What is pulmonary hypertension
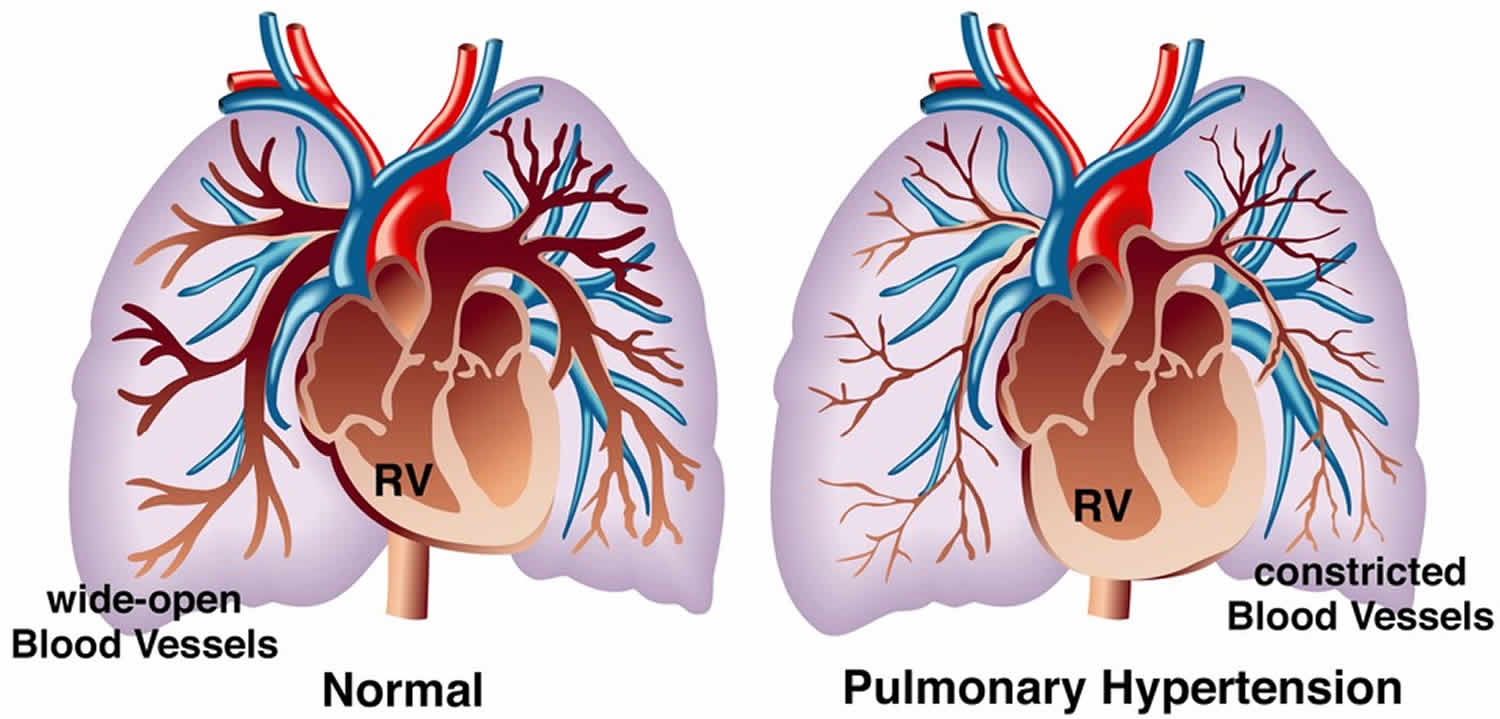
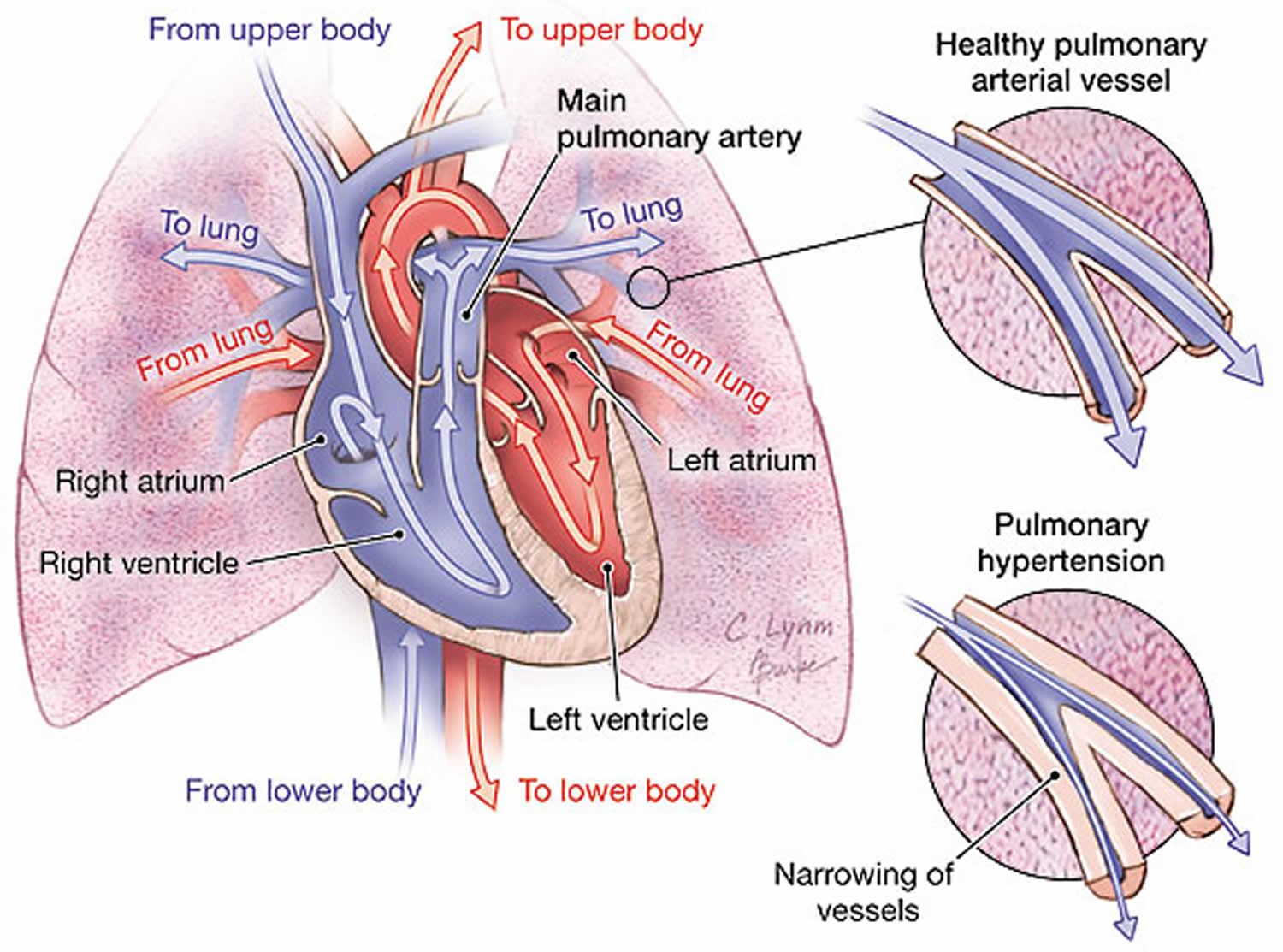
Pulmonary hypertension means high blood pressure in the blood vessels that supply your lungs (pulmonary arteries) (Figures 1 and 2). The pulmonary artery is the main blood vessel that carries blood from the heart to your lungs. For a person at rest, blood pressure in a normal pulmonary artery is between 8-20 millimeters of mercury (mm Hg). In an individual with pulmonary hypertension, resting mean pulmonary arterial blood pressure can be more than 25 mm Hg, with normal pulmonary capillary wedge pressure (less than 15mmHg) and increased pulmonary vascular resistance (above 3 Wood units (240 dyne/s/cm−5) at rest) 1. This increase in pulmonary artery pressure occurs when the small arteries of your lungs become abnormally narrow, thick and stiff, and can’t expand as well to allow blood through. The reduced blood flow makes it harder for the right-hand side of the heart to pump blood through the arteries. In pulmonary hypertension, the blood vessels specifically in the lungs are affected. They can become stiff, damaged or narrow, and the right side of the heart must work harder to pump blood through. If the right-hand side of your heart has to continually work harder, it can gradually become weaker. This can lead to heart failure. Pulmonary hypertension results in right ventricular pressure/volume overload leading to right ventricular heart failure and death 2.
