | 2 oz | Very High | 38 | ||
| Pancakes (dry mix) | 4 pancakes | Very High | 37 | ||
| General Mills Multi-Bran Chex | 1 cup | Very High | 36 | ||
| Post 40% Bran | 3/4 cup | Very High | 36 | ||
| Stuffing | 1 cup | Very High | 36 | ||
| Kellog Special K Low Carb | 1/2 Cup | Very High | *** | 35 | |
| Post Cranberry Almond Crunch (Morning Traditions) | 1 cup | Very High | 35 | ||
| Bamboo Shoots | 1 cup | Very High | 35 | ||
| Kellog Complete Wheat Bran | 3/4 cup | Very High | 34 | ||
| General Mills Total Raisin Bran | 1 cup | Very High | 31 | ||
| Rutabaga | 1/2 cup mashed | Very High | 31 | ||
| Walnuts | 1 cup or 7 nuts | Very High | 31 | ||
| Brownies | 1 oz or 1/2 brownie | Very High | 31 | ||
| Dried Pineapples | 1/2 cup | Very High | 30 | ||
| Turnip | 1/2 cup mashed | Very High | 30 | ||
| Mashed Potatoes | 1 cup | Very High | 29 | ||
| Orange | 1 fruit | Very High | 29 | ||
| Wheat Flour, Whole Grain | 1 cup | Very High | 29 | ||
| Wheat Flour, Whole Grain | 1 cup | Very High | 29 | ||
| Fudge Sauce | 2 Tbs | Very High | 28 | ||
| Fudge Sauce | 2 Tbs | Very High | 28 | ||
| Kellog Frosted Mini-Wheats | 1 cup | Very High | 28 | ||
| Sweet Potatoes | 1 cup | Very High | 28 | ||
| Kellog Raisin Bran Crunch | 1 cup | Very High | 27 | ||
| Peanuts | 1 oz | Very High | 27 | ||
| Soy Protein Isolate | 1 oz | Very High | 27 | ||
| Carrot Juice | 1 cup | Very High | 27 | ||
| Kellog All-Bran Original | 1/2 cup | Very High | 26 | ||
| Post 100% Bran | 1/3 cup | Very High | 25 | ||
| Post Banana Nut Crunch | 1 cup | Very High | 25 | ||
| Chili with Beans | 1 cup | Very High | 24 | ||
| Dates | 1 date | Very High | 24 | ||
| Dried Figs | 5 pieces/fruits | Very High | 24 | ||
| General Mills Oatmeal Crisp with Almonds | 1 cup | Very High | 24 | ||
| General Mills Raisin Nut Bran | 1 cup | Very High | 24 | ||
| Veggie Burger | 1 pattie | Very High | 24 | ||
| Brown Rice, cooked | 1 cup | Very High | 24 | ||
| General Mills Honey Nut Clusters | 1 cup | Very High | 23 | ||
| Lasagna | 1 serving | Very High | 23 | ||
| Lasagna with meat | 1 serving | Very High | 23 | ||
| Pancakes (Homemade) | 4 pancakes | Very High | 22 | ||
| Potato Chips | 1 oz | Very High | 21 | ||
| Potato Chips | 1 oz | Very High | 21 | ||
| Fava Beans | 1/2 cup | Very High | 20 | ||
| Kellog All-Bran Buds | 1/2 cup | Very High | 20 | ||
| Kellog Mueslix Apple & Almond Crunch | 2/3 cup | Very High | 20 | ||
| Soy Milk | 1 Cup | Very High | *** | 20 | |
| Celery Raw | 1/2 Cup | Very High | *** | 19 | |
| Avocados | 1 fruit | Very High | 19 | ||
| Cream of Wheat | 1 cup | Very High | 18 | ||
| Olives | approx 10 olives | Very High | 18 | ||
| Post Great Grains Crunch Pecan | 2/3 cup | Very High | 18 | ||
| V8 Juice | 1 cup | Very High | 18 | ||
| General Mills Basic 4 | 1 cup | Very High | 17 | ||
| Mueslix | 2/3 cup | Very High | 17 | ||
| Post Great Grains Raisin, Dates & Pecans | 2/3 cup | Very High | 17 | ||
| Potato Salad | 1/3 cup | Very High | 17 | ||
| Pumpkin Seeds | 1 cup, cooked | Very High | 17 | ||
| Tomato Sauce | 1/2 cup | Very High | 17 | ||
| All-Purpose Flour | 1 cup | Very High | 17 | ||
| All-Purpose Flour | 1 cup | Very High | 17 | ||
| Brussel Sprouts Raw | 1/2 Cup | Very High | *** | 17 | |
| Burritos with beans | 1 burrito | Very High | 17 | ||
| Farina Cereal | 1 cup | Very High | 16 | ||
| Kellog Low Fat Granola with Raisins | 2/3 cup | Very High | 16 | ||
| Kiwi | 1 fruit | Very High | 16 | ||
| Peanut Butter Reduced Fat | 1 Tbs | Very High | 16 | ||
| Refried Beans | 1/2 cup | Very High | 16 | ||