Pulmonary hypertension is a rare serious condition that can affect people of all ages, but it’s more common in people who have another heart or lung condition. Pulmonary hypertension can be present even if you have normal “regular” (systemic) blood pressure because the blood vessels in the lung are very different from the blood vessels in the rest of the body.
Pulmonary hypertension in general quite common; it is diagnosed in more than 2% of all patients discharged from U.S. hospitals and in up to 9% of echocardiograms performed in a community setting 3.
The changes in the pulmonary arteries that lead to pulmonary hypertension can be caused by:
- Problems with the smaller branches of the pulmonary arteries (pulmonary arterial hypertension or PAH)
- Conditions that affect the left side of the heart
- Shortage of oxygen in the body (hypoxia) due to heart or lung disease (such as chronic obstructive pulmonary disease [COPD]) or high altitude
- Blood clots (pulmonary embolism) that cause narrowing or a blockage in the pulmonary arteries
- Autoimmune diseases that damage the lungs, such as scleroderma and rheumatoid arthritis
- Birth defects of the heart
- Portal hypertension (resulting from liver disease)
- Heart failure
- Heart valve disease
- HIV infection
- Drugs and toxins (such as appetite suppressants, cocaine, or amphetamines)
- Myeloproliferative disorders (overproduction of red blood cells or white blood cells)
- Hemoglobinopathies (abnormal oxygen-carrying proteins in red blood cells, such as found in sickle cell anemia)
- Obesity with obstructive sleep apnea
- Thyroid disorders
- Lung disease, such as COPD or pulmonary fibrosis or any other severe chronic lung condition
Not all pulmonary hypertension is the same. Pulmonary hypertension is a general term used to describe high blood pressure in the lungs from any cause. There are five different groups of pulmonary hypertension based on different causes. These groups are defined by the World Health Organization (WHO) and are referred to as pulmonary hypertension WHO Groups. The majority of pulmonary hypertension diagnoses relate to left heart disease or lung disease, with only a small fraction accounted for by pulmonary arterial hypertension (PAH) (WHO group 1) and chronic thromboembolic pulmonary hypertension (WHO group 4). Idiopathic pulmonary hypertension (WHO group 5) in particular is rare, with an estimated incidence of approximately 1 case per million and a prevalence of 7 cases per million 3. Because current disease-specific pulmonary hypertension medications are approved only for idiopathic pulmonary hypertension (WHO group 5) and other pulmonary arterial hypertension WHO group 1 conditions, it is critical for treating physicians to have a thorough understanding of the differential diagnosis and workup that is required for patients with suspected pulmonary hypertension.
In many pulmonary hypertension cases, no cause can be identified, and in these cases the disease is referred to as idiopathic pulmonary hypertension (IPAH). Sometimes pulmonary hypertension can develop due to another medical condition, including connective tissue disease, congenital heart disease, liver disease, HIV, and others. This type of pulmonary hypertension is known as associated pulmonary arterial hypertension (APAH). Some families have a form of pulmonary hypertension that can be inherited. This is known as heritable pulmonary arterial hypertension (HPAH). Chronic thromboembolic pulmonary hypertension (CTEPH) is a form of pulmonary hypertension caused by old blood clots in the lungs (pulmonary embolism).
If left untreated, pulmonary hypertension can lead to right heart failure and death. Pulmonary hypertension can’t be cured, but treatments can reduce your symptoms and help you manage your condition. Fortunately, because of major advancements made in the past two decades, therapies that target the pulmonary arteries (pulmonary hypertension-targeted therapies) are available to help relieve symptoms, improve quality of life and slow down the progression of the disease in patients with WHO Group 1 pulmonary arterial hypertension (PAH).
Patients with WHO Groups 2 and 3 pulmonary hypertension can benefit from treating the underlying left heart and lung diseases, respectively. Patients with WHO Group 4 pulmonary hypertension can benefit from either a surgery to remove the clots or a pulmonary hypertension-targeted therapy if they are unable to have the surgery or have pulmonary hypertension remaining after the surgery.
Treating pulmonary hypertension
Pulmonary hypertension can’t be cured, but treatment can reduce the symptoms and help you manage your condition.
Pulmonary hypertension usually gets worse over time. Left untreated, it may cause heart failure, which can be fatal, so it’s important treatment is started as soon as possible.
If another condition is causing pulmonary hypertension, the underlying condition should be treated first. This can sometimes prevent the pulmonary arteries being permanently damaged.
Treatments for pulmonary hypertension may include anticoagulant medicines to reduce the blood’s ability to thicken (clot) and diuretics to remove excess fluid as a result of heart failure.
You may also be offered medication to widen the blood vessels.
Home oxygen treatment may also be prescribed if the level of oxygen in your blood is low. DO NOT change how much oxygen is flowing without asking your doctor. Have a backup supply of oxygen at home or with you when you go out. Keep the phone number of your oxygen supplier with you at all times.
A number of FDA-approved medications are available for the treatment of pulmonary hypertension. These medications are administered in several ways: directly into the vein (intravenously), beneath the skin (subcutaneously), orally, and by inhalation.
- Some pulmonary hypertension medications work by mimicking prostaglandin, a substance that pulmonary hypertension patients tend to be deficient in. These treatments are called are prostacyclins, and include epoprostenol (Flolan™), treprostinil (Remodulin™ and Tyvaso™), and iloprost (Ventavis™).
- Other pulmonary hypertension medications work by reversing the effects of endothelin, a substance that pulmonary hypertension patients tend to have in excess. These are called endothelin receptor antagonists, and include bosentan (Tracleer™) and ambrisentan (Letairis®).
- Still other pulmonary hypertension treatments work by allowing the lungs to produce more of their own natural vasodilators. Called PDE 5 Inhibitors, this category of treatment includes sildenafil (Revatio™) and tadalafil (Adcirca™).
- Doctors may also prescribe the anticoagulant warfarin (Coumadin™) to prevent blood clots, diuretics to reduce fluid retention, and supplemental oxygen to help patients breathe.
Other important tips to follow:
- Avoid pregnancy
- Avoid heavy physical activities and lifting
- Avoid traveling to high altitudes
- Get a yearly flu vaccine, as well as other vaccines such as the pneumonia vaccine
- Stop smoking
The Lung Association recommends patients and caregivers join:
- The Living with Lung Disease Support Community to connect with others facing this disease: https://www.inspire.com/groups/american-lung-association-lung-disease
- Pulmonary Hypertension Association: https://phassociation.org/
- Pulmonary Hypertension Association UK: http://www.phauk.org/
Figure 1. Pulmonary hypertension
Pulmonary Arterial Hypertension
WHO Group 1 refers to pulmonary arterial hypertension (PAH), which is caused when the arteries in the lungs become narrowed, thickened or stiff. The right side of the heart must work harder to push blood through these narrowed arteries. This extra stress can cause the heart to lose its ability to pump enough blood through the lungs to meet the needs of the rest of the body.
There are several types of pulmonary arterial hypertension. Idiopathic pulmonary arterial hypertension is pulmonary arterial hypertension that occurs without a clear cause. Heritable pulmonary arterial hypertension is linked to genes that are inherited from family members. Pulmonary arterial hypertension can also develop in association with other medical conditions including congenital heart disease, liver disease, HIV and connective tissue diseases — such as scleroderma and lupus. Pulmonary arterial hypertension can even be associated with past or present drug use, such as the use of methamphetamine or certain diet pills. While there are treatment options for pulmonary arterial hypertension, there is no known cure.
Key facts
- Pulmonary arterial hypertension (PAH) is a specific type of pulmonary hypertension where the tiny blood vessels in the lungs become scarred.
- The symptoms of pulmonary arterial hypertension (PAH) are common to other diseases which makes it more difficult to diagnose.
- Pulmonary arterial hypertension (PAH) is a complex condition that will usually worsen without the right treatment.
How serious is pulmonary arterial hypertension?
Pulmonary arterial hypertension (PAH) is a very serious disease. It is not the same as other, more common forms of pulmonary hypertension, which are usually caused by other underlying diseases of the heart, lungs, or other organs. PAH is a rare condition, affecting about 15-50 people per million in the US. Since patients with PAH are often not diagnosed until their symptoms are severe, they may only have a few years to live unless they get proper treatment. Fortunately, advances in therapies have led to impressive improvements for patients with pulmonary arterial hypertension.
Pulmonary Hypertension Due to Left Heart Disease
WHO Group 2 includes pulmonary hypertension due to left heart disease. In this group of pulmonary hypertension, the arteries and lungs are not as thick or stiff as WHO Group 1, but there are problems with how the heart squeezes or relaxes, or problems with the valves on the left side of the heart. Because of this, the left heart is unable to keep up with the blood returning from the lungs — causing a “backup” of blood which raises pressure in the lungs. WHO Group 2 is the most common form of pulmonary hypertension.
Pulmonary Hypertension Due to Lung Disease
WHO Group 3 includes pulmonary hypertension due to chronic lung disease and/or hypoxia (low oxygen levels). These lung diseases include obstructive lung disease where the lung airways narrow and make it harder to exhale (e.g. COPD or emphysema); restrictive lung disease in which the lungs have a tough time expanding when one inhales (e.g. interstitial lung disease or pulmonary fibrosis); sleep apnea; and living in an area of high altitude for a long period of time. Arteries in the lungs tighten so that blood can only go to areas of the lungs that are receiving the most air and oxygen. This tightening leads to high blood pressure throughout the lungs.
Pulmonary Hypertension Due to Chronic Blood Clots in the Lungs
WHO Group 4 is called chronic thromboembolic pulmonary hypertension (CTEPH). Chronic thromboembolic pulmonary hypertension can occur when the body is not able to dissolve a blood clot in the lungs. This can lead to scar tissue in the blood vessels of the lungs, which blocks normal blood flow and makes the right side of the heart work harder. This type of pulmonary hypertension is unique because it can potentially be cured through pulmonary thromboendarterectomy (PTE) surgery to remove the blood clots. However, not all chronic thromboembolic pulmonary hypertension patients are eligible for this surgery. A drug is also available for chronic thromboembolic pulmonary hypertension patients if a doctor determines that a patient is not a candidate for the pulmonary thromboendarterectomy surgery or if pulmonary hypertension remains after the surgery.
Pulmonary Hypertension Due to Unknown Causes
WHO Group 5 is where pulmonary hypertension is secondary to other diseases in ways that are not well understood. These associated conditions include, but are not limited to, sarcoidosis, sickle cell anemia, chronic hemolytic anemia, splenectomy (spleen removal) and certain metabolic disorders.
Could pulmonary hypertension run in my family?
Yes, but heritable PAH (HPAH) is relatively uncommon. Of the small percentage of people who do carry the pulmonary hypertension gene, only a small number of carriers will develop the disease. Genetic testing is available to find out if you carry the pulmonary hypertension gene.
Pulmonary hypertension life expectancy
There’s no simple answer to this question. Every pulmonary hypertension patient is different, and new research with the potential to improve the outlook for this disease is being conducted all the time. Your journey with pulmonary hypertension depends on many factors, including the severity of your disease and how you respond to treatment. pulmonary hypertension-specific therapies are available that can prolong and improve your quality of life. Once in the care of a pulmonary hypertension specialist and on treatment, many pulmonary hypertension patients live for many years.
The outlook for pulmonary hypertension varies, depending on factors such as:
- what’s causing it
- how quickly it’s diagnosed
- how advanced your symptoms are
- whether you have another underlying health condition
The specialist in charge of your care will be able to give you more detailed information.
Having pulmonary hypertension can affect your ability to carry out everyday activities.
Pulmonary hypertension symptoms
The most common symptoms of pulmonary hypertension can also be caused by other more common medical problems, such as asthma, emphysema or chronic obstructive pulmonary disease [COPD]. Therefore, diagnosing pulmonary hypertension is difficult and requires a specialist. Physical examination signs can include visible or enlarged veins on the side of the neck, irregular heart sounds or swelling in the abdomen or legs and feet.
Symptoms are common across all types of pulmonary hypertension, however the numbers below are reported for pulmonary arterial hypertension.
Symptoms of pulmonary hypertension include 4:
- Shortness of breath 86%
- Fatigue 27%
- Chest pain (angina) 22%
- Swelling (oedema) in the legs, ankles, feet or tummy (abdomen) 21%
- Fainting or light-headedness 15%
- A racing heartbeat (palpitations) 13%
- Rarely, patients will cough up blood or have a change in their voice.
The symptoms often get worse during exercise, which can limit your ability to take part in physical activities.
If you have a type of pulmonary hypertension known as pulmonary arterial hypertension (PAH), you may not have any symptoms until the condition is quite advanced.
See your doctor if you have any symptoms of pulmonary hypertension. They’ll ask you about your symptoms and medical history, and they may carry out a physical examination.
Correctly diagnosing pulmonary hypertension can sometimes take time because its symptoms are similar to those of many other heart and lung conditions.
Tests you may have include a type of heart scan called an echocardiogram, and right heart catheterisation, where a thin, flexible tube is inserted into your pulmonary artery.
Pulmonary hypertension causes
Pulmonary hypertension is caused by changes to the pulmonary arteries, the blood vessels that carry blood from the heart to the lungs.
There are five main types of pulmonary hypertension, depending on the underlying cause. These are described below.
Pulmonary arterial hypertension
WHO Group 1 pulmonary arterial hypertension (PAH) is a specific type of pulmonary hypertension that is caused by the development of scar tissue in the tiny blood vessels of the lung. This scar tissue blocks the blood flow through the lungs and causes the pressure in those blood vessels to increase.
The walls of the arteries become thick and stiff, narrowing the space for blood to pass through and increasing pulmonary artery blood pressure.
If you have been diagnosed with pulmonary arterial hypertension (PAH), you should find a specialist who deals with this disease.
- DOCTORS WHO TREAT PULMONARY HYPERTENSION: https://phassociation.org/patients/doctorswhotreatph/
- The treatment for PAH is very complicated and depends on many factors (see treatment in the treatment section below).