| Tahini | 1 Tbs | Very High | 16 | ||
| Burritos with beans & meat | 1 burrito | Very High | 16 | ||
| Cake (homemade) | 1 piece | Very High | 16 | ||
| Couscous | 1 cup | Very High | 15 | ||
| Kellog Cracklin’ Oat Bran | 3/4 cup | Very High | 15 | ||
| Kellog Smart Start | 1 cup | Very High | 15 | ||
| Lemonade (frozen from concentrate) | 8 oz | Very High | 15 | ||
| Quaker Low Fat 100% Natural Granola with Raisins | 3/4 cup | Very High | 15 | ||
| Parsnip | 1/2 cup | Very High | 15 | ||
| Red Kidney Beans | 1/2 cup | Very High | 15 | ||
| Trail Mix | 1 oz | Very High | 15 | ||
| Cake (store brand) | 1 piece | Very High | 15 | ||
| Carrots, raw | 1/2 Cup | Very High | *** | 15 | |
| Danish Pastry Homemade | 1 pastry | Very High | 14 | ||
| Kellog Kashi Go Lean | 3/4 cup | Very High | 14 | ||
| Pistachios | 1 oz or 48 kernels | Very High | 14 | ||
| Post Grape Nuts | 1/2 cup | Very High | 14 | ||
| Tea, Brewed | 1 cup | Very High | 14 | ||
| Tomato Juice | 1 cup | Very High | 14 | ||
| Cheeseburger with bun | 1 burger & bun | Very High | 13 | ||
| Clam Chowder | 1 cup | Very High | 13 | ||
| Enchilada with Cheese & beef | 1 enchilada | Very High | 13 | ||
| Enchilada with Chicken | 1 enchilada | Very High | 13 | ||
| French Toast | 2 slices | Very High | 13 | ||
| French Toast | 2 slices | Very High | 13 | ||
| General Mills Fiber One | 1/2 cup | Very High | 13 | ||
| General Mills Nature Valley Cinnimon & Raisins Granola | 3/4 cup | Very High | 13 | ||
| General Mills Oatmeal Raisin Crisp | 1 cup | Very High | 13 | ||
| Kellog Just Right Fruit & Nut | 1 cup | Very High | 13 | ||
| Kellog Puffed Kashi | 1 cup | Very High | 13 | ||
| Nachos with Cheese | 6-8 chips | Very High | 13 | ||
| Peanut Butter | 1 Tbs | Very High | 13 | ||
| Pizza with Cheese | 2 slices | Very High | 13 | ||
| Red River Cereal | 1/4 cup | Very High | 13 | ||
| Rice Dream | 1 cup | Very High | 13 | ||
| Sweet Rolls Low Fat | 1 pastry | Very High | 13 | ||
| Tofu | 3.5oz | Very High | 13 | ||
| Quaker 100% Natural Granola Oats & Honey | 1/2 cup | Very High | 13 | ||
| English Muffin Whole Wheat | 1 muffin | High | 12 | ||
| English Muffins Whole Wheat ONLY | 1 muffin | High | 12 | ||
| Grapefruit | 1/2 fruit | High | 12 | ||
| Grilled Cheese Sandwich | 1 sandwich | High | 12 | ||
| Sunflower Seeds | 1 cup | High | 12 | ||
| Tacos | 1 small taco | High | 12 | ||
| General Mills Harmony | 1 1/4 cup | High | 11 | ||
| General Mills Wheaties Raisin Bran | 1 cup | High | 11 | ||
| Kellog All-Bran with Extra Fiber | 1/2 cup | High | 11 | ||
| Kellog Cocoa Krispies | 3/4 cup | High | 11 | ||
| Pancakes (Homemade) | 4 cakes | High | 11 | ||
| Spaghetti | 1 cup cooked | High | 11 | ||
| Uncle Sam | 1 cup | High | 11 | ||
| White Rice Flour | 1 cup | High | 11 | ||
| White Rice Flour | 1 cup | High | 11 | ||
| Cake (Low Fat Only) | 1 piece | High | 11 | ||
| Celery, Cooked | 1 cup | High | 10 | ||
| Chocolate Chip Cookies (store brand) | 1 cookie | High | 10 | ||
| Collards | 1 cup | High | 10 | ||
| Kellog Kashi Good Friends | 3/4 cup | High | 10 | ||
| Quaker Oat Bran | 1 1/4 cup | High | 10 | ||
| Pancakes (mix) | 4 cakes | High | 10 | ||
| Pecans | 1 oz or 15 halves | High | 10 | ||
| Blueberry Muffins | 1 muffin | High | 9 | ||
| Other Brands of Cereal | |||||
| Quaker Cereals |
What is oxalate diet
Typical diets contain upward of 200 – 300 mg of oxalate. For stone prevention, a reasonable goal is below 100 mg of oxalate daily. An ideal would be about 50 mg daily if that can be accomplished.