How pulmonary arterial hypertension affects your body
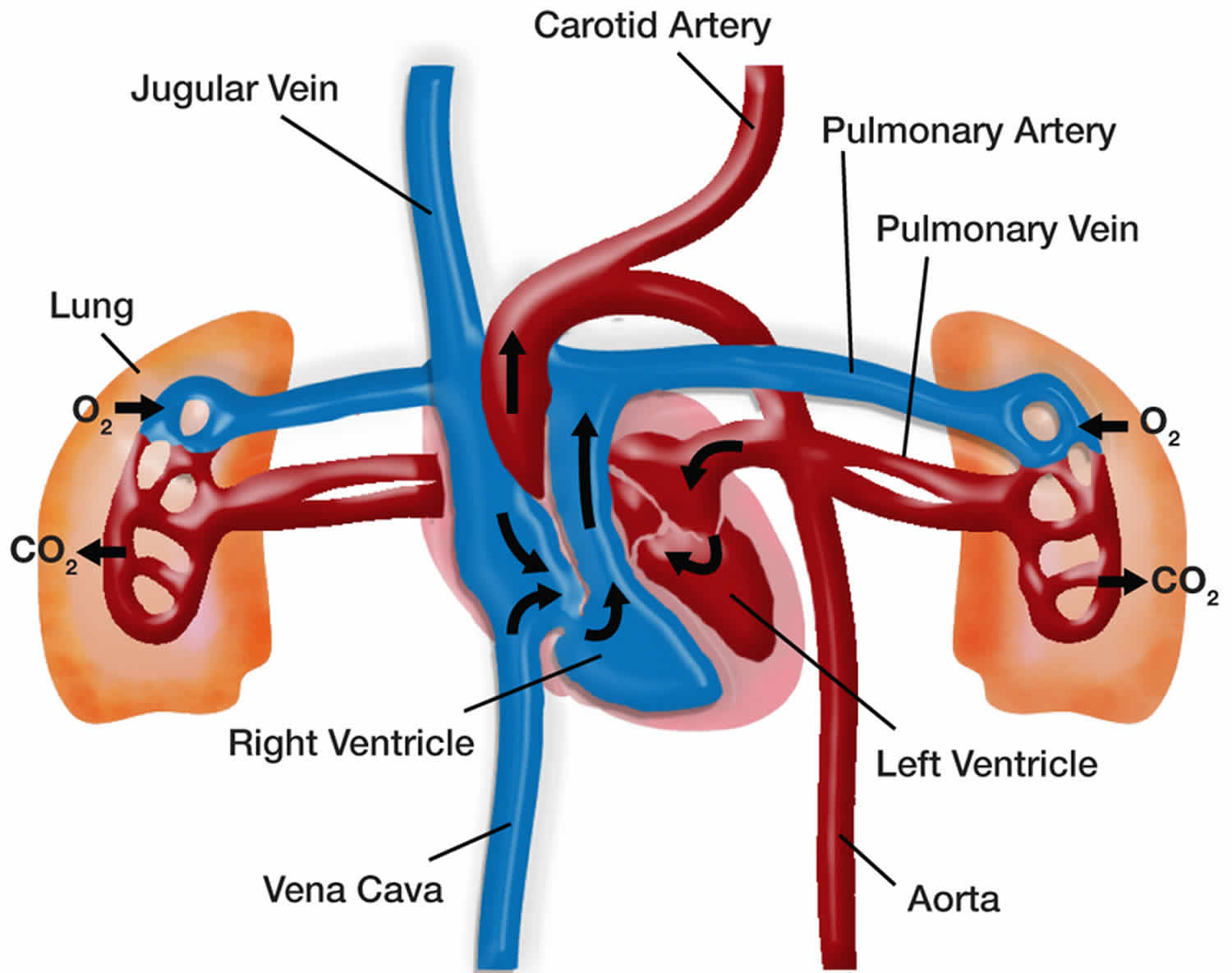
The heart and the lungs work together to deliver nourishing oxygen-rich blood throughout the body. The left side of the heart receives blood with high oxygen content from the lungs, and pumps it through the body via arteries. Oxygen is taken up by cells of the muscles and organs, and the low oxygen content blood is collected in the veins and returned to the right side of the heart. The right side of the heart pumps this blood back to the lungs where it picks up oxygen again.
Normally, the pressure in the right side of the heart and the blood vessels of the lungs is lower than in the rest of the body. This allows the blood to collect as much oxygen as possible while in the lungs. In someone with PAH, the scarred and narrowed blood vessels in the lungs make it harder for the blood to get through. This forces the right side of the heart to pump harder, under greater pressure. If this increased pressure is not treated, it can cause the right side of the heart to become overworked and possibly fail. This problem can also reduce the ability of the blood to collect enough oxygen to keep the body functioning normally.
What causes pulmonary arterial hypertension?
Pulmonary arterial hypertension (PAH) is characterized by progressive scarring of the tiny blood vessels going to the lungs. A number of diseases and conditions can cause this scarring including: connective tissue disorders like scleroderma and lupus; exposure to certain toxins and drugs, including methamphetamine and cocaine; infections, including HIV and schistosomiasis; cirrhosis of the liver; and congenital heart abnormalities. When the cause of pulmonary arterial hypertension (PAH) is unknown, it is called idiopathic pulmonary arterial hypertension (IPAH).
WHO Group 1 pulmonary arterial hypertension (PAH) can be associated with other conditions, including:
- Connective tissue diseases – such as scleroderma, a condition that causes thickened areas of skin and problems with blood vessels; sarcoidosis, or lupus
- Congenital heart problems – such as a hole in the heart
- PAH that’s inherited (passed from parents to children through genes).
- Portal hypertension – abnormally high blood pressure inside the liver, which causes veins to become swollen
- HIV infection
- Certain medications or drugs, such as street drugs and certain diet medicines
- Connective tissue diseases. (Connective tissue helps support all parts of your body, including your skin, eyes, and heart.)
- Thyroid gland disorder
- Glycogen storage disorders – glycogen is a carbohydrate that produces short-term energy
- Pulmonary veno-occlusive disease – a rare condition that causes high blood pressure in the lungs
- Pulmonary capillary hemangiomatosis – another rare condition where tiny blood vessels (capillaries) grow within the lungs, causing blockages
- Sickle cell anemia,
- Chronic hemolytic anemia,
- Schistosomiasis. This is an infection caused by a parasite. Schistosomiasis is one of the most common causes of PAH in many parts of the world.
- Splenectomy (spleen removal)
- Certain metabolic disorders
- Drugs and toxins (appetite suppressants, cocaine, amphetamines)
- Myeloproliferative disorders (overproduction of red or white blood cells)
A small number of people develop pulmonary arterial hypertension without having any other medical condition. This is called idiopathic pulmonary arterial hypertension (IPAH). In very rare cases, PAH can be inherited – this is known as heritable pulmonary arterial hypertension (HPAH).
What are risk factors for developing pulmonary arterial hypertension?
You are more likely to get pulmonary arterial hypertension (PAH) if you are a young female, since the idiopathic form of the disease occurs more often in women of childbearing age than in men. There is an inherited form of pulmonary arterial hypertension (PAH), so a family history of the disease may put you at increased risk. Patients with diseases like lupus, scleroderma, cirrhosis of the liver, and HIV infection can develop it as well. Methamphetamine and cocaine use increase the risk for developing this disease.
How pulmonary arterial hypertension is treated
The treatment of PAH has change rapidly over the last 15 years. PAH-specific medications come in pill, inhaled, and intravenous (IV)/subcutaneous forms. The medications are often used in a variety of combinations. The treatment of pulmonary arterial hypertension is very dependent on the patient, the severity of the symptoms, the test findings, and even the support that the patient has at home. In addition to specific drugs, patients with PAH are also often treated with anticoagulants (blood thinners) and supplemental oxygen either at night, as needed or continuously. There are also patients with PAH who would benefit from a specific program of pulmonary rehabilitation. All of these potential options should be discussed between the patient and the treating physician. If the disease continues to progress in spite of treatment, your doctor may talk to you about lung transplantation.
Persistent pulmonary hypertension of the newborn
In rare cases, newborn babies can have high pressure inside their blood vessels, which means their heart can’t pump enough oxygenated blood around their body. This is known as persistent pulmonary hypertension of the newborn (PPHN). Treatment in an intensive care unit may be needed if simple measures such as keeping the baby warm and giving oxygen don’t increase oxygen levels to normal.
Before a baby is born, they do not need to use their lungs to breathe, because they receive oxygen via the umbilical cord and placenta from their mother. In the womb, the lungs are filled with amniotic fluid, and the blood vessels (arteries and veins) which take blood from the heart to the lungs are constricted, or closed. This means that the pressure inside the blood vessels of the lungs is high – you will often hear doctors talk about ‘high pulmonary pressures’.
When a baby is born, they take a big breath or cry, and their lungs fill with air instead of fluid. When the lungs fill with air, the blood vessels which take blood from the heart to the lungs open up (dilate), and this means that oxygen can be carried from the lungs, back to the heart, and pumped to the brain and the rest of the body once the umbilical cord is cut. The pressure inside the lungs and the blood vessels is now low.
If there is a problem around the time of birth which interferes with this process, the blood vessels may not open up properly so the pressure inside them remains high. This is called persistent pulmonary hypertension of the newborn (PPHN). As a result of the blood vessels not opening up, blood cannot get into the lungs to pick up oxygen and then the body will not have enough oxygen for the brain and other organs, and this can make a baby unwell.
Who does persistent pulmonary hypertension of the newborn affect?
Persistent pulmonary hypertension of the newborn occurs in about two in every 1,000 births. It usually occurs in babies that are born at term (at nine months) but can occasionally occur in premature (born too early) babies as well.
What causes persistent pulmonary hypertension of the newborn?
Doctors do not always know the cause of persistent pulmonary hypertension of the newborn, but they do know that the following may be factors:
- Meconium aspiration: This is when a baby has passed faeces (poo) while still in the womb, and because the poo becomes mixed with the amniotic fluid (the fluid inside the womb), the baby can breathe it into their lungs.
Infection - Infections such as pneumonia (lung or chest infection) and bloodstream infections can make persistent pulmonary hypertension of the newborn more likely, and there may be an increased risk of these conditions if the waters broke a long time before the baby was delivered, or if there was a group B strep infection present.
- Congenital abnormalities of the heart and lungs: A small number of babies who get persistent pulmonary hypertension of the newborn will have it because they have been born with an abnormality of their heart or lungs such as a diaphragmatic hernia, or a blocked heart valve, or lungs that are smaller than they should be.
How do doctors diagnose persistent pulmonary hypertension of the newborn?
The main feature of persistent pulmonary hypertension of the newborn is that not enough oxygen is getting to the heart, brain and other organs. This causes babies to look blue or pale and to have difficulty in breathing. Doctors, nurses and midwives will use oxygen saturation monitoring to measure the amount of oxygen in the blood, expressed as a percentage.
Monitoring involves putting a small probe which looks like a sticky plaster around the baby’s hand or foot, then displaying a number on a screen. If this number is low (below 92 per cent), and does not come up to 100 per cent easily then doctors treat problems with breathing using oxygen or breathing machines, they may diagnose persistent pulmonary hypertension of the newborn.
In some hospitals, it may be possible to do an ultrasound of the baby’s heart called an echocardiogram, which can look to see if the blood vessels in the lungs are closed or constricted (pulmonary hypertension, sometimes called ‘high pulmonary pressures’) and also rule out any abnormality of the heart which may be causing the low oxygen levels.
It is likely that doctors will also do a chest X-ray to look at the baby’s lungs, and some blood tests to look for signs of infection.
How is persistent pulmonary hypertension of the newborn treated?
Initial treatment of persistent pulmonary hypertension of the newborn will consist of simple measures such as keeping the baby warm (but not too hot) and giving oxygen, usually through small prongs (short plastic tubes) in the nostrils, or in an incubator. Doctors will usually insert a cannula or drip into the baby’s hand or foot, and use this to give some antibiotics.
As a baby is not likely to feed well while they have persistent pulmonary hypertension of the newborn, they will receive fluids containing sugar for energy through a drip. If these simple measures do not bring the oxygen levels up easily, the baby is likely to need to be moved to a neonatal intensive care unit or NICU.
Treatment of persistent pulmonary hypertension of the newborn in the intensive care unit (PICU or NICU)
Ventilation (breathing machine)
It is likely that doctors will pass a breathing tube into the baby’s airway through their mouth or nose, which is connected to a breathing machine or ventilator. This will breathe for the baby while they are unwell. The machine reduces the amount of effort and energy needed to breathe, which in turn reduces the amount of oxygen that the baby needs and it also delivers the maximum possible amount of oxygen into the lungs. When the baby is connected to the breathing machine, doctors will give them some medicines to make them sleepy so that they do not feel any discomfort as well as some medicines to stop them from moving. As the breathing tube passes into their airway, the baby will not be able to cry or make noises while they are on the machine.
High Frequency Oscillation (oscillator)
This is another type of breathing machine that doctors use to help deliver oxygen into the lungs of babies with persistent pulmonary hypertension of the newborn. This machine pushes air in and out of the lungs very quickly, so it is very noisy.
Nitric oxide
This gas is a combination of nitrogen and oxygen which is given to a baby through the breathing machine, straight into the lungs. It works by opening up the closed blood vessels so that more blood flows into the lungs, and the high pressures are reduced.
Inotropes
These are medicines that are given directly into the bloodstream via a drip to help keep the baby’s blood pressure high, as this helps the heart to pump blood into the lungs.
Extra-corporeal membrane oxygenation (ECMO)
If doctors have tried all of the treatments described above, and the baby’s oxygen saturations are still low, they may consider a treatment called extra-corporeal membrane oxygenation (ECMO), which is like a heart bypass machine during heart surgery. It takes over the work of the heart and lungs, putting oxygen directly into a baby’s blood rather than relying on the lungs to add oxygen. For this treatment a baby will be moved to the Cardiac Intensive Care Unit.
Moving forward and discharge from intensive care
Once the baby’s oxygen saturation levels are normal, the doctors and nurses will start to reduce the amount of nitric oxide delivered though the breathing machine, until it is turned off altogether. They will then gradually reduce the amount of oxygen used, and the amount of breathing work being done by the ventilator. You may hear them referring to this as ‘weaning’. During this time the doctors will reduce the medicine that keeps the baby still and sleepy so that they will become more awake and aware of their surroundings.
At the same time, the doctors will gradually reduce the inotropes (medicines being given to raise blood pressure) and might consider stopping antibiotics if a full course has been given. At this time the nurses may use a feeding tube, passed into one of the baby’s nostrils and down the throat to the stomach, to start some milk feeds. These can be expressed breast milk or formula, depending on the parents’ preference.
Once the baby is doing most of the work of breathing themselves, with only a small amount of help from the breathing machine, doctors will try to take the baby off the breathing machine altogether. Once this has happened, it is likely that they will be ready to go back to their local hospital, where the baby will finish any antibiotics that are still needed, continue oxygen treatment until it is no longer needed, and help parents to establish feeding before they are discharged home.
What is the outlook for babies who have had persistent pulmonary hypertension of the newborn?
Persistent pulmonary hypertension of the newborn is a serious condition, and if a child has been moved to the intensive care unit, that is because the baby is doing very poorly. The mortality is thought to be under 10 per cent (fewer than 1 in 10 babies affected will die).
There are also some after-effects from the lack of oxygen to the brain during the illness, and up to a quarter of babies affected will have some impairment because of their illness as they grow older. This includes difficulties such as learning problems and deafness.
Pulmonary hypertension linked to left heart disease
WHO Group 2 includes pulmonary hypertension due to left heart disease. If there are problems with the left side of the heart, the right side has to work harder to pump blood through the lungs. This increases blood pressure in the pulmonary arteries.
Problems with the left side of the heart are thought to be the most common (68 percent) cause of pulmonary hypertension. These include mitral valve problems, left ventricle problems, aortic valve conditions or long-term high blood pressure.
Pulmonary hypertension linked with lung disease or lack of oxygen
WHO Group 3 pulmonary hypertension is linked with lung diseases or lack of oxygen (hypoxia), including:
- Chronic obstructive pulmonary disease (COPD) – a number of lung conditions that affect breathing
- Interstitial lung disease – a group of lung disorders that cause scarring of the lung tissue, which makes it difficult to get enough oxygen into your body
- Conditions that affect breathing while you’re in a deep sleep – such as obstructive sleep apnoea (OSA)
Low levels of oxygen in the blood make the pulmonary arteries narrow. This squeezes the blood into a smaller space, which increases blood pressure, causing pulmonary hypertension.