To get there, consider the oxalate contents in common serving portions of all of the foods, and make up a plan for yourself. For further help, we suggest discussing your diet with either your physician or a registered dietician.
Existing data on the oxalate content of food are conflicting, making it hard to know what foods can be included in a low oxalate diet. The Harvard School of Public Health maintains a database of foods analyzed for oxalate content 46.
Table 3. Low Oxalate Food Alternatives
| Foods High in Oxalate | Low Oxalate Alternatives |
| Nut Products (Almonds, Cashews, Peanuts, Pecans, Walnuts) | Popcorn |
| Potato Chips | Popcorn, Graham Crackers, Triscuits, Saltines |
| Chocolate Chip Cookies | Oatmeal Cookies, Fig Bars, Popsicles, Pudding, Jello |
| Rice Dream | Soy Milk |
| Grapefruit, Oranges, Tangerines | Cantaloupe, Honeydew Melon, Mango, Nectarines |
| Dates | Figs, Raisins |
| Canned Pineapple | Canned Peaches, Canned Pears |
| Dried Figs, Dried Pineapple | Dried Apricots, Apples or Cranberries |
| Fava, Navy or Refried Beans | Soybeans, Mung Beans |
| Spinach | Lettuce, Broccoli, Brussels Sprouts |
| Turnip, Yams | Yellow Squash |
| Asparagus | Broccoli, Brussels Sprouts, Cauliflower |
| Collards | Kale, Mustard Greens |
| Potatoes | White Rice, Macaroni & Cheese |
| Cream of Wheat, Red River Cereal, Farina Cereal, Corn Grits | Oatmeal Cereal, Granola Bars |
| French Toast, Pancakes | Cornbread, Eggs |
| Clam Chowder, Lentil Soup, Miso Soup | Chicken Noodle Soup |
| Cheeseburger | Hot Dog, Chicken Nuggets |
| Lasagna | Macaroni & Cheese |
| Peanut Butter | Apple Butter |
| Tomato Sauce | Cream Sauce, Olive Oil, Mozzarella Cheese |
| Blueberry Muffins | Oat Bran Muffin, Corn Bread |
Table 4. Low oxalate meal plan
| Choices Low Oxalate Diet | Serving size | Oxalate Content |
| Breakfast Meal (Early Morning) | ||
| Multi-Grain Cheerios | 1 cup | 4.3 |
| Milk (skim or 1%) | 3/4-1 cup | 0.5 |
| Cantaloupe | 1/4 fruit | 1.3 |
| Apple or Orange Juice(optional) | 6 oz | 1.7 |
| Coffee (decaff or reg) with or without cream & sugar | 1 cup | 1.0 |
| Total Oxalate | 8.8 | |
| Mid-Morning Snack | ||
| Yogurt with Fruit | 1 cup | 1.0 |
| Total Oxalate | 1.0 | |
| Lunch | ||
| Whole Wheat Bread | 2 slices | 11.4 |
| Tuna Salad | 3 oz | 2.5 |
| Lettuce & Tomato | slices | 1.0 |
| Cheese (american, swiss) | 2 slices | 1.2 |
| Mayonnaise | 1 TBS | 0.0 |
| Grapes | 1/2 cup | 1.0 |
| Chicken Noodle Soup | 1 cup | 3.0 |
| Total | 20.1 | |
| Mid-Afternoon Snack | ||
| Popcorn (air-popped) | 1 1/2 cups | 6.75 |
| Total | 6.75 | |
| Dinner | ||
| Any fresh fish (haddock, cod etc) | 3 oz | 1.0 |
| White Rice with stir-fryed Vegetables (mushrooms, onions, broccoli, zucchini) | 1 cup | 8.4 |
| Salad (use low oxalate veg) | small | 2.0 |
| Salad Dressing (oil based) | 2 TBS | 0.2 |
| Dinner roll | 1 roll | 5.9 |
| Diet Lemonade | 1 cup | 0.7 |
| Total | 18.2 | |
| Snack (Dessert) | ||
| Crackers (Ritz, Wheat etc) | 5 crackers | 2.5 |
| Cheddar Cheese | 5 oz | 0.5 |
| Red or White Wine | 4 oz | 1.0 |
| Total | 4.0 | |
| Total Oxalate | 58.9 |
- Hodgkinson A, 1977. Oxalate content of foods and nutrition. Hodgkinson A., editor. (ed.) Oxalic acid in biology and medicine. Academic Press, London, UK, pp. 193-212.
- Oxalate consumption by lactobacilli: evaluation of oxalyl-CoA decarboxylase and formyl-CoA transferase activity in Lactobacillus acidophilus. Turroni S, Vitali B, Bendazzoli C, Candela M, Gotti R, Federici F, Pirovano F, Brigidi P. J Appl Microbiol. 2007 Nov; 103(5):1600-9. https://www.ncbi.nlm.nih.gov/pubmed/17953571/
- Oxalate intake and the risk for nephrolithiasis. Taylor EN, Curhan GC. J Am Soc Nephrol. 2007 Jul; 18(7):2198-204. http://jasn.asnjournals.org/content/18/7/2198.long
- Hodgkinson A. 1977. Oxalic acid in biology and medicine. Academic Press, London, United Kingdom.
- Purification and characterization of oxalyl-coenzyme A decarboxylase from Oxalobacter formigenes. Baetz AL, Allison MJ. J Bacteriol. 1989 May; 171(5):2605-8. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC209940/
- OXALATE: FROM THE ENVIRONMENT TO KIDNEY STONES. Arh Hig Rada Toksikol 2013;64:609-630. https://www.degruyter.com/downloadpdf/j/aiht.2013.64.issue-4/10004-1254-64-2013-2428/10004-1254-64-2013-2428.pdf
- Microbiota Diversification and Crash Induced by Dietary Oxalate in the Mammalian Herbivore Neotoma albigula. mSphere. 2017 Sep-Oct; 2(5): e00428-17. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5646245/
- Kullin BR, Reid SJ, Abratt VR. 2016. The use of probiotic bacteria to treat recurrent calcium oxalate kidney stone disease, p 63–75. In Lange D, Chew B (ed), The role of bacteria in urology. Springer, Cham, Switzerland.
- A randomised Phase I/II trial to evaluate the efficacy and safety of orally administered Oxalobacter formigenes to treat primary hyperoxaluria. Hoppe B, Niaudet P, Salomon R, Harambat J, Hulton SA, Van’t Hoff W, Moochhala SH, Deschênes G, Lindner E, Sjögren A, Cochat P. Pediatr Nephrol. 2017 May; 32(5):781-790. https://www.ncbi.nlm.nih.gov/pubmed/27924398/
- Calcium oxalate crystals (Weddellite) within the secretions of ductal carcinoma in situ–a rare phenomenon. Singh N, Theaker JM. J Clin Pathol. 1999 Feb; 52(2):145-6. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC501061/pdf/jclinpath00275-0065.pdf
- Glycolate and glyoxylate metabolism in HepG2 cells. Baker PR, Cramer SD, Kennedy M, Assimos DG, Holmes RP. Am J Physiol Cell Physiol. 2004 Nov; 287(5):C1359-65. http://ajpcell.physiology.org/content/287/5/C1359.long
- Hyperoxaluria. Oxalosis and Hyperoxaluria Foundation. http://ohf.org/overview/
- Khneizer G, Al-Taee A, Mallick MS, Bastani B. Chronic dietary oxalate nephropathy after intensive dietary weight loss regimen. Journal of Nephropathology. 2017;6(3):126-129. doi:10.15171/jnp.2017.21. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5607971/
- Nelson WK, Houghton SG, Milliner DS, Lieske JC, Sarr MG. Enteric hyperoxaluria, nephrolithiasis, and oxalate nephropathy: potentially serious and unappreciated complications of Roux-en-Y gastric bypass. Surg Obes Relat Dis. 2005;1(5):481–5. https://www.ncbi.nlm.nih.gov/pubmed/16925274
- Hassan I, Juncos LA, Milliner DS, Sarmiento JM, Sarr MG. Chronic renal failure secondary to oxalate nephropathy: a preventable complication after jejunoileal bypass. Mayo Clin Proc. 2001;76(7):758–60. https://www.ncbi.nlm.nih.gov/pubmed/11444411