Pulmonary hypertension caused by blood clots
WHO Group 4 pulmonary hypertension is also called chronic thromboembolic pulmonary hypertension (CTEPH). Pulmonary hypertension can sometimes be caused by scars from previous blood clots that narrow or block the pulmonary arteries.
A blood clot that blocks one of the blood vessels that supply your lungs is called a pulmonary embolism.
Other causes of pulmonary hypertension
WHO Group 5 is where pulmonary hypertension is secondary to other diseases in ways that are not well understood. Other, less common, causes of pulmonary hypertension include:
- Sarcoidosis – a condition that causes inflammation of different organs, including the lungs and lymph nodes
- Histiocytosis X – a rare condition that causes scarring (granulomas) and air-filled cysts, mainly in the lungs
- Compression of the blood vessels in the lungs – for example, as the result of a tumor
- Blood disorders, such as polycythemia vera and essential thrombocythemia
- Systemic disorders, such as vasculitis. Systemic disorders involve many of the body’s organs.
- Metabolic disorders, such as thyroid disease and glycogen storage disease. (In glycogen storage disease, the body’s cells don’t use a form of glucose (sugar) properly.)
- Other conditions, such as tumors that press on the pulmonary arteries and kidney disease.
Pulmonary hypertension diagnosis
Pulmonary hypertension can be difficult to diagnose in a routine medical exam because the most common symptoms of pulmonary hypertension, such as breathlessness, fatigue and dizziness, are also associated with many other heart or lungs conditions. This means there can sometimes be a delay before a correct diagnosis is made.
See your doctor if you have symptoms of pulmonary hypertension, such as breathlessness and tiredness.
Initial assessment
If your doctor suspects that you have pulmonary hypertension, he or she will want to review your medical and family history, perform a physical exam and perform one or more diagnostic tests.
Your doctor will ask about:
- your symptoms and how they affect your life
- your family history – although rare, pulmonary arterial hypertension can run in families
- any medication you’re currently taking
- any other medical conditions you have
You may also have a physical examination where your doctor will listen to your heart and lungs, and check for any swelling in your legs or ankles.
Preliminary Tests
To determine if you have pulmonary hypertension and what type, your medical team will schedule specialized tests. If your medical team suspects pulmonary hypertension as a result of one or more of the following tests, they will go on to schedule a right-heart catheterization, which is required to confirm diagnosis.
Blood Tests
Blood tests check the oxygen levels in the blood, they observe liver and kidney function, and they identify whether the patient has collagen vascular disease, thyroid problems, signs of infection or HIV antibodies. One test, the brain natriuretic peptide, helps to assess the strain on the heart and may also be used to monitor response to treatment.
Chest X-Rays
Chest X-rays can reveal an enlarged right ventricle or pulmonary arteries. Chest X-rays can also show signs of emphysema or scarring (interstitial fibrosis) of the lungs.
Electrocardiogram (ECG)
An electrocardiogram checks the electrical impulses of the heart. Electrodes are attached to the patient’s skin, and a recording of these impulses is made. However, an ECG alone is not enough to indicate a pulmonary hypertension diagnosis. If your doctor performs an ECG, he or she will also perform one or more additional procedures to identify pulmonary hypertension.
Echocardiogram
In this procedure, electrodes are placed on the patient’s skin, and a sonogram (high-frequency sound waves to create an image of the heart) of the heart is taken. This painless procedure is often used to make a preliminary diagnosis by estimating the pressures in the right heart and assessing how well the heart is functioning. Other heart conditions that produce symptoms similar to pulmonary hypertension may be diagnosed with an echocardiogram. In addition, an echocardiogram may be used to monitor a patient’s condition.
Pulmonary Function Tests
These tests measure how much air your lungs can hold, how much air moves in and out of them and the lungs’ ability to exchange oxygen. These tests may be performed to potentially identify its cause.
Exercise Tolerance Test (Six-Minute Walk Test)
During this test, a patient will be asked to perform an exercise, most commonly a six-minute walk. The purpose is to identify the patient’s exercise tolerance level.
Nuclear Scan (Ventilation/Perfusion Scan or V/Q Scan)
This diagnostic tool tests for blood clots in the lungs by producing a picture of air and blood flow to the lungs. A small dose of radioactive material is breathed in and another small dose is injected via a blood vessel into the lungs. The doctor will review the images that are produced to evaluate the health of the lungs.
The Gold Standard for pulmonary hypertension Diagnosis
Right-Heart Catheterization
If the results of initial tests point to pulmonary hypertension, your doctor will schedule a right-heart catheterization (commonly referred to as a “right heart cath”). Right-heart catheterization is one of the most accurate and useful tests to get a definitive diagnosis for pulmonary hypertension. This is the only test that directly measures the pressure inside the pulmonary arteries, and it should be done in all patients at least once to confirm a patient’s diagnosis of pulmonary hypertension. During the test, doctors insert a thin, flexible tube (catheter) through a large vein in your neck, arm or groin. They then pass the catheter up into your pulmonary artery to confirm a diagnosis by accurately measuring the blood pressure in the right side of your heart and pulmonary arteries; it’s carried out in specialist national pulmonary hypertension centers.
Vasodilator Study (Acute Vasodilator Challenge)
This test is used for patients who have already been diagnosed with pulmonary hypertension to determine how much their pulmonary blood vessels can relax over a brief period of time. Its main purpose is to screen for patients who might respond favorably to calcium channel blockers, a form of medication. The test can also help determine the patient’s prognosis. With a right heart catheter in place, the patient is given drugs that relax the pulmonary arteries. The test drug is given to the patient in higher and higher doses, pausing at each dose to see how the patient reacts. Once a significant response occurs or the side effects become intolerable, the test is considered complete.
In patients with idiopathic and hereditary pulmonary arterial hypertension, acute vasodilator testing during right heart catheterization is strongly recommended based on current guidelines.
Classifying pulmonary hypertension
If you’re diagnosed with pulmonary hypertension, your condition will be classified depending on how severe your symptoms are. This is to help work out the best treatment for you.
It’s usually classified into four types:
- Class 1 has no limits. You can do regular physical activities, such as walking or climbing stairs. These activities don’t cause pulmonary hypertension symptoms, such as tiredness, shortness of breath, or chest pain.
- Class 2 has slight or mild limits. You’re comfortable while resting, but regular physical activity causes pulmonary hypertension symptoms.
- Class 3 has marked or noticeable limits. You’re comfortable while resting. However, walking even one or two blocks or climbing one flight of stairs can cause pulmonary hypertension symptoms.
- Class 4 has severe limits. You’re not able to do any physical activity without discomfort. You also may have pulmonary hypertension symptoms while at rest.
Exercise testing is used to find out the severity of pulmonary hypertension. This testing consists of either a 6-minute walk test or a cardiopulmonary exercise test.
A 6-minute walk test measures the distance you can quickly walk in 6 minutes. A cardiopulmonary exercise test measures how well your lungs and heart work while you exercise on a treadmill or bicycle.
During exercise testing, your doctor will rate your activity level. Your level is linked to the severity of your pulmonary hypertension.
Over time, you may need more exercise tests to find out how well your treatments are working. Each time testing is done, your doctor will compare your activity level with the previous one.
Pulmonary hypertension treatment
There is currently no cure for pulmonary hypertension, however, there are treatment options available and more are on the horizon. If the cause is identified and treated early, it may be possible to prevent permanent damage to your pulmonary arteries, the blood vessels that supply your lungs.
Your doctor will take into consideration the severity of your illness (referred to as your “functional class”) and the results of your cardiac catheterization to help determine which medication is right for you. As your symptoms and pressures change, your doctor may want to adjust the type and dosage of your medication accordingly.