- Hueppelshaeuser R, von Unruh GE, Habbig S, Beck BB, Buderus S, Hesse A. et al. Enteric hyperoxaluria, recurrent urolithiasis, and systemic oxalosis in patients with Crohn’s disease. Pediatr Nephrol. 2012;27(7):1103–9. doi: 10.1007/s00467-012-2126-8. https://www.ncbi.nlm.nih.gov/pubmed/22366809
- McDonald GB, Earnest DL, Admirand WH. Hyperoxaluria correlates with fat malabsorption in patients with sprue. Gut. 1977;18(7):561–6. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1411579/
- Humayun Y, Ball KC, Lewin JR, Lerant AA, Fulop T. Acute oxalate nephropathy associated with orlistat. J Nephropathol. 2016;5(2):79–83. doi: 10.15171/jnp.2016.14. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4844913/
- Brogren M, Savage GP. Bioavailability of soluble oxalate from spinach eaten with and without milk products. Asia Pac J Clin Nutr. 2003;12(2):219–24. https://www.ncbi.nlm.nih.gov/pubmed/12810415
- Contribution of dietary oxalate to urinary oxalate excretion. Holmes RP, Goodman HO, Assimos DG. Kidney Int. 2001 Jan; 59(1):270-6. http://www.kidney-international.theisn.org/article/S0085-2538(15)47462-9/fulltext
- Acute oxalate nephropathy due to ‘Averrhoa bilimbi’ fruit juice ingestion. Bakul G, Unni VN, Seethaleksmy NV, Mathew A, Rajesh R, Kurien G, Rajesh J, Jayaraj PM, Kishore DS, Jose PP. Indian J Nephrol. 2013 Jul; 23(4):297-300. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3741977/
- Holmes RP, Goodman HO, Assimos DG: Contribution of dietary oxalate to urinary oxalate excretion. Kidney Int 59 : 270 –276, 2001. http://www.kidney-international.theisn.org/article/S0085-2538(15)47462-9/fulltext
- Menon M, Mahle CJ: Oxalate metabolism and renal calculi. J Urol 127 : 148 –151, 1982. http://www.sciencedirect.com/science/article/pii/S0022534717536496
- Knight J, Jiang J, Assimos DG, Holmes RP: Hydroxyproline ingestion and urinary oxalate and glycolate excretion. Kidney Int 70 : 1929 –1934, 2006. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2268952/
- Traxer O, Huet B, Poindexter J, Pak CY, Pearle MS: Effect of ascorbic acid consumption on urinary stone risk factors. J Urol 170 : 397 –401, 2003. https://www.ncbi.nlm.nih.gov/pubmed/12853784
- Holmes, R.P., Goodman, H.O., and Assimos, D.G. Dietary oxalate and its intestinal absorption. Scanning Microsc. 1995; 9: 1109–1120. https://www.ncbi.nlm.nih.gov/pubmed/8819892
- Gambaro, G., Petrarulo, M., Nardelotto, A. et al. Erythrocyte transmembrane flux and renal clearance of oxalate in idiopathic calcium nephrolithiasis. Kidney Int. 1995; 48: 1549–1552. http://www.kidney-international.theisn.org/article/S0085-2538(15)59217-X/pdf
- Hesse, A., Schneeberger, W., Engfeld, S. et al. Intestinal hyperabsorption of oxalate in calcium oxalate stone formers: Application of a new test with [13C2]oxalate. J Am Soc Nephrol. 1999; 10: S329–S333. https://www.ncbi.nlm.nih.gov/pubmed/10541257
- Jonassen, J., Cooney, R., Kennington, L. et al. Oxalate-induced changes in the viability and growth of human renal epithelial cells. J Am Soc Nephrol. 1999; 10: S446–S451. https://www.ncbi.nlm.nih.gov/pubmed/10541281
- Calcium oxalate is associated with benign breast tissue. Can we avoid biopsy? Winston JS, Yeh IT, Evers K, Friedman AK. Am J Clin Pathol. 1993 Nov; 100(5):488-92. https://www.ncbi.nlm.nih.gov/pubmed/8249886/