Pulmonary hypertension treatments include conventional medical therapies and oral, inhaled, intravenous (into the vein) and subcutaneous (into the skin) options. Depending on the severity of pulmonary hypertension, heart or lung transplant may also be an option.
Remember that each patient is different. It is essential that you talk to your own doctor about what treatment options are best for you.
All Types of Pulmonary Hypertension
Several treatments may be used for all types of pulmonary hypertension. These treatments include:
- Diuretics, also called water pills. These medicines help reduce fluid buildup in your body, including swelling in your ankles and feet.
- Blood-thinning medicines. These medicines help prevent blood clots from forming or getting larger.
- Digoxin. This medicine helps the heart beat stronger and pump more blood. Digoxin sometimes is used to control the heart rate if abnormal heart rhythms, such as atrial fibrillation or atrial flutter, occur.
- Oxygen therapy. This treatment raises the level of oxygen in your blood.
- Physical activity. Regular activity may help improve your ability to be active. Talk with your doctor about a physical activity plan that’s safe for you.
Research is ongoing for better pulmonary hypertension treatments. These treatments offer hope for the future.
Treating underlying conditions
If pulmonary hypertension is caused by another condition, such as a heart or lung problem, treatments will focus on the underlying condition.
If pulmonary hypertension is caused by blood clots that block the pulmonary arteries, you may be offered anticoagulant medicines to prevent more clots forming. You may also be offered an operation known as a pulmonary endarterectomy.
If you have pulmonary arterial hypertension (PAH), you’ll be referred to a center that specializes in treating this form of the condition (https://phassociation.org/patients/doctorswhotreatph/).
Pulmonary hypertension medications
- Calcium Channel Blockers (CCB) – Help decrease blood pressure (Only appropriate for a small minority of patients demonstrating a favorable response to vasodilator testing at the time of heart catheterization.)
- Digoxin – Assists the pumping of the heart
- Diuretics – Rids excess fluid that puts pressure on the heart
- Oxygen – Inhaled by patients via a nasal cannula or face mask
- Warfarin (Coumadin®) – “Thins” blood and prevents it from clotting
Oral Treatment Options
Endothelin Receptor Antagonists (ERAs) help prevent blood vessels from narrowing.
- Ambrisentan (Letairis®)
- Bosentan (Tracleer®)
- Bosentan (Tracleer®) for Pediatric Use
- Macitentan (Opsumit®)
Phosphodiesterase Inhibitors (PDE 5 Inhibitors) allow the lungs to produce more of its own natural vasodilators.
- Sildenafil (Revatio™)
- Sildenafil (Revatio™) for Pediatric Use
- Tadalafil (Adcirca®)
Prostacyclin Analogue allows the blood vessels in the lungs relax
- Oral Treprostinil (Orenitram®)
Selective IP Receptor Agonist targets and activates a prostacyclin receptor helping the blood vessels in the lungs relax
- Selexipag (Uptravi®)
Soluble Guanylate Cyclase (sGC) Stimulators increase the interaction of sGC with another chemical (nitric oxide) to help the blood vessels in the lungs relax.
- Riociguat (Adempas®)
Inhaled Treatment Options
Inhaled Treatment Options, such as prostacyclins, relieve shortness of breath.
- Iloprost (Ventavis®)
- Inhaled Treprostinil (Tyvaso™)
Intravenous Treatment Options
Intravenous Treatment Options open up the blood vessels and help ease symptoms of pulmonary hypertension, including chest pain and shortness of breath.
- Intravenous Treprostinil (Remodulin®)
- Epoprostenol (Flolan®)
- Room Temperature Stable Epoprostenol (Veletri®)
Subcutaneous Treatment Options
Subcutaneous Treatment Options are delivered through a portable infusion pump to open up the blood vessels and ease the symptoms of pulmonary hypertension.
- Subcutaneous Treprostinil
Surgery
Many people with pulmonary hypertension are treated with both conventional and targeted therapies, although this can be different for different people. Some people with pulmonary hypertension may need surgery. How your pulmonary hypertension is treated will depend on a number of things, for example how severe your pulmonary hypertension is, what type of pulmonary hypertension you have, etc.
Some people with pulmonary hypertension may need surgery. The three types of surgery currently used are:
- Pulmonary endarterectomy – an operation to remove old blood clots from the pulmonary arteries in the lungs in people with chronic thromboembolic pulmonary hypertension
- Balloon pulmonary angioplasty – a new procedure where a tiny balloon is guided into the arteries and inflated for a few seconds to push the blockage aside and restore blood flow to the lung; it may be considered if pulmonary endarterectomy isn’t suitable, and has been shown to lower blood pressure in the lung arteries, improve breathing, and increase the ability to exercise
- Atrial septostomy – a small hole is made in the wall between the left and right atria of the heart using a cardiac catheter, a thin, flexible tube inserted into the heart’s chambers or blood vessels; it reduces the pressure in the right side of the heart, so the heart can pump more efficiently and the blood flow to the lungs can be improved
- Transplant – in severe cases, a lung transplant or a heart-lung transplant may be needed; this type of surgery is rarely used because effective medication is available
Lung or heart-lung transplant
Lung or heart-lung transplant is a treatment option reserved for patients who are not improving on medical therapies. While transplantation can prolong survival, improve quality of life and offers a potential cure for pulmonary hypertension, it also carries risk of significant complications and many factors need to be considered before going forward.
Deciding whether transplant is right for you is a process that will involve your team of medical professionals. Most candidates experience a significant waiting time between becoming listed and receiving a transplant since there are more transplant candidates than there are donor organs.
Treatments for pulmonary arterial hypertension
There are many treatments for pulmonary arterial hypertension (PAH). Which treatment or combination of treatments you’ll be offered will depend on a number of factors, including what’s causing PAH and the severity of your symptoms.
Treatments include:
- anticoagulant medicines – such as warfarin to help prevent blood clots
- diuretics (water tablets) – to remove excess fluid from the body caused by heart failure
- oxygen treatment – this involves inhaling air that contains a higher concentration of oxygen than normal
- digoxin – derived from the foxglove plant, digoxin can improve your symptoms by strengthening your heart muscle contractions and slowing down your heart rate
There are also a number of specialist treatments for PAH that help relax the arteries in the lungs and reduce the blood pressure in the lungs.
These medicines slow the progression of PAH, and may even reverse some of the damage to the heart and lungs.
Treatments include:
- endothelin receptor antagonists – such as bosentan, ambrisentan and macitentan
- phosphodiesterase 5 inhibitors – sildenafil and tadalafil
- prostaglandins – epoprostenol, iloprost and treprostinil
- soluble guanylate cyclase stimulators – such as riociguat
- calcium channel blockers – nifedipine, diltiazem, nicardipine and amlodipine
Living with pulmonary arterial hypertension
The therapies that exist for this disease range from pills that can be taken between one to three times a day to medications that have to be given continuously through an IV line using a pump that is similar to an insulin pump used by diabetic patients. How well a patient responds to medicine is somewhat unpredictable and depends on how advanced the disease is at diagnosis as well as the underlying cause. Patients without treatment usually quickly progress to death over the course of months to years. However, with treatment, survival has improved significantly.
Typically patients will be seen in the doctor’s office at least every 3-4 months at first. In many centers, there will be regular testing such as echocardiograms and 6 minute walk testing. Some centers will obtain yearly right heart catheterizations to assess the impact of therapies on pulmonary pressures and heart function.
Special considerations for patients with PAH need to be made. For example, pregnancy should be avoided at all costs as it represents significant risk to the female patient with PAH and to the fetus. Also, many of the medications used to treat PAH may harm the fetus as it develops. Because PAH is a rare and complex disease, good care for a patient with PAH involves a close relationship with an expert in PAH and support from family and friends.
To best manage your PAH you should:
- Take your medication exactly as directed.
- Do not stop a medication without consulting with your doctor.
- Take care to never run out of medication.