- Liebman, M. and Chai, W. Effect of dietary calcium on urinary oxalate excretion after oxalate loads. Am J Clin Nutr. 1997; 65: 1453–1459. https://www.ncbi.nlm.nih.gov/pubmed/9129476
- Contribution of dietary oxalate to urinary oxalate excretion. Holmes, Ross P. et al. Kidney International , Volume 59 , Issue 1 , 270 – 276. http://www.kidney-international.theisn.org/article/S0085-2538(15)47462-9/fulltext
- Curhan GC, Willett WC, Rimm EB, Stampfer MJ: A prospective study of dietary calcium and other nutrients and the risk of symptomatic kidney stones. N Engl J Med 328 : 833 –838, 1993. http://www.nejm.org/doi/full/10.1056/NEJM199303253281203
- Curhan GC, Willett WC, Knight EL, Stampfer MJ: Dietary factors and the risk of incident kidney stones in younger women (Nurses’ Health Study II). Arch Intern Med 164 : 885 –891, 2004. https://www.ncbi.nlm.nih.gov/pubmed/15111375
- von Unruh GE, Voss S, Sauerbruch T, Hesse A: Dependence of oxalate absorption on the daily calcium intake. J Am Soc Nephrol 15 : 1567 –1573, 2004. http://jasn.asnjournals.org/content/15/6/1567.full
- Liebman M, Costa G: Effects of calcium and magnesium on urinary oxalate excretion after oxalate loads. J Urol 163 : 1565 –1569, 2000. https://www.ncbi.nlm.nih.gov/pubmed/10751889
- Zimmermann DJ, Voss S, von Unruh GE, Hesse A: Importance of magnesium in absorption and excretion of oxalate. Urol Int 74 : 262 –267, 2005. https://www.karger.com/Article/Abstract/83560
- Goodman, H.O., Holmes, R.P., and Assimos, D.G. Genetic factors in calcium oxalate stone disease. J Urol. 1995; 153: 301–307. http://www.jurology.com/article/S0022-5347(01)67739-5/fulltext
- Pak, C.Y.C., Skurla, C., and Harvey, J. Graphic display of urinary risk factors for renal stone formation. J Urol. 1985; 134: 867–870. http://www.sciencedirect.com/science/article/pii/S0022534717474969
- Oxalate nephropathy with a granulomatous lesion due to excessive intake of peanuts. Sasaki M, Murakami M, Matsuo K, Matsuo Y, Tanaka S, Ono T, Mori N. Clin Exp Nephrol. 2008 Aug; 12(4):305-8. https://www.ncbi.nlm.nih.gov/pubmed/18335167/
- Food oxalate: factors affecting measurement, biological variation, and bioavailability. Massey LK. J Am Diet Assoc. 2007 Jul; 107(7):1191-4; quiz 1195-6. https://www.ncbi.nlm.nih.gov/pubmed/17604750/
- Nephropathy in dietary hyperoxaluria: A potentially preventable acute or chronic kidney disease. Glew RH, Sun Y, Horowitz BL, Konstantinov KN, Barry M, Fair JR, Massie L, Tzamaloukas AH. World J Nephrol. 2014 Nov 6; 3(4):122-42. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4220346/
- Holmes R, Kennedy M: Estimation of the oxalate content of foods and daily oxalate intake. Kidney Int 57 : 1662 –1667, 2000. http://www.kidney-international.theisn.org/article/S0085-2538(15)46915-7/fulltext
- Oxalate Intake and the Risk for Nephrolithiasis. JASN July 2007 vol. 18 no. 7 2198-2204. 10.1681/ASN.2007020219. http://jasn.asnjournals.org/content/18/7/2198.long
- How To Eat A Low Oxalate Diet. University of Chicago Kidney Stone Evaluation and Treatment Program. https://kidneystones.uchicago.edu/how-to-eat-a-low-oxalate-diet/
- Oxalate files. Harvard T.H. Chan School of Public Health Nutrition Department’s File Download Site. https://regepi.bwh.harvard.edu/health/Oxalate/files