- Avoid things that can put strain on the lungs and heart. This would include lifestyle choices such as smoking and the use of recreational drugs such as cocaine and amphetamines. There are also potential risks of worsening PAH during the course of normal pregnancy. These issues should be discussed between you and your doctor.
- Since PAH can lead to a form of heart failure, adhere to a low salt diet and limit fluid intake.
- Monitor your weight to recognize fluid retention. If your weight goes up, it is often helpful to let your physician or healthcare provider know, as an adjustment of medications may be needed.
- Develop strategies to help cope with fatigue and shortness of breath.
- Develop a careful exercise program with your healthcare providers.
- Get immunized against flu and pneumonia.
- Talk to your doctor about anxiety and depression, which are common in patients with PAH.
The Lung Association recommends patients and caregivers join:
- The Living with Lung Disease Support Community to connect with others facing this disease: https://www.inspire.com/groups/american-lung-association-lung-disease
- Pulmonary Hypertension Association: https://phassociation.org/
- Pulmonary Hypertension Association UK: http://www.phauk.org/
Group 2 Pulmonary Hypertension Due to Left Heart Disease
Conditions that affect the left side of the heart, such as mitral valve disease, can cause group 2 pulmonary hypertension. Treating the underlying condition will help treat pulmonary hypertension. Treatments may include lifestyle changes, medicines, and surgery.
Group 3 Pulmonary Hypertension Due to Lung Disease
Lung diseases, such as COPD (chronic obstructive pulmonary disease) and interstitial lung disease, can cause group 3 pulmonary hypertension. Certain sleep disorders, such as sleep apnea, also can cause group 3 pulmonary hypertension.
If you have this type of pulmonary hypertension, you may need oxygen therapy. This treatment raises the level of oxygen in your blood. You’ll likely get the oxygen through soft, plastic prongs that fit into your nose. Oxygen therapy can be done at home or in a hospital.
Your doctor also may recommend other treatments if you have an underlying lung disease.
Group 4 Pulmonary Hypertension Due to Chronic Blood Clots in the Lungs
Blood clots in the lungs or blood clotting disorders can cause group 4 pulmonary hypertension. If you have this type of pulmonary hypertension, your doctor will likely prescribe blood-thinning medicines. These medicines prevent clots from forming or getting larger.
Sometimes doctors use surgery to remove scarring in the pulmonary arteries due to old blood clots.
Group 5 Pulmonary Hypertension Due to Unknown Causes
Various diseases and conditions, such as thyroid disease and sarcoidosis, can cause group 5 pulmonary hypertension. An object, such as a tumor, pressing on the pulmonary arteries also can cause group 5 pulmonary hypertension.
Group 5 pulmonary hypertension is treated by treating its cause.
Living with pulmonary hypertension
Pulmonary hypertension has no cure. However, you can work with your doctor to manage your symptoms and slow the progress of the disease.
Ongoing Care
Follow your treatment plan as your doctor advises. Call your doctor if your pulmonary hypertension symptoms worsen or change. The earlier symptoms are addressed, the easier it is to treat them.
Some symptoms, such as chest pain, may require emergency treatment. Ask your doctor when you should call him or her or seek emergency care.
Also, talk with your doctor before taking any over-the-counter medicines. Some medicines can make your pulmonary hypertension worse or interfere with the medicines you’re taking for pulmonary hypertension. Ask your doctor whether you should get a pneumonia vaccine and a yearly flu shot.
You may have a complex schedule for taking medicines. Call your doctor or nurse if you’re having problems with this schedule. Knowing the names of your medicines and how they work is helpful. Keep a list of your medicines with you. Don’t stop or change medicines unless you talk with your doctor first.
Pay careful attention to your weight. You may want to keep a daily record of your weight. You should weigh yourself at the same time each day. If you notice a rapid weight gain (2 or more pounds in 1 day or 5 or more pounds in 1 week), call your doctor. This may be a sign that your pulmonary hypertension is worsening.
Pregnancy is risky for women who have pulmonary hypertension. Consider using birth control if there is a chance you may become pregnant. Ask your doctor which birth control methods are safe for you.
Lifestyle Changes
Making lifestyle changes can help you manage your symptoms. These changes will depend on the type of pulmonary hypertension you have. Talk with your doctor about which lifestyle changes can help you.
Quit Smoking
If you smoke, quit. Smoking makes pulmonary hypertension symptoms worse. Ask your doctor about programs and products that can help you quit. Also, avoid exposure to secondhand smoke.
Follow a Healthy Diet
Following a healthy diet and maintaining a healthy weight are part of a healthy lifestyle. A healthy diet includes a variety of fruits, vegetables, and whole grains. It also includes lean meats, poultry, fish, and fat-free or low-fat milk or milk products. A healthy diet also is low in saturated fat, trans fat, cholesterol, sodium (salt), and added sugar.
Talk with your doctor about whether you need to limit the amount of salt and fluids in your diet. Ask him or her whether you also need to regulate foods that contain vitamin K. These foods can affect how well blood-thinning medicines work. Vitamin K is found in green leafy vegetables and some oils, such as canola and soybean oil.
Be Physically Active
Physical activity is an important part of a healthy lifestyle. Try to do physical activity, such as walking, regularly. This will keep your muscles strong and help you stay active. Ask your doctor how much activity is safe for you. Your doctor may tell you to limit or avoid certain activities, such as:
- Those that cause straining, such as lifting heavy objects or weights.
- Sitting in a hot tub or sauna or taking long baths. These activities can lower your blood pressure too much.
- Flying in an airplane or traveling to high-altitude areas. Your doctor may ask you to use extra oxygen during air travel.
Avoid activities that cause breathing problems, dizziness, or chest pain. If you have any of these symptoms, seek care right away.
Emotional Issues and Support
Living with pulmonary hypertension may cause fear, anxiety, depression, and stress. You may worry about your medical condition, treatment, finances, and other issues.
Talk about how you feel with your health care team. Talking to a professional counselor also can help. If you’re very depressed, your doctor may recommend medicines or other treatments that can improve your quality of life.
Joining a patient support group may help you adjust to living with pulmonary hypertension. You can see how other people who have the same symptoms have coped with them. Talk with your doctor about local support groups or check with an area medical center.
Support from family and friends also can help relieve stress and anxiety. Let your loved ones know how you feel and what they can do to help you.
The Lung Association recommends patients and caregivers join:
- The Living with Lung Disease Support Community to connect with others facing this disease: https://www.inspire.com/groups/american-lung-association-lung-disease
- Pulmonary Hypertension Association: https://phassociation.org/
- Pulmonary Hypertension Association UK: http://www.phauk.org/
- Chapter 57 – Pulmonary Hypertension in Non-Pulmonary Arterial Hypertension Patients. Vascular Medicine: A Companion to Braunwald’s Heart Disease (Second Edition) 2013, Pages 687-696. https://doi.org/10.1016/B978-1-4377-2930-6.00057-4
- Right ventricular function and failure: report of a National Heart, Lung, and Blood Institute working group on cellular and molecular mechanisms of right heart failure. Voelkel NF, Quaife RA, Leinwand LA, Barst RJ, McGoon MD, Meldrum DR, Dupuis J, Long CS, Rubin LJ, Smart FW, Suzuki YJ, Gladwin M, Denholm EM, Gail DB, National Heart, Lung, and Blood Institute Working Group on Cellular and Molecular Mechanisms of Right Heart Failure. Circulation. 2006 Oct 24; 114(17):1883-91.
- 58 – Pulmonary Hypertension. Murray and Nadel’s Textbook of Respiratory Medicine (Sixth Edition) Volume 2, 2016, Pages 1031-1049.e4 https://doi.org/10.1016/B978-1-4557-3383-5.00058-0
- Brown LM, Chen H, Halpern S, et al. Delay in Recognition of Pulmonary Arterial Hypertension: Factors Identified From the REVEAL Registry. Chest. 2011;140(1):19-26. doi:10.1378/chest.10-1166. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3198486/